Bias against Vitamin C in Mainstream Medicine: Examples from Trials of Vitamin C for Infections
Abstract
1. Introduction
2. The Karlowski (1975) Trial in JAMA
| Trial [Refs] (1) | Total No. of Episodes | Total Citations from 1997–2020 (2) | Constituent of the Placebo | p for Testing Vitamin C Effect (2-t) |
|---|---|---|---|---|
| Karlowski (1975) [33] | 249 | 109 | Lactose | 0.046 |
| Lewis (1975) [34] (3) | 11 | |||
| Ludvigsson (1977) [51] (4) | 1279 | 20 | not stated (4) | 0.016 |
| Pitt (1979) [52] (5) | 1219 | 31 | citric acid | 0.023 |
| Anderson (1972) [53] (6) | 1170 | 7 | citric acid | 0.001 |
| Total excluding the Karlowski trial | 3668 | 41 | ||
| Hemilä (1996) re-analysis [47] of the Karlowski (1975) trial | 29 |
| Source [Ref.] | Statement |
|---|---|
| Cecil Textbook of Medicine (1996, 2000, 2004) [55,56,57] | “a variety of actually ineffective treatments have been reported to be effective due to inadequate blinding of placebo recipients. One example of this phenomenon was a study of large dose of vitamin C to prevent colds, in which many placebo recipients dropped out of the study because they could tell by tasting the medication that they were not receiving the vitamin C [Karlowski 1975]” |
| Principles and Practice of Infectious Diseases (1979, 1985, 1990, 1995) [58,59,60,61] | “Many participants correctly surmised from the taste of the contents of the capsules used whether they were receiving vitamin C or a placebo (Karlowski 1975)” |
| Textbook of Pediatric Infectious Diseases (1987, 1992, 1998) [62,63,64] | “It is most probable that the reported benefits are a result of statistical artifacts and placebo effect due to poor study design rather than specific pharmacologic drug effects [Karlowski 1975]” |
| Recommended Dietary Allowances, 9th ed (1980) [65] | “Karlowski et al. (1975) found that when those subjects who had guessed the nature of their medication (ascorbic acid or placebo) were eliminated from consideration, the differences between the vitamin and placebo groups were not significant” |
| Evolution of Evidence for Selected Nutrient and Disease Relationships (2002) [66] | “Karlowski and colleagues (1975) conducted a small, double-blind study with 311 employees of the National Institutes of Health and concluded that vitamin C had ‘at best only a minor influence on the duration and severity of colds,’ and ‘the effects demonstrated might be explained equally well by a break in the double blind.’ ” |
| CONSORT statement [67] | “Unblinded outcome adjudicators may differentially assess subjective outcomes…These biases have been well documented” [Karlowski (1975) as one of the references] |
| Cochrane Handbook (1994, 2002, 2004, 2006) [68,69,70,71] | “Some research suggests that such blinding is important in protecting against bias (Karlowski 1975) …there is evidence that participants who are aware of their assignment status report more symptoms, leading to biased results (Karlowski 1975) ...Blinding is likely to be particularly important in research with subjective outcome measures such as pain ...(Karlowski 1975)” |
| Fundamentals of Clinical Trials (1982,1985,1998,2010) [72,73,74,75] | “A trial of the possible benefits of ascorbic acid in the common cold started out as a double-blind study (Karlowski 1975). However, it soon became apparent that many of the participants, most of whom were medical staff, discovered whether they were on ascorbic acid or placebo…Among those participants who claimed not to know the identity of the treatment, ascorbic acid showed no benefit over placebo. In contrast, among participants who knew or suspected what they were on, ascorbic acid did better than placebo. Therefore preconceived notions about the benefit of a treatment, coupled with a subjective response variable, may have yielded biased reporting.” “An evaluation such as that provided by Karlowski and colleagues for a trial of vitamin C is commendable” |
| Clinical Epidemiology (1986, 1996, 2006) [76,77,78] | “Lack of blinding…Because a subject’s suspicion of the group to which he or she had been signed so strongly influenced the results, and because a subject’s suspicion was much more often right than wrong, the validity of the vitamin C-placebo comparison was seriously compromised [in Karlowski 1975]” |
| Clinical and Translational Science: Principles of Human Research (2017) [79] | “Blinding (or masking) is essential in most explanatory trials...examples of incorrect results due to bias in trials without blinding (Karlowski et al., 1975)...reinforce the value of blinding” |
| Principles and Practice of Clinical Research (2007) [80] | “Blinding is essential in most explanatory trials since the opportunity for bias is substantial...Despite the rarity of deceit in clinical research, examples of incorrect results due to bias in trials without blinding (Karlowski 1975) …reinforce the value of blinding” |
| BMJ (1976) [81] | “American study of adult employees of the National Institutes of Health reported in 1975 found no significant prophylactic or therapeutic benefit from ascorbic acid” |
3. Chalmers’ (1975) Review in American Journal of Medicine
| Source [Ref.] | Statement |
|---|---|
| Recommended Dietary Allowances, 10th ed (1989) [88] | “Several reviewers (Chalmers, 1975; Dykes and Meier, 1975) have concluded that any benefits of large doses of ascorbic acid for these conditions are too small to justify recommending routine intake of large amounts by the entire population” |
| Recommended Dietary Allowances, 9th ed (1980) [65] | “several reviewers (Chalmers, 1975; Dykes and Meier, 1975) believe that these benefits of large doses of ascorbic acid are too small to justify recommending routine intake of large amounts by the entire population” |
| American Medical Association (1987) [83] | “One of the most widely misused vitamins is ascorbic acid. There is no reliable evidence that large doses of ascorbic acid prevent colds or shorten their duration [Chalmers 1975]” |
| Principles and Practice of Infectious Diseases (1979, 1985, 1990, 1995) [58,59,60,61] | “Until truly effective and specific treatment becomes available, there will continue to be fads in the use of unproven remedies. The ingestion of large doses of vitamin C has been widely used as a preventive or therapeutic measure for colds. However, a careful analysis of the studies has indicated that a placebo effect could not be ruled out [Chalmers 1975]” |
| Human Nutrition and Dietetics, 10th ed (2000) [89] | “Chalmers (1975) carried out a similar analysis of 14 clinical trials and reported that severity of symptoms was significantly worse in patients who received the placebo. Unfortunately, many volunteers correctly guessed their treatment and when this was taken into account, differences in both the number and severity of colds were minor and insignificant” |
| Human Nutrition and Dietetics, 9th ed (1993) [90] | “... claiming that large daily doses of vitamin C reduced the likelihood of contracting the common cold. The popularity of this concept prompted at least 14 clinical trials, which failed to show an effect of vitamin C (Chalmers 1975)” |
| Nutrition, Concepts and Controversies, 2nd ed (1982), 6th ed (1994) [91,92] | “... in 1975 a physician [Chalmers] reviewed many of them. He found that, statistically, takers of vitamin C did indeed suffer fewer and milder colds than takers of placebos. The difference averaged … one tenth of one day per cold in favor of the vitamin C-takers” |
| Modern Nutrition in Health and Disease, 8th ed (1994) [93] | “The use of megadoses of vitamin C to prevent the common upper respiratory diseases remains an unproven claim. Fourteen studies have been reviewed of which eight were considered acceptable [Chalmers 1975]. Only minor and insignificant effects were noted in terms of the prophylactic benefit of administering megadoses of vitamin C” |
| New England Journal of Medicine (1980) [94] | “Other compounds, such as…vitamin C,…have been extensively studied in vitro and in vivo but have not been proved safe and effective antiviral agents [Chalmers (1975) and Dykes and Meier (1975)]” |
| Journal of the Royal Society of Medicine (2016) [95] | “[Chalmers (1975)] brought together 14 trials of ascorbic acid for the common cold and combined the results from eight of them…All differences in severity and duration were eliminated by analyzing only the data from those who did not know which drug they were taking” |
| Antimicrobial Agents and Chemotherapy (1988) [96] | “One clinical trial of ascorbic acid showed that the apparent benefit in the vitamin C recipients was accounted for by volunteers who had tasted the contents of their capsules and correctly identified the treatment. Reanalysis with omission of these subjects found no evidence of a treatment benefit [Chalmers (1975)]” |
4. Dykes and Meier (1975) Review in JAMA
5. Consequences of the Three 1975 Papers
6. CITRIS-ALI (2019) Trial in JAMA
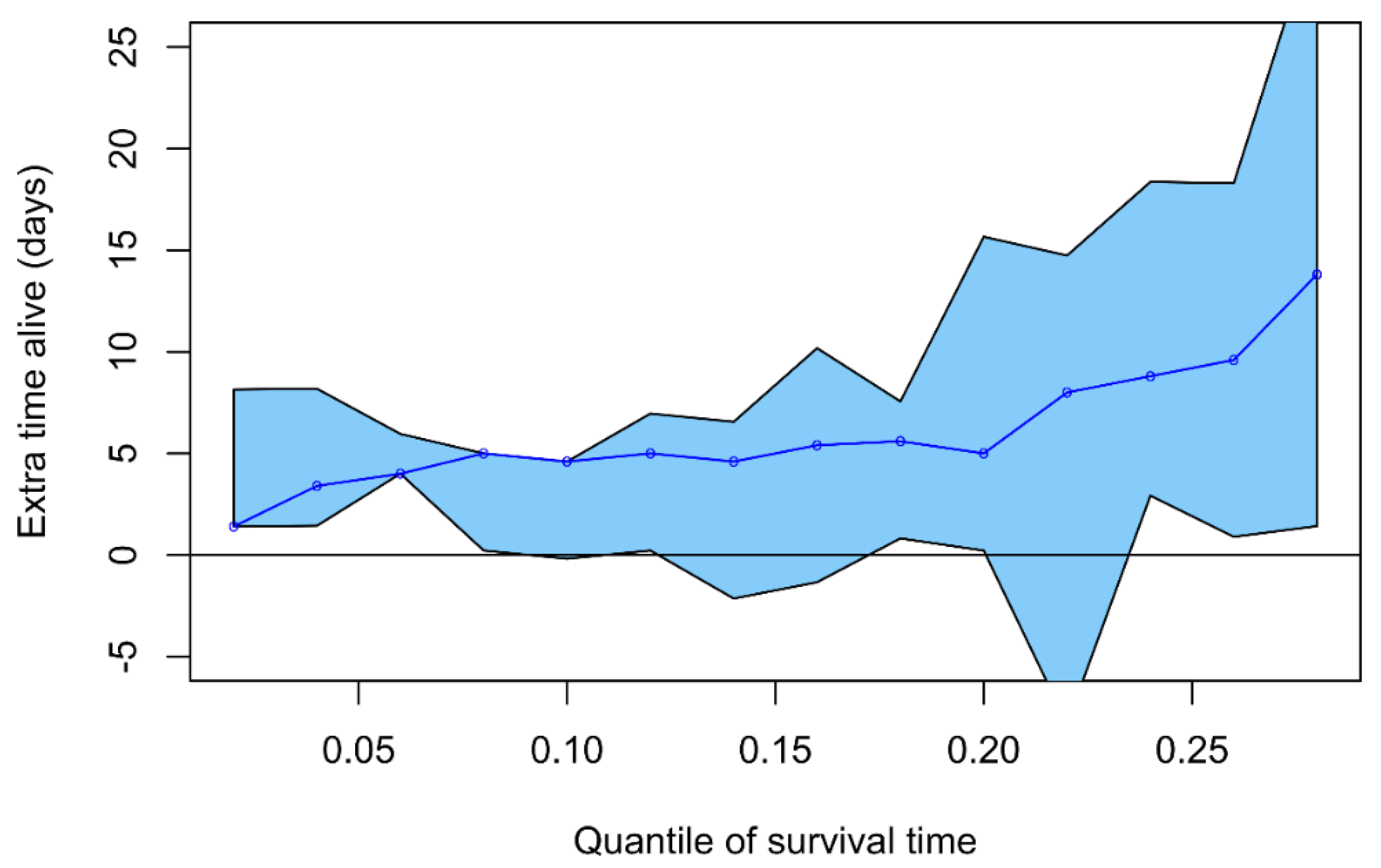
7. COVID-A to Z (2020) Trial in JAMA Network Open
8. Editorial on Vitamin C in JAMA by Brant and Angus
9. Editorial on Vitamin C in JAMA by Michos and Cainzos-Achirica
10. Editorial on Vitamin C in JAMA by Kalil
11. Why Is There Bias against Vitamin C for Conditions Other Than Scurvy?
12. Socio-Political Origins for the Bias against Vitamins
13. Bias against Micronutrients in Academic Medicine
14. The Great Influence of AMA and JAMA
15. Biases on Vitamin C and Cancer
16. Conclusions
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Pauling, L. The significance of the evidence about ascorbic acid and the common cold. Proc. Natl. Acad. Sci. USA 1971, 68, 2678–2681. [Google Scholar] [CrossRef]
- Pauling, L. Ascorbic acid and the common cold. Am. J. Clin. Nutr. 1971, 24, 1294–1299. [Google Scholar] [CrossRef] [PubMed]
- Pauling, L. Vitamin C and the Common Cold; Freeman: San Francisco, CA, USA, 1970. [Google Scholar]
- Hemilä, H.; Chalker, E. Vitamin C for preventing and treating the common cold. Cochrane Database Syst. Rev. 2013, 2013, CD000980. [Google Scholar] [CrossRef]
- Hemilä, H.; Chalker, E. Vitamin C for Preventing and Treating the Common Cold. Available online: http://www.mv.helsinki.fi/home/hemila/CC (accessed on 14 December 2021).
- Shamseer, L.; Vohra, S.; Bax, R.; Spee, L.; Madderom, M.; Hemilä, H. Commentaries on ‘Vitamin C for preventing and treating the common cold’ with responses from the review author. Evid. Based Child Health: A Cochrane Rev. J. 2008, 3, 723–728. [Google Scholar] [CrossRef]
- Hemilä, H. Vitamin C and common cold incidence: A review of studies with subjects under heavy physical stress. Int. J. Sports Med. 1996, 17, 379–383. Available online: https://helda.helsinki.fi/handle/10138/225881 (accessed on 14 December 2021). [CrossRef]
- Hemilä, H. Vitamin C intake and susceptibility to the common cold. Br. J. Nutr. 1997, 77, 59–72. [Google Scholar] [CrossRef]
- Bates, C.J.; Schorah, C.J.; Hemilä, H. Vitamin C intake and susceptibility to the common cold: Invited commentaries. Br. J. Nutr. 1998, 78, 857–866. [Google Scholar] [CrossRef]
- Vorilhon, P.; Arpajou, B.; Vaillant Roussel, H.; Merlin, É.; Pereira, B.; Cabaillot, A. Efficacy of vitamin C for the prevention and treatment of upper respiratory tract infection: A meta-analysis in children. Eur. J. Clin. Pharmacol. 2019, 75, 303–311. [Google Scholar] [CrossRef]
- Padhani, Z.A.; Moazzam, Z.; Ashraf, A.; Bilal, H.; Salam, R.A.; Das, J.K.; Bhutta, Z.A. Vitamin C supplementation for prevention and treatment of pneumonia. Cochrane Database Syst. Rev. 2020, 4, CD013134. [Google Scholar] [CrossRef]
- Cerullo, G.; Negro, M.; Parimbelli, M.; Pecoraro, M.; Perna, S.; Liguori, G.; Rondanelli, M.; Cena, H.; D’Antona, G. The long history of vitamin C: From prevention of the common cold to potential aid in the treatment of COVID-19. Front. Immunol. 2020, 11, 574029. [Google Scholar] [CrossRef]
- Ran, L.; Zhao, W.; Wang, J.; Wang, H.; Zhao, Y.; Tseng, Y.; Bu, H. Extra dose of vitamin C based on a daily supplementation shortens the common cold: A meta-analysis of 9 randomized controlled trials. Biomed. Res. Int. 2018, 2018, 1837634. [Google Scholar] [CrossRef]
- Li, R.; Guo, C.; Li, Y.; Liang, X.; Yang, L.; Huang, W. Therapeutic target and molecular mechanism of vitamin C-treated pneumonia: A systematic study of network pharmacology. Food Funct. 2020, 11, 4765–4772. [Google Scholar] [CrossRef] [PubMed]
- Hui, L.L.; Nelson, E.A.S.; Lin, S.L.; Zhao, J.V. The role of vitamin C in pneumonia and COVID-19 infection in adults with European ancestry: A Mendelian randomisation study. Eur. J. Clin. Nutr. 2021. [Google Scholar] [CrossRef] [PubMed]
- Hemilä, H.; Chalker, E. Meta-analysis on vitamin C and the common cold in children may be misleading. Eur. J. Clin. Pharmacol. 2019, 75, 1747–1748. Available online: https://helda.helsinki.fi/handle/10138/318103 (accessed on 14 December 2021). [CrossRef]
- Hemilä, H.; Chalker, E. Vitamin C and the common cold in children: Severe flaws in the meta-analyses by Vorilhon et al. 2019. Available online: https://helda.helsinki.fi/handle/10138/333365 (accessed on 14 December 2021).
- Vorilhon, P.; Arpajou, B.; Roussel, H.V.; Merlin, É.; Pereira, B.; Cabaillot, A. Retraction Note: Efficacy of vitamin C for the prevention and treatment of upper respiratory tract infection: A meta-analysis in children. Eur. J. Clin. Pharmacol. 2021, 77, 941. [Google Scholar] [CrossRef] [PubMed]
- Hemilä, H.; Chalker, E. Commentary: Vitamin C supplementation for prevention and treatment of pneumonia. Front Med (Lausanne) 2021, 7, 595988. [Google Scholar] [CrossRef]
- Hemilä, H.; Chalker, E. Commentary: The long history of vitamin C: From prevention of the common cold to potential aid in the treatment of COVID-19. Front. Immunol. 2021, 12, 659001. [Google Scholar] [CrossRef]
- Hemilä, H. Shortcomings in the Vitamin C and Common Cold Meta-Analysis by Ran et al. 2018. PubPeer 2021 Mar. Available online: https://pubpeer.com/publications/077EAB95E9141BE6A455C30F0A688E (accessed on 14 December 2021).
- Hemilä, H.; Carr, A. Comment on “Therapeutic target and molecular mechanism of vitamin C-treated pneumonia: A systematic study of network pharmacology” by R. Li, C. Guo, Y. Li, X. Liang, L. Yang and W. Huang. Food Funct. 2021, 12, 1371–1372. [Google Scholar] [CrossRef] [PubMed]
- Hemilä, H.; Chalker, E. Assessment of Vitamin C Effects on Pneumonia and COVID-19 Using Mendelian Randomization: Analysis May Be Misleading. PubPeer 2021 Dec. Available online: https://pubpeer.com/publications/DEB2ADB9FB83E83795C95E8D1FFEB7 (accessed on 14 December 2021).
- Hemilä, H. Do Vitamins C and E Affect Respiratory Infections? Ph.D. Thesis, University of Helsinki, Helsinki, Finland, 2006. Available online: https://helda.helsinki.fi/handle/10138/20335 (accessed on 14 December 2021).
- Hemilä, H. Vitamin C and the common cold. Br. J. Nutr. 1992, 67, 3–16. [Google Scholar] [CrossRef]
- Hemilä, H. Vitamin C supplementation and common cold symptoms: Factors affecting the magnitude of the benefit. Med Hypotheses 1999, 52, 171–178. Available online: https://helda.helsinki.fi/handle/10138/223761 (accessed on 14 December 2021). [CrossRef]
- Hemilä, H. Vitamin C supplementation and respiratory infections: A systematic review. Mil. Med. 2004, 169, 920–925. [Google Scholar] [CrossRef]
- Hemilä, H.; Louhiala, P. Vitamin C may affect lung infections. J. R. Soc. Med. 2007, 100, 495–498. [Google Scholar] [CrossRef]
- Hemilä, H.; Louhiala, P. Vitamin C for preventing and treating pneumonia. Cochrane Database Syst. Rev. 2013, CD005532. Available online: https://helda.helsinki.fi/handle/10138/225862 (accessed on 14 December 2021). [CrossRef]
- Hemilä, H.; Louhiala, P. Vitamin C for Preventing and Treating Pneumonia. Available online: http://www.mv.helsinki.fi/home/hemila/CP (accessed on 14 December 2021).
- Hemilä, H. Vitamin C and common cold-induced asthma: A systematic review and statistical analysis. Allergy Asthma Clin. Immunol. 2013, 9, 46. [Google Scholar] [CrossRef]
- Hemilä, H. Vitamin C and infections. Nutrients 2017, 9, 339. [Google Scholar] [CrossRef]
- Karlowski, T.R.; Chalmers, T.C.; Frenkel, L.D.; Kapikian, A.Z.; Lewis, T.L.; Lynch, J.M. Ascorbic acid for the common cold: A prophylactic and therapeutic trial. JAMA 1975, 231, 1038–1042. [Google Scholar] [CrossRef] [PubMed]
- Lewis, T.L.; Karlowski, T.R.; Kapikian, A.Z.; Lynch, J.M.; Shaffer, G.W.; George, D.A. A controlled clinical trial of ascorbic acid for the common cold. Ann. NY Acad. Sci. 1975, 258, 505–512. [Google Scholar] [CrossRef] [PubMed]
- Liberati, A. Thomas C Chalmers. Lancet 1996, 34, 188. [Google Scholar] [CrossRef]
- Dickersin, K. Thomas Clark Chalmers. JAMA 1996, 276, 656–657. [Google Scholar] [CrossRef]
- Lau, J. Tributes to Thomas Chalmers. Ann. Intern. Med. 1996, 124, 696. [Google Scholar] [CrossRef]
- Huth, E.J. Tributes to Thomas Chalmers. Ann. Intern. Med. 1996, 124, 696. [Google Scholar] [CrossRef]
- Mulrow, C. Tributes to Thomas Chalmers. Ann. Intern. Med. 1996, 124, 696. [Google Scholar] [CrossRef]
- Knatterud, G.; Greenhouse, S.W. Tributes to Dr. Thomas, C. Chalmers. Control. Clin. Trials 1996, 17, 473–475. [Google Scholar] [CrossRef]
- Chalmers, T.C. Dr. Tom Chalmers, 1917–1995: The trials of a randomizer. Interview by Malcolm Maclure. CMAJ 1996, 155, 757–760. [Google Scholar] [PubMed]
- Chalmers, T.C. Dr. Tom Chalmers, 1917–1995: The tribulations of a trialist. Interview by Malcolm Maclure. CMAJ 1996, 155, 986–988. [Google Scholar] [PubMed]
- Sackett, D. A 1955 clinical trial report that changed my career. J. R. Soc. Med. 2010, 103, 254–255. [Google Scholar] [CrossRef] [PubMed]
- Dickersin, K.; Chalmers, F. Thomas C Chalmers (1917-1995): A pioneer of randomised clinical trials and systematic reviews. J. R. Soc. Med. 2015, 108, 237–241. [Google Scholar] [CrossRef]
- Smith, R.; Rennie, D. Evidence based medicine: An oral history. BMJ 2014, 348, g371. [Google Scholar] [CrossRef] [PubMed]
- Chalmers, T.C. To the preceding article by H. Hemilä. J. Clin. Epidemiol. 1996, 49, 1085. [Google Scholar] [CrossRef]
- Hemilä, H. Vitamin C, the placebo effect, and the common cold: A case study of how preconceptions influence the analysis of results. J. Clin. Epidemiol. 1996, 49, 1079–1084. Available online: https://helda.helsinki.fi/handle/10250/8082 (accessed on 14 December 2021). [CrossRef]
- Hemilä, H. Assessment of blinding may be inappropriate after the trial. Contemp. Clin. Trials. 2005, 26, 512–514. Available online: https://helda.helsinki.fi/handle/10138/228099 (accessed on 14 December 2021). [CrossRef] [PubMed]
- Hemilä, H. Analysis of clinical data with breached blindness. Stat. Med. 2006, 25, 1434–1437. Available online: https://helda.helsinki.fi/handle/10138/228098 (accessed on 14 December 2021). [CrossRef]
- Hemilä, H. Assessment of the importance of double-blinding should be based on systematic reviews. J. Thromb. Haemost. 2008, 6, 1247–1248. Available online: https://helda.helsinki.fi/handle/10138/228091 (accessed on 14 December 2021). [CrossRef][Green Version]
- Ludvigsson, J.; Hansson, L.O.; Tibbling, G. Vitamin C as a preventive medicine against common colds in children. Scand. J. Infect. Dis. 1977, 9, 91–98. [Google Scholar] [CrossRef]
- Pitt, H.A.; Costrini, A.M. Vitamin C prophylaxis in marine recruits. JAMA 1979, 241, 908–911. [Google Scholar] [CrossRef] [PubMed]
- Anderson, T.W.; Reid, D.B.; Beaton, G.H. Vitamin C and the common cold: A double-blind trial. Can. Med. Assoc. J. 1972, 107, 503–508. [Google Scholar]
- Hemilä, H. To the dissent by Thomas Chalmers. J. Clin. Epidemiol. 1996, 49, 1087. Available online: https://helda.helsinki.fi/handle/10138/225873 (accessed on 14 December 2021). [CrossRef]
- Hendley, J.O. The common cold. In Cecil Textbook of Medicine, 20th ed.; Bennett, J.C., Blum, F., Eds.; Saunders: Philadelphia, PA, USA, 1996; pp. 1747–1749. [Google Scholar]
- Hendley, J.O. The common cold. In Cecil Textbook of Medicine, 21th ed.; Goldman, L., Bennett, J.C., Eds.; Saunders: Philadelphia, PA, USA, 2000; pp. 1790–1793. [Google Scholar]
- Hendley, J.O. The common cold. In Cecil Textbook of Medicine, 22th ed.; Goldman, L., Bennett, J.C., Eds.; Saunders: Philadelphia, PA, USA, 2004; pp. 1967–1969. [Google Scholar]
- Gwaltney, J.M. The common cold. In Principles and Practice of Infectious Diseases, 1st ed.; Mandell, G.L., Douglas, R.G., Bennett, J.E., Eds.; Churchill Livingstone: New York, NY, USA, 1979; pp. 429–435. [Google Scholar]
- Gwaltney, J.M. The common cold. In Principles and Practice of Infectious Diseases, 2nd ed.; Mandell, G.L., Douglas, R.G., Bennett, J.E., Eds.; Churchill Livingstone: New York, NY, USA, 1985; pp. 351–355. [Google Scholar]
- Gwaltney, J.M. The common cold. In Principles and Practice of Infectious Diseases, 3rd ed.; Mandell, G.L., Douglas, R.G., Bennett, J.E., Eds.; Churchill Livingstone: New York, NY, USA, 1990; pp. 489–493. [Google Scholar]
- Gwaltney, J.M. The common cold. In Principles and Practice of Infectious Diseases, 4th ed.; Mandell, G.L., Bennett, J.E., Dolin, R., Eds.; Churchill Livingstone: New York, NY, USA, 1995; pp. 561–566. [Google Scholar]
- Cherry, J.D. The common cold. In Textbook of Pediatric Infectious Diseases, 2nd ed.; Feigin, R.D., Cherry, J.D., Eds.; Saunders: Philadelphia, PA, USA, 1987; pp. 155–161. [Google Scholar]
- Cherry, J.D. The common cold. In Textbook of Pediatric Infectious Diseases, 3th ed.; Feigin, R.D., Cherry, J.D., Eds.; Saunders: Philadelphia, PA, USA, 1992; pp. 137–142. [Google Scholar]
- Cherry, J.D. The common cold. In Textbook of Pediatric Infectious Diseases, 4th ed.; Feigin, R.D., Cherry, J.D., Eds.; Saunders: Philadelphia, PA, USA, 1998; pp. 128–133. [Google Scholar]
- Food and Nutrition Board, National Research Council. Recommended Dietary Allowances, 9th ed.; National Academy of Sciences: Washington, DC, USA, 1980; pp. 72–82. [Google Scholar]
- Food and Nutrition Board, Institute of Medicine. Evolution of Evidence for Selected Nutrients and Disease Relationships; National Academy Press: Washington, DC, USA, 2002; pp. 36–38. Available online: https://www.ncbi.nlm.nih.gov/books/NBK220648 (accessed on 14 December 2021). [CrossRef]
- Moher, D.; Hopewell, S.; Schulz, K.F.; Montori, V.; Gøtzsche, P.C.; Devereaux, P.J.; Elbourne, D.; Egger, M.; Altman, D.G. CONSORT 2010 Explanation and Elaboration: Updated guidelines for reporting parallel group randomised trials. BMJ 2010, 340, c869. [Google Scholar] [CrossRef] [PubMed]
- Mulrow, C.D.; Oxman, A.D. The Cochrane Handbook 3.0; The Cochrane Collaboration, Update Software: Oxford, UK, 1994. [Google Scholar]
- Clarke, M.; Oxman, A.D. Cochrane Reviewers’ Handbook 4.1; The Cochrane Library: Hoboken, NJ, USA, 2000; pp. 39–40. [Google Scholar]
- Alderson, P.; Green, S.; Higgins, J.P.T. Cochrane Reviewers’ Handbook 4.2.2; The Cochrane Library: Oxford, UK, 2004; p. 52. [Google Scholar]
- Higgins, J.P.T.; Green, S. Cochrane Handbook for Systematic Reviews of Interventions 4.2.6; The Cochrane Library: Hoboken, NJ, USA, 2006; pp. 81–82. [Google Scholar]
- Friedman, L.M.; Furberg, C.D.; DeMets, D.L. Fundamentals of Clinical Trials, 1st ed.; John Wright: Boston, MA, USA, 1982; pp. 59, 206. [Google Scholar]
- Friedman, L.M.; Furberg, C.D.; DeMets, D.L. Fundamentals of Clinical Trials, 2nd ed.; PGN Publishing: Littleton, MA, USA, 1985; pp. 72, 279. [Google Scholar]
- Friedman, L.M.; Furberg, C.D.; DeMets, D.L. Fundamentals of Clinical Trials, 3rd ed.; Springer: New York, NY, USA, 1998; pp. 83, 337. [Google Scholar]
- Friedman, L.M.; Furberg, C.D.; DeMets, D.L. Fundamentals of Clinical Trials, 4th ed.; Springer: New York, NY, USA, 2010; pp. 120, 418. [Google Scholar] [CrossRef]
- Weiss, N.S. Clinical Epidemiology, 1st ed.; University of Oxford: New York, NY, USA, 1986; p. 55. [Google Scholar]
- Weiss, N.S. Clinical Epidemiology, 2nd ed.; University of Oxford: New York, NY, USA, 1996; p. 56. [Google Scholar]
- Weiss, N.S. Clinical Epidemiology, 3rd ed.; University of Oxford: New York, NY, USA, 2006; p. 54. [Google Scholar]
- Califf, R.M. Clinical trials. In Clinical and Translational Science: Principles of Human Research, 2nd ed.; Robertson, D., Williams, G.H., Eds.; Academic Press: Cambridge, MA, USA, 2017; pp. 25–52. [Google Scholar] [CrossRef]
- Califf, R.M. Large clinical trials and registries: Clinical research institutes. In Principles and Practice of Clinical Research, 2nd ed.; Gallin, J.I., Ognibene, F.P., Eds.; Academic Press: Cambridge, MA, USA, 2007; pp. 237–263. [Google Scholar] [CrossRef]
- Editorial. Vitamin C and the common cold. BMJ 1976, 1, 606. [CrossRef]
- Chalmers, T.C. Effects of ascorbic acid on the common cold: An evaluation of the evidence. Am. J. Med. 1975, 58, 532–536. [Google Scholar] [CrossRef]
- American Medical Association, Council of Scientific Affairs. Vitamin preparations as dietary supplements and as therapeutic agents. JAMA 1987, 257, 1929–1936. [Google Scholar] [CrossRef]
- Bastian, H.; Glasziou, P.; Chalmers, I. Seventy-five trials and eleven systematic reviews a day: How will we ever keep up? PLoS Med. 2010, 7, e1000326. [Google Scholar] [CrossRef] [PubMed]
- Hemilä, H. Thomas Chalmers, vitamin C and the common cold. J. R. Soc. Med. 2016, 109, 46. [Google Scholar] [CrossRef]
- Hemilä, H.; Herman, Z.S. Vitamin C and the common cold: A retrospective analysis of Chalmers’ review. J. Am. Coll. Nutr. 1995, 14, 116–123. Available online: https://helda.helsinki.fi/handle/10138/42358 (accessed on 14 December 2021). [CrossRef] [PubMed]
- Cowan, D.; Diehl, H.S.; Baker, A.B. Vitamins for the prevention of colds. JAMA 1942, 120, 1268–1271. [Google Scholar] [CrossRef]
- Food and Nutrition Board, National Research Council. Recommended Dietary Allowances, 10th ed.; National Academy Press: Washington, DC, USA, 1989; pp. 115–125. [Google Scholar] [CrossRef]
- Thurnham, D.I.; Bender, D.A.; Scott, J. Water-soluble vitamins. In Human Nutrition and Dietetics, 10th ed.; Garrow, J.S., James, W.P.T., Ralph, A., Eds.; Churchill Livingstone: London, UK, 2000; pp. 249–287. [Google Scholar]
- Halsted, C.H. Water-soluble vitamins. In Human Nutrition and Dietetics, 9th ed.; Garrow, J.S., James, W.P.T., Eds.; Churchill Livingstone: London, UK, 1993; pp. 239–263. [Google Scholar]
- Hamilton, E.M.N.; Whitney, E.N. Nutrition, Concepts and Controversies, 2nd ed.; West Publishing: New York, NY, USA, 1982; pp. 277–293. [Google Scholar]
- Hamilton, E.M.N.; Whitney, E.N. Nutrition, Concepts and Controversies, 6th ed.; West Publishing: New York, NY, USA, 1994; pp. 403–429. [Google Scholar]
- Shils, M.E.; Olson, J.A.; Shike, M. (Eds.) Modern Nutrition in Health and Disease, 8th ed.; Lea & Febiger: Malvern, PA, USA, 1994; pp. 652–661. [Google Scholar]
- Hirsch, M.S.; Swartz, M.N. Antiviral agents. N. Engl. J. Med. 1980, 302, 949–953. [Google Scholar] [CrossRef] [PubMed]
- Clarke, M. History of evidence synthesis to assess treatment effects: Personal reflections on something that is very much alive. J. R. Soc. Med. 2016, 109, 154–163. [Google Scholar] [CrossRef] [PubMed]
- Sperber, S.J.; Hayden, F.G. Chemotherapy of rhinovirus colds. Antimicrob. Agents Chemother. 1988, 32, 409–419. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Hemilä, H. Many continuous variables such as the duration of the common cold should be analyzed using the relative scale. J. Clin. Epidemiol. 2016, 78, 128–129. Available online: https://helda.helsinki.fi/handle/10138/173096 (accessed on 14 December 2021). [CrossRef]
- Hemilä, H. Duration of the common cold and similar continuous outcomes should be analyzed on the relative scale: A case study of two zinc lozenge trials. BMC Med. Res. Methodol. 2017, 17, 82. [Google Scholar] [CrossRef] [PubMed]
- Friedrich, J.O.; Adhikari, N.K.; Beyene, J. Ratio of means for analyzing continuous outcomes in meta-analysis performed as well as mean difference methods. J. Clin. Epidemiol. 2011, 64, 556–564. [Google Scholar] [CrossRef]
- Hemilä, H. Vitamin C supplementation and common cold symptoms: Problems with inaccurate reviews. Nutrition. 1996, 12, 804–809. Available online: https://helda.helsinki.fi/handle/10138/225877 (accessed on 14 December 2021). [CrossRef]
- Dykes, M.H.; Meier, P. Ascorbic acid and the common cold: Evaluation of its efficacy and toxicity. JAMA 1975, 231, 1073–1079. [Google Scholar] [CrossRef]
- Marks, H.M. A conversation with Paul Meier. Interview by Harry M Marks. Clin. Trials. 2004, 1, 131–138. [Google Scholar] [CrossRef]
- Pincock, S. Paul Meier. Lancet 2011, 378, 978. [Google Scholar] [CrossRef]
- Betts, K. Paul Meier: A man behind the method. Am. J. Public Health 2012, 102, 2026–2029. [Google Scholar] [CrossRef]
- Ritzel, G. Critical evaluation of vitamin C as a prophylactic and therapeutic agent in colds. Helv. Med. Acta. 1961, 28, 63–68. (In German). Available online: http://www.mv.helsinki.fi/home/hemila/T3.pdf (accessed on 14 December 2021). (In German).
- Ritzel, G. Ascorbic acid and the common cold. JAMA 1976, 235, 1108. [Google Scholar] [CrossRef] [PubMed]
- Coulehan, J.L.; Reisinger, K.S.; Rogers, K.D.; Bradley, D.W. Vitamin C prophylaxis in a boarding school. N. Engl. J. Med. 1974, 290, 6–10. [Google Scholar] [CrossRef]
- Pauling, L. Ascorbic acid and the common cold: Evaluation of its efficacy and toxicity. Part I. Med. Trib. 1976, 17, 18–19. Available online: http://www.mv.helsinki.fi/home/hemila/pauling/Pauling_1976_MT_1.pdf (accessed on 14 December 2021).
- Pauling, L. Medical establishment and vitamin C. In Vitamin C, the Common Cold, and the Flu; Freeman: San Francisco, CA, USA, 1976; pp. 121–138. [Google Scholar]
- Pauling, L. Organized medicine and the vitamins. In How to Live Longer and Feel Better; Freeman: San Francisco, CA, USA, 1986; pp. 225–236. [Google Scholar]
- Pauling, L. Ascorbic acid and the common cold. Part II. Medical Tribune 1976, 17, 37–38. Available online: http://www.mv.helsinki.fi/home/hemila/pauling/Pauling_1976_MT_2.pdf (accessed on 14 December 2021).
- Hemilä, H. Vitamin C supplementation and the common cold: Was Linus Pauling right or wrong? Int. J. Vitam. Nutr. Res. 1997, 67, 329–335. Available online: https://helda.helsinki.fi/handle/10250/7980 (accessed on 14 December 2021). [PubMed]
- Wilson, J.X.; Wu, F. Vitamin C in sepsis. Subcell. Biochem. 2012, 56, 67–83. [Google Scholar] [CrossRef] [PubMed]
- Fisher, B.J.; Kraskauskas, D.; Martin, E.J.; Farkas, D.; Wegelin, J.A.; Brophy, D.; Ward, K.R.; Voelkel, N.F.; Fowler, A.A.; Natarajan, R. Mechanisms of attenuation of abdominal sepsis induced acute lung injury by ascorbic acid. Am. J. Physiol. Lung Cell. Mol. Physiol. 2012, 303, L20–L32. [Google Scholar] [CrossRef]
- Fowler, A.A.; Truwit, J.D.; Hite, R.D.; Morris, P.E.; DeWilde, C.; Priday, A.; Fisher, B.; Thacker, L.R.; Natarajan, R.; Brophy, D.F.; et al. Effect of vitamin C infusion on organ failure and biomarkers of inflammation and vascular injury in patients with sepsis and severe acute respiratory failure: The CITRIS-ALI randomized clinical trial. JAMA 2019, 322, 1261–1270. [Google Scholar] [CrossRef]
- Hemilä, H.; Chalker, E. Reanalysis of the effect of vitamin C on mortality in the CITRIS-ALI trial: Important findings dismissed in the trial report. Front. Med. 2020, 7, 590853. [Google Scholar] [CrossRef]
- Fowler, A.A. Vitamin C infusion for Treatment in Sepsis Induced Acute Lung Injury (CITRIS-ALI) [Trial Registration; Last Update 2019-10-15]. ClinicalTrials.gov NCT02106975. Available online: https://clinicaltrials.gov/ct2/show/NCT02106975 (accessed on 14 December 2021).
- De Gruttola, V.; Fleming, T.; Lin, D.Y.; Coombs, R. Validating surrogate markers: Are we being naive? J. Infect. Dis. 1997, 175, 237–246. [Google Scholar] [CrossRef]
- Temple, R. Are surrogate markers adequate to assess cardiovascular disease drugs? JAMA 1999, 282, 790–795. [Google Scholar] [CrossRef]
- Grimes, D.A.; Schulz, K.F. Surrogate end points in clinical research: Hazardous to your health. Obstet. Gynecol. 2005, 105, 1114–1118. [Google Scholar] [CrossRef]
- Institute of Medicine. Evaluation of Biomarkers and Surrogate Endpoints in Chronic Disease; National Academies Press: Washington, DC, USA, 2010. [Google Scholar] [CrossRef]
- Hemilä, H.; Suonsyrjä, T. Vitamin C for preventing atrial fibrillation in high risk patients: A systematic review and meta-analysis. BMC Cardiovasc. Disord. 2018, 17, 49. [Google Scholar] [CrossRef]
- Hemilä, H.; Chalker, E. Vitamin C can shorten the length of stay in the ICU: A meta-analysis. Nutrients 2019, 11, 708. [Google Scholar] [CrossRef]
- Zabet, M.H.; Mohammadi, M.; Ramezani, M.; Khalili, H. Effect of high-dose ascorbic acid on vasopressor’s requirement in septic shock. J. Res. Pharm. Pract. 2016, 5, 94–100. [Google Scholar] [CrossRef]
- Montori, V.M.; Guyatt, G.H. Intention-to-treat principle. CMAJ 2001, 165, 1339–1341. [Google Scholar]
- McCoy, C.E. Understanding the intention-to-treat principle in randomized controlled trials. West. J. Emerg. Med. 2017, 18, 1075–1078. [Google Scholar] [CrossRef] [PubMed]
- DeMets, D.L.; Cook, T. Challenges of non-intention-to-treat analyses. JAMA 2019, 321, 145–146. [Google Scholar] [CrossRef] [PubMed]
- De Grooth, H.J.; Elbers, P.W.G.; Vincent, J.L. Vitamin C for sepsis and acute respiratory failure. JAMA 2020, 323, 792. [Google Scholar] [CrossRef]
- Fowler, A.A.; Fisher, B.J.; Kashiouris, M.G. Vitamin C for sepsis and acute respiratory failure: Reply. JAMA 2020, 323, 792–793. [Google Scholar] [CrossRef] [PubMed]
- Marik, P.E.; Payen, D. CITRIS-ALI: How statistics were used to obfuscate the true findings. Anaesth. Crit. Care Pain Med. 2019, 38, 575–577. [Google Scholar] [CrossRef]
- Koenker, R. quantreg: Quantile Regression. 2021. Available online: https://CRAN.R-project.org/package=quantreg (accessed on 14 December 2021).
- Hemilä, H.; de Man, A.M.E. Vitamin C and COVID-19. Front. Med. 2021, 7, 559811. [Google Scholar] [CrossRef]
- Thomas, S.; Patel, D.; Bittel, B.; Wolski, K.; Wang, Q.; Kumar, A.; Il’Giovine, Z.J.; Mehra, R.; McWilliams, C.; Nissen, S.E.; et al. Effect of high-dose zinc and ascorbic acid supplementation vs usual care on symptom length and reduction among ambulatory patients with SARS-CoV-2 infection: The COVID A to Z randomized clinical trial. JAMA Netw. Open. 2021, 4, e210369. [Google Scholar] [CrossRef]
- Hemilä, H.; Carr, A.; Chalker, E. Vitamin C may increase the recovery rate of outpatient cases of SARS-CoV-2 infection by 70%: Reanalysis of the COVID A to Z randomized clinical trial. Front. Immunol. 2021, 12, 674681. [Google Scholar] [CrossRef]
- Villa, J.; Pannu, T.; McWilliams, C.; Kizer, C.; Rosenthal, R.; Higuera, C.; Patel, P. Results of preoperative screening for COVID-19 correlate with the incidence of infection in the general population: A tertiary care experience. Hosp. Pract. 2021, 49, 216–220. [Google Scholar] [CrossRef]
- FDA approves first treatment for COVID-19 [FDA News Release October 22, 2020]. Available online: https://www.fda.gov/news-events/press-announcements/fda-approves-first-treatment-covid-19 (accessed on 14 December 2021).
- Brant, E.B.; Angus, D.C. Is high-dose vitamin C beneficial for patients with sepsis? JAMA 2019, 322, 1257–1258. [Google Scholar] [CrossRef] [PubMed]
- Hemilä, H. Biased editorial on vitamin C in JAMA. PubPeer 2020 October. Available online: https://pubpeer.com/publications/6C1E79E2B8EA7E2DEED9B46C2B717C (accessed on 14 December 2021).
- Pauling, L. Evolution and the need for ascorbic acid. Proc. Natl. Acad. Sci. USA 1970, 67, 1643–1648. [Google Scholar] [CrossRef]
- Cameron, E.; Pauling, L. Supplemental ascorbate in the supportive treatment of cancer: Prolongation of survival times in terminal human cancer. Proc. Natl. Acad. Sci. USA 1976, 73, 3685–3689. [Google Scholar] [CrossRef] [PubMed]
- Cameron, E.; Pauling, L. Supplemental ascorbate in the supportive treatment of cancer: Reevaluation of prolongation of survival times in terminal human cancer. Proc. Natl. Acad. Sci. USA 1978, 75, 4538–4542. [Google Scholar] [CrossRef] [PubMed]
- Cameron, E.; Pauling, L. Experimental studies designed to evaluate the management of patients with incurable cancer. Proc. Natl. Acad. Sci. USA 1978, 75, 6252. [Google Scholar] [CrossRef]
- Cameron, E.; Pauling, L.; Leibovitz, B. Ascorbic acid and cancer: A review. Cancer Res. 1979, 39, 663–681. [Google Scholar]
- Pauling, L. Vitamin C therapy of advanced cancer. N. Engl. J. Med. 1980, 302, 694. [Google Scholar] [CrossRef]
- Pauling, L.; Herman, Z.S. Criteria for the validity of clinical trials of treatments of cohorts of cancer patients based on the Hardin Jones principle. Proc. Natl. Acad. Sci. USA 1989, 86, 6835–6837. [Google Scholar] [CrossRef]
- Michos, E.D.; Cainzos-Achirica, M.C. Supplements for the treatment of mild COVID-19: Challenging health beliefs with science from A to Z. JAMA Netw. Open 2021, 4, e210431. [Google Scholar] [CrossRef]
- Hemilä, H. Misleading Editorial on the COVID A to Z trial. PubPeer 2021 February. Available online: https://pubpeer.com/publications/7C275B4F3B2A74D33320D4D9C37AA3 (accessed on 14 December 2021).
- Jayawardena, R.; Sooriyaarachchi, P.; Chourdakis, M.; Jeewandara, C.; Ranasinghe, P. Enhancing immunity in viral infections, with special emphasis on COVID-19: A review. Diabetes Metab. Syndr. 2020, 14, 367–382. [Google Scholar] [CrossRef]
- Padayatty, S.J.; Sun, H.; Wang, Y.; Riordan, H.D.; Hewitt, S.M.; Katz, A.; Wesley, R.A.; Levine, M. Vitamin C pharmacokinetics: Implications for oral and intravenous use. Ann. Intern. Med. 2004, 140, 533–537. [Google Scholar] [CrossRef]
- Anderson, T.W.; Suranyi, G.; Beaton, G.H. The effect on winter illness of large doses of vitamin C. Can. Med. Assoc. J. 1974, 111, 31–36. [Google Scholar]
- Kalil, A.C. Lack of benefit of high-dose vitamin C, thiamine, and hydrocortisone combination for patients with sepsis. JAMA 2020, 323, 419–420. [Google Scholar] [CrossRef] [PubMed]
- Fujii, T.; Luethi, N.; Young, P.J.; Frei, D.R.; Eastwood, G.M.; French, C.J.; Deane, A.M.; Shehabi, Y.; Hajjar, L.A.; Oliveira, G.; et al. Effect of vitamin C, hydrocortisone, and thiamine vs hydrocortisone alone on time alive and free of vasopressor support among patients with septic shock: The VITAMINS randomized clinical trial. JAMA 2020, 323, 423–431. [Google Scholar] [CrossRef]
- Hemilä, H. Misleading Editorial on Vitamin C in JAMA. PubPeer 2020 October. Available online: https://pubpeer.com/publications/07DCB1F79D50182367BF913CC69004 (accessed on 14 December 2021).
- Hodges, R.E.; Hood, J.; Canham, J.E.; Sauberlich, H.E.; Baker, E.M. Clinical manifestations of ascorbic acid deficiency in man. Am. J. Clin. Nutr. 1971, 24, 432–443. [Google Scholar] [CrossRef]
- Hunt, C.; Chakravorty, N.K.; Annan, G.; Habibzadeh, N.; Schorah, C.J. The clinical effects of vitamin C supplementation in elderly hospitalised patients with acute respiratory infections. Int. J. Vitam. Nutr. Res. 1994, 64, 212–219. Available online: http://www.mv.helsinki.fi/home/hemila/CP/Hunt_1994_ch.pdf (accessed on 14 December 2021). [PubMed]
- Fain, O.; Mathieu, E.; Thomas, M. Scurvy in patients with cancer. BMJ 1998, 316, 1661–1662. [Google Scholar] [CrossRef] [PubMed]
- Teixeira, A.; Carrie, A.S.; Genereau, T.; Herson, S.; Cherin, P. Vitamin C deficiency in elderly hospitalized patients. Am. J. Med. 2001, 111, 502. [Google Scholar] [CrossRef]
- Fain, O.; Paries, J.; Jacquart, B.; Le Moel, G.; Kettaneh, A.; Stirnemann, J.; Heron, C.; Sitbon, M.; Taleb, C.; Letellier, E.; et al. Hypovitaminosis C in hospitalized patients. Eur. J. Intern. Med. 2003, 14, 419–425. [Google Scholar] [CrossRef] [PubMed]
- Mayland, C.R.; Bennett, M.I.; Allan, K. Vitamin C deficiency in cancer patients. Palliat. Med. 2005, 19, 17–20. [Google Scholar] [CrossRef]
- Gan, R.; Eintracht, S.; Hoffer, L.J. Vitamin C deficiency in a university teaching hospital. J. Am. Coll. Nutr. 2008, 27, 428–433. [Google Scholar] [CrossRef]
- Raynaud-Simon, A.; Cohen-Bittan, J.; Gouronnec, A.; Pautas, E.; Senet, P.; Verny, M.; Boddaert, J. Scurvy in hospitalized elderly patients. J. Nutr. Health Aging 2010, 14, 407–410. [Google Scholar] [CrossRef] [PubMed]
- Carr, A.C.; Rosengrave, P.C.; Bayer, S.; Chambers, S.; Mehrtens, J.; Shaw, G.M. Hypovitaminosis C and vitamin C deficiency in critically ill patients despite recommended enteral and parenteral intakes. Crit. Care. 2017, 21, 300. [Google Scholar] [CrossRef]
- Hodges, R.E. What’s new about scurvy? Am. J. Clin. Nutr. 1971, 24, 383–384. [Google Scholar] [CrossRef] [PubMed]
- Ferrón-Celma, I.; Mansilla, A.; Hassan, L.; Garcia-Navarro, A.; Comino, A.M.; Bueno, P.; Ferrón, J.A. Effect of vitamin C administration on neutrophil apoptosis in septic patients after abdominal surgery. J. Surg. Res. 2009, 153, 224–230. [Google Scholar] [CrossRef]
- Fowler, A.A.; Syed, A.A.; Knowlson, S.; Sculthorpe, R.; Farthing, D.; DeWilde, C.; Farthing, C.A.; Larus, T.L.; Martin, E.; Brophy, D.F.; et al. Phase I safety trial of intravenous ascorbic acid in patients with severe sepsis. J. Transl. Med. 2014, 12, 32. [Google Scholar] [CrossRef]
- Nabil Habib, T.; Ahmed, I. Early adjuvant intravenous vitamin C treatment in septic shock may resolve the vasopressor dependence. Int. J. Microbiol. Adv. Immunol. 2017, 5, 77–81. [Google Scholar] [CrossRef]
- Galley, H.F.; Howdle, P.D.; Walker, B.E.; Webster, N.R. The effects of intravenous antioxidants in patients with septic shock. Free. Radic. Biol. Med. 1997, 23, 768–774. [Google Scholar] [CrossRef]
- Schneider, A.; Markowski, A.; Momma, M.; Seipt, C.; Luettig, B.; Hadem, J.; Wilhelmi, M.; Manns, M.P.; Wedemeyer, J. Tolerability and efficacy of a low-volume enteral supplement containing key nutrients in the critically ill. Clin. Nutr. 2011, 30, 599–603. [Google Scholar] [CrossRef] [PubMed]
- Hemilä, H.; Kaprio, J. Modification of the effect of vitamin E supplementation on the mortality of male smokers by age and dietary vitamin C. Am. J. Epidemiol. 2009, 169, 946–953. [Google Scholar] [CrossRef]
- Hemilä, H.; Kaprio, J. Vitamin E supplementation and pneumonia risk in males who initiated smoking at an early age: Effect modification by body weight and dietary vitamin C. Nutr. J. 2008, 7, 33. [Google Scholar] [CrossRef]
- Sample Size Calculator, ClinCalc. Available online: https://clincalc.com/stats/samplesize.aspx (accessed on 14 December 2021).
- Hess, A.F. Scurvy: Past and Present; Lippincott: Philadelphia, PA, USA, 1920; pp. 88, 99. Available online: https://archive.org/details/b29823778/page/n4/mode/2up (accessed on 14 December 2021).
- Hess, A.F. Diet, nutrition and infection. N. Engl. J. Med. 1932, 207, 637–648. [Google Scholar] [CrossRef]
- Clausen, S.W. The influence of nutrition upon resistance to infection. Physiol. Rev. 1934, 14, 309–350. [Google Scholar] [CrossRef]
- Robertson, E.C. The vitamins and resistance to infection. Medicine 1934, 13, 190–206. [Google Scholar] [CrossRef]
- Hochwald, A. Vitamin C in the treatment of croupous pneumonia. Dtsch. Med. Wochensch. R 1937, 63, 182–184. Available online: http://www.mv.helsinki.fi/home/hemila/T8.pdf (accessed on 14 December 2021). (In German). [CrossRef]
- Bohnholtzer, E. Contribution to the question of pneumonia treatment with vitamin C. Dtsch. Med. Wochenschr 1937, 63, 1001–1003. Available online: http://www.mv.helsinki.fi/home/hemila/T7.pdf (accessed on 14 December 2021). (In German). [CrossRef]
- Glazebrook, A.J.; Thomson, S. The administration of vitamin C in a large institution and its effect on general health and resistance to infection. J. Hyg. 1942, 42, 1–19. [Google Scholar] [CrossRef] [PubMed]
- Klenner, F.R. Virus pneumonia and its treatment with vitamin C. South. Med. Surg. 1948, 110, 36–38. [Google Scholar] [PubMed]
- Abbasy, M.A.; Harris, L.J.; Hill, N.G. Vitamin C and infection: Excretion of vitamin C in osteomyelitis. Lancet 1937, 230, 177–180. [Google Scholar] [CrossRef]
- Ruskin, S.L. Calcium cevitamate in the treatment of acute rhinitis. Ann. Otol. Rhinol. Laryngol. 1938, 47, 502–511. [Google Scholar] [CrossRef]
- Markwell, N.W. Vitamin C in the prevention of colds. Med. J. Aust. 1947, 2, 777–778. [Google Scholar] [CrossRef]
- Englard, S.; Seifter, S. The biochemical functions of ascorbic acid. Annu. Rev. Nutr. 1986, 6, 365–406. [Google Scholar] [CrossRef]
- Rice, M.E. Ascorbate regulation and its neuroprotective role in the brain. Trends Neurosci. 2000, 23, 209–216. [Google Scholar] [CrossRef]
- Mandl, J.; Szarka, A.; Bánhegyi, G. Vitamin C: Update on physiology and pharmacology. Br. J. Pharmacol. 2009, 157, 1097–1110. [Google Scholar] [CrossRef]
- May, J.M.; Harrison, F.E. Role of vitamin C in the function of the vascular endothelium. Antioxid. Redox Signal. 2013, 19, 2068–2083. [Google Scholar] [CrossRef] [PubMed]
- Padayatty, S.J.; Levine, M. Vitamin C: The known and the unknown and Goldilocks. Oral Dis. 2016, 22, 463–493. [Google Scholar] [CrossRef]
- Carr, A.C.; Shaw, G.M.; Fowler, A.A.; Natarajan, R. Ascorbate-dependent vasopressor synthesis: A rationale for vitamin C administration in severe sepsis and septic shock? Crit. Care 2015, 19, 418. [Google Scholar] [CrossRef]
- Kumar, D.; Mains, R.E.; Eipper, B.A. 60 YEARS OF POMC: From POMC and α-MSH to PAM, molecular oxygen, copper, and vitamin C. J. Mol. Endocrinol. 2016, 56, T63–T76. [Google Scholar] [CrossRef]
- Young, J.I.; Züchner, S.; Wang, G. Regulation of the epigenome by vitamin C. Annu. Rev. Nutr. 2015, 35, 545–564. [Google Scholar] [CrossRef] [PubMed]
- Lee Chong, T.; Ahearn, E.L.; Cimmino, L. Reprogramming the epigenome with vitamin C. Front. Cell. Dev. Biol. 2019, 7, 128. [Google Scholar] [CrossRef]
- Brabson, J.P.; Leesang, T.; Mohammad, S.; Cimmino, L. Epigenetic regulation of genomic stability by vitamin C. Front. Genet. 2021, 12, 675780. [Google Scholar] [CrossRef] [PubMed]
- Njus, D.; Kelley, P.M.; Tu, Y.J.; Schlegel, H.B. Ascorbic acid: The chemistry underlying its antioxidant properties. Free Radic. Biol. Med. 2020, 159, 37–43. [Google Scholar] [CrossRef]
- Manning, J.; Mitchell, B.; Appadurai, D.A.; Shakya, A.; Pierce, L.J.; Wang, H.; Nganga, V.; Swanson, P.C.; May, J.M.; Tantin, D.; et al. Vitamin C promotes maturation of T-cells. Antioxid. Redox Signal. 2013, 19, 2054–2067. [Google Scholar] [CrossRef] [PubMed]
- Carr, A.C.; Maggini, S. Vitamin C and immune function. Nutrients 2017, 9, 1211. [Google Scholar] [CrossRef]
- Ang, A.; Pullar, J.M.; Currie, M.J.; Vissers, M.C.M. Vitamin C and immune cell function in inflammation and cancer. Biochem. Soc. Trans. 2018, 46, 1147–1159. [Google Scholar] [CrossRef]
- Padayatty, S.J.; Levine, M. Vitamin and mineral supplements in the primary prevention of cardiovascular disease and cancer. Ann. Intern. Med. 2014, 160, 654. [Google Scholar] [CrossRef]
- Merchant, A.T.; Curhan, G.; Bendich, A.; Singh, V.N.; Willett, W.C.; Fawzi, W.W. Vitamin intake is not associated with community-acquired pneumonia in U.S. men. J. Nutr. 2004, 134, 439–444. [Google Scholar] [CrossRef] [PubMed]
- Food and Nutrition Board, Institute of Medicine. Dietary Reference Intakes for Vitamin C, Vitamin E, Selenium and Carotenoids; National Academy Press: Washington, DC, USA, 2000; pp. 95–185. [Google Scholar] [CrossRef]
- Rowe, S.; Carr, A.C. Global vitamin C status and prevalence of deficiency: A cause for concern? Nutrients 2020, 12, 2008. [Google Scholar] [CrossRef]
- Anderson, T.W.; Beaton, G.H.; Corey, P.; Spero, L. Winter illness and vitamin C: The effect of relatively low doses. Can. Med. Assoc. J. 1975, 112, 823–826. [Google Scholar]
- Sesso, H.D.; Buring, J.E.; Christen, W.G.; Kurth, T.; Belanger, C.; MacFadyen, J.; Bubes, V.; Manson, J.E.; Glynn, R.J.; Gaziano, J.M. Vitamins E and C in the prevention of cardiovascular disease in men: The Physicians’ Health Study II randomized controlled trial. JAMA 2008, 300, 2123–2133. [Google Scholar] [CrossRef]
- Schorah, C.J.; Newill, A.; Scott, D.L.; Morgan, D.B. Clinical effects of vitamin C in elderly inpatients with low blood-vitamin C levels. Lancet 1979, 1, 403–405. [Google Scholar] [CrossRef]
- Apple, R.D. Vitamania: Vitamins in American Culture; Rutgers University Press: Hoboken, NJ, USA, 1996. [Google Scholar]
- Gratzer, W. Fruits and nuts. Nature 1996, 383, 589–590. [Google Scholar] [CrossRef]
- Kinsey, J.D. Vitamania: Vitamins in American Culture by Rima, D. Apple. J. Consum. Aff. 1997, 31, 376–380. [Google Scholar]
- Whorton, J.C. Vitamins and science. Pharm. History 1995, 37, 153–154. [Google Scholar]
- Jefferson, J.W. Vitamania: Vitamins in American Culture by Rima D. Apple. Wisconsin Mag. History 1997, 80, 318–319. [Google Scholar]
- White, P.L. Megavitamin therapy. JAMA 1975, 234, 807. [Google Scholar] [CrossRef]
- Pauling, L. Megavitamin therapy. JAMA 1976, 235, 598. [Google Scholar] [CrossRef]
- Goodwin, J.S.; Tangum, M.R. Battling quackery: Attitudes about micronutrient supplements in American academic medicine. Arch. Intern. Med. 1998, 158, 2187–2191. [Google Scholar] [CrossRef]
- Herbert, V.; Jacob, E. Destruction of vitamin B12 by ascorbic acid. JAMA 1974, 230, 241–242. [Google Scholar] [CrossRef]
- Newmark, H.L.; Scheiner, M.S.; Marcus, M.; Prabhudesai, M. Stability of vitamin B12 in the presence of ascorbic acid. Am. J. Clin. Nutr. 1976, 29, 645–649. [Google Scholar] [CrossRef]
- Newmark, H.L.; Scheiner, J.M.; Marcus, M.; Prabhudesai, M. Ascorbic acid and vitamin B12. JAMA 1979, 242, 2319–2320. [Google Scholar] [CrossRef] [PubMed]
- White, P.L. Megavitamin this and megavitamin that. JAMA 1975, 233, 538–539. [Google Scholar] [CrossRef] [PubMed]
- Jukes, T.H. Megavitamin therapy. JAMA 1975, 233, 550–551. [Google Scholar] [CrossRef] [PubMed]
- Sackler, A.M. Megavitamin therapy. JAMA 1975, 234, 806. [Google Scholar] [CrossRef]
- Swann, J.P. The history of efforts to regulate dietary supplements in the USA. Drug Test. Anal. 2016, 8, 271–282. [Google Scholar] [CrossRef]
- Goodwin, J.S.; Goodwin, J.M. Failure to recognize efficacious treatments: A history of salicylate therapy in rheumatoid arthritis. Perspect. Biol. Med. 1981, 25, 78–92. [Google Scholar] [CrossRef]
- Goodwin, J.S.; Goodwin, J.M. The tomato effect: Rejection of highly efficacious therapies. JAMA 1984, 251, 2387–2390. [Google Scholar] [CrossRef]
- Richards, E. The politics of therapeutic evaluation: The vitamin C and cancer controversy. Soc. Stud. Sci. 1988, 18, 653–701. [Google Scholar] [CrossRef]
- Richards, E. Vitamin C and Cancer: Medicine or Politics? St. Martins Press: New York, NY, USA, 1991. [Google Scholar] [CrossRef]
- Segerstråle, U. Beleaguering the cancer establishment: Vitamin C and cancer: Medicine or politics? Science 1992, 255, 613–615. [Google Scholar] [CrossRef]
- Huxtable, R.J. Vitamin C and cancer: Medicine or politics? Trends Pharmacol. Sci. 1992, 13, 82–83. [Google Scholar] [CrossRef]
- Galloway, J. Crusades and rackets. Nature 1991, 353, 125. [Google Scholar] [CrossRef]
- Herxheimer, A. Challenge for clinical trialists. BMJ 1991, 303, 1076. [Google Scholar] [CrossRef]
- McCormick, W.J. Cancer: A collagen disease, secondary to a nutritional deficiency. Arch. Pediatr. 1959, 76, 166–171. [Google Scholar] [PubMed]
- Jaffey, M. Vitamin C and cancer: Examination of the Vale of Leven trial results using broad inductive reasoning. Med. Hypotheses. 1982, 8, 49–84. [Google Scholar] [CrossRef]
- Creagan, E.T.; Moertel, C.G.; O’Fallon, J.R.; Schutt, A.J.; O’Connell, M.J.; Rubin, J.; Frytak, S. Failure of high-dose vitamin C (ascorbic acid) therapy to benefit patients with advanced cancer: A controlled trial. N. Engl. J. Med. 1979, 301, 687–690. [Google Scholar] [CrossRef]
- Moertel, C.G.; Fleming, T.R.; Creagan, E.T.; Rubin, J.; O’Connell, M.J.; Ames, M.M. High-dose vitamin C versus placebo in the treatment of patients with advanced cancer who have had no prior chemotherapy: A randomized double-blind comparison. N Engl. J. Med. 1985, 312, 137–141. [Google Scholar] [CrossRef]
- Levine, M.; Conry-Cantilena, C.; Wang, Y.; Welch, R.W.; Washko, P.W.; Dhariwal, K.R.; Park, J.B.; Lazarev, A.; Graumlich, J.F.; King, J.; et al. Vitamin C pharmacokinetics in healthy volunteers: Evidence for a recommended dietary allowance. Proc. Natl. Acad. Sci. USA 1996, 93, 3704–3709. [Google Scholar] [CrossRef]
- Levine, M.; Padayatty, S.J.; Espey, M.G. Vitamin C: A concentration-function approach yields pharmacology and therapeutic discoveries. Adv. Nutr. 2011, 2, 78–88. [Google Scholar] [CrossRef]
- Chen, Q.; Espey, M.G.; Sun, A.Y.; Pooput, C.; Kirk, K.L.; Krishna, M.C.; Khosh, D.B.; Drisko, J.; Levine, M. Pharmacologic doses of ascorbate act as a prooxidant and decrease growth of aggressive tumor xenografts in mice. Proc. Natl. Acad. Sci. USA 2008, 105, 11105–11109. [Google Scholar] [CrossRef]
- Parrow, N.L.; Leshin, J.A.; Levine, M. Parenteral ascorbate as a cancer therapeutic: A reassessment based on pharmacokinetics. Antioxid Redox Signal. 2013, 19, 2141–2156. [Google Scholar] [CrossRef]
- Wohlrab, C.; Phillips, E.; Dachs, G.U. Vitamin C transporters in cancer: Current understanding and gaps in knowledge. Front. Oncol. 2017, 7, 74. [Google Scholar] [CrossRef]
- Cimmino, L.; Neel, B.G.; Aifantis, I. Vitamin C in stem cell reprogramming and cancer. Trends Cell Biol. 2018, 28, 698–708. [Google Scholar] [CrossRef] [PubMed]
- Shenoy, N.; Creagan, E.; Witzig, T.; Levine, M. Ascorbic acid in cancer treatment: Let the Phoenix fly. Cancer Cell 2018, 34, 700–706. [Google Scholar] [CrossRef]
- Ngo, B.; Van Riper, J.M.; Cantley, L.C.; Yun, J. Targeting cancer vulnerabilities with high-dose vitamin C. Nat. Rev. Cancer 2019, 19, 271–282. [Google Scholar] [CrossRef] [PubMed]
- Mikkelsen, S.U.; Gillberg, L.; Lykkesfeldt, J.; Grønbæk, K. The role of vitamin C in epigenetic cancer therapy. Free Radic. Biol. Med. 2021, 170, 179–193. [Google Scholar] [CrossRef] [PubMed]
- Padayatty, S.J.; Riordan, H.D.; Hewitt, S.M.; Katz, A.; Hoffer, L.J.; Levine, M. Intravenously administered vitamin C as cancer therapy: Three cases. CMAJ 2006, 174, 937–942. [Google Scholar] [CrossRef]
- Hoffer, L.J.; Robitaille, L.; Zakarian, R.; Melnychuk, D.; Kavan, P.; Agulnik, J.; Cohen, V.; Small, D.; Miller, W.H. High-dose intravenous vitamin C combined with cytotoxic chemotherapy in patients with advanced cancer: A phase I-II clinical trial. PLoS ONE 2015, 10, e0120228. [Google Scholar] [CrossRef]
- Ma, Y.; Chapman, J.; Levine, M.; Polireddy, K.; Drisko, J.; Chen, Q. High-dose parenteral ascorbate enhanced chemosensitivity of ovarian cancer and reduced toxicity of chemotherapy. Sci. Transl. Med. 2014, 6, 222ra18. [Google Scholar] [CrossRef]
- Davis, C.; Naci, H.; Gurpinar, E.; Poplavska, E.; Pinto, A.; Aggarwal, A. Availability of evidence of benefits on overall survival and quality of life of cancer drugs approved by European Medicines Agency: Retrospective cohort study of drug approvals 2009-13. BMJ 2017, 359, j4530. [Google Scholar] [CrossRef] [PubMed]
- Prasad, V. Do cancer drugs improve survival or quality of life? BMJ 2017, 359, j4528. [Google Scholar] [CrossRef] [PubMed]
- Cohen, D. Cancer drugs: High price, uncertain value. BMJ 2017, 359, j4543. [Google Scholar] [CrossRef]
- Naci, H.; Davis, C. Inappropriate use of progression-free survival in cancer drug approvals: New drugs should be judged on overall survival or quality of life, preferably both. BMJ 2020, 368, m770. [Google Scholar] [CrossRef]
- Knipschild, P.; Kleijnen, J.; ter Riet, G. Belief in the efficacy of alternative medicine among general practitioners in The Netherlands. Soc. Sci. Med. 1990, 31, 625–626. [Google Scholar] [CrossRef]
- National Center for Complementary and Integrative Health. Complementary, Alternative, or Integrative Health: What’s In a Name? Available online: https://www.nccih.nih.gov/health/complementary-alternative-or-integrative-health-whats-in-a-name (accessed on 14 December 2021).
- National Center for Complementary and Integrative Health. Flu and Colds: In Depth. Available online: https://www.nccih.nih.gov/health/flu-and-colds-in-depth (accessed on 14 December 2021).
- Wieland, L.S.; Manheimer, E.; Berman, B.M. Development and classification of an operational definition of complementary and alternative medicine for the Cochrane Collaboration. Altern. Ther. Health Med. 2011, 17, 50–59. [Google Scholar]
- Louhiala, P.; Hemilä, H. Can CAM treatments be evidence-based? Focus Altern. Complement. Ther. 2014, 19, 84–89. Available online: https://helda.helsinki.fi/handle/10138/228056 (accessed on 14 December 2021). [CrossRef]
| Ascorbic Acid | Placebo | ||||
|---|---|---|---|---|---|
| No. of Subjects | Mean Duration (Days) | No. of Subjects | Mean Duration (Days) | Difference in Duration (Days) | |
| Chalmers (1975) review [82]: | |||||
| Karlowski (1974) | 101 | 6.80 | 89 | 6.30 | +0.50 |
| Correct data [33,34]: | |||||
| Karlowski (1975) | 57 | 5.92 | 46 | 7.14 | −1.22 (p = 0.046) |
| Vitamin C | Placebo | |
|---|---|---|
| Total No. of children | 321 | 320 |
| No. of children ‘never ill on active surveillance’ | 143 | 93 |
| Comparison of groups: | ||
| p (Fisher test) | 0.000058 | |
| p (χ2 test) | 0.000048 | |
| RR (95% CI) | 1.53 (1.24–1.89) | |
| Trial | Mortality in Vitamin C Group, 95% CI of the RR | No. of Participants | Notes | ||
|---|---|---|---|---|---|
| Vitamin C | Control | Total | |||
| Fujii (2020) [152] | 0.69–2.0 | 107 | 104 | 211 | |
| Ferron-Celma (2009) [164] | 0.60–3.7 | 10 | 10 | 20 | |
| Fowler (2014) [165] | 0.32–1.5 | 16 | 8 | 24 | |
| Nabil Habib (2017) [166] | 0.36–1.2 | 50 | 50 | 100 | Not negative (1) |
| Galley (1997) [167] (2) | 0.69–2.1 | 16 | 14 | 30 | 400 mg vit E with vit C |
| Schneider (2011) [168] (2) | 0.37–2.7 | 29 | 29 | 58 | Vit E and other substances with vit C |
| Total participants | 228 | 215 | 443 | ||
| Total participants in actual vitamin C trials (2) | 183 | 172 | 355 | ||
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Hemilä, H.; Chalker, E. Bias against Vitamin C in Mainstream Medicine: Examples from Trials of Vitamin C for Infections. Life 2022, 12, 62. https://doi.org/10.3390/life12010062
Hemilä H, Chalker E. Bias against Vitamin C in Mainstream Medicine: Examples from Trials of Vitamin C for Infections. Life. 2022; 12(1):62. https://doi.org/10.3390/life12010062
Chicago/Turabian StyleHemilä, Harri, and Elizabeth Chalker. 2022. "Bias against Vitamin C in Mainstream Medicine: Examples from Trials of Vitamin C for Infections" Life 12, no. 1: 62. https://doi.org/10.3390/life12010062
APA StyleHemilä, H., & Chalker, E. (2022). Bias against Vitamin C in Mainstream Medicine: Examples from Trials of Vitamin C for Infections. Life, 12(1), 62. https://doi.org/10.3390/life12010062







