Individual Diet Modeling Shows How to Balance the Diet of French Adults with or without Excessive Free Sugar Intakes
Abstract
:1. Introduction
2. Materials and Methods
2.1. Dietary Survey and Population Sample
2.2. Demographic, Socio-Economic, Behavioral and Anthropometric Variables
2.3. Dietary Assessment
2.4. Food Composition Database and Free Sugars
2.5. Diet Quality Indicators
2.6. Diet Modeling
2.7. Identification of the Most Binding Nutrients
2.8. Statistical Analyses
3. Results
3.1. Sample Characteristics
3.2. Observed Nutritional Intakes and Diet Quality Indicators
3.3. Food Amounts in Observed Diets
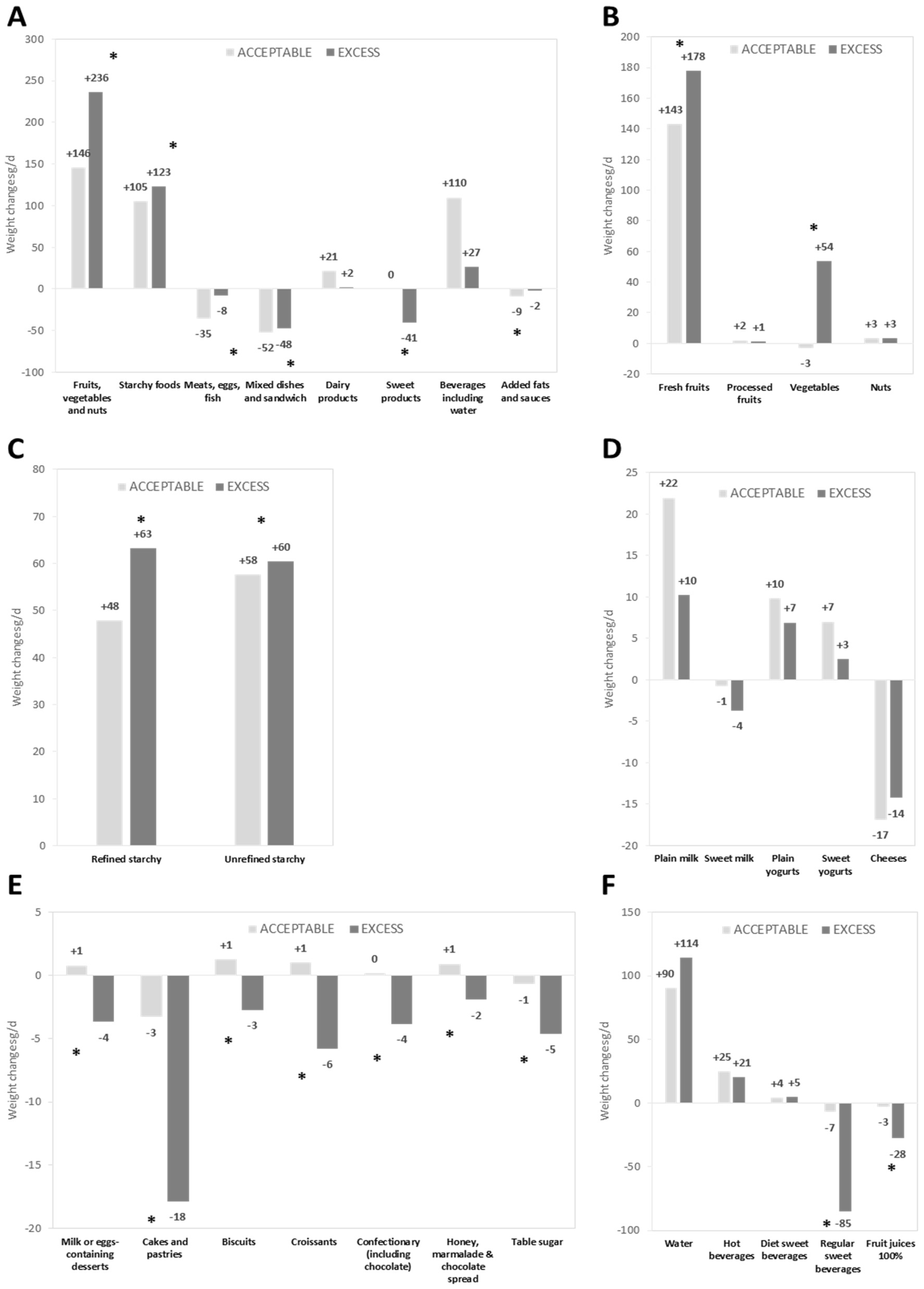
3.4. Food Amounts and Weight Variations after Optimization
3.5. Identification of the Most Binding Nutrients
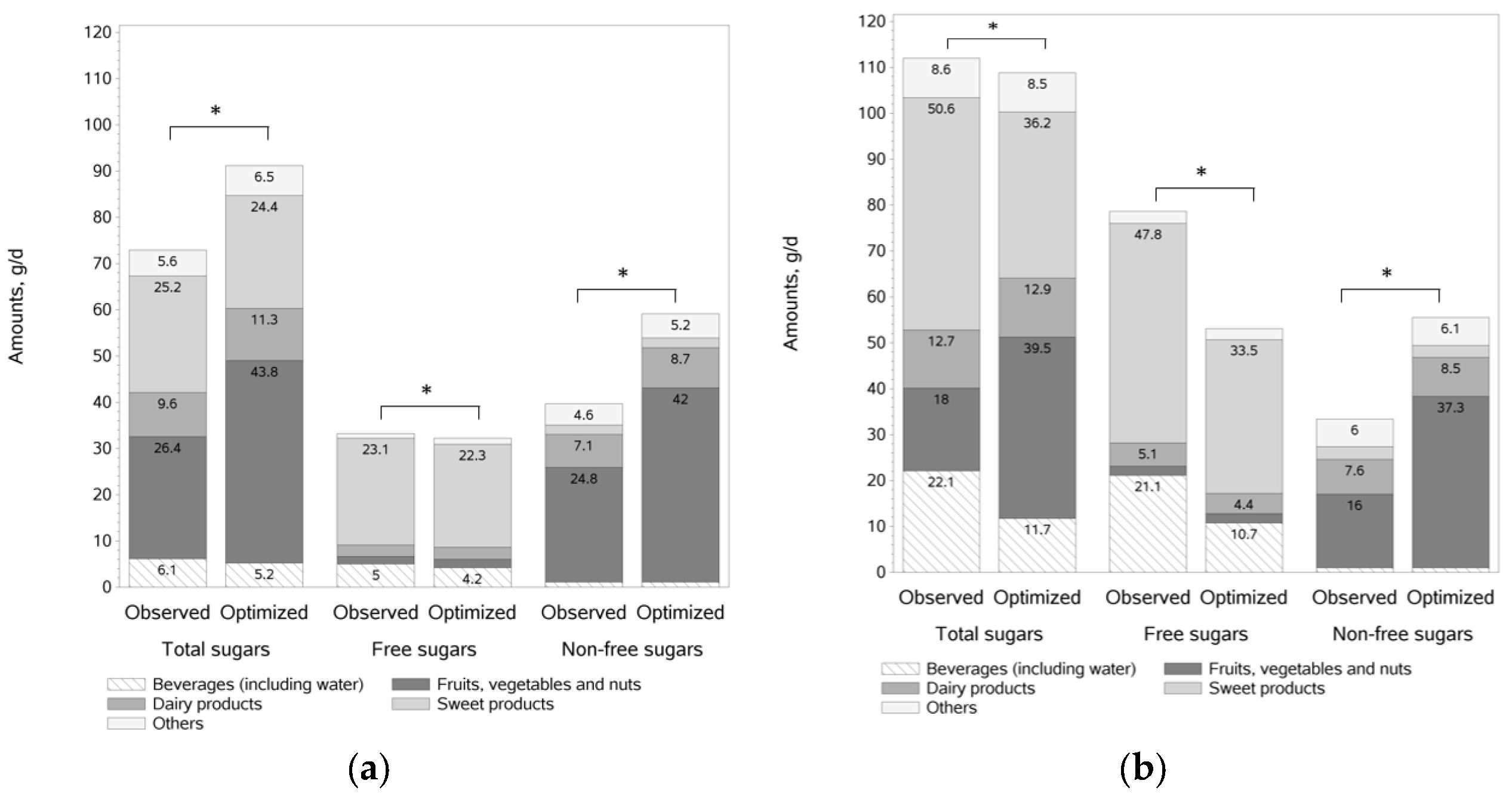
3.6. Changes in Sugar Balance after Optimization
4. Discussion
5. Conclusions
Supplementary Materials
Acknowledgments
Author Contributions
Conflicts of Interest
References
- Moynihan, P.J.; Kelly, S.A.M. Effect on caries of restricting sugars intake: Systematic review to inform WHO guidelines. J. Dent. Res. 2014, 93, 8–18. [Google Scholar] [CrossRef]
- Te Morenga, L.; Mallard, S.; Mann, J. Dietary sugars and body weight: Systematic review and meta-analyses of randomised controlled trials and cohort studies. BMJ 2013, 346, e7492. [Google Scholar] [CrossRef] [PubMed]
- Sonestedt, E.; Overby, N.C.; Laaksonen, D.E.; Birgisdottir, B.E. Does high sugar consumption exacerbate cardiometabolic risk factors and increase the risk of type 2 diabetes and cardiovascular disease? Food Nutr. Res. 2012, 56. [Google Scholar] [CrossRef] [PubMed]
- Greenwood, D.C.; Threapleton, D.E.; Evans, C.E.L.; Cleghorn, C.L.; Nykjaer, C.; Woodhead, C.; Burley, V.J. Association between sugar-sweetened and artificially sweetened soft drinks and type 2 diabetes: Systematic review and dose-response meta-analysis of prospective studies. Br. J. Nutr. 2014, 112, 725–734. [Google Scholar] [CrossRef] [PubMed]
- Johnson, R.K.; Appel, L.J.; Brands, M.; Howard, B.V.; Lefevre, M.; Lustig, R.H.; Sacks, F.; Steffen, L.M.; Wylie-Rosett, J. Dietary Sugars Intake and Cardiovascular Health. Circulation 2009, 120, 1011–1020. [Google Scholar] [CrossRef] [PubMed]
- Prasad, K.; Dhar, I. Oxidative stress as a mechanism of added sugar-induced cardiovascular disease. Int. J. Angiol. 2014, 23, 217–226. [Google Scholar] [PubMed]
- Te Morenga, L.A.; Howatson, A.J.; Jones, R.M.; Mann, J. Dietary sugars and cardiometabolic risk: Systematic review and meta-analyses of randomized controlled trials of the effects on blood pressure and lipids. Am. J. Clin. Nutr. 2014, 100, 65–79. [Google Scholar] [CrossRef] [PubMed]
- Louie, J.C.Y.; Tapsell, L.C. Association between intake of total vs added sugar on diet quality: A systematic review. Nutr. Rev. 2015, 73, 837–857. [Google Scholar] [CrossRef] [PubMed]
- World Health Organization. WHO Guideline: Sugars Intake for Adults and Children; World Health Organization: Geneva, Switzerland, 2015. [Google Scholar]
- World Health Organization. Diet, Nutrition and the Prevention of Chronic Diseases. Report of a Joint WHO/FAO Expert Consultation; World Health Organization: Geneva, Switzerland, 2003; Volume 916. [Google Scholar]
- Scientific Advisory Committee on Nutrition. Carbohydrates and Health; Scientific Advisory Committee on Nutrition: London, UK, 2015.
- U.S. Department of Agriculture; U.S. Department of Health and Human Services. Dietary Guidelines for Americans, 2015–2020, 8th ed.U.S. Government Printing Office: Washington, DC, USA, 2015.
- EFSA Panel on Dietetic Products Nutrition and Allergies (NDA). Scientific Opinion on Dietary Reference Values for carbohydrates and dietary fibre. EFSA J. 2010, 8, 1462. [Google Scholar]
- World Health Organization. WHO Calls on Countries to Reduce Sugars Intake among Adults and Children; World Health Organization: Geneva, Switzerland, 2015. [Google Scholar]
- Newens, K.J.; Walton, J. A review of sugar consumption from nationally representative dietary surveys across the world. J. Hum. Nutr. Diet. 2016, 29, 225–240. [Google Scholar] [CrossRef] [PubMed]
- Powell, E.S.; Smith-Taillie, L.P.; Popkin, B.M. Added Sugars Intake Across the Distribution of US Children and Adult Consumers: 1977–2012. J. Acad. Nutr. Diet. 2016, 116, 1543–1550. [Google Scholar] [CrossRef] [PubMed]
- Ervin, R.B.; Ogden, L.C. Consumption of Added Sugars Among U.S. Adults, 2005–2010. Natl. Cent. Heal. Stat. Data Brief 2013, 122, 1–8. [Google Scholar]
- Myhre, J.B.; Løken, E.B.; Wandel, M.; Andersen, L.F. The contribution of snacks to dietary intake and their association with eating location among Norwegian adults—Results from a cross-sectional dietary survey. BMC Public Health 2015, 15, 369. [Google Scholar] [CrossRef] [PubMed]
- Dubuisson, C.; Lioret, S.; Touvier, M.; Dufour, A.; Calamassi-Tran, G.; Volatier, J.-L.L.; Lafay, L. Trends in food and nutritional intakes of French adults from 1999 to 2007: Results from the INCA surveys. Br. J. Nutr. 2010, 103, 1035–1048. [Google Scholar] [CrossRef] [PubMed]
- Bertin, M.; Touvier, M.; Dubuisson, C.; Dufour, A.; Havard, S.; Lafay, L.; Volatier, J.-L.; Lioret, S. Dietary patterns of French adults: Associations with demographic, socio-economic and behavioural factors. J. Hum. Nutr. Diet. 2016, 29, 241–254. [Google Scholar] [CrossRef] [PubMed]
- Goldberg, G.R.; Black, A.E.; Jebb, S.A.; Cole, T.J.; Murgatroyd, P.R.; Coward, W.A.; Prentice, A.M. Critical evaluation of energy intake data using fundamental principles of energy physiology: 1. Derivation of cut-off limits to identify under-recording. Eur. J. Clin. Nutr. 1991, 45, 569–581. [Google Scholar] [PubMed]
- INSEE-Definitions and Methods—Consumption Unit. Available online: http://www.insee.fr/en/metadonnees/definition/c1802 (accessed on 16 February 2017).
- Craig, C.L.; Marshall, A.L.; Sjöström, M.; Bauman, A.E.; Booth, M.L.; Ainsworth, B.E.; Pratt, M.; Ekelund, U.; Yngve, A.; Sallis, J.F.; et al. International physical activity questionnaire: 12-country reliability and validity. Med. Sci. Sports Exerc. 2003, 35, 1381–1395. [Google Scholar] [CrossRef] [PubMed]
- World Health Organization Regional Office for Europe. The Challenges of Obesity in the WHO European Region and the Strategies for Response; WHO Regional Office for Europe: Copenhagen, Denmark, 2007. [Google Scholar]
- Hercberg, S.; Deheeger, M.; Preziosi, P. Portions Alimentaires Manuel Photos Pour l’estimation des Quantités—(Portion Sizes: Picture Booklet for the Estimation of Quantities); SU-VI-MAX; Polytechnica: Paris, France, 1994. [Google Scholar]
- Agence Nationale de SEcurité Sanitaire de L’alimentation, de L’environnement et du Travail (ANSES). French Food Composition Table Ciqual 2013. Available online: https://pro.anses.fr/TableCIQUAL/index.htm (accessed on 16 February 2017).
- Louie, J.C.Y.; Moshtaghian, H.; Boylan, S.; Flood, V.M.; Rangan, A.M.; Barclay, A.W.; Brand-Miller, J.C.; Gill, T.P. A systematic methodology to estimate added sugar content of foods. Eur. J. Clin. Nutr. 2015, 69, 154–161. [Google Scholar] [CrossRef] [PubMed]
- Ledikwe, J.H.; Blanck, H.M.; Khan, L.K.; Serdula, M.K.; Seymour, J.D.; Tohill, B.C.; Rolls, B.J. Dietary energy density determined by eight calculation methods in a nationally representative United States population. J. Nutr. 2005, 135, 273–278. [Google Scholar] [PubMed]
- Ledikwe, J.H.; Blanck, H.M.; Khan, L.K.; Serdula, M.K.; Seymour, J.D.; Tohill, B.C.; Rolls, B.J. Low-energy-density diets are associated with high diet quality in adults in the United States. J. Am. Diet. Assoc. 2006, 106, 1172–1180. [Google Scholar] [CrossRef] [PubMed]
- Krebs-Smith, S.M.; Smiciklas-Wright, H.; Guthrie, H.A.; Krebs-Smith, J. The effects of variety in food choices on dietary quality. J. Am. Diet. Assoc. 1987, 87, 897–903. [Google Scholar] [PubMed]
- Kant, A.K. Indexes of overall diet quality: A review. J. Am. Diet. Assoc. 1996, 96, 785–791. [Google Scholar] [CrossRef]
- Guthrie, H.A.; Scheer, J.C. Validity of a dietary score for assessing nutrient adequacy. J. Am. Diet. Assoc. 1981, 78, 240–245. [Google Scholar] [PubMed]
- Bocquier, A.; Vieux, F.; Lioret, S.; Dubuisson, C.; Caillavet, F.; Darmon, N. Socio-economic characteristics, living conditions and diet quality are associated with food insecurity in France. Public Health Nutr. 2015, 18, 1–10. [Google Scholar] [CrossRef] [PubMed]
- Vieux, F.; Soler, L.-G.; Touazi, D.; Darmon, N. High nutritional quality is not associated with low greenhouse gas emissions in self-selected diets of French adults. Am. J. Clin. Nutr. 2013, 97, 569–583. [Google Scholar] [CrossRef]
- Verger, E.O.; Holmes, B.A.; Huneau, J.F.; Mariotti, F. Simple changes within dietary subgroups can rapidly improve the nutrient adequacy of the diet of French adults. J. Nutr. 2014, 144, 929–936. [Google Scholar] [CrossRef] [PubMed]
- Maillot, M.; Vieux, F.; Amiot, M.J.; Darmon, N. Individual diet modeling translates nutrient recommendations into realistic and individual-specific food choices. Am. J. Clin. Nutr. 2010, 91, 421–430. [Google Scholar] [CrossRef] [PubMed]
- Sluik, D.; van Lee, L.; Engelen, A.I.; Feskens, E.J.M. Total, Free, and Added Sugar Consumption and Adherence to Guidelines: The Dutch National Food Consumption Survey 2007–2010. Nutrients 2016, 8, 70. [Google Scholar] [CrossRef]
- Maillot, M.; Darmon, N.; Darmon, M.; Lafay, L.; Drewnowski, A. Nutrient-dense food groups have high energy costs: An econometric approach to nutrient profiling. J. Nutr. 2007, 137, 1815–1820. [Google Scholar] [PubMed]
- Swinburn, B.A.; Caterson, I.; Seidell, J.C.; James, W.P.T. Diet, nutrition and the prevention of excess weight gain and obesity. Public Health Nutr. 2004, 7, 123–146. [Google Scholar] [PubMed]
- Hall, K.D.; Heymsfield, S.B.; Kemnitz, J.W.; Klein, S.; Schoeller, D.A.; Speakman, J.R. Energy balance and its components: Implications for body weight regulation123. Am. J. Clin. Nutr. 2012, 95, 989–994. [Google Scholar] [CrossRef] [PubMed]
- Hercberg, S.; Chat-Yung, S.; Chauliac, M. The French National Nutrition and Health Program: 2001–2006–2010. Int. J. Public Health 2008, 53, 68–77. [Google Scholar] [CrossRef] [PubMed]
- Ferguson, E.L.; Darmon, N.; Briend, A.; Premachandra, I.M. Food-based dietary guidelines can be developed and tested using linear programming analysis. J. Nutr. 2004, 134, 951–957. [Google Scholar] [PubMed]
- Scarborough, P.; Kaur, A.; Cobiac, L.; Owens, P.; Parlesak, A.; Sweeney, K.; Rayner, M. Eatwell Guide: Modelling the dietary and cost implications of incorporating new sugar and fibre guidelines. BMJ Open 2016, 6, e013182. [Google Scholar] [CrossRef] [PubMed]
- Horgan, G.W.; Perrin, A.; Whybrow, S.; Macdiarmid, J.I. Achieving dietary recommendations and reducing greenhouse gas emissions: Modelling diets to minimise the change from current intakes. Int. J. Behav. Nutr. Phys. Act. 2016, 13, 46. [Google Scholar] [CrossRef] [PubMed]
- Camilleri, G.M. Perception of Physical Sensations and Emotions in the Context of Eating Behavior: Associations with Food Intake and Weight Status in the General Population. Ph.D. Thesis, Paris 13 University, Villetaneuse, France, November 2015. [Google Scholar]
- U.S. Food & Drug Administration (FDA). Changes to the Nutrition Facts Label. Available online: http://www.fda.gov/Food/GuidanceRegulation/GuidanceDocumentsRegulatoryInformation/LabelingNutrition/ucm385663.htm (accessed on 16 February 2017).
- Laquatra, I.; Sollid, K.; Smith Edge, M.; Pelzel, J.; Turner, J. Including “Added Sugars” on the Nutrition Facts Panel: How Consumers Perceive the Proposed Change. J. Acad. Nutr. Diet. 2015, 115, 1758–1763. [Google Scholar] [CrossRef] [PubMed]
| ALL | FS-ACCEPTABLE | FS-EXCESS | p 1 | p 2 | |
|---|---|---|---|---|---|
| Individuals, n | 1693 | 1003 | 690 | ||
| Age, year 3 | 47.0 ± 15.02 | 51.1 ± 14.0 | 41.1 ± 14.5 | <0.001 | - |
| Age, % | |||||
| 20–34 | 25.4 | 15.1 | 40.3 | ||
| 35–49 | 29.8 | 28.9 | 31.3 | ||
| 50–64 | 29.0 | 35.0 | 20.3 | ||
| 65–75 | 15.8 | 21.0 | 8.2 | ||
| Gender, % | 0.087 | - | |||
| Male | 47.6 | 49.4 | 45.0 | ||
| Female | 52.4 | 50.6 | 55.0 | ||
| BMI, kg/m2 3,4 | 24.5 ± 4.3 | 25.2 ± 4.3 | 23.6 ± 4.0 | <0.001 | 0.001 |
| BMI, % | <0.001 | 0.001 | |||
| <18.5 kg/m2 | 4.2 | 3.0 | 6.0 | ||
| 18.5 to <25 kg/m2 | 55.7 | 49.2 | 65.1 | ||
| 25 to <30 kg/m2 | 30.6 | 35.4 | 23.7 | ||
| >30 kg/m2 | 9.5 | 12.4 | 5.3 | ||
| Household composition, % | |||||
| Couple with at least one child | 31.7 | 28.2 | 36.8 | <0.001 | |
| Couple with no child | 42.3 | 49.3 | 32.0 | ||
| Single with at least one child | 5.4 | 4.2 | 7.0 | ||
| Single with no child | 20.6 | 18.3 | 23.9 | ||
| Missing information | 0.1 | . | 0.2 | ||
| Socio-professional status, % | <0.001 | ||||
| Active | 56.2 | 52.6 | 61.5 | ||
| Unemployed | 4.2 | 3.4 | 5.3 | ||
| Student | 4.9 | 1.6 | 9.6 | ||
| Retired | 25.9 | 34.3 | 13.8 | ||
| Homemaker | 8.8 | 8.1 | 9.8 | ||
| ICU, euros/month 3 | 1328 ± 837 | 1359 ± 830 | 1285 ± 847 | 0.069 | |
| Current smoking status, % | <0.001 | 0.0216 | |||
| Smoker | 27.9 | 23.7 | 34.0 | ||
| Non-smoker | 70.3 | 74.8 | 63.7 | ||
| Missing | 1.8 | 1.5 | 2.3 | ||
| IPAQ, % | 0.156 | 0.239 | |||
| Low | 22.6 | 20.9 | 25.1 | ||
| Moderate | 30.5 | 31.2 | 29.6 | ||
| High | 45.7 | 46.8 | 44.0 | ||
| Missing information | 1.2 | 1.1 | 1.3 | ||
| Screen for leisure time, minutes/day 3,4 | 205 ± 138 | 195 ± 128 | 221 ± 151 | 0.002 | 0.020 |
| In front of computer | 60 ± 97 | 52 ± 94 | 73 ± 101 | <0.001 | 0.249 |
| In front of TV | 145 ± 98 | 143 ± 89 | 148 ± 110 | 0.442 | 0.040 |
| Frequency of eating between meals, as declared % | <0.001 | <0.001 | |||
| ≥4 times/day | 2.4 | 1.3 | 4.0 | ||
| 2 to 3 times/day | 15.1 | 11.8 | 19.8 | ||
| 1/day | 31.5 | 28.1 | 36.3 | ||
| >0 and <1/day | 25.3 | 26.6 | 23.4 | ||
| Never | 23.4 | 29.6 | 14.4 | ||
| Missing/invalid answers | 2.4 | 2.6 | 2.1 | ||
| Interest in diet, % | 0.001 | 0.010 | |||
| A lot | 32.8 | 36.4 | 27.7 | ||
| Little | 44.7 | 44.6 | 45.0 | ||
| Not really | 16.3 | 13.3 | 20.7 | ||
| Not at all | 4.9 | 4.5 | 5.3 | ||
| Missing/invalid answers | 1.3 | 1.2 | 1.3 |
| ALL | FS-ACCEPTABLE | FS-EXCESS | p 1 | p 2 | p 3 | |
|---|---|---|---|---|---|---|
| Individuals, n | 1693 | 1003 | 690 | |||
| Mean ± SD | ||||||
| Energy intake (kcal/day) 4 | 2151 ± 536 | 2123 ± 539 | 2192 ± 529 | 0.016 | 0.007 | 0.008 |
| from main meals (kcal/day) | 1969 ± 501 | 1992 ± 509 | 1935 ± 487 | 0.158 | 0.316 | 0.359 |
| from snacking occasions (kcal/day) | 183 ± 194 | 131 ± 154 | 258 ± 220 | <0.001 | <0.001 | <0.001 |
| Proteins, % of energy | 16.5 ± 2.7 | 17.3 ± 2.7 | 15.3 ± 2.2 | <0.001 | <0.001 | <0.001 |
| Fats, % of energy | 38.5 ± 5.7 | 39.4 ± 6.0 | 37.1 ± 4.8 | <0.001 | <0.001 | <0.001 |
| Carbohydrates, % of energy | 42.7 ± 6.1 | 40.8 ± 6.2 | 45.4 ± 5.0 | <0.001 | <0.001 | <0.001 |
| Free sugars, % of energy | 9.5 ± 5.1 | 6.3 ± 2.5 | 14.2 ± 4.2 | <0.001 | <0.001 | <0.001 |
| Starch, g/day | 141.1 ± 51.2 | 143.5 ± 55.7 | 137.7 ± 43.6 | <0.001 | <0.001 | <0.001 |
| Total sugars, g/day | 90.2 ± 37.3 | 75.1 ± 29.2 | 112.1 ± 37.1 | <0.001 | <0.001 | <0.001 |
| Free sugars g/day | 51.9 ± 33.1 | 33.5 ± 16.6 | 78.7 ± 33.1 | <0.001 | <0.001 | <0.001 |
| from main meals (g/day) | 39.4 ± 24.5 | 27.2 ± 14.4 | 57.0 ± 25.5 | <0.001 | <0.001 | <0.001 |
| from snacking occasions (g/day) | 12.6 ± 16.3 | 6.3 ± 7.2 | 21.7 ± 20.9 | <0.001 | <0.001 | <0.001 |
| Non-free sugars, g/day | 38.3 ± 19.6 | 41.6 ± 21.1 | 33.4 ± 16.0 | <0.001 | <0.001 | <0.001 |
| Alcohol, g/day | 0.22 ± 0.74 | 0.18 ± 0.63 | 0.27 ± 0.87 | 0.086 | 0.052 | 0.050 |
| Solid energy density, kcal/100 g | 173.4 ± 32.7 | 165.2 ± 14.9 | 185.3 ± 31.6 | <0.001 | <0.001 | <0.001 |
| Variety, number of foods/week | 58.4 ± 14.9 | 57.4 ± 7.6 | 60.0 ± 14.7 | 0.017 | 0.006 | 0.014 |
| PANDiet | 62.7 ± 7.5 | 64.3 ± 12.8 | 60.4 ± 6.6 | <0.001 | <0.001 | <0.001 |
| MAR, % | 83.8 ± 9.0 | 84.8 ± 23.9 | 82.4 ± 9.3 | <0.001 | <0.001 | <0.001 |
| MER, % | 32.2 ± 30.0 | 25.1 ± 14.9 | 42.6 ± 34.6 | <0.001 | <0.001 | <0.001 |
| Observed Diets | Optimized Diets | FS-Acceptable | FS-Excess | |||||||
|---|---|---|---|---|---|---|---|---|---|---|
| ALL | FS-ACCEPTABLE | FS-EXCESS | p 1 | ALL | FS-ACCEPTABLE | FS-EXCESS | p 1 | p 2 | p 2 | |
| Individuals, n | 1693 | 1003 | 690 | 1693 | 1003 | 690 | ||||
| Mean ± SD | Mean ± SD | |||||||||
| Fruits/vegetables/nuts | 379.7 ± 236.7 | 438.0 ± 248.1 | 294.8 ± 189.8 | a,b,c | 562.3 ± 177.2 | 583.8 ± 184.3 | 531.1 ± 161.4 | a,b,c | <0.001 | <0.001 |
| Fruits | 163.1 ± 148.8 | 190.8 ± 162.9 | 122.9 ± 114.1 | a,b,c | 322.3 ± 138.9 | 336.1 ± 144.9 | 302.2 ± 127.1 | a,b,c | <0.001 | <0.001 |
| Fresh | 149.6 ± 144.4 | 178.5 ± 159.1 | 107.4 ± 106.6 | a,b,c | 307.0 ± 137.2 | 321.8 ± 143.5 | 285.4 ± 124.5 | a,b,c | <0.001 | <0.001 |
| Processed | 13.6 ± 31.7 | 12.3 ± 31.1 | 15.5 ± 32.4 | a,b,c | 15.3 ± 31.9 | 14.3 ± 32.8 | 16.8 ± 30.4 | <0.001 | 0.063 | |
| Vegetables | 214.5 ± 142.3 | 245.2 ± 149.6 | 169.8 ± 117.4 | a,b,c | 234.6 ± 99.4 | 242.3 ± 102.8 | 223.4 ± 93.2 | 0.593 | <0.001 | |
| Nuts | 2.1 ± 5.8 | 2.0 ± 5.7 | 2.1 ± 6.0 | 5.4 ± 9.2 | 5.4 ± 9.3 | 5.5 ± 9.1 | <0.001 | <0.001 | ||
| Starchy foods | 254.2 ± 118.9 | 270.0 ± 127.1 | 231.2 ± 101.6 | a,b,c | 366.7 ± 109.4 | 375.4 ± 112.2 | 354.1 ± 104.1 | a,b,c | <0.001 | <0.001 |
| Refined | 168.8 ± 96.4 | 181.2 ± 102.5 | 150.7 ± 83.5 | a,b,c | 222.9 ± 92.2 | 229.1 ± 94.2 | 214.0 ± 88.4 | a,b,c | <0.001 | <0.001 |
| Unrefined | 80.5 ± 59.4 | 85.1 ± 64.6 | 73.9 ± 50.1 | a,b,c | 139.3 ± 56.6 | 142.7 ± 58.1 | 134.3 ± 53.8 | a,b,c | <0.001 | <0.001 |
| Ready-to-eat cereals | 4.9 ± 16.3 | 3.6 ± 13.4 | 6.7 ± 19.6 | 4.5 ± 14.2 | 3.6 ± 13.1 | 5.9 ± 15.5 | 0.881 | 0.033 | ||
| Meats/eggs/fish | 166.9 ± 70.2 | 179.9 ± 71.7 | 147.9 ± 63.4 | a,b,c | 142.8 ± 43.2 | 144.5 ± 42.2 | 140.2 ± 44.7 | <0.001 | 0.001 | |
| Mixed dishes and sandwiches | 120.9 ± 91.4 | 117.4 ± 93.7 | 125.9 ± 87.9 | 70.4 ± 53.8 | 65.1 ± 51.9 | 78.1 ± 55.6 | <0.001 | <0.001 | ||
| Dairy products | 209.4 ± 173.7 | 201.5 ± 174.4 | 221.0 ± 172.1 | 222.7 ± 146.0 | 222.7 ± 142.1 | 222.7 ± 151.6 | <0.001 | 0.754 | ||
| Milk | 94.4 ± 151.6 | 85.5 ± 153.1 | 107.5 ± 148.4 | 109.7 ± 138.0 | 106.7 ± 133.2 | 114.1 ± 144.7 | <0.001 | 0.183 | ||
| Plain milk | 86.8 ± 145.8 | 80.9 ± 151.6 | 95.5 ± 136.5 | 104.0 ± 134.3 | 102.9 ± 132.9 | 105.7 ± 136.4 | <0.001 | 0.034 | ||
| Sweet milk | 7.6 ± 38.2 | 4.6 ± 28.1 | 12.0 ± 49.0 | 5.7 ± 29.3 | 3.8 ± 23.7 | 8.3 ± 35.8 | 0.202 | 0.004 | ||
| Yogurts | 80.9 ± 81.3 | 78.9 ± 79.9 | 83.7 ± 83.1 | 94.7 ± 83.6 | 95.8 ± 83.3 | 93.2 ± 84.0 | <0.001 | 0.000 | ||
| Plain yogurts | 39.5 ± 60.5 | 44.8 ± 67.0 | 31.7 ± 48.6 | 48.1 ± 66.1 | 54.7 ± 71.6 | 38.7 ± 55.9 | <0.001 | <0.001 | ||
| Sweet yogurts | 41.4 ± 59.5 | 34.1 ± 53.4 | 52.0 ± 66.0 | a,b,c | 46.6 ± 61.4 | 41.1 ± 58.4 | 54.5 ± 64.8 | <0.001 | 0.227 | |
| Cheese | 34.1 ± 28.8 | 37.1 ± 29.8 | 29.8 ± 26.9 | a,b,c | 18.3 ± 14.0 | 20.2 ± 14.5 | 15.5 ± 12.9 | <0.001 | <0.001 | |
| Sweet products | 119.9 ± 76.0 | 91.1 ± 58.7 | 161.7 ± 79.2 | a,b,c | 103.4 ± 65.5 | 91.3 ± 62.5 | 121.2 ± 65.7 | a,b,c | 0.907 | <0.001 |
| Milk or eggs-containing desserts | 18.4 ± 31.0 | 12.3 ± 21.7 | 27.3 ± 39.3 | a,b,c | 17.4 ± 29.4 | 13.1 ± 23.9 | 23.6 ± 35.2 | a,b,c | 0.082 | <0.001 |
| Cakes and pastries | 48.3 ± 44.7 | 41.1 ± 38.5 | 58.9 ± 50.6 | a,b,c | 39.1 ± 37.1 | 37.7 ± 36.3 | 41.0 ± 38.1 | 0.006 | <0.001 | |
| Biscuits | 8.2 ± 18.4 | 4.6 ± 10.8 | 13.6 ± 24.9 | a,b,c | 7.9 ± 15.3 | 5.8 ± 12.5 | 10.8 ± 18.1 | a,b,c | <0.001 | 0.001 |
| Croissants | 17.5 ± 26.0 | 14.2 ± 23.6 | 22.1 ± 28.5 | a,b,c | 15.7 ± 24.3 | 15.3 ± 24.5 | 16.4 ± 24.0 | 0.267 | <0.001 | |
| Confectionery (incl. chocolate) | 5.8 ± 14.1 | 3.1 ± 6.4 | 9.9 ± 20.0 | a,b,c | 4.4 ± 7.9 | 3.2 ± 6.2 | 6.0 ± 9.6 | a,b,c | 0.229 | <0.001 |
| Honey, marmalade and chocolate spread | 13.8 ± 19.8 | 10.4 ± 15.8 | 18.6 ± 23.8 | a,b,c | 13.5 ± 17.5 | 11.3 ± 16.3 | 16.7 ± 18.7 | a,b,c | 0.009 | 0.003 |
| Table sugar | 7.8 ± 10.2 | 5.5 ± 7.6 | 11.3 ± 12.4 | a,b,c | 5.5 ± 6.9 | 4.8 ± 6.7 | 6.7 ± 7.0 | a,b,c | <0.001 | <0.001 |
| Beverages including water | 1322.6 ± 630.3 | 1288.5 ± 655.7 | 1372.1 ± 588.3 | 1398.4 ± 403.0 | 1398.1 ± 421.3 | 1398.8 ± 374.9 | <0.001 | 0.259 | ||
| Water | 798.6 ± 569.3 | 821.1 ± 596.0 | 765.7 ± 526.7 | a | 898.4 ± 412.1 | 911.2 ± 426.8 | 879.8 ± 389.3 | <0.001 | <0.001 | |
| Hot beverages | 389.4 ± 335.3 | 403.7 ± 332.1 | 368.4 ± 339.0 | 412.4 ± 334.3 | 428.4 ± 325.0 | 389.1 ± 346.2 | <0.001 | <0.001 | ||
| Diet beverages | 12.9 ± 62.2 | 10.2 ± 58.3 | 16.9 ± 67.3 | 17.6 ± 72.2 | 14.6 ± 69.2 | 21.9 ± 76.3 | 0.018 | 0.009 | ||
| Sugar-sweetened beverages | 62.4 ± 175.4 | 17.0 ± 46.4 | 128.3 ± 255.5 | a,b,c | 23.5 ± 60.8 | 10.1 ± 31.1 | 43.1 ± 83.9 | a,b,c | <0.001 | <0.001 |
| Fruit juices 100% | 59.4 ± 89.9 | 36.4 ± 62.2 | 92.8 ± 111.4 | a,b,c | 46.5 ± 67.2 | 33.7 ± 55.0 | 65.0 ± 78.4 | a,b,c | 0.012 | <0.001 |
| Added fats and sauces | 45.5 ± 23.4 | 48.1 ± 23.3 | 41.8 ± 23.1 | a,b,c | 39.4 ± 18.4 | 39.2 ± 19.0 | 39.8 ± 17.6 | <0.001 | 0.012 | |
| Foods based on soya | 3.5 ± 25.4 | 4.0 ± 25.9 | 2.9 ± 24.7 | 3.8 ± 25.5 | 4.0 ± 25.4 | 3.5 ± 25.6 | 0.907 | 0.168 | ||
© 2017 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license ( http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Lluch, A.; Maillot, M.; Gazan, R.; Vieux, F.; Delaere, F.; Vaudaine, S.; Darmon, N. Individual Diet Modeling Shows How to Balance the Diet of French Adults with or without Excessive Free Sugar Intakes. Nutrients 2017, 9, 162. https://doi.org/10.3390/nu9020162
Lluch A, Maillot M, Gazan R, Vieux F, Delaere F, Vaudaine S, Darmon N. Individual Diet Modeling Shows How to Balance the Diet of French Adults with or without Excessive Free Sugar Intakes. Nutrients. 2017; 9(2):162. https://doi.org/10.3390/nu9020162
Chicago/Turabian StyleLluch, Anne, Matthieu Maillot, Rozenn Gazan, Florent Vieux, Fabien Delaere, Sarah Vaudaine, and Nicole Darmon. 2017. "Individual Diet Modeling Shows How to Balance the Diet of French Adults with or without Excessive Free Sugar Intakes" Nutrients 9, no. 2: 162. https://doi.org/10.3390/nu9020162
APA StyleLluch, A., Maillot, M., Gazan, R., Vieux, F., Delaere, F., Vaudaine, S., & Darmon, N. (2017). Individual Diet Modeling Shows How to Balance the Diet of French Adults with or without Excessive Free Sugar Intakes. Nutrients, 9(2), 162. https://doi.org/10.3390/nu9020162






