Vitamin Status among Breastfed Infants in Bhaktapur, Nepal
Abstract
:1. Introduction
2. Subjects and Methods
2.1. Subjects
2.2. Enrollment Procedure
2.3. Sample Size Calculations
2.4. Blood Sampling and Biochemical Analysis
2.5. Data Analysis
3. Results
3.1. Baseline
3.2. Plasma Concentration of Vitamins and Markers for B-Vitamin Status (MMA and tHcy)
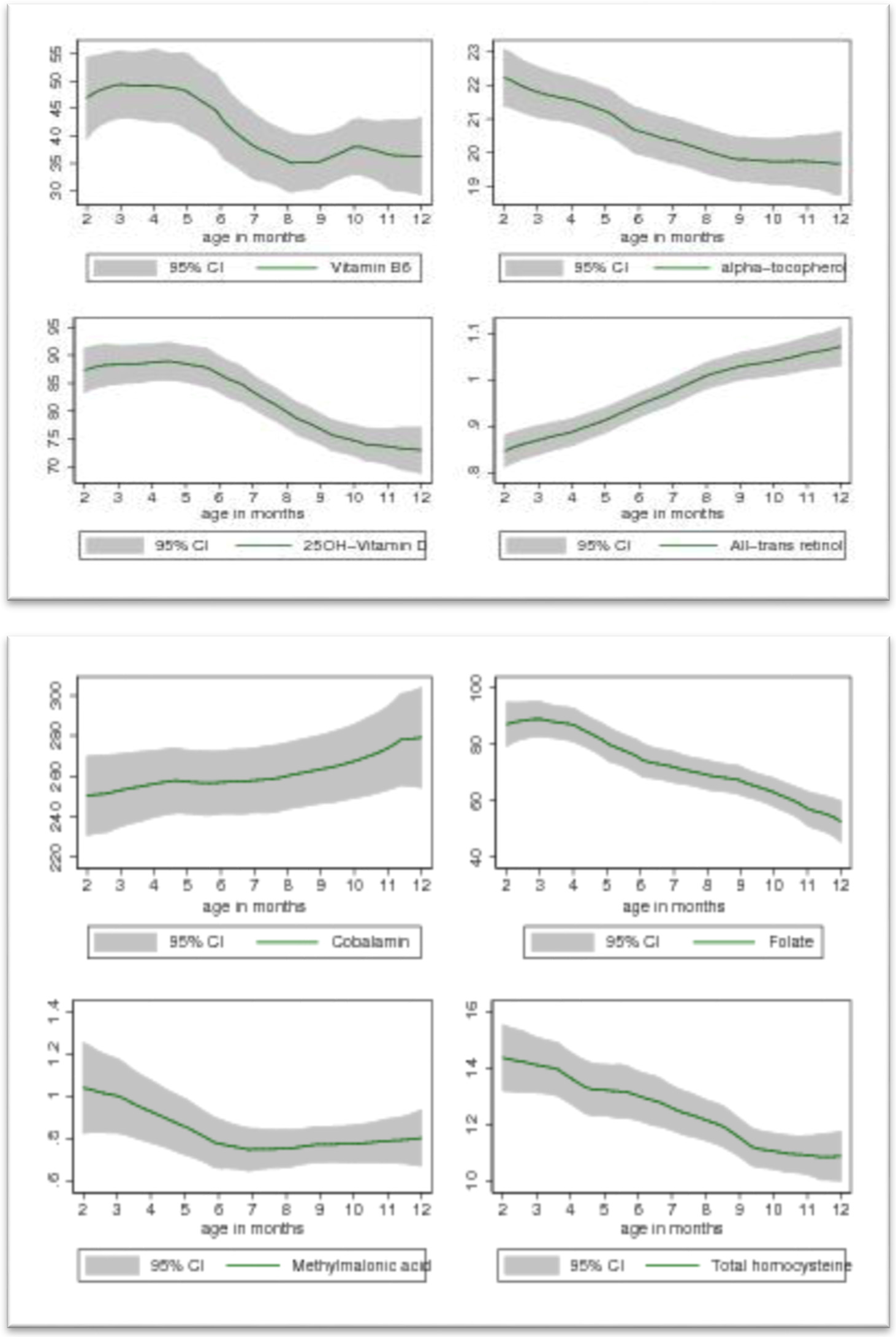
3.3. Age Related Changes of Plasma Vitamins and Metabolic Markers
3.4. Correlation Analyses
4. Discussion
5. Conclusions
Acknowledgments
Author Contributions
Conflicts of Interest
References
- Black, R.E.; Victora, C.G.; Walker, S.P.; Bhutta, Z.A.; Christian, P.; de Onis, M.; Ezzati, M.; Grantham-McGregor, S.; Katz, J.; Martorell, R.; et al. Maternal and child undernutrition and overweight in low-income and middle-income countries. Lancet 2013, 382, 427–451. [Google Scholar] [CrossRef]
- Singh, M. Role of micronutrients for physical growth and mental development. Indian J. Pediatr. 2004, 71, 59–62. [Google Scholar] [CrossRef] [PubMed]
- WHO. The World Health Report 2001: Reducing Risks, Promoting Healthy Life; World Health Organization: Geneva, Switzerland, 2001. [Google Scholar]
- Bhandari, S.; Banjara, M.R. Micronutrients deficiency, a hidden hunger in Nepal: Prevalence, causes, consequences, and solutions. Int. Sch. Res. Not. 2015, 2015, 9. [Google Scholar] [CrossRef]
- WHO. Guiding Principles for Feeding Non-Breastfed Children 6–24 Months of Age; World Health Organization: Geneva, Switzerland, 2005. [Google Scholar]
- Stephensen, C.B. Vitamin A, infection, and immune function. Annu. Rev. Nutr. 2001, 21, 167–192. [Google Scholar] [CrossRef] [PubMed]
- Thurnham, D.I. Micronutrients and immune function: Some recent developments. J. Clin. Pathol. 1997, 50, 887–891. [Google Scholar] [CrossRef] [PubMed]
- MOHP (Ministry of Health and Population (Nepal)). Nepal Demographic and Health Survey 2011; New Era, Calverton, Maryland and Icf International Inc.: Kathmandu, Nepal, 2011. [Google Scholar]
- Walker, V.P.; Modlin, R.L. The vitamin D connection to pediatric infections and immune function. Pediatr. Res. 2009, 65, 106R–113R. [Google Scholar] [CrossRef] [PubMed]
- Pletz, M.W.; Terkamp, C.; Schumacher, U.; Rohde, G.; Schutte, H.; Welte, T.; Bals, R.; Group, C.A.-S. Vitamin D deficiency in community-acquired pneumonia: Low levels of 1,25(OH)2 D are associated with disease severity. Respir. Res. 2014, 15, 53. [Google Scholar] [CrossRef] [PubMed]
- Jorde, R.; Mathiesen, E.B.; Rogne, S.; Wilsgaard, T.; Kjaergaard, M.; Grimnes, G.; Schirmer, H. Vitamin D and cognitive function: The tromso study. J. Neurol. Sci. 2015, 355, 155–161. [Google Scholar] [CrossRef] [PubMed]
- Jovanovich, A.J.; Ginde, A.A.; Holmen, J.; Jablonski, K.; Allyn, R.L.; Kendrick, J.; Chonchol, M. Vitamin D level and risk of community-acquired pneumonia and sepsis. Nutrients 2014, 6, 2196–2205. [Google Scholar] [CrossRef] [PubMed]
- Mithal, A.; Wahl, D.A.; Bonjour, J.P.; Burckhardt, P.; Dawson-Hughes, B.; Eisman, J.A.; El-Hajj Fuleihan, G.; Josse, R.G.; Lips, P.; Morales-Torres, J.; et al. Global vitamin D status and determinants of hypovitaminosis D. Osteoporos. Int. 2009, 20, 1807–1820. [Google Scholar] [CrossRef] [PubMed]
- Dror, D.K.; Allen, L.H. Vitamin E deficiency in developing countries. Food Nutr. Bull. 2011, 32, 124–143. [Google Scholar] [CrossRef] [PubMed]
- Strand, T.A.; Taneja, S.; Ueland, P.M.; Refsum, H.; Bahl, R.; Schneede, J.; Sommerfelt, H.; Bhandari, N. Cobalamin and folate status predicts mental development scores in north Indian children 12–18 months of age. Am. J. Clin. Nutr. 2013, 97, 310–317. [Google Scholar] [CrossRef] [PubMed]
- Kvestad, I.; Taneja, S.; Kumar, T.; Hysing, M.; Refsum, H.; Yajnik, C.S.; Bhandari, N.; Strand, T.A.; Folate and Vitamin B12 Study Group. Vitamin B12 and folic acid improve gross motor and problem-solving skills in young north Indian children: A randomized placebo-controlled trial. PLoS ONE 2015, 10, e0129915. [Google Scholar] [CrossRef] [PubMed]
- Strand, T.A.; Taneja, S.; Kumar, T.; Manger, M.S.; Refsum, H.; Yajnik, C.S.; Bhandari, N. Vitamin B-12, folic acid, and growth in 6- to 30-month-old children: A randomized controlled trial. Pediatrics 2015, 135, e918–e926. [Google Scholar] [CrossRef] [PubMed]
- Maggini, S.; Wintergerst, E.S.; Beveridge, S.; Hornig, D.H. Selected vitamins and trace elements support immune function by strengthening epithelial barriers and cellular and humoral immune responses. Br. J. Nutr. 2007, 98, S29–S35. [Google Scholar] [CrossRef] [PubMed]
- Horton, S.; Begin, F.; Greig, A.; Lakshman, A. Micronutrient supplements for child survival (vitamin A and zinc). Cph. Consens. Cent. 2009, 1, 21–27. [Google Scholar]
- Henjum, S.; Manger, M.; Skeie, E.; Ulak, M.; Thorne-Lyman, A.L.; Chandyo, R.; Shrestha, P.S.; Locks, L.; Ulvik, R.J.; Fawzi, W.W.; et al. Iron deficiency is uncommon among lactating women in urban Nepal, despite a high risk of inadequate dietary iron intake. Br. J. Nutr. 2014, 112, 132–141. [Google Scholar] [CrossRef] [PubMed]
- WHO. World Health Organization. Anthro 2005, Beta Version, feb17th, 2006: Software for Assessing Growth and Development of the World’s Children. Geneva. 2006. Available online: http://www.Who.Int/childgrowth/software/en/ (accessed on 6 July 2014).
- WHO. Indicators for Assessing Infant and Young Child Feeding Practices: Conclusions of a Consensus Meeting Held 6–8 November 2007 in Washington D.C., USA; WHO: Geneva, Switzerland, 2007. [Google Scholar]
- Kelleher, B.P.; Walshe, K.G.; Scott, J.M.; O’Broln, S.D. Microbiological assay for vitamin B12 with use of a colistin-sulfate-resistant organism. Clin. Chem. 1987, 33, 52–54. [Google Scholar] [PubMed]
- O’Broin, S.; Kelleher, B. Microbiological assay on microtitre plates of folate in serum and red cells. J. Clin. Pathol. 1992, 45, 344–347. [Google Scholar] [CrossRef] [PubMed]
- BEVITAL. Assesments of Nutrinal Status by Vitamins Marker. Laboratoriebygget, 9 ETG Jonas Lies veg 875021 Bergen, Norway. Available online: http://www.bevital.no/ (accessed on 17 February 2015).
- Windelberg, A.; Arseth, O.; Kvalheim, G.; Ueland, P.M. Automated assay for the determination of methylmalonic acid, total homocysteine, and related amino acids in human serum or plasma by means of methylchloroformate derivatization and gas chromatography-mass spectrometry. Clin. Chem. 2005, 51, 2103–2109. [Google Scholar] [CrossRef] [PubMed]
- Midttun, O.; Hustad, S.; Ueland, P.M. Quantitative profiling of biomarkers related to B-vitamin status, tryptophan metabolism and inflammation in human plasma by liquid chromatography/tandem mass spectrometry. Rapid Commun. Mass Spectrom. 2009, 23, 1371–1379. [Google Scholar] [CrossRef] [PubMed]
- Midttun, O.; Ueland, P.M. Determination of vitamins A, D and E in a small volume of human plasma by a high-throughput method based on liquid chromatography/tandem mass spectrometry. Rapid Commun. Mass Spectrom. 2011, 25, 1942–1948. [Google Scholar] [CrossRef] [PubMed]
- WHO. Iron Deficiency Anemia. Assesment, Prevention and Control. A Guide for Programme Manager; WHO: Geneva, Switzerland, 2001. [Google Scholar]
- INACG (International Nutritional Anemia Consultative Group). Adjusting hemoglobin values in program surveys. In Inacg Secretariat ilsi Human Nutrition Institute One Thomas Circle, Ninth Floor Internet; INACG: Washington, DC, USA, 2002. [Google Scholar]
- De Benoist, B. Conclusions of a who technical consultation on folate and vitamin B12 deficiencies. Food Nutr. Bull. 2008, 29, S238–S244. [Google Scholar] [CrossRef]
- Morris, M.S.; Picciano, M.F.; Jacques, P.F.; Selhub, J. Plasma pyridoxal 5′-phosphate in the us population: The national health and nutrition examination survey, 2003–2004. Am. J. Clin. Nutr. 2008, 87, 1446–1454. [Google Scholar] [PubMed]
- Allen, L.; de Benoist, B.; Dary, O.; Hurrell, R. Guidelines on Food Fortification with Micronutrients-Who/Fao; World Health Organization: Geneva, Switzerland, 2006. [Google Scholar]
- WHO. Global prevalence of vitamin a deficiency in populations at risk, 1995–2005. In Who Global Database on Vitamin a Deficiency; WHO: Geneva, Switzerland, 2009. [Google Scholar]
- IOM (Institute of Medicine). Dietary Reference Intakes for Calcium and Vitamin D; The National Academy Press: Washington, DC, USA, 2011. [Google Scholar]
- Jiang, T.; Christian, P.; Khatry, S.K.; Wu, L.; West, K.P., Jr. Micronutrient deficiencies in early pregnancy are common, concurrent, and vary by season among rural Nepali pregnant women. J. Nutr. 2005, 135, 1106–1112. [Google Scholar] [PubMed]
- Thurnham, D.I.; Mburu, A.S.; Mwaniki, D.L.; De Wagt, A. Micronutrients in childhood and the influence of subclinical inflammation. Proc. Nutr. Soc. 2005, 64, 502–509. [Google Scholar] [CrossRef] [PubMed]
- Ulak, M.; Chandyo, R.K.; Mellander, L.; Shrestha, P.S.; Strand, T.A. Infant feeding practices in bhaktapur, Nepal: A cross-sectional, health facility based survey. Int. Breastfeed. J. 2012, 7, 1. [Google Scholar] [CrossRef] [PubMed]
- Schulze, K.J.; Christian, P.; Wu, L.S.; Arguello, M.; Cui, H.; Nanayakkara-Bind, A.; Stewart, C.P.; Khatry, S.K.; LeClerq, S.; West, K.P., Jr. Micronutrient deficiencies are common in 6- to 8-year-old children of rural Nepal, with prevalence estimates modestly affected by inflammation. J. Nutr. 2014, 144, 979–987. [Google Scholar] [CrossRef] [PubMed]
- Allen, L.H. Maternal micronutrient malnutrition: Effects on breast milk and infant nutrition, and priorities for intervention. SCN News 1994, 21–24. [Google Scholar]
- Gittelsohn, J.; Thapa, M.; Landman, L.T. Cultural factors, caloric intake and micronutrient sufficiency in rural Nepali households. Soc. Sci. Med. 1997, 44, 1739–1749. [Google Scholar] [CrossRef]
- Nguyen, A.M.; Grover, D.S.; Sun, K.; Raju, V.K.; Semba, R.D.; Schaumerg, D.A. Coverage of the vitamin A supplementation programme for child survival in Nepal: Success and challenges. Paediatr. Int. Child Health 2012, 32, 233–238. [Google Scholar] [CrossRef] [PubMed]
- Avagyan, D.; Neupane, S.P.; Gundersen, T.E.; Madar, A.A. Vitamin D status in pre-school children in rural Nepal. Public Health Nutr. 2016, 19, 470–476. [Google Scholar] [CrossRef] [PubMed]
- Friso, S.; Jacques, P.F.; Wilson, P.W.; Rosenberg, I.H.; Selhub, J. Low circulating vitamin B(6) is associated with elevation of the inflammation marker C-reactive protein independently of plasma homocysteine levels. Circulation 2001, 103, 2788–2791. [Google Scholar] [CrossRef] [PubMed]
- Morris, M.S.; Sakakeeny, L.; Jacques, P.F.; Picciano, M.F.; Selhub, J. Vitamin B-6 intake is inversely related to, and the requirement is affected by, inflammation status. J. Nutr. 2010, 140, 103–110. [Google Scholar] [CrossRef] [PubMed]
- Vasilaki, A.T.; McMillan, D.C.; Kinsella, J.; Duncan, A.; O’Reilly, D.S.; Talwar, D. Relation between pyridoxal and pyridoxal phosphate concentrations in plasma, red cells, and white cells in patients with critical illness. Am. J. Clin. Nutr. 2008, 88, 140–146. [Google Scholar] [PubMed]
- Joosien, E.; van den Berg, A.; Riezler, R.; Naurath, H.J.; Lindenbaum, J.; Stabler, S.P.; Allen, R.H. Metabolic evidence that deficiencies of vitamin B-12 (cobalamin), folate, and vitamin B-6 occur commonly in elderly people. Am. J. Clin. Nutr. 1993, 58, 468–476. [Google Scholar]
- Scott, J.M.; Weir, D.G. The methyl folate trap. A physiological response in man to prevent methyl group deficiency in kwashiorkor (methionine deficiency) and an explanation for folic-acid induced exacerbation of subacute combined degeneration in pernicious anaemia. Lancet 1981, 2, 337–340. [Google Scholar] [CrossRef]
- Henjum, S.; Torheim, L.E.; Thorne-Lyman, A.L.; Chandyo, R.; Fawzi, W.W.; Shrestha, P.S.; Strand, T.A. Low dietary diversity and micronutrient adequacy among lactating women in a peri-urban area of Nepal. Public Health Nutr. 2015, 18, 3201–3210. [Google Scholar] [CrossRef] [PubMed]
- Ulak, M.; Chandyo, R.K.; Adhikari, R.K.; Sharma, P.R.; Sommerfelt, H.; Refsum, H.; Strand, T.A. Cobalamin and folate status in 6 to 35 months old children presenting with acute diarrhea in bhaktapur, Nepal. PLoS ONE 2014, 9, e90079. [Google Scholar] [CrossRef] [PubMed]
- Taneja, S.; Strand, T.A.; Kumar, T.; Mahesh, M.; Mohan, S.; Manger, M.S.; Refsum, H.; Yajnik, C.S.; Bhandari, N. Folic acid and vitamin B-12 supplementation and common infections in 6–30-month-old children in india: A randomized placebo-controlled trial. Am. J. Clin. Nutr. 2013, 98, 731–737. [Google Scholar] [CrossRef] [PubMed]
- Hay, G.; Johnston, C.; Whitelaw, A.; Trygg, K.; Refsum, H. Folate and cobalamin status in relation to breastfeeding and weaning in healthy infants. Am. J. Clin. Nutr. 2008, 88, 105–114. [Google Scholar] [PubMed]
- Bjorke-Monsen, A.L.; Ueland, P.M. Cobalamin status in children. J. Inherit. Metab. Dis. 2011, 34, 111–119. [Google Scholar] [CrossRef] [PubMed]
- Siegel, E.H.; Stoltzfus, R.J.; Khatry, S.K.; Leclerq, S.C.; Katz, J.; Tielsch, J.M. Epidemiology of anemia among 4- to 17-month-old children living in south central Nepal. Eur. J. Clin. Nutr. 2006, 60, 228–235. [Google Scholar] [CrossRef] [PubMed]
- Chandyo, R.K.; Henjum, S.; Ulak, M.; Thorne-Lyman, A.L.; Ulvik, R.J.; Shrestha, P.S.; Locks, L.; Fawzi, W.; Strand, T.A. The prevalence of anemia and iron deficiency is more common in breastfed infants than their mothers in bhaktapur, Nepal. Eur. J. Clin. Nutr. 2015. [Google Scholar] [CrossRef] [PubMed]
- Martti, A.; Siimes, E.V.; Kuitunen, P. Breast milk iron—A declining concentration during the course of lactation. Acta Paediatr. 1979, 68, 29–31. [Google Scholar]
- Hoddinott, J.; Rosegrant, M.; Torero, M. Hunger and Malnutrition, Copenhagen Consesus; Copenhagen Consensus Center: Copenhagen, Denmark, 2012. [Google Scholar]
- Jefferds, M.E.; Mirkovic, K.R.; Subedi, G.R.; Mebrahtu, S.; Dahal, P.; Perrine, C.G. Predictors of micronutrient powder sachet coverage in Nepal. Mater. Child Nutr. 2015, 11, 77–89. [Google Scholar] [CrossRef] [PubMed]
| Definition | Indicators | Cut off |
|---|---|---|
| Anemia [29] | Hemoglobin (Hb) | <110 g/L |
| Altitude adjusted anemia [30] | Hb | <113g/L |
| Vitamin B12 deficiency [31] | Cobalamin | <150 pmol/L |
| Marginal vitamin B12 deficiency | Cobalamin | <200 pmol/L |
| Folate deficiency [31] | plasma folate | <10 nmol/L |
| Vitamin B6 deficiency [32,33] | pyridoxal 5′-phosphate | <20 nmol/L |
| Vitamin A deficiency [33,34] | trans retinol | <0.70 µmol/L |
| Marginal vitamin A deficiency [34] | trans retinol | <1.05 µmol/L |
| Vitamin D deficiency [35] | 25 hydroxyvitamin D (25(OH)D) | <50 nmol/L |
| Marginal Vitamin D deficiency | 25(OH)D | <75 nmol/L |
| Vitamin E deficiency [36] | α- tocopherol | <9.3 µmol/L |
| Marginal vitamin E deficiency | α- tocopherol | <18.9 µmol/L |
| Hyperhomocysteinemia [17] | Total homocysteine (tHcy) | >10 µmol/L |
| Hypermethylmalonic acidemia | Methylmalonic acid (MMA) | >0.28 µmol/L |
| Characteristics | % | Mean | SD |
|---|---|---|---|
| Age in months | 6.8 | 2.9 | |
| Age ≤6 months | 45 | ||
| First born child | 42 | ||
| Male child | 56 | ||
| Home delivery | 9 | ||
| Birth weight, gm * | 2891 | 492 | |
| Low birth weight (<2500 gm) | 13 | ||
| Demographic features: | |||
| Illiterate or up to grade 5 education of mother | 53 | ||
| Illiterate or up to grade 5 education of father | 5 | ||
| Not working mother | 65 | ||
| Mother age | 25.5 | 2.2 | |
| Family residing in rented house | 37 | ||
| Family staying in joint family | 51 | ||
| Family having own land | 54 | ||
| Breastfeeding status: | |||
| Exclusive breastfeeding for 3 months or more † | 51 | ||
| Exclusive breastfeeding for 6 months or more | 17 | ||
| Nutritional status: | |||
| Underweight (weight for age Z score ≤ 2) | 5 | ||
| Stunting (length for age Z score ≤ 2) | 9 | ||
| Wasting (weight for length Z score ≤ 2) | 2 | ||
| Hemoglobin, g/L | 107 | 12 | |
| Anemia (hemoglobin <110 g/L) | 59 | ||
| Anemia (hemoglobin <113 g/L) | 70 | ||
| Infection/inflammation: | |||
| C-reactive protein >5 mg/L ‡ | 20 |
| Mean/Centile | Vit A (µmol/L) | Vit D (nmol/L) | Vit E (µmol/L) | Vit B6 (nmol/L) | Vit B12 (pmol/L) | Folate (nmol/L) | tHcy (µmol/L) | MMA (µmol/L) |
|---|---|---|---|---|---|---|---|---|
| Mean (SD) | 0.96 (0.25) | 82 (21) | 20.6 (4.9) | 41.3 (35.8) | 260 (131) | 73 (35.0) | 12.5 (5.5) | 0.84 (0.88) |
| 5% | 0.58 | 52 | 12.3 | 13.7 | 104 | 24.7 | 6.4 | 0.19 |
| 25% | 0.79 | 67 | 17.6 | 20.8 | 165 | 45.3 | 8.6 | 0.33 |
| 50% | 0.95 | 80 | 20.3 | 31 | 232 | 66.9 | 11.2 | 0.55 |
| 75% | 1.1 | 93 | 23.6 | 47.4 | 321 | 96.8 | 14.6 | 1 |
| 95% | 1.3 | 145 | 27.4 | 74 | 442 | 129.7 | 19.4 | 1.8 |
| Vitamins | n | % below or above Cut-off | 95% CI |
|---|---|---|---|
| Vitamin A (trans retinol) | 68 | 15 | 11, 18 |
| Marginal vitamin A | 304 | 65 | 61, 69 |
| Vitamin D 25(OH)D | 17 | 3.6 | 1.9, 5.4 |
| Marginal vitamin D 25(OH)D | 191 | 41 | 36, 45 |
| Vitamin E (α-tocopherol) | 6 | 1.3 | 0.3, 2 |
| Marginal vitamin E | 137 | 36 | 31, 40 |
| Vitamin B6 (pyridoxal 5′ phosphate) | 101 | 22 | 18, 25 |
| Vitamin B12 (cobalamin) | 80 | 17 | 14, 20 |
| Marginal vitamin B12 (cobalamin) | 185 | 40 | 35, 44 |
| Folate | 0 | 0 | 0 |
| Hypermethylmalonic academia | 384 | 82 | 78, 85 |
| Hyperhomocysteinemia | 289 | 62 | 57, 66 |
| Vitamins | % | ||||||||
| Vitamin D | 0.9 | 2.3 | |||||||
| Marginal vit D | 5.3 | 25.9 | |||||||
| Vitamin E | 0.6 | 1.3 | 0 | 0.9 | |||||
| Marginal vit E | 7.7 | 24.6 | 3 | 17.5 | |||||
| Vitamin B6 | 4.3 | 4.3 | 2.3 | 10.2 | 0.4 | 11.3 | |||
| Vitamin B12 | 3 | 12.4 | 1.3 | 2.1 | 0 | 8.3 | 4.5 | ||
| Marginal vit B12 | 8.1 | 31.7 | 2 | 18.6 | 0.9 | 21.6 | 10.7 | ||
| Anemia | 8.8 | 40 | 2.3 | 24.8 | 0.6 | 22.7 | 14.5 | 11.1 | 31.2 |
| Deficiencies of | Vit A | Marg vit A | Vit D | Marg vit D | Vit E | Marg vit E | Vit B6 | Vit B12 | Marg vit B12 |
| 25(OH)D | α-Tocopherol | PLP | Cobalamin | Folate | MMA | tHcy | CRP | HB | Age | |
|---|---|---|---|---|---|---|---|---|---|---|
| Trans retinol | −0.03 p = 0.42 | 0.19 p < 0.0001 | 0.12 p < 0.007 | 0.10 p = 0.023 | −0.23 p < 0.0001 | 0.05 p = 0.2 | −0.18 p = 0.0001 | −0.3 p < 0.0001 | 0.12 p < 0.005 | 0.36 p < 0.0001 |
| 25(OH)D | 0.17 p = 0.0001 | 0.13 p = 0.005 | −0.05 p = 0.23 | 0.3 p < 0.0001 | −0.02 p = 0.54 | −0.07 p = 0.12 | −0.02 p = 0.7 | −0.05 p = 0.28 | −0.28 p < 0.0001 | |
| α-Tocopherol | 0.29 p < 0.0001 | 0.22 p < 0.0001 | 0.01 p = 0.79 | −0.08 p = 0.06 | −0.004 p = 0.92 | −0.05 p = 0.25 | 0.01 p = 0.10 | −0.21 p < 0.0001 | ||
| PLP | 0.10 p = 0.026 | 0.05 p = 0.23 | 0.03 p = 0.42 | −0.08 p = 0.06 | −0.21 p < 0.0001 | 0.22 p < 0.0001 | −0.21 p < 0.0001 | |||
| Cobalamin | −0.25 p < 0.0001 | −0.36 p < 0.0001 | −0.52 p < 0.0001 | 0.11 p = 0.01 | 0.12 p = 0.006 | 0.05 p = 0.21 | ||||
| NS = p-value > 0.05 | Folate | 0.15 p < 0.001 | 0.32 p < 0.0001 | 0.03 p = 0.41 | 0.03 p = 0.52 | −0.31 p < 0.0001 | ||||
| MMA = Methylmalonic acid | ||||||||||
| tHcy = Total homocysteine | MMA | 0.45 p < 0.001 | −0.13 p = 0.005 | −0.02 p = 0.66 | −0.07 p = 0.12 | |||||
| Hb = Hemoglobin | ||||||||||
| PLP = Pyridoxal 5′phosphate | tHcy | −0.04 p = 0.35 | −0.13 p < 0.001 | −0.21 p < 0.0001 | ||||||
| CRP | −0.04 p = 0.35 | 0.06 p = 0.14 | ||||||||
| Hb | −0.07 p = 0.09 | |||||||||
© 2016 by the authors; licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons by Attribution (CC-BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Ulak, M.; Chandyo, R.K.; Thorne-Lyman, A.L.; Henjum, S.; Ueland, P.M.; Midttun, Ø.; Shrestha, P.S.; Fawzi, W.W.; Graybill, L.; Strand, T.A. Vitamin Status among Breastfed Infants in Bhaktapur, Nepal. Nutrients 2016, 8, 149. https://doi.org/10.3390/nu8030149
Ulak M, Chandyo RK, Thorne-Lyman AL, Henjum S, Ueland PM, Midttun Ø, Shrestha PS, Fawzi WW, Graybill L, Strand TA. Vitamin Status among Breastfed Infants in Bhaktapur, Nepal. Nutrients. 2016; 8(3):149. https://doi.org/10.3390/nu8030149
Chicago/Turabian StyleUlak, Manjeswori, Ram K. Chandyo, Andrew L. Thorne-Lyman, Sigrun Henjum, Per M. Ueland, Øivind Midttun, Prakash S. Shrestha, Wafaie W. Fawzi, Lauren Graybill, and Tor A. Strand. 2016. "Vitamin Status among Breastfed Infants in Bhaktapur, Nepal" Nutrients 8, no. 3: 149. https://doi.org/10.3390/nu8030149
APA StyleUlak, M., Chandyo, R. K., Thorne-Lyman, A. L., Henjum, S., Ueland, P. M., Midttun, Ø., Shrestha, P. S., Fawzi, W. W., Graybill, L., & Strand, T. A. (2016). Vitamin Status among Breastfed Infants in Bhaktapur, Nepal. Nutrients, 8(3), 149. https://doi.org/10.3390/nu8030149





