External Validation of an MRI-Derived Radiomics Model to Predict Biochemical Recurrence after Surgery for High-Risk Prostate Cancer
Abstract
1. Introduction
2. Methods
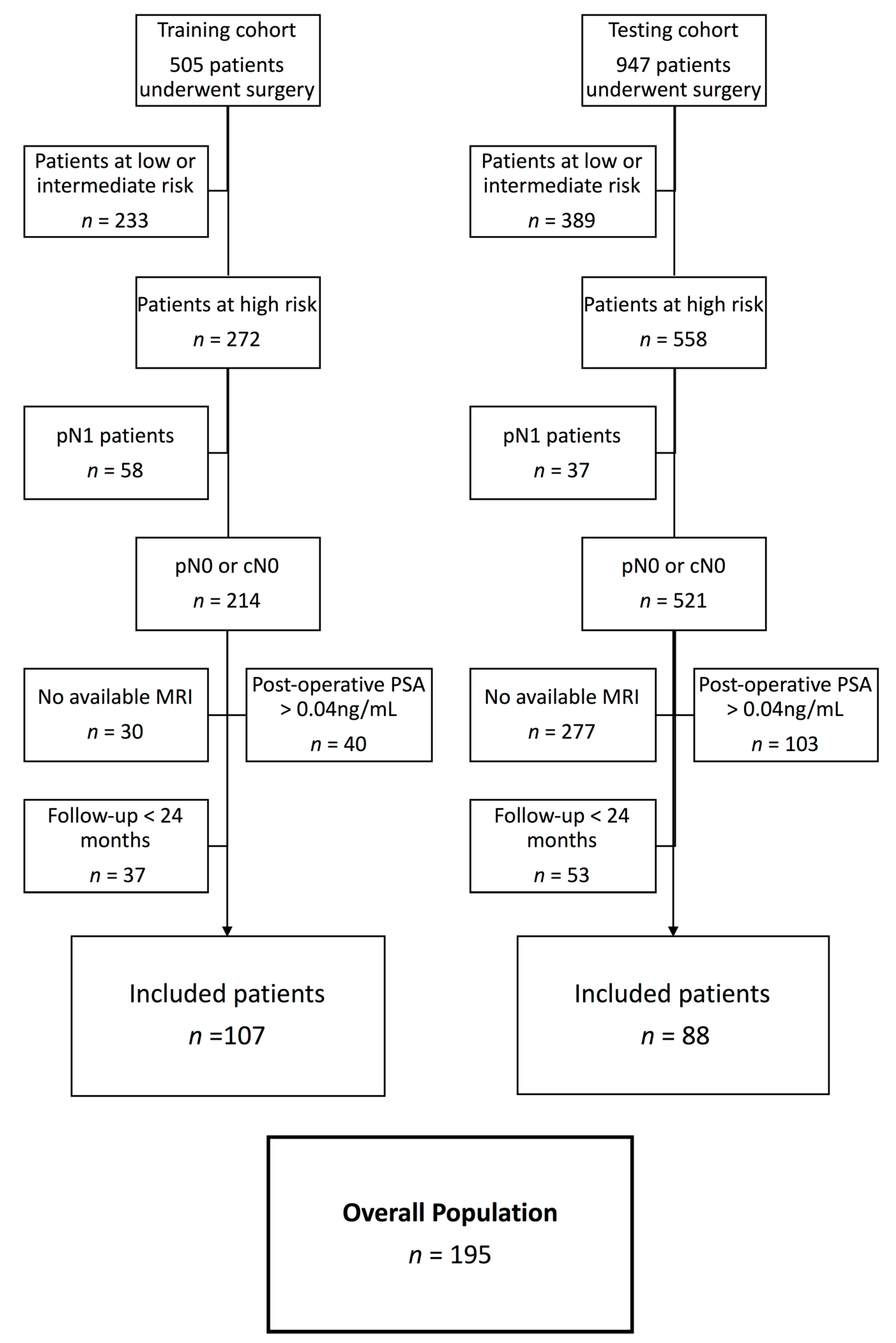
2.1. Selection of Patients
2.2. Endpoints
2.3. Surgery
2.4. MRI
2.5. Clinical Features
2.6. Tumor Delineation
2.7. Radiomics Features
2.8. Statistical Analysis
2.9. Harmonization Method
2.10. Inter-Reader Variability
3. Results
3.1. Patient Characteristics
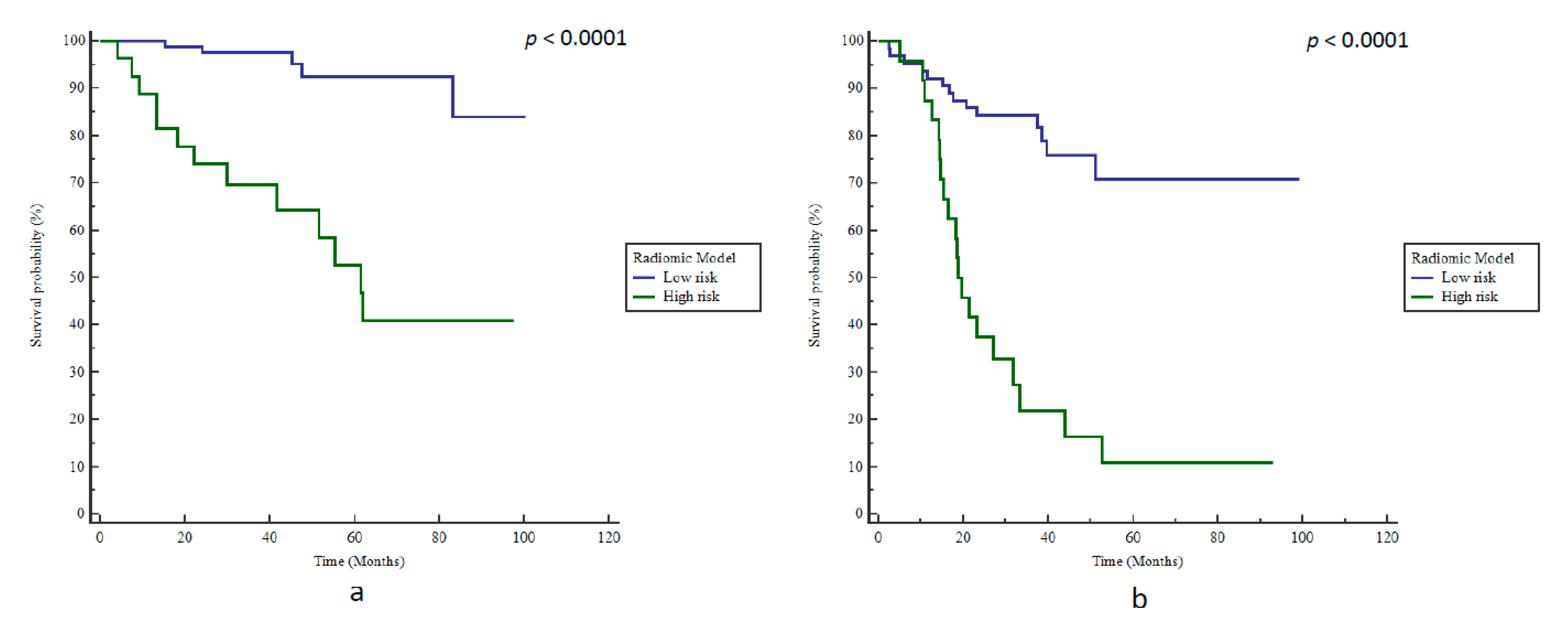
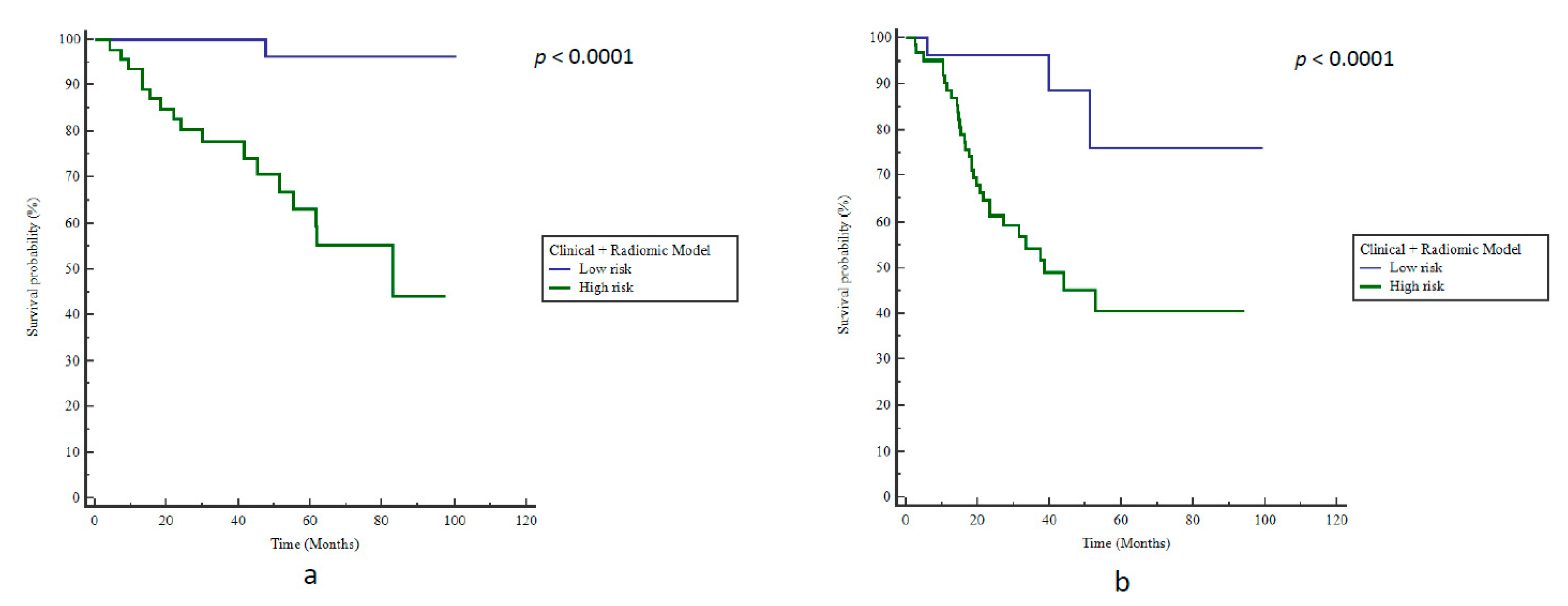
3.2. Outcome
3.3. Model Retraining
3.4. Model Evaluation in the Testing Cohort
3.5. ComBat Harmonization
3.6. Inter-Reader Variability
3.7. Radiomics Quality Score
4. Discussion
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Conflicts of Interest
References
- National Cancer Institute. Surveillance, Epidemiology, and End Results (Seer) Program Populations (1969–2018). In Surveillance Research Program 2019, Section 23. Available online: https://seer.cancer.gov/popdata/ (accessed on 21 March 2020).
- Marsh, S.; Walters, R.W.; Silberstein, P.T. Survival Outcomes of Radical Prostatectomy Versus Radiotherapy in Intermediate-Risk Prostate Cancer: A NCDB Study. Clin. Genitourin Cancer 2017. [Google Scholar] [CrossRef]
- Dotan, Z.A.; Bianco, F.J., Jr.; Rabbani, F.; Eastham, J.A.; Fearn, P.; Scher, H.I.; Kelly, K.W.; Chen, H.N.; Schoder, H.; Hricak, H.; et al. Pattern of prostate-specific antigen (PSA) failure dictates the probability of a positive bone scan in patients with an increasing PSA after radical prostatectomy. J. Clin. Oncol 2005, 23, 1962–1968. [Google Scholar] [CrossRef]
- Bolla, M.; van Poppel, H.; Collette, L.; van Cangh, P.; Vekemans, K.; Da Pozzo, L.; de Reijke, T.M.; Verbaeys, A.; Bosset, J.F.; van Velthoven, R.; et al. Postoperative radiotherapy after radical prostatectomy: A randomised controlled trial (EORTC trial 22911). Lancet 2005, 366, 572–578. [Google Scholar] [CrossRef]
- Bolla, M.; van Poppel, H.; Tombal, B.; Vekemans, K.; Da Pozzo, L.; de Reijke, T.M.; Verbaeys, A.; Bosset, J.F.; van Velthoven, R.; Colombel, M.; et al. Postoperative radiotherapy after radical prostatectomy for high-risk prostate cancer: Long-term results of a randomised controlled trial (EORTC trial 22911). Lancet 2012, 380, 2018–2027. [Google Scholar] [CrossRef]
- Thompson, I.M.; Tangen, C.M.; Paradelo, J.; Lucia, M.S.; Miller, G.; Troyer, D.; Messing, E.; Forman, J.; Chin, J.; Swanson, G.; et al. Adjuvant radiotherapy for pathological T3N0M0 prostate cancer significantly reduces risk of metastases and improves survival: Long-term followup of a randomized clinical trial. J. Urol. 2009, 181, 956–962. [Google Scholar] [CrossRef] [PubMed]
- Wiegel, T.; Bartkowiak, D.; Bottke, D.; Bronner, C.; Steiner, U.; Siegmann, A.; Golz, R.; Storkel, S.; Willich, N.; Semjonow, A.; et al. Adjuvant radiotherapy versus wait-and-see after radical prostatectomy: 10-year follow-up of the ARO 96-02/AUO AP 09/95 trial. Eur. Urol. 2014, 66, 243–250. [Google Scholar] [CrossRef]
- Kneebone, A.; Fraser-Browne, C.; Delprado, W.; Duchesne, G.; Fisher, R.; Frydenberg, M.; Haworth, A.; Herschtal, A.; Joseph, D.J.; Lim, T.S.; et al. A Phase III Multi-Centre Randomised Trial comparing adjuvant versus early salvage Radiotherapy following a Radical Prostatectomy: Results of the TROG 08.03 and ANZUP “RAVES” Trial. Int. J. Radiat. Oncol. Biol. Phys. 2019, 105, S37–S38. [Google Scholar] [CrossRef]
- Vale, C.L.; Brihoum, M.; Chabaud, S.; Cook, A.; Fisher, D.; Forcat, S.; Fraser-Browne, C.; Herschtal, A.; Kneebone, A.; Nénan, S.; et al. Adjuvant or Salvage Radiotherapy for the Treatment of Localised Prostate Cancer? A Prospectively Planned Aggregate Data Meta-Analysis. ESMO 2019. Available online: https://oncologypro.esmo.org/meeting-resources/esmo-2019-congress/Adjuvant-or-salvage-radiotherapy-for-the-treatment-of-localised-prostate-cancer-A-prospectively-planned-aggregate-data-meta-analysis (accessed on 21 March 2020). [CrossRef]
- Parker, C.; Clarke, N.W.; Cook, A.; Kynaston, H.G.; Petersen, P.M.; Cross, W.; Persad, R.; Catton, C.; Logue, J.; Payne, H.; et al. Timing of Radiotherapy (RT) After Radical Prostatectomy (RP): First Results from the RADICALS RT Randomised Controlled Trial (RCT). ESMO 2019. Available online: https://oncologypro.esmo.org/meeting-resources/esmo-2019-congress/Timing-of-Radiotherapy-RT-After-Radical-Prostatectomy-RP-First-Results-from-the-RADICALS-RT-Randomised-Controlled-Trial-RCT-NCT00541047 (accessed on 21 March 2020). [CrossRef]
- Bagher-Ebadian, H.; Janic, B.; Liu, C.; Pantelic, M.; Hearshen, D.; Elshaikh, M.; Movsas, B.; Chetty, I.J.; Wen, N. Detection of Dominant Intraprostatic Lesions in Patients With Prostate Cancer Using an Artificial Neural Network and MR Multimodal Radiomics Analysis. Int. J. Radiat. Oncol. Biol. Phys. 2017, 99, S82–S83. [Google Scholar] [CrossRef]
- Dou, T.; Aerts, H.; Coroller, T.P.; Mak, R.H. Radiomic-Based Phenotyping of Tumor Core and Rim to Predict Survival in Nonsmall Cell Lung Cancer. Int. J. Radiat. Oncol. Biol. Phys. 2017, 99, S84. [Google Scholar] [CrossRef][Green Version]
- Wang, J.; Shen, L.; Zhong, H.; Hu, P.; Zhang, Z. Radiomics Prediction Model for Locally Advanced Rectal Cancer. Int. J. Radiat. Oncol. Biol. Phys. 2017, 99, S184. [Google Scholar] [CrossRef]
- Bourbonne, V.; Vallieres, M.; Lucia, F.; Visvikis, D.; Tissot, V.; Pradier, O.; Hatt, M.; Schick, U. MRI-derived radiomics to guide posto-perative management for high-risk prostate cancer. Front. Oncol. 2019, 9, 807. [Google Scholar] [CrossRef]
- Mottet, N.; Bellmunt, J.; Bolla, M.; Briers, E.; Cumberbatch, M.G.; De Santis, M.; Fossati, N.; Gross, T.; Henry, A.M.; Joniau, S.; et al. EAU-ESTRO-SIOG Guidelines on Prostate Cancer. Part 1: Screening, Diagnosis, and Local Treatment with Curative Intent. Eur. Urol. 2017, 71, 618–629. [Google Scholar] [CrossRef] [PubMed]
- Cooperberg, M.R.; Hilton, J.F.; Carroll, P.R. The CAPRA-S score: A straightforward tool for improved prediction of outcomes after radical prostatectomy. Cancer 2011, 117, 5039–5046. [Google Scholar] [CrossRef] [PubMed]
- Roach, M., 3rd; Marquez, C.; Yuo, H.S.; Narayan, P.; Coleman, L.; Nseyo, U.O.; Navvab, Z.; Carroll, P.R. Predicting the risk of lymph node involvement using the pre-treatment prostate specific antigen and Gleason score in men with clinically localized prostate cancer. Int. J. Radiat. Oncol. Biol. Phys. 1994, 28, 33–37. [Google Scholar] [CrossRef]
- Zwanenburg, A.; Vallieres, M.; Abdalah, M.A.; Aerts, H.; Andrearczyk, V.; Apte, A.; Ashrafinia, S.; Bakas, S.; Beukinga, R.J.; Boellaard, R.; et al. The Image Biomarker Standardization Initiative: Standardized Quantitative Radiomics for High-Throughput Image-based Phenotyping. Radiology 2020. [Google Scholar] [CrossRef]
- Chatterjee, A.; Vallières, M.; Dohan, A.; Levesque, I.; Uemo, Y.; Bist, V.; Saif, S.; Reinhold, C.; Seuptjens, J. An Empirical Approach for Avoiding False Discoveries When Applying High-Dimensional Radiomics to Small Datasets. IEEE Trans. Radiat. Plasma Med. Sci. 2019, 3, 201–209. [Google Scholar] [CrossRef]
- Lambin, P.; Leijenaar, R.T.H.; Deist, T.M.; Peerlings, J.; de Jong, E.E.C.; van Timmeren, J.; Sanduleanu, S.; Larue, R.; Even, A.J.G.; Jochems, A.; et al. Radiomics: The bridge between medical imaging and personalized medicine. Nature reviews. Clin. Oncol. 2017, 14, 749–762. [Google Scholar]
- Johnson, W.E.; Li, C.; Rabinovic, A. Adjusting batch effects in microarray expression data using empirical Bayes methods. Biostatistics 2007, 8, 118–127. [Google Scholar] [CrossRef]
- Fortin, J.P.; Cullen, N.; Sheline, Y.I.; Taylor, W.D.; Aselcioglu, I.; Cook, P.A.; Adams, P.; Cooper, C.; Fava, M.; McGrath, P.J.; et al. Harmonization of cortical thickness measurements across scanners and sites. Neuroimage 2018, 167, 104–120. [Google Scholar] [CrossRef] [PubMed]
- Lucia, F.; Visvikis, D.; Vallieres, M.; Desseroit, M.C.; Miranda, O.; Robin, P.; Bonaffini, P.A.; Alfieri, J.; Masson, I.; Mervoyer, A.; et al. External validation of a combined PET and MRI radiomics model for prediction of recurrence in cervical cancer patients treated with chemoradiotherapy. Eur. J. Nucl. Med. Mol. Imaging 2018. [Google Scholar] [CrossRef] [PubMed]
- Zou, K.H.; Warfield, S.K.; Bharatha, A.; Tempany, C.M.; Kaus, M.R.; Haker, S.J.; Wells, W.M., 3rd; Jolesz, F.A.; Kikinis, R. Statistical validation of image segmentation quality based on a spatial overlap index. Acad. Radiol. 2004, 11, 178–189. [Google Scholar] [CrossRef]
- Bianchi, L.; Nini, A.; Bianchi, M.; Gandaglia, G.; Fossati, N.; Suardi, N.; Moschini, M.; Dell’Oglio, P.; Schiavina, R.; Montorsi, F.; et al. The Role of Prostate-specific Antigen Persistence After Radical Prostatectomy for the Prediction of Clinical Progression and Cancer-specific Mortality in Node-positive Prostate Cancer Patients. Eur. Urol. 2016, 69, 1142–1148. [Google Scholar] [CrossRef]
- Liesenfeld, L.; Kron, M.; Gschwend, J.E.; Herkommer, K. Prognostic Factors for Biochemical Recurrence More than 10 Years after Radical Prostatectomy. J. Urol. 2017, 197, 143–148. [Google Scholar] [CrossRef] [PubMed]
- Wibmer, A.G.; Vargas, H.A.; Hricak, H. Role of MRI in the diagnosis and management of prostate cancer. Future Oncol. 2015, 11, 2757–2766. [Google Scholar] [CrossRef]
- Cameron, A.; Khalvati, F.; Haider, M.A.; Wong, A. MAPS: A Quantitative Radiomics Approach for Prostate Cancer Detection. IEEE Trans. Biomed. Eng. 2016, 63, 1145–1156. [Google Scholar] [CrossRef] [PubMed]
- Shiradkar, R.; Ghose, S.; Jambor, I.; Taimen, P.; Ettala, O.; Purysko, A.S.; Madabhushi, A. Radiomic features from pretreatment biparametric MRI predict prostate cancer biochemical recurrence: Preliminary findings. J. Magn. Reson Imaging 2018. [Google Scholar] [CrossRef]
- Ryznarova, Z.; Dezortova, M.; Jiru, F.; Vik, V.; Zachoval, R.; Hajek, M. Comparision of 1.5T and 3T Prostate MR Examination using Surface Array Coils in Routine Clinical Practice. J. Diagn. Tech. Biomed. Anal. 2018. [Google Scholar] [CrossRef]
- Abdollah, F.; Suardi, N.; Cozzarini, C.; Gallina, A.; Capitanio, U.; Bianchi, M.; Sun, M.; Fossati, N.; Passoni, N.M.; Fiorino, C.; et al. Selecting the optimal candidate for adjuvant radiotherapy after radical prostatectomy for prostate cancer: A long-term survival analysis. Eur. Urol. 2013, 63, 998–1008. [Google Scholar] [CrossRef]
- Fossati, N.; Karnes, R.J.; Cozzarini, C.; Fiorino, C.; Gandaglia, G.; Joniau, S.; Boorjian, S.A.; Goldner, G.; Hinkelbein, W.; Haustermans, K.; et al. Assessing the Optimal Timing for Early Salvage Radiation Therapy in Patients with Prostate-specific Antigen Rise After Radical Prostatectomy. Eur. Urol. 2016, 69, 728–733. [Google Scholar] [CrossRef] [PubMed]
- Egawa, S.; Matsui, Y.; Matsumoto, K.; Suyama, K.; Arai, Y.; Kuwao, S.; Baba, S. Impact of biochemical failure on long-term clinical outcome after radical prostatectomy for prostate cancer in Japan. Prostate Cancer Prostatic. Dis. 2004, 7, 152–157. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Freedland, S.J.; Humphreys, E.B.; Mangold, L.A.; Eisenberger, M.; Dorey, F.J.; Walsh, P.C.; Partin, A.W. Risk of prostate cancer-specific mortality following biochemical recurrence after radical prostatectomy. JAMA 2005, 294, 433–439. [Google Scholar] [CrossRef] [PubMed]
- Pound, C.R.; Partin, A.W.; Eisenberger, M.A.; Chan, D.W.; Pearson, J.D.; Walsh, P.C. Natural history of progression after PSA elevation following radical prostatectomy. JAMA 1999, 281, 1591–1597. [Google Scholar] [CrossRef] [PubMed]
- Bosco, C.; Bosnyak, Z.; Malmberg, A.; Adolfsson, J.; Keating, N.L.; Van Hemelrijck, M. Quantifying observational evidence for risk of fatal and nonfatal cardiovascular disease following androgen deprivation therapy for prostate cancer: A meta-analysis. Eur. Urol. 2015, 68, 386–396. [Google Scholar] [CrossRef] [PubMed]
- Dalela, D.; Loppenberg, B.; Sood, A.; Sammon, J.; Abdollah, F. Contemporary Role of the Decipher(R) Test in Prostate Cancer Management: Current Practice and Future Perspectives. Rev. Urol. 2016, 18, 1–9. [Google Scholar]
- Klein, E.A.; Haddad, Z.; Yousefi, K.; Lam, L.L.; Wang, Q.; Choeurng, V.; Palmer-Aronsten, B.; Buerki, C.; Davicioni, E.; Li, J.; et al. Decipher Genomic Classifier Measured on Prostate Biopsy Predicts Metastasis Risk. Urology 2016, 90, 148–152. [Google Scholar] [CrossRef]
- Katz, A.; Liu, C.; Kosinski, K.E. Histopathologic correlation of PI-RADS V.2 lesions on 3T multiparametric prostate MRI. J. Clin. Oncol. 2017, 34. [Google Scholar] [CrossRef]
- Padhani, A.R.; Weinreb, J.; Rosenkrantz, A.B.; Villeirs, G.; Turkbey, B.; Barentsz, J. Prostate Imaging-Reporting and Data System Steering Committee: PI-RADS v2 Status Update and Future Directions. Eur. Urol. 2019, 75, 385–396. [Google Scholar] [CrossRef]
- Simmons, M.N.; Stephenson, A.J.; Klein, E.A. Natural history of biochemical recurrence after radical prostatectomy: Risk assessment for secondary therapy. Eur. Urol. 2007, 51, 1175–1184. [Google Scholar] [CrossRef]
- Rahman, S.; Cosmatos, H.; Dave, G.; Williams, S.; Tome, M. Predicting pelvic lymph node involvement in current-era prostate cancer. Int. J. Radiat. Oncol. Biol. Phys. 2012, 82, 906–910. [Google Scholar] [CrossRef] [PubMed]


| Patient Characteristics | Training (%) n = 107 | Testing (%) n = 88 | p-Value |
|---|---|---|---|
| Age at diagnosis (mean, y) | 65.2 | 66.2 | 0.25 |
| PSA (mean, ng/mL) | 9.3 | 8.5 | 0.37 |
| MRI characteristics | |||
| Siemens 1.5T Institution 1 (%) | 70.0 | ||
| Philips 3T Institution 1 (%) | 30.0 | ||
| Philips Institution 2 (%) | 55.7 | ||
| Siemens Institution 2 (%) | 44.4 | ||
| Surgical characteristics | |||
| Pathological tumor stage | |||
| pT1-pT2 | 34.6 | 43.2 | 0.28 |
| pT3-pT4 | 65.4 | 56.8 | |
| Lymph nodes dissection | |||
| yes | 68.2 | 96.6 | <0.0001 |
| no | 31.8 | 3.4 | |
| Surgical margins | |||
| R0 | 40.2 | 22.7 | 0.014 |
| R1 | 58.8 | 77.3 | |
| Gleason score | |||
| Gleason ≤ 7 | 86.0 | 83.0 | 0.71 |
| Gleason > 7 | 14.0 | 17.0 | |
| Median Capra-S Score | 4 | 4 | 1.00 |
| Mean postoperative PSA (ng/mL) | 0.014 | 0.017 | 0.22 |
| Median number of risk factors | 1 | 1 | |
| Median bRFS (months) | 49.2 | 33.3 | <0.0001 |
| Biochemical recurrence (%) | 16.8 | 38.6 | 0.0166 |
| Median Follow-up (months) | 57.0 | 41.9 | <0.0001 |
| Biochemical Reccurence | Univariate Analysis | Multivariate Analysis | ||||||
|---|---|---|---|---|---|---|---|---|
| Feature | AUC | Best Cut-Off | BAcc (%) | Se (%) | Sp (%) | p-value | HR | p-Value |
| ADC SZEGLSZM | 0.82 | ≤0.53 | 79 | 72 | 85 | <0.0001 | 10.9 | 0.0001 |
| Age at surgery (y) | 0.54 | >65.7 | 60 | 72 | 48 | 0.62 | ||
| Preoperative PSA (ng/mL) | 0.62 | >6.5 | 64 | 78 | 50 | 0.08 | ||
| Gleason score | 0.53 | >4 | 57 | 17 | 96 | 0.72 | ||
| T stage | 0.62 | >3 | 58 | 78 | 38 | 0.07 | ||
| Surgical Margins | 0.51 | >0 | 51 | 61 | 41 | 0.90 | ||
| Postoperative PSA (ng/mL) | 0.64 | >0.01 | 63 | 56 | 69 | 0.04 | 2.7 | 0.064 |
| Capra-S Score | 0.58 | >3 | 63 | 72 | 53 | 0.27 | ||
| Number of risk factors | 0.64 | >1 | 64 | 56 | 72 | 0.04 | 3.2 | 0.064 |
| Prediction Models | BCR Prediction | bRFS Stratification | ||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|
| Training | Testing | Training | Testing | |||||||||
| Model | AUC | p-Value | BAcc (%) | Se (%) | Sp (%) | BAcc (%) | Se (%) | Sp (%) | HR | p-Value | HR | p-Value |
| Clinical | 0.68 | 0.007 | 63 | 78 | 47 | 56 | 53 | 59 | 3.2 | 0.032 | 1.7 | 0.19 |
| Radiomics | 0.82 | <0.0001 | 78 | 72 | 84 | 76 | 59 | 93 | 8.7 | <0.0001 | 5.5 | <0.0001 |
| C + R | 0.86 | <0.0001 | 84 | 94 | 67 | 67 | 91 | 43 | 25 | <0.0001 | 5.7 | <0.0001 |
| Combat R | 0.82 | <0.0001 | 77 | 72 | 82 | 76 | 59 | 93 | 8.0 | <0.0001 | 5.5 | <0.0001 |
| Combat C + R | 0.82 | <0.0001 | 74 | 59 | 93 | 76 | 53 | 98 | 6.9 | <0.0001 | 6.8 | <0.0001 |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Bourbonne, V.; Fournier, G.; Vallières, M.; Lucia, F.; Doucet, L.; Tissot, V.; Cuvelier, G.; Hue, S.; Le Penn Du, H.; Perdriel, L.; et al. External Validation of an MRI-Derived Radiomics Model to Predict Biochemical Recurrence after Surgery for High-Risk Prostate Cancer. Cancers 2020, 12, 814. https://doi.org/10.3390/cancers12040814
Bourbonne V, Fournier G, Vallières M, Lucia F, Doucet L, Tissot V, Cuvelier G, Hue S, Le Penn Du H, Perdriel L, et al. External Validation of an MRI-Derived Radiomics Model to Predict Biochemical Recurrence after Surgery for High-Risk Prostate Cancer. Cancers. 2020; 12(4):814. https://doi.org/10.3390/cancers12040814
Chicago/Turabian StyleBourbonne, Vincent, Georges Fournier, Martin Vallières, François Lucia, Laurent Doucet, Valentin Tissot, Gilles Cuvelier, Stephane Hue, Henri Le Penn Du, Luc Perdriel, and et al. 2020. "External Validation of an MRI-Derived Radiomics Model to Predict Biochemical Recurrence after Surgery for High-Risk Prostate Cancer" Cancers 12, no. 4: 814. https://doi.org/10.3390/cancers12040814
APA StyleBourbonne, V., Fournier, G., Vallières, M., Lucia, F., Doucet, L., Tissot, V., Cuvelier, G., Hue, S., Le Penn Du, H., Perdriel, L., Bertrand, N., Staroz, F., Visvikis, D., Pradier, O., Hatt, M., & Schick, U. (2020). External Validation of an MRI-Derived Radiomics Model to Predict Biochemical Recurrence after Surgery for High-Risk Prostate Cancer. Cancers, 12(4), 814. https://doi.org/10.3390/cancers12040814





