Radiation-Induced Thyroid Cancers: Overview of Molecular Signatures
Abstract
1. Introduction
2. Childhood Thyroid Cancers after the Chernobyl Accident
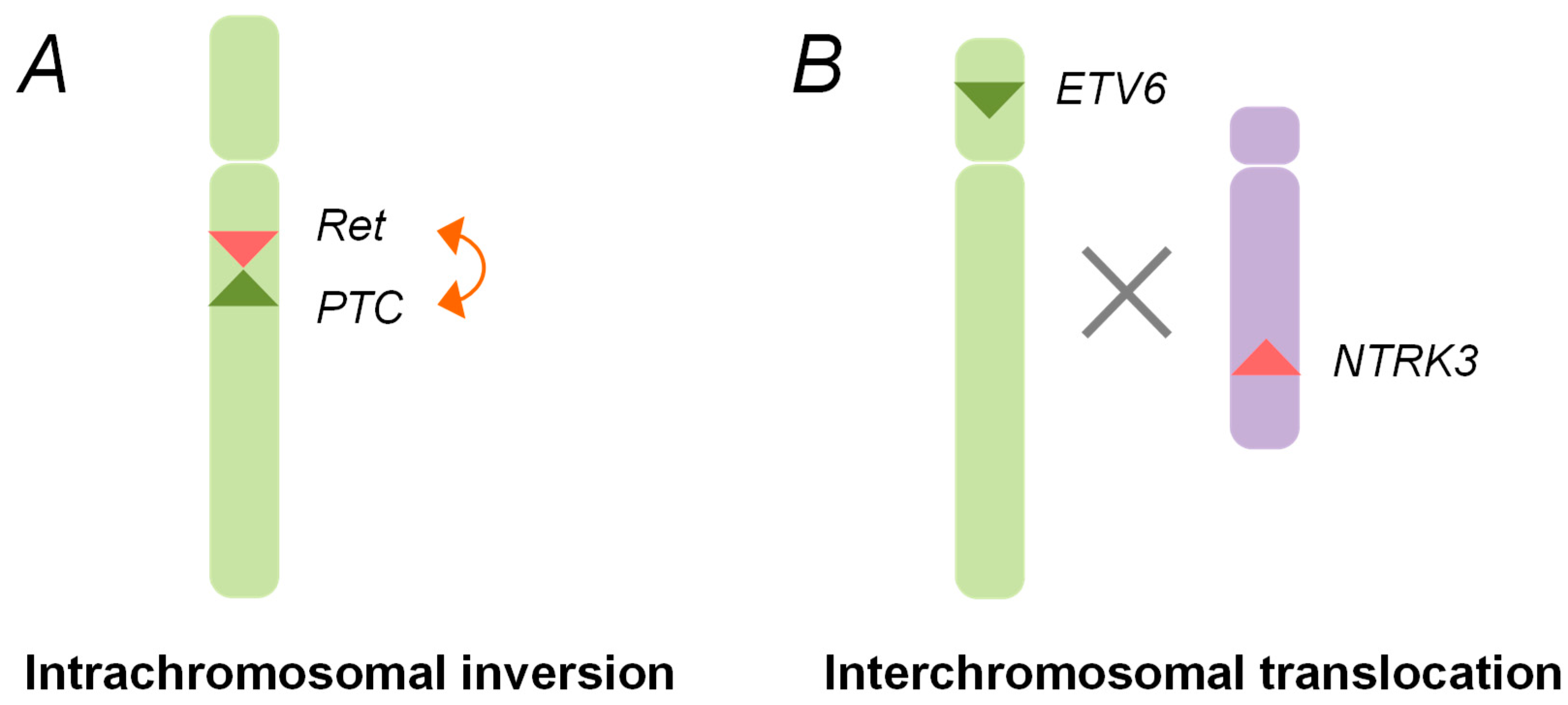
3. Oncogenic Rearrangements in Childhood Thyroid Cancer
4. Thyroid Cancers among A-Bomb Survivors
5. Thyroid Cancers among the Patients Who Received External Medical Radiation in Childhood
6. Radiation Signatures and Possible Mechanism of Radiation Carcinogenesis
7. Conclusions
Author Contributions
Funding
Conflicts of Interest
References
- Ozasa, K.; Shimizu, Y.; Suyama, A.; Kasagi, F.; Soda, M.; Grant, E.J.; Sakata, R.; Sugiyama, H.; Kodama, K. Studies of the mortality of atomic bomb survivors, Report 14, 1950–2003: An overview of cancer and noncancer diseases. Radiat. Res. 2012, 177, 229–243. [Google Scholar] [CrossRef]
- Ozasa, K.; Cullings, H.M.; Ohishi, W.; Hida, A.; Grant, E.J. Epidemiological studies of atomic bomb radiation at the Radiation Effects Research Foundation. Int. J. Radiat. Biol. 2019, 95, 879–891. [Google Scholar] [CrossRef]
- Williams, D. Radiation carcinogenesis: Lessons from Chernobyl. Oncogene 2008, 27, S9–S18. [Google Scholar] [CrossRef] [PubMed]
- Saenko, V.; Ivanov, V.; Tsyb, A.; Bogdanova, T.; Tronko, M.; Demidchik, Y.; Yamashita, S. The Chernobyl accident and its consequences. Clin. Oncol. 2011, 23, 234–243. [Google Scholar] [CrossRef]
- Thomas, G.A.; Tronko, M.; Tsyb, A.F.; Tuttle, R.M. What have we learnt from Chernobyl? What have we still to learn? Clin. Oncol. 2011, 23, 229–233. [Google Scholar] [CrossRef] [PubMed]
- Hatch, M.; Cardis, E. Somatic health effects of Chernobyl: 30 years on. Eur. J. Epidemiol. 2017, 32, 1047–1054. [Google Scholar] [CrossRef]
- Brenner, A.V.; Tronko, M.D.; Hatch, M.; Bogdanova, T.I.; Oliynik, V.A.; Lubin, J.H.; Zablotska, L.B.; Tereschenko, V.P.; McConnell, R.J.; Zamotaeva, G.A.; et al. I-131 dose response for incident thyroid cancers in Ukraine related to the Chernobyl accident. Environ. Health Perspect. 2011, 119, 933–939. [Google Scholar] [CrossRef] [PubMed]
- Ivanov, V.K.; Kashcheev, V.V.; Chekin, S.Y.; Maksioutov, M.A.; Tumanov, K.A.; Vlasov, O.K.; Shchukina, N.V.; Tsyb, A.F. Radiation-epidemiological studies of thyroid cancer incidence in Russia after the Chernobyl accident (Estimation of radiation risks, 1991–2008 follow-up period). Radiat. Prot. Dosim. 2012, 151, 489–499. [Google Scholar] [CrossRef] [PubMed]
- Zablotska, L.B.; Ron, E.; Rozhko, A.V.; Hatch, M.; Polyanskaya, O.N.; Brenner, A.V.; Lubin, J.; Romanov, G.N.; McConnell, R.J.; O’Kane, P.; et al. Thyroid cancer risk in Belarus among children and adolescents exposed to radioiodine after the Chornobyl accident. Br. J. Cancer 2011, 104, 181–187. [Google Scholar] [CrossRef]
- Ron, E.; Lubin, J.H.; Shore, R.E.; Mabuchi, K.; Modan, B.; Pottern, L.M.; Schneider, A.B.; Tucker, M.A.; Boice, J.D., Jr. Thyroid cancer after exposure to external radiation: A pooled analysis of seven studies. Radiat. Res. 1995, 141, 259–277. [Google Scholar] [CrossRef] [PubMed]
- Tronko, M.; Brenner, A.V.; Bogdanova, T.; Shpak, V.; Oliynyk, V.; Cahoon, E.K.; Drozdovitch, V.; Little, M.P.; Tereshchenko, V.; Zamotayeva, G.; et al. Thyroid neoplasia risk is increased bearly 30 years after the Chernobyl accident. Int. J. Cancer 2017, 141, 1585–1588. [Google Scholar] [CrossRef]
- Thomas, G. Radiation and thyroid cancer-an overview. Radiat. Prot. Dosim. 2018, 182, 53–57. [Google Scholar] [CrossRef] [PubMed]
- Weiss, W. Chernobyl thyroid cancer: 30 years of follow-up overview. Radiat. Prot. Dosim. 2018, 182, 58–61. [Google Scholar] [CrossRef]
- 1986–2016: Chernobyl at 30, WHO. 2016. Available online: https://www.who.int/ionizing_radiation/chernobyl/Chernobyl-update.pdf (accessed on 25 April 2016).
- Demidchik, Y.E.; Saenko, V.A.; Yamashita, S. Childhood thyroid cancer in Belarus, Russia, and Ukraine after Chernobyl and at present. Arq. Bras. Endocrinol. Metab. 2007, 51, 748–762. [Google Scholar] [CrossRef]
- Cardis, E.; Kesminiene, A.; Ivanov, V.; Malakhova, I.; Shibata, Y.; Khrouch, V.; Drozdovitch, V.; Maceika, E.; Zvonova, I.; Vlassov, O.; et al. Risk of thyroid cancer after exposure to 131I in childhood. J. Natl. Cancer Inst. 2005, 97, 724–732. [Google Scholar] [CrossRef]
- Tronko, M.D.; Howe, G.R.; Bogdanova, T.I.; Bouville, A.C.; Epstein, O.V.; Brill, A.B.; Likhtarev, I.A.; Fink, D.J.; Markov, V.V.; Greenebaum, E.; et al. A cohort study of thyroid cancer and other thyroid diseases after the chornobyl accident: Thyroid cancer in Ukraine detected during first screening. J. Natl. Cancer Inst. 2006, 98, 897–903. [Google Scholar] [CrossRef]
- Ron, E. Thyroid cancer incidence among people living in areas contaminated by radiation from the Chernobyl accident. Health Phys. 2007, 93, 502–511. [Google Scholar] [CrossRef]
- Likhtarov, I.; Kovgan, L.; Vavilov, S.; Chepurny, M.; Ron, E.; Lubin, J.; Bouville, A.; Tronko, N.; Bogdanova, T.; Gulak, L.; et al. Post-Chernobyl thyroid cancers in Ukraine. Report 2: Risk analysis. Radiat. Res. 2006, 166, 375–386. [Google Scholar] [CrossRef]
- Yamashita, S.; Saenko, V. Mechanisms of disease: Molecular genetics of childhood thyroid cancers. Nat. Rev. Endocrinol. 2007, 3, 422–429. [Google Scholar] [CrossRef] [PubMed]
- Tuttle, R.M.; Vaisman, F.; Tronko, M.D. Clinical presentation and clinical outcomes in Chernobyl-related paediatric thyroid cancers: What do we know now? What can we expect in the future? Clin. Oncol. 2011, 23, 268–275. [Google Scholar] [CrossRef] [PubMed]
- Williams, E.D.; Abrosimov, A.; Bogdanova, T.; Demidchik, E.P.; Ito, M.; LiVolsi, V.; Lushnikov, E.; Rosai, J.; Tronko, M.D.; Tsyb, A.F.; et al. Morphologic characteristics of Chernobyl-related childhood papillary thyroid carcinomas are independent of radiation exposure but vary with iodine intake. Thyroid 2008, 18, 847–852. [Google Scholar] [CrossRef] [PubMed]
- Bogdanova, T.I.; Saenko, V.A.; Brenner, A.V.; Zurnadzhy, L.Y.; Rogounovitch, T.I.; Likhtarov, I.A.; Masiuk, S.V.; Kovgan, L.M.; Shpak, V.M.; Thomas, G.A.; et al. Comparative histopathologic analysis of “radiogenic” and “sporadic” papillary thyroid carcinoma: Patients born before and after the Chernobyl accident. Thyroid 2018, 28, 880–890. [Google Scholar] [CrossRef] [PubMed]
- Suzuki, K.; Mitsutake, N.; Saenko, V.; Yamashita, S. Radiation signatures in childhood thyroid cancers after the Chernobyl accident: Possible roles of radiation in carcinogenesis. Cancer Sci. 2015, 106, 127–133. [Google Scholar] [CrossRef] [PubMed]
- Fugazzola, L.; Pilotti, S.; Pinchera, A.; Vorontsova, T.V.; Mondellini, P.; Bongarzone, I.; Greco, A.; Astakhova, L.; Butti, M.G.; Demidchik, E.P.; et al. Oncogenic rearrangements of the RET proto-oncogene in papillary thyroid carcinomas from children exposed to the Chernobyl nuclear accident. Cancer Res. 1995, 55, 5617–5620. [Google Scholar] [PubMed]
- Klugbauer, S.; Lengfelder, E.; Demidchik, E.P.; Rabes, H.M. High prevalence of RET rearrangement in thyroid tumors of children from Belarus after the Chernobyl reactor accident. Oncogene 1995, 11, 2459–2467. [Google Scholar] [PubMed]
- Nikiforov, Y.E.; Rowland, J.M.; Bove, K.E.; Monforte-Munoz, H.; Fagin, J.A. Distinct pattern of ret oncogene rearrangements in morphological variants of radiation-induced and sporadic thyroid papillary carcinomas in children. Cancer Res. 1997, 57, 1690–1694. [Google Scholar] [PubMed]
- Pisarchik, A.V.; Ermak, G.; Demidchik, E.P.; Mikhalevich, L.S.; Kartel, N.A.; Figge, J. Low prevalence of the ret/PTC3r1 rearrangement in a series of papillary thyroid carcinomas presenting in Belarus ten years post-Chernobyl. Thyroid 1998, 8, 1003–1008. [Google Scholar] [CrossRef] [PubMed]
- Nikiforov, Y.E.; Nikiforova, M.N. Molecular genetics and diagnosis of thyroid cancer. Nat. Rev. Endocrinol. 2011, 7, 569–580. [Google Scholar] [CrossRef]
- Santoro, M.; Carlomagno, F. Oncogenic rearrangements driving ionizing radiation-associated human cancer. J. Clin. Invest. 2013, 11, 4566–4568. [Google Scholar] [CrossRef] [PubMed]
- Kodama, Y.; Asai, N.; Kawai, K.; Jijiwa, M.; Murakumo, Y.; Ichihara, M.; Takahashi, M. The RET proto-oncogene: A molecular therapeutic target in thyroid cancer. Cancer Sci. 2005, 96, 143–148. [Google Scholar] [CrossRef] [PubMed]
- Nikiforov, Y.E. Thyroid cancer in 2015: Molecular landscape of thyroid cancer continues to be deciphered. Nat. Rev. Endocrinol. 2016, 12, 67–68. [Google Scholar] [CrossRef] [PubMed]
- Romei, C.; Ciampi, R.; Elisei, R. A comprehensive overview of the role of the RET proto-oncogene in thyroid carcinoma. Nat. Rev. Endocrinol. 2016, 12, 192–202. [Google Scholar] [CrossRef] [PubMed]
- Zitzelsberger, H.; Bauer, V.; Thomas, G.; Unger, K. Molecular rearrangements in papillary thyroid carcinomas. Clin. Chim. Acta 2010, 411, 301–308. [Google Scholar] [CrossRef]
- Menicali, E.; Moretti, S.; Voce, P.; Romagnoli, S.; Avenia, N.; Puxeddu, E. Intracellular signal transduction and modification of the tumor microenvironment induced by RET/PTCs in papillary thyroid carcinoma. Front. Endocrinol. 2012, 3, 1–23. [Google Scholar] [CrossRef] [PubMed]
- Santoro, M.; Carlomagno, F. Central role of RET in thyroid cancer. Cold Spring Harb. Perspect. Biol. 2013, 5, 1–17. [Google Scholar] [CrossRef] [PubMed]
- Mulligan, L.M. RET revisited: Expanding the oncogenic portfolio. Nat. Rev. Cancer 2014, 14, 173–186. [Google Scholar] [CrossRef]
- Ricarte-Filho, J.C.; Li, S.; Garcia-Rendueles, M.E.; Montero-Conde, C.; Voza, F.; Knauf, J.A.; Heguy, A.; Viale, A.; Bogdanova, T.; Thomas, G.A.; et al. Identification of kinase fusion oncogenes in Post-Chernobyl radiation-induced thyroid cancers. J. Clin. Invest. 2013, 123, 4935–4944. [Google Scholar] [CrossRef] [PubMed]
- Leeman-Neill, R.J.; Kelly, L.M.; Liu, P.; Brenner, A.V.; Little, M.P.; Bogdanova, T.I.; Evdokimova, V.N.; Hatch, M.; Zurnadzy, L.Y.; Nikiforova, M.N.; et al. ETV6-NTRK3 is a common chromosomal rearrangement in radiation-associated thyroid cancer. Cancer 2014, 120, 799–807. [Google Scholar] [CrossRef]
- Arndt, A.; Steinestel, K.; Rump, A.; Sroya, M.; Bogdanova, T.; Kovgan, L.; Port, M.; Abend, M.; Eder, S. Anaplastic lymphoma kinase (ALK) gene rearrangements in radiation-related human papillary thyroid carcinoma after the Chernobyl accident. J. Pathol. Clin. Res. 2018, 4, 175–183. [Google Scholar] [CrossRef] [PubMed]
- Efanov, A.A.; Brenner, A.V.; Bogdanova, T.I.; Kelly, L.M.; Liu, P.; Little, M.P.; Wald, A.I.; Hatch, M.; Zurnadzy, L.Y.; Nikiforova, M.N.; et al. Investigation of the relationship between radiation dose and gene mutations and fusions in Post-Chernobyl thyroid cancer. J. Natl. Cancer Inst. 2018, 110, 371–378. [Google Scholar] [CrossRef]
- Xing, M. BRAF mutation in thyroid cancer. Endocr. Relat. Cancer 2005, 12, 245–262. [Google Scholar] [CrossRef] [PubMed]
- Handkiewicz-Junak, D.; Swierniak, M.; Rusinek, D.; Oczko-Wojciechowska, M.; Dom, G.; Maenhaut, C.; Unger, K.; Detours, V.; Bogdanova, T.; Thomas, G.; et al. Gene signature of the Post-Chernobyl papillary thyroid cancer. Eur. J. Nucl. Med. Mol. Imaging 2016, 43, 1267–1277. [Google Scholar] [CrossRef] [PubMed]
- Yamashita, S.; Suzuki, S.; Suzuki, S.; Shimura, H.; Saenko, V. Lessons from Fukushima: Latest findings of thyroid cancer after the Fukushima nuclear power plant accident. Thyroid 2018, 28, 11–22. [Google Scholar] [CrossRef] [PubMed]
- Mitsutake, N.; Fukushima, T.; Matsuse, M.; Rogounovitch, T.; Saenko, V.; Uchino, S.; Ito, K.; Suzuki, K.; Suzuki, S.; Yamashita, S. BRAFV600E mutation is highly prevalent in thyroid carcinomas in the young population in Fukushima: A different oncogenic profile from Chernobyl. Sci. Rep. 2015, 5, 19675. [Google Scholar] [CrossRef] [PubMed]
- Furukawa, K.; Preston, D.; Funamoto, S.; Yonehara, S.; Ito, M.; Tokuoka, S.; Sugiyama, H.; Soda, M.; Ozasa, K.; Mabuchi, K. Long-term trend of thyroid cancer risk among Japanese atomic-bomb survivors: 60 years after exposure. Int. J. Cancer 2013, 132, 1222–1226. [Google Scholar] [CrossRef] [PubMed]
- Hamatani, K.; Eguchi, H.; Ito, R.; Mukai, M.; Takahashi, K.; Taga, M.; Imai, K.; Cologne, J.; Soda, M.; Arihiro, K.; et al. RET/PTC rearrangements preferentially occurred in papillary thyroid cancer among atomic bomb survivors exposed to high radiation dose. Cancer Res. 2008, 68, 7176–7182. [Google Scholar] [CrossRef]
- Hamatani, K.; Mukai, M.; Takahashi, K.; Hayashi, Y.; Nakachi, K.; Kusunoki, Y. Rearranged anaplastic lymphoma kinase (ALK) gene in adult-onset papillary thyroid cancer amongst atomic bomb survivors. Thyroid 2012, 22, 1153–1159. [Google Scholar] [CrossRef]
- Hamatani, K.; Eguchi, H.; Koyama, K.; Mukai, M.; Nakachi, K.; Kusunoki, Y. A novel RET rearrangement (ACBD5/RET) by pericentric inversion, inv(10) (p12.1;q11.2), in papillary thyroid cancer from an atomic bomb survivor exposed to high-dose radiation. Oncol. Rep. 2014, 32, 1809–1814. [Google Scholar] [CrossRef][Green Version]
- Ron, E.; Modan, B.; Preston, D.; Alfandary, E.; Stovall, M.; Boice, J.D. Thyroid neoplasia following radiation in childhood. Radiat. Res. 1989, 120, 516–531. [Google Scholar] [CrossRef]
- Bounacer, A.; Wicker, R.; Caillou, B.; Cailleux, A.F.; Sarasin, A.; Schlumberger, M.; Suarez, H.G. High prevalence of activating ret proto-oncogene rearrangements, in thyroid tumors from patients who had received external radiation. Oncogene 1997, 15, 1263–1273. [Google Scholar] [CrossRef]
- Collins, B.J.; Chiappetta, G.; Schneider, A.B.; Santoro, M.; Pentimalli, F.; Fogelfeld, L.; Gierlowski, T.; Shore-Freedman, E.; Jaffe, G.; Fusco, A. RET expression in papillary thyroid cancer from patients irradiated in childhood for benign conditions. J. Clin. Endocrinol. Metab. 2002, 87, 3941–3946. [Google Scholar] [CrossRef] [PubMed]
- Sadetzki, S.; Calderon-Margalit, R.; Modan, B.; Srivastava, S.; Tuttle, R.M. Ret/PTC activation in benign and malignant thyroid tumors rising in a population in childhood. J. Clin. Endocrinol. Metab. 2004, 89, 2281–2289. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Nikiforova, M.N.; Stringer, J.R.; Blough, R.; Medvedovic, M.; Fagin, J.A.; Nikiforov, Y.E. Proximity of chromosomal loci that participate in radiation-induced rearrangements in human cells. Science 2000, 290, 138–141. [Google Scholar] [CrossRef] [PubMed]
- Gandhi, M.; Medvedovic, M.; Stringer, J.R.; Nikiforov, Y.E. Interphase chromosome folding determines spatial proximity of genes participating in carcinogenic RET/PTC rearrangements. Oncogene 2006, 25, 2360–2366. [Google Scholar] [CrossRef] [PubMed]
- Ito, T.; Seyama, T.; Iwamoto, K.S.; Hayashi, T.; Mizuno, T.; Tsuyama, N.; Dohi, K.; Nakamura, N.; Akiyama, M. In vitro irradiation is able to cause RET oncogene rearrangement. Cancer Res. 1993, 53, 2940–2943. [Google Scholar] [PubMed]
- Mizuno, T.; Iwamoto, K.S.; Kyoizumi, S.; Nagamura, H.; Shinohara, T.; Koyama, K.; Seyama, T.; Hamatani, K. Preferential induction of RET/PTC rearrangement by X-ray irradiation. Oncogene 2000, 19, 438–443. [Google Scholar] [CrossRef]
- Caudill, C.M.; Zhu, Z.; Ciampi, R.; Stringer, J.R.; Nikiforov, Y.E. Dose-dependent generation of RET/PTC in human thyroid cells after in vitro exposure to gamma-radiation: A model of carcinogenic chromosomal rearrangement induced by ionizing radiation. J. Clin. Endocrinol. Metab. 2005, 90, 2364–2369. [Google Scholar] [CrossRef] [PubMed]
- Nikiforova, M.N.; Ciampi, R.; Salvatore, G.; Santoro, M.; Gandhi, M.; Knauf, J.A.; Thomas, G.A.; Jeremiah, S.; Bogdanova, T.I.; Tronko, M.D.; et al. Low prevalence of BRAF mutations in radiation-induced thyroid tumors in contrast to sporadic papillary carcinomas. Cancer Lett. 2004, 209, 1–6. [Google Scholar] [CrossRef]
- Cordioli, M.I.; Moraes, L.; Cury, A.N.; Cerutti, J.M. Are we really at the dawn of understanding sporadic pediatric thyroid carcinoma? Endocr. Relat. Cancer 2015, 22, R311–R324. [Google Scholar] [CrossRef]
- Thomas, G.A.; Bunnell, H.; Cook, H.A.; Williams, E.D.; Nerovnya, A.; Cherstvoy, E.D.; Tronko, N.D.; Bogdanova, T.I.; Chiappetta, G.; Viglietto, G.; et al. High prevalence of RET/PTC rearrangements in Ukrainian and Belarussian Post-Chernobyl thyroid papillary carcinomas: A strong correlation between RET/PTC3 and the solid-follicular variant. J. Clin. Endocrinol. Metab. 1999, 84, 4232–4238. [Google Scholar] [CrossRef]
- Elisei, R.; Romei, C.; Vorontsova, T.; Cosci, B.; Veremeychik, V.; Kuchinskaya, E.; Basolo, F.; Demidchik, E.P.; Miccoli, P.; Pinchera, A.; et al. RET/PTC rearrangements in thyroid nodules: Studies in irradiated and not irradiated, malignant and benign thyroid lesions in children and adults. J. Clin. Endocrinol. Metab. 2001, 86, 3211–3216. [Google Scholar]
- Rabes, H.M.; Demidchik, E.P.; Sidorow, J.D.; Lengfelder, E.; Beimfohr, C.; Hoelzel, D.; Klugbauer, S. Pattern of radiation-induced RET and NTRK1 rearrangements in Post-Chernobyl papillary thyroid carcinomas: Biological, phenotypic, and clinical implications. Clin. Cancer Res. 2000, 6, 1093–1103. [Google Scholar] [PubMed]
- Fenton, C.L.; Lukes, Y.; Nicholson, D.; Dinauer, C.A.; Francis, G.L.; Tuttle, R.M. The ret/ptc mutations are common in sporadic papillary thyroid carcinoma of children and young adults. J. Clin. Endocrinol. Metab. 2000, 85, 1170–1175. [Google Scholar] [CrossRef] [PubMed]
- Nikita, M.E.; Jiang, W.; Cheng, S.M.; Hantash, F.M.; McPhaul, M.J.; Newbury, R.O.; Phillips, S.A.; Reitz, R.E.; Waldman, F.M.; Newfield, R.S. Mutational analysis in pediatric thyroid cancer and correlations with age, ethnicity, and clinical presentation. Thyroid 2016, 26, 227–234. [Google Scholar] [CrossRef] [PubMed]
- Cordioli, M.I.; Moraes, L.; Bastos, A.U.; Besson, P.; Alves, M.T.; Delcelo, R.; Monte, O.; Longui, C.; Cury, A.N.; Cerutti, J.M. Fusion oncogenes are the main genetic events found in sporadic papillary thyroid carcinomas from children. Thyroid 2017, 27, 182–188. [Google Scholar] [CrossRef] [PubMed]
- Pekova, B.; Dvorakova, S.; Sykorova, V.; Vacinova, G.; Vaclavikova, E.; Moravcova, J.; Katra, R.; Vlcek, P.; Sykorova, P.; Kodetova, D.; et al. Somatic genetic alterations in a large cohort of pediatric thyroid nodules. Endocr. Connect. 2019, 8, 796–805. [Google Scholar] [CrossRef]
- Tronko, M.; Bogdanova, T.; Voskoboynyk, L.; Zurnadzhy, L.; Shpak, V.; Gulak, L. Radiation induced thyroid cancer: Fundamental and applied aspects. Exp. Oncol. 2010, 32, 200–204. [Google Scholar] [PubMed]
- Dinets, A.; Hulchiy, M.; Sofiadis, A.; Ghaderi, M.; Höög, A.; Larsson, C.; Zedenius, J. Clinical, genetic, and immunohistochemical characterization of 70 Ukrainian adult cases with Post-Chornobyl papillary thyroid carcinoma. Eur. J. Endocrinol. 2012, 166, 1049–1060. [Google Scholar] [CrossRef] [PubMed]
- Jung, C.K.; Little, M.P.; Lubin, J.H.; Brenner, A.V.; Wells, S.A.; Sigurdson, A.J.; Nikiforov, Y.E. The increase in thyroid cancer incidence during the last four decades is accompanied by a high frequency of BRAF mutations and a sharp increase in RAS mutations. J. Clin. Endocrinol. Metab. 2014, 99, e276–e285. [Google Scholar] [CrossRef] [PubMed]
- Vuong, H.G.; Altibi, A.M.A.; Sbdelhamid, A.H.; Ngoc, P.U.D.; Quan, V.D.; Tantawi, M.Y.; Elfil, M.; Vu, T.L.H.; Elgebaly, A.; Oishi, N.; et al. The changing characteristics and molecular profiles of papillary thyroid carcinoma over time: A systematic review. Oncotarget 2017, 8, 10637–10649. [Google Scholar] [CrossRef]
- Powell, N.; Jeremiah, S.; Morishita, M.; Dudley, E.; Bethel, J.; Bogdanova, T.; Tronko, M.; Thomas, G. Frequency of BRAF T1796A mutation in papillary thyroid carcinoma relates to age of patient at diagnosis and not to radiation exposure. J. Pathol. 2005, 205, 558–564. [Google Scholar] [CrossRef]
- Tuttle, R.M.; Lukes, Y.; Onstad, L.; Lushnikov, E.; Abrosimov, A.; Troshin, V.; Tsyb, A.; Davis, S.; Kopecky, K.J.; Francis, G. Ret/PTC activation is not associated with individual radiation dose estimates in a pilot study of neoplastic thyroid nodules arising in Russian children and adults exposed to Chernobyl fallout. Thyroid 2008, 18, 839–846. [Google Scholar] [CrossRef]
- Reddi, H.V.; McIver, B.; Grebe, S.K.; Eberhardt, N.L. The paired box-8/peroxisome proliferator-activated receptor-gamma oncogene in thyroid tumorigenesis. Endocrinology 2007, 148, 932–935. [Google Scholar] [CrossRef][Green Version]
- Raman, P.; Koenig, R.J. PAX8-PPAR γ fusion protein in thyroid carcinoma. Nat. Rev. Endocrinol. 2014, 10, 616–623. [Google Scholar] [CrossRef]
- Leeman-Neill, R.J.; Brenner, A.V.; Little, M.P.; Bogdanova, T.I.; Hatch, M.; Zurnadzy, L.Y.; Mabuchi, K.; Tronko, M.D.; Nikiforov, Y.E. RET/PTC and PAX8/PPARγ chromosomal rearrangements in post-Chernobyl thyroid cancer and their association with iodine-131 radiation dose and other characteristics. Cancer 2013, 119, 1792–1799. [Google Scholar] [CrossRef]
- Hess, J.; Thomas, G.; Braselmann, H.; Bauer, V.; Bogdanova, T.; Wienberg, J.; Zitzelsberger, H.; Unger, K. Gain of chromosome band 7q11 in papillary thyroid carcinomas of young patients is associated with exposure to low-dose irradiation. Proc. Natl. Acad. Sci. USA 2011, 108, 9595–9600. [Google Scholar] [CrossRef]
- Selmansberger, M.; Feuchtinger, A.; Zurnadzhy, L.; Michna, A.; Kaiser, J.C.; Abend, M.; Brenner, A.; Bogdanova, T.; Walch, A.; Unger, K.; et al. CLIP2 as radiation biomarker in papillary thyroid carcinoma. Oncogene 2015, 34, 3917–3925. [Google Scholar] [CrossRef]
- Takahashi, M.; Saenko, V.A.; Rogounovitch, T.I.; Kawaguchi, T.; Drozd, V.M.; Takigawa-Imamura, H.; Akulevich, N.M.; Ratanajaraya, C.; Mitsutake, N.; Takamura, N.; et al. The FOXE1 locus is a major genetic determinant for radiation-related thyroid carcinoma in Chernobyl. Hum. Mol. Genet. 2010, 19, 2516–2523. [Google Scholar] [CrossRef]
| Oncogenes | Rearrangement Partners | Chromosome Location | Type of Rearrangements |
|---|---|---|---|
| RET rearrangements | |||
| RET/PTC1 | CCDC6 (also H4) | 10q11.21/10q21 | Inversion |
| RET/PTC2 | PRKAR1A | 10q11.21/17q24.2 | Translocation |
| RET/PTC3 | NCOA4 (also Ele) | 10q11.21/10q11.22 | Inversion |
| RET/PTC4 | NCOA4 (also Ele) | 10q11.21/10q11.22 | Inversion |
| RET/PTC5 | GOLGA5 (also RFG5) | 10q11.21/14q32.12 | Translocation |
| RET/PTC6 | TRIM24 | 10q11.21/7q32-q34 | Translocation |
| RET/PTC7 | TRIM33 (also RFG7) | 10q11.21/1p13.1 | Translocation |
| RET/PTC8 | KTN1 | 10q11.21/14q22.1 | Translocation |
| RET/PTC9 | RFG9 (also MBD1) | 10q11.21/18q21 | Translocation |
| SPECC1L-RET | SPECC1L | 22q11.23/10q11.21 | Translocation |
| SQSTM1-RET | SQSTM1 | 5q35.3/10q11.21 | Translocation |
| BRAF rearrangements | |||
| AKAP9/BRAF | AKAP9 | 7q21.2/7q34 | Inversion |
| AGK/BRAF | AGK | 7q34/7q34 | Inversion |
| SND1-BRAF | SND1 | 7q32.1/7q34 | Inversion |
| MBP-BRAF | MBP | 18q23/7q34 | Translocation |
| POR-BRAF | POR | 7q11.23/7q34 | Inversion |
| ZBTB8A-BRAF | ZBTB8A | 1p35.1/7q34 | Translocation |
| MACF-BRAF | MACF1 | 1p34.3/7q34 | Translocation |
| NTRK rearrangements | |||
| TPR/NTRK1 | TPR | 1q31.1/1q23.1 | Inversion |
| BANP-NTRK1 | BANP | 16q24.2/1q23.1 | Translocation |
| ETV6/NTRK3 | ETV6 | 12p13.1/15q25.3 | Translocation |
| PPARg rearrangements | |||
| PAX8/PPARg | PAX8 | 2q14.1/3p25.2 | Translocation |
| CREB3L2/PPARg | CREB3L2 | 7q33/3p25.2 | Translocation |
| Other rearrangements | |||
| STRN-ALK | ALK | 2p22.2/2p23.2-p23.1 | Inversion |
| THADA-IGF2BP3 | 2p21/7p15.3 | Translocation | |
| Studies | Prevalence (Positive Cases/Total (%)) | ||
|---|---|---|---|
| RET/PTC1 Rearrangement | Ref | ||
| Chernobyl-related | Sporadic | ||
| Nikiforov et al. (1997) | 5/22 | 6/14 | 27 |
| Thomas et al. (1999) | 12/63 | 61 | |
| Rabes et al. (2000) | 40/172 | 62 | |
| Elisei et al. (2001) | 6/25 | 5/25 | 63 |
| Ricarte-Filho et al. (2013) | 3/18 | 1/18 | 38 |
| Leeman-Neill et al. (2013) | 14/62 | 76 | |
| Total | 80/362 (22.1) | 12/57 (21.1) | |
© 2019 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Suzuki, K.; Saenko, V.; Yamashita, S.; Mitsutake, N. Radiation-Induced Thyroid Cancers: Overview of Molecular Signatures. Cancers 2019, 11, 1290. https://doi.org/10.3390/cancers11091290
Suzuki K, Saenko V, Yamashita S, Mitsutake N. Radiation-Induced Thyroid Cancers: Overview of Molecular Signatures. Cancers. 2019; 11(9):1290. https://doi.org/10.3390/cancers11091290
Chicago/Turabian StyleSuzuki, Keiji, Vladimir Saenko, Shunichi Yamashita, and Norisato Mitsutake. 2019. "Radiation-Induced Thyroid Cancers: Overview of Molecular Signatures" Cancers 11, no. 9: 1290. https://doi.org/10.3390/cancers11091290
APA StyleSuzuki, K., Saenko, V., Yamashita, S., & Mitsutake, N. (2019). Radiation-Induced Thyroid Cancers: Overview of Molecular Signatures. Cancers, 11(9), 1290. https://doi.org/10.3390/cancers11091290





