Immune-Related Erythema Nodosum Mimicking in Transit Melanoma Metastasis on [18F]-FDG PET/CT
Abstract
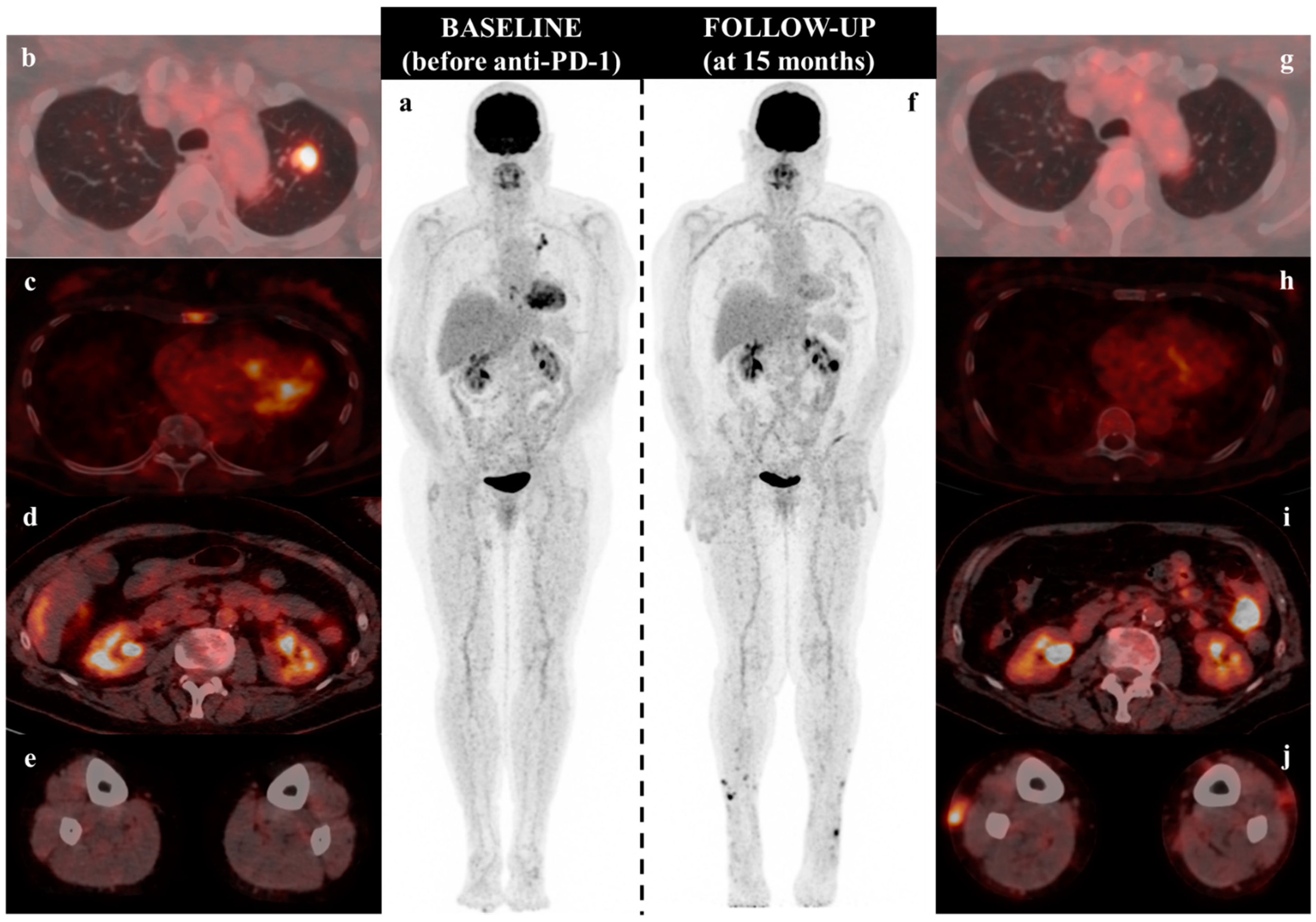
:
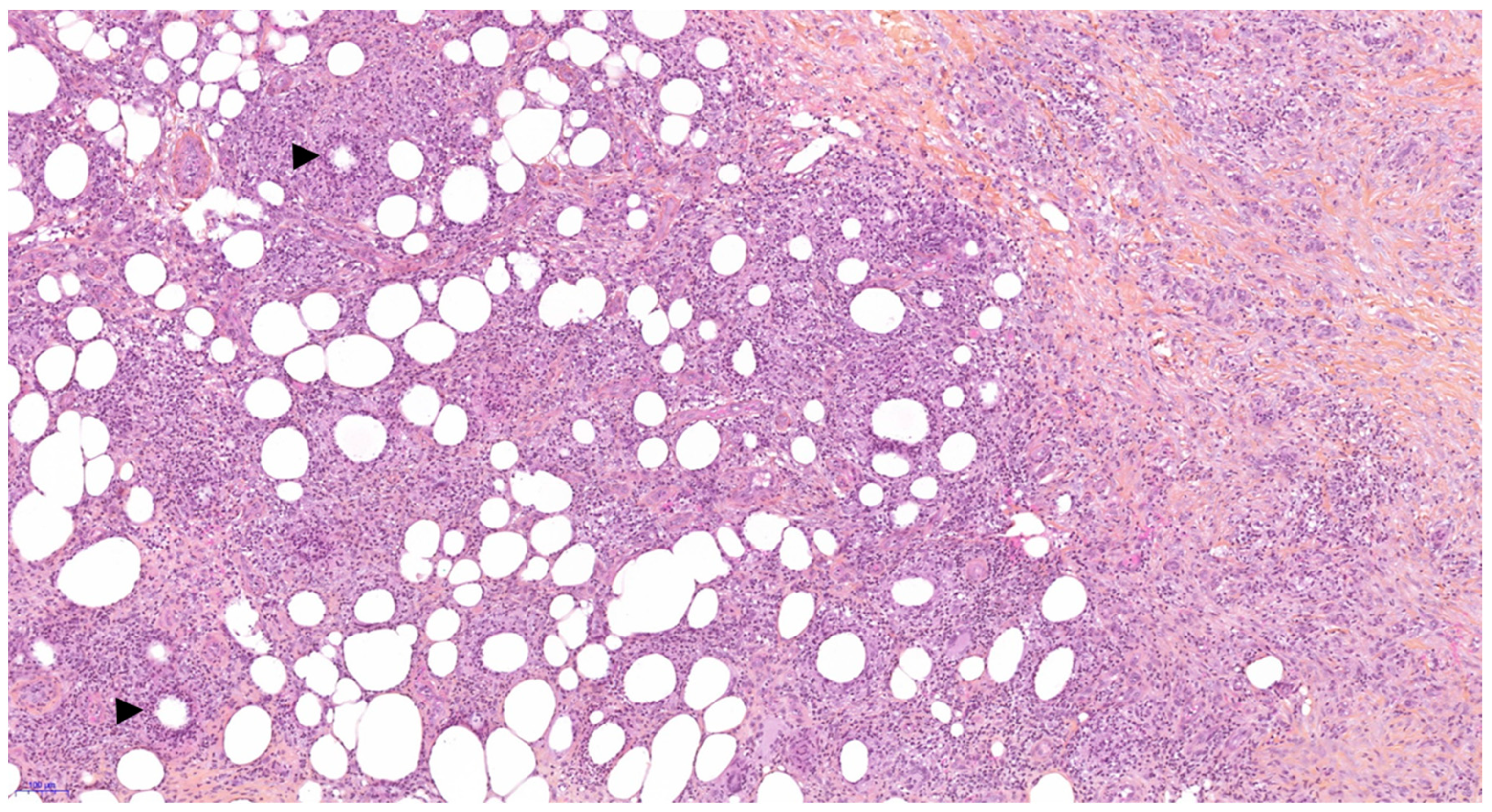
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Paolini, L.; Poli, C.; Blanchard, S.; Urban, T.; Croué, A.; Rousselet, M.-C.; Le Roux, S.; Labarrière, N.; Jeannin, P.; Hureaux, J. Thoracic and cutaneous sarcoid-like reaction associated with anti-PD-1 therapy: Longitudinal monitoring of PD-1 and PD-L1 expression after stopping treatment. J. Immunother. Cancer 2018, 6, 52. [Google Scholar] [CrossRef] [PubMed]
- Choi, M.E.; Lee, K.H.; Won, C.H.; Chang, S.E.; Lee, M.W.; Choi, J.H.; Lee, W.J. A case of erythema nodosum-like panniculitis induced by nivolumab in a patient with oesophageal cancer. Australas. J. Dermatol. 2019, 60, 154–156. [Google Scholar] [CrossRef] [PubMed]
- Laroche, A.; Chinchilla, E.A.; Bourgeault, E.; Doré, M.-A. Erythema Nodosum as the Initial Presentation of Nivolumab-Induced Sarcoidosis-Like Reaction. J. Cutan. Med. Surg. 2018, 22, 627–629. [Google Scholar] [CrossRef] [PubMed]
- Martínez-Rodríguez, I.; García-Castaño, A.; Quirce, R.; Jiménez-Bonilla, J.; Banzo, I. Erythema Nodosum–Like Panniculitis as a False-Positive 18F-FDG PET/CT in Advanced Melanoma Treated with Dabrafenib and Trametinib. Clin. Nucl. Med. 2017, 42, 44–46. [Google Scholar] [CrossRef] [PubMed]
- Tetzlaff, M.T.; Nelson, K.C.; Diab, A.; Staerkel, G.A.; Nagarajan, P.; Torres-Cabala, C.A.; Chasen, B.A.; Wargo, J.A.; Prieto, V.G.; Amaria, R.N.; et al. Granulomatous/sarcoid-like lesions associated with checkpoint inhibitors: A marker of therapy response in a subset of melanoma patients. J. Immunother. Cancer 2018, 6, 14. [Google Scholar] [CrossRef] [PubMed]
- Tetzlaff, M.T.; Jazaeri, A.A.; Torres-Cabala, C.A.; Korivi, B.R.; Landon, G.A.; Nagarajan, P.; Choksi, A.; Chen, L.; Uemura, M.; Aung, P.P.; et al. Erythema nodosum-like panniculitis mimicking disease recurrence: A novel toxicity from immune checkpoint blockade therapy-Report of 2 patients. J. Cutan. Pathol. 2017, 44, 1080–1086. [Google Scholar] [CrossRef] [PubMed]
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Seban, R.-D.; Vermersch, C.; Champion, L.; Bonsang, B.; Roger, A.; Ghidaglia, J. Immune-Related Erythema Nodosum Mimicking in Transit Melanoma Metastasis on [18F]-FDG PET/CT. Diagnostics 2021, 11, 747. https://doi.org/10.3390/diagnostics11050747
Seban R-D, Vermersch C, Champion L, Bonsang B, Roger A, Ghidaglia J. Immune-Related Erythema Nodosum Mimicking in Transit Melanoma Metastasis on [18F]-FDG PET/CT. Diagnostics. 2021; 11(5):747. https://doi.org/10.3390/diagnostics11050747
Chicago/Turabian StyleSeban, Romain-David, Camille Vermersch, Laurence Champion, Benjamin Bonsang, Anissa Roger, and Jerome Ghidaglia. 2021. "Immune-Related Erythema Nodosum Mimicking in Transit Melanoma Metastasis on [18F]-FDG PET/CT" Diagnostics 11, no. 5: 747. https://doi.org/10.3390/diagnostics11050747
APA StyleSeban, R.-D., Vermersch, C., Champion, L., Bonsang, B., Roger, A., & Ghidaglia, J. (2021). Immune-Related Erythema Nodosum Mimicking in Transit Melanoma Metastasis on [18F]-FDG PET/CT. Diagnostics, 11(5), 747. https://doi.org/10.3390/diagnostics11050747





