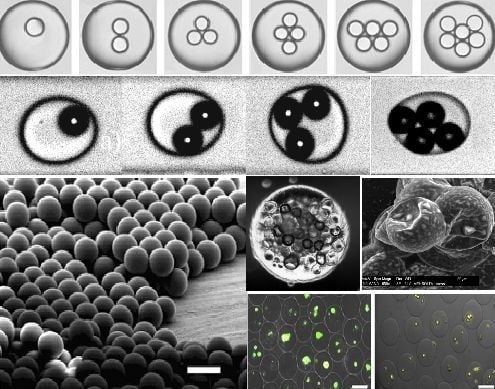
Microfluidic-Based Synthesis of Hydrogel Particles for Cell Microencapsulation and Cell-Based Drug Delivery
Abstract
:1. Introduction
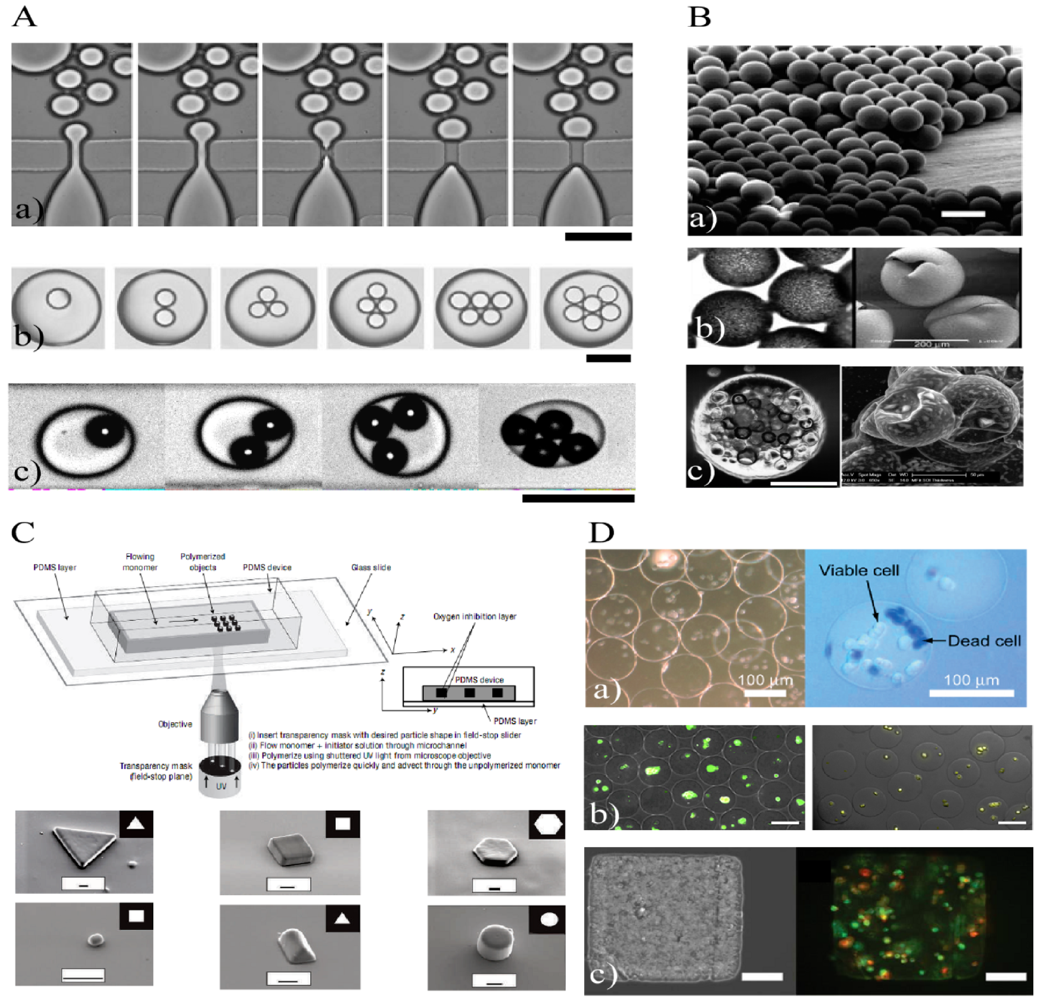
2. Natural and Synthetic Hydrogels
2.1. Introduction
2.2. Natural Hydrogel
2.2.1. Protein-Based Hydrogel
| Types of hydrogel material | Precursor and gelation mechanism | Crosslink method | Advantages for cell encapsulation | Disadvantages for cell encapsulation |
|---|---|---|---|---|
| Protein-based hydrogel | ||||
| Collagen | The precursor contains a characteristic triple helix structure; gel is formed by aggregation of the triple helix structures (microfibril) under chemical, physical, or enzymatic treatments | Using glutaraldehyde, water-soluble carbodiimide, UV irradiation, dehydrothermal, or enzymatic method to crosslink precursors | Collagen hydrogel offers direct cell-matrix interactions | Poor mechanical property |
| Gelatin | It is derived from collagen and is negatively or positively charged depending on the treatment method | Using glutaraldehyde, water-soluble carbodiimide, UV irradiation, dehydrothermal, or ionic interactions to crosslink precursors | Geltatin hydrogel also offers direct cell-matrix interactions | Soluble in water; the chemical or physical crosslinking is required to form stable gels |
| Fibrin | The precursor, fibrinogen, has three polypeptide chains (Aα, Bβ, and γ), which can self-associate or crosslink to form fibrin gels | Using thrombin, blood coagulation factor XIIIa, or genipin to crosslink fibrinogen | Fibrin offers a high seeding efficiency, a uniform cell distribution, and a distinct adhesion capability | Low mechanical stiffness |
| Elastin-like polypeptides(ELPs) | A repeating pentapeptide motif, Val-Pro-Gly-Xaa-Gly, is the characteristic of ELPs; gelation is achieved via a temperature -dependent phase transition of the polymer | Increase the temperature to be above its critical solution temperature | The critical solution temperature can be varied by changing the composition and distribution of the X residue and the molecular weight of ELPs. | Biosynthesis of ELPs is commonly needed |
| Polysaccharide-based hydrogel | ||||
| Alginate | (1-4)-linked β-L-guluronic (G block) and α-D-mannuronic acids (M block); gelation is achieved via ionic interactions between G blocks and divalent cations | Adding divalent cations, e.g., calcium ions, to an alginate solution | Gelation occurs rapidly under mild conditions | There is a diffusion issue associated with the gelation process |
| Hyaluronic acid (HA) | β-(1-4)-linked glucuronic acid and β-(1-3)-linked N-acetyl-D-glucos-amine; gelation is achieved by modifying chemically the functional groups on HA | Crosslink via thiol- modified HA, dihydrazide-modified HA, aldehyde-modified HA, or click reactions. | Biocompatible | Soluble in water; the chemical modification is required to form polymer gels |
| Chitosan | β-(1-4)-linked 2-acetamido-2-deoxy-β-D-glucopyranose and 2-amino-2-deoxy-β-D-glycopyranose; gel forms via ionic interactions or chemical modifications of the amine groups on chitosan | Ionic interactions between positively charged chitosan and negatively charged polyelectrolyte; chemically crosslink the amine groups | Chitosan is biocompatible and made from abundant renewable resources | The chemical modification may introduce toxicity to the polymer gel |
| Agarose | The precursor is a combination of several types of sugar residues; it forms gels by aggregating single or double helices at a decreased temperature | Decrease the temperature to its critical solution temperature | Biocompatible | The gelation temperature needs to be adjusted to be physiologically relevant |
| Poly(ethylene glycol) (PEG)-based hydrogel | ||||
| PEG | Poly(ethylene glycol) diacrylate (PEG-DA); the radical polymerization | Crosslink by expose PEG-DA solutions to a UV irradiation | Bioinert, well-tuned structure-function relations; convenient incorporation of bioactive and biodegradable groups; suitable for micro fabrication | Incorporation of bioactive and biodegradable groups is necessary; radicals and heavy metal ions for polymerization may induce cytotoxicity |
| PEG with acrylate and thiol end groups; the Michael addition reaction | Crosslink by mixing the solution of PEG with acrylate groups with the solution of PEG with thiol end groups at the room temperature | |||
| PEG with azide and alkyne end groups; the click chemistry | Crosslink by mixing the solution of PEG with azide groups with the solution of PEG with alkyne end groups in the presence of Cu 2+ | |||
2.2.2. Polysaccharide-Based Hydrogel
2.3. Synthetic Hydrogel
3. Microfluidic-Based Synthesis of Hydrogel Particles for Cell Microencapsulation
3.1. Microfluidic-Controlled Encapsulation of Cells in Emulsion Droplets
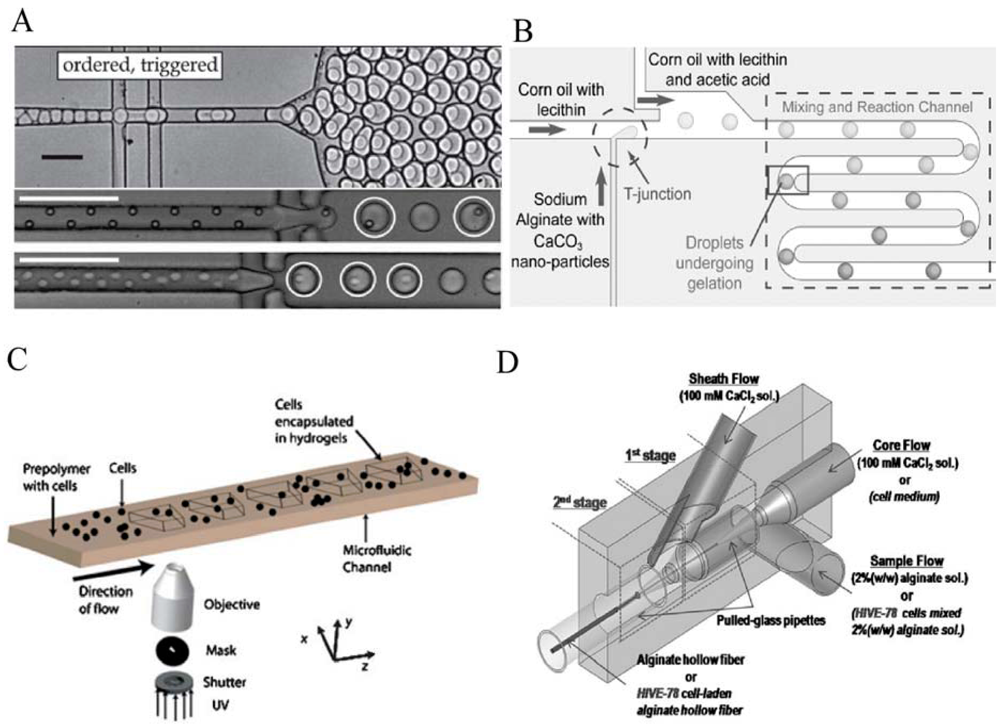
3.2. Synthesis of Hydrogel Particles Using Microdroplets as Templates
3.3. Synthesis of Hydrogel Particles Using the Stop-Flow Lithography
4. Microfluidic-Based Synthesis of Hydrogel Fibers for Cell Microencapsulation
5. Applications of Encapsulated Cells in Hydrogel for Cancer Therapy
6. Conclusion and Outlook
Acknowledgments
References
- Williams, D.F. On the nature of biomaterials. Biomaterials 2009, 30, 5897–5909. [Google Scholar]
- Orive, G.; Hernandez, R.M.; Rodriguez Gascon, A.; Calafiore, R.; Chang, T.M.S.; de Vos, P.; Hortelano, G.; Hunkeler, D.; Lacik, I.; Pedraz, J.L. History, challenges and perspectives of cell microencapsulation. Trends Biotechnol. 2004, 22, 87–92. [Google Scholar]
- Orive, G.; Hernandez, R.M.; Murua, A.; Pedraz, J.L. Recent advances in the use of encapsulated cells for effective delivery of therapeutics. Ther. Deliv. 2010, 1, 387–396. [Google Scholar]
- Orive, G.; Gascon, A.R.; Hernandez, R.M.; Igartua, M.; Luis Pedraz, J. Cell microencapsulation technology for biomedical purposes: novel insights and challenges. Trends Pharmacol. Sci. 2003, 24, 207–210. [Google Scholar]
- Hernandez, R.M.; Orive, G.; Murua, A.; Pedraz, J.L. Microcapsules and microcarriers for in situ cell delivery. Adv. Drug Deliv. Rev. 2010, 62, 711–730. [Google Scholar]
- Murua, A.; Portero, A.; Orive, G.; Hernandez, R.M.; de Castro, M.; Pedraz, J.L. Cell microencapsulation technology: Towards clinical application. J. Control. Release 2008, 132, 76–83. [Google Scholar]
- Sakai, S.M.; Mu, C.; Kawabata, K.; Hashimoto, I.; Kawakami, K. Biocompatibility of subsieve-size capsules versus conventiona l-size microcapsules. J. Biomed. Mater. Res. 2006, 78, 394–398. [Google Scholar]
- Sugiura, S.; Oda, T.; Izumida, Y.; Aoyagi, Y.; Satake, M.; Ochiai, A.; Ohkohchi, N.; Nakajima, M. Size control of calcium alginate beads containing living cells using micro-nozzle array. Biomaterials 2005, 26, 3327–3331. [Google Scholar]
- Christopher, G.F.; Anna, S.L. Microfluidic methods for generating continuous droplet streams. J. Phys. D: Appl. Phys. 2007, 40, R319–R336. [Google Scholar] [CrossRef]
- Chu, L.-Y.; Utada, A.S.; Shah, R.K.; Kim, J.W.; Weitz, D.A. Controllable monodisperse multiple emulsions. Angew. Chem. Int. Ed. 2007, 46, 8970–8974. [Google Scholar]
- Shui, L.; Eijkel, J.C.T.; van den Berg, A. Multiphase flow in microfluidic systems—Control and applications of droplets and interfaces. Adv. Colloid Interface Sci. 2007, 133, 35–49. [Google Scholar]
- Anna, S.L.; Bontoux, N.; Stone, H.A. Formation of dispersions using “flow focusing” in microchannels. Appl. Phys. Lett. 2003, 82, 364–366. [Google Scholar]
- Wan, J.; Bick, A.; Sullivan, M.; Stone, H.A. Controllable microfluidic production of microbubbles in water-in-oil emulsions and the formation of porous microparticles. Adv. Mater. 2008, 20, 3314–3318. [Google Scholar]
- Ziemecka, I.; van Steijn, V.; Koper, G.J.M.; Rosso, M.; Brizard, A.M.; van Esch, J.H.; Kreutzer, M.T. Monodisperse hydrogel microspheres by forced droplet formation in aqueous two-phase systems. Lab on a Chip 2011, 11, 620–624. [Google Scholar]
- Zhang, H.; Tumarkin, E.; Peerani, R.; Nie, Z.; Sullan, R.M.A.; Walker, G.C.; Kumacheva, E. Microfluidic production of biopolymer microcapsules with controlled morphology. J. Am. Chem. Soc. 2006, 128, 12205–12210. [Google Scholar]
- Hung, L.H.; Teh, S.Y.; Jester, J.; Lee, A.P. PLGA micro/nanosphere synthesis by droplet microfluidic solvent evaporation and extraction approaches. Lab Chip 2010, 10, 1820–1825. [Google Scholar]
- Tumarkin, E.; Kumacheva, E. Microfluidic generation of microgels from synthetic and natural polymers. Chem. Soci. Rev. 2009, 38, 2161–2168. [Google Scholar]
- Park, J.I.; Saffari, A.; Kumar, S.; Gunther, A.; Kumacheva, E. Microfluidic synthesis of polymer and inorganic particulate materials. Annu. Rev. Mater. Res. 2010, 40, 415–443. [Google Scholar]
- Utada, A.S.; Lorenceau, E.; Link, D.R.; Kaplan, P.D.; Stone, H.A.; Weitz, D.A. Monodisperse double emulsions generated from a microcapillary device. Science 2005, 308, 537–541. [Google Scholar]
- Wan, J.; Stone, H.A. Coated gas bubbles for the continuous synthesis of hollow inorganic particles. Langmuir 2012, 28, 37–41. [Google Scholar]
- Seo, M.; Nie, Z.; Xu, S.; Mok, M.; Lewis, P.C.; Graham, R.; Kumacheva, E. Continuous microfluidic reactors for polymer particles. Langmuir 2005, 21, 11614–11622. [Google Scholar]
- Suh, S.K.; Bong, K.W.; Hatton, T.A.; Doyle, P.S. Using stop-flow lithography to produce opaque microparticles: Synthesis and modeling. Langmuir 2011, 27, 13813–13819. [Google Scholar]
- Hwang, D.K.; Oakey, J.; Toner, M.; Arthur, J.A.; Anseth, K.S.; Lee, S.; Zeiger, A.; van Vliet, K.J.; Doyle, P.S. Stop-flow lithography for the production of shape-evolving degradable microgel particles. J. Am. Chem. Soc. 2009, 131, 4499–4504. [Google Scholar]
- Hwang Dae, K.; Dendukuri, D.; Doyle Patrick, S. Microfluidic-based synthesis of non-spherical magnetic hydrogel microparticles. Lab Chip 2008, 8, 1640–1647. [Google Scholar]
- Dendukuri, D.; Pregibon, D.C.; Collins, J.; Hatton, T.A.; Doyle, P.S. Continuous-flow lithography for high-throughput microparticle synthesis. Nat. Mater. 2006, 5, 365–369. [Google Scholar]
- Panda, P.; Ali, S.; Lo, E.; Chung, B.G.; Hatton, T.A.; Khademhosseini, A.; Doyle, P.S. Stop-flow lithography to generate cell-laden microgel particles. Lab Chip 2008, 8, 1056–1061. [Google Scholar]
- Kumachev, A.; Greener, J.; Tumarkin, E.; Eiser, E.; Zandstra, P.W.; Kumacheva, E. High-throughput generation of hydrogel microbeads with varying elasticity for cell encapsulation. Biomaterials 2011, 32, 1477–1483. [Google Scholar]
- Tan, W.-H.; Takeuchi, S. Monodisperse alginate hydrogel microbeads for cell encapsulation. Adv. Mater. 2007, 19, 2696–2701. [Google Scholar]
- Edd, J.F.; Di Carlo, D.; Humphry, K.J.; Koster, S.; Irimia, D.; Weitz, D.A.; Toner, M. Controlled encapsulation of single-cells into monodisperse picolitre drops. Lab Chip 2008, 8, 1262–1264. [Google Scholar]
- Balakrishnan, B.; Banerjee, R. Biopolymer-based hydrogels for cartilage tissue engineering. Chem. Rev. 2011, 111, 4453–4474. [Google Scholar]
- Zimmermann, H.; Ehrhart, F.; Zimmermann, D.; Mueller, K.; Katsen-Globa, A.; Behringer, M.; Feilen, P.J.; Gessner, P.; Zimmermann, G.; Shirley, S.G.; Weber, M.M.; Metze, J.; Zimmermann, U. Hydrogel-based encapsulation of biological, functional tissue: fundamentals, technologies and applications. Appl. Phys. A Mater. Sci. Process. 2007, 89, 909–922. [Google Scholar]
- Lee, K.Y.; Mooney, D.J. Hydrogels for tissue engineering. Chem. Rev. 2001, 101, 1869–1879. [Google Scholar]
- Alberts, B.; Johnson, A.; Lewis, J.; Raff, M.; Roberts, K.; Walter, P. Molecular Biology of The Cell; Garland Science: New York, NY, USA, 2002. [Google Scholar]
- Parenteau-Bareil, R.; Gauvin, R.; Berthod, F. Collagen-based biomaterials for tissue engineering applications. Materials 2010, 3, 1863–1887. [Google Scholar]
- Smethurst, P.A.; Onley, D.J.; Jarvis, G.E.; O’Connor, M.N.; Knight, C.G.; Herr, A.B.; Ouwehand, W.H.; Farndale, R.W. Structural Basis for the platelet-collagen interaction: The smallest motif within collagen that recognized and activates platelet glycoprotein VI contains two glycine-proline-hydroxyproline triplets. J. Biol. Chem. 2007, 282, 1296–1304. [Google Scholar]
- Wu, X.; Black, L.; Santacana-Laffitte, G.; Patrick, C.W., Jr. Preparation and assessment of glutaraldehyde-crosslinked collagen-chitosan hydrogels for adipose tissue engineering. J. Biomed. Mater. Res. A 2007, 81A, 59–65. [Google Scholar]
- Weadock, K.S.; Miller, E.J.; Bellincampi, L.D.; Zawadsky, J.P.; Dunn, M.D. Physical crosslinking of collagen fibers: Comparison of ultraviolet irradiation and dehydrothermal treatment. J. Biomed. Mater. Res. 1995, 29, 1373–1379. [Google Scholar]
- Garcia, Y.; Hemantkumar, N.; Collighan, R.; Griffin, M.; Rodriguez-Cabello, J.C.; Pandit, A. In vitro characterization of a collagen scaffold enzymatically cross-linked with a tailored elastin-like polymer. Tissue Eng. A 2009, 15, 887–899. [Google Scholar]
- Tabata, Y.; Ikada, Y. Protein release from gelatin matrixes. Adv. Drug Deliv. Rev. 1998, 31, 287–301. [Google Scholar]
- Weiner, A.A.; Moore, M.C.; Walker, A.H.; Shastri, V.P. Modulation of protein release from photocrosslinked networks by gelatin microparticles. Int. J. Pharm. 2008, 360, 107–114. [Google Scholar]
- Young, S.; Wong, M.; Tabata, Y.; Mikos, A.G. Gelatin as a delivery vehicle for the controlled release of bioactive molecules. J. Control. Release 2005, 109, 256–274. [Google Scholar]
- Mosesson, M.W. Fibrinogen and fibrin structure and functions. J. Thromb.Haemost. 2005, 3, 1894–1904. [Google Scholar]
- Mosesson, M.W.; Siebenlist, K.R.; Meh, D.A. The structure and biological features of fibrinogen and fibrin. Ann. NY Acad. Sci. 2001, 936, 11–30. [Google Scholar]
- Schense, J.C.; Hubbell, J.A. Crosslinking exogenous bifunctional peptides into fibrin gels with factor XIIIa. Bioconjugate Chem. 1999, 10, 75–81. [Google Scholar]
- Ahmed, T.A.E.; Dare, E.V.; Hincke, M. Fibrin: A versatile scaffold for tissue engineering applications. Tissue Eng. B Rev. 2008, 14, 199–215. [Google Scholar]
- Sandberg, L.B.; Soskel, N.T.; Leslie, J.G. Elastin structure, biosynthesis, and relation to disease states. New Eng. J. Med. 1981, 304, 566–579. [Google Scholar]
- Urry, D.W. Physical chemistry of biological free energy transduction as demonstrated by elastic protein-based polymers. J. Phys. Chem. B 1997, 101, 11007–11028. [Google Scholar]
- Meyer, D.E.; Chilkoti, A. Purification of recombinant proteins by fusion with thermally-responsive polypeptides. Nat. Biotech. 1999, 17, 1112–1115. [Google Scholar]
- MacEwan, S.R.; Chilkoti, A. Elastin-like polypeptides: Biomedical applications of tunable biopolymers. Biopolymers 2010, 94, 60–77. [Google Scholar]
- Nettles, D.L.; Chilkoti, A.; Setton, L.A. Applications of elastin-like polypeptides in tissue engineering. Adv. Drug Deliv. Rev. 2010, 62, 1479–1485. [Google Scholar]
- Dusseault, J.; Halle, J.P. Alginate hydrogels for cell microencapsulation and immunoprotection. In Recent Advances in Biomaterials Research; Research Signpost: Kerala, India, 2008; pp. 23–42. [Google Scholar]
- Thu, B.; Bruheim, P.; Espevik, T.; Smidsroed, O.; Soon-Shiong, P.; Skjak-Braek, G. Alginate polycation microcapsules. I. Interaction between alginate and polycation. Biomaterials 1996, 17, 1031–1040. [Google Scholar]
- Santos, E.; Zarate, J.; Orive, G.; Hernandez, R.M.; Pedraz, J.L. Biomaterials in cell microencapsulation. Adv. Exp. Med. Biol. 2010, 670, 5–21. [Google Scholar]
- Toole, B.P. Hyaluronan: from extracellular glue to pericellular cue. Nat. Rev. Cancer 2004, 4, 528–539. [Google Scholar]
- Toole, B.P. Biological roles of hyaluronan. Carbohydr. Chem. Biol. 2000, 4, 685–699. [Google Scholar]
- Burdick, J.A.; Prestwich, G.D. Hyaluronic Acid Hydrogels for Biomedical Applications. Adv. Mater. 2011, 23, H41–H56. [Google Scholar]
- Sahoo, D.; Nayak, P.L. Chitosan: The most valuable derivative of chitin. In Biopolymers: Biomedical and Environmental Applications; Kalia, S., Avérous, L., Eds.; John Wiley & Sons, Inc.: Hoboken, NJ, USA, 2011; pp. 129–166. [Google Scholar]
- Il'ina, A.V.; Varlamov, V.P. Chitosan-based polyelectrolyte complexes: A review. Appl. Biochem. Microbiol. 2005, 41, 5–11. [Google Scholar]
- Wu, Z.M.; Zhang, X.G.; Zheng, C.; Li, C.X.; Zhang, S.M.; Dong, R.N.; Yu, D.M. Disulfide-crosslinked chitosan hydrogel for cell viability and controlled protein release. Eur. J. Pharm. Sci. 2009, 37, 198–206. [Google Scholar]
- Berger, J.; Reist, M.; Mayer, J.M.; Felt, O.; Peppas, N.A.; Gurny, R. Structure and interactions in covalently and ionically crosslinked chitosan hydrogels for biomedical applications. Eur. J. Pharm. Biopharm. 2004, 57, 19–34. [Google Scholar]
- Bhattarai, N.; Gunn, J.; Zhang, M. Chitosan-based hydrogels for controlled, localized drug delivery. Adv. Drug Deliv. Rev. 2010, 62, 83–99. [Google Scholar]
- Dash, M.; Chiellini, F.; Ottenbrite, R.M.; Chiellini, E. Chitosan—A versatile semi-synthetic polymer in biomedical applications. Prog. Polym. Sci. 2011, 36, 98–1014. [Google Scholar]
- Lahaye, M. Developments on gelling algal galactans, their structure and physico-chemistry. J. Appl. Phycol. 2001, 13, 17–184. [Google Scholar]
- Borkenhagen, M.; Clemence, J.F.; Sigrist, H.; Aebischer, P. Three-dimensional extracellular matrix engineering in the nervous system. J. Biomed. Mater. Res. 1998, 40, 392–400. [Google Scholar]
- Zhang, J.; Tokatlian, T.; Zhong, J.; Ng, Q.K.T.; Patterson, M.; Lowry, W.E.; Carmichael, S.T.; Segura, T. Physically associated synthetic hydrogels with long-term covalent stabilization for cell culture and stem cell transplantation. Adv. Mater. 2011, 23, 5098–5103. [Google Scholar]
- Krishna, O.D.; Kiick, K.L. Protein- and peptide-modified synthetic polymeric biomaterials. Biopolymers 2010, 94, 32–48. [Google Scholar]
- Sionkowska, A. Current research on the blends of natural and synthetic polymers as new biomaterials: Review. Prog. Polym. Sci. 2011, 36, 1254–1276. [Google Scholar]
- Hern, D.L.; Hubbell, J.A. Incorporation of adhesion peptides into nonadhesive hydrogels useful for tissue resurfacing. J. Biomed. Mater. Res. 1998, 39, 266–276. [Google Scholar]
- Nuttelman, C.R.; Rice, M.A.; Rydholm, A.E.; Salinas, C.N.; Shah, D.N.; Anseth, K.S. Macromolecular monomers for the synthesis of hydrogel niches and their application in cell encapsulation and tissue engineering. Prog. Polym. Sci. 2008, 33, 167–179. [Google Scholar]
- Trongsatitkul, T.; Budhlall, B.M. Multicore-shell PNIPAm-co-PEGMa microcapsules for cell encapsulation. Langmuir 2011, 27, 13468–13480. [Google Scholar]
- Yu, L.; Ding, J. Injectable hydrogels as unique biomedical materials. Chem. Soc. Rev. 2008, 37, 1473–1481. [Google Scholar]
- Nicodemus, G.D.; Bryant, S.J. Cell encapsulation in biodegradable hydrogels for tissue engineering applications. Tissue Eng. B Rev. 2008, 14, 149–165. [Google Scholar]
- Lin, C.C.; Anseth, K.S. PEG hydrogels for the controlled release of biomolecules in regenerative medicine. Pharm. Res. 2009, 26, 631–643. [Google Scholar]
- Zguris, J.C.; Itle, L.J.; Koh, W.G.; Pishko, M.V. A novel single-step fabrication technique to create heterogeneous poly(ethylene glycol) hydrogel microstructures containing multiple phenotypes of mammalian cells. Langmuir 2005, 21, 4168–4174. [Google Scholar]
- Liu, J.; Gao, D.; Li, H.-F.; Lin, J.-M. Controlled photopolymerization of hydrogel microstructures inside microchannels for bioassays. Lab Chip 2009, 9, 1301–1305. [Google Scholar]
- Liu, S.Q.; Tay, R.; Khan, M.; Ee, P.L.R.; Hedrick, J.L.; Yang, Y.Y. Synthetic hydrogels for controlled stem cell differentiation. Soft Matter 2010, 6, 67–81. [Google Scholar]
- Rydholm, A.E.; Bowman, C.N.; Anseth, K.S. Degradable thiol-acrylate photopolymers: Polymerization and degradation behavior of an in situ forming biomaterial. Biomaterials 2005, 26, 4495–4506. [Google Scholar]
- Murua, A.; de Castro, M.; Orive, G.; Hernandez, R.M.; Pedraz, J.L. In vitro characterization and in vivo functionality of erythropoietin-secreting cells immobilized in alginate-poly-L-lysine-alginate microcapsules. Biomacromolecules 2007, 8, 3302–3307. [Google Scholar]
- Kobayashi, T.; Aomatsu, Y.; Kanehiro, H.; Hisanaga, M.; Nakajima, Y. Protection of NOD islet isograft from autoimmune destruction by agarose microencapsulation. Transplant. Proc. 2003, 35, 484–485. [Google Scholar]
- Khademhosseini, A.; May, M.H.; Sefton, M.V. Conformal coating of mammalian cells immobilized onto magnetically driven beads. Tissue Eng. 2006, 11, 1797–1806. [Google Scholar]
- Schaffellner, S.; Stadlbauer, V.; Stiegler, P.; Hauser, O.; Halwachs, G.; Lackner, C.; Iberer, F.; Tscheliessnigg, K.H. Porcine islet cells microencapsulated in sodium cellulose sulfate. Transplant. Proc. 2005, 37, 248–252. [Google Scholar]
- Abate, A.R.; Chen, C.-H.; Agresti, J.J.; Weitz, D.A. Beating Poisson encapsulation statistics using close-packed ordering. Lab Chip 2009, 9, 2628–2631. [Google Scholar]
- Xu, S.; Nie, Z.; Seo, M.; Lewis, P.; Kumacheva, E.; Stone, H.A.; Garstecki, P.; Weibel, D.B.; Gitlin, I.; Whitesides, G.W. Generation of monodisperse particles by using microfluidics: Control over size, shape, and composition. Angew. Chem. Int. Ed. 2005, 44, 724–728. [Google Scholar]
- Shepherd, R.F.; Conrad, J.C.; Rhodes, S.K.; Link, D.R.; Marquez, M.; Weitz, D.A.; Lewis, J.A. Microfluidic assembly of homogeneous and janus colloid-filled hydrogel granules. Langmuir 2006, 22, 8618–8622. [Google Scholar]
- Orive, G.; De Castro, M.; Kong, H.J.; Hernandez, R.M.; Ponce, S.; Mooney, D.J.; Pedraz, J.L. Bioactive cell-hydrogel microcapsules for cell-based drug delivery. J. Control. Release 2009, 135, 203–210. [Google Scholar]
- Li, L.; Davidovich, A.E.; Schloss, J.M.; Chippada, U.; Schloss, R.R.; Langrana, N.A.; Yarmush, M.L. Neural lineage differentiation of embryonic stem cells within alginate microbeads. Biomaterials 2011, 32, 4489–4497. [Google Scholar]
- Hoesli, C.A.; Raghuram, K.; Kiang, R.L.J.; Mocinecova, D.; Hu, X.; Johnson, J.D.; Lacik, I.; Kieffer, T.J.; Piret, J.M. Pancreatic cell immobilization in alginate beads produced by emulsion and internal gelation. Biotechnol. Bioeng. 2010, 108, 424–434. [Google Scholar]
- Seifert, D.B.; Phillips, J.A. Production of Small, Monodispersed alginate beads for cell immobilization. Biotechnol. Prog. 1997, 13, 562–568. [Google Scholar]
- Zimmermann, H.; Shirley, S.G.; Zimmermann, U. Alginate-based encapsulation of cells: Past, present, and future. Curr. Diabetes Rep. 2007, 7, 314–320. [Google Scholar]
- Chan, L.W.; Lee, H.Y.; Heng, P.W.S. Mechanisms of external and internal gelation and their impact on the functions of alginate as a coat and delivery system. Carbohydr. Polym. 2006, 63, 176–187. [Google Scholar]
- Chan, L.W.; Lee, H.Y.; Heng, P.W.S. Production of alginate microspheres by internal gelation using an emulsification method. Int. J. Pharm. 2002, 242, 259–262. [Google Scholar]
- Chan, E.-S.; Lim, T.-K.; Ravindra, P.; Mansa, R.F.; Islam, A. The effect of low air-to-liquid mass flow rate ratios on the size, size distribution and shape of calcium alginate particles produced using the atomization method. J. Food Eng. 2011, 108, 297–303. [Google Scholar]
- Fundueanu, G.; Nastruzzi, C.; Carpov, A.; Desbrieres, J.; Rinaudo, M. Physico-chemical characterization of Ca-alginate microparticles produced with different methods. Biomaterials 1999, 20, 1427–1435. [Google Scholar]
- Chan, E.-S.; Lee, B.-B.; Ravindra, P.; Poncelet, D. Prediction models for shape and size of ca-alginate macrobeads produced through extrusion-dripping method. J. Colloid Interface Sci. 2009, 338, 63–72. [Google Scholar]
- Choi, C.H.; Lee, J.H.; Shim, H.W.; Lee, N.R.; Jung, J.H.; Yoon, T.H.; Kim, D.P.; Lee, C.S. Encapsulation of cell into monodispersed hydrogels on microfluidic device. Proc. SPIE-Int. Soc. Opt. Eng. 2007, 6416, 641613. [Google Scholar]
- Zhao, L.B.; Pan, L.; Zhang, K.; Guo, S.S.; Liu, W.; Wang, Y.; Chen, Y.; Zhao, X.Z.; Chan, H.L.W. Generation of Janus alginate hydrogel particles with magnetic anisotropy for cell encapsulation. Lab Chip 2009, 9, 2981–2986. [Google Scholar]
- Liu, K.; Ding, H.J.; Liu, J.; Chen, Y.; Zhao, X.Z. Shape-Controlled Production of Biodegradable Calcium Alginate Gel Microparticles Using a Novel Microfluidic Device. Langmuir 2006, 22, 9468–9472. [Google Scholar]
- Neel, E.A.A.; Young, A.M.; Nazhat, S.N.; Knowles, J.C. A facile synthesis route to prepare microtubes from phosphate glass fibres. Adv. Mater. 2007, 19, 2856–2862. [Google Scholar]
- Hwang, C.M.; Khademhosseini, A.; Park, Y.; Sun, K.; Lee, S.H. Microfluidic chip-based fabrication of plga microfiber scaffolds for tissue engineering. Langmuir 2008, 24, 6845–6851. [Google Scholar]
- Lee, B.R.; Lee, K.H.; Kang, E.; Kim, D.S.; Lee, S.H. Microfluidic wet spinning of chitosan-alginate microfibers and encapsulation of HepG2 cells in fibers. Biomicrofluidics 2011, 5, 022208: 1–022208: 9. [Google Scholar]
- D'Alessandro, D.; Battolla, B.; Trombi, L.; Barachini, S.; Cascone, M.G.; Bernardini, N.; Petrini, M.; Mattii, L. Embedding methods for poly(-lactic acid) microfiber mesh/human mesenchymal stem cell constructs. Micron 2009, 40, 605–611. [Google Scholar]
- Lee, K.H.; Shin, S.J.; Park, Y.; Lee, S.H. Synthesis of cell-laden alginate hollow fibers using microfluidic chips and microvascularized tissue-engineering applications. Small 2009, 5, 1264–1268. [Google Scholar]
- Kidoaki, S.; Kwon Il, K.; Matsuda, T. Mesoscopic spatial designs of nano- and microfiber meshes for tissue-engineering matrix and scaffold based on newly devised multilayering and mixing electrospinning techniques. Biomaterials 2005, 26, 37–46. [Google Scholar]
- Hu, M.; Deng, R.; Schumacher, K.M.; Kurisawa, M.; Ye, H.; Purnamawati, K.; Ying, J.Y. Hydrodynamic spinning of hydrogel fibers. Biomaterials 2010, 31, 863–869. [Google Scholar]
- Gupta, B.; Revagade, N.; Hilborn, J. Poly(lactic acid) fiber: An overview. Prog. Polym. Sci. 2007, 32, 455–482. [Google Scholar]
- Chung, B.G.; Lee, K.H.; Khademhosseini, A.; Lee, S.H. Microfluidic fabrication of microengineered hydrogels and their application in tissue engineering. Lab Chip 2012, 12, 45–59. [Google Scholar]
- Shin, S.J.; Park, J.Y.; Lee, J.Y.; Park, H.; Park, Y.D.; Lee, K.B.; Whang, C.M.; Lee, S.H. “On the fly” continuous generation of alginate fibers using a microfluidic device. Langmuir 2007, 23, 9104–9108. [Google Scholar]
- Lee, K.H.; Shin, S.J.; Kim, C.B.; Kim, J.K.; Cho, Y.W.; Chung, B.G.; Lee, S.H. Microfluidic synthesis of pure chitosan microfibers for bio-artificial liver chip. Lab Chip 2010, 10, 1328–1334. [Google Scholar]
- Jung, J.H.; Choi, C.H.; Chung, S.; Chung, Y.M.; Lee, C.S. Microfluidic synthesis of a cell adhesive Janus polyurethane microfiber. Lab Chip 2009, 9, 2596–2602. [Google Scholar]
- Asthana, A.; Lee, K.H.; Shin, S.J.; Perumal, J.; Butler, L.; Lee, S.H.; Kim, D.P. Bromo-oxidation reaction in enzyme-entrapped alginate hollow microfibers. Biomicrofluidics 2011, 5, 024117: 1–024117: 11. [Google Scholar]
- Sugiura, S.; Oda, T.; Aoyagi, Y.; Satake, M.; Ohkohchi, N.; Nakajima, M. Tubular gel fabrication and cell encapsulation in laminar flow stream formed by microfabricated nozzle array. Lab Chip 2008, 8, 1255–1257. [Google Scholar]
- Takei, T.; Kishihara, N.; Sakai, S.; Kawakami, K. Novel technique to control inner and outer diameter of calcium-alginate hydrogel hollow microfibers, and immobilization of mammalian cells. Biochem. Eng. J. 2010, 49, 143–147. [Google Scholar]
- Elliott, R.B.; Escobar, L.; Calafiore, R.; Basta, G.; Garkavenko, O.; Vasconcellos, A.; Bambra, C. Transplantation of micro- and macroencapsulated piglet islets into mice and monkeys. Transplant. Proc. 2005, 37, 466–469. [Google Scholar]
- Zilberman, Y.; Turgeman, G.; Pelled, G.; Xu, N.; Moutsatsos, I.K.; Hortelano, G.; Gazit, D. Polymer-encapsulated engineered adult mesenchymal stem cells secrete exogenously regulated rhBMP-2, and induce osteogenic and angiogenic tissue formation. Polym. Adv. Technol. 2002, 13, 863–870. [Google Scholar]
- Sabel Michael, S.; Arora, A.; Su, G.; Mathiowitz, E.; Reineke Joshua, J.; Chang Alfred, E. Synergistic effect of intratumoral IL-12 and TNF-alpha microspheres: systemic anti-tumor immunity is mediated by both CD8+ CTL and NK cells. Surgery 2007, 142, 749–760. [Google Scholar]
- Paul, A.; Ge, Y.; Prakash, S.; Shum-Tim, D. Microencapsulated stem cells for tissue repairing: Implications in cell-based myocardial therapy. Regen. Med. 2009, 4, 733–745. [Google Scholar]
- Borlongan Cesario, V.; Skinner Steve, J.M.; Geaney, M.; Vasconcellos Alfred, V.; Elliott Robert, B.; Emerich Dwaine, F. Neuroprotection by encapsulated choroid plexus in a rodent model of Huntington's disease. Neuroreport 2004, 15, 2521–2525. [Google Scholar]
- Salmons, B.; Gunzburg, W.H. Therapeutic application of cell microencapsulation in cancer. Adv. Exp. Med. Biol. 2010, 670, 92–103. [Google Scholar]
- Loehr, J.M.; Heuchel, R.; Jesnowski, R.; Wallrapp, C. Therapy with cell encapsulation for substitution of organ function and tumor treatment. Adv. Biomater. 2009, B129–B135. [Google Scholar]
- Schwenter, F.; Zarei, S.; Luy, P.; Padrun, V.; Bouche, N.; Lee, J.S.; Mulligan, R.C.; Morel, P.; Mach, N. Cell encapsulation technology as a novel strategy for human anti-tumor immunotherapy. Cancer Gene Ther. 2011, 18, 553–562. [Google Scholar]
- Visted, T.; Furmanek, T.; Sakariassen, P.; Foegler, W.B.; Sim, K.; Westphal, H.; Bjerkvig, R.; Lund-Johansen, M. Prospects for delivery of recombinant Angiostatin by cell-encapsulation therapy. Human Gene Ther. 2003, 14, 1429–1440. [Google Scholar]
- Cirone, P.; Bourgeois, J.M.; Shen, F.; Chang, P.L. Combined immunotherapy and antiangiogenic therapy of cancer with microencapsulated cells. Human Gene Ther. 2004, 15, 945–959. [Google Scholar]
- Lohr, M.; Muller, P.; Karle, P.; Stange, J.; Mitzner, S.; Jesnowski, R.; Nizze, H.; Nebe, B.; Liebe, S.; Salmons, B.; Gunzburg, W.H. Targeted chemotherapy by intratumour injection of encapsulated cells engineered to produce CYP2B1, an ifosfamide activating cytochrome P450. Gene Ther. 1998, 5, 1070–1078. [Google Scholar]
- Karle, P.; Muller, P.; Renz, R.; Jesnowski, R.; Saller, R.; Von Rombs, K.; Nizze, H.; Liebe, S.; Gunzburg, W.H.; Salmons, B.; Lohr, M. Intratumoral injection of encapsulated cells producing an oxazaphosphorine activating cytochrome P450 for targeted chemotherapy. Adv. Exp. Med. Biol. 1998, 451, 97–106. [Google Scholar]
- Lohr, M.; Bago, Z.T.; Bergmeister, H.; Ceijna, M.; Freund, M.; Gelbmann, W.; Gunzburg, W.H.; Jesnowski, R.; Hain, J.; Hauenstein, K.; Henninger, W.; Hoffmeyer, A.; Karle, P.; Kroger, J.C.; Kundt, G.; Liebe, S.; Losert, U.; Muller, P.; Probst, A.; Puschel, K.; Renner, M.; Renz, R.; Saller, R.; Salmons, B.; Schuh, M.; Schwendenwein, I.; Von Rombs, K.; Wagner, T.; Walter, I. Cell therapy using microencapsulated 293 cells transfected with a gene construct expressing CYP2B1, an ifosfamide converting enzyme, instilled intra-arterially in patients with advanced-stage pancreatic carcinoma: A phase I/II study. J. Mol. Med. 1999, 77, 393–398. [Google Scholar]
- Kauer, T.M.; Figueiredo, J.-L.; Hingtgen, S.; Shah, K. Encapsulated therapeutic stem cells implanted in the tumor resection cavity induce cell death in gliomas. Nat. Neurosci. 2012, 15, 197–204. [Google Scholar]
- Goren, A.; Dahan, N.; Goren, E.; Baruch, L.; Machluf, M. Encapsulated human mesenchymal stem cells: A unique hypoimmunogenic platform for long-term cellular therapy. FASEB J. 2009, 24, 22–31. [Google Scholar]
- Bruzewicz, D.A.; McGuigan, A.P.; Whitesides, G.M. Fabrication of a modular tissue construct in a microfluidic chip. Lab Chip 2008, 8, 663–671. [Google Scholar]
© 2012 by the authors; licensee MDPI, Basel, Switzerland. This article is an open-access article distributed under the terms and conditions of the Creative Commons Attribution license (http://creativecommons.org/licenses/by/3.0/).
Share and Cite
Wan, J. Microfluidic-Based Synthesis of Hydrogel Particles for Cell Microencapsulation and Cell-Based Drug Delivery. Polymers 2012, 4, 1084-1108. https://doi.org/10.3390/polym4021084
Wan J. Microfluidic-Based Synthesis of Hydrogel Particles for Cell Microencapsulation and Cell-Based Drug Delivery. Polymers. 2012; 4(2):1084-1108. https://doi.org/10.3390/polym4021084
Chicago/Turabian StyleWan, Jiandi. 2012. "Microfluidic-Based Synthesis of Hydrogel Particles for Cell Microencapsulation and Cell-Based Drug Delivery" Polymers 4, no. 2: 1084-1108. https://doi.org/10.3390/polym4021084
APA StyleWan, J. (2012). Microfluidic-Based Synthesis of Hydrogel Particles for Cell Microencapsulation and Cell-Based Drug Delivery. Polymers, 4(2), 1084-1108. https://doi.org/10.3390/polym4021084