Lung Ultrasound Versus Chest Radiography for Acute Heart Failure: Impact of Heart Failure History and Pleural Effusion
Abstract
1. Introduction
2. Materials and Methods
2.1. Study Design
2.2. Population
2.3. Lung Ultrasound
2.4. Radiology
2.5. Comprehensive Echocardiography
2.6. Clinical Reference Standard: Acute Heart Failure
- (1)
- Cardiologist-adjudicated AHF, adjudicated by two cardiologists. AHF was adjudicated based on the comprehensive echocardiography and medical record information, but without direct evaluation of radiology images or LUS. The AHF diagnosis was restricted to patients with AHF in the absence of concomitant clinically significant acute pulmonary disease. In sensitivity analyses presented in the Supplementary Material, we also report results for patients diagnosed with AHF who had concomitant significant acute pulmonary disease, as adjudicated by an expert panel of pulmonologists.
- (2)
- A secondary, objective Echo-BNP AHF diagnosis. This was established to eliminate circular reasoning from medical record review that the radiology images might have influenced. It is based on four objective criteria: echocardiographic evidence of abnormal structure or function, elevated NT-proBNP, signs of increased left ventricular filling pressure, and treatment with loop diuretics.
2.7. Statistics
3. Results
3.1. Baseline Characteristics
3.2. Diagnostic Accuracy of LUS and Chest Radiography Using LDCT as Comparator
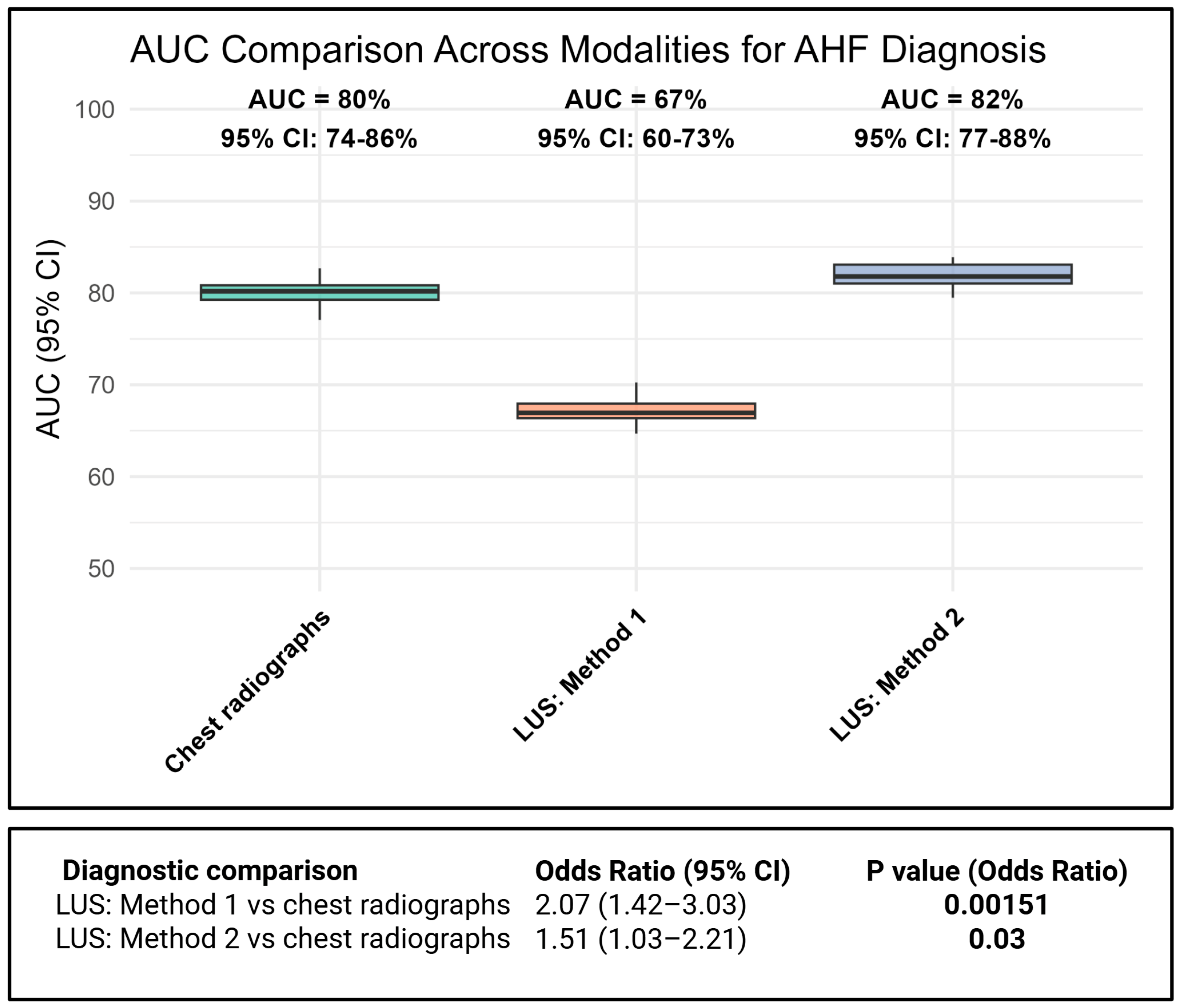
3.3. Relative Diagnostic Accuracy and Influence of Chronic Heart Failure
3.4. Interobserver Variability
4. Discussion
4.1. Main Findings
4.2. LUS Versus Chest Radiographs
4.3. The Optimal LUS Approach in the Acute Setting
4.4. Diagnostic Performance of LUS in Patients with and Without a History of Heart Failure
4.5. LDCT as Objective Comparator
4.6. Strengths and Limitations
5. Conclusions
Clinical Applicability
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
Abbreviations
| AHF | Acute heart failure |
| AUC | Area Under the Receiver Operating Characteristic Curve |
| OR | Conditional Odds Ratio |
| CT | Computed Tomography |
| CXR | Chest Radiography (Chest X-ray) |
| HF | Heart Failure |
| IQR | Interquartile Range |
| LDCT | Low-dose, Non-contrast Chest Computed Tomography |
| LUS | Lung Ultrasound |
| LVEF | Left Ventricular Ejection Fraction |
| NLR | Negative Likelihood Ratio |
| NPV | Negative Predictive Value |
| NT-proBNP | NT-proBrain Natriuretic Peptide |
| NYHA | New York Heart Association Functional Classification |
| PLR | Positive Likelihood Ratio |
| PPV | Positive Predictive Value |
| ROC | Receiver Operating Characteristic Curve |
| SD | Standard Deviation |
| TNR | True Negative Rate |
| TPR | True Positive Rate |
Appendix A. Overview of the Reference Standards for AHF
- (1)
- Clinical Reference AHF: Adjudicated by two cardiologists (and a third in case of disagreement) according to a modified version of the 2017 cardiovascular and stroke endpoint definitions for clinical trials consensus report [12,20,21,34,35] based on the following information:
- (A)
- Review of comprehensive echocardiography images with evidence of abnormal structure, function, and LV filling pressures (grade II + III)
- (B)
- Review of medical record information including history and blood samples, but without direct evaluation of radiology images.
- (C)
- Review of the presence of clinically significant concomitant acute pulmonary disease as a potential cause of acute dyspnea

- (2)
- Echo-BNP AHF: An operator independent objective diagnosis established to eliminate any bias and circular reasoning cardiologists would obtain by reviewing the medical record review that the radiology imaging modalities might have influenced.Based only on the presence of all four objective criteria:
- (1)
- Echocardiographic abnormal structure or function; left ventricular ejection fraction (LVEF) ≤ 40%, LVEF 41–49%, LVEF ≥ 50% with diastolic dysfunction or severe valve disease [34];
- (2)
- NT-proBNP >300 pg/mL [34];
- (3)
- Signs of elevated LV filling pressure on echocardiography (grade II + III) [21];
- (4)
- Administration of loop diuretics orally or intravenously any time during admission or at dis-charge
References
- Gargani, L.; Girerd, N.; Platz, E.; Pellicori, P.; Stankovic, I.; Palazzuoli, A.; Pivetta, E.; Miglioranza, M.H.; Soliman-Aboumarie, H.; Agricola, E.; et al. Lung ultrasound in acute and chronic heart failure. A Clinical Consensus Statement of the European Association of Cardiovascular Imaging (EACVI). Eur. Heart J. Cardiovasc. Imaging 2023, 24, 1569–1582. [Google Scholar] [CrossRef]
- Siwik, D.; Apanasiewicz, W.; Żukowska, M.; Jaczewski, G.; Dąbrowska, M. Diagnosing Lung Abnormalities Related to Heart Failure in Chest Radiogram, Lung Ultrasound and Thoracic Computed Tomography. Adv. Respir. Med. 2023, 91, 103–122. [Google Scholar] [CrossRef]
- Maw, A.M.; Hassanin, A.; Ho, P.M.; McInnes, M.D.F.F.; Moss, A.; Juarez-Colunga, E.; Soni, N.J.; Miglioranza, M.H.; Platz, E.; DeSanto, K.; et al. Diagnostic Accuracy of Point-of-Care Lung Ultrasonography and Chest Radiography in Adults With Symptoms Suggestive of Acute Decompensated Heart Failure: A Systematic Review and Meta-analysis. JAMA Netw. Open 2019, 2, e190703. [Google Scholar] [CrossRef] [PubMed]
- McGivery, K.; Atkinson, P.; Lewis, D.; Taylor, L.; Harris, T.; Gadd, K.; Fraser, J.; Stoica, G. Emergency department ultrasound for the detection of B-lines in the early diagnosis of acute decompensated heart failure: A systematic review and meta-analysis. Can. J. Emerg. Med. 2018, 20, 343–352. [Google Scholar] [CrossRef] [PubMed]
- Miglioranza, M.H.; Gargani, L.; Sant’Anna, R.T.; Rover, M.M.; Martins, V.M.; Mantovani, A.; Weber, C.; Moraes, M.A.; Feldman, C.J.; Kalil, R.A.K.; et al. Lung ultrasound for the evaluation of pulmonary congestion in outpatients: A comparison with clinical assessment, natriuretic peptides, and echocardiography. JACC Cardiovasc. Imaging 2013, 6, 1141–1151. [Google Scholar] [CrossRef]
- Pivetta, E.; Goffi, A.; Lupia, E.; Tizzani, M.; Porrino, G.; Ferreri, E.; Volpicelli, G.; Balzaretti, P.; Banderali, A.; Iacobucci, A.; et al. Lung ultrasound-implemented diagnosis of acute decompensated heart failure in the ED: A SIMEU multicenter study. Chest 2015, 148, 202–210. [Google Scholar] [CrossRef]
- Picano, E.; Frassi, F.; Agricola, E.; Gligorova, S.; Gargani, L.; Mottola, G. Ultrasound lung comets: A clinically useful sign of extravascular lung water. J. Am. Soc. Echocardiogr. 2006, 19, 356–363. [Google Scholar] [CrossRef]
- Neesse, A.; Jerrentrup, A.; Hoffmann, S.; Sattler, A.; Görg, C.; Kill, C.; Gress, T.M.; Kunsch, S. Prehospital chest emergency sonography trial in Germany: A prospective study. Eur. J. Emerg. Med. 2012, 19, 161–166. [Google Scholar] [CrossRef]
- Celutkiene, J.; Lainscak, M.; Anderson, L.; Gayat, E.; Grapsa, J.; Harjola, V.-P.; Manka, R.; Nihoyannopoulos, P.; Filardi, P.P.; Vrettou, R.; et al. Imaging in patients with suspected acute heart failure: Timeline approach position statement on behalf of the Heart Failure Association of the European Society of Cardiology. Eur. J. Heart Fail. 2019, 22, 181–195. [Google Scholar] [CrossRef]
- Buessler, A.; Chouihed, T.; Duarte, K.; Bassand, A.; Huot-Marchand, M.; Gottwalles, Y.; Pénine, A.; André, E.; Nace, L.; Jaeger, D.; et al. Accuracy of Several Lung Ultrasound Methods for the Diagnosis of Acute Heart Failure in the ED: A Multicenter Prospective Study. Chest 2020, 157, 99–110. [Google Scholar] [CrossRef]
- Pivetta, E.; Goffi, A.; Nazerian, P.; Castagno, D.; Tozzetti, C.; Tizzani, P.; Tizzani, M.; Porrino, G.; Ferreri, E.; Busso, V.; et al. Lung ultrasound integrated with clinical assessment for the diagnosis of acute decompensated heart failure in the emergency department: A randomized controlled trial. Eur. J. Heart Fail. 2019, 21, 754–766. [Google Scholar] [CrossRef]
- Miger, K.; Overgaard Olesen, A.S.; Grand, J.; Fabricius-Bjerre, A.; Sajadieh, A.; Høst, N.; Køber, N.; Abild, A.; Pedersen, L.; Lawaetz Schultz, H.H.; et al. Computed tomography or chest X-ray to assess pulmonary congestion in dyspnoeic patients with acute heart failure. ESC Heart Fail. 2024, 11, 1163–1173. [Google Scholar] [CrossRef]
- Laursen, C.B.; Sloth, E.; Lambrechtsen, J.; Lassen, A.T.; Madsen, P.H.; Henriksen, D.P.; Davidsen, J.R.; Rasmussen, F. Focused sonography of the heart, lungs, and deep veins identifies missed life-threatening conditions in admitted patients with acute respiratory symptoms. Chest 2013, 144, 1868–1875. [Google Scholar] [CrossRef]
- Volpicelli, G.; Elbarbary, M.; Blaivas, M.; Lichtenstein, D.A.; Mathis, G.; Kirkpatrick, A.W.; Melniker, L.; Gargani, L.; Noble, V.E.; Via, G.; et al. International evidence-based recommendations for point-of-care lung ultrasound. Intensive Care Med. 2012, 38, 577–591. [Google Scholar] [CrossRef]
- Coiro, S.; Rossignol, P.; Ambrosio, G.; Carluccio, E.; Alunni, G.; Murrone, A.; Tritto, I.; Zannad, F.; Girerd, N. Prognostic value of residual pulmonary congestion at discharge assessed by lung ultrasound imaging in heart failure. Eur. J. Heart Fail. 2015, 17, 1172–1181. [Google Scholar] [CrossRef]
- Austin, J.H.M.; Naidich, P.; Muller, L.; Hansell, M.; Zerhouni, A. Thoracic for CT of the Lungs: Of the Nomenclature Fleischner Society. Radiology 1996, 200, 327–331. [Google Scholar] [CrossRef]
- Christe, A.; Charimo-Torrente, J.; Roychoudhury, K.; Vock, P.; Roos, J.E. Accuracy of low-dose computed tomography (CT) for detecting and characterizing the most common CT-patterns of pulmonary disease. Eur. J. Radiol. 2013, 82, e142–e150. [Google Scholar] [CrossRef] [PubMed]
- Austin, J.H.; Müller, N.L.; Friedman, P.J.; Hansell, D.M.; Naidich, D.P.; Remy-Jardin, M.; Webb, W.R.; Zerhouni, E.A. Glossary of terms for CT of the lungs: Recommendations of the Nomenclature Committee of the Fleischner Society. Radiology 1996, 200, 327–331. [Google Scholar] [CrossRef] [PubMed]
- Miger, K.C.; Fabricius-Bjerre, A.; Overgaard Olesen, A.S.; Sajadieh, A.; Høst, N.; Køber, N.; Abild, A.; Winkler Wille, M.M.; Wamberg, J.; Pedersen, L.; et al. Chest computed tomography features of heart failure: A prospective observational study in patients with acute dyspnea. Cardiol. J. 2022, 29, 235–244. [Google Scholar] [CrossRef] [PubMed]
- Ponikowski, P.; Voors, A.A.; Anker, S.D.; Bueno, H.; Cleland, J.G.F.; Coats, A.J.S.; Falk, V.; González-Juanatey, J.R.; Harjola, V.-P.; Jankowska, E.A.; et al. 2016 ESC Guidelines for the diagnosis and treatment of acute and chronic heart failure: The Task Force for the diagnosis and treatment of acute and chronic heart failure of the European Society of Cardiology (ESC) Developed with the special contribution of the Heart Failure Association (HFA) of the ESC. Eur. Heart J. 2016, 37, 2129–2200. [Google Scholar] [CrossRef]
- Nagueh, S.F.; Smiseth, O.A.; Appleton, C.P.; Byrd, B.F.; Dokainish, H.; Edvardsen, T.; Flachskampf, F.A.; Gillebert, T.C.; Klein, A.L.; Lancellotti, P.; et al. Recommendations for the Evaluation of Left Ventricular Diastolic Function by Echocardiography: An Update from the American Society of Echocardiography and the European Association of Cardiovascular Imaging. Eur. Heart J. Cardiovasc. Imaging 2016, 17, 1321–1360. [Google Scholar] [CrossRef]
- Hajian-Tilaki, K. Sample size estimation in diagnostic test studies of biomedical informatics. J. Biomed. Inform. 2014, 48, 193–204. [Google Scholar] [CrossRef]
- Olesen, A.S.O.; Miger, K.; Fabricius-Bjerre, A.; Sandvang, K.D.; Kjesbu, I.E.; Sajadieh, A.; Høst, N.; Køber, N.; Wamberg, J.; Pedersen, L.; et al. Remote dielectric sensing to detect acute heart failure in patients with dyspnoea: A prospective observational study in the emergency department. Eur. Heart J. Open 2022, 2, oeac073. [Google Scholar] [CrossRef] [PubMed]
- Olesen, A.S.O.; Miger, K.; Fabricius-bjerre, A.; Maschmann, C. Diagnostic value of Remote Dielectric Sensing (ReDS) technology to predict pulmonary congestion on computed tomography in consecutive patients with acute dyspnea. Eur. J. Heart Fail. 2019, 21, 110. [Google Scholar]
- Chiu, L.; Jairam, M.P.; Chow, R.; Chiu, N.; Shen, M.; Alhassan, A.; Lo, C.-H.; Chen, A.; Kennel, P.J.; Poterucha, T.J.; et al. Meta-Analysis of Point-of-Care Lung Ultrasonography Versus Chest Radiography in Adults With Symptoms of Acute Decompensated Heart Failure. Am. J. Cardiol. 2022, 174, 89–95. [Google Scholar] [CrossRef] [PubMed]
- Sartini, S.; Frizzi, J.; Borselli, M.; Sarcoli, E.; Granai, C.; Gialli, V.; Cevenini, G.; Guazzi, G.; Bruni, F.; Gonnelli, S.; et al. Which method is best for an early accurate diagnosis of acute heart failure? Comparison between lung ultrasound, chest X-ray and NT pro-BNP performance: A prospective study. Intern. Emerg. Med. 2017, 12, 861–869. [Google Scholar] [CrossRef]
- Rahmani, E.; Farrokhi, M.; Farrokhi, M.; Nouri, S.; Moghadam Fard, A.; Hoorshad, B.; Atighi, R.; Ghadirzadeh, E.; Tajik, M.; Afshang, H.; et al. Accuracy of Lung Ultrasonography for Diagnosis of Heart Failure; a Systematic Review and Meta-analysis. Arch. Acad. Emerg. Med. 2025, 13, e33. [Google Scholar] [CrossRef]
- Volpicelli, G.; Caramello, V.; Cardinale, L.; Mussa, A.; Bar, F.; Frascisco, M.F. Bedside ultrasound of the lung for the monitoring of acute decompensated heart failure. Am. J. Emerg. Med. 2008, 26, 585–591. [Google Scholar] [CrossRef]
- Perrone, T.; Maggi, A.; Sgarlata, C.; Palumbo, I.; Mossolani, E.; Ferrari, S.; Melloul, A.; Mussinelli, R.; Boldrini, M.; Raimondi, A.; et al. Lung ultrasound in internal medicine: A bedside help to increase accuracy in the diagnosis of dyspnea. Eur. J. Intern. Med. 2017, 46, 61–65. [Google Scholar] [CrossRef]
- Miger, K.; Fabricius-Bjerre, A.; Olesen, A.S.O.; Nielsen, R.; Fredriksen, C.A.; Pryds, K.; Petersen, J.; Nielsen, O.W. Early Detection of Pulmonary Congestion Using Quantitative CT and Lung US in a Porcine Model. Radiogr. Cardiothorac. Imaging 2025, in press. [Google Scholar]
- Hendee, W.R.; O’Connor, M.K. Radiation risks of medical imaging: Separating fact from fantasy. Radiology 2012, 264, 312–321. [Google Scholar] [CrossRef] [PubMed]
- Sundhedsstyrelsen, S. Stråling i sundhedsvidenskabelige forsøg. Natl. Vidensk. Komité 2011, 2, 2–4. [Google Scholar]
- Mosterd, A.; Hoes, A.W. Clinical epidemiology of heart failure. Heart 2007, 93, 1137–1146. [Google Scholar] [CrossRef]
- McDonagh, T.A.; Metra, M.; Adamo, M.; Gardner, R.S.; Baumbach, A.; Böhm, M.; Burri, H.; Butler, J.; Celutkiene, J.; Chioncel, O.; et al. 2021 ESC Guidelines for the diagnosis and treatment of acute and chronic heart failure. Eur. Heart J. 2021, 42, 3599–3726. [Google Scholar] [CrossRef]
- Hicks, K.A.; Mahaffey, K.W.; Mehran, R.; Nissen, S.E.; Wiviott, S.D.; Dunn, B.; Solomon, S.D.; Marler, J.R.; Teerlink, J.R.; Farb, A.; et al. 2017 Cardiovascular and Stroke Endpoint Definitions for Clinical Trials. Circulation 2018, 137, 961–972. [Google Scholar] [CrossRef] [PubMed]


| All Patients | No History of HF | History of HF | p-Value | |
|---|---|---|---|---|
| N: 240 | N: 182 | N: 58 | ||
| History | ||||
| Age (years), mean (SD) | 74.0 (10.2) | 73.5 (10.5) | 75.7 (9.06) | 0.096 |
| Sex (male), N (%) | 133 (55.4) | 94 (51.6) | 39 (67.2) | 0.054 |
| Diabetes (I+II), N (%) | 59 (24.6) | 42 (23.1) | 17 (29.3) | 0.432 |
| Hypercholesterolaemia, N (%) | 71 (29.6) | 43 (23.6) | 28 (48.3) | 0.001 |
| Hypertension, N (%) | 148 (61.7) | 111 (61.0) | 37 (63.8) | 0.820 |
| Kidney disease, N (%) | 22 (9.17) | 10 (5.46) | 12 (20.3) | 0.001 |
| COPD, N (%) | 126 (52.5) | 102 (56.0) | 24 (41.4) | 0.072 |
| Clinical examination | ||||
| BMI (kg/m2), median [IQR] | 25.8 [22.7;29.9] | 25.8 [22.9;29.4] | 26.4 [22.3;30.6] | 0.657 |
| Systolic blood pressure (mmHg), mean (SD) | 144 (27.8) | 145 (27.7) | 138 (27.5) | 0.082 |
| Respiratory frequency (N/minute), median [IQR] | 22.0 [18.0;24.0] | 22.0 [19.0;24.0] | 20.5 [18.0;25.5] | 0.633 |
| Orthopnoea, N (%) | 117 (48.8) | 79 (43.4) | 38 (65.5) | 0.005 |
| Pedal oedema, N (%) | 72 (30.0) | 52 (28.6) | 20 (34.5) | 0.490 |
| Fever, N (%) | 29 (12.1) | 25 (13.7) | 4 (6.90) | 0.246 |
| Cough, N (%) | 180 (75.0) | 140 (76.9) | 40 (69.0) | 0.296 |
| Systolic murmur, N (%) | 74 (30.8) | 51 (28.0) | 23 (39.7) | 0.132 |
| Bilateral rales, N (%) | 89 (37.1) | 62 (34.1) | 27 (46.6) | 0.119 |
| Rhonchi, N (%) | 76 (31.7) | 65 (35.7) | 11 (19.0) | 0.026 |
| Pao2/fio2 ratio, mean (SD) | 320 (107) | 317 (105) | 330 (111) | 0.431 |
| NYHA class, N (%) | 0.603 | |||
| II | 76 (31.7) | 61 (33.5) | 15 (25.9) | |
| III | 105 (43.8) | 76 (41.8) | 29 (50.0) | |
| IV | 58 (24.2) | 44 (24.2) | 14 (24.1) | |
| NT-proBNP (pg/mL), median [IQR] | 867 [228;3209] | 599 [169;2385] | 2694 [814;6008] | <0.001 |
| C-reactive protein (mg/L), median [IQR] | 16.9 [5.88;61.7] | 15.2 [5.06;61.0] | 21.0 [7.25;61.3] | 0.316 |
| eGFR (mL/min/1.73 m2), median [IQR] | 69.5 [49.0;85.0] | 75.0 [52.0;88.9] | 54.5 [42.2;70.0] | <0.001 |
| Echocardiography | ||||
| LVEF (%), median [IQR] | 55.0 [45.0;60.0] | 60.0 [50.0;60.0] | 40.0 [25.0;50.0] | <0.001 |
| TR velocity (m/s), mean (SD) | 275 (74.4) | 272 (76.6) | 284 (67.0) | 0.269 |
| Average E/e, median [IQR] | 10.6 [7.90;14.5] | 10.3 [7.57;13.4] | 12.4 [8.30;18.5] | 0.007 |
| LA-volume index (mL/m2), mean (SD) | 34.2 (15.5) | 31.9 (14.7) | 41.6 (15.8) | <0.001 |
| Increased filling pressure (II+III), N (%) | 94 (39.2) | 59 (32.4) | 35 (60.3) | <0.001 |
| Echocardiographic cardiac function, N (%) | ||||
| Severe valvular heart disease | 9 (3.75) | 8 (4.40) | 1 (1.72) | 0.691 |
| LVEF ≤ 40 | 54 (22.5) | 24 (13.2) | 30 (51.7) | <0.001 |
| LVEF 41–49 | 24 (10.0) | 9 (4.95) | 15 (25.9) | <0.001 |
| LVEF > 50 + (definite diastolic dysfunction or LAE/LVH) | 48 (20.0) | 38 (20.9) | 10 (17.2) | 0.678 |
| DIAGNOSTIC MODALITY | Sensitivity (%) | Specificity (%) | PPV (%) | NPV (%) | PLR | NLR |
|---|---|---|---|---|---|---|
| (95% CI) | (95% CI) | (95% CI) | (95% CI) | (95% CI) | (95% CI) | |
| LUNG ULTRASOUND | ||||||
| Method 1 | 47 | 86 | 56 | 81 | 3.41 | 0.62 |
| (≥3 B-lines in one zone bilaterally) | (35–60) | (80–91) | (42–70) | (75–86) | (2.17–5.35) | (0.49–0.78) |
| Method 2 | 80 | 84 | 66 | 92 | 5.18 | 0.23 |
| (≥3 B-lines in one zone bilaterally and/or bilateral PE) | (69–89) | (78–90) | (55–76) | (87–96) | (3.59-7.47) | (0.14–0.38) |
| RADIOLOGY | ||||||
| Chest radiography | 68 | 91 | 75 | 88 | 7.91 | 0.35 |
| (56–79) | (86–95) | (62–85) | (83–93) | (4.74–13.18) | (0.24–0.50) | |
| LDCT | 74 | 96 | 88 | 91 | 18.45 | 0.27 |
| (62–84) | (92–98) | (76–95) | (86–95) | (8.81–38.66) | (0.18–0.40) |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2025 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Miger, K.C.; Overgaard Olesen, A.S.; Grand, J.; Boesen, M.P.; Thune, J.J.; Wendelboe Nielsen, O. Lung Ultrasound Versus Chest Radiography for Acute Heart Failure: Impact of Heart Failure History and Pleural Effusion. Diagnostics 2025, 15, 3047. https://doi.org/10.3390/diagnostics15233047
Miger KC, Overgaard Olesen AS, Grand J, Boesen MP, Thune JJ, Wendelboe Nielsen O. Lung Ultrasound Versus Chest Radiography for Acute Heart Failure: Impact of Heart Failure History and Pleural Effusion. Diagnostics. 2025; 15(23):3047. https://doi.org/10.3390/diagnostics15233047
Chicago/Turabian StyleMiger, Kristina Cecilia, Anne Sophie Overgaard Olesen, Johannes Grand, Mikael Ploug Boesen, Jens Jakob Thune, and Olav Wendelboe Nielsen. 2025. "Lung Ultrasound Versus Chest Radiography for Acute Heart Failure: Impact of Heart Failure History and Pleural Effusion" Diagnostics 15, no. 23: 3047. https://doi.org/10.3390/diagnostics15233047
APA StyleMiger, K. C., Overgaard Olesen, A. S., Grand, J., Boesen, M. P., Thune, J. J., & Wendelboe Nielsen, O. (2025). Lung Ultrasound Versus Chest Radiography for Acute Heart Failure: Impact of Heart Failure History and Pleural Effusion. Diagnostics, 15(23), 3047. https://doi.org/10.3390/diagnostics15233047






