Consuming Two Eggs per Day, as Compared to an Oatmeal Breakfast, Decreases Plasma Ghrelin while Maintaining the LDL/HDL Ratio
Abstract
:1. Introduction
2. Materials and Methods
2.1. Experimental Design
2.2. Dietary Intervention
2.3. Blood Collection and Processing
2.4. Anthropometrics, Blood Pressure, Waist Circumference, and Dietary Intake
2.5. Plasma Lipids, Glucose, and Liver Enzymes
2.6. Measures of Satiety
2.7. Statistical Analysis
3. Results
3.1. Study Flow Chart
3.2. Baseline Characteristics
3.3. Dietary Intake
3.4. Anthropometrics, Blood Pressure, Plasma Lipids, Glucose, and Liver Enzymes
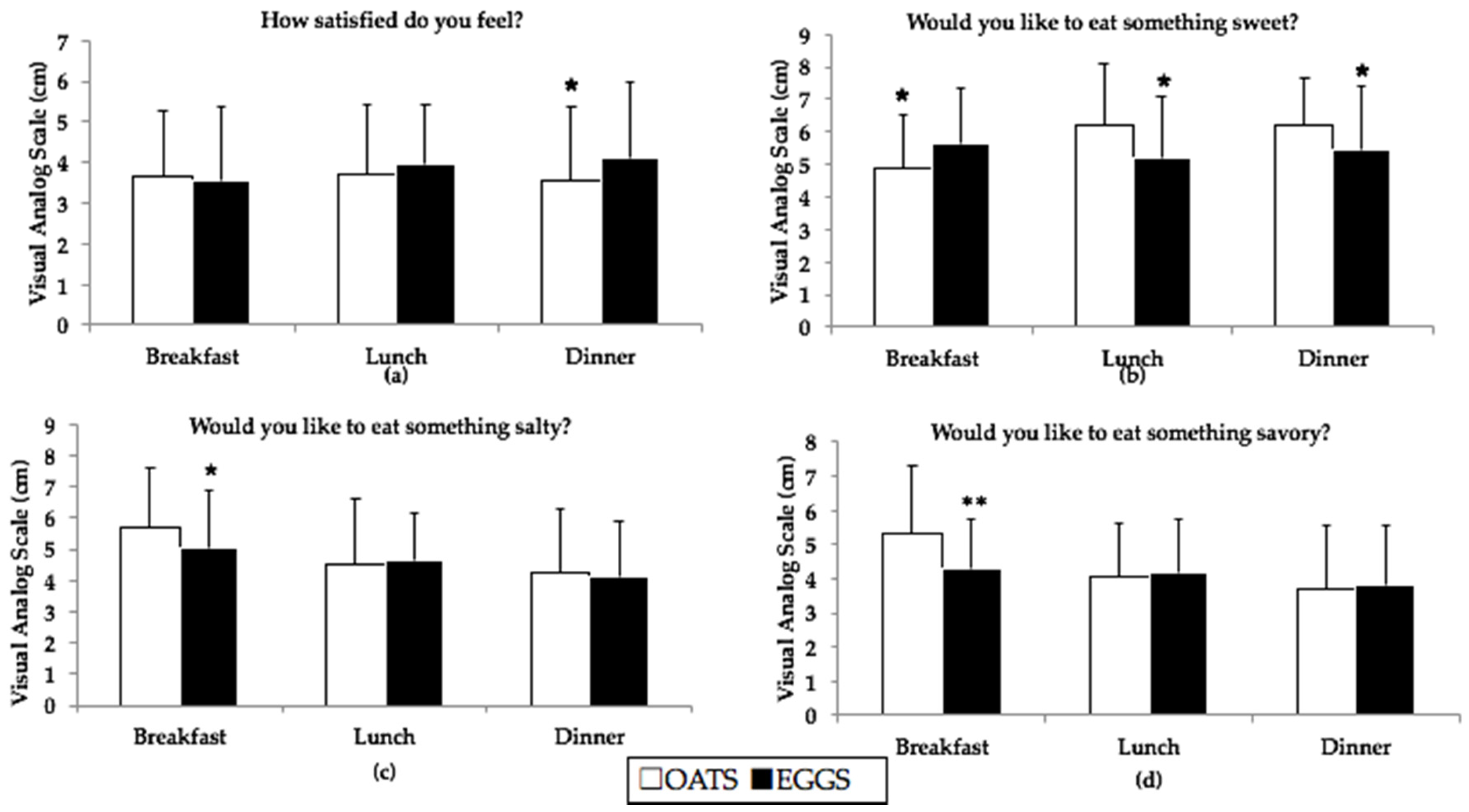
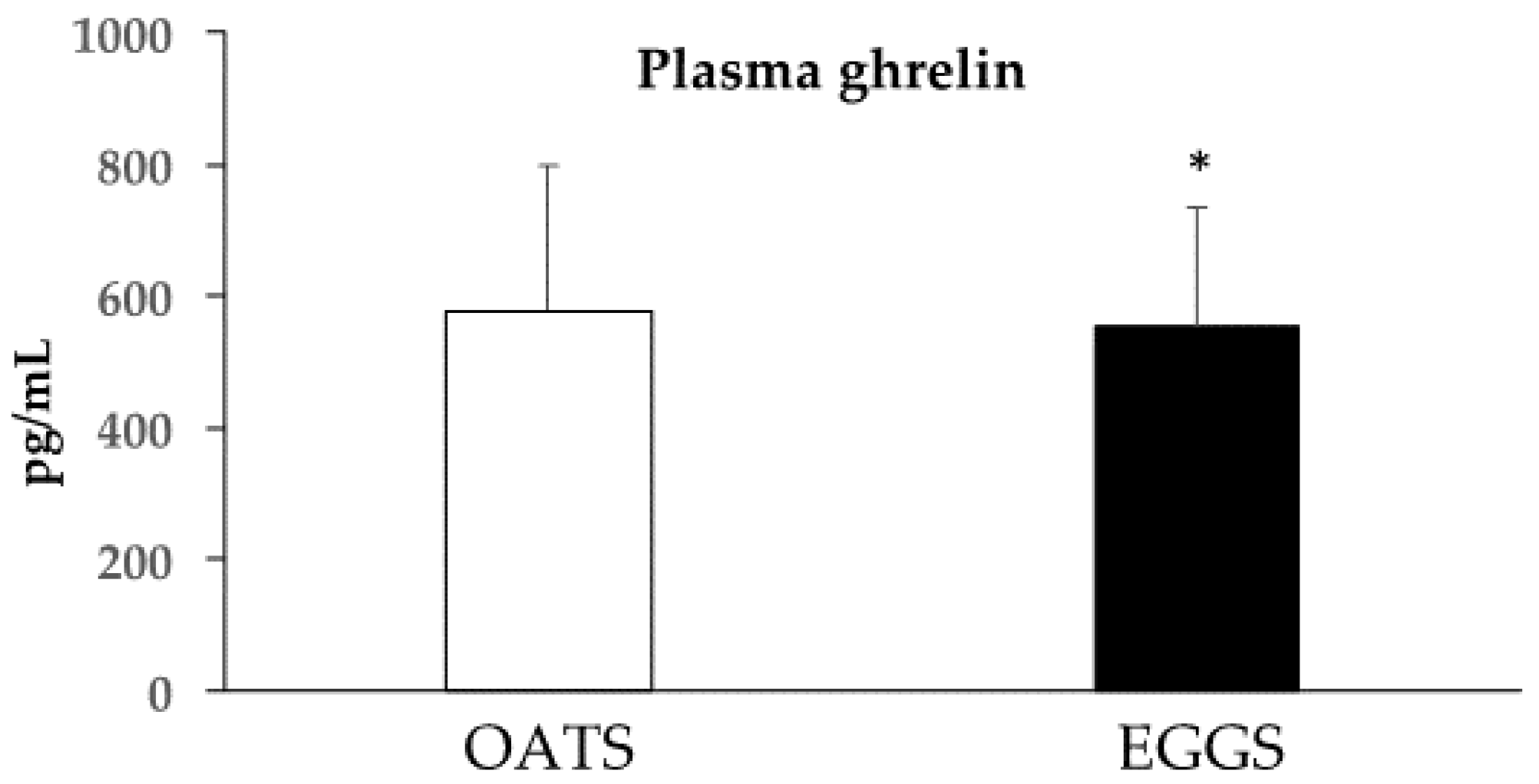
3.5. Measurements of Satiety: VAS and Plasma Ghrelin
4. Discussion
Acknowledgments
Author Contributions
Conflicts of Interest
References
- Kupper, W.; Hamm, C.W.; Bleifeld, W. Distribution of ApoA-I-Containing HDL Subpopulations in Patients With Coronary Heart Disease. Arterioscler. Thromb. Vasc. Biol. 2000, 20, 2670–2676. [Google Scholar]
- Tolfrey, K.; Zakrzewski, J.K. Breakfast, glycaemic index and health in young people. J. Sport Heal. Sci. 2012, 1, 149–159. [Google Scholar] [CrossRef]
- Nicklas, T.A.; Reger, C.; Myers, L.; O’Neil, C. Breakfast consumption with and without vitamin-mineral supplement use favorably impacts daily nutrient intake of ninth-grade students. J. Adolesc. Health 2000, 27, 314–321. [Google Scholar] [CrossRef]
- Kovacs-Nolan, J.; Phillips, M.; Mine, Y. Advances in the value of eggs and egg components for human health. J. Agric. Food Chem. 2005, 53, 8421–8431. [Google Scholar] [CrossRef] [PubMed]
- McNamara, D.J. The fifty year rehabilitation of the egg. Nutrients 2015, 7, 8716–8722. [Google Scholar] [CrossRef] [PubMed]
- American Heart Association. Heart and Stroke Encyclopedia: Eggs. Available online: http://www.heart.org/HEARTORG/ (accessed on 11 January 2016).
- U.S. Department of Health and Human Services; U.S. Department of Agriculture. Available online: http://health.gov/dietaryguidelines/2015/ (accessed on 15 January 2016).
- Mutungi, G.; Waters, D.; Ratliff, J.; Puglisi, M.; Clark, R.M.; Volek, J.S.; Fernandez, M.L. Eggs distinctly modulate plasma carotenoid and lipoprotein subclasses in adult men following a carbohydrate-restricted diet. J. Nutr. Biochem. 2010, 21, 261–267. [Google Scholar] [CrossRef] [PubMed]
- Herron, K.L.; Vega-Lopez, S.; Conde, K.; Ramjiganesh, T.; Shachter, N.S.; Fernandez, M.L. Men classified as hypo- or hyperresponders to dietary cholesterol feeding exhibit differences in lipoprotein metabolism. J. Nutr. 2003, 133, 1036–1042. [Google Scholar] [PubMed]
- Barona, J.; Fernandez, M.L. Dietary cholesterol affects plasma lipid levels, the intravascular processing of lipoproteins and reverse cholesterol transport without increasing the risk for heart disease. Nutrients 2012, 4, 1015–1025. [Google Scholar] [CrossRef] [PubMed]
- Blesso, C.N.; Andersen, C.J.; Barona, J.; Volek, J.S.; Fernandez, M.L. Whole egg consumption improves lipoprotein profiles and insulin sensitivity to a greater extent than yolk-free egg substitute in individuals with metabolic syndrome. Metabolism 2013, 62, 400–410. [Google Scholar] [CrossRef] [PubMed]
- Ballesteros, M.N.; Valenzuela, F.; Robles, A.E.; Artalejo, E.; Aguilar, D.; Andersen, C.J.; Valdez, H.; Fernandez, M.L. One egg per day improves inflammation when compared to an oatmeal-based breakfast without increasing other cardiometabolic risk factors in diabetic patients. Nutrients 2015, 7, 3449–3463. [Google Scholar] [CrossRef] [PubMed]
- Vander Wal, J.S.; Marth, J.M.; Khosla, P.; Jen, K.-L.C.; Dhurandhar, N.V. Short-term effect of eggs on satiety in overweight and obese subjects. J. Am. Coll. Nutr. 2005, 24, 510–515. [Google Scholar] [CrossRef] [PubMed]
- Iannotti, L.L.; Lutter, C.K.; Bunn, D.A.; Stewart, C.P. Eggs: The uncracked potential for improving maternal and young child nutrition among the world’s poor. Nutr. Rev. 2014, 72, 355–368. [Google Scholar] [CrossRef] [PubMed]
- Ratliff, J.; Leite, J.O.; de Ogburn, R.; Puglisi, M.J.; van Heest, J.; Fernandez, M.L. Consuming eggs for breakfast influences plasma glucose and ghrelin, while reducing energy intake during the next 24 h in adult men. Nutr. Res. 2010, 30, 96–103. [Google Scholar] [CrossRef] [PubMed]
- Rueda, J.M.; Khosla, P. Impact of breakfasts (with or without eggs) on body weight regulation and blood lipids in university students over a 14-week semester. Nutrients 2013, 5, 5097–5113. [Google Scholar] [CrossRef] [PubMed]
- Kral, T.V.E.; Bannon, A.L.; Chittams, J.; Moore, R.H. Comparison of the satiating properties of egg- versus cereal grain-based breakfasts for appetite and energy intake control in children. Eat. Behav. 2016, 20, 14–20. [Google Scholar] [CrossRef] [PubMed]
- Weigle, D.S.; Breen, P.A.; Matthys, C.C.; Callahan, H.S.; Meeuws, K.E.; Burden, V.R.; Purnell, J.Q. A high-protein diet induces sustained reductions in appetite, ad libitum caloric intake, and body weight despite compensatory changes in diurnal plasma leptin and ghrelin concentrations. Am. J. Clin. Nutr. 2005, 82, 41–48. [Google Scholar] [PubMed]
- Laurila, M.; Santaniemi, M.; Kesäniemi, Y.A.; Ukkola, O. Peptides High plasma ghrelin protects from coronary heart disease and Leu72Leu polymorphism of ghrelin gene from cancer in healthy adults during the 19 years follow-up study. Peptides 2014, 61, 122–129. [Google Scholar] [CrossRef] [PubMed]
- Chou, C.-C.; Bai, C.-H.; Tsai, S.-C.; Wu, M.-S. Low serum acylated ghrelin levels are associated with the development of cardiovascular disease in hemodialysis patients. Intern. Med. 2010, 49, 2057–2064. [Google Scholar] [CrossRef] [PubMed]
- Mao, Y.; Tokudome, T.; Kishimoto, I. Ghrelin as a treatment for cardiovascular diseases. Hypertension 2014, 64, 450–454. [Google Scholar] [CrossRef] [PubMed]
- Greenberg, A.S.; Obin, M.S. Obesity and the role of adipose tissue in inflammation and metabolism. Am. J. Clin. Nutr. 2006, 83, 461–465. [Google Scholar]
- Moran, L.J.; Noakes, M.; Clifton, P.M.; Wittert, G.A.; Tomlinson, L.; Galletly, C.; Luscombe, N.D.; Norman, R.J. Ghrelin and measures of satiety are altered in polycystic ovary syndrome but not differentially affected by diet composition. J. Clin. Endocrinol. Metab. 2004, 89, 3337–3344. [Google Scholar] [CrossRef] [PubMed]
- Otto, B.; Heldwein, W.; Otto, C.; Huptas, S.; Parhofer, K.G. Effect of a high-fat meal on the postprandial ghrelin response. Am. J. Clin. Nutr. 2006, 84, 664–665. [Google Scholar] [PubMed]
- Zakhari, J.S.; Zorrilla, E.P.; Zhou, B.; Mayorov, A.V.; Janda, K.D. Oligoclonal antibody targeting ghrelin increases energy expenditure and reduces food intake in fasted mice. Mol. Pharm. 2013, 9, 281–289. [Google Scholar] [CrossRef] [PubMed]
- American Heart Association. Whole Grains. Available online: http://www.heart.org/HEARTORG/Encyclopedia/Heart-Encyclopedia_UCM_445084_Encyclopedia.jsp?levelSelected=17&title=whole grains (accessed on 11 January 2016).
- Davy, B.M.; Davy, K.P.; Ho, R.C.; Beske, S.D.; Davrath, L.R.; Melby, C.L. High-fiber oat cereal compared with wheat cereal consumption favorably alters LDL-cholesterol subclass and particle numbers in middle-aged and older men. Am. J. Clin. Nutr. 2002, 76, 351–358. [Google Scholar] [PubMed]
- Fukuyama, N.; Homma, K.; Wakana, N.; Kudo, K.; Suyama, A.; Ohazama, H.; Tsuji, C.; Ishiwata, K.; Eguchi, Y.; Nakazawa, H.; et al. Validation of the Friedewald Equation for Evaluation of Plasma LDL-Cholesterol. J. Clin. Biochem. Nutr. 2008, 43, 1–5. [Google Scholar] [CrossRef] [PubMed]
- Chung, H.-Y.; Rasmussen, H.M.; Johnson, E.J. Lutein bioavailability is higher from lutein-enriched eggs than from supplements and spinach in men. J. Nutr. 2004, 134, 1887–1893. [Google Scholar] [PubMed]
- USDA Dietary Guidelines for Americans 2015–2020. 2015. Available online: https://health.gov/dietaryguidelines/ (accessed on 15 November 2016).
- Van Der Wulp, M.Y.M.; Verkade, H.J.; Groen, A.K. Regulation of cholesterol homeostasis. Mol. Cell. Endocrinol. 2013, 368, 1–16. [Google Scholar] [CrossRef] [PubMed]
- Fernandez, M.L. Effects of eggs on plasma lipoproteins in healthy populations. Food Funct. 2010, 1, 156–160. [Google Scholar] [CrossRef] [PubMed]
- Ratliff, J.; Mutungi, G.; Puglisi, M.J.; Volek, J.S.; Fernandez, M.L. Carbohydrate restriction (with or without additional dietary cholesterol provided by eggs) reduces insulin resistance and plasma leptin without modifying appetite hormones in adult men. Nutr. Res. 2009, 29, 262–268. [Google Scholar] [CrossRef] [PubMed]
- Spence, J.D.; Jenkins, D.J.A.; Davignon, J. Dietary cholesterol and egg yolks: Not for patients at risk of vascular disease. Can. J. Cardiol. 2010, 26, e336–e339. [Google Scholar] [CrossRef]
- Lewis, G.F.; Rader, D.J. New insights into the regulation of HDL metabolism and reverse cholesterol transport. Circ. Res. 2005, 96, 1221–1232. [Google Scholar] [CrossRef] [PubMed]
- Yancey, P.G.; de La Llera-Moya, M.; Swarnakar, S.; Monzo, P.; Klein, S.M.; Connelly, M.A.; Johnson, W.J.; Williams, D.L.; Rothblat, G.H. High density lipoprotein phospholipid composition is a major determinant of the bi-directional flux and net movement of cellular free cholesterol mediated by scavenger receptor BI. J. Biol. Chem. 2000, 275, 36596–36604. [Google Scholar] [CrossRef] [PubMed]
- Andersen, C.J.; Blesso, C.N.; Lee, J.; Barona, J.; Shah, D.; Thomas, M.J.; Fernandez, M.L. Egg consumption modulates HDL lipid composition and increases the cholesterol-accepting capacity of serum in metabolic syndrome. Lipids 2013, 48, 557–567. [Google Scholar] [CrossRef] [PubMed]
- Shin, J.; Xun, P.; Nakamura, Y.; He, K. Egg consumption in relation to risk of cardiovascular disease and diabetes: A systematic review and meta-analysis. Am. J. Clin. Nutr. 2013, 98, 146–159. [Google Scholar] [CrossRef] [PubMed]
- Rong, Y.; Chen, L.; Zhu, T.; Song, Y.; Yu, M.; Shan, Z.; Sands, A.; Hu, F.B.; Liu, L. Egg consumption and risk of coronary heart disease and stroke: Dose-response meta-analysis of prospective cohort studies. BMJ 2013, 346, e8539. [Google Scholar] [CrossRef] [PubMed]
- Nutrition Data Glycemic Index, Glycemic Load. Available online: http://nutritiondata.self.com/topics/glycemic-index (accessed on 25 October 2016).
- Blesso, C.N.; Andersen, C.J.; Barona, J.; Volk, B.; Volek, J.S.; Fernandez, M.L. Effects of carbohydrate restriction and dietary cholesterol provided by eggs on clinical risk factors in metabolic syndrome. J. Clin. Lipidol. 2013, 7, 463–471. [Google Scholar] [CrossRef] [PubMed]
- Venn, B.J.; Green, T.J. Glycemic index and glycemic load: Measurement issues and their effect on diet-disease relationships. Eur. J. Clin. Nutr. 2007, 61 (Suppl. 1), S122–S131. [Google Scholar] [CrossRef] [PubMed]
- Tschop, M.; Weyer, C.; Tataranni, P.A.; Devanarayan, V.; Ravussin, E.; Heiman, M.L. Circulating ghrelin levels are decreased in obesity. Diabetes 2001, 50, 707–709. [Google Scholar] [CrossRef] [PubMed]
- Liu, A.G.; Puyau, R.S.; Han, H.; Johnson, W.D.; Greenway, F.L.; Dhurandhar, N.V. The Effect of an Egg Breakfast on Satiety in Children and Adolescents: A Randomized Crossover Trial. J. Am. Coll. Nutr. 2015, 34, 37–54. [Google Scholar] [CrossRef] [PubMed]
- Martens, M.J.I.; Rutters, F.; Lemmens, S.G.T.; Born, J.M.; Westerterp-Plantenga, M.S. Effects of single macronutrients on serum cortisol concentrations in normal weight men. Physiol. Behav. 2010, 101, 563–567. [Google Scholar] [CrossRef] [PubMed]
- Rodríguez, A. Novel molecular aspects of ghrelin and leptin in the control of adipobiology and the cardiovascular system. Obes. Facts 2014, 7, 82–95. [Google Scholar] [CrossRef] [PubMed]
- Shiiya, T.; Nakazato, M.; Mizuta, M.; Date, Y.; Mondal, M.S.; Tanaka, M.; Nozoe, S.-I.; Hosoda, H.; Kangawa, K.; Matsukura, S. Plasma Ghrelin Levels in Lean and Obese Humans and the Effect of Glucose on Ghrelin Secretion. J. Clin. Endocrinol. Metab. 2009, 87, 240–244. [Google Scholar] [CrossRef] [PubMed]
- Nakazato, M.; Murakami, N.; Date, Y.; Kojima, M.; Matsuo, H.; Kangawa, K.; Matsukura, S. A role for ghrelin in the central regulation of feeding. Nature 2001, 409, 194–198. [Google Scholar] [CrossRef] [PubMed]
- Gerstein, D.E.; Woodward-Lopez, G.; Evans, A.E.; Kelsey, K.; Drewnowski, A. Clarifying concepts about macronutrients’ effects on satiation and satiety. J. Am. Diet. Assoc. 2004, 104, 1151–1153. [Google Scholar] [CrossRef] [PubMed]
- Clark, L.C.; Byer, H.; Murlin, J.R. Relative to egg biological values and replacement values of some cereal proteins in human subjects. J. Nutr. 1949, 38, 405–420. [Google Scholar] [PubMed]


| Parameter | Values |
|---|---|
| Age (years) | 23.3 ± 3.1 |
| Gender (n = F/M) | 26/24 |
| BMI (kg/m2) | 23.2 ± 2.1 |
| WC (cm) | 81.3 ± 6.5 |
| Systolic BP (mmHg) | 112.1 ± 12.4 |
| Diastolic BP (mmHg) | 72.7 ± 7.0 |
| Total Cholesterol (mmol/L) | 3.9 ± 0.7 |
| LDL-C (mmol/L) | 1.9 ± 0.6 |
| HDL-C (mmol/L) | 1.7 ± 0.5 |
| LDL-C/HDL-C | 1.2 ± 0.07 |
| Triglycerides (mmol/L) | 0.9 ± 0.04 |
| Glucose (mmol/L) | 5.1 ± 0.3 |
| CRP (mg/dL) | 0.2 ± 0.8 |
| Parameter | Eggs | Oatmeal |
|---|---|---|
| Weight (kg) | 68.2 ± 11.2 | 68.2 ± 11.1 |
| Energy (kcal) | 1937 ± 630 | 2016 ± 1461 |
| Protein (%) | 19.2 ± 4.4 | 17.6 ± 4.1 |
| Carbohydrate (%) | 41.4 ± 6.2 ** | 48.9 ± 8.2 |
| Total Fat (%) | 37.2 ± 5.1 ** | 32.2 ± 6.7 |
| SFA (g/day) | 27.3 ± 11.9 ** | 21.1 ± 8.1 |
| MUFA (g/day) | 30.4 ± 11.6 ** | 23.2 ± 9.6 |
| PUFA (g/day) | 16.6 ± 7.4 | 15.7 ± 11.5 |
| Total Fiber (g/day) | 18.3 ± 7.0 | 20.9 ± 11.4 |
| Soluble Fiber (g/day) | 5.6 ± 2.6 * | 7.0 ± 4.0 |
| Insoluble Fiber (g/day) | 12.7 ± 7.4 | 13.9 ± 8.0 |
| Cholesterol (mg/day) | 546.1 ± 96.6 ** | 173.1 ± 90.6 |
| Lutein + Zeaxanthin (µg/day) | 2820 ± 3443 | 2327 ± 3997 |
| Glycemic Index | 59.0 ± 5.9 | 59.9 ± 6.0 |
| Glycemic Load | 109.9 ± 42.4 * | 122.6 ± 49.1 |
| Parameter | Eggs | Oatmeal |
|---|---|---|
| BMI (kg/m2) | 23.2 ± 2.2 | 22.7 ± 2.6 |
| WC (cm) | 81.9 ± 6.4 | 82.6 ± 6.6 |
| Systolic BP (mmHg) | 110.3 ± 10.1 | 111.2 ± 11.7 |
| Diastolic BP (mmHg) | 74.4 ± 6.4 | 73.4 ± 6.3 |
| Total cholesterol (mmol/L) | 4.2 ± 0.7 * | 4.0 ± 0.7 |
| LDL cholesterol (mmol/L) | 2.1 ± 0.7 * | 1.9 ± 0.6 |
| HDL cholesterol (mmol/L) | 1.71 ± 0.48 * | 1.62 ± 0.47 |
| LDL-C/HDL-C | 1.35 ± 0.62 | 1.30 ± 0.56 |
| Triglycerides (mmol/L) | 0.89 ± 0.37 | 0.91 ± 0.41 |
| Glucose (mmol/L) | 5.1 ± 0.4 | 5.0 ± 0.4 |
| ALT (U/L) | 18.2 ± 7.9 | 17.6 ± 6.0 |
| AST (U/L) | 24.5 ± 7.8 | 24.5 ± 8.8 |
© 2017 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license ( http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Missimer, A.; DiMarco, D.M.; Andersen, C.J.; Murillo, A.G.; Vergara-Jimenez, M.; Fernandez, M.L. Consuming Two Eggs per Day, as Compared to an Oatmeal Breakfast, Decreases Plasma Ghrelin while Maintaining the LDL/HDL Ratio. Nutrients 2017, 9, 89. https://doi.org/10.3390/nu9020089
Missimer A, DiMarco DM, Andersen CJ, Murillo AG, Vergara-Jimenez M, Fernandez ML. Consuming Two Eggs per Day, as Compared to an Oatmeal Breakfast, Decreases Plasma Ghrelin while Maintaining the LDL/HDL Ratio. Nutrients. 2017; 9(2):89. https://doi.org/10.3390/nu9020089
Chicago/Turabian StyleMissimer, Amanda, Diana M. DiMarco, Catherine J. Andersen, Ana Gabriela Murillo, Marcela Vergara-Jimenez, and Maria Luz Fernandez. 2017. "Consuming Two Eggs per Day, as Compared to an Oatmeal Breakfast, Decreases Plasma Ghrelin while Maintaining the LDL/HDL Ratio" Nutrients 9, no. 2: 89. https://doi.org/10.3390/nu9020089
APA StyleMissimer, A., DiMarco, D. M., Andersen, C. J., Murillo, A. G., Vergara-Jimenez, M., & Fernandez, M. L. (2017). Consuming Two Eggs per Day, as Compared to an Oatmeal Breakfast, Decreases Plasma Ghrelin while Maintaining the LDL/HDL Ratio. Nutrients, 9(2), 89. https://doi.org/10.3390/nu9020089






