Multidisciplinary Approach for Bone Metastasis: A Review
Abstract
:1. Introduction
2. Epidemiology of Bone Metastasis
3. Pathophysiology of Bone Metastasis
4. Skeletal-Related Events
5. Early Diagnosis and Prophylactic Approach for Bone Management
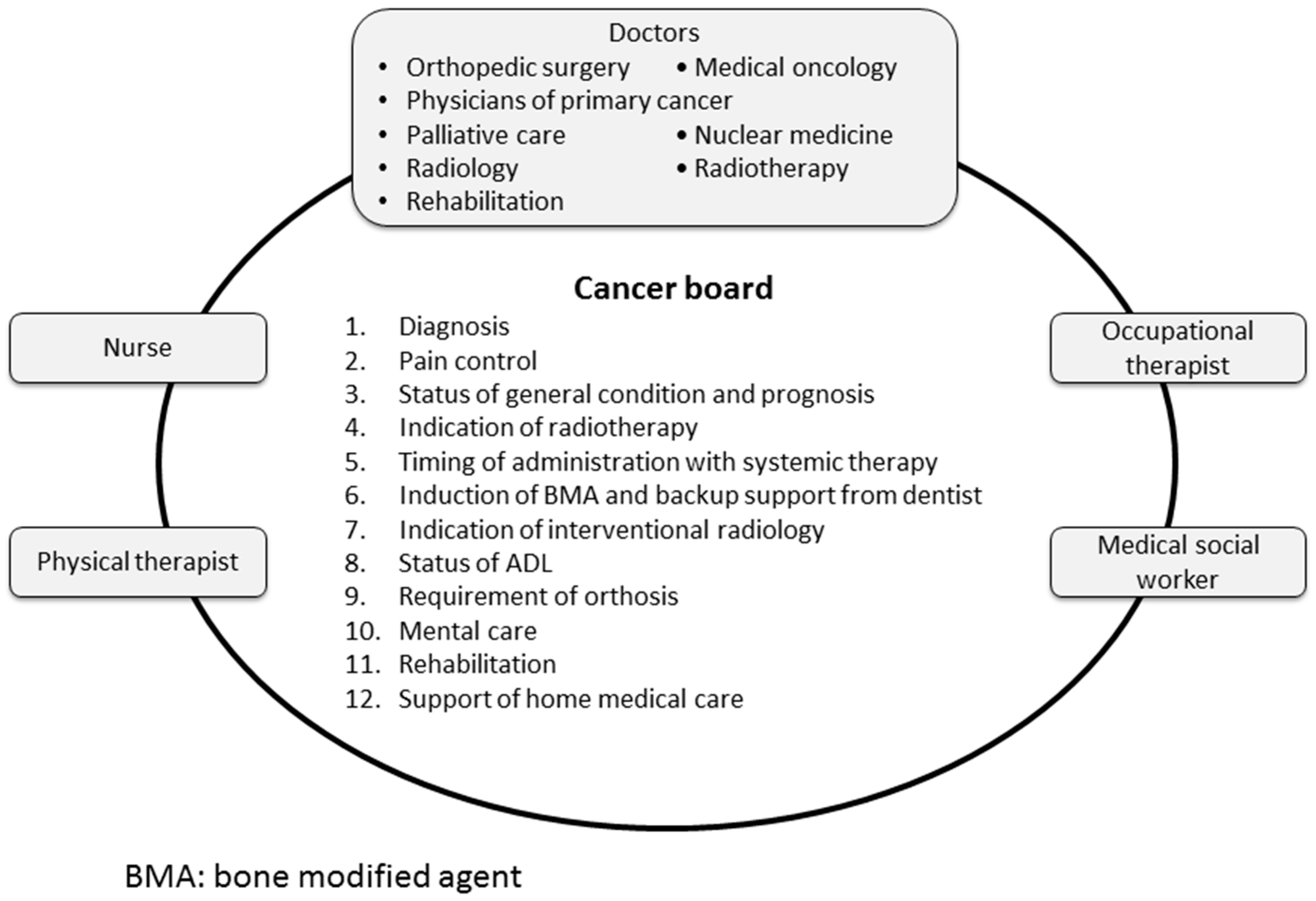
6. Comprehensive Approach as a Cancer Board
7. Current Pitfalls and Future Directions
8. Conclusions
Funding
Conflicts of Interest
References
- Ibrahim, T.; Flamini, E.; Fabbri, L.; Serra, P.; Mercatali, L.; Ricci, R.; Sacanna, E.; Falasconi, M.C.; Casadei, R.; Galassi, R.; et al. Multidisciplinary approach to the treatment of bone metastases: Osteo-oncology center, a new organizational model. Tumori 2009, 95, 291–297. [Google Scholar] [CrossRef] [PubMed]
- Bandini, M.; Pompe, R.S.; Marchioni, M.; Zaffuto, E.; Gandaglia, G.; Fossati, N.; Cindolo, L.; Montorsi, F.; Briganti, A.; Saad, F.; et al. Improved cancer-specific free survival and overall free survival in contemporary metastatic prostate cancer patients: A population-based study. Int. Urol. Nephrol. 2018, 50, 71–78. [Google Scholar] [CrossRef] [PubMed]
- Coleman, R.E. Metastatic bone disease: Clinical features, pathophysiology and treatment strategies. Cancer Treat. Rev. 2001, 27, 165–176. [Google Scholar] [CrossRef] [PubMed]
- Coleman, R.E. Skeletal complications of malignancy. Cancer 1997, 80, 1588–1594. [Google Scholar] [CrossRef]
- Plunkett, T.A.; Rubens, R.D. The biology and management of bone metastases. Crit. Rev. Oncol. Hematol. 1999, 31, 89–96. [Google Scholar] [CrossRef]
- Norgaard, M.; Jensen, A.O.; Jacobsen, J.B.; Cetin, K.; Fryzek, J.P.; Sorensen, H.T. Skeletal related events, bone metastasis and survival of prostate cancer: A population based cohort study in Denmark (1999 to 2007). J. Urol. 2010, 184, 162–167. [Google Scholar] [CrossRef] [PubMed]
- Yong, M.; Jensen, A.O.; Jacobsen, J.B.; Norgaard, M.; Fryzek, J.P.; Sorensen, H.T. Survival in breast cancer patients with bone metastases and skeletal-related events: A population-based cohort study in Denmark (1999–2007). Breast Cancer Res. Treat. 2011, 129, 495–503. [Google Scholar] [CrossRef] [PubMed]
- Sathiakumar, N.; Delzell, E.; Morrisey, M.A.; Falkson, C.; Yong, M.; Chia, V.; Blackburn, J.; Arora, T.; Kilgore, M.L. Mortality following bone metastasis and skeletal-related events among men with prostate cancer: A population-based analysis of us medicare beneficiaries, 1999–2006. Prostate Cancer Prostatic Dis. 2011, 14, 177–183. [Google Scholar] [CrossRef] [PubMed]
- Roodman, G.D. Mechanisms of bone metastasis. N. Engl. J. Med. 2004, 350, 1655–1664. [Google Scholar] [CrossRef] [PubMed]
- Xiong, Z.; Deng, G.; Huang, X.; Li, X.; Xie, X.; Wang, J.; Shuang, Z.; Wang, X. Bone metastasis pattern in initial metastatic breast cancer: A population-based study. Cancer Manag. Res. 2018, 10, 287–295. [Google Scholar] [CrossRef] [PubMed]
- Dawood, S.; Broglio, K.; Ensor, J.; Hortobagyi, G.N.; Giordano, S.H. Survival differences among women with de novo stage iv and relapsed breast cancer. Ann. Oncol. 2010, 21, 2169–2174. [Google Scholar] [CrossRef] [PubMed]
- Yang, Y.; Ma, Y.; Sheng, J.; Huang, Y.; Zhao, Y.; Fang, W.; Hong, S.; Tian, Y.; Xue, C.; Zhang, L. A multicenter, retrospective epidemiologic survey of the clinical features and management of bone metastatic disease in China. Chin. J. Cancer 2016, 35, 40. [Google Scholar] [CrossRef] [PubMed]
- Hage, W.D.; Aboulafia, A.J.; Aboulafia, D.M. Incidence, location, and diagnostic evaluation of metastatic bone disease. Orthop. Clin. N. Am. 2000, 31, 515–528. [Google Scholar] [CrossRef]
- Pezaro, C.; Omlin, A.; Lorente, D.; Rodrigues, D.N.; Ferraldeschi, R.; Bianchini, D.; Mukherji, D.; Riisnaes, R.; Altavilla, A.; Crespo, M.; et al. Visceral disease in castration-resistant prostate cancer. Eur. Urol. 2014, 65, 270–273. [Google Scholar] [CrossRef] [PubMed]
- Blum, R.H.; Novetsky, D.; Shasha, D.; Fleishman, S. The multidisciplinary approach to bone metastases. Oncology 2003, 17, 845–857; discussion 862–863, 867. [Google Scholar] [PubMed]
- Solomayer, E.F.; Diel, I.J.; Meyberg, G.C.; Gollan, C.; Bastert, G. Metastatic breast cancer: Clinical course, prognosis and therapy related to the first site of metastasis. Breast Cancer Res. Treat. 2000, 59, 271–278. [Google Scholar] [CrossRef] [PubMed]
- Hosono, N.; Yonenobu, K.; Fuji, T.; Ebara, S.; Yamashita, K.; Ono, K. Orthopaedic management of spinal metastases. Clin. Orthop. Relat. Res. 1995, 312, 148–159. [Google Scholar]
- Karr, J.P.; Yamanaka, H. Prostate Cancer and Bone Metastasis, 1st ed.; Springer: New York, NY, USA, 1992. [Google Scholar]
- Moriwaki, S. Histopathology and statistical analysis of spinal metastases of carcinomas in autopsy cases. Orthop. Surg. Traumatol. 1993, 36, 233–241. [Google Scholar]
- Olechnowicz, S.W.; Edwards, C.M. Contributions of the host microenvironment to cancer-induced bone disease. Cancer Res. 2014, 74, 1625–1631. [Google Scholar] [CrossRef] [PubMed]
- Tsuzuki, S.; Park, S.H.; Eber, M.R.; Peters, C.M.; Shiozawa, Y. Skeletal complications in cancer patients with bone metastases. Int. J. Urol. 2016, 23, 825–832. [Google Scholar] [CrossRef] [PubMed]
- Shiozawa, Y.; Pedersen, E.A.; Havens, A.M.; Jung, Y.; Mishra, A.; Joseph, J.; Kim, J.K.; Patel, L.R.; Ying, C.; Ziegler, A.M.; et al. Human prostate cancer metastases target the hematopoietic stem cell niche to establish footholds in mouse bone marrow. J. Clin. Investig. 2011, 121, 1298–1312. [Google Scholar] [CrossRef] [PubMed]
- Clines, G.A.; Guise, T.A. Hypercalcaemia of malignancy and basic research on mechanisms responsible for osteolytic and osteoblastic metastasis to bone. Endocr. Relat. Cancer 2005, 12, 549–583. [Google Scholar] [CrossRef] [PubMed]
- Chien, A.J.; Goss, P.E. Aromatase inhibitors and bone health in women with breast cancer. J. Clin. Oncol. 2006, 24, 5305–5312. [Google Scholar] [CrossRef] [PubMed]
- Henry, N.L.; Giles, J.T.; Ang, D.; Mohan, M.; Dadabhoy, D.; Robarge, J.; Hayden, J.; Lemler, S.; Shahverdi, K.; Powers, P.; et al. Prospective characterization of musculoskeletal symptoms in early stage breast cancer patients treated with aromatase inhibitors. Breast Cancer Res. Treat. 2008, 111, 365–372. [Google Scholar] [CrossRef] [PubMed]
- Miyazawa, Y.; Sekine, Y.; Syuto, T.; Nomura, M.; Koike, H.; Matsui, H.; Shibata, Y.; Ito, K.; Suzuki, K. Evaluation of bone turnover/quality markers and bone mineral density in prostate cancer patients receiving androgen deprivation therapy with or without denosumab. Anticancer Res. 2017, 37, 3667–3671. [Google Scholar] [PubMed]
- Miyazawa, Y.; Sekine, Y.; Syuto, T.; Nomura, M.; Koike, H.; Matsui, H.; Shibata, Y.; Ito, K.; Suzuki, K. Effect of androgen-deprivation therapy on bone mineral density in Japanese patients with prostate cancer. In Vivo 2018, 32, 409–412. [Google Scholar] [PubMed]
- Van den Beuken-van Everdingen, M.H.; de Rijke, J.M.; Kessels, A.G.; Schouten, H.C.; van Kleef, M.; Patijn, J. Prevalence of pain in patients with cancer: A systematic review of the past 40 years. Ann. Oncol. 2007, 18, 1437–1449. [Google Scholar] [CrossRef] [PubMed]
- McKay, R.; Haider, B.; Duh, M.S.; Valderrama, A.; Nakabayashi, M.; Fiorillo, M.; Ristovska, L.; Wen, L.; Kantoff, P. Impact of symptomatic skeletal events on health-care resource utilization and quality of life among patients with castration-resistant prostate cancer and bone metastases. Prostate Cancer Prostatic Dis. 2017, 20, 276–282. [Google Scholar] [CrossRef] [PubMed]
- Howard, L.E.; De Hoedt, A.M.; Aronson, W.J.; Kane, C.J.; Amling, C.L.; Cooperberg, M.R.; Terris, M.K.; Divers, C.H.; Valderrama, A.; Freedland, S.J. Do skeletal-related events predict overall survival in men with metastatic castration-resistant prostate cancer? Prostate Cancer Prostatic Dis. 2016, 19, 380–384. [Google Scholar] [CrossRef] [PubMed]
- Rosen, L.S.; Gordon, D.; Kaminski, M.; Howell, A.; Belch, A.; Mackey, J.; Apffelstaedt, J.; Hussein, M.A.; Coleman, R.E.; Reitsma, D.J.; et al. Long-term efficacy and safety of zoledronic acid compared with pamidronate disodium in the treatment of skeletal complications in patients with advanced multiple myeloma or breast carcinoma: A randomized, double-blind, multicenter, comparative trial. Cancer 2003, 98, 1735–1744. [Google Scholar] [CrossRef] [PubMed]
- Rosen, L.S.; Gordon, D.; Tchekmedyian, S.; Yanagihara, R.; Hirsh, V.; Krzakowski, M.; Pawlicki, M.; de Souza, P.; Zheng, M.; Urbanowitz, G.; et al. Zoledronic acid versus placebo in the treatment of skeletal metastases in patients with lung cancer and other solid tumors: A phase iii, double-blind, randomized trial—The zoledronic acid lung cancer and other solid tumors study group. J. Clin. Oncol. 2003, 21, 3150–3157. [Google Scholar] [CrossRef] [PubMed]
- Lipton, A.; Fizazi, K.; Stopeck, A.T.; Henry, D.H.; Brown, J.E.; Yardley, D.A.; Richardson, G.E.; Siena, S.; Maroto, P.; Clemens, M.; et al. Superiority of denosumab to zoledronic acid for prevention of skeletal-related events: A combined analysis of 3 pivotal, randomised, phase 3 trials. Eur. J. Cancer 2012, 48, 3082–3092. [Google Scholar] [CrossRef] [PubMed]
- Fizazi, K.; Carducci, M.; Smith, M.; Damiao, R.; Brown, J.; Karsh, L.; Milecki, P.; Shore, N.; Rader, M.; Wang, H.; et al. Denosumab versus zoledronic acid for treatment of bone metastases in men with castration-resistant prostate cancer: A randomised, double-blind study. Lancet 2011, 377, 813–822. [Google Scholar] [CrossRef]
- Aaron, A.D. Treatment of metastatic adenocarcinoma of the pelvis and the extremities. J. Bone Jt. Surg. Am. 1997, 79, 917–932. [Google Scholar] [CrossRef]
- Bohm, P.; Huber, J. The surgical treatment of bony metastases of the spine and limbs. J. Bone Jt. Surg. Br. 2002, 84, 521–529. [Google Scholar] [CrossRef]
- Hansen, B.H.; Keller, J.; Laitinen, M.; Berg, P.; Skjeldal, S.; Trovik, C.; Nilsson, J.; Walloe, A.; Kalen, A.; Wedin, R. The scandinavian sarcoma group skeletal metastasis register. Survival after surgery for bone metastases in the pelvis and extremities. Acta Orthop. Scand. Suppl. 2004, 75, 11–15. [Google Scholar] [CrossRef] [PubMed]
- Mavrogenis, A.F.; Pala, E.; Romagnoli, C.; Romantini, M.; Calabro, T.; Ruggieri, P. Survival analysis of patients with femoral metastases. J. Surg. Oncol. 2012, 105, 135–141. [Google Scholar] [CrossRef] [PubMed]
- Bryson, D.J.; Wicks, L.; Ashford, R.U. The investigation and management of suspected malignant pathological fractures: A review for the general orthopaedic surgeon. Injury 2015, 46, 1891–1899. [Google Scholar] [CrossRef] [PubMed]
- Frassica, D.A. General principles of external beam radiation therapy for skeletal metastases. Clin. Orthop. Relat. Res. 2003, 415, S158–S164. [Google Scholar] [CrossRef] [PubMed]
- Prasad, D.; Schiff, D. Malignant spinal-cord compression. Lancet Oncol. 2005, 6, 15–24. [Google Scholar] [CrossRef]
- Ushio, Y.; Posner, R.; Posner, J.B.; Shapiro, W.R. Experimental spinal cord compression by epidural neoplasm. Neurology 1977, 27, 422–429. [Google Scholar] [CrossRef] [PubMed]
- Ramsey, R.; Doppman, J.L. The effects of epidural masses on spinal cord blood flow. An experimental study in monkeys. Radiology 1973, 107, 99–103. [Google Scholar] [CrossRef] [PubMed]
- Kato, A.; Ushio, Y.; Hayakawa, T.; Yamada, K.; Ikeda, H.; Mogami, H. Circulatory disturbance of the spinal cord with epidural neoplasm in rats. J. Neurosurg. 1985, 63, 260–265. [Google Scholar] [CrossRef] [PubMed]
- Cole, J.S.; Patchell, R.A. Metastatic epidural spinal cord compression. Lancet Neurol. 2008, 7, 459–466. [Google Scholar] [CrossRef]
- Patchell, R.A.; Tibbs, P.A.; Regine, W.F.; Payne, R.; Saris, S.; Kryscio, R.J.; Mohiuddin, M.; Young, B. Direct decompressive surgical resection in the treatment of spinal cord compression caused by metastatic cancer: A randomised trial. Lancet 2005, 366, 643–648. [Google Scholar] [CrossRef]
- Rades, D.; Abrahm, J.L. The role of radiotherapy for metastatic epidural spinal cord compression. Nat. Rev. Clin. Oncol. 2010, 7, 590–598. [Google Scholar] [CrossRef] [PubMed]
- Rades, D.; Segedin, B.; Conde-Moreno, A.J.; Garcia, R.; Perpar, A.; Metz, M.; Badakhshi, H.; Schreiber, A.; Nitsche, M.; Hipp, P.; et al. Radiotherapy with 4 gy x 5 versus 3 gy x 10 for metastatic epidural spinal cord compression: Final results of the score-2 trial (aro 2009/01). J. Clin. Oncol. 2016, 34, 597–602. [Google Scholar] [CrossRef] [PubMed]
- Stewart, A.F. Clinical practice. Hypercalcemia associated with cancer. N. Engl. J. Med. 2005, 352, 373–379. [Google Scholar] [CrossRef] [PubMed]
- Hosking, D.J.; Cowley, A.; Bucknall, C.A. Rehydration in the treatment of severe hypercalcaemia. QJM Int. J. Med. 1981, 50, 473–481. [Google Scholar]
- Thosani, S.; Hu, M.I. Denosumab: A new agent in the management of hypercalcemia of malignancy. Future Oncol. 2015, 11, 2865–2871. [Google Scholar] [CrossRef] [PubMed]
- Maranzano, E.; Latini, P. Effectiveness of radiation therapy without surgery in metastatic spinal cord compression: Final results from a prospective trial. Int. J. Radiat. Oncol. Biol. Phys. 1995, 32, 959–967. [Google Scholar] [CrossRef]
- Helweg-Larsen, S. Clinical outcome in metastatic spinal cord compression. A prospective study of 153 patients. Acta Neurol. Scand. 1996, 94, 269–275. [Google Scholar] [CrossRef] [PubMed]
- Loven, D.; Gornish, M.; Fenig, G.E.; Sulkes, A.; Rappaport, Z.; Klir, I.; Rotenberg, Z.; Gadoth, N. malignant epidural cord compression. Harefuah 1996, 131, 457–462, 536. [Google Scholar] [PubMed]
- Solberg, A.; Bremnes, R.M. Metastatic spinal cord compression: Diagnostic delay, treatment, and outcome. Anticancer Res. 1999, 19, 677–684. [Google Scholar] [PubMed]
- Johnson, S.K.; Knobf, M.T. Surgical interventions for cancer patients with impending or actual pathologic fractures. Orthop. Nurs. 2008, 27, 160–171. [Google Scholar] [CrossRef] [PubMed]
- Ward, W.G.; Holsenbeck, S.; Dorey, F.J.; Spang, J.; Howe, D. Metastatic disease of the femur: Surgical treatment. Clin. Orthop. Relat. Res. 2003, 415, S230–S244. [Google Scholar] [CrossRef] [PubMed]
- Ristevski, B.; Jenkinson, R.J.; Stephen, D.J.; Finkelstein, J.; Schemitsch, E.H.; McKee, M.D.; Kreder, H.J. Mortality and complications following stabilization of femoral metastatic lesions: A population-based study of regional variation and outcome. Can. J. Surg. 2009, 52, 302–308. [Google Scholar] [PubMed]
- Mirels, H. Metastatic disease in long bones: A proposed scoring system for diagnosing impending pathologic fractures. Clin Orthop Relat Res. 1989, 249, 256–264. [Google Scholar] [CrossRef]
- Damron, T.A.; Morgan, H.; Prakash, D.; Grant, W.; Aronowitz, J.; Heiner, J. Critical evaluation of mirels’ rating system for impending pathologic fractures. Clin. Orthop. Relat. Res. 2003, 415, S201–S207. [Google Scholar] [CrossRef] [PubMed]
- Jawad, M.U.; Scully, S.P. In brief: Classifications in brief: Mirels’ classification: Metastatic disease in long bones and impending pathologic fracture. Clin. Orthop. Relat. Res. 2010, 468, 2825–2827. [Google Scholar] [CrossRef] [PubMed]
- Van der Linden, Y.M.; Dijkstra, P.D.; Kroon, H.M.; Lok, J.J.; Noordijk, E.M.; Leer, J.W.; Marijnen, C.A. Comparative analysis of risk factors for pathological fracture with femoral metastases. J. Bone Jt. Surg. Br. 2004, 86, 566–573. [Google Scholar] [CrossRef]
- Takagi, T. Comprehensive approach for spinal metastases: Transdisciplinary managementa takagi. J. Jt. Surg. 2016, 35, 368–373. [Google Scholar]
| Skeletal Related Event | Management | Effects |
|---|---|---|
| Bone pain | NSAIDs, Opioids | Analgesic effects |
| Bisphosphonates | Inhibition of pathological bone resorption Analgesic effects | |
| Denosumab | Inhibition of pathological bone resorption Analgesic effects | |
| Radiation | Analgesic effects Tumor shrinkage | |
| Pathological bone fracture | Surgery | Stabilization of fracture |
| Radiation | Supportive therapy to prevent local recurrence | |
| Bisphosphonates | Prophylaxis | |
| Denosumab | Prophylaxis | |
| Spinal cord compression | Steroids | Stabilization of vascular membranes Reduction of inflammation and edema |
| Radiation | Tumor shrinkage effects | |
| Surgery | Relief for the compression | |
| Bisphosphonates | Prophylaxis | |
| Denosumab | Prophylaxis | |
| Hypercalcemia | Hydration | Promotion of renal calciuresis |
| Loop diuretics | Promotion of renal calciuresis | |
| Bisphosphonates | Inhibition of pathological bone resorption | |
| Denosumab | Inhibition of pathological bone resorption |
| Score | Site of Lesion | Size of Lesion | Nature of Lesion | Pain |
|---|---|---|---|---|
| 1 | Upper limb | <1/3 of cortex | Blastic | Mild |
| 2 | Lower limb | 1/3–2/3 of cortex | Mixed | Moderate |
| 3 | Trochanteric region | >2/3 of cortex | Lytic | Functional |
© 2018 by the author. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Kimura, T. Multidisciplinary Approach for Bone Metastasis: A Review. Cancers 2018, 10, 156. https://doi.org/10.3390/cancers10060156
Kimura T. Multidisciplinary Approach for Bone Metastasis: A Review. Cancers. 2018; 10(6):156. https://doi.org/10.3390/cancers10060156
Chicago/Turabian StyleKimura, Takahiro. 2018. "Multidisciplinary Approach for Bone Metastasis: A Review" Cancers 10, no. 6: 156. https://doi.org/10.3390/cancers10060156
APA StyleKimura, T. (2018). Multidisciplinary Approach for Bone Metastasis: A Review. Cancers, 10(6), 156. https://doi.org/10.3390/cancers10060156





