A High Fiber Cookie Made with Resistant Starch Type 4 Reduces Post-Prandial Glucose and Insulin Responses in Healthy Adults
Abstract
:1. Introduction
2. Materials and Methods
2.1. Study Subjects
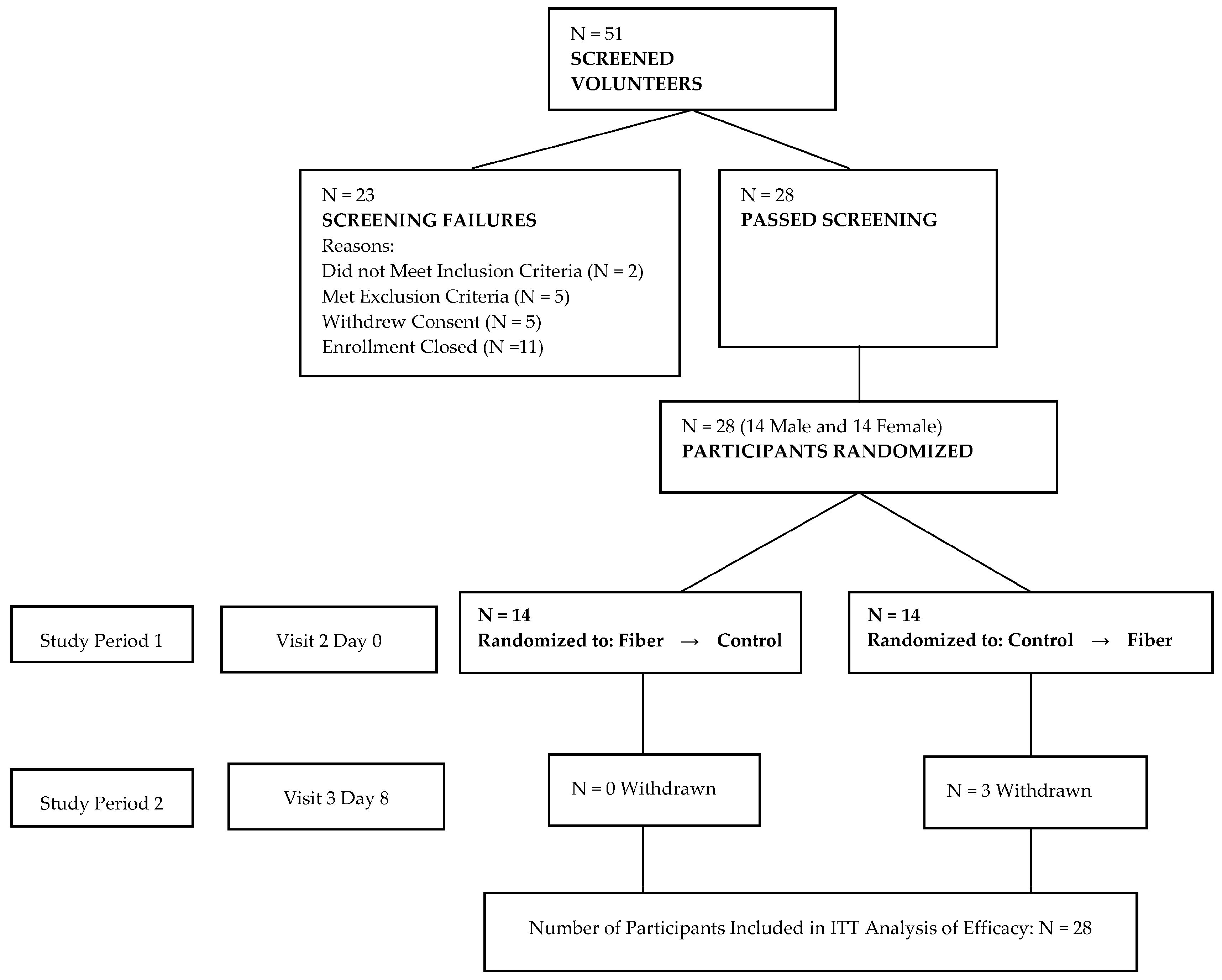
2.2. Study Design
2.3. Study Foods
2.4. Sample Size Calculation
2.5. Statistical Analysis
3. Results
3.1. Demographics
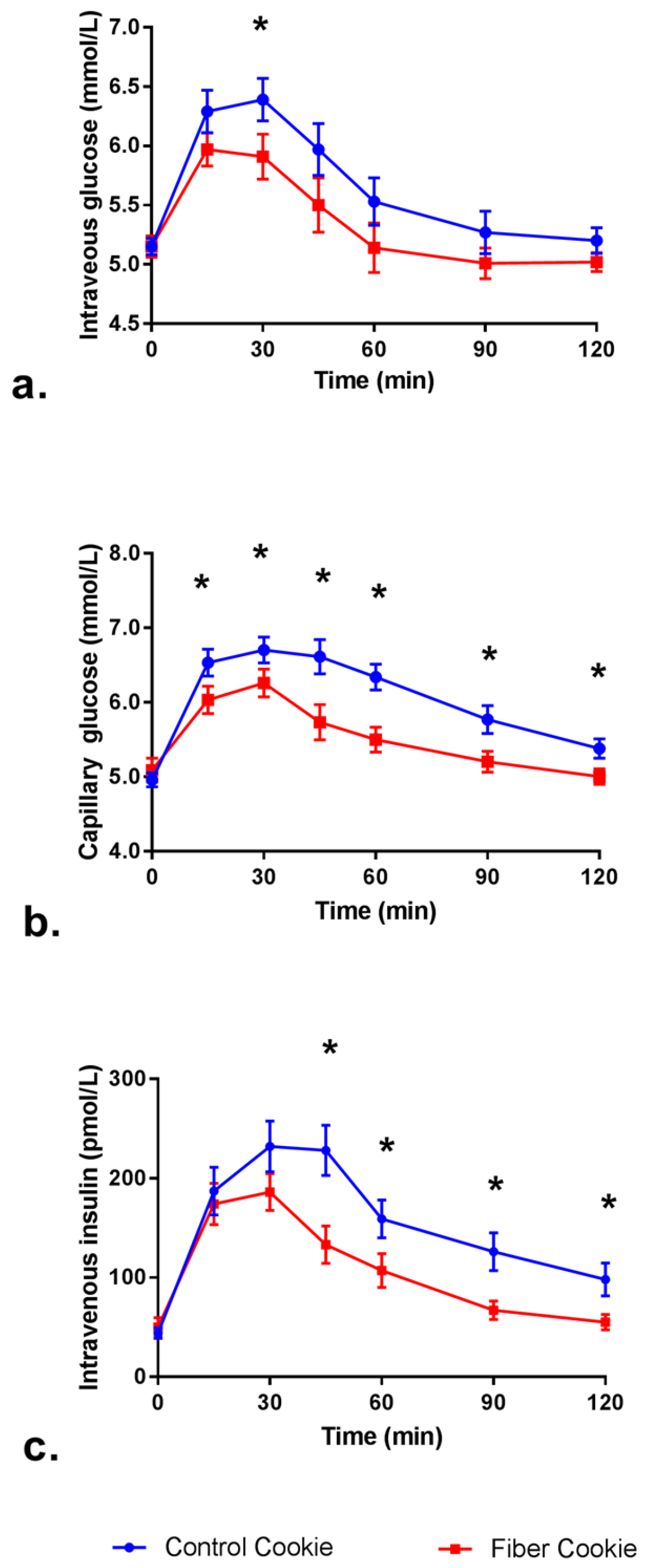
3.2. Post-Prandial Blood Glucose and Insulin Response
4. Discussion
Acknowledgments
Author Contributions
Conflicts of Interest
References
- Birt, D.F.; Boylston, T.; Hendrich, S.; Jane, J.L.; Hollis, J.; Li, L.; McClelland, J.; Moore, S.; Phillips, G.J.; Rowling, M.; et al. Resistant starch: Promise for improving human health. Adv. Nutr. 2013, 4, 587–601. [Google Scholar] [CrossRef] [PubMed]
- Maningat, C.C.; Seib, P.A. Rs4-Type Resistant Starch: Chemistry, Functionality and Health Benefits. In Resistant Starch: Sources, Applications and Health Benefits; Shi, Y.C., Maningat, C.C., Eds.; John Wiley & Sons: Hoboken, NJ, USA, 2013; pp. 43–77. [Google Scholar]
- Shen, D.; Bai, H.; Li, Z.; Yu, Y.; Zhang, H.; Chen, L. Positive effects of resistant starch supplementation on bowel function in healthy adults: A systematic review and meta-analysis of randomized controlled trials. Int. J. Food Sci. Nutr. 2017, 68, 149–157. [Google Scholar] [CrossRef] [PubMed]
- Bindels, L.B.; Walter, J.; Ramer-Tait, A.E. Resistant starches for the management of metabolic diseases. Curr. Opin. Clin. Nutr. Metab. Care 2015, 18, 559–565. [Google Scholar] [CrossRef] [PubMed]
- Heijnen, M.-L.A.; Beynen, A.C. Consumption of retrograded (rs3) but not uncooked (rs2) resistant starch shifts nitrogen excretion from urine to feces in cannulated piglets. J. Nutr. 1997, 127, 1828–1832. [Google Scholar] [PubMed]
- Martínez, I.; Kim, J.H.; Duffy, P.R.; Schlegel, V.L.; Walter, J. Resistant starches types 2 and 4 have differential effects on the composition of the fecal microbiota in human subjects. PLoS ONE 2010, 5, e15046. [Google Scholar] [CrossRef] [PubMed]
- IngredionIncorporated. Technical Specifications: Versafibe 1490 tm Resistant Starch. Available online: http://www.ingredion.us/content/dam/ingredion/technical-documents/na/VERSAFIBE%201490%20%20%2006400400%20%20%20Technical%20Specification.pdf (accessed on 15 December 2016).
- Woo, K.S.; Seib, P.A. Cross-linked resistant starch: Preparation and properties. Cereal Chem. 2002, 79, 819–825. [Google Scholar] [CrossRef]
- Sang, Y.J.; Seib, P.A.; Herrera, A.I.; Prakash, O.; Shi, Y.-C. Effects of alkaline treatment on the structure of phosphorylated wheat starch and its digestibility. Food Chem. 2010, 118, 323–327. [Google Scholar] [CrossRef]
- Al-Tamimi, E.K.; Seib, P.A.; Snyder, B.S.; Haub, M.D. Consumption of cross-linked resistant starch (rs4(xl)) on glucose and insulin responses in humans. J. Nutr. Metab. 2010. [Google Scholar] [CrossRef] [PubMed]
- Haub, M.D.; Hubach, K.L.; Al-Tamimi, E.K.; Ornelas, S.; Seib, P.A. Different types of resistant starch elicit different glucose reponses in humans. J. Nutr. Metab. 2010. [Google Scholar] [CrossRef] [PubMed]
- Nichenametla, S.N.; Weidauer, L.A.; Wey, H.E.; Beare, T.M.; Specker, B.L.; Dey, M. Resistant starch type 4-enriched diet lowered blood cholesterols and improved body composition in a double blind controlled cross-over intervention. Mol. Nutr. Food Res. 2014, 58, 1365–1369. [Google Scholar] [CrossRef] [PubMed]
- Upadhyaya, B.; McCormack, L.; Fardin-Kia, A.R.; Juenemann, R.; Nichenametla, S.; Clapper, J.; Specker, B.; Dey, M. Impact of dietary resistant starch type 4 on human gut microbiota and immunometabolic functions. Sci. Rep. 2016, 6, 28797. [Google Scholar] [CrossRef] [PubMed]
- Haub, M.D.; Louk, J.A.; Lopez, T.C. Novel resistant potato starches on glycemia and satiety in humans. J. Nutr. Metab. 2012, 2012, 478043. [Google Scholar] [CrossRef] [PubMed]
- Wolever, T.M.; Vorster, H.H.; Bjorck, I.; Brand-Miller, J.; Brighenti, F.; Mann, J.I.; Ramdath, D.D.; Granfeldt, Y.; Holt, S.; Perry, T.L.; et al. Determination of the glycaemic index of foods: Interlaboratory study. Eur. J. Clin. Nutr. 2003, 57, 475–482. [Google Scholar] [CrossRef] [PubMed]
- Wolever, T.M. Effect of blood sampling schedule and method of calculating the area under the curve on validity and precision of glycaemic index values. Br. J. Nutr. 2004, 91, 295–301. [Google Scholar] [CrossRef] [PubMed]
- Cnaan, A.; Laird, N.M.; Slasor, P. Using the general linear mixed model to analyse unbalanced repeated measures and longitudinal data. Stat. Med. 1997, 16, 2349–2380. [Google Scholar] [CrossRef]
- Pinheiro, J.; Bates, D.; DebRoy, S.; Sarkar, D.; R Core Team. Nlme: Linear and Nonlinear Mixed Effects Models; R Foundation: Vienna, Austria, 2015. [Google Scholar]
- Medicine, I.O. Dietary, Functional, and Total Fiber. In Dietary Reference Intakes for Energy, Carbohydrate, Fiber, Fat, Fatty Acids, Cholesterol, Protein, and Amino Acids; National Academies Press: Washington, DC, USA, 2005; pp. 339–421. [Google Scholar]
- Janzen, J.G. Digestibility of starch and phosphate starches by pancreatin. Starke 1969, 21, 231–235. [Google Scholar] [CrossRef]
| Per Serving, As-Eaten | Control Cookie | Fiber Cookie |
|---|---|---|
| Weight (g) | 47.02 | 48.00 |
| Calories (kcal) | 214.7 | 129.7 |
| Fat (g) | 3.99 | 3.92 |
| Saturated fat (g) | 0.56 | 0.54 |
| Protein (g) | 5.36 | 4.92 |
| Total Carbohydrates (g) | 36.84 | 36.84 |
| Available Carbohydrates (g) | 36.28 | 12.71 |
| Dietary Fiber (g) * | 0.55 | 24.13 |
| Sugars (g) | 11.51 | 11.72 |
| Mean ± SD | All Participants (n = 28) |
|---|---|
| Age (y) | 42.8 ± 18.5 |
| Sex (male/female) | 14/14 |
| Race (white/nonwhite) | 23/5 |
| Weight (kg) | 71.3 ± 12.0 |
| Body Mass Index (kg/m2) | 24.7 ± 3.3 |
| Fasting blood glucose (mmol/L) | 5.03 ± 0.34 |
| Mean ± SD | Control Cookie | Fiber Cookie | p-Value § |
|---|---|---|---|
| Intravenous blood glucose * | |||
| iAUC0-120min (mmol/L *·h) | 1.31 ± 0.75 | 0.73 ± 0.90 | 0.004 |
| Cmax0-120min (mmol/L *·h) | 6.83 ± 0.90 | 6.29 ± 0.82 | 0.001 |
| Capillary blood glucose † | |||
| iAUC0-120min (mmol/L *·h) | 2.35 ± 0.94 | 1.22 ± 1.18 | <0.001 |
| Cmax0-120min (mmol/L *·h) | 7.22 ± 1.00 | 6.60 ± 1.00 | 0.005 |
| Intravenous serum insulin ‡ | |||
| iAUC0-120min (pmol/L *·h) | 229 ± 124 | 124 ± 94 | <0.001 |
| Cmax0-120min (pmol/L *·h) | 280 ± 129 | 215 ± 94 | 0.007 |
| Question | Fiber Cookie | Control Cookie | Between Group p Value § |
|---|---|---|---|
| Mean ± SD (n) | Mean ± SD (n) | ||
| Rate the appearance of the cookie | 5.69 ± 2.02 (26) | 5.61 ± 1.89 (28) | 0.811 |
| Rate the texture of the cookie | 6.23 ± 2.07 (26) | 5.93 ± 2.07 (28) | 0.525 |
| Rate the flavor of the cookie | 6.46 ± 2.14 (26) | 6.79 ± 1.62 (28) | 0.355 |
| What is your overall acceptance of the cookie? | 6.54 ± 2.21 (26) | 6.50 ± 1.58 (28) | 0.970 |
© 2017 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license ( http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Stewart, M.L.; Zimmer, J.P. A High Fiber Cookie Made with Resistant Starch Type 4 Reduces Post-Prandial Glucose and Insulin Responses in Healthy Adults. Nutrients 2017, 9, 237. https://doi.org/10.3390/nu9030237
Stewart ML, Zimmer JP. A High Fiber Cookie Made with Resistant Starch Type 4 Reduces Post-Prandial Glucose and Insulin Responses in Healthy Adults. Nutrients. 2017; 9(3):237. https://doi.org/10.3390/nu9030237
Chicago/Turabian StyleStewart, Maria L., and J. Paul Zimmer. 2017. "A High Fiber Cookie Made with Resistant Starch Type 4 Reduces Post-Prandial Glucose and Insulin Responses in Healthy Adults" Nutrients 9, no. 3: 237. https://doi.org/10.3390/nu9030237
APA StyleStewart, M. L., & Zimmer, J. P. (2017). A High Fiber Cookie Made with Resistant Starch Type 4 Reduces Post-Prandial Glucose and Insulin Responses in Healthy Adults. Nutrients, 9(3), 237. https://doi.org/10.3390/nu9030237




