“Spazio Huntington”: Tracing the Early Motor, Cognitive and Behavioral Profiles of Kids with Proven Pediatric Huntington Disease and Expanded Mutations > 80 CAG Repeats
Abstract
:1. Introduction
2. Materials and Methods
3. Results
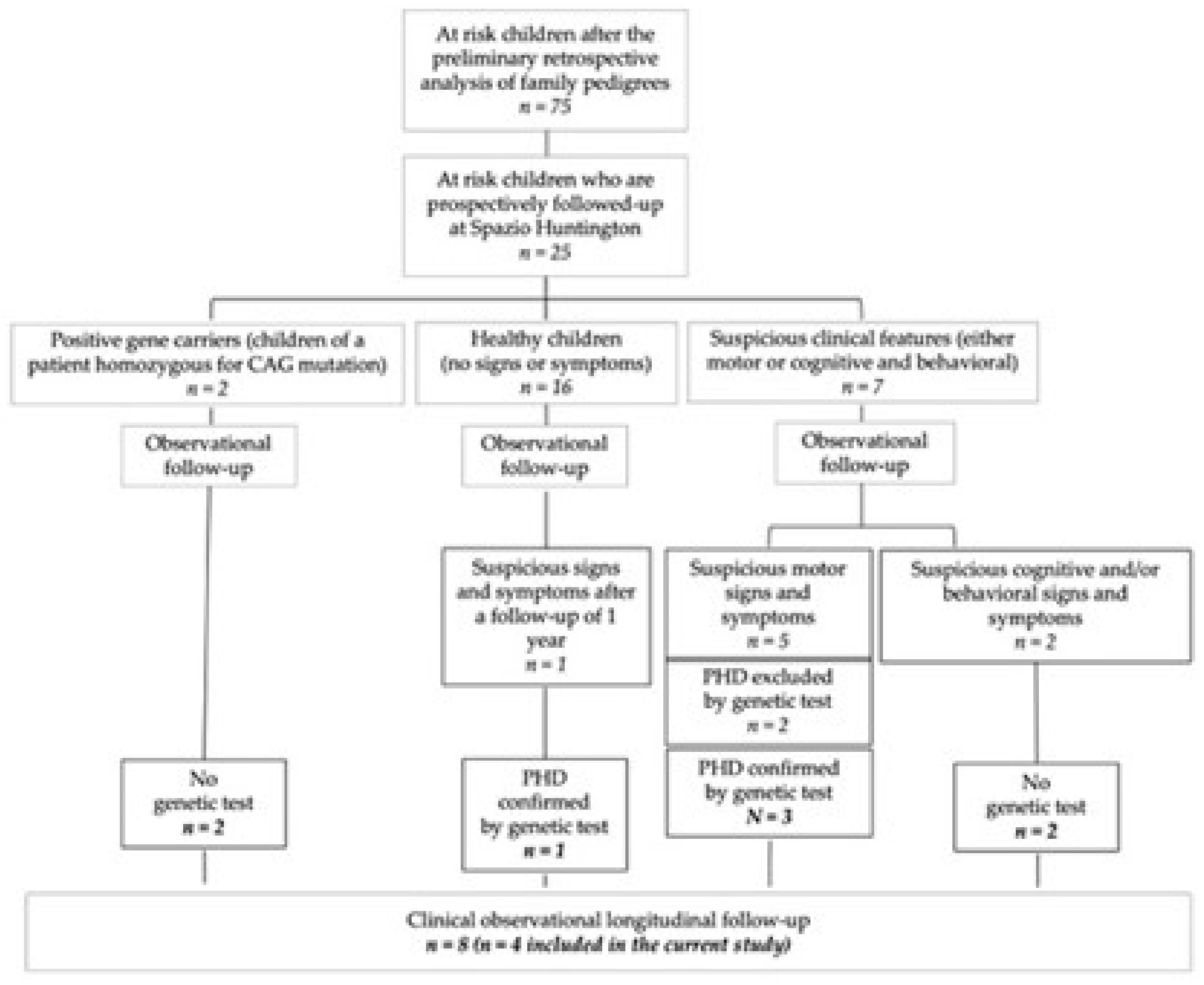
3.1. Clinical Overview
3.2. Longitudinal Clinical History
3.2.1. Case 1
3.2.2. Case 2
3.2.3. Case 3
3.2.4. Case 4
4. Discussion
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- MacDonald, M.E.; Ambrose, C.M.; Duyao, M.P.; Myers, R.H.; Lin, C.; Srinidhi, L.; Barnes, G.; Taylor, S.A.; James, M.; Groot, N.; et al. The Huntington’s Disease Collaborative Research Group: A novel gene containing a trinucleotide repeat that is expanded and unstable on Huntington’s disease chromosomes. Cell 1993, 72, 971–983. [Google Scholar] [CrossRef]
- Quarrell, O.W.J.; Brewer, H.M.; Squitieri, F.; Barker, R.A.; Nance, M.A.; Landwehrmeyer, G.B. (Eds.) Juvenile Huntington’s Disease; Oxford University Press: Oxford, UK, 2009. [Google Scholar]
- Squitieri, F. ‘Fifty shades of grey’ in the Huntington disease gene. Nat. Rev. Neurol. 2013, 9, 421–422. [Google Scholar] [CrossRef]
- Ghosh, R.; Tabrizi, S.J. Clinical Features of Huntington’s Disease. In Polyglutamine Disorders; Nóbrega, C., Pereira de Almeida, L., Eds.; Springer: Cham, Switzerland, 2018; Volume 1049. [Google Scholar] [CrossRef]
- Squitieri, F.; Berardelli, A.; Nargi, E.; Castellotti, B.; Mariotti, C.; Cannella, M.; Lavitrano, M.L.; De Grazia, U.; Gellera, C.; Ruggieri, S. Atypical movement disorders in the early stages of Huntington’s disease: Clinical and genetic analysis. Clin. Genet. 2000, 58, 50–56. [Google Scholar] [CrossRef] [PubMed]
- Quarrell, O.; O’Donovan, K.L.; Bandmann, O.; Strong, M. The Prevalence of Juvenile Huntington’s Disease: A Review of the Literature and Meta-Analysis. PLoS Curr. 2012, 4. [Google Scholar] [CrossRef]
- Quarrell, O.W.J.; Nance, M.A.; Nopoulos, P.; Reilmann, R.; Oosterloo, M.; Tabrizi, S.J.; Furby, H.; Saft, C.; Roos, R.A.C.; Squitieri, F.; et al. Defining pediatric huntington disease: Time to abandon the term Juvenile Huntington Disease? Mov. Disord. 2019, 34, 584–585. [Google Scholar] [CrossRef]
- Fusilli, C.; Migliore, S.; Mazza, T.; Consoli, F.; De Luca, A.; Barbagallo, G.; Ciammola, A.; Gatto, E.M.; Cesarini, M.; Etcheverry, J.L.; et al. Biological and clinical manifestations of juvenile Huntington’s disease: A retrospective analysis. Lancet Neurol. 2018, 17, 986–993. [Google Scholar] [CrossRef]
- Gonzalez-Alegre, P.; Afifi, A.K. Clinical Characteristics of Childhood-Onset (Juvenile) Huntington Disease: Report of 12 Patients and Review of the Literature. J. Child Neurol. 2006, 21, 223–229. [Google Scholar] [CrossRef]
- Gencik, M.; Hammans, C.; Strehl, H.; Wagner, N.; Epplen, J.T. Chorea Huntington: A Rare Case with Childhood Onset. Neuropediatrics 2002, 33, 90–92. [Google Scholar] [CrossRef] [PubMed]
- Cannella, M.; Gellera, C.; Maglione, V.; Giallonardo, P.; Cislaghi, G.; Muglia, M.; Quattrone, A.; Pierelli, F.; Di Donato, S.; Squitieri, F. The gender effect in juvenile Huntington disease patients of Italian origin. Am. J. Med. Genet. 2003, 125B, 92–98. [Google Scholar] [CrossRef]
- Nicolas, G.; Devys, D.; Goldenberg, A.; Maltête, D.; Hervé, C.; Hannequin, D.; Guyant-Maréchal, L. Juvenile Huntington disease in an 18-month-old boy revealed by global developmental delay and reduced cerebellar volume. Am. J. Med. Genet. Part A 2011, 155, 815–818. [Google Scholar] [CrossRef] [PubMed]
- Gómez-Tortosa, E.; Del Barrio, A.; Ruiz, P.J.G.; Pernaute, R.S.; Benítez, J.; Barroso, A.; Jiménez, F.J.; Yébenes, J.G. Severity of Cognitive Impairment in Juvenile and Late-Onset Huntington Disease. Arch. Neurol. 1998, 55, 835–843. [Google Scholar] [CrossRef] [Green Version]
- Moser, A.D.; Epping, E.; Espe-Pfeifer, P.; Martin, E.; Zhorne, L.; Mathews, K.; Nance, M.; Hudgell, D.; Quarrell, O.; Nopoulos, P. A survey-based study identifies common but unrecognized symptoms in a large series of juvenile Huntington’s disease. Neurodegener. Dis. Manag. 2017, 7, 307–315. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Degenkolb, T.; Vilcinskas, A. Metabolites from nematophagous fungi and nematicidal natural products from fungi as an alternative for biological control. Part I: Metabolites from nematophagous ascomycetes. Appl. Microbiol. Biotechnol. 2016, 100, 3799–3812. [Google Scholar] [CrossRef] [PubMed]
- Ribaï, P.; Nguyen, K.; Hahn-Barma, V.; Gourfinkel-An, I.; Vidailhet, M.; Legout, A.; Dodé, C.; Brice, A.; Dürr, A. Psychiatric and Cognitive Difficulties as Indicators of Juvenile Huntington Disease Onset in 29 Patients. Arch. Neurol. 2007, 64, 813–819. [Google Scholar] [CrossRef] [Green Version]
- Bakels, H.S.; Roos, R.A.; Roon-Mom, W.M.; Bot, S.T. Juvenile-Onset Huntington Disease Pathophysiology and Neurodevelopment: A Review. Mov. Disord. 2021. [Google Scholar] [CrossRef] [PubMed]
- Squitieri, F.; Griguoli, A.; Capelli, G.; Porcellini, A.; D’Alessio, B. Epidemiology of Huntington disease: First post-HTTgene analysis of prevalence in Italy. Clin. Genet. 2015, 89, 367–370. [Google Scholar] [CrossRef] [PubMed]
- Anderson, J.; Hayeems, R.; Shuman, C.; Szego, M.; Monfared, N.; Bowdin, S.; Shaul, R.Z.; Meyn, M.S. Predictive genetic testing for adult-onset disorders in minors: A critical analysis of the arguments for and against the 2013 ACMG guidelines. Clin. Genet. 2014, 87, 301–310. [Google Scholar] [CrossRef] [PubMed]
- Unified Huntington’s disease rating scale: Reliability and consistency. Mov. Disord. 1996, 11, 136–142. [CrossRef] [PubMed]
- Migliore, S.; Jankovic, J.; Squitieri, F. Genetic Counseling in Huntington’s Disease: Potential New Challenges on Horizon? Front. Neurol. 2019, 10, 453. [Google Scholar] [CrossRef]
- Cornoldi, C.; Giofrè, D.; Belacchi, C. Procedure Di Somministrazione e Scoring Dei Subtest. In Leiter-3 Leiter International Scale, 3rd ed.; Di Roid, G.H., Miller, L.J., Pomplun, M., Koch, C., Eds.; Giunti O.S. Organizzazioni Speciali: Firenze, Italy, 2016; pp. 23–85. [Google Scholar]
- Harrison, P.L.; Oakland, T. Adaptive Behavior Assessment System Manual, 3rd ed.; Western Psychological Services: Torrance, CA, USA, 2015. [Google Scholar]
- Stella, G.; Pizzioli, C.; Tressoldi, P.E. Peabody-Test di Vocabolario Recettivo. In Adattamento Italiano e Standardizzazione; Omega Edizioni: Torino, Italy, 2000. [Google Scholar]
- Achenbach, T.M.; Rescorla, L.A. Manual for the ASEBA School-Age Forms & Profiles; University of Vermont, Research Center for Children, Youth, & Families: Burlington, VT, USA, 2001. [Google Scholar]
- Kaufman, J.; Birmaher, B.; Brent, D.; Rao, U.; Flynn, C.; Moreci, P.; Williamson, D.; Ryan, N. Schedule for Affective Disorders and Schizophrenia for School-Age Children-Present and Lifetime Version (K-SADS-PL): Initial Reliability and Validity Data. J. Am. Acad. Child Adolesc. Psychiatry 1997, 36, 980–988. [Google Scholar] [CrossRef]
- Scahill, L.; Riddle, M.A.; McSwiggin-Hardin, M.; Ort, S.I.; King, R.A.; Goodman, W.K.; Cicchetti, D.; Leckman, J.F. Children’s Yale-Brown Obsessive Compulsive Scale: Reliability and Validity. J. Am. Acad. Child Adolesc. Psychiatry 1997, 36, 844–852. [Google Scholar] [CrossRef]
- De Luca, A.; Morella, A.; Consoli, F.; Fanelli, S.; Thibert, J.; Statt, S.; Latham, G.; Squitieri, F. A Novel Triplet-Primed PCR Assay to Detect the Full Range of Trinucleotide CAG Repeats in the Huntingtin Gene (HTT). Int. J. Mol. Sci. 2021, 22, 1689. [Google Scholar] [CrossRef]
- Squitieri, F.; Mazza, T.; Maffi, S.; De Luca, A.; AlSalmi, Q.; AlHarasi, S.; Collins, J.A.; Kay, C.; Baine-Savanhu, F.; Landwhermeyer, B.G.; et al. Tracing the mutated HTT and haplotype of the African ancestor who spread Huntington disease into the Middle East. Genet. Med. 2020, 22, 1903–1908. [Google Scholar] [CrossRef]
- Quarrell, O.W.; Nance, A.M.; Nopoulos, P.; Paulsen, J.S.; Smith, A.J.; Squitieri, F. Managing juvenile Huntington’s disease. Neurodegener. Dis. Manag. 2013, 3, 267–276. [Google Scholar] [CrossRef] [Green Version]
- Langbehn, K.E.; Cochran, A.M.; Van Der Plas, E.; Conrad, A.L.; Epping, E.; Martin, E.; Espe-Pfeifer, P.; Nopoulos, P. Behavioral Deficits in Juvenile Onset Huntington’s Disease. Brain Sci. 2020, 10, 543. [Google Scholar] [CrossRef] [PubMed]
- Cloud, L.J.; Rosenblatt, A.; Margolis, R.L.; Ross, C.A.; Pillai, J.A.; Corey-Bloom, J.; Tully, H.M.; Bird, T.; Panegyres, P.K.; Nichter, C.A.; et al. Seizures in juvenile Huntington’s disease: Frequency and characterization in a multicenter cohort. Mov. Disord. 2012, 27, 1797–1800. [Google Scholar] [CrossRef]
- Khair, A.M.; Do, J.K.; Falchek, S. Drug-Resistant Epilepsy in Children with Juvenile Huntington’s Disease: A Challenging Case and Brief Review. Qatar Med. J. 2020, 2020, 18. [Google Scholar] [CrossRef]
- Scahill, R.; Zeun, P.; Osborne-Crowley, K.; Johnson, E.B.; Gregory, S.; Parker, C.; Lowe, J.; Nair, A.; O’Callaghan, C.; Langley, C.; et al. Biological and clinical characteristics of gene carriers far from predicted onset in the Huntington’s disease Young Adult Study (HD-YAS): A cross-sectional analysis. Lancet Neurol. 2020, 19, 502–512. [Google Scholar] [CrossRef]
- Latimer, C.S.; Flanagan, M.E.; Cimino, P.J.; Jayadev, S.; Davis, M.; Hoffer, Z.S.; Montine, T.J.; Gonzalez-Cuyar, L.F.; Bird, T.D.; Keene, C.D. Neuropathological Comparison of Adult Onset and Juvenile Huntington’s Disease with Cerebellar Atrophy: A Report of a Father and Son. J. Huntington’s Dis. 2017, 6, 337–348. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- European Medicines Agency Decision CW/0001/2015. Available online: http://www.ema.europa.eu/docs/en_GB/document_library/Other/2015/07/WC500190385.pdf (accessed on 21 December 2018).


| Patient No. | Patient Code | CAG Exp. | Gender M/F | Genetic Transmission | Age at Onset (Years) | Age at Diagnosis (Years) |
|---|---|---|---|---|---|---|
| 1 | HD130 05 | 95 | F | paternal | 2 | 6 |
| 2 | HD379 05 | 87 | M | paternal | 4 | 7 |
| 3 | HD707 02 | 114 | M | paternal | 3.5 | 5 |
| 4 | HD636 01 | 84 | F | paternal | 2 | 6 |
| Patient No. | Patient Code | Gender | CAG Exp. | Major Mother’s Pregnancy Events | Weight at Birth (gr) | Walking (First Independent Steps) | Balance (Tendency to Fall) | Speech Production (First Words) | Language Acquisition |
|---|---|---|---|---|---|---|---|---|---|
| 1 | HD130 05 | F | 95 | Birth at term | 3000 | 18–19 months | Unstable | 24–30 months | Blurred speech |
| 2 | HD379 05 | M | 87 | Birth at term | 3550 | 12 months | Unstable | 10–12 months | Stuttering |
| 3 | HD707 02 | M | 114 | Birth at term, gestational diabetes and pregnancy hypertension | 3670 | 12 months | Ok | 12 months | Fluid language |
| 4 | HD636 01 | F | 84 | Birth at term, gestational diabetes | 3640 | 20–22 months | Falls | 18 months | Never fluid |
| Patient No. | Patient Code | Age at Evaluation (Years) | LEITER Cognitive Level | ABAS Adaptive Functioning | PPVT Receptive Language | CY-BOCS Obsession and Compulsions | CBCL Behavior Problems—Parent(s) Report | K-SADS Behavior Problems—Health Professional’s Interview |
|---|---|---|---|---|---|---|---|---|
| 1 | HD130 05 | 10 | IQ = 70 | IQ = 63 | IQ = 76 | 22/40 | Anxiety and affective problems | Explosive outbursts, low impulsivity control, avoidant/restrictive food intake disorder |
| 2 | HD379 05 | 12 | IQ = 68 | IQ = 34 | IQ < 65 | 0/40 | Social and affective problems | Explosive outbursts, low impulsivity control and attention deficit disorder |
| 3 | HD707 02 | 4 | IQ = 73 | IQ = 68 | IQ = 70 | 0/40 | No | Explosive outburst and social isolation |
| 4 | HD636 01 | 11 | NA | NA | NA | 20/40 | Anxiety, social and affective problems | Learning difficulties, explosive outbursts with hetero and auto-aggressive behavior, low impulsivity control and social isolation |
| Patient No. | Patient Code | Age at the First Assay in Years (Age at Onset) | TMS at the First Assay | Age at the Last Assay (Years) | TMS at the Last Assay | Gain of TMS Units from the First to the Last Assay | Total Motor Score Units/Year from Onset Age | Age of First Epileptic Seizure (Years) |
|---|---|---|---|---|---|---|---|---|
| 1 | HD130 05 | 7 (2) | 27 | 10 | 72 | +45 | 9 | 9 |
| 2 | HD379 05 | 9 (4) | 41 | 13 | 71 | +30 | 7.8 | 8 |
| 3 | HD707 02 | 4 (3.5) | NA | 5 | NA | NA | NA | No |
| 4 | HD636 01 | 8 (2) | 31 | 11 | 57 | +26 | 6.3 | 13 |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Graziola, F.; Maffi, S.; Grasso, M.; Garone, G.; Migliore, S.; Scaricamazza, E.; Ceccarelli, C.; Casella, M.; Busi, L.; D’Alessio, B.; et al. “Spazio Huntington”: Tracing the Early Motor, Cognitive and Behavioral Profiles of Kids with Proven Pediatric Huntington Disease and Expanded Mutations > 80 CAG Repeats. J. Pers. Med. 2022, 12, 120. https://doi.org/10.3390/jpm12010120
Graziola F, Maffi S, Grasso M, Garone G, Migliore S, Scaricamazza E, Ceccarelli C, Casella M, Busi L, D’Alessio B, et al. “Spazio Huntington”: Tracing the Early Motor, Cognitive and Behavioral Profiles of Kids with Proven Pediatric Huntington Disease and Expanded Mutations > 80 CAG Repeats. Journal of Personalized Medicine. 2022; 12(1):120. https://doi.org/10.3390/jpm12010120
Chicago/Turabian StyleGraziola, Federica, Sabrina Maffi, Melissa Grasso, Giacomo Garone, Simone Migliore, Eugenia Scaricamazza, Consuelo Ceccarelli, Melissa Casella, Ludovica Busi, Barbara D’Alessio, and et al. 2022. "“Spazio Huntington”: Tracing the Early Motor, Cognitive and Behavioral Profiles of Kids with Proven Pediatric Huntington Disease and Expanded Mutations > 80 CAG Repeats" Journal of Personalized Medicine 12, no. 1: 120. https://doi.org/10.3390/jpm12010120
APA StyleGraziola, F., Maffi, S., Grasso, M., Garone, G., Migliore, S., Scaricamazza, E., Ceccarelli, C., Casella, M., Busi, L., D’Alessio, B., De Luca, A., Colafati, G. S., Sabatini, U., Capuano, A., & Squitieri, F. (2022). “Spazio Huntington”: Tracing the Early Motor, Cognitive and Behavioral Profiles of Kids with Proven Pediatric Huntington Disease and Expanded Mutations > 80 CAG Repeats. Journal of Personalized Medicine, 12(1), 120. https://doi.org/10.3390/jpm12010120








