Higher Protein Intake Does Not Improve Lean Mass Gain When Compared with RDA Recommendation in Postmenopausal Women Following Resistance Exercise Protocol: A Randomized Clinical Trial
Abstract
:1. Introduction
2. Methods
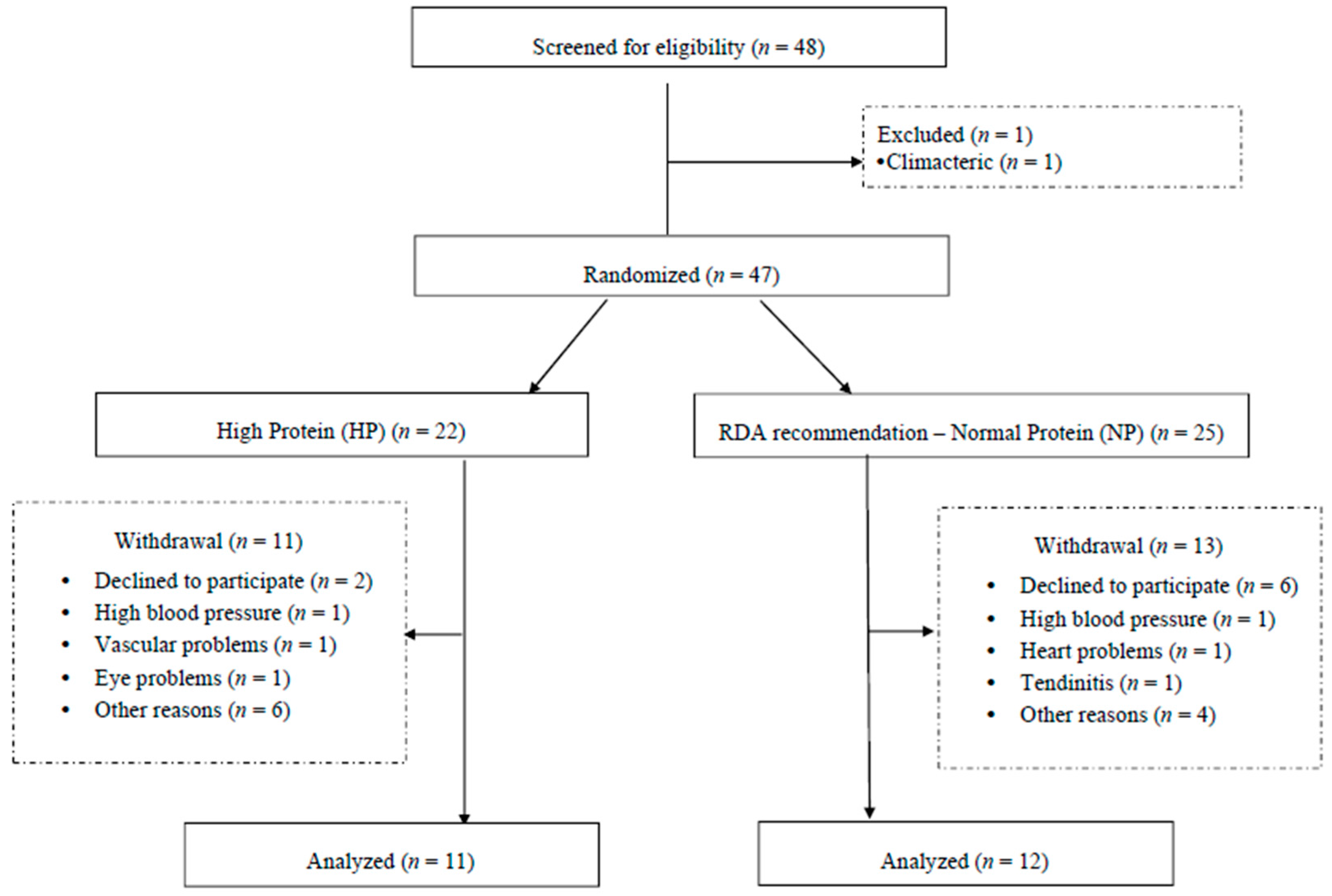
2.1. Research Participants
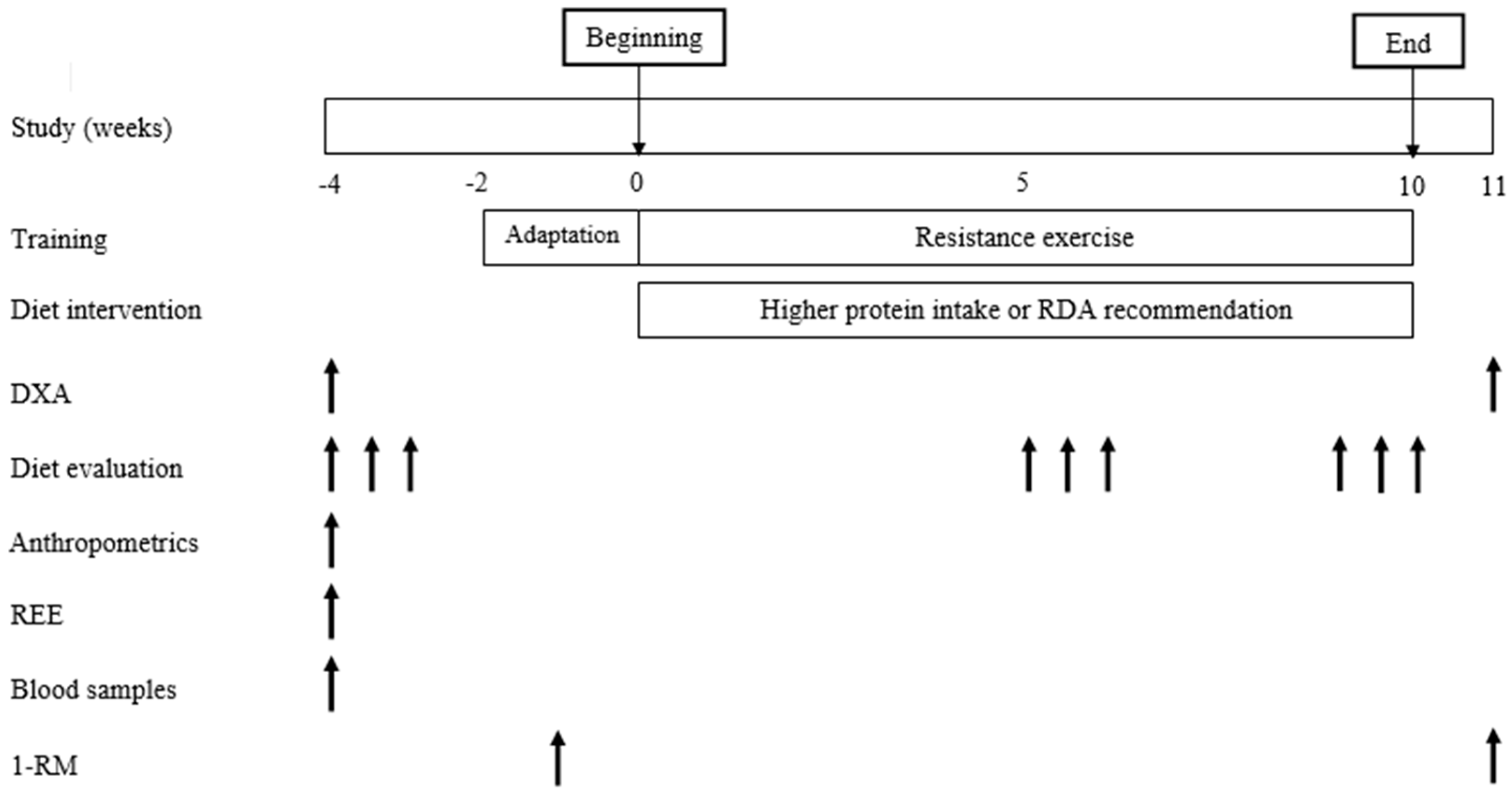
2.2. Study Design
2.3. Assessments
2.3.1. Anthropometry
2.3.2. Body Composition
2.4. Strength Measurement
2.5. Resting Energy Expenditure (REE) and Total Energy Expenditure (TEE)
2.6. Dietary Assessment
2.7. Blood Samples
2.8. Experimental Protocol
2.8.1. Dietary Intervention
2.8.2. Resistance Training
2.8.3. Statistics
3. Results
3.1. Baseline Characteristics
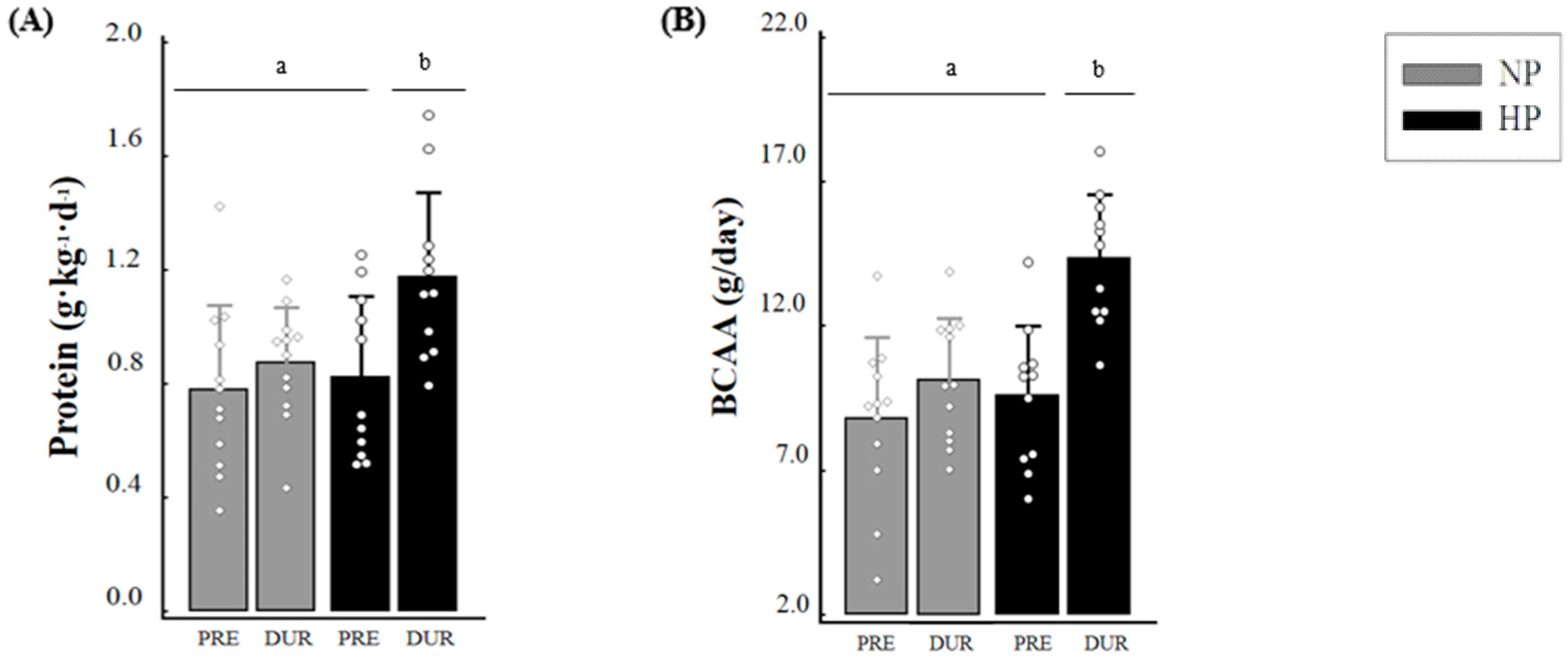
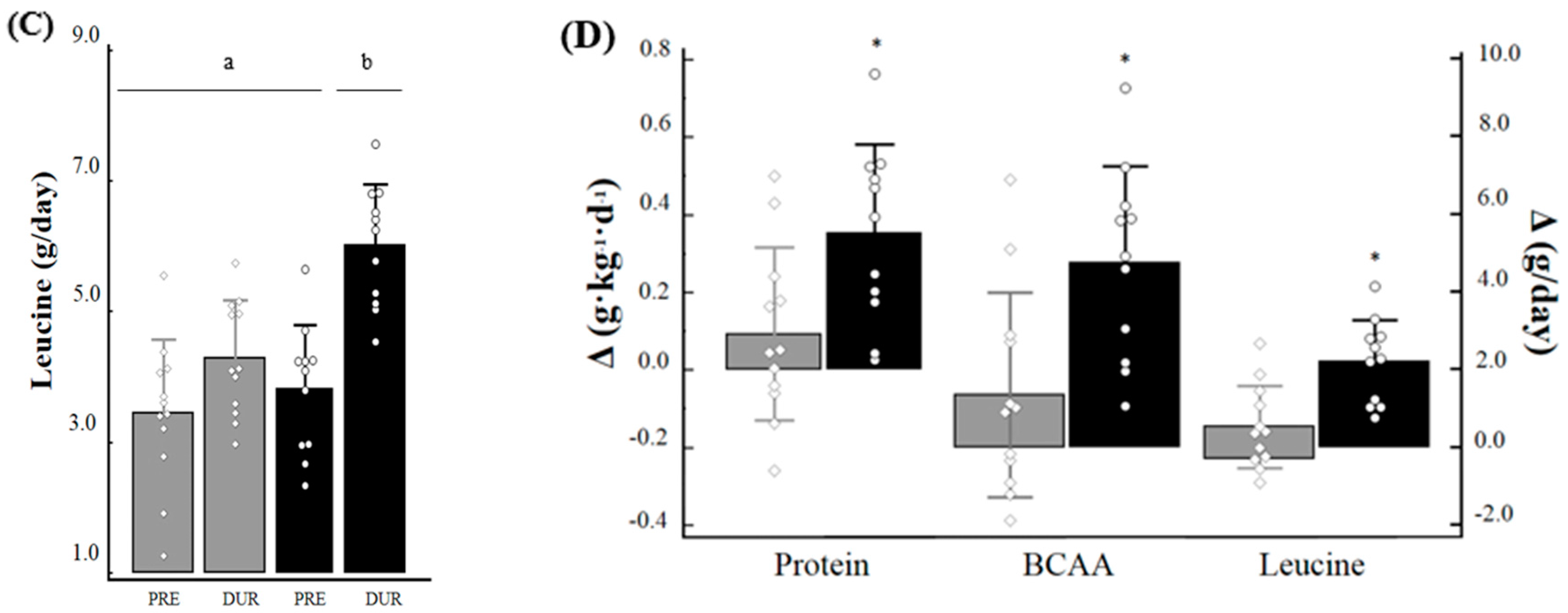
3.2. Dietary Intake
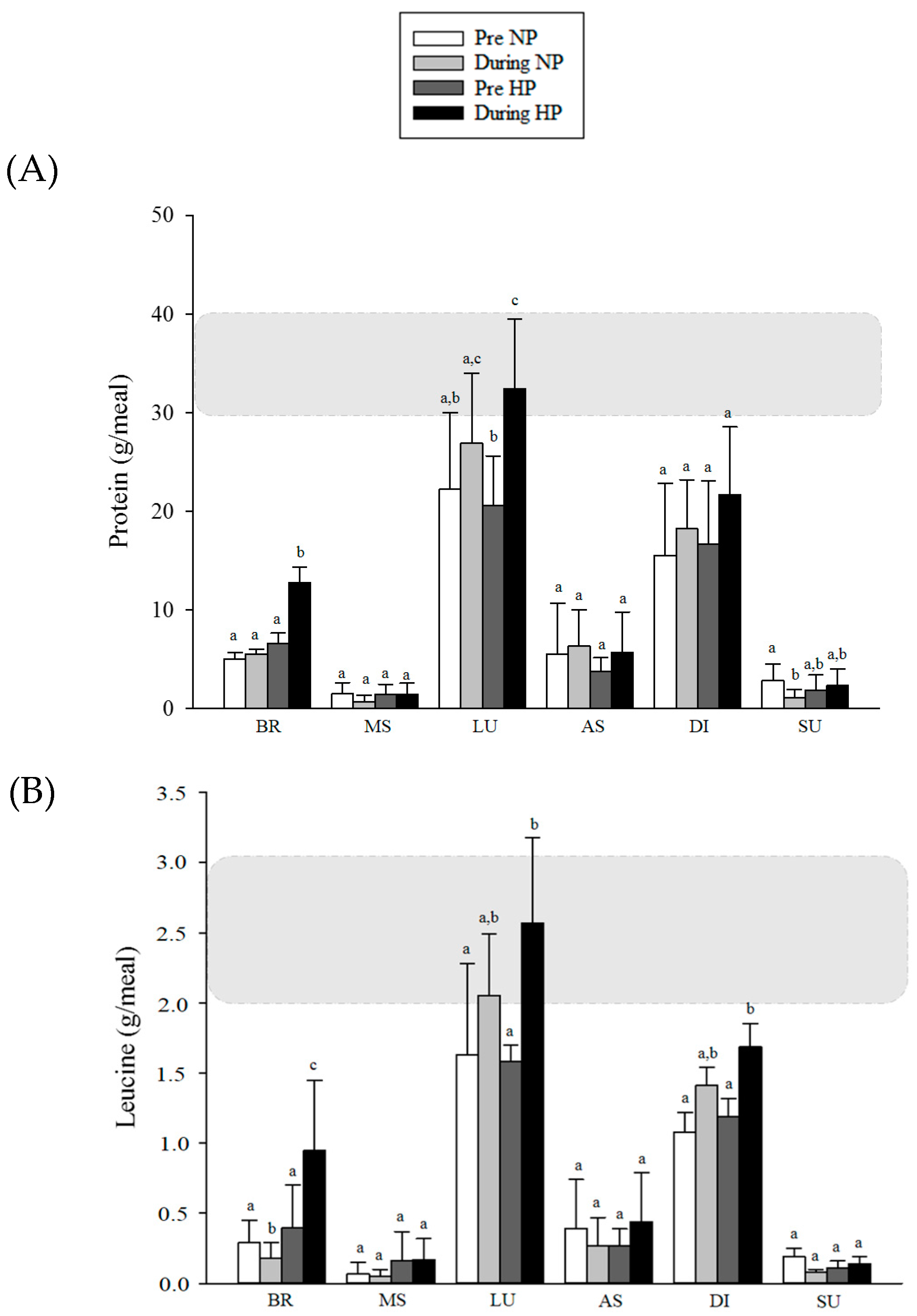
3.3. Distribution of Protein and Leucine during the Day
3.4. Strength
3.5. Body Composition
4. Discussion
5. Conclusions
Acknowledgments
Author Contributions
Conflicts of Interest
Appendix A
| Variables | NP (n = 12) | HP (n = 11) | p-Value | ||||
|---|---|---|---|---|---|---|---|
| Pre | Post | Pre | Post | Time | Treatment | Time × Treatment | |
| Strength | |||||||
| Bench press RM (kg) | 33.0 ± 4.9 a,b | 35.5 ±5.6 a,b | 32.2 ± 6.3 a | 34.3 ± 7.9 b | 0.002 | 0.644 | 0.215 |
| Leg extension RM (kg) | 71.1 ± 15.8 a,b | 77.8 ± 22.2 a,b | 75.3 ± 14.8 a | 84.7 ± 14.6 b | <0.001 | 0.394 | 0.498 |
References
- Fielding, R.A.; Vellas, B.; Evans, W.J.; Bhasin, S.; Morley, J.E.; Newman, A.B.; Abellan van Kan, G.; Andrieu, S.; Bauer, J.; Breuille, D.; et al. Sarcopenia: An undiagnosed condition in older adults. Current consensus definition: Prevalence, etiology, and consequences. International working group on sarcopenia. J. Am. Med. Dir. Assoc. 2011, 12, 249–256. [Google Scholar] [CrossRef] [PubMed]
- Kim, T.N.; Choi, K.M. Sarcopenia: Definition, epidemiology, and pathophysiology. J. Bone Metab. 2013, 20, 1–10. [Google Scholar] [CrossRef] [PubMed]
- Moore, D.R.; Churchward-Venne, T.A.; Witard, O.; Breen, L.; Burd, N.A.; Tipton, K.D.; Phillips, S.M. Protein ingestion to stimulate myofibrillar protein synthesis requires greater relative protein intakes in healthy older versus younger men. J. Gerontol. A Biol. Sci. Med. Sci. 2015, 70, 57–62. [Google Scholar] [CrossRef] [PubMed]
- Wall, B.T.; Gorissen, S.H.; Pennings, B.; Koopman, R.; Groen, B.B.L.; Verdijk, L.B.; van Loon, L.J.C. Aging is accompanied by a blunted muscle protein synthetic response to protein ingestion. PLoS ONE 2015, 10, e0140903. [Google Scholar] [CrossRef] [PubMed]
- English, K.L.; Mettler, J.A.; Ellison, J.B.; Mamerow, M.M.; Arentson-Lantz, E.; Pattarini, J.M.; Ploutz-Snyder, R.; Sheffield-Moore, M.; Paddon-Jones, D. Leucine partially protects muscle mass and function during bed rest in middle-aged adults. Am. J. Clin. Nutr. 2016, 103, 465–473. [Google Scholar] [CrossRef] [PubMed]
- Burger, H.G.; Hale, G.E.; Robertson, D.M.; Dennerstein, L. A review of hormonal changes during the menopausal transition: Focus on findings from the Melbourne Women’s Midlife Health Project. Hum. Reprod. Update 2007, 13, 559–565. [Google Scholar] [CrossRef] [PubMed]
- Hall, J.E. Endocrinology of the Menopause. Endocrinol. Metab. Clin. N. Am. 2015, 44, 485–496. [Google Scholar] [CrossRef] [PubMed]
- Orsatti, F.L.; de Oliveira, E.P.; Burini, R.C. Relationship between plasma hormones and anthropometric measures of muscle mass in postmenopausal women. In Handbook of Anthropometry; Springer: New York, NY, USA, 2012; pp. 1481–1490. [Google Scholar]
- Kamel, H.K.; Maas, D.; Duthie, E.H., Jr. Role of hormones in the pathogenesis and management of sarcopenia. Drugs Aging 2002, 19, 865–877. [Google Scholar] [CrossRef] [PubMed]
- Shaw, B.S.; Gouveia, M.; McIntyre, S.; Shaw, I. Anthropometric and cardiovascular responses to hypertrophic resistance training in postmenopausal women. Menopause 2016, 23, 1176–1181. [Google Scholar] [CrossRef] [PubMed]
- Cermak, N.M.; Res, P.T.; de Groot, L.C.; Saris, W.H.; van Loon, L.J. Protein supplementation augments the adaptive response of skeletal muscle to resistance-type exercise training: A meta-analysis. Am. J. Clin. Nutr. 2012, 96, 1454–1464. [Google Scholar] [CrossRef] [PubMed]
- Lixandrao, M.E.; Damas, F.; Chacon-Mikahil, M.P.; Cavaglieri, C.R.; Ugrinowitsch, C.; Bottaro, M.; Vechin, F.C.; Conceicao, M.S.; Berton, R.; Libardi, C.A. Time course of resistance training-induced muscle hypertrophy in the elderly. J. Strength Cond. Res. 2016, 30, 159–163. [Google Scholar] [CrossRef] [PubMed]
- Tieland, M.; Dirks, M.L.; van der Zwaluw, N.; Verdijk, L.B.; van de Rest, O.; de Groot, L.C.; van Loon, L.J. Protein supplementation increases muscle mass gain during prolonged resistance-type exercise training in frail elderly people: A randomized, double-blind, placebo-controlled trial. J. Am. Med. Dir. Assoc. 2012, 13, 713–719. [Google Scholar] [CrossRef] [PubMed]
- Breen, L.; Phillips, S.M. Nutrient interaction for optimal protein anabolism in resistance exercise. Curr. Opin. Clin. Nutr. Metab. Care 2012, 15, 226–232. [Google Scholar] [CrossRef] [PubMed]
- IOM. Dietary Reference Intakes for Energy, Carbohydrate, Fiber, Fat, Fatty Acids, Cholesterol, Protein, and Amino Acids; National Academies Press: Washington, DC, USA, 2005. [Google Scholar]
- McDonald, C.K.; Ankarfeldt, M.Z.; Capra, S.; Bauer, J.; Raymond, K.; Heitmann, B.L. Lean body mass change over 6 years is associated with dietary leucine intake in an older Danish population. Br. J. Nutr. 2016, 115, 1556–1562. [Google Scholar] [CrossRef] [PubMed]
- Bauer, J.; Biolo, G.; Cederholm, T.; Cesari, M.; Cruz-Jentoft, A.J.; Morley, J.E.; Phillips, S.; Sieber, C.; Stehle, P.; Teta, D.; et al. Evidence-based recommendations for optimal dietary protein intake in older people: A position paper from the PROT-AGE Study Group. J. Am. Med. Dir. Assoc. 2013, 14, 542–559. [Google Scholar] [CrossRef] [PubMed]
- Phillips, S.M.; Chevalier, S.; Leidy, H.J. Protein “requirements” beyond the RDA, implications for optimizing health. Appl. Physiol. Nutr. Metab. 2016, 41, 565–572. [Google Scholar] [CrossRef] [PubMed]
- Paddon-Jones, D.; Campbell, W.W.; Jacques, P.F.; Kritchevsky, S.B.; Moore, L.L.; Rodriguez, N.R.; van Loon, L.J. Protein and healthy aging. Am. J. Clin. Nutr. 2015. [Google Scholar] [CrossRef] [PubMed]
- Rafii, M.; Chapman, K.; Owens, J.; Elango, R.; Campbell, W.W.; Ball, R.O.; Pencharz, P.B.; Courtney-Martin, G. Dietary protein requirement of female adults >65 years determined by the indicator amino acid oxidation technique is higher than current recommendations. J. Nutr. 2015, 145, 18–24. [Google Scholar] [CrossRef] [PubMed]
- Tang, M.; McCabe, G.P.; Elango, R.; Pencharz, P.B.; Ball, R.O.; Campbell, W.W. Assessment of protein requirement in octogenarian women with use of the indicator amino acid oxidation technique. Am. J. Clin. Nutr. 2014, 99, 891–898. [Google Scholar] [CrossRef] [PubMed]
- Murphy, C.; Devries, M.C.; Mcglory, C.; Phillips, S.M. Leucine supplementation enhances integrative myofibrillar protein synthesis in free-living older men consuming lower- and higher-protein diets: A parallel-group crossover study. Am. J. Clin. Nutr. 2016, 104, 1594–1606. [Google Scholar] [CrossRef] [PubMed]
- Mitchell, C.J.; Churchward-Venne, T.A.; Parise, G.; Bellamy, L.; Baker, S.K.; Smith, K.; Atherton, P.J.; Phillips, S.M. Acute post-exercise myofibrillar protein synthesis is not correlated with resistance training-induced muscle hypertrophy in young men. PLoS ONE 2014, 9, e89431. [Google Scholar] [CrossRef] [PubMed]
- Faul, F.; Erdfelder, E.; Lang, A.G.; Buchner, A. G*Power 3: A flexible statistical power analysis program for the social, behavioral, and biomedical sciences. Behav. Res. Methods 2007, 39, 175–191. [Google Scholar] [CrossRef] [PubMed]
- Lohman, T.G.; Roche, A.F.; Martorell, R. Anthropometric Standardization Reference Manual; Human Knectis: Champaign, IL, USA, 1988. [Google Scholar]
- Orsatti, F.L.; Nahas, E.A.; Orsatti, C.L.; de Oliveira, E.P.; Nahas-Neto, J.; da Mota, G.R.; Burini, R.C. Muscle mass gain after resistance training is inversely correlated with trunk adiposity gain in postmenopausal women. J. Strength Cond. Res. 2012, 26, 2130–2139. [Google Scholar] [CrossRef] [PubMed]
- Damask, M.C.; Weissman, C.; Askanazi, J.; Hyman, A.I.; Rosenbaum, S.H.; Kinney, J.M. A systematic method for validation of gas exchange measurements. Anesthesiology 1982, 57, 213–218. [Google Scholar] [CrossRef] [PubMed]
- De Oliveira, E.P.; Orsatti, F.L.; Teixeira, O.; Maesta, N.; Burini, R.C. Comparison of predictive equations for resting energy expenditure in overweight and obese adults. J. Obes. 2011, 2011. [Google Scholar] [CrossRef] [PubMed]
- Weir, J.B. New methods for calculating metabolic rate with special reference to protein metabolism. J. Physiol. 1949, 109, 1–9. [Google Scholar] [CrossRef] [PubMed]
- Food and Agriculture Organization of the United Nations (FAO); World Health Organization (WHO); United Nations University (UNU). Energy and Protein Requirements; Report of a Joint FAO/WHO/UNU Expert Consultation; World Health Organization Technical Report Series; World Health Organization: Geneva, Switzerland, 1985; Volume 742, pp. 1–206. [Google Scholar]
- Ainsworth, B.E.; Haskell, W.L.; Leon, A.S.; Jacobs, D.R., Jr.; Montoye, H.J.; Sallis, J.F.; Paffenbarger, R.S., Jr. Compendium of physical activities: Classification of energy costs of human physical activities. Med. Sci. Sports Exerc. 1993, 25, 71–80. [Google Scholar] [CrossRef] [PubMed]
- Volek, J.S.; Forsythe, C.E.; Kraemer, W.J. Nutritional aspects of women strength athletes. Br. J. Sports Med. 2006, 40, 742–748. [Google Scholar] [CrossRef] [PubMed]
- United States Department of Agriculture (USDA) Food Composition Databases; slightly revised May; United States Department of Agriculture (USDA): Washington, DC, USA, 2006.
- United States Department of Agriculture (USDA). Food Composition Databases; Release 20 slightly revised; United States Department of Agriculture (USDA): Washington, DC, USA, 2006.
- Naderi, A.; de Oliveira, E.P.; Ziegenfuss, T.N.; Willems, M.E.T. Timing optimal dose and intake duration of dietary supplements with evidence-based use in sports nutrition. J. Exerc. Nutr. Biochem. 2016, 20, 1–12. [Google Scholar] [CrossRef] [PubMed]
- American College of Sports Medicine (ACSM). American College of Sports Medicine’s Health-Related Physical Fitness Assessment Manual; American College of Sports Medicine (ACSM): Indianapolis, IN, USA, 2013. [Google Scholar]
- Stark, M.; Lukaszuk, J.; Prawitz, A.; Salacinski, A. Protein timing and its effects on muscular hypertrophy and strength in individuals engaged in weight-training. J. Int. Soc. Sports Nutr. 2012, 9, 54. [Google Scholar] [CrossRef] [PubMed]
- Trumbo, P.; Schlicker, S.; Yates, A.A.; Poos, M. Food and Nutrition Board of the Institute of Medicine, the National Academies. Dietary Reference Intakes for Energy, Carbohydrate, Fiber, Fat, Fatty Acids, Cholesterol, Protein, and Amino Acids and Protein and Amino Acids. J. Am. Diet Assoc. 2002, 102, 1621–1630. [Google Scholar] [CrossRef]
- Thomas, D.T.; Erdman, K.A.; Burke, L.M. American college of sports medicine joint position statement. nutrition and athletic performance. Med. Sci. Sports Exerc. 2016, 48, 543–568. [Google Scholar] [PubMed]
- Paddon-Jones, D.; Leidy, H. Dietary protein and muscle in older persons. Curr. Opin. Clin. Nutr. Metab. Care 2014, 17, 5–11. [Google Scholar] [CrossRef] [PubMed]
- Murphy, C.H.; Oikawa, S.Y.; Phillips, S.M. Dietary protein to maintain muscle mass in aging: A case for per-meal protein recommendations. J. Frailty Aging 2016, 5, 49–58. [Google Scholar] [PubMed]
- Farsijani, S.; Morais, J.; Payette, H.; Gaudreau, P.; Shatenstein, B.; Gray-Donald, K.; Chevalier, S. Relation between mealtime distribution of protein intake and lean mass loss in free-living older adults of the NuAge study. Am. J. Clin. Nutr. 2016, 103, 694–703. [Google Scholar] [CrossRef] [PubMed]
- Loenneke, J.P.; Loprinzi, P.D.; Murphy, C.H.; Phillips, S.M. Per meal dose and frequency of protein consumption is associated with lean mass and muscle performance. Clin. Nutr. 2016, 35, 1506–1511. [Google Scholar] [CrossRef] [PubMed]
- Casperson, S.L.; Sheffield-Moore, M.; Hewlings, S.J.; Paddon-Jones, D. Leucine supplementation chronically improves muscle protein synthesis in older adults consuming the RDA for protein. Clin. Nutr. 2012, 31, 512–519. [Google Scholar] [CrossRef] [PubMed]
- Yang, Y.; Breen, L.; Burd, N.A.; Hector, A.J.; Churchward-Venne, T.A.; Josse, A.R.; Tarnopolsky, M.A.; Phillips, S.M. Resistance exercise enhances myofibrillar protein synthesis with graded intakes of whey protein in older men. Br. J. Nutr. 2012, 108, 1780–1788. [Google Scholar] [CrossRef] [PubMed]
- Breen, L.; Phillips, S.M. Skeletal muscle protein metabolism in the elderly: Interventions to counteract the ‘anabolic resistance’ of ageing. Nutr. Metab. 2011, 8, 68. [Google Scholar] [CrossRef] [PubMed]
- Chrusch, M.J.; Chilibeck, P.D.; Chad, K.E.; Davison, K.S.; Burke, D.G. Creatine supplementation combined with resistance training in older men. Med. Sci. Sports Exerc. 2001, 33, 2111–2117. [Google Scholar] [CrossRef] [PubMed]
- Weinheimer, E.M.; Sands, L.P.; Campbell, W.W. A systematic review of the separate and combined effects of energy restriction and exercise on fat-free mass in middle-aged and older adults: Implications for sarcopenic obesity. Nutr. Rev. 2010, 68, 375–388. [Google Scholar] [CrossRef] [PubMed]
- Platte, P.; Pirke, K.M.; Wade, S.E.; Trimborn, P.; Fichter, M.M. Physical activity, total energy expenditure, and food intake in grossly obese and normal weight women. Int. J. Eat. Disord. 1995, 17, 51–57. [Google Scholar] [CrossRef]
- Orsatti, F.L.; Maestá, N.; de Oliveira, E.P.; Nahas-Neto, J.; Burini, R.C.; Nunes, P.R.P.; Souza, A.P.; Nahas, E.A.P. Adding soy protein to milk enhance the effect of resistance training on muscle strength in postmenopausal women. J. Diet. Suppl. 2017. [Google Scholar] [CrossRef] [PubMed]
- Ribeiro, A.S.; Tomeleri, C.M.; Souza, M.F.; Pina, F.L.; Schoenfeld, B.J.; Nascimento, M.A.; Venturini, D.; Barbosa, D.S.; Cyrino, E.S. Effect of resistance training on C-reactive protein, blood glucose and lipid profile in older women with differing levels of RT experience. Age (Dordr.) 2015, 37, 109. [Google Scholar] [CrossRef] [PubMed]
- Lafay, L.; Mennen, L.; Basdevant, A.; Charles, M.A.; Borys, J.M.; Eschwege, E.; Romon, M. Does energy intake underreporting involve all kinds of food or only specific food items? Results from the Fleurbaix Laventie Ville Sante (FLVS) study. Int. J. Obes. Relat. Metab. Disord. 2000, 24, 1500–1506. [Google Scholar] [CrossRef] [PubMed]

| Variables | NP | HP | p-Value |
|---|---|---|---|
| n = 12 | n = 11 | ||
| Age, years | 63.0 ± 8.6 | 63.4 ± 7.6 | 0.895 |
| Anthropometrics | |||
| Weight, kg | 69.0 ± 17.1 | 67.6 ± 15.6 | 0.840 |
| Height, m | 1.56 ± 0.08 | 1.55 ± 0.06 | 0.824 |
| BMI, kg/m2 | 28.4 ± 6.0 | 28.1 ± 5.5 | 0.894 |
| Body Composition | |||
| Total lean mass, kg | 37.6 ± 6.2 | 37.1 ± 6.2 | 0.857 |
| Leg lean mass, kg | 12.7 ± 2.6 | 12.7 ± 2.9 | 0.969 |
| MMI, kg/m2 | 6.9 ± 0.9 | 6.9 ± 1.2 | 0.934 |
| Total fat mass, kg * | 24.5 (20.5–33.5) | 27.7 (20.6–34.2) | 0.786 |
| Total fat mass, % | 40.7 ± 7.0 | 40.9 ± 4.7 | 0.938 |
| Trunk fat mass, kg * | 13.2 (11.2–19.6) | 13.6 (11.6–18.2) | 0.740 |
| Strength | |||
| Bench press 1-RM (kg) | 33.0 ± 4.9 | 32.2 ± 6.3 | 0.900 |
| Leg extension 1-RM (kg) | 71.1 ± 15.8 | 75.3 ± 14.8 | 0.518 |
| Biochemical parameters | |||
| Creatinine, mg/dL | 0.78 ± 0.16 | 0.80 ± 0.18 | 0.768 |
| Urea, mg/dL * | 27.7 (24.4–35.8) | 34.1 (30.3–36.0) | 0.104 |
| Energy expenditure | |||
| REE, kcal | 1582 ± 566 | 1394 ± 291 | 0.324 |
| TEE, kcal | 2127 ± 750 | 1881 ± 388 | 0.332 |
| Variables | NP (n = 12) | HP (n = 11) | p-Value | ||||
|---|---|---|---|---|---|---|---|
| Pre | During | Pre | During | Time | Intervention | Interaction | |
| Calories, kcal | 1342 ± 423 a | 1439 ± 205 a | 1412 ± 382 a | 1502 ± 214 a | 0.267 | 0.494 | 0.968 |
| Carbohydrate, g | 161.6 ± 54.4 a | 168.7 ± 31.0 a | 182.3 ± 52.6 a | 179.9 ± 33.3 a | 0.829 | 0.237 | 0.668 |
| Carbohydrate, % | 48.4 ± 8.1 a,b | 46.9 ± 6.2 a,b | 51.5 ± 3.7 a | 47.7 ± 3.6 b | 0.024 | 0.296 | 0.326 |
| Lipids, g | 51.9 ± 16.7 | 56.4 ± 12.5 a | 53.9 ± 16.5 a | 53.3 ± 10.1 a | 0.642 | 0.895 | 0.535 |
| Lipids, % | 35.0 ± 6.3 | 35.4 ± 6.9 a | 34.1 ± 2.7 a | 32.0 ± 3.1 a | 0.400 | 0.219 | 0.205 |
| Protein, g | 51.5 ± 15.3 a | 58.7 ± 10.4 a | 53.2 ± 13.5 a | 77.4 ± 10.5 b | <0.001 | 0.012 | 0.004 |
| Protein, % | 15.5 ± 2.9 a | 16.4 ± 2.2 a | 15.3 ± 2.7 a | 20.6 ± 2.6 b | <0.001 | 0.009 | <0.001 |
| Isoleucine, g * | 1.9 ± 0.6 a | 2.4 ± 0.5 b,c | 2.1 ± 0.5 a,c | 3.4 ± 0.5 d | <0.001 | 0.008 | 0.011 |
| Valine, g | 3.4 ± 1.0 a | 3.4 ± 0.7 a | 3.6 ± 0.9 a | 4.9 ± 0.8 b | 0.002 | 0.009 | 0.008 |
© 2017 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Rossato, L.T.; Nahas, P.C.; De Branco, F.M.S.; Martins, F.M.; Souza, A.P.; Carneiro, M.A.S.; Orsatti, F.L.; De Oliveira, E.P. Higher Protein Intake Does Not Improve Lean Mass Gain When Compared with RDA Recommendation in Postmenopausal Women Following Resistance Exercise Protocol: A Randomized Clinical Trial. Nutrients 2017, 9, 1007. https://doi.org/10.3390/nu9091007
Rossato LT, Nahas PC, De Branco FMS, Martins FM, Souza AP, Carneiro MAS, Orsatti FL, De Oliveira EP. Higher Protein Intake Does Not Improve Lean Mass Gain When Compared with RDA Recommendation in Postmenopausal Women Following Resistance Exercise Protocol: A Randomized Clinical Trial. Nutrients. 2017; 9(9):1007. https://doi.org/10.3390/nu9091007
Chicago/Turabian StyleRossato, Luana T., Paula C. Nahas, Flávia M. S. De Branco, Fernanda M. Martins, Aletéia P. Souza, Marcelo A. S. Carneiro, Fábio L. Orsatti, and Erick P. De Oliveira. 2017. "Higher Protein Intake Does Not Improve Lean Mass Gain When Compared with RDA Recommendation in Postmenopausal Women Following Resistance Exercise Protocol: A Randomized Clinical Trial" Nutrients 9, no. 9: 1007. https://doi.org/10.3390/nu9091007
APA StyleRossato, L. T., Nahas, P. C., De Branco, F. M. S., Martins, F. M., Souza, A. P., Carneiro, M. A. S., Orsatti, F. L., & De Oliveira, E. P. (2017). Higher Protein Intake Does Not Improve Lean Mass Gain When Compared with RDA Recommendation in Postmenopausal Women Following Resistance Exercise Protocol: A Randomized Clinical Trial. Nutrients, 9(9), 1007. https://doi.org/10.3390/nu9091007






