Abstract
Aging can be seen as process characterized by accumulation of oxidative stress induced damage. Oxidative stress derives from different endogenous and exogenous processes, all of which ultimately lead to progressive loss in tissue and organ structure and functions. The oxidative stress theory of aging expresses itself in age-related diseases. Aging is in fact a primary risk factor for many diseases and in particular for cardiovascular diseases and its derived morbidity and mortality. Here we highlight the role of oxidative stress in age-related cardiovascular aging and diseases. We take into consideration the molecular mechanisms, the structural and functional alterations, and the diseases accompanied to the cardiovascular aging process.
1. Introduction
One of the main risk factors for cardiovascular diseases (CVD) is aging [1]. CVDs and aging go hand in hand, both from a prevalence perspective and from a cause-and-effect point of view [2]. Aging is inevitable and the role of oxidative stress in this process is undeniable [3]. By 2030, one-fifth of the world population will be over 65 and CVDs rate will rise exponentially [4]. The rise of concomitant comorbidities, such as metabolic syndrome and diabetes will furthermore weight on the sustainability of health care cost and management [5]. The understanding of the mechanisms behind oxidative stress age-related CVD has led to an overturning on prevention [6]. Seeing cardiovascular aging as a modifiable risk factor opens the horizons to prevention in older patients and to a possible beneficial effect on reducing, morbidity, disability, and health care costs [7].
Many CVDs have been associated, in part or completely, with oxidative stress [8,9,10,11]. Intracellular excess production of reactive oxygen species (ROS) is mainly driven by mitochondrial metabolism and by the NOX family enzymes [12]. Although ROS are essential for various cellular functions, DNA, proteins, and lipids are affected negatively by oxidative stress giving various degrees of alterations on signaling pathways, gene expression and overall cell functioning [13,14,15]. Oxidative stress increases throughout the aging process, also interacting intensively with the longevity network and the longevity genes [16]. Overall, this is the oxidative stress theory of aging based on the hypothesis that oxidative based-damage accumulation leads to cellular senescence [17].
This review will shed some light on the role of oxidative stress age-related CVD, first from a molecular and genetic standpoint and then from a pathophysiology and clinical standpoint.
2. Behind the Scenes of Cardiovascular Aging
2.1. Sources of Oxidative Stress and Oxidative Damage
The oxidative stress theory of aging is based on the hypothesis that age-related loss of functions of tissues is due to the accumulation of oxidative damage to macromolecules (DNA, proteins, and lipids) [17]. These damages are mediated by free radicals formed in redox reactions where a reductant product is oxidized donating an electron to an oxidant. Free radicals, like reactive species of oxygen (ROS) and nitrogen (RNS), are generated as products of redox reaction with one or more unpaired electrons in external shell [18]. Our biologic systems have mechanisms to neutralize oxidative stress, but these decline with aging process and this contributing to imbalance between generation and clearance of ROS, increasing ROS-mediated damage [19]. The main endogenous process who generates ROS is oxidative phosphorylation [18]. This is a compound of mitochondrial reactions during electrons from nicotinamide adenine nucleotide (NADH) and flavin adenine dinucleotide (FADH) are processed via four mitochondrial enzymes with formation of adenosine triphosphate (ATP) from adenosine diphosphate (ADP). Electrons lost during the process form superoxide radical that lead functional impairment of tissues damaging macromolecules [20]. Furthermore, superoxide can react with nitric oxide with production of peroxynitrite, a powerful membrane permeable oxidant that inactivate several enzymes though nitration. Superoxide anion can also convert in hydrogen peroxide trough superoxide dismutase. The hydrogen peroxide through Fenton reaction produce highly reactive radical named hydroxyl radical [21]. These ROS produced via mitochondria are the most important for cardiac tissue in consideration of 45% of hearth’s cell volume is formed by mitochondria [22]. These mechanisms are also implicated in age related damage to vasculature [23]. Mitochondrial ROS can activate some transcription factors like NF-kb and AP-1 promoting an inflammatory pathway on tissues [24]. Mitochondria derived ROS produced severe vascular disfunction mediated by the downregulation of Nrf2 (an antioxidant pathway against oxidative stress), the reduction of NO bioavailability, and the increasing production of vasoconstrictor molecules [25]. The oxidation process cause rupture of mitochondrial membranes with the release of pro apoptotic molecules to the cytosol increasing plaque cell apoptosis and plaque fragility, stimulating smooth muscle cell proliferation, and increasing leukocyte adhesion and inflammatory response [16]. ROS generated from NADPH oxidases during inflammatory responses plays an important role in free radical endogenous production [26]. These transmembrane enzymes oxidize NADPH producing NADP and H2O2 whose can diffuse through membranes [27]. The importance of ROS in the host immune response is demonstrated by the fact that people with an inherited deficiency in NOX2 develop chronic granulomatous disease and are enabled to respond in front of common infections. A basal concentration of ROS is indispensable for cellular homeostasis, on the other hand excessive levels of ROS cause damage to cellular macromolecules and it is one of the main mechanisms implicated in aging and CVDs. Endothelial disfunction mediated by NADPH oxidation is suggest by the findings of an improved endothelial vasodilation after NADPH oxidase inhibition with apocynin [28].
Another mechanism of ROS production is NOS uncoupling, caused by BH4 and L-arginine deficiency [29], with consequent increasing production of superoxide anion [30]. Both eNOS and iNOS are subject of uncoupling in absence of the same substrates [31]. Mitochondrial ROS, activation of NADPH oxidases and uncoupling of NOS establish a positive feedback each other causing an increment of ROS concentration [32]. Other sources of exogenous ROS and RNS are air, water, tobacco, alcohol, heavy or transition metals, drugs (e.g., cyclosporine, gentamycin, and others), industrial solvents, cooking (e.g., smoked meat, waste oil, and fat), and radiation, which inside the body are metabolized in free radicals [33].
ROS and RNS, whether they are endogenous or exogenous, cause oxidative modification of each of the major cellular macromolecules (carbohydrates, lipids, proteins, and DNA). Protein carbonyl is formed by Fenton reaction of oxidants with lysine, arginine, proline, and threonine residues of the protein side chains [34]. Carbonyl groups may also derive from the binding of aldehydic lipid oxidation products to lysine, cysteine, or histidine residues called Michael-addition reactions [35]. Reactions between RNS and tyrosine residues free or within polypeptide sequences induce the formation of nitrotyrosine [35]. Low-density lipoproteins (LDL) are the major carriers of cholesterol to body tissues. RNS and ROS have a central role in atherosclerosis development oxidizing low density lipoproteins. In fact, ox-LDL enter the subendothelial spaces and lead the atherosclerosis process forming atheroma, as explained previously. Important targets of lipid peroxidation are poly-unsaturated fatty acids (PUFAs), in particular linoleic and arachidonic acids, trough hydroxyl, and peroxyl radicals. Depending on the type of PUFAs undergoing lipid oxidation, some different reactive aldehydes are produced, such as trans-4-hydroxy-2-nonenal, malondialdehyde, and isoprostanes [36]. The amino groups of lysine and arginine react with the carbonyl groups of carbohydrates in glycoxidation process, results in advanced glycation end products (AGE). Major AGEs are hydroimidazolone, pentosidine, and glucosepane. Oxidative stress is also well known to be implicated in negatively effects on telomeres loss. Telomeres are structures of repeating nucleotides at the end of eukaryotic chromatids that shorten replication after replication. This mechanism protects important genetic data lost by incomplete replication. Telomeres length is determined from unknown genetic factors, but a lot of conditions are associated with their shortening like insulin resistance, hypertension, and oxidative stress [37]. When shortened to critical length telomeres lead cells towards a senescence state. The telomeres deterioration is associated with cardiovascular decline, congestive heart failure and peripheral vascular disease [38]. Advanced biological age is characterized by the accumulation of epigenetic changes that can be correlated with CVDs [39].
The precise mechanism of oxidative stress-induced aging is still not clear. It is well established that elevated ROS levels lead to cellular senescence. This mechanism stops cellular proliferation in response to damages occurring during replication. Senescent cells acquire an irreversible senescence-associated secretory phenotype involving secretion of soluble factors (interleukins, chemokines, and growth factors), degradative enzymes like matrix metalloproteases (MMP), and insoluble proteins/extracellular matrix (ECM) components [40,41]. ROS induces cellular senescence activating many mechanisms, the main are:
- production of IL-1α leading to a proinflammatory state, which increases nuclear factor kappa-β (NFκβ) activity [40];
- induction of MMPs expression, which is associated with age-related and chronic diseases such as cancer, Alzheimer’s, atherosclerosis, osteoarthritis, and lung emphysema [40];
- inhibition of FOXO (Forkhead box) proteins activity, which is involved in insulin/insulin-like growth factor-1-mediated protection from oxidative stress [40];
- reduction of sarco/endoplasmic reticulum Ca2+-ATPase activity leading to cardiac senescence;
- inhibition of sirtuins activity leading to an increased production of ROS and RNS by SOD inhibition, a proinflammatory state by preventing their inhibition of tumor necrosis factor alpha (TNFα) and NFκB, and tumorigenic effect by preventing their inhibitory effect on c-Jun and c-Myc [42];
- regulation of p16INK4a/pRB and p53/p21 pathways leading to senescence [40].
2.2. Aging, Oxidative Stress and Cellular Dysfunction
Age-dependent oxidative stress cellular dysfunction is a condition determined by various intrinsic factors. The heart cell, the cardiomyocytes, exert a high aerobic metabolism in order to guarantee their functions. In this scenario cellular metabolism is guaranteed by mitochondrial function [43]. Mitochondria occupy 30% of total cardiomyocyte volume, this guarantees the high energy demands of the heart. Mitochondrial oxidative phosphorylation fueled by catabolism of lipids and carbohydrates is the main source of ATP for heart function. The Krebs cycle is important for ATP generation but its balance and regulation are fundamental for oxidative stress management [44]. Cardiomyocytes aging is one of the main factors leading to cardiovascular diseases. Understanding the processes behind cellular dysfunction in the aging process has led to many findings in relation to mitochondrial dysfunction and its genomic instability and epigenetic regulation [45]. In fact, studies on longevity have highlighted the importance of mitochondria and oxidative stress in the senescence process [46]. As described before, free radicals are generated in different compartments of the cell. However, the main source of free radicals is mitochondria and in particular the electron transport chain located in the inner mitochondrial membrane. The continuous production of free radicals in the mitochondria leads to oxidation of macromolecules and DNA [47]. In particular, during aging nuclear and mitochondrial DNA stability is compromised [48]. Mitochondrial DNA lesions have been shown to carry mutagenic and cytotoxic affects ultimately leading to DNA replication alterations [49,50]. The genomic instability is partially prevented by DNA repair pathways in both mitochondria and nucleus [51]. Despite this DNA damage increases and accumulates during the aging process. Aged mice heart mitochondria have a threefold higher frequency of mitochondrial DNA mutation and deletions [52]. Accumulation of DNA alterations is a driving factor in aging leading to cellular loss of function. Animal models with increased mitochondrial DNA instability mediated by disruption of mitochondrial transcription factor A, showed alteration of mitochondrial morphology leading to higher rates of apoptosis and ultimately to dilated cardiomyopathy [53,54]. An early aging phenotype is characterized by high mitochondrial DNA point mutation as highlighted in mice [55,56]. New animal models have been developed to study the effect of increased mitochondrial DNA deletions in the myocardium. These models have highlighted that mitochondrial DNA dysfunction is not only associated with tissue dysfunction but also with development of premature arrhythmias [57]. Mitochondrial dysfunction and instability contribute to the aging process in other ways as is the case with calcium homeostasis and redox signaling [58,59]. Overall, the aging process and the mitochondrial alterations lead to metabolic changes. Normally up to 90% of cardiac ATP is generated by the use of long-chain fatty acid, only 10% from glucose, lactate, ketone bodies, and amino acids [60,61]. The Randle cycle highlights the substrate selection and interaction. Development of heart disease and aging has been associated with the inversion of metabolic substrate selection [61]. With aging increased glucose metabolism expression, increased glycolytic proteins and the concomitant decline in fatty acid oxidation has shown to be a premature sign of heart failure in younger individuals [62]. As we will mention afterwards, metabolic inversion and heart failure are associated with a reactive hyper-adrenergic state closely linked to impaired glucose metabolism and inevitably to insulin resistance [61].
Another important cellular dysfunction point to address is increased apoptosis during aging [63]. Accumulation of lipofuscin on lysosomes, loss of autophagic management, accumulation of non-functional damaged cell components, in particular mitochondria, leads to activation of the apoptotic pathway [64]. These changes in cardiomyocytes also increase alteration in calcium cellular handling. Calcium plays a crucial role in modulating cardiac function by modulation of myocardial contractility through a complex system of ion channels, ryanodine receptors, and sodium calcium exchangers. On the other hand, myocardial relaxation is mediated by sarcoplasmatic/endoplasmatic reticulum calcium-ATPase (SERCA2a) which seizes calcium to the sarcoplasmic reticulum [65]. The importance of cellular SERCA2a function has been highlighted in oxidative stress and aging. In particular, SERCA2a impairment and consequent increase in calcium stagnation in cytoplasm causes diastolic relaxation impairment [3]. Moreover, animal models by the same mechanism of prolonged cellular contraction showed alterations in myosin heavy chain expression [66]. These changes influence negatively cardiomyocytes contractile and electrical efficiency [66]. Alteration of the contraction and relaxation coupling of cardiomyocytes is at the base of the compensation mechanism that we will describe in the next chapters [67]. In fact, we will see how depletion of cardiomyocytes and inadequate contraction efficiency leads to cardiac hypertrophic remodeling and not only [68].
2.3. Aging in Cardiac Structural and Patho-Physiological Changes
Cardiac structural modifications due to aging bring about various functional and adaptive consequences in heart capacity [69]. Cardiac aging causes fibrosis, left ventricle hypertrophy, diastolic dysfunction, and filling ultimately leading to reduction in cardiac overall compliance and ejection fraction output [70,71]. Gene expression in aging human hearts highlights a shift in cellular capacity. Upregulation of genes for sarcomere and cytoskeletal proteins and downregulation of proteasome components expression reflects the process of myocyte hypertrophy and decreased in protein turnover [72]. This is accompanied by downregulation in Troponin T, SERCA2, and alpha-MHC with a switch towards beta-MHC, with a decrement in contractile efficiency [73]. Mitochondrial disfunction in mice aging cardiomyocytes is an important source of oxidative stress [74]. The inefficiency of aging rat mitochondria is characterized by increase in size, reduction in number of cristae with an overall reduction in ATP production per cell [75]. The high-rate production of reactive oxygen species leads to a vicious cycle [76,77]. In fact, in order to maintain functional demands the aging heart undergoes a process of hypertrophy [78]. This adaptation allows the heart to respond to increase in pressure demand in consequence to vascular stiffness [79]. However, this mechanism fails when heart demands exceed bringing about heart failure [78]. Cardiac hypertrophy in human aging-heart is characterized by increase in cardiomyocyte size with asymmetric left ventricle ventricular wall thickening mainly of the intraventricular septum [80]. These alterations cause alterations in human heart geometry and shape initially granting increase in contractility but on the long run causing oxygen impairment and reduction in contractility [81]. Aging in both mice models and humans is associated with apoptosis and loss of myocytes with a rate of about 45 million per year compensated by increase in single myocyte median volume [82,83,84,85]. The overload of the remaining myocytes is an additional reason for compensatory hypertrophy [86]. In addition, the loss of vascular elasticity and the increase in vascular stiffness increases the mechanical load of the aging heart accelerating the way to heart failure [87]. Age-related left ventricle hypertrophy in humans occurs independently of underlining story of hypertension or other causes [88]. Overall, a healthy human aging heart with preserved ejection fraction (EF) shows no change in stroke volume, heart rate, and cardiac output [81]. The main difference is highlight in diastolic function, in fact, the capacity of the ventricle to receive blood results altered by the reduction in ventricle wall elastic compliance [89]. Hemodynamically this can be seen in a reduction in early diastolic filling with an increase in tele systolic filling with an inversion of the E/A parameter and an increase in E/e’ better seen in echocardiographic studies [90,91,92]. This compensatory system present at rest however is not efficacious in case of cardiac demands. The aging-heart in fact compensates the contractile and diastolic function reduction with increase in peak heart rate [93]. Another important age-related alteration in animal model hearts is the calcification of the valves associated with proliferation of fibroblasts and deposition of collagen [94,95,96]. The cardiac extracellular matrix in the aging heart fills with glycoproteins, proteoglycans, glycosaminoglycans, integrins, and collagen [97]. Interesting is the switch from collagen type III to type I, seen in children, young adults, and elderly, which is less distensible and stiffer [98]. This also effects negatively the propagation of the electrical signals of the myocytes and of the myofibrillar bundles giving arrhythmias [99,100].
2.4. Endothelial Dysfunction
Age-dependent endothelial dysfunction is a multifactorial disease characterized by vascular endothelial cell structural and functional deterioration [28]. The reducing property of vasodilatation of the human aging endothelium is due to the loss of the homeostasis between vasoconstrictor and vasodilator molecules, and is associated with an increased mobility, and mortality [101,102,103]. In fact, the enzyme cyclooxygenases (COXs) are able to produce both contractile and vasodilators factors like TXA2, prostacyclin, and prostaglandin I2 (PGI2), respectively [104]. In the elderly, the loss of prostacyclin endothelium-dependent vasodilatation [105,106] and an increasing production of TXA2 by COX, ultimately causes an increasing endothelium-dependent contraction. As seen in eNOS knockout mice, the COX pathway is heavily influenced by the interaction with NO pathway, this is one of the main factors associated with cardiovascular health and longevity [107,108]. NO is a vasodilator, produced by NO synthase, an enzyme with three isoforms: neuronal NOS (nNOS), inducible NOS (iNOS), and endothelial NOS (eNOS). eNOS is the responsible of the vasodilatation in response to artery sheer-stress derived. In aging endothelium the eNOS activity reduction [109] reduces NO bioavailability [110]. Furthermore, in an aging endothelium high reaction rate between NO and superoxide anion results in NO activity reduction and generate peroxynitrite. This RNS can penetrate the cell membrane and react with macromolecules such as lipids and DNA with consequent premature aging [111]. Furthermore, in diabetic humans peroxynitrite seems to be a ROS production promoter factor establishing a vicious cycle [112]. This inflammatory pathway self-induced by the endothelium seems have a link with the vascular smooth cell expression of MMP-2 and MMP-9 with a devasting effect on vessels remodeling. In fact, in diabetic patients the impaired vasodilatation mechanism is followed by arterial stiffness thus indicating a link by endothelial disfunction and morphologic arterial changes [113]. Macroscopically aging vasculature is characterized by large elongated and tortuous arteries with a thickened wall and an enlarged lumen [114]. In the elderly, the reduction of endothelial cells turnover contributes greatly to endothelial dysfunction. This can be demonstrated by the decreased number and malfunction of the endothelial progenitor cells in aged humans [115]. The turnover of the endothelial cell is essential to preserve integrity, maintenance, and regeneration of the endothelial layer. This lack reduce vasodilatation/contraction endothelium mediated and reduced capacity in repair of injured arteries [116,117]. Moreover, in aging vasculature is evident the reduction of elastin and an increase of collagen fibers with the consequent reduction of the skill to transfer the blood flow pulse wave caused by the loss of the distensibility [118]. To guarantee a structural integrity collagen and elastin are kept together by an enzymatic cross-linking but in elderly vessels this link is mediated by a non-enzymatic glycation which lead an inflammatory response and a low resistance to the MMP activity, increasing fibrosis of tissues [68,119]. The mechanisms described earlier cause a negative hemodynamic cycle characterized for an increase of the peripheral resistance and pulse pressure with cardiovascular and systemic devasting consequences.
2.5. Aging and Autonomic Nervous System Adaptations
With aging an increasing plasma catecholamine concentrations and sympathetic tone of autonomic nervous system (ANS) [120,121] could impair adaptivity of elderly individuals to the environment [122]. Aging has been implicated in the impairment of alfa and beta-adrenergic receptor sensitivity and vascular responsiveness [102,123] with a predominance of the alfa tone in muscle vasculature. In fact, in older women we can observe a higher decrease of arterial blood pressure in front of younger ones after an autonomic blockade [103]. Age-related alterations in ANS influence blood pressure, cerebral blood flow, bladder function, and heart rate variability (HRV) [79,124,125]. HRV is an indicator of arrhythmic complications and a strong predictor of mortality and sudden death [126]. Nocturnal reduction of parasympathetic activity in elderly individuals is the result of a low vagal hearth control due to the prevalence of the adrenergic tone of SNA. The increase in heart rate combined with the HRV reduction is due to the degeneration of cardiac autonomic function during aging [127] and increases the incidence of cardiovascular events [128]. Active lifestyle is important for the health of the elderly. Intensive physical exercise, increasing muscle mass and fatigue resistance [129], could minimize autonomic dysfunction in aging with training [130]. A physical training regime could improve adaptations of the autonomic function [131]. Although intensive exercise seems to have benefit for older individuals, there is a need for further studies to realize a regimen of exercise programs. The ANS abnormalities were thought to be a common underlying pathophysiology of CVDs such as hypertension and heart failure [132]. Another issue due to the impairment between the two ANS deregulation is atrial fibrillation, the most common arrhythmia in older people [133,134]. Denervation of ANS has been shown to be efficient against AF [135]. Patients with AF had reduction in cardiac performance due to the loss of the atrial contraction in ventricular filling.
2.6. Genetic and Epigenetic Regulation on Cardiovascular Aging and Oxidative Stress
In addition to being a common denominator to many chronic disease manifestations, oxidative stress-induced endothelial dysfunction is the key mechanism linking aging to increased risk of clinical cardiovascular disease and death [31]. As we age, the continuous imbalance between the generation of ROS—which increases progressively—and the ability of endogenous anti-oxidant defense mechanisms—which becomes increasingly reduced—results in reduced NO bioavailability and impaired vasodilatory function [136,137]. Longitudinal studies conducted in long-lived and very long-lived cohorts, including “centenarians” have demonstrated the undeniable role of genetic variations in the regulation of the oxidative stress response in aging [138,139,140], referred to as the capacity of triggering various regulatory processes in response to oxidative stress. Among the antioxidant enzymes, Soerensen and colleagues [140] showed that a major role in longevity seems to be attributed to manganese superoxide dismutase (MnSOD) and glutathione peroxidase 1 (GPX1), indicating that variation in these genes may affect human life span.
In age-related cardiovascular diseases, a prominent role of sirtuins has also been thoroughly explored. Sirtuins (Sirt) belong to class III histone deacetylases that have been associated with aging for their nicotinamide adenine dinucleotide (NAD+)-dependent enzymatic activity. Seven sirtuin family members have been identified so far, denoted as Sirt1-Sirt7, each of which displays differential subcellular localizations: Sirt1, 6, and 7 are localized in the nucleus, Sirt2 is cytosolic, Sirt3 to Sirt5 are found in the mitochondrial compartment, the major source of intracellular ROS [141]. Many existing studies have demonstrated a protective role of the sirtuins against both accelerated vascular aging and atherosclerosis [142,143,144,145,146,147]. For instance, Sirt1 deficiency increases oxidative stress, inflammation, and foam cell formation and induced the senescence of endothelial as well as vascular smooth muscle cells. In support of this notion, using human vascular smooth muscle cells (VSMC) isolated from donors (from 12 to 88-year-old subjects), Thompson and colleagues [148] demonstrated an inverse correlation between the endogenous Sirt1 protein expression and the donor age. In an independent study conducted in 3763 subjects, the authors showed that homozygous minor allele genotypes within rs2841505 (Sirt5) and rs107251 (Sirt6) negatively influenced survival, whereas homozygous minor allele genotypes within rs511744 (Sirt3) were associated with an increased lifespan [149]. Furthermore, while partial Sirt1 deletion in atherosclerotic mice enhanced atherogenesis [150], Sirt1 overexpression reduced atherosclerotic plaque formation in ApoE−/− mice following 10 weeks of high-fat diet feeding [151]. In an attempt to investigate the molecular mechanisms behind the role of Sirt1 in inducing lifespan expansion, deletion of Beclin 1/Autophagy protein (Atg) 6 was found to abrogate longevity in C. Elegans [152]. In fact, besides being implicated in a variety of cellular processes, including energy metabolism cell stress response and cell/tissue survival, recent studies have also identified a role for sirtuins in the regulation of autophagy, a cellular housekeeping process, which is critical for the maintenance of tissue homeostasis during aging, particularly cardiac and vascular health [153]. For example, in response to cellular stress, including caloric restriction, Sirt1 upregulated the expression and directly deacetylated several Atg proteins, including Atg7 and Atg8, thereby inducing autophagy [154]. Likewise, Sirt1-null mice have increased basal acetylation of autophagic proteins and a reduced autophagy function [154]. In addition, knockdown of Sirt1 prevented the induction of autophagy by its indirect activator resveratrol and by nutrient deprivation in human cells [152]. Acting in a distinct manner from that of Sirt1, Sirt3 also regulated autophagy both positively and negatively. In particular, it has been reported that Sirt3 overexpression activated the mammalian target of rapamycin complex 1 (mTORC1), a consistent inhibitor of autophagy. In addition, Sirt3 gene silencing promoted autophagy and protected human hepatocytes from lipotoxicity [155]. In contrast, by inducing autophagy, Sirt3 prevented ischemia-induced neuronal apoptosis in cortical neurons cells [156]. Recent findings have also reported the beneficial role for Sirt6-mediated autophagy against cardiovascular diseases [157]. Indeed, using an in vitro model, Sirt6 reduced the formation of foam cells through an autophagy-dependent pathway, thus suggesting the protective role of Sirt6 in preventing atherosclerosis [157].
The mitochondrial adaptor protein p66Shc is another key determinant of aging since its genetic deletion induces stress resistance and prolongs lifespan by 30% [158]. The mammalian SHC locus encodes for three different isoforms carrying a Src-homology 2 domain. Owing to its unique N-terminal region, p66Shc is the only protein playing a critical role in redox metabolism [158]. Genetic deletion of p66Shc has been shown to reduce the production of free radicals in the brain, improve stroke outcome, and preserve neurological function in an ischemia-reperfusion injury model [159]. In patients with acute ischemic stroke, p66Shc expression was transiently increased and correlated with short-term neurological outcome [160]. Furthermore, p66Shc has also been involved in hyperglycemia-associated changes in endothelial function. In a mouse model of streptozotocin-induced diabetes, deletion of p66Shc protein protected mice against oxidative stress-induced endothelial dysfunction as well as lipid peroxidation in aortic tissue [161].
By modulating the expression of several antioxidant enzymes, the proto-oncogene JunD has been suggested as a potential target to prevent ROS-driven age-related cardiovascular diseases; indeed, JunD knockout mice exhibited impaired endothelium-dependent relaxation and reduced life span [162,163]. Conversely, in vivo JunD overexpression rescued age-induced endothelial dysfunction [162]. Moreover, low levels of JunD have been reported in monocytes of old healthy subjects when compared with young individuals, and the decrease was correlated with the expression of scavenging and oxidative enzymes [162].
Bactericidal/permeability-increasing fold-containing-family-B-member-4 (BPIFB4) has recently emerged as another molecule with important role in regulating aging and longevity. Recent studies have shown the role of a polymorphic variant in the gene encoding BPIFB4 in determining exceptional longevity in 3 independent populations [164]. In addition, homozygous carriers of the so-called longevity-associated variant (LAV)-BPIFB4 exhibited higher circulating BPIFB4 levels and increased eNOS activity in circulating mononuclear cells [165]. In line with these findings, circulating BPIFB4 levels were closely linked with the health status of long-living individuals [165]. Interestingly, LAV-BPIFB4 gene transfer decelerated frailty progression in aged mice and homozygous LAV-BPIFB4 haplotype inversely correlated with frailty in elderly subjects [166].
Growing evidence suggests microRNAs (miRNA) as critical regulators of aging and cardiovascular disease [167,168,169]. Acting at the post-transcriptional levels, these small non-coding RNA molecules are able to negatively regulate gene expression by inducing mRNA degradation or translational repression of their targets [170].
First discovered in Caenorhabditis elegans, several miRNAs have been found to both positive and negatively regulate longevity through canonical pathways during aging, including insulin signaling, heat-shock factors (HSFs), AMP-activated protein kinases (AMPKs), mitogen-activated protein kinases (MAPKs), sirtuins, target of rapamycin (TOR), and mitochondria [169,171]. Because miRNAs and aging signaling pathways are conserved across species, from nematodes to humans, studies on C. Elegans have provided clues to understanding mechanisms of age-related processes. For example, it has been shown that adult-specific loss of argonaute-like gene-1 activity resulted in a shorter lifespan when compared with that of wild-type [172]. Furthermore, a loss-of-function mutation in lin-4 and gain-of-function mutants of its target lin-14 displayed a reduced lifespan, which was rescued to a significant extent by knockdown of lin-14 only during adulthood [173]. Van Almen et al. found decreased miR-18 and miR-19 levels in aged heart failure-prone mice when compared to age-matched controls [174]. Importantly, these findings were also confirmed in cardiac biopsies of idiopathic cardiomyopathy patients at old age, where decreased miR-18a, miR-19a, and miR-19b expression was associated with severe heart failure [174]. Together with increased ROS production, miR-21 was found to be upregulated in heart, liver, kidney, and aorta of spontaneous hypertensive rats (SHR). Interestingly, exposure to exogenous miR-21 was able to lower blood pressure levels in the SHR rats, indicating miRNAs as novel potential therapeutic target in hypertension [175]. Among the most studied miRNAs, circulating levels of miR-126, miR-130a, miR-142, miR-21, and miR-93 have been found to be associated with human aging [176]. For example, miR-21 level is increased with aging process and aging associated-diseases, but its expression level decreased in individuals aged over 80 and in centenarians, suggesting the beneficial effects of low levels of miR-21 for longevity [176]. Menghini et al. found that miR-217 is widely expressed in aged but not young endothelial cells, and that its overexpression can induce endothelial cell senescence formation, thus suggesting the involvement of miR-217 in the pathogenesis of cardiovascular diseases [177]. Finally, using PCR arrays, Smith-Vikos et al. [167] identified multiple differentially expressed microRNA in serum samples from individuals who had documented lifespans from 58 to 92. Interestingly, six of these circulating miRNAs significantly correlated with subsequent longevity, suggesting that these miRNAs may serve as useful biomarkers of human aging [167].
Along with findings from several clinical trials that have failed to show long-term improvement with antioxidants [178,179], the above studies suggest the importance of directly acting on upstream signaling rather than adopting strategies to scavenge formed ROS to delay age-related disease onset.
3. Aging, Oxidative Stress, and Cardiovascular Diseases
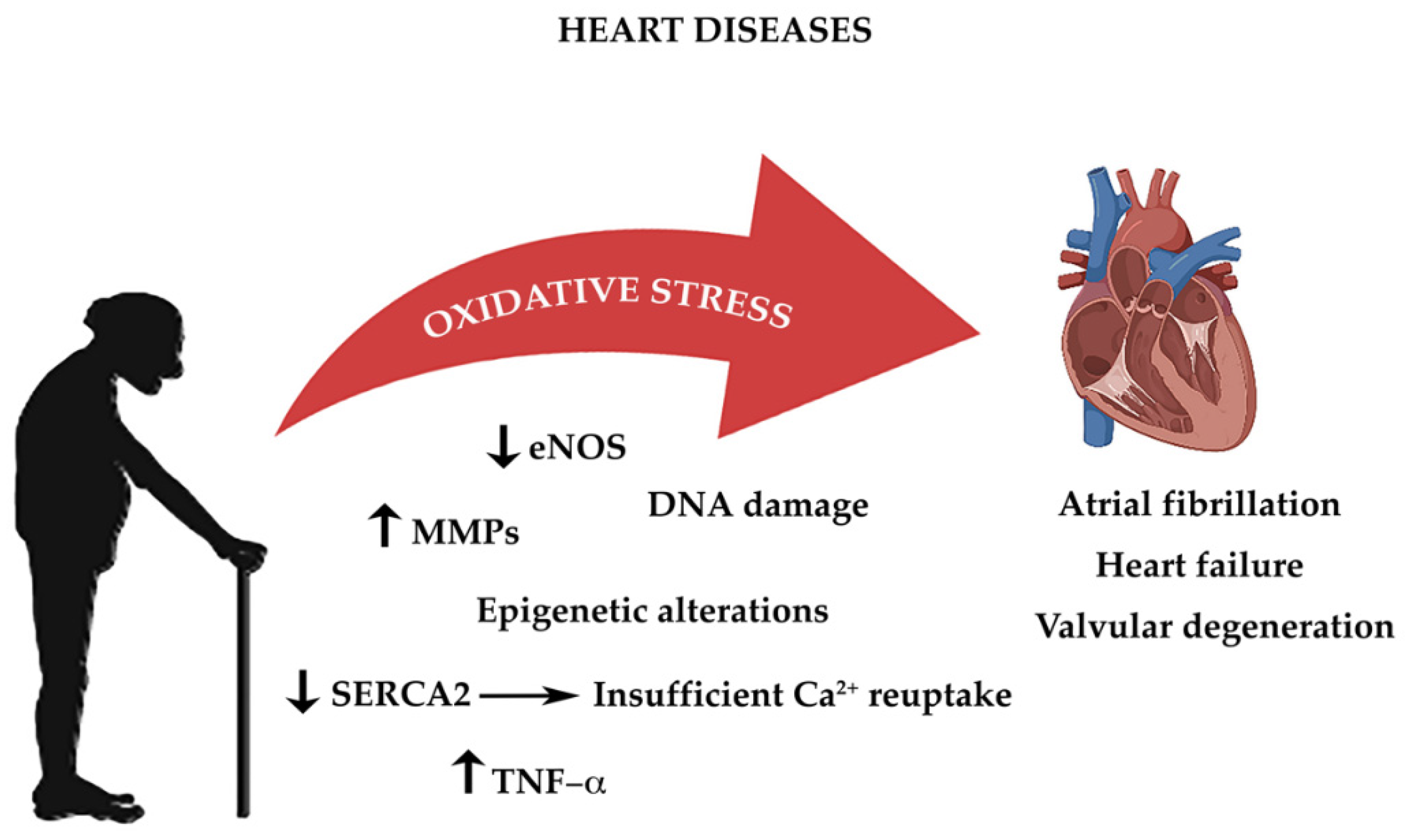
As highlighted above, all cells constantly undergo reactions which require transfer of electrons, in order to acquire energy [41]. These complex mechanisms, which occur principally in the mitochondria, require a constant turnover in the oxidative state [180]. The redox reactions and the reactive oxygen species (ROS) generated are highly reactive and are the main source of oxidative stress [18]. The heart’s cellular volume is made up for 45% by mitochondria [181]. Oxidative phosphorylation generates radical species, when electrons are lost from mitochondrial complexes I and II, in order to produce adenosine triphosphate (ATP) [18]. The mitochondrial pathway also characterized by formation of NADH and FADH which react with other redox compounds [182]. As cardiomyocytes and endothelial cells age, they produce more ROS. Increased production of ROS leads to functional impairment due to reduction in biological activity of nitric oxide and formation of peroxynitrite, which deactivates several free radical scavengers [23]. Another important origin of oxidative stress is aberrant Ca2+ reuptake, due to SERCA2 downregulation [183]. Constant high concentration of Ca2+ levels in the cardiomyocyte’s cytosol increases ROS production [184,185]. As highlighted before the RAAS system also plays an important role in age-related cardiac oxidative stress with direct and indirect involvement of NADPH oxidase complex and of ROS production [186,187]. Thus age-dependent increase in oxidative damage is the one of the leading causes of CVD (Figure 1) [188].
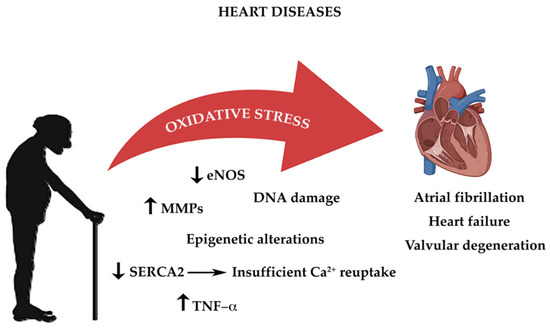
Figure 1.
The impact of oxidative stress on age-associated heart diseases.
3.1. Atrial Fibrillation
Atrial fibrillation is the most common chronic cardiac rhythm disturbance, it affects 1–2% of the population and the chances of developing this condition increases with age, particularly after age 65 [189]. It consists in a rapid heartbeat (tachyarrhythmia) that originates in the upper chambers of the heart, called the atria, preventing them from functioning properly [190]. In such circumstances, the atria are no longer able to expel all the blood, which will remain partially inside the atria with the risk of clot formation [191]. Clot formation due to AF is one the leading causes of cerebrovascular thrombosis [192,193]. In aging the main cause of AF can be found in the hearts structural and functional alteration, as described earlier. Aging itself is the single most important risk factor for AF [194]. Among all the previously described alteration, the electrical conduction disturbances, ectopic activity leading to atrial arrhythmogenesis is atrial fibrosis and so dilation [195]. Atrial fibrosis in the human aging heart is associated with excessive accumulation of collagen fibers, in particular type I fibers, and the increase of cross-linking between fibers [196]. Oxidative stress plays an important role in extracellular matrix (ECM) turnover and metabolism. The increase of matrix metalloproteinase (MMP) in human aging hearts with atrial fibrillation has been widely highlighted [197,198]. Age-related alteration are a summation of structural and electrophysiological remodeling leading to alteration of the mechano-electrical feedback [199]. Overall, this means that the atria are no longer capable of modulating the electric functions of the heart with the induction of mechanical load on the cardiomyocytes [200]. In conclusion, aging is associated with an increase in acute-phase inflammatory cytokines an important stimulus for AF, as it directly increases arrhythmogenicity and calcium homeostasis dysregulation [201,202]. Moreover, as seen in human atrial tissues, ROS and mitochondrial disfunction influence AF due to accumulation of age-related mitochondrial DNA deletion and mutation [203,204]. Oxidative stress and inflammation in aging influence greatly both functional and structural modifications causing electrophysiological remodeling and correlated diseases [205].
3.2. Heart Failure
Heart failure (HF) is a complex clinical syndrome defined by the inability of the heart to supply blood in adequate quantities for the body’s actual demand or the inability to meet this demand only at ventricular filling pressures above the norm [206]. According to statistics, as the population ages and the number of patients who survive a myocardial infarction increases, the incidence of heart failure continues to rise [207]. If we refer to hemodynamics, heart failure is characterized by reduced contractility of the myocardium measured as ejection fraction (EF), this universally used parameter can actually be not very specific in identifying the cause of cardiac dysfunction. In fact, this condition can be caused by both organic and functional problems. Among the most common causes are myocardial infarction, myocardial ischemia, hypertension, valvulopathies, cardiomyopathies, metabolic diseases, and autoimmune diseases [44]. HF is the most important complication of any heart disease. In the United States of America, it is estimated that in 2006 there were more than 600,000 new cases [208]. In Italy about 5% of the general population (3,000,000 individuals) is affected by overt or asymptomatic HF [209]. Age is a very important risk factor, the incidence remains low in people between 40 and 50 years, while it rises up to 10% in people over 75 years of age [210]. The incidence of this pathology is in rapid increase due to the overall increased survival rate following acute myocardial infarction and to longer life expectancy [211]. Aging (with consequent organ degeneration) causes cardiac efficiency to decrease, amplifying the effect of any pathologies. HF is generally thought to be involved in all those deaths from aging without apparent symptoms. In fact, when cardiac contractility is progressively reduced, whatever the cause, the final effect is hypo-perfusion of the organs vital and in particular of the brain, kidneys, and liver with the progressive functional deterioration [212].
Systolic HF is characterized by the reduced performance of the left ventricle, easily identifiable in patients with a universally adopted echocardiographic parameter such as the ejection fraction (FE), which, however, can vary considerably with the different biomedical imaging methods [213]. The force of contraction of the heart is directly proportional to the conditions of the myocyte, the cell of which the heart muscle is composed: any insult that affects the myocytes is reflected on the compliance of the left ventricle and therefore on the force of contraction (the FE is generally lower than 45%) [214]. Ventricular hypertrophy is one of the adaptation mechanisms of the heart subjected to increased stress that persists for long periods of time; this attempt at correction may be a factor involved in the progression of heart failure [215]. It is certainly not the mechanism that leads to myocardial hypertrophy, it is certain that an increase in systolic wall tension in association with an increase in afterload would cause concentric hypertrophy; on the contrary, an increase in diastolic wall tension in association with an increase in preload would lead to eccentric hypertrophy [216]. In both situations the synthesis of the unit of the myocyte known as sarcomere would be stimulated: in the first case the production of sarcomeres would be stimulated in parallel and in the second in series [217]. Myocytes and their components can be damaged by inflammatory diseases (myocarditis) and by infiltrates (amyloidosis), by toxins or by drugs. The most common mechanism is certainly myocardial ischemia: with the death of myocytes, the myocardium is replaced with fibrous or connective tissue, which have no contractile properties and are similar to scars. These scars can initiate the heart remodeling process, which in turn can lead to heart failure [218]. Heart failure caused by diastolic dysfunction, like systolic dysfunction, may be symptom-free in a compensated patient [219]. What characterizes this alteration is the inability of the left ventricle to adequately relax and this is secondary to the increased stiffness of the ventricular chamber. This attitude of the heart muscle leads to a reduced ventricular filling in diastole, which translates into a reduction in output. The inability to obtain optimal relaxation leads to an increase in end-diastolic pressures, which affect the atria and pulmonary veins [220]. Diastolic dysfunction and systolic dysfunction have many causes in common, most notably older age, high blood pressure, diabetes mellitus, and left ventricular hypertrophy. We can consider separately female sex, diseases of the pericardium and hypertrophic, accumulation and infiltrative cardiomyopathies [221]. Restrictive cardiomyopathy is one of the diseases that most affect diastolic dysfunction. Restrictive cardiomyopathies are characterized by a restrictive filling and a reduced diastolic volume; they are classified into primary and secondary [217].
In the failing aging heart, oxidative stress plays an important role. Both normal aging and pathological aging human hearts show increased levels of ROS [222]. Aging and oxidative stress can be accompanied by other pathological conditions such as diabetes, endothelial dysfunction, atherosclerosis, hypertension, and degenerative diseases increasing the imbalance between ROS production and antioxidant systems [187,223]. With aging, the compensatory mechanisms do not effectively manage ROS accumulation in mice models. This generates increased oxidation of proteins, lipids, and mitochondrial DNA damage. Electron leak in mitochondria is considered one of the main sources of ROS and adenine nucleotide translocase (ANT) seems to be why [224,225,226,227]. ANT oxidative and carbonyl modifications reduce mitochondrial energy output [228,229,230,231]. The uncoupling of ATP synthesis disrupts the mitochondrial matrix disrupting Ca2+ stabilization [232]. In fact, failing senescent mice hearts in conditions of stress, increase by two-fold Ca2+ levels, increasing ischemic and reperfusion damage [233]. Progression to heart failure and heart failure itself includes various mechanisms. As seen before, oxidative stress in aging also leads to increased cardiomyocytes apoptosis, ECM remodeling, and altered response to stress all important factors for HF [85]. For all the reasons above, heart failure and aging are synonyms. The aging process and all the changes involved lead to heart failure.
3.3. Valvular Heart Disease
Age is the main driving factor for valvular myxomatous degeneration and valvular sclerosis. Elderly patients have a prevalence of 30–80% of aortic valve sclerosis [234,235,236]. With age echocardiographic examination in these patients shows an increase in calcification of the aortic valve leaflets and anulus [237,238]. Elderly patients also have concomitant risk factors for rapid progression of valve degeneration such as hypertension, LVH, hyperlipidemia, and kidney failure [239]. Moreover, there is a linear correlation between aortic valve degeneration and atherosclerosis in elderly patients [240]. Valve sclerosis does not have a hemodynamic impact but can evolve into stenosis. Aortic stenosis is characterized by the reduction in the opening of the valve leaflets with consequent increased in pressure gradient between the left ventricle and the aorta [239]. To guarantee the necessity of the increased pressure gradient the heart undergoes myocardial hypertrophy to maintain an adequate systolic function and cardiac output [235]. This mechanism of compensation leads to left ventricle dilatation and deterioration of systolic function on the long run. Another aortic valve degeneration consequence is aortic regurgitation, a situation where the leaflets do not close properly and a backward blood flow in generated. This second condition causes a rapid diastolic filling and eccentric hypertrophy of the heart in order to increase the blood volume output [235]. Same is true for the mitral valve, with aging there is degenerative process involving the annulus and the leaflets [241,242]. In this case, however, valve regurgitation is more common than stenosis [243]. As for the aortic valve, hypertension, kidney failure, and aortic alterations are risk factors mitral calcification and patients with this such alteration have an increased risk for heart failure, atrial fibrillation, stroke, coronary artery diseases, and overall adverse cardiovascular events and mortality [234]. In humans, mitral valve regurgitation is mainly associated with ischemic heart disease and myxomatous degeneration while mitral stenosis is associated with rheumatic disease [244]. Mitral and aortic valve vices are one of the most common cause of surgery in older population [245]. Interesting are the recent discoveries that associated reduction in telomere length with degenerative valve disease. In particular elderly patients with aortic stenosis had a reduction in leukocyte telomere length [246]. Although more research is required to fully understand ROS-induced damage to telomeric DNA, studies suggests that this may be an important factor to take into consideration [247]. Furthermore, even if oxidative stress and telomere shortening in humans still have not been directly correlated, there is a great association with frailty typical of the elderly [248]. Oxidative stress and inflammation play an important role in valvular calcification. The underlining mechanisms are not fully known but local inflammation by hyperlipidemia and diabetes has been shown to be a great promoter of valve and vascular sclerosis [249]. Moreover, human studies have assessed that oxidized lipids seem to be one of the main inflammatory driving factors [250,251,252]. Increased levels of circulating oxidized phospholipid, ox-LDL and of TNF-alpha and inflammatory cells have been highlighted in patients with higher degrease of valvular degeneration [253,254]. High levels of ox-LDL increase the expression of osteogenic factors such as BMP-2, activating TLR expression [255,256]. The vicious cycle of lipid oxidation induces chemokines release and recruitment of monocytes and enhanced expression of ICAM, and MMP, factors leading to reduction NO production [257,258,259,260,261]. In conclusion, valvular heart disease is probably associated to oxidative stress in the aging heart by ROS increase with NO synthase uncoupling mediated mainly by ox-LDL expression of NADPH [262,263,264,265,266].
4. Aging, Oxidative Stress, and Vascular Diseases
An increasing production of reactive oxygen species is associated with a many cardiovascular diseases [8,11]. ROS family is composed of both oxygen free radicals and non-radicals [267]. As highlighted earlier in the article mitochondria are the main productor of ROS, other sources are NADPH oxidases. Other cell organelles, including peroxisome and endoplasmic reticulum, contribute to intracellular ROS production through enzymes like xanthine oxidase, nitric oxide synthase, cyclooxygenases, cytochrome P450 enzymes, and lipoxygenase. Proteins, lipids, and DNA are the primary cellular structures affected hit by ROS and RNS. The generation of ROS is a natural part of aerobic life; indeed, basal levels of ROS are necessary to exert various cellular functions, such as signal transduction pathways, defense against invading microorganisms, gene expression, and the promotion of cell growth or death [13]. Human tissues have protective measures against ROS like superoxide dismutase (SOD), catalase, peroxiredoxin, and glutathione peroxidase, and non-enzymatic compounds tocopherol/vitamin E, beta-carotene, ascorbate, glutathione, and nicotinamide [14]. Imbalance of oxidant signaling may accelerate some pathological conditions and the rate of aging. Oxidative stress and inflammatory response are strictly related with endothelial dysfunction, the key to cardiovascular disease.
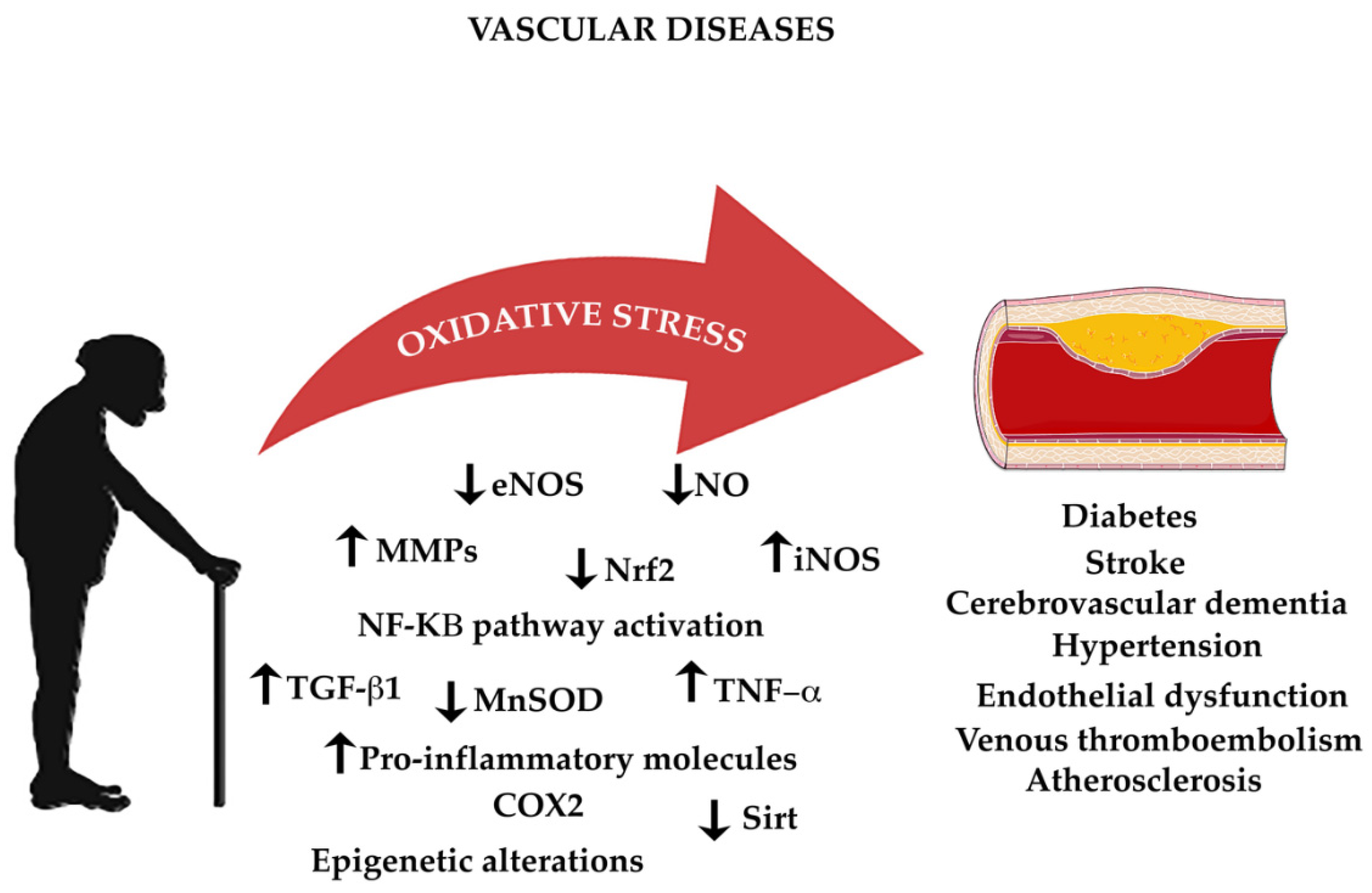
The endothelium is an organ composed by a highly active monolayer of cells that modulates important functions such as vascular tone, cellular adhesion, thromboresistance, smooth muscle cell proliferation, and vessel wall inflammation. This is mediated by the release of vasodilator and contracting factors. The vasoactive molecules that relax or constrict vessels regulate tone and diameter of the vascular tree directly influencing the balance of tissue oxygen supply, long-term organ perfusion, remodeling of vascular structures, and metabolic demand [268,269]. eNOS generates the vasoprotective molecule NO, which activates soluble guanylyl cyclase and increases cyclic guanosine monophosphate (cGMP) [29]. NO can also inhibit leukocyte adhesion to the vessel wall, blocking the first step of the development of atherosclerosis [29]. Traditional cardiovascular risk factors are related with endothelial disfunction such as smoking, sedentary lifestyle, aging, hypercholesterolemia, arterial hypertension, hyperglycemia, and a family history of premature atherosclerotic disease [270]. Increased levels of superoxide anions are led by inactivation of NO. This represents a critical mechanism leading to endothelial dysfunction [271]. NADPH oxidase is a key enzyme in reducing oxidative stress and normalization of endothelial dysfunction in mice [272]. Another character related with endothelial disfunction is inflammation. In endothelial dysfunction, activation of the nuclear factor-kappa B (NF-κB) pathway has highlighted elevated levels of pro-inflammatory cytokines such as tumor necrosis factor-alpha, interleukin-1beta (IL-1 β), interleukin-6 (IL-6), and interferon gamma (IFN-γ) [273,274]. NF-κB is an important transcription factor regulating the gene expression of inflammation and redox status enzymes and playing an important role in the CVD development in humans [275]. The NF-κB pathway can be activated by a wide of stimuli including ROS, inflammatory cytokines, and mechanical forces acting on the vascular endothelial wall. The activation of a kinase (IκK) mediated phosphorylation and the degradation of the inhibitors of NF-κB (IκB) consent the translocation of the NF-κB heterodimer to the nucleus, where it binds to promoters of gene targets. Other pro-inflammatory molecules are related to endothelial dysfunction, like IL-6, TNF-α, monocyte chemoattractant protein 1 (MCP-1), and the pro-oxidant enzyme NADPH oxidase, all of which predispose the vasculature to CVD (Figure 2) [276].
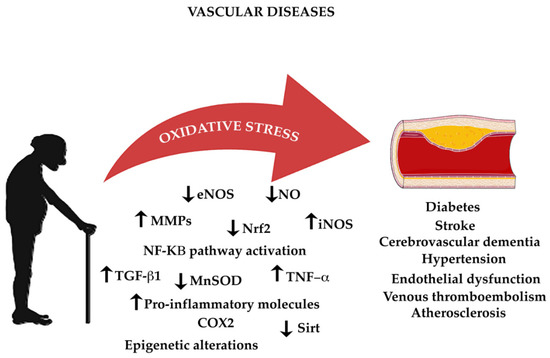
Figure 2.
The impact of oxidative stress on age-associated vascular diseases.
4.1. Aging in Vascular Structural and Patho-Physiological Changes
Structural and physiological changes of the endothelium and smooth muscle cells can be detected in aging vasculature. The early manifestation of arterial aging is the impaired endothelial vasodilation that precedes in years the clinical manifestations of vascular dysfunction [277]. Another hallmark of vascular aging is an increase in arterial stiffness due to the loss of arterial elasticity, compromising vascular adaptation to blood flow and pressure changes [119]. Elastic fibers undergo fragmentation due to the enhanced MMPs activity, in fact Increased expression and activity of MMP-2 have been reported in vessels from both aged animals [278,279] and humans [280]. Alteration of morphology and composition of extracellular matrix cause an increased speed of propagation of pressure and flow waves that can be measured by different ways like the determination of the pulse wave velocity (PWV). Although MMP-2 upregulation is more commonly related to vascular aging, plasma MMP-1 and circulating markers of type 1 collagen (MMP-1 substrate) degradation positively correlate with PWV and augmentation index as indicators of arterial stiffness in human subjects [281]. The increased severity of vascular diseases observed in aging vasculature is in part due to functional decline of endothelium repair capacity observed in elderly [116]. This could be related to the decreased number of endothelial progenitor cells (EPC) and to the impairment of their functions with consequent the loss of function in mechanisms for endothelial regeneration and maintenance [117]. Several studies have demonstrated the impaired reendothelization ability of EPCs [282] and a reduced number or circulating EPCs in elderly subjects [115,283]. The first and most important alteration of aging vasculature is endothelial dysfunction, a determinant factor for macro and microvascular dysfunction, related with an elevated morbidity and mortality [101,102]. Arterial stiffness is always preceded by an impaired endothelial vasodilation, suggesting that this arterial alteration is also linked to endothelial dysfunction [113]. In particular, aging is an independent factor associated with the reduction in the endothelium-dependent vasodilatation even in the absence of other cardiovascular risk factors [28,284]. In fact, it is described both in vitro and in vivo in different on old animals [31,103] and humans [102]. NO is a molecule key to cardiovascular health produced by NO synthase isoforms, most importantly eNOS [108]. NO production seems to have an important role in longevity [285]. The mechanisms of endothelial dysfunction involve a diminished availability of NO, and an imbalance between the endothelium-derived vasodilators and vasoconstrictors. Aging is associated with deficit in NO bioavailability; however, the impact of aging on eNOS expression is controversial. eNOS expression in aged vessels could be unchanged [286] decreased [287], or increased [3,288]. In contrast, it is well accepted that eNOS activity is reduced with aging [109]. Although reduced eNOS activity possibly accounts for the decline in endothelial vasodilation with aging; other two mechanisms are responsible for endothelial dysfunction in aging: an excessive chronic oxidative stress and an increased proinflammatory activity both compromising the bioavailability of nitric oxide as discussed previously [137,289].
4.2. Hypertension
Hypertension is a clinical condition in which the blood pressure in the arteries of the systemic circulation is elevated. Blood pressure is summarized by two measures, systolic and diastolic, which depend on the fact that the heart muscle contracts (systole) and relaxes (diastole) between one beat and another. Hypertension is considered if there is a pressure frequently equal to or greater than 140/90 mmHg [290]. Hypertension is classified as primary (essential) or secondary. About 90–95% of cases are classified as “primary hypertension,” which means there is high blood pressure with no obvious underlying medical cause. The remaining 5–10% of cases classified as “secondary hypertension” are caused by other diseases affecting the kidneys, arteries, heart, or endocrine system [291]. Hypertension is a risk factor for stroke, myocardial infarction, heart failure, arterial aneurysms, peripheral arterial disease and is a cause of chronic kidney disease [292]. Even moderate elevations in arterial blood pressure are associated with a reduction in life expectancy [293]. Hypertension is the largest contributor to the global burden of CVD and is for many states a heavy burden on the socio-economic expenses [294]. Both aging and hypertension are associated with morphological and functional changes in the vascular tree characterized by increased arterial stiffness, reduced elasticity, impaired distensibility, endothelial dysfunction, and increased vascular tone. The relationship between aging and vascular stiffening is evident in patients with progeria (premature aging), who exhibit accelerated vascular aging and often die of cardiovascular disease [295]. Findings from noninvasive vascular phenotyping studies in healthy individuals have demonstrated that intima-media thickness increases 2- to 3-fold between 20 and 90 years of age [118] The precise factors causing progressive intimal thickening with aging is still not clear, but a number of distinctive changes at cellular and morphologic levels have been identified: increased collagen deposition, cellular senescence, unfit elastin fibers turnover, and dysregulated cell proliferation. The remodeling of the ECM, which is an essential component of the connective tissue surrounding the vascular wall, has a key role in vascular aging. The ECM is composed of structural elements like collagen and elastin and more specialized proteins including fibronectin and proteoglycans. The ECM is a dynamic structure regulated by MMPs and TIMPs. Dysregulation of these processes, together with alterations in profibrotic and proinflammatory pathways, contributes to structural modification occurring with aging. Both large and small arteries are interested by fibrosis. In large vessels, vascular stiffening leads to hemodynamic damage to peripheral tissues [296]. Aortic wall stiffening causes increased pulse wave velocity (PWV) and premature reflected waves with elevated central hemodynamic load leading to damage of peripheral small arteries [297]. Arterial stiffness can be evaluated by measuring PWV, measuring the speed of the pressure pulse from the heart propagated to the arteries. This can be calculated by relating the distance travelled and the time taken to travel a defined distance. Stiffer arteries increase time travel resulting in higher PWV. Carotid-femoral PWV is the gold standard for measuring aortic stiffness [298]. Arterial stiffness has a bidirectional causal relationship with blood pressure because high blood pressure causes arterial wall injury, which in turn promotes stiffening. This is the main mechanism of increasing systolic blood pressure in aging vasculature [299,300]. A lot of evidence has shown an important relationship between oxidative stress, inflammation, and hypertension [301,302]. Oxidative stress is the main character of vascular inflammation and the consequent inflammatory responses [303,304]. Immunosenescent T cells have an important role in hypertension and the susceptibility of T cells to changes associated with aging like by loss of CD28 marker and appearance of CD57 [305]. They produce tumor necrosis factor-α and interferon-γ which affect vascular changes [306]. T cells are key in vascular disease [307,308] and several clinical studies indicate that their role is due to a close interaction with other elements of innate, cellular, and humoral immunity [307]. B cells also seem to be essential in hypertension, as their lack is related with a reduced vascular oxidative stress [309]. In fact, B cells may explicate their effects with antibodies and with cytokine production like TNFα, which has been shown to be prohypertensive and pro-atherosclerotic [310]. By the same rational, macrophages also have an evident role in hypertension and atherosclerosis [311,312] closely linked to NADPH oxidases abundance in their cytosol [313]. NADPH oxidase also participates in vascular damage, inflammation, and fibrosis [314,315]. TNFα acts as a pro apoptotic factor stimulating ROS production. This mechanism promotes accelerated vascular aging [316] as well as cognitive impairment [317]. Inflammation and oxidative stress are important for microvascular dysfunction. This has particularly relevance in conditions associated with small vessel disease and cognitive impairment. In fact, hypertension has been shown to exacerbate Alzheimer disease through reduced NO bioavailability trough eNOS and nNOS activity [318]. Important microvascular dysfunction leading to cognitive impairment is dependent on NADPH oxidase activation in macrophages infiltrating perivascular space in the brain [317]. This seems to be a mechanism for NO decrease and neurovascular unit impairment [317] demonstrating the role of inflammation in cognitive dysfunction. The interaction between inflammatory response and oxidative stress influence vascular remodeling through mediators like MMPs, which degrade collagen and elastin and promote fibrosis mechanisms. Their inhibition retards arterial remodeling decreases stiffness and improves endothelial function in animal models [319]. This is because MMPs create an inflammatory condition that contributes to shift the phenotypes of endothelial cells and smooth muscle media cells toward secretory and senescent phenotype which in turn increase MMP levels in vasculature. The effects of MMPs are mediated by ROS [320]. In fact, MMP genes are redox sensitive and are regulated by increased NADPH oxidase activity [321]. In summary MMPs promote arterial remodeling in aging, hypertension, and atherosclerosis [322]. Therefore, tissue inhibitors of metalloproteinases, such as TIMP-2, play protective role like suppressor of vascular remodeling of the ECM [323]. In summary, the key to vascular aging is the senescence of the vascular wall cells which promotes chronic ECM degradation and perivascular inflammation. Multiple factors contribute to vascular aging and hypertension. In aging vasculature, increased levels of Ang II [324], angiotensin-converting enzyme [325,326,327], mineralocorticoid receptors [328], and endothelin-converting enzyme-1 have been highlighted [329,330], contributing to structural and mechanical changes in the vascular tree. In particular by activation of AT-1 receptors Ang II AT1 plays a major role in the production of ECM proteins [331,332]. This was demonstrated by studies where the antagonism of Ang II receptors resulted in decreased fibrosis [333,334]. The precise signaling events involved in Ang II-induced vascular fibrosis is still not clear but is known that activity is increased by Ang II [331]. TGF-β1 is expressed in endothelial cells, vascular smooth muscle cells, myofibroblasts, and adventitial macrophages. Activation of vascular TGF-β1, and its downstream signaling effector SMAD results in excessive matrix accumulation, in part due to the inhibition of ECM degradation [335]. Several studies highlighted aldosterone as an important pathophysiological mediator in cardiovascular remodeling promoting vascular hypertrophy, fibrosis, inflammation, and oxidative stress [336,337]. In fact, chronic blockade of mineralocorticoid receptors, through which aldosterone signaling works, showed reduction of cardiovascular fibrosis. This effect may be due to the increasing collagen I synthesis [338,339]. Another vascular factor that influences the hypertension phenotype is endothelin (ET). The vascular actions of ET are mediated by 2 distinct endothelin receptor subtypes: ETA and ETB receptors located on vascular smooth muscle and on endothelial cells. ET modulates ECM stimulating fibroblast-induced collagen synthesis and acts as a hypertrophic and mitogenic factor. ET-1 stimulates synthesis of collagen through both ETA and ETB receptor subtypes [340,341]. Moreover, arterial stiffening derives from imbalance between excessive fibrosis due to excessive accumulation of vascular collagen and degradation of elastin. It is a dynamic phenomenon and one of the main markers of vascular aging in hypertension and other cardiovascular diseases.
4.3. Atherosclerosis
Atherosclerosis (AS) is a chronic disease of the arterial wall [342] and one of the most common cause of CVDs [343], which widely affects public health in our society. Specifically, the accumulation and rupture of atheromatous plaques in arteries can lead to ischemic heart disease, ischemic stroke, and peripheral arterial disease [342]. The disease has a latency of many years and frequently coexists in more than one vascular bed [344]. In particular, the central arteries undergo substantial structural and functional alterations with aging: they dilate, leading to an increase in lumen size, while intima becomes thickened, and the media exhibits an increased collagen content and frayed elastin [345,346]. The thickness of the arterial wall, which arises mostly in the intimal layer, increases two-to three-fold between 20 and 90 years, consequently increasing the risk of AS [118,345]. Furthermore, the intimal medial thickness is a marker of subclinical vascular disease: a 0.1 mm increase in carotid artery intimal medial thickens is associated with an 18% increase for stroke and 15% for myocardial infarction [347]. In particular, AS is a peculiar form of inflammation triggered by cholesterol-rich lipoproteins and other noxious factors such as blood pressure, cigarette smoking, diabetes mellitus, and chronic kidney disease [348]. However, genetics also play an important role in the disease, accounting for about 40% of the risk [348]. Briefly, AS is a multifactorial and progressive disease. In fact, there is an emerging indication that inflammatory pathways play a crucial role in atheroma construction. Stimulation of pro-inflammatory signaling pathways, expression of cytokine/chemokine, and increased oxidative stress are some of the pathways leading to AS [11]. Noxious factors lead to qualitative changes in endothelial cells, encouraging the expression of adhesion and chemotactic molecules and an amplified permeability to macromolecules [6]. This enables the infiltration of subendothelial spaces of arteries by oxidized lipoprotein. This leads to the formation of plaques, cholesterol deposits (atheroma) with a fibrous cap (sclerosis), characterize the inflammatory process of AS [79]. The aging process could accelerate structural and compositional changes observed in AS [79]. As known, endothelial cell injury and AS suggest the susceptibility of aged vessels to the lesion [349]. Previous studies compared old and young rabbits subjected to a long period of hyperlipidemic diet: old rabbit arteries constantly develop fibroatheromatous plaques [350]. Some studies have addressed the implications of cellular senescence in the AS pathway [351]; specifically, the cellular senescence could occur in two forms: replicative and stress-induced premature senescence [352]. The replicative pathway is due to DNA damage-induced telomere shortening, which could result from the high content of reactive oxygen species (ROS) and oncogenes [79]. Furthermore, biomarker such as senescence-associated β galactosidase (SAβG) was found in senescent human cells [353]. A high amount of SAβG-positive in atherosclerotic lesions and old vessels reinforced the association between atherosclerosis and senescence [354]. ROS are the major candidates responsible for senescence and age-related diseases in which the redox balance is invalidated and generates oxidative stress [355]. Age-related oxidative stress is essential to the pathologic changes of AS, because the generation and clearance of oxidative stress in the vasculature is a significant regulator. On one hand, endothelial cells and vascular smooth muscle cells produce reactive oxygen and nitrogen species, which oxidize low-density lipoproteins (LDL); moreover, the oxidation process increases mitochondrial rupture and the release of proapoptotic molecules to the cytosol, increasing plaque cell apoptosis [356]. On the other hand, the scavenging process for reactive nitrogen species increases endothelial dysfunction, smooth muscle cell proliferation, leukocyte adhesion, and inflammatory responses [357]. Some research on AS have linked nutrition to age-induced vascular changes [358]; specifically, caloric restriction (CR) could be a dietary intervention for promoting longevity and delaying age-related diseases, such as AS [359]. Kitada and colleagues [359] demonstrated that CR-induced Sirt1 has an antiaging property, with many physiological benefits: reduced apoptosis, enhanced mitochondrial biogenesis, inhibition of inflammation, regulation of glucose and lipid metabolism, and adaptations to cellular stresses. Further, observational data collected in humans show that the ingestion of antioxidants is associated with prevention of cardiovascular disease [360] and intrinsic antioxidant systems in the mitochondria could be therapeutic targets [355]. On the other hand, exercise is known to reduce the risk of cardiovascular disease. In particular, the beneficial effect of exercise on improvement of serum atherogenic lipoprotein profiles include reduction of serum triglycerides, increase in HDL cholesterol, and increase in average size of low-density lipoprotein (LDL) particles [361]. Furthermore, higher physical activity has also been shown to reduce carotid artery intima-media thickness, a clear marker of atherosclerotic burden [85].
4.4. Deep Vein Thrombosis
Venous thromboembolism (VTE) refers to the interconnected diagnoses of deep vein thrombosis (DVT) and pulmonary embolism (PE). Specifically, DVT is the formation or presence of a thrombus in the deep veins [362]. VTE is globally the third most frequent acute cardiovascular syndrome behind myocardial infarction and stroke [363], and thromboembolic events count among the most common complication of hospitalization [364]. VTE is a significant cause of mortality and disability, affecting 1–2 per 1000 people annually, presenting with a rather wide range of symptoms, which can pose a diagnostic challenge [365]. Particularly, DVT and PE account for 60,000 to 100,000 deaths annually in the United States [366], while in Europe, this number rises to greater than 500,000 deaths annually [364]. Considerable research has been done to identify risk factors and to provide appropriate prevention where indicated. However, VTE remains a growing public health concern [364].
Venous thrombosis is the development of a platelet and fibrin clot in the vascular lumen. Thrombosis formation is a dynamic, multicausal process that hinges on a fine balance of physical and biochemical features [366]. In particular, DVT is considered to be the result of the interaction between patient-related (usually permanent) risk factors and setting-related (usually temporary) risk factors [367]. According to Virchow’s triad, the pathophysiological mechanisms involved in DVT are three: damage to the vessel wall, blood flow turbulence, and hypercoagulability [368]. Clinically significant thrombi are shaped in vessels with large lumens such as the deep veins of the legs, pelvis, and arms; however, the clot can then propagate with proximal extension [364]. Moreover, if the clot dislodges, it can embolize to a distant site, and the most common site of embolization is in the pulmonary vasculature [364].
Aging is associated with an increased risk for thrombosis. It has been documented that the incidence of VTE is two to seven times higher in patients above the age of 55 as compared to a younger cohort [369]. Specifically, several factors related to aging have been observed: increased frequency of illness and periods of prolonged immobility, greater prevalence of obesity, comorbidity, and an increase in the level of procoagulants without a commensurate increase in anticoagulants [370]. Rumley and colleagues [371] demonstrated that the increase in risk of VTE in men between age 60 and 79 years may be related in part to increased activation of blood coagulation, fibrinolysis, and inflammation. They highlighted a marked increase in fibrin D-dimer and CRP in this population as relevant to the pathogenesis of VTE with increasing age. On the other hand, aging is associated with increased production of ROS, which indirectly creates a discrepancy between thrombosis and hemorrhage [372,373].
Up-regulation of ROS-producing enzymes (e.g., NADPH oxidase and myeloperoxidase), along with down-regulation of antioxidant enzymes (e.g., SOD and glutathione peroxidase GPx), occur in the elderly. This imbalance may lead to thrombosis by damaging red blood cell (RBC) shape and function, causing endothelial dysfunction, and triggering platelets and leukocytes, therefore affecting the clotting system [374]. RBCs can be a major source of oxidative stress in elderly, since RBC redox homeostasis is usually compromised. In fact, ROS con easily accumulate within the RBC due to constant autoxidation of endogenous hemoglobin (Hb) and to NADPH oxidase activation. Moreover, RBC in their path uptake extracellular ROS released by other cells in the circulation [374]. Specifically, ROS affect the RBC membrane structure and function, causing loss of membrane integrity, and decreased deformability [374]. This process impairs RBC function in hemostasis and thrombosis, supporting a hypercoagulable state. Overall, these changes lead to enhanced RBC aggregation by increased binding to endothelial cells which also affects nitric oxide availability [375]. Accelerated aging and hemolysis is also a key factor as shown by increased RBC-induced platelet activation, RBC interaction with coagulation factors, increased RBC phosphatidylserine exposure and release of microvesicles [374].
In summary, aging and oxidative stress influences greatly RBC deformability, blood rheology, altering blood flow in the circulation [376]. All the above combined with genetic polymorphisms and mutations can trigger venous prothrombotic events [377], thus predisposing the elderly to age-related VTE [374]. In conclusion, a further better understanding of the detailed mechanisms by which aging, and the associated oxidative stress disrupt the coagulation cascade to initiate venous thrombosis would provide new targets for tailored therapies to prevent VTE in the elderly.
4.5. Stroke, TIA, and Cerebrovascular Dementia
A stroke or cerebrovascular accident is an acute compromise of the cerebral perfusion or vasculature [378]. Almost 85% of strokes are ischemic and the rest are hemorrhagic [379]. On the other hand, a transient ischemic attack (TIA) is defined as a transient episode of neurologic dysfunction due to the focal brain, spinal cord, or retinal ischemia, without acute infarction or tissue injury [380]. Over the past several decades, the incidence of stroke and mortality is decreasing; however, the burden of stroke in the US remains enormous and stroke is the second most frequent cause of death after ischemic heart in developed countries [381]. Furthermore, this disease commonly occurs in individuals over 65 years [382] and is the leading cause of adult disability worldwide [378]. Moreover, the estimated overall prevalence of TIA among adults in the US is about 2% [383]. Ischemic stroke can result from embolic, thrombotic, and lacunar events. Generally, the common risk factors for stroke include hypertension, diabetes, smoking, obesity, atrial fibrillation, and drug use. Hemorrhagic etiologies can result from hypertension, arteriovenous malformations, aneurysm rupture, venous angiomas, amyloid angiopathy, and other obscure etiologies. Of all ischemic strokes, lacunar strokes represent 20% and results from occlusion of the small penetrating branches of the middle cerebral artery, vertebral or basilar artery, or the lenticulostriate vessels [378].
Atherosclerosis is the most significant underlying pathology in stroke and leads to the formation of atherothrombotic plaques in the arteries supplying the brain [384]. Plaque rupture causes exposure of the underlying cholesterol crystals which attract platelets and fibrin, and formation of fibrin-platelet-rich emboli leads to stroke in the distal territories [384].
In summary, stroke is the result of ischemia in an area of the brain. When there is a break of blood supply by a thrombus, the immediately adjacent neurons lose their supply of oxygen and nutrients. The inability to use aerobic metabolism and produce ATP causes the Na+/K+ ATPase pumps to fail, causing an accumulation of Na+ inside the cells and K+ outside the cells [384].
Consequently, ischemia leads to depolarization of cells which results in calcium influx into cells, elevated lactic acid, acidosis, and free radicals’ formation [385]. Cell death increases glutamate and leads to a cascade of chemicals (excitotoxicity) [378,385].
It has been reported that the incidence of stroke increases with age [386] and numerous researches have proved that aging or senescence is a risk factor that exacerbates stroke. Moreover, oxidative stress is certainly connected to age-associated cognitive decline [387].
Specifically, a recent study revealed that both amplified oxidative stress biomarkers connected with raised levels of inflammatory cytokines were related to poor cognitive performance in elderly people [41,388]. At midlife, neuronal atrophic and glial cell changes begin at the same time with degeneration of white matter. Consequently, aging-induced alterations of white matter can influence the susceptibility of axons to ischemia. The aging process influences the brain microvasculature by a great extent. The structural and functional degeneration of the blood-brain barrier (BBB) during aging could disrupt local blood perfusion and nutrient supply [79].
Cerebral vessel modifications in the elderly may decrease cerebrovascular reservoirs and make the brain more prone to ischemic damage and vascular insufficiency [389]. All these alterations could lead to an ischemic stroke and vascular cognitive deficiency in aging.
In vascular inefficiency, ROS and reactive nitrogen species (RNS) cause an increased concentration of H+ and H2O2, leading to DNA injury, endothelial alteration, and mitochondrial dysfunction [390]. Moreover, this is worsened by damage through ROS-mediated inflammation, apoptosis, autophagy, and the microbial-gut-brain axis [390]. The depletion of energy in ischemic stroke can cause a series of injuries to promote the progress or recurrence of stroke, and OS is involved in all phases of ischemic stroke evolution. As reported, energy expenditure leads to the accumulation of H+ concentration and H2O2. Then, ROS increases vasoconstriction and triggers platelet aggregation and endothelial cell permeability, affecting blood circulation [391]. Additionally, RNS plays a role in mitochondrial functions, for instance, by reducing DNA and suppressing enzymes of the mitochondria [390]. Finally, ROS and RNS bring about DNA damage, protein destruction, lipid peroxidation, and cell death, leading to poor outcomes [390,392]. As expected, the results of clinical studies have confirmed that higher plasma levels of oxidized low-density lipoprotein led to a worse prognosis [393], an increased risk of death [394] and a higher prevalence of cognitive impairment [395].
Finally, there are important molecular and signaling pathways modifications with aging [390]. Under ischemia/hypoxia conditions in the elderly, Sirt1 expression and the mitochondrial unfolded protein response decrease in aging, leading to poor mitochondrial function and fitness [396]. This condition leads to an inadequate post-translational regulation of molecular mediators, such as hypoxia-inducible factor 1α and Sirt1, and of the glycolytic-mitochondrial energy axis, all fundamental in response to hypoxic-ischemic injury [397]. In summary, OS has a central role in the “aging-stroke” system. First, when a stroke occurs in animals or patients, there is an excessive generation of ROS, causing cellular damage and brain injury [390]. Second, OS mediates inflammation, apoptosis, and the microbiota-gut-brain axis to increase the accumulation of ROS, followed by brain alteration [390]. Third, aging is a risk factor and exacerbates the progress of stroke via OS and OS-induced pathways [390]. Consequently, the administration of antioxidants could provide therapeutic ways for stroke. Indeed, the use of antioxidants in animals has been successful in treating stroke [398]; furthermore, several clinical trials show that co-antioxidants exert protections in stroke, including flavonoid and melatonin [399,400]. Moreover, clinical trials show that also acupuncture stimulates the inherent antioxidant enzyme system and inhibits the disproportionate generation of ROS, by regulating a series of molecular signaling pathways in redox modulation [401]. Acupuncture therapy has the potential in alleviating oxidative stress caused by cerebral ischemia, which may be associated with the neuroprotective effect of acupuncture [401]. In conclusion, reducing stroke frequency by preventive measures, as well as cerebrovascular dementia, is essential to avoid the natural trend of increase in the human, economic and social burden of these diseases.
5. Possible Antiaging and Antioxidant Interventions
Thanks to the technological advancements in medicine many research groups have tried to find therapeutical options for aging and its correlated effects like oxidative stress.
A well-established strategy against aging is dietary restriction (DR). This intervention has been shown to increase life span and decrease the onset and progression of age-relates pathologies, like the ones discussed in our review. Although the true mechanisms behind these beneficial effects are still to be fully grasped, many model organisms agree [402,403,404,405,406]. In particular, dietary restriction in rodents and non-human primates has shown to have cardiac preventing properties [403,407,408]. This beneficial pattern has been also confirmed in humans by trials using alternated day fasting [409]. The activation of the pathways associated with dietary restriction overlap those associated with exercise training including mTOR inhibition and Sirt activation [410,411,412]. These two pathways are strongly NO signaling associated [413,414]. These findings are backed by an increasing number of studies on cardiac aging. In fact, nutrient mediated signaling by DR influences the heart by affecting cardiac stem cells, mitochondrial efficiency, and ROS production [407,415,416]. The use of DR in clinical settings are still to be sufficiently schematized. Since the beneficial effects of DR on preventing CVD and on cardiac aging are undoubted, future studies must investigate on the application of this therapeutic strategy.
As seen throughout our review oxidative stress plays a crucial role in CVDs. For this reason, many studies have suggested the possible therapeutic application of antioxidants. Ten of thousands clinicals trials have evaluated antioxidants effects on CV events and mortality but results so far have been controversial [417,418]. Among antioxidants, vitamins have shown some effect in short term secondary CV prevention as in the case of vitamin E and C, although long term follow-up was non encouraging in humans [417]. Even more controversial is the supplementation with Vitamin A, which even worsened outcome in all-cause mortality [419,420]. Taken this disappointing outcome in vitamins use, there are still many other types of antioxidant agents and there are many potential reasons for the failure of these clinical trials [421]. Unfortunately, it is as of now impossible to use endogenous antioxidant enzymes, SOD, catalase or GPx, or any synthetic deriving molecule. Several attempts have been made to create such molecules, mimetics and or scavenging enzymes, but so far, no elements have been successful, and other molecules are still in trial [422,423,424,425,426].
Antioxidant elements of great interest in the last year for their many properties are nutraceuticals [427,428]. Nutraceuticals are nutrients contained in foods that have beneficial effects on health. They are found in nature and can be extracted, used for food supplements, or added to food as it is rare to find them in sufficient quantities to obtain benefits in natural foods [429]. Nutraceutical foods are also commonly referred to as functional foods. These are such if the food naturally contains the nutrients in the minimum quantities to obtain beneficial effects. Often the latter are obtained through chemical syntheses. Nutraceuticals are normally derived from plants, foods, and microbial sources [430]. Examples of nutraceuticals are probiotics, polyunsaturated fatty acids (omega-3, and omega-6), vitamins, and enzyme complexes. They are typically used to prevent chronic disease, improve health, delay the aging process, and increase life expectancy [431]. Nutraceuticals can be taken either in the form of a “naturally nutraceutical food” or as a “food enriched” with a specific active ingredient (for example, milk with added vitamin D or omega-3 acids). They can also be taken in the form of food supplements in liquid formulations, in tablets, capsules, and in isolated or combination [428,432]. The wide range of these molecules and the lack of knowledge in the single and combined effects make it difficult to have a precise consideration of the therapeutic strategy to implement in clinical settings [433,434]. Among these, resveratrol and Sirts activation as a DR-mimetic have elicited great research interest. Resveratrol is a compound found in grapes and wine and has been associated with many cardioprotective effects including antioxidant, cardiac anti-aging, antiaggregating, enhance eNOS signaling effects, and LDL-ox reduction effects [433,435,436]. Worth noting is resveratrol’s effect on cardiac diastolic dysfunction, in insulin resistance, and on transcriptional profile [437].
As seen before, the renin-angiotensin system (RAS) and the autonomic nervous system (ANS) play an important role in development of CVD. In particular, hypertension is the main disease deriving from these systems alteration. Angiotensin-converting enzyme inhibitors (ACE-i), which inhibits Ang-II formation, and AT-1 receptor blockers (ARB), that blocks directly Ang-II receptor activation, have been extensively used and have shown not only anti-hypertensive properties but also antioxidant ones [438]. Ang-II is a potent vasoconstrictor and pro-inflammatory factor [439]. It has been shown to activate and recruit monocytes and macrophages into the vascular wall acting as pro-fibrotic agent [440]. Therefore, basic clinical evidence has shown that attenuation of Ang-II effects leads to immediate reduction of arterial blood pressure, but some beneficial effects of ARB and ACE-I are independent from this aspect [441,442]. Inhibition of RAS is beneficial even when it is not at the stem of hypertension [443]. Thus, independently from hemodynamic effects ACE-I and ARB can exert beneficial tissue effect. In particular, ACE-I is also involved in accumulation of bradykinin which induces release of nitric oxide (NO), prostacyclin and endothelium hyperpolarizing factor [444]. By the same logic, ARB can also stimulate bradykinin, NO, and prostaglandin release [445]. Thanks to their activity ACE-I and ARB can reduce superoxide generation, increasing NO bioavailability [446,447]. Mainly, in vitro studies on captopril, enalapril and lisinopril have highlighted ACE-I scavenger properties to contrast free radicals [448]. However, not all reports agree and some highlight that only sulfhydryl ACE-I have this property and that even these may not have in vivo effect due to low tissue concentration in normal therapeutic use [449,450]. Nevertheless, studies on mice with non-hypotensive doses of ACE-I for 11-weeks increased antioxidant enzymes and glutathione content in tissues [451,452]. Interestingly, the erythrocytes of these mice were more resistant to oxidative stress [453]. Lastly, these drugs also elicited positive effects against oxidative stress in streptozotocin-induced diabetic rats [451].
Worth mentioning are mTOR inhibitors agents, like rapamycin (Sirolimus) and Everolimus [454]. These gerosuppressant drugs have been shown to slow down the aging process and extend the life span of different species [455]. Inhibitors of mTOR from worms to mammals can prevent age-related diseases like the ones we have discussed in this review [456]. Before diving in, we must remember that mTOR is a signaling pathway integrated by two protein complexes, mTORC1 and mTORC2 [457]. These two complexes differ in regulatory proteins as the first is regulated by Raptor while the second by Rictor [458]. mTOR and WNT pathways work in concert to guarantee cardiac and endothelial cells life cycle [459,460,461,462]. Overall, mTOR function has been seen to regulate proliferation/differentiation of embryonic stem cells, maintaining pluripotency of embryonic stem cells when needed [463,464]. It regulates apoptosis and autophagic cell death modulating programmed cell death [465,466]. Mice models have highlighted how mTOR can protect cardiomyocytes against ischemia/reperfusion oxidative damage and can prevent cardiac atrophy inhibiting cardiomyocytes autophagy [456,467,468,469,470,471]. Similar models have also shown how mTOR can promote proliferation of endothelial progenitor cells and endothelial cells promoting angiogenesis as well as preventing induction of matrix metalloproteinases [457,460,472,473]. Rapamycin has been used in healthy volunteers with minimal side effects to investigate its anti-aging properties [474]. Its main application so far has been in patients with transplants. Fortunately, this application has made and will allow extensive research on human subjects [475,476]. The vital regulatory pathways of mTOR as still to be completely discovered but its new therapeutic beneficial effects are so far quite fascinating [468].
The latest discoveries in the frontier of senolytic agents involve chimeric antigen receptor (CAR) T cells [477]. As extensively described before chronic accumulation of senescent cells, oxidative stress, fibrosis, and many other factors contribute to the onset of age-correlated diseases [478]. Elimination of any of these factors could be the next step to finding therapeutic strategies against aging and aging diseases [479]. To this regard, CAR-T cells have been engineered to target senescent cells in disease models. To achieve this, Amor et al. engineered CAR-T cells that could target urokinase-type plasminogen activator receptor (uPAR). This senescent-specific cell-surface protein is upregulated in senescent cells both in vivo and in vitro [480]. Amor et al. [481] have used these cells in an array of senescence-induced disease models such as lung adenocarcinoma and carbon tetrachloride and non-alcoholic steatohepatitis (NASH)-induced liver fibrosis [481,482]. The yielded results are truly promising both for efficacy and safety profile [481]. The range of therapeutic application of this new technique is broad and as of now engineered T cells are at test against cardiac fibrosis and other aging correlated diseases [483,484]. A table summarizing the trials aimed at reducing cardiovascular aging is provided (Table 1).

Table 1.
Summary results of intervention studies exploring the effect of antiaging and antioxidant strategies.
6. Conclusions and Future Perspectives
CVDs are the leading causes of death in industrialized countries of the western world and aging is one of the most significant risk factors. These countries are characterized by a constant increase in the elderly population which by 2030 is predicted to become more than 20% of the population [485]. The rapid increase of the aging population highlights the necessity to develop new and better therapeutic molecules and strategies in order to prevent, treat and better overall outcome of CVDs [3]. In order to face up to this objective it is mandatory to prevent in elderly myocardial dysfunction, left ventricle hypertrophy, diastolic dysfunction, hypertension, and all those factors that we have previously described. Addressing these aging and oxidative stress induced pathologies is fundamental in order to better cardiovascular and overall outcome [486]. Many steps are still required to fully understand all the processes linked to aging and to oxidative stress related modifications in CVD in order to prevent, better, or delay cardiovascular decay. Studies are required at all levels to reach such an ambitious goal. In particular, clinical trials are still at the beginning and although some anti-aging and antioxidant molecules have had a disappointing start, it is important to keep clinical trials going. Finding new molecules and new ways to address aging and oxidative stress is fundamental to find new potential application for cardiovascular prevention and treatment.
Author Contributions
C.I., original concept; C.I., P.V., P.D.P., V.V., A.S., and N.V., writing the article; M.C., G.G., A.C., and C.V., critical revision of the manuscript. All authors have read and agreed to the published version of the manuscript.
Funding
This research received no external funding.
Conflicts of Interest
The authors declare no conflict of interest.
References
- Hayflick, L. Biological aging is no longer an unsolved problem. Ann. N. Y. Acad. Sci. 2007, 1100, 1–13. [Google Scholar] [CrossRef] [PubMed]
- Pepe, S.; Lakatta, E.G. Aging hearts and vessels: Masters of adaptation and survival. Cardiovasc. Res. 2005, 66, 190–193. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Izzo, C.; Carrizzo, A.; Alfano, A.; Virtuoso, N.; Capunzo, M.; Calabrese, M.; De Simone, E.; Sciarretta, S.; Frati, G.; Oliveti, M.; et al. The Impact of Aging on Cardio and Cerebrovascular Diseases. Int. J. Mol. Sci. 2018, 19, 481. [Google Scholar] [CrossRef] [PubMed]
- Heidenreich, P.A.; Trogdon, J.G.; Khavjou, O.A.; Butler, J.; Dracup, K.; Ezekowitz, M.D.; Finkelstein, E.A.; Hong, Y.; Johnston, S.C.; Khera, A.; et al. Forecasting the future of cardiovascular disease in the United States: A policy statement from the American Heart Association. Circulation 2011, 123, 933–944. [Google Scholar] [CrossRef]
- Tarride, J.E.; Lim, M.; DesMeules, M.; Luo, W.; Burke, N.; O’Reilly, D.; Bowen, J.; Goeree, R. A review of the cost of cardiovascular disease. Can. J. Cardiol. 2009, 25, 195–202. [Google Scholar] [CrossRef]
- Senoner, T.; Dichtl, W. Oxidative Stress in Cardiovascular Diseases: Still a Therapeutic Target? Nutrients 2019, 11, 2090. [Google Scholar] [CrossRef]
- Scuteri, A.; Lakatta, E.G. Bringing prevention in geriatrics: Evidences from cardiovascular medicine supporting the new challenge. Exp. Gerontol. 2013, 48, 64–68. [Google Scholar] [CrossRef][Green Version]
- Tsutsui, H.; Kinugawa, S.; Matsushima, S. Oxidative stress and heart failure. Am. J. Physiol. Heart Circ. Physiol. 2011, 301, 2181–2190. [Google Scholar] [CrossRef]
- Tahhan, A.S.; Sandesara, P.B.; Hayek, S.S.; Alkhoder, A.; Chivukula, K.; Hammadah, M.; Mohamed-Kelli, H.; O’Neal, W.T.; Topel, M.; Ghasemzadeh, N.; et al. Association between oxidative stress and atrial fibrillation. Heart Rhythm 2017, 14, 1849–1855. [Google Scholar] [CrossRef]
- Baradaran, A.; Nasri, H.; Rafieian-Kopaei, M. Oxidative stress and hypertension: Possibility of hypertension therapy with antioxidants. J. Res. Med. Sci. 2014, 19, 358–367. [Google Scholar]
- Kattoor, A.J.; Pothineni, N.V.K.; Palagiri, D.; Mehta, J.L. Oxidative Stress in Atherosclerosis. Curr. Atheroscler. Rep. 2017, 19, 42. [Google Scholar] [CrossRef] [PubMed]
- Holmstrom, K.M.; Finkel, T. Cellular mechanisms and physiological consequences of redox-dependent signalling. Nat. Rev. Mol. Cell Biol. 2014, 15, 411–421. [Google Scholar] [CrossRef] [PubMed]
- Finkel, T. Signal transduction by reactive oxygen species. J. Cell Biol. 2011, 194, 7–15. [Google Scholar] [CrossRef] [PubMed]
- Balaban, R.S.; Nemoto, S.; Finkel, T. Mitochondria, oxidants, and aging. Cell 2005, 120, 483–495. [Google Scholar] [CrossRef]
- Sies, H.; Berndt, C.; Jones, D.P. Oxidative Stress. Annu. Rev. Biochem. 2017, 86, 715–748. [Google Scholar] [CrossRef]
- North, B.J.; Sinclair, D.A. The intersection between aging and cardiovascular disease. Circ. Res. 2012, 110, 1097–1108. [Google Scholar] [CrossRef]
- Beckman, K.B.; Ames, B.N. The free radical theory of aging matures. Physiol. Rev. 1998, 78, 547–581. [Google Scholar] [CrossRef]
- Cosentino, F.; Francia, P.; Camici, G.G.; Pelicci, P.G.; Luscher, T.F.; Volpe, M. Final common molecular pathways of aging and cardiovascular disease: Role of the p66Shc protein. Arterioscler. Thromb. Vasc. Biol. 2008, 28, 622–628. [Google Scholar] [CrossRef]
- Sudheesh, N.P.; Ajith, T.A.; Ramnath, V.; Janardhanan, K.K. Therapeutic potential of Ganoderma lucidum (Fr.) P. Karst. against the declined antioxidant status in the mitochondria of post-mitotic tissues of aged mice. Clin. Nutr. 2010, 29, 406–412. [Google Scholar] [CrossRef]
- Raha, S.; Robinson, B.H. Mitochondria, oxygen free radicals, disease and ageing. Trends Biochem. Sci. 2000, 25, 502–508. [Google Scholar] [CrossRef]
- Lyu, S.Y.; Kwon, Y.J.; Joo, H.J.; Park, W.B. Preparation of alginate/chitosan microcapsules and enteric coated granules of mistletoe lectin. Arch. Pharm. Res. 2004, 27, 118–126. [Google Scholar] [CrossRef]
- Piquereau, J.; Caffin, F.; Novotova, M.; Lemaire, C.; Veksler, V.; Garnier, A.; Ventura-Clapier, R.; Joubert, F. Mitochondrial dynamics in the adult cardiomyocytes: Which roles for a highly specialized cell? Front. Physiol. 2013, 4, 102. [Google Scholar] [CrossRef]
- van der Loo, B.; Labugger, R.; Skepper, J.N.; Bachschmid, M.; Kilo, J.; Powell, J.M.; Palacios-Callender, M.; Erusalimsky, J.D.; Quaschning, T.; Malinski, T.; et al. Enhanced peroxynitrite formation is associated with vascular aging. J. Exp. Med. 2000, 192, 1731–1744. [Google Scholar] [CrossRef]
- Ungvari, Z.; Bagi, Z.; Feher, A.; Recchia, F.A.; Sonntag, W.E.; Pearson, K.; de Cabo, R.; Csiszar, A. Resveratrol confers endothelial protection via activation of the antioxidant transcription factor Nrf2. Am. J. Physiol. Heart Circ. Physiol. 2010, 299, 18–24. [Google Scholar] [CrossRef]
- Zhang, D.X.; Gutterman, D.D. Mitochondrial reactive oxygen species-mediated signaling in endothelial cells. Am. J. Physiol. Heart Circ. Physiol. 2007, 292, 2023–2031. [Google Scholar] [CrossRef]
- Krause, K.H. Aging: A revisited theory based on free radicals generated by NOX family NADPH oxidases. Exp. Gerontol. 2007, 42, 256–262. [Google Scholar] [CrossRef]
- Guzik, T.J.; Chen, W.; Gongora, M.C.; Guzik, B.; Lob, H.E.; Mangalat, D.; Hoch, N.; Dikalov, S.; Rudzinski, P.; Kapelak, B.; et al. Calcium-dependent NOX5 nicotinamide adenine dinucleotide phosphate oxidase contributes to vascular oxidative stress in human coronary artery disease. J. Am. Coll. Cardiol. 2008, 52, 1803–1809. [Google Scholar] [CrossRef]
- Rodriguez-Manas, L.; El-Assar, M.; Vallejo, S.; Lopez-Doriga, P.; Solis, J.; Petidier, R.; Montes, M.; Nevado, J.; Castro, M.; Gomez-Guerrero, C.; et al. Endothelial dysfunction in aged humans is related with oxidative stress and vascular inflammation. Aging Cell 2009, 8, 226–238. [Google Scholar] [CrossRef]
- Forstermann, U.; Munzel, T. Endothelial nitric oxide synthase in vascular disease: From marvel to menace. Circulation 2006, 113, 1708–1714. [Google Scholar] [CrossRef]
- Stuehr, D.; Pou, S.; Rosen, G.M. Oxygen reduction by nitric-oxide synthases. J. Biol. Chem. 2001, 276, 14533–14536. [Google Scholar] [CrossRef]
- Brandes, R.P.; Fleming, I.; Busse, R. Endothelial aging. Cardiovasc. Res. 2005, 66, 286–294. [Google Scholar] [CrossRef] [PubMed]
- Dikalov, S. Cross talk between mitochondria and NADPH oxidases. Free Radic. Biol. Med. 2011, 51, 1289–1301. [Google Scholar] [CrossRef] [PubMed]
- Phaniendra, A.; Jestadi, D.B.; Periyasamy, L. Free radicals: Properties, sources, targets, and their implication in various diseases. Indian J. Clin. Biochem. 2015, 30, 11–26. [Google Scholar] [CrossRef] [PubMed]
- Barreiro, E. Role of Protein Carbonylation in Skeletal Muscle Mass Loss Associated with Chronic Conditions. Proteomes 2016, 4, 18. [Google Scholar] [CrossRef]
- Frijhoff, J.; Winyard, P.G.; Zarkovic, N.; Davies, S.S.; Stocker, R.; Cheng, D.; Knight, A.R.; Taylor, E.L.; Oettrich, J.; Ruskovska, T.; et al. Clinical Relevance of Biomarkers of Oxidative Stress. Antioxid. Redox Signal. 2015, 23, 1144–1170. [Google Scholar] [CrossRef]
- Spickett, C.M. The lipid peroxidation product 4-hydroxy-2-nonenal: Advances in chemistry and analysis. Redox Biol. 2013, 1, 145–152. [Google Scholar] [CrossRef]
- Demissie, S.; Levy, D.; Benjamin, E.J.; Cupples, L.A.; Gardner, J.P.; Herbert, A.; Kimura, M.; Larson, M.G.; Meigs, J.B.; Keaney, J.F.; et al. Insulin resistance, oxidative stress, hypertension, and leukocyte telomere length in men from the Framingham Heart Study. Aging Cell 2006, 5, 325–330. [Google Scholar] [CrossRef]
- Fitzpatrick, A.L.; Kronmal, R.A.; Gardner, J.P.; Psaty, B.M.; Jenny, N.S.; Tracy, R.P.; Walston, J.; Kimura, M.; Aviv, A. Leukocyte telomere length and cardiovascular disease in the cardiovascular health study. Am. J. Epidemiol. 2007, 165, 14–21. [Google Scholar] [CrossRef]
- Liu, S.; Hui, K.S.; Hui, K.N. Flower-like Copper Cobaltite Nanosheets on Graphite Paper as High-Performance Supercapacitor Electrodes and Enzymeless Glucose Sensors. ACS Appl. Mater. Interfaces 2016, 8, 3258–3267. [Google Scholar] [CrossRef]
- Chandrasekaran, A.; Idelchik, M.; Melendez, J.A. Redox control of senescence and age-related disease. Redox Biol. 2017, 11, 91–102. [Google Scholar] [CrossRef]
- Liguori, I.; Russo, G.; Curcio, F.; Bulli, G.; Aran, L.; Della-Morte, D.; Gargiulo, G.; Testa, G.; Cacciatore, F.; Bonaduce, D.; et al. Oxidative stress, aging, and diseases. Clin. Interv. Aging 2018, 13, 757–772. [Google Scholar] [CrossRef] [PubMed]
- Ferrara, N.; Rinaldi, B.; Corbi, G.; Conti, V.; Stiuso, P.; Boccuti, S.; Rengo, G.; Rossi, F.; Filippelli, A. Exercise training promotes SIRT1 activity in aged rats. Rejuvenation Res. 2008, 11, 139–150. [Google Scholar] [CrossRef]
- Ren, J.; Pulakat, L.; Whaley-Connell, A.; Sowers, J.R. Mitochondrial biogenesis in the metabolic syndrome and cardiovascular disease. J. Mol. Med. 2010, 88, 993–1001. [Google Scholar] [CrossRef] [PubMed]
- Neubauer, S. The failing heart—An engine out of fuel. N. Engl. J. Med. 2007, 356, 1140–1151. [Google Scholar] [CrossRef] [PubMed]
- López-Otín, C.; Blasco, M.A.; Partridge, L.; Serrano, M.; Kroemer, G. The hallmarks of aging. Cell 2013, 153, 1194–1217. [Google Scholar] [CrossRef] [PubMed]
- Harman, D. The biologic clock: The mitochondria? J. Am. Geriatr. Soc. 1972, 20, 145–147. [Google Scholar] [CrossRef]
- Garinis, G.A.; van der Horst, G.T.; Vijg, J.; Hoeijmakers, J.H. DNA damage and ageing: New-age ideas for an age-old problem. Nat. Cell Biol. 2008, 10, 1241–1247. [Google Scholar] [CrossRef]
- Gredilla, R.; Bohr, V.A.; Stevnsner, T. Mitochondrial DNA repair and association with aging—An update. Exp. Gerontol. 2010, 45, 478–488. [Google Scholar] [CrossRef]
- Grollman, A.P.; Moriya, M. Mutagenesis by 8-oxoguanine: An enemy within. Trends Genet. 1993, 9, 246–249. [Google Scholar] [CrossRef]
- Kavli, B.; Otterlei, M.; Slupphaug, G.; Krokan, H.E. Uracil in DNA—General mutagen, but normal intermediate in acquired immunity. DNA Repair 2007, 6, 505–516. [Google Scholar] [CrossRef]
- Gredilla, R.; Garm, C.; Stevnsner, T. Nuclear and mitochondrial DNA repair in selected eukaryotic aging model systems. Oxidative Med. Cell. Longev. 2012, 2012, 282438. [Google Scholar] [CrossRef] [PubMed]
- Dai, D.F.; Rabinovitch, P.S. Cardiac aging in mice and humans: The role of mitochondrial oxidative stress. Trends Cardiovasc. Med. 2009, 19, 213–220. [Google Scholar] [CrossRef] [PubMed]
- Wang, J.; Wilhelmsson, H.; Graff, C.; Li, H.; Oldfors, A.; Rustin, P.; Brüning, J.C.; Kahn, C.R.; Clayton, D.A.; Barsh, G.S.; et al. Dilated cardiomyopathy and atrioventricular conduction blocks induced by heart-specific inactivation of mitochondrial DNA gene expression. Nat. Genet. 1999, 21, 133–137. [Google Scholar] [CrossRef] [PubMed]
- Wang, J.; Silva, J.P.; Gustafsson, C.M.; Rustin, P.; Larsson, N.G. Increased in vivo apoptosis in cells lacking mitochondrial DNA gene expression. Proc. Natl. Acad. Sci. USA 2001, 98, 4038–4043. [Google Scholar] [CrossRef]
- Vermulst, M.; Wanagat, J.; Kujoth, G.C.; Bielas, J.H.; Rabinovitch, P.S.; Prolla, T.A.; Loeb, L.A. DNA deletions and clonal mutations drive premature aging in mitochondrial mutator mice. Nat. Genet. 2008, 40, 392–394. [Google Scholar] [CrossRef]
- Edgar, D.; Shabalina, I.; Camara, Y.; Wredenberg, A.; Calvaruso, M.A.; Nijtmans, L.; Nedergaard, J.; Cannon, B.; Larsson, N.G.; Trifunovic, A. Random point mutations with major effects on protein-coding genes are the driving force behind premature aging in mtDNA mutator mice. Cell Metab. 2009, 10, 131–138. [Google Scholar] [CrossRef]
- Baris, O.R.; Ederer, S.; Neuhaus, J.F.; von Kleist-Retzow, J.C.; Wunderlich, C.M.; Pal, M.; Wunderlich, F.T.; Peeva, V.; Zsurka, G.; Kunz, W.S.; et al. Mosaic Deficiency in Mitochondrial Oxidative Metabolism Promotes Cardiac Arrhythmia during Aging. Cell Metab. 2015, 21, 667–677. [Google Scholar] [CrossRef]
- Kujoth, G.C.; Leeuwenburgh, C.; Prolla, T.A. Mitochondrial DNA mutations and apoptosis in mammalian aging. Cancer Res. 2006, 66, 7386–7389. [Google Scholar] [CrossRef]
- Tower, J. Programmed cell death in aging. Ageing Res. Rev. 2015, 23, 90–100. [Google Scholar] [CrossRef]
- Modrego, J.; de las Heras, N.; Zamorano-León, J.J.; Mateos-Cáceres, P.J.; Martín-Fernández, B.; Valero-Muñoz, M.; Lahera, V.; López-Farré, A.J. Changes in cardiac energy metabolic pathways in overweighed rats fed a high-fat diet. Eur. J. Nutr. 2013, 52, 847–856. [Google Scholar] [CrossRef]
- Opie, L.H.; Knuuti, J. The adrenergic-fatty acid load in heart failure. J. Am. Coll. Cardiol. 2009, 54, 1637–1646. [Google Scholar] [CrossRef] [PubMed]
- Dai, D.F.; Hsieh, E.J.; Liu, Y.; Chen, T.; Beyer, R.P.; Chin, M.T.; MacCoss, M.J.; Rabinovitch, P.S. Mitochondrial proteome remodelling in pressure overload-induced heart failure: The role of mitochondrial oxidative stress. Cardiovasc. Res. 2012, 93, 79–88. [Google Scholar] [CrossRef] [PubMed]
- De Meyer, G.R.; De Keulenaer, G.W.; Martinet, W. Role of autophagy in heart failure associated with aging. Heart Fail. Rev. 2010, 15, 423–430. [Google Scholar] [CrossRef] [PubMed]
- Terman, A.; Kurz, T.; Navratil, M.; Arriaga, E.A.; Brunk, U.T. Mitochondrial turnover and aging of long-lived postmitotic cells: The mitochondrial-lysosomal axis theory of aging. Antioxid. Redox Signal. 2010, 12, 503–535. [Google Scholar] [CrossRef]
- Upadhya, B.; Taffet, G.E.; Cheng, C.P.; Kitzman, D.W. Heart failure with preserved ejection fraction in the elderly: Scope of the problem. J. Mol. Cell. Cardiol. 2015, 83, 73–87. [Google Scholar] [CrossRef]
- Campbell, S.G.; Haynes, P.; Kelsey Snapp, W.; Nava, K.E.; Campbell, K.S. Altered ventricular torsion and transmural patterns of myocyte relaxation precede heart failure in aging F344 rats. Am. J. Physiol. Heart Circ. Physiol. 2013, 305, 676–686. [Google Scholar] [CrossRef]
- Boluyt, M.O.; Converso, K.; Hwang, H.S.; Mikkor, A.; Russell, M.W. Echocardiographic assessment of age-associated changes in systolic and diastolic function of the female F344 rat heart. J. Appl. Physiol. 2004, 96, 822–828. [Google Scholar] [CrossRef]
- Maruyama, Y. Aging and arterial-cardiac interactions in the elderly. Int. J. Cardiol. 2012, 155, 14–19. [Google Scholar] [CrossRef]
- Juhaszova, M.; Rabuel, C.; Zorov, D.B.; Lakatta, E.G.; Sollott, S.J. Protection in the aged heart: Preventing the heart-break of old age? Cardiovasc. Res. 2005, 66, 233–244. [Google Scholar] [CrossRef]
- Mirza, M.; Strunets, A.; Shen, W.K.; Jahangir, A. Mechanisms of arrhythmias and conduction disorders in older adults. Clin. Geriatr. Med. 2012, 28, 555–573. [Google Scholar] [CrossRef]
- Strait, J.B.; Lakatta, E.G. Aging-associated cardiovascular changes and their relationship to heart failure. Heart Fail. Clin. 2012, 8, 143–164. [Google Scholar] [CrossRef]
- Dhahbi, J.M.; Tsuchiya, T.; Kim, H.J.; Mote, P.L.; Spindler, S.R. Gene expression and physiologic responses of the heart to the initiation and withdrawal of caloric restriction. J. Gerontol. A Biol. Sci. Med. Sci. 2006, 61, 218–231. [Google Scholar] [CrossRef] [PubMed]
- Lakatta, E.G. Cardiovascular regulatory mechanisms in advanced age. Physiol. Rev. 1993, 73, 413–467. [Google Scholar] [CrossRef] [PubMed]
- Coleman, R.; Silbermann, M.; Gershon, D.; Reznick, A.Z. Giant mitochondria in the myocardium of aging and endurance-trained mice. Gerontology 1987, 33, 34–39. [Google Scholar] [CrossRef] [PubMed]
- Muscari, C.; Finelli, C.; Stefanelli, C.; Flamigni, F.; Guarnieri, C.; Caldarera, C.M. Age-dependent differences of ATP breakdown and ATP-catabolite release in ischemic and reperfused hearts. Mech. Ageing Dev. 1993, 67, 1–11. [Google Scholar] [CrossRef]
- Muscari, C.; Caldarera, C.M.; Guarnieri, C. Age-dependent production of mitochondrial hydrogen peroxide, lipid peroxides and fluorescent pigments in the rat heart. Basic Res. Cardiol. 1990, 85, 172–178. [Google Scholar] [CrossRef] [PubMed]
- Sohal, R.S.; Sohal, B.H. Hydrogen peroxide release by mitochondria increases during aging. Mech. Ageing Dev. 1991, 57, 187–202. [Google Scholar] [CrossRef]
- Liu, F.; Li, N.; Long, B.; Fan, Y.Y.; Liu, C.Y.; Zhou, Q.Y.; Murtaza, I.; Wang, K.; Li, P.F. Cardiac hypertrophy is negatively regulated by miR-541. Cell Death Dis. 2014, 5, e1171. [Google Scholar] [CrossRef]
- Fajemiroye, J.O.; da Cunha, L.C.; Saavedra-Rodriguez, R.; Rodrigues, K.L.; Naves, L.M.; Mourao, A.A.; da Silva, E.F.; Williams, N.E.E.; Martins, J.L.R.; Sousa, R.B.; et al. Aging-Induced Biological Changes and Cardiovascular Diseases. Biomed. Res. Int. 2018, 2018, 7156435. [Google Scholar] [CrossRef]
- Olivetti, G.; Melissari, M.; Capasso, J.M.; Anversa, P. Cardiomyopathy of the aging human heart. Myocyte loss and reactive cellular hypertrophy. Circ. Res. 1991, 68, 1560–1568. [Google Scholar] [CrossRef]
- Hees, P.S.; Fleg, J.L.; Lakatta, E.G.; Shapiro, E.P. Left ventricular remodeling with age in normal men versus women: Novel insights using three-dimensional magnetic resonance imaging. Am. J. Cardiol. 2002, 90, 1231–1236. [Google Scholar] [CrossRef]
- Olivetti, G.; Giordano, G.; Corradi, D.; Melissari, M.; Lagrasta, C.; Gambert, S.R.; Anversa, P. Gender differences and aging: Effects on the human heart. J. Am. Coll. Cardiol. 1995, 26, 1068–1079. [Google Scholar] [CrossRef]
- Kajstura, J.; Cheng, W.; Sarangarajan, R.; Li, P.; Li, B.; Nitahara, J.A.; Chapnick, S.; Reiss, K.; Olivetti, G.; Anversa, P. Necrotic and apoptotic myocyte cell death in the aging heart of Fischer 344 rats. Am. J. Physiol. 1996, 271, 1215–1228. [Google Scholar] [CrossRef]
- Sheydina, A.; Riordon, D.R.; Boheler, K.R. Molecular mechanisms of cardiomyocyte aging. Clin. Sci. 2011, 121, 315–329. [Google Scholar] [CrossRef]
- Dai, D.F.; Chen, T.; Johnson, S.C.; Szeto, H.; Rabinovitch, P.S. Cardiac aging: From molecular mechanisms to significance in human health and disease. Antioxid. Redox Signal. 2012, 16, 1492–1526. [Google Scholar] [CrossRef]
- Leon, L.J.; Gustafsson, A.B. Staying young at heart: Autophagy and adaptation to cardiac aging. J. Mol. Cell. Cardiol. 2016, 95, 78–85. [Google Scholar] [CrossRef]
- AlGhatrif, M.; Lakatta, E.G. The conundrum of arterial stiffness, elevated blood pressure, and aging. Curr. Hypertens. Rep. 2015, 17, 12. [Google Scholar] [CrossRef]
- Gerstenblith, G.; Frederiksen, J.; Yin, F.C.; Fortuin, N.J.; Lakatta, E.G.; Weisfeldt, M.L. Echocardiographic assessment of a normal adult aging population. Circulation 1977, 56, 273–278. [Google Scholar] [CrossRef]
- Schulman, S.P.; Lakatta, E.G.; Fleg, J.L.; Lakatta, L.; Becker, L.C.; Gerstenblith, G. Age-related decline in left ventricular filling at rest and exercise. Am. J. Physiol. 1992, 263, 1932–1938. [Google Scholar] [CrossRef]
- Miller, T.R.; Grossman, S.J.; Schectman, K.B.; Biello, D.R.; Ludbrook, P.A.; Ehsani, A.A. Left ventricular diastolic filling and its association with age. Am. J. Cardiol. 1986, 58, 531–535. [Google Scholar] [CrossRef]
- Howden, E.J.; Carrick-Ranson, G.; Sarma, S.; Hieda, M.; Fujimoto, N.; Levine, B.D. Effects of Sedentary Aging and Lifelong Exercise on Left Ventricular Systolic Function. Med. Sci. Sports Exerc. 2018, 50, 494–501. [Google Scholar] [CrossRef] [PubMed]
- Peverill, R.E. Aging and the relationships between long-axis systolic and early diastolic excursion, isovolumic relaxation time and left ventricular length-Implications for the interpretation of aging effects on e. PLoS ONE 2019, 14, e0210277. [Google Scholar] [CrossRef]
- Fleg, J.L.; O’Connor, F.; Gerstenblith, G.; Becker, L.C.; Clulow, J.; Schulman, S.P.; Lakatta, E.G. Impact of age on the cardiovascular response to dynamic upright exercise in healthy men and women. J. Appl. Physiol. 1995, 78, 890–900. [Google Scholar] [CrossRef] [PubMed]
- Silaghi, A.; Piercecchi-Marti, M.D.; Grino, M.; Leonetti, G.; Alessi, M.C.; Clement, K.; Dadoun, F.; Dutour, A. Epicardial adipose tissue extent: Relationship with age, body fat distribution, and coronaropathy. Obesity 2008, 16, 2424–2430. [Google Scholar] [CrossRef]
- Horn, M.A.; Trafford, A.W. Aging and the cardiac collagen matrix: Novel mediators of fibrotic remodelling. J. Mol. Cell. Cardiol. 2016, 93, 175–185. [Google Scholar] [CrossRef]
- Biernacka, A.; Frangogiannis, N.G. Aging and Cardiac Fibrosis. Aging Dis. 2011, 2, 158–173. [Google Scholar]
- Jugdutt, B.I.; Jelani, A.; Palaniyappan, A.; Idikio, H.; Uweira, R.E.; Menon, V.; Jugdutt, C.E. Aging-related early changes in markers of ventricular and matrix remodeling after reperfused ST-segment elevation myocardial infarction in the canine model: Effect of early therapy with an angiotensin II type 1 receptor blocker. Circulation 2010, 122, 341–351. [Google Scholar] [CrossRef]
- Mendes, A.B.; Ferro, M.; Rodrigues, B.; Souza, M.R.; Araujo, R.C.; Souza, R.R. Quantification of left ventricular myocardial collagen system in children, young adults, and the elderly. Medicina 2012, 72, 216–220. [Google Scholar]
- Burstein, B.; Nattel, S. Atrial fibrosis: Mechanisms and clinical relevance in atrial fibrillation. J. Am. Coll. Cardiol. 2008, 51, 802–809. [Google Scholar] [CrossRef]
- Everett, T.H.T.; Li, H.; Mangrum, J.M.; McRury, I.D.; Mitchell, M.A.; Redick, J.A.; Haines, D.E. Electrical, morphological, and ultrastructural remodeling and reverse remodeling in a canine model of chronic atrial fibrillation. Circulation 2000, 102, 1454–1460. [Google Scholar] [CrossRef]
- Virdis, A.; Ghiadoni, L.; Giannarelli, C.; Taddei, S. Endothelial dysfunction and vascular disease in later life. Maturitas 2010, 67, 20–24. [Google Scholar] [CrossRef] [PubMed]
- Toda, N. Age-related changes in endothelial function and blood flow regulation. Pharmacol. Ther. 2012, 133, 159–176. [Google Scholar] [CrossRef] [PubMed]
- Matz, R.L.; Andriantsitohaina, R. Age-related endothelial dysfunction: Potential implications for pharmacotherapy. Drugs Aging 2003, 20, 527–550. [Google Scholar] [CrossRef] [PubMed]
- Qian, H.; Luo, N.; Chi, Y. Aging-shifted prostaglandin profile in endothelium as a factor in cardiovascular disorders. J. Aging Res. 2012, 2012, 121390. [Google Scholar] [CrossRef] [PubMed]
- Schrage, W.G.; Eisenach, J.H.; Joyner, M.J. Ageing reduces nitric-oxide- and prostaglandin-mediated vasodilatation in exercising humans. J. Physiol. 2007, 579, 227–236. [Google Scholar] [CrossRef]
- Nicholson, W.T.; Vaa, B.; Hesse, C.; Eisenach, J.H.; Joyner, M.J. Aging is associated with reduced prostacyclin-mediated dilation in the human forearm. Hypertension 2009, 53, 973–978. [Google Scholar] [CrossRef]
- Dere, E.; De Souza Silva, M.A.; Topic, B.; Fiorillo, C.; Li, J.S.; Sadile, A.G.; Frisch, C.; Huston, J.P. Aged endothelial nitric oxide synthase knockout mice exhibit higher mortality concomitant with impaired open-field habituation and alterations in forebrain neurotransmitter levels. Genes Brain Behav. 2002, 1, 204–213. [Google Scholar] [CrossRef]
- Zhong, L.; D’Urso, A.; Toiber, D.; Sebastian, C.; Henry, R.E.; Vadysirisack, D.D.; Guimaraes, A.; Marinelli, B.; Wikstrom, J.D.; Nir, T.; et al. The histone deacetylase Sirt6 regulates glucose homeostasis via Hif1alpha. Cell 2010, 140, 280–293. [Google Scholar] [CrossRef]
- Cau, S.B.; Carneiro, F.S.; Tostes, R.C. Differential modulation of nitric oxide synthases in aging: Therapeutic opportunities. Front. Physiol. 2012, 3, 218. [Google Scholar] [CrossRef]
- Yang, Y.M.; Huang, A.; Kaley, G.; Sun, D. eNOS uncoupling and endothelial dysfunction in aged vessels. Am. J. Physiol. Heart Circ. Physiol. 2009, 297, H1829–H1836. [Google Scholar] [CrossRef]
- Szabo, C.; Ischiropoulos, H.; Radi, R. Peroxynitrite: Biochemistry, pathophysiology and development of therapeutics. Nat. Rev. Drug Discov. 2007, 6, 662–680. [Google Scholar] [CrossRef] [PubMed]
- Guzik, T.J.; Mussa, S.; Gastaldi, D.; Sadowski, J.; Ratnatunga, C.; Pillai, R.; Channon, K.M. Mechanisms of increased vascular superoxide production in human diabetes mellitus: Role of NAD(P)H oxidase and endothelial nitric oxide synthase. Circulation 2002, 105, 1656–1662. [Google Scholar] [CrossRef] [PubMed]
- Scuteri, A.; Tesauro, M.; Rizza, S.; Iantorno, M.; Federici, M.; Lauro, D.; Campia, U.; Turriziani, M.; Fusco, A.; Cocciolillo, G.; et al. Endothelial function and arterial stiffness in normotensive normoglycemic first-degree relatives of diabetic patients are independent of the metabolic syndrome. Nutr. Metab. Cardiovasc. Dis. 2008, 18, 349–356. [Google Scholar] [CrossRef] [PubMed]
- Virmani, R.; Avolio, A.P.; Mergner, W.J.; Robinowitz, M.; Herderick, E.E.; Cornhill, J.F.; Guo, S.Y.; Liu, T.H.; Ou, D.Y.; O’Rourke, M. Effect of aging on aortic morphology in populations with high and low prevalence of hypertension and atherosclerosis. Comparison between occidental and Chinese communities. Am. J. Pathol. 1991, 139, 1119–1129. [Google Scholar] [PubMed]
- Tao, J.; Wang, Y.; Yang, Z.; Tu, C.; Xu, M.G.; Wang, J.M. Circulating endothelial progenitor cell deficiency contributes to impaired arterial elasticity in persons of advancing age. J. Hum. Hypertens. 2006, 20, 490–495. [Google Scholar] [CrossRef]
- Edelberg, J.M.; Reed, M.J. Aging and angiogenesis. Front. Biosci. 2003, 8, 1199–1209. [Google Scholar] [CrossRef]
- Williamson, K.; Stringer, S.E.; Alexander, M.Y. Endothelial progenitor cells enter the aging arena. Front. Physiol. 2012, 3, 30. [Google Scholar] [CrossRef]
- Lakatta, E.G.; Levy, D. Arterial and cardiac aging: Major shareholders in cardiovascular disease enterprises: Part I: Aging arteries: A “set up” for vascular disease. Circulation 2003, 107, 139–146. [Google Scholar] [CrossRef]
- Greenwald, S.E. Ageing of the conduit arteries. J. Pathol. 2007, 211, 157–172. [Google Scholar] [CrossRef]
- Elliott, H.L.; Sumner, D.J.; McLean, K.; Reid, J.L. Effect of age on the responsiveness of vascular alpha-adrenoceptors in man. J. Cardiovasc. Pharmacol. 1982, 4, 388–392. [Google Scholar] [CrossRef]
- Vaitkevicius, P.V.; Fleg, J.L.; Engel, J.H.; O’Connor, F.C.; Wright, J.G.; Lakatta, L.E.; Yin, F.C.; Lakatta, E.G. Effects of age and aerobic capacity on arterial stiffness in healthy adults. Circulation 1993, 88, 1456–1462. [Google Scholar] [CrossRef] [PubMed]
- Egashira, K.; Inou, T.; Hirooka, Y.; Kai, H.; Sugimachi, M.; Suzuki, S.; Kuga, T.; Urabe, Y.; Takeshita, A. Effects of age on endothelium-dependent vasodilation of resistance coronary artery by acetylcholine in humans. Circulation 1993, 88, 77–81. [Google Scholar] [CrossRef] [PubMed]
- Taddei, S.; Virdis, A.; Mattei, P.; Ghiadoni, L.; Gennari, A.; Fasolo, C.B.; Sudano, I.; Salvetti, A. Aging and endothelial function in normotensive subjects and patients with essential hypertension. Circulation 1995, 91, 1981–1987. [Google Scholar] [CrossRef] [PubMed]
- Hotta, H.; Uchida, S. Aging of the autonomic nervous system and possible improvements in autonomic activity using somatic afferent stimulation. Geriatr. Gerontol. Int. 2010, 10, 127–136. [Google Scholar] [CrossRef] [PubMed]
- Niu, S.W.; Huang, J.C.; Chen, S.C.; Lin, H.Y.; Kuo, I.C.; Wu, P.Y.; Chiu, Y.W.; Chang, J.M. Association between Age and Changes in Heart Rate Variability after Hemodialysis in Patients with Diabetes. Front. Aging Neurosci. 2018, 10, 43. [Google Scholar] [CrossRef]
- Bonnemeier, H.; Richardt, G.; Potratz, J.; Wiegand, U.K.; Brandes, A.; Kluge, N.; Katus, H.A. Circadian profile of cardiac autonomic nervous modulation in healthy subjects: Differing effects of aging and gender on heart rate variability. J. Cardiovasc. Electrophysiol. 2003, 14, 791–799. [Google Scholar] [CrossRef] [PubMed]
- Britton, A.; Shipley, M.; Malik, M.; Hnatkova, K.; Hemingway, H.; Marmot, M. Changes in heart rate and heart rate variability over time in middle-aged men and women in the general population (from the Whitehall II Cohort Study). Am. J. Cardiol. 2007, 100, 524–527. [Google Scholar] [CrossRef]
- Lipsitz, L.A.; Mietus, J.; Moody, G.B.; Goldberger, A.L. Spectral characteristics of heart rate variability before and during postural tilt. Relations to aging and risk of syncope. Circulation 1990, 81, 1803–1810. [Google Scholar] [CrossRef]
- Kanegusuku, H.; Queiroz, A.C.; Silva, V.J.; de Mello, M.T.; Ugrinowitsch, C.; Forjaz, C.L. High-Intensity Progressive Resistance Training Increases Strength With No Change in Cardiovascular Function and Autonomic Neural Regulation in Older Adults. J. Aging Phys. Act. 2015, 23, 339–345. [Google Scholar] [CrossRef]
- Masuki, S.; Morikawa, M.; Nose, H. Interval Walking Training Can Increase Physical Fitness in Middle-Aged and Older People. Exerc. Sport Sci. Rev. 2017, 45, 154–162. [Google Scholar] [CrossRef]
- Guedes, J.M.; Pieri, B.; Luciano, T.F.; Marques, S.O.; Guglielmo, L.G.A.; Souza, C.T. Muscular resistance, hypertrophy and strength training equally reduce adiposity, inflammation and insulin resistance in mice with diet-induced obesity. Einstein 2020, 18, eAO4784. [Google Scholar] [CrossRef]
- Masuda, M.; Yamada, T.; Mizuno, H.; Minamiguchi, H.; Konishi, S.; Ohtani, T.; Yamaguchi, O.; Okuyama, Y.; Uematsu, M.; Sakata, Y. Impact of atrial fibrillation ablation on cardiac sympathetic nervous system in patients with and without heart failure. Int. J. Cardiol. 2015, 199, 65–70. [Google Scholar] [CrossRef] [PubMed]
- Tegene, E.; Tadesse, I.; Markos, Y.; Gobena, T. Prevalence and risk factors for atrial fibrillation and its anticoagulant requirement in adults aged >/=40 in Jimma Town, Southwest Ethiopia: A community based cross-sectional study. Int. J. Cardiol. Heart Vasc. 2019, 22, 199–204. [Google Scholar] [CrossRef] [PubMed]
- Xi, Y.; Cheng, J. Dysfunction of the autonomic nervous system in atrial fibrillation. J. Thorac. Dis. 2015, 7, 193–198. [Google Scholar] [CrossRef] [PubMed]
- Stavrakis, S.; Nakagawa, H.; Po, S.S.; Scherlag, B.J.; Lazzara, R.; Jackman, W.M. The role of the autonomic ganglia in atrial fibrillation. JACC Clin. Electrophysiol. 2015, 1, 1–13. [Google Scholar] [CrossRef]
- Newaz, M.A.; Yousefipour, Z.; Oyekan, A. Oxidative stress-associated vascular aging is xanthine oxidase-dependent but not NAD(P)H oxidase-dependent. J. Cardiovasc. Pharmacol. 2006, 48, 88–94. [Google Scholar] [CrossRef]
- Donato, A.J.; Eskurza, I.; Silver, A.E.; Levy, A.S.; Pierce, G.L.; Gates, P.E.; Seals, D.R. Direct evidence of endothelial oxidative stress with aging in humans: Relation to impaired endothelium-dependent dilation and upregulation of nuclear factor-kappaB. Circ. Res. 2007, 100, 1659–1666. [Google Scholar] [CrossRef]
- Paolisso, G.; Tagliamonte, M.R.; Rizzo, M.R.; Manzella, D.; Gambardella, A.; Varricchio, M. Oxidative stress and advancing age: Results in healthy centenarians. J. Am. Geriatr. Soc. 1998, 46, 833–838. [Google Scholar] [CrossRef]
- Suzuki, M.; Willcox, D.C.; Rosenbaum, M.W.; Willcox, B.J. Oxidative stress and longevity in okinawa: An investigation of blood lipid peroxidation and tocopherol in okinawan centenarians. Curr. Gerontol. Geriatr. Res. 2010, 2010, 380460. [Google Scholar] [CrossRef]
- Soerensen, M.; Christensen, K.; Stevnsner, T.; Christiansen, L. The Mn-superoxide dismutase single nucleotide polymorphism rs4880 and the glutathione peroxidase 1 single nucleotide polymorphism rs1050450 are associated with aging and longevity in the oldest old. Mech. Ageing Dev. 2009, 130, 308–314. [Google Scholar] [CrossRef]
- Schiattarella, G.G.; Hill, J.A. Metabolic control and oxidative stress in pathological cardiac remodelling. Eur. Heart J. 2017, 38, 1399–1401. [Google Scholar] [CrossRef] [PubMed]
- Laina, A.; Stellos, K.; Stamatelopoulos, K. Vascular ageing: Underlying mechanisms and clinical implications. Exp. Gerontol. 2018, 109, 16–30. [Google Scholar] [CrossRef] [PubMed]
- Mattagajasingh, I.; Kim, C.S.; Naqvi, A.; Yamamori, T.; Hoffman, T.A.; Jung, S.B.; DeRicco, J.; Kasuno, K.; Irani, K. SIRT1 promotes endothelium-dependent vascular relaxation by activating endothelial nitric oxide synthase. Proc. Natl. Acad. Sci. USA 2007, 104, 14855–14860. [Google Scholar] [CrossRef] [PubMed]
- Donato, A.J.; Magerko, K.A.; Lawson, B.R.; Durrant, J.R.; Lesniewski, L.A.; Seals, D.R. SIRT-1 and vascular endothelial dysfunction with ageing in mice and humans. J. Physiol. 2011, 589, 4545–4554. [Google Scholar] [CrossRef] [PubMed]
- Zarzuelo, M.J.; Lopez-Sepulveda, R.; Sanchez, M.; Romero, M.; Gomez-Guzman, M.; Ungvary, Z.; Perez-Vizcaino, F.; Jimenez, R.; Duarte, J. SIRT1 inhibits NADPH oxidase activation and protects endothelial function in the rat aorta: Implications for vascular aging. Biochem. Pharmacol. 2013, 85, 1288–1296. [Google Scholar] [CrossRef] [PubMed]
- Ota, H.; Akishita, M.; Eto, M.; Iijima, K.; Kaneki, M.; Ouchi, Y. Sirt1 modulates premature senescence-like phenotype in human endothelial cells. J. Mol. Cell. Cardiol. 2007, 43, 571–579. [Google Scholar] [CrossRef] [PubMed]
- Luo, J.; Nikolaev, A.Y.; Imai, S.; Chen, D.; Su, F.; Shiloh, A.; Guarente, L.; Gu, W. Negative control of p53 by Sir2alpha promotes cell survival under stress. Cell 2001, 107, 137–148. [Google Scholar] [CrossRef]
- Thompson, A.M.; Wagner, R.; Rzucidlo, E.M. Age-related loss of SirT1 expression results in dysregulated human vascular smooth muscle cell function. Am. J. Physiol. Heart Circ. Physiol. 2014, 307, 533–541. [Google Scholar] [CrossRef]
- TenNapel, M.J.; Lynch, C.F.; Burns, T.L.; Wallace, R.; Smith, B.J.; Button, A.; Domann, F.E. SIRT6 minor allele genotype is associated with >5-year decrease in lifespan in an aged cohort. PLoS ONE 2014, 9, e115616. [Google Scholar] [CrossRef]
- Stein, S.; Lohmann, C.; Schafer, N.; Hofmann, J.; Rohrer, L.; Besler, C.; Rothgiesser, K.M.; Becher, B.; Hottiger, M.O.; Boren, J.; et al. SIRT1 decreases Lox-1-mediated foam cell formation in atherogenesis. Eur. Heart J. 2010, 31, 2301–2309. [Google Scholar] [CrossRef]
- Zhang, Q.J.; Wang, Z.; Chen, H.Z.; Zhou, S.; Zheng, W.; Liu, G.; Wei, Y.S.; Cai, H.; Liu, D.P.; Liang, C.C. Endothelium-specific overexpression of class III deacetylase SIRT1 decreases atherosclerosis in apolipoprotein E-deficient mice. Cardiovasc. Res. 2008, 80, 191–199. [Google Scholar] [CrossRef]
- Morselli, E.; Maiuri, M.C.; Markaki, M.; Megalou, E.; Pasparaki, A.; Palikaras, K.; Criollo, A.; Galluzzi, L.; Malik, S.A.; Vitale, I.; et al. Caloric restriction and resveratrol promote longevity through the Sirtuin-1-dependent induction of autophagy. Cell Death Dis. 2010, 1, e10. [Google Scholar] [CrossRef]
- Lee, I.H.; Yun, J.; Finkel, T. The emerging links between sirtuins and autophagy. Methods Mol. Biol 2013, 1077, 259–271. [Google Scholar] [CrossRef]
- Lee, I.H.; Cao, L.; Mostoslavsky, R.; Lombard, D.B.; Liu, J.; Bruns, N.E.; Tsokos, M.; Alt, F.W.; Finkel, T. A role for the NAD-dependent deacetylase Sirt1 in the regulation of autophagy. Proc. Natl. Acad. Sci. USA 2008, 105, 3374–3379. [Google Scholar] [CrossRef]
- Li, S.; Dou, X.; Ning, H.; Song, Q.; Wei, W.; Zhang, X.; Shen, C.; Li, J.; Sun, C.; Song, Z. Sirtuin 3 acts as a negative regulator of autophagy dictating hepatocyte susceptibility to lipotoxicity. Hepatology 2017, 66, 936–952. [Google Scholar] [CrossRef]
- Dai, S.H.; Chen, T.; Li, X.; Yue, K.Y.; Luo, P.; Yang, L.K.; Zhu, J.; Wang, Y.H.; Fei, Z.; Jiang, X.F. Sirt3 confers protection against neuronal ischemia by inducing autophagy: Involvement of the AMPK-mTOR pathway. Free Radic. Biol. Med. 2017, 108, 345–353. [Google Scholar] [CrossRef]
- He, J.; Zhang, G.; Pang, Q.; Yu, C.; Xiong, J.; Zhu, J.; Chen, F. SIRT6 reduces macrophage foam cell formation by inducing autophagy and cholesterol efflux under ox-LDL condition. FEBS J. 2017, 284, 1324–1337. [Google Scholar] [CrossRef]
- Migliaccio, E.; Giorgio, M.; Mele, S.; Pelicci, G.; Reboldi, P.; Pandolfi, P.P.; Lanfrancone, L.; Pelicci, P.G. The p66shc adaptor protein controls oxidative stress response and life span in mammals. Nature 1999, 402, 309–313. [Google Scholar] [CrossRef]
- Spescha, R.D.; Shi, Y.; Wegener, S.; Keller, S.; Weber, B.; Wyss, M.M.; Lauinger, N.; Tabatabai, G.; Paneni, F.; Cosentino, F.; et al. Deletion of the ageing gene p66(Shc) reduces early stroke size following ischaemia/reperfusion brain injury. Eur. Heart J. 2013, 34, 96–103. [Google Scholar] [CrossRef]
- Spescha, R.D.; Klohs, J.; Semerano, A.; Giacalone, G.; Derungs, R.S.; Reiner, M.F.; Rodriguez Gutierrez, D.; Mendez-Carmona, N.; Glanzmann, M.; Savarese, G.; et al. Post-ischaemic silencing of p66Shc reduces ischaemia/reperfusion brain injury and its expression correlates to clinical outcome in stroke. Eur. Heart J. 2015, 36, 1590–1600. [Google Scholar] [CrossRef]
- Camici, G.G.; Schiavoni, M.; Francia, P.; Bachschmid, M.; Martin-Padura, I.; Hersberger, M.; Tanner, F.C.; Pelicci, P.; Volpe, M.; Anversa, P.; et al. Genetic deletion of p66(Shc) adaptor protein prevents hyperglycemia-induced endothelial dysfunction and oxidative stress. Proc. Natl. Acad. Sci. USA 2007, 104, 5217–5222. [Google Scholar] [CrossRef]
- Paneni, F.; Osto, E.; Costantino, S.; Mateescu, B.; Briand, S.; Coppolino, G.; Perna, E.; Mocharla, P.; Akhmedov, A.; Kubant, R.; et al. Deletion of the activated protein-1 transcription factor JunD induces oxidative stress and accelerates age-related endothelial dysfunction. Circulation 2013, 127, 1229–1240. [Google Scholar] [CrossRef]
- Laurent, G.; Solari, F.; Mateescu, B.; Karaca, M.; Castel, J.; Bourachot, B.; Magnan, C.; Billaud, M.; Mechta-Grigoriou, F. Oxidative stress contributes to aging by enhancing pancreatic angiogenesis and insulin signaling. Cell Metab. 2008, 7, 113–124. [Google Scholar] [CrossRef][Green Version]
- Villa, F.; Carrizzo, A.; Spinelli, C.C.; Ferrario, A.; Malovini, A.; Maciag, A.; Damato, A.; Auricchio, A.; Spinetti, G.; Sangalli, E.; et al. Genetic Analysis Reveals a Longevity-Associated Protein Modulating Endothelial Function and Angiogenesis. Circ. Res. 2015, 117, 333–345. [Google Scholar] [CrossRef]
- Villa, F.; Malovini, A.; Carrizzo, A.; Spinelli, C.C.; Ferrario, A.; Maciag, A.; Madonna, M.; Bellazzi, R.; Milanesi, L.; Vecchione, C.; et al. Serum BPIFB4 levels classify health status in long-living individuals. Immun. Ageing 2015, 12, 27. [Google Scholar] [CrossRef]
- Malavolta, M.; Dato, S.; Villa, F.; Rango, F.; Iannone, F.; Ferrario, A.; Maciag, A.; Ciaglia, E.; D’Amato, A.; Carrizzo, A.; et al. LAV-BPIFB4 associates with reduced frailty in humans and its transfer prevents frailty progression in old mice. Aging (Albany N. Y.) 2019, 11, 6555–6568. [Google Scholar] [CrossRef]
- Smith-Vikos, T.; Liu, Z.; Parsons, C.; Gorospe, M.; Ferrucci, L.; Gill, T.M.; Slack, F.J. A serum miRNA profile of human longevity: Findings from the Baltimore Longitudinal Study of Aging (BLSA). Aging (Albany N. Y.) 2016, 8, 2971–2987. [Google Scholar] [CrossRef]
- Quiat, D.; Olson, E.N. MicroRNAs in cardiovascular disease: From pathogenesis to prevention and treatment. J. Clin. Investig. 2013, 123, 11–18. [Google Scholar] [CrossRef]
- Kinser, H.E.; Pincus, Z. MicroRNAs as modulators of longevity and the aging process. Hum. Genet. 2020, 139, 291–308. [Google Scholar] [CrossRef]
- Bartel, D.P. MicroRNAs: Genomics, biogenesis, mechanism, and function. Cell 2004, 116, 281–297. [Google Scholar] [CrossRef]
- Smith-Vikos, T.; Slack, F.J. MicroRNAs and their roles in aging. J. Cell Sci. 2012, 125, 7–17. [Google Scholar] [CrossRef]
- Kato, M.; Chen, X.; Inukai, S.; Zhao, H.; Slack, F.J. Age-associated changes in expression of small, noncoding RNAs, including microRNAs, in C. elegans. RNA 2011, 17, 1804–1820. [Google Scholar] [CrossRef] [PubMed]
- Boehm, M.; Slack, F. A developmental timing microRNA and its target regulate life span in C. elegans. Science 2005, 310, 1954–1957. [Google Scholar] [CrossRef] [PubMed]
- van Almen, G.C.; Verhesen, W.; van Leeuwen, R.E.; van de Vrie, M.; Eurlings, C.; Schellings, M.W.; Swinnen, M.; Cleutjens, J.P.; van Zandvoort, M.A.; Heymans, S.; et al. MicroRNA-18 and microRNA-19 regulate CTGF and TSP-1 expression in age-related heart failure. Aging Cell 2011, 10, 769–779. [Google Scholar] [CrossRef]
- Li, H.; Zhang, X.; Wang, F.; Zhou, L.; Yin, Z.; Fan, J.; Nie, X.; Wang, P.; Fu, X.D.; Chen, C.; et al. MicroRNA-21 Lowers Blood Pressure in Spontaneous Hypertensive Rats by Upregulating Mitochondrial Translation. Circulation 2016, 134, 734–751. [Google Scholar] [CrossRef]
- Olivieri, F.; Capri, M.; Bonafe, M.; Morsiani, C.; Jung, H.J.; Spazzafumo, L.; Vina, J.; Suh, Y. Circulating miRNAs and miRNA shuttles as biomarkers: Perspective trajectories of healthy and unhealthy aging. Mech. Ageing Dev. 2017, 165, 162–170. [Google Scholar] [CrossRef]
- Menghini, R.; Casagrande, V.; Cardellini, M.; Martelli, E.; Terrinoni, A.; Amati, F.; Vasa-Nicotera, M.; Ippoliti, A.; Novelli, G.; Melino, G.; et al. MicroRNA 217 modulates endothelial cell senescence via silent information regulator 1. Circulation 2009, 120, 1524–1532. [Google Scholar] [CrossRef]
- Drummond, G.R.; Selemidis, S.; Griendling, K.K.; Sobey, C.G. Combating oxidative stress in vascular disease: NADPH oxidases as therapeutic targets. Nat. Rev. Drug Discov. 2011, 10, 453–471. [Google Scholar] [CrossRef]
- Morris, C.D.; Carson, S. Routine vitamin supplementation to prevent cardiovascular disease: A summary of the evidence for the U.S. Preventive Services Task Force. Ann. Intern. Med. 2003, 139, 56–70. [Google Scholar] [CrossRef] [PubMed]
- Valko, M.; Leibfritz, D.; Moncol, J.; Cronin, M.T.; Mazur, M.; Telser, J. Free radicals and antioxidants in normal physiological functions and human disease. Int. J. Biochem. Cell Biol. 2007, 39, 44–84. [Google Scholar] [CrossRef] [PubMed]
- Kaasik, A.; Kuum, M.; Joubert, F.; Wilding, J.; Ventura-Clapier, R.; Veksler, V. Mitochondria as a source of mechanical signals in cardiomyocytes. Cardiovasc. Res. 2010, 87, 83–91. [Google Scholar] [CrossRef] [PubMed]
- Iribe, G.; Kaihara, K.; Yamaguchi, Y.; Nakaya, M.; Inoue, R.; Naruse, K. Mechano-sensitivity of mitochondrial function in mouse cardiac myocytes. Prog. Biophys. Mol. Biol. 2017, 130, 315–322. [Google Scholar] [CrossRef] [PubMed]
- Lakatta, E.G.; Sollott, S.J. Perspectives on mammalian cardiovascular aging: Humans to molecules. Comp. Biochem. Physiol. A Mol. Integr. Physiol. 2002, 132, 699–721. [Google Scholar] [CrossRef]
- Lakatta, E.G. Age-associated cardiovascular changes in health: Impact on cardiovascular disease in older persons. Heart Fail. Rev. 2002, 7, 29–49. [Google Scholar] [CrossRef] [PubMed]
- Lakatta, E.G.; Sollott, S.J.; Pepe, S. The old heart: Operating on the edge. In Novartis Foundation Symposium; Chichester: New York, NY, USA; John Wiley: Hoboken, NJ, USA, 1999; Volume 235, pp. 172–196. [Google Scholar]
- Sadoshima, J.; Xu, Y.; Slayter, H.S.; Izumo, S. Autocrine release of angiotensin II mediates stretch-induced hypertrophy of cardiac myocytes in vitro. Cell 1993, 75, 977–984. [Google Scholar] [CrossRef]
- Cave, A.C.; Brewer, A.C.; Narayanapanicker, A.; Ray, R.; Grieve, D.J.; Walker, S.; Shah, A.M. NADPH oxidases in cardiovascular health and disease. Antioxid. Redox Signal. 2006, 8, 691–728. [Google Scholar] [CrossRef]
- Papaconstantinou, J. The Role of Signaling Pathways of Inflammation and Oxidative Stress in Development of Senescence and Aging Phenotypes in Cardiovascular Disease. Cells 2019, 8, 1383. [Google Scholar] [CrossRef]
- Aronow, W.S. Etiology, pathophysiology, and treatment of atrial fibrillation: Part 1. Cardiol. Rev. 2008, 16, 181–188. [Google Scholar] [CrossRef]
- Schueller, P.O.; Steiner, S.; Hennersdorf, M.G. Atrial fibrillation. Med. Mon. Pharm. 2009, 32, 204–210. [Google Scholar]
- Schotten, U.; Verheule, S.; Kirchhof, P.; Goette, A. Pathophysiological mechanisms of atrial fibrillation: A translational appraisal. Physiol. Rev. 2011, 91, 265–325. [Google Scholar] [CrossRef]
- Iwasaki, Y.K.; Nishida, K.; Kato, T.; Nattel, S. Atrial fibrillation pathophysiology: Implications for management. Circulation 2011, 124, 2264–2274. [Google Scholar] [CrossRef] [PubMed]
- Hindricks, G.; Potpara, T.; Dagres, N.; Arbelo, E.; Bax, J.J.; Blomstrom-Lundqvist, C.; Boriani, G.; Castella, M.; Dan, G.A.; Dilaveris, P.E.; et al. 2020 ESC Guidelines for the diagnosis and management of atrial fibrillation developed in collaboration with the European Association of Cardio-Thoracic Surgery (EACTS). Eur. Heart J. 2020. [Google Scholar] [CrossRef] [PubMed]
- Pan, N.H.; Tsao, H.M.; Chang, N.C.; Chen, Y.J.; Chen, S.A. Aging dilates atrium and pulmonary veins: Implications for the genesis of atrial fibrillation. Chest 2008, 133, 190–196. [Google Scholar] [CrossRef] [PubMed]
- Ravassa, S.; Ballesteros, G.; Diez, J. Aging and atrial fibrillation: A matter of fibrosis. Aging (Albany N. Y.) 2019, 11, 9965–9966. [Google Scholar] [CrossRef]
- Ravassa, S.; Lopez, B.; Querejeta, R.; Echegaray, K.; San Jose, G.; Moreno, M.U.; Beaumont, F.J.; Gonzalez, A.; Diez, J. Phenotyping of myocardial fibrosis in hypertensive patients with heart failure. Influence on clinical outcome. J. Hypertens. 2017, 35, 853–861. [Google Scholar] [CrossRef] [PubMed]
- Zhan, G.; Wenhua, G.; Jie, H.; Xiang, Q.; Lingzhi, C.; Xue, X.; Xing-Xing, C.; Qianli, Z.; Weijian, H.; Hao, Z. Potential roles of circulating matrix metalloproteinase-28 (MMP-28) in patients with atrial fibrillation. Life Sci. 2018, 204, 15–19. [Google Scholar] [CrossRef]
- Lewkowicz, J.; Knapp, M.; Tankiewicz-Kwedlo, A.; Sawicki, R.; Kaminska, M.; Waszkiewicz, E.; Musial, W.J. MMP-9 in atrial remodeling in patients with atrial fibrillation. In Annales de Cardiologie et D’angeiologie; Elsevier Masson: Paris, France, 2015; Volume 64, pp. 285–291. [Google Scholar] [CrossRef]
- Kamkin, A.; Kiseleva, I.; Isenberg, G.; Wagner, K.D.; Gunther, J.; Theres, H.; Scholz, H. Cardiac fibroblasts and the mechano-electric feedback mechanism in healthy and diseased hearts. Prog. Biophys. Mol. Biol. 2003, 82, 111–120. [Google Scholar] [CrossRef]
- Chang, S.L.; Chen, Y.C.; Chen, Y.J.; Wangcharoen, W.; Lee, S.H.; Lin, C.I.; Chen, S.A. Mechanoelectrical feedback regulates the arrhythmogenic activity of pulmonary veins. Heart 2007, 93, 82–88. [Google Scholar] [CrossRef]
- Ferrucci, L.; Corsi, A.; Lauretani, F.; Bandinelli, S.; Bartali, B.; Taub, D.D.; Guralnik, J.M.; Longo, D.L. The origins of age-related proinflammatory state. Blood 2005, 105, 2294–2299. [Google Scholar] [CrossRef]
- Lee, S.H.; Chen, Y.C.; Chen, Y.J.; Chang, S.L.; Tai, C.T.; Wongcharoen, W.; Yeh, H.I.; Lin, C.I.; Chen, S.A. Tumor necrosis factor-alpha alters calcium handling and increases arrhythmogenesis of pulmonary vein cardiomyocytes. Life Sci. 2007, 80, 1806–1815. [Google Scholar] [CrossRef]
- Lai, L.P.; Tsai, C.C.; Su, M.J.; Lin, J.L.; Chen, Y.S.; Tseng, Y.Z.; Huang, S.K. Atrial fibrillation is associated with accumulation of aging-related common type mitochondrial DNA deletion mutation in human atrial tissue. Chest 2003, 123, 539–544. [Google Scholar] [CrossRef] [PubMed]
- Tsuboi, M.; Hisatome, I.; Morisaki, T.; Tanaka, M.; Tomikura, Y.; Takeda, S.; Shimoyama, M.; Ohtahara, A.; Ogino, K.; Igawa, O.; et al. Mitochondrial DNA deletion associated with the reduction of adenine nucleotides in human atrium and atrial fibrillation. Eur. J. Clin. Investig. 2001, 31, 489–496. [Google Scholar] [CrossRef] [PubMed]
- Lin, Y.K.; Chen, Y.A.; Lee, T.I.; Chen, Y.C.; Chen, S.A.; Chen, Y.J. Aging Modulates the Substrate and Triggers Remodeling in Atrial Fibrillation. Circ. J. 2018, 82, 1237–1244. [Google Scholar] [CrossRef] [PubMed]
- McMurray, J.J.; Pfeffer, M.A. Heart failure. Lancet 2005, 365, 1877–1889. [Google Scholar] [CrossRef]
- Lloyd-Jones, D.; Adams, R.; Carnethon, M.; De Simone, G.; Ferguson, T.B.; Flegal, K.; Ford, E.; Furie, K.; Go, A.; Greenlund, K.; et al. Heart disease and stroke statistics—2009 update: A report from the American Heart Association Statistics Committee and Stroke Statistics Subcommittee. Circulation 2009, 119, 21–181. [Google Scholar] [CrossRef]
- Mosterd, A.; Hoes, A.W. Clinical epidemiology of heart failure. Heart 2007, 93, 1137–1146. [Google Scholar] [CrossRef]
- Orso, F.; Fabbri, G.; Maggioni, A.P. Epidemiology of Heart Failure. Handb. Exp. Pharmacol. 2017, 243, 15–33. [Google Scholar] [CrossRef]
- Ziaeian, B.; Fonarow, G.C. Epidemiology and aetiology of heart failure. Nat. Rev. Cardiol. 2016, 13, 368–378. [Google Scholar] [CrossRef]
- Kurmani, S.; Squire, I. Acute Heart Failure: Definition, Classification and Epidemiology. Curr. Heart Fail. Rep. 2017, 14, 385–392. [Google Scholar] [CrossRef]
- Goldstein, S. The changing epidemiology of sudden death in heart failure. Curr. Heart Fail. Rep. 2004, 1, 93–97. [Google Scholar] [CrossRef]
- Penjaskovic, D.; Sakac, D.; Dejanovic, J.; Zec, R.; Zec Petkovic, N.; Stojsic Milosavljevic, A. Left ventricular diastolic dysfunction in patients with metabolic syndrome. Med. Pregl. 2012, 65, 18–22. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Cil, H.; Bulur, S.; Turker, Y.; Kaya, A.; Alemdar, R.; Karabacak, A.; Aslantas, Y.; Ekinozu, I.; Albayrak, S.; Ozhan, H.; et al. Impact of body mass index on left ventricular diastolic dysfunction. Echocardiography 2012, 29, 647–651. [Google Scholar] [CrossRef] [PubMed]
- Katz, S.D. Pathophysiology of Chronic Systolic Heart Failure. A View from the Periphery. Ann. Am. Thorac. Soc. 2018, 15, 38–41. [Google Scholar] [CrossRef] [PubMed]
- McMurray, J.J. Clinical practice. Systolic heart failure. N. Engl. J. Med. 2010, 362, 228–238. [Google Scholar] [CrossRef] [PubMed]
- Chatterjee, K. Pathophysiology of systolic and diastolic heart failure. Med. Clin. 2012, 96, 891–899. [Google Scholar] [CrossRef]
- Henes, J.; Rosenberger, P. Systolic heart failure: Diagnosis and therapy. Curr. Opin. Anesthesiol. 2016, 29, 55–60. [Google Scholar] [CrossRef]
- Ennezat, P.V.; Le Jemtel, T.H.; Logeart, D.; Marechaux, S. Heart failure with preserved ejection fraction: A systemic disorder? Rev. Med. Interne 2012, 33, 370–380. [Google Scholar] [CrossRef]
- Wachter, R. Diastolic heart failure. Internist 2014, 55, 663–668. [Google Scholar] [CrossRef]
- Del Buono, M.G.; Buckley, L.; Abbate, A. Primary and Secondary Diastolic Dysfunction in Heart Failure with Preserved Ejection Fraction. Am. J. Cardiol. 2018, 122, 1578–1587. [Google Scholar] [CrossRef]
- Lodi, R.; Tonon, C.; Calabrese, V.; Schapira, A.H. Friedreich’s ataxia: From disease mechanisms to therapeutic interventions. Antioxid. Redox Signal. 2006, 8, 438–443. [Google Scholar] [CrossRef]
- Kaneto, H.; Katakami, N.; Kawamori, D.; Miyatsuka, T.; Sakamoto, K.; Matsuoka, T.A.; Matsuhisa, M.; Yamasaki, Y. Involvement of oxidative stress in the pathogenesis of diabetes. Antioxid. Redox Signal. 2007, 9, 355–366. [Google Scholar] [CrossRef] [PubMed]
- Bianchi, M.; Panerai, A.E. Formalin injection in the tail facilitates hindpaw withdrawal reflexes induced by thermal stimulation in the rat: Effect of paracetamol. Neurosci. Lett. 1997, 237, 89–92. [Google Scholar] [CrossRef]
- Murphy, M.P. How mitochondria produce reactive oxygen species. Biochem. J. 2009, 417, 1–13. [Google Scholar] [CrossRef] [PubMed]
- Sohal, R.S.; Arnold, L.A.; Sohal, B.H. Age-related changes in antioxidant enzymes and prooxidant generation in tissues of the rat with special reference to parameters in two insect species. Free Radic. Biol. Med. 1990, 9, 495–500. [Google Scholar] [CrossRef]
- Yan, L.J.; Sohal, R.S. Mitochondrial adenine nucleotide translocase is modified oxidatively during aging. Proc. Natl. Acad. Sci. USA 1998, 95, 12896–12901. [Google Scholar] [CrossRef]
- Kim, J.H.; Woldgiorgis, G.; Elson, C.E.; Shrago, E. Age-related changes in respiration coupled to phosphorylation. I. Hepatic mitochondria. Mech. Ageing Dev. 1988, 46, 263–277. [Google Scholar] [CrossRef]
- Yokozawa, T.; Satoh, A.; Cho, E.J. Ginsenoside-Rd attenuates oxidative damage related to aging in senescence-accelerated mice. J. Pharm. Pharmacol. 2004, 56, 107–113. [Google Scholar] [CrossRef]
- Judge, S.; Jang, Y.M.; Smith, A.; Hagen, T.; Leeuwenburgh, C. Age-associated increases in oxidative stress and antioxidant enzyme activities in cardiac interfibrillar mitochondria: Implications for the mitochondrial theory of aging. FASEB J. 2005, 19, 419–421. [Google Scholar] [CrossRef]
- Mo, J.Q.; Hom, D.G.; Andersen, J.K. Decreases in protective enzymes correlates with increased oxidative damage in the aging mouse brain. Mech. Ageing Dev. 1995, 81, 73–82. [Google Scholar] [CrossRef]
- Hoffmann, B.; Stockl, A.; Schlame, M.; Beyer, K.; Klingenberg, M. The reconstituted ADP/ATP carrier activity has an absolute requirement for cardiolipin as shown in cysteine mutants. J. Biol. Chem. 1994, 269, 1940–1944. [Google Scholar] [CrossRef]
- Nehal, M.; Azam, M.; Baquer, N.Z. Changes in the levels of catecholamines, hexokinase and glucose 6-phosphate dehydrogenase in red cell aging. Biochem. Int. 1990, 22, 517–522. [Google Scholar] [PubMed]
- Karavidas, A.; Lazaros, G.; Tsiachris, D.; Pyrgakis, V. Aging and the cardiovascular system. Hell. J. Cardiol. 2010, 51, 421–427. [Google Scholar]
- Nassimiha, D.; Aronow, W.S.; Ahn, C.; Goldman, M.E. Association of coronary risk factors with progression of valvular aortic stenosis in older persons. Am. J. Cardiol. 2001, 87, 1313–1314. [Google Scholar] [CrossRef]
- Stewart, B.F.; Siscovick, D.; Lind, B.K.; Gardin, J.M.; Gottdiener, J.S.; Smith, V.E.; Kitzman, D.W.; Otto, C.M. Clinical factors associated with calcific aortic valve disease. Cardiovascular Health Study. J. Am. Coll. Cardiol. 1997, 29, 630–634. [Google Scholar] [CrossRef]
- Freeman, R.V.; Otto, C.M. Spectrum of calcific aortic valve disease: Pathogenesis, disease progression, and treatment strategies. Circulation 2005, 111, 3316–3326. [Google Scholar] [CrossRef] [PubMed]
- Otto, C.M.; Lind, B.K.; Kitzman, D.W.; Gersh, B.J.; Siscovick, D.S. Association of aortic-valve sclerosis with cardiovascular mortality and morbidity in the elderly. N. Engl. J. Med. 1999, 341, 142–147. [Google Scholar] [CrossRef]
- Olsen, M.H.; Wachtell, K.; Bella, J.N.; Gerdts, E.; Palmieri, V.; Nieminen, M.S.; Smith, G.; Ibsen, H.; Devereux, R.B.; Substudy, L. Aortic valve sclerosis relates to cardiovascular events in patients with hypertension (a LIFE substudy). Am. J. Cardiol. 2005, 95, 132–136. [Google Scholar] [CrossRef]
- Otto, C.M. Why is aortic sclerosis associated with adverse clinical outcomes? J. Am. Coll. Cardiol. 2004, 43, 176–178. [Google Scholar] [CrossRef]
- Faggiano, P.; Antonini-Canterin, F.; Erlicher, A.; Romeo, C.; Cervesato, E.; Pavan, D.; Piazza, R.; Huang, G.; Nicolosi, G.L. Progression of aortic valve sclerosis to aortic stenosis. Am. J. Cardiol. 2003, 91, 99–101. [Google Scholar] [CrossRef]
- Jeon, D.S.; Atar, S.; Brasch, A.V.; Luo, H.; Mirocha, J.; Naqvi, T.Z.; Kraus, R.; Berman, D.S.; Siegel, R.J. Association of mitral annulus calcification, aortic valve sclerosis and aortic root calcification with abnormal myocardial perfusion single photon emission tomography in subjects age < or =65 years old. J. Am. Coll. Cardiol. 2001, 38, 1988–1993. [Google Scholar] [CrossRef]
- Fulkerson, P.K.; Beaver, B.M.; Auseon, J.C.; Graber, H.L. Calcification of the mitral annulus: Etiology, clinical associations, complications and therapy. Am. J. Med. 1979, 66, 967–977. [Google Scholar] [CrossRef]
- Correia, L.C.; Lakatta, E.G.; O’Connor, F.C.; Becker, L.C.; Clulow, J.; Townsend, S.; Gerstenblith, G.; Fleg, J.L. Attenuated cardiovascular reserve during prolonged submaximal cycle exercise in healthy older subjects. J. Am. Coll. Cardiol. 2002, 40, 1290–1297. [Google Scholar] [CrossRef]
- Akins, C.W.; Daggett, W.M.; Vlahakes, G.J.; Hilgenberg, A.D.; Torchiana, D.F.; Madsen, J.C.; Buckley, M.J. Cardiac operations in patients 80 years old and older. Ann. Thorac. Surg. 1997, 64, 606–614. [Google Scholar] [CrossRef]
- Kurz, D.J.; Kloeckener-Gruissem, B.; Akhmedov, A.; Eberli, F.R.; Buhler, I.; Berger, W.; Bertel, O.; Luscher, T.F. Degenerative aortic valve stenosis, but not coronary disease, is associated with shorter telomere length in the elderly. Arterioscler. Thromb. Vasc. Biol. 2006, 26, 114–117. [Google Scholar] [CrossRef] [PubMed]
- Barnes, R.P.; Fouquerel, E.; Opresko, P.L. The impact of oxidative DNA damage and stress on telomere homeostasis. Mech. Ageing Dev. 2019, 177, 37–45. [Google Scholar] [CrossRef] [PubMed]
- Martinez-Ezquerro, J.D.; Rodriguez-Castaneda, A.; Ortiz-Ramirez, M.; Sanchez-Garcia, S.; Rosas-Vargas, H.; Sanchez-Arenas, R.; Garcia-de la Torre, P. Oxidative Stress, Telomere Length, and Frailty in an Old Age Population. bioRxiv 2019, 71, 414680. [Google Scholar] [CrossRef]
- Cho, K.I.; Sakuma, I.; Sohn, I.S.; Jo, S.H.; Koh, K.K. Inflammatory and metabolic mechanisms underlying the calcific aortic valve disease. Atherosclerosis 2018, 277, 60–65. [Google Scholar] [CrossRef]
- Demer, L.L.; Tintut, Y. Inflammatory, metabolic, and genetic mechanisms of vascular calcification. Arterioscler. Thromb. Vasc. Biol. 2014, 34, 715–723. [Google Scholar] [CrossRef]
- van Dijk, R.A.; Kolodgie, F.; Ravandi, A.; Leibundgut, G.; Hu, P.P.; Prasad, A.; Mahmud, E.; Dennis, E.; Curtiss, L.K.; Witztum, J.L.; et al. Differential expression of oxidation-specific epitopes and apolipoprotein(a) in progressing and ruptured human coronary and carotid atherosclerotic lesions. J. Lipid Res. 2012, 53, 2773–2790. [Google Scholar] [CrossRef]
- Ravandi, A.; Leibundgut, G.; Hung, M.Y.; Patel, M.; Hutchins, P.M.; Murphy, R.C.; Prasad, A.; Mahmud, E.; Miller, Y.I.; Dennis, E.A.; et al. Release and capture of bioactive oxidized phospholipids and oxidized cholesteryl esters during percutaneous coronary and peripheral arterial interventions in humans. J. Am. Coll. Cardiol. 2014, 63, 1961–1971. [Google Scholar] [CrossRef]
- Cote, C.; Pibarot, P.; Despres, J.P.; Mohty, D.; Cartier, A.; Arsenault, B.J.; Couture, C.; Mathieu, P. Association between circulating oxidised low-density lipoprotein and fibrocalcific remodelling of the aortic valve in aortic stenosis. Heart 2008, 94, 1175–1180. [Google Scholar] [CrossRef] [PubMed]
- Mohty, D.; Pibarot, P.; Despres, J.P.; Cote, C.; Arsenault, B.; Cartier, A.; Cosnay, P.; Couture, C.; Mathieu, P. Association between plasma LDL particle size, valvular accumulation of oxidized LDL, and inflammation in patients with aortic stenosis. Arterioscler. Thromb. Vasc. Biol. 2008, 28, 187–193. [Google Scholar] [CrossRef] [PubMed]
- Meng, X.; Ao, L.; Song, Y.; Babu, A.; Yang, X.; Wang, M.; Weyant, M.J.; Dinarello, C.A.; Cleveland, J.C., Jr.; Fullerton, D.A. Expression of functional Toll-like receptors 2 and 4 in human aortic valve interstitial cells: Potential roles in aortic valve inflammation and stenosis. Am. J. Physiol. Cell Physiol. 2008, 294, 29–35. [Google Scholar] [CrossRef] [PubMed]
- Yang, X.; Fullerton, D.A.; Su, X.; Ao, L.; Cleveland, J.C., Jr.; Meng, X. Pro-osteogenic phenotype of human aortic valve interstitial cells is associated with higher levels of Toll-like receptors 2 and 4 and enhanced expression of bone morphogenetic protein 2. J. Am. Coll. Cardiol. 2009, 53, 491–500. [Google Scholar] [CrossRef]
- Yeang, C.; Wilkinson, M.J.; Tsimikas, S. Lipoprotein(a) and oxidized phospholipids in calcific aortic valve stenosis. Curr. Opin. Cardiol. 2016, 31, 440–450. [Google Scholar] [CrossRef]
- Murugesan, G.; Sandhya Rani, M.R.; Gerber, C.E.; Mukhopadhyay, C.; Ransohoff, R.M.; Chisolm, G.M.; Kottke-Marchant, K. Lysophosphatidylcholine regulates human microvascular endothelial cell expression of chemokines. J. Mol. Cell. Cardiol. 2003, 35, 1375–1384. [Google Scholar] [CrossRef]
- Chang, M.C.; Lee, J.J.; Chen, Y.J.; Lin, S.I.; Lin, L.D.; Jein-Wen Liou, E.; Huang, W.L.; Chan, C.P.; Huang, C.C.; Jeng, J.H. Lysophosphatidylcholine induces cytotoxicity/apoptosis and IL-8 production of human endothelial cells: Related mechanisms. Oncotarget 2017, 8, 106177–106189. [Google Scholar] [CrossRef]
- Rolin, J.; Vego, H.; Maghazachi, A.A. Oxidized lipids and lysophosphatidylcholine induce the chemotaxis, up-regulate the expression of CCR9 and CXCR4 and abrogate the release of IL-6 in human monocytes. Toxins 2014, 6, 2840–2856. [Google Scholar] [CrossRef]
- Inoue, N.; Takeshita, S.; Gao, D.; Ishida, T.; Kawashima, S.; Akita, H.; Tawa, R.; Sakurai, H.; Yokoyama, M. Lysophosphatidylcholine increases the secretion of matrix metalloproteinase 2 through the activation of NADH/NADPH oxidase in cultured aortic endothelial cells. Atherosclerosis 2001, 155, 45–52. [Google Scholar] [CrossRef]
- Miller, J.D.; Chu, Y.; Brooks, R.M.; Richenbacher, W.E.; Pena-Silva, R.; Heistad, D.D. Dysregulation of antioxidant mechanisms contributes to increased oxidative stress in calcific aortic valvular stenosis in humans. J. Am. Coll. Cardiol. 2008, 52, 843–850. [Google Scholar] [CrossRef]
- Kuzkaya, N.; Weissmann, N.; Harrison, D.G.; Dikalov, S. Interactions of peroxynitrite, tetrahydrobiopterin, ascorbic acid, and thiols: Implications for uncoupling endothelial nitric-oxide synthase. J. Biol. Chem. 2003, 278, 22546–22554. [Google Scholar] [CrossRef] [PubMed]
- Li, H.; Forstermann, U. Uncoupling of endothelial NO synthase in atherosclerosis and vascular disease. Curr. Opin. Pharmacol. 2013, 13, 161–167. [Google Scholar] [CrossRef] [PubMed]
- Milstien, S.; Katusic, Z. Oxidation of tetrahydrobiopterin by peroxynitrite: Implications for vascular endothelial function. Biochem. Biophys. Res. Commun. 1999, 263, 681–684. [Google Scholar] [CrossRef] [PubMed]
- Rueckschloss, U.; Galle, J.; Holtz, J.; Zerkowski, H.R.; Morawietz, H. Induction of NAD(P)H oxidase by oxidized low-density lipoprotein in human endothelial cells: Antioxidative potential of hydroxymethylglutaryl coenzyme A reductase inhibitor therapy. Circulation 2001, 104, 1767–1772. [Google Scholar] [CrossRef] [PubMed]
- Liochev, S.I. Reactive oxygen species and the free radical theory of aging. Free Radic. Biol. Med. 2013, 60, 1–4. [Google Scholar] [CrossRef]
- Godo, S.; Shimokawa, H. Endothelial Functions. Arterioscler. Thromb. Vasc. Biol. 2017, 37, 108–114. [Google Scholar] [CrossRef]
- Deanfield, J.E.; Halcox, J.P.; Rabelink, T.J. Endothelial function and dysfunction: Testing and clinical relevance. Circulation 2007, 115, 1285–1295. [Google Scholar] [CrossRef]
- Favero, G.; Paganelli, C.; Buffoli, B.; Rodella, L.F.; Rezzani, R. Endothelium and its alterations in cardiovascular diseases: Life style intervention. Biomed. Res. Int. 2014, 2014, 801896. [Google Scholar] [CrossRef]
- Ghosh, A.; Gao, L.; Thakur, A.; Siu, P.M.; Lai, C.W.K. Role of free fatty acids in endothelial dysfunction. J. Biomed. Sci. 2017, 24, 50. [Google Scholar] [CrossRef]
- Durrant, J.R.; Seals, D.R.; Connell, M.L.; Russell, M.J.; Lawson, B.R.; Folian, B.J.; Donato, A.J.; Lesniewski, L.A. Voluntary wheel running restores endothelial function in conduit arteries of old mice: Direct evidence for reduced oxidative stress, increased superoxide dismutase activity and down-regulation of NADPH oxidase. J. Physiol. 2009, 587, 3271–3285. [Google Scholar] [CrossRef]
- Pierce, G.L.; Lesniewski, L.A.; Lawson, B.R.; Beske, S.D.; Seals, D.R. Nuclear factor-κB activation contributes to vascular endothelial dysfunction via oxidative stress in overweight/obese middle-aged and older humans. Circulation 2009, 119, 1284–1292. [Google Scholar] [CrossRef] [PubMed]
- Dichtl, W.; Dulak, J.; Frick, M.; Alber, H.F.; Schwarzacher, S.P.; Ares, M.P.; Nilsson, J.; Pachinger, O.; Weidinger, F. HMG-CoA reductase inhibitors regulate inflammatory transcription factors in human endothelial and vascular smooth muscle cells. Arterioscler. Thromb. Vasc. Biol. 2003, 23, 58–63. [Google Scholar] [CrossRef] [PubMed]
- Donato, A.J.; Pierce, G.L.; Lesniewski, L.A.; Seals, D.R. Role of NFkappaB in age-related vascular endothelial dysfunction in humans. Aging (Albany N. Y.) 2009, 1, 678–680. [Google Scholar] [CrossRef]
- Anrather, J.; Racchumi, G.; Iadecola, C. NF-kappaB regulates phagocytic NADPH oxidase by inducing the expression of gp91phox. J. Biol. Chem. 2006, 281, 5657–5667. [Google Scholar] [CrossRef] [PubMed]
- Seals, D.R.; Moreau, K.L.; Gates, P.E.; Eskurza, I. Modulatory influences on ageing of the vasculature in healthy humans. Exp. Gerontol. 2006, 41, 501–507. [Google Scholar] [CrossRef] [PubMed]
- Li, Z.; Froehlich, J.; Galis, Z.S.; Lakatta, E.G. Increased expression of matrix metalloproteinase-2 in the thickened intima of aged rats. Hypertension 1999, 33, 116–123. [Google Scholar] [CrossRef]
- Denver, R.J.; Licht, P. Modulation of neuropeptide-stimulated pituitary hormone secretion in hatchling turtles. Gen. Comp. Endocrinol. 1990, 77, 107–115. [Google Scholar] [CrossRef]
- Chung, A.W.; Booth, A.D.; Rose, C.; Thompson, C.R.; Levin, A.; van Breemen, C. Increased matrix metalloproteinase 2 activity in the human internal mammary artery is associated with ageing, hypertension, diabetes and kidney dysfunction. J. Vasc. Res. 2008, 45, 357–362. [Google Scholar] [CrossRef]
- McNulty, M.; Mahmud, A.; Spiers, P.; Feely, J. Collagen type-I degradation is related to arterial stiffness in hypertensive and normotensive subjects. J. Hum. Hypertens. 2006, 20, 867–873. [Google Scholar] [CrossRef]
- Xia, W.H.; Li, J.; Su, C.; Yang, Z.; Chen, L.; Wu, F.; Zhang, Y.Y.; Yu, B.B.; Qiu, Y.X.; Wang, S.M.; et al. Physical exercise attenuates age-associated reduction in endothelium-reparative capacity of endothelial progenitor cells by increasing CXCR4/JAK-2 signaling in healthy men. Aging Cell 2012, 11, 111–119. [Google Scholar] [CrossRef]
- Thum, T.; Hoeber, S.; Froese, S.; Klink, I.; Stichtenoth, D.O.; Galuppo, P.; Jakob, M.; Tsikas, D.; Anker, S.D.; Poole-Wilson, P.A.; et al. Age-dependent impairment of endothelial progenitor cells is corrected by growth-hormone-mediated increase of insulin-like growth-factor-1. Circ. Res. 2007, 100, 434–443. [Google Scholar] [CrossRef] [PubMed]
- Angulo, J.; Vallejo, S.; El Assar, M.; Garcia-Septiem, J.; Sanchez-Ferrer, C.F.; Rodriguez-Manas, L. Age-related differences in the effects of alpha and gamma peroxisome proliferator-activated receptor subtype agonists on endothelial vasodilation in human microvessels. Exp. Gerontol. 2012, 47, 734–740. [Google Scholar] [CrossRef] [PubMed]
- Tsutsui, M.; Shimokawa, H.; Otsuji, Y.; Ueta, Y.; Sasaguri, Y.; Yanagihara, N. Nitric oxide synthases and cardiovascular diseases: Insights from genetically modified mice. Circ. J. 2009, 73, 986–993. [Google Scholar] [CrossRef] [PubMed]
- Sun, D.; Huang, A.; Yan, E.H.; Wu, Z.; Yan, C.; Kaminski, P.M.; Oury, T.D.; Wolin, M.S.; Kaley, G. Reduced release of nitric oxide to shear stress in mesenteric arteries of aged rats. Am. J. Physiol. Heart Circ. Physiol. 2004, 286, 2249–2256. [Google Scholar] [CrossRef]
- Challah, M.; Nadaud, S.; Philippe, M.; Battle, T.; Soubrier, F.; Corman, B.; Michel, J.B. Circulating and cellular markers of endothelial dysfunction with aging in rats. Am. J. Physiol. 1997, 273, 1941–1948. [Google Scholar] [CrossRef]
- Cernadas, M.R.; Sanchez de Miguel, L.; Garcia-Duran, M.; Gonzalez-Fernandez, F.; Millas, I.; Monton, M.; Rodrigo, J.; Rico, L.; Fernandez, P.; de Frutos, T.; et al. Expression of constitutive and inducible nitric oxide synthases in the vascular wall of young and aging rats. Circ. Res. 1998, 83, 279–286. [Google Scholar] [CrossRef]
- Taddei, S.; Virdis, A.; Ghiadoni, L.; Versari, D.; Salvetti, A. Endothelium, aging, and hypertension. Curr. Hypertens. Rep. 2006, 8, 84–89. [Google Scholar] [CrossRef]
- Bakris, G.; Ali, W.; Parati, G. ACC/AHA Versus ESC/ESH on Hypertension Guidelines: JACC Guideline Comparison. J. Am. Coll. Cardiol. 2019, 73, 3018–3026. [Google Scholar] [CrossRef]
- Burnier, M.; Wuerzner, G. Hypertension. Rev. Med. Suisse 2017, 13, 61–65. [Google Scholar]
- Oparil, S.; Acelajado, M.C.; Bakris, G.L.; Berlowitz, D.R.; Cifkova, R.; Dominiczak, A.F.; Grassi, G.; Jordan, J.; Poulter, N.R.; Rodgers, A.; et al. Hypertension. Nat. Rev. Dis. Primers 2018, 4, 18014. [Google Scholar] [CrossRef]
- Pereira da Silva, A.; Matos, A.; Aguiar, L.; Ramos-Marques, N.; Ribeiro, R.; Gil, A.; Gorjao-Clara, J.; Bicho, M. Hypertension and longevity: Role of genetic polymorphisms in renin-angiotensin-aldosterone system and endothelial nitric oxide synthase. Mol. Cell Biochem. 2019, 455, 61–71. [Google Scholar] [CrossRef] [PubMed]
- Whitworth, J.A.; World Health Organization. 2003 World Health Organization (WHO)/International Society of Hypertension (ISH) statement on management of hypertension. J. Hypertens. 2003, 21, 1983–1992. [Google Scholar] [CrossRef] [PubMed]
- Baker, P.B.; Baba, N.; Boesel, C.P. Cardiovascular abnormalities in progeria. Case report and review of the literature. Arch. Pathol. Lab. Med. 1981, 105, 384–386. [Google Scholar] [PubMed]
- Huveneers, S.; Daemen, M.J.; Hordijk, P.L. Between Rho(k) and a hard place: The relation between vessel wall stiffness, endothelial contractility, and cardiovascular disease. Circ. Res. 2015, 116, 895–908. [Google Scholar] [CrossRef] [PubMed]
- Nilsson, P.M.; Boutouyrie, P.; Cunha, P.; Kotsis, V.; Narkiewicz, K.; Parati, G.; Rietzschel, E.; Scuteri, A.; Laurent, S. Early vascular ageing in translation: From laboratory investigations to clinical applications in cardiovascular prevention. J. Hypertens. 2013, 31, 1517–1526. [Google Scholar] [CrossRef] [PubMed]
- Van Bortel, L.M.; Laurent, S.; Boutouyrie, P.; Chowienczyk, P.; Cruickshank, J.K.; De Backer, T.; Filipovsky, J.; Huybrechts, S.; Mattace-Raso, F.U.; Protogerou, A.D.; et al. Expert consensus document on the measurement of aortic stiffness in daily practice using carotid-femoral pulse wave velocity. J. Hypertens. 2012, 30, 445–448. [Google Scholar] [CrossRef] [PubMed]
- Harvey, A.; Montezano, A.C.; Lopes, R.A.; Rios, F.; Touyz, R.M. Vascular Fibrosis in Aging and Hypertension: Molecular Mechanisms and Clinical Implications. Can. J. Cardiol. 2016, 32, 659–668. [Google Scholar] [CrossRef] [PubMed]
- Kotsis, V.; Stabouli, S.; Karafillis, I.; Nilsson, P. Early vascular aging and the role of central blood pressure. J. Hypertens. 2011, 29, 1847–1853. [Google Scholar] [CrossRef]
- Iwaki, T.; Nagahashi, K.; Takano, K.; Suzuki-Inoue, K.; Kanayama, N.; Umemura, K.; Urano, T. Mutation in a highly conserved glycine residue in strand 5B of plasminogen activator inhibitor 1 causes polymerisation. Thromb. Haemost. 2017, 117, 860–869. [Google Scholar] [CrossRef]
- Guzik, T.J.; Mikolajczyk, T. In search of the T cell involved in hypertension and target organ damage. Hypertension 2014, 64, 224–226. [Google Scholar] [CrossRef][Green Version]
- Mikolajczyk, T.P.; Nosalski, R.; Szczepaniak, P.; Budzyn, K.; Osmenda, G.; Skiba, D.; Sagan, A.; Wu, J.; Vinh, A.; Marvar, P.J.; et al. Role of chemokine RANTES in the regulation of perivascular inflammation, T-cell accumulation, and vascular dysfunction in hypertension. FASEB J. 2016, 30, 1987–1999. [Google Scholar] [CrossRef] [PubMed]
- Scheiermann, C.; Frenette, P.S.; Hidalgo, A. Regulation of leucocyte homeostasis in the circulation. Cardiovasc. Res. 2015, 107, 340–351. [Google Scholar] [CrossRef] [PubMed]
- Czesnikiewicz-Guzik, M.; Lee, W.W.; Cui, D.; Hiruma, Y.; Lamar, D.L.; Yang, Z.Z.; Ouslander, J.G.; Weyand, C.M.; Goronzy, J.J. T cell subset-specific susceptibility to aging. Clin. Immunol. 2008, 127, 107–118. [Google Scholar] [CrossRef] [PubMed]
- Youn, J.C.; Yu, H.T.; Lim, B.J.; Koh, M.J.; Lee, J.; Chang, D.Y.; Choi, Y.S.; Lee, S.H.; Kang, S.M.; Jang, Y.; et al. Immunosenescent CD8+ T cells and C-X-C chemokine receptor type 3 chemokines are increased in human hypertension. Hypertension 2013, 62, 126–133. [Google Scholar] [CrossRef] [PubMed]
- Itani, H.A.; McMaster, W.G., Jr.; Saleh, M.A.; Nazarewicz, R.R.; Mikolajczyk, T.P.; Kaszuba, A.M.; Konior, A.; Prejbisz, A.; Januszewicz, A.; Norlander, A.E.; et al. Activation of Human T Cells in Hypertension: Studies of Humanized Mice and Hypertensive Humans. Hypertension 2016, 68, 123–132. [Google Scholar] [CrossRef] [PubMed]
- Yodoi, K.; Yamashita, T.; Sasaki, N.; Kasahara, K.; Emoto, T.; Matsumoto, T.; Kita, T.; Sasaki, Y.; Mizoguchi, T.; Sparwasser, T.; et al. Foxp3+ regulatory T cells play a protective role in angiotensin II-induced aortic aneurysm formation in mice. Hypertension 2015, 65, 889–895. [Google Scholar] [CrossRef] [PubMed]
- Jang, S.; Yu, X.M.; Odorico, S.; Clark, M.; Jaskula-Sztul, R.; Schienebeck, C.M.; Kupcho, K.R.; Harrison, A.D.; Winston-McPherson, G.N.; Tang, W.; et al. Novel analogs targeting histone deacetylase suppress aggressive thyroid cancer cell growth and induce re-differentiation. Cancer Gene Ther. 2015, 22, 410–416. [Google Scholar] [CrossRef] [PubMed]
- Drummond, G.R.; Vinh, A.; Guzik, T.J.; Sobey, C.G. Immune mechanisms of hypertension. Nat. Rev. Immunol. 2019, 19, 517–532. [Google Scholar] [CrossRef]
- Urbanski, K.; Ludew, D.; Filip, G.; Filip, M.; Sagan, A.; Szczepaniak, P.; Grudzien, G.; Sadowski, J.; Jasiewicz-Honkisz, B.; Sliwa, T.; et al. CD14(+)CD16(++) “nonclassical” monocytes are associated with endothelial dysfunction in patients with coronary artery disease. Thromb. Haemost. 2017, 117, 971–980. [Google Scholar] [CrossRef]
- Weber, C.; Shantsila, E.; Hristov, M.; Caligiuri, G.; Guzik, T.; Heine, G.H.; Hoefer, I.E.; Monaco, C.; Peter, K.; Rainger, E.; et al. Role and analysis of monocyte subsets in cardiovascular disease. Joint consensus document of the European Society of Cardiology (ESC) Working Groups “Atherosclerosis & Vascular Biology” and “Thrombosis”. Thromb. Haemost. 2016, 116, 626–637. [Google Scholar] [CrossRef]
- Gerhardt, T.; Ley, K. Monocyte trafficking across the vessel wall. Cardiovasc. Res. 2015, 107, 321–330. [Google Scholar] [CrossRef] [PubMed]
- Moore, J.P.; Vinh, A.; Tuck, K.L.; Sakkal, S.; Krishnan, S.M.; Chan, C.T.; Lieu, M.; Samuel, C.S.; Diep, H.; Kemp-Harper, B.K.; et al. M2 macrophage accumulation in the aortic wall during angiotensin II infusion in mice is associated with fibrosis, elastin loss, and elevated blood pressure. Am. J. Physiol. Heart Circ. Physiol. 2015, 309, 906–917. [Google Scholar] [CrossRef] [PubMed]
- Skiba, D.S.; Nosalski, R.; Mikolajczyk, T.P.; Siedlinski, M.; Rios, F.J.; Montezano, A.C.; Jawien, J.; Olszanecki, R.; Korbut, R.; Czesnikiewicz-Guzik, M.; et al. Anti-atherosclerotic effect of the angiotensin 1–7 mimetic AVE0991 is mediated by inhibition of perivascular and plaque inflammation in early atherosclerosis. Br. J. Pharmacol. 2017, 174, 4055–4069. [Google Scholar] [CrossRef] [PubMed]
- Madrigal-Matute, J.; Fernandez-Laso, V.; Sastre, C.; Llamas-Granda, P.; Egido, J.; Martin-Ventura, J.L.; Zalba, G.; Blanco-Colio, L.M. TWEAK/Fn14 interaction promotes oxidative stress through NADPH oxidase activation in macrophages. Cardiovasc. Res. 2015, 108, 139–147. [Google Scholar] [CrossRef] [PubMed]
- Harrison, D.G.; Guzik, T.J. Macrophages come to mind as keys to cognitive decline. J. Clin. Investig. 2016, 126, 4393–4395. [Google Scholar] [CrossRef]
- Cifuentes, D.; Poittevin, M.; Dere, E.; Broqueres-You, D.; Bonnin, P.; Benessiano, J.; Pocard, M.; Mariani, J.; Kubis, N.; Merkulova-Rainon, T.; et al. Hypertension accelerates the progression of Alzheimer-like pathology in a mouse model of the disease. Hypertension 2015, 65, 218–224. [Google Scholar] [CrossRef]
- Wang, X.; Khalil, R.A. Matrix Metalloproteinases, Vascular Remodeling, and Vascular Disease. Adv. Pharmacol. 2018, 81, 241–330. [Google Scholar] [CrossRef]
- Hopps, E.; Lo Presti, R.; Caimi, G. Matrix Metalloproteases in Arterial Hypertension and their Trend after Antihypertensive Treatment. Kidney Blood Press. Res. 2017, 42, 347–357. [Google Scholar] [CrossRef]
- Bunbupha, S.; Pakdeechote, P.; Maneesai, P.; Prachaney, P.; Boonprom, P. Carthamus Tinctorius L. extract attenuates cardiac remodeling in L-NAME-induced hypertensive rats by inhibiting the NADPH oxidase-mediated TGF-beta1 and MMP-9 pathway. Ann. Anat. Anat. Anz. 2019, 222, 120–128. [Google Scholar] [CrossRef]
- Di Gregoli, K.; George, S.J.; Jackson, C.L.; Newby, A.C.; Johnson, J.L. Differential effects of tissue inhibitor of metalloproteinase (TIMP)-1 and TIMP-2 on atherosclerosis and monocyte/macrophage invasion. Cardiovasc. Res. 2016, 109, 318–330. [Google Scholar] [CrossRef]
- Ma, Y.; Chiao, Y.A.; Clark, R.; Flynn, E.R.; Yabluchanskiy, A.; Ghasemi, O.; Zouein, F.; Lindsey, M.L.; Jin, Y.F. Deriving a cardiac ageing signature to reveal MMP-9-dependent inflammatory signalling in senescence. Cardiovasc. Res. 2015, 106, 421–431. [Google Scholar] [CrossRef] [PubMed]
- Stout, L.C.; Whorton, E.B., Jr.; Vaghela, M. Pathogenesis of diffuse intimal thickening (DIT) in non-human primate thoracic aortas. Atherosclerosis 1983, 47, 1–6. [Google Scholar] [CrossRef]
- Petersen-Jones, H.G.; Johnson, K.B.; Hitomi, K.; Tykocki, N.R.; Thompson, J.M.; Watts, S.W. Transglutaminase activity is decreased in large arteries from hypertensive rats compared with normotensive controls. Am. J. Physiol. Heart Circ. Physiol. 2015, 308, 592–602. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Wang, M.; Zhang, J.; Jiang, L.Q.; Spinetti, G.; Pintus, G.; Monticone, R.; Kolodgie, F.D.; Virmani, R.; Lakatta, E.G. Proinflammatory profile within the grossly normal aged human aortic wall. Hypertension 2007, 50, 219–227. [Google Scholar] [CrossRef]
- Neves, K.B.; Nguyen Dinh Cat, A.; Lopes, R.A.; Rios, F.J.; Anagnostopoulou, A.; Lobato, N.S.; de Oliveira, A.M.; Tostes, R.C.; Montezano, A.C.; Touyz, R.M. Chemerin Regulates Crosstalk Between Adipocytes and Vascular Cells Through Nox. Hypertension 2015, 66, 657–666. [Google Scholar] [CrossRef]
- Krug, A.W.; Allenhofer, L.; Monticone, R.; Spinetti, G.; Gekle, M.; Wang, M.; Lakatta, E.G. Elevated mineralocorticoid receptor activity in aged rat vascular smooth muscle cells promotes a proinflammatory phenotype via extracellular signal-regulated kinase 1/2 mitogen-activated protein kinase and epidermal growth factor receptor-dependent pathways. Hypertension 2010, 55, 1476–1483. [Google Scholar] [CrossRef]
- Spiers, J.P.; Kelso, E.J.; Siah, W.F.; Edge, G.; Song, G.; McDermott, B.J.; Hennessy, M. Alterations in vascular matrix metalloproteinase due to ageing and chronic hypertension: Effects of endothelin receptor blockade. J. Hypertens. 2005, 23, 1717–1724. [Google Scholar] [CrossRef]
- Park, J.B.; Schiffrin, E.L. Cardiac and vascular fibrosis and hypertrophy in aldosterone-infused rats: Role of endothelin-1. Am. J. Hypertens. 2002, 15, 164–169. [Google Scholar] [CrossRef]
- Weigert, C.; Brodbeck, K.; Klopfer, K.; Haring, H.U.; Schleicher, E.D. Angiotensin II induces human TGF-beta 1 promoter activation: Similarity to hyperglycaemia. Diabetologia 2002, 45, 890–898. [Google Scholar] [CrossRef]
- Carver, K.A.; Smith, T.L.; Gallagher, P.E.; Tallant, E.A. Angiotensin-(1-7) prevents angiotensin II-induced fibrosis in cremaster microvessels. Microcirculation 2015, 22, 19–27. [Google Scholar] [CrossRef]
- Ishidoya, S.; Morrissey, J.; McCracken, R.; Reyes, A.; Klahr, S. Angiotensin II receptor antagonist ameliorates renal tubulointerstitial fibrosis caused by unilateral ureteral obstruction. Kidney Int. 1995, 47, 1285–1294. [Google Scholar] [CrossRef] [PubMed]
- Ruiz-Ortega, M.; Gonzalez, S.; Seron, D.; Condom, E.; Bustos, C.; Largo, R.; Gonzalez, E.; Ortiz, A.; Egido, J. ACE inhibition reduces proteinuria, glomerular lesions and extracellular matrix production in a normotensive rat model of immune complex nephritis. Kidney Int. 1995, 48, 1778–1791. [Google Scholar] [CrossRef] [PubMed]
- Duncan, M.R.; Frazier, K.S.; Abramson, S.; Williams, S.; Klapper, H.; Huang, X.; Grotendorst, G.R. Connective tissue growth factor mediates transforming growth factor beta-induced collagen synthesis: Down-regulation by cAMP. FASEB J. 1999, 13, 1774–1786. [Google Scholar] [CrossRef]
- Sakurabayashi-Kitade, S.; Aoka, Y.; Nagashima, H.; Kasanuki, H.; Hagiwara, N.; Kawana, M. Aldosterone blockade by Spironolactone improves the hypertensive vascular hypertrophy and remodeling in angiotensin II overproducing transgenic mice. Atherosclerosis 2009, 206, 54–60. [Google Scholar] [CrossRef] [PubMed]
- Callera, G.E.; Yogi, A.; Briones, A.M.; Montezano, A.C.; He, Y.; Tostes, R.C.; Schiffrin, E.L.; Touyz, R.M. Vascular proinflammatory responses by aldosterone are mediated via c-Src trafficking to cholesterol-rich microdomains: Role of PDGFR. Cardiovasc. Res. 2011, 91, 720–731. [Google Scholar] [CrossRef]
- Savoia, C.; Touyz, R.M.; Amiri, F.; Schiffrin, E.L. Selective mineralocorticoid receptor blocker eplerenone reduces resistance artery stiffness in hypertensive patients. Hypertension 2008, 51, 432–439. [Google Scholar] [CrossRef]
- Briones, A.M.; Nguyen Dinh Cat, A.; Callera, G.E.; Yogi, A.; Burger, D.; He, Y.; Correa, J.W.; Gagnon, A.M.; Gomez-Sanchez, C.E.; Gomez-Sanchez, E.P.; et al. Adipocytes produce aldosterone through calcineurin-dependent signaling pathways: Implications in diabetes mellitus-associated obesity and vascular dysfunction. Hypertension 2012, 59, 1069–1078. [Google Scholar] [CrossRef]
- Horstmeyer, A.; Licht, C.; Scherr, G.; Eckes, B.; Krieg, T. Signalling and regulation of collagen I synthesis by ET-1 and TGF-beta1. FEBS J. 2005, 272, 6297–6309. [Google Scholar] [CrossRef]
- Hafizi, S.; Wharton, J.; Chester, A.H.; Yacoub, M.H. Profibrotic effects of endothelin-1 via the ETA receptor in cultured human cardiac fibroblasts. Cell Physiol. Biochem. 2004, 14, 285–292. [Google Scholar] [CrossRef]
- Libby, P.; Ridker, P.M.; Hansson, G.K. Progress and challenges in translating the biology of atherosclerosis. Nature 2011, 473, 317–325. [Google Scholar] [CrossRef]
- Sanada, F.; Taniyama, Y.; Muratsu, J.; Otsu, R.; Shimizu, H.; Rakugi, H.; Morishita, R. Gene-Therapeutic Strategies Targeting Angiogenesis in Peripheral Artery Disease. Medicines 2018, 5, 31. [Google Scholar] [CrossRef]
- Herrington, W.; Lacey, B.; Sherliker, P.; Armitage, J.; Lewington, S. Epidemiology of Atherosclerosis and the Potential to Reduce the Global Burden of Atherothrombotic Disease. Circ. Res. 2016, 118, 535–546. [Google Scholar] [CrossRef] [PubMed]
- Jakovljevic, D.G. Physical activity and cardiovascular aging: Physiological and molecular insights. Exp. Gerontol. 2018, 109, 67–74. [Google Scholar] [CrossRef] [PubMed]
- Lam, C.S.; Xanthakis, V.; Sullivan, L.M.; Lieb, W.; Aragam, J.; Redfield, M.M.; Mitchell, G.F.; Benjamin, E.J.; Vasan, R.S. Aortic root remodeling over the adult life course: Longitudinal data from the Framingham Heart Study. Circulation 2010, 122, 884–890. [Google Scholar] [CrossRef] [PubMed]
- Lorenz, M.W.; Markus, H.S.; Bots, M.L.; Rosvall, M.; Sitzer, M. Prediction of clinical cardiovascular events with carotid intima-media thickness: A systematic review and meta-analysis. Circulation 2007, 115, 459–467. [Google Scholar] [CrossRef] [PubMed]
- Goldschmidt-Clermont, P.J.; Dong, C.; Seo, D.M.; Velazquez, O.C. Atherosclerosis, inflammation, genetics, and stem cells: 2012 update. Curr. Atheroscler. Rep. 2012, 14, 201–210. [Google Scholar] [CrossRef][Green Version]
- Song, Y.; Shen, H.; Schenten, D.; Shan, P.; Lee, P.J.; Goldstein, D.R. Aging enhances the basal production of IL-6 and CCL2 in vascular smooth muscle cells. Arterioscler. Thromb. Vasc. Biol. 2012, 32, 103–109. [Google Scholar] [CrossRef]
- Spagnoli, L.G.; Orlandi, A.; Mauriello, A.; Santeusanio, G.; de Angelis, C.; Lucreziotti, R.; Ramacci, M.T. Aging and atherosclerosis in the rabbit. 1. Distribution, prevalence and morphology of atherosclerotic lesions. Atherosclerosis 1991, 89, 11–24. [Google Scholar] [CrossRef]
- Wang, J.; Uryga, A.K.; Reinhold, J.; Figg, N.; Baker, L.; Finigan, A.; Gray, K.; Kumar, S.; Clarke, M.; Bennett, M. Vascular Smooth Muscle Cell Senescence Promotes Atherosclerosis and Features of Plaque Vulnerability. Circulation 2015, 132, 1909–1919. [Google Scholar] [CrossRef]
- Childs, B.G.; Baker, D.J.; Wijshake, T.; Conover, C.A.; Campisi, J.; van Deursen, J.M. Senescent intimal foam cells are deleterious at all stages of atherosclerosis. Science 2016, 354, 472–477. [Google Scholar] [CrossRef]
- Dimri, G.P.; Lee, X.; Basile, G.; Acosta, M.; Scott, G.; Roskelley, C.; Medrano, E.E.; Linskens, M.; Rubelj, I.; Pereira-Smith, O.; et al. A biomarker that identifies senescent human cells in culture and in aging skin in vivo. Proc. Natl. Acad. Sci. USA 1995, 92, 9363–9367. [Google Scholar] [CrossRef] [PubMed]
- Childs, B.G.; Durik, M.; Baker, D.J.; van Deursen, J.M. Cellular senescence in aging and age-related disease: From mechanisms to therapy. Nat. Med. 2015, 21, 1424–1435. [Google Scholar] [CrossRef] [PubMed]
- Puca, A.A.; Carrizzo, A.; Villa, F.; Ferrario, A.; Casaburo, M.; Maciag, A.; Vecchione, C. Vascular ageing: The role of oxidative stress. Int. J. Biochem. Cell. Biol. 2013, 45, 556–559. [Google Scholar] [CrossRef] [PubMed]
- Chang, J.C.; Kou, S.J.; Lin, W.T.; Liu, C.S. Regulatory role of mitochondria in oxidative stress and atherosclerosis. World J. Cardiol. 2010, 2, 150–159. [Google Scholar] [CrossRef] [PubMed]
- Yang, X.; Li, Y.; Li, Y.; Ren, X.; Zhang, X.; Hu, D.; Gao, Y.; Xing, Y.; Shang, H. Oxidative Stress-Mediated Atherosclerosis: Mechanisms and Therapies. Front. Physiol. 2017, 8, 600. [Google Scholar] [CrossRef]
- Fontana, L.; Vinciguerra, M.; Longo, V.D. Growth factors, nutrient signaling, and cardiovascular aging. Circ. Res. 2012, 110, 1139–1150. [Google Scholar] [CrossRef]
- Kitada, M.; Ogura, Y.; Koya, D. The protective role of Sirt1 in vascular tissue: Its relationship to vascular aging and atherosclerosis. Aging (Albany N. Y.) 2016, 8, 2290–2307. [Google Scholar] [CrossRef]
- Romano, A.D.; Serviddio, G.; de Matthaeis, A.; Bellanti, F.; Vendemiale, G. Oxidative stress and aging. J. Nephrol. 2010, 23, 29–36. [Google Scholar]
- Leon, A.S.; Rice, T.; Mandel, S.; Despres, J.P.; Bergeron, J.; Gagnon, J.; Rao, D.C.; Skinner, J.S.; Wilmore, J.H.; Bouchard, C. Blood lipid response to 20 weeks of supervised exercise in a large biracial population: The HERITAGE Family Study. Metabolism 2000, 49, 513–520. [Google Scholar] [CrossRef]
- Badireddy, M.; Mudipalli, V.R. Deep Venous Thrombosis Prophylaxis. In StatPearls; StatPearls Publishing: Treasure Island, FL, USA, 2020. [Google Scholar]
- Jimenez, D.; Bikdeli, B.; Quezada, A.; Muriel, A.; Lobo, J.L.; de Miguel-Diez, J.; Jara-Palomares, L.; Ruiz-Artacho, P.; Yusen, R.D.; Monreal, M.; et al. Hospital volume and outcomes for acute pulmonary embolism: Multinational population based cohort study. BMJ 2019, 366, l4416. [Google Scholar] [CrossRef]
- Vaqar, S.; Graber, M. Thromboembolic Event. In StatPearls; StatPearls Publishing: Treasure Island, FL, USA, 2020. [Google Scholar]
- Price, C.P.; Fay, M.; Hopstaken, R.M. Point-of-Care Testing for D-Dimer in the Diagnosis of Venous Thromboembolism in Primary Care: A Narrative Review. Cardiol. Ther. 2020. [Google Scholar] [CrossRef]
- Stone, J.; Hangge, P.; Albadawi, H.; Wallace, A.; Shamoun, F.; Knuttien, M.G.; Naidu, S.; Oklu, R. Deep vein thrombosis: Pathogenesis, diagnosis, and medical management. Cardiovasc. Diagn. Ther. 2017, 7, 276–284. [Google Scholar] [CrossRef]
- Konstantinides, S.V.; Meyer, G.; Becattini, C.; Bueno, H.; Geersing, G.J.; Harjola, V.P.; Huisman, M.V.; Humbert, M.; Jennings, C.S.; Jimenez, D.; et al. 2019 ESC Guidelines for the diagnosis and management of acute pulmonary embolism developed in collaboration with the European Respiratory Society (ERS). Eur. Heart J. 2020, 41, 543–603. [Google Scholar] [CrossRef]
- Waheed, S.M.; Kudaravalli, P.; Hotwagner, D.T. Deep Vein Thrombosis. In StatPearls; StatPearls Publishing: Treasure Island, FL, USA, 2020. [Google Scholar]
- Tsai, A.W.; Cushman, M.; Rosamond, W.D.; Heckbert, S.R.; Polak, J.F.; Folsom, A.R. Cardiovascular risk factors and venous thromboembolism incidence: The longitudinal investigation of thromboembolism etiology. Arch. Intern. Med. 2002, 162, 1182–1189. [Google Scholar] [CrossRef]
- Esmon, C.T. Basic mechanisms and pathogenesis of venous thrombosis. Blood Rev. 2009, 23, 225–229. [Google Scholar] [CrossRef]
- Rumley, A.; Emberson, J.R.; Wannamethee, S.G.; Lennon, L.; Whincup, P.H.; Lowe, G.D. Effects of older age on fibrin D-dimer, C-reactive protein, and other hemostatic and inflammatory variables in men aged 60–79 years. J. Thromb. Haemost. 2006, 4, 982–987. [Google Scholar] [CrossRef] [PubMed]
- Favaloro, E.J.; Franchini, M.; Lippi, G. Aging hemostasis: Changes to laboratory markers of hemostasis as we age—A narrative review. In Seminars in Thrombosis and Hemostasis; Thieme Medical Publishers: New York, NY, USA, 2014; Volume 40, pp. 621–633. [Google Scholar] [CrossRef]
- Versteeg, H.H.; Heemskerk, J.W.; Levi, M.; Reitsma, P.H. New fundamentals in hemostasis. Physiol. Rev. 2013, 93, 327–358. [Google Scholar] [CrossRef] [PubMed]
- Wang, Q.; Zennadi, R. Oxidative Stress and Thrombosis during Aging: The Roles of Oxidative Stress in RBCs in Venous Thrombosis. Int. J. Mol. Sci. 2020, 21, 4259. [Google Scholar] [CrossRef]
- Carrizzo, A.; Izzo, C.; Oliveti, M.; Alfano, A.; Virtuoso, N.; Capunzo, M.; Di Pietro, P.; Calabrese, M.; De Simone, E.; Sciarretta, S.; et al. The Main Determinants of Diabetes Mellitus Vascular Complications: Endothelial Dysfunction and Platelet Hyperaggregation. Int. J. Mol. Sci. 2018, 19, 2968. [Google Scholar] [CrossRef]
- Lopes, R.A.; Neves, K.B.; Tostes, R.C.; Montezano, A.C.; Touyz, R.M. Downregulation of Nuclear Factor Erythroid 2-Related Factor and Associated Antioxidant Genes Contributes to Redox-Sensitive Vascular Dysfunction in Hypertension. Hypertension 2015, 66, 1240–1250. [Google Scholar] [CrossRef]
- Csiszar, A.; Pacher, P.; Kaley, G.; Ungvari, Z. Role of oxidative and nitrosative stress, longevity genes and poly(ADP-ribose) polymerase in cardiovascular dysfunction associated with aging. Curr. Vasc. Pharmacol. 2005, 3, 285–291. [Google Scholar] [CrossRef] [PubMed]
- Khaku, A.S.; Tadi, P. Cerebrovascular Disease. In StatPearls; StatPearls Publishing: Treasure Island, FL, USA, 2020. [Google Scholar]
- Writing Group, M.; Mozaffarian, D.; Benjamin, E.J.; Go, A.S.; Arnett, D.K.; Blaha, M.J.; Cushman, M.; Das, S.R.; de Ferranti, S.; Despres, J.P.; et al. Heart Disease and Stroke Statistics-2016 Update: A Report From the American Heart Association. Circulation 2016, 133, 38–360. [Google Scholar] [CrossRef]
- Panuganti, K.K.; Tadi, P.; Lui, F. Transient Ischemic Attack. In StatPearls; StatPearls Publishing: Treasure Island, FL, USA, 2020. [Google Scholar]
- Di Carlo, A. Human and economic burden of stroke. Age Ageing 2009, 38, 4–5. [Google Scholar] [CrossRef] [PubMed]
- Rosamond, W.; Flegal, K.; Furie, K.; Go, A.; Greenlund, K.; Haase, N.; Hailpern, S.M.; Ho, M.; Howard, V.; Kissela, B.; et al. Heart disease and stroke statistics—2008 update: A report from the American Heart Association Statistics Committee and Stroke Statistics Subcommittee. Circulation 2008, 117, 25–146. [Google Scholar] [CrossRef]
- Navis, A.; Garcia-Santibanez, R.; Skliut, M. Epidemiology and Outcomes of Ischemic Stroke and Transient Ischemic Attack in the Adult and Geriatric Population. J. Stroke Cerebrovasc. Dis. 2019, 28, 84–89. [Google Scholar] [CrossRef]
- Tadi, P.; Lui, F. Acute Stroke. In StatPearls; StatPearls Publishing: Treasure Island, FL, USA, 2020. [Google Scholar]
- Xing, C.; Arai, K.; Lo, E.H.; Hommel, M. Pathophysiologic cascades in ischemic stroke. Int. J. Stroke 2012, 7, 378–385. [Google Scholar] [CrossRef]
- Rothwell, P.M.; Coull, A.J.; Silver, L.E.; Fairhead, J.F.; Giles, M.F.; Lovelock, C.E.; Redgrave, J.N.; Bull, L.M.; Welch, S.J.; Cuthbertson, F.C.; et al. Population-based study of event-rate, incidence, case fatality, and mortality for all acute vascular events in all arterial territories (Oxford Vascular Study). Lancet 2005, 366, 1773–1783. [Google Scholar] [CrossRef]
- Kandlur, A.; Satyamoorthy, K.; Gangadharan, G. Oxidative Stress in Cognitive and Epigenetic Aging: A Retrospective Glance. Front. Mol. Neurosci. 2020, 13, 41. [Google Scholar] [CrossRef]
- Baierle, M.; Nascimento, S.N.; Moro, A.M.; Brucker, N.; Freitas, F.; Gauer, B.; Durgante, J.; Bordignon, S.; Zibetti, M.; Trentini, C.M.; et al. Relationship between inflammation and oxidative stress and cognitive decline in the institutionalized elderly. Oxidative Med. Cell. Longev. 2015, 2015, 804198. [Google Scholar] [CrossRef]
- Ueno, M.; Tomimoto, H.; Akiguchi, I.; Wakita, H.; Sakamoto, H. Blood-brain barrier disruption in white matter lesions in a rat model of chronic cerebral hypoperfusion. J. Cereb. Blood Flow Metab. 2002, 22, 97–104. [Google Scholar] [CrossRef]
- Shao, A.; Lin, D.; Wang, L.; Tu, S.; Lenahan, C.; Zhang, J. Oxidative Stress at the Crossroads of Aging, Stroke and Depression. Aging Dis. 2020, 11, 1537–1566. [Google Scholar] [CrossRef] [PubMed]
- Anwar, M.A.; Eid, A.H. Determination of Vascular Reactivity of Middle Cerebral Arteries from Stroke and Spinal Cord Injury Animal Models Using Pressure Myography. Methods Mol. Biol. 2016, 1462, 611–624. [Google Scholar] [CrossRef] [PubMed]
- Zitnanova, I.; Siarnik, P.; Kollar, B.; Chomova, M.; Pazderova, P.; Andrezalova, L.; Jezovicova, M.; Konarikova, K.; Laubertova, L.; Krivosikova, Z.; et al. Oxidative Stress Markers and Their Dynamic Changes in Patients after Acute Ischemic Stroke. Oxidative Med. Cell. Longev. 2016, 2016, 9761697. [Google Scholar] [CrossRef] [PubMed]
- Wang, A.; Cui, Y.; Meng, X.; Su, Z.; Cao, Y.; Yang, Y.; Liu, C.; Dai, L.; Wang, Y.; Wang, Y. The relationship between oxidized low-density lipoprotein and the NIHSS score among patients with acute ischemic stroke: The SOS-Stroke Study. Atherosclerosis 2018, 270, 21–25. [Google Scholar] [CrossRef]
- Wang, A.; Yang, Y.; Su, Z.; Yue, W.; Hao, H.; Ren, L.; Wang, Y.; Cao, Y.; Wang, Y. Association of Oxidized Low-Density Lipoprotein With Prognosis of Stroke and Stroke Subtypes. Stroke 2017, 48, 91–97. [Google Scholar] [CrossRef]
- Wang, A.; Liu, J.; Meng, X.; Li, J.; Wang, H.; Wang, Y.; Su, Z.; Zhang, N.; Dai, L.; Wang, Y.; et al. Association between oxidized low-density lipoprotein and cognitive impairment in patients with ischemic stroke. Eur. J. Neurol. 2018, 25, 185–191. [Google Scholar] [CrossRef]
- Mendelsohn, A.R.; Larrick, J.W. The NAD+/PARP1/SIRT1 Axis in Aging. Rejuvenation Res. 2017, 20, 244–247. [Google Scholar] [CrossRef]
- Ham, P.B., 3rd; Raju, R. Mitochondrial function in hypoxic ischemic injury and influence of aging. Prog. Neurobiol. 2017, 157, 92–116. [Google Scholar] [CrossRef]
- Rodrigo, R.; Fernandez-Gajardo, R.; Gutierrez, R.; Matamala, J.M.; Carrasco, R.; Miranda-Merchak, A.; Feuerhake, W. Oxidative stress and pathophysiology of ischemic stroke: Novel therapeutic opportunities. CNS Neurol. Disord. Drug Targets 2013, 12, 698–714. [Google Scholar] [CrossRef]
- Tang, Z.; Li, M.; Zhang, X.; Hou, W. Dietary flavonoid intake and the risk of stroke: A dose-response meta-analysis of prospective cohort studies. BMJ Open 2016, 6, e008680. [Google Scholar] [CrossRef]
- Targum, S.D.; Wedel, P.C.; Fava, M. Changes in cognitive symptoms after a buspirone-melatonin combination treatment for Major Depressive Disorder. J. Psychiatr. Res. 2015, 68, 392–396. [Google Scholar] [CrossRef] [PubMed]
- Su, X.T.; Wang, L.; Ma, S.M.; Cao, Y.; Yang, N.N.; Lin, L.L.; Fisher, M.; Yang, J.W.; Liu, C.Z. Mechanisms of Acupuncture in the Regulation of Oxidative Stress in Treating Ischemic Stroke. Oxidative Med. Cell. Longev. 2020, 2020, 7875396. [Google Scholar] [CrossRef] [PubMed]
- Colman, R.J.; Anderson, R.M.; Johnson, S.C.; Kastman, E.K.; Kosmatka, K.J.; Beasley, T.M.; Allison, D.B.; Cruzen, C.; Simmons, H.A.; Kemnitz, J.W.; et al. Caloric restriction delays disease onset and mortality in rhesus monkeys. Science 2009, 325, 201–204. [Google Scholar] [CrossRef] [PubMed]
- Cruzen, C.; Colman, R.J. Effects of caloric restriction on cardiovascular aging in non-human primates and humans. Clin. Geriatr. Med. 2009, 25, 733–743. [Google Scholar] [CrossRef]
- Fowler, C.G.; Chiasson, K.B.; Leslie, T.H.; Thomas, D.; Beasley, T.M.; Kemnitz, J.W.; Weindruch, R. Auditory function in rhesus monkeys: Effects of aging and caloric restriction in the Wisconsin monkeys five years later. Hear. Res. 2010, 261, 75–81. [Google Scholar] [CrossRef]
- Kastman, E.K.; Willette, A.A.; Coe, C.L.; Bendlin, B.B.; Kosmatka, K.J.; McLaren, D.G.; Xu, G.; Canu, E.; Field, A.S.; Alexander, A.L.; et al. A calorie-restricted diet decreases brain iron accumulation and preserves motor performance in old rhesus monkeys. J. Neurosci. 2010, 30, 7940–7947. [Google Scholar] [CrossRef]
- McKiernan, S.H.; Colman, R.J.; Lopez, M.; Beasley, T.M.; Aiken, J.M.; Anderson, R.M.; Weindruch, R. Caloric restriction delays aging-induced cellular phenotypes in rhesus monkey skeletal muscle. Exp. Gerontol. 2011, 46, 23–29. [Google Scholar] [CrossRef]
- Niemann, B.; Chen, Y.; Issa, H.; Silber, R.E.; Rohrbach, S. Caloric restriction delays cardiac ageing in rats: Role of mitochondria. Cardiovasc. Res. 2010, 88, 267–276. [Google Scholar] [CrossRef]
- Shinmura, K.; Tamaki, K.; Sano, M.; Murata, M.; Yamakawa, H.; Ishida, H.; Fukuda, K. Impact of long-term caloric restriction on cardiac senescence: Caloric restriction ameliorates cardiac diastolic dysfunction associated with aging. J. Mol. Cell. Cardiol. 2011, 50, 117–127. [Google Scholar] [CrossRef]
- Varady, K.A.; Hellerstein, M.K. Alternate-day fasting and chronic disease prevention: A review of human and animal trials. Am. J. Clin. Nutr. 2007, 86, 7–13. [Google Scholar] [CrossRef]
- Palacios, O.M.; Carmona, J.J.; Michan, S.; Chen, K.Y.; Manabe, Y.; Ward, J.L., 3rd; Goodyear, L.J.; Tong, Q. Diet and exercise signals regulate SIRT3 and activate AMPK and PGC-1alpha in skeletal muscle. Aging (Albany N. Y.) 2009, 1, 771–783. [Google Scholar] [CrossRef]
- Goswami, S.K.; Das, D.K. Autophagy in the myocardium: Dying for survival? Exp. Clin. Cardiol. 2006, 11, 183–188. [Google Scholar] [PubMed]
- Wohlgemuth, S.E.; Julian, D.; Akin, D.E.; Fried, J.; Toscano, K.; Leeuwenburgh, C.; Dunn, W.A., Jr. Autophagy in the heart and liver during normal aging and calorie restriction. Rejuvenation Res. 2007, 10, 281–292. [Google Scholar] [CrossRef]
- Saifutdinov, R.G.; Trifonova, E.V. Investigation on mice of the common toxicity of methyl-tert-butyl ether, substance for contact chemical litholys of cholesterol stones in a gallbladder. Exp. Clin. Gastroenterol. 2011, 4, 70–73. [Google Scholar]
- Shinmura, K.; Tamaki, K.; Bolli, R. Impact of 6-mo caloric restriction on myocardial ischemic tolerance: Possible involvement of nitric oxide-dependent increase in nuclear Sirt1. Am. J. Physiol. Heart Circ. Physiol. 2008, 295, 2348–2355. [Google Scholar] [CrossRef]
- Hepple, R.T.; Baker, D.J.; McConkey, M.; Murynka, T.; Norris, R. Caloric restriction protects mitochondrial function with aging in skeletal and cardiac muscles. Rejuvenation Res. 2006, 9, 219–222. [Google Scholar] [CrossRef]
- Rohrbach, S.; Niemann, B.; Abushouk, A.M.; Holtz, J. Caloric restriction and mitochondrial function in the ageing myocardium. Exp. Gerontol. 2006, 41, 525–531. [Google Scholar] [CrossRef]
- Kris-Etherton, P.M.; Lichtenstein, A.H.; Howard, B.V.; Steinberg, D.; Witztum, J.L.; Nutrition Committee of the American Heart Association Council on Nutrition, Physical Activity, and Metabolism. Antioxidant vitamin supplements and cardiovascular disease. Circulation 2004, 110, 637–641. [Google Scholar] [CrossRef]
- Martinez Gonzalez, J.M.; Grana Gomez, J.L.; Trujillo Mendoza, H. Longitudinal study on quality of life, craving and psychological adjustment in alcohol-dependent patients: Variations depending on the personality disorders. Adicciones 2011, 23, 227–235. [Google Scholar]
- Lennox, S.D.; Mulkerrin, E.; Penney, M.; Woodhouse, K. Plasma atrial natriuretic polypeptide in the elderly: Age or hypertension? Arch. Gerontol. Geriatr. 1994, 19, 1–5. [Google Scholar] [CrossRef]
- Bjelakovic, G.; Nikolova, D.; Gluud, L.L.; Simonetti, R.G.; Gluud, C. Mortality in randomized trials of antioxidant supplements for primary and secondary prevention: Systematic review and meta-analysis. JAMA 2007, 297, 842–857. [Google Scholar] [CrossRef] [PubMed]
- Steinhubl, S.R. Why have antioxidants failed in clinical trials? Am. J. Cardiol. 2008, 101, 14–19. [Google Scholar] [CrossRef] [PubMed]
- Patel, K.R.; Scott, E.; Brown, V.A.; Gescher, A.J.; Steward, W.P.; Brown, K. Clinical trials of resveratrol. Ann. N. Y. Acad. Sci. 2011, 1215, 161–169. [Google Scholar] [CrossRef] [PubMed]
- Rodrigo, R.; Miranda, A.; Vergara, L. Modulation of endogenous antioxidant system by wine polyphenols in human disease. Clin. Chim. Acta 2011, 412, 410–424. [Google Scholar] [CrossRef]
- van Empel, V.P.; Bertrand, A.T.; van Oort, R.J.; van der Nagel, R.; Engelen, M.; van Rijen, H.V.; Doevendans, P.A.; Crijns, H.J.; Ackerman, S.L.; Sluiter, W.; et al. EUK-8, a superoxide dismutase and catalase mimetic, reduces cardiac oxidative stress and ameliorates pressure overload-induced heart failure in the harlequin mouse mutant. J. Am. Coll. Cardiol. 2006, 48, 824–832. [Google Scholar] [CrossRef]
- Medina-Remon, A.; Zamora-Ros, R.; Rotches-Ribalta, M.; Andres-Lacueva, C.; Martinez-Gonzalez, M.A.; Covas, M.I.; Corella, D.; Salas-Salvado, J.; Gomez-Gracia, E.; Ruiz-Gutierrez, V.; et al. Total polyphenol excretion and blood pressure in subjects at high cardiovascular risk. Nutr. Metab. Cardiovasc. Dis. 2011, 21, 323–331. [Google Scholar] [CrossRef]
- Bakker, G.C.; van Erk, M.J.; Pellis, L.; Wopereis, S.; Rubingh, C.M.; Cnubben, N.H.; Kooistra, T.; van Ommen, B.; Hendriks, H.F. An antiinflammatory dietary mix modulates inflammation and oxidative and metabolic stress in overweight men: A nutrigenomics approach. Am. J. Clin. Nutr. 2010, 91, 1044–1059. [Google Scholar] [CrossRef]
- Sachdeva, V.; Roy, A.; Bharadvaja, N. Current Prospects of Nutraceuticals: A Review. Curr. Pharm. Biotechnol. 2020, 21, 884–896. [Google Scholar] [CrossRef]
- Carrizzo, A.; Moltedo, O.; Damato, A.; Martinello, K.; Di Pietro, P.; Oliveti, M.; Acernese, F.; Giugliano, G.; Izzo, R.; Sommella, E.; et al. New Nutraceutical Combination Reduces Blood Pressure and Improves Exercise Capacity in Hypertensive Patients Via a Nitric Oxide-Dependent Mechanism. J. Am. Heart Assoc. 2020, 9, e014923. [Google Scholar] [CrossRef]
- Santini, A.; Cammarata, S.M.; Capone, G.; Ianaro, A.; Tenore, G.C.; Pani, L.; Novellino, E. Nutraceuticals: Opening the debate for a regulatory framework. Br. J. Clin. Pharmacol. 2018, 84, 659–672. [Google Scholar] [CrossRef]
- Helal, N.A.; Eassa, H.A.; Amer, A.M.; Eltokhy, M.A.; Edafiogho, I.; Nounou, M.I. Nutraceuticals’ Novel Formulations: The Good, the Bad, the Unknown and Patents Involved. Recent Pat. Drug Deliv. Formul. 2019, 13, 105–156. [Google Scholar] [CrossRef] [PubMed]
- Sauer, S.; Plauth, A. Health-beneficial nutraceuticals-myth or reality? Appl. Microbiol. Biotechnol. 2017, 101, 951–961. [Google Scholar] [CrossRef] [PubMed]
- Biesalski, H.K.; Tinz, J. Multivitamin/mineral supplements: Rationale and safety—A systematic review. Nutrition 2017, 33, 76–82. [Google Scholar] [CrossRef] [PubMed]
- Carrizzo, A.; Izzo, C.; Forte, M.; Sommella, E.; Di Pietro, P.; Venturini, E.; Ciccarelli, M.; Galasso, G.; Rubattu, S.; Campiglia, P.; et al. A Novel Promising Frontier for Human Health: The Beneficial Effects of Nutraceuticals in Cardiovascular Diseases. Int. J. Mol. Sci. 2020, 21, 8706. [Google Scholar] [CrossRef] [PubMed]
- Schwingshackl, L.; Boeing, H.; Stelmach-Mardas, M.; Gottschald, M.; Dietrich, S.; Hoffmann, G.; Chaimani, A. Dietary Supplements and Risk of Cause-Specific Death, Cardiovascular Disease, and Cancer: A Systematic Review and Meta-Analysis of Primary Prevention Trials. Adv. Nutr. 2017, 8, 27–39. [Google Scholar] [CrossRef]
- Carrizzo, A.; Forte, M.; Damato, A.; Trimarco, V.; Salzano, F.; Bartolo, M.; Maciag, A.; Puca, A.A.; Vecchione, C. Antioxidant effects of resveratrol in cardiovascular, cerebral and metabolic diseases. Food Chem. Toxicol. 2013, 61, 215–226. [Google Scholar] [CrossRef]
- Carrizzo, A.; Puca, A.; Damato, A.; Marino, M.; Franco, E.; Pompeo, F.; Traficante, A.; Civitillo, F.; Santini, L.; Trimarco, V.; et al. Resveratrol improves vascular function in patients with hypertension and dyslipidemia by modulating NO metabolism. Hypertension 2013, 62, 359–366. [Google Scholar] [CrossRef]
- Barger, J.L.; Kayo, T.; Vann, J.M.; Arias, E.B.; Wang, J.; Hacker, T.A.; Wang, Y.; Raederstorff, D.; Morrow, J.D.; Leeuwenburgh, C.; et al. A low dose of dietary resveratrol partially mimics caloric restriction and retards aging parameters in mice. PLoS ONE 2008, 3, e2264. [Google Scholar] [CrossRef]
- de Cavanagh, E.M.; Piotrkowski, B.; Fraga, C.G. Concerted action of the renin-angiotensin system, mitochondria, and antioxidant defenses in aging. Mol. Asp. Med. 2004, 25, 27–36. [Google Scholar] [CrossRef]
- Forrester, S.J.; Booz, G.W.; Sigmund, C.D.; Coffman, T.M.; Kawai, T.; Rizzo, V.; Scalia, R.; Eguchi, S. Angiotensin II Signal Transduction: An Update on Mechanisms of Physiology and Pathophysiology. Physiol. Rev. 2018, 98, 1627–1738. [Google Scholar] [CrossRef]
- Gaddam, R.R.; Chambers, S.; Bhatia, M. ACE and ACE2 in inflammation: A tale of two enzymes. Inflamm. Allergy Drug Targets 2014, 13, 224–234. [Google Scholar] [CrossRef] [PubMed]
- Waugh, W.J. Factors to consider in selecting an angiotensin-converting-enzyme inhibitor. Am. J. Health Syst. Pharm. 2000, 57, 26–30. [Google Scholar] [CrossRef] [PubMed]
- Simões, E.; Silva, A.C.; Teixeira, M.M. ACE inhibition, ACE2 and angiotensin-(1-7) axis in kidney and cardiac inflammation and fibrosis. Pharmacol. Res. 2016, 107, 154–162. [Google Scholar] [CrossRef] [PubMed]
- Williams, B. The renin angiotensin system and cardiovascular disease: Hope or hype? J. Renin Angiotensin Aldosterone Syst. 2000, 1, 142–146. [Google Scholar] [CrossRef]
- Vanhoutte, P.M.; Boulanger, C.M.; Illiano, S.C.; Nagao, T.; Vidal, M.; Mombouli, J.V. Endothelium-dependent effects of converting-enzyme inhibitors. J. Cardiovasc. Pharmacol. 1993, 22, 10–16. [Google Scholar] [CrossRef]
- Xu, Y.; Clanachan, A.S.; Jugdutt, B.I. Enhanced expression of angiotensin II type 2 receptor, inositol 1,4, 5-trisphosphate receptor, and protein kinase cepsilon during cardioprotection induced by angiotensin II type 2 receptor blockade. Hypertension 2000, 36, 506–510. [Google Scholar] [CrossRef]
- Kees, F.; Bucher, M.; Schweda, F.; Gschaidmeier, H.; Faerber, L.; Seifert, R. Neoimmun versus Neoral: A bioequivalence study in healthy volunteers and influence of a fat-rich meal on the bioavailability of Neoimmun. Naunyn Schmiedeberg’s Arch. Pharmacol. 2007, 375, 393–399. [Google Scholar] [CrossRef][Green Version]
- Rueckschloss, U.; Quinn, M.T.; Holtz, J.; Morawietz, H. Dose-dependent regulation of NAD(P)H oxidase expression by angiotensin II in human endothelial cells: Protective effect of angiotensin II type 1 receptor blockade in patients with coronary artery disease. Arterioscler. Thromb. Vasc. Biol. 2002, 22, 1845–1851. [Google Scholar] [CrossRef]
- Mira, M.L.; Silva, M.M.; Queiroz, M.J.; Manso, C.F. Angiotensin converting enzyme inhibitors as oxygen free radical scavengers. Free Radic. Res. Commun. 1993, 19, 173–181. [Google Scholar] [CrossRef]
- Chopra, M.; Beswick, H.; Clapperton, M.; Dargie, H.J.; Smith, W.E.; McMurray, J. Antioxidant effects of angiotensin-converting enzyme (ACE) inhibitors: Free radical and oxidant scavenging are sulfhydryl dependent, but lipid peroxidation is inhibited by both sulfhydryl- and nonsulfhydryl-containing ACE inhibitors. J. Cardiovasc. Pharmacol. 1992, 19, 330–340. [Google Scholar] [CrossRef]
- Bagchi, D.; Prasad, R.; Das, D.K. Direct scavenging of free radicals by captopril, an angiotensin converting enzyme inhibitor. Biochem. Biophys Res. Commun. 1989, 158, 52–57. [Google Scholar] [CrossRef]
- de Cavanagh, E.M.; Inserra, F.; Toblli, J.; Stella, I.; Fraga, C.G.; Ferder, L. Enalapril attenuates oxidative stress in diabetic rats. Hypertension 2001, 38, 1130–1136. [Google Scholar] [CrossRef] [PubMed]
- de Cavanagh, E.M.; Inserra, F.; Ferder, L.; Romano, L.; Ercole, L.; Fraga, C.G. Superoxide dismutase and glutathione peroxidase activities are increased by enalapril and captopril in mouse liver. FEBS Lett. 1995, 361, 22–24. [Google Scholar] [CrossRef]
- de Cavanagh, E.M.; Inserra, F.; Ferder, L.; Fraga, C.G. Enalapril and captopril enhance glutathione-dependent antioxidant defenses in mouse tissues. Am. J. Physiol. Regul. Integr. Comp. Physiol. 2000, 278, 572–577. [Google Scholar] [CrossRef]
- Maiese, K.; Chong, Z.Z.; Hou, J.; Shang, Y.C. Oxidative stress: Biomarkers and novel therapeutic pathways. Exp. Gerontol. 2010, 45, 217–234. [Google Scholar] [CrossRef]
- Blagosklonny, M.V. From rapalogs to anti-aging formula. Oncotarget 2017, 8, 35492–35507. [Google Scholar] [CrossRef]
- Hwang, S.K.; Kim, H.H. The functions of mTOR in ischemic diseases. BMB Rep. 2011, 44, 506–511. [Google Scholar] [CrossRef]
- Humar, R.; Kiefer, F.N.; Berns, H.; Resink, T.J.; Battegay, E.J. Hypoxia enhances vascular cell proliferation and angiogenesis in vitro via rapamycin (mTOR)-dependent signaling. FASEB J. 2002, 16, 771–780. [Google Scholar] [CrossRef]
- Chong, Z.Z.; Shang, Y.C.; Maiese, K. Cardiovascular disease and mTOR signaling. Trends Cardiovasc. Med. 2011, 21, 151–155. [Google Scholar] [CrossRef]
- Chong, Z.Z.; Hou, J.; Shang, Y.C.; Wang, S.; Maiese, K. EPO relies upon novel signaling of Wnt1 that requires Akt1, FoxO3a, GSK-3β, and β-catenin to foster vascular integrity during experimental diabetes. Curr. Neurovasc. Res. 2011, 8, 103–120. [Google Scholar] [CrossRef]
- Dormond, O.; Madsen, J.C.; Briscoe, D.M. The effects of mTOR-Akt interactions on anti-apoptotic signaling in vascular endothelial cells. J. Biol. Chem. 2007, 282, 23679–23686. [Google Scholar] [CrossRef] [PubMed]
- Maiese, K.; Li, F.; Chong, Z.Z.; Shang, Y.C. The Wnt signaling pathway: Aging gracefully as a protectionist? Pharmacol. Ther. 2008, 118, 58–81. [Google Scholar] [CrossRef] [PubMed]
- Vigneron, F.; Dos Santos, P.; Lemoine, S.; Bonnet, M.; Tariosse, L.; Couffinhal, T.; Duplaà, C.; Jaspard-Vinassa, B. GSK-3β at the crossroads in the signalling of heart preconditioning: Implication of mTOR and Wnt pathways. Cardiovasc. Res. 2011, 90, 49–56. [Google Scholar] [CrossRef] [PubMed]
- Chen, C.; Liu, Y.; Zheng, P. mTOR regulation and therapeutic rejuvenation of aging hematopoietic stem cells. Sci. Signal. 2009, 2, 75. [Google Scholar] [CrossRef] [PubMed]
- Easley, C.A.; Ben-Yehudah, A.; Redinger, C.J.; Oliver, S.L.; Varum, S.T.; Eisinger, V.M.; Carlisle, D.L.; Donovan, P.J.; Schatten, G.P. mTOR-mediated activation of p70 S6K induces differentiation of pluripotent human embryonic stem cells. Cell Reprogram. 2010, 12, 263–273. [Google Scholar] [CrossRef]
- Das, J.; Ghosh, J.; Manna, P.; Sil, P.C. Taurine suppresses doxorubicin-triggered oxidative stress and cardiac apoptosis in rat via up-regulation of PI3-K/Akt and inhibition of p53, p38-JNK. Biochem. Pharmacol. 2011, 81, 891–909. [Google Scholar] [CrossRef]
- Gangloff, Y.G.; Mueller, M.; Dann, S.G.; Svoboda, P.; Sticker, M.; Spetz, J.F.; Um, S.H.; Brown, E.J.; Cereghini, S.; Thomas, G.; et al. Disruption of the mouse mTOR gene leads to early postimplantation lethality and prohibits embryonic stem cell development. Mol. Cell Biol. 2004, 24, 9508–9516. [Google Scholar] [CrossRef]
- Földes, G.; Mioulane, M.; Wright, J.S.; Liu, A.Q.; Novak, P.; Merkely, B.; Gorelik, J.; Schneider, M.D.; Ali, N.N.; Harding, S.E. Modulation of human embryonic stem cell-derived cardiomyocyte growth: A testbed for studying human cardiac hypertrophy? J. Mol. Cell. Cardiol. 2011, 50, 367–376. [Google Scholar] [CrossRef]
- Hernández, G.; Lal, H.; Fidalgo, M.; Guerrero, A.; Zalvide, J.; Force, T.; Pombo, C.M. A novel cardioprotective p38-MAPK/mTOR pathway. Exp. Cell Res. 2011, 317, 2938–2949. [Google Scholar] [CrossRef]
- Jaber, N.; Dou, Z.; Chen, J.S.; Catanzaro, J.; Jiang, Y.P.; Ballou, L.M.; Selinger, E.; Ouyang, X.; Lin, R.Z.; Zhang, J.; et al. Class III PI3K Vps34 plays an essential role in autophagy and in heart and liver function. Proc. Natl. Acad. Sci. USA 2012, 109, 2003–2008. [Google Scholar] [CrossRef]
- Lajoie, C.; El-Helou, V.; Proulx, C.; Clément, R.; Gosselin, H.; Calderone, A. Infarct size is increased in female post-MI rats treated with rapamycin. Can. J. Physiol. Pharmacol. 2009, 87, 460–470. [Google Scholar] [CrossRef] [PubMed]
- Zhang, D.; Contu, R.; Latronico, M.V.; Zhang, J.; Zhang, J.L.; Rizzi, R.; Catalucci, D.; Miyamoto, S.; Huang, K.; Ceci, M.; et al. MTORC1 regulates cardiac function and myocyte survival through 4E-BP1 inhibition in mice. J. Clin. Investig. 2010, 120, 2805–2816. [Google Scholar] [CrossRef] [PubMed]
- Lemaître, V.; Dabo, A.J.; D’Armiento, J. Cigarette smoke components induce matrix metalloproteinase-1 in aortic endothelial cells through inhibition of mTOR signaling. Toxicol. Sci. 2011, 123, 542–549. [Google Scholar] [CrossRef]
- Miriuka, S.G.; Rao, V.; Peterson, M.; Tumiati, L.; Delgado, D.H.; Mohan, R.; Ramzy, D.; Stewart, D.; Ross, H.J.; Waddell, T.K. mTOR inhibition induces endothelial progenitor cell death. Am. J. Transplant. 2006, 6, 2069–2079. [Google Scholar] [CrossRef]
- Leelahavanichkul, A.; Areepium, N.; Vadcharavivad, S.; Praditpornsilpa, K.; Avihingsanon, Y.; Karnjanabuchmd, T.; Eiam-Ong, S.; Tungsanga, K. Pharmacokinetics of sirolimus in Thai healthy volunteers. J. Med. Assoc. Thail. 2005, 88, 157–162. [Google Scholar]
- Singh, M.; Jensen, M.D.; Lerman, A.; Kushwaha, S.; Rihal, C.S.; Gersh, B.J.; Behfar, A.; Tchkonia, T.; Thomas, R.J.; Lennon, R.J.; et al. Effect of Low-Dose Rapamycin on Senescence Markers and Physical Functioning in Older Adults with Coronary Artery Disease: Results of a Pilot Study. J. Frailty Aging 2016, 5, 204–207. [Google Scholar] [CrossRef]
- Krebs, M.; Brunmair, B.; Brehm, A.; Artwohl, M.; Szendroedi, J.; Nowotny, P.; Roth, E.; Fürnsinn, C.; Promintzer, M.; Anderwald, C.; et al. The Mammalian target of rapamycin pathway regulates nutrient-sensitive glucose uptake in man. Diabetes 2007, 56, 1600–1607. [Google Scholar] [CrossRef]
- Stower, H. Senolytic CAR T cells. Nat. Med. 2020, 26, 1009. [Google Scholar] [CrossRef]
- Hajdu, K.L.; Bonamino, M.H. Senolytic chimeric antigen receptor (CAR) T cell: Driving the immune system to fight cell senescence. Immunol. Cell Biol. 2020, 98, 709–711. [Google Scholar] [CrossRef]
- Ravichandra, A.; Filliol, A.; Schwabe, R.F. CAR-T cells as senolytic and antifibrotic therapy. Hepatology 2020. [Google Scholar] [CrossRef]
- Li, J.H.; Chen, Y.Y. A Fresh Approach to Targeting Aging Cells: CAR-T Cells Enhance Senolytic Specificity. Cell Stem Cell 2020, 27, 192–194. [Google Scholar] [CrossRef]
- Amor, C.; Feucht, J.; Leibold, J.; Ho, Y.J.; Zhu, C.; Alonso-Curbelo, D.; Mansilla-Soto, J.; Boyer, J.A.; Li, X.; Giavridis, T.; et al. Senolytic CAR T cells reverse senescence-associated pathologies. Nature 2020, 583, 127–132. [Google Scholar] [CrossRef]
- Senolytic CAR T Cells Targeting uPAR Treat Lung Cancer in Mice. Cancer Discov. 2020, 10, 1093. [CrossRef]
- Childs, B.G.; Gluscevic, M.; Baker, D.J.; Laberge, R.M.; Marquess, D.; Dananberg, J.; van Deursen, J.M. Senescent cells: An emerging target for diseases of ageing. Nat. Rev. Drug Discov. 2017, 16, 718–735. [Google Scholar] [CrossRef]
- Aghajanian, H.; Kimura, T.; Rurik, J.G.; Hancock, A.S.; Leibowitz, M.S.; Li, L.; Scholler, J.; Monslow, J.; Lo, A.; Han, W.; et al. Targeting cardiac fibrosis with engineered T cells. Nature 2019, 573, 430–433. [Google Scholar] [CrossRef]
- Joseph, P.; Leong, D.; McKee, M.; Anand, S.S.; Schwalm, J.D.; Teo, K.; Mente, A.; Yusuf, S. Reducing the Global Burden of Cardiovascular Disease, Part 1: The Epidemiology and Risk Factors. Circ. Res. 2017, 121, 677–694. [Google Scholar] [CrossRef]
- Paneni, F.; Diaz Canestro, C.; Libby, P.; Luscher, T.F.; Camici, G.G. The Aging Cardiovascular System: Understanding It at the Cellular and Clinical Levels. J. Am. Coll. Cardiol. 2017, 69, 1952–1967. [Google Scholar] [CrossRef]
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).