Connecting Mechanism for Artificial Blood Vessels with High Biocompatibility
Abstract
1. Introduction
2. Design and Assembly of the Connector
2.1. Biocompatibility
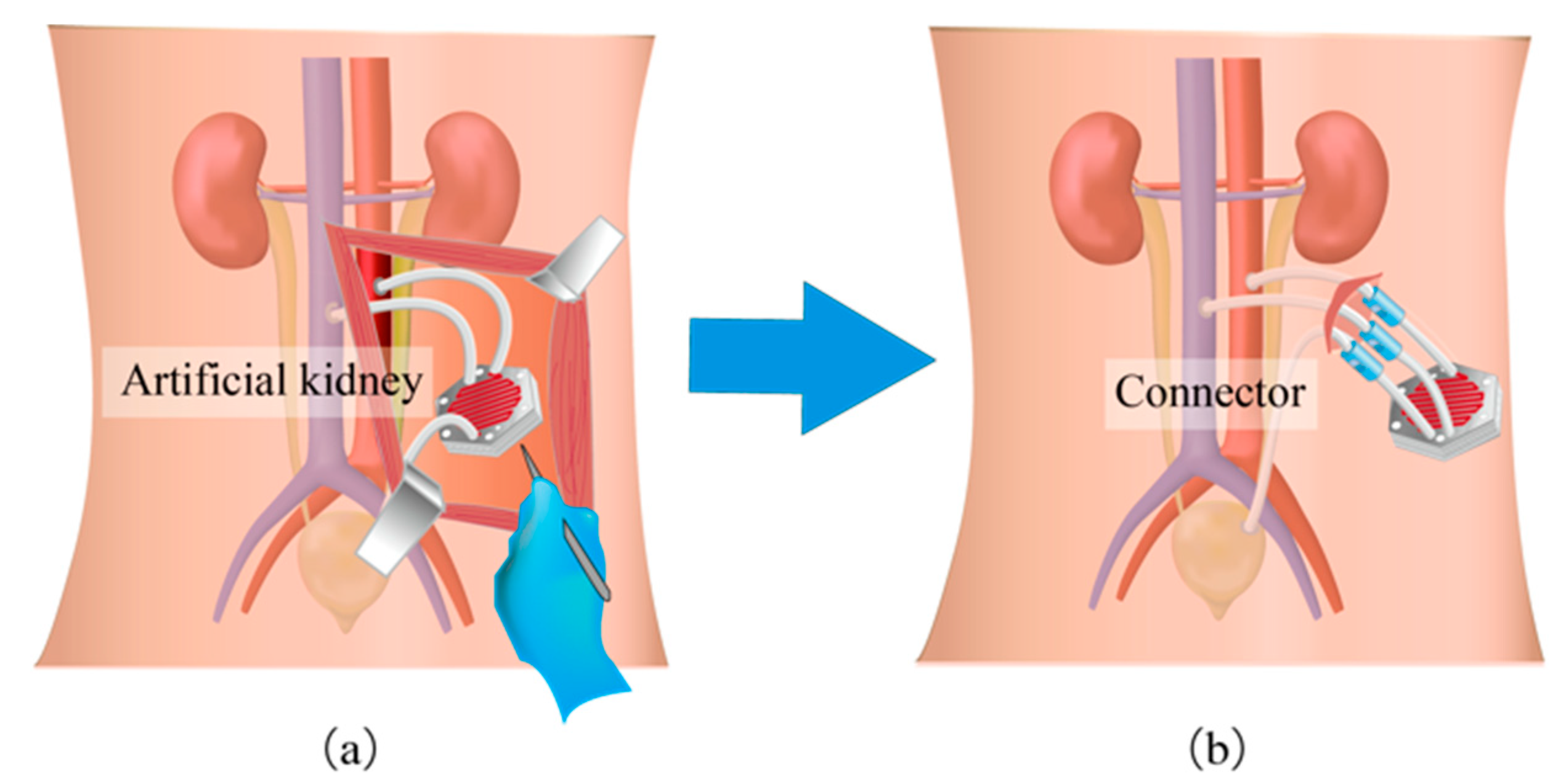
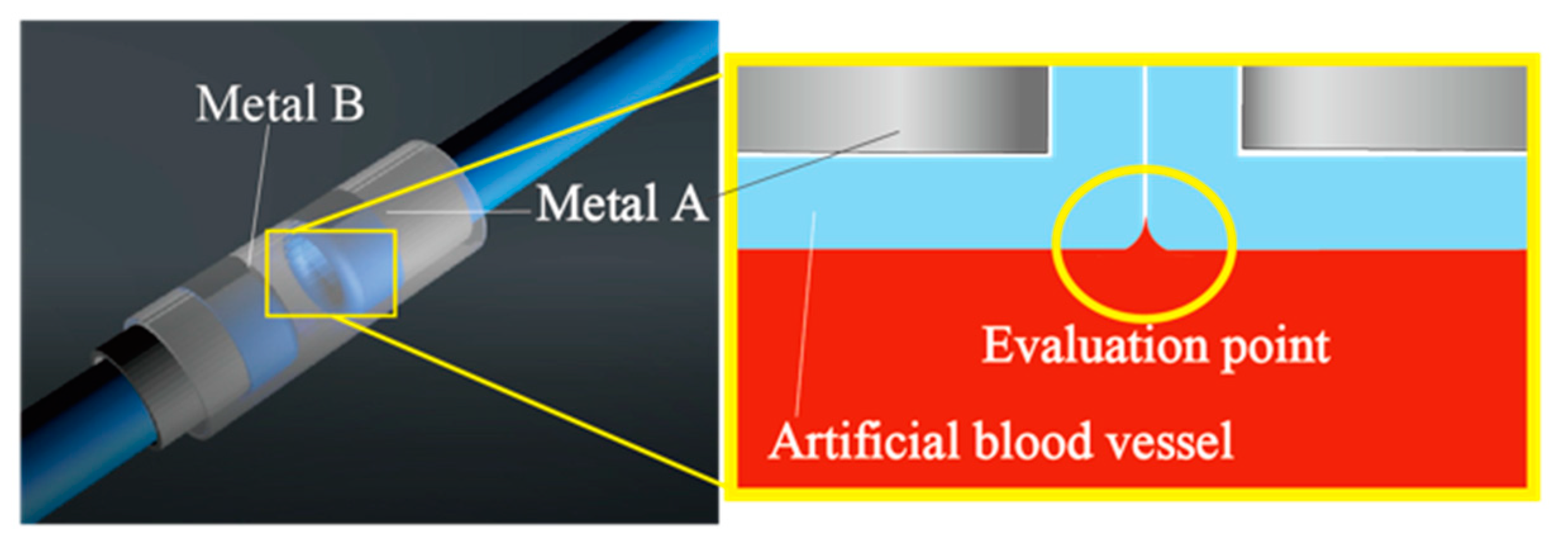
2.2. Mechanism Design and Assembly
2.3. Micro Filtering Device as the Artificial Kidney
3. Experimental Methods
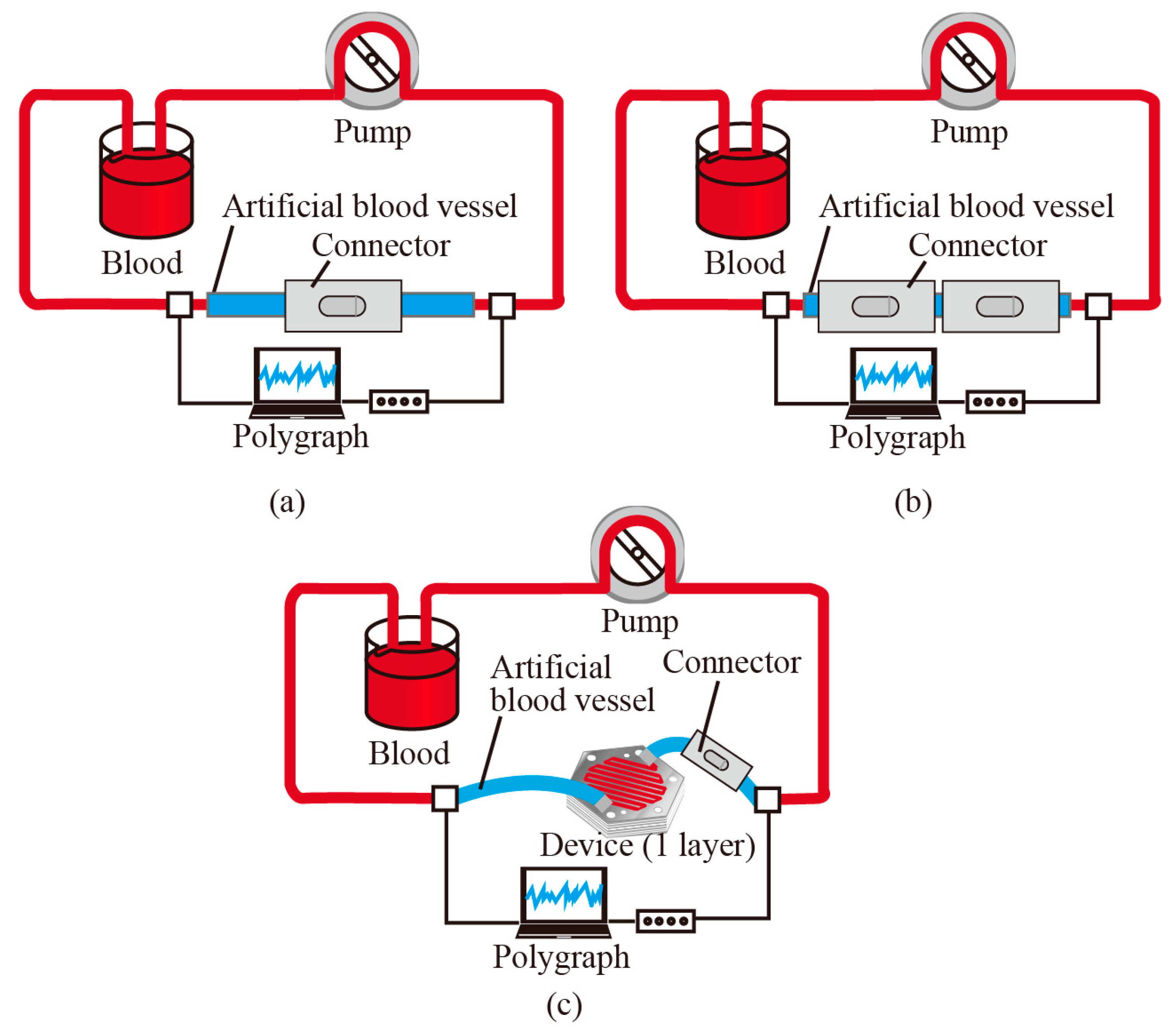
3.1. Thrombus Formation Tests In Vitro
3.2. Blood Coagulation Tests In Vitro
3.3. Blood Coagulation Tests with the Micro Filtering Device In Vitro
4. Experimental Results and Discussion
4.1. Thrombus Formation inside the Artificial Blood Vessel
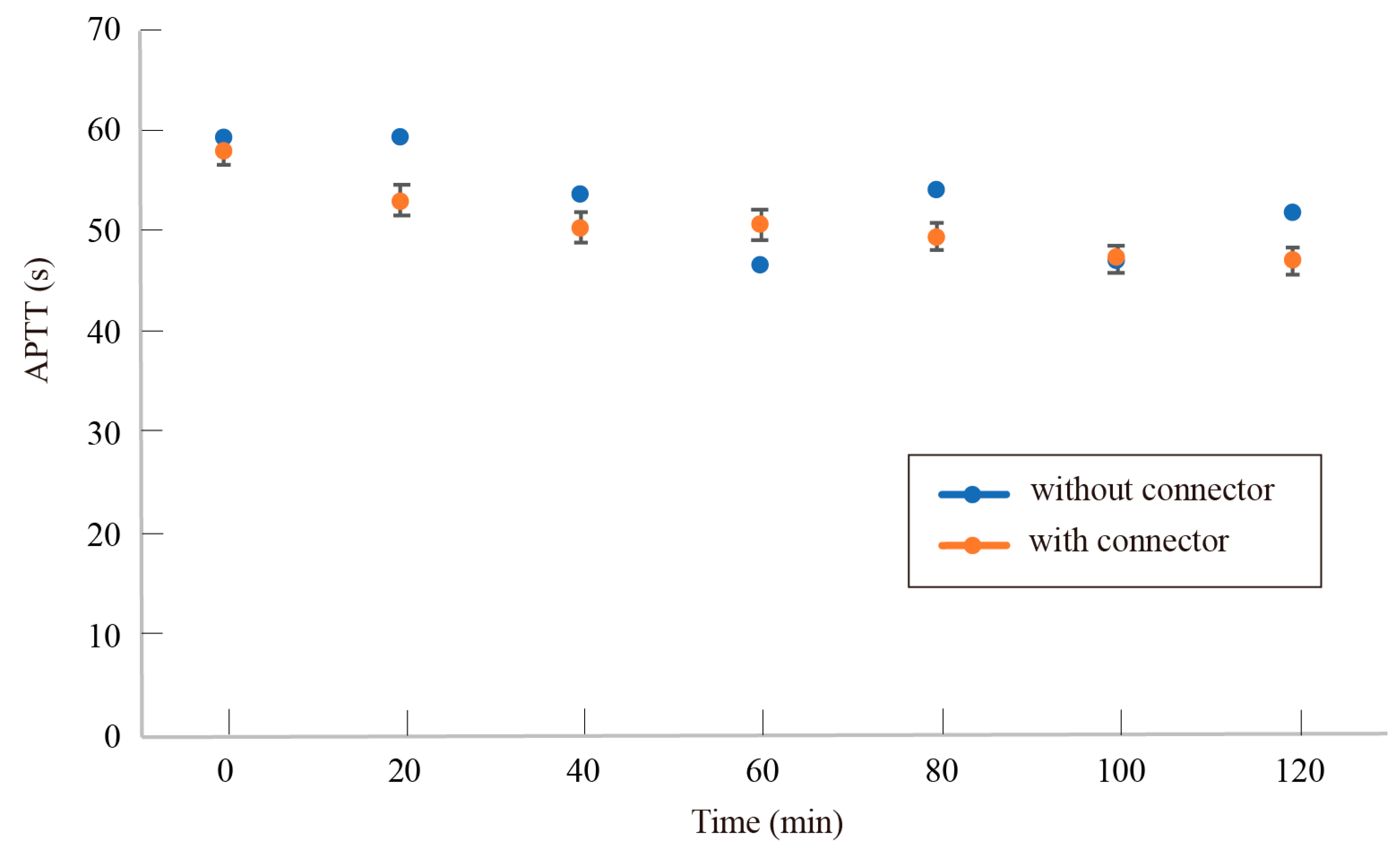
4.2. Blood Coagulation Caused by the Connector
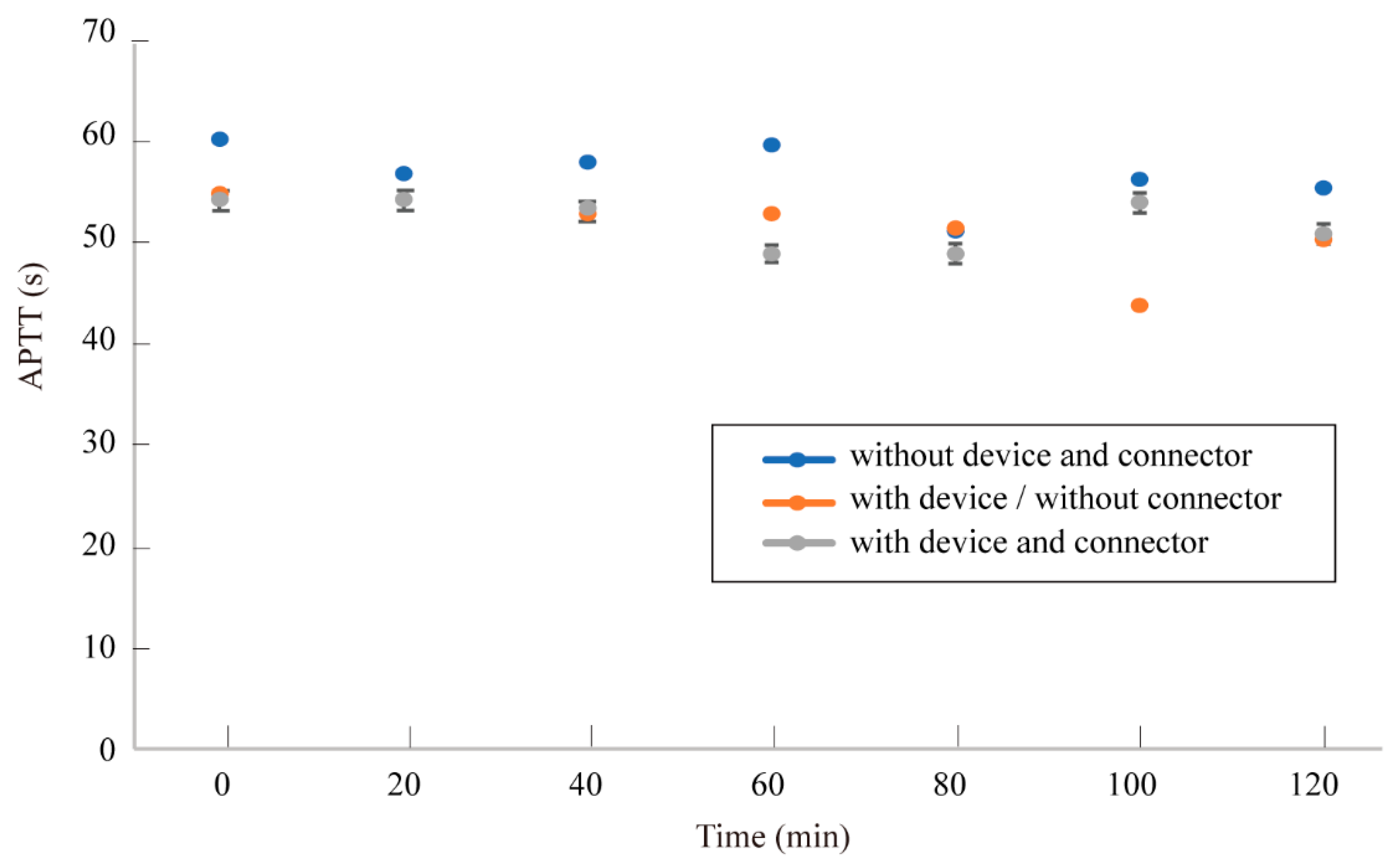
4.3. Blood Coagulation Caused by the Connector and the Filtering Device
5. Conclusions
Author Contributions
Funding
Conflicts of Interest
References
- Receveur, R.A.M.; Lindemans, F.W.; de Rooij, N.F. Microsystem technollgies for implantable applications. J. Micromech. Microeng. 2007, 17, R50–R80. [Google Scholar] [CrossRef]
- Alici, G. Towards soft robotic devices for site-specific drug delievery. Expert Rev. Med. Devices 2015, 12, 703–715. [Google Scholar] [CrossRef] [PubMed]
- Meng, E.; Sheybani, R. Insight: Implantable mediclal devices. Lab Chip 2014, 14, 3233. [Google Scholar] [CrossRef] [PubMed]
- Zahn, J.D.; Talbot, N.H.; Liepmann, D.; Pisano, A.P. Microfabricated polysilicon microneedles for minimally invasive biomedical devices. Biomed. Dev. 2000, 2, 295–303. [Google Scholar] [CrossRef]
- Arai, M.; Kudo, Y.; Miki, N. Polymer-based candle-shaped microneedle electrodes for electroencephalography on hairy skin. Jpn. J. Appl. Phys. 2016, 55, 06GP16. [Google Scholar] [CrossRef]
- Miki, N.; Kanno, Y. Development of a nanotechnology-based dialysis device. In Home Dialysis in Japan; Karger Publishers: Basel, Switzerland, 2012; pp. 178–183. [Google Scholar]
- To, N.; Sanada, I.; Ito, H.; Prihandana, G.S.; Morita, S.; Kanno, Y.; Miki, N. Water-permeable dialysis membranes for multi-layered microdialysis system. Front. Bioeng. Biotechnol. 2015, 3, 70. [Google Scholar] [CrossRef]
- Ota, T.; To, N.; Kanno, Y.; Miki, N. Evaluation of biofouling in stainless microfluidic channels for implantable multilayered dialysis device. Jpn. J. Appl. Phys. 2017, 56, 06GN10. [Google Scholar] [CrossRef]
- Mineshima, M.; Kawanishi, H.; Ase, T.; Kwasaki, T.; Tomo, T.; Nakamoto, H. 2016 update Japanese Society for Dialysis Therapy Standard of fluids for hemodialysis and related therapy. Ren. Replace Ther. 2018, 4, 15. [Google Scholar] [CrossRef]
- Van der Tol, A.; Lameire, N.; Morton, R.L.; Biesen, W.V.; Vanholder, R. An international analysis of dialysis services reimbursement. Clin. J. Am. Soc. Nephrol. 2019, 14, 84–93. [Google Scholar] [CrossRef]
- Kakisis, J.D.; Liapis, C.D.; Breuer, C.; Sumpio, B.E. Artificial blood vessel: The Holy Grail of peripheral vascular surgery. J. Vasc. Surg. 2005, 41, 349–354. [Google Scholar] [CrossRef]
- Byrom, M.J.; Ng, M.K.C.; Bannon, P.G. Biomechanics and biocompatibility of the perfect conduit—Can we build one? Ann. Cardiothorac. Surg. 2013, 2, 435–443. [Google Scholar] [CrossRef] [PubMed]
- Ito, E.; Okano, T. Artificial blood vessels: Structure and property of blood contacting surface. J. Surf. Finish. Soc. Jpn. 1998, 49, 715–721. [Google Scholar] [CrossRef]
- Palta, S.; Saroa, R.; Palta, A. Overview of the coagulation system. Indian J. Anaesth. 2014, 58, 515–523. [Google Scholar] [CrossRef] [PubMed]
- Fogelson, A.L.; Guy, R.D. Platelet-wall interactions in continuum models of platelet thrombosis: Formulation and numerical solution. Math. Med. Biol. 2004, 21, 293–334. [Google Scholar] [CrossRef] [PubMed]
- Basmadjian, D. The effect of flow and mass-transport in thrombogenesis. Ann. Biomed. Eng. 1990, 18, 685–709. [Google Scholar] [CrossRef] [PubMed]
- Shinoda, T.; Arakura, H.; Katakura, M.; Shirota, T.; Nakagawa, S. Usefulness of thrombelastgraphy for dosage monitoring of low molecular weight heparin and unfractionated heparin during hemodialysis. Artif. Organs 1990, 14, 413–415. [Google Scholar] [CrossRef] [PubMed]
- Chen, C.C.; You, J.Y.; Ho, C.H. The aPTT assay as a monitor of heparin anticoagulation efficacy in clinical settings. Adv. Ther. 2003, 20, 231–236. [Google Scholar] [CrossRef]
- Prihandana, G.S.; Sanada, I.; Ito, H.; Noborisaka, M.; Kanno, Y.; Suzuki, T.; Miki, N. Antithrombogenicity of fluorinated diamond-like carbon films coated nano porous polyethersulfone (PES) membrane. Materials 2013, 6, 4309–4323. [Google Scholar] [CrossRef]
- Ye, G.; Miki, N. Multilayered microfilter using PES nano porous membrane applicable as the dialyzer of a wearable artificial kidney. J. Micromech. Microeng. 2009, 19, 065031. [Google Scholar]
- Weber, M.; Steinle, H.; Golombek, S.; Hann, L.; Schlensak, C.; Wendel, H.P.; Avci-Adali, M. Blood-contacting biomaterials: In vitro evaluation of the hemocompatibility. Front. Bioeng. Biotechnol. 2018, 6, 99. [Google Scholar] [CrossRef]
- Van Oeveren, W.; Haan, J.; Lagerman, P.; Schoen, P. Comparison of coagulation activity tests in vitro for selected biomaterials. Artif. Organs 2002, 26, 506–511. [Google Scholar] [CrossRef] [PubMed]
- Stang, K.; Krajewski, S.; Neumann, B.; Kurz, J.; Post, M.; Stoppelkamp, S.; Fennrich, S.; Avci-Adali, M.; Armbruster, D.; Schlensak, C.; et al. Hemocompatibility testing according to ISO 10993-4: Discrimination between pyrogen-and device-induced hemostatic activation. Mater. Sci. Eng. C 2014, 42, 422–428. [Google Scholar] [CrossRef] [PubMed]
- Noishiki, N. A concept of tissue engineering in the development of small diameter vascular prothesis. Artif. Organ. 1998, 27, 601–607. [Google Scholar] [CrossRef]
- Xue, L.; Greisler, H.P. Biomaterials in the development and future of vascular grafts. J. Vasc. Surg. 2003, 37, 472–480. [Google Scholar] [CrossRef] [PubMed]


© 2019 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Watanabe, A.; Miki, N. Connecting Mechanism for Artificial Blood Vessels with High Biocompatibility. Micromachines 2019, 10, 429. https://doi.org/10.3390/mi10070429
Watanabe A, Miki N. Connecting Mechanism for Artificial Blood Vessels with High Biocompatibility. Micromachines. 2019; 10(7):429. https://doi.org/10.3390/mi10070429
Chicago/Turabian StyleWatanabe, Ai, and Norihisa Miki. 2019. "Connecting Mechanism for Artificial Blood Vessels with High Biocompatibility" Micromachines 10, no. 7: 429. https://doi.org/10.3390/mi10070429
APA StyleWatanabe, A., & Miki, N. (2019). Connecting Mechanism for Artificial Blood Vessels with High Biocompatibility. Micromachines, 10(7), 429. https://doi.org/10.3390/mi10070429





