Image-Guided Multisession Radiosurgery of Skull Base Meningiomas
Abstract
Simple Summary
Abstract
1. Introduction
1.1. Background/Rationale
1.2. Objective
2. Material and Methods
2.1. Study Design
2.2. Setting
2.3. Inclusion Criteria
2.4. Participants and Sample Size
2.5. Ethics
2.6. Imaging and Treatment
2.6.1. Neuroimaging
2.6.2. The Planning Procedure Included Several Sequential Steps
- (1)
- Contouring: the contouring of the tumor and the critical volumes was performed on co-registered MR-CT images. The volumes were manually outlined on axial images, with a simultaneous overlay of these contours on coronal and sagittal reconstructions. In all of the cases, the planning treatment volume (PTV) and gross tumor volume (GTV) coincided.
- (2)
- Dose selection: the marginal and maximal dose, as well as the number of sessions were influenced by a multitude of factors, including patient age, tumor volume, length and volume of the irradiated critical organs (optic nerve, chiasm, or brainstem), and neurological function. Adopting an α/β of 2, the target biologically equivalent dose (BED) to be used in the different fractionation schedules was 87.5 Gy2, corresponding to that of a 25 Gy in a five fractions schedule [13,27]. The dose to any portion of the anterior visual pathway was set not to exceed a maximum of 500 cGy per fraction [13].
- (3)
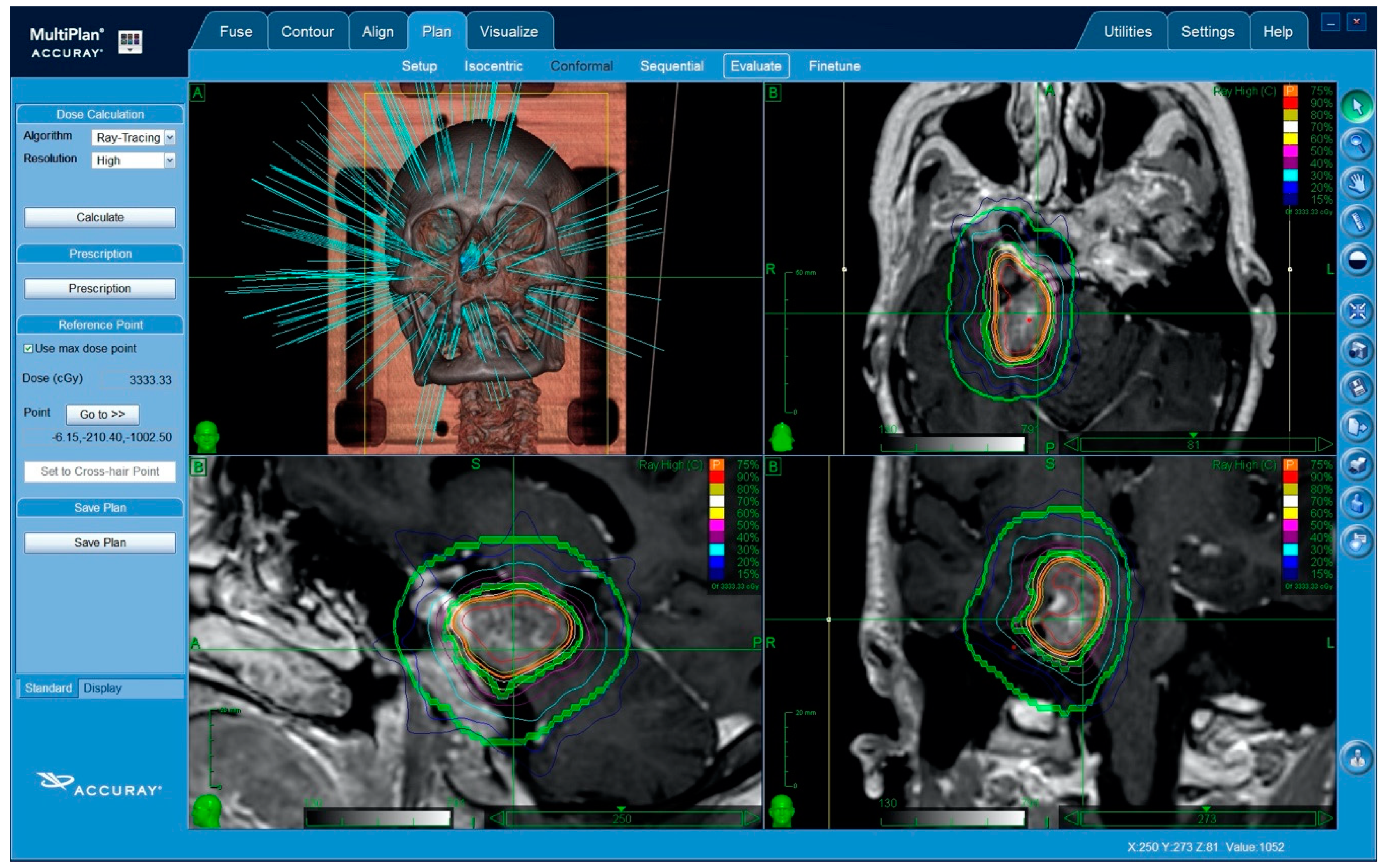
- Planning: An inverse planning algorithm using a nonisocentric technique determined the optimal treatment planning program. The ray-tracing algorithm was routinely used for this purpose. Some of the methods used included the following: (a) selection of the size and number of collimators, balancing the necessity of target coverage, reduction in the number of radiation beams, and monitor units with the necessity of steep dose gradients in specific areas; (b) the addition of tuning structures to reduce uncontrolled dose diffusion (Figure 1); (c) definition of dose constraints and their weight to the target volume and critical structures; and (d) maximization of the resolution of a dose calculation using the smallest calculation grid. (e) Plan evaluation, including: a visual analysis of the dose–volume histograms for the target and all of the critical structures, and evaluation of the PTV coverage and the dose conformity. Conformity was expressed with respect to the PTV as the new conformality index (nCI), defined as the inverse Paddick conformity index [28], where
2.6.3. Treatment Delivery
2.7. Data Sources and Patient Assessment
2.8. Bias and Assessment of Outcome Variables
2.9. Statistical Methods
3. Results
3.1. Participants
3.2. Descriptive Data of Radiosurgical Doses and Schedules
3.3. Tumor Control
3.4. Clinical Outcome
3.5. Upfront versus Adjuvant Treatment
4. Discussion
4.1. Key Results
4.2. Interpretation
4.3. Study Limitations
5. Conclusions
Author Contributions
Funding
Conflicts of Interest
References
- DiBiase, S.J.; Kwok, Y.; Yovino, S.; Arena, C.; Naqvi, S.; Temple, R.; Regine, W.F.; Amin, P.; Guo, C.; Chin, L.S. Factors predicting local tumor control after gamma knife stereotactic radiosurgery for benign intracranial meningiomas. Int. J. Radiat. Oncol. Biol. Phys. 2004, 60, 1515–1519. [Google Scholar] [CrossRef] [PubMed]
- Hasegawa, T.; Kida, Y.; Yoshimoto, M.; Koike, J.; Iizuka, H.; Ishii, D. Long-term outcomes of Gamma Knife surgery for cavernous sinus meningioma. J. Neurosurg. 2007, 107, 745–751. [Google Scholar] [CrossRef] [PubMed]
- Iwai, Y.; Yamanaka, K.; Ikeda, H. Gamma Knife radiosurgery for skull base meningioma: Long-term results of low-dose treatment. J. Neurosurg. 2008, 109, 804–810. [Google Scholar] [CrossRef] [PubMed]
- Liscak, R.; Kollová, A.; Vladyka, V.; Šimonová, G.; Novotný, J., Jr. Gamma Knife Radiosurgery of Skull Base Meningiomas. Acta Neurochir. Suppl. 2004, 91, 65–74. [Google Scholar] [CrossRef] [PubMed]
- Kondziolka, D.; Mathieu, D.; Lunsford, L.D.; Martin, J.J.; Madhok, R.; Niranjan, A.; Flickinger, J. Radiosurgery as definitive management of intracranial meningiomas. Neurosurgery 2008, 62, 53–60. [Google Scholar] [CrossRef] [PubMed]
- Kreil, W.; Luggin, J.; Fuchs, I.; Weigl, V.; Eustacchio, S.; Papaefthymiou, G. Long term experience of gamma knife radiosurgery for benign skull base meningiomas. J. Neurol. Neurosurg. Psychiatry 2005, 76, 1425–1430. [Google Scholar] [CrossRef]
- Lee, J.Y.K.; Niranjan, A.; McInerney, J.; Kondziolka, D.; Flickinger, J.C.; Lunsford, L.D. Stereotactic radiosurgery providing long-term tumor control of cavernous sinus meningiomas. J. Neurosurg. 2002, 97, 65–72. [Google Scholar] [CrossRef]
- Minniti, G.; Amichetti, M.; Maurizi, E.R. Radiotherapy and radiosurgery for benign skull base meningiomas. Radiat. Oncol. 2009, 4, 42. [Google Scholar] [CrossRef]
- Nicolato, A.; Foroni, R.; Alessandrini, F.; Maluta, S.; Bricolo, A.; Gerosa, M. The role of Gamma Knife radiosurgery in the management of cavernous sinus meningiomas. Int. J. Radiat. Oncol. Biol. Phys. 2002, 53, 992–1000. [Google Scholar] [CrossRef]
- Stafford, S.L.; Pollock, B.E.; Foote, R.L.; Link, M.J.; Gorman, D.A.; Schomberg, P.J.; Leavitt, J.A. Meningioma radiosurgery: Tumor control, outcomes, and complications among 190 consecutive patients. Neurosurgery 2001, 49, 1028–1037. [Google Scholar]
- Starke, R.M.; Przybylowski, C.J.; Sugoto, M.; Fezeu, F.; Awad, A.J.; Ding, D.; Nguyen, J.H.; Sheehan, J.P. Gamma Knife radiosurgery of large skull base meningiomas. J. Neurosurg. 2015, 122, 363–372. [Google Scholar] [CrossRef] [PubMed]
- Kondziolka, D.; Niranjan, A.; Lunsford, L.D.; Flickinger, J.C. Stereotactic radiosurgery for meningiomas. Neurosurg. Clin. N. Am. 1999, 10, 317–325. [Google Scholar] [CrossRef]
- Conti, A.; Pontoriero, A.; Midili, F.; Iatì, G.; Siragusa, C.; Tomasello, C.; La Torre, D.; Cardali, S.M.; Pergolizzi, S.; De Renzis, C. CyberKnife multisession stereotactic radiosurgery and hypofractionated stereotactic radiotherapy for perioptic meningiomas: Intermediate-term results and radiobiological considerations. SpringerPlus 2015, 4, 1–8. [Google Scholar] [CrossRef] [PubMed]
- Conti, A.; Pontoriero, A.; Salamone, I.; Siragusa, C.; Midili, F.; La Torre, D.; Calisto, A.; Granata, F.; Romanelli, P.; De Renzis, C.; et al. Protecting venous structures during radiosurgery for parasagittal meningiomas. Neurosurg. Focus 2009, 27, E11. [Google Scholar] [CrossRef]
- Conti, A.; Pontoriero, A.; Siddi, F.; Iatì, G.; Cardali, S.; Angileri, F.F.; Granata, F.; Pergolizzi, S.; Germanò, A.; Francesco, T.; et al. Post-Treatment Edema after Meningioma Radiosurgery is a Predictable Complication. Cureus 2016, 8. [Google Scholar] [CrossRef]
- Adler, J.R., Jr.; Gibbs, I.C.; Puataweepong, P.; Chang, S.D. Visual field preservation after multisession cyberknife radiosurgery for perioptic lesions. Neurosurgery 2008, 62, 733–743. [Google Scholar] [CrossRef]
- Choi, C.Y.H.; Soltys, S.G.; Gibbs, I.C.; Harsh, G.R.; Jackson, P.; Lieberson, R.E.; Chang, S.D.; Adler, J.R. Cyberknife Stereotactic Radiosurgery for Treatment of Atypical (Who Grade II) Cranial Meningiomas. Neurosurgery 2010, 67, 1180–1188. [Google Scholar] [CrossRef]
- Colombo, F.; Casentini, L.; Cavedon, C.; Scalchi, P.; Cora, S.; Francescon, P. Cyberknife radiosurgery for benign meningiomas: Short-term results in 199 patients. Neurosurgery 2009, 64, A7–A13. [Google Scholar] [CrossRef]
- Manabe, Y.; Murai, T.; Ogino, H.; Tamura, T.; Iwabuchi, M.; Mori, Y.; Iwata, H.; Suzuki, H.; Shibamoto, Y. CyberKnife Stereotactic Radiosurgery and Hypofractionated Stereotactic Radiotherapy as First-line Treatments for Imaging-diagnosed Intracranial Meningiomas. Neurol. Med. Chir. 2017, 57, 627–633. [Google Scholar] [CrossRef]
- Patil, C.G.; Hoang, S.; Borchers, D.J., 3rd; Sakamoto, G.; Soltys, S.G.; Gibbs, I.C.; Harsh, G.R.; Chang, S.D.; Adler, J.R. Predictors of peritumoral edema after stereotactic radiosurgery of supratentorial meningiomas. Neurosurgery 2008, 63, 435–442. [Google Scholar] [CrossRef]
- Pham, C.J.; Chang, S.D.; Gibbs, I.C.; Jones, P.; Heilbrun, M.P.; Adler, J.R., Jr. Preliminary visual field preservation after staged CyberKnife radiosurgery for perioptic lesions. Neurosurgery 2004, 54, 799–812. [Google Scholar] [CrossRef] [PubMed]
- Romanelli, P.; Bianchi, L.; Muacevic, A.; Beltramo, G. Staged image guided robotic radiosurgery for optic nerve sheath meningiomas. Comput. Aided Surg. 2011, 16, 257–266. [Google Scholar] [CrossRef] [PubMed]
- Romanelli, P.; Wowra, B.; Muacevic, A. Multisession CyberKnife radiosurgery for optic nerve sheath meningiomas. Neurosurg. Focus 2007, 23, E10. [Google Scholar] [CrossRef] [PubMed]
- Marchetti, M.; Bianchi, S.; Milanesi, I.; Bergantin, A.; Bianchi, L.; Broggi, G.; Fariselli, L. Multisession radiosurgery for optic nerve sheath meningiomas—An effective option: Preliminary results of a single-center experience. Neurosurgery 2011, 69, 1116–1123. [Google Scholar] [CrossRef]
- Marchetti, M.; Bianchi, S.; Pinzi, V.; Tramacere, I.; Fumagalli, M.L.; Milanesi, I.M.; Ferroli, P.; Frazini, A.; Saini, M.; DiMeco, F.; et al. Multisession Radiosurgery for Sellar and Parasellar Benign Meningiomas: Long-term Tumor Growth Control and Visual Outcome. Neurosurgery 2016, 78, 638–646. [Google Scholar] [CrossRef]
- Shrieve, D.C.; Hazard, L.; Boucher, K.; Jensen, R.L. Dose fractionation in stereotactic radiotherapy for parasellar meningiomas: Radiobiological considerations of efficacy and optic nerve tolerance. J. Neurosurg. 2004, 101, 390–395. [Google Scholar] [CrossRef]
- Marchetti, M.; Conti, A.; Beltramo, G.; Pinzi, V.; Pontoriero, A.; Tramacere, I.; Senger, C.; Pergolizzi, S.; Fariselli, L. Multisession radiosurgery for perioptic meningiomas: Medium-to-long term results from a CyberKnife cooperative study. J. Neuro Oncol. 2019, 143, 597–604. [Google Scholar] [CrossRef]
- Paddick, I. A simple scoring ratio to index the conformity of radiosurgical treatment plans. J. Neurosurg. 2000, 93 (Suppl. 3), 219–222. [Google Scholar] [CrossRef]
- Combs, S.E.; Adeberg, S.; Dittmar, J.-O.; Welzel, T.; Rieken, S.; Habermehl, D.; Huber, P.E.; Debus, J. Skull base meningiomas: Long-term results and patient self-reported outcome in 507 patients treated with fractionated stereotactic radiotherapy (FSRT) or intensity modulated radiotherapy (IMRT). Radiother. Oncol. 2013, 106, 186–191. [Google Scholar] [CrossRef]
- Kaul, D.; Budach, V.; Wurm, R.; Grün, A.; Graaf, L.; Habbel, P.; Badakhshi, H. Linac-based stereotactic radiotherapy and radiosurgery in patients with meningioma. Radiat. Oncol. 2014, 9, 78. [Google Scholar] [CrossRef]
- Solda, F.; Wharram, B.; Gunapala, R.; Brada, M. Fractionated Stereotactic Conformal Radiotherapy for Optic Nerve Sheath Meningiomas. Clin. Oncol. 2012, 24, e106–e112. [Google Scholar] [CrossRef] [PubMed]
- Steinvorth, S.; Welzel, G.; Fuss, M.; Debus, J.; Wildermuth, S.; Wannenmacher, M.; Wenz, F. Neuropsychological outcome after fractionated stereotactic radiotherapy (FSRT) for base of skull meningiomas: A prospective 1-year follow-up. Radiother. Oncol. 2003, 69, 177–182. [Google Scholar] [CrossRef]
- Fokas, E.; Henzel, M.; Surber, G.; Hamm, K.; Engenhart-Cabillic, R. Stereotactic Radiation Therapy for Benign Meningioma: Long-Term Outcome in 318 Patients. Int. J. Radiat. Oncol. Biol. Phys. 2014, 89, 569–575. [Google Scholar] [CrossRef] [PubMed]
- Andrews, D.W.; Faroozan, R.; Yang, B.P.; Hudes, R.S.; Werner-Wasik, M.; Kim, S.M.; Sergott, R.C.; Savino, P.J.; Shields, J.; Shields, C.; et al. Fractionated stereotactic radiotherapy for the treatment of optic nerve sheath meningiomas: Preliminary observations of 33 optic nerves in 30 patients with historical comparison to observation with or without prior surgery. Neurosurgery 2002, 51, 890–904. [Google Scholar] [PubMed]
- Combs, S.E.; Ganswindt, U.; Foote, R.L.; Kondziolka, D.; Tonn, J.-C. State-of-the-art treatment alternatives for base of skull meningiomas: Complementing and controversial indications for neurosurgery, stereotactic and robotic based radiosurgery or modern fractionated radiation techniques. Radiat. Oncol. 2012, 7, 226. [Google Scholar] [CrossRef] [PubMed]
- Astner, S.T.; Theodorou, M.; Dobrei-Ciuchendea, M.; Auer, F.; Kopp, C.; Molls, M.; Grosu, A.-L. Tumor Shrinkage Assessed by Volumetric MRI in the Long-Term Follow-Up after Stereotactic Radiotherapy of Meningiomas. Strahlenther. Onkol. 2010, 186, 423–429. [Google Scholar] [CrossRef] [PubMed]
- Milker-Zabel, S.; Bois, A.Z.-D.; Henze, M.; Huber, P.; Schulz-Ertner, D.; Hoess, A.; Haberkorn, U.; Debus, J. Improved target volume definition for fractionated stereotactic radiotherapy in patients with intracranial meningiomas by correlation of CT, MRI, and [68Ga]-DOTATOC-PET. Int. J. Radiat. Oncol. Biol. Phys. 2006, 65, 222–227. [Google Scholar] [CrossRef]
- Jeremic, B.; Pitz, S. Primary optic nerve sheath meningioma: Stereotactic fractionated radiation therapy as an emerging treatment of choice. Cancer 2007, 110, 714–722. [Google Scholar] [CrossRef]
- Pacelli, R.; Cella, L.; Conson, M.; Tranfa, F.; Strianese, D.; Liuzzi, R.; Solla, R.; Farella, A.; Salvatore, M.; Bonavolontà, G. Fractionated Stereotactic Radiation Therapy for Orbital Optic Nerve Sheath Meningioma—A Single Institution Experience and a Short Review of the Literature. J. Radiat. Res. 2011, 52, 82–87. [Google Scholar] [CrossRef]
- Afshar-Oromieh, A.; Wolf, M.B.; Kratochwil, C.; Giesel, F.L.; Combs, S.E.; Dimitrakopoulou-Strauss, A.; Gnirs, R.; Roethke, M.C.; Schlemmer, H.P.; Haberkorn, U. Comparison of 68Ga-DOTATOC-PET/CT and PET/MRI hybrid systems in patients with cranial meningioma: Initial results. Neuro Oncol. 2015, 17, 312–319. [Google Scholar] [CrossRef]
- Farzin, M.; Molls, M.; Kampfer, S.; Astner, S.T.; Schneider, R.; Roth, K.; Dobrei, M.; Combs, S.E.; Straube, C. Optic toxicity in radiation treatment of meningioma: A retrospective study in 213 patients. J. Neuro Oncol. 2016, 127, 597–606. [Google Scholar] [CrossRef] [PubMed]
- Mozes, P.; Dittmar, J.-O.; Habermehl, D.; Tonndorf-Martini, E.; Hideghéty, K.; Dittmar, A.; Debus, J.; Combs, S.E. Volumetric response of intracranial meningioma after photon or particle irradiation. Acta Oncol. 2016, 56, 431–437. [Google Scholar] [CrossRef] [PubMed]
- Stade, F.; Dittmar, J.-O.; Jäkel, O.; Kratochwil, C.; Haberkorn, U.; Debus, J.; Combs, S.E. Influence of 68Ga-DOTATOC on sparing of normal tissue for radiation therapy of skull base meningioma: Differential impact of photon and proton radiotherapy. Radiat. Oncol. 2018, 13, 58. [Google Scholar] [CrossRef] [PubMed]
- Combs, S.E.; Farzin, M.; Boehmer, J.; Oehlke, O.; Molls, M.; Debus, J.; Grosu, A.-L. Clinical outcome after high-precision radiotherapy for skull base meningiomas: Pooled data from three large German centers for radiation oncology. Radiother. Oncol. 2018, 127, 274–279. [Google Scholar] [CrossRef]
- Kessel, K.A.; Fischer, H.; Oechnser, M.; Zimmer, C.; Meyer, B.; Combs, S.E. High-precision radiotherapy for meningiomas: Long-term results and patient-reported outcome (PRO). Strahlenther Onkol. 2017, 193, 921–930. [Google Scholar] [CrossRef]
- Lo, S.S.; Cho, K.H.; Hall, W.A.; Kossow, R.J.; Hernandez, W.L.; McCollow, K.K.; Gerbi, B.J.; Higgins, P.D.; Lee, C.K.; Dusenbery, K.E. Single dose versus fractionated stereotactic radiotherapy for meningiomas. Can. J. Neurol. Sci. 2002, 29, 240–248. [Google Scholar] [CrossRef]
- Metellus, P.; Regis, J.; Muracciole, X.; Fuentes, S.; Dufour, H.; Nanni, I.; Chinot, O.; Martin, P.-M.; Grisoli, F. Evaluation of Fractionated Radiotherapy and Gamma Knife Radiosurgery in Cavernous Sinus Meningiomas: Treatment Strategy. Neurosurgery 2005, 57, 873–886. [Google Scholar] [CrossRef]
- Torres, R.C.; Frighetto, L.; De Salles, A.A.F.; Goss, B.; Medin, P.; Solberg, T.; Ford, J.M.; Selch, M. Radiosurgery and stereotactic radiotherapy for intracranial meningiomas. Neurosurg. Focus 2003, 14, 1–6. [Google Scholar] [CrossRef]
- Conti, A.; Romanelli, P.; Pantelis, E.; Soltys, S.G.; Cho, Y.H.; Lim, M. (Eds.) CyberKnife NeuroRadiosurgery A Practical Guide; Springer: Cham, Switzerland, 2020. [Google Scholar]
- Girvigian, M.R.; Chen, J.C.; Rahimian, J.; Miller, M.J.; Tome, M. Comparison of early complications for patients with convexity and parasagittal meningiomas treated with either stereotactic radiosurgery or fractionated stereotactic radiotherapy. Neurosurgery 2008, 62 (Suppl. 5), A19–A28. [Google Scholar] [CrossRef]
- Unger, K.R.; Lominska, C.E.; Chanyasulkit, J.; Randolph-Jackson, P.; White, R.L.; Aulisi, E.; Jacobson, J.; Jean, W.C.; Gagnon, G.J. Risk Factors for Posttreatment Edema in Patients Treated With Stereotactic Radiosurgery for Meningiomas. Neurosurgery 2011, 70, 639–645. [Google Scholar] [CrossRef]
- Acker, G.; Meinert, F.; Conti, A.; Kufeld, M.; Jelgersma, C.; Nguyen, P.; Kluge, A.; Lukas, M.; Loebel, F.; Pasemann, D.; et al. Image-Guided Robotic Radiosurgery for Treatment of Recurrent Grade II and III Meningiomas. A Single-Center Study. World Neurosurg. 2019, 131, e96–e107. [Google Scholar] [CrossRef] [PubMed]
- Nahum, A.E. The Radiobiology of Hypofractionation. Clin. Oncol. 2015, 27, 260–269. [Google Scholar] [CrossRef] [PubMed]






| Variations | Value |
|---|---|
| No. of Patients | 156 |
| Gender (M/F) | 37/119 |
| Age at the treatment time (years) | |
| Mean (range) | 58 ± 11.4 (30–81) |
| Follow-up (months) | |
| Mean (±SD) Median (range) | 36.2 (±29.1) 36.6 (2–137) |
| KPS | |
| Mean (±SD) Median (range) | 88 (±9.1) 90 (70–100) |
| Treatment Modality | |
| Upfront Adjuvant Residual Recurrence | 107 49 22 27 |
| Tumor Site | |
| Perioptic/ACF/LSW PetroClival PCF Cavernous sinus | 72 (46.1%) 46 (28.5%) 15 (9.4%) 23 (14.7%) |
| Pretreatment Cranial Nerves deficit | 35 (22.4%) |
| II III–IV–VI V VII VIII IX–X | 13 (8.3%) 7 (4.5%) 9 (5.8%) 3 (1.9%) 2 (1.3%) 1 (0.6%) |
| Histology | |
| Yes | 49 (31.4%) |
| Variations | Value |
|---|---|
| Patients | 156 |
| PTV | |
| Mean ± SD Median | 10.3 ± 11.9 mL 7.5 mL |
| Dose | |
| Mean ± SD Median | 25 ± 5.3 Gy 25 Gy |
| Number of Fractions | |
| Mean ± SD Median | 5 ± 2 5 |
| BED (Gy) | |
| Mean ± SD | 87.2 ± 15.1 |
| Median | 87.5 |
| EqD2 (Gy) | |
| Mean ± SD | 43.6 ± 7.6 |
| Median | 43.8 |
| New Conformality Index | |
| Mean ± SD | 1.5 ± 0.3 |
| Median (range) | 1.4 |
| Prescription Isodose | |
| Mean ± SD | 76.5 ± 5.1 |
| Median | 77 |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Conti, A.; Pontoriero, A.; Iatì, G.; Cardali, S.M.; Brogna, A.; Friso, F.; Rosetti, V.; Zoli, M.; Parisi, S.; Cacciola, A.; et al. Image-Guided Multisession Radiosurgery of Skull Base Meningiomas. Cancers 2020, 12, 3569. https://doi.org/10.3390/cancers12123569
Conti A, Pontoriero A, Iatì G, Cardali SM, Brogna A, Friso F, Rosetti V, Zoli M, Parisi S, Cacciola A, et al. Image-Guided Multisession Radiosurgery of Skull Base Meningiomas. Cancers. 2020; 12(12):3569. https://doi.org/10.3390/cancers12123569
Chicago/Turabian StyleConti, Alfredo, Antonio Pontoriero, Giuseppe Iatì, Salvatore M. Cardali, Anna Brogna, Filippo Friso, Vittoria Rosetti, Matteo Zoli, Silvana Parisi, Alberto Cacciola, and et al. 2020. "Image-Guided Multisession Radiosurgery of Skull Base Meningiomas" Cancers 12, no. 12: 3569. https://doi.org/10.3390/cancers12123569
APA StyleConti, A., Pontoriero, A., Iatì, G., Cardali, S. M., Brogna, A., Friso, F., Rosetti, V., Zoli, M., Parisi, S., Cacciola, A., Lillo, S., Pergolizzi, S., & Mazzatenta, D. (2020). Image-Guided Multisession Radiosurgery of Skull Base Meningiomas. Cancers, 12(12), 3569. https://doi.org/10.3390/cancers12123569







