Prototypes of User Interfaces for Mobile Applications for Patients with Diabetes
Abstract
:1. Introduction
2. Current Mobile Application for Diabetes Mellitus
3. Methods
3.1. Study Design
3.2. Data Analysis
3.3. Data Calculation
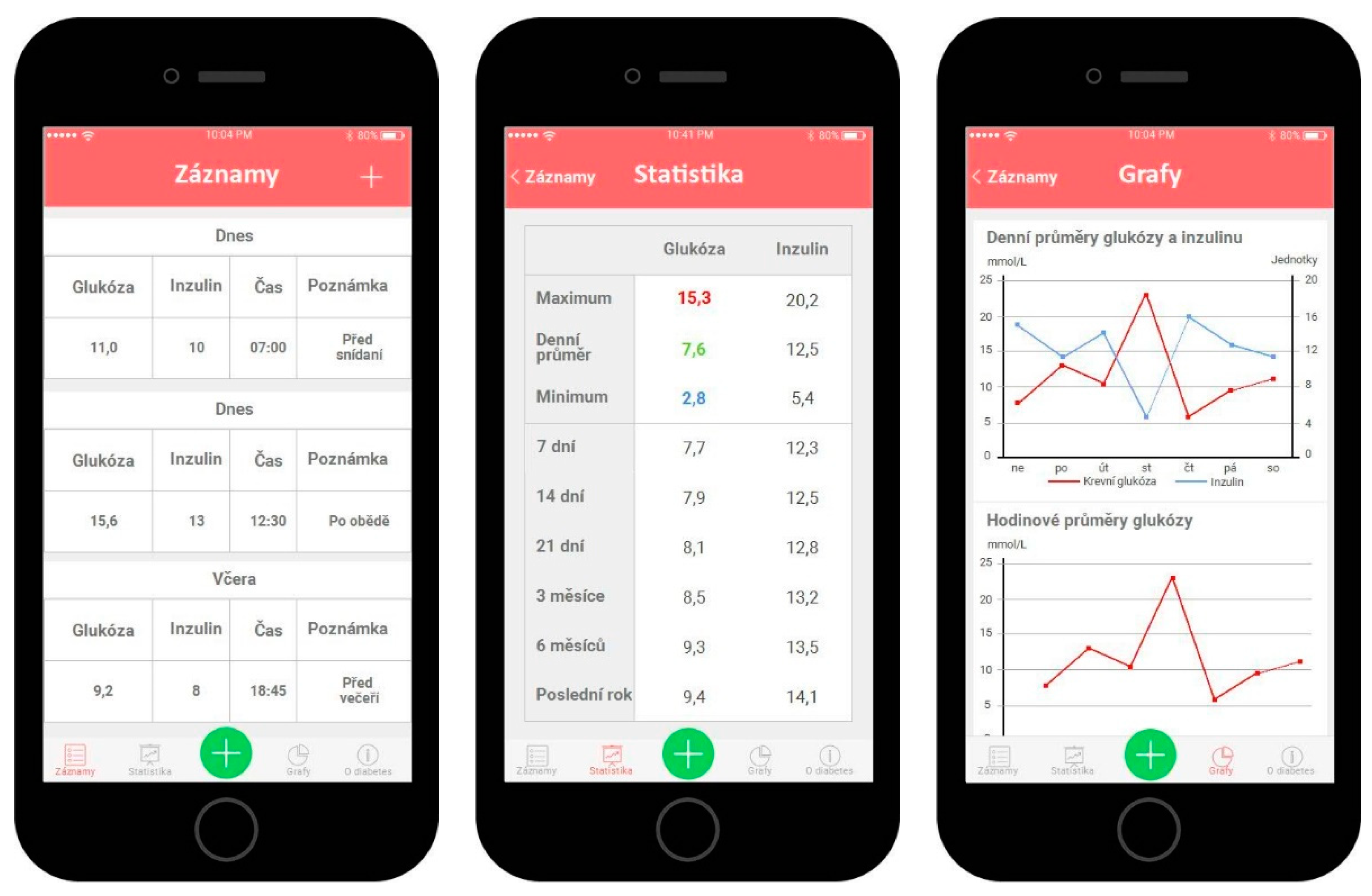
3.3.1. A Prototype according to the Current State of the Applications
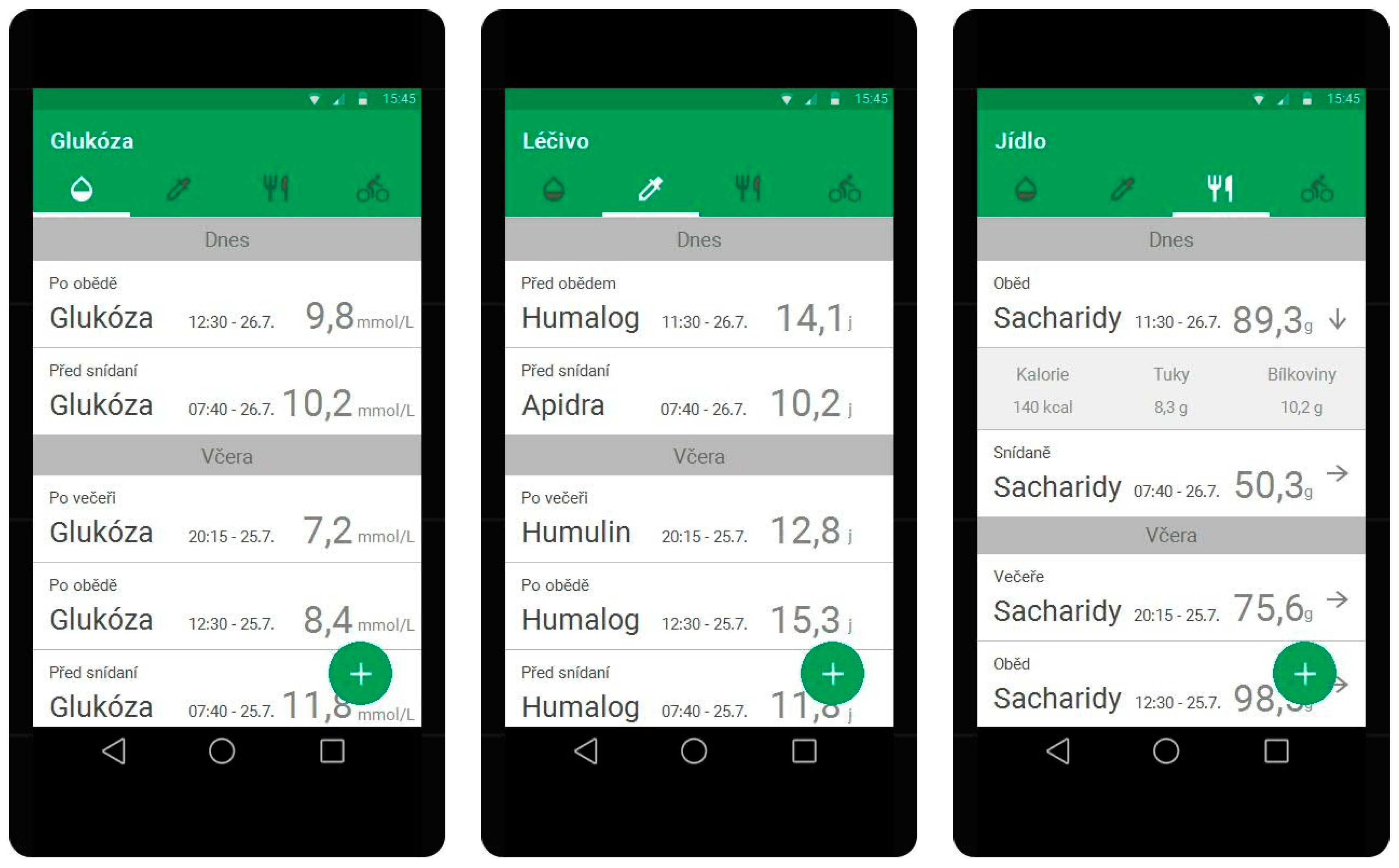
3.3.2. A Prototype with Key Functions
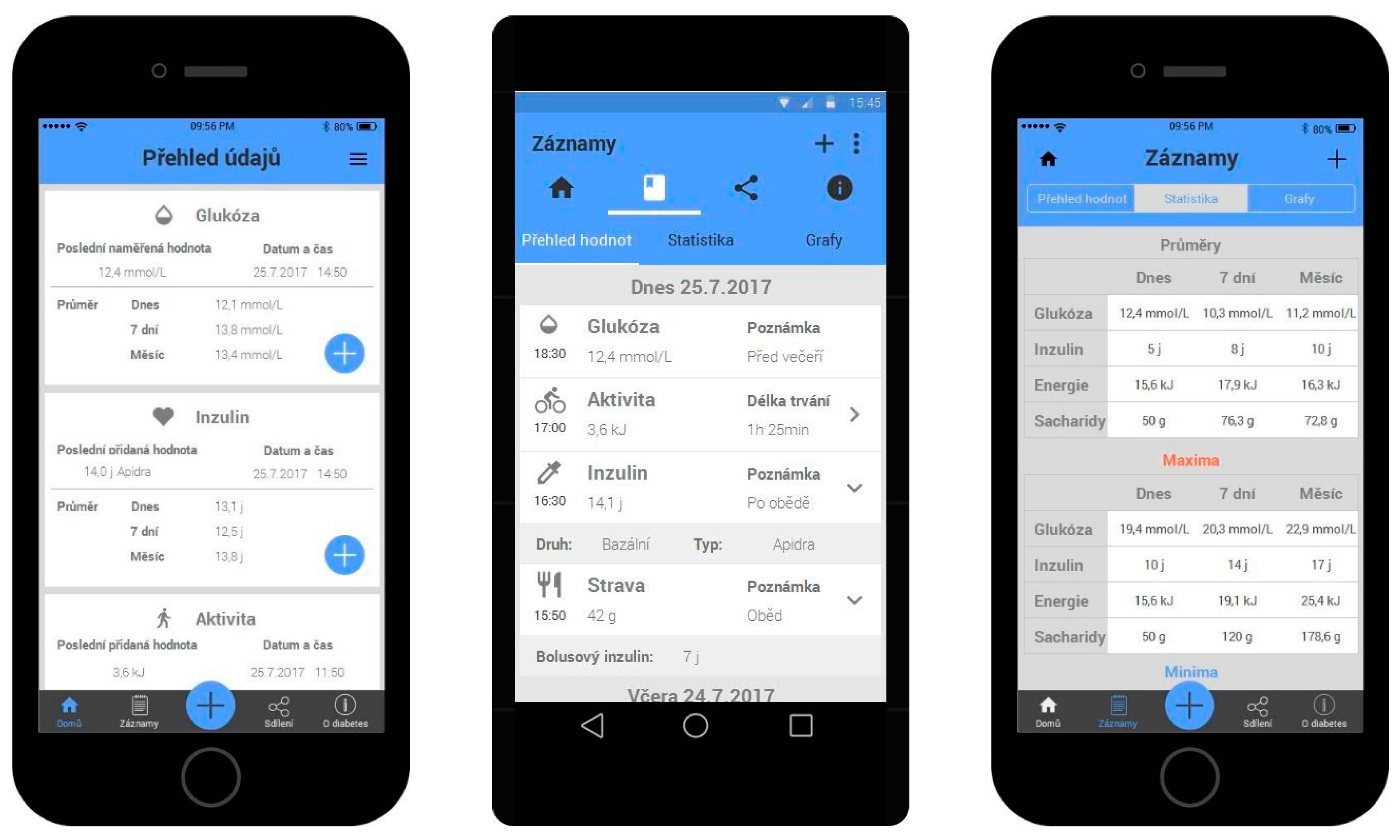
3.3.3. A Prototype with Extra Functions
3.4. Formulated Assumptions
4. Solution Testing Developed
4.1. Respondent Sample Description
4.2. Health and Technical Information Overview
4.3. Overview of Responses Concerning the Application Prototypes
5. Discussion
- functions that support personalized feedback,
- informative functions intended to modify the user’s behavior in keeping with the limitations imposed by the disease,
- and functions that exploit the communication potential of smartphones.
6. Conclusions
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- Pires, I.M.; Garcia, N.M.; Pombo, N.; Florez-Revuelta, F.; Spinsante, S. Approach for the Development of a Framework for the Identification of Activities of Daily Living Using Sensors in Mobile Devices. Sensors 2018, 18, 640. [Google Scholar] [CrossRef]
- Zdravevski, E.; Lameski, P.; Trajkovik, V.; Kulakov, A.; Chorbev, I.; Goleva, R.; Pombo, N.; Garcia, N. Improving Activity Recognition Accuracy in Ambient-Assisted Living Systems by Automated Feature Engineering. IEEE Access 2017, 5, 5262–5280. [Google Scholar] [CrossRef] [Green Version]
- Cui, M.; Wu, X.; Mao, J.; Wang, X.; Nie, M. T2DM Self-Management via Smartphone Applications: A Systematic Review and Meta-Analysis. PLoS ONE 2016, 11, e0166718. [Google Scholar] [CrossRef] [PubMed]
- Mosa, A.S.M.; Yoo, I.; Sheets, L. A Systematic Review of Healthcare Applications for Smartphones. BMC Med. Inform. Decis. Mak. 2012, 12, 67. [Google Scholar] [CrossRef]
- Chomutare, T.; Fernandez-Luque, L.; Arsand, E.; Hartvigsen, G. Features of Mobile Diabetes Applications: Review of the Literature and Analysis of Current Applications Compared Against Evidence-Based Guidelines. J. Med. Internet Res. 2011, 13, e65. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Cafazzo, J.A.; Casselman, M.; Hamming, N.; Katzman, D.K.; Palmert, M.R. Design of an mHealth App for the Self-management of Adolescent Type 1 Diabetes: A Pilot Study. J. Med. Internet Res. 2012, 14, 171–183. [Google Scholar] [CrossRef]
- Fiordelli, M.; Diviani, N.; Schulz, P.J. Mapping mHealth Research: A Decade of Evolution. J. Med. Internet Res. 2013, 15, e95. [Google Scholar] [CrossRef]
- Aune, D.; Norat, T.; Leitzmann, M.; Tonstad, S.; Vatten, L.J. Physical activity and the risk of type 2 diabetes: A systematic review and dose-response meta-analysis. Eur. J. Epidemiol. 2015, 30, 529–542. [Google Scholar] [CrossRef] [PubMed]
- Laine, T.H. Mobile Educational Augmented Reality Games: A Systematic Literature Review and Two Case Studies. Computers 2018, 7, 19. [Google Scholar] [CrossRef]
- Awasthi, A.; Awasthi, A.; Riordan, D.; Walsh, J. Non-Invasive Sensor Technology for the Development of a Dairy Cattle Health Monitoring System. Computers 2016, 5, 23. [Google Scholar] [CrossRef]
- Kelly, S.; Martin, S.; Kuhn, I.; Cowan, A.; Brayne, C.; Lafortune, L. Barriers and Facilitators to the Uptake and Maintenance of Healthy Behaviours by People at Mid-Life: A Rapid Systematic Review. PLoS ONE 2016, 11, e0145074. [Google Scholar] [CrossRef] [PubMed]
- Griffin, S.J.; Leaver, J.K.; Irving, G.J. Impact of metformin on cardiovascular disease: A meta-analysis of randomised trials among people with type 2 diabetes. Diabetologia 2017, 60, 1620–1629. [Google Scholar] [CrossRef] [PubMed]
- Launer, L.J.; Miller, M.E.; Williamson, J.D.; Lazar, R.M.; Gerstein, H.C.; Murray, A.M.; Sullivan, M.; Horowitz, K.R.; Ding, J.; Marcovina, S.; et al. Effects of intensive glucose lowering on brain structure and function in people with type 2 diabetes (ACCORD MIND): A randomised open-label substudy. Lancet Neurol. 2011, 10, 969–977. [Google Scholar] [CrossRef]
- Rollo, M.E.; Aguiar, E.J.; Williams, R.L.; Wynne, K.; Kriss, M.; Callister, R.; Collins, C.E. eHealth technologies to support nutrition and physical activity behaviors in diabetes self-management. Diabetes Metab. Syndr. Obes.Targets Ther. 2014, 9, 381–390. [Google Scholar] [CrossRef] [PubMed]
- Hidalgo, J.I.; Maqueda, E.; Risco-Martin, J.L.; Cuesta-Infante, A.; Colmenar, J.M.; Nobel, J. glUCModel: A monitoring and modeling system for chronic diseases applied to diabetes. J. Biomed. Inform. 2014, 48, 183–192. [Google Scholar] [CrossRef] [PubMed]
- Hoppe, C.D.; Cade, J.E.; Carter, M. An evaluation of diabetes targeted apps for Android smartphone in relation to behaviour change techniques. J. Hum. Nutr. Diet. 2017, 30, 326–338. [Google Scholar] [CrossRef] [PubMed]
- McKay, F.H.; Cheng, C.; Wright, A.; Shill, J.; Stephens, H.; Uccellini, M. Evaluating mobile phone applications for health behaviour change: A systematic review. J. Telemed. Telecare 2018, 24, 22–30. [Google Scholar] [CrossRef]
- Brzan, P.P.; Rotman, E.; Pajnkihar, M.; Klanjsek, P. Mobile Applications for Control and Self Management of Diabetes: A Systematic Review. J. Med. Syst. 2016, 40, 210. [Google Scholar] [CrossRef]
- Georga, E.I.; Protopappas, V.C.; Bellos, C.V.; Fotiadis, D.I. Wearable systems and mobile applications for diabetes disease management. Health Technol. 2014, 4, 101–112. [Google Scholar] [CrossRef]
- Desveaux, L.; Agarwal, P.; Shaw, J.; Hensel, J.M.; Mukerji, G.; Onabajo, N.; Marani, H.; Jamieson, T.; Bhattacharyya, O.; Martin, D.; et al. A randomized wait-list control trial to evaluate the impact of a mobile application to improve self-management of individuals with type 2 diabetes: A study protocol. BMC Med. Inform. Decis. Mak. 2016, 16, 144. [Google Scholar] [CrossRef]
- Ryan, E.A.; Holland, J.; Stroulia, E.; Bazelli, B.; Babwik, S.A.; Li, H.; Senior, P.; Greiner, R. Improved A1C Levels in Type 1 Diabetes with Smartphone App Use. Can. J. Diabetes 2017, 41, 33–40. [Google Scholar] [CrossRef] [PubMed]
- Shah, V.N.; Garg, S.K. Managing diabetes in the digital age. Clin. Diabetes Endocrinol. 2015, 1, 16. [Google Scholar] [CrossRef]
- Goyal, S.; Morita, P.; Lewis, G.F.; Yu, C.; Seto, E.; Cafazzo, J.A. The Systematic Design of a Behavioural Mobile Health Application for the Self-Management of Type 2 Diabetes. Can. J. Diabetes 2016, 40, 95–104. [Google Scholar] [CrossRef] [PubMed]
- Hong, M.K.; Cho, Y.Y.; Rha, M.Y.; Kim, J.H.; Lee, M.-K. Six-month Outcomes of Mobile Phone Application-based Self-management in a Patient with Type 2 Diabetes. Clin. Nutr. Res. 2015, 4, 2015. [Google Scholar] [CrossRef] [PubMed]
- Mobiab Dieta. Available online: https://play.google.com/store/apps/details?id=cz.asleep&hl=cs. (accessed on 22 December 2018).
- DiaMonitor. 2018. Available online: https://diamonitor.com/dm/ (accessed on 22 December 2018).
- Diabetes—Glucose Daybook: Application. Available online: https://play.google.com/store/apps/details?id=com.szyk.diabetes&hl=cs (accessed on 22 December 2018).
- Diabetes Kit Blood Glucose Logbook. Available online: https://itunes.apple.com/us/app/diabetes-kit-blood-glucose-logbook/id962075451?mt=8 (accessed on 22 December 2018).
- Apps: Mobiab Diet. Available online: https://apkpure.com/it/mobiab-diet/cz.asleep (accessed on 22 December 2018).
- Diabetes Kit App. Available online: http://www.diabeteskitpp.com (accessed on 22 December 2018).
- Gerstweiler, G.; Platzer, K.; Kaufmann, H. DARGS: Dynamic AR Guiding System for Indoor Environments. Computers 2018, 7, 5. [Google Scholar] [CrossRef]
- Sharma, S. mHealth Design for Patients with Gestational Diabetes. Master’s Thesis, The University of Bergen, Bergen, Norway, 2017. [Google Scholar]
- Holtz, B.E.; Murray, K.M.; Hershey, D.D.; Dunneback, J.K.; Cotten, S.R.; Holmstrom, A.J.; Vyas, A.; Kaiser, M.K.; Wood, M.A. Developing a Patient-Centered mHealth App: A Tool for Adolescents With Type 1 Diabetes and Their Parents. JMIR mHealth uHealth 2017, 5, e53. [Google Scholar] [CrossRef]
- LeRouge, C.; Wickramasinghe, N. A Review of User-Centered Design for Diabetes-Related Consumer Health Informatics Technologies. J. Diabetes Sci. Technol. 2013, 7, 1039–1056. [Google Scholar] [CrossRef] [Green Version]
- Perneger, T.V.; Courvoisier, D.S.; Hudelson, P.M.; Gayet-Ageron, A. Sample size for pre-tests of questionnaires. Qual. Life Res. 2015, 24, 147–151. [Google Scholar] [CrossRef]
- Maresova, P.; Klimova, B. Selected aspects in searching for health information on the internet among generation Y. In Lecture Notes in Computer Science (Including Subseries Lecture Notes in Artificial Intelligence and Lecture Notes in Bioinformatics); Springer: Berlin, Germany, 2017; Volume 10595, pp. 221–226. [Google Scholar]
- Klimova, B.; Maresova, P. Elderly people and their attitude towards mobile phones and their applications—A review study. Lect. Notes Electr. Eng. 2016, 393, 31–36. [Google Scholar]
- Kostak, M.; Dvorak, J.; Selamat, A.; Krejcar, O. Intelligent notepad for windows phone that uses GPS data. In Lecture Notes in Computer Science (Including Subseries Lecture Notes in Artificial Intelligence and Lecture Notes in Bioinformatics); Springer: Berlin, Germany, 2017; Volume 10486, pp. 90–103. [Google Scholar]
- Krejcar, O.; Slanina, Z.; Stambachr, J.; Silber, P.; Frischer, R. Noninvasive continuous blood pressure measurement and GPS position monitoring of patients. In Proceedings of the IEEE Vehicular Technology Conference, Anchorage, AK, USA, 20–23 September 2009. [Google Scholar]
- Mervart, P.; Dvorak, J.; Krejcar, O. Ringtone adaptation based on location and surrounding noise. In Lecture Notes in Computer Science (Including Subseries Lecture Notes in Artificial Intelligence and Lecture Notes in Bioinformatics); Springer: Berlin, Germany, 2016; Volume 9847, pp. 43–55. [Google Scholar]
- Scholz, M.; Gordon, D.; Ramirez, L.; Sigg, S.; Dyrks, T.; Beigl, M. A concept for support of firefighter frontline communication. Future Internet 2013, 5, 113–127. [Google Scholar] [CrossRef]
- Leopold, J.H.; van Hooijdonk, R.T.M.; Boshuizen, M.; Winters, T.; Bos, L.D.; Abu-Hanna, A.; Hoek, A.M.T.; Fischer, J.C.; van Dongen-Lases, E.C.; Schultz, M.J. Point and trend accuracy of a continuous intravenous microdialysis-based glucose-monitoring device in critically ill patients: A prospective study. Ann. Intensive Care 2016, 6, 68. [Google Scholar] [CrossRef] [PubMed]
- Whitehead, L.; Seaton, P. The Effectiveness of Self-Management Mobile Phone and Tablet Apps in Long-term Condition Management: A Systematic Review. J. Med. Internet Res. 2016, 18, e97. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Lewis, T.L.; Wyatt, J.C. mHealth and Mobile Medical Apps: A Framework to Assess Risk and Promote Safer Use. J. Med. Internet Res. 2014, 16, e210. [Google Scholar] [CrossRef] [PubMed]
- Ahmadi, M.M.; Jullien, G.A. A Wireless-Implantable Microsystem for Continuous Blood Glucose Monitoring. IEEE Trans. Biomed. Circuits Syst. 2009, 3, 169–180. [Google Scholar] [CrossRef] [PubMed]
- Tsuchiya, K.; Nakanishi, N.; Uetsuji, Y.; Nakamachi, E. Development of blood extraction system for health monitoring system. Biomed. Microdevices 2005, 7, 347–353. [Google Scholar] [CrossRef] [PubMed]
- Krejcar, O.; Janckulik, D.; Motalova, L.; Kufel, J. Mobile Monitoring Stations and Web Visualization of Biotelemetric System—Guardian II. In Communications Infrastructure: Systems and Applications in Europe; Mehmood, R., Cerqueira, E., Piesiewicz, R., Chlamtac, I., Eds.; Springer: New York, NY, USA, 2009; Volume 16, pp. 286–293. [Google Scholar]
- Maresova, P.; Sobeslav, V.; Krejcar, O. Cost–benefit analysis–evaluation model of cloud computing deployment for use in companies. Appl. Econ. 2017, 49, 521–533. [Google Scholar] [CrossRef]
- Maresova, P.; Novotny, M.; Klímová, B.; Kuča, K. Treatment cost of narcolepsy with cataplexy in Central Europe. Ther. Clin. Risk Manag. 2016, 12, 1709–1715. [Google Scholar] [CrossRef]
- Mohelska, H.; Maresova, P.; Valis, M.; Kuca, K. Alzheimer’s disease and its treatment costs: Case study in the Czech Republic. Neuropsychiatr. Dis. Treat. 2015, 11, 2349–2354. [Google Scholar]
- Wang, Y.; Xue, H.; Huang, Y.; Huang, L.; Zhang, D. A Systematic Review of Application and Effectiveness of mHealth Interventions for Obesity and Diabetes Treatment and Self-Management. Adv. Nutr. 2017, 8, 449–462. [Google Scholar] [CrossRef] [Green Version]
- Lamprinos, I.; Demski, H.; Mantwill, S.; Kabak, Y.; Hildebrand, C.; Ploessnig, M. Modular ICT-based patient empowerment framework for self-management of diabetes: Design perspectives and validation results. Int. J. Med. Inform. 2016, 91, 31–43. [Google Scholar] [CrossRef]

| MOBIAB | DIAMO-NITOR | DIABETES-GLUCOSE DAYBOOK | DIABETES: M | DIABETES KIT BLOOD GLUCOSE LOGBOOK | |
|---|---|---|---|---|---|
| MOBILE APPLICATION | × | ||||
| WEB APPLICATION | × | × | × | ||
| SUPPORTED PLATFORMS | Android | × | Android | Android | iOS |
| MONITORING OF BLOOD GLUCOSE | |||||
| DRUG MANAGEMENT | × | ||||
| DIET MANAGEMENT | × | × | |||
| MANAGEMENT OF PHYSICAL ACTIVITY | × | × | |||
| USER EDUCATION ABOUT THE DISEASE | × | × | × | × | |
| GAMIFICATION METHODS | × | × | × | × | |
| RESULTS SHARING WITH DOCTOR | × | ||||
| SYNCHRONISATION WITH OTHER DEVICES | × | ||||
| STATISTICS | only web part | ||||
| GRAPHS | × | ||||
| CLARITY OF ENVIRONMENT (1-5(BEST)) | 2 | 4 | 3 | 3 | 5 |
| GENERATING REPORTS | × | × | |||
| INSULIN DOSE CALCULATOR | × | × | × | ||
| COMMUNICATION WITH SMART WATCHES | × | × | × | ||
| USER EVALUATIONS (GOOGLE PLAY AND APP STORE) | 3,8/5 | × | 4,4/5 | 4,7/5 | 4,6/5 |
| DIABETES TYPE | All types | First and second type | All types | All types | All types |
| PROS | Czech | Easy | Easy | Complex | Comprehensive and complex |
| CONS | Comprehensive | Low complexity of solution | No basic functions | Lover uncomprehensive | No detailed statistics |
| All Respondents. N = 30 | |
|---|---|
| Gender Male Female | 13 (43%) 17 (57%) |
| Age 15–18 19–22 23–26 27–30 | 5 (17%) 7 (23%) 9 (30%) 9 (30%) |
| Highest attained education Elementary Secondary Secondary with a school leaving exam Tertiary vocational Tertiary | 3 (10%) 2 (7%) 9 (30%) 5 (17%) 11 (37%) |
| Diabetes mellitus type 1. Type 2. Type No diabetes | 17 (57%) 10 (33%) 3 (10%) |
| SmartPhone OS 1. OS Android 2. OS iOS | 22 (73%) 8 (27%) |
| Using of mobile app for treatment of diabetes 1. Yes 2. No | 11 (37%) 19 (63%) |
| Prototype | ||||
|---|---|---|---|---|
| Reflecting the Current State Yes (No) | With Key Functions | With Extra Functions—iOS | With Extra Functions—Android | |
| Does the application include all the expected functions? Yes (no) | 5 (25) | 16 (14) | 26 (4) | 25 (5) |
| What is your impression of the graphic design? very good/good/bad/very bad | 8/19/3/0 | 14/14/2/0 | 22/6/2/0 | 18/11/1/0 |
| What is your impression of the functions? very good/good/bad/very bad | 2/5/19/4 | 4/14/10/2 | 16/14/0/0 | 17/13/0/0 |
| If you selected “Yes” in question no. 8, state how likely you would be to switch to this prototype from your current application. 100/70/30/0 [%] | 0/0/0/9 | 0/0/0/9 | 0/2/3/4 | 2/2/3/2 |
© 2018 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Pavlas, J.; Krejcar, O.; Maresova, P.; Selamat, A. Prototypes of User Interfaces for Mobile Applications for Patients with Diabetes. Computers 2019, 8, 1. https://doi.org/10.3390/computers8010001
Pavlas J, Krejcar O, Maresova P, Selamat A. Prototypes of User Interfaces for Mobile Applications for Patients with Diabetes. Computers. 2019; 8(1):1. https://doi.org/10.3390/computers8010001
Chicago/Turabian StylePavlas, Jan, Ondrej Krejcar, Petra Maresova, and Ali Selamat. 2019. "Prototypes of User Interfaces for Mobile Applications for Patients with Diabetes" Computers 8, no. 1: 1. https://doi.org/10.3390/computers8010001
APA StylePavlas, J., Krejcar, O., Maresova, P., & Selamat, A. (2019). Prototypes of User Interfaces for Mobile Applications for Patients with Diabetes. Computers, 8(1), 1. https://doi.org/10.3390/computers8010001






