Polymer-Based Constructs for Flexor Tendon Repair: A Review
Abstract
:1. Introduction
2. Flexor Tendon
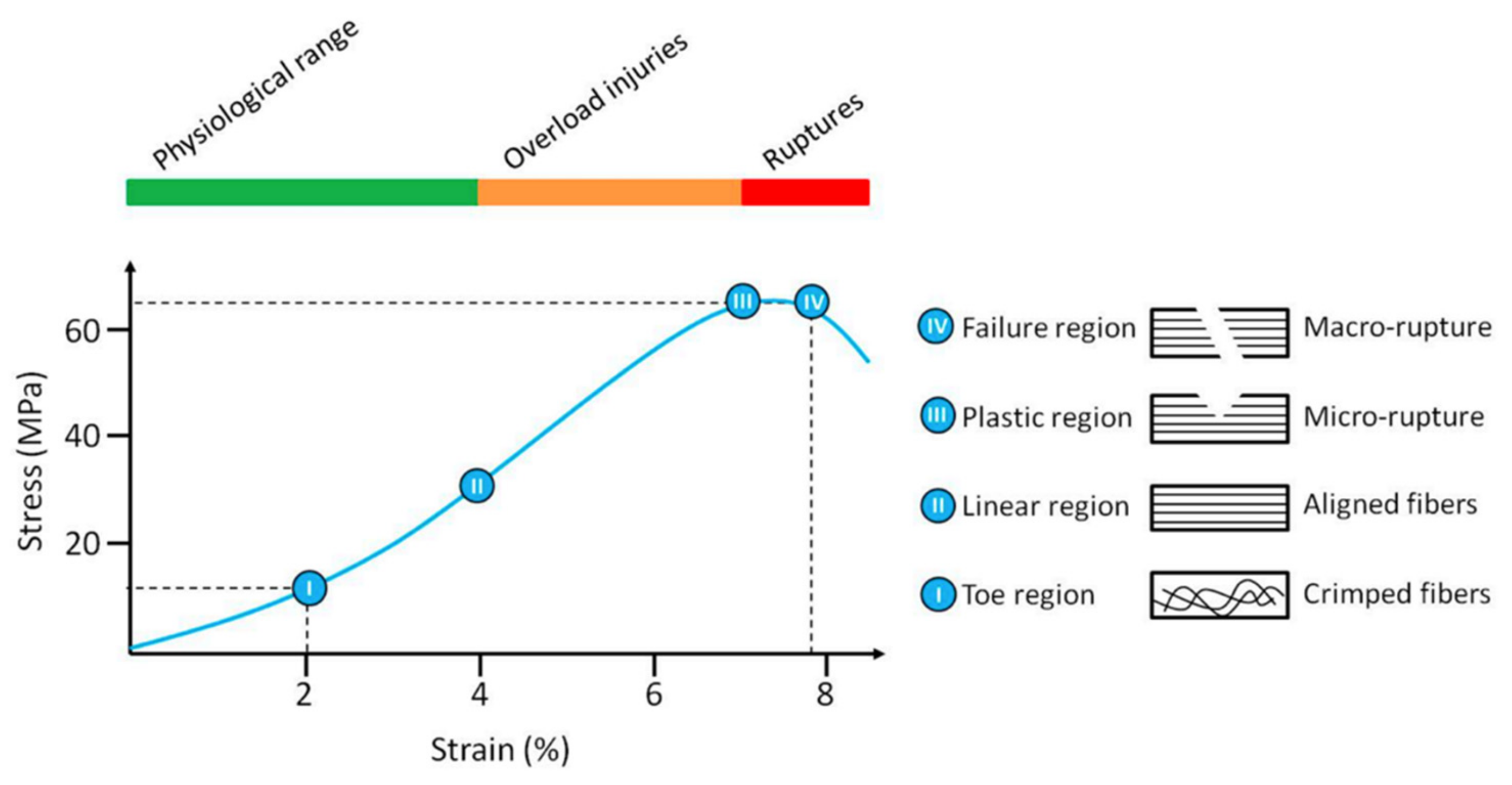
2.1. Flexor Tendon and Function: Composition and Structure
2.2. Flexor Tendon and Function: Causes and Impact
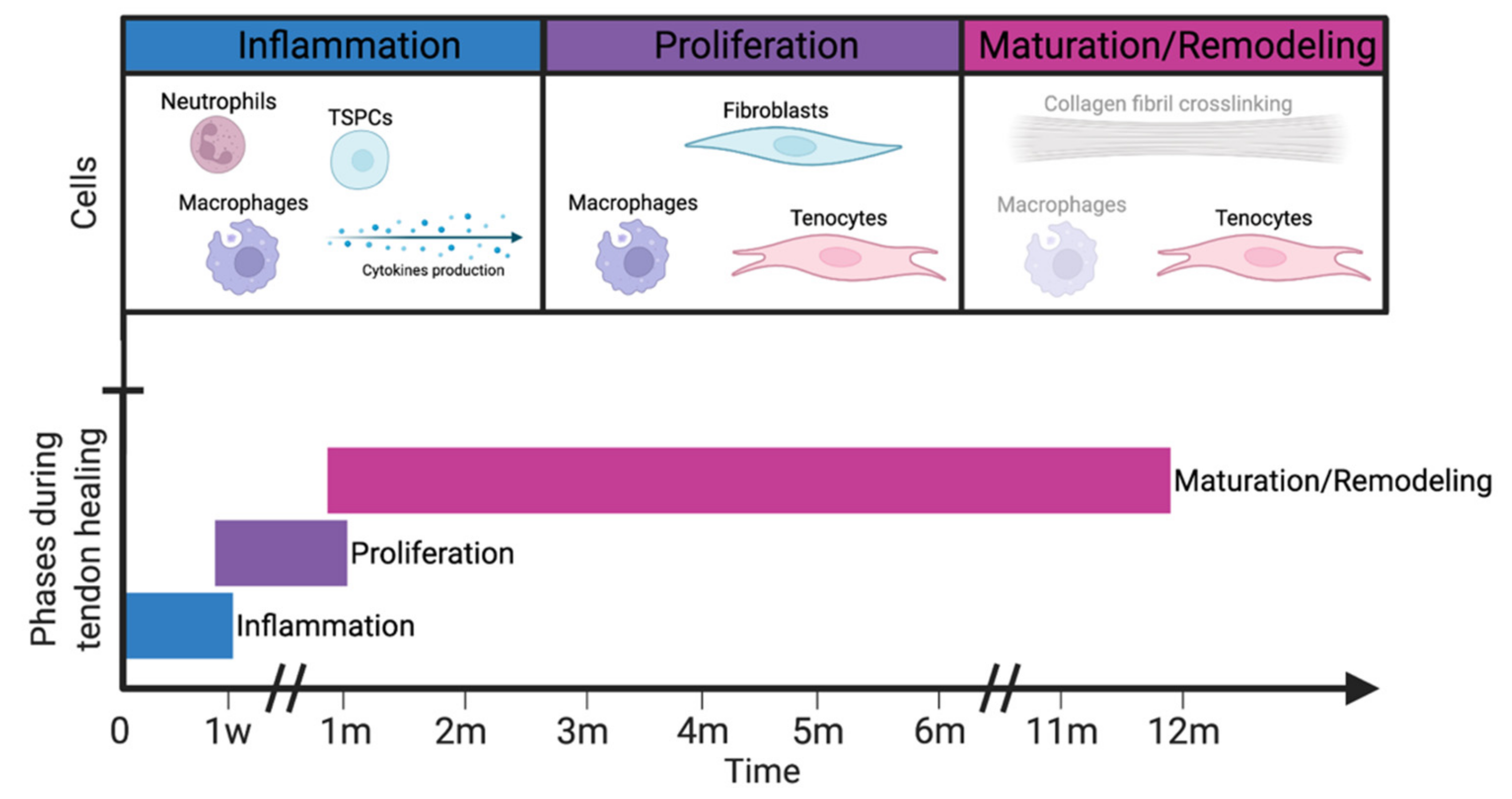
2.3. Flexor Tendon and Function: Regeneration and Repair
3. Traditional Strategies for the Repair of Flexor Tendon Injuries
3.1. Suture Techniques
3.2. Graft Transplantation Techniques
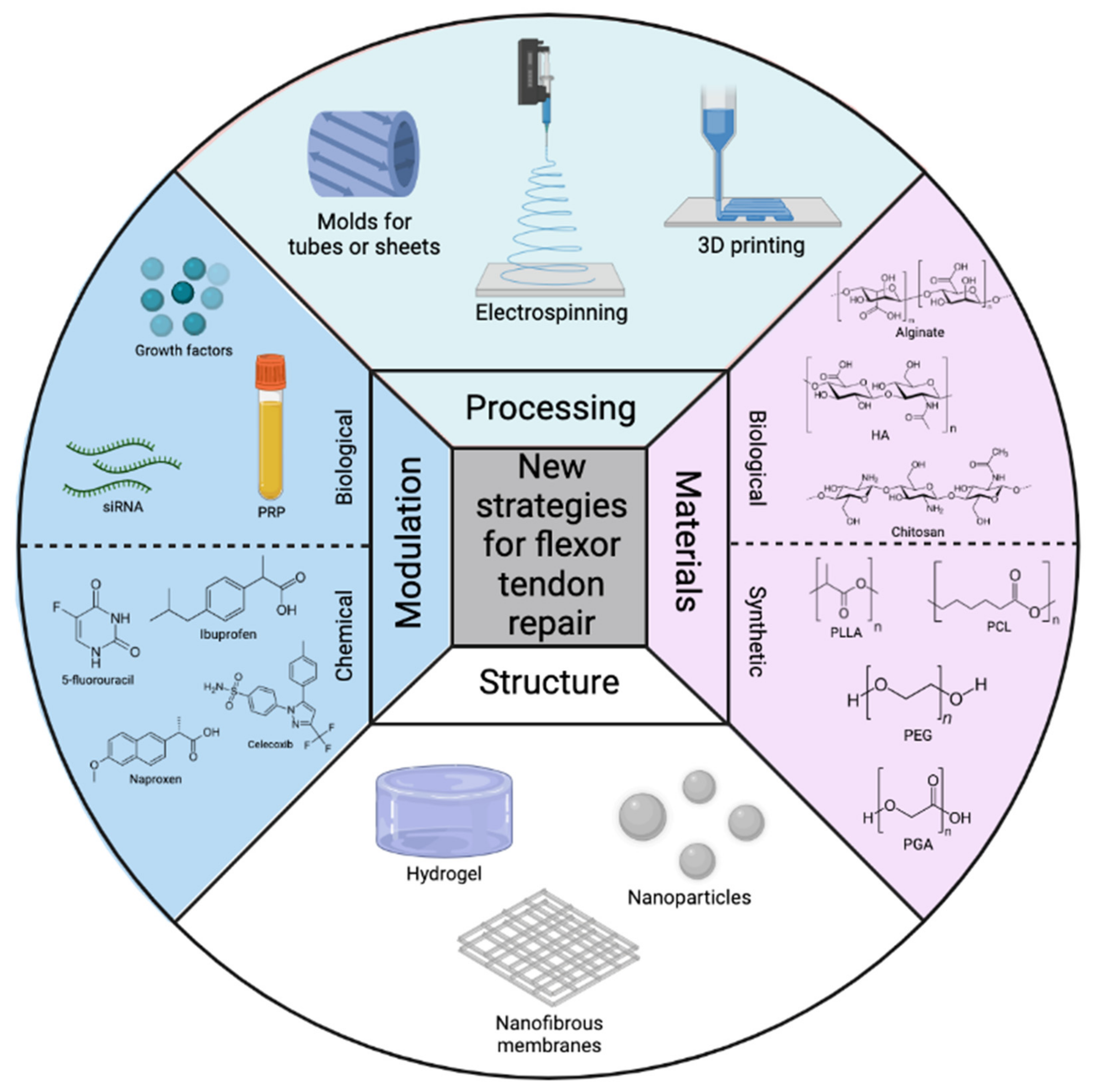
4. New Strategies for the Repair of Flexor Tendon Injuries
4.1. Biochemical Solutions for Postoperative Complications
4.1.1. Peritendinous Adhesion Formation
4.1.2. Infections
4.2. Requirements of Polymeric Materials for Flexor Tendon Repair
- (i)
- Biodegradability
- (ii)
- Biocompatibility
- (iii)
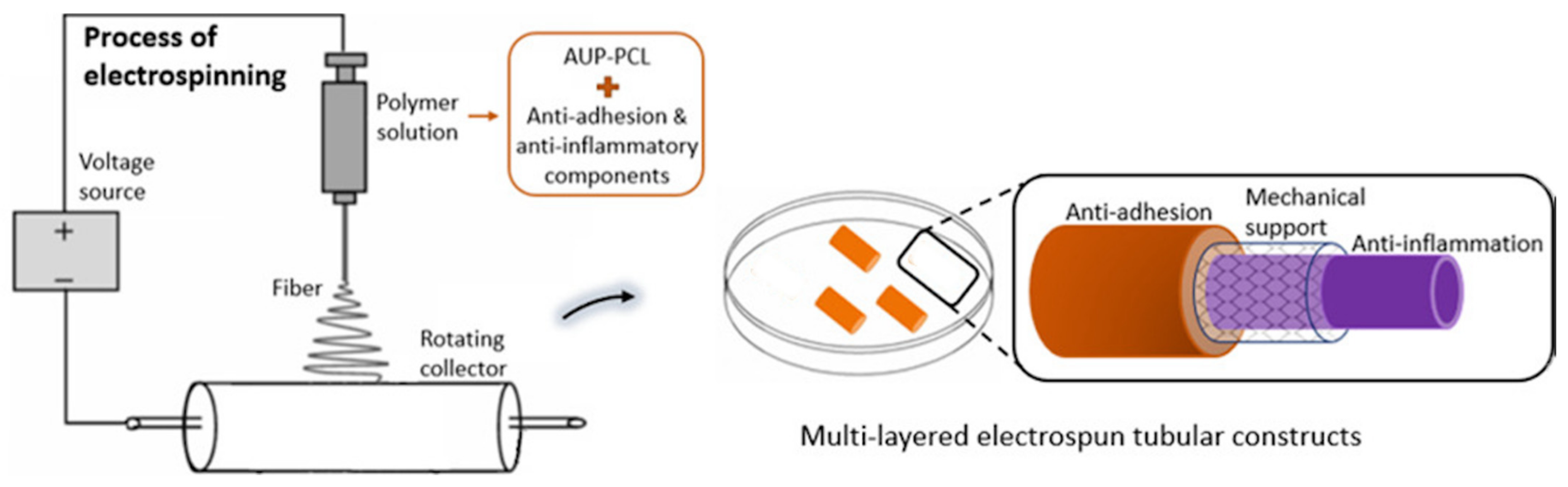
- Processability and Structure Architecture
- (iv)
- Mechanical Properties
4.3. Materials for Flexor Tendon Scaffold and Construct Designs
4.3.1. Biological Polymer Constructs
4.3.2. Synthetic Polymer Constructs
4.3.3. Semi-Synthetic Polymer Constructs
5. Conclusions and Perspectives
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Kirkendall, D.T.; Garrett, W.E. Function and biomechanics of tendons. Scand. J. Med. Sci. Sport. 1997, 7, 62–66. [Google Scholar] [CrossRef] [PubMed]
- Snedeker, J.G.; Foolen, J. Tendon injury and repair—A perspective on the basic mechanisms of tendon disease and future clinical therapy. Acta Biomater. 2017, 63, 18–36. [Google Scholar] [CrossRef] [PubMed]
- Banik, B.L.; Lewis, G.S.; Brown, J.L. Multiscale Poly-(ϵ-caprolactone) Scaffold Mimicking Non-linearity in Tendon Tissue Mechanics. Regen. Eng. Transl. Med. 2016, 2, 1–9. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Ghiya, M.N.; Murty, S.; Shetty, N.; D’Cunha, R. A descriptive study of hand injuries presenting to the adult emergency department of a tertiary care center in urban India. J. Emerg. Trauma. Shock 2017, 10, 19–25. [Google Scholar] [CrossRef]
- Clark, D.P.; Scott, R.N.; Anderson, I.W. Hand problems in an accident and emergency department. J. Hand Surg. Br. 1985, 10, 297–299. [Google Scholar] [CrossRef]
- Citeroni, M.R.; Ciardulli, M.C.; Russo, V.; Della Porta, G.; Mauro, A.; El Khatib, M.; Di Mattia, M.; Galesso, D.; Barbera, C.; Forsyth, N.R.; et al. Review in vitro innovation of tendon tissue engineering strategies. Int. J. Mol. Sci. 2020, 21, 1–78. [Google Scholar] [CrossRef]
- Titan, A.L.; Foster, D.S.; Chang, J.; Longaker, M.T. Flexor Tendon: Development, Healing, Adhesion Formation, and Contributing Growth Factors. Plast. Reconstr. Surg. 2019, 144, 639e–647e. [Google Scholar] [CrossRef]
- Legrand, A.; Kaufman, Y.; Long, C.; Fox, P.M. Molecular Biology of Flexor Tendon Healing in Relation to Reduction of Tendon Adhesions. J. Hand Surg. Am. 2017, 42, 722–726. [Google Scholar] [CrossRef]
- Woo, S.L.Y.; Gelberman, R.H.; Cobb, N.G.; Amiel, D.; Lothringer, K.; Akeson, W.H. the importance of controlled passive mobilization on flexor tendon healing: A biomechanical study. Acta Orthop. 1981, 52, 615–622. [Google Scholar] [CrossRef]
- Buschmann, J.; Meier Bürgisser, G. Autograft, allograft, and xenograft scaffolds for tendon and ligament repair. In Biomechanics of Tendons and Ligaments; Woodhead Publishing: Sawston, UK, 2017; ISBN 9780081004890. [Google Scholar]
- Rawson, S.; Cartmell, S.; Wong, J. Suture techniques for tendon repair; a comparative review. Muscles Ligaments Tendons J. 2013, 3, 220–228. [Google Scholar] [CrossRef] [Green Version]
- Vasiliadis, A.V.; Katakalos, K. The role of scaffolds in tendon tissue engineering. J. Funct. Biomater. 2020, 11, 78. [Google Scholar] [CrossRef] [PubMed]
- Sigal, I.R.; Grande, D.A.; Dines, D.M.; Dines, J.; Drakos, M. Biologic and Tissue Engineering Strategies for Tendon Repair. Regen. Eng. Transl. Med. 2016, 2, 107–125. [Google Scholar] [CrossRef] [Green Version]
- Zhou, H.; Lu, H. Advances in the Development of Anti-Adhesive Biomaterials for Tendon Repair Treatment. Tissue Eng. Regen. Med. 2021, 18, 1–14. [Google Scholar] [CrossRef] [PubMed]
- Beldjilali-Labro, M.; Garcia, A.G.; Farhat, F.; Bedoui, F.; Grosset, J.F.; Dufresne, M.; Legallais, C. Biomaterials in tendon and skeletal muscle tissue engineering: Current trends and challenges. Materials 2018, 11, 1116. [Google Scholar] [CrossRef] [Green Version]
- Rademakers, T.; Horvath, J.M.; van Blitterswijk, C.A.; LaPointe, V.L.S. Oxygen and nutrient delivery in tissue engineering: Approaches to graft vascularization. J. Tissue Eng. Regen. Med. 2019, 13, 1815–1829. [Google Scholar] [CrossRef]
- Cravedi, P.; Farouk, S.; Angeletti, A.; Edgar, L.; Tamburrini, R.; Duisit, J.; Perin, L.; Orlando, G. Regenerative immunology: The immunological reaction to biomaterials. Transpl. Int. 2017, 30, 1199–1208. [Google Scholar] [CrossRef] [Green Version]
- No, Y.J.; Castilho, M.; Ramaswamy, Y.; Zreiqat, H. Role of Biomaterials and Controlled Architecture on Tendon/Ligament Repair and Regeneration. Adv. Mater. 2020, 32, 1904511. [Google Scholar] [CrossRef]
- Chen, S.H.; Chen, C.H.; Fong, Y.T.; Chen, J.P. Prevention of peritendinous adhesions with electrospun chitosan-grafted polycaprolactone nanofibrous membranes. Acta Biomater. 2014, 10, 4971–4982. [Google Scholar] [CrossRef]
- Kannus, P. Structure of the tendon connective tissue. Scand. J. Med. Sci. Sports 2000, 10, 312–320. [Google Scholar] [CrossRef]
- Benjamin, M.; Ralphs, J.R. The cell and developmental biology of tendons and ligaments. Int. Rev. Cytol. 2000, 196, 85–130. [Google Scholar] [CrossRef]
- Wang, J.H.C.; Guo, Q.; Li, B. Tendon biomechanics and mechanobiology—A minireview of basic concepts and recent advancements. J. Hand Ther. 2012, 25, 133–141. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Walden, G.; Liao, X.; Donell, S.; Raxworthy, M.J.; Riley, G.P.; Saeed, A. A Clinical, Biological, and Biomaterials Perspective into Tendon Injuries and Regeneration. Tissue Eng. Part B Rev. 2017, 23, 44–58. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Steinmann, S.; Pfeifer, C.G.; Brochhausen, C.; Docheva, D. Spectrum of tendon pathologies: Triggers, trails and end-state. Int. J. Mol. Sci. 2020, 21, 844. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Silver, F.H.; Freeman, J.W.; Seehra, G.P. Collagen self-assembly and the development of tendon mechanical properties. J. Biomech. 2003, 36, 1529–1553. [Google Scholar] [CrossRef]
- Tempfer, H.; Lehner, C.; Grütz, M.; Gehwolf, R.; Traweger, A. Biological Augmentation for Tendon Repair: Lessons to be Learned from Development, Disease, and Tendon Stem Cell Research. In Cell Engineering and Regeneration. Reference Series in Biomedical Engineering; Gimble, J., Marolt Presen, D., Oreffo, R., Wolbank, S., Redl, H., Eds.; Springer: Cham, Switzerland, 2017; ISBN 9783319370767. [Google Scholar]
- Canty, E.G.; Kadler, K.E. Collagen fibril biosynthesis in tendon: A review and recent insights. Comp. Biochem. Physiol. A Mol. Integr. Physiol. 2002, 133, 979–985. [Google Scholar] [CrossRef]
- Zuskov, A.; Freedman, B.R.; Gordon, J.A.; Sarver, J.J.; Buckley, M.R.; Soslowsky, L.J. Tendon Biomechanics and Crimp Properties Following Fatigue Loading Are Influenced by Tendon Type and Age in Mice. J. Orthop. Res. 2020, 38, 36–42. [Google Scholar] [CrossRef]
- Rosario, M.V.; Roberts, T.J. Loading Rate Has Little Influence on Tendon Fascicle Mechanics. Front. Physiol. 2020, 11, 255. [Google Scholar] [CrossRef] [Green Version]
- Silver, F.H.; Christiansen, D.L.; Snowhill, P.B.; Chen, Y. Role of Storage on Changes in the Mechanical Properties of Tendon and Self-Assembled Collagen Fibers. Connect. Tissue Res. 2000, 41, 155–164. [Google Scholar] [CrossRef]
- Mccormick, R.J. Extracellular modifications to muscle collagen: Implications for meat quality. Poult. Sci. 1999, 78, 785–791. [Google Scholar] [CrossRef]
- Franchi, M.; Trirè, A.; Quaranta, M.; Orsini, E.; Ottani, V. Collagen structure of tendon relates to function. ScientificWorldJournal 2007, 7, 404–420. [Google Scholar] [CrossRef]
- Johnson, G.A.; Tramaglini, D.M.; Levine, R.E.; Ohno, K.; Choi, N.-Y.; Woo, S.L.-Y. Tensile and viscoelastic properties of human patellar tendon. J. Orthop. Res. 1994, 12, 796–803. [Google Scholar] [CrossRef] [PubMed]
- Martin, R.B.; Burr, D.B.; Sharkey, N.A.; Fyhrie, D.P. Mechanical Properties of Ligament and Tendon In Skeletal Tissue Mechanics; Springer: New York, NY, USA, 2015. [Google Scholar]
- Zhang, C.; Zhu, J.; Zhou, Y.; Thampatty, B.P.; Wang, J.H.C. Tendon Stem/Progenitor Cells and Their Interactions with Extracellular Matrix and Mechanical Loading. Stem Cells Int. 2019, 2019, 3674647. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Lin, T.W.; Cardenas, L.; Soslowsky, L.J. Biomechanics of tendon injury and repair. J. Biomech. 2004, 37, 865–877. [Google Scholar] [CrossRef] [PubMed]
- Millar, N.L.; Murrell, G.A.C.; Mcinnes, I.B. Inflammatory mechanisms in tendinopathy—Towards translation. Nat. Rev. Rheumatol. 2017, 13, 110–122. [Google Scholar] [CrossRef] [PubMed]
- Fatemi, M.J.; Shirani, S.; Sobhani, R.; Lebaschi, A.H.; Gharegozlou, M.J.; Bagheri, T.; Pedram, M.; Saberi, M.; Araghi, S.; Fatemi, M.A. Prevention of Peritendinous Adhesion Formation After the Flexor Tendon Surgery in Rabbits: A Comparative Study Between Use of Local Interferon-α, Interferon-β, and 5-Fluorouracil. Ann. Plast. Surg. 2018, 80, 171–175. [Google Scholar] [CrossRef] [PubMed]
- D’Addona, A.; Maffulli, N.; Formisano, S.; Rosa, D. Inflammation in tendinopathy. Surgeon 2017, 15, 297–302. [Google Scholar] [CrossRef]
- de Jong, J.P.; Nguyen, J.T.; Sonnema, A.J.M.; Nguyen, E.C.; Amadio, P.C.; Moran, S.L. The incidence of acute traumatic tendon injuries in the hand and wrist: A 10-year population-based study. Clin. Orthop. Surg. 2014, 6, 196–202. [Google Scholar] [CrossRef]
- Sharma, P.; Maffulli, N. Tendon Injury and Tendinopathy. J. Bone Jt. Surg. 2005, 87, 187–202. [Google Scholar] [CrossRef] [Green Version]
- Yang, G.; Rothrauff, B.B.; Tuan, R.S. Tendon and ligament regeneration and repair: Clinical relevance and developmental paradigm. Birth Defects Res. Part C Embryo Today Rev. 2013, 99, 203–222. [Google Scholar] [CrossRef] [Green Version]
- Gault, D.T. Reduction of grip strength, finger flexion pressure, finger pinch pressure and key pinch following flexor tendon repair. J. Hand Surg. Br. 1987, 12, 182–184. [Google Scholar] [CrossRef]
- Rodrigues, M.T.; Reis, R.L.; Gomes, M.E. Engineering tendon and ligament tissues: Present developments towards successful clinical products. J. Tissue Eng. Regen. Med. 2013, 7, 673–686. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Docheva, D.; Müller, S.A.; Majewski, M.; Evans, C.H. Biologics for tendon repair. Adv. Drug Deliv. Rev. 2015, 84, 222–239. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Strickland, J.W. Flexor Tendon Injuries: I. Foundations of Treatment. J. Am. Acad. Orthop. Surg. 1995, 3, 44–54. [Google Scholar] [CrossRef]
- Gelberman, R.H.; Manske, P.R.; de Van Berg, J.S.; Lesker, P.A.; Akeson, W.H. Flexor tendon repair in vitro: A comparative histologic study of the rabbit, chicken, dog, and monkey. J. Orthop. Res. 1984, 2, 39–48. [Google Scholar] [CrossRef] [PubMed]
- Beredjiklian, P.K. Biologic aspects of flexor tendon laceration and repair. J. Bone Jt. Surg. Ser. A 2003, 85, 539–550. [Google Scholar] [CrossRef]
- Pearce, O.; Brown, M.T.; Fraser, K.; Lancerotto, L. Flexor tendon injuries: Repair & Rehabilitation. Injury 2021, 52, 2053–2067. [Google Scholar] [CrossRef]
- Thomopoulos, S.; Parks, W.C.; Rifkin, D.B.; Derwin, K.A. Mechanisms of tendon injury and repair. J. Orthop. Res. 2015, 33, 832–839. [Google Scholar] [CrossRef] [Green Version]
- Leong, N.L.; Kator, J.L.; Clemens, T.L.; James, A.; Enamoto-Iwamoto, M.; Jiang, J. Tendon and Ligament Healing and Current Approaches to Tendon and Ligament Regeneration. J. Orthop. Res. 2020, 38, 7–12. [Google Scholar] [CrossRef]
- Galvez, M.G.; Crowe, C.; Farnebo, S.; Chang, J. Tissue engineering in flexor tendon surgery: Current state and future advances. J. Hand Surg. Eur. Vol. 2014, 39, 71–78. [Google Scholar] [CrossRef]
- Voleti, P.B.; Buckley, M.R.; Soslowsky, L.J. Tendon healing: Repair and regeneration. Annu. Rev. Biomed. Eng. 2012, 14, 47–71. [Google Scholar] [CrossRef]
- Jung, H.-J.; Fisher, M.B.; Woo, S.L.-Y. Role of biomechanics in the understanding of normal, injured, and healing ligaments and tendons. BMC Sports Sci. Med. Rehabil. 2009, 1, 9. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Drapé, J.L.; Tardif-Chastenet De Gery, S.; Silbermann-Hoffman, O.; Chevrot, A.; Houvet, P.; Alnot, J.Y.; Benacerraf, R. Closed ruptures of the flexor digitorum tendons: MRI evaluation. Skelet. Radiol. 1998, 27, 617–624. [Google Scholar] [CrossRef] [PubMed]
- Ivanova, N.; Gugleva, V.; Dobreva, M.; Pehlivanov, I.; Stefanov, S.; Andonova, V. Management of Flexor Tendon Injuries in Hand. In Intech; IntechOpen: London, UK, 2016; Volume i, p. 13. [Google Scholar]
- Lee, D.H.; Robbin, M.L.; Galliott, R.; Graveman, V.A. Ultrasound evaluation of flexor tendon lacerations. J. Hand Surg. Am. 2000, 25, 236–241. [Google Scholar] [CrossRef] [PubMed]
- Kumar, B.A.; Tolat, A.R.; Threepuraneni, G.; Jones, B. The role of magnetic resonance imaging in late presentation of isolated injuries of the flexor digitorum profundus tendon in the finger. J. Hand Surg. Br. 2000, 25, 95–97. [Google Scholar] [CrossRef]
- Sandvall, B.K.; Kuhlman-Wood, K.; Recor, C.; Friedrich, J.B. Flexor tendon repair, rehabilitation, and reconstruction. Plast. Reconstr. Surg. 2013, 132, 1493–1503. [Google Scholar] [CrossRef]
- Güntürk, Ö.B.; Kayalar, M.; Kaplan, İ.; Uludağ, A.; Özaksar, K.; Keleşoğlu, B. Results of 4-strand modified Kessler core suture and epitendinous interlocking suture followed by modified Kleinert protocol for flexor tendon repairs in Zone 2. Acta Orthop. Traumatol. Turc. 2018, 52, 382–386. [Google Scholar] [CrossRef]
- Sebastin, S.J.; Ho, A.; Karjalainen, T.; Chung, K.C. History and evolution of the Kessler repair. J. Hand Surg. Am. 2013, 38, 552–561. [Google Scholar] [CrossRef] [Green Version]
- Wada, A.; Kubota, H.; Hatanaka, H.; Hotokezaka, S.; Miura, H.; Iwamoto, Y. The mechanical properties of locking and grasping suture loop configurations in four-strand core suture techniques. J. Hand Surg. Br. 2000, 25, 548–551. [Google Scholar] [CrossRef]
- Thurman, R.T.; Trumble, T.E.; Hanel, D.P.; Tencer, A.F.; Kiser, P.K. Two-, four-, and six-strand zone II flexor tendon repairs: An in situ biomechanical comparison using a cadaver model. J. Hand Surg. Am. 1998, 23, 261–265. [Google Scholar] [CrossRef]
- Viinikainen, A.; Göransson, H.; Huovinen, K.; Kellomäki, M.; Rokkanen, P. A comparative analysis of the biomechanical behaviour of five flexor tendon core sutures. J. Hand Surg. Br. 2004, 29, 536–543. [Google Scholar] [CrossRef]
- Winters, S.C.; Gelberman, R.H.; Woo, S.L.; Chan, S.S.; Grewal, R.; Seiler, J.G., 3rd. The effects of multiple-strand suture methods on the strength and excursion of repaired intrasynovial flexor tendons: A biomechanical study in dogs. J. Hand Surg. Am. 1998, 23, 97–104. [Google Scholar] [CrossRef]
- Lawrence, T.M.; Davis, T.R.C. A biomechanical analysis of suture materials and their influence on a four-strand flexor tendon repair. J. Hand Surg. Am. 2005, 30, 836–841. [Google Scholar] [CrossRef]
- McDonald, E.; Gordon, J.A.; Buckley, J.M.; Gordon, L. Comparison of a multifilament stainless steel suture with FiberWire for flexor tendon repairs--an in vitro biomechanical study. J. Hand Surg. Eur. Vol. 2013, 38, 418–423. [Google Scholar] [CrossRef] [PubMed]
- Trail, I.A.; Powell, E.S.; Noble, J. An evaluation of suture materials used in tendon surgery. J. Hand Surg. Br. 1989, 14, 422–427. [Google Scholar] [CrossRef]
- Dy, C.J.; Hernandez-Soria, A.; Ma, Y.; Roberts, T.R.; Daluiski, A. Complications after flexor tendon repair: A systematic review and meta-analysis. J. Hand Surg. Am. 2012, 37, 543–552. [Google Scholar] [CrossRef] [PubMed]
- Zhao, C.; Amadio, P.C.; Zobitz, M.E.; Momose, T.; Couvreur, P.; An, K.-N. Effect of synergistic motion on flexor digitorum profundus tendon excursion. Clin. Orthop. Relat. Res. 2002, 223–230. [Google Scholar] [CrossRef] [PubMed]
- Stark, H.H.; Anderson, D.R.; Zemel, N.P.; Boyes, J.H.; Ashworth, C.R.; Rickard, T.A. Bridge flexor tendon grafts. Clin. Orthop. Relat. Res. 1989, 51–59. [Google Scholar] [CrossRef]
- Jakubietz, M.; Jakubietz, D.; Gruenert, J.G.P.; Zahn, R.; Meffert, R.; Jakubietz, R. Adequacy of Palmaris Longus and Plantaris Tendons for Tendon Grafting. J. Hand Surg. Am. 2011, 36, 695–698. [Google Scholar] [CrossRef] [PubMed]
- Jackson, D.W.; Corsetti, J.; Simon, T.M. Biologic Incorporation of Allograft Anterior Cruciate Ligament Replacements. Clin. Orthop. Relat. Res. 1996, 324, 126–133. [Google Scholar] [CrossRef]
- Robertson, A.; Nutton, R.W.; Keating, J.F. Current trends in the use of tendon allografts in orthopaedic surgery. J. Bone Jt. Surg. Br. 2006, 88, 988–992. [Google Scholar] [CrossRef] [Green Version]
- Poehling, G.G.; Curl, W.W.; Lee, C.A.; Ginn, T.A.; Rushing, J.T.; Naughton, M.J.; Holden, M.B.; Martin, D.F.; Smith, B.P. Analysis of Outcomes of Anterior Cruciate Ligament Repair With 5-Year Follow-up: Allograft Versus Autograft. Arthrosc. J. Arthrosc. Relat. Surg. 2005, 21, 774.e1–774.e15. [Google Scholar] [CrossRef] [PubMed]
- Taras, J.S.; Lamb, M.J. Treatment of flexor tendon injuries: Surgeons’ perspective. J. Hand Ther. Off. J. Am. Soc. Hand Ther. 1999, 12, 141–148. [Google Scholar] [CrossRef]
- Derby, B.M.; Wilhelmi, B.J.; Zook, E.G.; Neumeister, M.W. Flexor tendon reconstruction. Clin. Plast. Surg. 2011, 38, 607–619. [Google Scholar] [CrossRef] [PubMed]
- Ramesh, R.; Kumar, N.; Sharma, A.K.; Maiti, S.K.; Singh, G.R. Acellular and glutaraldehyde-preserved tendon allografts for reconstruction of superficial digital flexor tendon in bovines: Part I—Clinical, radiological and angiographical observations. J. Vet. Med. A Physiol. Pathol. Clin. Med. 2003, 50, 511–519. [Google Scholar] [CrossRef]
- Zhang, C.-H.; Jiang, Y.-L.; Ning, L.-J.; Li, Q.; Fu, W.-L.; Zhang, Y.-J.; Zhang, Y.-J.; Xia, C.-C.; Li, J.; Qin, T.-W. Evaluation of Decellularized Bovine Tendon Sheets for Achilles Tendon Defect Reconstruction in a Rabbit Model. Am. J. Sports Med. 2018, 46, 2687–2699. [Google Scholar] [CrossRef]
- Moshiri, A.; Oryan, A. Role of tissue engineering in tendon reconstructive surgery and regenerative medicine: Current concepts, approaches and concerns. Hard Tissue 2012, 1, 11. [Google Scholar] [CrossRef] [Green Version]
- Allman, A.J.; McPherson, T.B.; Badylak, S.F.; Merrill, L.C.; Kallakury, B.; Sheehan, C.; Raeder, R.H.; Metzger, D.W. Xenogeneic extracellular matrix grafts elicit a TH2-restricted immune response. Transplantation 2001, 71, 1631–1640. [Google Scholar] [CrossRef] [PubMed]
- Oryan, A.; Moshiri, A.; Meimandi-Parizi, A. Graft selection in ACL reconstructive surgery: Past, present, and future. Curr. Orthop. Pract. 2013, 24, 321–333. [Google Scholar] [CrossRef]
- Van Der Merwe, W.; Lind, M.; Faunø, P.; Van Egmond, K.; Zaffagnini, S.; Marcacci, M.; Cugat, R.; Verdonk, R.; Ibañez, E.; Guillen, P.; et al. Xenograft for anterior cruciate ligament reconstruction was associated with high graft processing infection. J. Exp. Orthop. 2020, 7, 79. [Google Scholar] [CrossRef]
- Pridgen, B.C.; Woon, C.Y.L.; Kim, M.; Thorfinn, J.; Lindsey, D.; Pham, H.; Chang, J. Flexor tendon tissue engineering: Acellularization of human flexor tendons with preservation of biomechanical properties and biocompatibility. Tissue Eng. Part C Methods 2011, 17, 819–828. [Google Scholar] [CrossRef]
- Veillette, C.J.; Cunningham, K.D.; Hart, D.A.; Fritzler, M.J.; Frank, C.B. Localization and characterization of porcine patellar tendon xenograft antigens in a rabbit model of medial collateral ligament replacement. Transplantation 1998, 65, 486–493. [Google Scholar] [CrossRef] [PubMed]
- Hunter, J. ARTIFICIAL TENDONS. EARLY DEVELOPMENT AND APPLICATION. Am. J. Surg. 1965, 109, 325–338. [Google Scholar] [CrossRef]
- Hunter, J.M.; Salisbury, R.E. Use of gliding artificial implants to produce tendon sheaths. Techniques and results in children. Plast. Reconstr. Surg. 1970, 45, 564–572. [Google Scholar] [CrossRef] [PubMed]
- Abdullah, S. Usage of synthetic tendons in tendon reconstruction. BMC Proc. 2015, 9, A68. [Google Scholar] [CrossRef] [Green Version]
- Murray, A.W.; MacNicol, M.F. 10–16 year results of Leeds-Keio anterior cruciate ligament reconstruction. Knee 2004, 11, 9–14. [Google Scholar] [CrossRef]
- Bashaireh, K.M.; Audat, Z.; Radaideh, A.M.; Aleshawi, A.J. The Effectiveness of Autograft Used in Anterior Cruciate Ligament Reconstruction of the Knee: Surgical Records for the New Generations of Orthopedic Surgeons and Synthetic Graft Revisit. Orthop. Res. Rev. 2020, 12, 61–67. [Google Scholar] [CrossRef]
- Satora, W.; Królikowska, A.; Czamara, A.; Reichert, P. Synthetic grafts in the treatment of ruptured anterior cruciate ligament of the knee joint. Polim. Med. 2017, 47, 55–59. [Google Scholar] [CrossRef]
- McLaughlin, R.M. Complications After Treatment of Flexor Tendon Injuries. Small Anim. Surg. Secrets Second Ed. 2004, 14, 327–330. [Google Scholar] [CrossRef]
- Pien, N.; Peeters, I.; Deconinck, L.; Van Damme, L.; De Wilde, L.; Martens, A.; Van Vlierberghe, S.; Dubruel, P.; Mignon, A. Design and development of a reinforced tubular electrospun construct for the repair of ruptures of deep flexor tendons. Mater. Sci. Eng. C 2021, 119, 111504. [Google Scholar] [CrossRef]
- Chen, S.; Wang, G.; Wu, T.; Zhao, X.; Liu, S.; Li, G.; Cui, W.; Fan, C. Silver nanoparticles/ibuprofen-loaded poly(L-lactide) fibrous membrane: Anti-infection and anti-adhesion effects. Int. J. Mol. Sci. 2014, 15, 14014–14025. [Google Scholar] [CrossRef] [Green Version]
- Liu, S.; Hu, C.; Li, F.; Li, X.J.; Cui, W.; Fan, C. Prevention of peritendinous adhesions with electrospun ibuprofen-loaded poly(l-Lactic Acid)-polyethylene glycol fibrous membranes. Tissue Eng. Part A 2013, 19, 529–537. [Google Scholar] [CrossRef] [PubMed]
- Hu, C.; Liu, S.; Zhang, Y.; Li, B.; Yang, H.; Fan, C.; Cui, W. Long-term drug release from electrospun fibers for in vivo inflammation prevention in the prevention of peritendinous adhesions. Acta Biomater. 2013, 9, 7381–7388. [Google Scholar] [CrossRef] [PubMed]
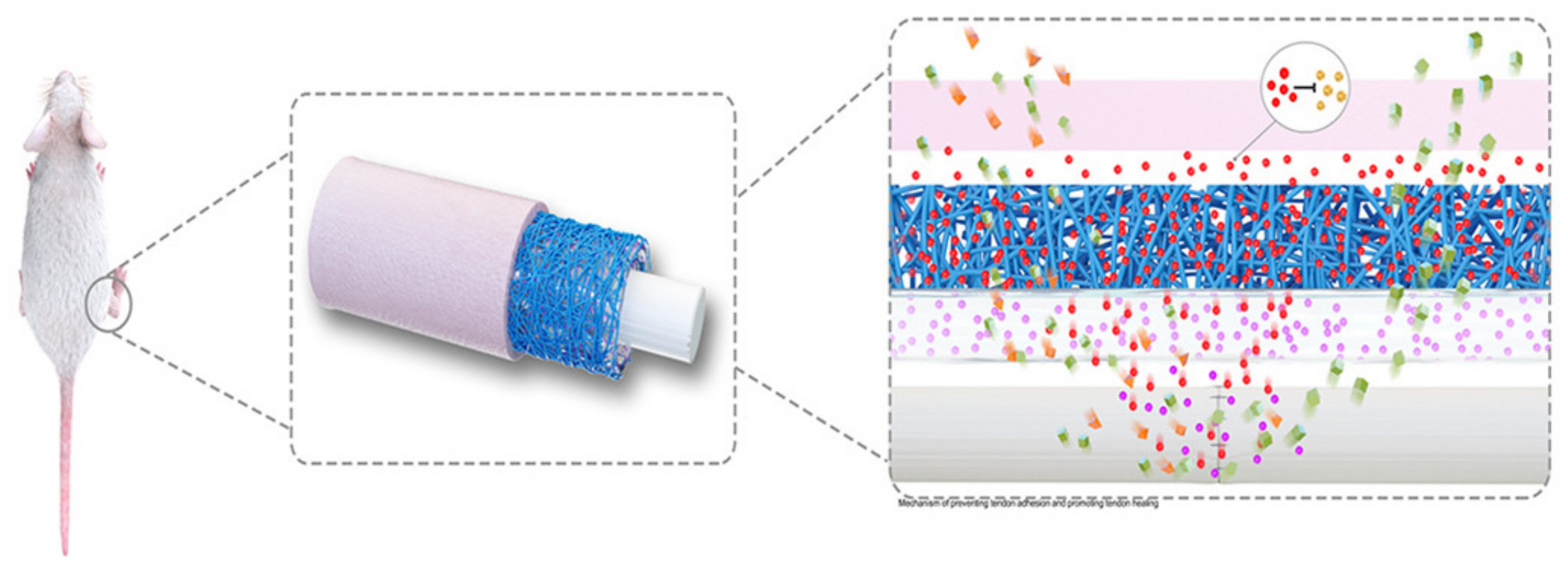
- Yan, Z.; Meng, X.; Su, Y.; Chen, Y.; Zhang, L.; Xiao, J. Double layer composite membrane for preventing tendon adhesion and promoting tendon healing. Mater. Sci. Eng. C 2021, 123, 111941. [Google Scholar] [CrossRef] [PubMed]
- Chen, C.T.; Chen, C.H.; Sheu, C.; Chen, J.P. Ibuprofen-loaded hyaluronic acid nanofibrous membranes for prevention of postoperative tendon adhesion through reduction of inflammation. Int. J. Mol. Sci. 2019, 20, 5038. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Yuan, B.; He, C.; Dong, X.; Wang, J.; Gao, Z.; Wang, Q.; Tian, H.; Chen, X. 5-Fluorouracil loaded thermosensitive PLGA-PEG-PLGA hydrogels for the prevention of postoperative tendon adhesion. RSC Adv. 2015, 5, 25295–25303. [Google Scholar] [CrossRef]
- Li, L.; Zheng, X.; Fan, D.; Yu, S.; Wu, D.; Fan, C.; Cui, W.; Ruan, H. Release of celecoxib from a bi-layer biomimetic tendon sheath to prevent tissue adhesion. Mater. Sci. Eng. C 2016, 61, 220–226. [Google Scholar] [CrossRef]
- Jiang, S.; Zhao, X.; Chen, S.; Pan, G.; Song, J.; He, N.; Li, F.; Cui, W.; Fan, C. Down-regulating ERK1/2 and SMAD2/3 phosphorylation by physical barrier of celecoxib-loaded electrospun fibrous membranes prevents tendon adhesions. Biomaterials 2014, 35, 9920–9929. [Google Scholar] [CrossRef]
- Jiang, S.; Yan, H.; Fan, D.; Song, J.; Fan, C. Multi-layer electrospun membrane mimicking tendon sheath for prevention of tendon adhesions. Int. J. Mol. Sci. 2015, 16, 6932–6944. [Google Scholar] [CrossRef] [Green Version]
- Wu, Q.; Wang, N.; He, T.; Shang, J.; Li, L.; Song, L.; Yang, X.; Li, X.; Luo, N.; Zhang, W.; et al. Thermosensitive hydrogel containing dexamethasone micelles for preventing postsurgical adhesion in a repeated-injury model. Sci. Rep. 2015, 5, 13553. [Google Scholar] [CrossRef] [Green Version]
- Chen, C.H.; Chen, S.H.; Shalumon, K.T.; Chen, J.P. Dual functional core-sheath electrospun hyaluronic acid/polycaprolactone nanofibrous membranes embedded with silver nanoparticles for prevention of peritendinous adhesion. Acta Biomater. 2015, 26, 225–235. [Google Scholar] [CrossRef]
- Peeters, I.; Pien, N.; Mignon, A.; Van Damme, L.; Dubruel, P.; Van Vlierberghe, S.; Mantovani, D.; Vermeulen, V.; Creytens, D.; Van Tongel, A.; et al. Flexor tendon repair using a reinforced tubular, medicated electrospun construct. J. Orthop. Res. 2021, 40, 750–760. [Google Scholar] [CrossRef]
- Liu, S.; Zhao, J.; Ruan, H.; Tang, T.; Liu, G.; Yu, D.; Cui, W.; Fan, C. Biomimetic sheath membrane via electrospinning for antiadhesion of repaired tendon. Biomacromolecules 2012, 13, 3611–3619. [Google Scholar] [CrossRef] [PubMed]
- Chen, S.H.; Chen, C.H.; Shalumon, K.T.; Chen, J.P. Preparation and characterization of antiadhesion barrier film from hyaluronic acid-grafted electrospun poly(caprolactone) nanofibrous membranes for prevention of flexor tendon postoperative peritendinous adhesion. Int. J. Nanomed. 2014, 9, 4079–4092. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Chen, C.H.; Cheng, Y.H.; Chen, S.H.; Chuang, A.D.C.; Chen, J.P. Functional hyaluronic acid-polylactic acid/silver nanoparticles core-sheath nanofiber membranes for prevention of post-operative tendon adhesion. Int. J. Mol. Sci. 2021, 22, 8781. [Google Scholar] [CrossRef] [PubMed]
- Deepthi, S.; Nivedhitha Sundaram, M.; Deepti Kadavan, J.; Jayakumar, R. Layered chitosan-collagen hydrogel/aligned PLLA nanofiber construct for flexor tendon regeneration. Carbohydr. Polym. 2016, 153, 492–500. [Google Scholar] [CrossRef] [PubMed]
- Woythal, L.; Hølmer, P.; Brorson, S. Splints, with or without wrist immobilization, following surgical repair of flexor tendon lesions of the hand: A systematic review. Hand Surg. Rehabil. 2019, 38, 217–222. [Google Scholar] [CrossRef] [PubMed]
- Neiduski, R.L.; Powell, R.K. Flexor tendon rehabilitation in the 21st century: A systematic review. J. Hand Ther. 2019, 32, 165–174. [Google Scholar] [CrossRef]
- Pan, Z.J.; Xu, Y.F.; Pan, L.; Chen, J. Zone 2 flexor tendon repairs using a tensioned strong core suture, sparse peripheral stitches and early active motion: Results in 60 fingers. J. Hand Surg. (Eur. Vol.) 2019, 44, 361–366. [Google Scholar] [CrossRef]
- Silfverskiöld, K.L.; May, E.J. Flexor tendon repair in zone II with a new suture technique and an early mobilization program combining passive and active flexion. J. Hand Surg. Am. 1994, 19, 53–60. [Google Scholar] [CrossRef]
- Silfverskiöld, K.L.; Andersson, C.H. Two new methods of tendon repair: An in vitro evaluation of tensile strength and gap formation. J. Hand Surg. Am. 1993, 18, 58–65. [Google Scholar] [CrossRef]
- Fathy Sadek, A.; Azmy, M.M.; Nady Saleh Elsaid, A.; Zein, A.M.N.; Yehya Hasan, M. Repair of flexor digitorum profundus avulsions including the palmar plate: A retrospective comparative study of 56 cases. J. Hand Surg. (Eur. Vol.) 2022, 17531934221074514. [Google Scholar] [CrossRef] [PubMed]
- Kheiran, A.; Palial, V.; Rollett, R.; Wildin, C.J.; Chatterji, U.; Singh, H.P. Cat bite: An injury not to underestimate. J. Plast. Surg. Hand Surg. 2019, 53, 341–346. [Google Scholar] [CrossRef]
- Malizos, K.N.; Papadopoulou, Z.K.; Ziogkou, A.N.; Rigopoulos, N.; Athanaselis, E.D.; Varitimidis, S.E.; Dailiana, Z.C. Infections of Deep Hand and Wrist Compartments. Microorganisms 2020, 8, 838. [Google Scholar] [CrossRef] [PubMed]
- Pickrell, B.B.; Eberlin, K.R. Secondary Surgery Following Replantation and Revascularization. Hand Clin. 2019, 35, 231–240. [Google Scholar] [CrossRef] [PubMed]
- Mamane, W.; Lippmann, S.; Israel, D.; Ramdhian-Wihlm, R.; Temam, M.; Mas, V.; Pierrart, J.; Masmejean, E.H. Infectious flexor hand tenosynovitis: State of knowledge. A study of 120 cases. J. Orthop. 2018, 15, 701–706. [Google Scholar] [CrossRef] [PubMed]
- Stone, J.F.; Davidson, J.S. The role of antibiotics and timing of repair in flexor tendon injuries of the hand. Ann. Plast. Surg. 1998, 40, 7–13. [Google Scholar] [CrossRef]
- Chapman, T.; Ilyas, A.M. Pyogenic Flexor Tenosynovitis: Evaluation and Treatment Strategies. J. Hand Microsurg. 2019, 11, 121–126. [Google Scholar]
- Chan, E.; Robertson, B.F.; Johnson, S.M. Kanavel signs of flexor sheath infection: A cautionary tale. Br. J. Gen. Pract. J. R. Coll. Gen. Pract. 2019, 69, 315–316. [Google Scholar] [CrossRef]
- Shalumon, K.T.; Sheu, C.; Chen, C.H.; Chen, S.H.; Jose, G.; Kuo, C.Y.; Chen, J.P. Multi-functional electrospun antibacterial core-shell nanofibrous membranes for prolonged prevention of post-surgical tendon adhesion and inflammation. Acta Biomater. 2018, 72, 121–136. [Google Scholar] [CrossRef]
- Bilal, M.; Rasheed, T.; Iqbal, H.M.N.; Li, C.; Hu, H.; Zhang, X. Development of silver nanoparticles loaded chitosan-alginate constructs with biomedical potentialities. Int. J. Biol. Macromol. 2017, 105, 393–400. [Google Scholar] [CrossRef]
- Humayun, A.; Luo, Y.; Elumalai, A.; Mills, D.K. 3D printed antimicrobial PLA constructs functionalised with zinc- coated halloysite nanotubes-Ag-chitosan oligosaccharide lactate. Mater. Technol. 2022, 37, 28–35. [Google Scholar] [CrossRef]
- Khan, F.; Tanaka, M. Designing smart biomaterials for tissue engineering. Int. J. Mol. Sci. 2018, 19, 17. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Silva, M.; Ferreira, F.N.; Alves, N.M.; Paiva, M.C. Biodegradable polymer nanocomposites for ligament/tendon tissue engineering. J. Nanobiotechnol. 2020, 18, 23. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Engineer, C.; Parikh, J.K.; Raval, A. Hydrolytic Degradation Behavior of Biodegradable Polymers from Controlled Drug Delivery System. Trends Biomater. Artif. Organs 2011, 25, 79–85. [Google Scholar]
- Vroman, I.; Tighzert, L. Biodegradable polymers. Materials 2009, 2, 307–344. [Google Scholar] [CrossRef]
- Migliaresi, C.; Fambri, L.; Cohn, D. A study on the in vitro degradation of poly(lactic acid). J. Biomater. Sci. Polym. Ed. 1994, 5, 591–606. [Google Scholar] [CrossRef]
- Duek, E.A.R.; Zavaglia, C.A.C.; Belangero, W.D. In vitro study of poly(lactic acid) pin degradation. Polymer 1999, 40, 6465–6473. [Google Scholar] [CrossRef]
- Jenkins, M.J.; Harrison, K.L. The effect of crystalline morphology on the degradation of polycaprolactone in a solution of phosphate buffer and lipase. Polym. Adv. Technol. 2008, 19, 1901–1906. [Google Scholar] [CrossRef]
- Guo, M.; Chu, Z.; Yao, J.; Feng, W.; Wang, Y.; Wang, L.; Fan, Y. The effects of tensile stress on degradation of biodegradable PLGA membranes: A quantitative study. Polym. Degrad. Stab. 2016, 124, 95–100. [Google Scholar] [CrossRef]
- Fan, Y.B.; Li, P.; Zeng, L.; Huang, X.J. Effects of mechanical load on the degradation of poly(d,l-lactic acid) foam. Polym. Degrad. Stab. 2008, 93, 677–683. [Google Scholar] [CrossRef]
- Cooper, J.A.; Lu, H.H.; Ko, F.K.; Freeman, J.W.; Laurencin, C.T. Fiber-based tissue-engineered scaffold for ligament replacement: Design considerations and in vitro evaluation. Biomaterials 2005, 26, 1523–1532. [Google Scholar] [CrossRef] [PubMed]
- Goh, J.C.; Sahoo, S. Scaffolds for tendon and ligament tissue engineering. In Regenerative Medicine and Biomaterials for the Repair of Connective Tissues; Woodhead Publishing: Sawston, UK, 2010. [Google Scholar]
- Groth, T.; Falck, P.; Miethke, R.-R. Cytotoxicity of Biomaterials—Basic Mechanisms and In Vitro Test Methods: A Review. Altern. Lab. Anim. 1995, 23, 790–799. [Google Scholar] [CrossRef]
- Cannella, V.; Altomare, R.; Leonardi, V.; Russotto, L.; Di Bella, S.; Mira, F.; Guercio, A. In Vitro Biocompatibility Evaluation of Nine Dermal Fillers on L929 Cell Line. Biomed Res. Int. 2020, 2020, 8676343. [Google Scholar] [CrossRef] [PubMed]
- Yang, S.; Leong, K.F.; Du, Z.; Chua, K. The Design of Scaffolds for Use in Tissue Engineering. Part I. Traditional Factors. Tissue Eng. 2002, 7, 679–689. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Song, A.; Rane, A.A.; Christman, K.L. Antibacterial and cell-adhesive polypeptide and poly(ethylene glycol) hydrogel as a potential scaffold for wound healing. Acta Biomater. 2012, 8, 41–50. [Google Scholar] [CrossRef] [Green Version]
- Pring, D.J.; Amis, A.A.; Coombs, R.R.H. The mechanical properties of human flexor tendons in relation to artificial tendons. J. Hand Surg. Br. Eur. Vol. 1985, 10, 331–336. [Google Scholar] [CrossRef]
- Verdan, C.; Potenza, A.D. Tendon Surgery of the Hand. Plast. Reconstr. Surg. 1980, 66, 1493–1503. [Google Scholar] [CrossRef]
- Tang, J.B.; Gu, Y.T.; Rice, K.; Chen, F.; Pan, C.Z. Evaluation of four methods of flexor tendon repair for postoperative active mobilization. Plast. Reconstr. Surg. 2001, 107, 742–749. [Google Scholar] [CrossRef]
- Mano, J.F.; Silva, G.A.; Azevedo, H.S.; Malafaya, P.B.; Sousa, R.A.; Silva, S.S.; Boesel, L.F.; Oliveira, J.M.; Santos, T.C.; Marques, A.P.; et al. Natural origin biodegradable systems in tissue engineering and regenerative medicine: Present status and some moving trends. J. R. Soc. Interface 2007, 4, 999–1030. [Google Scholar] [CrossRef] [Green Version]
- Sensini, A.; Cristofolini, L. Biofabrication of electrospun scaffolds for the regeneration of tendons and ligaments. Materials 2018, 11, 1963. [Google Scholar] [CrossRef] [Green Version]
- Narayanan, N.; Kuang, L.; Del Ponte, M.; Chain, C.; Deng, M. 1—Design and fabrication of nanocomposites for musculoskeletal tissue regeneration. In Nanocomposites for Musculoskeletal Tissue Regeneration; Liu, H., Ed.; Woodhead Publishing: Oxford, UK, 2016; pp. 3–29. ISBN 978-1-78242-452-9. [Google Scholar]
- Smith, B.D.; Grande, D.A. The current state of scaffolds for musculoskeletal regenerative applications. Nat. Rev. Rheumatol. 2015, 11, 213–222. [Google Scholar] [CrossRef] [PubMed]
- Langer, R.; Vacanti, J.P. Tissue Engineering. Science 1993, 260, 920–926. [Google Scholar] [CrossRef] [Green Version]
- Sithole, M.N.; Choonara, Y.E.; du Toit, L.C.; Kumar, P.; Pillay, V. A review of semi-synthetic biopolymer complexes: Modified polysaccharide nano-carriers for enhancement of oral drug bioavailability. Pharm. Dev. Technol. 2017, 22, 283–295. [Google Scholar] [CrossRef] [PubMed]
- Monti, P.; Freddi, G.; Bertoluzza, A.; Kasai, N.; Tsukada, M. Raman spectroscopic studies of silk fibroin from Bombyx mori. J. Raman Spectrosc. 1998, 29, 297–304. [Google Scholar] [CrossRef]
- Vieira, A.C.; Guedes, R.M.; Marques, A.T. Development of ligament tissue biodegradable devices: A review. J. Biomech. 2009, 42, 2421–2430. [Google Scholar] [CrossRef] [Green Version]
- Meinel, L.; Betz, O.; Fajardo, R.; Hofmann, S.; Nazarian, A.; Cory, E.; Hilbe, M.; McCool, J.; Langer, R.; Vunjak-Novakovic, G.; et al. Silk based biomaterials to heal critical sized femur defects. Bone 2006, 39, 922–931. [Google Scholar] [CrossRef]
- Zhao, H.; Guan, H.G.; Gu, J.; Luo, Z.P.; Zhang, W.; Chen, B.; Gu, Q.L.; Yang, H.L.; Shi, Q. Collagen membrane alleviates peritendinous adhesion in the rat Achilles tendon injury model. Chin. Med. J. 2013, 126, 729–733. [Google Scholar] [CrossRef]
- Turner, J.B.; Corazzini, R.L.; Butler, T.J.; Garlick, D.S.; Rinker, B.D. Evaluating adhesion reduction efficacy of type I/III collagen membrane and collagen-GAG resorbable matrix in primary flexor tendon repair in a chicken model. Hand 2015, 10, 482–488. [Google Scholar] [CrossRef] [Green Version]
- Wichelhaus, D.A.; Beyersdoerfer, S.T.; Gierer, P.; Vollmar, B.; Mittlmeier, T. The effect of a collagen-elastin matrix on adhesion formation after flexor tendon repair in a rabbit model. Arch. Orthop. Trauma Surg. 2016, 136, 1021–1029. [Google Scholar] [CrossRef]
- Seo, Y.K.; Kim, J.H.; Eo, S.R. Co-effect of silk and amniotic membrane for tendon repair. J. Biomater. Sci. Polym. Ed. 2016, 27, 1232–1247. [Google Scholar] [CrossRef]
- Hortensius, R.A.; Ebens, J.H.; Dewey, M.J.; Harley, B.A.C. Incorporation of the Amniotic Membrane as an Immunomodulatory Design Element in Collagen Scaffolds for Tendon Repair. ACS Biomater. Sci. Eng. 2018, 4, 4367–4377. [Google Scholar] [CrossRef] [PubMed]
- Zukawa, M.; Okabe, M.; Osada, R.; Makino, H.; Nogami, M.; Seki, S.; Yoshida, T.; Kimura, T.; Kawaguchi, Y. Effect of hyperdry amniotic membrane in preventing tendon adhesion in a rabbit model. J. Orthop. Sci. 2021, in press. [CrossRef] [PubMed]
- Prakash, S.; Kalra, P.; Dhal, A. Flexor tendon repair with amniotic membrane. Int. Orthop. 2020, 44, 2037–2045. [Google Scholar] [CrossRef] [PubMed]
- Cristino, S.; Grassi, F.; Toneguzzi, S.; Piacentini, A.; Grigolo, B.; Santi, S.; Riccio, M.; Tognana, E.; Facchini, A.; Lisignoli, G. Analysis of mesenchymal stem cells grown on a three-dimensional HYAFF 11-based prototype ligament scaffold. J. Biomed. Mater. Res. A 2005, 73, 275–283. [Google Scholar] [CrossRef] [PubMed]
- Patterson, J.; Siew, R.; Herring, S.W.; Lin, A.S.P.; Guldberg, R.; Stayton, P.S. Hyaluronic acid hydrogels with controlled degradation properties for oriented bone regeneration. Biomaterials 2010, 31, 6772–6781. [Google Scholar] [CrossRef] [Green Version]
- Yilmaz, E.; Avci, M.; Bulut, M.; Kelestimur, H.; Karakurt, L.; Ozercan, I. The Effect of Seprafilm on Adhesion Formation and Tendon Healing After Flexor Tendon Repair in Chicken. Orthopedics 2010, 33, 164–170. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Işik, S.; Öztürk, S.; Gürses, S.; Yetmez, M.; Güler, M.M.; Selmanpakoglu, N.; Günhan, Ö. Prevention of restrictive adhesions in primary tendon repair by HA-membrane: Experimental research in chickens. Br. J. Plast. Surg. 1999, 52, 373–379. [Google Scholar] [CrossRef]
- Na, S.Y.; Oh, S.H.; Song, K.S.; Lee, J.H. Hyaluronic acid/mildly crosslinked alginate hydrogel as an injectable tissue adhesion barrier. J. Mater. Sci. Mater. Med. 2012, 23, 2303–2313. [Google Scholar] [CrossRef]
- Sun, J.; Tan, H. Alginate-Based Biomaterials for Regenerative Medicine Applications. Materials 2013, 6, 1285–1309. [Google Scholar] [CrossRef]
- Namba, J.; Shimada, K.; Saito, M.; Murase, T.; Yamada, H.; Yoshikawa, H. Modulation of peritendinous adhesion formation by alginate solution in a rabbit flexor tendon model. J. Biomed. Mater. Res. Part B Appl. Biomater. 2007, 80, 273–279. [Google Scholar] [CrossRef]
- Shao, H.J.; Lee, Y.T.; Chen, C.S.; Wang, J.H.; Young, T.H. Modulation of gene expression and collagen production of anterior cruciate ligament cells through cell shape changes on polycaprolactone/chitosan blends. Biomaterials 2010, 31, 4695–4705. [Google Scholar] [CrossRef] [PubMed]
- Xia, C.-S.; Hong, G.-X.; Dou, R.-R.; Yang, X.-Y. Effects of chitosan on cell proliferation and collagen production of tendon sheath fibroblasts, epitenon tenocytes, and endotenon tenocytes. Chin. J. Traumatol. (Zhonghua Chuang Shang Za Zhi) 2005, 8, 369–374. [Google Scholar] [PubMed]
- Chen, Q.; Lu, H.U.I.; Yang, H.U. Chitosan prevents adhesion during rabbit flexor tendon repair via the sirtuin 1 signaling pathway. Mol. Med. Rep. 2015, 12, 4598–4603. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Radwan, M.A.; Farrag, S.A.A.; Abu-Elamayem, M.M.; Ahmed, N.S. Extraction, characterization, and nematicidal activity of chitin and chitosan derived from shrimp shell wastes. Biol. Fertil. Soils 2012, 48, 463–468. [Google Scholar] [CrossRef]
- Busch, F.; Mobasheri, A.; Shayan, P.; Stahlmann, R.; Shakibaei, M. Sirt-1 is required for the inhibition of apoptosis and inflammatory responses in human tenocytes. J. Biol. Chem. 2012, 287, 25770–25781. [Google Scholar] [CrossRef] [Green Version]
- Chen, C.H.; Chen, S.H.; Mao, S.H.; Tsai, M.J.; Chou, P.Y.; Liao, C.H.; Chen, J.P. Injectable thermosensitive hydrogel containing hyaluronic acid and chitosan as a barrier for prevention of postoperative peritoneal adhesion. Carbohydr. Polym. 2017, 173, 721–731. [Google Scholar] [CrossRef]
- Yousefi, A.; Sarrafzadeh-Rezaei, F.; Asri-Rezaei, S.; Farshid, A.-A.; Behfar, M. Fabrication of novel tubular scaffold for tendon repair from chitosan in combination with zinc oxide nanoparticles. Vet. Res. Forum 2018, 9, 105–111. [Google Scholar] [CrossRef]
- Jayasuriya, A.C.; Aryaei, A.; Jayatissa, A.H. ZnO nanoparticles induced effects on nanomechanical behavior and cell viability of chitosan films. Mater. Sci. Eng. C Mater. Biol. Appl. 2013, 33, 3688–3696. [Google Scholar] [CrossRef] [Green Version]
- Saper, R.B.; Rash, R. Zinc: An essential micronutrient. Am. Fam. Physician 2009, 79, 768–772. [Google Scholar]
- Sudheesh Kumar, P.T.; Lakshmanan, V.-K.; Anilkumar, T.V.; Ramya, C.; Reshmi, P.; Unnikrishnan, A.G.; Nair, S.V.; Jayakumar, R. Flexible and Microporous Chitosan Hydrogel/Nano ZnO Composite Bandages for Wound Dressing: In Vitro and In Vivo Evaluation. ACS Appl. Mater. Interfaces 2012, 4, 2618–2629. [Google Scholar] [CrossRef]
- Ganji, F.; Abdekhodaie, M.J.; Ramazani, A. Gelation time and degradation rate of chitosan-based injectable hydrogel. J. Sol-Gel Sci. Technol. 2007, 42, 47–53. [Google Scholar] [CrossRef]
- Yang, Q.Q.; Zhang, L.; Ju, F.; Zhou, Y.L. Sustained-Release Hydrogel-Based Rhynchophylline Delivery System Improved Injured Tendon Repair. Colloids Surf. B BioInterfaces 2021, 205, 111876. [Google Scholar] [CrossRef] [PubMed]
- Ahmed, E.M. Hydrogel: Preparation, characterization, and applications: A review. J. Adv. Res. 2015, 6, 105–121. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Liao, J.C.Y.; He, M.; Gan, A.W.T.; Wen, F.; Tan, L.P.; Chong, A.K.S. The effects of bi-functional anti-adhesion scaffolds on flexor tendon healing in a rabbit model. J. Biomed. Mater. Res. Part B Appl. Biomater. 2018, 106, 2605–2614. [Google Scholar] [CrossRef]
- Nifant’ev, I.; Ivchenko, P. Coordination ring-opening polymerization of cyclic esters: A critical overview of DFT modeling and visualization of the reaction mechanisms. Molecules 2019, 24, 4117. [Google Scholar] [CrossRef] [Green Version]
- Kade, J.C.; Dalton, P.D. Polymers for Melt Electrowriting. Adv. Healthc. Mater. 2021, 10, 2001232. [Google Scholar] [CrossRef]
- King, W.E.; Bowlin, G.L. Near-Field Electrospinning and Melt Electrowriting of Biomedical Polymers—Progress and Limitations. Polymers 2021, 13, 1097. [Google Scholar] [CrossRef]
- Chiulan, I.; Frone, A.N.; Brandabur, C.; Panaitescu, D.M. Recent Advances in 3D Printing of Aliphatic Polyesters. Bioengineering 2018, 5, 2. [Google Scholar] [CrossRef] [Green Version]
- Jain, S.; Fuoco, T.; Yassin, M.A.; Mustafa, K.; Finne-Wistrand, A. Printability and Critical Insight into Polymer Properties during Direct-Extrusion Based 3D Printing of Medical Grade Polylactide and Copolyesters. Biomacromolecules 2020, 21, 388–396. [Google Scholar] [CrossRef]
- Vieira, A.F.C.; Vieira, J.F.C.; Marques, A.T.; Guedes, R.M. Biomechanics of biomaterials used in soft tissue regenerative medicine. Biomecánica 2009, 17, 7–14. [Google Scholar] [CrossRef]
- Liu, S.; Qin, M.; Hu, C.; Wu, F.; Cui, W.; Jin, T.; Fan, C. Tendon healing and anti-adhesion properties of electrospun fibrous membranes containing bFGF loaded nanoparticles. Biomaterials 2013, 34, 4690–4701. [Google Scholar] [CrossRef] [PubMed]
- Liu, S.; Pan, G.; Liu, G.; das Neves, J.; Song, S.; Chen, S.; Cheng, B.; Sun, Z.; Sarmento, B.; Cui, W.; et al. Electrospun fibrous membranes featuring sustained release of ibuprofen reduce adhesion and improve neurological function following lumbar laminectomy. J. Control. Release 2017, 264, 1–13. [Google Scholar] [CrossRef] [PubMed]
- Wang, W.; Wang, Y.; Lou, T.; Ding, M.; Li, J.; Xiong, H.; Yao, Z.; Ma, Y.; Chen, H.; Liu, S. Celecoxib-Loaded Electrospun Fibrous Antiadhesion Membranes Reduce COX-2/PGE2 Induced Inflammation and Epidural Fibrosis in a Rat Failed Back Surgery Syndrome Model. Neural Plast. 2021, 2021, 6684176. [Google Scholar] [CrossRef]
- Gunasekaran, T.; Nigusse, T.; Dhanaraju, M.D. Silver Nanoparticles as Real Topical Bullets for Wound Healing. J. Am. Coll. Clin. Wound Spec. 2011, 3, 82–96. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Ge, L.; Li, Q.; Wang, M.; Ouyang, J.; Li, X.; Xing, M.M.Q. Nanosilver particles in medical applications: Synthesis, performance, and toxicity. Int. J. Nanomed. 2014, 9, 2399–2407. [Google Scholar] [CrossRef] [Green Version]
- Wong, K.K.Y.; Liu, X. Silver nanoparticles—The real “silver bullet” in clinical medicine? Med. Chem. Commun. 2010, 1, 125–131. [Google Scholar] [CrossRef]
- Chen, C.H.; Chen, S.H.; Shalumon, K.T.; Chen, J.P. Prevention of peritendinous adhesions with electrospun polyethylene glycol/polycaprolactone nanofibrous membranes. Colloids Surf. B Biointerfaces 2015, 133, 221–230. [Google Scholar] [CrossRef]
- Malikmammadov, E.; Tanir, T.E.; Kiziltay, A.; Hasirci, V.; Hasirci, N. PCL and PCL-based materials in biomedical applications. J. Biomater. Sci. Polym. Ed. 2018, 29, 863–893. [Google Scholar] [CrossRef]
- Liu, C.; Tian, S.; Bai, J.; Yu, K.; Liu, L.; Liu, G.; Dong, R.; Tian, D. Regulation of ERK1/2 and SMAD2/3 pathways by using multi-layered electrospun PCL–amnion nanofibrous membranes for the prevention of post-surgical tendon adhesion. Int. J. Nanomed. 2020, 15, 927–942. [Google Scholar] [CrossRef] [Green Version]
- Yu, H.; Mei, S.; Zhao, L.; Zhao, M.; Wang, Y.; Zhu, H.; Wang, Y.; Wu, J.; Cui, C.; Xu, W.; et al. RGD-peptides modifying dexamethasone: To enhance the anti-inflammatory efficacy and limit the risk of osteoporosis. Medchemcomm 2015, 6, 1345–1351. [Google Scholar] [CrossRef]
- The Manchester General Practitioner Group. A study of naproxen and ibuprofen in patients with osteoarthritis seen in general practice. Curr. Med. Res. Opin. 1984, 9, 41–46. [Google Scholar] [CrossRef] [PubMed]
- Cooper, S.A.; Desjardins, P.; Brain, P.; Paredes-Diaz, A.; Troullos, E.; Centofanti, R.; An, B. Longer analgesic effect with naproxen sodium than ibuprofen in post-surgical dental pain: A randomized, double-blind, placebo-controlled, single-dose trial. Curr. Med. Res. Opin. 2019, 35, 2149–2158. [Google Scholar] [CrossRef] [PubMed]
- Seager, J.M.; Cullen, D.J.; Pearson, G.; Holmes, S.; Doherty, M.; Wilson, J.V.; Garrud, P.; Garner, S.; Maynard, A.; Logan, R.F.; et al. Ibuprofen versus other non-steroidal anti-inflammatory drugs: Use in general practice and patient perception. Aliment. Pharmacol. Ther. 2000, 14, 187–191. [Google Scholar] [CrossRef] [PubMed]
- Chen, C.H.; Li, D.L.; Chuang, A.D.C.; Dash, B.S.; Chen, J.P. Tension stimulation of tenocytes in aligned hyaluronic acid/platelet-rich plasma-polycaprolactone core-sheath nanofiber membrane scaffold for tendon tissue engineering. Int. J. Mol. Sci. 2021, 22, 11215. [Google Scholar] [CrossRef]
- Yoshimi, R.; Yamada, Y.; Ito, K.; Nakamura, S.; Abe, A.; Nagasaka, T.; Okabe, K.; Kohgo, T.; Baba, S.; Ueda, M. Self-Assembling Peptide Nanofiber Scaffolds, Platelet-Rich Plasma, and Mesenchymal Stem Cells for Injectable Bone Regeneration with Tissue Engineering. J. Craniofac. Surg. 2009, 20, 1523–1530. [Google Scholar] [CrossRef]
- Wang, X.; Qiu, Y.; Triffitt, J.; Carr, A.; Xia, Z.; Sabokbar, A. Proliferation and differentiation of human tenocytes in response to platelet rich plasma: An in vitro and in vivo study. J. Orthop. Res. Off. Publ. Orthop. Res. Soc. 2012, 30, 982–990. [Google Scholar] [CrossRef]
- Liu, S.; Wu, F.; Gu, S.; Wu, T.; Chen, S.; Chen, S.; Wang, C.; Huang, G.; Jin, T.; Cui, W.; et al. Gene Silencing via PDA/ERK2-siRNA-Mediated Electrospun Fibers for Peritendinous Antiadhesion. Adv. Sci. 2019, 6, 1801217. [Google Scholar] [CrossRef]
- Heidenreich, O. Targeting oncogenes with siRNAs. Methods Mol. Biol. 2009, 487, 221–242. [Google Scholar] [CrossRef]
- Kurrikoff, K.; Gestin, M.; Langel, Ü. Recent in vivo advances in cell-penetrating peptide-assisted drug delivery. Expert Opin. Drug Deliv. 2016, 13, 373–387. [Google Scholar] [CrossRef]
- Gwak, S.-J.; Nice, J.; Zhang, J.; Green, B.; Macks, C.; Bae, S.; Webb, K.; Lee, J.S. Cationic, amphiphilic copolymer micelles as nucleic acid carriers for enhanced transfection in rat spinal cord. Acta Biomater. 2016, 35, 98–108. [Google Scholar] [CrossRef] [Green Version]
- Xiang, B.; Jia, X.-L.; Qi, J.-L.; Yang, L.-P.; Sun, W.-H.; Yan, X.; Yang, S.-K.; Cao, D.-Y.; Du, Q.; Qi, X.-R. Enhancing siRNA-based cancer therapy using a new pH-responsive activatable cell-penetrating peptide-modified liposomal system. Int. J. Nanomed. 2017, 12, 2385–2405. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Hinterleitner, R.; Gruber, T.; Pfeifhofer-Obermair, C.; Lutz-Nicoladoni, C.; Tzankov, A.; Schuster, M.; Penninger, J.M.; Loibner, H.; Lametschwandtner, G.; Wolf, D.; et al. Adoptive transfer of siRNA Cblb-silenced CD8+ T lymphocytes augments tumor vaccine efficacy in a B16 melanoma model. PLoS ONE 2012, 7, e44295. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Yeh, Y.-C.; Huang, T.-H.; Yang, S.-C.; Chen, C.-C.; Fang, J.-Y. Nano-Based Drug Delivery or Targeting to Eradicate Bacteria for Infection Mitigation: A Review of Recent Advances. Front. Chem. 2020, 8, 286. [Google Scholar] [CrossRef] [PubMed]
- Yoshizaki, Y.; Yuba, E.; Komatsu, T.; Udaka, K.; Harada, A.; Kono, K. Improvement of Peptide-Based Tumor Immunotherapy Using pH-Sensitive Fusogenic Polymer-Modified Liposomes. Molecules 2016, 21, 1284. [Google Scholar] [CrossRef] [Green Version]
- Gandhi, A.; Paul, A.; Sen, S.O.; Sen, K.K. Studies on thermoresponsive polymers: Phase behaviour, drug delivery and biomedical applications. Asian J. Pharm. Sci. 2015, 10, 99–107. [Google Scholar] [CrossRef] [Green Version]
- Dong, M.; Shi, B.; Liu, D.; Liu, J.-H.; Zhao, D.; Yu, Z.-H.; Shen, X.-Q.; Gan, J.-M.; Shi, B.; Qiu, Y.; et al. Conductive Hydrogel for a Photothermal-Responsive Stretchable Artificial Nerve and Coalescing with a Damaged Peripheral Nerve. ACS Nano 2020, 14, 16565–16575. [Google Scholar] [CrossRef]
- Zhang, K.; Lv, H.; Zheng, Y.; Yao, Y.; Li, X.; Yu, J.; Ding, B. Nanofibrous hydrogels embedded with phase-change materials: Temperature-responsive dressings for accelerating skin wound healing. Compos. Commun. 2021, 25, 100752. [Google Scholar] [CrossRef]


| Year | Material and Structure | Material Processing Technique | Mechanical Response 1 | Biological Response 1 | Ref. |
|---|---|---|---|---|---|
| 1999 | Membrane of HA | Crosslinking | - | Decrease in adhesion formation | [163] |
| 2006 | Coating of ALG solution | Sodium ALG derived from Lassonia nigrescens, non-crosslinked and sterilized | Higher flexion region | Decrease in scar tissue formation Tendon healing with longitudinal remodeling compared to random remodeling in control | [166] |
| 2010 | Membrane of HA | - | Increased UTS | Decrease in adhesion formation | [162] |
| 2012 | Hydrogel of mildly crosslinked ALG embedded with HA (HA/mcALG) | Crosslinking | Sustained release of HA | Slower degradation rate of HA/mcALG compared to the pure HA hydrogel Decrease in adhesion formation for both HA as well as HA/mcALG constructs | [164] |
| 2013 | Membrane of collagen | Bovine derived, freeze-dried, and sterilized | Increased UTS after 8 weeks | Decrease in adhesion formation | [153] |
| 2015 | Membrane of collagen | Porcine derived, sterilized, and rehydrated | - | Decrease in adhesion formation for both the collagen membrane and collagen-GAG matrix sheet | [154] |
| Porous matrix sheet of Collagen-GAG | Crosslinked and rehydrated | ||||
| 2015 | Hydrogel of CHI | - | Increased UTS | Decrease in adhesion formation CHI-induced SIRT1 protein expression | [169] |
| 2016 | Membrane of collagen/elastin | Matriderm® | Increased gapping | Decrease in adhesion formation | [155] |
| 2016 | Amnionic membrane combined with silk | Sericin removed by solution, soaked in 1% collagen/HA, and dried, freeze-dried, and sterilized. Amnionic membranes harvested from human placenta | Increased UTS | No immigration of inflammatory cells or fibroblast-like cells Formation of new blood vessels | [156] |
| 2017 | Thermoresponsive hydrogel of HA-CHI-PNIPAm | Copolymer by grafting CHI on PNIPAm whereafter dissolved in HA solution | Sol-gel in-situ transition at an LCST of 31.4 °C | Decrease in adhesion formation Decrease in fibroblast migration Limited cytotoxicity | [172] |
| 2018 | Tubular construct of CHI with zinc oxide nanoparticles | Mold with CHI solution containing ZnO NP followed by freeze-drying | Complete biodegradation in 8 weeks | Decrease in adhesion Improved gliding Improved collagen synthesis due to Zn | [173] |
| 2021 | Hydrogel of HA embedded with rhynchophylline | Crosslinking | Sustained release of rhynchophylline Increased healing strength | Decrease in adhesion formation Increased expression of type I and III collagen Increased gliding excursion | [178] |
| Year | Material and Structure | Chemical/Biological Modulation and Concentration | Material Processing Technique | Mechanical Response 1 | Biological Response 1 | Ref. |
|---|---|---|---|---|---|---|
| 2013 | NFM of PLLA | bFGFs loaded in DGNs | Electrospinning | Blending of DGNs decreased UTS and maximum elongation | Improved cell proliferation Improved intrinsic tendon healing | [187] |
| 2013 | NFM of PLLA-b-PELA | IBU | Electrospinning | - | Idem [187] Decrease in inflammation and adhesion formation | [95] |
| 2013 | NFM of PLLA–MMS | IBU | Electrospinning | Controlled release of IBU, without initial burst | Idem [95] | [96] |
| 2014 | NFM of PLLA-c-PELA | Celecoxib | Electrospinning | Controlled release of celecoxib | Idem [95] Decreased expression of type I and type III collagen | [101] |
| 2014 | NFM of PLLA | IBU + Ag NPs | Electrospinning | Controlled release of IBU, without initial burst | Idem [95] Antimicrobial response | [94] |
| 2015 | NFM of PCL/PEG blend (0, 25, 50 and 75 wt% PEG) | - | Electrospinning | Increasing wt% PEG decreased UTS and maximum elongation | Decrease in adhesion formation Higher PEG wt% led to decreased fibroblast attachment Good permeability for nutrients, growth factors, and cytokines | [193] |
| 2015 | Hydrogel of PLGA-PEG-PLGA | 5-Fluorouracil | - | Sol-gel phase transition depending on temperature | Decrease in adhesion formation Full in vivo degradation in 28 days | [99] |
| 2015 | Hydrogel of PEG-b-PLC-b-PEG | DEX micelles | PEG-b-PLC-b-PEG dissolved in saline at 4 °C | Sol-gel phase transition depending on temperature | Decrease in adhesion formation Low cytotoxicity of hydrogel and micelles Full in vivo degradation in 20 days | [103] |
| 2017 | NFM of PLGA | IBU | Electrospinning of PCL Amniotic membrane was freeze-dried and decellularized | Increased UTS Sustainable release of IBU | Decrease in adhesion formation Inhibition of fibrosis via the COX2 pathway Reduced pain and neurological deficits | [188] |
| 2020 | MNFM of an amniotic membrane between two layers of PCL | bFGFs | Electrospinning | Increased work of flexion Decreased UTS | Increased phosphorylation of ERK1/2 and SMAD2/3 Enhanced collagen synthesis | [195] |
| 2021 | MNFM of PCL/AUP outer layer and inner layer, with braided monofilament PE as middle layer | Naproxen and HA loaded in PCL/AUP | Electrospinning | Significant increase in UTS No degradation prior to 9 weeks | Decrease in adhesion formation naproxen introduced no cytotoxicity | [93,105] |
| Year | Material and Structure | Chemical/Biological Modulation and Concentration | Material Processing Technique | Mechanical Response 1 | Biological Response 1 | Ref. |
|---|---|---|---|---|---|---|
| 2012 | CSNFM of PCL shell with a HA/PCL core | HA | Sequential and microgel electrospinning | Increasing wt% HA decreased UTS | Decrease in adhesion formation Increased wt% HA resulted in higher cell viability and cell proliferation after 1 day in culture | [106] |
| 2014 | NFM of PCL-sg-CHI | CHI | Electrospinning | Increased UTS for healed flexor tendons treated with the PCL-g-CHI membrane compared to Seprafilm and PCL membrane | Decrease in adhesion formation CHI showed no cytotoxicity | [19] |
| 2014 | NFM PCL-sg-HA | HA | Electrospinning | Increased UTS, maximum elongation, and Young’s modulus for PCL-g-HA compared to PCL | Decrease in adhesion formation Unaffected cell proliferation | [107] |
| 2015 | CSNFM of PCL shell with a HA core | Ag NPs + HA | Co-axial electrospinning | Decreased pull-out force for HA/PCL+Ag NPs Increased UTS for healed tendons treated with HA/PCL+Ag NPs compared to PCL membrane | Decrease in adhesion formation Ag NPs as an antimicrobial effect without significant cytotoxicity | [104] |
| 2015 | MNFM of PELA outer layer, HA middle layer, and PELA inner layer | HA + Celecoxib | Sequential electrospinning | Lower work of flexion | Decrease in adhesion formation Good permeability for nutrients, growth factors, and cytokines | [102] |
| 2016 | NFM of PLLA blended with collagen/CHI hydrogel, coated with ALG | CHI + ALG | Microgel electrospinning and solution coating | - | Decrease in adhesion formation Promotion of tendon gliding | [109] |
| 2016 | CSNFM with celecoxib loaded PELA shell with a HA/PELA core | Celecoxib + HA | Microgel and sequential electrospinning | No decrease in mechanical properties due to the use of celecoxib | Decrease in adhesion formation Promotion of tendon gliding Decreased expression of type I and type III collagen Decrease in cell proliferation | [100] |
| 2018 | CSNFM of PCL/PEG shell with HA core | HA embedded with IBU and PCL/PEG loaded with Ag NPs | Co-axial electrospinning | Elongation at break decreased and Young’s modulus and UTS increased for higher IBU wt% IBU showed fast release during first 8 h, but slows down over time | Decrease in adhesion formation Reduced fibroblast attachment and proliferation Higher IBU concentrations lead to substantial cytotoxicity in vitro and in vivo Promotion of tendon gliding Ag NPs as an antimicrobial effect without additional cytotoxicity | [123] |
| 2018 | NFM of PLCL-sg-HA | HA | Electrospinning | Decreased UTS Release rate of HA was controlled by sheath thickness | Decrease in adhesion formation Prevention of penetrating fibroblasts | [180] |
| 2019 | NFM of HA | IBU | Electrospinning followed by covalently crosslinking to BDDE and ionic crosslinking to FeCl3 | Higher IBU loading increased UTS and Young’s modulus | Decrease in adhesion formation Prevention of cell attachment and penetration | [98] |
| 2019 | NFM of PLLA-HA | PDA loaded with ERK2-siRNA + HA | Electrospinning | Cumulative release of 80% ERK2-siRNA in 30 days | Decreased expression of type I and type III collagen Decrease in cell proliferation | [203] |
| 2021 | CSNFM of PLA shell with HA core | PLA loaded with Ag NPs + HA | Co-axial electrospinning | Sustainable release of HA | Best decrease in adhesion formation observed for thin shell fibers Ag NPs as an antimicrobial effect | [108] |
| 2021 | CSNFM of PCL shell with HA core | HA loaded with PRP | Co-axial electrospinning | Controlled release of proteins from PRP | Aligned fibers provided optimal cell proliferation Aligned fibers provided increase in type I and decrease in type III collagen Ag NPs as an antimicrobial effect without additional cytotoxicity | [200] |
| 2021 | NFM of PLGA coated with PEG-PLV hydrogel | IBU + bFGFs | Electrospinning followed by hydrogel coating | No obvious effect on tendon mechanical properties | Decrease in adhesion formation Increased expression of type I and III collagen | [97] |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Brebels, J.; Mignon, A. Polymer-Based Constructs for Flexor Tendon Repair: A Review. Polymers 2022, 14, 867. https://doi.org/10.3390/polym14050867
Brebels J, Mignon A. Polymer-Based Constructs for Flexor Tendon Repair: A Review. Polymers. 2022; 14(5):867. https://doi.org/10.3390/polym14050867
Chicago/Turabian StyleBrebels, Jef, and Arn Mignon. 2022. "Polymer-Based Constructs for Flexor Tendon Repair: A Review" Polymers 14, no. 5: 867. https://doi.org/10.3390/polym14050867
APA StyleBrebels, J., & Mignon, A. (2022). Polymer-Based Constructs for Flexor Tendon Repair: A Review. Polymers, 14(5), 867. https://doi.org/10.3390/polym14050867







