The Role of Receptor–Ligand Interaction in Somatostatin Signaling Pathways: Implications for Neuroendocrine Tumors
Abstract
Simple Summary
Abstract
1. Somatostatin Receptors: Localization and Function
| Gene | SSTR1 | SSTR2 | SSTR3 | SSTR4 | SSTR5 |
|---|---|---|---|---|---|
| Genomic location (by HGNC) | Chromosome 14: 14q13 | Chromosome 17: 17q25.1 | Chromosome 22: 22q13.1 | Chromosome 20: 20p11.21 | Chromosome 16: 16p13.3 |
| Exon count | 3 | 2 | 6 | 1 | 2 |
| Transcriptional Factors | e.g., POLR2A, RAD21, STAT3, HNF4A, ZNF48, SP1, NCOR1, CREB1, FOS | e.g., AML1a, AP-1, En-1, ER-alpha, GATA-2, MyoD, NF-kappaB, Pbx1a, ZIC2 | e.g., SP1, ZNF207, JUND, TCF7, GATA2, SMAD5, EGR2, RAD51, WT1 | e.g., HNF4A, FOXJ2, Meis-1, NF-kappaB, p53, Pax-4a | e.g., Sp1, Bach2, C/EBPalpha, CREB E47, LCR-F1, p53, Pax-4a |
| Epigenetic modifications affecting expression | Hypermethylation promoter | Differential methylation of promoter regions, histone modifications (e.g., H3K4 methylation), ubiquitination | Promoter methylation | Hypomethylation of the promoter region | Methylation of the 4 CpG islands |
| MicroRNA regulators | e.g., miR-4285, miR-149-3p, miR-1207-5p, miR-502-3p | e.g., miR-378a-5p, miR-191-3p, miR-106a-3p, miR-122-5p, miR-130b-3p, hsa-miR-203b-3p, miR-215-5p | e.g., miR-328-5p, miR-623, miR-3667-3p, miR-766-3p | miR-132, miR-211, miR-204 | miR-129-5p, miR-204, miR-375 |
| Sequence variations with clinical significance | V351A, R380P, L326V, V153L (missense variants), rs146928458 (synonymous variant) | I87V, T30N, N22S, N318S (missense variants) | S7T, E288K, I125T, V175L, V145M (missense variants) | F114L, R377H, V125D, C366Y, S253W (missense variants) | R137H, P17R, R154H, R248H, P17L (missense variants) |
| Structural variations | nsv832773 (loss), esv3584282 (gain), nsv952830 (deletion) | nsv833534 (loss), nsv4263666 (deletion) | nsv4278013 and nsv966108 (duplications); nsv829203, nsv459883, and nsv834188 (loss) | nsv4336704 (sequence alteration), nsv4276734 (duplication), nsv524981 and nsv520810 (loss) | esv2422427 (duplication), nsv952898 (deletion), nsv457315 and nsv571046 (gain), sv471066 (loss) |
| Differences in protein sequence | 391 amino acids; longer extracellular fragments in domains 1, 2, 4, and 7 | 369 amino acids; shorter extracellular fragments in domains 2, 4, and 7 | 418 amino acids; longer extracellular fragments in domains 1, 2, and 7 | 388 amino acids; shorter extracellular fragment in domain 3 | 364 amino acids; longer extracellular fragments in domains 1, 3, and 4 |
| Subtype Receptor | Tissue Localization | Intracellular Signalling | Physiological Functions |
|---|---|---|---|
| Somatostatin receptor type 1 | Nervous system, stomach, colon, small intestine, lung, liver, kidney, duodenum, pancreas, salivary glands, basal ganglia, heart, blood vessels | Inhibition of cAMP, inhibition of cGMP production | Regulation of hormone secretion (e.g., insulin, glucagon), impact on cognitive processes, neuroprotective effects |
| Somatostatin receptor type 2 splicing variants A and B | Nervous system, kidney, spleen, stomach, appendix, liver, adrenal glands, thyroid | Inhibition of cAMP, activation of phospholipase C (PLC) pathway | Inhibition of growth hormone, insulin, glucagon secretion, regulation of gastrointestinal motility, inhibition of bile secretion |
| Somatostatin receptor type 3 | Nervous system, testis, ovary, gastrointestinal tract, pancreas, salivary glands, basal ganglia, lymph node | Inhibition of cAMP, activation of phospholipase C (PLC) pathway | Regulation of hormone secretion (e.g., insulin, glucagon), impact on cognitive processes, regulation of gastrointestinal motility |
| Somatostatin receptor type 4 | Nervous system, gastrointestinal tract, pancreas, salivary glands, heart, blood vessels | Inhibition of cAMP | Regulation of hormone secretion (e.g., insulin, glucagon), regulation of gastrointestinal motility, impact on heart and blood vessel function |
| Somatostatin receptor type 5 | Nervous system, kidney, adrenal, gallbladder, stomach, prostate, duodenum, colon | Inhibition of cAMP, activation of phospholipase C (PLC) pathway, activation of MAP kinase pathway | Regulation of hormone secretion (e.g., insulin, glucagon, thyrotropin, cortisol), impact on cognitive processes, regulation of gastrointestinal motility, anti-proliferative effects |
2. Diagnostics of the Expression of Somatostatin Receptors
3. Ligand–Receptor Interactions in Neuroendocrine Tumors
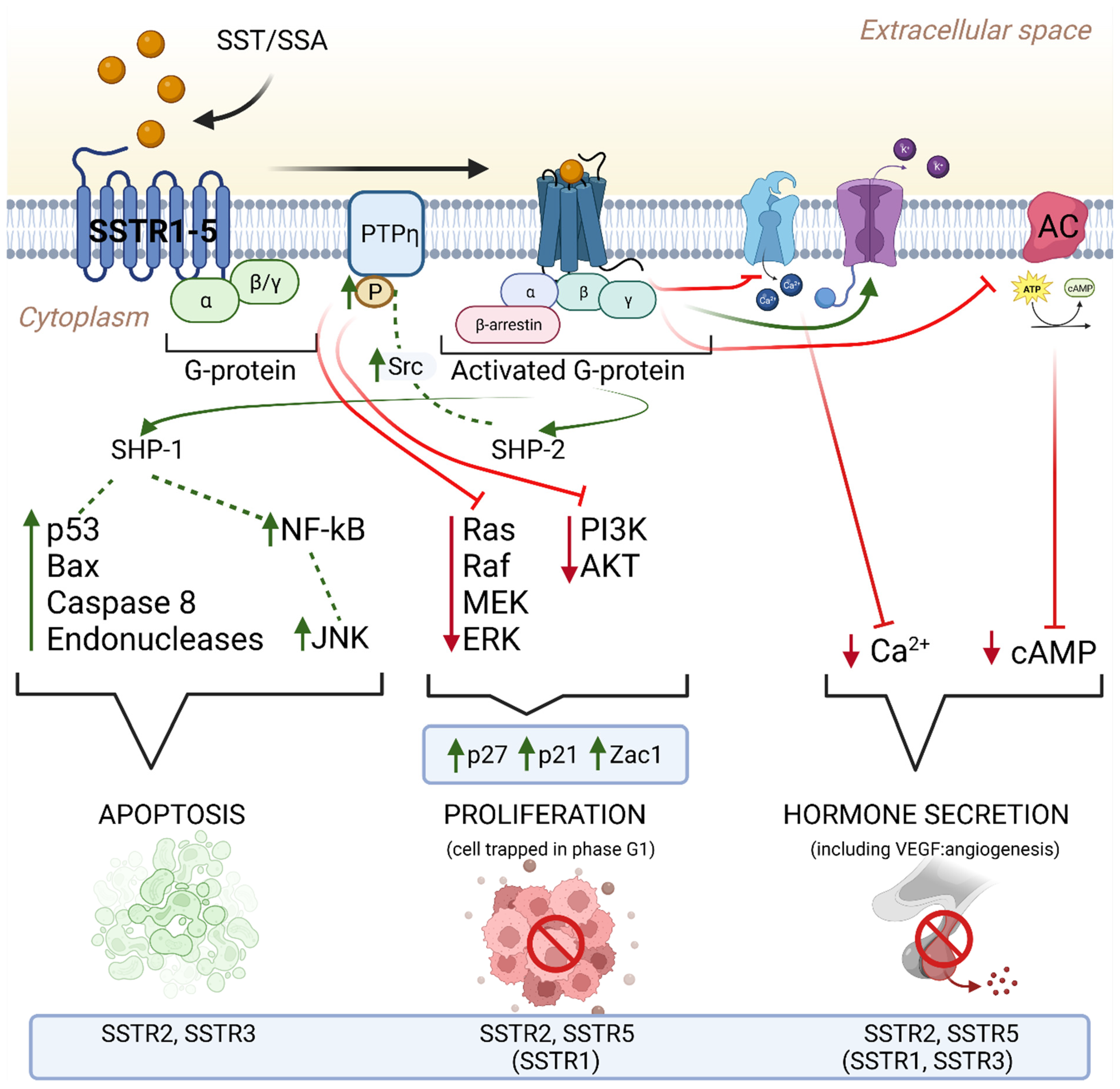
4. Intracellular Signaling Pathways of Somatostatin Receptors
5. Role of Somatostatin Receptors in Neuroendocrine Tumors
6. Somatostatin and Its Analogues in Neuroendocrine Tumor Therapy
7. Challenges in NET Therapy: Navigating Resistance, Diagnostic Sensitivity, and Long-Term Effectiveness
8. Conclusions and Future Perspectives
Author Contributions
Funding
Conflicts of Interest
References
- Patel, Y.C. Somatostatin and its receptor family. Front. Neuroendocrinol. 1999, 20, 157–198. [Google Scholar] [CrossRef] [PubMed]
- Yamada, Y.; Stoffel, M.; Espinosa, R., 3rd; Xiang, K.S.; Seino, M.; Seino, S.; Le Beau, M.M.; Bell, G.I. Human somatostatin receptor genes: Localization to human chromosomes 14, 17, and 22 and identification of simple tandem repeat polymorphisms. Genomics 1993, 15, 449–452. [Google Scholar] [CrossRef]
- Smith, C.M.; Steitz, J.A. Classification of gas5 as a multi-small-nucleolar-RNA (snoRNA) host gene and a member of the 5′-terminal oligopyrimidine gene family reveals common features of snoRNA host genes. Mol. Cell Biol. 1998, 18, 6897–6909. [Google Scholar] [CrossRef] [PubMed]
- O’Carroll, A.M.; Raynor, K.; Lolait, S.J.; Reisine, T. Characterization of cloned human somatostatin receptor SSTR5. Mol. Pharmacol. 1994, 46, 291–298. [Google Scholar]
- Patel, Y.C. Molecular pharmacology of somatostatin receptor subtypes. J. Endocrinol. Investig. 1997, 20, 348–367. [Google Scholar] [CrossRef] [PubMed]
- Yamada, Y.; Post, S.R.; Wang, K.; Tager, H.S.; Bell, G.I.; Seino, S. Cloning and functional characterization of a family of human and mouse somatostatin receptors expressed in brain, gastrointestinal tract, and kidney. Proc. Natl. Acad. Sci. USA 1992, 89, 251–255. [Google Scholar] [CrossRef] [PubMed]
- Bruno, J.F.; Xu, Y.; Song, J.; Berelowitz, M. Molecular cloning and functional expression of a brain-specific somatostatin receptor. Proc. Natl. Acad. Sci. USA 1992, 89, 11151–11155. [Google Scholar] [CrossRef]
- Cescato, R.; Schulz, S.; Waser, B.; Eltschinger, V.; Rivier, J.E.; Wester, H.J.; Culler, M.; Ginj, M.; Liu, Q.; Schonbrunn, A.; et al. Internalization of sst2, sst3, and sst5 receptors: Effects of somatostatin agonists and antagonists. J. Nucl. Med. 2006, 47, 502–511. [Google Scholar]
- Rocheville, M.; Lange, D.C.; Kumar, U.; Sasi, R.; Patel, R.C.; Patel, Y.C. Subtypes of the somatostatin receptor assemble as functional homo- and heterodimers. J. Biol. Chem. 2000, 275, 7862–7869. [Google Scholar] [CrossRef]
- Peverelli, E.; Lania, A.G.; Mantovani, G.; Beck-Peccoz, P.; Spada, A. Characterization of intracellular signaling mediated by human somatostatin receptor 5: Role of the DRY motif and the third intracellular loop. Endocrinology 2009, 150, 3169–3176. [Google Scholar] [CrossRef]
- Bo, Q.; Yang, F.; Li, Y.; Meng, X.; Zhang, H.; Zhou, Y.; Ling, S.; Sun, D.; Lv, P.; Liu, L.; et al. Structural insights into the activation of somatostatin receptor 2 by cyclic SST analogues. Cell Discov. 2022, 8, 47. [Google Scholar] [CrossRef] [PubMed]
- Stelzer, G.; Rosen, N.; Plaschkes, I.; Zimmerman, S.; Twik, M.; Fishilevich, S.; Stein, T.I.; Nudel, R.; Lieder, I.; Mazor, Y.; et al. The GeneCards Suite: From Gene Data Mining to Disease Genome Sequence Analyses. Curr. Protoc. Bioinform. 2016, 54, 1–30. [Google Scholar] [CrossRef] [PubMed]
- Ghosh, S.; Choritz, L.; Geibel, J.; Coca-Prados, M. Somatostatin modulates PI3K-Akt, eNOS and NHE activity in the ciliary epithelium. Mol. Cell Endocrinol. 2006, 253, 63–75. [Google Scholar] [CrossRef] [PubMed]
- Klomp, M.J.; Dalm, S.U.; de Jong, M.; Feelders, R.A.; Hofland, J.; Hofland, L.J. Epigenetic regulation of somatostatin and somatostatin receptors in neuroendocrine tumors and other types of cancer. Rev. Endocr. Metab. Disord. 2021, 22, 495–510. [Google Scholar] [CrossRef] [PubMed]
- Yamada, Y.; Reisine, T.; Law, S.F.; Ihara, Y.; Kubota, A.; Kagimoto, S.; Seino, M.; Seino, Y.; Bell, G.I.; Seino, S. Somatostatin receptors, an expanding gene family: Cloning and functional characterization of human SSTR3, a protein coupled to adenylyl cyclase. Mol. Endocrinol. 1992, 6, 2136–2142. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Rohrer, L.; Raulf, F.; Bruns, C.; Buettner, R.; Hofstaedter, F.; Schule, R. Cloning and characterization of a fourth human somatostatin receptor. Proc. Natl. Acad. Sci. USA 1993, 90, 4196–4200. [Google Scholar] [CrossRef] [PubMed]
- Havt, A.; Schally, A.V.; Halmos, G.; Varga, J.L.; Toller, G.L.; Horvath, J.E.; Szepeshazi, K.; Koster, F.; Kovitz, K.; Groot, K.; et al. The expression of the pituitary growth hormone-releasing hormone receptor and its splice variants in normal and neoplastic human tissues. Proc. Natl. Acad. Sci. USA 2005, 102, 17424–17429. [Google Scholar] [CrossRef]
- Rekasi, Z.; Czompoly, T.; Schally, A.V.; Halmos, G. Isolation and sequencing of cDNAs for splice variants of growth hormone-releasing hormone receptors from human cancers. Proc. Natl. Acad. Sci. USA 2000, 97, 10561–10566. [Google Scholar] [CrossRef]
- Reisine, T.; Kong, H.; Raynor, K.; Yano, H.; Takeda, J.; Yasuda, K.; Bell, G.I. Splice variant of the somatostatin receptor 2 subtype, somatostatin receptor 2B, couples to adenylyl cyclase. Mol. Pharmacol. 1993, 44, 1016–1020. [Google Scholar]
- Vanetti, M.; Kouba, M.; Wang, X.; Vogt, G.; Hollt, V. Cloning and expression of a novel mouse somatostatin receptor (SSTR2B). FEBS Lett. 1992, 311, 290–294. [Google Scholar] [CrossRef]
- Duran-Prado, M.; Gahete, M.D.; Martinez-Fuentes, A.J.; Luque, R.M.; Quintero, A.; Webb, S.M.; Benito-Lopez, P.; Leal, A.; Schulz, S.; Gracia-Navarro, F.; et al. Identification and characterization of two novel truncated but functional isoforms of the somatostatin receptor subtype 5 differentially present in pituitary tumors. J. Clin. Endocrinol. Metab. 2009, 94, 2634–2643. [Google Scholar] [CrossRef] [PubMed]
- Samim, A.; Tytgat, G.A.M.; Bleeker, G.; Wenker, S.T.M.; Chatalic, K.L.S.; Poot, A.J.; Tolboom, N.; van Noesel, M.M.; Lam, M.; de Keizer, B. Nuclear Medicine Imaging in Neuroblastoma: Current Status and New Developments. J. Pers. Med. 2021, 11, 270. [Google Scholar] [CrossRef] [PubMed]
- Curtis, S.B.; Hewitt, J.; Yakubovitz, S.; Anzarut, A.; Hsiang, Y.N.; Buchan, A.M. Somatostatin receptor subtype expression and function in human vascular tissue. Am. J. Physiol. Heart Circ. Physiol. 2000, 278, H1815–H1822. [Google Scholar] [CrossRef]
- Kumar, U.; Singh, S. Role of Somatostatin in the Regulation of Central and Peripheral Factors of Satiety and Obesity. Int. J. Mol. Sci. 2020, 21, 2568. [Google Scholar] [CrossRef]
- Perez, J.; Rigo, M.; Kaupmann, K.; Bruns, C.; Yasuda, K.; Bell, G.I.; Lubbert, H.; Hoyer, D. Localization of somatostatin (SRIF) SSTR-1, SSTR-2 and SSTR-3 receptor mRNA in rat brain by in situ hybridization. Naunyn Schmiedebergs Arch. Pharmacol. 1994, 349, 145–160. [Google Scholar] [CrossRef] [PubMed]
- Kumar, U.; Sasi, R.; Suresh, S.; Patel, A.; Thangaraju, M.; Metrakos, P.; Patel, S.C.; Patel, Y.C. Subtype-selective expression of the five somatostatin receptors (hSSTR1-5) in human pancreatic islet cells: A quantitative double-label immunohistochemical analysis. Diabetes 1999, 48, 77–85. [Google Scholar] [CrossRef] [PubMed]
- Somvanshi, R.K.; Jhajj, A.; Heer, M.; Kumar, U. Characterization of somatostatin receptors and associated signaling pathways in pancreas of R6/2 transgenic mice. Biochim. Biophys. Acta (BBA)–Mol. Basis Dis. 2018, 1864, 359–373. [Google Scholar] [CrossRef]
- Voros, I.; Saghy, E.; Pohoczky, K.; Makkos, A.; Onodi, Z.; Brenner, G.B.; Baranyai, T.; Agg, B.; Varadi, B.; Kemeny, A.; et al. Somatostatin and Its Receptors in Myocardial Ischemia/Reperfusion Injury and Cardioprotection. Front. Pharmacol. 2021, 12, 663655. [Google Scholar] [CrossRef]
- Wu, W.; Zhou, Y.; Wang, Y.; Liu, L.; Lou, J.; Deng, Y.; Zhao, P.; Shao, A. Clinical Significance of Somatostatin Receptor (SSTR) 2 in Meningioma. Front. Oncol. 2020, 10, 1633. [Google Scholar] [CrossRef]
- Kailey, B.; van de Bunt, M.; Cheley, S.; Johnson, P.R.; MacDonald, P.E.; Gloyn, A.L.; Rorsman, P.; Braun, M. SSTR2 is the functionally dominant somatostatin receptor in human pancreatic β- and α-cells. Am. J. Physiol.-Endocrinol. Metab. 2012, 303, E1107–E1116. [Google Scholar] [CrossRef]
- Hankus, J.; Tomaszewska, R. Neuroendocrine neoplasms and somatostatin receptor subtypes expression. Nucl. Med. Rev. Cent. East. Eur. 2016, 19, 111–117. [Google Scholar] [CrossRef] [PubMed]
- Watanabe, H.; Fujishima, F.; Unno, M.; Sasano, H.; Suzuki, T. Somatostatin receptor 2 in 10 different types of human non-neoplastic gastrointestinal neuroendocrine cells. Pathol. Res. Pract. 2023, 244, 154418. [Google Scholar] [CrossRef] [PubMed]
- Meirovitz, A.; Shouchane-Blum, K.; Maly, A.; Bersudski, E.; Hirshoren, N.; Abrams, R.; Popovtzer, A.; Orevi, M.; Weinberger, J. The potential of somatostatin receptor 2 as a novel therapeutic target in salivary gland malignant tumors. J. Cancer Res. Clin. Oncol. 2021, 147, 1335–1340. [Google Scholar] [CrossRef] [PubMed]
- Anzola, L.K.; Rivera, J.N.; Dierckx, R.A.; Lauri, C.; Valabrega, S.; Galli, F.; Moreno Lopez, S.; Glaudemans, A.; Signore, A. Value of Somatostatin Receptor Scintigraphy with (99m)Tc-HYNIC-TOC in Patients with Primary Sjogren Syndrome. J. Clin. Med. 2019, 8, 763. [Google Scholar] [CrossRef] [PubMed]
- Martel, G.; Dutar, P.; Epelbaum, J.; Viollet, C. Somatostatinergic systems: An update on brain functions in normal and pathological aging. Front. Endocrinol. 2012, 3, 154. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Schreff, M.; Schulz, S.; Handel, M.; Keilhoff, G.; Braun, H.; Pereira, G.; Klutzny, M.; Schmidt, H.; Wolf, G.; Hollt, V. Distribution, targeting, and internalization of the sst4 somatostatin receptor in rat brain. J. Neurosci. 2000, 20, 3785–3797. [Google Scholar] [CrossRef]
- Pedraza-Arevalo, S.; Ibanez-Costa, A.; Blazquez-Encinas, R.; Branco, M.R.; Vazquez-Borrego, M.C.; Herrera-Martinez, A.D.; Venegas-Moreno, E.; Serrano-Blanch, R.; Arjona-Sanchez, A.; Galvez-Moreno, M.A.; et al. Epigenetic and post-transcriptional regulation of somatostatin receptor subtype 5 (SST(5)) in pituitary and pancreatic neuroendocrine tumors. Mol. Oncol. 2022, 16, 764–779. [Google Scholar] [CrossRef]
- Zou, S.; Somvanshi, R.K.; Kumar, U. Somatostatin receptor 5 is a prominent regulator of signaling pathways in cells with coexpression of Cannabinoid receptors 1. Neuroscience 2017, 340, 218–231. [Google Scholar] [CrossRef]
- Lukomska, A.; Dobrzanski, G.; Liguz-Lecznar, M.; Kossut, M. Somatostatin receptors (SSTR1-5) on inhibitory interneurons in the barrel cortex. Brain Struct. Funct. 2020, 225, 387–401. [Google Scholar] [CrossRef]
- Beck-Peccoz, P.; Persani, L.; Mantovani, S.; Cortelazzi, D.; Asteria, C. Thyrotropin-secreting pituitary adenomas. Metabolism 1996, 45 (Suppl. S1), 75–79. [Google Scholar] [CrossRef]
- Rai, U.; Thrimawithana, T.R.; Valery, C.; Young, S.A. Therapeutic uses of somatostatin and its analogues: Current view and potential applications. Pharmacol. Ther. 2015, 152, 98–110. [Google Scholar] [CrossRef] [PubMed]
- Pepe, G.; Moncayo, R.; Bombardieri, E.; Chiti, A. Somatostatin receptor SPECT. Eur. J. Nucl. Med. Mol. Imaging 2012, 39 (Suppl. S1), S41–S51. [Google Scholar] [CrossRef] [PubMed]
- Oberg, K. Future aspects of somatostatin-receptor-mediated therapy. Neuroendocrinology 2004, 80 (Suppl. S1), 57–61. [Google Scholar] [CrossRef] [PubMed]
- Muscarella, L.A.; D’Alessandro, V.; la Torre, A.; Copetti, M.; De Cata, A.; Parrella, P.; Sperandeo, M.; Pellegrini, F.; Frusciante, V.; Maiello, E.; et al. Gene expression of somatostatin receptor subtypes SSTR2a, SSTR3 and SSTR5 in peripheral blood of neuroendocrine lung cancer affected patients. Cell Oncol. 2011, 34, 435–441. [Google Scholar] [CrossRef] [PubMed]
- Mizutani, G.; Nakanishi, Y.; Watanabe, N.; Honma, T.; Obana, Y.; Seki, T.; Ohni, S.; Nemoto, N. Expression of Somatostatin Receptor (SSTR) Subtypes (SSTR-1, 2A, 3, 4 and 5) in Neuroendocrine Tumors Using Real-time RT-PCR Method and Immunohistochemistry. Acta Histochem. Cytochem. 2012, 45, 167–176. [Google Scholar] [CrossRef] [PubMed]
- Kulaksiz, H.; Eissele, R.; Rossler, D.; Schulz, S.; Hollt, V.; Cetin, Y.; Arnold, R. Identification of somatostatin receptor subtypes 1, 2A, 3, and 5 in neuroendocrine tumours with subtype specific antibodies. Gut 2002, 50, 52–60. [Google Scholar] [CrossRef] [PubMed]
- Kanakis, G.; Grimelius, L.; Spathis, A.; Tringidou, R.; Rassidakis, G.Z.; Oberg, K.; Kaltsas, G.; Tsolakis, A.V. Expression of Somatostatin Receptors 1-5 and Dopamine Receptor 2 in Lung Carcinoids: Implications for a Therapeutic Role. Neuroendocrinology 2015, 101, 211–222. [Google Scholar] [CrossRef]
- Jonas, S.; John, M.; Boese-Landgraf, J.; Haring, R.; Prevost, G.; Thomas, F.; Rosewicz, S.; Riecken, E.O.; Wiedenmann, B.; Neuhaus, P. Somatostatin receptor subtypes in neuroendocrine tumor cell lines and tumor tissues. Langenbecks Arch. Chir. 1995, 380, 90–95. [Google Scholar] [CrossRef]
- Hofland, L.J.; Lamberts, S.W. Somatostatin receptors and disease: Role of receptor subtypes. Baillieres Clin. Endocrinol. Metab. 1996, 10, 163–176. [Google Scholar] [CrossRef]
- Dizeyi, N.; Konrad, L.; Bjartell, A.; Wu, H.; Gadaleanu, V.; Hansson, J.; Helboe, L.; Abrahamsson, P.A. Localization and mRNA expression of somatostatin receptor subtypes in human prostatic tissue and prostate cancer cell lines. Urol. Oncol. 2002, 7, 91–98. [Google Scholar] [CrossRef]
- De Herder, W.W.; Lamberts, S.W. Somatostatin and somatostatin analogues: Diagnostic and therapeutic uses. Curr. Opin. Oncol. 2002, 14, 53–57. [Google Scholar] [CrossRef] [PubMed]
- Cakir, M.; Dworakowska, D.; Grossman, A. Somatostatin receptor biology in neuroendocrine and pituitary tumours: Part 1–Molecular pathways. J. Cell Mol. Med. 2010, 14, 2570–2584. [Google Scholar] [CrossRef] [PubMed]
- Breeman, W.A.; de Jong, M.; Kwekkeboom, D.J.; Valkema, R.; Bakker, W.H.; Kooij, P.P.; Visser, T.J.; Krenning, E.P. Somatostatin receptor-mediated imaging and therapy: Basic science, current knowledge, limitations and future perspectives. Eur. J. Nucl. Med. 2001, 28, 1421–1429. [Google Scholar] [CrossRef] [PubMed]
- Atkinson, H.; England, J.A.; Rafferty, A.; Jesudason, V.; Bedford, K.; Karsai, L.; Atkin, S.L. Somatostatin receptor expression in thyroid disease. Int. J. Exp. Pathol. 2013, 94, 226–229. [Google Scholar] [CrossRef] [PubMed]
- Appetecchia, M.; Baldelli, R. Somatostatin analogues in the treatment of gastroenteropancreatic neuroendocrine tumours, current aspects and new perspectives. J. Exp. Clin. Cancer Res. 2010, 29, 19. [Google Scholar] [CrossRef] [PubMed]
- Florio, T.; Thellung, S.; Arena, S.; Corsaro, A.; Bajetto, A.; Schettini, G.; Stork, P.J.S. Somatostatin receptor 1 (SSTR1)-mediated inhibition of cell proliferation correlates with the activation of the MAP kinase cascade: Role of the phosphotyrosine phosphatase SHP-2. J. Physiol.-Paris 2000, 94, 239–250. [Google Scholar] [CrossRef] [PubMed]
- Ben-Shlomo, A.; Melmed, S. Pituitary somatostatin receptor signaling. Trends Endocrinol. Metab. 2010, 21, 123–133. [Google Scholar] [CrossRef]
- Rorsman, P.; Huising, M.O. The somatostatin-secreting pancreatic δ-cell in health and disease. Nat. Rev. Endocrinol. 2018, 14, 404–414. [Google Scholar] [CrossRef]
- Chen, D.; Taché, Y.; Wang, L.; Piqueras, L.; Martinez, V.; Zhao, C.-M. Control of Gastric Acid Secretion in Somatostatin Receptor 2 Deficient Mice: Shift from Endocrine/Paracrine to Neurocrine Pathways. Endocrinology 2008, 149, 498–505. [Google Scholar] [CrossRef]
- Egerod, K.L.; Engelstoft, M.S.; Lund, M.L.; Grunddal, K.V.; Zhao, M.; Barir-Jensen, D.; Nygaard, E.B.; Petersen, N.; Holst, J.J.; Schwartz, T.W. Transcriptional and Functional Characterization of the G Protein-Coupled Receptor Repertoire of Gastric Somatostatin Cells. Endocrinology 2015, 156, 3909–3923. [Google Scholar] [CrossRef]
- Shamsi, B.H.; Chatoo, M.; Xu, X.K.; Xu, X.; Chen, X.Q. Versatile Functions of Somatostatin and Somatostatin Receptors in the Gastrointestinal System. Front. Endocrinol. 2021, 12, 652363. [Google Scholar] [CrossRef] [PubMed]
- Gonkowski, S.; Rytel, L. Somatostatin as an Active Substance in the Mammalian Enteric Nervous System. Int. J. Mol. Sci. 2019, 20, 4461. [Google Scholar] [CrossRef] [PubMed]
- Chatterjee, S.; De Man, J.; Van Marck, E. Somatostatin and intestinal schistosomiasis: Therapeutic and neuropathological implications in host-parasite interactions. Trop. Med. Int. Health 2001, 6, 1008–1015. [Google Scholar] [CrossRef] [PubMed]
- Csaba, Z.; Dournaud, P. Internalization of somatostatin receptors in brain and periphery. Prog. Mol. Biol. Transl. Sci. 2023, 196, 43–57. [Google Scholar] [CrossRef] [PubMed]
- Kossut, M.; Lukomska, A.; Dobrzanski, G.; Liguz-Lecznar, M. Somatostatin receptors in the brain. Postep. Biochem. 2018, 64, 213–221. [Google Scholar] [CrossRef] [PubMed]
- Christenn, M.; Kindler, S.; Schulz, S.; Buck, F.; Richter, D.; Kreienkamp, H.J. Interaction of brain somatostatin receptors with the PDZ domains of PSD-95. FEBS Lett. 2007, 581, 5173–5177. [Google Scholar] [CrossRef] [PubMed]
- Florio, T.; Thellung, S.; Schettini, G. Intracellular transducing mechanisms coupled to brain somatostatin receptors. Pharmacol. Res. 1996, 33, 297–305. [Google Scholar] [CrossRef]
- Ampofo, E.; Nalbach, L.; Menger, M.D.; Laschke, M.W. Regulatory Mechanisms of Somatostatin Expression. Int. J. Mol. Sci. 2020, 21, 4170. [Google Scholar] [CrossRef]
- Lu, Y.Y.; Gao, J.H.; Zhao, C.; Wen, S.L.; Tang, C.W.; Wang, Y.F. Cyclooxygenase-2 up-regulates hepatic somatostatin receptor 2 expression. Sci. Rep. 2018, 8, 11033. [Google Scholar] [CrossRef]
- Somvanshi, R.K.; Zou, S.; Qiu, X.; Kumar, U. Somatostatin receptor-2 negatively regulates beta-adrenergic receptor mediated Ca(2+) dependent signaling pathways in H9c2 cells. Biochim. Biophys. Acta 2014, 1843, 735–745. [Google Scholar] [CrossRef]
- Psilopatis, I.; Garmpis, N.; Garmpi, A.; Vrettou, K.; Sarantis, P.; Koustas, E.; Antoniou, E.A.; Dimitroulis, D.; Kouraklis, G.; Karamouzis, M.V.; et al. The Emerging Role of Histone Deacetylase Inhibitors in Cervical Cancer Therapy. Cancers 2023, 15, 2222. [Google Scholar] [CrossRef] [PubMed]
- Kaemmerer, D.; Athelogou, M.; Lupp, A.; Lenhardt, I.; Schulz, S.; Luisa, P.; Hommann, M.; Prasad, V.; Binnig, G.; Baum, R.P. Somatostatin receptor immunohistochemistry in neuroendocrine tumors: Comparison between manual and automated evaluation. Int. J. Clin. Exp. Pathol. 2014, 7, 4971–4980. [Google Scholar] [PubMed]
- Remes, S.M.; Leijon, H.L.; Vesterinen, T.J.; Arola, J.T.; Haglund, C.H. Immunohistochemical Expression of Somatostatin Receptor Subtypes in a Panel of Neuroendocrine Neoplasias. J. Histochem. Cytochem. 2019, 67, 735–743. [Google Scholar] [CrossRef] [PubMed]
- Viollet, C.; Faivre-Bauman, A.; Zhang, J.; Llorens-Cortes, C.; Loudes, C.; Kordon, C.; Epelbaum, J. Differential expression of somatostatin receptors by quantitative PCR in the rat brain. C R. Acad. Sci. III 1995, 318, 851–857. [Google Scholar] [PubMed]
- Bhandari, S.; Watson, N.; Long, E.; Sharpe, S.; Zhong, W.; Xu, S.Z.; Atkin, S.L. Expression of somatostatin and somatostatin receptor subtypes 1-5 in human normal and diseased kidney. J. Histochem. Cytochem. 2008, 56, 733–743. [Google Scholar] [CrossRef] [PubMed]
- Ameri, P.; Gatto, F.; Arvigo, M.; Villa, G.; Resmini, E.; Minuto, F.; Murialdo, G.; Ferone, D. Somatostatin receptor scintigraphy in thoracic diseases. J. Endocrinol. Investig. 2007, 30, 889–902. [Google Scholar] [CrossRef] [PubMed]
- Bombardieri, E.; Coliva, A.; Maccauro, M.; Seregni, E.; Orunesu, E.; Chiti, A.; Lucignani, G. Imaging of neuroendocrine tumours with gamma-emitting radiopharmaceuticals. Q. J. Nucl. Med. Mol. Imaging 2010, 54, 3–15. [Google Scholar]
- Koopmans, K.P.; Neels, O.N.; Kema, I.P.; Elsinga, P.H.; Links, T.P.; de Vries, E.G.; Jager, P.L. Molecular imaging in neuroendocrine tumors: Molecular uptake mechanisms and clinical results. Crit. Rev. Oncol. Hematol. 2009, 71, 199–213. [Google Scholar] [CrossRef]
- Teunissen, J.J.; Kwekkeboom, D.J.; Valkema, R.; Krenning, E.P. Nuclear medicine techniques for the imaging and treatment of neuroendocrine tumours. Endocr. Relat. Cancer 2011, 18 (Suppl. S1), S27–S51. [Google Scholar] [CrossRef]
- Baghdadi, A.; Ghadimi, M.; Mirpour, S.; Hazhirkarzar, B.; Motaghi, M.; Pawlik, T.M.; Kamel, I.R. Imaging neuroendocrine tumors: Characterizing the spectrum of radiographic findings. Surg. Oncol. 2021, 37, 101529. [Google Scholar] [CrossRef]
- Brom, M.; Boerman, O.; Gotthardt, M.; Oyen, W.J. Preclinical studies of SPECT and PET tracers for NET. PET Clin. 2014, 9, 63–69. [Google Scholar] [CrossRef] [PubMed]
- Gabriel, M.; Andergassen, U.; Putzer, D.; Kroiss, A.; Waitz, D.; Von Guggenberg, E.; Kendler, D.; Virgolini, I.J. Individualized peptide-related-radionuclide-therapy concept using different radiolabelled somatostatin analogs in advanced cancer patients. Q. J. Nucl. Med. Mol. Imaging 2010, 54, 92–99. [Google Scholar] [PubMed]
- Raphael, M.J.; Chan, D.L.; Law, C.; Singh, S. Principles of diagnosis and management of neuroendocrine tumours. Can. Med. Assoc. J. 2017, 189, E398–E404. [Google Scholar] [CrossRef] [PubMed]
- Hallet, J.; Law, C.H.L.; Cukier, M.; Saskin, R.; Liu, N.; Singh, S. Exploring the rising incidence of neuroendocrine tumors: A population-based analysis of epidemiology, metastatic presentation, and outcomes. Cancer 2015, 121, 589–597. [Google Scholar] [CrossRef]
- Lewis, J.S.; Anderson, C.J. Radiometal-labeled somatostatin analogs for applications in cancer imaging and therapy. Methods Mol. Biol. 2007, 386, 227–240. [Google Scholar] [CrossRef]
- Froidevaux, S.; Eberle, A.N. Somatostatin analogs and radiopeptides in cancer therapy. Biopolymers 2002, 66, 161–183. [Google Scholar] [CrossRef]
- Modlin, I.M.; Pavel, M.; Kidd, M.; Gustafsson, B.I. Review article: Somatostatin analogues in the treatment of gastroenteropancreatic neuroendocrine (carcinoid) tumours. Aliment. Pharmacol. Ther. 2010, 31, 169–188. [Google Scholar] [CrossRef]
- Oberg, K. Neuroendocrine tumors of the digestive tract: Impact of new classifications and new agents on therapeutic approaches. Curr. Opin. Oncol. 2012, 24, 433–440. [Google Scholar] [CrossRef]
- Stewart, P.M.; James, R.A. The future of somatostatin analogue therapy. Baillieres Best. Pract. Res. Clin. Endocrinol. Metab. 1999, 13, 409–418. [Google Scholar] [CrossRef]
- Rinke, A.; Muller, H.H.; Schade-Brittinger, C.; Klose, K.J.; Barth, P.; Wied, M.; Mayer, C.; Aminossadati, B.; Pape, U.F.; Blaker, M.; et al. Placebo-controlled, double-blind, prospective, randomized study on the effect of octreotide LAR in the control of tumor growth in patients with metastatic neuroendocrine midgut tumors: A report from the PROMID Study Group. J. Clin. Oncol. 2009, 27, 4656–4663. [Google Scholar] [CrossRef]
- Hoyer, D.; Bell, G.I.; Berelowitz, M.; Epelbaum, J.; Feniuk, W.; Humphrey, P.P.; O’Carroll, A.M.; Patel, Y.C.; Schonbrunn, A.; Taylor, J.E.; et al. Classification and nomenclature of somatostatin receptors. Trends Pharmacol. Sci. 1995, 16, 86–88. [Google Scholar] [CrossRef] [PubMed]
- Vaudry, H.; Solarski, M.; Williams, D.; Mehrabian, M.; Wang, H.; Wille, H.; Schmitt-Ulms, G. The human brain somatostatin interactome: SST binds selectively to P-type family ATPases. PLoS ONE 2019, 14, e0217392. [Google Scholar] [CrossRef]
- Li, F.; Ryu, B.Y.; Krueger, R.L.; Heldt, S.A.; Albritton, L.M. Targeted Entry via Somatostatin Receptors Using a Novel Modified Retrovirus Glycoprotein That Delivers Genes at Levels Comparable to Those of Wild-Type Viral Glycoproteins. J. Virol. 2012, 86, 373–381. [Google Scholar] [CrossRef] [PubMed]
- Greenwood, M.T.; Hukovic, N.; Kumar, U.; Panetta, R.; Hjorth, S.A.; Srikant, C.B.; Patel, Y.C. Ligand Binding Pocket of the Human Somatostatin Receptor 5: Mutational Analysis of the Extracellular Domains. Mol. Pharmacol. 1997, 52, 807–814. [Google Scholar] [CrossRef] [PubMed]
- Kristiansen, K. Molecular mechanisms of ligand binding, signaling, and regulation within the superfamily of G-protein-coupled receptors: Molecular modeling and mutagenesis approaches to receptor structure and function. Pharmacol. Ther. 2004, 103, 21–80. [Google Scholar] [CrossRef] [PubMed]
- Nagarajan, S.K.; Babu, S.; Kulkarni, S.A.; Vadivelu, A.; Devaraju, P.; Sohn, H.; Madhavan, T. Understanding the influence of lipid bilayers and ligand molecules in determining the conformational dynamics of somatostatin receptor 2. Sci. Rep. 2021, 11, 7677. [Google Scholar] [CrossRef]
- Borzsei, R.; Zsido, B.Z.; Balint, M.; Helyes, Z.; Pinter, E.; Hetenyi, C. Exploration of Somatostatin Binding Mechanism to Somatostatin Receptor Subtype 4. Int. J. Mol. Sci. 2022, 23, 6878. [Google Scholar] [CrossRef]
- Kaupmann, K.; Bruns, C.; Raulf, F.; Weber, H.P.; Mattes, H.; Lubbert, H. Two amino acids, located in transmembrane domains VI and VII, determine the selectivity of the peptide agonist SMS 201-995 for the SSTR2 somatostatin receptor. EMBO J. 1995, 14, 727–735. [Google Scholar] [CrossRef]
- Cervia, D.; Bagnoli, P. An update on somatostatin receptor signaling in native systems and new insights on their pathophysiology. Pharmacol. Ther. 2007, 116, 322–341. [Google Scholar] [CrossRef]
- Kleuss, C.; Scherubl, H.; Hescheler, J.; Schultz, G.; Wittig, B. Selectivity in signal transduction determined by gamma subunits of heterotrimeric G proteins. Science 1993, 259, 832–834. [Google Scholar] [CrossRef]
- Kleuss, C.; Hescheler, J.; Ewel, C.; Rosenthal, W.; Schultz, G.; Wittig, B. Assignment of G-protein subtypes to specific receptors inducing inhibition of calcium currents. Nature 1991, 353, 43–48. [Google Scholar] [CrossRef] [PubMed]
- Komatsuzaki, K.; Murayama, Y.; Giambarella, U.; Ogata, E.; Seino, S.; Nishimoto, I. A novel system that reports the G-proteins linked to a given receptor: A study of type 3 somatostatin receptor. FEBS Lett. 1997, 406, 165–170. [Google Scholar] [CrossRef]
- Bockaert, J.; Fagni, L.; Dumuis, A.; Marin, P. GPCR interacting proteins (GIP). Pharmacol. Ther. 2004, 103, 203–221. [Google Scholar] [CrossRef] [PubMed]
- Jean-Baptiste, G.; Yang, Z.; Greenwood, M.T. Regulatory mechanisms involved in modulating RGS function. Cell Mol. Life Sci. 2006, 63, 1969–1985. [Google Scholar] [CrossRef] [PubMed]
- Zitzer, H.; Honck, H.H.; Bachner, D.; Richter, D.; Kreienkamp, H.J. Somatostatin receptor interacting protein defines a novel family of multidomain proteins present in human and rodent brain. J. Biol. Chem. 1999, 274, 32997–33001. [Google Scholar] [CrossRef] [PubMed]
- Kong, J.L.; Panetta, R.; Song, W.; Somerville, W.; Greenwood, M.T. Inhibition of somatostatin receptor 5-signaling by mammalian regulators of G-protein signaling (RGS) in yeast. Biochim. Biophys. Acta 2002, 1542, 95–105. [Google Scholar] [CrossRef] [PubMed]
- Elberg, G.; Hipkin, R.W.; Schonbrunn, A. Homologous and heterologous regulation of somatostatin receptor 2. Mol. Endocrinol. 2002, 16, 2502–2514. [Google Scholar] [CrossRef]
- Liu, Q.; Schonbrunn, A. Agonist-induced phosphorylation of somatostatin receptor subtype 1 (sst1). Relationship to desensitization and internalization. J. Biol. Chem. 2001, 276, 3709–3717. [Google Scholar] [CrossRef]
- Roth, A.; Kreienkamp, H.J.; Meyerhof, W.; Richter, D. Phosphorylation of four amino acid residues in the carboxyl terminus of the rat somatostatin receptor subtype 3 is crucial for its desensitization and internalization. J. Biol. Chem. 1997, 272, 23769–23774. [Google Scholar] [CrossRef]
- Brasselet, S.; Guillen, S.; Vincent, J.-P.; Mazella, J. β-Arrestin is involved in the desensitization but not in the internalization of the somatostatin receptor 2A expressed in CHO cells. FEBS Lett. 2002, 516, 124–128. [Google Scholar] [CrossRef]
- Kreuzer, O.J.; Krisch, B.; Dery, O.; Bunnett, N.W.; Meyerhof, W. Agonist-mediated endocytosis of rat somatostatin receptor subtype 3 involves beta-arrestin and clathrin coated vesicles. J. Neuroendocrinol. 2001, 13, 279–287. [Google Scholar] [CrossRef] [PubMed]
- Tulipano, G.; Schulz, S. Novel insights in somatostatin receptor physiology. Eur. J. Endocrinol. 2007, 156 (Suppl. S1), S3–S11. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Tulipano, G.; Stumm, R.; Pfeiffer, M.; Kreienkamp, H.J.; Hollt, V.; Schulz, S. Differential beta-arrestin trafficking and endosomal sorting of somatostatin receptor subtypes. J. Biol. Chem. 2004, 279, 21374–21382. [Google Scholar] [CrossRef] [PubMed]
- Schonbrunn, A. Selective agonism in somatostatin receptor signaling and regulation. Mol. Cell Endocrinol. 2008, 286, 35–39. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Csaba, Z.; Bernard, V.; Helboe, L.; Bluet-Pajot, M.T.; Bloch, B.; Epelbaum, J.; Dournaud, P. In vivo internalization of the somatostatin sst2A receptor in rat brain: Evidence for translocation of cell-surface receptors into the endosomal recycling pathway. Mol. Cell Neurosci. 2001, 17, 646–661. [Google Scholar] [CrossRef]
- Csaba, Z.; Dournaud, P. Cellular biology of somatostatin receptors. Neuropeptides 2001, 35, 1–23. [Google Scholar] [CrossRef]
- Olias, G.; Viollet, C.; Kusserow, H.; Epelbaum, J.; Meyerhof, W. Regulation and function of somatostatin receptors. J. Neurochem. 2004, 89, 1057–1091. [Google Scholar] [CrossRef]
- Jacobs, S.; Schulz, S. Intracellular trafficking of somatostatin receptors. Mol. Cell Endocrinol. 2008, 286, 58–62. [Google Scholar] [CrossRef]
- Grant, M.; Collier, B.; Kumar, U. Agonist-dependent dissociation of human somatostatin receptor 2 dimers: A role in receptor trafficking. J. Biol. Chem. 2004, 279, 36179–36183. [Google Scholar] [CrossRef]
- Grant, M.; Patel, R.C.; Kumar, U. The role of subtype-specific ligand binding and the C-tail domain in dimer formation of human somatostatin receptors. J. Biol. Chem. 2004, 279, 38636–38643. [Google Scholar] [CrossRef]
- Pfleger, K.D.; Eidne, K.A. Monitoring the formation of dynamic G-protein-coupled receptor-protein complexes in living cells. Biochem. J. 2005, 385, 625–637. [Google Scholar] [CrossRef] [PubMed]
- Milligan, G. G protein-coupled receptor dimerization: Function and ligand pharmacology. Mol. Pharmacol. 2004, 66, 1–7. [Google Scholar] [CrossRef] [PubMed]
- Csaba, Z.; Peineau, S.; Dournaud, P. Molecular mechanisms of somatostatin receptor trafficking. J. Mol. Endocrinol. 2012, 48, R1–R12. [Google Scholar] [CrossRef] [PubMed]
- Schulz, S.; Lohse, M.J.; Nikolaev, V.O.; Calebiro, D.; Jacobs, S. Real-Time Monitoring of Somatostatin Receptor-cAMP Signaling in Live Pituitary. Endocrinology 2010, 151, 4560–4565. [Google Scholar] [CrossRef]
- Siehler, S.; Hoyer, D. Characterisation of human recombinant somatostatin receptors. 4. Modulation of phospholipase C activity. Naunyn-Schmiedeberg’s Arch. Pharmacol. 1999, 360, 522–532. [Google Scholar] [CrossRef] [PubMed]
- Kim, J.K.; Kwon, O.; Kim, J.; Kim, E.-K.; Park, H.K.; Lee, J.E.; Kim, K.L.; Choi, J.W.; Lim, S.; Seok, H.; et al. PDZ Domain-containing 1 (PDZK1) Protein Regulates Phospholipase C-β3 (PLC-β3)-specific Activation of Somatostatin by Forming a Ternary Complex with PLC-β3 and Somatostatin Receptors. J. Biol. Chem. 2012, 287, 21012–21024. [Google Scholar] [CrossRef] [PubMed]
- Kharmate, G.; Rajput, P.S.; Watt, H.L.; Somvanshi, R.K.; Chaudhari, N.; Qiu, X.; Kumar, U. Role of somatostatin receptor 1 and 5 on epidermal growth factor receptor mediated signaling. Biochim. Biophys. Acta 2011, 1813, 1172–1189. [Google Scholar] [CrossRef]
- Florio, T.; Yao, H.; Carey, K.D.; Dillon, T.J.; Stork, P.J.S. Somatostatin Activation of Mitogen-Activated Protein Kinase via Somatostatin Receptor 1 (SSTR1). Mol. Endocrinol. 1999, 13, 24–37. [Google Scholar] [CrossRef][Green Version]
- New, D.C.; Wu, K.; Kwok, A.W.S.; Wong, Y.H. G protein-coupled receptor-induced Akt activity in cellular proliferation and apoptosis. FEBS J. 2007, 274, 6025–6036. [Google Scholar] [CrossRef]
- Porta, C.; Paglino, C.; Mosca, A. Targeting PI3K/Akt/mTOR Signaling in Cancer. Front. Oncol. 2014, 4, 64. [Google Scholar] [CrossRef]
- Liguz-Lecznar, M.; Urban-Ciecko, J.; Kossut, M. Somatostatin and Somatostatin-Containing Neurons in Shaping Neuronal Activity and Plasticity. Front. Neural Circuits 2016, 10, 48. [Google Scholar] [CrossRef] [PubMed]
- Pittaluga, A.; Roggeri, A.; Vallarino, G.; Olivero, G. Somatostatin, a Presynaptic Modulator of Glutamatergic Signal in the Central Nervous System. Int. J. Mol. Sci. 2021, 22, 5864. [Google Scholar] [CrossRef] [PubMed]
- Hauge-Evans, A.C.; King, A.J.; Carmignac, D.; Richardson, C.C.; Robinson, I.C.A.F.; Low, M.J.; Christie, M.R.; Persaud, S.J.; Jones, P.M. Somatostatin Secreted by Islet δ-Cells Fulfills Multiple Roles as a Paracrine Regulator of Islet Function. Diabetes 2009, 58, 403–411. [Google Scholar] [CrossRef] [PubMed]
- Ballian, N.; Brunicardi, F.C.; Wang, X.-P. Somatostatin and its Receptors in the Development of the Endocrine Pancreas. Pancreas 2006, 33, 1–12. [Google Scholar] [CrossRef] [PubMed]
- Corleto, V.D. Somatostatin and the gastrointestinal tract. Curr. Opin. Endocrinol. Diabetes Obes. 2010, 17, 63–68. [Google Scholar] [CrossRef] [PubMed]
- Grozinsky-Glasberg, S.; Shimon, I.; Korbonits, M.; Grossman, A.B. Somatostatin analogues in the control of neuroendocrine tumours: Efficacy and mechanisms. Endocr. Relat. Cancer 2008, 15, 701–720. [Google Scholar] [CrossRef]
- Solcia, E.; Rindi, G.; Larosa, S.; Capella, C. Morphological, molecular, and prognostic aspects of gastric endocrine tumors. Microsc. Res. Tech. 2000, 48, 339–348. [Google Scholar] [CrossRef]
- Rindi, G.; Capella, C.; Solcia, E. Introduction to a revised clinicopathological classification of neuroendocrine tumors of the gastroenteropancreatic tract. Q. J. Nucl. Med. 2000, 44, 13–21. [Google Scholar]
- Ioachimescu, A.G. Management of Neuroendocrine Tumors in the Twenty-First Century. Endocrinol. Metab. Clin. N. Am. 2018, 47, xiii–xiv. [Google Scholar] [CrossRef]
- Rindi, G.; Klimstra, D.S.; Abedi-Ardekani, B.; Asa, S.L.; Bosman, F.T.; Brambilla, E.; Busam, K.J.; de Krijger, R.R.; Dietel, M.; El-Naggar, A.K.; et al. A common classification framework for neuroendocrine neoplasms: An International Agency for Research on Cancer (IARC) and World Health Organization (WHO) expert consensus proposal. Mod. Pathol. 2018, 31, 1770–1786. [Google Scholar] [CrossRef]
- Schimmack, S.; Svejda, B.; Lawrence, B.; Kidd, M.; Modlin, I.M. The diversity and commonalities of gastroenteropancreatic neuroendocrine tumors. Langenbecks Arch. Surg. 2011, 396, 273–298. [Google Scholar] [CrossRef] [PubMed]
- Lee, M.S.; O’Neil, B.H. Summary of emerging personalized medicine in neuroendocrine tumors: Are we on track? J. Gastrointest. Oncol. 2016, 7, 804–818. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Kloppel, G. Neuroendocrine Neoplasms: Dichotomy, Origin and Classifications. Visc. Med. 2017, 33, 324–330. [Google Scholar] [CrossRef] [PubMed]
- Inzani, F.; Petrone, G.; Rindi, G. The New World Health Organization Classification for Pancreatic Neuroendocrine Neoplasia. Endocrinol. Metab. Clin. N. Am. 2018, 47, 463–470. [Google Scholar] [CrossRef] [PubMed]
- Popa, O.; Taban, S.M.; Pantea, S.; Plopeanu, A.D.; Barna, R.A.; Cornianu, M.; Pascu, A.A.; Dema, A.L.C. The new WHO classification of gastrointestinal neuroendocrine tumors and immunohistochemical expression of somatostatin receptor 2 and 5. Exp. Ther. Med. 2021, 22, 1179. [Google Scholar] [CrossRef] [PubMed]
- Gaudenzi, G.; Carra, S.; Dicitore, A.; Cantone, M.C.; Persani, L.; Vitale, G. Fishing for neuroendocrine tumors. Endocr. Relat. Cancer 2020, 27, R163–R176. [Google Scholar] [CrossRef] [PubMed]
- Lopes, M.B.S. The 2017 World Health Organization classification of tumors of the pituitary gland: A summary. Acta Neuropathol. 2017, 134, 521–535. [Google Scholar] [CrossRef]
- Amlashi, F.G.; Tritos, N.A. Thyrotropin-secreting pituitary adenomas: Epidemiology, diagnosis, and management. Endocrine 2016, 52, 427–440. [Google Scholar] [CrossRef]
- Colao, A.; Faggiano, A.; Pivonello, R. Somatostatin analogues: Treatment of pituitary and neuroendocrine tumors. Prog. Brain Res. 2010, 182, 281–294. [Google Scholar] [CrossRef]
- Dhillon, K.S.; Cohan, P.; Kelly, D.F.; Darwin, C.H.; Iyer, K.V.; Chopra, I.J. Treatment of hyperthyroidism associated with thyrotropin-secreting pituitary adenomas with iopanoic acid. J. Clin. Endocrinol. Metab. 2004, 89, 708–711. [Google Scholar] [CrossRef][Green Version]
- Ma, Z.-Y.; Gong, Y.-F.; Zhuang, H.-K.; Zhou, Z.-X.; Huang, S.-Z.; Zou, Y.-P.; Huang, B.-W.; Sun, Z.-H.; Zhang, C.-Z.; Tang, Y.-Q.; et al. Pancreatic neuroendocrine tumors: A review of serum biomarkers, staging, and management. World J. Gastroenterol. 2020, 26, 2305–2322. [Google Scholar] [CrossRef] [PubMed]
- De Herder, W.W.; Hofland, L.J.; van der Lely, A.J.; Lamberts, S.W. Somatostatin receptors in gastroentero-pancreatic neuroendocrine tumours. Endocr. Relat. Cancer 2003, 10, 451–458. [Google Scholar] [CrossRef] [PubMed]
- Modlin, I.M.; Oberg, K.; Chung, D.C.; Jensen, R.T.; de Herder, W.W.; Thakker, R.V.; Caplin, M.; Delle Fave, G.; Kaltsas, G.A.; Krenning, E.P.; et al. Gastroenteropancreatic neuroendocrine tumours. Lancet Oncol. 2008, 9, 61–72. [Google Scholar] [CrossRef] [PubMed]
- Pape, U.F.; Hocker, M.; Seuss, U.; Wiedenmann, B. New molecular aspects in the diagnosis and therapy of neuroendocrine tumors of the gastroenteropancreatic system. Recent. Results Cancer Res. 2000, 153, 45–60. [Google Scholar] [CrossRef]
- Oberg, K. The Genesis of the Neuroendocrine Tumors Concept: From Oberndorfer to 2018. Endocrinol. Metab. Clin. North Am. 2018, 47, 711–731. [Google Scholar] [CrossRef]
- Massironi, S.; Sciola, V.; Peracchi, M.; Ciafardini, C.; Spampatti, M.P.; Conte, D. Neuroendocrine tumors of the gastro-entero-pancreatic system. World J. Gastroenterol. 2008, 14, 5377–5384. [Google Scholar] [CrossRef]
- Hu, Y.; Ye, Z.; Wang, F.; Qin, Y.; Xu, X.; Yu, X.; Ji, S. Role of Somatostatin Receptor in Pancreatic Neuroendocrine Tumor Development, Diagnosis, and Therapy. Front. Endocrinol. 2021, 12, 679000. [Google Scholar] [CrossRef]
- Qian, Z.R.; Li, T.; Ter-Minassian, M.; Yang, J.; Chan, J.A.; Brais, L.K.; Masugi, Y.; Thiaglingam, A.; Brooks, N.; Nishihara, R.; et al. Association between Somatostatin Receptor Expression and Clinical Outcomes in Neuroendocrine Tumors. Pancreas 2016, 45, 1386–1393. [Google Scholar] [CrossRef]
- Corleto, V.D.; Falconi, M.; Panzuto, F.; Milione, M.; De Luca, O.; Perri, P.; Cannizzaro, R.; Bordi, C.; Pederzoli, P.; Scarpa, A.; et al. Somatostatin Receptor Subtypes 2 and 5 Are Associated with Better Survival in Well-Differentiated Endocrine Carcinomas. Neuroendocrinology 2009, 89, 223–230. [Google Scholar] [CrossRef]
- Diakatou, E.; Kaltsas, G.; Tzivras, M.; Kanakis, G.; Papaliodi, E.; Kontogeorgos, G. Somatostatin and Dopamine Receptor Profile of Gastroenteropancreatic Neuroendocrine Tumors: An Immunohistochemical Study. Endocr. Pathol. 2011, 22, 24–30. [Google Scholar] [CrossRef]
- Papotti, M.; Bongiovanni, M.; Volante, M.; Allìa, E.; Landolfi, S.; Helboe, L.; Schindler, M.; Cole, S.; Bussolati, G. Expression of somatostatin receptor types 1–5 in 81 cases of gastrointestinal and pancreatic endocrine tumors. Virchows Arch. 2014, 440, 461–475. [Google Scholar] [CrossRef] [PubMed]
- Zamora, V.; Cabanne, A.; Salanova, R.; Bestani, C.; Domenichini, E.; Marmissolle, F.; Giacomi, N.; O’Connor, J.; Méndez, G.; Roca, E. Immunohistochemical expression of somatostatin receptors in digestive endocrine tumours. Dig. Liver Dis. 2010, 42, 220–225. [Google Scholar] [CrossRef] [PubMed]
- Wang, Y.; Wang, W.; Jin, K.; Fang, C.; Lin, Y.; Xue, L.; Feng, S.; Zhou, Z.; Shao, C.; Chen, M.; et al. Somatostatin receptor expression indicates improved prognosis in gastroenteropancreatic neuroendocrine neoplasm, and octreotide long-acting release is effective and safe in Chinese patients with advanced gastroenteropancreatic neuroendocrine tumors. Oncol. Lett. 2017, 13, 1165–1174. [Google Scholar] [CrossRef] [PubMed]
- Kaemmerer, D.; Träger, T.; Hoffmeister, M.; Sipos, B.; Hommann, M.; Sänger, J.; Schulz, S.; Lupp, A. Inverse expression of somatostatin and CXCR4 chemokine receptors in gastroenteropancreatic neuroendocrine neoplasms of different malignancy. Oncotarget 2015, 6, 27566–27579. [Google Scholar] [CrossRef] [PubMed]
- Righi, L.; Volante, M.; Tavaglione, V.; Billè, A.; Daniele, L.; Angusti, T.; Inzani, F.; Pelosi, G.; Rindi, G.; Papotti, M. Somatostatin receptor tissue distribution in lung neuroendocrine tumours: A clinicopathologic and immunohistochemical study of 218 ‘clinically aggressive’ cases. Ann. Oncol. 2010, 21, 548–555. [Google Scholar] [CrossRef] [PubMed]
- Srirajaskanthan, R.; Watkins, J.; Marelli, L.; Khan, K.; Caplin, M.E. Expression of Somatostatin and Dopamine 2 Receptors in Neuroendocrine Tumours and the Potential Role for New Biotherapies. Neuroendocrinology 2009, 89, 308–314. [Google Scholar] [CrossRef] [PubMed]
- Vitali, E.; Piccini, S.; Trivellin, G.; Smiroldo, V.; Lavezzi, E.; Zerbi, A.; Pepe, G.; Lania, A.G. The impact of SST2 trafficking and signaling in the treatment of pancreatic neuroendocrine tumors. Mol. Cell. Endocrinol. 2021, 527, 111226. [Google Scholar] [CrossRef]
- Theodoropoulou, M.; Stalla, G.K. Somatostatin receptors: From signaling to clinical practice. Front. Neuroendocrinol. 2013, 34, 228–252. [Google Scholar] [CrossRef]
- Costanzi, E.; Simioni, C.; Conti, I.; Laface, I.; Varano, G.; Brenna, C.; Neri, L.M. Two neuroendocrine G protein-coupled receptor molecules, somatostatin and melatonin: Physiology of signal transduction and therapeutic perspectives. J. Cell. Physiol. 2020, 236, 2505–2518. [Google Scholar] [CrossRef]
- Briest, F.; Grabowski, P. PI3K-AKT-mTOR-Signaling and beyond: The Complex Network in Gastroenteropancreatic Neuroendocrine Neoplasms. Theranostics 2014, 4, 336–365. [Google Scholar] [CrossRef]
- De La Torre, N.G.; Wass, J.A.H.; Turner, H.E. Antiangiogenic effects of somatostatin analogues. Clin. Endocrinol. 2002, 57, 425–441. [Google Scholar] [CrossRef] [PubMed]
- Annunziata, M.; Luque, R.M.; Duran-Prado, M.; Baragli, A.; Grande, C.; Volante, M.; Gahete, M.D.; Deltetto, F.; Camanni, M.; Ghigo, E.; et al. Somatostatin and somatostatin analogues reduce PDGF-induced endometrial cell proliferation and motility. Human. Reprod. 2012, 27, 2117–2129. [Google Scholar] [CrossRef] [PubMed]
- Pola, S.; Cattaneo, M.G.; Vicentini, L.M. Anti-migratory and Anti-invasive Effect of Somatostatin in Human Neuroblastoma Cells. J. Biol. Chem. 2003, 278, 40601–40606. [Google Scholar] [CrossRef] [PubMed]
- Gatto, F.; Barbieri, F.; Arvigo, M.; Thellung, S.; Amarù, J.; Albertelli, M.; Ferone, D.; Florio, T. Biological and Biochemical Basis of the Differential Efficacy of First and Second Generation Somatostatin Receptor Ligands in Neuroendocrine Neoplasms. Int. J. Mol. Sci. 2019, 20, 3940. [Google Scholar] [CrossRef] [PubMed]
- Dasgupta, P. Somatostatin analogues: Multiple roles in cellular proliferation, neoplasia, and angiogenesis. Pharmacol. Ther. 2004, 102, 61–85. [Google Scholar] [CrossRef] [PubMed]
- Reubi, J.; Waser, B.; Schaer, J.-C.; Laissue, J.A. Somatostatin receptor sst1–sst5 expression in normal and neoplastic human tissues using receptor autoradiography with subtype-selective ligands. Eur. J. Nucl. Med. 2001, 28, 836–846. [Google Scholar] [CrossRef] [PubMed]
- Reubi, J.C.; Laissue, J.; Waser, B.; Horisberger, U.; Schaer, J.C. Expression of somatostatin receptors in normal, inflamed, and neoplastic human gastrointestinal tissues. Ann. N. Y. Acad. Sci. 1994, 733, 122–137. [Google Scholar] [CrossRef]
- Wang, L.; Tang, K.; Zhang, Q.; Li, H.; Wen, Z.; Zhang, H.; Zhang, H. Somatostatin receptor-based molecular imaging and therapy for neuroendocrine tumors. Biomed. Res. Int. 2013, 2013, 102819. [Google Scholar] [CrossRef]
- Xu, C.; Zhang, H. Somatostatin receptor based imaging and radionuclide therapy. Biomed. Res. Int. 2015, 2015, 917968. [Google Scholar] [CrossRef]
- Kim, K.; Kim, S.J. Lu-177-Based Peptide Receptor Radionuclide Therapy for Advanced Neuroendocrine Tumors. Nucl. Med. Mol. Imaging 2018, 52, 208–215. [Google Scholar] [CrossRef]
- Liu, Y.; Ren, Y.N.; Cui, Y.; Liu, S.; Yang, Z.; Zhu, H.; Li, N. Inspired by novel radiopharmaceuticals: Rush hour of nuclear medicine. Chin. J. Cancer Res. 2023, 35, 470–482. [Google Scholar] [CrossRef] [PubMed]
- Eychenne, R.; Bouvry, C.; Bourgeois, M.; Loyer, P.; Benoist, E.; Lepareur, N. Overview of Radiolabeled Somatostatin Analogs for Cancer Imaging and Therapy. Molecules 2020, 25, 4012. [Google Scholar] [CrossRef] [PubMed]
- De Herder, W.W. When and How to Use Somatostatin Analogues. Endocrinol. Metab. Clin. N. Am. 2018, 47, 549–555. [Google Scholar] [CrossRef] [PubMed]
- Fehmann, H.C.; Wulbrand, U.; Arnold, R. Treatment of endocrine gastroenteropancreatic tumors with somatostatin analogues. Recent. Results Cancer Res. 2000, 153, 15–22. [Google Scholar] [CrossRef] [PubMed]
- Ferone, D.; Resmini, E.; Boschetti, M.; Arvigo, M.; Albanese, V.; Ceresola, E.; Pivonello, R.; Albertelli, M.; Bianchi, F.; Giusti, M.; et al. Potential indications for somatostatin analogues: Immune system and limphoproliferative disorders. J. Endocrinol. Investig. 2005, 28 (Suppl. S11), 111–117. [Google Scholar]
- Bertherat, J.; Brue, T.; Enjalbert, A.; Gunz, G.; Rasolonjanahary, R.; Warnet, A.; Jaquet, P.; Epelbaum, J. Somatostatin receptors on thyrotropin-secreting pituitary adenomas: Comparison with the inhibitory effects of octreotide upon in vivo and in vitro hormonal secretions. J. Clin. Endocrinol. Metab. 1992, 75, 540–546. [Google Scholar] [CrossRef] [PubMed]
- Bornschein, J.; Drozdov, I.; Malfertheiner, P. Octreotide LAR: Safety and tolerability issues. Expert. Opin. Drug Saf. 2009, 8, 755–768. [Google Scholar] [CrossRef]
- Caron, P.; Arlot, S.; Bauters, C.; Chanson, P.; Kuhn, J.M.; Pugeat, M.; Marechaud, R.; Teutsch, C.; Vidal, E.; Sassano, P. Efficacy of the long-acting octreotide formulation (octreotide-LAR) in patients with thyrotropin-secreting pituitary adenomas. J. Clin. Endocrinol. Metab. 2001, 86, 2849–2853. [Google Scholar] [CrossRef]
- Gourgiotis, L.; Skarulis, M.C.; Brucker-Davis, F.; Oldfield, E.H.; Sarlis, N.J. Effectiveness of long-acting octreotide in suppressing hormonogenesis and tumor growth in thyrotropin-secreting pituitary adenomas: Report of two cases. Pituitary 2001, 4, 135–143. [Google Scholar] [CrossRef]
- Shimatsu, A.; Murabe, H.; Kamoi, K.; Suzuki, Y.; Nakao, K. Treatment of thyrotropin-secreting pituitary adenomas with octreotide. Endocr. J. 1999, 46, 113–123. [Google Scholar] [CrossRef][Green Version]
- Canobbio, L.; Cannata, D.; Miglietta, L.; Pace, M.; Boccardo, F. Use of long-acting somatostatin analog, lanreotide, in neuroendocrine tumors. Oncol. Rep. 1994, 1, 129–131. [Google Scholar] [CrossRef] [PubMed]
- Ducreux, M.; Ruszniewski, P.; Chayvialle, J.A.; Blumberg, J.; Cloarec, D.; Michel, H.; Raymond, J.M.; Dupas, J.L.; Gouerou, H.; Jian, R.; et al. The antitumoral effect of the long-acting somatostatin analog lanreotide in neuroendocrine tumors. Am. J. Gastroenterol. 2000, 95, 3276–3281. [Google Scholar] [CrossRef] [PubMed]
- Kuhn, J.M.; Arlot, S.; Lefebvre, H.; Caron, P.; Cortet-Rudelli, C.; Archambaud, F.; Chanson, P.; Tabarin, A.; Goth, M.I.; Blumberg, J.; et al. Evaluation of the treatment of thyrotropin-secreting pituitary adenomas with a slow release formulation of the somatostatin analog lanreotide. J. Clin. Endocrinol. Metab. 2000, 85, 1487–1491. [Google Scholar] [CrossRef] [PubMed]
- Ben-Shlomo, A.; Melmed, S. Pasireotide—A somatostatin analog for the potential treatment of acromegaly, neuroendocrine tumors and Cushing’s disease. IDrugs 2007, 10, 885–895. [Google Scholar] [PubMed]
- Cives, M.; Kunz, P.L.; Morse, B.; Coppola, D.; Schell, M.J.; Campos, T.; Nguyen, P.T.; Nandoskar, P.; Khandelwal, V.; Strosberg, J.R. Phase II clinical trial of pasireotide long-acting repeatable in patients with metastatic neuroendocrine tumors. Endocr. Relat. Cancer 2015, 22, 1–9. [Google Scholar] [CrossRef] [PubMed]
- Feelders, R.A.; de Herder, W.W.; Neggers, S.J.; van der Lely, A.J.; Hofland, L.J. Pasireotide, a multi-somatostatin receptor ligand with potential efficacy for treatment of pituitary and neuroendocrine tumors. Drugs Today 2013, 49, 89–103. [Google Scholar] [CrossRef] [PubMed]
- Kvols, L.K.; Oberg, K.E.; O’Dorisio, T.M.; Mohideen, P.; de Herder, W.W.; Arnold, R.; Hu, K.; Zhang, Y.; Hughes, G.; Anthony, L.; et al. Pasireotide (SOM230) shows efficacy and tolerability in the treatment of patients with advanced neuroendocrine tumors refractory or resistant to octreotide LAR: Results from a phase II study. Endocr. Relat. Cancer 2012, 19, 657–666. [Google Scholar] [CrossRef]
- Mohamed, A.; Blanchard, M.P.; Albertelli, M.; Barbieri, F.; Brue, T.; Niccoli, P.; Delpero, J.R.; Monges, G.; Garcia, S.; Ferone, D.; et al. Pasireotide and octreotide antiproliferative effects and sst2 trafficking in human pancreatic neuroendocrine tumor cultures. Endocr. Relat. Cancer 2014, 21, 691–704. [Google Scholar] [CrossRef]
- Vitale, G.; Dicitore, A.; Sciammarella, C.; Di Molfetta, S.; Rubino, M.; Faggiano, A.; Colao, A. Pasireotide in the treatment of neuroendocrine tumors: A review of the literature. Endocr. Relat. Cancer 2018, 25, R351–R364. [Google Scholar] [CrossRef]
- Walls, G.V.; Stevenson, M.; Soukup, B.S.; Lines, K.E.; Grossman, A.B.; Schmid, H.A.; Thakker, R.V. Pasireotide Therapy of Multiple Endocrine Neoplasia Type 1-Associated Neuroendocrine Tumors in Female Mice Deleted for an Men1 Allele Improves Survival and Reduces Tumor Progression. Endocrinology 2016, 157, 1789–1798. [Google Scholar] [CrossRef]
- Plöckinger, U.; Hoffmann, U.; Geese, M.; Lupp, A.; Buchfelder, M.; Flitsch, J.; Vajkoczy, P.; Jakob, W.; Saeger, W.; Schulz, S.; et al. DG3173 (somatoprim), a unique somatostatin receptor subtypes 2-, 4- and 5-selective analogue, effectively reduces GH secretion in human GH-secreting pituitary adenomas even in Octreotide non-responsive tumours. Eur. J. Endocrinol. 2012, 166, 223–234. [Google Scholar] [CrossRef] [PubMed]
- Shimon, I.; Rubinek, T.; Hadani, M.; Alhadef, N. PTR-3173 (Somatoprim™), a novel somatostatin analog with affinity for somatostatin receptors 2, 4 and 5 is a potent inhibitor of human GH secretion. J. Endocrinol. Investig. 2014, 27, 721–727. [Google Scholar] [CrossRef] [PubMed]
- Strosberg, J.; Kvols, L. Antiproliferative effect of somatostatin analogs in gastroenteropancreatic neuroendocrine tumors. World J. Gastroenterol. 2010, 16, 2963–2970. [Google Scholar] [CrossRef] [PubMed]
- Serri, O.; Brazeau, P.; Kachra, Z.; Posner, B. Octreotide inhibits insulin-like growth factor-I hepatic gene expression in the hypophysectomized rat: Evidence for a direct and indirect mechanism of action. Endocrinology 1992, 130, 1816–1821. [Google Scholar] [CrossRef] [PubMed]
- Zapata, P.D.; Ropero, R.M.; Valencia, A.M.; Buscail, L.; López, J.I.; Martín-Orozco, R.M.; Prieto, J.C.; Angulo, J.; Susini, C.; López-Ruiz, P.; et al. Autocrine Regulation of Human Prostate Carcinoma Cell Proliferation by Somatostatin through the Modulation of the SH2 Domain Containing Protein Tyrosine Phosphatase (SHP)-1. J. Clin. Endocrinol. Metab. 2002, 87, 915–926. [Google Scholar] [CrossRef]
- Thangaraju, M.; Sharma, K.; Liu, D.; Shen, S.H.; Srikant, C.B. Interdependent regulation of intracellular acidification and SHP-1 in apoptosis. Cancer Res. 1999, 59, 1649–1654. [Google Scholar]
- Caplin, M.E.; Pavel, M.; Cwikla, J.B.; Phan, A.T.; Raderer, M.; Sedlackova, E.; Cadiot, G.; Wolin, E.M.; Capdevila, J.; Wall, L.; et al. Lanreotide in metastatic enteropancreatic neuroendocrine tumors. N. Engl. J. Med. 2014, 371, 224–233. [Google Scholar] [CrossRef]
- Yao, J.C.; Shah, M.H.; Ito, T.; Bohas, C.L.; Wolin, E.M.; Van Cutsem, E.; Hobday, T.J.; Okusaka, T.; Capdevila, J.; de Vries, E.G.; et al. Everolimus for advanced pancreatic neuroendocrine tumors. N. Engl. J. Med. 2011, 364, 514–523. [Google Scholar] [CrossRef]
- Florio, T. Molecular mechanisms of the antiproliferative activity of somatostatin receptors (SSTRs) in neuroendocrine tumors. Front. Biosci. 2008, 13, 822–840. [Google Scholar] [CrossRef][Green Version]
- Barbieri, F.; Bajetto, A.; Pattarozzi, A.; Gatti, M.; Würth, R.; Thellung, S.; Corsaro, A.; Villa, V.; Nizzari, M.; Florio, T. Peptide Receptor Targeting in Cancer: The Somatostatin Paradigm. Int. J. Pept. 2013, 2013, 1–20. [Google Scholar] [CrossRef]
- Batista, D.L.; Zhang, X.; Gejman, R.; Ansell, P.J.; Zhou, Y.; Johnson, S.A.; Swearingen, B.; Hedley-Whyte, E.T.; Stratakis, C.A.; Klibanski, A. The Effects of SOM230 on Cell Proliferation and Adrenocorticotropin Secretion in Human Corticotroph Pituitary Adenomas. J. Clin. Endocrinol. Metab. 2006, 91, 4482–4488. [Google Scholar] [CrossRef] [PubMed]
- Guillermet, J.; Saint-Laurent, N.; Rochaix, P.; Cuvillier, O.; Levade, T.; Schally, A.V.; Pradayrol, L.; Buscail, L.; Susini, C.; Bousquet, C. Somatostatin receptor subtype 2 sensitizes human pancreatic cancer cells to death ligand-induced apoptosis. Proc. Natl. Acad. Sci. USA 2002, 100, 155–160. [Google Scholar] [CrossRef] [PubMed]
- Kumar, M.; Liu, Z.-R.; Thapa, L.; Chang, Q.; Wang, D.-Y.; Qin, R.-Y. Antiangiogenic effect of somatostatin receptor subtype 2 on pancreatic cancer cell line: Inhibition of vascular endothelial growth factor and matrix metalloproteinase-2 expressionin vitro. World J. Gastroenterol. 2004, 10, 393–399. [Google Scholar] [CrossRef] [PubMed]
- Wang, C.; Tang, C. Inhibition of human gastric cancer metastasis by ocreotide in vitro and in vivo. Zhonghua Yi Xue Za Zhi 2002, 82, 19–22. [Google Scholar]
- Herrera-Martinez, A.D.; Hofland, J.; Hofland, L.J.; Brabander, T.; Eskens, F.; Galvez Moreno, M.A.; Luque, R.M.; Castano, J.P.; de Herder, W.W.; Feelders, R.A. Targeted Systemic Treatment of Neuroendocrine Tumors: Current Options and Future Perspectives. Drugs 2019, 79, 21–42. [Google Scholar] [CrossRef]
- Angelousi, A.; Koumarianou, A.; Chatzellis, E.; Kaltsas, G. Resistance of neuroendocrine tumours to somatostatin analogs. Expert. Rev. Endocrinol. Metab. 2023, 18, 33–52. [Google Scholar] [CrossRef]
- Maxwell, J.E.; Sherman, S.K.; Menda, Y.; Wang, D.; O’Dorisio, T.M.; Howe, J.R. Limitations of somatostatin scintigraphy in primary small bowel neuroendocrine tumors. J. Surg. Res. 2014, 190, 548–553. [Google Scholar] [CrossRef]
- Wolin, E.M. The expanding role of somatostatin analogs in the management of neuroendocrine tumors. Gastrointest. Cancer Res. 2012, 5, 161–168. [Google Scholar]
- Tollefsen, S.E.; Solheim, O.; Mjones, P.; Torp, S.H. Meningiomas and Somatostatin Analogs: A Systematic Scoping Review on Current Insights and Future Perspectives. Int. J. Mol. Sci. 2023, 24, 4793. [Google Scholar] [CrossRef]
- Gomes-Porras, M.; Cardenas-Salas, J.; Alvarez-Escola, C. Somatostatin Analogs in Clinical Practice: A Review. Int. J. Mol. Sci. 2020, 21, 1682. [Google Scholar] [CrossRef]
- Gariani, K.; Meyer, P.; Philippe, J. Implications of Somatostatin Analogues in the Treatment of Acromegaly. Eur. Endocrinol. 2013, 9, 132–135. [Google Scholar] [CrossRef] [PubMed]
- Tawfik, B.; Ray, D.; Moynihan, M.; Princic, N. Costs of treatment change following first-line somatostatin analog monotherapy among patients with neuroendocrine tumors. J. Med. Econ. 2021, 24, 1337–1345. [Google Scholar] [CrossRef] [PubMed]
- Huynh, L.; Cai, B.; Cheng, M.; Lax, A.; Lejeune, D.; Duh, M.S.; Kim, M.K. Analysis of Real-World Treatment Patterns, Healthcare Resource Utilization, and Costs between Octreotide and Lanreotide among Patients with Neuroendocrine Tumors. Pancreas 2019, 48, 1126–1135. [Google Scholar] [CrossRef] [PubMed]
- Broder, M.S.; Cai, B.; Chang, E.; Yan, T.; Benson, A.B., 3rd. First-line systemic treatment adherence, healthcare resource utilization, and costs in patients with gastrointestinal neuroendocrine tumors (GI NETs) in the USA. J. Med. Econ. 2018, 21, 821–826. [Google Scholar] [CrossRef]
- Stueven, A.K.; Kayser, A.; Wetz, C.; Amthauer, H.; Wree, A.; Tacke, F.; Wiedenmann, B.; Roderburg, C.; Jann, H. Somatostatin Analogues in the Treatment of Neuroendocrine Tumors: Past, Present and Future. Int. J. Mol. Sci. 2019, 20, 49. [Google Scholar] [CrossRef]
- Mazziotti, G.; Mosca, A.; Frara, S.; Vitale, G.; Giustina, A. Somatostatin analogs in the treatment of neuroendocrine tumors: Current and emerging aspects. Expert. Opin. Pharmacother. 2017, 18, 1679–1689. [Google Scholar] [CrossRef]
- Andreasi, V.; Partelli, S.; Muffatti, F.; Manzoni, M.F.; Capurso, G.; Falconi, M. Update on gastroenteropancreatic neuroendocrine tumors. Dig. Liver Dis. 2021, 53, 171–182. [Google Scholar] [CrossRef]
- Cives, M.; Strosberg, J. An update on gastroenteropancreatic neuroendocrine tumors. Oncology 2014, 28, 749–756, 758. [Google Scholar]
- Shankaran, H.; Wiley, H.S.; Resat, H. Receptor downregulation and desensitization enhance the information processing ability of signalling receptors. BMC Syst. Biol. 2007, 1, 48. [Google Scholar] [CrossRef]
- Anthony, L.B.; O’Dorisio, T.M. Opportunities to Improve Symptom Control with Somatostatin Congeners in GEP-NETs: A Review of Key Issues. Oncologist 2021, 26, e1171–e1178. [Google Scholar] [CrossRef]
- Ramirez, J.L.; Mouchantaf, R.; Kumar, U.; Otero Corchon, V.; Rubinstein, M.; Low, M.J.; Patel, Y.C. Brain somatostatin receptors are up-regulated in somatostatin-deficient mice. Mol. Endocrinol. 2002, 16, 1951–1963. [Google Scholar] [CrossRef] [PubMed]
- Scott, A.T.; Howe, J.R. Evaluation and Management of Neuroendocrine Tumors of the Pancreas. Surg. Clin. N. Am. 2019, 99, 793–814. [Google Scholar] [CrossRef] [PubMed]
- Spada, F.; Rossi, R.E.; Kara, E.; Laffi, A.; Massironi, S.; Rubino, M.; Grimaldi, F.; Bhoori, S.; Fazio, N. Carcinoid Syndrome and Hyperinsulinemic Hypoglycemia Associated with Neuroendocrine Neoplasms: A Critical Review on Clinical and Pharmacological Management. Pharmaceuticals 2021, 14, 539. [Google Scholar] [CrossRef] [PubMed]
- Brighi, N.; Panzuto, F.; Modica, R.; Gelsomino, F.; Albertelli, M.; Pusceddu, S.; Massironi, S.; Lamberti, G.; Rinzivillo, M.; Faggiano, A.; et al. Biliary Stone Disease in Patients with Neuroendocrine Tumors Treated with Somatostatin Analogs: A Multicenter Study. Oncologist 2020, 25, 259–265. [Google Scholar] [CrossRef]
| Somatostatin Analogue | Affinity for Somatostatin Receptors | Selectivity | Duration of Action | Application in NET |
|---|---|---|---|---|
| Octreotide | SSTR2 > SSTR5 > SSTR3 > SSTR1 > SSTR4 | high | Long | Symptom control, growth inhibition, and hormone control in pancreatic, intestinal, lung, neck, and thyroid NET |
| Lanreotide | SSTR2 = SSTR5 > SSTR3 > SSTR1 > SSTR4 | high | Long | Symptom control, growth inhibition, and hormone control in pancreatic, intestinal, lung, and neck NET |
| Pasireotide | SSTR5 > SSTR2 > SSTR3 > SSTR1 > SSTR4 | high | Long | Symptom control, growth inhibition, and hormone control in pancreatic and intestinal NET |
| Vapreotide | SSTR2 > SSTR5 > SSTR3 > SSTR1 > SSTR4 | high | Short | Diagnosis and assessment of somatostatin receptors in NETs |
| Somatuline | SSTR2 > SSTR5 > SSTR3 > SSTR1 > SSTR4 | high | Medium | Symptom control, growth inhibition, and hormone control in pancreatic, intestinal, lung, neck, and thyroid NET |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2023 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Milewska-Kranc, A.; Ćwikła, J.B.; Kolasinska-Ćwikła, A. The Role of Receptor–Ligand Interaction in Somatostatin Signaling Pathways: Implications for Neuroendocrine Tumors. Cancers 2024, 16, 116. https://doi.org/10.3390/cancers16010116
Milewska-Kranc A, Ćwikła JB, Kolasinska-Ćwikła A. The Role of Receptor–Ligand Interaction in Somatostatin Signaling Pathways: Implications for Neuroendocrine Tumors. Cancers. 2024; 16(1):116. https://doi.org/10.3390/cancers16010116
Chicago/Turabian StyleMilewska-Kranc, Agnieszka, Jarosław B. Ćwikła, and Agnieszka Kolasinska-Ćwikła. 2024. "The Role of Receptor–Ligand Interaction in Somatostatin Signaling Pathways: Implications for Neuroendocrine Tumors" Cancers 16, no. 1: 116. https://doi.org/10.3390/cancers16010116
APA StyleMilewska-Kranc, A., Ćwikła, J. B., & Kolasinska-Ćwikła, A. (2024). The Role of Receptor–Ligand Interaction in Somatostatin Signaling Pathways: Implications for Neuroendocrine Tumors. Cancers, 16(1), 116. https://doi.org/10.3390/cancers16010116





