MiR-101: An Important Regulator of Gene Expression and Tumor Ecosystem
Abstract
Simple Summary
Abstract
1. Introduction
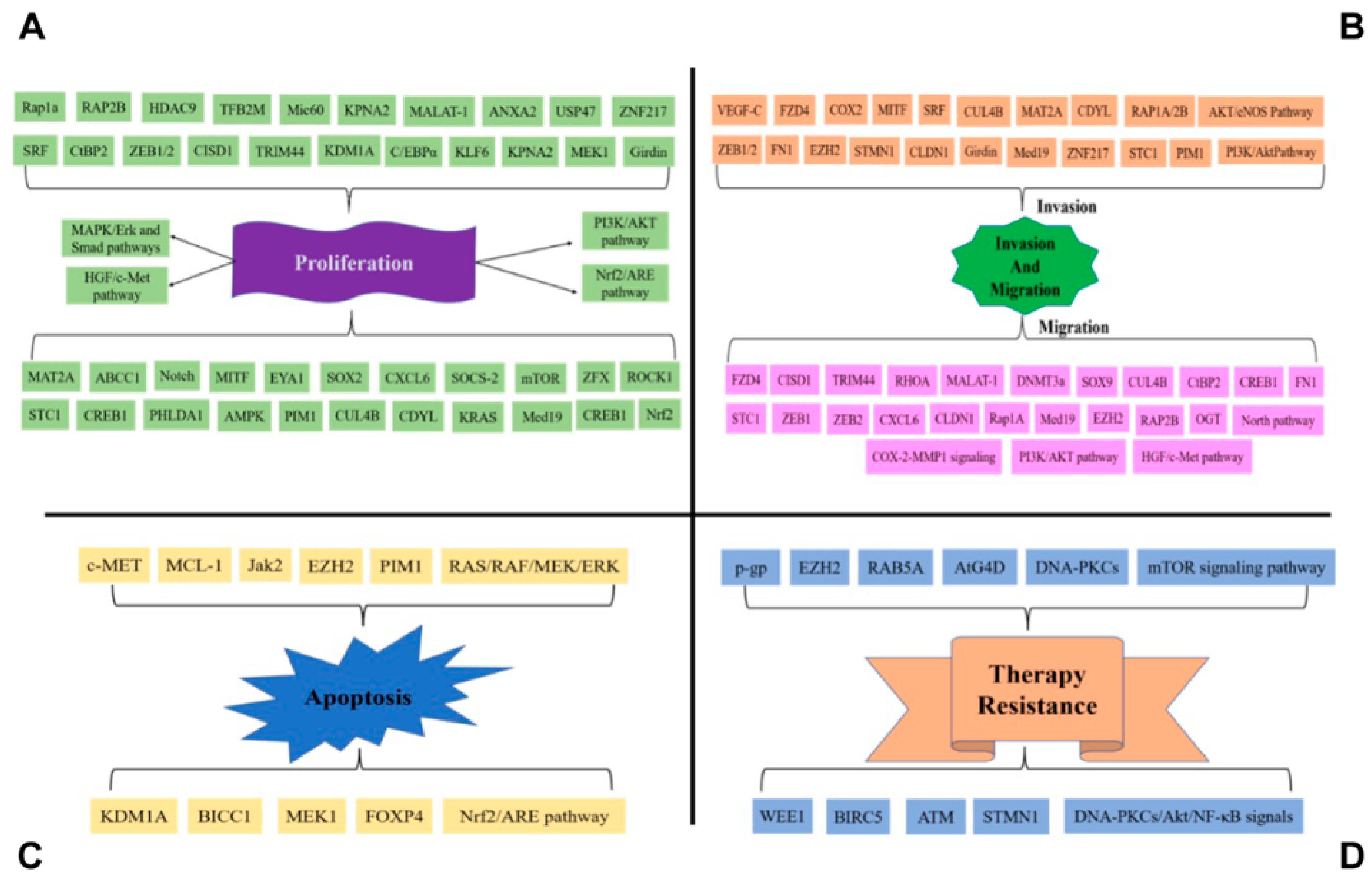
2. MiR-101 Regulates Cancer Growth, Metastasis, and Therapeutic Resistance via Several Essential Oncogenic Processes
2.1. The Role of miR-101 in Cell Proliferation
2.2. The Role of miR-101 in Migration
2.3. MiR-101 and Invasion
2.4. MiR-101 in Apoptosis
2.5. miR-101 and Tumor Chemoresistance
2.6. miR-101 and Radiosensitivity
3. MiR-101 Inhibits Cancer by Remodeling the Tumor Ecosystem
3.1. Crosstalk between MiR-101 and Microenvironment
3.2. MiR-101 and Tumor Angiogenesis
3.3. miR-101 and Tumor Immunology
4. Conclusions
Author Contributions
Funding
Conflicts of Interest
References
- Lee, R.C.; Feinbaum, R.L.; Ambros, V. The C. elegans heterochronic gene lin-4 encodes small RNAs with antisense complementarity to lin-14. Cell 1993, 75, 843–854. [Google Scholar] [CrossRef] [PubMed]
- Kozomara, A.; Birgaoanu, M.; Griffiths-Jones, S. miRBase: From microRNA sequences to function. Nucleic Acids Res. 2019, 47, D155–D162. [Google Scholar] [CrossRef] [PubMed]
- Lin, S.; Gregory, R.I. MicroRNA biogenesis pathways in cancer. Nat. Rev. Cancer 2015, 15, 321–333. [Google Scholar] [CrossRef] [PubMed]
- Lorenzi, L.; Chiu, H.S.; Avila Cobos, F.; Gross, S.; Volders, P.J.; Cannoodt, R.; Nuytens, J.; Vanderheyden, K.; Anckaert, J.; Lefever, S.; et al. The RNA Atlas expands the catalog of human non-coding RNAs. Nat. Biotechnol. 2021, 39, 1453–1465. [Google Scholar] [CrossRef]
- Jens, M.; Rajewsky, N. Competition between target sites of regulators shapes post-transcriptional gene regulation. Nat. Rev. Genet. 2015, 16, 113–126. [Google Scholar] [CrossRef]
- Gu, J.; Wang, Y.; Wu, X. MicroRNA in the pathogenesis and prognosis of esophageal cancer. Curr. Pharm. Des. 2013, 19, 1292–1300. [Google Scholar]
- Volinia, S.; Galasso, M.; Sana, M.E.; Wise, T.F.; Palatini, J.; Huebner, K.; Croce, C.M. Breast cancer signatures for invasiveness and prognosis defined by deep sequencing of microRNA. Proc. Natl. Acad. Sci. USA 2012, 109, 3024–3029. [Google Scholar] [CrossRef]
- Boeri, M.; Verri, C.; Conte, D.; Roz, L.; Modena, P.; Facchinetti, F.; Calabrò, E.; Croce, C.M.; Pastorino, U.; Sozzi, G. MicroRNA signatures in tissues and plasma predict development and prognosis of computed tomography detected lung cancer. Proc. Natl. Acad. Sci. USA 2011, 108, 3713–3718. [Google Scholar] [CrossRef] [PubMed]
- Lee, Y.S.; Dutta, A. MicroRNAs in cancer. Annu Rev. Pathol. 2009, 4, 199–227. [Google Scholar] [CrossRef]
- Zhao, X.; Wang, K.; Hu, F.; Qian, C.; Guan, H.; Feng, K.; Zhou, Y.; Chen, Z. MicroRNA-101 protects cardiac fibroblasts from hypoxia-induced apoptosis via inhibition of the TGF-beta signaling pathway. Int. J. Biochem. Cell Biol. 2015, 65, 155–164. [Google Scholar] [CrossRef] [PubMed]
- Wang, L.; Li, L.; Guo, R.; Li, X.; Lu, Y.; Guan, X.; Gitau, S.C.; Xu, C.; Yang, B.; Shan, H. miR-101 promotes breast cancer cell apoptosis by targeting Janus kinase 2. Cell. Physiol. Biochem. 2014, 34, 413–422. [Google Scholar] [CrossRef]
- Zhu, Q.Y.; Liu, Q.; Chen, J.X.; Lan, K.; Ge, B.X. MicroRNA-101 targets MAPK phosphatase-1 to regulate the activation of MAPKs in macrophages. J. Immunol. 2010, 185, 7435–7442. [Google Scholar] [CrossRef]
- Wang, J.; Zeng, H.; Li, H.; Chen, T.; Wang, L.; Zhang, K.; Chen, J.; Wang, R.; Li, Q.; Wang, S. MicroRNA-101 Inhibits Growth, Proliferation and Migration and Induces Apoptosis of Breast Cancer Cells by Targeting Sex-Determining Region Y-Box 2. Cell. Physiol. Biochem. 2017, 43, 717–732. [Google Scholar] [CrossRef] [PubMed]
- Guan, H.; Dai, Z.; Ma, Y.; Wang, Z.; Liu, X.; Wang, X. MicroRNA-101 inhibits cell proliferation and induces apoptosis by targeting EYA1 in breast cancer. Int. J. Mol. Med. 2016, 37, 1643–1651. [Google Scholar] [CrossRef] [PubMed]
- Wang, C.Z.; Deng, F.; Li, H.; Wang, D.D.; Zhang, W.; Ding, L.; Tang, J.H. MiR-101: A potential therapeutic target of cancers. Am. J. Transl. Res. 2018, 10, 3310–3321. [Google Scholar]
- Varambally, S.; Cao, Q.; Mani, R.S.; Shankar, S.; Wang, X.; Ateeq, B.; Laxman, B.; Cao, X.; Jing, X.; Ramnarayanan, K.; et al. Genomic loss of microRNA-101 leads to overexpression of histone methyltransferase EZH2 in cancer. Science 2008, 322, 1695–1699. [Google Scholar] [CrossRef] [PubMed]
- Iorio, M.V.; Ferracin, M.; Liu, C.G.; Veronese, A.; Spizzo, R.; Sabbioni, S.; Magri, E.; Pedriali, M.; Fabbri, M.; Campiglio, M.; et al. MicroRNA gene expression deregulation in human breast cancer. Cancer Res. 2005, 65, 7065–7070. [Google Scholar] [CrossRef]
- Yanaihara, N.; Caplen, N.; Bowman, E.; Seike, M.; Kumamoto, K.; Yi, M.; Stephens, R.M.; Okamoto, A.; Yokota, J.; Tanaka, T.; et al. Unique microRNA molecular profiles in lung cancer diagnosis and prognosis. Cancer Cell 2006, 9, 189–198. [Google Scholar] [CrossRef]
- Cui, T.X.; Kryczek, I.; Zhao, L.; Zhao, E.; Kuick, R.; Roh, M.H.; Vatan, L.; Szeliga, W.; Mao, Y.; Thomas, D.G.; et al. Myeloid-derived suppressor cells enhance stemness of cancer cells by inducing microRNA101 and suppressing the corepressor CtBP2. Immunity 2013, 39, 611–621. [Google Scholar] [CrossRef]
- Calastri, M.C.J.; Ferreira, R.F.; Tenani, G.D.; Spinola, L.P.; Vieira, G.F.; Rabaca Roque Botelho, M.F.; Abrantes, A.M.C.; Tralhao, J.; De Brito, A.F.M.; Da Silva, R.F.; et al. Investigating VEGF. miR-145-3p, and miR-101-3p Expression in Patients with Cholangiocarcinoma. Asian Pac. J. Cancer Prev. 2022, 23, 2233–2241. [Google Scholar] [CrossRef]
- Hu, Q.; Li, Y.; Chen, H.; Liao, H.; He, Y.; Zheng, Q. CCDC88A Post-Transcriptionally Regulates VEGF via miR-101 and Subsequently Regulates Hepatocellular Carcinoma. Front. Immunol. 2022, 13, 859331. [Google Scholar] [CrossRef]
- Meng, X.; Shi, Y.; Xiang, X.; Li, C.; Ge, X.; Pan, K.; Liang, Y. Influence of miR-101 on proliferation of liver cancer cells through the MAPK/ERK signaling pathway. Oncol. Lett. 2020, 19, 1310–1316. [Google Scholar] [CrossRef] [PubMed]
- Liu, Y.; Tan, J.; Ou, S.; Chen, J.; Chen, L. MicroRNA-101-3p suppresses proliferation and migration in hepatocellular carcinoma by targeting the HGF/c-Met pathway. Invest. N. Drugs 2020, 38, 60–69. [Google Scholar] [CrossRef]
- Si, W.; Zhao, Y.; Zhou, J.; Zhang, Q.; Zhang, Y. The coordination between ZNF217 and LSD1 contributes to hepatocellular carcinoma progress and is negatively regulated by miR-101. Exp. Cell Res. 2019, 379, 1–10. [Google Scholar] [CrossRef] [PubMed]
- Wu, F.; Huang, W.; Yang, L.; Xu, F. MicroRNA-101-3p regulates gastric cancer cell proliferation, invasion and apoptosis by targeting PIM 1 expression. Cell Mol. Biol. 2019, 65, 118–122. [Google Scholar] [CrossRef] [PubMed]
- Cao, S.; Lin, L.; Xia, X.; Wu, H. lncRNA SPRY4-IT1 Regulates Cell Proliferation and Migration by Sponging miR-101-3p and Regulating AMPK Expression in Gastric Cancer. Mol. Ther. Nucleic Acids 2019, 17, 455–464. [Google Scholar] [CrossRef]
- Zhou, H.; Li, L.; Wang, Y.; Wang, D. Long non-coding RNA SNHG6 promotes tumorigenesis in melanoma cells via the microRNA-101-3p/RAP2B axis. Oncol. Lett. 2020, 20, 323. [Google Scholar] [CrossRef]
- Shao, N.; Song, L.; Sun, X. Exosomal circ_PIP5K1A regulates the progression of non-small cell lung cancer and cisplatin sensitivity by miR-101/ABCC1 axis. Mol. Cell. Biochem. 2021, 476, 2253–2267. [Google Scholar] [CrossRef]
- Han, L.; Chen, W.; Xia, Y.; Song, Y.; Zhao, Z.; Cheng, H.; Jiang, T. MiR-101 inhibits the proliferation and metastasis of lung cancer by targeting zinc finger E-box binding homeobox 1. Am. J. Transl. Res. 2018, 10, 1172–1183. [Google Scholar]
- Li, K.; Jiang, Y.; Xiang, X.; Gong, Q.; Zhou, C.; Zhang, L.; Ma, Q.; Zhuang, L. Long non-coding RNA SNHG6 promotes the growth and invasion of non-small cell lung cancer by downregulating miR-101-3p. Thorac. Cancer 2020, 11, 1180–1190. [Google Scholar] [CrossRef]
- Shahverdi, M.; Amri, J.; Karami, H.; Baazm, M. Knockdown of Myeloid Cell Leukemia-1 by MicroRNA-101 Increases Sensitivity of A549 Lung Cancer Cells to Etoposide. Iran. J. Med. Sci. 2021, 46, 298–307. [Google Scholar] [PubMed]
- Zhang, X.; He, X.; Liu, Y.; Zhang, H.; Chen, H.; Guo, S.; Liang, Y. MiR-101-3p inhibits the growth and metastasis of non-small cell lung cancer through blocking PI3K/AKT signal pathway by targeting MALAT-1. Biomed. Pharm. 2017, 93, 1065–1073. [Google Scholar] [CrossRef] [PubMed]
- Chen, H.; Gu, B.; Zhao, X.; Zhao, Y.; Huo, S.; Liu, X.; Lu, H. Circular RNA hsa_circ_0007364 increases cervical cancer progression through activating methionine adenosyltransferase II alpha (MAT2A) expression by restraining microRNA-101-5p. Bioengineered 2020, 11, 1269–1279. [Google Scholar] [CrossRef] [PubMed]
- Zhang, X.; Gao, D.; Fang, K.; Guo, Z.; Li, L. Med19 is targeted by miR-101-3p/miR-422a and promotes breast cancer progression by regulating the EGFR/MEK/ERK signaling pathway. Cancer Lett. 2019, 444, 105–115. [Google Scholar] [CrossRef]
- Yi, J.; Huang, W.Z.; Wen, Y.Q.; Yi, Y.C. Effect of miR-101 on proliferation and oxidative stress-induced apoptosis of breast cancer cells via Nrf2 signaling pathway. Eur. Rev. Med. Pharmacol. Sci. 2019, 23, 8931–8939. [Google Scholar]
- Luan, C.; Li, Y.; Liu, Z.; Zhao, C. Long Noncoding RNA MALAT1 Promotes the Development of Colon Cancer by Regulating miR-101-3p/STC1 Axis. OncoTargets Ther. 2020, 13, 3653–3665. [Google Scholar] [CrossRef]
- Yang, Q.; Yu, W.; Han, X. Overexpression of microRNA101 causes antitumor effects by targeting CREB1 in colon cancer. Mol. Med. Rep. 2019, 19, 3159–3167. [Google Scholar]
- Wu, H.B.; Huang, S.S.; Lu, C.G.; Tian, S.D.; Chen, M. CircAPLP2 regulates the proliferation and metastasis of colorectal cancer by targeting miR-101-3p to activate the Notch signalling pathway. Am. J. Transl. Res. 2020, 12, 2554–2569. [Google Scholar]
- Zhu, L.; Chen, Y.; Nie, K.; Xiao, Y.; Yu, H. MiR-101 inhibits cell proliferation and invasion of pancreatic cancer through targeting STMN1. Cancer Biomark 2018, 23, 301–309. [Google Scholar] [CrossRef]
- Chen, J.H.; Tong, W.; Pu, X.F.; Wang, J.Z. Long noncoding RNA CRNDE promotes proliferation, migration and invasion in prostate cancer through miR-101/Rap1A. Neoplasma 2020, 67, 584–594. [Google Scholar] [CrossRef]
- Jin, Q.; He, W.; Chen, L.; Yang, Y.; Shi, K.; You, Z. MicroRNA-101-3p inhibits proliferation in retinoblastoma cells by targeting EZH2 and HDAC9. Exp. Ther. Med. 2018, 16, 1663–1670. [Google Scholar] [CrossRef] [PubMed]
- Jiang, X.; Yuan, Y.; Tang, L.; Wang, J.; Zhang, D.; Duan, L. Systematic Analysis and Validation of the Prognosis, Immunological Role and Biology Function of the Ferroptosis-Related lncRNA GSEC/miRNA-101-3p/CISD1 Axis in Lung Adenocarcinoma. Front. Mol. Biosci. 2021, 8, 793732. [Google Scholar] [CrossRef] [PubMed]
- Ziemann, M.; Lim, S.C.; Kang, Y.; Samuel, S.; Sanchez, I.L.; Gantier, M.; Stojanovski, D.; McKenzie, M. MicroRNA-101-3p Modulates Mitochondrial Metabolism via the Regulation of Complex II Assembly. J. Mol. Biol. 2022, 434, 167361. [Google Scholar] [CrossRef]
- Ding, C.; Xi, G.; Wang, G.; Cui, D.; Zhang, B.; Wang, H.; Jiang, G.; Song, J.; Xu, G.; Wang, J. Exosomal Circ-MEMO1 Promotes the Progression and Aerobic Glycolysis of Non-small Cell Lung Cancer Through Targeting MiR-101-3p/KRAS Axis. Front. Genet. 2020, 11, 962. [Google Scholar] [CrossRef] [PubMed]
- Ma, S.; Cheng, J.; Wang, H.; Ding, N.; Zhou, F.; Ji, R.; Zhu, L.; Zhu, C.; Pan, Y. A novel regulatory loop miR-101/ANXA2/EGR1 mediates malignant characteristics of liver cancer stem cells. Carcinogenesis 2021, 42, 93–104. [Google Scholar] [CrossRef] [PubMed]
- Park, J.; Cho, M.; Cho, J.; Kim, E.E.; Song, E.J. MicroRNA-101-3p Suppresses Cancer Cell Growth by Inhibiting the USP47-Induced Deubiquitination of RPL11. Cancers 2022, 14, 964. [Google Scholar] [CrossRef]
- Xie, F.W.; Liu, J.C. LncRNA SNHG12 regulates the miR-101-3p/CUL4B axis to mediate the proliferation, migration and invasion of non-small cell lung cancer. Kaohsiung J. Med. Sci. 2021, 37, 664–674. [Google Scholar] [CrossRef]
- Gu, Z.; You, Z.; Yang, Y.; Ding, R.; Wang, M.; Pu, J.; Chen, J. Inhibition of MicroRNA miR-101-3p on prostate cancer progression by regulating Cullin 4B (CUL4B) and PI3K/AKT/mTOR signaling pathways. Bioengineered 2021, 12, 4719–4735. [Google Scholar] [CrossRef]
- Wang, H.; Xiao, R.; Yang, B. MiR-101-3p Suppresses Progression of Cervical Squamous Cell Carcinoma by Targeting and Down-Regulating KPNA2. Technol. Cancer Res. Treat. 2021, 20, 15330338211055948. [Google Scholar] [CrossRef]
- Tesi, R.J. MDSC; The Most Important Cell You Have Never Heard Of. Trends Pharmacol. Sci. 2019, 40, 4–7. [Google Scholar] [CrossRef]
- Chase, A.; Cross, N.C. Aberrations of EZH2 in cancer. Clin. Cancer Res. 2011, 17, 2613–2618. [Google Scholar] [CrossRef] [PubMed]
- Smits, M.; Nilsson, J.; Mir, S.E.; van der Stoop, P.M.; Hulleman, E.; Niers, J.M.; de Witt Hamer, P.C.; Marquez, V.E.; Cloos, J.; Krichevsky, A.M.; et al. miR-101 is down-regulated in glioblastoma resulting in EZH2-induced proliferation, migration, and angiogenesis. Oncotarget 2010, 1, 710–720. [Google Scholar] [CrossRef] [PubMed]
- Qian, K.; Liu, G.; Tang, Z.; Hu, Y.; Fang, Y.; Chen, Z.; Xu, X. The long non-coding RNA NEAT1 interacted with miR-101 modulates breast cancer growth by targeting EZH2. Arch. Biochem. Biophys. 2017, 615, 1–9. [Google Scholar] [CrossRef] [PubMed]
- Chakravarthi, B.V.; Goswami, M.T.; Pathi, S.S.; Robinson, A.D.; Cieslik, M.; Chandrashekar, D.S.; Agarwal, S.; Siddiqui, J.; Daignault, S.; Carskadon, S.L.; et al. MicroRNA-101 regulated transcriptional modulator SUB1 plays a role in prostate cancer. Oncogene 2016, 35, 6330–6340. [Google Scholar] [CrossRef]
- Huang, D.; Wang, X.; Zhuang, C.; Shi, W.; Liu, M.; Tu, Q.; Zhang, D.; Hu, L. Reciprocal negative feedback loop between EZH2 and miR-101-1 contributes to miR-101 deregulation in hepatocellular carcinoma. Oncol. Rep. 2016, 35, 1083–1090. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Liu, D.; Li, Y.; Luo, G.; Xiao, X.; Tao, D.; Wu, X.; Wang, M.; Huang, C.; Wang, L.; Zeng, F.; et al. LncRNA SPRY4-IT1 sponges miR-101-3p to promote proliferation and metastasis of bladder cancer cells through up-regulating EZH2. Cancer Lett. 2017, 388, 281–291. [Google Scholar] [CrossRef] [PubMed]
- Chen, T.; Li, E. Structure and function of eukaryotic DNA methyltransferases. Curr. Top. Dev. Biol. 2004, 60, 55–89. [Google Scholar] [PubMed]
- Wei, X.; Xiang, T.; Ren, G.; Tan, C.; Liu, R.; Xu, X.; Wu, Z. miR-101 is down-regulated by the hepatitis B virus x protein and induces aberrant DNA methylation by targeting DNA methyltransferase 3A. Cell Signal. 2013, 25, 439–446. [Google Scholar] [CrossRef] [PubMed]
- Liu, J.; Pang, Y.; Wang, H.; Li, Y.; Sun, X.; Xu, F.; Ren, H.; Liu, D. miR-101 inhibits the proliferation and migration of breast cancer cells via downregulating the expression of DNA methyltransferase 3a. Xi Bao Yu Fen Zi Mian Yi Xue Za Zhi 2016, 32, 299–303. [Google Scholar] [PubMed]
- Liu, X.; Lei, Q.; Yu, Z.; Xu, G.; Tang, H.; Wang, W.; Wang, Z.; Li, G.; Wu, M. MiR-101 reverses the hypomethylation of the LMO3 promoter in glioma cells. Oncotarget 2015, 6, 7930–7943. [Google Scholar] [CrossRef] [PubMed]
- Guo, X.; Chen, M.; Cao, L.; Hu, Y.; Li, X.; Zhang, Q.; Ren, Y.; Wu, X.; Meng, Z.; Xu, K. Cancer-Associated Fibroblasts Promote Migration and Invasion of Non-Small Cell Lung Cancer Cells via miR-101-3p Mediated VEGFA Secretion and AKT/eNOS Pathway. Front. Cell Dev. Biol. 2021, 9, 764151. [Google Scholar] [CrossRef]
- Suzuki, M.; Cao, K.; Kato, S.; Mizutani, N.; Tanaka, K.; Arima, C.; Tai, M.C.; Nakatani, N.; Yanagisawa, K.; Takeuchi, T.; et al. CERS6 required for cell migration and metastasis in lung cancer. J. Cell. Mol. Med. 2020, 24, 11949–11959. [Google Scholar] [CrossRef] [PubMed]
- Shen, W.; Xie, X.Y.; Liu, M.R.; Wang, L.L. MicroRNA-101-5p inhibits the growth and metastasis of cervical cancer cell by inhibiting CXCL6. Eur. Rev. Med. Pharmacol. Sci. 2019, 23, 1957–1968. [Google Scholar] [PubMed]
- Chen, Q.; Liu, D.; Hu, Z.; Luo, C.; Zheng, S.L. miRNA-101-5p inhibits the growth and aggressiveness of NSCLC cells through targeting CXCL6. OncoTargets Ther. 2019, 12, 835–848. [Google Scholar] [CrossRef] [PubMed]
- Yan, F.; Shen, N.; Pang, J.; Xie, D.; Deng, B.; Molina, J.R.; Yang, P.; Liu, S. Restoration of miR-101 suppresses lung tumorigenesis through inhibition of DNMT3a-dependent DNA methylation. Cell Death Dis. 2014, 5, e1413. [Google Scholar] [CrossRef] [PubMed]
- Du, Y.L.; Liang, Y.; Cao, Y.; Liu, L.; Li, J.; Shi, G.Q. LncRNA XIST Promotes Migration and Invasion of Papillary Thyroid Cancer Cell by Modulating MiR-101-3p/CLDN1 Axis. Biochem. Genet. 2021, 59, 437–452. [Google Scholar] [CrossRef]
- Zhou, Z.; Xu, H.; Duan, Y.; Liu, B. MicroRNA-101 suppresses colorectal cancer progression by negative regulation of Rap1b. Oncol. Lett. 2020, 20, 2225–2231. [Google Scholar] [CrossRef] [PubMed]
- Xiong, W.C.; Han, N.; Wu, N.; Zhao, K.L.; Han, C.; Wang, H.X.; Ping, G.F.; Zheng, P.F.; Feng, H.; Qin, L.; et al. Interplay between long noncoding RNA ZEB1-AS1 and miR-101/ZEB1 axis regulates proliferation and migration of colorectal cancer cells. Am. J. Transl. Res. 2018, 10, 605–617. [Google Scholar] [PubMed]
- Liang, H.; Yu, M.; Yang, R.; Zhang, L.; Zhu, D.; Luo, H.; Hong, Y.; Yu, T.; Sun, J.; Shan, H.; et al. A PTAL-miR-101-FN1 Axis Promotes EMT and Invasion-Metastasis in Serous Ovarian Cancer. Mol. Ther. -Oncolytics 2020, 16, 53–62. [Google Scholar] [CrossRef] [PubMed]
- Harati, R.; Mohammad, M.G.; Tlili, A.; El-Awady, R.A.; Hamoudi, R. Loss of miR-101-3p Promotes Transmigration of Metastatic Breast Cancer Cells through the Brain Endothelium by Inducing COX-2/MMP1 Signaling. Pharmaceuticals 2020, 13, 144. [Google Scholar] [CrossRef]
- Chen, L.; Long, Y.; Han, Z.; Yuan, Z.; Liu, W.; Yang, F.; Li, T.; Shu, L.; Zhong, Y. MicroRNA-101 inhibits cell migration and invasion in bladder cancer via targeting FZD4. Exp. Ther. Med. 2019, 17, 1476–1485. [Google Scholar] [CrossRef] [PubMed]
- Li, L.; Shao, M.Y.; Zou, S.C.; Xiao, Z.F.; Chen, Z.C. MiR-101-3p inhibits EMT to attenuate proliferation and metastasis in glioblastoma by targeting TRIM44. J. Neurooncol. 2019, 141, 19–30. [Google Scholar] [CrossRef] [PubMed]
- Wang, L.; Zhang, X.; Jia, L.T.; Hu, S.J.; Zhao, J.; Yang, J.D.; Wen, W.H.; Wang, Z.; Wang, T.; Wang, R.A.; et al. c-Myc-mediated epigenetic silencing of MicroRNA-101 contributes to dysregulation of multiple pathways in hepatocellular carcinoma. Hepatology 2014, 59, 1850–1863. [Google Scholar] [CrossRef] [PubMed]
- Aigner, K.; Dampier, B.; Descovich, L.; Mikula, M.; Sultan, A.; Schreiber, M.; Mikulits, W.; Brabletz, T.; Strand, D.; Obrist, P.; et al. The transcription factor ZEB1 (deltaEF1) promotes tumour cell dedifferentiation by repressing master regulators of epithelial polarity. Oncogene 2007, 26, 6979–6988. [Google Scholar] [CrossRef] [PubMed]
- Georgakopoulos-Soares, I.; Chartoumpekis, D.V.; Kyriazopoulou, V.; Zaravinos, A. EMT Factors and Metabolic Pathways in Cancer. Front. Oncol. 2020, 10, 499. [Google Scholar] [CrossRef]
- Guo, F.; Cogdell, D.; Hu, L.; Yang, D.; Sood, A.K.; Xue, F.; Zhang, W. MiR-101 suppresses the epithelial-to-mesenchymal transition by targeting ZEB1 and ZEB2 in ovarian carcinoma. Oncol. Rep. 2014, 31, 2021–2028. [Google Scholar] [CrossRef] [PubMed]
- Chandra Mangalhara, K.; Manvati, S.; Saini, S.K.; Ponnusamy, K.; Agarwal, G.; Abraham, S.K.; Bamezai, R.N.K. ERK2-ZEB1-miR-101-1 axis contributes to epithelial-mesenchymal transition and cell migration in cancer. Cancer Lett. 2017, 391, 59–73. [Google Scholar] [CrossRef] [PubMed]
- Lin, H.; Zheng, X.; Lu, T.; Gu, Y.; Zheng, C.; Yan, H. The proliferation and invasion of osteosarcoma are inhibited by miR-101 via targetting ZEB2. Biosci. Rep. 2019, 39, 2. [Google Scholar] [CrossRef] [PubMed]
- Wu, X.; Zhou, J.; Wu, Z.; Chen, C.; Liu, J.; Wu, G.; Zhai, J.; Liu, F.; Li, G. miR-101-3p Suppresses HOX Transcript Antisense RNA (HOTAIR)-Induced Proliferation and Invasion Through Directly Targeting SRF in Gastric Carcinoma Cells. Oncol. Res. 2017, 25, 1383–1390. [Google Scholar] [CrossRef]
- Liu, Z.; Wang, J.; Mao, Y.; Zou, B.; Fan, X. MicroRNA-101 suppresses migration and invasion via targeting vascular endothelial growth factor-C in hepatocellular carcinoma cells. Oncol. Lett. 2016, 11, 433–438. [Google Scholar] [CrossRef] [PubMed]
- Cao, K.; Li, J.; Zhao, Y.; Wang, Q.; Zeng, Q.; He, S.; Yu, L.; Zhou, J.; Cao, P. miR-101 Inhibiting Cell Proliferation, Migration and Invasion in Hepatocellular Carcinoma through Downregulating Girdin. Mol. Cells 2016, 39, 96–102. [Google Scholar]
- Wang, H.; Guo, Y.; Mi, N.; Zhou, L. miR-101-3p and miR-199b-5p promote cell apoptosis in oral cancer by targeting BICC1. Mol. Cell. Probes 2020, 52, 101567. [Google Scholar] [CrossRef] [PubMed]
- Xue, P.; Huang, S.; Han, X.; Zhang, C.; Yang, L.; Xiao, W.; Fu, J.; Li, H.; Zhou, Y. Exosomal miR-101-3p and miR-423-5p inhibit medulloblastoma tumorigenesis through targeting FOXP4 and EZH2. Cell Death Differ. 2022, 29, 82–95. [Google Scholar] [CrossRef] [PubMed]
- Huang, Y.; Zou, Y.; Lin, L.; Ma, X.; Zheng, R. miR-101 regulates cell proliferation and apoptosis by targeting KDM1A in diffuse large B cell lymphoma. Cancer Manag. Res. 2019, 11, 2739–2746. [Google Scholar] [CrossRef] [PubMed]
- Huang, Y.; Zou, Y.; Lin, L.; Ma, X.; Zheng, R. miR101 regulates the cell proliferation and apoptosis in diffuse large Bcell lymphoma by targeting MEK1 via regulation of the ERK/MAPK signaling pathway. Oncol. Rep. 2019, 41, 377–386. [Google Scholar] [PubMed]
- Wu, R.S.; Qiu, E.H.; Zhu, J.J.; Wang, J.R.; Lin, H.L. MiR-101 promotes nasopharyngeal carcinoma cell apoptosis through inhibiting Ras/Raf/MEK/ERK signaling pathway. Eur. Rev. Med Pharmacol. Sci. 2020, 24, 8240. [Google Scholar]
- Zhu, J.; Li, Z. Overexpression of miR-101 promotes TRAIL-induced mitochondrial apoptosis in papillary thyroid carcinoma by targeting c-met and MCL-1. Oncotarget 2017, 8, 108665–108675. [Google Scholar] [CrossRef] [PubMed]
- Bao, J.; Xu, Y.; Wang, Q.; Zhang, J.; Li, Z.; Li, D.; Li, J. miR-101 alleviates chemoresistance of gastric cancer cells by targeting ANXA2. Biomed. Pharmacother 2017, 92, 1030–1037. [Google Scholar] [CrossRef] [PubMed]
- Chai, Z.; Yin, X.; Chen, J.; Shi, J.; Sun, J.; Liu, C.; Liu, F.; Cheng, S. MicroRNA-101 modulates cisplatin chemoresistance in liver cancer cells via the DNA-PKcs signaling pathway. Oncol. Lett. 2019, 18, 3655–3663. [Google Scholar] [CrossRef] [PubMed]
- Li, B.; Xie, D.; Zhang, H. MicroRNA-101-3p advances cisplatin sensitivity in bladder urothelial carcinoma through targeted silencing EZH2. J. Cancer 2019, 10, 2628–2634. [Google Scholar] [CrossRef] [PubMed]
- Cai, T.; Liu, Y.; Xiao, J. Long noncoding RNA MALAT1 knockdown reverses chemoresistance to temozolomide via promoting microRNA-101 in glioblastoma. Cancer Med. 2018, 7, 1404–1415. [Google Scholar] [CrossRef] [PubMed]
- Normann, L.S.; Haugen, M.H.; Aure, M.R.; Kristensen, V.N.; Maelandsmo, G.M.; Sahlberg, K.K. miR-101-5p Acts as a Tumor Suppressor in HER2-Positive Breast Cancer Cells and Improves Targeted Therapy. Breast Cancer 2022, 14, 25–39. [Google Scholar] [CrossRef] [PubMed]
- Xu, Y.; An, Y.; Wang, Y.; Zhang, C.; Zhang, H.; Huang, C.; Jiang, H.; Wang, X.; Li, X. miR-101 inhibits autophagy and enhances cisplatin-induced apoptosis in hepatocellular carcinoma cells. Oncol. Rep. 2013, 29, 2019–2024. [Google Scholar] [CrossRef]
- Zhang, X.; Zhao, P.; Wang, C.; Xin, B. SNHG14 enhances gemcitabine resistance by sponging miR-101 to stimulate cell autophagy in pancreatic cancer. Biochem. Biophys. Res. Commun. 2019, 510, 508–514. [Google Scholar] [CrossRef] [PubMed]
- Chang, Z.; Huo, L.; Li, K.; Wu, Y.; Hu, Z. Blocked autophagy by miR-101 enhances osteosarcoma cell chemosensitivity in vitro. Sci. World J. 2014, 794756, 9. [Google Scholar]
- van Gent, D.C.; Hoeijmakers, J.H.; Kanaar, R. Chromosomal stability and the DNA double-stranded break connection. Nat. Rev. Genet. 2001, 2, 196–206. [Google Scholar] [CrossRef]
- Yan, D.; Ng, W.L.; Zhang, X.; Wang, P.; Zhang, Z.; Mo, Y.Y.; Mao, H.; Hao, C.; Olson, J.J.; Curran, W.J.; et al. Targeting DNA-PKcs and ATM with miR-101 sensitizes tumors to radiation. PLoS ONE 2010, 5, 0011397. [Google Scholar] [CrossRef]
- Chen, X.; Zhang, N. Downregulation of lncRNA NEAT1_2 radiosensitizes hepatocellular carcinoma cells through regulation of miR-101-3p/WEE1 axis. Cell Biol. Int. 2019, 43, 44–55. [Google Scholar] [CrossRef]
- Sun, Q.; Liu, T.; Zhang, T.; Du, S.; Xie, G.X.; Lin, X.; Chen, L.; Yuan, Y. MiR-101 sensitizes human nasopharyngeal carcinoma cells to radiation by targeting stathmin 1. Mol. Med. Rep. 2015, 11, 3330–3336. [Google Scholar] [CrossRef][Green Version]
- Li, Z.; Qu, Z.; Wang, Y.; Qin, M.; Zhang, H. miR-101-3p sensitizes non-small cell lung cancer cells to irradiation. Open Med. 2020, 15, 413–423. [Google Scholar] [CrossRef]
- Chen, M.; Liu, P.; Chen, Y.; Chen, Z.; Shen, M.; Liu, X.; Li, X.; Li, A.; Lin, Y.; Yang, R.; et al. Long Noncoding RNA FAM201A Mediates the Radiosensitivity of Esophageal Squamous Cell Cancer by Regulating ATM and mTOR Expression via miR-101. Front. Genet. 2018, 9, 611. [Google Scholar] [CrossRef] [PubMed]
- Meng, X.; Sun, Y.; Liu, S.; Mu, Y. miR-101-3p sensitizes lung adenocarcinoma cells to irradiation via targeting BIRC5. Oncol. Lett. 2021, 21, 282. [Google Scholar] [CrossRef] [PubMed]
- Fan, M.J.; Zou, Y.H.; He, P.J.; Zhang, S.; Sun, X.M.; Li, C.Z. Long non-coding RNA SPRY4-IT1 promotes epithelial-mesenchymal transition of cervical cancer by regulating the miR-101-3p/ZEB1 axis. Biosci. Rep. 2019, 39, 6. [Google Scholar] [CrossRef] [PubMed]
- Liu, Y.; Li, H.; Zhao, C.; Jia, H. MicroRNA-101 inhibits angiogenesis via COX-2 in endometrial carcinoma. Mol. Cell. Biochem. 2018, 448, 61–69. [Google Scholar] [CrossRef] [PubMed]
- Wang, H.; Wang, L.; Zhang, G.; Lu, C.; Chu, H.; Yang, R.; Zhao, G. MALAT1/miR-101-3p/MCL1 axis mediates cisplatin resistance in lung cancer. Oncotarget 2018, 9, 7501–7512. [Google Scholar] [CrossRef] [PubMed]
- Kong, X.; Zhao, Y.; Li, X.; Tao, Z.; Hou, M.; Ma, H. Overexpression of HIF-2alpha-Dependent NEAT1 Promotes the Progression of Non-Small Cell Lung Cancer through miR-101-3p/SOX9/Wnt/beta-Catenin Signal Pathway. Cell Physiol Biochem 2019, 52, 368–381. [Google Scholar] [PubMed]
- Zhang, H.; Wang, X.; Hu, B.; Zhang, F.; Wei, H.; Li, L. Circular RNA ZFR accelerates non-small cell lung cancer progression by acting as a miR-101-3p sponge to enhance CUL4B expression. Artif. Cells Nanomed. Biotechnol. 2019, 47, 3410–3416. [Google Scholar] [CrossRef]
- Liang, H.; Yu, T.; Han, Y.; Jiang, H.; Wang, C.; You, T.; Zhao, X.; Shan, H.; Yang, R.; Yang, L.; et al. LncRNA PTAR promotes EMT and invasion-metastasis in serous ovarian cancer by competitively binding miR-101-3p to regulate ZEB1 expression. Mol. Cancer 2018, 17, 119. [Google Scholar] [CrossRef]
- Wei, M.; Jin, H.; Yang, S.; Li, Z.; Wang, X.; Li, L.; Jia, Y.; Cui, M. MicroRNA-101 inhibits growth and metastasis of human ovarian cancer cells by targeting PI3K/AKT. Arch. Med. Sci. 2021, 17, 127–134. [Google Scholar] [CrossRef] [PubMed]
- Jiang, H.; Li, L.; Zhang, J.; Wan, Z.; Wang, Y.; Hou, J.; Yu, Y. MiR-101-3p and Syn-Cal14.1a Synergy in Suppressing EZH2-Induced Progression of Breast Cancer. OncoTargets Ther. 2020, 13, 9599–9609. [Google Scholar] [CrossRef] [PubMed]
- Huang, Z.; Wu, X.; Li, J. miR-101 suppresses colon cancer cell migration through the regulation of EZH2. Rev. Esp. Enferm. Dig. 2021, 113, 255–260. [Google Scholar] [CrossRef] [PubMed]
- Wang, G.; Han, J.; Wu, X.; Huang, Y.; Wu, M.; Chen, Y. ERO1alpha mediates endoplasmic reticulum stress-induced apoptosis via microRNA-101/EZH2 axis in colon cancer RKO and HT-29 cells. Hum. Cell 2021, 34, 932–944. [Google Scholar] [CrossRef] [PubMed]
- Cai, Y.; Liu, J.; Cai, S.K.; Miao, E.Y.; Jia, C.Q.; Fan, Y.Z.; Li, Y.B. Eicosapentaenoic acid’s metabolism of 15-LOX-1 promotes the expression of miR-101 thus inhibits Cox2 pathway in colon cancer. OncoTargets Ther. 2020, 13, 5605–5616. [Google Scholar] [CrossRef]
- Jiang, M.; Xu, B.; Li, X.; Shang, Y.; Chu, Y.; Wang, W.; Chen, D.; Wu, N.; Hu, S.; Zhang, S.; et al. O-GlcNAcylation promotes colorectal cancer metastasis via the miR-101-O-GlcNAc/EZH2 regulatory feedback circuit. Oncogene 2019, 38, 301–316. [Google Scholar] [CrossRef] [PubMed]
- Tao, L.; Xu, C.; Shen, W.; Tan, J.; Li, L.; Fan, M.; Sun, D.; Lai, Y.; Cheng, H. HIPK3 Inhibition by Exosomal hsa-miR-101-3p Is Related to Metabolic Reprogramming in Colorectal Cancer. Front. Oncol. 2021, 11, 758336. [Google Scholar] [CrossRef]
- Wang, K.; Ma, L.; Tang, J.; Yu, Q.; Shen, Y.; Wei, Y.; Zhu, C.; Deng, Z.; Zhang, W. LncRNA00518 promotes cell proliferation through regulating miR-101 in bladder cancer. J. Cancer 2020, 11, 1468–1477. [Google Scholar] [CrossRef]
- Liu, P.; Li, X.; Cui, Y.; Chen, J.; Li, C.; Li, Q.; Li, H.; Zhang, X.; Zu, X. LncRNA-MALAT1 mediates cisplatin resistance via miR-101-3p/VEGF-C pathway in bladder cancer. Acta Biochim. Et Biophys. Sin. 2019, 51, 1148–1157. [Google Scholar] [CrossRef]
- Cao, C.; Xu, Y.; Du, K.; Mi, C.; Yang, C.; Xiang, L.; Xie, Y.; Liu, W. LINC01303 functions as a competing endogenous RNA to regulate EZH2 expression by sponging miR-101-3p in gastric cancer. J. Cell Mol. Med. 2019, 23, 7342–7348. [Google Scholar] [CrossRef] [PubMed]
- Ding, A.; Wang, C.; Zhang, L. Effects of miR-101, miR-345 on HBV replication regulation and on the growth of liver cancer cells. Oncol. Lett. 2019, 17, 1167–1171. [Google Scholar] [CrossRef] [PubMed]
- Qiu, B.Q.; Lin, X.H.; Ye, X.D.; Huang, W.; Pei, X.; Xiong, D.; Long, X.; Zhu, S.Q.; Lu, F.; Lin, K.; et al. Long non-coding RNA PSMA3-AS1 promotes malignant phenotypes of esophageal cancer by modulating the miR-101/EZH2 axis as a ceRNA. Aging 2020, 12, 1843–1856. [Google Scholar] [CrossRef] [PubMed]
- Sachdeva, M.; Wu, H.; Ru, P.; Hwang, L.; Trieu, V.; Mo, Y.Y. MicroRNA-101-mediated Akt activation and estrogen-independent growth. Oncogene 2011, 30, 822–831. [Google Scholar] [CrossRef]
- Kim, J.H.; Lee, K.S.; Lee, D.K.; Kim, J.; Kwak, S.N.; Ha, K.S.; Choe, J.; Won, M.H.; Cho, B.R.; Jeoung, D.; et al. Hypoxia-responsive microRNA-101 promotes angiogenesis via heme oxygenase-1/vascular endothelial growth factor axis by targeting cullin 3. Antioxid. Redox Signal. 2014, 21, 2469–2482. [Google Scholar] [CrossRef]
- Liu, N.; Xia, W.Y.; Liu, S.S.; Chen, H.Y.; Sun, L.; Liu, M.Y.; Li, L.F.; Lu, H.M.; Fu, Y.J.; Wang, P.; et al. MicroRNA-101 targets von Hippel-Lindau tumor suppressor (VHL) to induce HIF1α mediated apoptosis and cell cycle arrest in normoxia condition. Sci. Rep. 2016, 6, 20489. [Google Scholar] [CrossRef]
- Liu, H.T.; Xing, A.Y.; Chen, X.; Ma, R.R.; Wang, Y.W.; Shi, D.B.; Zhang, H.; Li, P.; Chen, H.F.; Li, Y.H.; et al. MicroRNA-27b, microRNA-101 and microRNA-128 inhibit angiogenesis by down-regulating vascular endothelial growth factor C expression in gastric cancers. Oncotarget 2015, 6, 37458–37470. [Google Scholar] [CrossRef]
- Zhang, J.; Han, C.; Zhu, H.; Song, K.; Wu, T. miR-101 inhibits cholangiocarcinoma angiogenesis through targeting vascular endothelial growth factor (VEGF). Am. J. Pathol. 2013, 182, 1629–1639. [Google Scholar] [CrossRef] [PubMed]
- Chanmee, T.; Ontong, P.; Konno, K.; Itano, N. Tumor-associated macrophages as major players in the tumor microenvironment. Cancers 2014, 6, 1670–1690. [Google Scholar] [CrossRef] [PubMed]
- Zhao, Y.; Yu, Z.; Ma, R.; Zhang, Y.; Zhao, L.; Yan, Y.; Lv, X.; Zhang, L.; Su, P.; Bi, J.; et al. lncRNA-Xist/miR-101-3p/KLF6/C/EBPalpha axis promotes TAM polarization to regulate cancer cell proliferation and migration. Mol. Ther. Nucleic Acids 2021, 23, 536–551. [Google Scholar] [CrossRef] [PubMed]
- Niespolo, C.; Johnston, J.M.; Deshmukh, S.R.; Satam, S.; Shologu, Z.; Villacanas, O.; Sudbery, I.M.; Wilson, H.L.; Kiss-Toth, E. Tribbles-1 Expression and Its Function to Control Inflammatory Cytokines, Including Interleukin-8 Levels are Regulated by miRNAs in Macrophages and Prostate Cancer Cells. Front. Immunol. 2020, 11, 574046. [Google Scholar] [CrossRef] [PubMed]
- Wei, X.; Tang, C.; Lu, X.; Liu, R.; Zhou, M.; He, D.; Zheng, D.; Sun, C.; Wu, Z. MiR-101 targets DUSP1 to regulate the TGF-beta secretion in sorafenib inhibits macrophage-induced growth of hepatocarcinoma. Oncotarget 2015, 6, 18389–18405. [Google Scholar] [CrossRef] [PubMed]
- Hu, S.; Zhang, J.; Guo, G.; Zhang, L.; Dai, J.; Gao, Y. Comprehensive analysis of GSEC/miR-101-3p/SNX16/PAPOLG axis in hepatocellular carcinoma. PLoS ONE 2022, 17, e0267117. [Google Scholar] [CrossRef] [PubMed]
- Takashima, Y.; Kawaguchi, A.; Iwadate, Y.; Hondoh, H.; Fukai, J.; Kajiwara, K.; Hayano, A.; Yamanaka, R. miR-101, miR-548b, miR-554, and miR-1202 are reliable prognosis predictors of the miRNAs associated with cancer immunity in primary central nervous system lymphoma. PLoS ONE 2020, 15, e0229577. [Google Scholar] [CrossRef] [PubMed]
- Wang, H.; Tang, F.; Tang, P.; Zhang, L.; Gan, Q.; Li, Y. Noncoding RNAs-mediated overexpression of KIF14 is associated with tumor immune infiltration and unfavorable prognosis in lung adenocarcinoma. Aging 2022, 14, 8013–8031. [Google Scholar] [CrossRef] [PubMed]
- Wang, W.; Zhang, J.; Wang, Y.; Xu, Y.; Zhang, S. Non-coding ribonucleic acid-mediated CAMSAP1 upregulation leads to poor prognosis with suppressed immune infiltration in liver hepatocellular carcinoma. Front. Genet. 2022, 13, 916847. [Google Scholar] [CrossRef] [PubMed]
- Yin, L.; Wang, Y. Extracellular vesicles derived from M2-polarized tumor-associated macrophages promote immune escape in ovarian cancer through NEAT1/miR-101-3p/ZEB1/PD-L1 axis. Cancer Immunol. Immunother. 2022, 1–16. [Google Scholar] [CrossRef]
- Chen, F.; Yang, D.; Ru, Y.; Cao, S.; Gao, A. MicroRNA-101 Targets CXCL12-Mediated Akt and Snail Signaling Pathways to Inhibit Cellular Proliferation and Invasion in Papillary Thyroid Carcinoma. Oncol. Res. 2019, 27, 691–701. [Google Scholar] [CrossRef] [PubMed]
- Semaan, A.; Qazi, A.M.; Seward, S.; Chamala, S.; Bryant, C.S.; Kumar, S.; Morris, R.; Steffes, C.P.; Bouwman, D.L.; Munkarah, A.R.; et al. MicroRNA-101 inhibits growth of epithelial ovarian cancer by relieving chromatin-mediated transcriptional repression of p21(waf¹/cip¹). Pharm. Res. 2011, 28, 3079–3090. [Google Scholar] [CrossRef] [PubMed]
- Zhang, S.; Wang, M.; Li, Q.; Zhu, P. MiR-101 reduces cell proliferation and invasion and enhances apoptosis in endometrial cancer via regulating PI3K/Akt/mTOR. Cancer Biomark. 2017, 21, 179–186. [Google Scholar] [CrossRef]
- Jiang, W.; Pan, J.J.; Deng, Y.H.; Liang, M.R.; Yao, L.H. Down-regulated serum microRNA-101 is associated with aggressive progression and poor prognosis of cervical cancer. J. Gynecol. Oncol. 2017, 28, 6. [Google Scholar] [CrossRef] [PubMed]
- Si, Y.; Yang, Z.; Ge, Q.; Yu, L.; Yao, M.; Sun, X.; Ren, Z.; Ding, C. Long non-coding RNA Malat1 activated autophagy, hence promoting cell proliferation and inhibiting apoptosis by sponging miR-101 in colorectal cancer. Cell Mol. Biol. Lett. 2019, 24, 019–0175. [Google Scholar] [CrossRef]
- Lu, J.; Getz, G.; Miska, E.A.; Alvarez-Saavedra, E.; Lamb, J.; Peck, D.; Sweet-Cordero, A.; Ebert, B.L.; Mak, R.H.; Ferrando, A.A.; et al. MicroRNA expression profiles classify human cancers. Nature 2005, 435, 834–838. [Google Scholar] [CrossRef] [PubMed]
- Kumar, M.S.; Lu, J.; Mercer, K.L.; Golub, T.R.; Jacks, T. Impaired microRNA processing enhances cellular transformation and tumorigenesis. Nat. Genet. 2007, 39, 673–677. [Google Scholar] [CrossRef] [PubMed]
- Solinas, G.; Germano, G.; Mantovani, A.; Allavena, P. Tumor-associated macrophages (TAM) as major players of the cancer-related inflammation. J. Leukoc. Biol. 2009, 86, 1065–1073. [Google Scholar] [CrossRef] [PubMed]
- Zhao, X.; Qu, J.; Sun, Y.; Wang, J.; Liu, X.; Wang, F.; Zhang, H.; Wang, W.; Ma, X.; Gao, X.; et al. Prognostic significance of tumor-associated macrophages in breast cancer: A meta-analysis of the literature. Oncotarget 2017, 8, 30576–30586. [Google Scholar] [CrossRef] [PubMed]

| Disease | Target Genes | References | Participation |
|---|---|---|---|
| Cervical Cancer | ZEB1 | Fan, M.J., et al. [103]. | EMT |
| CXCL6 | Shen, W., et al. [63]. | Growth/metastasis | |
| MAT2A | Chen, H.F., et al. [33]. | Proliferation/invasion | |
| KPNA2 | Wang, H., et al. [49]. | Proliferation | |
| COX-2 | Liu, Y., et al. [104]. | Angiogenesis | |
| NSCLC | mTOR-signaling pathway | Li, Z.H., et al. [100]. | Irradiation |
| MCL1 | Wang, H.Q., et al. [105]. | Drug resistance | |
| ABCC1 | Shao, N., et al. [28]. | Proliferation/Drug resistance | |
| CUL4B | Xie, F.W., et al. [47]. | Proliferation/migration/invasion | |
| ZEB1 | Han, L., et al. [29]. | Proliferation/metastasis | |
| CDYL | Li, K., et al. [30]. | Proliferation/invasion | |
| KRAS | Ding, C.Z., et al. [44]. | Proliferation/glycolysis | |
| SOX9 | Kong, X.J., et al. [106]. | Progression | |
| CUL4B | Zhang, H.F., et al. [107]. | progression | |
| Mcl-1 | Shahverdi, et al. [31]. | Proliferation/apoptosis | |
| CISD1 | Jiang, X.L., et al. [42]. | Proliferation/migration | |
| USP47 | Park, et al. [46]. | Proliferation | |
| MALAT-1 | Zhang, X.Q., et al. [32]. | Proliferation/metastasis | |
| DNMT3a | Yan, F., et al. [65]. | Migration | |
| Ovarian Cancer | ZEB1 | Liang, H.H., et al. [108]. | Invasion/metastasis |
| ZEB1/ZEB2 | Guo, F., et al. [76]. | EMT | |
| FN1 | Liang, H.H., et al. [69]. | Invasion/migration | |
| PI3K/AKT | Wei, M., et al. [109] | Growth/metastasis | |
| CtBP2 | Cui, T.X., et al. [19]. | Sphere formation/ metastasis | |
| Breast Cancer | EZH2 | Jiang, H.B., et al. [110]. | Proliferation/apoptosis |
| Invasion/ migration | |||
| Nrf2 | Yi, J., et al. [35]. | Proliferation/apoptosis | |
| Med19 | Zhang, X.F., et al. [34]. | Proliferation/migration /invasion | |
| Jak2 | Wang, L., et al. [11]. | Apoptosis | |
| COX-2-MMP1 signaling | Harati, et al. [70]. | Metastasis | |
| HER-2 positive Breast Cancer | Normann, et al. [92]. | Drug sensitivity | |
| Oral Cancer | BICC1 | Wang, H., et al. [82]. | Apoptosis |
| Colon Cancer | EZH2 | Huang, Z.R., et al. [111]. | Migration |
| EZH2 | Wang, G.Q., et al. [112]. | Apoptosis | |
| STC1 | Luan, C.Y., et al. [36]. | Proliferation/migration /invasion | |
| Cox2 | Cai, Y., et al. [113]. | ||
| CREB1 | Yang, Q.L., et al. [37]. | Proliferation/migration | |
| Colorectal Cancer | OGT/EZH2 | Jiang, M.Z., et al. [114]. | Metastasis |
| Notch1 | Wu, H.B., et al. [38]. | Proliferation/metastasis | |
| ZEB1 | Xiong, W.C., et al. [68]. | Proliferation/migration | |
| HIPK3 | Tao, L.P., et al. [115]. | Drug resistance | |
| Rap1b | Zhou, Z.Y., et al. [67]. | Progression | |
| Pancreatic Cancer | STMN1 | Zhu, L., et al. [39]. | Proliferation/invasion |
| autophagy | Zhang, X.F., et al. [94]. | Drug resistance | |
| Prostate Cancer | CUL4B | Gu, Z.H., et al. [48]. | Proliferation/migrating /invasion |
| Rap1A | Chen, J.H., et al. [40]. | Proliferation/migration /invasion | |
| Bladder Cancer | EZH2 | Wang, K.P., et al. [116]. | Proliferative/invasion /migration |
| VEGF-C | Liu, P.H., et al. [117]. | Drug resistance | |
| FZD4 | Chen, L., et al. [71]. | Migration/invasion | |
| Papillary Thyroid Cancer | CLDN1 | Du, Y.L., et al. [66]. | Migration/invasion |
| c-met and MCL-1 | Zhu, J., et al. [87]. | Apoptosis | |
| Gastric Cancer | AMPK | Cao, S.G., et al. [26]. | Proliferation |
| EZH2 | Cao, C., et al. [118]. | Proliferation/migration and invasion | |
| PIM 1 | Wu, F.B., et al. [25]. | Proliferation/invasion /apoptosis | |
| SRF | Wu, X.Y., et al. [79]. | Proliferation/invasion | |
| Liver Cancer | ANXA2 | Ma, S., et al. [45]. | Proliferation |
| MAPK/ERK pathway | Meng, X., et al. [22]. | Proliferation | |
| Ding, A.K., et al. [119]. | Proliferation/HBV replication | ||
| HGF/c-Met pathway | Liu, Y., et al. [23]. | Proliferation/migration | |
| ZNF217 | Si, W.Z., et al. [24]. | Proliferation/invasion | |
| VEGF-C | Liu, Z.Y., et al. [80]. | Migration/invasion | |
| Girdin | Cao, K., et al. [81]. | Proliferation/migration and invasion | |
| Esophageal Squamous Cell Cancer | ATM and mTOR | Chen, M.Q., et al. [101]. | Irradiation |
| EZH2 | Qiu, B.Q., et al. [120]. | Proliferation/migration /invasion | |
| Retinoblastoma | EZH2, HDAC9 | Jin, Q.F., et al. [41]. | Proliferation |
| Melanoma | RAP2B | Zhou, H., et al. [27]. | Proliferation/migration/invasion |
| Glioblastoma | TRIM44 | Li, L., et al. [72]. | Proliferation/migration/invasion |
| Osteosarcoma | ZEB2 | Lin, H.P., et al. [78]. | Proliferation/invasion |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Liu, N.; Yang, C.; Gao, A.; Sun, M.; Lv, D. MiR-101: An Important Regulator of Gene Expression and Tumor Ecosystem. Cancers 2022, 14, 5861. https://doi.org/10.3390/cancers14235861
Liu N, Yang C, Gao A, Sun M, Lv D. MiR-101: An Important Regulator of Gene Expression and Tumor Ecosystem. Cancers. 2022; 14(23):5861. https://doi.org/10.3390/cancers14235861
Chicago/Turabian StyleLiu, Ning, Chunsheng Yang, Ang Gao, Meili Sun, and Deguan Lv. 2022. "MiR-101: An Important Regulator of Gene Expression and Tumor Ecosystem" Cancers 14, no. 23: 5861. https://doi.org/10.3390/cancers14235861
APA StyleLiu, N., Yang, C., Gao, A., Sun, M., & Lv, D. (2022). MiR-101: An Important Regulator of Gene Expression and Tumor Ecosystem. Cancers, 14(23), 5861. https://doi.org/10.3390/cancers14235861






