EV-Associated miRNAs from Peritoneal Lavage are a Source of Biomarkers in Endometrial Cancer
Abstract
1. Introduction
2. Results
3. Discussion
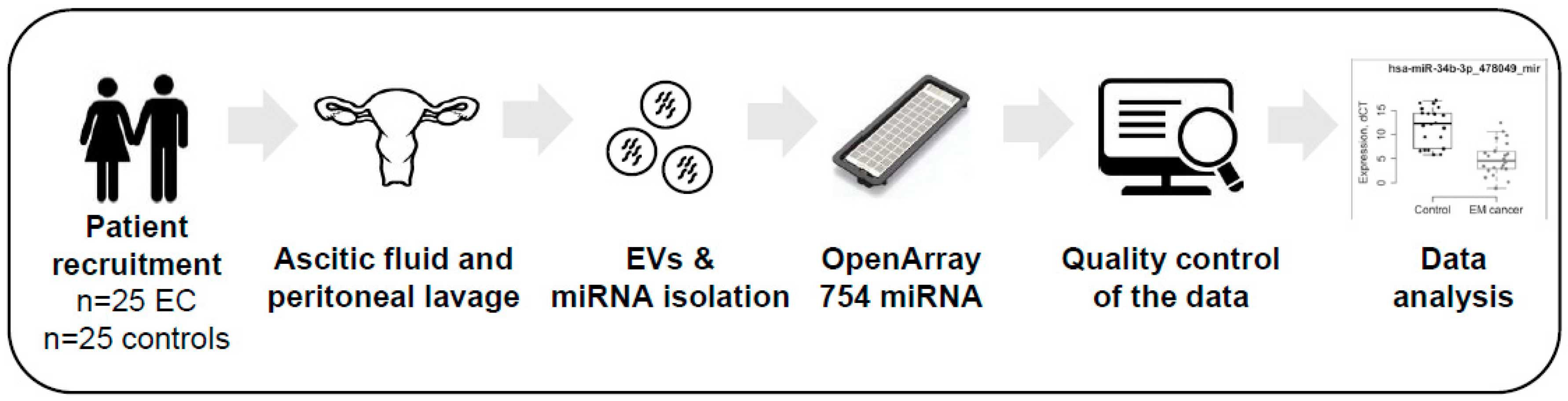
4. Materials and Methods
4.1. Patients and Ascitic Fluid and Peritoneal Lavage Collection
4.2. EV Isolation
4.3. Nanoparticle Tracking Analysis
4.4. Total RNA Extraction and OpenArray Analysis
4.5. Preprocessing and Differential Expression Analysis
4.6. Development of Predictors
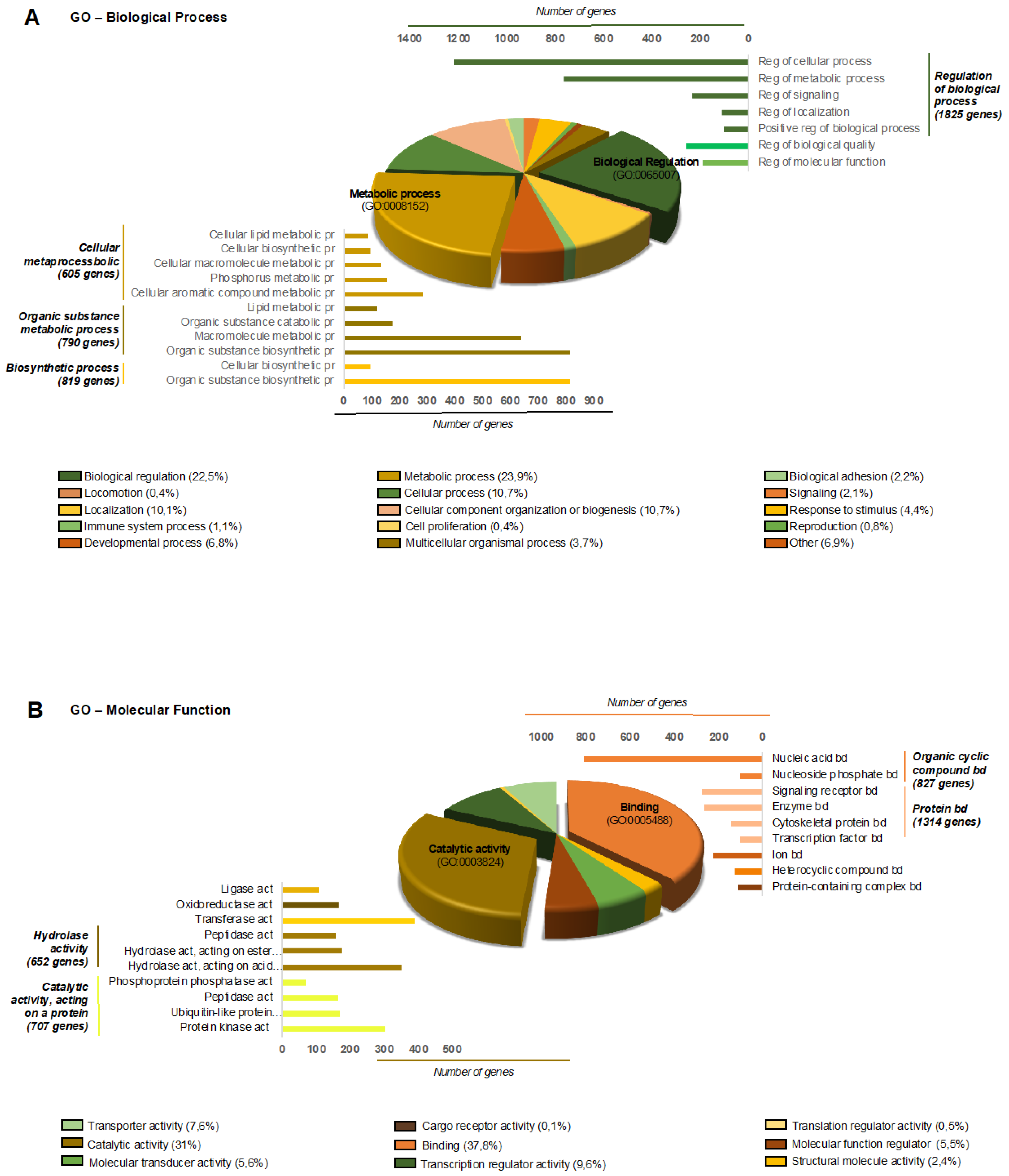
4.7. miRNA Target Gene Prediction and Bioinformatics Analysis
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- Bray, F.; Ferlay, J.; Soerjomataram, I.; Siegel, R.L.; Torre, L.A.; Jemal, A. Global cancer statistics 2018: GLOBOCAN estimates of incidence and mortality worldwide for 36 cancers in 185 countries. CA Cancer J. Clin. 2018, 68, 394–424. [Google Scholar] [CrossRef]
- Amant, F.; Moerman, P.; Neven, P.; Timmerman, D.; Van Limbergen, E.; Vergote, I. Endometrial cancer. Lancet 2005, 366, 491–505. [Google Scholar] [CrossRef]
- Siegel, R.L.; Miller, K.D.; Jemal, A. Cancer statistics, 2018. CA Cancer J. Clin. 2018, 68, 7–30. [Google Scholar] [CrossRef] [PubMed]
- Vitale, S.G.; Rossetti, D.; Tropea, A.; Biondi, A.; Laganà, A.S. Fertility sparing surgery for stage IA type I and G2 endometrial cancer in reproductive-aged patients: Evidence-based approach and future perspectives. Updates Surg. 2017, 69, 29–34. [Google Scholar] [CrossRef] [PubMed]
- Montagnana, M.; Benati, M.; Danese, E.; Giudici, S.; Perfranceschi, M.; Ruzzenenete, O.; Salvagno, G.L.; Bassi, A.; Gelati, M.; Paviati, E.; et al. Aberrant MicroRNA Expression in Patients with Endometrial Cancer. Int. J. Gynecol. Cancer 2017, 27, 459–466. [Google Scholar] [CrossRef]
- Banno, K.; Yanokura, M.; Kisu, I.; Yamagami, W.; Susumu, N.; Aoki, D. MicroRNAs in endometrial cancer. Int. J. Clin. Oncol. 2013, 18, 186–192. [Google Scholar] [CrossRef] [PubMed]
- Wilczynski, M.; Danielska, J.; Dzieniecka, M.; Szymanska, B.; Wojciechowski, M.; Malinowski, A. Prognostic and Clinical Significance of miRNA-205 in Endometrioid Endometrial Cancer. PLoS ONE 2016, 11, e0164687. [Google Scholar] [CrossRef]
- Vasilatou, D.; Sioulas, V.D.; Pappa, V.; Papageorgiou, S.G.; Vlahos, N.F. The role of miRNAs in endometrial cancer. Epigenomics 2015, 7, 951–959. [Google Scholar] [CrossRef] [PubMed]
- Muinelo-Romay, L.; Casas-Arozamena, C.; Abal, M. Liquid Biopsy in Endometrial Cancer: New Opportunities for Personalized Oncology. Int. J. Mol. Sci. 2018, 19, 2311. [Google Scholar] [CrossRef] [PubMed]
- Yáñez-Mó, M.; Siljander, P.R.-M.; Andreu, Z.; Bedina Zavec, A.; Borràs, F.E.; Buzas, E.I.; Buzas, K.; Casal, E.; Cappello, F.; Carvalho, J.; et al. Biological properties of extracellular vesicles and their physiological functions. J. Extracell. Vesicles 2015, 4, 27066. [Google Scholar] [CrossRef]
- Gilabert-Estelles, J.; Braza-Boils, A.; Ramon, L.A.; Zorio, E.; Medina, P.; Espana, F. Estelles Role of microRNAs in Gynecological Pathology. Curr. Med. Chem. 2012, 19, 2406–2413. [Google Scholar] [CrossRef] [PubMed]
- Torres, A.; Torres, K.; Pesci, A.; Ceccaroni, M.; Paszkowski, T.; Cassandrini, P.; Zamboni, G.; Maciejewski, R. Deregulation of miR-100, miR-99a and miR-199b in tissues and plasma coexists with increased expression of mTOR kinase in endometrioid endometrial carcinoma. BMC Cancer 2012, 12, 369. [Google Scholar] [CrossRef] [PubMed]
- Zavesky, L.; Jandakova, E.; Turyna, R.; Langmeierova, L.; Weinberger, V.; Minar, L. Supernatant versus exosomal urinary microRNAs. Two fractions with different outcomes in gynaecological cancers. Neoplasma 2016, 63, 121–132. [Google Scholar] [CrossRef] [PubMed]
- Théry, C.; Amigorena, S.; Raposo, G.; Clayton, A. Isolation and Characterization of Exosomes from Cell Culture Supernatants and Biological Fluids. Curr. Protoc. Cell Biol. 2006, 30, 3.22.1–3.22.29. [Google Scholar] [CrossRef] [PubMed]
- Srivastava, A.; Moxley, K.; Ruskin, R.; Dhanasekaran, D.N.; Zhao, Y.D.; Ramesh, R. A Non-invasive Liquid Biopsy Screening of Urine-Derived Exosomes for miRNAs as Biomarkers in Endometrial Cancer Patients. AAPS J. 2018, 20, 82. [Google Scholar] [CrossRef] [PubMed]
- Xu, H.; Gong, Z.; Shen, Y.; Fang, Y.; Zhong, S. Circular RNA expression in extracellular vesicles isolated from serum of patients with endometrial cancer. Epigenomics 2018, 10, 187–197. [Google Scholar] [CrossRef]
- Martinez-Garcia, E.; Lesur, A.; Devis, L.; Cabrera, S.; Matias-Guiu, X.; Hirschfeld, M.; Asberger, J.; van Oostrum, J.; de los Ángeles Casares de Cal, M.; Gómez-Tato, A.; et al. Targeted Proteomics Identifies Proteomic Signatures in Liquid Biopsies of the Endometrium to Diagnose Endometrial Cancer and Assist in the Prediction of the Optimal Surgical Treatment. Clin. Cancer Res. 2017, 23, 6458–6467. [Google Scholar] [CrossRef] [PubMed]
- Hiroki, E.; Akahira, J.; Suzuki, F.; Nagase, S.; Ito, K.; Suzuki, T.; Sasano, H.; Yaegashi, N. Changes in microRNA expression levels correlate with clinicopathological features and prognoses in endometrial serous adenocarcinomas. Cancer Sci. 2010, 101, 241–249. [Google Scholar] [CrossRef]
- Misso, G.; Di Martino, M.T.; De Rosa, G.; Farooqi, A.A.; Lombardi, A.; Campani, V.; Zarone, M.R.; Gullà, A.; Tagliaferri, P.; Tassone, P.; et al. Mir-34: A New Weapon Against Cancer? Mol. Ther. Nucleic Acids 2014, 3, e195. [Google Scholar] [CrossRef]
- Korpal, M.; Kang, Y. The emerging role of miR-200 family of MicroRNAs in epithelial-mesenchymal transition and cancer metastasis. RNA Biol. 2008, 5, 115–119. [Google Scholar] [CrossRef]
- Laganà, A.S.; Vitale, S.G.; Salmeri, F.M.; Triolo, O.; Ban Frangež, H.; Vrtačnik-Bokal, E.; Stojanovska, L.; Apostolopoulos, V.; Granese, R.; Sofo, V. Unus pro omnibus, omnes pro uno: A novel, evidence-based, unifying theory for the pathogenesis of endometriosis. Med Hypotheses 2017, 103, 10–20. [Google Scholar] [CrossRef] [PubMed]
- Vetvicka, V.; Laganà, A.S.; Salmeri, F.M.; Triolo, O.; Palmara, V.I.; Vitale, S.G.; Sofo, V.; Králíčková, M. Regulation of apoptotic pathways during endometriosis: From the molecular basis to the future perspectives. Arch. Gynecol. Obstet. 2016, 294, 897–904. [Google Scholar] [CrossRef] [PubMed]
- Schultheis, A.M.; Ng, C.K.Y.; De Filippo, M.R.; Piscuoglio, S.; Macedo, G.S.; Gatius, S.; Perez Mies, B.; Soslow, R.A.; Lim, R.S.; Viale, A.; et al. Massively Parallel Sequencing-Based Clonality Analysis of Synchronous Endometrioid Endometrial and Ovarian Carcinomas. J. Natl. Cancer Inst. 2015, 108, djv427. [Google Scholar] [CrossRef] [PubMed]
- Campoy, I.; Lanau, L.; Altadill, T.; Sequeiros, T.; Cabrera, S.; Cubo-Abert, M.; Pérez-Benavente, A.; Garcia, A.; Borrós, S.; Santamaria, A.; et al. Exosome-like vesicles in uterine aspirates: A comparison of ultracentrifugation-based isolation protocols. J. Transl. Med. 2016, 14, 180. [Google Scholar] [CrossRef] [PubMed]
- Huber, W.; Carey, V.J.; Gentleman, R.; Anders, S.; Carlson, M.; Carvalho, B.S.; Bravo, H.C.; Davis, S.; Gatto, L.; Girke, T.; et al. Orchestrating high-throughput genomic analysis with Bioconductor. Nat. Methods 2015, 12, 115–121. [Google Scholar] [CrossRef] [PubMed]
- R Foundation for Statistical Computing. R: A Language and Environment for Statistical Computing; R Foundation for Statistical Computing: Vienna, Austria, 2018. [Google Scholar]
- Dvinge, H.; Bertone, P. HTqPCR: High-throughput analysis and visualization of quantitative real-time PCR data in R. Bioinformatics 2009, 25, 3325–3326. [Google Scholar] [CrossRef] [PubMed]
- Ritchie, M.E.; Phipson, B.; Wu, D.; Hu, Y.; Law, C.W.; Shi, W.; Smyth, G.K. limma powers differential expression analyses for RNA-sequencing and microarray studies. Nucleic Acids Res. 2015, 43, e47. [Google Scholar] [CrossRef]
- Benjaminit, Y.; Hochberg, Y. Controlling the False Discovery Rate: A Practical and Powerful Approach to Multiple Testing. J. R. Stat. Soc. Ser. B 1995, 57, 289–300. [Google Scholar]
- Dweep, H.; Gretz, N. miRWalk2.0: A comprehensive atlas of microRNA-target interactions. Nat. Methods 2015, 12, 697. [Google Scholar] [CrossRef]
- Mi, H.; Muruganujan, A.; Casagrande, J.T.; Thomas, P.D. Large-scale gene function analysis with the PANTHER classification system. Nat. Protoc. 2013, 8, 1551–1566. [Google Scholar] [CrossRef]
| Clinical Parameters | Endometrial Cancer | Control |
|---|---|---|
| Age | ||
| Median | 61.4 | 65.5 |
| Minimum | 46 | 52 |
| Maximum | 78 | 90 |
| Gender | ||
| Female | 22 | 4 |
| Male | - | 18 |
| Pathology | ||
| Endometrial Cancer | - | |
| EEC | 19 | - |
| NEEC | 3 | - |
| Hepatic cirrhoses | - | 20 |
| Other | - | 22 |
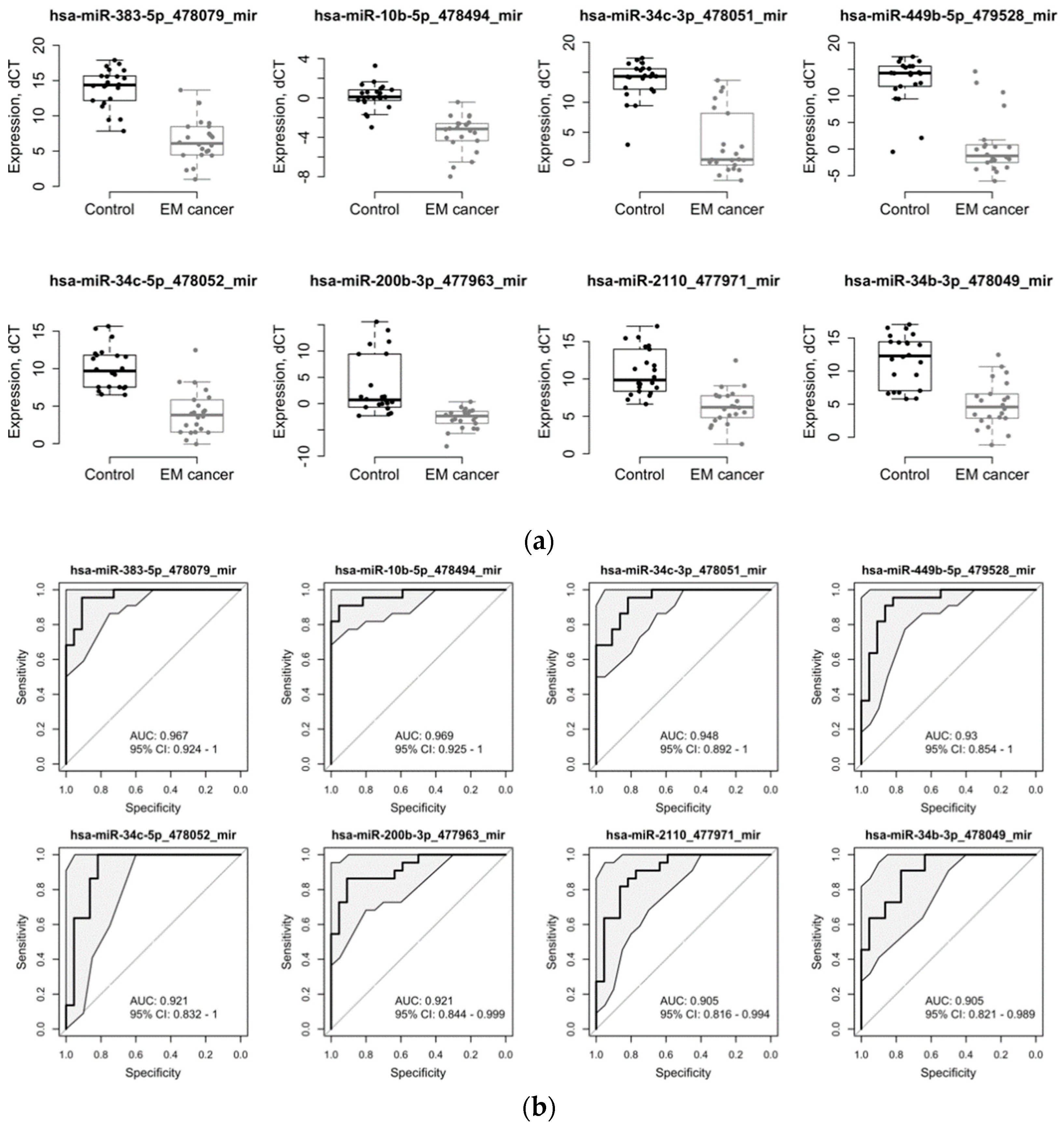
| miRNA | logFC | p-Value | adj.p-Value | AUC | AUC_95%CI_Lower | AUC_95%CI_Upper | Accuracy | Sensitivity | Specificity |
|---|---|---|---|---|---|---|---|---|---|
| hsa-miR-383-5p_478079_mir | −7.56 | 2.86E-14 | 1.02E-11 | 0.961 | 0.938 | 0.985 | 0.884 | 0.876 | 0.892 |
| hsa-miR-10b-5p_478494_mir | −3.75 | 2.62E-11 | 3.10E-09 | 0.958 | 0.93 | 0.987 | 0.897 | 0.864 | 0.93 |
| hsa-miR-34c-3p_478051_mir | −10.56 | 9.57E-10 | 6.79E-08 | 0.948 | 0.925 | 0.97 | 0.843 | 0.893 | 0.794 |
| hsa-miR-449b-5p_479528_mir | −12.18 | 2.58E-11 | 3.10E-09 | 0.927 | 0.896 | 0.959 | 0.864 | 0.896 | 0.83 |
| hsa-miR-34c-5p_478052_mir | −5.97 | 5.60E-10 | 4.97E-08 | 0.924 | 0.891 | 0.957 | 0.845 | 0.86 | 0.83 |
| hsa-miR-200b-3p_477963_mir | −6.10 | 2.73E-06 | 6.91E-05 | 0.917 | 0.888 | 0.946 | 0.846 | 0.824 | 0.869 |
| hsa-miR-2110_477971_mir | −4.57 | 7.27E-07 | 2.58E-05 | 0.906 | 0.875 | 0.938 | 0.802 | 0.748 | 0.855 |
| hsa-miR-34b-3p_478049_mir | −6.73 | 4.17E-07 | 2.12E-05 | 0.903 | 0.874 | 0.932 | 0.752 | 0.719 | 0.786 |
| hsa-miR-200c-3p_478351_mir | −10.29 | 3.42E-09 | 2.02E-07 | 0.897 | 0.863 | 0.931 | 0.799 | 0.744 | 0.853 |
| hsa-miR-150-5p_477918_mir | 2.89 | 9.74E-06 | 2.26E-04 | 0.892 | 0.856 | 0.928 | 0.861 | 0.908 | 0.814 |
| hsa-miR-1180-3p_477869_mir | −4.62 | 9.40E-07 | 3.04E-05 | 0.89 | 0.854 | 0.926 | 0.791 | 0.738 | 0.844 |
| hsa-miR-29c-5p_478005_mir | −2.39 | 1.35E-06 | 3.70E-05 | 0.883 | 0.849 | 0.918 | 0.773 | 0.773 | 0.774 |
| hsa-miR-190a-5p_478358_mir | −2.51 | 1.42E-03 | 9.18E-03 | 0.871 | 0.831 | 0.911 | 0.816 | 0.813 | 0.82 |
| hsa-miR-708-5p_478197_mir | −5.51 | 1.19E-06 | 3.52E-05 | 0.865 | 0.826 | 0.903 | 0.77 | 0.684 | 0.856 |
| hsa-miR-218-5p_477977_mir | −6.70 | 1.27E-05 | 2.59E-04 | 0.859 | 0.816 | 0.901 | 0.715 | 0.53 | 0.9 |
| hsa-miR-99a-3p_479224_mir | −3.23 | 4.78E-05 | 7.78E-04 | 0.858 | 0.818 | 0.897 | 0.732 | 0.733 | 0.73 |
| hsa-miR-196b-5p_478585_mir | −6.63 | 5.15E-07 | 2.29E-05 | 0.85 | 0.805 | 0.894 | 0.766 | 0.624 | 0.908 |
| hsa-miR-142-5p_477911_mir | 8.86 | 1.89E-05 | 3.35E-04 | 0.849 | 0.808 | 0.889 | 0.748 | 0.898 | 0.599 |
| hsa-miR-193a-3p_478306_mir | −2.49 | 1.31E-03 | 8.93E-03 | 0.849 | 0.807 | 0.891 | 0.789 | 0.853 | 0.725 |
| hsa-miR-193a-5p_477954_mir | −3.10 | 1.02E-05 | 2.26E-04 | 0.848 | 0.808 | 0.888 | 0.791 | 0.78 | 0.802 |
| hsa-miR-181a-5p_477857_mir | −1.71 | 1.01E-04 | 1.49E-03 | 0.847 | 0.807 | 0.887 | 0.755 | 0.831 | 0.678 |
| hsa-miR-125b-5p_477885_mir | −1.86 | 5.22E-05 | 8.06E-04 | 0.845 | 0.803 | 0.887 | 0.744 | 0.784 | 0.704 |
| hsa-miR-429_477849_mir | −3.07 | 2.17E-04 | 2.65E-03 | 0.843 | 0.797 | 0.89 | 0.792 | 0.817 | 0.767 |
| hsa-miR-30a-3p_478273_mir | −1.72 | 4.82E-05 | 7.78E-04 | 0.841 | 0.803 | 0.88 | 0.698 | 0.738 | 0.657 |
| hsa-miR-196a-5p_478230_mir | −6.80 | 1.89E-05 | 3.35E-04 | 0.837 | 0.801 | 0.873 | 0.743 | 0.803 | 0.682 |
| hsa-miR-34b-5p_478050_mir | −7.34 | 6.87E-07 | 2.58E-05 | 0.835 | 0.787 | 0.884 | 0.795 | 0.855 | 0.735 |
| hsa-miR-769-5p_478203_mir | −2.81 | 1.60E-03 | 1.01E-02 | 0.833 | 0.788 | 0.878 | 0.768 | 0.724 | 0.812 |
| hsa-miR-20a-5p_478586_mir | −1.74 | 2.60E-04 | 2.88E-03 | 0.832 | 0.789 | 0.875 | 0.727 | 0.738 | 0.716 |
| hsa-miR-320a_478594_mir | −8.30 | 8.68E-04 | 6.84E-03 | 0.831 | 0.796 | 0.867 | 0.698 | 0.59 | 0.806 |
| hsa-miR-30d-5p_478606_mir | −2.36 | 1.01E-02 | 3.59E-02 | 0.827 | 0.785 | 0.869 | 0.728 | 0.746 | 0.709 |
| hsa-miR-409-3p_478084_mir | 3.24 | 2.24E-04 | 2.65E-03 | 0.822 | 0.777 | 0.868 | 0.779 | 0.872 | 0.687 |
| hsa-miR-30b-5p_478007_mir | −2.57 | 1.65E-03 | 1.01E-02 | 0.82 | 0.777 | 0.863 | 0.714 | 0.736 | 0.693 |
| hsa-miR-598-3p_478172_mir | −1.84 | 3.68E-04 | 3.53E-03 | 0.82 | 0.778 | 0.861 | 0.723 | 0.677 | 0.77 |
| hsa-miR-369-3p_478067_mir | 4.94 | 1.32E-04 | 1.81E-03 | 0.816 | 0.772 | 0.86 | 0.709 | 0.895 | 0.523 |
| hsa-miR-187-3p_477941_mir | −6.40 | 1.10E-04 | 1.56E-03 | 0.815 | 0.768 | 0.861 | 0.749 | 0.638 | 0.86 |
| hsa-miR-210-3p_477970_mir | −1.85 | 1.37E-04 | 1.81E-03 | 0.813 | 0.768 | 0.859 | 0.699 | 0.713 | 0.686 |
| hsa-miR-29c-3p_479229_mir | −2.84 | 1.63E-03 | 1.01E-02 | 0.812 | 0.773 | 0.851 | 0.742 | 0.749 | 0.735 |
| hsa-miR-885-5p_478207_mir | −3.98 | 3.50E-04 | 3.45E-03 | 0.812 | 0.768 | 0.857 | 0.713 | 0.741 | 0.686 |
| hsa-miR-142-3p_477910_mir | 3.77 | 2.85E-04 | 2.98E-03 | 0.81 | 0.764 | 0.857 | 0.71 | 0.775 | 0.645 |
| hsa-miR-342-3p_478043_mir | 2.17 | 5.34E-03 | 2.44E-02 | 0.808 | 0.763 | 0.854 | 0.721 | 0.739 | 0.703 |
| hsa-miR-17-3p_477932_mir | −6.78 | 2.76E-04 | 2.97E-03 | 0.806 | 0.762 | 0.85 | 0.739 | 0.826 | 0.652 |
| hsa-miR-92a-3p_477827_mir | −1.49 | 5.35E-04 | 4.87E-03 | 0.805 | 0.763 | 0.848 | 0.711 | 0.796 | 0.626 |
| hsa-miR-29a-5p_478002_mir | −6.21 | 2.46E-03 | 1.34E-02 | 0.803 | 0.762 | 0.843 | 0.681 | 0.802 | 0.561 |
| hsa-miR-30e-3p_478388_mir | −4.45 | 6.43E-03 | 2.78E-02 | 0.796 | 0.749 | 0.844 | 0.633 | 0.426 | 0.839 |
| hsa-miR-125a-5p_477884_mir | −1.39 | 1.17E-03 | 8.33E-03 | 0.794 | 0.749 | 0.839 | 0.746 | 0.768 | 0.723 |
| hsa-miR-130a-3p_477851_mir | −1.76 | 4.73E-04 | 4.42E-03 | 0.793 | 0.744 | 0.842 | 0.723 | 0.836 | 0.61 |
| hsa-miR-485-3p_478125_mir | 2.34 | 6.14E-03 | 2.72E-02 | 0.793 | 0.746 | 0.841 | 0.694 | 0.692 | 0.698 |
| hsa-miR-223-3p_477983_mir | 1.80 | 6.62E-04 | 5.73E-03 | 0.79 | 0.744 | 0.837 | 0.714 | 0.756 | 0.672 |
| hsa-miR-21-5p_477975_mir | 1.63 | 7.79E-04 | 6.55E-03 | 0.787 | 0.738 | 0.836 | 0.714 | 0.706 | 0.721 |
| hsa-miR-194-5p_477956_mir | −1.29 | 7.80E-03 | 3.18E-02 | 0.785 | 0.735 | 0.835 | 0.749 | 0.746 | 0.752 |
| hsa-miR-29a-3p_478587_mir | −2.40 | 8.07E-03 | 3.22E-02 | 0.784 | 0.736 | 0.833 | 0.663 | 0.746 | 0.581 |
| hsa-miR-887-3p_479189_mir | −5.02 | 2.54E-04 | 2.88E-03 | 0.784 | 0.736 | 0.832 | 0.652 | 0.46 | 0.843 |
| hsa-miR-135a-5p_478581_mir | −5.63 | 7.93E-04 | 6.55E-03 | 0.775 | 0.727 | 0.823 | 0.698 | 0.663 | 0.732 |
| hsa-miR-31-5p_478015_mir | −2.16 | 8.14E-04 | 6.56E-03 | 0.775 | 0.727 | 0.823 | 0.671 | 0.769 | 0.573 |
| hsa-miR-29b-2-5p_478003_mir | −2.82 | 8.96E-04 | 6.92E-03 | 0.773 | 0.723 | 0.824 | 0.671 | 0.688 | 0.654 |
| hsa-miR-26b-5p_478418_mir | −1.47 | 1.01E-03 | 7.45E-03 | 0.771 | 0.722 | 0.82 | 0.669 | 0.822 | 0.516 |
| hsa-miR-656-3p_479137_mir | 4.06 | 1.73E-03 | 1.04E-02 | 0.771 | 0.72 | 0.822 | 0.693 | 0.7 | 0.686 |
| hsa-miR-33b-5p_478479_mir | −4.09 | 1.48E-02 | 4.82E-02 | 0.767 | 0.718 | 0.816 | 0.64 | 0.591 | 0.69 |
| hsa-miR-141-3p_478501_mir | −8.97 | 1.31E-05 | 2.59E-04 | 0.765 | 0.715 | 0.815 | 0.718 | 0.847 | 0.589 |
| hsa-miR-423-3p_478327_mir | −1.80 | 3.02E-04 | 3.07E-03 | 0.765 | 0.714 | 0.816 | 0.679 | 0.67 | 0.687 |
| hsa-miR-28-3p_477999_mir | −2.33 | 2.24E-03 | 1.28E-02 | 0.764 | 0.714 | 0.813 | 0.658 | 0.621 | 0.695 |
| hsa-miR-29b-3p_478369_mir | −2.44 | 6.09E-04 | 5.40E-03 | 0.761 | 0.715 | 0.808 | 0.684 | 0.63 | 0.737 |
| hsa-let-7b-5p_478576_mir | −1.43 | 1.22E-03 | 8.51E-03 | 0.76 | 0.715 | 0.806 | 0.624 | 0.648 | 0.6 |
| hsa-miR-551b-3p_478159_mir | −4.13 | 2.14E-03 | 1.25E-02 | 0.76 | 0.711 | 0.809 | 0.671 | 0.751 | 0.591 |
| hsa-miR-154-3p_478725_mir | 3.28 | 2.78E-03 | 1.47E-02 | 0.759 | 0.704 | 0.814 | 0.673 | 0.738 | 0.608 |
| hsa-miR-18a-3p_477944_mir | −2.84 | 7.96E-03 | 3.21E-02 | 0.759 | 0.707 | 0.81 | 0.67 | 0.696 | 0.644 |
| hsa-miR-26a-5p_477995_mir | −1.33 | 6.71E-03 | 2.87E-02 | 0.759 | 0.709 | 0.809 | 0.685 | 0.622 | 0.748 |
| hsa-miR-181d-5p_479517_mir | −5.43 | 4.75E-03 | 2.31E-02 | 0.757 | 0.709 | 0.805 | 0.654 | 0.524 | 0.784 |
| hsa-miR-151a-3p_477919_mir | −1.65 | 1.05E-03 | 7.59E-03 | 0.756 | 0.701 | 0.811 | 0.731 | 0.794 | 0.667 |
| hsa-miR-449a_478561_mir | −5.77 | 2.18E-04 | 2.65E-03 | 0.755 | 0.701 | 0.808 | 0.712 | 0.812 | 0.611 |
| hsa-miR-219a-5p_477980_mir | −3.58 | 2.31E-03 | 1.30E-02 | 0.752 | 0.704 | 0.8 | 0.686 | 0.708 | 0.664 |
| hsa-miR-584-5p_478167_mir | −5.62 | 2.55E-03 | 1.37E-02 | 0.752 | 0.703 | 0.801 | 0.662 | 0.778 | 0.545 |
| hsa-miR-20b-5p_477804_mir | −4.91 | 3.96E-03 | 2.04E-02 | 0.747 | 0.698 | 0.796 | 0.674 | 0.784 | 0.563 |
| hsa-miR-24-3p_477992_mir | −1.30 | 5.35E-03 | 2.44E-02 | 0.747 | 0.696 | 0.798 | 0.665 | 0.688 | 0.642 |
| hsa-miR-33a-5p_478347_mir | −3.72 | 2.83E-03 | 1.48E-02 | 0.742 | 0.689 | 0.795 | 0.672 | 0.586 | 0.757 |
| hsa-let-7e-5p_478579_mir | −6.66 | 4.07E-03 | 2.06E-02 | 0.741 | 0.685 | 0.797 | 0.709 | 0.794 | 0.623 |
| hsa-miR-543_478155_mir | 2.69 | 1.40E-03 | 9.18E-03 | 0.741 | 0.687 | 0.795 | 0.685 | 0.544 | 0.826 |
| hsa-miR-126-5p_477888_mir | 5.31 | 1.01E-03 | 7.45E-03 | 0.74 | 0.686 | 0.795 | 0.723 | 0.826 | 0.62 |
| hsa-miR-139-5p_478312_mir | −3.63 | 5.34E-03 | 2.44E-02 | 0.738 | 0.69 | 0.787 | 0.641 | 0.433 | 0.849 |
| hsa-miR-652-3p_478189_mir | −1.13 | 1.11E-02 | 3.75E-02 | 0.737 | 0.687 | 0.786 | 0.613 | 0.621 | 0.605 |
| hsa-miR-200a-3p_478490_mir | −4.89 | 6.25E-03 | 2.74E-02 | 0.735 | 0.682 | 0.788 | 0.709 | 0.79 | 0.629 |
| hsa-miR-21-3p_477973_mir | 2.34 | 8.87E-03 | 3.42E-02 | 0.735 | 0.679 | 0.791 | 0.689 | 0.738 | 0.641 |
| hsa-miR-181c-5p_477934_mir | −1.86 | 1.08E-02 | 3.73E-02 | 0.734 | 0.68 | 0.789 | 0.678 | 0.659 | 0.698 |
| hsa-miR-361-5p_478056_mir | −1.20 | 4.86E-03 | 2.31E-02 | 0.727 | 0.677 | 0.777 | 0.688 | 0.75 | 0.626 |
| hsa-miR-296-5p_477836_mir | −4.15 | 4.87E-03 | 2.31E-02 | 0.726 | 0.673 | 0.778 | 0.631 | 0.536 | 0.726 |
| hsa-miR-1271-5p_478674_mir | −4.54 | 1.01E-02 | 3.59E-02 | 0.725 | 0.674 | 0.776 | 0.643 | 0.783 | 0.502 |
| hsa-miR-125b-2-3p_478666_mir | −3.58 | 9.83E-03 | 3.58E-02 | 0.724 | 0.672 | 0.776 | 0.637 | 0.761 | 0.514 |
| hsa-miR-130b-3p_477840_mir | −4.14 | 4.77E-03 | 2.31E-02 | 0.723 | 0.673 | 0.774 | 0.684 | 0.66 | 0.707 |
| hsa-miR-545-3p_479002_mir | −3.15 | 1.06E-02 | 3.69E-02 | 0.723 | 0.67 | 0.775 | 0.648 | 0.526 | 0.77 |
| hsa-miR-331-3p_478323_mir | −5.14 | 7.33E-03 | 3.10E-02 | 0.722 | 0.669 | 0.775 | 0.673 | 0.753 | 0.594 |
| hsa-miR-128-3p_477892_mir | −1.40 | 2.39E-03 | 1.33E-02 | 0.72 | 0.667 | 0.772 | 0.642 | 0.647 | 0.638 |
| hsa-miR-148b-3p_477824_mir | −1.40 | 7.60E-03 | 3.17E-02 | 0.72 | 0.662 | 0.778 | 0.663 | 0.746 | 0.58 |
| hsa-miR-30a-5p_479448_mir | −5.80 | 1.43E-02 | 4.70E-02 | 0.716 | 0.658 | 0.774 | 0.654 | 0.716 | 0.592 |
| hsa-miR-222-3p_477982_mir | −1.46 | 1.25E-02 | 4.20E-02 | 0.712 | 0.655 | 0.77 | 0.653 | 0.645 | 0.661 |
| hsa-miR-451a_478107_mir | −4.53 | 1.40E-03 | 9.18E-03 | 0.711 | 0.654 | 0.768 | 0.61 | 0.613 | 0.606 |
| hsa-miR-203a-3p_478316_mir | −4.92 | 9.36E-03 | 3.50E-02 | 0.708 | 0.653 | 0.764 | 0.664 | 0.804 | 0.524 |
| hsa-miR-758-3p_479166_mir | 3.56 | 9.37E-03 | 3.50E-02 | 0.705 | 0.653 | 0.756 | 0.652 | 0.692 | 0.612 |
| hsa-miR-452-5p_478109_mir | −2.16 | 1.11E-02 | 3.75E-02 | 0.703 | 0.644 | 0.762 | 0.598 | 0.571 | 0.626 |
| hsa-miR-505-3p_478145_mir | −1.91 | 6.03E-03 | 2.71E-02 | 0.703 | 0.647 | 0.759 | 0.604 | 0.553 | 0.655 |
| hsa-miR-504-5p_478144_mir | −2.25 | 1.06E-02 | 3.69E-02 | 0.701 | 0.647 | 0.756 | 0.624 | 0.58 | 0.667 |
| hsa-miR-182-5p_477935_mir | −5.24 | 9.84E-03 | 3.58E-02 | 0.7 | 0.639 | 0.761 | 0.686 | 0.683 | 0.688 |
| hsa-miR-551a_478158_mir | −4.09 | 1.58E-02 | 4.93E-02 | 0.7 | 0.644 | 0.756 | 0.639 | 0.772 | 0.507 |
| hsa-miR-101-3p_477863_mir | −2.79 | 4.16E-03 | 2.08E-02 | 0.699 | 0.645 | 0.752 | 0.626 | 0.417 | 0.835 |
| hsa-miR-31-3p_478012_mir | −3.59 | 8.29E-03 | 3.27E-02 | 0.699 | 0.647 | 0.751 | 0.675 | 0.718 | 0.632 |
| hsa-miR-140-3p_477908_mir | −2.87 | 1.56E-02 | 4.90E-02 | 0.697 | 0.642 | 0.753 | 0.622 | 0.439 | 0.805 |
| hsa-miR-214-5p_478768_mir | −3.30 | 8.46E-03 | 3.30E-02 | 0.696 | 0.641 | 0.751 | 0.649 | 0.707 | 0.591 |
| hsa-miR-199b-5p_478486_mir | −4.83 | 1.49E-02 | 4.82E-02 | 0.695 | 0.646 | 0.744 | 0.623 | 0.631 | 0.614 |
| hsa-miR-337-5p_478036_mir | 3.17 | 1.27E-02 | 4.22E-02 | 0.688 | 0.631 | 0.745 | 0.711 | 0.9 | 0.523 |
| hsa-miR-154-5p_477925_mir | 2.07 | 9.88E-03 | 3.58E-02 | 0.687 | 0.631 | 0.742 | 0.657 | 0.773 | 0.541 |
| hsa-miR-582-5p_478166_mir | −3.50 | 1.52E-02 | 4.83E-02 | 0.681 | 0.618 | 0.743 | 0.644 | 0.702 | 0.587 |
| hsa-miR-126-3p_477887_mir | 5.32 | 1.82E-03 | 1.08E-02 | 0.678 | 0.616 | 0.739 | 0.738 | 0.832 | 0.643 |
| hsa-miR-143-3p_477912_mir | −1.54 | 9.06E-03 | 3.46E-02 | 0.674 | 0.616 | 0.731 | 0.677 | 0.745 | 0.608 |
| hsa-miR-324-5p_478024_mir | −1.34 | 1.52E-02 | 4.83E-02 | 0.651 | 0.588 | 0.714 | 0.572 | 0.603 | 0.542 |
| hsa-miR-145-5p_477916_mir | −1.70 | 7.80E-03 | 3.18E-02 | 0.649 | 0.591 | 0.708 | 0.646 | 0.723 | 0.57 |
© 2019 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Roman-Canal, B.; Moiola, C.P.; Gatius, S.; Bonnin, S.; Ruiz-Miró, M.; González, E.; González-Tallada, X.; Llordella, I.; Hernández, I.; Porcel, J.M.; et al. EV-Associated miRNAs from Peritoneal Lavage are a Source of Biomarkers in Endometrial Cancer. Cancers 2019, 11, 839. https://doi.org/10.3390/cancers11060839
Roman-Canal B, Moiola CP, Gatius S, Bonnin S, Ruiz-Miró M, González E, González-Tallada X, Llordella I, Hernández I, Porcel JM, et al. EV-Associated miRNAs from Peritoneal Lavage are a Source of Biomarkers in Endometrial Cancer. Cancers. 2019; 11(6):839. https://doi.org/10.3390/cancers11060839
Chicago/Turabian StyleRoman-Canal, Berta, Cristian Pablo Moiola, Sònia Gatius, Sarah Bonnin, Maria Ruiz-Miró, Esperanza González, Xavier González-Tallada, Ivanna Llordella, Isabel Hernández, José M. Porcel, and et al. 2019. "EV-Associated miRNAs from Peritoneal Lavage are a Source of Biomarkers in Endometrial Cancer" Cancers 11, no. 6: 839. https://doi.org/10.3390/cancers11060839
APA StyleRoman-Canal, B., Moiola, C. P., Gatius, S., Bonnin, S., Ruiz-Miró, M., González, E., González-Tallada, X., Llordella, I., Hernández, I., Porcel, J. M., Gil-Moreno, A., Falcón-Pérez, J. M., Ponomarenko, J., Matias-Guiu, X., & Colas, E. (2019). EV-Associated miRNAs from Peritoneal Lavage are a Source of Biomarkers in Endometrial Cancer. Cancers, 11(6), 839. https://doi.org/10.3390/cancers11060839






