25-Hydroxy-Vitamin D Concentration Is Not Affected by Severe or Non-Severe Pneumonia, or Inflammation, in Young Children
Abstract
:1. Introduction
2. Materials and Methods
2.1. Study Population and Study Design
2.2. Data Collection and Laboratory Procedures
2.3. Statistics
3. Results
3.1. Child Characteristics
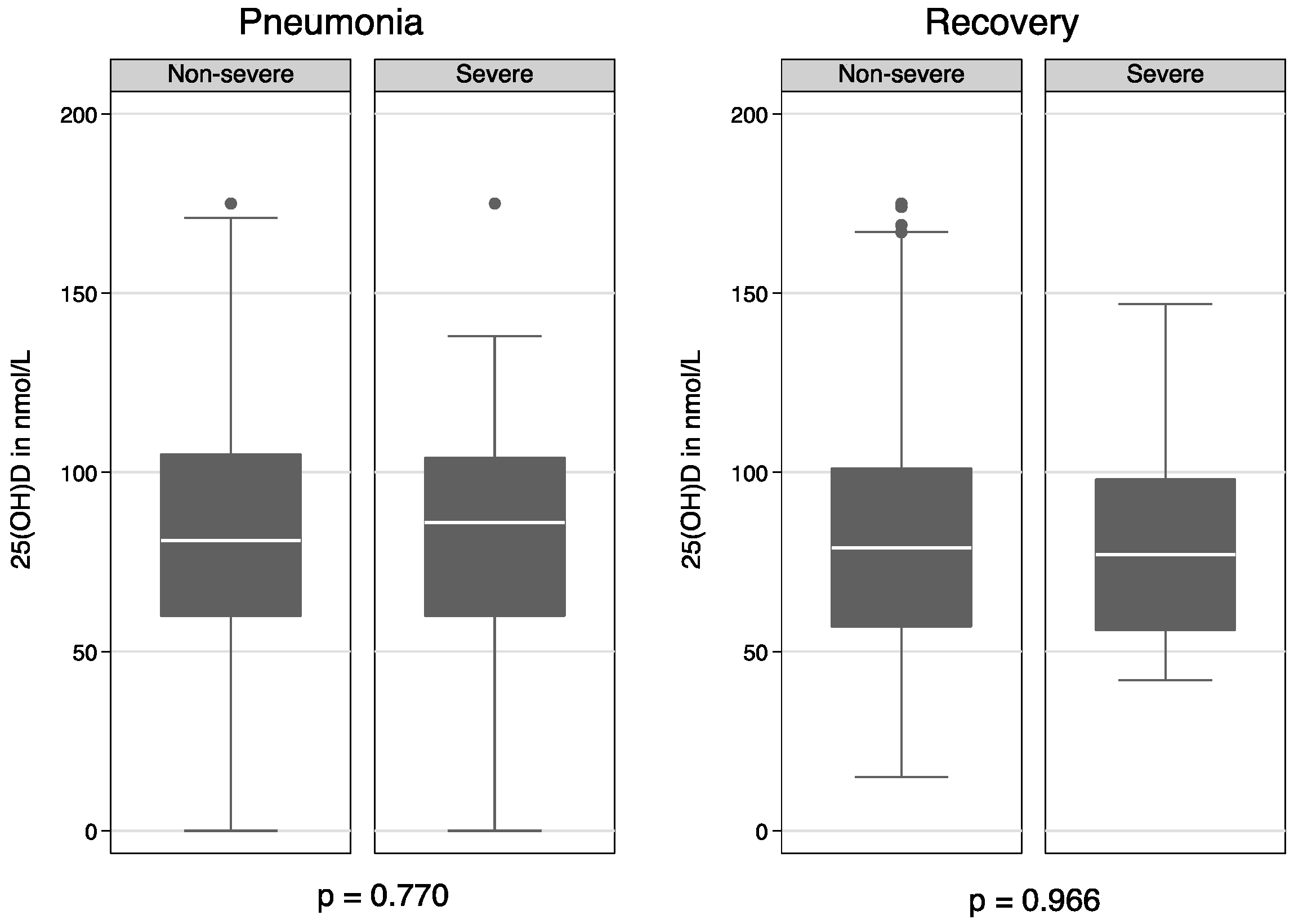
3.2. Concentrations and Correlations of 25(OH)D and Inflammatory Markers
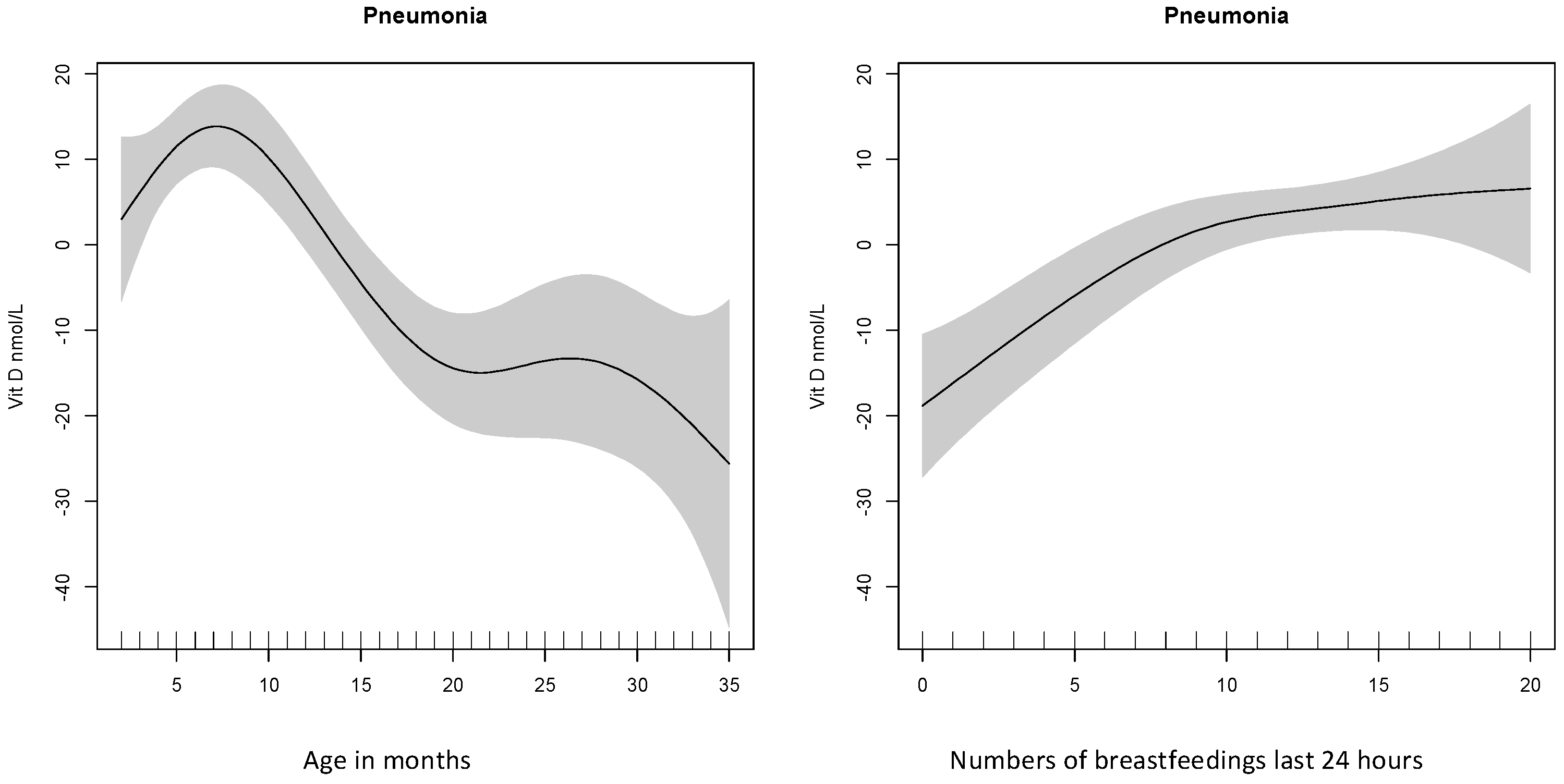
3.3. Predictors of 25(OH)D Concentration
4. Discussion
5. Conclusions
Supplementary Materials
Acknowledgments
Author Contributions
Conflicts of Interest
References
- Laaksi, I.; Ruohola, J.P.; Tuohimaa, P.; Auvinen, A.; Haataja, R.; Pihlajamaki, H.; Ylikomi, T. An association of serum vitamin D concentrations <40 nmol/L with acute respiratory tract infection in young Finnish men. Am. J. Clin. Nutr. 2007, 86, 714–717. [Google Scholar] [PubMed]
- Karatekin, G.; Kaya, A.; Salihoglu, O.; Balci, H.; Nuhoglu, A. Association of subclinical vitamin D deficiency in newborns with acute lower respiratory infection and their mothers. Eur. J. Clin. Nutr. 2009, 63, 473–477. [Google Scholar] [CrossRef] [PubMed]
- McNally, J.D.; Leis, K.; Matheson, L.A.; Karuananyake, C.; Sankaran, K.; Rosenberg, A.M. Vitamin D deficiency in young children with severe acute lower respiratory infection. Pediatr. Pulmonol. 2009, 44, 981–988. [Google Scholar] [CrossRef] [PubMed]
- Wayse, V.; Yousafzai, A.; Mogale, K.; Filteau, S. Association of subclinical vitamin D deficiency with severe acute lower respiratory infection in Indian children under 5 years. Eur. J. Clin. Nutr. 2004, 58, 563–567. [Google Scholar] [CrossRef] [PubMed]
- Kamen, D.L.; Tangpricha, V. Vitamin D and molecular actions on the immune system: Modulation of innate and autoimmunity. J. Mol. Med. (Berl.) 2010, 88, 441–450. [Google Scholar] [CrossRef] [PubMed]
- Holick, M.F. Vitamin D deficiency. N. Engl. J. Med. 2007, 357, 266–281. [Google Scholar] [CrossRef] [PubMed]
- Liu, P.T.; Stenger, S.; Li, H.; Wenzel, L.; Tan, B.H.; Krutzik, S.R.; Ochoa, M.T.; Schauber, J.; Wu, K.; Meinken, C.; et al. Toll-like receptor triggering of a vitamin D-mediated human antimicrobial response. Science 2006, 311, 1770–1773. [Google Scholar] [CrossRef] [PubMed]
- Gombart, A.F.; Borregaard, N.; Koeffler, H.P. Human cathelicidin antimicrobial peptide (CAMP) gene is a direct target of the vitamin D receptor and is strongly up-regulated in myeloid cells by 1,25-dihydroxyvitamin D3. FASEB J. 2005, 19, 1067–1077. [Google Scholar] [CrossRef] [PubMed]
- Wang, T.T.; Nestel, F.P.; Bourdeau, V.; Nagai, Y.; Wang, Q.; Liao, J.; Tavera-Mendoza, L.; Lin, R.; Hanrahan, J.W.; Mader, S.; et al. Cutting edge: 1,25-dihydroxyvitamin D3 is a direct inducer of antimicrobial peptide gene expression. J. Immunol. 2004, 173, 2909–2912. [Google Scholar] [CrossRef] [PubMed]
- Bergman, P.; Lindh, A.U.; Bjorkhem-Bergman, L.; Lindh, J.D. Vitamin D and Respiratory Tract Infections: A Systematic Review and Meta-Analysis of Randomized Controlled Trials. PLoS ONE 2013, 8, e65835. [Google Scholar] [CrossRef] [PubMed]
- Xiao, L.; Xing, C.; Yang, Z.; Xu, S.; Wang, M.; Du, H.; Liu, K.; Huang, Z. Vitamin D supplementation for the prevention of childhood acute respiratory infections: A systematic review of randomised controlled trials. Br. J. Nutr. 2015, 114, 1026–1034. [Google Scholar] [CrossRef] [PubMed]
- Jolliffe, D.A.; Griffiths, C.J.; Martineau, A.R. Vitamin D in the prevention of acute respiratory infection: Systematic review of clinical studies. J. Steroid Biochem. Mol. Biol. 2013, 136, 321–329. [Google Scholar] [CrossRef] [PubMed]
- Waldron, J.L.; Ashby, H.L.; Cornes, M.P.; Bechervaise, J.; Razavi, C.; Thomas, O.L.; Chugh, S.; Deshpande, S.; Ford, C.; Gama, R. Vitamin D: A negative acute phase reactant. J. Clin. Pathol. 2013, 66, 620–622. [Google Scholar] [CrossRef] [PubMed]
- Reid, D.; Toole, B.J.; Knox, S.; Talwar, D.; Harten, J.; O’Reilly, D.S.; Blackwell, S.; Kinsella, J.; McMillan, D.C.; Wallace, A.M. The relation between acute changes in the systemic inflammatory response and plasma 25-hydroxyvitamin D concentrations after elective knee arthroplasty. Am. J. Clin. Nutr. 2011, 93, 1006–1011. [Google Scholar] [CrossRef] [PubMed]
- Bang, U.C.; Novovic, S.; Andersen, A.M.; Fenger, M.; Hansen, M.B.; Jensen, J.E. Variations in serum 25-hydroxyvitamin D during acute pancreatitis: An exploratory longitudinal study. Endocr. Res. 2011, 36, 135–141. [Google Scholar] [CrossRef] [PubMed]
- Silva, M.C.; Furlanetto, T.W. Does serum 25-hydroxyvitamin D decrease during acute-phase response? A systematic review. Nutr. Res. 2015, 35, 91–96. [Google Scholar] [CrossRef] [PubMed]
- Newens, K.; Filteau, S.; Tomkins, A. Plasma 25-hydroxyvitamin D does not vary over the course of a malarial infection. Trans. R. Soc. Trop. Med. Hyg. 2006, 100, 41–44. [Google Scholar] [CrossRef] [PubMed]
- Binfield, A.; Aird, C.; Murdoch, D.R.; Elder, P.; Walls, T. Are vitamin D levels affected by acute bacterial infections in children? J. Paediatr. Child Health 2014, 50, 643–646. [Google Scholar] [CrossRef] [PubMed]
- Valentiner-Branth, P.; Shrestha, P.S.; Chandyo, R.K.; Mathisen, M.; Basnet, S.; Bhandari, N.; Adhikari, R.K.; Sommerfelt, H.; Strand, T.A. A randomized controlled trial of the effect of zinc as adjuvant therapy in children 2–35 months of age with severe or nonsevere pneumonia in Bhaktapur, Nepal. Am. J. Clin. Nutr. 2010, 91, 1667–1674. [Google Scholar] [CrossRef] [PubMed]
- World Health Organization. Integrated Management of Childhood Illness; World Health Organization: Geneva, Switzerland, 2002. [Google Scholar]
- Haugen, J.; Chandyo, R.K.; Brokstad, K.A.; Mathisen, M.; Ulak, M.; Basnet, S.; Valentiner-Branth, P.; Strand, T.A. Cytokine Concentrations in Plasma from Children with Severe and Non-Severe Community Acquired Pneumonia. PLoS ONE 2015, 10, e0138978. [Google Scholar] [CrossRef] [PubMed]
- Chandyo, R.K.; Shrestha, P.S.; Valentiner-Branth, P.; Mathisen, M.; Basnet, S.; Ulak, M.; Adhikari, R.K.; Sommerfelt, H.; Strand, T.A. Two weeks of zinc administration to Nepalese children with pneumonia does not reduce the incidence of pneumonia or diarrhea during the next six months. J. Nutr. 2010, 140, 1677–1682. [Google Scholar] [CrossRef] [PubMed]
- BioRad Laboratories. Bio-Plex Pro™ Cytokine, Chemokine, and Growth Factor Assays Instruction Manual; BioRad Inc. Life Science Research: Hercules, CA, USA, 2016. [Google Scholar]
- Wood, S. Modelling and Smoothing Parameter Estimation with Multiple Quadratic Penalties. J. R. Stat. Soc. B 2000, 62, 413–428. [Google Scholar] [CrossRef]
- Hosmer, D.W.; Lemeshow, S. Applied Logistic Regression, 2nd ed.; John Wiley & Sons Inc.: New York, NY, USA, 2000. [Google Scholar]
- Adhikari, K.R. Estimation of Global Solar Radiation for Four Selected Sites in Nepal Using Sunshine Hours, Temperature and Relative Humidity. J. Power Energy Eng. 2013, 1, 1–9. [Google Scholar] [CrossRef]
- Ministry of Health and Population (MOHP); New ERA; ICF International Inc. Nepal Demographic and Health Survey 2011. Available online: http://reliefweb.int/sites/reliefweb.int/files/resources/nepal%20demographic%20and%20health%20survey%202011.pdf (accessed on 9 January 2017).
- Avagyan, D.; Neupane, S.P.; Gundersen, T.E.; Madar, A.A. Vitamin D status in pre-school children in rural Nepal. Public Health Nutr. 2015, 1–7. [Google Scholar] [CrossRef] [PubMed]
- Hollis, B.W.; Wagner, C.L.; Howard, C.R.; Ebeling, M.; Shary, J.R.; Smith, P.G.; Taylor, S.N.; Morella, K.; Lawrence, R.A.; Hulsey, T.C. Maternal Versus Infant Vitamin D Supplementation During Lactation: A Randomized Controlled Trial. Pediatrics 2015, 136, 625–634. [Google Scholar] [CrossRef] [PubMed]
- Hollis, B.W.; Wagner, C.L. Vitamin D requirements during lactation: High-dose maternal supplementation as therapy to prevent hypovitaminosis D for both the mother and the nursing infant. Am. J. Clin. Nutr. 2004, 80 (Suppl. 6), 1752S–1758S. [Google Scholar] [PubMed]
- Wall, C.R.; Stewart, A.W.; Camargo, C.A., Jr.; Scragg, R.; Mitchell, E.A.; Ekeroma, A.; Crane, J.; Milne, T.; Rowden, J.; Horst, R.; et al. Vitamin D activity of breast milk in women randomly assigned to vitamin D3 supplementation during pregnancy. Am. J. Clin. Nutr. 2016, 103, 382–388. [Google Scholar] [CrossRef] [PubMed]
- Greer, F.R.; Hollis, B.W.; Cripps, D.J.; Tsang, R.C. Effects of maternal ultraviolet B irradiation on vitamin D content of human milk. J. Pediatr. 1984, 105, 431–433. [Google Scholar] [CrossRef]
- Roche Diagnostics International Ltd. Elecsys Vitamin D total assay. Electro-chemiluminescence Binding Assay (ECLIA) for the in Vitro Determination of Total 25-hydroxyvitamin D. Roche Diagnostics International Ltd.: Rotkreuz, Switzerland, 2012. [Google Scholar]
- Bailey, D.; Veljkovic, K.; Yazdanpanah, M.; Adeli, K. Analytical measurement and clinical relevance of vitamin D(3) C3-epimer. Clin. Biochem. 2013, 46, 190–196. [Google Scholar] [CrossRef] [PubMed]
- Singh, R.J.; Taylor, R.L.; Reddy, G.S.; Grebe, S.K. C-3 epimers can account for a significant proportion of total circulating 25-hydroxyvitamin D in infants, complicating accurate measurement and interpretation of vitamin D status. J. Clin. Endocrinol. Metab. 2006, 91, 3055–3061. [Google Scholar] [CrossRef] [PubMed]
| Child Characteristics | Non-Severe | Severe | |||
|---|---|---|---|---|---|
| n | Value | n | Value | ||
| Demographic data | |||||
| Age of child (months) | mean ± SD | 387 | 14.1 ± 8.5 | 43 | 7.7 ± 7.4 |
| Boys | n (%) | 387 | 205 (53.0) | 43 | 26 (60.5) |
| Breastfed—yes | n (%) | 387 | 367 (94.8) | 43 | 41 (95.3) |
| Number of breast feedings past 24 h | mean ± SD | 387 | 10.6 ± 5.6 | 11.4 ± 6.0 | |
| Family ownership of land | n (%) | 387 | 185 (47.8) | 43 | 20 (46.5) |
| Living in nuclear family (*) | n (%) | 387 | 188 (48.6) | 43 | 24 (55.8) |
| Number of family members | mean ± SD | 387 | 6.2 ± 3.3 | 43 | 5.5 ± 3.0 |
| Indoor smoking | n (%) | 386 | 248 (64.2) | 42 | 22 (52.4) |
| Z-score weights for age | mean ± SD | 387 | −0.8 ± 1.1 | 43 | −0.8 ± 1.3 |
| Z-score length/height for age | mean ± SD | 387 | −1.1 ± 1.2 | 43 | −0.7 ± 1.5 |
| Z-score weight for length/height | mean ± SD | 386 | −0.3 ± 1.0 | 43 | −0.5 ± 1.1 |
| Clinical characteristics | |||||
| Axillary temperature (°C) | mean ± SD | 387 | 37.3 ± 0.9 | 43 | 37.3 ± 0.7 |
| Duration of cough (days) | mean ± SD | 387 | 3.2 ± 2.0 | 43 | 3.1 ± 1.8 |
| Duration of difficulty breathing (days) | mean ± SD | 387 | 1.7 ± 1.9 | 43 | 1.8 ± 1.5 |
| Duration of fever (days) | median (IQR) | 387 | 2 (1–3) | 43 | 2 (1–3) |
| Respiratory rate/min | mean ± SD | 387 | 53 ± 6.7 | 43 | 66.0 ± 9.2 |
| Presence of lower chest indrawing (LCI) | n (%) | 387 | 0 (0.0) | 43 | 42 (97.7) |
| SpO2 (%) | median (IQR) | 387 | 93.5 (91.5–96.5) | 43 | 91.5 (90.5–95.0) |
| Hypoxia (SpO2 < 90%) | n (%) | 387 | 3 (0.8) | 43 | 9 (20.9) |
| Time until recovery (days) (**) | median (IQR) | 387 | 3 (2–5) | 43 | 6 (4–8) |
| CRP (mg/L) | median (IQR) | 387 | 12 (0–26) | 43 | 25 (0–50) |
| CRP > 40 (mg/L) | n (%) | 387 | 48 (12.4) | 43 | 14 (32.6) |
| Hemoglobin (g/dL) | mean ± SD | 387 | 11.2 ± 1.3 | 43 | 10.7 ± 1.5 |
| Vitamin D status | |||||
| Plasma-25(OH)D (nmol/L) | mean ± SD | 373 | 83.4 ± 34.7 | 40 | 85.6 ± 32.1 |
| Plasma-25(OH)D ˂ 30 (nmol/L) | n (%) | 373 | 20 (5.4) | 40 | 1 (2.5) |
| Plasma-25(OH)D 30–49 (nmol/L) | n (%) | 373 | 42 (11.3) | 40 | 1 (2.5) |
| Plasma-25(OH)D ≥ 50 (nmol/L) | n (%) | 373 | 312 (83.6) | 40 | 39 (97.5) |
| During Pneumonia | After Recovery | |||||
|---|---|---|---|---|---|---|
| n | Mean (*) | SD | n | Mean (*) | SD | |
| All children regardless of time for 2nd sample | 412 | 84.4 | 33.6 | 343 | 80.6 | 35.4 |
| Children with 2nd sample after 14 days | 196 | 82.9 | 32.9 | 180 | 80.0 | 32.5 |
| Children with 2nd sample after 45 days | 102 | 96.7 | 35.8 | 82 | 90.8 | 33.3 |
| Children with 2nd sample after 90 days | 114 | 76.1 | 29.7 | 81 | 71.6 | 38.4 |
| Inflammatory Markers | Baseline (VITD1) (n = 407 or 408) | After Recovery (*) (VITD2) (n = 338 or 339) | ||
|---|---|---|---|---|
| rs | p | rs | p | |
| CRP | 0.035 | 0.484 | 0.202 | <0.001 |
| IL-1β | 0.095 | 0.056 | 0.017 | 0.753 |
| IL-1ra | 0.011 | 0.824 | 0.061 | 0.265 |
| IL-4 | 0.062 | 0.213 | 0.111 | 0.041 |
| IL-6 | 0.133 | 0.007 | 0.160 | 0.003 |
| IL-8 | −0.040 | 0.424 | 0.006 | 0.912 |
| IL-9 | 0.085 | 0.087 | 0.213 | <0.001 |
| IL-10 | −0.043 | 0.382 | 0.027 | 0.622 |
| IL-15 | 0.209 | <0.001 | 0.222 | <0.001 |
| eotaxin | 0.124 | 0.013 | 0.121 | 0.027 |
| Basic-FGF | 0.020 | 0.690 | 0.080 | 0.141 |
| G-CSF | 0.070 | 0.156 | 0.123 | 0.024 |
| GM-CSF | 0.161 | 0.001 | 0.205 | <0.001 |
| TNF-α | −0.033 | 0.504 | 0.058 | 0.284 |
| IP-10 | −0.046 | 0.357 | 0.122 | 0.025 |
| VEGF | 0.018 | 0.715 | 0.035 | 0.523 |
| 25(OH)D during Pneumonia | Crude (n = 412) | Adjusted (n = 411) | |||||
|---|---|---|---|---|---|---|---|
| Coeff | 95% CI | p | Coeff | 95% CI | p | Beta | |
| Age in months | −1.9 | −2.2, −1.6 | <0.001 | −1.5 | −1.9, −1.1 | <0.001 | −0.4 |
| No. of breast feedings last 24 h | 2.3 | 1.8, 2.8 | <0.001 | 1.1 | 0.5, 1.7 | <0.001 | 0.2 |
| Ownership of agricultural land (*) | −7.4 | −13.9, −0.9 | 0.025 | −7.6 | −12.5−1.3 | 0.016 | −0.1 |
| 25(OH)D | Crude | Adjusted | |||||
|---|---|---|---|---|---|---|---|
| Coeff | 95% CI | p | Coeff | 95% CI | p | Beta | |
| Baseline plasma sample (ref) | |||||||
| 14 days plasma sample | −4.7 | −8.8, −0.6 | 0.026 | −3.0 | −6.7, 0.7 | 0.117 | −0.0 |
| 45 days plasma sample | 6.1 | −0.7, 12.8 | 0.077 | 2.3 | −3.9, 8.5 | 0.469 | 0.0 |
| 90 days plasma sample | −12.6 | −21.7, −3.5 | 0.007 | −2.1 | −10.4, 6.1 | 0.615 | −0.0 |
| Age in months | −1.9 | −2.2, −1.6 | <0.001 | −1.9 | −2.2, −1.6 | <0.001 | −0.5 |
| Ownership of agricultural land | −6.0 | −12.0, 0.6 | 0.076 | −5.8 | −11.6, −0.0 | 0.048 | −0.1 |
© 2017 by the authors; licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC-BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Haugen, J.; Chandyo, R.K.; Ulak, M.; Mathisen, M.; Basnet, S.; Brokstad, K.A.; Valentiner-Branth, P.; Shrestha, P.S.; Strand, T.A. 25-Hydroxy-Vitamin D Concentration Is Not Affected by Severe or Non-Severe Pneumonia, or Inflammation, in Young Children. Nutrients 2017, 9, 52. https://doi.org/10.3390/nu9010052
Haugen J, Chandyo RK, Ulak M, Mathisen M, Basnet S, Brokstad KA, Valentiner-Branth P, Shrestha PS, Strand TA. 25-Hydroxy-Vitamin D Concentration Is Not Affected by Severe or Non-Severe Pneumonia, or Inflammation, in Young Children. Nutrients. 2017; 9(1):52. https://doi.org/10.3390/nu9010052
Chicago/Turabian StyleHaugen, Johanne, Ram K. Chandyo, Manjeswori Ulak, Maria Mathisen, Sudha Basnet, Karl A. Brokstad, Palle Valentiner-Branth, Prakash S. Shrestha, and Tor A. Strand. 2017. "25-Hydroxy-Vitamin D Concentration Is Not Affected by Severe or Non-Severe Pneumonia, or Inflammation, in Young Children" Nutrients 9, no. 1: 52. https://doi.org/10.3390/nu9010052
APA StyleHaugen, J., Chandyo, R. K., Ulak, M., Mathisen, M., Basnet, S., Brokstad, K. A., Valentiner-Branth, P., Shrestha, P. S., & Strand, T. A. (2017). 25-Hydroxy-Vitamin D Concentration Is Not Affected by Severe or Non-Severe Pneumonia, or Inflammation, in Young Children. Nutrients, 9(1), 52. https://doi.org/10.3390/nu9010052






