A Review and In Silico Analysis of Tissue and Exosomal Circular RNAs: Opportunities and Challenges in Thyroid Cancer
Abstract
Simple Summary
Abstract
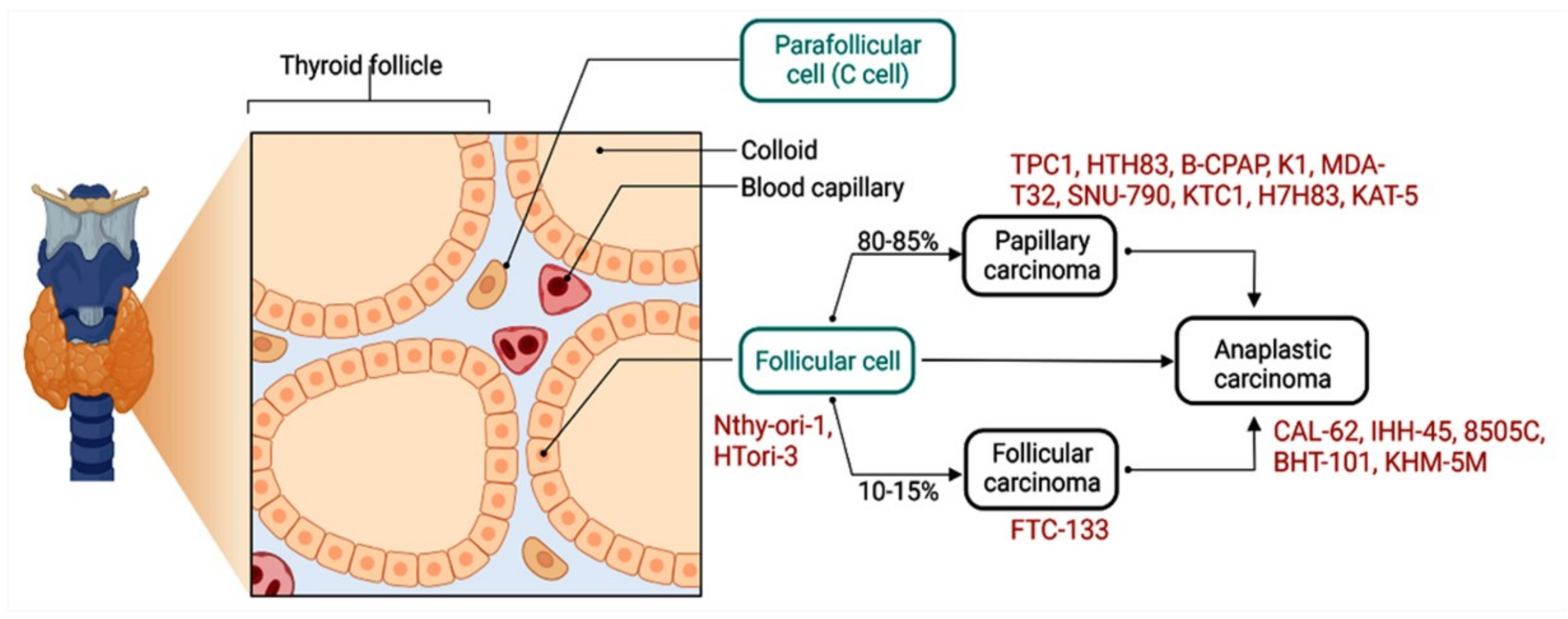
1. Introduction
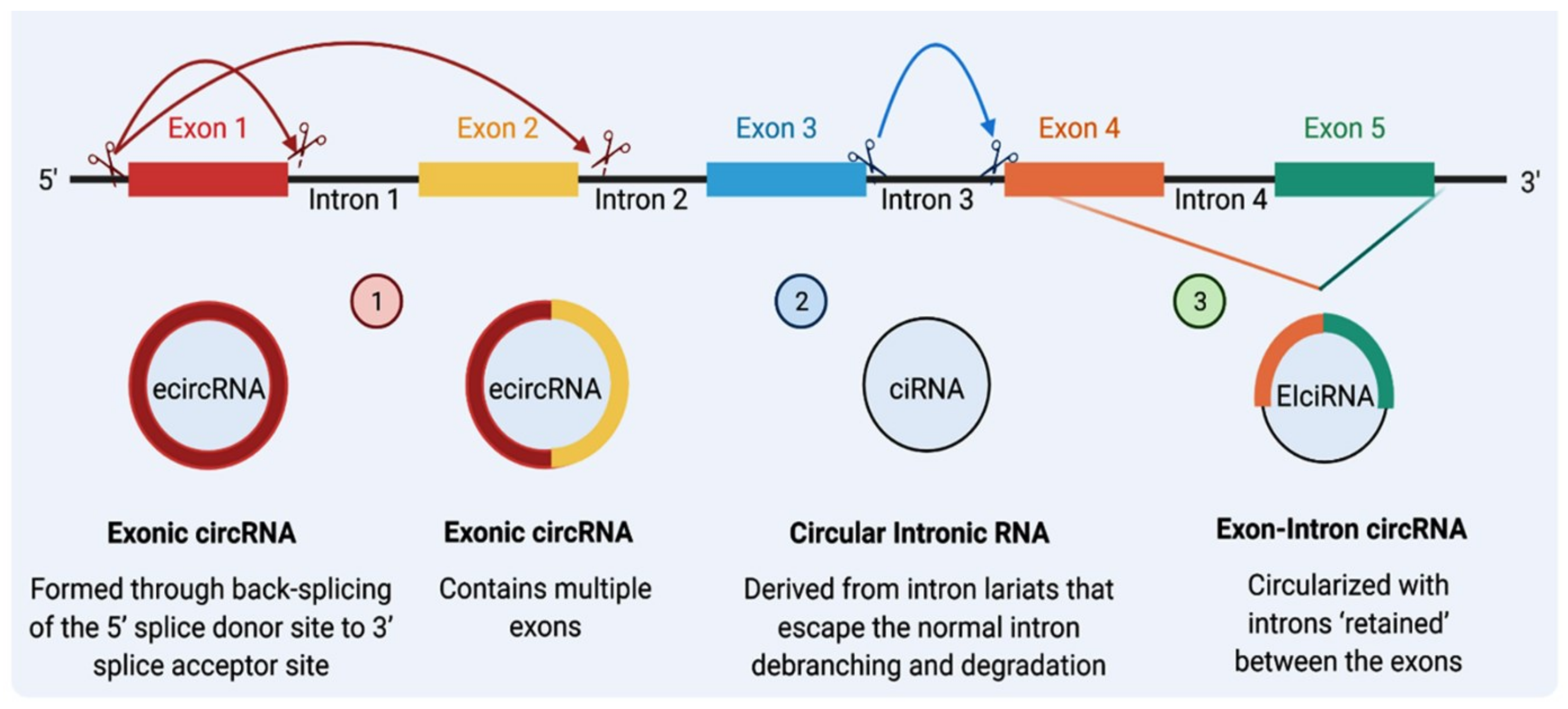
1.1. CircRNA Nomenclature
1.2. CircRNA Biogenesis, Export, and Turnover
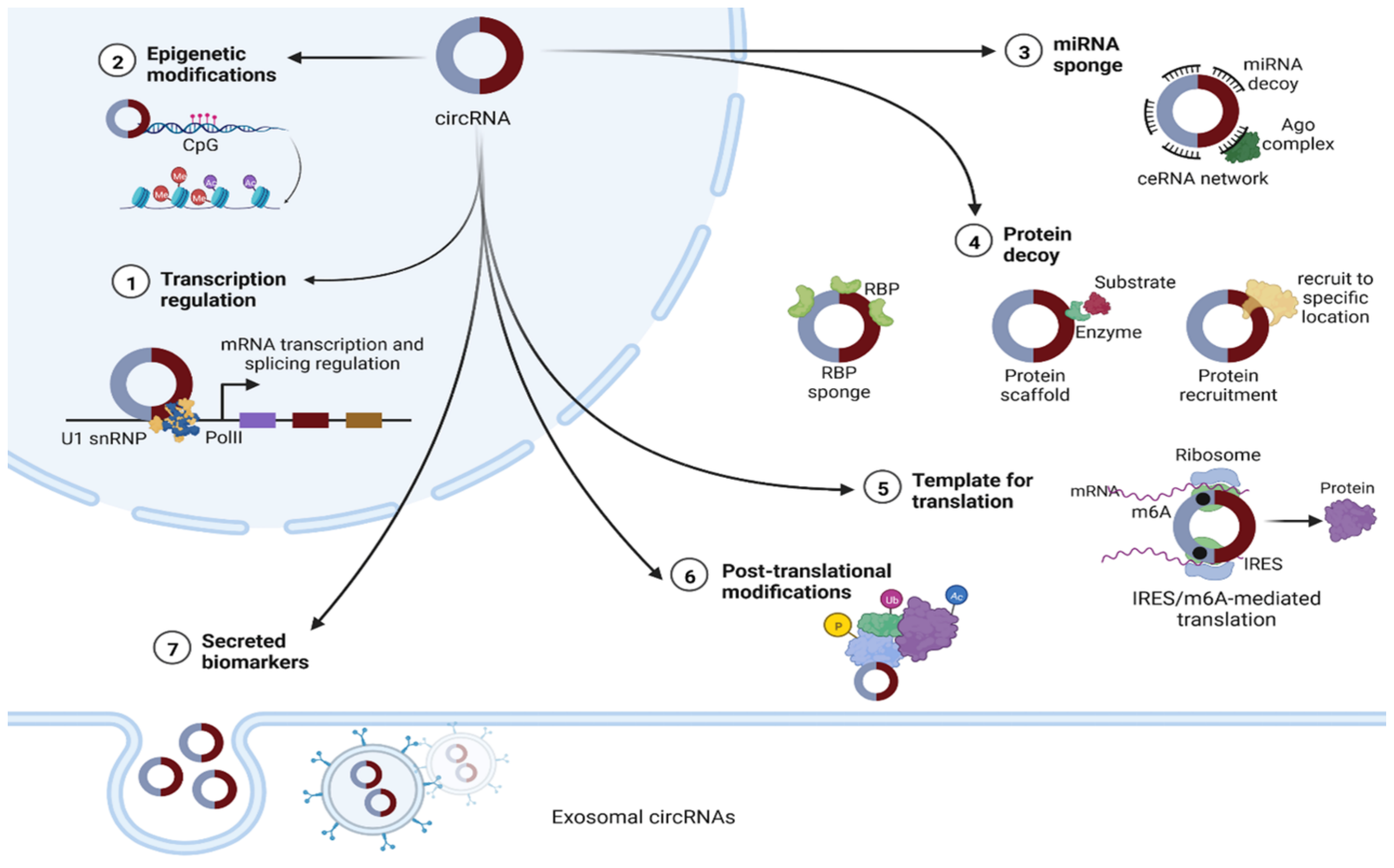
1.3. Biological Activity of circRNAs
1.3.1. Epigenetic Regulators
1.3.2. Transcription Regulators
1.3.3. Regulation of Transcription Factors
| Transcription Factors | Type of TF | circRNA | Parental Gene | miRNA Sponge | Reference |
|---|---|---|---|---|---|
| Upregulated TF | |||||
| ↑MTA1 | Homeodomain TF | circ_0039411 | ↓miR-1179, miR-1205 | [49] | |
| ↑ZEB1 | C2H2 zinc finger TF | circ-FAT1(e2) | FATI | ↓miR-873 | [62] |
| ↑SOX2 | HMG box TF | circ_0005273 | ↓miR-1138 | [64] | |
| ↑SOX4 | HMG box TF | circ_0001018 | ↓ miR-338-3p | [63] | |
| ↑STAT1 | DNA-binding TF | circ-NRIP1 | NRIP1 | ↓miR-195-5p | [65] |
| ↑E2F3 | General TF | circ-PRKCI | PRKCI | ↓miR-335 | [66] |
| Downregulated TF | |||||
| ↓TCF3, TCF4, LEF1 | Basic helix-loop-helix TF | circ_102171 | [27] | ||
| ↓TP53 | P53-like TF | circ-TP53 | TP53 | ↓miR-1233-3p | [30] |
| ↓KLF6 | C2H2 zinc finger TF | circ-ABCB10 | ABCB10 | [47] |
1.3.4. Acting as Molecular Sponges
1.3.5. Acting as Regulators of Translation into Protein
1.3.6. Acting as Protein Decoys
1.4. Online Databases and Resources
2. Evidence Acquisition
3. Results
3.1. Diagnostic and Prognostic Utility of circRNAs in TC Patients
| circRNAs | T | N | M | ETE | Clinical Stage | Poor Survival | Ref. |
|---|---|---|---|---|---|---|---|
| Upregulated biomarkers | |||||||
| circ_PSD3 | [109] | ||||||
| circ-UMAD1 | ● | [115] | |||||
| circ_0058124 | ● | ● | ● | ● | ● | [110] | |
| circ-NRIP1 | ● | [65] | |||||
| circ_0005273 | ● | [64] | |||||
| circ_0067934 | ● | ● | ● | ● | [113] | ||
| circ_BACH2 | ● | ● | ● | ● | [3] | ||
| circ_0008274 | ● | ● | [111,112] | ||||
| circ_0004458 | ● | ● | ● | [116] | |||
| circ_0062389 | ● | ● | [117] | ||||
| circ_0011290 | ● | [32] | |||||
| circ-NRIP1 | ● | [65] | |||||
| circ_0001666 | ● | [118] | |||||
| Downregulated biomarkers | |||||||
| circ_ITCH | [71] | ||||||
| circ_0137287 | ● | ● | ● | [114] |
3.2. Circular RNAs Mediate Tumor Progression In Vivo and In Vitro
3.2.1. Tumor-Suppression-Related circRNAs
3.2.2. Tumorigenesis-Related circRNAs
| CircRNA | Parental Gene | Model | Source | miRNA | Target Gene | Mechanism | Ref. |
|---|---|---|---|---|---|---|---|
| circ-TP53 | TP53 | In vitro, in vivo | TPC-1 | ↓miR-1233-3p | ↑MDM2, ↓TP53 | Promotes cancer cell viability and proliferation | [30] |
| circ_0004458 | In vitro, in vivo, human (N = 48) | BCPAP, TPC-1, K1, IHH4 | ↓miR-885-5p | ↑RAC1 | Promotes cell growth and inhibits apoptosis and cell cycle arrest | [116] | |
| circ-ABCB10 | ABCB10 | In vitro, in vivo, human (N = 40) | ↓KLF6 | Enhances proliferation and invasion | [47] | ||
| circ_0025033 | In vitro | ↓miR-1233, miR-1304 | Promotes cell growth, invasion, and metastasis, triggers clone formation and prevents apoptosis | [48] | |||
| circ_0039411 | In vitro, human (N = 46) | K1, TPC-1, FTC-133, SW579 | ↓miR-1179, miR-1205 | ↑ MTA1, ABCA9 | Promotes cell proliferation/motility and inhibits apoptosis | [49] | |
| circ-BACH2 | BACH2 | In vitro | ↓miR-139-5p | ↑LMO4 | Initiates tumor | [3] | |
| circ_0058124 | In vivo, in vitro, human (N = 92) | TPC-1, K1 | ↓miR-218-5p | ↑NUMB, NOTCH3, GATAD2A | Acts as oncogene | [110] | |
| circ_0058124 | In vitro, in vivo | TPC-1, IHH-4 | ↓miR-370-3p | ↑LMO4 | Promotes progression, colony formation, migration, invasion, inhibits apoptosis and tumor growth | [131] | |
| circ_0058124 | In vitro, in vivo, human (N = 51) | BCPAP, TPC-1, IHH-4, HTH83 | ↓miR-940 | Acts as oncogene | [28] | ||
| circ-LDLR | LDLR | In vitro, in vivo, human (N = 60) | ↓miR-195-5p | ↑LIPH | Promotes malignant behavior, colony formation, proliferation, migration, and invasion, and inhibits apoptosis | [132] | |
| circ_ZFR | ZFR | In vitro, human (N = 41) | k1, TPC-1, SW579, FTC133 | ↓miR-1261 | ↑C8orf4 | Triggers tumor growth | [31] |
| circ_102171 | In vitro, in vivo, human (N = 47) | TPC-1, NPA87, KAT-5 | ↓CTNNB1P1, TCF3, TCF4, LEF1 | Promotes progression, cell proliferation, migration, activation of the beta-catenin pathway, inhibits apoptosis | [27] | ||
| circ_0011290 | In vitro | NIM-1, HTH83, TPC-1, K1, BCPAP | ↓miR-1252 | ↑FSTL1 | Promotes cell viability, proliferation, apoptosis, and glucose metabolisms | [32] | |
| circ_0058129 | In vitro, in vivo, human (N = 70) | TPC-1, SNU-790 | ↓miR-873-5p | ↑FSTL1 | Fosters cell proliferation, invasion, and migration | [133] | |
| circ_0005273 | In vitro | KTC-1, IHH-4, BCPAP, TPC-1 | ↓miR-1138 | ↑SOX2 | Promotes cell viability, proliferation, invasion, and migration | [64] | |
| circ_0005273 | In vitro, human | ↓miR-1138 | Acts as oncogene | [113] | |||
| circ-NEK6 | NEK6 | ↓miR-370-3p | ↑FZD8 | Promotes progression, invasion, and metastasis, activates Wnt signaling pathway | [73] | ||
| circ-FAT1(e2) | FATI | ↓miR-873 | ↑ZEB1 | Promotes PTC cell growth, migration, and invasion | [62] | ||
| circ-PSD3 | PSD3 | In vitro, in vivo | ↓miR-637 | ↑ HEMGN | Activates PI3K/Akt signaling, promote cell cycle progression, proliferation and metastasis and impedes apoptosis | [109] | |
| circ_0008274 | In vitro, in vivo | ↓miR-154-3p | ↑SLC7A11 | Regulates apoptosis, migration, and adhesion | [111] | ||
| circ_0008274 | In vitro, human | ↑AMPK, mTOR | Promotes proliferation/invasion through the “AMPK/mTOR” signaling pathway | [112] | |||
| circ_0067934 | In vitro, human (N = 57) | ↑PI3K, AKT | Promotes EMT, PI3K/AKT signaling pathway, cell proliferation, invasion, migration, and inhibits apoptosis. | [121] | |||
| circ_0067934 | In vitro, in vivo | ↓miR-1304 | CXCR1, PRKCI | Increases cell proliferation, migration, and invasion | [113] | ||
| circ_0067934 | |||||||
| circ-DOCK1 | DOCK1 | In vitro | FTC-133, TPC-1 | ↓miR-124 | Induces tumorigenesis | [134] | |
| circ-PRMT5 | PRMT5 | In vitro | K1, TPC-1, IHH4, BCPAP cells | ↓miR-30c | Induces tumorigenesis | [135] | |
| circ-FOXM1 | FOXM1 | In vitro, in vivo, human (N = 78) | K1, IHH-4, BCPAP, TCP-1 | ↓miR-1179 | Increases tumor growth | [136] | |
| circ_0011385 | In vitro, in vivo | BCPAP | ↓miR-361-3p | Increases cell proliferation, invasion, and migration, inhibits apoptosis and regulates metastasis-related proteins | [137] | ||
| circ-RAPGEF5 | RAPGEF5 | In vitro, in vivo | BCPAP, KTC-1, K1, HEK293 | ↓miR-198 | ↑FGFR1 | Knockdown inhibits cell proliferation, migration, and invasion | [138] |
| circ_0103552 | In vitro, human (N = 56) | TPC-1, SW579, 8505C | Regulator for invasion and migration | [139] | |||
| circ-UMAD1 | UMAD1 | Human (N = 50) | ↓miR-873 | ↑Gal3 | Poor prognosis, lymph node metastasis | [115] | |
| circ_IPCEF1 | Human (N = 50) | ↓miR-3619-5p | ↑CASR, CDC25B, NFκB1 and SHOC2 | Of 158 deregulated circRNAs, it showed the best predictive power | [140] | ||
| circ_0001666 | In vitro, in vivo, human | ↓miR-330-5p, miR-193a-5p, miR-326 | ↑ETV4 | Enhances G1 phase cell cycle progression | [118] | ||
| circ-UBAP2 | UBAP2 | In vitro | ↓miR-370-3p | Regulates proliferation, apoptosis, and invasion | [141] | ||
| circ-PVT1 | PVT1 | In vitro | ↓ miR-195 | ↑VEGFA | Activates the Wnt/β-catenin signaling pathway | [142] | |
| circ-PUM1 | PUM1 | In vitro | ↓miR-21 | ↑MAPK1 | Promotes cell growth, metastasis, and glycolysis | [143] | |
| circ-PRKCI | PRKCI | ↓miR-335 | ↑E2F3, MMP2, MMP9, snail | Promotes cell progression and glycolysis | [66] | ||
| circ_0079558 | In vitro, human | ↓miR-26b-5p | ↑MET/AKT | Facilitates the proliferation and motility | [144] | ||
| circ-RPS28 | RPS28 | In vitro | ↓miR-345-5p | ↑FZD8, MMP2, MMP9, BAX1 | Regulates cell growth and motility | [145] | |
| circ-NRIP1 | NRIP1 | In vitro, in vivo, human | ↓miR-195-5p | ↑p38, JAK2, STAT1 | Promotes cell proliferation/invasion and inhibits apoptosis | [65] | |
| circ_0001018 | In vitro | ↓ miR-338-3p | ↑SOX4 | Facilitates cell survival, invasion, G1/S cell cycle progression, and represses cell apoptosis | [63] | ||
| circ_0067934 | In vitro, in vivo, human | ↓ miR-1301-3p | ↑HMGB1 | Increases growth, colony formation, migration, invasion, EMT | [146] | ||
| circ_0062389 | In vitro, human | ↓miR-1179 | ↑HMGB1 | Promotes proliferation, migration, and EMT | [117] | ||
| circ-HIPK3 | In vitro | ↓miR-338-3p | ↑RAB23 | Promotes invasiveness, migration, invasion, and proliferation | [147] | ||
| circ_0059354 | In vitro, in vivo | ↓miR-766-3p | ↑ARFGEF1 | Aggravates cell proliferation, migration, invasion, and angiogenesis | [123] | ||
| circ-NEURL4 | NEURL4 | ↓ miR-1278 | ↑LATS1 | Enhances cell proliferation and invasion | [148] | ||
| circ-TIAM1 | TIAM1 | In vitro, in vivo, human (N = 60) | K1, TPC-1, IHH-4, B-CPAP | ↓miR-646 | ↑hnRNPA1 | Promotes cell migration, adhesion, growth, and polarity | [149] |
| circ-ITGA7 | ITGA7 | In vitro | TPC1 and CAL-62 | ↓miR-198 | ↑FGFR1 | Promotes migration and invasion | [72] |
| ciRS-7 | ↓miR-7 | ↑EGFR | Promotes tumor growth, EMT | [78] | |||
| circ_0001681 | ↓miR-942-5p | ↑TWIST1 | [150] |
3.3. Tumor-Cell-Derived Exosomal circRNAs
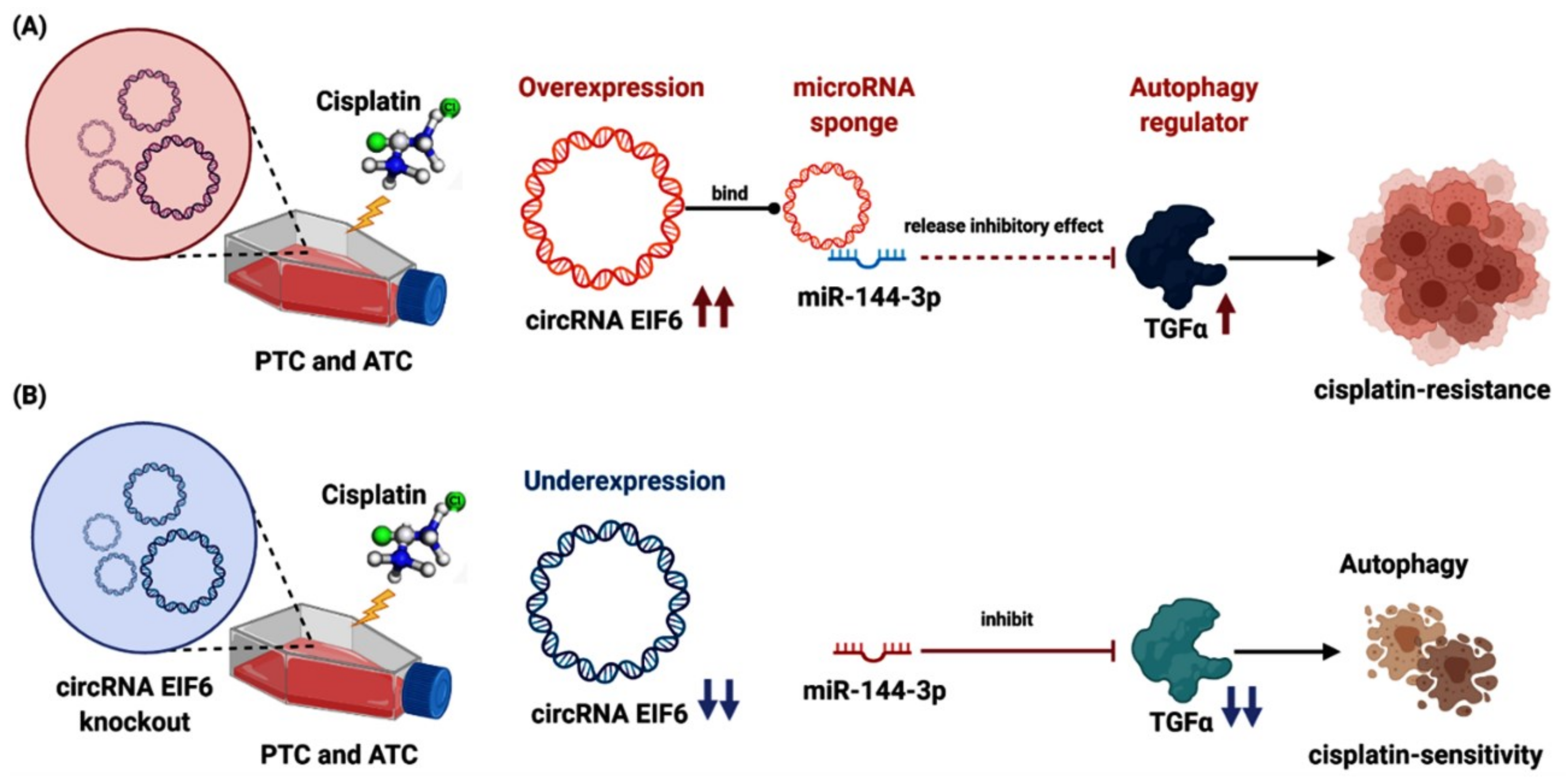
3.4. Circular RNAs and Treatment Resistance
3.5. Functional Enrichment Analysis for the Deregulated Markers
3.6. Genome-Wide Circular RNA Screening
3.6.1. Data Source and Processing
3.6.2. Identification of Differentially Expressed circRNAs (DEC)
4. Discussion of the Current Challenges in Clinical Practice and Future Perspectives
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- Cabanillas, M.E.; McFadden, D.G.; Durante, C. Thyroid cancer. Lancet 2016, 388, 2783–2795. [Google Scholar] [CrossRef]
- Kitahara, C.M.; Sosa, J.A. The changing incidence of thyroid cancer. Nat. Rev. Endocrinol. 2016, 12, 646–653. [Google Scholar] [CrossRef] [PubMed]
- Cai, X.; Zhao, Z.; Dong, J.; Lv, Q.; Yun, B.; Liu, J.; Shen, Y.; Kang, J.; Li, J. Circular RNA circBACH2 plays a role in papillary thyroid carcinoma by sponging miR-139-5p and regulating LMO4 expression. Cell Death Dis. 2019, 10, 1–12. [Google Scholar] [CrossRef]
- Toraih, E.A.; Fawzy, M.S.; Mohammed, E.A.; Hussein, M.H.; El-Labban, M.M. MicroRNA-196a2 Biomarker and Targetome Network Analysis in Solid Tumors. Mol. Diagn. Ther. 2016, 20, 559–577. [Google Scholar] [CrossRef] [PubMed]
- Toraih, E.A.; Aly, N.M.; Abdallah, H.Y.; Al-Qahtani, S.A.; Shaalan, A.A.; Hussein, M.H.; Fawzy, M.S. MicroRNA-target cross-talks: Key players in glioblastoma multiforme. Tumour Biol. 2017, 39, 1010428317726842. [Google Scholar] [CrossRef]
- Toraih, E.A.; Mohammed, E.A.; Farrag, S.; Ramsis, N.; Hosny, S. Pilot Study of Serum MicroRNA-21 as a Diagnostic and Prognostic Biomarker in Egyptian Breast Cancer Patients. Mol. Diagn. Ther. 2015, 19, 179–190. [Google Scholar] [CrossRef] [PubMed]
- Toraih, E.A.; Alghamdi, S.A.; El-Wazir, A.; Hosny, M.; Hussein, M.H.; Khashana, M.; Fawzy, M.S. Dual biomarkers long non-coding RNA GAS5 and microRNA-34a co-expression signature in common solid tumors. PLoS ONE 2018, 13, e0198231. [Google Scholar] [CrossRef]
- Hsu, M.-T.; Coca-Prados, M. Electron microscopic evidence for the circular form of RNA in the cytoplasm of eukaryotic cells. Nature 1979, 280, 339–340. [Google Scholar] [CrossRef]
- Du, W.W.; Fang, L.; Yang, W.; Wu, N.; Awan, F.M.; Yang, Z.; Yang, B.B. Induction of tumor apoptosis through a circular RNA enhancing Foxo3 activity. Cell Death Differ. 2016, 24, 357–370. [Google Scholar] [CrossRef]
- Werfel, S.; Nothjunge, S.; Schwarzmayr, T.; Strom, T.-M.; Meitinger, T.; Engelhardt, S. Characterization of circular RNAs in human, mouse and rat hearts. J. Mol. Cell. Cardiol. 2016, 98, 103–107. [Google Scholar] [CrossRef]
- Lasda, E.; Parker, R. Circular RNAs: Diversity of form and function. RNA 2014, 20, 1829–1842. [Google Scholar] [CrossRef]
- Capel, B.; Swain, A.; Nicolis, S.; Hacker, A.; Walter, M.; Koopman, P.; Goodfellow, P.; Lovell-Badge, R. Circular transcripts of the testis-determining gene Sry in adult mouse testis. Cell 1993, 73, 1019–1030. [Google Scholar] [CrossRef]
- Cocquerelle, C.; Mascrez, B.; Hétuin, D.; Bailleul, B. Mis-splicing yields circular RNA molecules. FASEB J. 1993, 7, 155–160. [Google Scholar] [CrossRef]
- Hansen, T.B.; Jensen, T.I.; Clausen, B.H.; Bramsen, J.B.; Finsen, B.; Damgaard, C.K.; Kjems, J. Natural RNA circles function as efficient microRNA sponges. Nature 2013, 495, 384–388. [Google Scholar] [CrossRef]
- Zhang, Y.; Zhang, X.-O.; Chen, T.; Xiang, J.-F.; Yin, Q.-F.; Xing, Y.-H.; Zhu, S.; Yang, L.; Chen, L.-L. Circular Intronic Long Noncoding RNAs. Mol. Cell 2013, 51, 792–806. [Google Scholar] [CrossRef]
- Ashwal-Fluss, R.; Meyer, M.; Pamudurti, N.R.; Ivanov, A.; Bartok, O.; Hanan, M.; Evantal, N.; Memczak, S.; Rajewsky, N.; Kadener, S. circRNA biogenesis competes with pre-mRNA splicing. Mol. Cell 2014, 56, 55–66. [Google Scholar] [CrossRef]
- Kristensen, L.S.; Hansen, T.B.; Venø, M.T.; Kjems, J. Circular RNAs in cancer: Opportunities and challenges in the field. Oncogene 2018, 37, 555–565. [Google Scholar] [CrossRef]
- Liu, J.; Zhang, X.; Yan, M.; Li, H. Emerging Role of Circular RNAs in Cancer. Front. Oncol. 2020, 10, 663. [Google Scholar] [CrossRef]
- Brown, J.R.; Chinnaiyan, A.M. The Potential of Circular RNAs as Cancer Biomarkers. Cancer Epidemiol. Biomark. Prev. 2020, 29, 2541–2555. [Google Scholar] [CrossRef]
- Nielsen, A.F.; Bindereif, A.; Bozzoni, I.; Hanan, M.; Hansen, T.B.; Irimia, M.; Kadener, S.; Kristensen, L.S.; Legnini, I.; Morlando, M.; et al. Best practice standards for circular RNA research. Nat. Methods 2022, 1–13. [Google Scholar] [CrossRef]
- Hu, W.; Bi, Z.; Chen, Z.-L.; Liu, C.; Li, L.-L.; Zhang, F.; Zhou, Q.; Song, Y.-Y.; Zhan, B.-T.; Zhang, Q.; et al. Emerging landscape of circular RNAs in lung cancer. Cancer Lett. 2018, 427, 18–27. [Google Scholar] [CrossRef]
- Han, D.; Li, J.; Wang, H.; Su, X.; Hou, J.; Gu, Y.; Qian, C.; Lin, Y.; Liu, X.; Huang, M.; et al. Circular RNA circMTO1 acts as the sponge of microRNA-9 to suppress hepatocellular carcinoma progression. Hepatology 2017, 66, 1151–1164. [Google Scholar] [CrossRef]
- Hsiao, K.-Y.; Lin, Y.-C.; Gupta, S.K.; Chang, N.; Yen, L.; Sun, H.S.; Tsai, S.-J. Noncoding Effects of Circular RNA CCDC66 Promote Colon Cancer Growth and Metastasis. Cancer Res. 2017, 77, 2339–2350. [Google Scholar] [CrossRef]
- Su, H.; Tao, T.; Yang, Z.; Kang, X.; Zhang, X.; Kang, D.; Wu, S.; Li, C. Circular RNA cTFRC acts as the sponge of MicroRNA-107 to promote bladder carcinoma progression. Mol. Cancer 2019, 18, 1–15. [Google Scholar] [CrossRef]
- Xia, W.; Qiu, M.; Chen, R.; Wang, S.; Leng, X.; Wang, J.; Xu, Y.; Hu, J.; Dong, G.; Xu, L.; et al. Circular RNA has_circ_0067934 is upregulated in esophageal squamous cell carcinoma and promoted proliferation. Sci. Rep. 2016, 6, 35576. [Google Scholar] [CrossRef]
- Yang, R.; Xing, L.; Zheng, X.; Sun, Y.; Wang, X.; Chen, J. RETRACTED ARTICLE: The circRNA circAGFG1 acts as a sponge of miR-195-5p to promote triple-negative breast cancer progression through regulating CCNE1 expression. Mol. Cancer 2019, 18, 1–19. [Google Scholar] [CrossRef]
- Bi, W.; Huang, J.; Nie, C.; Liu, B.; He, G.; Han, J.; Pang, R.; Ding, Z.; Xu, J.; Zhang, J. CircRNA circRNA_102171 promotes papillary thyroid cancer progression through modulating CTNNBIP1-dependent activation of β-catenin pathway. J. Exp. Clin. Cancer Res. 2018, 37, 1–9. [Google Scholar] [CrossRef]
- Borran, S.; Ahmadi, G.; Rezaei, S.; Anari, M.M.; Modabberi, M.; Azarash, Z.; Razaviyan, J.; Derakhshan, M.; Akhbari, M.; Mirzaei, H. Circular RNAs: New players in thyroid cancer. Pathol.-Res. Pract. 2020, 216, 153217. [Google Scholar] [CrossRef]
- Zhong, Z.; Huang, M.; Lv, M.; He, Y.; Duan, C.; Zhang, L.; Chen, J. Circular RNA MYLK as a competing endogenous RNA promotes bladder cancer progression through modulating VEGFA/VEGFR2 signaling pathway. Cancer Lett. 2017, 403, 305–317. [Google Scholar] [CrossRef]
- Ma, W.; Zhao, P.; Zang, L.; Zhang, K.; Liao, H.; Hu, Z. CircTP53 promotes the proliferation of thyroid cancer via targeting miR-1233-3p/MDM2 axis. J. Endocrinol. Investig. 2020, 44, 353–362. [Google Scholar] [CrossRef]
- Wei, H.; Pan, L.; Tao, D.; Li, R. Circular RNA circZFR contributes to papillary thyroid cancer cell proliferation and invasion by sponging miR-1261 and facilitating C8orf4 expression. Biochem. Biophys. Res. Commun. 2018, 503, 56–61. [Google Scholar] [CrossRef] [PubMed]
- Hu, Z.; Zhao, P.; Zhang, K.; Zang, L.; Liao, H.; Ma, W. Hsa_circ_0011290 regulates proliferation, apoptosis and glycolytic phenotype in papillary thyroid cancer via miR-1252/ FSTL1 signal pathway. Arch. Biochem. Biophys. 2020, 685, 108353. [Google Scholar] [CrossRef] [PubMed]
- Seal, R.L.; Chen, L.; Griffiths-Jones, S.; Lowe, T.M.; Mathews, M.B.; O’Reilly, D.; Pierce, A.J.; Stadler, P.F.; Ulitsky, I.; Wolin, S.L.; et al. A guide to naming human non-coding RNA genes. EMBO J. 2020, 39, e103777. [Google Scholar] [CrossRef] [PubMed]
- Zhang, Y.; Xue, W.; Li, X.; Zhang, J.; Chen, S.; Zhang, J.-L.; Yang, L.; Chen, L.-L. The Biogenesis of Nascent Circular RNAs. Cell Rep. 2016, 15, 611–624. [Google Scholar] [CrossRef] [PubMed]
- Jeck, W.R.; Sorrentino, J.A.; Wang, K.; Slevin, M.K.; Burd, C.E.; Liu, J.; Marzluff, W.F.; Sharpless, N.E. Circular RNAs are abundant, conserved, and associated with ALU repeats. RNA 2013, 19, 141–157. [Google Scholar] [CrossRef] [PubMed]
- Kristensen, L.S.; Andersen, M.S.; Stagsted, L.V.W.; Ebbesen, K.K.; Hansen, T.B.; Kjems, J. The biogenesis, biology and characterization of circular RNAs. Nat. Rev. Genet. 2019, 20, 675–691. [Google Scholar] [CrossRef]
- Salzman, J.; Chen, R.E.; Olsen, M.N.; Wang, P.L.; Brown, P.O. Cell-type specific features of circular RNA expression. PLoS Genet. 2013, 9, e1003777. [Google Scholar] [CrossRef]
- Huang, A.; Zheng, H.; Wu, Z.; Chen, M.; Huang, Y. Circular RNA-protein interactions: Functions, mechanisms, and identification. Theranostics 2020, 10, 3503–3517. [Google Scholar] [CrossRef]
- Wu, Q.; Li, P.; Wu, M.; Liu, Q. Deregulation of Circular RNAs in Cancer from the Perspectives of Aberrant Biogenesis, Transport and Removal. Front. Genet. 2019, 10, 16. [Google Scholar] [CrossRef]
- Chen, L.-L.; Yang, L. Regulation of circRNA biogenesis. RNA Biol. 2015, 12, 381–388. [Google Scholar] [CrossRef]
- Memczak, S.; Jens, M.; Elefsinioti, A.; Torti, F.; Krueger, J.; Rybak, A.; Maier, L.; Mackowiak, S.D.; Gregersen, L.H.; Munschauer, M.; et al. Circular RNAs are a large class of animal RNAs with regulatory potency. Nature 2013, 495, 333–338. [Google Scholar] [CrossRef]
- Kristensen, L.S.; Jakobsen, T.; Hager, H.; Kjems, J. The emerging roles of circRNAs in cancer and oncology. Nat. Rev. Clin. Oncol. 2021, 19, 188–206. [Google Scholar] [CrossRef]
- Zhou, C.; Molinie, B.; Daneshvar, K.; Pondick, J.V.; Wang, J.; Van Wittenberghe, N.; Xing, Y.; Giallourakis, C.C.; Mullen, A.C. Genome-Wide Maps of m6A circRNAs Identify Widespread and Cell-Type-Specific Methylation Patterns That Are Distinct from mRNAs. Cell Rep. 2017, 20, 2262–2276. [Google Scholar] [CrossRef]
- Li, Y.; Zheng, Q.; Bao, C.; Li, S.; Guo, W.; Zhao, J.; Chen, D.; Gu, J.; He, X.; Huang, S. Circular RNA is enriched and stable in exosomes: A promising biomarker for cancer diagnosis. Cell Res. 2015, 25, 981–984. [Google Scholar] [CrossRef]
- Dou, Y.; Cha, D.J.; Franklin, J.L.; Higginbotham, J.N.; Jeppesen, D.K.; Weaver, A.M.; Prasad, N.; Levy, S.; Coffey, R.J.; Patton, J.G.; et al. Circular RNAs are down-regulated in KRAS mutant colon cancer cells and can be transferred to exosomes. Sci. Rep. 2016, 6, 37982. [Google Scholar] [CrossRef]
- Wang, S.; Dong, Y.; Gong, A.; Kong, H.; Gao, J.; Hao, X.; Liu, Y.; Wang, Z.; Fan, Y.; Liu, C.; et al. Exosomal circRNAs as novel cancer biomarkers: Challenges and opportunities. Int. J. Biol. Sci. 2021, 17, 562–573. [Google Scholar] [CrossRef]
- Han, X.-T.; Jiang, J.-Q.; Li, M.-Z.; Cong, Q.-M. Circular RNA circ-ABCB10 promotes the proliferation and invasion of thyroid cancer by targeting KLF6. Eur. Rev. Med. Pharmacol. Sci. 2020, 24, 1271–1277. [Google Scholar]
- Pan, Y.; Xu, T.; Liu, Y.; Li, W.; Zhang, W. Upregulated circular RNA circ_0025033 promotes papillary thyroid cancer cell proliferation and invasion via sponging miR-1231 and miR-1304. Biochem. Biophys. Res. Commun. 2019, 510, 334–338. [Google Scholar] [CrossRef]
- Yang, Y.; Ding, L.; Li, Y.; Xuan, C. Hsa_circ_0039411 promotes tumorigenesis and progression of papillary thyroid cancer by miR-1179/ABCA9 and miR-1205/MTA1 signaling pathways. J. Cell. Physiol. 2020, 235, 1321–1329. [Google Scholar] [CrossRef]
- Zheng, Q.; Bao, C.; Guo, W.; Li, S.; Chen, J.; Chen, B.; Luo, Y.; Lyu, D.; Li, Y.; Shi, G.; et al. Circular RNA profiling reveals an abundant circHIPK3 that regulates cell growth by sponging multiple miRNAs. Nat. Commun. 2016, 7, 11215. [Google Scholar] [CrossRef]
- Liu, C.-X.; Li, X.; Nan, F.; Jiang, S.; Gao, X.; Guo, S.-K.; Xue, W.; Cui, Y.; Dong, K.; Ding, H.; et al. Structure and Degradation of Circular RNAs Regulate PKR Activation in Innate Immunity. Cell 2019, 177, 865–880.e21. [Google Scholar] [CrossRef] [PubMed]
- Li, Z.; Huang, C.; Bao, C.; Chen, L.; Lin, M.; Wang, X.; Zhong, G.; Yu, B.; Hu, W.; Dai, L.; et al. Exon-intron circular RNAs regulate transcription in the nucleus. Nat. Struct. Mol. Biol. 2015, 22, 256–264, Erratum in Nat. Struct. Mol. Biol. 2017, 24, 194. [Google Scholar] [CrossRef] [PubMed]
- Meng, S.; Zhou, H.; Feng, Z.; Xu, Z.; Tang, Y.; Li, P.; Wu, M. CircRNA: Functions and properties of a novel potential biomarker for cancer. Mol. Cancer 2017, 16, 1–8. [Google Scholar] [CrossRef] [PubMed]
- Armakola, M.; Higgins, M.J.; Figley, M.D.; Barmada, S.J.; Scarborough, E.A.; Diaz, Z.; Fang, X.; Shorter, J.; Krogan, N.J.; Finkbeiner, S.; et al. Inhibition of RNA lariat debranching enzyme suppresses TDP-43 toxicity in ALS disease models. Nat. Genet. 2012, 44, 1302–1309. [Google Scholar] [CrossRef]
- Du, W.W.; Yang, W.; Liu, E.; Yang, Z.; Dhaliwal, P.; Yang, B.B. Foxo3 circular RNA retards cell cycle progression via forming ternary complexes with p21 and CDK2. Nucleic Acids Res. 2016, 44, 2846–2858. [Google Scholar] [CrossRef]
- Amicone, L.; Marchetti, A.; Cicchini, C. Exosome-Associated circRNAs as Key Regulators of EMT in Cancer. Cells 2022, 11, 1716. [Google Scholar] [CrossRef]
- Dai, X.; Chen, C.; Yang, Q.; Xue, J.; Chen, X.; Sun, B.; Luo, F.; Liu, X.; Xiao, T.; Xu, H.; et al. Exosomal circRNA_100284 from arsenite-transformed cells, via microRNA-217 regulation of EZH2, is involved in the malignant transformation of human hepatic cells by accelerating the cell cycle and promoting cell proliferation. Cell Death Dis. 2018, 9, 1–14. [Google Scholar] [CrossRef]
- Chen, N.; Zhao, G.; Yan, X.; Lv, Z.; Yin, H.; Zhang, S.; Song, W.; Li, X.; Li, L.; Du, Z.; et al. A novel FLI1 exonic circular RNA promotes metastasis in breast cancer by coordinately regulating TET1 and DNMT1. Genome Biol. 2018, 19, 1–14. [Google Scholar] [CrossRef]
- Zhao, X.; Cai, Y.; Xu, J. Circular RNAs: Biogenesis, Mechanism, and Function in Human Cancers. Int. J. Mol. Sci. 2019, 20, 3926. [Google Scholar] [CrossRef]
- Bolisetty, M.T.; Graveley, B.R. Circuitous Route to Transcription Regulation. Mol. Cell 2013, 51, 705–706. [Google Scholar] [CrossRef]
- Gao, X.; Ma, X.-K.; Li, X.; Li, G.-W.; Liu, C.-X.; Zhang, J.; Wang, Y.; Wei, J.; Chen, J.; Chen, L.-L.; et al. Knockout of circRNAs by base editing back-splice sites of circularized exons. Genome Biol. 2022, 23, 1–22. [Google Scholar] [CrossRef]
- Liu, J.; Li, H.; Wei, C.; Ding, J.; Lu, J.; Pan, G.; Mao, A. circFAT1(e2) Promotes Papillary Thyroid Cancer Proliferation, Migration, and Invasion via the miRNA-873/ZEB1 Axis. Comput. Math. Methods Med. 2020, 2020, 1–9. [Google Scholar] [CrossRef]
- Luo, Q.; Guo, F.; Fu, Q.; Sui, G. hsa_circ_0001018 promotes papillary thyroid cancer by facilitating cell survival, invasion, G1/S cell cycle progression, and repressing cell apoptosis via crosstalk with miR-338-3p and SOX4. Mol. Ther.-Nucleic Acids 2021, 24, 591–609. [Google Scholar] [CrossRef]
- Zhang, W.; Zhang, H.; Zhao, X. circ_0005273 promotes thyroid carcinoma progression by SOX2 expression. Endocr.-Relat. Cancer 2020, 27, 11–21. [Google Scholar] [CrossRef]
- Li, C.; Zhu, L.; Fu, L.; Han, M.; Li, Y.; Meng, Z.; Qiu, X. CircRNA NRIP1 promotes papillary thyroid carcinoma progression by sponging mir-195-5p and modulating the P38 MAPK and JAK/STAT pathways. Diagn. Pathol. 2021, 16, 1–11. [Google Scholar] [CrossRef]
- Liu, Y.; Chen, G.; Wang, B.; Wu, H.; Zhang, Y.; Ye, H. Silencing circRNA protein kinase C iota (circ-PRKCI) suppresses cell progression and glycolysis of human papillary thyroid cancer through circ-PRKCI/miR-335/E2F3 ceRNA axis. Endocr. J. 2021, 68, 713–727. [Google Scholar] [CrossRef]
- Fabian, M.R.; Sonenberg, N.; Filipowicz, W. Regulation of mRNA Translation and Stability by microRNAs. Annu. Rev. Biochem. 2010, 79, 351–379. [Google Scholar] [CrossRef]
- Salmena, L.; Poliseno, L.; Tay, Y.; Kats, L.; Pandolfi, P.P. A ceRNA hypothesis: The Rosetta Stone of a hidden RNA language? Cell 2011, 146, 353–358. [Google Scholar] [CrossRef]
- Shifman, B.M.; Platonova, N.M.; Vasilyev, E.V.; Abdulkhabirova, F.M.; Kachko, V.A. Circular RNAs and thyroid cancer: Closed molecules, open possibilities. Crit. Rev. Oncol. 2022, 173, 103662. [Google Scholar] [CrossRef]
- Bai, Q.; Pan, Z.; Nabi, G.; Rashid, F.; Liu, Y.; Khan, S. Emerging role of competing endogenous RNA and associated noncoding RNAs in thyroid cancer. Am. J. Cancer Res. 2022, 12, 961–973. [Google Scholar]
- Wang, M.; Chen, B.; Ru, Z.; Cong, L. CircRNA circ-ITCH suppresses papillary thyroid cancer progression through miR-22-3p/CBL/β-catenin pathway. Biochem. Biophys. Res. Commun. 2018, 504, 283–288. [Google Scholar] [CrossRef]
- Li, S.; Yang, J.; Liu, X.; Guo, R.; Zhang, R. circITGA7 Functions as an Oncogene by Sponging miR-198 and Upregulating FGFR1 Expression in Thyroid Cancer. BioMed Res. Int. 2020, 2020, 1–8. [Google Scholar] [CrossRef]
- Chen, F.; Feng, Z.; Zhu, J.; Liu, P.; Yang, C.; Huang, R.; Deng, Z. Emerging roles of circRNA_NEK6 targeting miR-370-3p in the proliferation and invasion of thyroid cancer via Wnt signaling pathway. Cancer Biol. Ther. 2018, 19, 1139–1152. [Google Scholar] [CrossRef]
- Abe, N.; Matsumoto, K.; Nishihara, M.; Nakano, Y.; Shibata, A.; Maruyama, H.; Shuto, S.; Matsuda, A.; Yoshida, M.; Ito, Y.; et al. Rolling Circle Translation of Circular RNA in Living Human Cells. Sci. Rep. 2015, 5, 16435. [Google Scholar] [CrossRef]
- Chen, C.-Y.; Sarnow, P. Initiation of Protein Synthesis by the Eukaryotic Translational Apparatus on Circular RNAs. Science 1995, 268, 415–417. [Google Scholar] [CrossRef]
- Zhang, M.; Huang, N.; Yang, X.; Luo, J.; Yan, S.; Xiao, F.; Chen, W.; Gao, X.; Zhao, K.; Zhou, H.; et al. A novel protein encoded by the circular form of the SHPRH gene suppresses glioma tumorigenesis. Oncogene 2018, 37, 1805–1814. [Google Scholar] [CrossRef]
- Peng, L.; Yuan, X.Q.; Li, G.C. The emerging landscape of circular RNA ciRS-7 in cancer (Review). Oncol. Rep. 2015, 33, 2669–2674. [Google Scholar] [CrossRef]
- Han, J.Y.; Guo, S.; Wei, N.; Xue, R.; Li, W.; Dong, G.; Li, J.; Tian, X.; Chen, C.; Qiu, S.; et al. ciRS-7 Promotes the Proliferation and Migration of Papillary Thyroid Cancer by Negatively Regulating the miR-7/Epidermal Growth Factor Receptor Axis. Biomed. Res. Int. 2020, 2020, 9875636. [Google Scholar] [CrossRef]
- Abdelmohsen, K.; Panda, A.C.; Munk, R.; Grammatikakis, I.; Dudekula, D.B.; De, S.; Kim, J.; Noh, J.H.; Kim, K.M.; Martindale, J.L.; et al. Identification of HuR target circular RNAs uncovers suppression of PABPN1 translation by CircPABPN1. RNA Biol. 2017, 14, 361–369. [Google Scholar] [CrossRef]
- Ghosal, S.; Das, S.; Sen, R.; Basak, P.; Chakrabarti, J. Circ2Traits: A comprehensive database for circular RNA potentially associated with disease and traits. Front. Genet. 2013, 4, 283. [Google Scholar] [CrossRef]
- Dudekula, D.B.; Panda, A.C.; Grammatikakis, I.; De, S.; Abdelmohsen, K.; Gorospe, M. CircInteractome: A web tool for exploring circular RNAs and their interacting proteins and microRNAs. RNA Biol. 2016, 13, 34–42. [Google Scholar] [CrossRef] [PubMed]
- Liu, Y.-C.; Li, J.-R.; Sun, C.-H.; Andrews, E.; Chao, R.-F.; Lin, F.-M.; Weng, S.-L.; Hsu, S.-D.; Huang, C.-C.; Cheng, C.; et al. CircNet: A database of circular RNAs derived from transcriptome sequencing data. Nucleic Acids Res. 2015, 44, D209–D215. [Google Scholar] [CrossRef] [PubMed]
- Chen, X.; Han, P.; Zhou, T.; Guo, X.; Song, X.; Li, Y. circRNADb: A comprehensive database for human circular RNAs with protein-coding annotations. Sci. Rep. 2016, 6, 34985. [Google Scholar] [CrossRef] [PubMed]
- Xia, S.; Feng, J.; Chen, K.; Ma, Y.; Gong, J.; Cai, F.; Jin, Y.; Gao, Y.; Xia, L.; Chang, H.; et al. CSCD: A database for cancer-specific circular RNAs. Nucleic Acids Res. 2017, 46, D925–D929. [Google Scholar] [CrossRef]
- Xia, S.; Feng, J.; Lei, L.; Hu, J.; Xia, L.; Wang, J.; Xiang, Y.; Liu, L.; Zhong, S.; Han, L.; et al. Comprehensive characterization of tissue-specific circular RNAs in the human and mouse genomes. Brief. Bioinform. 2016, 18, 984–992. [Google Scholar] [CrossRef]
- Dong, R.; Ma, X.K.; Li, G.W.; Yang, L. CIRCpedia v2: An Updated Database for Comprehensive Circular RNA Annotation and Expression Comparison. Genom. Proteom. Bioinform. 2018, 16, 226–233. [Google Scholar] [CrossRef]
- Yao, D.; Zhang, L.; Zheng, M.; Sun, X.; Lu, Y.; Liu, P. Circ2Disease: A manually curated database of experimentally validated circRNAs in human disease. Sci. Rep. 2018, 8, 1–6. [Google Scholar] [CrossRef]
- Zhao, Z.; Wang, K.; Wu, F.; Wang, W.; Zhang, K.; Hu, H.; Liu, Y.; Jiang, T. circRNA disease: A manually curated database of experimentally supported circRNA-disease associations. Cell Death Dis. 2018, 9, 1–2. [Google Scholar] [CrossRef]
- Meng, X.; Hu, D.; Zhang, P.; Chen, Q.; Chen, M. CircFunBase: A database for functional circular RNAs. Database 2019, 2019, baz003. [Google Scholar] [CrossRef]
- Li, J.H.; Liu, S.; Zhou, H.; Qu, L.H.; Yang, J.H. starBase v2.0: Decoding miRNA-ceRNA, miRNA-ncRNA and protein-RNA interaction networks from large-scale CLIP-Seq data. Nucleic Acids Res. 2014, 42, D92–D97. [Google Scholar] [CrossRef]
- Gokool, A.; Anwar, F.; Voineagu, I. The Landscape of Circular RNA Expression in the Human Brain. Biol. Psychiatry 2020, 87, 294–304. [Google Scholar] [CrossRef]
- Liu, M.; Wang, Q.; Shen, J.; Yang, B.B.; Ding, X. Circbank: A comprehensive database for circRNA with standard nomenclature. RNA Biol. 2019, 16, 899–905. [Google Scholar] [CrossRef]
- Meng, X.; Chen, Q.; Zhang, P.; Chen, M. CircPro: An integrated tool for the identification of circRNAs with protein-coding potential. Bioinformatics 2017, 33, 3314–3316. [Google Scholar] [CrossRef]
- Cardenas, J.; Balaji, U.; Gu, J. Cerina: Systematic circRNA functional annotation based on integrative analysis of ceRNA interactions. Sci. Rep. 2020, 10, 1–14. [Google Scholar] [CrossRef]
- Wu, W.; Ji, P.; Zhao, F. CircAtlas: An integrated resource of one million highly accurate circular RNAs from 1070 vertebrate transcriptomes. Genome Biol. 2020, 21, 1–14. [Google Scholar] [CrossRef]
- Zheng, L.-L.; Ling-Ling, Z.; Wu, J.; Sun, W.-J.; Liu, S.; Wang, Z.-L.; Zhou, H.; Yang, J.-H.; Qu, L.-H. deepBase v2.0: Identification, expression, evolution and function of small RNAs, LncRNAs and circular RNAs from deep-sequencing data. Nucleic Acids Res. 2015, 44, D196–D202. [Google Scholar] [CrossRef]
- Rophina, M.; Sharma, D.; Poojary, M.; Scaria, V. Circad: A comprehensive manually curated resource of circular RNA associated with diseases. Database 2020, 2020, baaa019. [Google Scholar] [CrossRef]
- Lan, W.; Zhu, M.; Chen, Q.; Chen, B.; Liu, J.; Li, M.; Chen, Y.-P.P. CircR2Cancer: A manually curated database of associations between circRNAs and cancers. Database 2020, 2020, baaa085. [Google Scholar] [CrossRef]
- Li, S.; Li, Y.; Chen, B.; Zhao, J.; Yu, S.; Tang, Y.; Zheng, Q.; Li, Y.; Wang, P.; He, X.; et al. exoRBase: A database of circRNA, lncRNA and mRNA in human blood exosomes. Nucleic Acids Res. 2017, 46, D106–D112. [Google Scholar] [CrossRef]
- Vo, J.N.; Cieslik, M.; Zhang, Y.; Shukla, S.; Xiao, L.; Zhang, Y.; Wu, Y.-M.; Dhanasekaran, S.M.; Engelke, C.G.; Cao, X.; et al. The Landscape of Circular RNA in Cancer. Cell 2019, 176, 869–881.e13. [Google Scholar] [CrossRef]
- Xin, R.; Gao, Y.; Wang, R.; Kadash-Edmondson, K.E.; Liu, B.; Wang, Y.; Lin, L.; Xing, Y. isoCirc catalogs full-length circular RNA isoforms in human transcriptomes. Nat. Commun. 2021, 12, 1–11. [Google Scholar] [CrossRef]
- Wu, J.; Li, Y.; Wang, C.; Cui, Y.; Xu, T.; Wang, C.; Wang, X.; Sha, J.; Jiang, B.; Wang, K.; et al. CircAST: Full-length Assembly and Quantification of Alternatively Spliced Isoforms in Circular RNAs. Genom. Proteom. Bioinform. 2019, 17, 522–534. [Google Scholar] [CrossRef]
- Ruan, H.; Xiang, Y.; Ko, J.; Li, S.; Jing, Y.; Zhu, X.; Han, L. Comprehensive characterization of circular RNAs in ~1000 human cancer cell lines. Genome Med. 2019. 11, 55. [CrossRef]
- Tang, Z.; Li, X.; Zhao, J.; Qian, F.; Feng, C.; Li, Y.; Zhang, J.; Jiang, Y.; Yang, Y.; Wang, Q.; et al. TRCirc: A resource for transcriptional regulation information of circRNAs. Brief. Bioinform. 2018, 20, 2327–2333. [Google Scholar] [CrossRef]
- Wang, P.; Li, X.; Gao, Y.; Guo, Q.; Wang, Y.; Fang, Y.; Ma, X.; Zhi, H.; Zhou, D.; Shen, W.; et al. LncACTdb 2.0: An updated database of experimentally supported ceRNA interactions curated from low- and high-throughput experiments. Nucleic Acids Res. 2018, 47, D121–D127. [Google Scholar] [CrossRef]
- Zhang, W.; Yao, G.; Wang, J.; Yang, M.; Wang, J.; Zhang, H.; Li, W. ncRPheno: A comprehensive database platform for identification and validation of disease related noncoding RNAs. RNA Biol. 2020, 17, 943–955. [Google Scholar] [CrossRef]
- Teng, X.; Chen, X.; Xue, H.; Tang, Y.; Zhang, P.; Kang, Q.; Hao, Y.; Chen, R.; Zhao, Y.; He, S. NPInter v4.0: An integrated database of ncRNA interactions. Nucleic Acids Res. 2019, 48, D160–D165. [Google Scholar] [CrossRef]
- Toraih, E.A.; Sedhom, J.A.; Haidari, M.; Fawzy, M.S. Applications of noncoding RNAs in renal cancer patients. In Clinical Applications of Non-Coding RNAs in Cancer; Elsevier: Amsterdam, The Netherlands, 2022; pp. 211–284. [Google Scholar] [CrossRef]
- Li, Z.; Huang, X.; Liu, A.; Xu, J.; Lai, J.; Guan, H.; Ma, J. Circ_PSD3 promotes the progression of papillary thyroid carcinoma via the miR-637/HEMGN axis. Life Sci. 2021, 264, 118622. [Google Scholar] [CrossRef]
- Yao, Y.; Chen, X.; Yang, H.; Chen, W.; Qian, Y.; Yan, Z.; Liao, T.; Yao, W.; Wu, W.; Yu, T.; et al. Hsa_circ_0058124 promotes papillary thyroid cancer tumorigenesis and invasiveness through the NOTCH3/GATAD2A axis. J. Exp. Clin. Cancer Res. 2019, 38, 318. [Google Scholar] [CrossRef]
- Zhou, G.-K.; Zhang, G.-Y.; Yuan, Z.-N.; Pei, R.; Liu, D.-M. Has_circ_0008274 promotes cell proliferation and invasion involving AMPK/mTOR signaling pathway in papillary thyroid carcinoma. Eur. Rev. Med. Pharmacol. Sci. 2018, 22, 8772–8780. [Google Scholar]
- Ma, J.; Kan, Z. Circular RNA circ_0008274 enhances the malignant progression of papillary thyroid carcinoma via modulating solute carrier family 7 member 11 by sponging miR-154-3p. Endocr. J. 2021, 68, 543–552. [Google Scholar] [CrossRef] [PubMed]
- Zhang, H.; Ma, X.-P.; Li, X.; Deng, F.-S. Circular RNA circ_0067934 exhaustion expedites cell apoptosis and represses cell proliferation, migration and invasion in thyroid cancer via sponging miR-1304 and regulating CXCR1 expression. Eur. Rev. Med. Pharmacol. Sci. 2019, 23, 10851–10866. [Google Scholar] [PubMed]
- Lan, X.; Cao, J.; Xu, J.; Chen, C.; Zheng, C.; Wang, J.; Zhu, X.; Zhu, X.; Ge, M. Decreased expression of hsa_circ_0137287 predicts aggressive clinicopathologic characteristics in papillary thyroid carcinoma. J. Clin. Lab. Anal. 2018, 32, e22573. [Google Scholar] [CrossRef] [PubMed]
- Yu, W.; Ma, B.; Zhao, W.; Liu, J.; Yu, H.; Tian, Z.; Fan, Z.; Han, H. The combination of circRNA-UMAD1 and Galectin-3 in peripheral circulation is a co-biomarker for predicting lymph node metastasis of thyroid carcinoma. Am. J. Transl. Res. 2020, 12, 5399–5415. [Google Scholar] [PubMed]
- Jin, X.; Wang, Z.; Pang, W.; Zhou, J.; Liang, Y.; Yang, J.; Yang, L.; Zhang, Q. Upregulated hsa_circ_0004458 Contributes to Progression of Papillary Thyroid Carcinoma by Inhibition of miR-885-5p and Activation of RAC1. Med. Sci. Monit. 2018, 24, 5488–5500. [Google Scholar] [CrossRef] [PubMed]
- Wang, Y.; Zong, H.; Zhou, H. Circular RNA circ_0062389 modulates papillary thyroid carcinoma progression via the miR-1179/high mobility group box 1 axis. Bioengineered 2021, 12, 1484–1494. [Google Scholar] [CrossRef] [PubMed]
- Qi, Y.; He, J.; Zhang, Y.; Wang, L.; Yu, Y.; Yao, B.; Tian, Z. Circular RNA hsa_circ_0001666 sponges miR-330-5p, miR-193a-5p and miR-326, and promotes papillary thyroid carcinoma progression via upregulation of ETV4. Oncol. Rep. 2021, 45, 1–12. [Google Scholar] [CrossRef]
- Liu, F.; Zhang, J.; Qin, L.; Yang, Z.; Xiong, J.; Zhang, Y.; Li, R.; Li, S.; Wang, H.; Yu, B.; et al. Circular RNA EIF6 (Hsa_circ_0060060) sponges miR-144-3p to promote the cisplatin-resistance of human thyroid carcinoma cells by autophagy regulation. Aging 2018, 10, 3806–3820. [Google Scholar] [CrossRef]
- Rong, D.; Sun, H.; Li, Z.; Liu, S.; Dong, C.; Fu, K.; Tang, W.; Cao, H. An emerging function of circRNA-miRNAs-mRNA axis in human diseases. Oncotarget 2017, 8, 73271–73281. [Google Scholar] [CrossRef]
- Wang, H.; Yan, X.; Zhang, H.; Zhan, X. CircRNA circ_0067934 Overexpression Correlates with Poor Prognosis and Promotes Thyroid Carcinoma Progression. Med. Sci. Monit. 2019, 25, 1342–1349. [Google Scholar] [CrossRef]
- Liao, J.-Y.; Wu, J.; Wang, Y.-J.; He, J.-H.; Deng, W.-X.; Hu, K.; Zhang, Y.-C.; Zhang, Y.; Yan, H.; Wang, D.-L.; et al. Deep sequencing reveals a global reprogramming of lncRNA transcriptome during EMT. Biochim. Biophys. Acta Mol. Cell Res. 2017, 1864, 1703–1713. [Google Scholar] [CrossRef]
- Li, Z.; Xu, J.; Guan, H.; Lai, J.; Yang, X.; Ma, J. Circ_0059354 aggravates the progression of papillary thyroid carcinoma by elevating ARFGEF1 through sponging miR-766-3p. J. Endocrinol. Investig. 2021, 45, 825–836. [Google Scholar] [CrossRef]
- Cai, Z.; Li, H. Circular RNAs and Bladder Cancer. OncoTargets Ther. 2020, 13, 9573–9586. [Google Scholar] [CrossRef]
- Zeng, Y.; Xu, Y.; Shu, R.; Sun, L.; Tian, Y.; Shi, C.; Zheng, Z.; Wang, K.; Luo, H. Altered expression profiles of circular RNA in colorectal cancer tissues from patients with lung metastasis. Int. J. Mol. Med. 2017, 40, 1818–1828. [Google Scholar] [CrossRef]
- Schweppe, R.E.; Klopper, J.P.; Korch, C.; Pugazhenthi, U.; Benezra, M.; Knauf, J.A.; Fagin, J.A.; Marlow, L.A.; Copland, J.A.; Smallridge, R.C.; et al. Deoxyribonucleic Acid Profiling Analysis of 40 Human Thyroid Cancer Cell Lines Reveals Cross-Contamination Resulting in Cell Line Redundancy and Misidentification. J. Clin. Endocrinol. Metab. 2008, 93, 4331–4341. [Google Scholar] [CrossRef]
- Fan, Y.X.; Shi, H.Y.; Hu, Y.L.; Jin, X.L. Circ_0000144 facilitates the progression of thyroid cancer via the miR-217/AKT3 pathway. J. Gene Med. 2020, 22, e3269. [Google Scholar] [CrossRef]
- Landa, I.; Pozdeyev, N.; Korch, C.; Marlow, L.A.; Smallridge, R.C.; Copland, J.A.; Henderson, Y.C.; Lai, S.Y.; Clayman, G.L.; Onoda, N.; et al. Comprehensive Genetic Characterization of Human Thyroid Cancer Cell Lines: A Validated Panel for Preclinical Studies. Clin. Cancer Res. 2019, 25, 3141–3151. [Google Scholar] [CrossRef]
- Fogh, J. Human Tumor Lines for Cancer Research. Cancer Investig. 1986, 4, 157–184. [Google Scholar] [CrossRef]
- Peng, N.; Shi, L.; Zhang, Q.; Hu, Y.; Wang, N.; Ye, H. Microarray profiling of circular RNAs in human papillary thyroid carcinoma. PLoS ONE 2017, 12, e0170287. [Google Scholar] [CrossRef]
- Liu, L.; Yan, C.; Tao, S.; Wang, H. Circ_0058124 Aggravates the Progression of Papillary Thyroid Carcinoma by Activating LMO4 Expression via Targeting miR-370-3p. Cancer Manag. Res. 2020, 12, 9459–9470. [Google Scholar] [CrossRef]
- Gui, X.; Li, Y.; Zhang, X.; Su, K.; Cao, W. Circ_LDLR promoted the development of papillary thyroid carcinoma via regulating miR-195-5p/LIPH axis. Cancer Cell Int. 2020, 20, 1–14. [Google Scholar] [CrossRef]
- Tan, X.; Zhao, J.; Lou, J.; Zheng, W.; Wang, P. Hsa_circ_0058129 regulates papillary thyroid cancer development via miR-873-5p/follistatin-like 1 axis. J. Clin. Lab. Anal. 2022, 36, e24401. [Google Scholar] [CrossRef]
- Cui, W.; Xue, J. Circular RNA DOCK1 downregulates microRNA -124 to induce the growth of human thyroid cancer cell lines. BioFactors 2020, 46, 591–599. [Google Scholar] [CrossRef]
- Xue, C.; Cheng, Y.; Wu, J.; Ke, K.; Miao, C.; Chen, E.; Zhang, L. Circular RNA CircPRMT5 Accelerates Proliferation and Invasion of Papillary Thyroid Cancer Through Regulation of miR-30c/E2F3 Axis. Cancer Manag. Res. 2020, 12, 3285–3291. [Google Scholar] [CrossRef]
- Ye, M.; Hou, H.; Shen, M.; Dong, S.; Zhang, T. Circular RNA circFOXM1 Plays a Role in Papillary Thyroid Carcinoma by Sponging miR-1179 and Regulating HMGB1 Expression. Mol. Ther.-Nucleic Acids 2019, 19, 741–750. [Google Scholar] [CrossRef]
- Xia, F.; Chen, Y.; Jiang, B.; Bai, N.; Li, X. Hsa_circ_0011385 accelerates the progression of thyroid cancer by targeting miR-361-3p. Cancer Cell Int. 2020, 20, 1–14. [Google Scholar] [CrossRef]
- Liu, W.; Zhao, J.; Jin, M.; Zhou, M. circRAPGEF5 Contributes to Papillary Thyroid Proliferation and Metastatis by Regulation miR-198/FGFR1. Mol. Ther. Nucleic Acids 2019, 14, 609–616. [Google Scholar] [CrossRef]
- Zheng, F.-B.; Chen, D.; Ding, Y.-Y.; Wang, S.-R.; Shi, D.-D.; Zhu, Z.-P. Circular RNA circ_0103552 promotes the invasion and migration of thyroid carcinoma cells by sponging miR-127. Eur. Rev. Med. Pharmacol. Sci. 2020, 24, 2572–2578. [Google Scholar]
- Guo, M.; Sun, Y.; Ding, J.; Li, Y.; Yang, S.; Zhao, Y.; Jin, X.; Li, S.-S. Circular RNA profiling reveals a potential role of hsa_circ_IPCEF1 in papillary thyroid carcinoma. Mol. Med. Rep. 2021, 24, 1–15. [Google Scholar] [CrossRef]
- Xiong, H.; Yu, J.; Jia, G.; Su, Y.; Zhang, J.; Xu, Q.; Sun, X. Emerging roles of circUBAP2 targeting miR-370-3p in proliferation, apoptosis, and invasion of papillary thyroid cancer cells. Hum. Cell 2021, 34, 1866–1877. [Google Scholar] [CrossRef] [PubMed]
- Zeng, L.; Yuan, S.; Zhou, P.; Gong, J.; Kong, X.; Wu, M. Circular RNA Pvt1 oncogene (CircPVT1) promotes the progression of papillary thyroid carcinoma by activating the Wnt/β-catenin signaling pathway and modulating the ratio of microRNA-195 (miR-195) to vascular endothelial growth factor A (VEGFA) expression. Bioengineered 2021, 12, 11795–11810. [Google Scholar] [CrossRef] [PubMed]
- Li, Y.; Qin, J.; He, Z.; Cui, G.; Zhang, K.; Wu, B. Knockdown of circPUM1 impedes cell growth, metastasis and glycolysis of papillary thyroid cancer via enhancing MAPK1 expression by serving as the sponge of miR-21-5p. Genes Genom. 2021, 43, 141–150. [Google Scholar] [CrossRef] [PubMed]
- Zheng, H.; Fu, Q.; Ma, K.; Shi, S.; Fu, Y. Circ_0079558 promotes papillary thyroid cancer progression by binding to miR-26b-5p to activate MET/AKT signaling. Endocr. J. 2021, 68, 1247–1266. [Google Scholar] [CrossRef]
- Mao, Y.; Huo, Y.; Li, J.; Zhao, Y.; Wang, Y.; Sun, L.; Kang, Z. circRPS28 (hsa_circ_0049055) is a novel contributor for papillary thyroid carcinoma by regulating cell growth and motility via functioning as ceRNA for miR-345-5p to regulate frizzled family receptor 8 (FZD8). Endocr. J. 2021, 68, 1267–1281. [Google Scholar] [CrossRef]
- Dong, L.-P.; Chen, L.-Y.; Bai, B.; Qi, X.-F.; Liu, J.-N.; Qin, S. circ_0067934 promotes the progression of papillary thyroid carcinoma cells through miR-1301-3p/HMGB1 axis. Neoplasma 2022, 69, 1–15. [Google Scholar] [CrossRef]
- Shu, T.; Yang, L.; Sun, L.; Lu, J.; Zhan, X. CircHIPK3 Promotes Thyroid Cancer Tumorigenesis and Invasion through the Mirna-338-3p/RAB23 Axis. Med. Princ. Pr. 2020, 30, 412–420. [Google Scholar] [CrossRef]
- Ding, W.; Shi, Y.; Zhang, H. Circular RNA circNEURL4 inhibits cell proliferation and invasion of papillary thyroid carcinoma by sponging miR-1278 and regulating LATS1 expression. Am. J. Transl. Res. 2021, 13, 5911–5927. [Google Scholar]
- Zhang, D.; Tao, L.; Xu, N.; Lu, X.; Wang, J.; He, G.; Chu, J. CircRNA circTIAM1 promotes papillary thyroid cancer progression through the miR-646/HNRNPA1 signaling pathway. Cell Death Discov. 2022, 8, 21. [Google Scholar] [CrossRef]
- Wang, T.; Huang, Y. Downregulation of hsa_circ_0001681 suppresses epithelial-mesenchymal transition in thyroid carcinoma via targeting to miR-942-5p/TWIST1 signaling pathway. J. Bioenerg. Biomembr. 2021, 53, 609–620. [Google Scholar] [CrossRef]
- Keller, S.; Sanderson, M.P.; Stoeck, A.; Altevogt, P. Exosomes: From biogenesis and secretion to biological function. Immunol. Lett. 2006, 107, 102–108. [Google Scholar] [CrossRef]
- Tuo, B.; Chen, Z.; Dang, Q.; Chen, C.; Zhang, H.; Hu, S.; Sun, Z. Roles of exosomal circRNAs in tumour immunity and cancer progression. Cell Death Dis. 2022, 13, 1–9. [Google Scholar] [CrossRef]
- Lin, Q.; Qi, Q.; Hou, S.; Chen, Z.; Jiang, N.; Zhang, L.; Lin, C. Exosomal circular RNA hsa_circ_007293 promotes proliferation, migration, invasion, and epithelial-mesenchymal transition of papillary thyroid carcinoma cells through regulation of the microRNA-653-5p/paired box 6 axis. Bioengineered 2021, 12, 10136–10149. [Google Scholar] [CrossRef]
- Liu, Y.; Xia, L.; Dong, L.; Wang, J.; Xiao, Q.; Yu, X.; Zhu, H. CircHIPK3 Promotes Gemcitabine (GEM) Resistance in Pancreatic Cancer Cells by Sponging miR-330-5p and Targets RASSF1. Cancer Manag. Res. 2020, 12, 921–929. [Google Scholar] [CrossRef]
- Yuan, W.; Zhou, R.; Wang, J.; Han, J.; Yang, X.; Yu, H.; Lu, H.; Zhang, X.; Li, P.; Tao, J.; et al. Circular RNA Cdr1as sensitizes bladder cancer to cisplatin by upregulating APAF1 expression through miR-1270 inhibition. Mol. Oncol. 2019, 13, 1559–1576. [Google Scholar] [CrossRef]
- Sang, Y.; Chen, B.; Song, X.; Li, Y.; Liang, Y.; Han, D.; Zhang, N.; Zhang, H.; Liu, Y.; Chen, T.; et al. circRNA_0025202 Regulates Tamoxifen Sensitivity and Tumor Progression via Regulating the miR-182-5p/FOXO3a Axis in Breast Cancer. Mol. Ther. 2019, 27, 1638–1652. [Google Scholar] [CrossRef]
- Suzuki, H.; Zuo, Y.; Wang, J.; Zhang, M.Q.; Malhotra, A.; Mayeda, A. Characterization of RNase R-digested cellular RNA source that consists of lariat and circular RNAs from pre-mRNA splicing. Nucleic Acids Res. 2006, 34, e63. [Google Scholar] [CrossRef]
- Panda, A.; De, S.; Grammatikakis, I.; Munk, R.; Yang, X.; Piao, Y.; Dudekula, D.B.; Abdelmohsen, K.; Gorospe, M. High-purity circular RNA isolation method (RPAD) reveals vast collection of intronic circRNAs. Nucleic Acids Res. 2017, 45, e116. [Google Scholar] [CrossRef]
- Conn, V.; Conn, S.J. SplintQuant: A method for accurately quantifying circular RNA transcript abundance without reverse transcription bias. RNA 2019, 25, 1202–1210. [Google Scholar] [CrossRef]
- Hansen, T.B. Improved circRNA Identification by Combining Prediction Algorithms. Front. Cell Dev. Biol. 2018, 6, 20. [Google Scholar] [CrossRef]



Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Toraih, E.A.; Hussein, M.H.; Fawzy, M.S.; Kandil, E. A Review and In Silico Analysis of Tissue and Exosomal Circular RNAs: Opportunities and Challenges in Thyroid Cancer. Cancers 2022, 14, 4728. https://doi.org/10.3390/cancers14194728
Toraih EA, Hussein MH, Fawzy MS, Kandil E. A Review and In Silico Analysis of Tissue and Exosomal Circular RNAs: Opportunities and Challenges in Thyroid Cancer. Cancers. 2022; 14(19):4728. https://doi.org/10.3390/cancers14194728
Chicago/Turabian StyleToraih, Eman A., Mohammad H. Hussein, Manal S. Fawzy, and Emad Kandil. 2022. "A Review and In Silico Analysis of Tissue and Exosomal Circular RNAs: Opportunities and Challenges in Thyroid Cancer" Cancers 14, no. 19: 4728. https://doi.org/10.3390/cancers14194728
APA StyleToraih, E. A., Hussein, M. H., Fawzy, M. S., & Kandil, E. (2022). A Review and In Silico Analysis of Tissue and Exosomal Circular RNAs: Opportunities and Challenges in Thyroid Cancer. Cancers, 14(19), 4728. https://doi.org/10.3390/cancers14194728