A Fifteen-Year Analysis of Rare Isolated Fallopian Tube Torsions in Adolescent Children: A Case Series
Abstract
1. Introduction
2. Materials and Methods
Study Design and Population
3. Statistical Analysis
4. Results
5. Discussion
6. Conclusions
Author Contributions
Funding
Conflicts of Interest
References
- Artunç, B.; Şilfeler, D.B.; Erdemoğlu, M. Isolated tubal torsion as a cause of acute abdomen in the early adolescent period. Rev. Indeks J. Kartal Train. Res. Hosp. 2009, 20, 99–102. [Google Scholar]
- Orazi, C.; Inserra, A.; Lucchetti, M.C.; Schingo, P.M. Isolated tubal torsion: A rare cause of pelvic pain at menarche. Sonographic and MR findings. Pediatric Radiol. 2006, 36, 1316–1318. [Google Scholar] [CrossRef] [PubMed]
- Gross, M.; Blumstein, S.L.; Chow, L.C. Isolated Fallopian Tube Torsion: A Rare Twist on a Common Theme. Am. J. Roentgenol. 2005, 185, 1590–1592. [Google Scholar] [CrossRef] [PubMed]
- Krissi, H.; Shalev, J.; Bar-Hava, I.; Langer, R.; Herman, A.; Kaplan, B. Fallopian tube torsion: Laparoscopic evaluation and treatment of a rare gynecological entity. J. Am. Board Fam. Pr. 2001, 14, 274–277. [Google Scholar]
- Raban, O.; Zilber, H.; Hadar, E.; Efrat, Z.; Krissi, H.; Wiznitzer, A.; Meizner, I.; Bardin, R. Isolated Fallopian Tube Torsion: A Unique Ultrasound Identity or a Serial Copycat? J. Ultrasound Med. 2018, 37, 2387–2393. [Google Scholar] [CrossRef] [PubMed]
- Webster, K.W.; Scott, S.M.; Huguelet, P.S. Clinical Predictors of Isolated Tubal Torsion: A Case Series. J. Pediatric Adolesc. Gynecol. 2017, 30, 578–581. [Google Scholar] [CrossRef] [PubMed]
- Bertozzi, M.; Noviello, C.; Molinaro, F.; Ratta, A.; Lisi, G.; Cobellis, G.; Federici, S.; Chiesa, P.L.; Martino, A.; Messina, M. Isolated fallopian tube torsion in pediatric age: An Italian multicenter retrospective study. J. Pediatric Surg. 2019. [Google Scholar] [CrossRef] [PubMed]
- Casey, R.K.; Damle, L.F.; Gomez-Lobo, V. Isolated fallopian tube torsion in pediatric and adolescent females: A retrospective review of 15 cases at a single institution. J. Pediatric Adolesc. Gynecol. 2013, 26, 189–192. [Google Scholar] [CrossRef] [PubMed]
- Ho, P.-L.; Liang, S.-J.; Su, H.-W.; Chang, C.-Y.; Hsu, C.-S.; Ling, T.-H. Isolated Torsion of the Fallopian Tube: A Rare Diagnosis in an Adolescent Without Sexual Experience. Taiwan. J. Obstet. Gynecol. 2008, 47, 235–237. [Google Scholar] [CrossRef]
- Visnjic, S.; Kralj, R.; Zupancic, B. Isolated fallopian tube torsion with partial hydrosalpinx in a premenarcheal girl: A case report. J. Med. Case Rep. 2014, 8, 197. [Google Scholar] [CrossRef] [PubMed]
- Yancey, L.M. Intermittent Torsion of a Normal Ovary in a Child Associated with Use of a Trampoline. J. Emerg. Med. 2012, 42, 409–412. [Google Scholar] [CrossRef] [PubMed]
- Romano, M.; Di Giuseppe, J.; Serri, M.; Noviello, C.; Martino, A.; Cobellis, G.; Ciavattini, A. A possible association between sports and isolated fallopian tube torsion in children and adolescent females. Gynecol. Endocrinol. 2015, 31, 688–692. [Google Scholar] [CrossRef] [PubMed]
- Harmon, J.C.; Binkovitz, L.A.; Binkovitz, L.E. Isolated fallopian tube torsion: Sonographic and CT findings. Pediatric Radiol. 2008, 38, 175. [Google Scholar] [CrossRef] [PubMed]
- Chang, H.C.; Bhatt, S.; Dogra, V.S. Pearls and Pitfalls in Diagnosis of Ovarian Torsion. Radiographics 2008, 28, 1355–1368. [Google Scholar] [CrossRef] [PubMed]
- Wong, S.W.A.; Suen, S.H.S.; Lao, T.; Chung, K.H.T. Isolated fallopian tube torsion: A series of six cases. Acta Obstet. Et Gynecol. Scand. 2010, 89, 1354–1356. [Google Scholar] [CrossRef] [PubMed]
- Dietrich, J.E.; Heard, M.J.; Edwards, C. Uteroovarian Ligament Torsion of the Due to a Paratubal Cyst. J. Pediatric Adolesc. Gynecol. 2005, 18, 125–127. [Google Scholar] [CrossRef] [PubMed]
- Mazouni, C.; Bretelle, F.; Menard, J.P.; Blanc, B.; Gamerre, M. Diagnosis of adnexal torsion and predictive factors of adnexal necrosis. Gynecol. Obstet. Fertil. 2005, 33, 102–106. [Google Scholar] [CrossRef] [PubMed]
- Fagotti, A.; Rossitto, C.; Marocco, F.; Gallotta, V.; Bottoni, C.; Scambia, G.; Fanfani, F. Perioperative Outcomes of Laparoendoscopic Single-Site Surgery (LESS) Versus Conventional Laparoscopy for Adnexal Disease: A Case—Control Study. Surg. Innov. 2011, 18, 29–33. [Google Scholar] [CrossRef] [PubMed]
- Bertozzi, M.; Magrini, E.; Riccioni, S.; Giovenali, P.; Appignani, A. Isolated fallopian tube torsion with hydrosalpinx: Review of a debated management in a pediatric population. J. Pediatric Surg. 2017, 52, 1553–1560. [Google Scholar] [CrossRef] [PubMed]
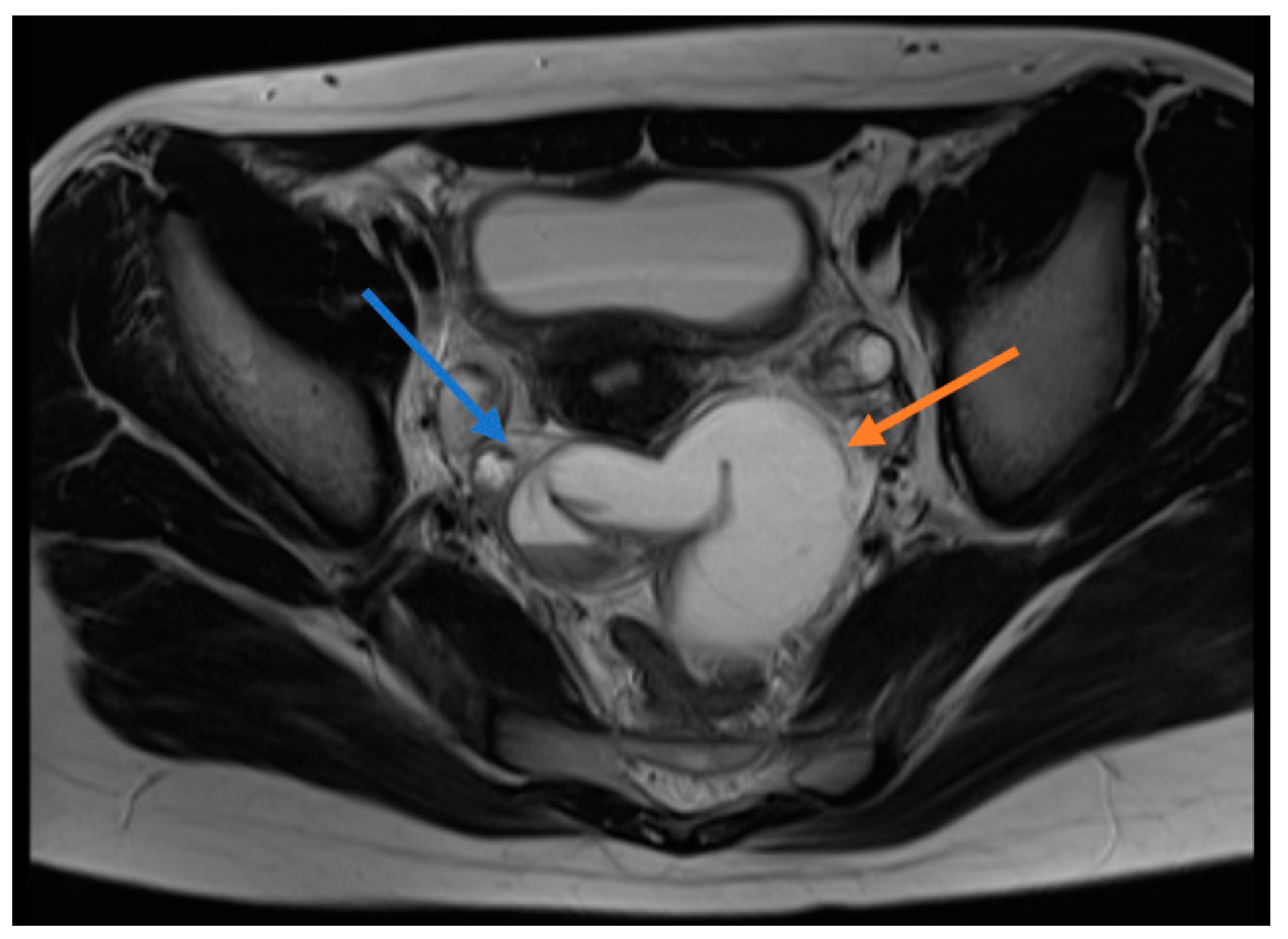
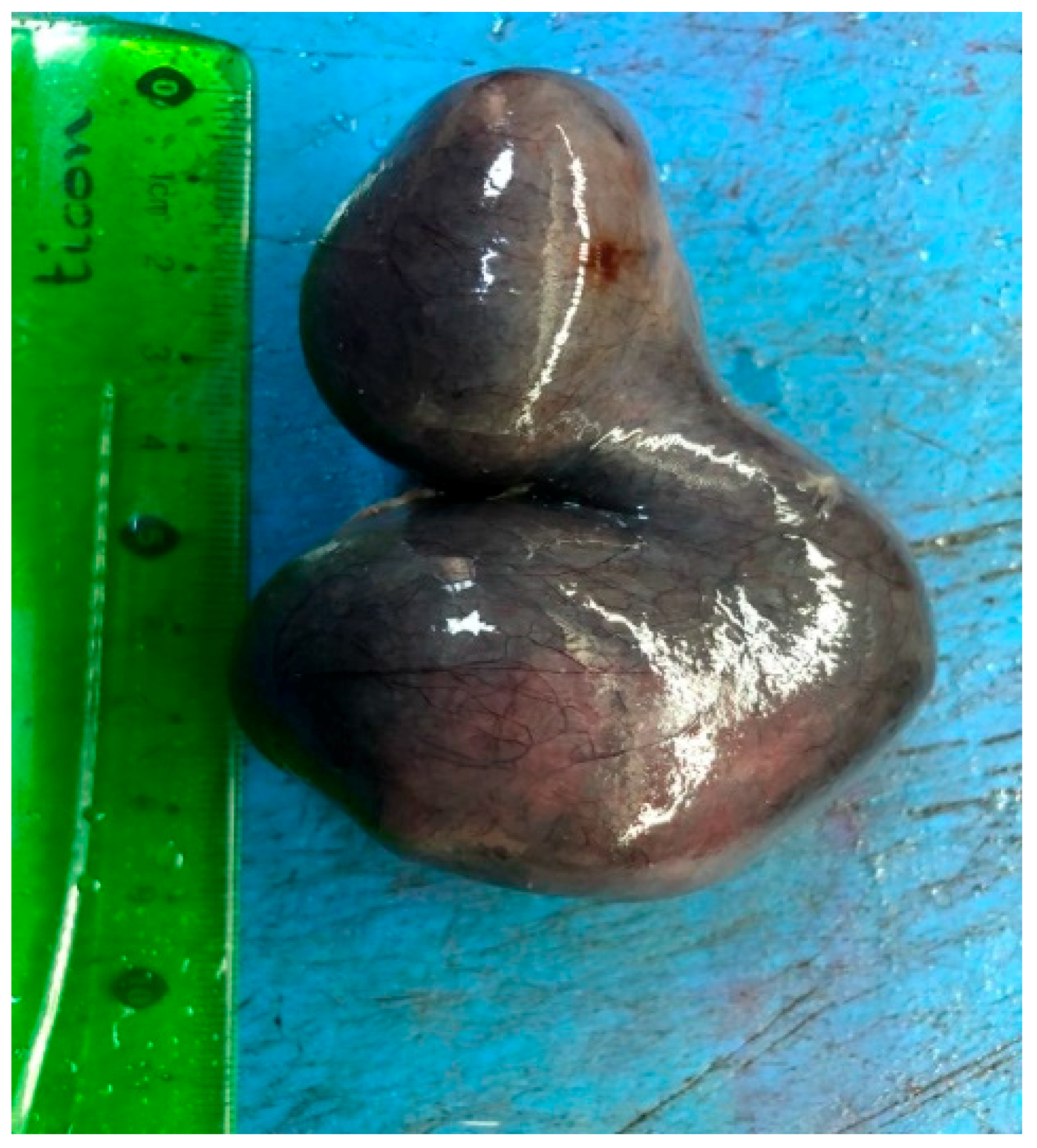
| Isolated Fallopian Tube Torsion | |
|---|---|
| All Patients | n (%) |
| Baseline Characteristics | |
| Age, mean ± SD, years | 14.5 ± 1.43 |
| Laboratory Findings | |
| WBC, mg/dL | 10.47 ± 2.40 |
| Neutrophils, % | 76.9 ± 7.58 |
| Lymphocytes, % | 18.1 ± 5.94 |
| BUN, mg/dL | 16.24 ± 8.19 |
| Crea, mg/dL | 0.73 ± 0.24 |
| ALT, mg/dL | 17.21 ± 7.23 |
| AST, mg/dL | 19.44 ± 7.31 |
| ALP, mg/dL | 86.24 ± 48.51 |
| BS, mg/dL | 94.11 ± 18.82 |
| Clinical Findings | |
| Presence of pain | 10 (100) |
| Time to start pain | |
| Less than 24h | 7 (70) |
| More than 24h | 3 (30) |
| Shape of pain | |
| Colic | 3 (30) |
| Continuous pain | 7 (70) |
| Nausea | 5 (50) |
| Vomiting | 5 (50) |
| Vaginal discharge | 0 (0) |
| Menarche | 9 (90) |
| Physical examination | |
| Abdominal tenderness | 9 (90) |
| Abdominal defender | 5 (50) |
| Abdominal rebound | 3 (30) |
| Imaging methods | |
| Direct abdominal radiography | 10 (100) |
| US | 10 (100) |
| MRI | 2 (20) |
| Tumor Markers | 2 (20) |
| Paraovarian cyst | 7 (70) |
| Doppler current reduction/absence | 3 (30) |
| Surgical intervention method | |
| Open surgery | 8 (80) |
| Laparoscopic | 2 (20) |
| Place of torsion | |
| Right | 5 (50) |
| Left | 5 (50) |
| Operation performed | |
| Detorsion | 5 (50) |
| Salpingectomy | 5 (50) |
| Age | Pain Localization | RDUS | MRI | Preop Diagnosis | Postop Diagnosis | Accompanying Pathology | Procedure |
|---|---|---|---|---|---|---|---|
| 14 | Lower left | Left paraovarian cyst, free liquid | None | Acute abdomen | Left IFTT | None | Open salpingectomy |
| 13 | Lower right | Normal | None | Acute abdomen | Right IFTT | None | Open detorsion, cyst excision |
| 14 | Lower left | Right paraovarian mass | Semi-solid cystic paraadnexial | Paraovarian mass | Right IFTT | Paratubal cyst | Open salpingectomy, cyst excision |
| 15 | All abdomen | Right paraovarian cyst, free liquid | None | Right ovarian torsion | Right IFTT | Paratubal cyst | Open salpingectomy, cyst excision |
| 17 | Lower left | Left paraovarian cyst | None | Left ovarian torsion, left IFTT | Left IFTT | None | LAP detorsion |
| 16 | Lower right | Right paraovarian cyst, free liquid | None | Right ovarian torsion | Right IFTT | None | LAPdetorsion |
| 12 | All abdomen | Normal | Fallopian tube wall thickening, hydrohematosalpinx | IFTT | Right IFTT | None | Opensalpingectomy |
| 15 | Lower left | Free liquid | None | Ovarian cyst rupture | Left IFTT | Paratubal cyst | Open detorsion, cyst excision |
| 14 | Sub-dial | Left paraovarian cyst | None | Acute abdomen | Left IFTT | Paratubal cyst | |
| 15 | Lower left | Left paraovarian cyst | None | Left ovarian torsion | Left IFTT | None | Open detorsion |
© 2019 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Güney, C.; Coskun, A. A Fifteen-Year Analysis of Rare Isolated Fallopian Tube Torsions in Adolescent Children: A Case Series. Diagnostics 2019, 9, 110. https://doi.org/10.3390/diagnostics9030110
Güney C, Coskun A. A Fifteen-Year Analysis of Rare Isolated Fallopian Tube Torsions in Adolescent Children: A Case Series. Diagnostics. 2019; 9(3):110. https://doi.org/10.3390/diagnostics9030110
Chicago/Turabian StyleGüney, Cengiz, and Abuzer Coskun. 2019. "A Fifteen-Year Analysis of Rare Isolated Fallopian Tube Torsions in Adolescent Children: A Case Series" Diagnostics 9, no. 3: 110. https://doi.org/10.3390/diagnostics9030110
APA StyleGüney, C., & Coskun, A. (2019). A Fifteen-Year Analysis of Rare Isolated Fallopian Tube Torsions in Adolescent Children: A Case Series. Diagnostics, 9(3), 110. https://doi.org/10.3390/diagnostics9030110





