The Protective Effect of the Crosstalk between Zinc Hair Concentration and Lymphocyte Count—Preliminary Report
Abstract
1. Introduction
2. Materials and Methods
2.1. Patients
2.2. Hair–Scalp Trace Element and Blood Sample Measurements
2.3. Analytical Figures of Merit
2.4. Statistical Analysis
3. Results
3.1. Coronary Artery Group
3.2. Carotid Group
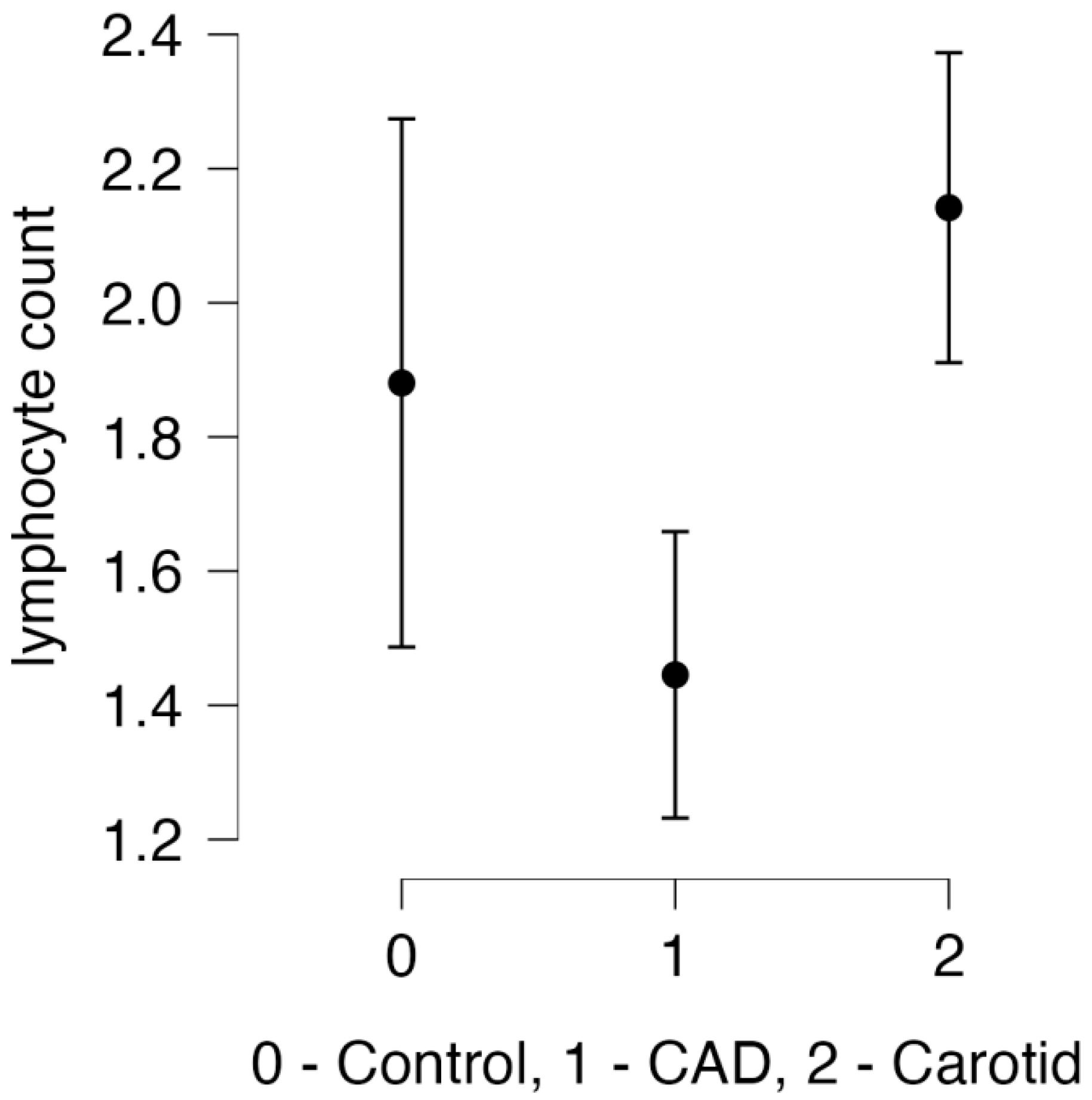
3.3. Laboratory Results
3.4. Trace Elements Results
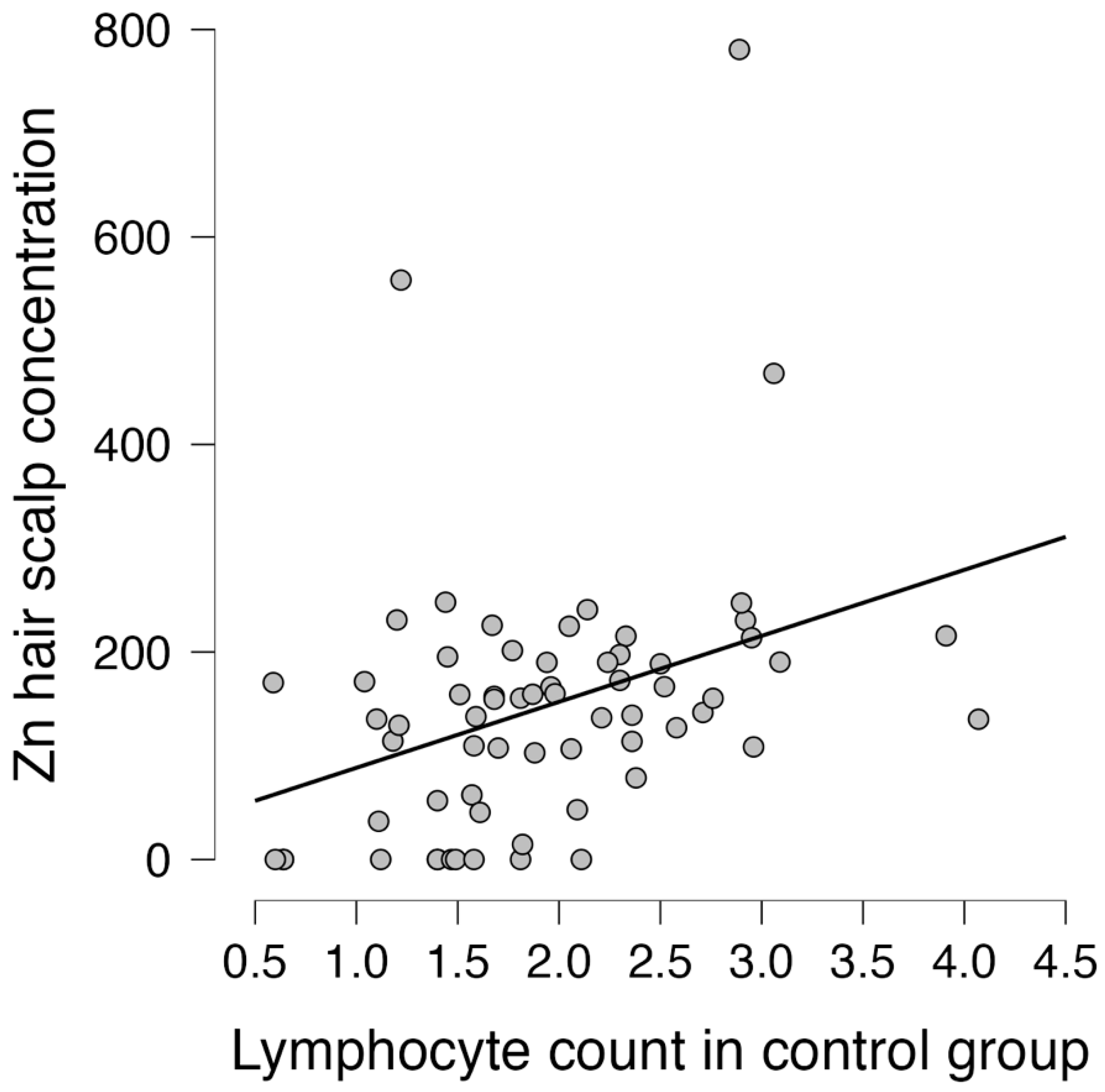
3.5. Correlation between Trace Elements and Lymphocytes
3.6. Multivariable Analysis
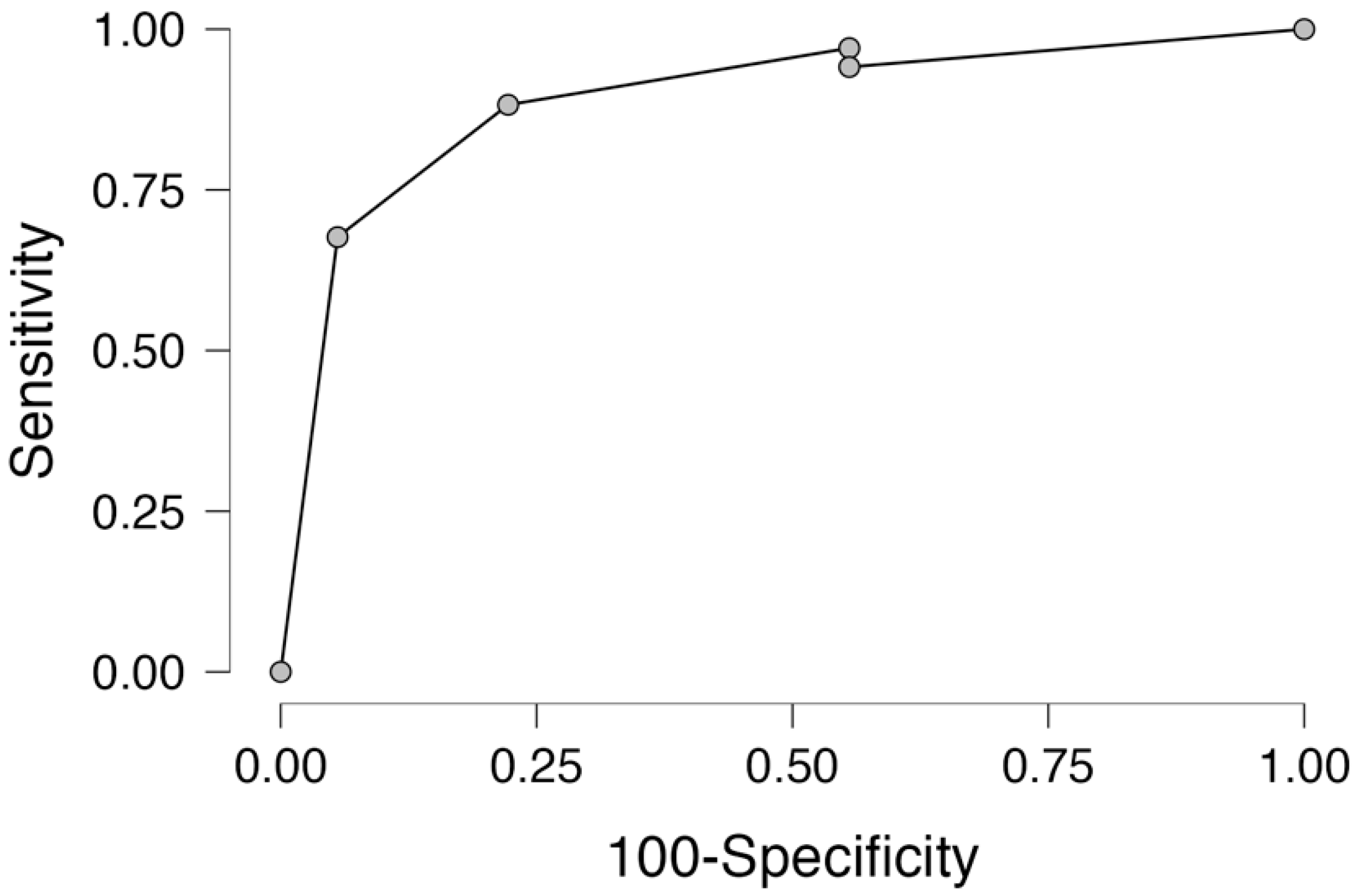
3.7. Receiver Operator Curve Analysis
4. Discussion
5. Study Limitation
6. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Wessels; Fischer, H.J.; Rink, L. Update on the multi-layered levels of zinc-mediated immune regulation. Semin. Cell Dev. Biol. 2021, 115, 62–69. [Google Scholar] [CrossRef] [PubMed]
- Haase, H.; Rink, L. Functional significance of zinc-related signaling pathways in immune cells. Annu. Rev. Nutr. 2009, 29, 133–142. [Google Scholar] [CrossRef] [PubMed]
- Wessels, I.; Maywald, M.; Rink, L. Zinc as a Gatekeeper of Immune Function. Nutrients 2017, 9, 1286. [Google Scholar] [CrossRef] [PubMed]
- Zalewski, P.D.; Beltrame, J.F.; Wawer, A.A.; Abdo, A.I.; Murgia, C. Roles for endothelial zinc homeostasis in vascular physiology and coronary artery disease. Crit. Rev. Food Sci. Nutr. 2019, 21, 213511–213525. [Google Scholar] [CrossRef] [PubMed]
- Alrashidi, H.E.; Alotiby, A.A. Zinc Modulates the Priming of T Helper 1, T Helper 17, and T Regulatory Cells in Allogeneic and Autologous in vitro Models. J. Inflamm. Res. 2022, 30, 6931–6939. [Google Scholar] [CrossRef] [PubMed]
- Liu, F.; Wang, Y.; Yu, J. Role of inflammation and immune response in atherosclerosis: Mechanisms, modulations, and therapeutic targets. Hum. Immunol. 2023, 84, 439–449. [Google Scholar] [CrossRef] [PubMed]
- Laish-Farkash, A.; Sevilya, Z.; Brezinov, O.P.; Fortis, L.; Lev, E. Inflammatory cytokines differ between patients with high versus low CHA2DS2-VASc scores in sinus rhythm-a possible mechanism for adverse cardiovascular events. Int. J. Cardiol. Cardiovasc. Risk Prev. 2022, 15, 200155. [Google Scholar] [CrossRef] [PubMed]
- Aviram, M. Review of human studies on oxidative damage and antioxidant protection related to cardiovascular diseases. Free. Radic. Res. 2000, 33, S85–S97. [Google Scholar] [PubMed]
- Fernandez, D.M.; Giannarelli, C. Immune cell profiling in atherosclerosis: Role in research and precision medicine. Nat. Rev. Cardiol. 2022, 19, 43–58. [Google Scholar] [CrossRef]
- Imazio, M.; Nidorf, M. Colchicine and the heart. Eur. Heart J. 2021, 42, 2745–2760. [Google Scholar] [CrossRef]
- Crea, F.; Libby, P. Acute Coronary Syndromes: The Way Forward from Mechanisms to Precision Treatment. Circulation 2017, 136, 1155–1166. [Google Scholar] [CrossRef] [PubMed]
- Mulvihill, N.T.; Foley, J.B. Inflammation in acute coronary syndromes. Heart 2002, 87, 201–204. [Google Scholar] [CrossRef]
- Lutgens, E.; Atzler, D.; Döring, Y.; Duchene, J.; Steffens, S.; Weber, C. Immunotherapy for cardiovascular disease. Eur. Heart J. 2019, 40, 3937–3946. [Google Scholar] [CrossRef]
- Zernecke, A.; Winkels, H.; Cochain, C.; Williams, J.W.; Wolf, D.; Soehnlein, O.; Robbins, C.S.; Monaco, C.; Park, I.; McNamara, C.A.; et al. Meta-Analysis of Leukocyte Diversity in Atherosclerotic Mouse Aortas. Circ. Res. 2020, 127, 402–426. [Google Scholar] [CrossRef]
- Alsalmi, D.K.; Abdeen, R. Prevalence and Risk Factors of Carotid Artery Stenosis (CAS) among Cardiac Surgery Patients. Cureus 2023, 15, e37634. [Google Scholar] [CrossRef]
- Song, P.; Fang, Z.; Wang, H.; Cai, Y.; Rahimi, K.; Zhu, Y.; Fowkes, F.G.R.; Fowkes, F.J.I.; Rudan, I. Global and regional prevalence, burden, and risk factors for carotid atherosclerosis: A systematic review, meta-analysis, and modelling study. Lancet Glob. Health 2020, 8, e721–e729. [Google Scholar] [CrossRef]
- Abdel Hay, R.; Sayed, K.S.; Hegazi, S.A.; Nada, A.; Amer, M.A. Trichoscopic features of hair and scalp in noncomplaining individuals: A descriptive study. J. Cosmet. Dermatol. 2022, 21, 3934. [Google Scholar] [CrossRef] [PubMed]
- Baj, J.; Kowalska, B.; Barbachowska, A.; Forma, A.; Flieger, M.; Majerek, D.; Teresiński, G.; Flieger, W.; Portincasa, P.; Buszewicz, G.; et al. Linking Metallic Micronutrients and Toxic Xenobiotics to Atherosclerosis and Fatty Liver Disease—Postmortem ICP-MS Analysis of Selected Human Tissues. Nutrients 2023, 15, 3458. [Google Scholar] [CrossRef] [PubMed]
- Urbanowicz, T.; Hanć, A.; Olasińska-Wiśniewska, A.; Rodzki, M.; Witkowska, A.; Michalak, M.; Perek, B.; Haneya, A.; Jemielity, M. Serum copper concentration reflect inflammatory activation in the complex coronary artery disease—A pilot study. J. Trace Elem. Med. Biol. 2022, 74, 127064. [Google Scholar] [CrossRef]
- Hamedifar, Z.; Farrokhian, A.; Reiner, Ž.; Bahmani, F.; Asemi, Z.; Ghotbi, M.; Taghizadeh, M. The effects of combined magnesium and zinc supplementation on metabolic status in patients with type 2 diabetes mellitus and coronary heart disease. Lipids Health Dis. 2020, 19, 112–121. [Google Scholar] [CrossRef]
- Banik, S.; Ghosh, A. Zinc status and coronary artery disease: A systematic review and meta-analysis. J. Trace Elem. Med. Biol. 2022, 73, 127018. [Google Scholar] [CrossRef] [PubMed]
- Meng, H.; Ruan, J.; Chen, Y.; Yan, Z.; Meng, X.; Li, X.; Liu, J.; Mao, C.; Yang, P. Serum Zinc Ion Concentration Associated with Coronary Heart Disease: A Systematic Review and Meta-Analysis. Cardiol. Res. Pr. 2022, 2022, 4352484. [Google Scholar] [CrossRef] [PubMed]
- Liu, M.; Liu, Z.; Zhu, H.; Wang, L.; Yang, H.; Yan, K.; Gong, F.; Pan, H.; Zeng, Y. Serum Zinc-α2-Glycoprotein Levels in Patients with or without Coronary Artery Disease in Chinese North Population. Int. J. Endocrinol. 2020, 2020, 7864721. [Google Scholar] [CrossRef] [PubMed]
- Zhang, D.; Zhu, Y.; Li, H.; Wang, Y.; Niu, Z.; Zhou, W.; Wang, D. Associations of Whole Blood Zinc Levels with Coronary Artery Calcification and Future Cardiovascular Events in CKD Patients. Biol. Trace Elem. Res. 2024, 202, 46–55. [Google Scholar] [CrossRef] [PubMed]
- Mendis, S. Magnesium, zinc, and manganese in atherosclerosis of the aorta. Biol. Trace Elem. Res. 1989, 22, 251–256. [Google Scholar] [CrossRef] [PubMed]
- Stadler, N.; Stanley, N.; Heeneman, S.; Vacata, V.; Daemen, M.J.; Bannon, P.G.; Waltenberger, J.; Davies, M.J. Accumulation of zinc in human atherosclerotic lesions correlates with calcium levels but does not protect against protein oxidation. Arter. Thromb. Vasc. Biol. 2008, 28, 1024–1030. [Google Scholar] [CrossRef] [PubMed]
- Kopriva, D.; Kisheev, A.; Meena, D.; Pelle, S.; Karnitsky, M.; Lavoie, A.; Buttigieg, J. The Nature of Iron Deposits Differs between Symptomatic and Asymptomatic Carotid Atherosclerotic Plaques. PLoS ONE 2015, 10, e0143138. [Google Scholar] [CrossRef]
- Fernandez, D.M.; Rahman, A.H.; Fernandez, N.F.; Chudnovskiy, A.; Amir, E.D.; Amadori, L.; Khan, N.S.; Wong, C.K.; Shamailova, R.; Hill, C.A.; et al. Single-cell immune landscape of human atherosclerotic plaques. Nat. Med. 2019, 25, 1576–1588. [Google Scholar] [CrossRef]
- Li, J.; Ley, K. Lymphocyte migration into atherosclerotic plaque. Arter. Thromb. Vasc. Biol. 2015, 35, 40–49. [Google Scholar] [CrossRef]
- Taylor, C.G.; Giesbrecht, J.A. Dietary zinc deficiency and expression of T lymphocyte signal transduction proteins. Can. J. Physiol. Pharmacol. 2000, 78, 823–828. [Google Scholar] [CrossRef]
- Lepage, L.M.; Giesbrecht, J.A.; Taylor, C.G. Expression of T lymphocyte p56(lck), a zinc-finger signal transduction protein, is elevated by dietary zinc deficiency and diet restriction in mice. J. Nutr. 1999, 129, 620–627. [Google Scholar] [CrossRef] [PubMed]
- Elmadfa, I.; Meyer, A.L. The Role of the Status of Selected Micronutrients in Shaping the Immune Function. Endocr. Metab. Immune Disord. Drug Targets 2019, 19, 1100–1115. [Google Scholar] [CrossRef]
- Jeong, S.Y.; Shim, H.Y.; Lee, Y.J.; Park, B. Association between Copper-Zinc Ratio in Hair and Neutrophil-Lymphocyte Ratio within the Context of a Normal White Blood Cell Count among Overweight or Obese Korean Individuals: A Pilot Study. Korean J. Fam. Med. 2021, 42, 240–244. [Google Scholar] [CrossRef] [PubMed]
- Schmitt, A.K.; Puppa, M.A.; Wessels, I.; Rink, L. Vitamin D3 and zinc synergistically induce regulatory T cells and suppress interferon-γ production in mixed lymphocyte culture. J. Nutr. Biochem. 2022, 102, 108942. [Google Scholar] [CrossRef] [PubMed]
- Tubek, S. Zinc supplementation or regulation of its homeostasis: Advantages and threats. Biol. Trace Elem. Res. 2007, 119, 1–9. [Google Scholar] [CrossRef] [PubMed]
- Rolles, B.; Maywald, M.; Rink, L. Intracellular zinc during cell activation and zinc deficiency. J. Trace Elem. Med. Biol. 2021, 68, 126864. [Google Scholar] [CrossRef]
- Wessels, I.; Fischer, H.J.; Rink, I. Dietary and Physiological Effects of Zinc on the Immune System. Annu. Rev. Nutr. 2021, 41, 133–175. [Google Scholar] [CrossRef]
| Group 1 | Group 2 | Group 3 | p | p | p | |
|---|---|---|---|---|---|---|
| CAD = 13 | Control = 18 | Carotid = 34 | 1–2 | 1–3 | 2–3 | |
| Age (years, median, Q1–Q3) | 70 (59–73) | 66 (61–71) | 68 (64–73) | 1 | 1 | 0.938 |
| BMI (median, Q1–Q3) | 27 (25–29) | 30 (27–34) | 28 (26–30) | 0.689 | 0.945 | 0.756 |
| Sex (M (%), F (%)) | 11 (85)/2 (15) | 10 (56)/8 (44) | 15 (44)/19 (56) | 0.044 * | 0.051 | 0.324 |
| Co-morbidities | ||||||
| HA (n, %) | 13 (100) | 15 (83) | 29 (85) | 0.876 | 0.478 | 0.866 |
| DM (n, %) | 10 (77) | 2 (11) | 9 (26) | 0.027 * | 0.067 | 0.041 * |
| COPD (n, %) | 2 (15) | 0 (0) | 1 (3) | 0.233 | 0.532 | 0.272 |
| Hypercholesterolemia (n, %) | 13 (100) | 12 (67) | 29 (85) | 0.784 | 0.407 | 0.148 |
| Thyroid disease (n, %) | 3 (23) | 2 (11) | 10 (29) | 0.567 | 0.337 | 0.324 |
| AF (n, %) | 5 (38) | 0 (0) | 4 (12) | 0.049 * | 0.058 | 0.155 |
| Smoking history (n, %) | 8 (62) | 8 (44) | 18 (63) | 0.453 | 0.867 | 0.703 |
| Current smoker (n, %) | 5 (38) | 4 (22) | 11 (32) | 0.958 | 0.578 | 0.842 |
| Parameters | Group 1 | Group 2 | Group 3 | p | p | p |
|---|---|---|---|---|---|---|
| (Median (Q1–Q3) | CAD n = 13 | Control n = 18 | Carotid n = 34 | 1–2 | 1–3 | 2–3 |
| Laboratory: | ||||||
| WBC (K/μL) | 8.2 (7.1–8.8) | 8.2 (6.3–9.9) | 8.5 (6.8–9.8) | 1 | 0.956 | 0.986 |
| Neu (K/μL) | 6.0 (4.9–6.6) | 4.6 (3.8–7.3) | 5.3 (4.4–6.9) | 0.974 | 1 | 0.867 |
| Lym (K/μL) | 1.5 (1.2–1.6) | 1.9 (1.4–2.4) | 2.1 (1.6–2.8) | 0.149 | 0.004 * | 0.787 |
| NLR | 3.8 (3.5–4.5) | 2.3 (1.8–3.7) | 2.4 (1.9–3.6) | 0.128 | 0.049 * | 1 |
| SII | 888 (747–1288) | 537 (406–921) | 594 (452–920) | 0.147 | 0.186 | 1 |
| AISI | 358 (314–513) | 317 (147–844) | 240 (169–468) | 1 | 0.352 | 1 |
| Mon (K/μL) | 0.45 (0.4–0.5) | 0.54 (0.40–0.68) | 0.5 (0.4–0.6) | 0.473 | 1 | 0.292 |
| MLR | 0.3 (0.2–0.4) | 0.3 (0.2–0.4) | 0.2 (0.2–0.3) | 1 | 0.06 | 0.206 |
| LUC (K/μL) | 0.10 (0.09–0.12) | 0.13 (0.10–0.15) | 0.16 (0.12–0.19) | 0.318 | 0.003 * | 0.298 |
| Rbc (M/μL) | 4.86 (4.35–5.02) | 4.76 (4.20–5.07) | 4.54 (4.16–4.69) | 1 | 0.122 | 0.537 |
| Hb (mml/L) | 9.0 (8.4–9.2) | 8.8 (8.4–9.8) | 8.7 (8.0–9.3) | 1 | 0.989 | 1 |
| Hct (%) | 43 (40–45) | 43 (41–49) | 41 (38–44) | 1 | 0.728 | 0.141 |
| MCV (fL) | 90 (88–92) | 92 (88–97) | 92 (89–96) | 0.481 | 0.282 | 1 |
| MCHC | 20.7 (20.4–21.1) | 20.4 (20.1–20.7) | 21.0 (20.9–21.3) | 0.475 | 0.088 | <0.001 * |
| RDW (%) | 13.6 (13.1–14.1) | 13.7 (13.4–14.3) | 13.7 (13.3–14.5) | 1 | 1 | 1 |
| Plt (K/uL) | 214 (190–245) | 218 (201–250) | 248 (204–300) | 1 | 0.495 | 0.545 |
| MPV (fL) | 8.2 (7.4–8.7) | 8.7 (8.2–9.4) | 8.2 (7.7–8.7) | 0.181 | 1 | 0.17 |
| Lipid profiles | ||||||
| (median (Q1–Q3): | ||||||
| Total (mmol/L) | 3.99 (3.58–4.58) | 4.1 (3.7–4.2) | 3.69 (3.02–4.00) | 1 | 0.866 | 0.187 |
| HDL (mmol/L) | 1.14 (0.91–1.35) | 1.04 (0.94–1.46) | 1.11 (0.92–1.41) | 1 | 1 | 1 |
| LDL (mmol/L) | 2.43 (2.04–2.75) | 2.34 (1.97–2.61) | 2.25 (1.36–2.62) | 0.967 | 0.897 | 0.901 |
| GFR (median (Q1–Q3) | ||||||
| (mL//min) | 78 (73–86) | 59 (53–76) | 76 (70–85) | 0.234 | 1 | 0.278 |
| Hb1Ac (mean (SD) (%) | 6.2 (0.2) | 6.1 (0.3) | 6.2 (0.3) | 0.921 | 0.978 | 0.967 |
| CRP | ||||||
| (median (Q1–Q3) | 3.5 (2.5–4.0) | 2.0 (1.8–2.3) | 1.9 (1.5–2.4) | 0.125 | 0.098 | 0.93 |
| Trace elements | ||||||
| (median (Q1–Q3): | ||||||
| Cr | 1.65 (1.08–7.56) | 1.86 (1.21–3.61) | 8.3 (5.3–12.7) | 1 | 0.002 * | <0.001 * |
| Mn | 1.19 (0.79–2.09) | 1.09 (0.28–2.09) | 1.14 (0.69–1.83) | 1 | 1 | 1 |
| Fe | 26.9 (15.8–34.9) | 18.6 (9.9–40.7) | 27.9 (17.9–37.4) | 1 | 1 | 0.699 |
| Cu | 17.4 (12.2–21.8) | 23.5 (19.1–32.6) | 52.2 (38.0–80.0) | 0.672 | <0.001 * | 0.013 * |
| Zn | 45.4 (0.0–155.4) | 105.0 (0.0–127) | 190 (155–225) | <0.001 * | <0.001 * | <0.001 * |
| Group 1 CAD n = 13 | Group 2 Control n = 18 | Group 3 Carotid n = 34 | ||||
|---|---|---|---|---|---|---|
| Spearman R | p-Value | Spearman R | p-Value | Spearman R | p-Value | |
| Lymphocyte count and Cr | 0.063 | 0.837 | −0.244 | 0.330 | −0.040 | 0.822 |
| Lymphocyte count and Mn | 0.104 | 0.734 | −0.442 | 0.066 | 0.143 | 0.421 |
| Lymphocyte count and Fe | 0.028 | 0.929 | −0.233 | 0.351 | 0.040 | 0.822 |
| Lymphocyte count and Cu | 0.382 | 0.197 | 0.061 | 0.810 | −0.052 | 0.770 |
| Lymphocyte count and Zn | 0.357 | 0.232 | 0.733 * | <0.001 * | 0.120 | 0.499 |
| Parameters | Univariable Analysis | Multivariable Analysis | ||||
|---|---|---|---|---|---|---|
| OR | 95% CI | p | OR | 95% CI | p | |
| Demographic: | ||||||
| 1. Age | 1.06 | 0.88–1.28 | 0.541 | |||
| 2. Sex | 2.23 | 0.29–17.39 | 0.443 | |||
| Clinical: | ||||||
| 1. Arterial hypertension | 1.33 | 0.08–21.13 | 0.841 | |||
| 2. Diabetes mellitus | 1.36 | 0.21–1.59 | 0.124 | |||
| 3. Hypercholesterolemia | 1.34 | 0.10–18.13 | 0.828 | |||
| 4. Active smoking | 1.18 | 0.74–8.57 | 0.89 | |||
| Hair–scalp trace elements: | ||||||
| 1. Zinc (Zn) | 1.03 | 1.01–10.5 | 0.006 * | 1.03 | 1.01–1.05 | 0.001 * |
| 2. Copper (Cu) | 1.02 | 0.98–1.07 | 0.289 | |||
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2024 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Urbanowicz, T.; Hanć, A.; Tomczak, J.; Michalak, M.; Olasińska-Wiśniewska, A.; Rzesoś, P.; Szot, M.; Filipiak, K.J.; Krasińska, B.; Krasiński, Z.; et al. The Protective Effect of the Crosstalk between Zinc Hair Concentration and Lymphocyte Count—Preliminary Report. Life 2024, 14, 571. https://doi.org/10.3390/life14050571
Urbanowicz T, Hanć A, Tomczak J, Michalak M, Olasińska-Wiśniewska A, Rzesoś P, Szot M, Filipiak KJ, Krasińska B, Krasiński Z, et al. The Protective Effect of the Crosstalk between Zinc Hair Concentration and Lymphocyte Count—Preliminary Report. Life. 2024; 14(5):571. https://doi.org/10.3390/life14050571
Chicago/Turabian StyleUrbanowicz, Tomasz, Anetta Hanć, Jolanta Tomczak, Michał Michalak, Anna Olasińska-Wiśniewska, Patrycja Rzesoś, Mateusz Szot, Krzysztof J. Filipiak, Beata Krasińska, Zbigniew Krasiński, and et al. 2024. "The Protective Effect of the Crosstalk between Zinc Hair Concentration and Lymphocyte Count—Preliminary Report" Life 14, no. 5: 571. https://doi.org/10.3390/life14050571
APA StyleUrbanowicz, T., Hanć, A., Tomczak, J., Michalak, M., Olasińska-Wiśniewska, A., Rzesoś, P., Szot, M., Filipiak, K. J., Krasińska, B., Krasiński, Z., Tykarski, A., & Jemielity, M. (2024). The Protective Effect of the Crosstalk between Zinc Hair Concentration and Lymphocyte Count—Preliminary Report. Life, 14(5), 571. https://doi.org/10.3390/life14050571







