Effects of Flexor Digitorum Longus Muscle Anatomical Structure on the Response to Botulinum Toxin Treatment in Patients with Post-Stroke Claw Foot Deformity
Abstract
1. Introduction
2. Results
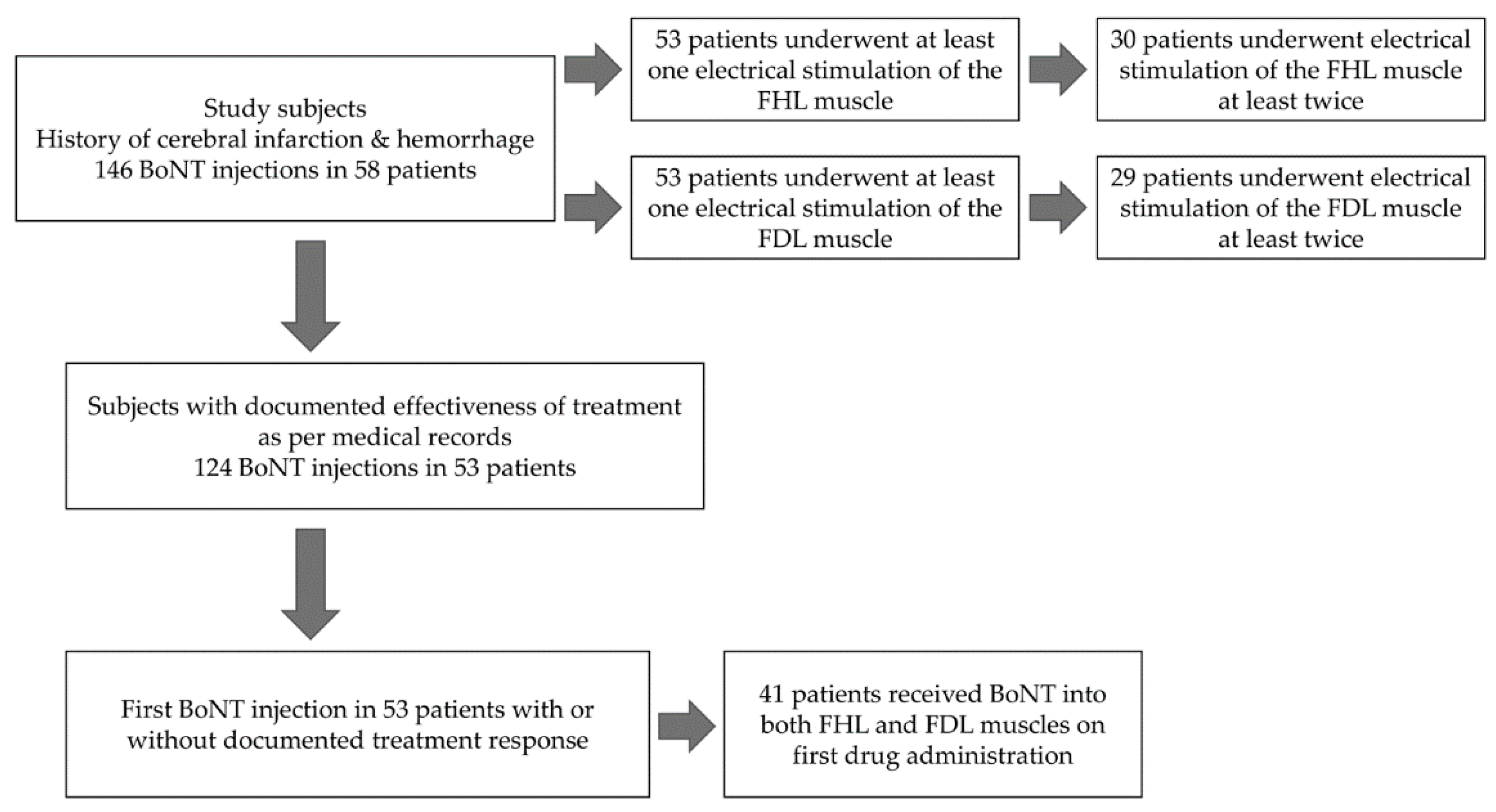
2.1. Overview of All Injections Performed
2.2. Classification According to the Induced Toe Movement
2.2.1. Classification about FHL Muscle
2.2.2. Classification about FDL Muscle
2.3. The Degree of “Variability” in FHL and FDL Control of Each Toe
2.4. Changes in Subjective Symptoms after BoNT Injection
2.5. The Effects of MCT or NSM on Therapeutic Effects of BoNT Injection
2.5.1. About Therapeutic Effects of All BoNT Injection (n = 124)
2.5.2. About Therapeutic Effects of the First BoNT Injection (n = 53)
2.6. Correlation between the NSM of the FHL and the NSM of the FDL
3. Discussion
4. Conclusions
5. Materials and Methods
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Takekawa, T.; Mochio, K.; Sato, T.; Katsurada, K.; Fukata, M.; Aoto, M.; Kinoshita, K.; Abo, M. An Important Consideration when Using Botulinum Toxin Injections for Treating Claw Foot Deformity. Jpn. J. Rehabil. Med. 2015, 52, 615–620. (In Japanese) [Google Scholar] [CrossRef][Green Version]
- Takekawa, T.; Takagi, S.; Kitajima, T.; Sato, T.; Kinoshita, K.; Abo, M. Claw Toe: Anatomic Guide for Injection of Botulinum Toxin into Foot Muscles. Can. J. Neurol. Sci. 2021, 1–7. [Google Scholar] [CrossRef] [PubMed]
- Kaji, R.; Osako, Y.; Suyama, K.; Maeda, T.; Uechi, Y.; Iwasaki, M.; GSK1358820 Spasticity Study Group. Botulinum Toxin Type A in Post-Stroke Lower Limb Spasticity: A Multicenter, Double-Blind. Placebo-Control. Trial. J. Neurol. 2010, 257, 1330–1337. [Google Scholar]
- Kimura, A.; Abo, M.; Kawate, N.; Ohsako, Y.; Suyama, K.; Maeda, T.; Uechi, Y.; Iwasaki, M. Clinical evaluation of botulinum toxin type A for post-stroke limb spasticity: Placebo-controlled double-blind intergroup comparison study and open label repeated dose study. Jpn. J. Rehabil. Med. 2010, 47, 626–636. (In Japanese) [Google Scholar] [CrossRef]
- Hesse, S.; Lucke, D.; Malezic, M.; Bertelt, C.; Friedrich, H.; Gregoric, M.; Mauritz, K.H. Botulinum Toxin Treatment for Lower Limb Extensor Spasticity in Chronic Hemiparetic Patients. J. Neurol. Neurosurg. Psychiatry 1994, 57, 1321–1324. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Dunne, J.W.; Heye, N.; Dunne, S.L. Treatment of Chronic Limb Spasticity with Botulinum Toxin A. J. Neurol. Neurosurg. Psychiatry 1995, 58, 232–235. [Google Scholar] [CrossRef] [PubMed]
- Laurent, G.; Valentini, F.; Loiseau, K.; Hennebelle, D.; Robain, G. Claw Toes in Hemiplegic Patients After Stroke. Ann. Phys. Rehabil. Med. 2010, 53, 77–85. [Google Scholar] [CrossRef] [PubMed]
- Lim, E.C.; Ong, B.K.; Seet, R.C. Botulinum Toxin-A Injections for Spastic Toe Clawing. Parkinsonism Relat. Disord. 2006, 12, 43–47. [Google Scholar] [CrossRef] [PubMed]
- Lee, J.H.; Han, S.H.; Ye, J.F.; Lee, B.N.; An, X.; Kwon, S.O. Effective Zone of Botulinum Toxin a Injections in Hallux Claw Toe Syndrome: An Anatomical Study. Muscle Nerv. 2012, 45, 217–221. [Google Scholar] [CrossRef] [PubMed]
- Ishikawa, K.; Yamashita, S.; Akaoka, S.; Fujisawa, M.; Katagi, Y. Botulinum toxin treatment for claw toe. Curr. Pr. Neurosurg. 2013, 23, 89–93. (In Japanese) [Google Scholar]
- Dan, S.; Tomaru, T.; Igarashi, Y.; Ishihama, H.; Kanamori, H.; Momma, H.; Chino, N.; Takahashi, H.; Okajima, Y. A case report of Botulinum toxin type: A injection for effective treatment of hammer toes and foot inversion caused by spastic hemiplegia. Gen. Rehabil. 2014, 42, 261–264. (In Japanese) [Google Scholar]
- Ishikawa, K.; Yamashita, S.; Fujisawa, M.; Katagi, Y. Botulinum toxin treatment for different deformities of toe flexion after stroke: Case report. Gen. Rehabil. 2014, 42, 989–992. (In Japanese) [Google Scholar]
- O’Sullivan, E.; Carare-Nnadi, R.; Greenslade, J.; Bowyer, G. Clinical Significance of Variations in the Interconnections between Flexor Digitorum Longus and Flexor Hallucis Longus in the Region of the Knot of Henry. Clin. Anat. 2005, 18, 121–125. [Google Scholar] [CrossRef] [PubMed]
- Matsui, T.; Kinoshita, M.; Taguchi, Y. Tendinous Fusion of the Flexor Pollicis Longus Muscle and Flexor Digitorum Longus Muscle. Seik. Geka. 1971, 22, 228–231. [Google Scholar]
- Beger, O.; Elvan, Ö.; Keskinbora, M.; Ün, B.; Uzmansel, D.; Kurtoğlu, Z. Anatomy of Master Knot of Henry: A Morphometric Study on Cadavers. Acta Orthop. Traumatol. Turc. 2018, 52, 134–142. [Google Scholar] [CrossRef] [PubMed]
- LaRue, B.G.; Anctil, E.P. Distal Anatomical Relationship of the Flexor Hallucis Longus and Flexor Digitorum Longus Tendons. Foot Ankle Int. 2006, 27, 528–532. [Google Scholar] [CrossRef] [PubMed]
- Hur, M.S.; Kim, J.H.; Woo, J.S.; Choi, B.Y.; Kim, H.J.; Lee, K.S. An Anatomic Study of the Quadratus Plantae in Relation to Tendinous Slips of the Flexor Hallucis Longus for Gait Analysis. Clin. Anat. 2011, 24, 768–773. [Google Scholar] [CrossRef] [PubMed]
- Edama, M.; Kubo, M.; Onishi, H.; Takabayashi, T.; Yokoyama, E.; Inai, T.; Watanabe, H.; Nashimoto, S.; Kageyama, I. Anatomical Study of Toe Flexion by Flexor Hallucis Longus. Ann. Anat. 2016, 204, 80–85. [Google Scholar] [CrossRef] [PubMed]
- Ali, S.; Griffin, N.L.; Ellis, W.; Meyr, A.J. Communication of Contrast in the Flexor Hallucis Longus Tendon with Other Pedal Tendons at the Master Knot of Henry. J. Am. Podiatr. Med. Assoc. 2017, 107, 166–170. [Google Scholar] [CrossRef] [PubMed]
- Bohannon, R.W.; Smith, M.B. Interrater Reliability of a Modified Ashworth Scale of Muscle Spasticity. Phys. Ther. 1987, 67, 206–207. [Google Scholar] [CrossRef] [PubMed]
- Full prescribing information for BOTOX. BOTOX® (OnabotulinumtoxinA) for Injection, for Intramuscular, Intradetrusor, or Intradermal Use. Available online: https://www.rxabbvie.com/pdf/botox_pi.pdf (accessed on 23 September 2022).
- Royal College of Physicians; British Society of Rehabilitation Medicine; Chartered Society of Physiotherapy; Association of Chartered Physiotherapists Interested in Neurology. Spasticity in Adults; National Guidelines: London, UK, 2009. [Google Scholar]

| NSM | 1st Toe | 2nd Toe | 3rd Toe | 4th Toe | 5th Toe | MCT | |
|---|---|---|---|---|---|---|---|
| 1 | + | - | - | - | - | I | |
| 5 | |||||||
| 1 | + | ± | - | - | - | >II | |
| 1 | |||||||
| 2 | + | + | - | - | - | II | |
| 17 | |||||||
| 2 | + | + | ± | - | - | >III | |
| 2 | |||||||
| 3 | + | + | + | - | - | III | |
| 19 | |||||||
| 3 | + | + | + | ± | - | >IV | |
| 4 | |||||||
| 4 | + | + | + | + | - | IV | |
| 3 | |||||||
| 4 | + | + | + | + | ± | >V | |
| 2 | |||||||
| 5 | + | + | + | + | + | V | |
| 0 | |||||||
| total number | 53 |
| NSM | 1st Toe | 2nd Toe | 3rd Toe | 4th Toe | 5th Toe | MCT | |
|---|---|---|---|---|---|---|---|
| 1 | + | + | + | + | + | I | |
| 0 | |||||||
| 2 | ± | + | + | + | + | <I | |
| 1 | |||||||
| 2 | - | + | + | + | ± | >II | |
| 2 | |||||||
| 2 | - | + | + | + | + | II | |
| 16 | |||||||
| 3 | - | ± | + | + | ± | <>II | |
| 0 | |||||||
| 3 | - | ± | + | + | + | <II | |
| 18 | |||||||
| 3 | - | - | + | + | + | III | |
| 12 | |||||||
| 4 | - | - | ± | + | ± | <>III | |
| 1 | |||||||
| 4 | - | - | ± | + | + | <III | |
| 0 | |||||||
| 4 | - | - | - | + | + | IV | |
| 1 | |||||||
| 5 | - | - | - | ± | ± | <>IV | |
| 1 | |||||||
| 5 | - | - | - | ± | + | <IV | |
| 0 | |||||||
| 5 | - | - | - | - | + | V | |
| 1 | |||||||
| total number | 53 |
| OR | 95% CI | p Value | |
|---|---|---|---|
| MCT of FHL | 0.883 | 0.512–1.522 | 0.653 |
| NSM of FHL | 0.778 | 0.494–1.226 | 0.279 |
| MCT of FDL | 0.384 | 0.176–0.837 | 0.016 |
| NSM of FDL | 0.601 | 0.372–0.970 | 0.037 |
| MCT of FDL | 0.400 | 0.162–0.987 | 0.047 |
| disease | 5.787 | 2.369–14.134 | 0.000 |
| NSM of FDL | 0.685 | 0.419–1.119 | 0.130 |
| disease | 3.306 | 1.699–6.433 | 0.000 |
| OR | 95% CI | p Value | |
|---|---|---|---|
| NSM of FHL | * | ||
| disease | |||
| MCT of FHL | 1.031 | 0.484–2.196 | 0.936 |
| disease | 0.054 | 0.006–0.473 | 0.008 |
| NSM of FDL | 0.404 | 0.142–1.151 | 0.090 |
| disease | 5.712 | 1.056–30.884 | 0.043 |
| MCT of FDL | 0.168 | 0.033–0.857 | 0.032 |
| disease | 8.732 | 1.379–55.315 | 0.021 |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Takekawa, T.; Kobayashi, K.; Yamada, N.; Takagi, S.; Hara, T.; Kitajima, T.; Sato, T.; Sugihara, H.; Kinoshita, K.; Abo, M. Effects of Flexor Digitorum Longus Muscle Anatomical Structure on the Response to Botulinum Toxin Treatment in Patients with Post-Stroke Claw Foot Deformity. Toxins 2022, 14, 666. https://doi.org/10.3390/toxins14100666
Takekawa T, Kobayashi K, Yamada N, Takagi S, Hara T, Kitajima T, Sato T, Sugihara H, Kinoshita K, Abo M. Effects of Flexor Digitorum Longus Muscle Anatomical Structure on the Response to Botulinum Toxin Treatment in Patients with Post-Stroke Claw Foot Deformity. Toxins. 2022; 14(10):666. https://doi.org/10.3390/toxins14100666
Chicago/Turabian StyleTakekawa, Toru, Kazushige Kobayashi, Naoki Yamada, Satoshi Takagi, Takatoshi Hara, Tomohide Kitajima, Tomoharu Sato, Hiroshi Sugihara, Kazuo Kinoshita, and Masahiro Abo. 2022. "Effects of Flexor Digitorum Longus Muscle Anatomical Structure on the Response to Botulinum Toxin Treatment in Patients with Post-Stroke Claw Foot Deformity" Toxins 14, no. 10: 666. https://doi.org/10.3390/toxins14100666
APA StyleTakekawa, T., Kobayashi, K., Yamada, N., Takagi, S., Hara, T., Kitajima, T., Sato, T., Sugihara, H., Kinoshita, K., & Abo, M. (2022). Effects of Flexor Digitorum Longus Muscle Anatomical Structure on the Response to Botulinum Toxin Treatment in Patients with Post-Stroke Claw Foot Deformity. Toxins, 14(10), 666. https://doi.org/10.3390/toxins14100666






