Intention to Inform Relatives, Rates of Cascade Testing, and Preference for Patient-Mediated Communication in Families Concerned with Hereditary Breast and Ovarian Cancer and Lynch Syndrome: The Swiss CASCADE Cohort
Abstract
:Simple Summary
Abstract
1. Introduction
2. Material and Methods
3. Data Analyses
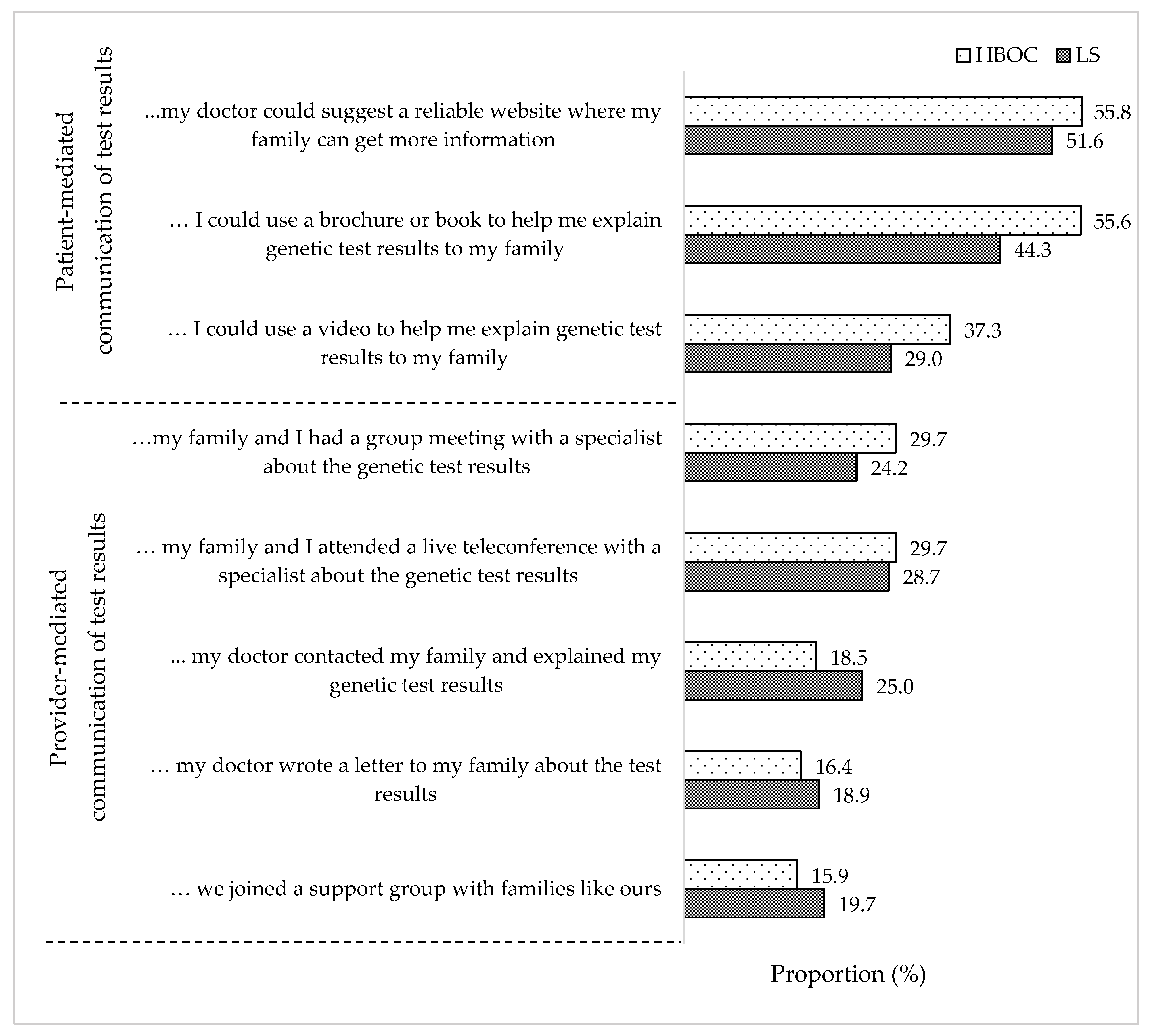
4. Results
5. Discussion
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Ferlay, J.; Soerjomataram, I.; Dikshit, R.; Eser, S.; Mathers, C.; Rebelo, M.; Parkin, D.M.; Forman, D.; Bray, F. Cancer incidence and mortality worldwide: Sources, methods and major patterns in GLOBOCAN 2012. Int. J. Cancer 2015, 136, E359–E386. [Google Scholar] [CrossRef] [PubMed]
- Balmana, J.; Diez, O.; Rubio, I.T.; Cardoso, F. BRCA in breast cancer: ESMO Clinical Practice Guidelines. Ann. Oncol. 2011, 22 (Suppl. 6), vi31–vi34. [Google Scholar] [CrossRef] [PubMed]
- Weiss, J.M.; Gupta, S.; Burke, C.A.; Axell, L.; Chen, L.M.; Chung, D.C.; Clayback, K.M.; Dallas, S.; Felder, S.; Gbolahan, O.; et al. NCCN Guidelines(R) Insights: Genetic/Familial High-Risk Assessment: Colorectal, Version 1.2021. J. Natl. Compr. Canc. Netw. 2021, 19, 1122–1132. [Google Scholar] [PubMed]
- Crosbie, E.J.; Ryan, N.A.J.; Arends, M.J.; Bosse, T.; Burn, J.; Cornes, J.M.; Crawford, R.; Eccles, D.; Frayling, I.M.; Ghaem-Maghami, S.; et al. The Manchester International Consensus Group recommendations for the management of gynecological cancers in Lynch syndrome. Genet. Med. 2019, 21, 2390–2400. [Google Scholar] [CrossRef] [Green Version]
- Vos, J.R.; Giepmans, L.; Rohl, C.; Geverink, N.; Hoogerbrugge, N.; Ligtenberg, M.; Kets, M.; Sijmons, R.; Evans, G.; Woodward, E.; et al. Boosting care and knowledge about hereditary cancer: European Reference Network on Genetic Tumour Risk Syndromes. Fam. Cancer 2019, 18, 281–284. [Google Scholar] [CrossRef] [Green Version]
- Therkildsen, C.; Jensen, L.H.; Rasmussen, M.; Bernstein, I. An Update on Immune Checkpoint Therapy for the Treatment of Lynch Syndrome. Clin. Exp. Gastroenterol. 2021, 14, 181–197. [Google Scholar] [CrossRef]
- Hampel, H. Genetic counseling and cascade genetic testing in Lynch syndrome. Fam. Cancer 2016, 15, 423–427. [Google Scholar] [CrossRef]
- Khoury, M.J.; Iademarco, M.F.; Riley, W.T. Precision Public Health for the Era of Precision Medicine. Am. J. Prev. Med. 2016, 50, 398–401. [Google Scholar] [CrossRef] [Green Version]
- Ficarazzi, F.; Vecchi, M.; Ferrari, M.; Pierotti, M.A. Towards population-based genetic screenings for breast and ovarian cancer: A comprehensive review from economic evaluations to patient perspectives. Breast 2021, 58, 121–129. [Google Scholar] [CrossRef]
- Hao, J.; Hassen, D.; Gudgeon, J.M.; Snyder, S.R.; Hampel, H.; Williams, M.S.; Sharaf, R.N.; Lu, C.Y.; Williams, J.L.; Schlieder, V.; et al. Economic Evaluation of Universal Lynch Syndrome Screening Protocols among Newly Diagnosed Patients with Colorectal Cancer. J. Pers. Med. 2021, 11, 1284. [Google Scholar] [CrossRef]
- Salikhanov, I.; Heinimann, K.; Chappuis, P.; Buerki, N.; Graffeo, R.; Heinzelmann, V.; Rabaglio, M.; Taborelli, M.; Wieser, S.; Katapodi, M.C. Swiss cost-effectiveness analysis of universal screening for Lynch syndrome of patients with colorectal cancer followed by cascade genetic testing of relatives. J. Med Genet. 2021. [Google Scholar] [CrossRef] [PubMed]
- Woodward, E.R.; Green, K.; Burghel, G.J.; Bulman, M.; Clancy, T.; Lalloo, F.; Schlecht, H.; Wallace, A.J.; Evans, D.G. 30 year experience of index case identification and outcomes of cascade testing in high-risk breast and colorectal cancer predisposition genes. Eur. J. Hum. Genet. 2021, 1–7. [Google Scholar] [CrossRef] [PubMed]
- Menko, F.H.; Ter Stege, J.A.; Van Der Kolk, L.E.; Jeanson, K.N.; Schats, W.; Moha, D.A.; Bleiker, E.M.A. The uptake of presymptomatic genetic testing in hereditary breast-ovarian cancer and Lynch syndrome: A systematic review of the literature and implications for clinical practice. Fam. Cancer 2018, 18, 127–135. [Google Scholar] [CrossRef] [PubMed]
- Sharaf, R.N.; Myer, P.; Stave, C.; Diamond, L.C.; Ladabaum, U. Uptake of Genetic Testing by Relatives of Lynch Syndrome Probands: A Systematic Review. Clin. Gastroenterol. Hepatol. 2013, 11, 1093–1100. [Google Scholar] [CrossRef] [PubMed]
- Muller, C.; Nielsen, S.M.; Hatchell, K.E.; Yang, S.; Michalski, S.T.; Hamlington, B.; Nussbaum, R.L.; Esplin, E.D.; Kupfer, S.S. Underdiagnosis of Hereditary Colorectal Cancers Among Medicare Patients: Genetic Testing Criteria for Lynch Syndrome Miss the Mark. JCO Precis. Oncol. 2021, 5, 1103–1111. [Google Scholar] [CrossRef] [PubMed]
- Ward, M.; Elder, B.; Habtemariam, M. Current Testing Guidelines: A Retrospective Analysis of a Community-Based Hereditary Cancer Program. J. Adv. Pract. Oncol. 2021, 12, 693–701. [Google Scholar]
- Nicolosi, P.; Ledet, E.; Yang, S.; Michalski, S.; Freschi, B.; O’Leary, E.; Esplin, E.D.; Nussbaum, R.L.; Sartor, O. Prevalence of Germline Variants in Prostate Cancer and Implications for Current Genetic Testing Guidelines. JAMA Oncol. 2019, 5, 523–528. [Google Scholar] [CrossRef] [Green Version]
- Katapodi, M.C.; Viassolo, V.; Caiata-Zufferey, M.; Nikolaidis, C.; Bührer-Landolt, R.; Buerki, N.; Graffeo, R.; Horváth, H.C.; Kurzeder, C.; Rabaglio, M.; et al. Cancer Predisposition Cascade Screening for Hereditary Breast/Ovarian Cancer and Lynch Syndromes in Switzerland: Study Protocol. JMIR Res. Protoc. 2017, 6, e184. [Google Scholar] [CrossRef]
- Ajzen, I. The theory of planned behavior-Organizational behavior and human decision processes. J. Appl. Soc. Psychol. 1991, 50, 179–211. [Google Scholar]
- Katapodi, M.C.; Facione, N.C.; Miaskowski, C.; Dodd, M.J.; Waters, C. The Influence of Social Support on Breast Cancer Screening in a Multicultural Community Sample. Oncol. Nurs. Forum 2002, 29, 845–852. [Google Scholar] [CrossRef]
- R Core Team. R: A Language and Environment for Statistical Computing; R Foundation for Statistical Computing: Vienna, Austria, 2013. [Google Scholar]
- Su, Y.-S.; Gelman, A.; Hill, J.; Yajima, M. Multiple Imputation with Diagnostics (mi) inR: Opening Windows into the Black Box. J. Stat. Softw. 2011, 45, 1–31. [Google Scholar] [CrossRef] [Green Version]
- Friedman, J.H.; Hastie, T.; Tibshirani, R. Regularization Paths for Generalized Linear Models via Coordinate Descent. J. Stat. Softw. 2010, 33, 1–22. [Google Scholar] [CrossRef] [Green Version]
- Cilluffo, G.; Sottile, G.; La Grutta, S.; Muggeo, V.M. The Induced Smoothed lasso: A practical framework for hypothesis testing in high dimensional regression. Stat. Methods Med Res. 2019, 29, 765–777. [Google Scholar] [CrossRef] [PubMed]
- Campion, W.M. Multiple Imputation for Nonresponse in Surveys-Rubin, D.B. J. Mark. Res. 1989, 26, 485–486. [Google Scholar]
- MacInnis, R.J.; Knight, J.A.; Chung, W.K.; Milne, R.L.; Whittemore, A.S.; Buchsbaum, R.; Liao, Y.; Zeinomar, N.; Dite, G.S.; Southey, M.C.; et al. Comparing 5-Year and Lifetime Risks of Breast Cancer using the Prospective Family Study Cohort. JNCI: J. Natl. Cancer Inst. 2021, 113, 785–791. [Google Scholar] [CrossRef]
- Bopp, M.; Spoerri, A.; Zwahlen, M.; Gutzwiller, F.; Paccaud, F.; Braun-Fahrländer, C.; Rougemont, A.; Egger, M. Cohort Profile: The Swiss National Cohort--a longitudinal study of 6.8 million people. Int. J. Epidemiol. 2009, 38, 379–384. [Google Scholar] [CrossRef] [Green Version]
- Griffin, N.E.; Buchanan, T.R.; Smith, S.H.; Leon, A.A.; Meyer, M.F.; Liu, J.; Tabak, R.G.; Fuh, K.C.; Thaker, P.H.; Powell, M.A.; et al. Low rates of cascade genetic testing among families with hereditary gynecologic cancer: An opportunity to improve cancer prevention. Gynecol. Oncol. 2020, 156, 140–146. [Google Scholar] [CrossRef] [Green Version]
- Abul-Husn, N.S.; Soper, E.R.; Braganza, G.T.; Rodriguez, J.E.; Zeid, N.; Cullina, S.; Bobo, D.; Moscati, A.; Merkelson, A.; Loos, R.J.F.; et al. Implementing genomic screening in diverse populations. Genome Med. 2021, 13, 1–11. [Google Scholar] [CrossRef]
- Cortesi, L.; Baldassarri, B.; Ferretti, S.; Razzaboni, E.; Bella, M.; Bucchi, L.; Canuti, D.; De Iaco, P.; De Santis, G.; Falcini, F.; et al. A regional population-based hereditary breast cancer screening tool in Italy: First 5-year results. Cancer Med. 2020, 9, 2579–2589. [Google Scholar] [CrossRef]
- Menko, F.H.; Jeanson, K.N.; Bleiker, E.M.; van Tiggelen, C.W.; Hogervorst, F.B.; Ter Stege, J.A.; Moha, D.A.; van der Kolk, L.E. The uptake of predictive DNA testing in 40 families with a pathogenic BRCA1/BRCA2 variant. An evaluation of the proband-mediated procedure. Eur. J. Hum. Genet. 2020, 28, 1020–1027. [Google Scholar] [CrossRef]
- Healey, E.; Taylor, N.; Greening, S.; Wakefield, C.E.; Warwick, L.; Williams, R.; Tucker, K. Quantifying family dissemination and identifying barriers to communication of risk information in Australian BRCA families. Genet. Med. 2017, 19, 1323–1331. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Lieberman, S.; Lahad, A.; Tomer, A.; Koka, S.; BenUziyahu, M.; Raz, A.; Levy-Lahad, E. Familial communication and cascade testing among relatives of BRCA population screening participants. Genet. Med. 2018, 20, 1446–1454. [Google Scholar] [CrossRef] [PubMed]
- Braley, E.F.; Bedard, A.C.; Nuk, J.; Hong, Q.; Bedard, J.E.J.; Sun, S.; Schrader, K.A. Patient ethnicity and cascade genetic testing: A descriptive study of a publicly funded hereditary cancer program. Fam. Cancer 2021, 2021, 1–6. [Google Scholar] [CrossRef] [PubMed]
- Beard, V.K.; Bedard, A.C.; Nuk, J.; Lee, P.W.; Hong, Q.; Bedard, J.E.; Sun, S.; Schrader, K.A. Genetic testing in families with hereditary colorectal cancer in British Columbia and Yukon: A retrospective cross-sectional analysis. CMAJ Open 2020, 8, E637–E642. [Google Scholar] [CrossRef]
- Suttman, A.; Pilarski, R.; Agnese, D.M.; Senter, L. “Second-class status?” Insight into communication patterns and common concerns among men with hereditary breast and ovarian cancer syndrome. J. Genet. Couns. 2018, 27, 885–893. [Google Scholar]
- Dean, M.; Tezak, A.L.; Johnson, S.; Pierce, J.K.; Weidner, A.; Clouse, K.; Pal, T.; Cragun, D. Sharing genetic test results with family members of BRCA, PALB2, CHEK2, and ATM carriers. Patient Educ. Couns. 2021, 104, 720–725. [Google Scholar] [CrossRef]
- Gill, G.; Beard, C.; Storey, K.; Taylor, S.; Sexton, A. “It wasn’t just for me”: Motivations and implications of genetic testing for women at a low risk of hereditary breast and ovarian cancer syndrome. Psycho-Oncology 2020, 29, 1303–1311. [Google Scholar] [CrossRef]
- Unger, S.; Simond, E.; Davoine, E.; Katapodi, M.C. Dissemination of Genetic Information in Swiss Families with Lynch Syndrome: A Qualitative Exploratory Study. Clin. Oncol. Res. 2020, 2020, 1–5. [Google Scholar] [CrossRef] [Green Version]
- Caswell-Jin, J.; Zimmer, A.D.; Stedden, W.; Kingham, K.E.; Zhou, A.Y.; Kurian, A.W. Cascade Genetic Testing of Relatives for Hereditary Cancer Risk: Results of an Online Initiative. J. Natl. Cancer Inst. 2019, 111, 95–98. [Google Scholar] [CrossRef]
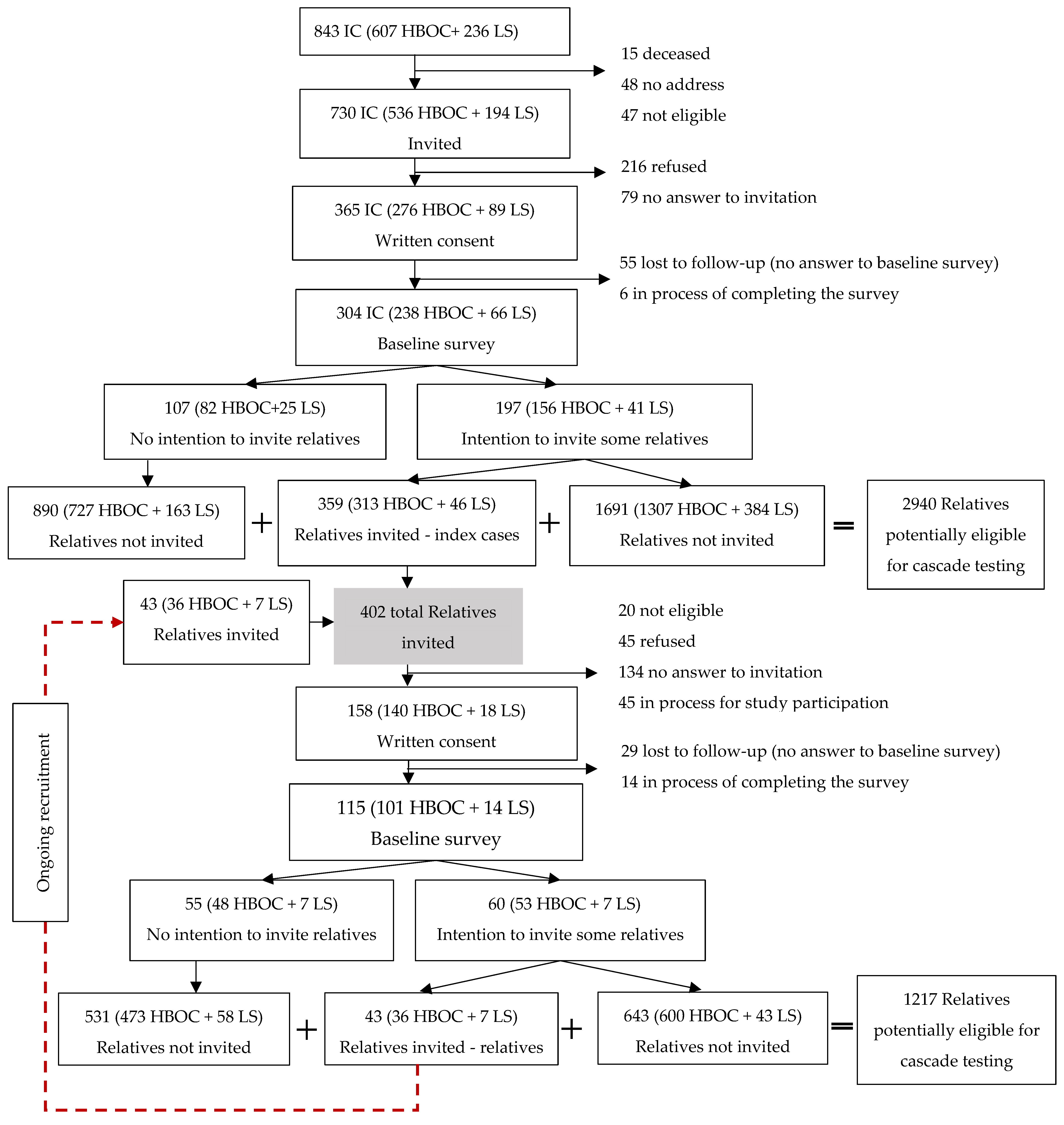
| Index Cases | Total n = 304 (% or ± SD) | HBOC n = 238 (% or ± SD) | LS n = 66 (% or ± SD) | HBOC vs. LS p-Values a |
|---|---|---|---|---|
| Gender | F = 255 (83.9) | F = 214 (89.9) | F = 41 (62.1) | <0.01 |
| Caucasian origin | 254 (83.6) | 199 (83.6) | 55 (83.3) | 1 |
| Age | 52.3 (±12.6) | 52.1 (±12.2) | 52.9 (±14.0) | 0.67 |
| Education level (12th years of education or higher) | 258 (84.9) | 206 (86.6) | 52 (78.8) | 0.17 |
| Married or living as married | 224 (73.7) | 183 (76.9) | 41 (62.1) | 0.02 |
| Cancer affected c | 195 (64.1) | 145 (60.9) | 50 (75.8) | 0.04 |
| Breast cancer (invasive) | 95 (39.9) | 3 (4.5) | - | |
| Ovarian cancer | 29 (12.2) | 4 (6.1) | - | |
| Prostate cancer | 1 (0.4) | 2 (3.0) | - | |
| Pancreatic cancer | 0 | 0 | - | |
| Colon or rectal cancer | 2 (0.9) | 30 (45.5) | - | |
| Endometrial cancer | 5 (2.1) | 8 (12.1) | - | |
| Other d | 49 (20.6) | 13 (19.7) | - | |
| Age at 1st cancer diagnosis | 47.7 (±11.7) | 47.4 (±11.7) | 48.3 (±11.7) | 0.80 |
| Genetic testing ≤5 years ago | 137 (45.1) | 108 (45.4) | 29 (43.9) | 0.95 |
| Has a routine source of care (ref: >2 healthcare professionals) | 288 (94.7) | 223 (93.7) | 65 (95.5) | 0.22 |
| Provider seen most often is specialist (ref: generalist) | 175 (57.6) | 150 (63.0) | 25 (37.9) | <0.01 |
| Out of pocket cost is a barrier to accessing care | 18 (5.9) | 17 (7.1) | 1 (1.5) | 0.14 b |
| Relatives | Total n = 115 (% or ± SD) | HBOC n = 101 (% or ± SD) | LS n = 14 (% or ± SD) | HBOC vs. LS p-values a |
| Gender | F = 78 (67.8) | F = 69 (68.3) | F = 9 (64.3) | 1 |
| Caucasian origin | 108 (93.9) | 94 (93.1) | 14 (100) | 0.67 |
| Age | 49.7 (±16.9) | 50.4 (±17.2) | 44.6 (±14.3) | 0.19 |
| Education level (12th years of education or higher) | 104 (90.4) | 91 (90.1) | 13 (92.9) | 1 |
| Married or living as married | 84 (73.0) | 78 (77.2) | 6 (42.9) | 0.34 b |
| Cancer affected | 23 (20.0) | 19 (18.8) | 4 (28.6) | 0.50 b |
| Breast cancer (invasive) | 13 (12.9) | 0 | - | |
| Ovarian cancer | 3 (3.0) | 2 (14.3) | - | |
| Prostate cancer | 1 (1.0) | 0 | - | |
| Pancreatic cancer | 0 | 0 | - | |
| Colon or rectal cancer | 0 | 1 (7.1) | - | |
| Endometrial cancer | 0 | 0 | - | |
| Other d | 7 (6.9) | 2 (14.3) | - | |
| Age at 1st cancer diagnosis | 48.4 (±11.1) | 52.7 (±12.8) | 46.4 (±8.8) | 0.47 |
| Had genetic testing | 71 (61.7) | 61 (60.4) | 10 (71.4) | 0.82 b |
| Familial pathogenic variant identified | 54 (47.0) | 47 (46.5) | 7 (50.0) | 1 b |
| Familial pathogenic variant excluded | 17 (14.8) | 14 (13.9) | 3 (21.4) | 0.46 b |
| Genetic testing ≤5 years ago | 32 (27.8) | 28 (27.7) | 4 (28.6) | 1 b |
| Has a routine source of care (ref: >2 healthcare professionals) | 104 (90.4) | 93 (92.1) | 11 (78.6) | 0.26 |
| Provider seen most often is specialist (ref: generalist) | 45 (39.1) | 43 (42.6) | 2 (14.3) | 0.24 b |
| Out of pocket cost is a barrier to access care | 5 (4.3) | 3 (3.0) | 2 (14.3) | 0.13 b |
| Degree of Relationship | HBOC | LS | HBOC vs. LS a | |||
|---|---|---|---|---|---|---|
| Eligible (n) | Intend to Invite (n, %) | Eligible (n) | Intend to Invite (n, %) | p (Intend to Invite) | ||
| First-degree | Daughters | 173 | 76 (43.9%) | 42 | 18 (42.9%) | 1 |
| Sons | 175 | 86 (49.1%) | 38 | 15 (39.5%) | 0.37 | |
| Sisters | 235 | 78 (33.2%) | 40 | 14 (35.0%) | 0.97 | |
| Brothers | 215 | 84 (39.1%) | 49 | 18 (36.7%) | 0.89 | |
| Parents | 306 | 85 (27.8%) | 71 | 20 (28.2%) | 1 | |
| Sum | 1104 | 409 (37.0%) | 240 | 85 (35.4%) | 0.69 | |
| Second-degree | Granddaughters | 39 | 13 (33.3%) | 5 | 0 | 0.07 c |
| Grandsons | 33 | 8 (24.2%) | 10 | 2 (20.0%) | 1 b | |
| Nieces | 174 | 43 (24.7%) | 39 | 2 (5.1%) | 0.02 b | |
| Nephews | 214 | 47 (22.0%) | 39 | 7 (17.9%) | 0.83 b | |
| Half-sisters | 23 | 3 (13.0) | 7 | 2 (28.6%) | 0.59 b | |
| Half-brothers | 16 | 3 (18.8%) | 10 | 2 (20.0%) | 1 b | |
| Aunts | 322 | 47 (14.6%) | 60 | 6 (10.0%) | 0.54 b | |
| Uncles | 283 | 41 (14.5%) | 61 | 10 (16.4%) | 0.70 b | |
| Sum | 1104 | 205 (18.6%) | 231 | 31 (13.4%) | 0.08 | |
| Third-degree | Female cousins | 607 | 98 (16.1%) | 101 | 13 (12.9%) | 0.49 |
| Male cousins | 641 | 80 (12.5) | 129 | 18 (14.0%) | 0.75 | |
| Sum | 1248 | 178 (14.3%) | 230 | 31 (13.4%) | 0.83 | |
| Total | 3456 | 792 (22.9%) | 701 | 147 (21%) | 0.88 | |
| Between Degree of Relationship P (Sum) d | <0.01 | <0.01 | ||||
| Between Gender P (Sum) d | 0.36 | 0.90 | ||||
| Predictors | HBOC | LS | |||
|---|---|---|---|---|---|
| OR | 95% CI | OR | 95% CI | ||
| Demographic Characteristics | Age | 1.01 | 1.00–1.03 | - | - |
| <12 years of education (reference group) | - | - | |||
| High school graduate | 0.84 | 0.35–1.98 | - | - | |
| University degree or higher | 0.61 | 0.25–1.48 | - | - | |
| Clinical Characteristics | Carrying a pathogenic variant (ref: no variant or untested) | 3.03 | 1.68–5.46 | 4.53 | 1.20–17.10 |
| No cancer | - | - | |||
| Cancer diagnosis <5 years | 1.50 | 0.70–3.23 | - | - | |
| Cancer diagnosis >5 years | 0.81 | 0.45–1.44 | - | - | |
| Knowledge and Attitudes | Genetic affinity | 1.14 | 0.93–1.39 | - | - |
| Family environment | Married or living as married (ref: single or living alone) | - | - | 2.03 | 0.81–5.09 |
| Family Support in Illness | 1.32 | 1.01–1.73 | - | - | |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Sarki, M.; Ming, C.; Aissaoui, S.; Bürki, N.; Caiata-Zufferey, M.; Erlanger, T.E.; Graffeo-Galbiati, R.; Heinimann, K.; Heinzelmann-Schwarz, V.; Monnerat, C.; et al. Intention to Inform Relatives, Rates of Cascade Testing, and Preference for Patient-Mediated Communication in Families Concerned with Hereditary Breast and Ovarian Cancer and Lynch Syndrome: The Swiss CASCADE Cohort. Cancers 2022, 14, 1636. https://doi.org/10.3390/cancers14071636
Sarki M, Ming C, Aissaoui S, Bürki N, Caiata-Zufferey M, Erlanger TE, Graffeo-Galbiati R, Heinimann K, Heinzelmann-Schwarz V, Monnerat C, et al. Intention to Inform Relatives, Rates of Cascade Testing, and Preference for Patient-Mediated Communication in Families Concerned with Hereditary Breast and Ovarian Cancer and Lynch Syndrome: The Swiss CASCADE Cohort. Cancers. 2022; 14(7):1636. https://doi.org/10.3390/cancers14071636
Chicago/Turabian StyleSarki, Mahesh, Chang Ming, Souria Aissaoui, Nicole Bürki, Maria Caiata-Zufferey, Tobias Ephraim Erlanger, Rossella Graffeo-Galbiati, Karl Heinimann, Viola Heinzelmann-Schwarz, Christian Monnerat, and et al. 2022. "Intention to Inform Relatives, Rates of Cascade Testing, and Preference for Patient-Mediated Communication in Families Concerned with Hereditary Breast and Ovarian Cancer and Lynch Syndrome: The Swiss CASCADE Cohort" Cancers 14, no. 7: 1636. https://doi.org/10.3390/cancers14071636
APA StyleSarki, M., Ming, C., Aissaoui, S., Bürki, N., Caiata-Zufferey, M., Erlanger, T. E., Graffeo-Galbiati, R., Heinimann, K., Heinzelmann-Schwarz, V., Monnerat, C., Probst-Hensch, N., Rabaglio, M., Zürrer-Härdi, U., Chappuis, P. O., Katapodi, M. C., & on behalf of the CASCADE Consortium. (2022). Intention to Inform Relatives, Rates of Cascade Testing, and Preference for Patient-Mediated Communication in Families Concerned with Hereditary Breast and Ovarian Cancer and Lynch Syndrome: The Swiss CASCADE Cohort. Cancers, 14(7), 1636. https://doi.org/10.3390/cancers14071636









