Glycosaminoglycans as Biomarkers for Mucopolysaccharidoses and Other Disorders
Abstract
:1. Introduction
2. Materials and Methods
2.1. Subjects
2.2. Enzymes and Standards
2.3. Sample Preparations
2.4. LC-MS/MS
2.5. Statistical Analysis
3. Results
3.1. Conditions with Elevated GAG Levels
3.2. Encephalopathy GAG Levels
3.3. GAG Levels of Various Conditions
3.4. GAG Levels of Newborns
4. Discussion
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Miyata, S.; Kitagawa, H. Formation and remodeling of the brain extracellular matrix in neural plasticity: Roles of chondroitin sulfate and hyaluronan. Biochim. Biophys. Acta Gen. Subj. 2017, 1861, 2420–2434. [Google Scholar] [CrossRef]
- Caterson, B.; Melrose, J. Keratan sulfate, a complex glycosaminoglycan with unique functional capability. Glycobiology 2018, 28, 182–206. [Google Scholar] [CrossRef]
- Zimmermann, D.R.; Dours-Zimmermann, M.T. Extracellular matrix of the central nervous system: From neglect to challenge. Histochem. Cell. Biol. 2008, 130, 635–653. [Google Scholar] [CrossRef] [Green Version]
- Smith, P.D.; Coulson-Thomas, V.J.; Foscarin, S.; Kwok, J.C.; Fawcett, J.W. “GAG-ing with the neuron”: The role of glycosaminoglycan patterning in the central nervous system. Exp. Neurol. 2015, 274 Pt B, 100–114. [Google Scholar] [CrossRef]
- Thomsen, M.S.; Routhe, L.J.; Moos, T. The vascular basement membrane in the healthy and pathological brain. J. Cerebr. Blood Flow Met. 2017, 37, 3300–3317. [Google Scholar] [CrossRef]
- Kubaski, F.; Mason, R.W.; Nakatomi, A.; Shintaku, H.; Xie, L.; van Vlies, N.N.; Church, H.; Giugliani, R.; Kobayashi, H.; Yamaguchi, S.; et al. Newborn screening for mucopolysaccharidoses: A pilot study of measurement of glycosaminoglycans by tandem mass spectrometry. J. Inherit. Metab. Dis. 2017, 40, 151–158. [Google Scholar] [CrossRef] [Green Version]
- Stapleton, M.; Kubaski, F.; Mason, R.W.; Shintaku, H.; Kobayashi, H.; Yamaguchi, S.; Taketani, T.; Suzuki, Y.; Orii, K.; Orii, T.; et al. Newborn screening for mucopolysaccharidoses: Measurement of glycosaminoglycans by LC-MS/MS. Mol. Genet. Metab. Rep. 2020, 22, 100563. [Google Scholar] [CrossRef]
- Pihtili, A.; Bingol, Z.; Kiyan, E. Serum endocan levels in patients with stable COPD. Int. J. Chron. Obstruct. Pulmon. Dis. 2018, 13, 3367–3372. [Google Scholar] [CrossRef] [Green Version]
- Nikaido, T.; Tanino, Y.; Wang, X.; Sato, S.; Misa, K.; Fukuhara, N.; Sato, Y.; Fukuhara, A.; Uematsu, M.; Suzuki, Y.; et al. Serum Syndecan-4 as a possible biomarker in patients with acute pneumonia. J. Infect. Dis. 2015, 212, 1500–1508. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Schmidt, E.P.; Li, G.; Li, L.; Fu, L.; Yang, Y.; Overdier, K.H.; Douglas, I.S.; Lindhardt, R.J. The circulating glycosaminoglycan signature of respiratory failure in critically ill adults. J. Biol. Chem. 2014, 289, 8194–8202. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Grundmann, S.; Fink, K.; Rabadzhieva, L.; Bourgeois, N.; Schwab, T.; Moser, M.; Bode, C.; Busch, H.J. Perturbation of the endothelial glycocalyx in post cardiac arrest syndrome. Resuscitation 2012, 83, 715–720. [Google Scholar] [CrossRef]
- Khan, S.A.; Mason, R.W.; Giugliani, R.; Orii, K.; Fukao, T.; Suzuki, Y.; Yamaguchi, S.; Kobayashi, H.; Orii, T.; Tomatsu, S. Glycosaminoglycans analysis in blood and urine of patients with mucopolysaccharidosis. Mol. Genet. Metab. 2018, 125, 44–52. [Google Scholar] [CrossRef]
- Tomatsu, S.; Shimada, T.; Mason, R.W.; Kelly, J.; LaMarr, W.A.; Yasuda, E.; Shibata, Y.; Futatsumori, H.; Montano, A.M.; Yamaguchi, S.; et al. Assay for glycosaminoglycans by Tandem Mass Spectrometry and its applications. J. Anal. Bioanal. Technol. 2014, 2014 (Suppl. 2), 6. [Google Scholar] [CrossRef]
- Tomatsu, S.; Fujii, T.; Fukushi, M.; Oguma, T.; Shimada, T.; Maeda, M.; Kida, K.; Shibata, Y.; Futatsumori, H.; Montaño, A.M.; et al. Newborn screening and diagnosis of mucopolysaccharidoses. Minireview Mol. Genet Metab. 2013, 110, 42–53. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Kubaski, F.; Suzuki, Y.; Orii, K.; Giugliani, R.; Church, H.J.; Mason, R.W.; Dung, V.C.; Ngoc, C.T.; Yamaguchi, S.; Kobayashi, H.; et al. Glycosaminoglycan levels in dried blood spots of patients with mucopolysaccharidoses and mucolipidoses. Mol. Genet. Metab. 2017, 120, 247–254. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Shimada, T.; Tomatsu, S.; Mason, R.W.; Yasuda, E.; Mackenzie, W.G.; Hossain, J.; Shibata, Y.; Montano, A.M.; Kubaski, F.; Giugliani, R.; et al. Di-sulfated keratan sulfate as a novel biomarker for mucopolysaccharidosis II, IVA, and IVB. JIMD Rep. 2015, 21, 1–13. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Shimada, T.; Tomatsu, S.; Yasuda, E.; Mason, R.W.; Mackenzie, W.G.; Shibata, Y.; Kubaski, F.; Giugliani, R.; Yamaguchi, S.; Suzuki, Y.; et al. Chondroitin 6-sulfate as a novel biomarker for mucopolysaccharidosis IVA and VII. JIMD Rep. 2014, 16, 15–24. [Google Scholar] [CrossRef] [Green Version]
- Ligthelm, R.J.; Borzì, V.; Gumprecht, J.; Kawamori, R.; Wenying, Y.; Valensi, P. Importance of observational studies in clinical practice. Clin. Ther. 2007, 29 Pt 1, 1284–1292. [Google Scholar] [CrossRef]
- Celik, B.; Tomatsu, S.C.; Tomatsu, S.; Khan, S.A. Epidemiology of mucopolysaccharidoses update. Diagnostics 2021, 11, 273. [Google Scholar] [CrossRef]
- Nelson, A.; Berkestedt, I.; Bodelsson, M. Circulating glycosaminoglycans species in septic shock. Acta. Anaesthesiol. Scand. 2014, 58, 36–43. [Google Scholar] [CrossRef]
- Scarpa, M.; Lourenço, C.M.; Amartino, H. Epilepsy in mucopolysaccharidosis disorders. Mol. Genet. Metab. 2017, 122, 55–61. [Google Scholar] [CrossRef] [PubMed]
- Okamoto, M.; Sakiyama, J.; Mori, S.; Kurazono, S.; Usui, S.; Hasegawa, M.; Oohira, A. Kainic acid-induced convulsions cause prolonged changes in the chondroitin sulfate proteoglycans neurocan and phosphacan in the limbic structures. Exp. Neurobiol. 2003, 184, 179–195. [Google Scholar] [CrossRef]
- Leistner, C.M.; Gruen-Bernhard, S.; Glebe, D. Role of glycosaminoglycans for binding and infection of hepatitis B virus. Cell Microbiol. 2008, 10, 122–133. [Google Scholar] [CrossRef] [PubMed]
- WuDunn, D.; Spear, P.G. Initial interaction of herpes simplex virus with cells is binding to heparan sulfate. J. Virol. 1989, 63, 52–58. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- DellaValle, B.; Hasseldam, H.; Johansen, F.F.; Iversen, H.K.; Rungby, J.; Hempel, C. Multiple soluble components of the glycocalyx are increased in patient plasma after ischemic stroke. Stroke 2019, 50, 2948–2951. [Google Scholar] [CrossRef]
- Li, J.; Li, J.P.; Zhang, X.; Lu, Z.; Yu, S.P.; Wei, L. Expression of heparanase in vasculature cells and astrocytes of the mouse brain after focal cerebral ischemia. Brain Res. 2012, 1433, 137–144. [Google Scholar] [CrossRef] [Green Version]
- McKeon, R.J.; Schreiber, R.C.; Rudge, J.S.; Silver, J. Reduction of neurite outgrowth in a model of glial scarring following CNS injury is correlated with the expression of inhibitory molecules on reactive astrocytes. J. Neurosci. 1991, 11, 3398–3411. [Google Scholar] [CrossRef] [Green Version]
- Kato, Y.; Hayatsu, N.; Kaneko, M.K.; Ogasawara, S.; Hamano, T.; Takahashi, S.; Nishikawa, R.; Matsutani, M.; Mishima, K.; Narimatsu, H. Increased expression of highly sulfated keratan sulfate synthesized in malignant astrocytic tumors. Biochem. Biophys. Res. Commun. 2006, 369, 1041–1046. [Google Scholar] [CrossRef]
- Leadbeater, W.E.; Gonzalez, A.-M.; Logaras, N.; Berry, M.; Turnbull, J.E.; Logan, A. Intracellular trafficking in neurons and glia of fibroblast growth factor-2, fibroblast growth factor receptor 1 and heparan sulphate proteoglycans in the injured adult rat cerebral cortex. J. Neurochem. 2006, 96, 1189–1200. [Google Scholar] [CrossRef]
- Hippensteel, J.A.; Anderson, B.J.; Orfila, J.E.; McMurtry, S.A.; Dietz, R.M.; Su, G.; Ford, J.A.; Oshima, K.; Yang, Y.; Zhang, F.; et al. Circulating heparan sulfate fragments mediate septic cognitive dysfunction. J. Clin. Investig. 2019, 129, 1779–1784. [Google Scholar] [CrossRef] [Green Version]
- Lukas Martin, L.; Peters, C.; Schmitz, S.; Moellmann, J.; Martincuks, A.; Heussen, N.; Lehrke, M.; Müller-Newen, G.; Marx, G.; Schuerholz, T. Soluble Heparan Sulfate in Serum of Septic Shock Patients Induces Mitochondrial Dysfunction in Murine Cardiomyocytes. Shock 2015, 44, 569–577. [Google Scholar] [CrossRef] [PubMed]
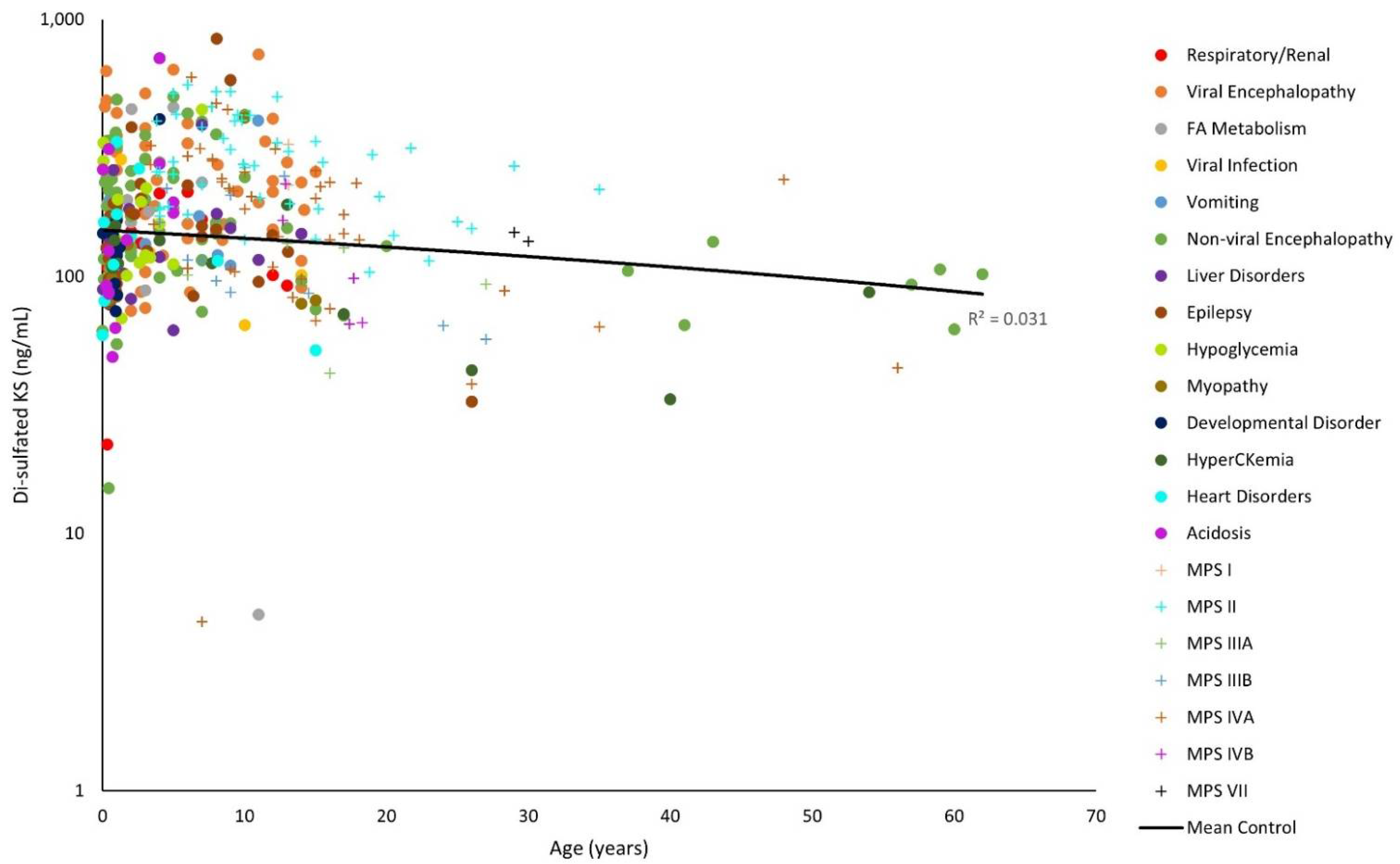
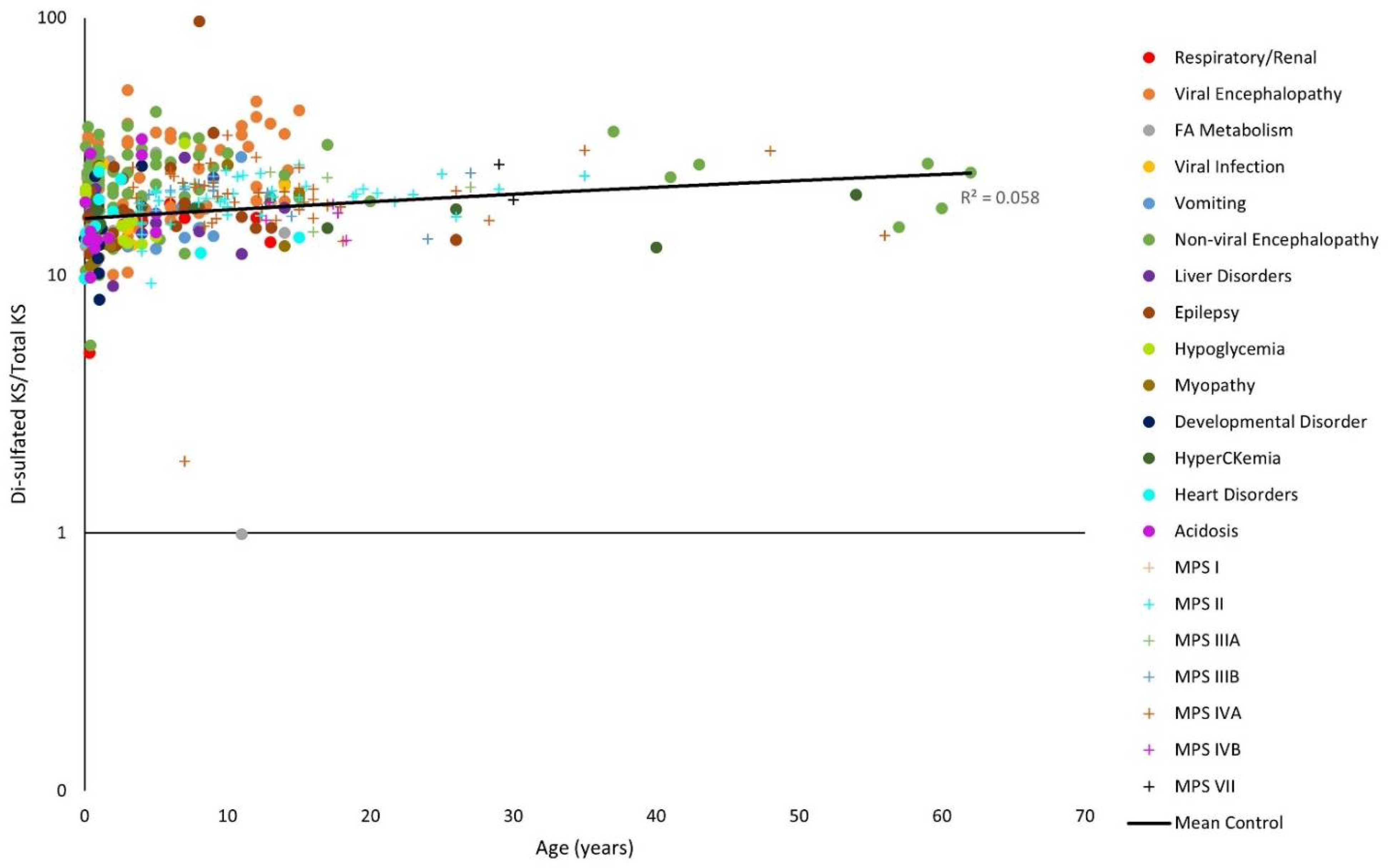
| Diagnosis | Total | 0–2.9 | 3–4.9 | 5–9.9 | 10–14.9 | 15–19.9 | 20+ |
|---|---|---|---|---|---|---|---|
| MPS I | 2 | -- | -- | -- | 2 | -- | -- |
| MPS II | 47 | -- | 7 | 17 | 9 | 7 | 7 |
| MPS IIIA | 6 | -- | -- | 2 | 1 | 2 | 1 |
| MPS IIIB | 11 | -- | 2 | 5 | 2 | -- | 2 |
| MPS IVA | 42 | -- | 3 | 15 | 8 | 11 | 5 |
| MPS IVB | 5 | -- | -- | -- | 2 | 3 | -- |
| MPS VII | 2 | -- | -- | -- | -- | -- | 2 |
| GAG | Total | 0–2.9 | 3–4.9 | 5–9.9 | 10–14.9 | 15–19.9 | 20+ |
|---|---|---|---|---|---|---|---|
| DiHS-0S | 260 | 125 | 33 | 52 | 27 | 8 | 15 |
| DiHS-NS | 274 | 142 | 34 | 49 | 27 | 7 | 15 |
| Di-4S | 283 | 149 | 35 | 57 | 27 | 7 | 8 |
| Mono-sulfated KS | 313 | 166 | 36 | 58 | 32 | 8 | 13 |
| Di-sulfated KS | 282 | 146 | 32 | 50 | 31 | 8 | 15 |
| Di-S KS/Total KS | 264 | 139 | 29 | 47 | 28 | 7 | 14 |
| DiHS-0S | DiHS-NS | Di-4S | Di-Sulfated KS | Mono-Sulfated KS | Di-Sulfated/ Total KS | ||
|---|---|---|---|---|---|---|---|
| Age | Diagnosis | Median (Min, Max) | Median (Min, Max) | Median (Min, Max) | Median (Min, Max) | Median (Min, Max) | Median (Min, Max) |
| 0–2.9 | Control | 74.5 (21, 137) | 11 (1, 28) | 21.4 (2, 40) | 129.1 (15, 285) | 731 (253, 1193) | 14.4 (5, 27) |
| NVE | 116.7 (24, 1129) § | 17.6 (1, 393) § | 26.5 (2, 70) § | 184.1 (15, 488) § | 633.5 (253, 1201) | 21.9 (5, 38) § | |
| VE | 236.1 (40, 928) § | 37.5 (4, 353) § | 38.1 (5, 113) § | 305.3 (74, 630) § | 825.2 (375, 1458) | 23.9 (10, 35) § | |
| MPS I | -- | -- | -- | -- | -- | -- | |
| MPS II | -- | -- | -- | -- | -- | -- | |
| MPS IIIA | -- | -- | -- | -- | -- | -- | |
| MPS IIIB | -- | -- | -- | -- | -- | -- | |
| MPS IVA | -- | -- | -- | -- | -- | -- | |
| MPS IVB | -- | -- | -- | -- | -- | -- | |
| MPS VII | -- | -- | -- | -- | -- | -- | |
| p value | <0.001 * | 0.003 * | <0.001 * | <0.001 * | 0.06 | <0.001 * | |
| 3–4.9 | Control | 62.9 (3, 99) | 7.3 (0, 19) | 20.1 (1, 33) | 143.7 (75, 288) | 687.9 (293, 1199) | 16.2 (10, 29) |
| NVE | 64.7 (58, 189) | 8.9 (5, 28) | 25.1 (15, 41) | 278.5 (99, 355) | 622.4 (400, 853) | 25 (20, 38) § | |
| VE | 64.9 (3, 3227) | 8.9 (0, 1934) | 15.9 (1, 158) | 179.2 (75, 516) | 659.4 (293, 1042) | 18.1 (10, 52) | |
| MPS I | -- | -- | -- | -- | -- | -- | |
| MPS II | 140.5 (65, 222) § | 55 (18, 85) § | 137.3 (6, 223) § | 187.3 (172, 403) | 1306.7 (915, 1879) § | 15.8 (9, 19) | |
| MPS IIIA | -- | -- | -- | -- | -- | -- | |
| MPS IIIB | 258.2 (189, 327) § | 79.7 (53, 106) § | 30.3 (24, 36) | 191.5 (162, 221) | 775.6 (702, 850) | 19.7 (19, 21) | |
| MPS IVA | 38.2 (16, 65) | 9.2 (1, 14) | 2.4 (1, 3) | 272 (160, 323) | 761 (643, 1142) | 22 (20, 26) | |
| MPS IVB | -- | -- | -- | -- | -- | -- | |
| MPS VII | -- | -- | -- | -- | -- | -- | |
| p value | 0.001 * | 0.001 * | 0.002 * | 0.157 | 0.002 * | 0.005 * | |
| 5–9.9 | Control | 63.7 (20, 97) | 7.9 (1, 15) | 19.8 (2, 33) | 160.4 (62, 330) | 694.6 (284, 1068) | 18 (12, 31) |
| NVE | 78 (32, 140) | 14.3 (1, 24) § | 21 (2, 50) | 173.7 (73, 501) | 613.4 (284, 1135) | 26.6 (12, 43) § | |
| VE | 67.2 (30, 123) | 8.8 (3, 33) | 22.5 (16, 33) | 160.4 (87, 639) | 669.9 (405, 1140) | 22.3 (16, 36) § | |
| MPS I | -- | -- | -- | -- | -- | -- | |
| MPS II | 147.9 (35, 393) § | 50.4 (8, 99) § | 89.7 (25, 315) § | 402.3 (174, 557) § | 1556.9 (795, 2198) § | 20.9 (16, 26) | |
| MPS IIIA | 141.8 (93, 190) | 41.3 (30, 52) | 24.1 (16, 32) | 158.6 (102, 216) | 594.7 (401, 788) | 20.8 (20, 22) | |
| MPS IIIB | 131.2 (83, 214) § | 45.1 (23, 75) § | 19.2 (16, 34) | 114.8 (87, 207) | 418.3 (322, 730) | 21.5 (21, 23) | |
| MPS IVA | 35.3 (11, 449) | 5.2 (3, 226) | 2.9 (1, 25) § | 241.2 (5, 595) § | 997 (235, 1860) | 22.6 (2, 27) | |
| MPS IVB | -- | -- | -- | -- | -- | -- | |
| MPS VII | -- | -- | -- | -- | -- | -- | |
| p value | <0.001 * | <0.001 * | <0.001 * | <0.001 * | <0.001 * | 0.015 * | |
| 10–14.9 | Control | 67.2 (8, 97) | 8.2 (4, 13) | 20.1 (1, 28) | 124.8 (5, 283) | 525.8 (218, 840) | 18.7 (1, 39) |
| NVE | 88.2 (13, 159) | 10 (0, 20) | 19.9 (15, 33) | 199 (96, 427) | 638.7 (296, 1006) | 25.7 (20, 30) | |
| VE | 96.5 (62, 827) § | 13.5 (8, 278) § | 48.7 (18, 106) § | 223.2 (91, 731) § | 447.6 (218, 1189) | 33.4 (19, 47) § | |
| MPS I | 55.5 (48, 63) | 9.4 (9, 10) | 2.5 (2, 3) | 277.1 (227, 327) | 1176.6 (973, 1380) | 19 (19, 19) | |
| MPS II | 73.1 (41, 301) | 61.6 (14, 122) § | 48 (27, 398) § | 270.3 (139, 501) § | 1000.6 (613, 2442) § | 20.8 (17, 25) | |
| MPS IIIA | 94.3 (94, 94) | 27.6 (28, 28) | 23 (23, 23) | 135.1 (135, 135) | 401.4 (401, 401) | 25.2 (25, 25) | |
| MPS IIIB | 134.5 (56, 213) | 40 (15, 65) | 19.9 (18, 22) | 166.2 (86, 246) | 675.1 (421, 929) | 19 (17, 21) | |
| MPS IVA | 26.3 (13, 130) | 4.4 (1, 47) | 2.3 (1, 15) § | 163.2 (83, 313) | 534 (270, 1181) | 20.9 (16, 35) | |
| MPS IVB | 26.2 (22, 30) | 5.8 (4, 7) | 2 (2, 2) | 197.3 (165, 229) | 903.9 (842, 966) | 17.8 (16, 19) | |
| MPS VII | -- | -- | -- | -- | -- | -- | |
| p value | 0.004 * | <0.001 * | <0.001 * | 0.037 * | 0.008 * | 0.029 * | |
| 15–19.9 | Control | 41.3 (35, 84) | 6.7 (4, 15) | 16.9 (1, 25) | 73 (52, 256) | 322.8 (149, 469) | 20.1 (14, 32) |
| NVE | 56.2 (35, 78) | 10.7 (7, 15) | 20.2 (16, 25) | 72.5 (70, 75) | 222.7 (149, 297) | 26.1 (20, 32) | |
| VE | 84.4 (84, 84) | 24.5 (24, 24) | 20.8 (21, 21) | 255.6 (256, 256) | 329.2 (329, 329) | 43.7 (44, 44) | |
| MPS I | -- | -- | -- | -- | -- | -- | |
| MPS II | 61.1 (39, 413) | 64.5 (12, 290) § | 50.9 (24, 594) § | 204.9 (104, 335) | 787.4 (380, 1336) § | 20.7 (19, 27) | |
| MPS IIIA | 108.2 (99, 117) | 30.4 (27, 34) | 16.5 (11, 22) | 85.7 (42, 129) | 326.9 (243, 411) | 19.4 (15, 24) | |
| MPS IIIB | -- | -- | -- | -- | -- | -- | |
| MPS IVA | 30.3 (17, 129) | 6.9 (2, 63) | 4.7 (1, 21) | 174.2 (67, 259) | 885.1 (189, 1161) | 18.8 (14, 26) | |
| MPS IVB | 15.7 (13, 18) § | 3.7 (3, 7) | 2.9 (2, 4) | 66.1 (65, 98) | 416.5 (280, 464) | 17.5 (14, 19) | |
| MPS VII | -- | -- | -- | -- | -- | -- | |
| p value | 0.001 * | 0.005 * | 0.001 * | 0.009 * | 0.013 * | 0.141 | |
| 20+ | Control | 45.5 (31, 88) | 6.4 (5, 12) | 15.2 (4, 70) | 86.8 (33, 207) | 280.7 (183, 424) | 18.8 (13, 30) |
| NVE | 52.5 (33, 88) | 9.8 (5, 12) | 43.9 (4, 90) | 103.9 (62, 136) | 296 (186, 547) | 24.6 (15, 36) | |
| VE | -- | -- | -- | -- | -- | -- | |
| MPS I | -- | -- | -- | -- | -- | -- | |
| MPS II | 31.9 (27, 177) | 58.9 (13, 101) § | 25.6 (7, 210) | 163.1 (115, 316) § | 677.5 (444, 1317) § | 20.9 (17, 25) | |
| MPS IIIA | 85.1 (85, 85) | 26.5 (27, 27) | 13.6 (14, 14) | 93.6 (94, 94) | 331 (331, 331) | 22.1 (22, 22) | |
| MPS IIIB | 184.9 (140, 230) | 47.5 (44, 51) | 21.3 (15, 27) | 60.7 (57, 64) | 286.2 (171, 401) | 19.4 (14, 25) | |
| MPS IVA | 39.4 (16, 141) | 12.6 (4, 69) | 4.4 (2, 17) | 63.7 (38, 239) | 265.6 (141, 544) | 21.3 (14, 31) | |
| MPS IVB | -- | -- | -- | -- | -- | -- | |
| MPS VII | 238.6 (37, 440) | 82.6 (8, 157) | 37.7 (13, 62) | 142.9 (137, 148) | 482.2 (402, 562) | 23.3 (20, 27) | |
| p value | 0.302 | 0.003 * | 0.124 | 0.005 * | 0.008 * | 0.765 |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Amendum, P.C.; Khan, S.; Yamaguchi, S.; Kobayashi, H.; Ago, Y.; Suzuki, Y.; Celik, B.; Rintz, E.; Hossain, J.; Xiao, W.; et al. Glycosaminoglycans as Biomarkers for Mucopolysaccharidoses and Other Disorders. Diagnostics 2021, 11, 1563. https://doi.org/10.3390/diagnostics11091563
Amendum PC, Khan S, Yamaguchi S, Kobayashi H, Ago Y, Suzuki Y, Celik B, Rintz E, Hossain J, Xiao W, et al. Glycosaminoglycans as Biomarkers for Mucopolysaccharidoses and Other Disorders. Diagnostics. 2021; 11(9):1563. https://doi.org/10.3390/diagnostics11091563
Chicago/Turabian StyleAmendum, Paige C., Shaukat Khan, Seiji Yamaguchi, Hironori Kobayashi, Yasuhiko Ago, Yasuyuki Suzuki, Betul Celik, Estera Rintz, Jobayer Hossain, Wendi Xiao, and et al. 2021. "Glycosaminoglycans as Biomarkers for Mucopolysaccharidoses and Other Disorders" Diagnostics 11, no. 9: 1563. https://doi.org/10.3390/diagnostics11091563
APA StyleAmendum, P. C., Khan, S., Yamaguchi, S., Kobayashi, H., Ago, Y., Suzuki, Y., Celik, B., Rintz, E., Hossain, J., Xiao, W., & Tomatsu, S. (2021). Glycosaminoglycans as Biomarkers for Mucopolysaccharidoses and Other Disorders. Diagnostics, 11(9), 1563. https://doi.org/10.3390/diagnostics11091563








