Type and Gene Location of KIT Mutations Predict Progression-Free Survival to First-Line Imatinib in Gastrointestinal Stromal Tumors: A Look into the Exon
Abstract
Simple Summary
Abstract
1. Introduction
2. Results
2.1. Pathogenic Variant Classification of GIST Patients
2.2. Metastatic GIST Patients
2.2.1. Clinicopathological Characteristics According to Critical Mutations
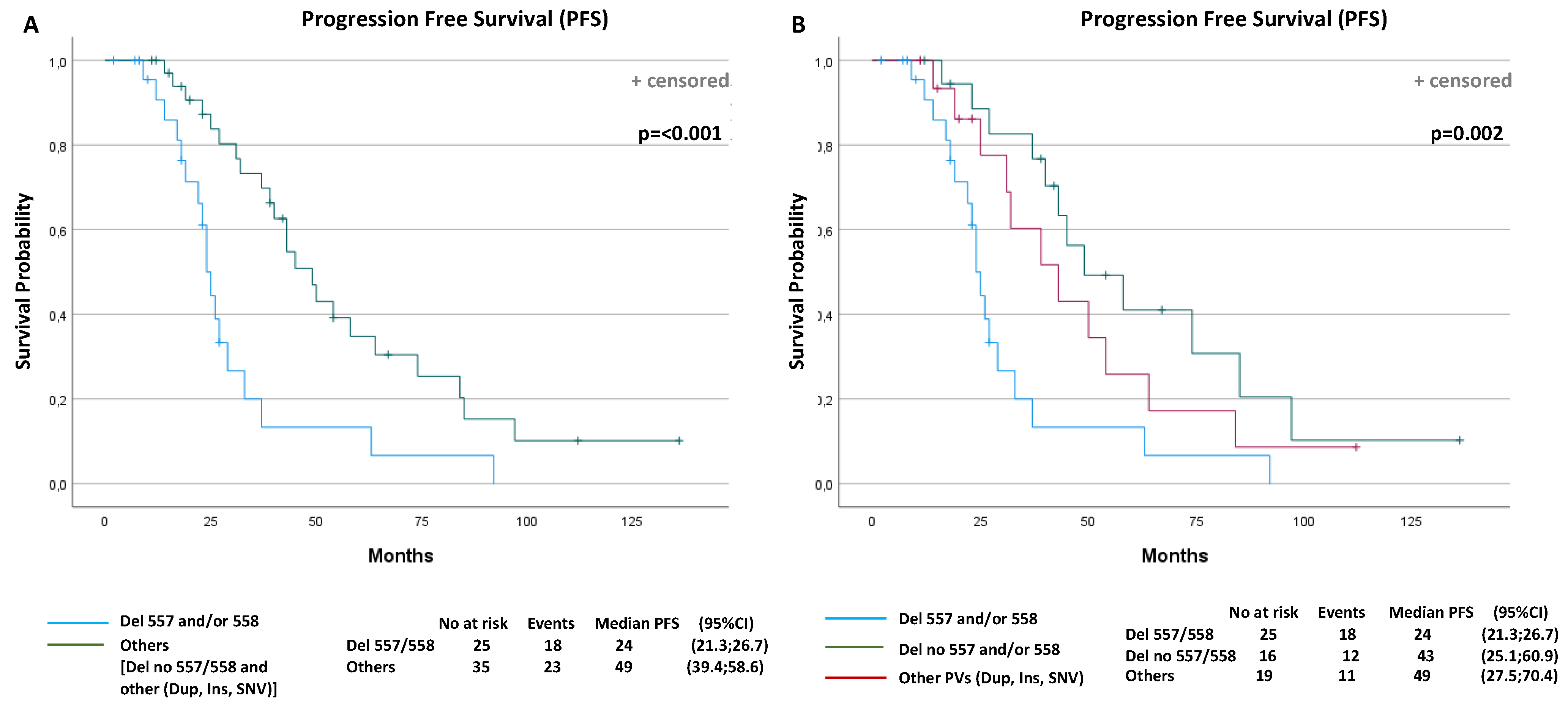
2.2.2. Outcome Analysis and Objective Response in KIT Exon 11 Metastatic Patients
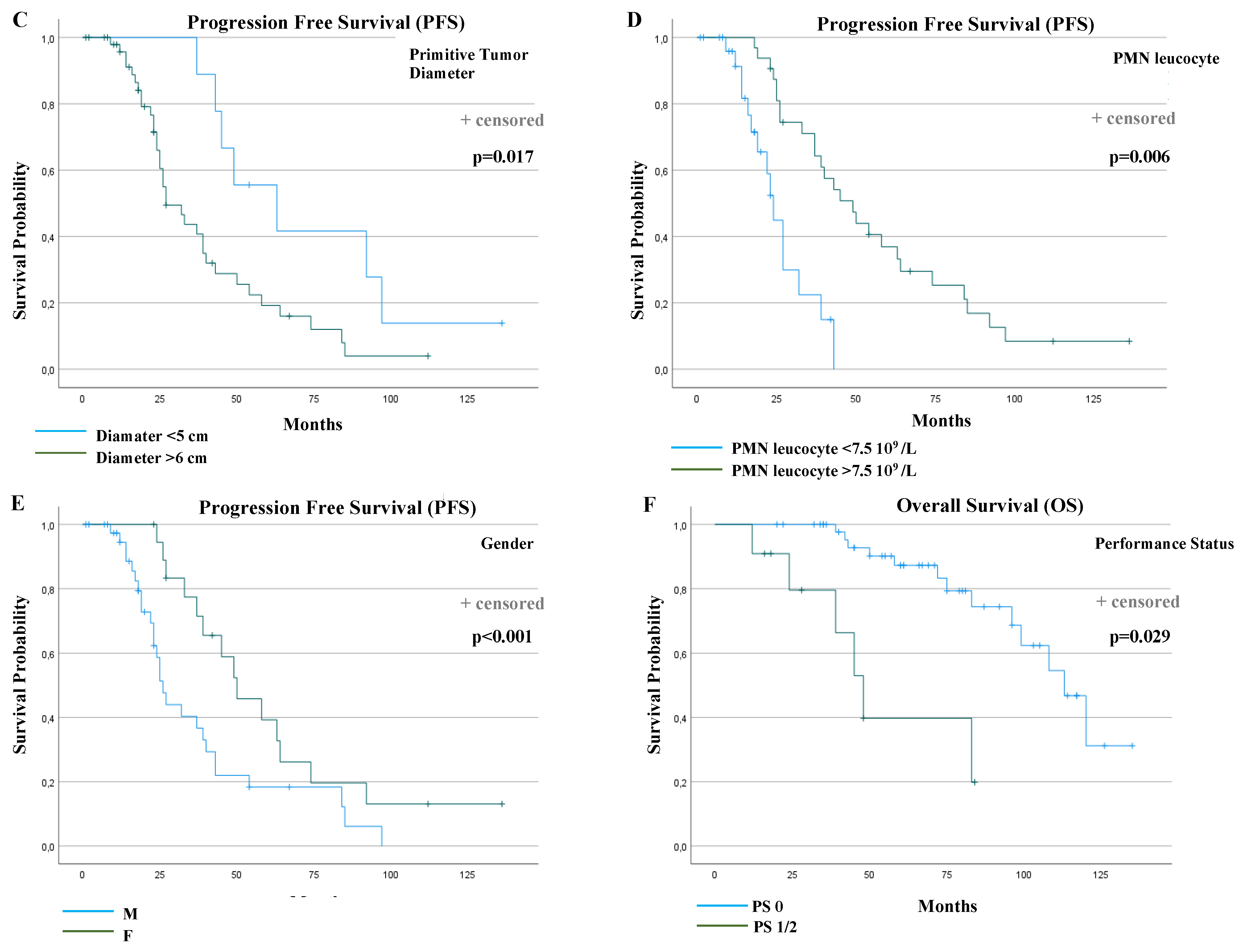
2.2.3. Univariate and Multivariate Analysis
3. Discussion
4. Patients and Methods
4.1. Study Population
4.2. Mutation Analysis
4.3. Statistical Analysis
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Corless, C.L.; Barnett, C.M.; Heinrich, M.C. Gastrointestinal stromal tumours: Origin and molecular oncology. Nat. Rev. Cancer 2011, 11, 865–878. [Google Scholar] [CrossRef]
- Pantuso, G.; Macaione, I.; Taverna, A.; Guercio, G.; Incorvaia, L.; Di Piazza, M.; Di Grado, F.; Cilluffo, G.; Badalamenti, G.; Cipolla, C. Surgical treatment of primary gastrointestinal stromal tumors (GISTs): Management and prognostic role of R1 resections. Am. J. Surg. 2020, 220, 359–364. [Google Scholar] [CrossRef]
- Hirota, S.; Isozaki, K.; Moriyama, Y.; Hashimoto, K.; Nishida, T.; Ishiguro, S.; Kawano, K.; Hanada, M.; Kurata, A.; Takeda, M.; et al. Gain-of-function mutations of c-kit in human gastrointestinal stromal tumors. Science 1998, 279, 577–580. [Google Scholar] [CrossRef] [PubMed]
- Heinrich, M.C.; Corless, C.L.; Duensing, A.; McGreevey, L.; Chen, C.J.; Joseph, N.; Singer, S.; Griffith, D.J.; Haley, A.; Town, A.; et al. PDGFRA activating mutations in gastrointestinal stromal tumors. Science 2003, 299, 708–710. [Google Scholar] [CrossRef] [PubMed]
- Corless, C.L.; Schroeder, A.; Griffith, D.; Town, A.; McGreevey, L.; Harrell, P.; Shiraga, S.; Bainbridge, T.; Morich, J.; Heinrich, M.C. PDGFRA Mutations in Gastrointestinal Stromal Tumors: Frequency, Spectrum and In Vitro Sensitivity to Imatinib. J. Clin. Oncol. 2005, 23, 5357–5364. [Google Scholar] [CrossRef] [PubMed]
- Wu, C.-E.; Tzen, C.-Y.; Wang, S.-Y.; Yeh, C.-N. Clinical Diagnosis of Gastrointestinal Stromal Tumor (GIST): From the Molecular Genetic Point of View. Cancers 2019, 11, 679. [Google Scholar] [CrossRef]
- Boikos, S.A.; Pappo, A.S.; Killian, J.K.; LaQuaglia, M.P.; Weldon, C.B.; George, S.; Trent, J.C.; Von Mehren, M.; Wright, J.A.; Schiffman, J.D.; et al. Molecular Subtypes of KIT/PDGFRA Wild-Type Gastrointestinal Stromal Tumors: A Report From the National Institutes of Health Gastrointestinal Stromal Tumor Clinic. JAMA Oncol. 2016, 2, 922–928. [Google Scholar] [CrossRef]
- Vanden Bempt, I.; Vander Borght, S.; Sciot, R.; Spans, L.; Claerhout, S.; Brems, H.; Lehnert, S.; Dehaspe, L.; Fransis, S.; Neuville, B.; et al. Comprehensive targeted NGS approach in the molecular diagnosis of GIST. Genes Chromosomes Cancer 2020, 60, 239–249. [Google Scholar] [CrossRef]
- Miettinen, M.; Killian, J.K.; Wang, Z.-F.; Lasota, J.; Lau, C.; Jones, L.; Walker, R.; Pineda, M.; Zhu, Y.J.; Kim, S.Y.; et al. Immunohistochemical Loss of Succinate Dehydrogenase Subunit A (SDHA) in Gastrointestinal Stromal Tumors (GISTs) Signals SDHA Germline Mutation. Am. J. Surg. Pathol. 2013, 37, 234–240. [Google Scholar] [CrossRef]
- Cocco, E.; Scaltriti, M.; Drilon, A. NTRK fusion-positive cancers and TRK inhibitor therapy. Nat. Rev. Clin. Oncol. 2018, 15, 731–747. [Google Scholar] [CrossRef]
- Li, F.; Huynh, H.; Li, X.; Ruddy, D.A.; Wang, Y.; Ong, R.; Chow, P.; Qiu, S.; Tam, A.; Rakiec, D.P.; et al. FGFR-Mediated Reactivation of MAPK Signaling Attenuates Antitumor Effects of Imatinib in Gastrointestinal Stromal Tumors. Cancer Discov. 2015, 5, 438–451. [Google Scholar] [CrossRef]
- Heinrich, M.C.; Corless, C.L.; Demetri, G.D.; Blanke, C.D.; Von Mehren, M.; Joensuu, H.; McGreevey, L.S.; Chen, C.-J.; Abbeele, A.D.V.D.; Druker, B.J.; et al. Kinase Mutations and Imatinib Response in Patients With Metastatic Gastrointestinal Stromal Tumor. J. Clin. Oncol. 2003, 21, 4342–4349. [Google Scholar] [CrossRef]
- Debiec-Rychter, M.; Sciot, R.; Le Cesne, A.; Schlemmer, M.; Hohenberger, P.; van Oosterom, A.T.; Blay, J.-Y.; Leyvraz, S.; Stul, M.; Casali, P.G.; et al. KIT mutations and dose selection for imatinib in patients with advanced gastrointestinal stromal tumours. Eur. J. Cancer 2006, 42, 1093–1103. [Google Scholar] [CrossRef]
- Serrano, C.; George, S. Gastrointestinal Stromal Tumor: Challenges and Opportunities for a New Decade. Clin. Cancer Res. 2020, 26, 5078–5085. [Google Scholar] [CrossRef]
- Vincenzi, B.; Nannini, M.; Badalamenti, G.; Grignani, G.; Fumagalli, E.; Gasperoni, S.; D’Ambrosio, L.; Incorvaia, L.; Stellato, M.; Ceruso, M.S.; et al. Imatinib rechallenge in patients with advanced gastrointestinal stromal tumors following progression with imatinib, sunitinib and regorafenib. Ther. Adv. Med Oncol. 2018, 10. [Google Scholar] [CrossRef]
- Casali, P.G.; Zalcberg, J.; Le Cesne, A.; Reichardt, P.; Blay, J.-Y.; Lindner, L.H.; Judson, I.R.; Schöffski, P.; Leyvraz, S.; Italiano, A.; et al. Ten-Year Progression-Free and Overall Survival in Patients With Unresectable or Metastatic GI Stromal Tumors: Long-Term Analysis of the European Organisation for Research and Treatment of Cancer, Italian Sarcoma Group, and Australasian Gastrointestinal Trials Group Intergroup Phase III Randomized Trial on Imatinib at Two Dose Levels. J. Clin. Oncol. 2017, 35, 1713–1720. [Google Scholar] [CrossRef]
- Nannini, M.; Nigro, M.C.; Vincenzi, B.; Fumagalli, E.; Grignani, G.; D’Ambrosio, L.; Badalamenti, G.; Incorvaia, L.; Bracci, R.; Gasperoni, S.; et al. Personalization of regorafenib treatment in metastatic gastrointestinal stromal tumours in real-life clinical practice. Ther. Adv. Med Oncol. 2017, 9, 731–739. [Google Scholar] [CrossRef] [PubMed]
- Joensuu, H.; Wardelmann, E.; Sihto, H.; Eriksson, M.; Hall, K.S.; Reichardt, A.; Hartmann, J.T.; Pink, D.; Cameron, S.; Hohenberger, P.; et al. Effect of KIT and PDGFRA Mutations on Survival in Patients with Gastrointestinal Stromal Tumors Treated With Adjuvant Imatinib: An Exploratory Analysis of a Randomized Clinical Trial. JAMA Oncol. 2017, 3, 602–609. [Google Scholar] [CrossRef] [PubMed]
- Wozniak, A.; Rutkowski, P.; Schöffski, P.; Ray-Coquard, I.; Hostein, I.; Schildhaus, H.-U.; Le Cesne, A.; Bylina, E.; Limon, J.; Blay, J.-Y.; et al. Tumor Genotype Is an Independent Prognostic Factor in Primary Gastrointestinal Stromal Tumors of Gastric Origin: A European Multicenter Analysis Based on ConticaGIST. Clin. Cancer Res. 2014, 20, 6105–6116. [Google Scholar] [CrossRef] [PubMed]
- Martin-Broto, J.; Gutierrez, A.; Garcia-Del-Muro, X.; Lopez-Guerrero, J.; Martinez-Trufero, J.; De Sande, L.; Lainez, N.; Maurel, J.; De Juan, A.; Losa, F.; et al. Prognostic time dependence of deletions affecting codons 557 and/or 558 of KIT gene for relapse-free survival (RFS) in localized GIST: A Spanish Group for Sarcoma Research (GEIS) Study. Ann. Oncol. 2010, 21, 1552–1557. [Google Scholar] [CrossRef]
- Patrikidou, A.; Domont, J.; Chabaud, S.; Ray-Coquard, I.; Coindre, J.-M.; Bui-Nguyen, B.; Adenis, A.; Rios, M.; Bertucci, F.; Duffaud, F.; et al. Long-term outcome of molecular subgroups of GIST patients treated with standard-dose imatinib in the BFR14 trial of the French Sarcoma Group. Eur. J. Cancer 2016, 52, 173–180. [Google Scholar] [CrossRef]
- Lasota, J.; Dobosz, A.J.V.; Wasag, B.; Woźniak, A.; Kraszewska, E.; Michej, W.; Ptaszynski, K.; Rutkowski, P.; Sarlomo-Rikala, M.; Steigen, S.E.; et al. Presence of homozygous KIT exon 11 mutations is strongly associated with malignant clinical behavior in gastrointestinal stromal tumors. Lab. Investig. 2007, 87, 1029–1041. [Google Scholar] [CrossRef] [PubMed]
- Bachet, J.B.; Hostein, I.; Le Cesne, A.; Brahimi, S.; Beauchet, A.; Tabone-Eglinger, S.; Subra, F.; Bui, B.; Duffaud, F.; Terrier, P.; et al. Prognosis and predictive value of KIT exon 11 deletion in GISTs. Br. J. Cancer 2009, 101, 7–11. [Google Scholar] [CrossRef] [PubMed]
- Reichardt, P.; Demetri, G.D.; Gelderblom, H.; Rutkowski, P.; Im, S.-A.; Gupta, S.; Kang, Y.-K.; Schöffski, P.; Schuette, J.; Soulières, D.; et al. Correlation of KIT and PDGFRA mutational status with clinical benefit in patients with gastrointestinal stromal tumor treated with sunitinib in a worldwide treatment-use trial. BMC Cancer 2016, 16. [Google Scholar] [CrossRef]
- Badalamenti, G.; Rodolico, V.; Fulfaro, F.; Cascio, S.; Cipolla, C.; Cicero, G.; Incorvaia, L.; Sanfilippo, M.; Intrivici, C.; Sandonato, L.; et al. Gastrointestinal stromal tumors (GISTs): Focus on histopathological diagnosis and biomolecular features. Ann. Oncol. 2007, 18, vi136–vi140. [Google Scholar] [CrossRef]
- Casali, P.; Abecassis, N.; Bauer, S.; Biagini, R.; Bielack, S.; Bonvalot, S.; Boukovinas, I.; Bovee, J.; Brodowicz, T.; Broto, J.; et al. Gastrointestinal stromal tumours: ESMO–EURACAN Clinical Practice Guidelines for diagnosis, treatment and follow-up. Ann. Oncol. 2018, 29, iv68–iv78. [Google Scholar] [CrossRef]
- Agaram, N.P.; Besmer, P.; Wong, G.C.; Guo, T.; Socci, N.D.; Maki, R.G.; DeSantis, D.; Brennan, M.F.; Singer, S.; DeMatteo, R.P.; et al. Pathologic and Molecular Heterogeneity in Imatinib-Stable or Imatinib-Responsive Gastrointestinal Stromal Tumors. Clin. Cancer Res. 2007, 13, 170–181. [Google Scholar] [CrossRef]
- Kim, T.S.; Cavnar, M.J.; Cohen, N.A.; Sorenson, E.C.; Greer, J.B.; Seifert, A.M.; Crawley, M.H.; Green, B.L.; Popow, R.; Pillarsetty, N.; et al. Increased KIT Inhibition Enhances Therapeutic Efficacy in Gastrointestinal Stromal Tumor. Clin. Cancer Res. 2014, 20, 2350–2362. [Google Scholar] [CrossRef] [PubMed]
- Liegl, B.; Kepten, I.; Le, C.; Zhu, M.; Demetri, G.D.; Heinrich, M.C.; Fletcher, C.D.M.; Corless, C.L.; Fletcher, J.A. Heterogeneity of kinase inhibitor resistance mechanisms in GIST. J. Pathol. 2008, 216, 64–74. [Google Scholar] [CrossRef] [PubMed]
- Gastrointestinal Stromal Tumor Meta-Analysis Group (MetaGIST). Comparison of two doses of imatinib for the treatment of unresectable or metastatic gastrointestinal stromal tumors: A meta-analysis of 1640 patients. J. Clin. Oncol. 2010, 28, 1247–1253. [Google Scholar] [CrossRef]
- Antonescu, C.R.; Besmer, P.; Guo, T.; Arkun, K.; Hom, G.; Koryotowski, B.; Leversha, M.A.; Jeffrey, P.D.; DeSantis, D.; Singer, S.; et al. Acquired Resistance to Imatinib in Gastrointestinal Stromal Tumor Occurs Through Secondary Gene Mutation. Clin. Cancer Res. 2005, 11, 4182–4190. [Google Scholar] [CrossRef]
- Szucs, Z.; Thway, K.; Fisher, C.; Bulusu, R.; Constantinidou, A.; Benson, C.; Van Der Graaf, W.T.A.; Jones, R.L. Molecular subtypes of gastrointestinal stromal tumors and their prognostic and therapeutic implications. Future Oncol. 2017, 13, 93–107. [Google Scholar] [CrossRef] [PubMed]
- Bauer, S.; Duensing, A.; Demetri, G.D.; Fletcher, J.A. KIT oncogenic signaling mechanisms in imatinib-resistant gastrointestinal stromal tumor: PI3-kinase/AKT is a crucial survival pathway. Oncogene 2007, 26, 7560–7568. [Google Scholar] [CrossRef]
- Ma, Y.; Cunningham, M.E.; Wang, X.; Ghosh, I.; Regan, L.; Longley, B.J. Inhibition of Spontaneous Receptor Phosphorylation by Residues in a Putative α-Helix in the KIT Intracellular Juxtamembrane Region. J. Biol. Chem. 1999, 274, 13399–13402. [Google Scholar] [CrossRef] [PubMed]
- Judson, I.; Ma, P.; Peng, B.; Verweij, J.; Racine, A.; Di Paola, E.D.; Van Glabbeke, M.; Dimitrijevic, S.; Scurr, M.; Dumez, H.; et al. Imatinib pharmacokinetics in patients with gastrointestinal stromal tumour: A retrospective population pharmacokinetic study over time. EORTC Soft Tissue and Bone Sarcoma Group. Cancer Chemother. Pharmacol. 2004, 55, 379–386. [Google Scholar] [CrossRef] [PubMed]
- Ramaswamy, A.; Bal, M.; Swami, R.; Shetty, O.; Bose, S.; Pai, T.; Gurav, M.; Gupta, S.; Ostwal, V. Early outcomes of exon 11 mutants in GIST treated with standard dose Imatinib. Ann. Transl. Med. 2017, 5, 134. [Google Scholar] [CrossRef]
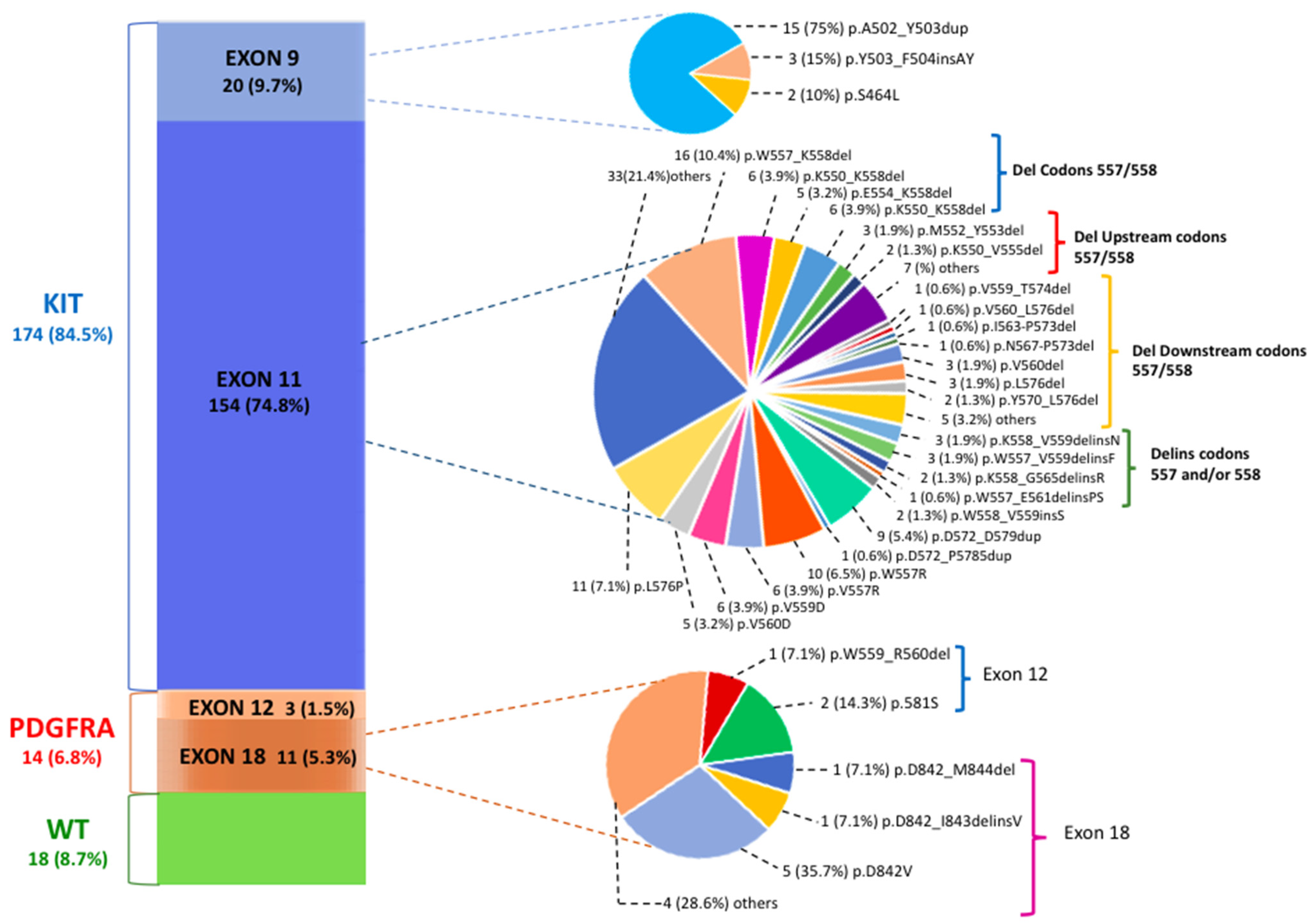

| Gene | Exon | Mutation Type | Number of Patients (%) | Pathogenic Variant | N. | |
|---|---|---|---|---|---|---|
| KIT n. 174 (84.5%) | Exon 9 20 (9.7%) | Duplication | 15 (7.3%) | p.A502_Y503dup | 15 | |
| Insertion | 3 (1.5%) | p.Y503_F504insAY | 3 | |||
| SNV | 2 (1%) | p.S464L | 2 | |||
| Exon 11 154 (74.8%) | Deletion | 95 (46.1%) | Codons 557–558 60 (29.1%) | p.W557_K558del | 16 | |
| p.K550_K558del | 6 | |||||
| p.E554_K558del | 5 | |||||
| Others * | 33 | |||||
| Upstream codon 557 18 (8.7%) | p.K550_E554del | 6 | ||||
| p.M552_Y553del | 3 | |||||
| p.K550_V555del | 2 | |||||
| Others * | 7 | |||||
| Downstream codon 558 17 (8.2%) | Involving codons 568–570: p.V559_T574del p.V560_L576del p.I563-P573del p.N567_P573del | 1 1 1 1 | ||||
| Other codons: p.V560del p.L576del p.Y570_L576del Others | 3 3 2 5 | |||||
| Deletion/Insertion | 9 (4.4%) | p.K558_V559delinsN | 3 | |||
| p.W557_V559delinsF | 3 | |||||
| p.K558_G565delinsR | 2 | |||||
| p.W557_E561delinsPS | 1 | |||||
| Insertion | 2 (1%) | p.K558_V559insS | 2 | |||
| Duplication | 10 (4.8%) | p.D572_D579dup | 9 | |||
| p.D572_P585dup | 1 | |||||
| SNV | 38 (18.4%) | p.W557R | 10 | |||
| p.V559D | 6 | |||||
| p.V560D | 6 | |||||
| p.L576P | 5 | |||||
| Others | 11 | |||||
| PDGFRA n. 14 (6.8%) | Exon 12 3 (1.5%) | Deletion | 1 (0.5%) | p.W559_R560del | 1 | |
| SNV | 2 (1%) | p.P581S | 2 | |||
| Exon 18 11 (5.3%) | Deletion | 1 (0.5%) | p.D842_M844del | 1 | ||
| Deletion/Insertion | 1 (0.5%) | p.D842_I843delinsV | 1 | |||
| SNV | 5 (1.9%) | p.D842V | 5 | |||
| Others | 4 (1.9%) | 4 | ||||
| KIT/PDGFRA Wild Type n. 18 (8.7%) | - | - | - | - | ||
| Characteristic | N. of Patients (%) | KIT | PDGFRA | KIT/ PDGFRA WT | ||||
|---|---|---|---|---|---|---|---|---|
| Exon 11 * | Exon 9 | Exons 12, 14, 18 | - | |||||
| Del/ Delins Codons 557/558 | Others 1 | p.A502_Y503dup | Others 2 | no-D842V | D842V | - | ||
| N. of patients (%) | 80 | 25 (31.3) | 35 (43.7) | 8 (10) | 2 (2.5) | 5 (6.2) | 2 (2.5) | 3 (3.8) |
| Sex | ||||||||
| Male Female | 50 (62.5) 30 (37.5) | 16 (64) 9 (36) | 25 (71.4) 10 (28.6) | 3 (37.5) 5 (62.5) | 2 (100) 0 (0) | 2 (40) 3 (60) | 1 (50) 1 (50) | 1 (33.3) 2 (66.7) |
| Age at diagnosis (y): | ||||||||
| Median Range | 57 30–81 | 57 45–74 | 57 31–81 | 59 49–77 | 37 30–44 | 50 36–59 | 57.5 36–79 | 50 50–58 |
| Site of origin | ||||||||
| Gastric Small bowel Other GI | 27 (33.8) 34 (42.5) 19 (23.7) | 15 (60) 7 (28) 3 (12) | 8 (22.8) 18 (51.5) 9 (25.7) | 0 (0) 5 (62.5) 3 (37.5) | 0 (0) 1 (50) 1 (50) | 1 (20) 2 (40) 2 (40) | 1 (50) 1 (50) 0 (0) | 2 (66.7) 0 (0) 1 (33.3) |
| Primitive tumor diameter | ||||||||
| ≤5 cm >5 cm | 14 (17.5) 66 (82.5) | 2 (8) 23 (92) | 8 (22.8) 27 (77.2) | 2 (25) 6 (75) | 0 (0) 2 (100) | 2 (40) 3 (60) | 0 (0) 2 (100) | 0 (0) 3 (100) |
| Mitosis | ||||||||
| ≤5/50 HPF >5/50 HPF | 25 (31.3) 55 (68.7) | 6 (24) 19 (76) | 13 (37.2) 22 (62.8) | 2 (25) 6 (75) | 0 (0) 2 (100) | 3 (60) 2 (40) | 1 (50) 1 (50) | 0 (0) 3 (100) |
| Site of metastases | ||||||||
| Liver Peritoneum Liver and peritoneum | 31 (38.7) 31 (38.7) 18 (22.6) | 10 (40) 11 (44) 4 (16) | 15 (42.9) 13 (37.1) 7 (20) | 2 (25) 4 (50) 2 (25) | 0 (0) 2 (100) 0 (0) | 2 (40) 1 (20) 2 (40) | 0 (0) 0 (0) 2 (100) | 2 (66.7) 0 (0) 1 (33.3) |
| PFS | Univariate Cox Regression | Multivariable Cox Regression | ||
|---|---|---|---|---|
| HR (95%CI) | p-Value | HR (95%CI) | p-Value | |
| Gender (F vs. M) | 0.46 (0.24–0.89) | 0.022 | 0.23 (0.09–0.53) | <0.001 |
| Performance status (PS) (1/2 vs. 0) | 3.64 (1.47–9.03) | 0.005 | 3.13 (0.89–10.98) | 0.073 |
| Primitive tumor diameter (≤5 cm vs. >5 cm) | 2.62 (1.13–6.07) | 0.025 | 3.39 (1.25–9.22) | 0.017 |
| Mitosis (≤5/50 HPF vs. >5/50 HPF) | 1.14 (0.59–2.21) | NS | ||
| Gastric site of origin (No vs. yes) | 1.27 (0.58–2.81) | NS | ||
| Liver and peritoneal involvement (No vs. yes) | 0.83 (0.32–2.14) | NS | ||
| Lymphopenia (≤1 vs. <1 G/L) | 2.11 (1.01–4.42) | 0.046 | 1.05 (0.35–3.19) | 0.92 |
| Polymorphonuclear leucocyte (>7.5 × 109 vs. ≤7.5 × 109/L) | 0.24 (0.11–0.51) | <0.001 | 0.27 (0.10–0.68) | 0.006 |
| Exon 11 Del or Delins 557 and/or 558 (No vs. yes) | 0.36 (0.19–0.69) | 0.002 | 0.12 (0.04–0.31) | <0.001 |
| OS | Univariate Cox Regression | Multivariable Cox Regression | ||
| HR (95%CI) | p-value | HR (95%CI) | p-value | |
| Gender (F vs. M) | 1.19 (0.48–2.98) | NS | ||
| Performance status (PS) (1/2 vs. 0) | 6.35 (2.17–18.58) | <0.001 | 3.97 (1.15–13.68) | 0.029 |
| Primitive Tumor diameter (≤5 cm vs. >5 cm) | 2.17 (0.60–7.73) | NS | ||
| Mitosis (≤5/50 HPF vs. >5/50 HPF) | 1.39 (0.50–3.83) | NS | ||
| Gastric site of origin (No vs. yes) | 0.40 (0.13–1.21) | NS | ||
| Liver and peritoneal involvement (No vs. yes) | 2.38 (0.63–9.07) | NS | ||
| Lymphopenia (≤1 vs. <1 G/L) | 3.54 (1.35–9.27) | 0.01 | 2.16 (0.71–6.55) | NS |
| Polymorphonuclear leucocyte (>7.5 × 109 vs. ≤7.5 × 109/L) | 0.38 (0.15–9.81) | 0.04 | 0.76 (0.25–2.38) | NS |
| Exon 11 Del or Delins 557 and/or 558 (No vs. yes) | 0.49 (0.20–1.24) | NS | ||
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Incorvaia, L.; Fanale, D.; Vincenzi, B.; De Luca, I.; Bartolotta, T.V.; Cannella, R.; Pantuso, G.; Cabibi, D.; Russo, A.; Bazan, V.; et al. Type and Gene Location of KIT Mutations Predict Progression-Free Survival to First-Line Imatinib in Gastrointestinal Stromal Tumors: A Look into the Exon. Cancers 2021, 13, 993. https://doi.org/10.3390/cancers13050993
Incorvaia L, Fanale D, Vincenzi B, De Luca I, Bartolotta TV, Cannella R, Pantuso G, Cabibi D, Russo A, Bazan V, et al. Type and Gene Location of KIT Mutations Predict Progression-Free Survival to First-Line Imatinib in Gastrointestinal Stromal Tumors: A Look into the Exon. Cancers. 2021; 13(5):993. https://doi.org/10.3390/cancers13050993
Chicago/Turabian StyleIncorvaia, Lorena, Daniele Fanale, Bruno Vincenzi, Ida De Luca, Tommaso Vincenzo Bartolotta, Roberto Cannella, Gianni Pantuso, Daniela Cabibi, Antonio Russo, Viviana Bazan, and et al. 2021. "Type and Gene Location of KIT Mutations Predict Progression-Free Survival to First-Line Imatinib in Gastrointestinal Stromal Tumors: A Look into the Exon" Cancers 13, no. 5: 993. https://doi.org/10.3390/cancers13050993
APA StyleIncorvaia, L., Fanale, D., Vincenzi, B., De Luca, I., Bartolotta, T. V., Cannella, R., Pantuso, G., Cabibi, D., Russo, A., Bazan, V., & Badalamenti, G. (2021). Type and Gene Location of KIT Mutations Predict Progression-Free Survival to First-Line Imatinib in Gastrointestinal Stromal Tumors: A Look into the Exon. Cancers, 13(5), 993. https://doi.org/10.3390/cancers13050993








