Abstract
The DePEC-Nutrition trial is a complex dietary and behavioural intervention of salt intake reduction combined with increased high-nitrate vegetable consumption among Malaysian middle-aged and older adults with elevated blood pressure. This study aimed to assess the feasibility and acceptability of the trial. Participants were recruited from the South East Asia Community Observatory (SEACO) database and randomised into one of four groups: (1) low salt; (2) high-nitrate vegetable; (3) combined high-nitrate vegetable and low salt; and (4) control. The intervention included a combination of group counselling sessions, information booklets, reinforcement videos and text messages to modify dietary behaviour. The primary outcomes evaluated were the measures of feasibility and acceptability of (1) recruitment, follow-up attendance and retention; (2) data collection procedures and clinical outcome measures; and (3) individual and combined multi-modal dietary interventions. A total of 74 participants were recruited, and the 10-month retention rate was 73%. Data collection procedures were acceptable with minimal missing data. All intervention strategies were feasible and acceptable, with group counselling being the most acceptable strategy. This study provides important insights into improving the screening process of participants, facilitating their access to the research facilities and refining the measurement protocols and dietary recommendations, which are instrumental in formulating the design of a full-scale definitive DePEC-Nutrition trial.
1. Introduction
Dementia is a neurodegenerative disease characterised by a progressive and significant impairment of cognitive and physical function [1]. The pathogenesis of dementia is complex and linked to the multi-factorial contribution of metabolic and vascular changes, genetics and environmental factors, which occur alongside age-related changes in brain structure and function [2,3]. Globally, approximately 50 million people have dementia and this number is projected to triple by 2050, with 70% of dementia cases occurring in low- and middle-income countries (LMICs) [4].
A certain degree of overlap characterises the risk factor profiles of cardiovascular diseases (CVD) and dementia, and factors such as age, smoking, obesity, physical inactivity and depression are significant contributors to both conditions [5]. High blood pressure is an important modifiable risk factor for both CVD and dementia [6,7,8,9], and evidence from clinical trials has reported significant associations between decreased blood pressure, improved cognition, and reduced CVD [10,11] and dementia risk [12,13,14]. At the same time, interventions focused on dietary changes have been shown to have lowering effects on blood pressure and are also linked to a reduced risk of dementia. The Mediterranean diet and the Dietary Approach to Stop Hypertension (DASH) are examples of recognised healthy dietary patterns with strong evidence-based protective effects against both cardiovascular and dementia risk [15,16,17]. Sodium and inorganic nitrate (via the formation of nitric oxide (NO)) are two of the key protective nutrients with health-promoting properties via mechanisms involving the control of vascular tone, fluid balance and neurotransmission [18,19].
Observational studies have reported an association between a high inorganic nitrate intake with a reduced risk of coronary heart disease and cardiovascular mortality [20,21,22], and the effect was more prominent in younger age groups. In addition, 24-h urinary inorganic nitrate concentrations, measured as an objective marker of dietary nitrate intake, were indirectly associated with resting systolic blood pressure among older Italian subjects recruited as part of the InChianti cohort [23]. Several clinical trials have also reported the blood pressure lowering effects of dietary nitrate supplementation [24,25,26,27,28,29,30], and the effect size of interventions on systolic and diastolic blood pressure have been summarised in a recent meta-analysis [31]. Research has demonstrated that consuming foods rich in inorganic nitrate increases NO production [29,32] and has positive effects on brain function [33]. In particular, improvements in cognitive function (executive function) and motor skills following dietary nitrate supplementation have been observed, which appears to be mediated by augmented cerebral blood flow and the efficiency of neuronal cellular metabolism [34,35]. The modification of dietary nitrate intake is, therefore, a potential target for reducing dementia risk in a high-risk population with elevated blood pressure.
Observational studies have consistently shown significant associations between high sodium intake and increased blood pressure [36,37], which have been confirmed in several clinical trials reporting the lowering effects of low salt diets on blood pressure [38,39]. A recent meta-analysis reported a significant association between blood pressure reduction and a lower risk of cognitive impairment and incident dementia [40]. However, a small number of epidemiological studies have observed mixed associations between sodium intake and cognitive performance in older adults [41,42,43,44,45].
There are currently limited data on effective multi-modal dietary and lifestyle interventions that prevent cognitive decline and dementia in LMICs [46]. The DePEC (Dementia Prevention and Enhanced Care)-Nutrition trial is a complex dietary and behavioural intervention evaluating the feasibility of the combination of salt intake reduction and increased high-nitrate vegetable consumption among middle-aged and older Malaysian adults with elevated blood pressure [47]. This trial was designed according to the Medical Research Council (MRC) guidelines for developing and evaluating complex interventions. The guidelines highlight the importance of practical and methodological difficulties in such interventions, which need to be identified through feasibility testing before evaluating the efficacy of full-scale definitive interventions [48]. The present study aimed to assess (1) the feasibility of screening, recruitment, follow-up and retention rate, (2) the suitability and acceptability of data collection procedures and clinical outcome measures within the DePEC-Nutrition trial, and (3) the feasibility and acceptability of long-term (>6 months) individual and combined multi-modal dietary interventions aimed at modifying dietary nitrate (increase) and sodium (decrease) intake in middle-aged and older Malaysian adults with elevated blood pressure.
2. Materials and Methods
2.1. Study Design
The DePEC-Nutrition trial was a randomised, controlled 2 × 2 factorial nutritional intervention conducted between June 2019 and December 2020. This study was approved by the Monash University Human Research Committee (Project ID: 17864) and the Malaysian Medical Research Ethics Committee (NMRR-19-617-45916), and was registered with the clinical trial registry (ISRCTN47562685). Detailed information on the study design and visits can be found elsewhere [47].
2.2. Participants and Recruitment
Potential participants were identified from the South East Asia Community Observatory (SEACO) database: a health and demographic surveillance site (HDSS) within a middle-income community in Segamat, Johor, Malaysia. The following eligibility criteria were applied: (1) aged 50–75 years; (2) resided within a 5 km radius of the study site, Health Clinic Sungai Segamat; (3) systolic blood pressure of 120–159 mmHg or diastolic blood pressure 80–99 mmHg or diagnosed hypertensive; and (4) Body Mass Index (BMI) > 18.5 kg/m2. A list of participants who matched these eligibility criteria was generated from the database. Participants were randomly selected and approached via a telephone call or home visit to arrange a screening visit to confirm their eligibility. If they agreed to participate in the study, a home screening visit was arranged. The detailed study inclusion and exclusion criteria are listed in Table A1 in Appendix A.
During the screening visit, participants first signed an informed consent form for participation. Information on demographics, comorbidities, medication use and history, cognitive function (Mini-Mental State Examination, MMSE) [49], body weight, height and resting blood pressure were collected. Eligible participants were then invited to take part in the study, and a baseline assessment visit was arranged. If participants declined to take part in the study, they were asked for a specific reason for not participating.
2.3. Dietary Interventions
Participants were randomised into one of four groups in a factorial design: (1) low salt consumption; (2) high-nitrate vegetable consumption; (3) combined high-nitrate vegetable consumption plus low salt consumption; or (4) a control group. Participants allocated to the intervention groups received the DePEC-Nutrition intervention, which consisted of the five strategies outlined below. All intervention strategies were delivered in the participants’ preferred language (English/Malay/Chinese), except for group nutritional counselling, which was offered in Malay. A copy of the intervention resources is available in the Online Supplementary Material.
- Group nutritional counselling was delivered during the baseline clinic visit by a trained medical officer using PowerPoint slides and practical activities. Each session lasted between 1–1.5 hours. The topics addressed at the counselling session included health benefits, sources, recommended intakes and practical tips related to the allocated intervention of increasing dietary nitrate and/or reducing salt intake. Participants in the low salt group were advised to consume less than 5 g of salt in accordance with the recommendations from the World Health Organization (WHO) [50]. Advice was delivered on how to reduce salt intake during home cooking, eating out and shopping for food (reading food labels). Participants in the high-nitrate groups were recommended to consume vegetables rich in dietary nitrate at least three times per week or more to achieve an intake of approximately 1000–1500 mg of dietary nitrate per week. A list of commonly consumed nitrate-rich vegetables (i.e., broccoli, cabbage, spinach, cauliflower, lettuce and eggplant) was provided in the information booklet, along with the recommended portion size. In addition, practical tips for increasing dietary nitrate intake and retaining the nitrate content in the vegetables when cooking were also provided.
- Information booklets were provided during the group counselling sessions. In addition to the detailed information discussed during the sessions, the booklet contained recipes of low salt and/or high-nitrate meals that participants could prepare at home. The booklet also provided several sources and links for further information.
- A salt measuring spoon (Atila GmbH, Neidenstein, Germany, see the picture in the Online Supplementary Material) was provided to the participants who were randomised into the salt interventions (low salt and combined high-nitrate vegetable plus low salt consumption groups) to support them in understanding portion sizes and measuring salt intake. The measuring spoon had a dual side with nine adjustable scales (0.5, 1, 2, 3.5, 5, 7, 9, 11 and 13 g). Participants were taught how to use the spoon during the group counselling sessions.
- Biweekly text messages were sent to all participants in the intervention groups. The text messages included educational messages and reminders of the key dietary behaviour changes to encourage adherence.
- Reinforcement video messages were delivered to the participants in the intervention groups at the interim visits to remind participants of the key dietary advice that was discussed during the baseline counselling sessions. The reinforcement videos were hosted on the YouTube platform and only viewable to those who had access to the video link. Video clip links were sent to the participants via WhatsApp (WhatsApp Inc., Mountain View, CA, USA).
Participants in the control group were provided with an information booklet during their baseline clinic visit. The booklet contained the Malaysian Food Pyramid and 11 key messages on healthy eating and lifestyle recommendations derived from Malaysian dietary guidelines [51]. Participants were reinforced with similar key messages via the WhatsApp application during the interim 3 visit (8 months) of the study.
2.4. Randomisation
The randomisation of individual participants into a particular trial group was undertaken once they passed the screening visit and confirmed their participation in the trial. A block randomisation method with a block size of four was performed. A block randomisation list was generated using R software (randomizeR) [52] by a member of the research team who was not involved in data collection.
2.5. Study Procedures
Baseline assessments were conducted in person over two visits (first at the participant’s home and then at the health clinic) and within two days. During the home visit, the data collectors explained the study procedures and obtained written informed consent for participation in the trial. Participants were asked about any newly diagnosed diseases and prescriptions or changes in their medication following their last visit during screening to further confirm their eligibility. Eligible participants were then provided with instructions and containers to collect 24-h urine samples and return them when attending the clinic visit. Participants attended the clinic visit in the morning between 8 a.m. and 10 a.m., and they were asked to refrain from strenuous exercise and from consuming stimulating substances (i.e., coffee, tea). A number of assessments were conducted, including resting blood pressure, body composition, 24-h dietary recall, Food Frequency Questionnaire (FFQ) and the collection of biological samples (blood, dried blood spot, saliva, salivary strips and spot urine samples). Detailed information on these assessment methods has been published elsewhere [47].
At interim 1 (2 months), reinforcement messages were provided to participants in the intervention groups to enhance compliance with the intervention. Adherence questionnaires were administered at the same time. At the interim 2 visit (4 months), another set of reinforcement messages was sent to the intervention groups, while adherence questionnaires were administered to all participants, including those in the control group. In addition, at the interim 3 visits (8 months), all participants were provided with videos messages to reinforce the key dietary messages for their respective interventions. A feedback questionnaire was administered at the end of the study to obtain detailed feedback on the overall study process.
2.6. Outcomes
The primary outcomes were to evaluate the feasibility of the recruitment, follow-up, retention, data collection procedures, clinical outcome measures and interventions to inform the design and delivery of a full-scale DePEC-Nutrition trial. Secondary outcomes included clinical and nutritional measures: blood pressure; Montreal Cognitive Assessment (MoCA) test; auditory verbal learning test (AVLT); 24-h recall; Food Frequency Questionnaire (FFQ); and nitrate concentrations in urine, saliva and blood samples. The Bahasa Malay version of the MoCA (intra-class correlation coefficient = 0.81) [53] and AVLT (factor loading 0.66 to 0.98) [54] have been previously validated among the Malaysian population. In addition, the FFQ is widely used in the Malaysian Adult Nutrition Survey (MANS) 2014 [55]. These are key for informing the calculation of sample size and recruitment strategies in the definitive DePEC-Nutrition RCT. A mixed-method approach was used, including quantitative measures of feasibility, acceptability and clinical outcomes and a qualitative evaluation of the experience of the study participants and data collectors. A detailed description of the outcome measurements is provided in Table A2 in Appendix A. The primary outcomes were measured at three time points: interim 1 (2 months); interim 2 (4 months); and end of study (6 month). Self-rated acceptability data collection procedures and the usefulness of the interventions strategies and materials were assessed using a questionnaire developed and pre-tested by the research team. The questionnaire included a mixture of open-ended and close-ended questions. A copy of the questionnaire is available in the Online Supplementary Material.
2.7. Protocol Changes Implemented during the COVID-19 Outbreak
The baseline assessment started in November 2019. In March, when the coronavirus disease 2019 (COVID-19) was declared as a global pandemic by the World Health Organization, this trial was in the baseline assessment and interim 1 stage (for some of the participants). By 13 March 2020, two days before the Malaysian government announced a movement restriction order, a total of 97 participants had consented to participate, 74 participants had completed the baseline assessment, and 18 participants had completed the interim 1 assessment. To allow the continuity of this trial during COVID-19, the original DePEC-Nutrition trial’s protocol was adapted, as follows:
- Methodology of data collectionThe data collection at interim 1, interim 2 and the end of study visits was initially planned to be conducted in person at the participant’s home. However, due to the COVID-19 outbreak, the need for social distancing and the movement restriction imposed by the Malaysian government, data collection by home visit was not possible. Hence, to continue the study during the COVID-19 pandemic, the data collection at interim 1, 2 and the end of study visits were conducted via telephone interview. The collection of information related to the primary outcomes of evaluating the acceptability and feasibility of the intervention was prioritised. The measurement of the secondary outcomes (i.e., physical assessment and biological samples) was not performed.
- TimeframeInitially, the planned duration of the DePEC-Nutrition feasibility study was six months, with interim 1 in the second month and interim 2 in the fourth month after the baseline. The shift from face-to-face data collection to telephone-based data collection required an extension of the study in order to implement the necessary changes to the protocol, including (1) obtaining approval from the ethics committee, SEACO and Monash University Malaysia on the amendment of the study protocol, (2) the development of the telephone-based data collection protocol, including the adaptation of the questionnaires, and (3) the re-training of the data collectors. Therefore, the total duration of the study was extended to 10 months and an additional interim 3 was added at month eight.
- Intervention deliveryThe reinforcement was originally planned to be delivered by the data collectors during the interim 1 and 2 visits. Due to the COVID-19 outbreak and the need for social distancing, video reinforcements were instead sent to each participant through WhatsApp. Participants without a mobile phone number were informed of the video content by the data collectors or had their close relative receive the video message on their behalf. In addition, the videos were also copied onto a compact disc and posted to participants who did not have access to a mobile phone. The reinforcement video included a comprehensive review of the key dietary messages delivered through nutritional counselling at the start of the study and provided specific information on adapting and making dietary changes during the pandemic.
2.8. Sample Size
The initial recruitment target was 30 participants per group. With a dropout rate of ≤20%, it was expected that more than 100 participants would complete the trial. This pragmatic sample size was based on guidelines by Whitehead et al. (2016) [56], which indicate that a sample size of greater than 25 individuals per group would provide a 90% power to detect a small effect size ranging between 0.1 and 0.3 for changes in blood pressure.
2.9. Data Presentation and Statistical Analysis
Continuous data were checked for normality using the Shapiro–Wilk test and skewness z-score [57]. The mean and standard deviation (SD) were presented for normally distributed variables, whereas the median and interquartile range (IQR) were presented for skewed variables. Categorical variables were reported as frequency and proportions. One-way ANOVA or Kruskal–Wallis tests were used to compare baseline characteristics between intervention groups. Categorical variables were analysed by Chi-squared or Fisher’s exact tests. Screening, eligibility, consent, retention, completion and missing data rates were described as numbers and proportions. Reasons for non-participation, non-responses and the acceptability of study visits were described in a narrative format. The acceptability of the reduced salt and high-nitrate vegetable consumption interventions was tested by contrasting two a priori factors based on the 2 × 2 factorial design: (1) a low salt factor (low salt consumption and combined high-nitrate vegetable plus low salt consumption) vs. no low salt (high-nitrate vegetable consumption and control groups) and (2) a high nitrate factor (high-nitrate vegetable and combined high-nitrate vegetable consumption plus low salt groups) vs. non-nitrate (low salt and control groups). All statistical analyses were performed using SPSS version 26.0 (SPSS Inc., Chicago, IL, USA). Statistical significance was set at p < 0.05.
3. Results
3.1. Recruitment, Follow-Up Response and Retention
3.1.1. Recruitment
Figure 1 shows the flow of the participants through the trial. Of the 699 potential participants who were screened, 225 (32.2%) participants were considered eligible. The major reasons for ineligibility were: medication use (31.6%, 150/474); acute or chronic medical condition (15.6%, 74/474); and insulin therapy (10.8%, 51/474) (Supplementary Material, Table S1). Of the 225 eligible participants, 97 (43%, 97/225) consented to participate in the study, almost a quarter (51/225, 23%) were unable to arrange the baseline assessment and about a quarter (26%, 58/225) of participants did not agree to participate. The major reasons for not agreeing to participate included: (1) lack of interest in the study (62%, 36/58); (2) not a suitable time (14%, 8/58); and (3) the study visits were too frequent (12%, 7/58) (Supplementary Material, Table S2). The proportion of participants agreeing to participate was significantly lower for Malay participants compared to Chinese participants (57.3% vs. 78.4%, p = 0.031), single vs. married (45.7% vs. 67.5%, p = 0.019) and alcohol consumers compared to non-alcohol consumers (100% vs. 60%, p = 0.014) (Supplementary Material, Table S3).
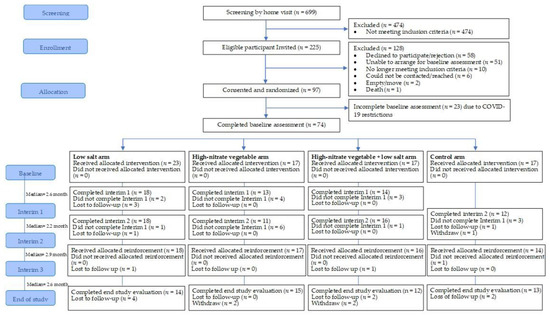
Figure 1.
The flow of participants through the pilot study.
The baseline assessments and recruitment were stopped due to restrictions imposed by COVID-19, and therefore, reaching the target sample size (n = 120) was not possible. Of the consenting participants, 74 were recruited and completed the baseline assessment within the restricted time frame (26 November 2019 to 13 March 2020). Additional logistic challenges related to scheduling baseline visits, included (1) difficulties in contacting potential participants, (2) the burden of research phone calls, and (3) work commitments or child-minding duties.
3.1.2. Follow-Up Response Rate and Retention
The overall follow-up attendance rate for interim 1 and interim 2 were 79% (45/57) and 77% (57/74), respectively. There were no related or unexpected adverse events reported. The median intervention period was 10.5 months (Range = 9.4–11.7 months). At the end of the study, 54 of the 74 participants completed the end study evaluation and the overall retention rate was 73%. There was no evidence that the retention rate differed between the study groups (low salt: 61% (14/23); high-nitrate vegetable: 88% (15/17); combined high-nitrate vegetable plus low salt: 71% (12/17); and control: 76% (13/17); Fisher’s exact p-value = 0.291). A total of 20 participants (27%) dropped out of the study and reasons included being uncontactable (n = 10), no longer being interested in the study (n = 5), work or childcare commitments (n = 4) and moving out of the study location (n = 1). Participants retained until the end of the study had higher MMSE (p = 0.022) and MoCA scores (p = 0.023) than participants who dropped out (Supplementary Material, Table S3).
3.1.3. Characteristics of Study Participants
A total of 74 participants were enrolled in the DePEC-Nutrition study and randomised into one of the four intervention groups: low salt group (n = 23); high-nitrate vegetable group (n = 17); high-nitrate vegetable and low salt group (n = 17); and control group (n = 17). The baseline characteristics of the study participants are presented in Table 1. The mean ± SD age of participants was 61.6 ± 6.7 years. About half of the participants worked full-time (35.1%) or part-time (12.2%). Almost half of the participants (48.6%) had secondary education, and the mean MoCA score was 20.8 ± 4.0. All characteristics were similar between the intervention and control groups. Based on 24-h dietary recall data, the baseline median total energy and sodium intake was 1797 (Q1–Q3: 1229–2477) kcal/day and 2777 (Q1–Q3: 1813–4330) mg/day, respectively. An analysis of the FFQ baseline data showed that the median frequency of intake for green leafy vegetables was 3.0 (Q1–Q3: 1.0–7.0) times per week, with 37.5% (27/72) of the participants consuming green leafy vegetables daily.

Table 1.
The baseline characteristics of the participants.
3.2. Suitability and Acceptability of Data Collection Procedures and Outcomes Measures
3.2.1. Study Visits
Data collectors considered home visits appropriate and safe. Similarly, the majority of participants reported that the number (90.7%, 49/54) and duration of the visits (84.9%, 45/53) were appropriate and convenient (96.2%, 50/52) (Table 2). Six participants (6/53, 11.3%) mentioned that the duration of the clinic visits was long for them and their dependents. Similarly, five of the data collectors mentioned that the duration of the home and clinic visits ranged from 30 to 120 min and in some instances, this was too long. In addition, five of the data collectors felt that clinics were not a suitable setting for data collection because the clinic was crowded and the process may have been uncomfortable for the participants. In addition, assessments were performed in different rooms within the clinic and participants were required to frequently move to the different stations.

Table 2.
The quantitative and qualitative results regarding the acceptability of screening and recruitment.
3.2.2. Questionnaire
At baseline, most clinical outcome measures were completed by the participants without significant difficulty apart from the Trail Making B test, which was not completed by 10 illiterate participants who could not recognise alphabets (n = 6) or had difficulties understanding the instructions (n = 4). Data collectors also indicated that the duration of baseline assessments may have been too long and that this may have been stressful for some participants (Supplementary Material, Table S4).
Overall, 43 (58%, 43/74) participants provided a complete set of follow-up and end of study data, and 65 (88%, 65/74) provided at least either follow-up (interim) data or end of study data. Participants answered the majority of the questions with very little missing data (<5%). However, data collectors indicated that it was challenging to explain the questions to participants over the phone.
“Phone interviews were quite challenging when the respondent can’t imagine or even understand the score and questions given as the choice of the answer was confusing”.(Data collector 3)
3.2.3. Biological Sample Collection and Physical Measurements
During the baseline assessment, most of the participants (96%, 71/74) provided blood sample, dried blood spot sample, saliva sample, 24-h urine, spot urine samples, blood pressure and anthropometry data. Specifically, 61 participants provided complete dried blood spots while 64 collected complete matched 24-h and spot urine samples according to the predefined criteria. Overall, the anthropometry and blood pressure measurement and blood collection procedures were acceptable for most of the participants (Figure 2). Similarly, the data collectors found that the methods for collecting blood pressure, anthropometry data and biological samples (blood samples, dried blood spot sample, 24-h urine, spot urine) were easy. About 30% of participants indicated that providing the saliva sample was difficult, which was also reflected in the feedback provided by the data collectors.
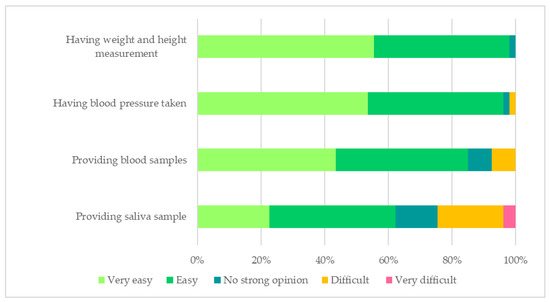
Figure 2.
The acceptability of the baseline assessments. Missing information: providing blood samples (n = 1); providing saliva sample (n = 1).
3.3. Feasibility and Acceptability of Various Nutrition Education Strategies
All participants allocated to the three interventions groups (100%, 47/47) attended the group counselling sessions (Table 3). More participants read the text messages (80%, 33/41) and watched the video (85%, 35/41) than read the information booklet (69%, 31/45). Participants who did not have access to messaging services received the reinforcement via a telephone call (Interim 1: n = 4; Interim 2: n = 11; and Interim 3: n = 7) or a compact disc with the video was sent via post (Interim 3: n = 2). Half of the participants from the intervention groups (51%, 21/41) claimed that they tried the recipes in the booklet provided. About one third (37%, 15/41) claimed that they accessed additional material suggested in the further reading section.

Table 3.
Summary of feasibility and acceptability of the intervention strategies.
The majority of participants indicated the usefulness of the group counselling (90%, 37/41), text messages (94%, 31/33), videos (94%, 33/35) and the information booklet (89%, 47/53) (Figure 3). While most participants agreed that the information booklet was easy to understand (83%, 44/53), relevant (89%, 47/53) and culturally appropriate (83%, 44/53), a small proportion thought that the information in the booklet was moderately useful (11%, 6/53), difficult or very difficult to understand (6%, 3/53), irrelevant (2%, 1/53) and culturally inappropriate (2%, 1/53). Those who rated the information in the booklet as moderately useful and irrelevant were from the high-nitrate vegetable (n = 5) or high-nitrate vegetable plus low salt groups (n = 1). This is consistent with the qualitative data, in which two Chinese participants from the high-nitrate vegetable group mentioned that the booklet contained mostly recipes tailored for the Malay community.
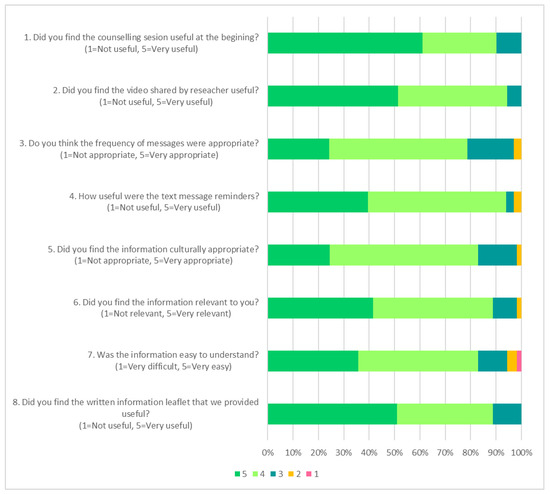
Figure 3.
The acceptability and suitability of the intervention materials. The response rate for each question was: 1 (n = 41/41); 2 (35/41); 3 (33/41); 4 (33/41); 5 to 8 (53/54). Question 1 to 4 was only applicable to the intervention groups (n = 41) and responded to by those engaged with the intervention strategies.
Overall, a significant number of participants mentioned the usefulness of the group counselling sessions, text messages and the information booklet for providing information and knowledge and serving as a reminder to them to comply with the relevant intervention. Several participants felt positive about the group counselling sessions because the face-to-face counselling enabled them to engage with doctors (n = 4). Participants highlighted that the session was convincing and that they were confident in the messages delivered as the counselling was conducted by a doctor (n = 2). On the other hand, the delivery of text messages and reinforcement videos was indicated as poor by the data collectors. The participants were incompetent and uncomfortable with the use of the text messenger and WhatsApp applications.
3.4. Acceptability of Low Salt and High-Nitrate Vegetable Intervention
Forty participants were randomised into the low salt interventions (low salt group n = 23; combined high-nitrate vegetable consumption plus low salt group n = 17), and the low salt acceptability data assessed at the end of the study were available for 26 participants. Most participants (81%, 21/26) found that changing to a low salt diet was either acceptable or very acceptable, and more than half of the participants (62%, 16/26) rated food with less salt as tasting either good or very good (Figure 4). Twenty participants in the low salt intervention (77%, 20/26) said they had used the salt measuring spoon and reported that it was rather easy to use (Supplementary Material, Table S5).
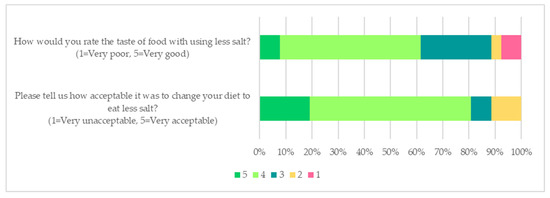
Figure 4.
The self-rated acceptability of low salt diet.
The reasons provided by six participants for not using the measuring spoon provided were related to: (1) personal preference, they were more comfortable in using their own measurement spoon as they claimed it to be more convenient and easier to keep; (2) family’s food habits, where the participant was either not the one who cooked in the household or meals were prepared according to the family’s palate; and (3) the perceived lack of benefit, where the participant did not see any use for the spoon.
Overall, the low salt and high-nitrate vegetable interventions were well accepted by the participants and all participants indicated that they would continue to follow the dietary recommendations. Most participants (80%, 33/41) indicated that they would recommend similar interventions to their family and friends.
4. Discussion
The current study was designed to examine the feasibility and acceptability of the recruitment, retention, data collection procedures, outcomes measures and intervention strategies of a dietary and behaviour intervention to reduce salt and increase high-nitrate vegetable intake. The high number of participants who were screened (n = 699) in a short time (about four months) demonstrated the advantage of using the SEACO database to identify and recruit potential participants. Whilst we met more than 60% (74/120) of our target sample size of 120 participants, recruitment ended prematurely as a result of the COVID-19 pandemic. The sample size of 74 would have provided the power of around 80% to detect a small effect size between 0.1 and 0.3 [56] if the trial had not been impacted by the COVID-19 pandemic. Other obstacles were related to logistical challenges, such as the scheduling of the baseline assessment visits, and participants’ barriers, including lack of interest, work commitments or child-minding duties. Similar factors affecting the enrolment of older participants in dementia research have been reported [58,59,60].
The challenges relating to scheduling baseline assessments and barriers to participation could be solved by adopting more efficient recruitment methods and study procedures. Previous studies have demonstrated that conducting recruitment at a convenient location (own home or easy to reach location) can enhance recruitment [58,61]. We have shown in this feasibility study that using a face-to-face home visit as a method to invite study participants is a successful approach for recruitment and we believe this represented one of the crucial factors in motivating an individual’s participation in the study. Whilst there is no “gold standard” recruitment method, researchers are encouraged to develop tailored and study-specific frameworks to optimise recruitment strategies through the monitoring of recruitment flow and the implementation of appropriate adaptations [62].
The original study duration was extended to approximately ten months in order to account for the COVID-19 restrictions in Malaysia, and despite the significant extension, the follow-up attendance and retention rate was over 70%. This result could be attributed to the trial being embedded within SEACO’s health and demographic surveillance site. A good relationship established between SEACO data collectors and the local community through community engagement certainly facilitated the recruitment and retention of the study. Our findings support previous studies that have found the benefit of community engagement [63] in increasing the participation in Alzheimer’s disease prevention trials [64,65]. The majority of the participants indicated that they enjoyed being part of the study and wanted to keep up to date on health- and nutrition-related information. A considerable number of dropouts were not contactable, and we do not have sufficient evidence to suggest that the change in the trial protocol might have affected the retention or that the dropouts were due to difficulties in conducting follow-up appointments through telephone calls. However, our findings warrant further work to analyse the feasibility and barriers of telephone-based data collection among these groups of participants. Other reasons (no longer interested or other commitments) might have been related to time constraints or the lack of motivation.
Evidence from previous studies supports the effectiveness of nutrition education in improving nutrition knowledge [66], diet and health in older adults [61,62,67,68]. Nutrition counselling is a vital strategy for imparting nutrition education to older adults, especially among illiterate individuals [69,70]. Consistent with other studies, we showed that group counselling was the best strategy to engage with participants. The group counselling enabled a two-way conversation between the participants and medical officers, which was considered a vital component to enhancing motivation and active participation. This could be further improved by adding more infographic materials and hands-on activities in the group counselling session.
Previous studies have shown the acceptability and use of text message reminders in improving adherence for the treatment of high blood pressure [71] and health-related behaviour among hypertensive patients [72] in LMICs. In our study, the text message was also found to be a helpful reminder, a source of information and a follow-up by the majority of participants who claimed to have read the text messages. However, the utility of the text message reminders and video messages might have been affected by the limited knowledge of some participants in the use of mobile apps. A recent feasibility study conducted among community-dwelling older Malaysians has also reported the modest acceptability and retention of information delivered via electronic media [73]. Older adults may be unfamiliar with the latest electronic devices and their facets, and they often rely on younger family members to explain and access the devices. Therefore, future studies should consider the addition of training sessions on the use of technology and communication devices in order to enhance retention and engagement with the study protocol.
This study provided learning points that are useful for informing and refining future study procedures, clinical outcomes measures, intervention materials and delivery. Key actions emerging from the study findings include a review of the screening eligibility criteria for the selection of participants using the SEACO health database to ensure screening and recruitment are efficient.
The recruitment of older participants in research trials has been acknowledged as one of the common challenges encountered in many studies [58,74]. These barriers may be related to selective eligibility criteria that may exclude participants based on the presence of comorbidities, medication use and limited mobility, which are common features in this age group [58]. Similar challenges were also encountered in this study and were one of the primary reasons for ineligibility. Specifically, participants prescribed with sodium-altering and psychiatric drugs and hormonal therapies and those diagnosed with acute and chronic medical conditions were excluded as these may have affected the outcomes of the study. In future studies, the efficiency of recruitment could be improved by applying broader selection criteria, if possible.
The comparison of the socio-demographic and health-related characteristics of the participants, included vs. excluded, is not only important for improving recruitment in future studies but also for having a significant impact on the generalisability of the study findings [59]. A careful analysis of the characteristics linked with a non-response is key to designing future screening strategies. For example, we observed that excluded participants and dropouts had lower MMSE and MoCA scores. This is consistent with a previous study by Sano et al. [75], which found that those who abandoned their Alzheimer’s Disease Cooperative Study Home-Based Assessment (HBA) trial had similarly lower MMSE scores. We also observed that Malay and single participants were less likely to take part in the study. A further assessment of the barriers, motivational drivers and health-related factors is needed to inform the recruitment strategies of trials recruiting older participants.
An additional consideration emerging from the results is related to the location of the study visits and, specifically, whether visits conducted in a clinical setting would be more appropriate and well-received by participants compared to those conducted in a non-clinical environment, such as the SEACO office space. Our findings indicated several challenges faced by the research team in scheduling the baseline clinic visits. For example, visits could only be scheduled during office hours and weekdays while some of the participants were only available during weekends. Hence, we conducted some of the visits at the SEACO office during weekends to increase the number of participants, which was further improved when we fully shifted the baseline assessments to the SEACO office in order to try to increase our recruitment efforts following the start of the pandemic. These findings suggest that having flexibility in scheduling the visits both in relation to the time and location of the visits could confer great advantages in trying to match study milestones with the preferences of older participants.
Future studies should also aim to prioritise the measurement of essential outcomes to reduce the burden on participants. All of the outcome measures in this study have been commonly applied in older adults, including validated cognitive assessment tools, health and lifestyle questionnaires and functional performance tests. The baseline assessment visits were time-consuming (~60 min), but all participants were able to complete the assessments. The measurement protocols were largely feasible with minimal missing data, with the exception of the Trail Making B test as illiterate participants could not read English letters. The challenges in performing the Trail Making B test with participants with a low education have been reported previously, particularly in non-native English speakers [76,77]. Future trials should carefully select cognitive testing tools, especially in less-educated participants, and a rational selection of the outcome measures is needed to limit the burden to participants.
Finally, our findings indicated that a revision of the information material provided to participants is warranted in a future study. The use of written educational material is often adopted to support and enhance nutritional counselling. In the present study, the information booklet was not consulted by some participants. The primary reasons for not checking the booklet were difficulties with reading the text (n = 2), no time to read (n = 1) and misplacement and inability to find the information booklet (n = 5). The limited engagement was also reflected by the number of participants (51%) who tried the recipes or accessed the additional material suggested in the booklet (37%). Participants who expressed dissatisfaction (not useful, difficult to understand and irrelevant) or neutral opinions about the information booklet were among those that misplaced the information booklet or did not read the booklet. This may indicate that some of the content of the booklet may have been difficult to understand, leading to a loss of interest in reading the material. We also found that the majority of the criticisms were from the high-nitrate vegetable group. Specifically, the recipes were criticised for being culturally inappropriate for the Chinese population. This important finding is in agreement with previous research suggesting that the cultural background of older adults may affect their perception of food and that traditions may also act as barriers to the adoption of healthier nutrition behaviours [78]. Potential modifications that may improve the material presented in the booklet include (1) increasing the font size of the text, (2) refining the information and recipes to ensure that the content is tailored for a range of ethnicities and (3) incorporating more images and illustrations to facilitate the understanding of the health messages.
Quantitative and qualitative data collected from both participants and data collectors provided useful learning points to inform the design of a full-scale DePEC-Nutrition trial. Various strategies were adopted in the DePEC-Nutrition trial, including group counselling, an information booklet, text messages and video messages. The findings provided valuable insights into the type of strategies that may be more feasible and acceptable and suggested key modifications to improve the feasibility and acceptability of future strategies among this target group. Limitations included not being able to conduct a full pilot study as planned due to the COVID-19 pandemic and the consequently imposed movement restrictions. While these unprecedented conditions certainly limited our ability to establish the full feasibility of the study, particularly in relation to the measurement of quantitative outcomes, the data clearly demonstrated the feasibility of the study protocols and dietary interventions. We suggest that the definitive DePEC-Nutrition trial should employ a mixed-method approach to deliver the interventions with sessions organised both live and remotely through a telephone or other digital platforms.
5. Conclusions
This study successfully demonstrated the feasibility and acceptability of a combined multi-modal dietary intervention aimed at modifying dietary nitrate (increase) and sodium (decrease) intake in middle-aged and older Malaysian adults with elevated blood pressure. The interventions were well-received with a satisfying completion rate and minimal missing data for the outcome measures. The present study identified some useful learning points to inform the refinements of the study procedure, clinical outcomes selection and measurements and the amendment of the intervention materials for a design and delivery of a full-scale DePEC feasibility and RCT.
Supplementary Materials
The following are available online at https://www.mdpi.com/article/10.3390/nu14030430/s1: Table S1, reasons for exclusion from the study (n = 474); Table S2, reasons for the rejection of study participation (n = 58); Table S3, the characteristics of consented and rejected to participate in the DePEC intervention; Table S4, a summary table of the data collector feedback on data collection; Table S5, participant feedback on the salt measuring spoon. DePEC-Nutrition Resources.
Author Contributions
L.R., P.A., D.D.R., M.S., B.C.M.S. and D.M. acquired funding; M.S., D.D.R. and D.M. were involved in the conception and trial design; M.S., A.M. and A.M.H. developed and designed the intervention; D.M., Y.C.S. and M.A. operationalised the study with the SEACO team; T.T.S. facilitated the trial in SEACO and Z.b.K. and A.N.b.M.G. facilitated study in health clinics; U.D.P. guided the bio sample collection process and storage; S.S.L. analysed the data, with input from D.M., A.M. and M.S., and prepared the first draft. All authors have read and agreed to the published version of the manuscript.
Funding
This study was funded by the National Institute for Health Research (NIHR) GHR Group: 16/137/62 NIHR Global Health Research Group on Dementia Prevention and Enhanced Care (DePEC), Newcastle University, UK using UK aid from the UK Government to support global health research.
Institutional Review Board Statement
This study was conducted according to the guidelines of the Declaration of Helsinki and approved by the Monash University Human Research Committee (Project ID 17864) and the Malaysian Medical Research Ethics Committee (NMRR-19-617-45916).
Informed Consent Statement
Informed consent was obtained from all subjects involved in the study.
Data Availability Statement
The data are not publicly available due to privacy concerns.
Acknowledgments
We would like to thank the study participants, Esther Chua Pei Wei, Pang Sia Yen and the staff of SEACO for coordinating the field operations. We also would like to acknowledge the medical officers who were involved in the group nutritional counselling for the study: Melissha binti Luqman, Balqis Asma Saidah binti Abdul Shukor, Nurul A’in binti Mohamed, Ahmad Ghazie bin Muhammad Sharif, Rudi bin Nasib and Teoh See Wie. We acknowledge the support provided by the members of the NIHR DePEC group in the development and conduct of the study.
Conflicts of Interest
The authors declare no conflict of interest.
Appendix A

Table A1.
Eligibility criteria for trial participants.
Table A1.
Eligibility criteria for trial participants.
| Inclusion criteria |
|
| Exclusion criteria |
|

Table A2.
The outcome measures for the DePEC-Nutrition feasibility study.
Table A2.
The outcome measures for the DePEC-Nutrition feasibility study.
| Outcome Measures | Description of Measures Used |
|---|---|
| Primary outcomes | |
| Screening, recruitment, follow-up rate and retention | Number screened: The number of people assessed for eligibility using inclusion/exclusion criteria. Eligibility rate: The number of people screened for eligibility by the number who met inclusion criteria. Reason for exclusion: Reason for ineligibility recorded by data collectors as in the field notes. Consented rate: The number of people who are eligible by the number who consented to participate in the study. Reason for declining: Reason provided by participants who declined to participate was recorded by data collectors in the field notes. |
| Follow-up rate: The number of participants who were assessed during interim follow-ups. Retention rate: The number of participants who remained in the study. Reason for dropped out: Reason provided by participants for withdrawing recorded by data collectors in the field notes. Motivation to participation: Reason provided by participants for participation in the study during the end of study evaluation. | |
| Suitability and acceptability of data collection procedures and outcomes measures | Self-rating appropriateness and suitability of intervention timing and location Feedback from data collectors on home visits and clinic visits Missing data from questionnaires: Number of participants with invalid data for specific instruments. Number of participants provided biological sample and physical measurements (blood pressure and anthropometric measurement) Participants’ self-rating acceptability of providing biological samples and physical measurement Data collectors’ feedback on the acceptability of collecting biological samples and physical measurement |
| Feasibility and acceptability of the intervention strategies | Engagement with the intervention: Meaningful engagement was determined by whether the information booklet provided was read by the participants. For the text messages and reinforcement video, engagement was determined by whether the participants opened, read and responded to the text messages and video. Participants self-rating of usefulness of interventions strategies or materials |
| Low salt and nitrate intervention | Participant self-rated acceptability of low salt diet Participant self-reported use of salt measuring spoon and easiness of use Number of participants interviewed who will continue to follow the recommended diet Number of participants interviewed who will recommend participation in a similar study to their family and friends |
| Outcomes for a definitive trial * | |
| Demographic and medical history | Demographic, medical and medication history |
| Health and lifestyle | Global Physical Activity Questionnaire (GPAQ), Global Activity Limitation Indicator (GALI), smoking and alcohol use, Geriatric Depression Scale (GDS) (short form) |
| Cognitive assessment | Montreal Cognitive Assessment (MoCA) test, Auditory Verbal Learning Test (AVLT), Trail Making Test Part B, Animal Naming Test |
| Blood pressure | Three consecutive measurements of resting blood pressure readings in a sitting position using OMRON automated monitor (OMRON HEM 907, OMRON Healthcare, Milton Keynes, UK) |
| Anthropometry and body composition | Height (m), weight (kg), BMI (kg/m2) and body composition were measured using a portable bioelectrical impedance analysis (BIA) scale (Tanita DC-430MA Body Composition Analyzer, Tanita Corporation, Japan) with a 0.1 kg precision |
| Functional performance | Hand grip strength dynamometer, 4-metre gait speed test, Timed Up and Go (TUG) test |
| Dietary assessment | Food Frequency Questionnaire, 24-h diet recall |
| Biological sample collection | 15 mL whole venous blood, 24-h urine sample, spot urine sample, whole saliva collected using passive drool technique, salivary strips and dried blood spot |
* These outcomes were collected at baseline only due to the COVID-19 pandemic and require further pilot testing in a definitive trial.
References
- Robinson, L.; Tang, E.; Taylor, J.P. Dementia: Timely diagnosis and early intervention. BMJ (Clin. Res. Ed.) 2015, 350, h3029. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Hou, Y.; Dan, X.; Babbar, M.; Wei, Y.; Hasselbalch, S.G.; Croteau, D.L.; Bohr, V.A. Ageing as a risk factor for neurodegenerative disease. Nat. Rev. Neurol. 2019, 15, 565–581. [Google Scholar] [CrossRef] [PubMed]
- Vermunt, L.; Sikkes, S.A.M.; van den Hout, A.; Handels, R.; Bos, I.; van der Flier, W.M.; Kern, S.; Ousset, P.-J.; Maruff, P.; Skoog, I.; et al. Duration of preclinical, prodromal, and dementia stages of Alzheimer’s disease in relation to age, sex, and APOE genotype. Alzheimer’s Dement. 2019, 15, 888–898. [Google Scholar] [CrossRef] [PubMed]
- Patterson, C. Wolrd Alzheimer Report 2018; Alzheimer’s Disease International: London, UK, 2018. [Google Scholar]
- Grande, G.; Qiu, C.; Fratiglioni, L. Prevention of dementia in an ageing world: Evidence and biological rationale. Ageing Res. Rev. 2020, 64, 101045. [Google Scholar] [CrossRef]
- Livingston, G.; Huntley, J.; Sommerlad, A.; Ames, D.; Ballard, C.; Banerjee, S.; Brayne, C.; Burns, A.; Cohen-Mansfield, J.; Cooper, C.; et al. Dementia prevention, intervention, and care: 2020 report of the Lancet Commission. Lancet 2020, 396, 413–446. [Google Scholar] [CrossRef]
- McGrath, E.R.; Beiser, A.S.; DeCarli, C.; Plourde, K.L.; Vasan, R.S.; Greenberg, S.M.; Seshadri, S. Blood pressure from mid- to late life and risk of incident dementia. Neurology 2017, 89, 2447–2454. [Google Scholar] [CrossRef]
- Pase, M.P.; Beiser, A.; Enserro, D.; Xanthakis, V.; Aparicio, H.; Satizabal, C.L.; Himali, J.J.; Kase, C.S.; Vasan, R.S.; DeCarli, C.; et al. Association of Ideal Cardiovascular Health with Vascular Brain Injury and Incident Dementia. Stroke 2016, 47, 1201–1206. [Google Scholar] [CrossRef] [Green Version]
- Abell, J.G.; Kivimäki, M.; Dugravot, A.; Tabak, A.G.; Fayosse, A.; Shipley, M.; Sabia, S.; Singh-Manoux, A. Association between systolic blood pressure and dementia in the Whitehall II cohort study: Role of age, duration, and threshold used to define hypertension. Eur. Heart J. 2018, 39, 3119–3125. [Google Scholar] [CrossRef]
- Ettehad, D.; Emdin, C.A.; Kiran, A.; Anderson, S.G.; Callender, T.; Emberson, J.; Chalmers, J.; Rodgers, A.; Rahimi, K. Blood pressure lowering for prevention of cardiovascular disease and death: A systematic review and meta-analysis. Lancet 2016, 387, 957–967. [Google Scholar] [CrossRef] [Green Version]
- Bundy, J.D.; Li, C.; Stuchlik, P.; Bu, X.; Kelly, T.N.; Mills, K.T.; He, H.; Chen, J.; Whelton, P.K.; He, J. Systolic Blood Pressure Reduction and Risk of Cardiovascular Disease and Mortality: A Systematic Review and Network Meta-analysis. JAMA Cardiol. 2017, 2, 775–781. [Google Scholar] [CrossRef] [Green Version]
- Smith, P.J.; Blumenthal, J.A.; Babyak, M.A.; Craighead, L.; Welsh-Bohmer, K.A.; Browndyke, J.N.; Strauman, T.A.; Sherwood, A. Effects of the dietary approaches to stop hypertension diet, exercise, and caloric restriction on neurocognition in overweight adults with high blood pressure. Hypertension 2010, 55, 1331–1338. [Google Scholar] [CrossRef] [PubMed]
- Blumenthal, J.A.; Smith, P.J.; Mabe, S.; Hinderliter, A.; Lin, P.H.; Liao, L.; Welsh-Bohmer, K.A.; Browndyke, J.N.; Kraus, W.E.; Doraiswamy, P.M.; et al. Lifestyle and neurocognition in older adults with cognitive impairments: A randomized trial. Neurology 2019, 92, e212–e223. [Google Scholar] [CrossRef] [Green Version]
- Williamson, J.D.; Pajewski, N.M.; Auchus, A.P.; Bryan, R.N.; Chelune, G.; Cheung, A.K.; Cleveland, M.L.; Coker, L.H.; Crowe, M.G.; Cushman, W.C.; et al. Effect of Intensive vs Standard Blood Pressure Control on Probable Dementia: A Randomized Clinical Trial. JAMA 2019, 321, 553–561. [Google Scholar] [CrossRef]
- Siervo, M.; Lara, J.; Chowdhury, S.; Ashor, A.; Oggioni, C.; Mathers, J.C. Effects of the Dietary Approach to Stop Hypertension (DASH) diet on cardiovascular risk factors: A systematic review and meta-analysis. Br. J. Nutr. 2015, 113, 1–15. [Google Scholar] [CrossRef] [Green Version]
- Siervo, M.; Shannon, O.M.; Llewellyn, D.J.; Stephan, B.C.; Fontana, L. Mediterranean diet and cognitive function: From methodology to mechanisms of action. Free Radic. Biol. Med. 2021, 176, 105–117. [Google Scholar] [CrossRef]
- Duplantier, S.C.; Gardner, C.D. A Critical Review of the Study of Neuroprotective Diets to Reduce Cognitive Decline. Nutrients 2021, 13, 2264. [Google Scholar] [CrossRef] [PubMed]
- Bailey, J.C.; Feelisch, M.; Horowitz, J.D.; Frenneaux, M.P.; Madhani, M. Pharmacology and therapeutic role of inorganic nitrite and nitrate in vasodilatation. Pharmacol. Ther. 2014, 144, 303–320. [Google Scholar] [CrossRef] [Green Version]
- Grillo, A.; Salvi, L.; Coruzzi, P.; Salvi, P.; Parati, G. Sodium Intake and Hypertension. Nutrients 2019, 11, 1970. [Google Scholar] [CrossRef] [Green Version]
- Blekkenhorst, L.C.; Bondonno, C.P.; Lewis, J.R.; Devine, A.; Woodman, R.J.; Croft, K.D.; Lim, W.H.; Wong, G.; Beilin, L.J.; Prince, R.L.; et al. Association of dietary nitrate with atherosclerotic vascular disease mortality: A prospective cohort study of older adult women. Am. J. Clin. Nutr. 2017, 106, 207–216. [Google Scholar] [CrossRef] [Green Version]
- Bonilla Ocampo, D.A.; Paipilla, A.F.; Marín, E.; Vargas-Molina, S.; Petro, J.L.; Pérez-Idárraga, A. Dietary Nitrate from Beetroot Juice for Hypertension: A Systematic Review. Biomolecules 2018, 8, 134. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Siervo, M.; Scialò, F.; Shannon, O.M.; Stephan, B.C.M.; Ashor, A.W. Does dietary nitrate say NO to cardiovascular ageing? Current evidence and implications for research. Proc. Nutr. Soc. 2018, 77, 112–123. [Google Scholar] [CrossRef] [Green Version]
- Smallwood, M.J.; Ble, A.; Melzer, D.; Winyard, P.G.; Benjamin, N.; Shore, A.C.; Gilchrist, M. Relationship Between Urinary Nitrate Excretion and Blood Pressure in the InChianti Cohort. Am. J. Hypertens. 2017, 30, 707–712. [Google Scholar] [CrossRef] [PubMed]
- Kapil, V.; Khambata, R.S.; Robertson, A.; Caulfield, M.J.; Ahluwalia, A. Dietary nitrate provides sustained blood pressure lowering in hypertensive patients: A randomized, phase 2, double-blind, placebo-controlled study. Hypertension 2015, 65, 320–327. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Kapil, V.; Milsom, A.B.; Okorie, M.; Maleki-Toyserkani, S.; Akram, F.; Rehman, F.; Arghandawi, S.; Pearl, V.; Benjamin, N.; Loukogeorgakis, S.; et al. Inorganic nitrate supplementation lowers blood pressure in humans: Role for nitrite-derived NO. Hypertension 2010, 56, 274–281. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Siervo, M.; Shannon, O.; Kandhari, N.; Prabhakar, M.; Fostier, W.; Köchl, C.; Rogathi, J.; Temu, G.; Stephan, B.C.M.; Gray, W.K.; et al. Nitrate-Rich Beetroot Juice Reduces Blood Pressure in Tanzanian Adults with Elevated Blood Pressure: A Double-Blind Randomized Controlled Feasibility Trial. J. Nutr. 2020, 150, 2460–2468. [Google Scholar] [CrossRef] [PubMed]
- Webb, A.J.; Patel, N.; Loukogeorgakis, S.; Okorie, M.; Aboud, Z.; Misra, S.; Rashid, R.; Miall, P.; Deanfield, J.; Benjamin, N.; et al. Acute blood pressure lowering, vasoprotective, and antiplatelet properties of dietary nitrate via bioconversion to nitrite. Hypertension 2008, 51, 784–790. [Google Scholar] [CrossRef] [Green Version]
- Ashworth, A.; Mitchell, K.; Blackwell, J.R.; Vanhatalo, A.; Jones, A.M. High-nitrate vegetable diet increases plasma nitrate and nitrite concentrations and reduces blood pressure in healthy women. Public Health Nutr. 2015, 18, 2669–2678. [Google Scholar] [CrossRef] [Green Version]
- Bondonno, C.P.; Yang, X.; Croft, K.D.; Considine, M.J.; Ward, N.C.; Rich, L.; Puddey, I.B.; Swinny, E.; Mubarak, A.; Hodgson, J.M. Flavonoid-rich apples and nitrate-rich spinach augment nitric oxide status and improve endothelial function in healthy men and women: A randomized controlled trial. Free Radic. Biol. Med. 2012, 52, 95–102. [Google Scholar] [CrossRef] [PubMed]
- Liu, A.H.; Bondonno, C.P.; Croft, K.D.; Puddey, I.B.; Woodman, R.J.; Rich, L.; Ward, N.C.; Vita, J.A.; Hodgson, J.M. Effects of a nitrate-rich meal on arterial stiffness and blood pressure in healthy volunteers. Nitric Oxide Biol. Chem. 2013, 35, 123–130. [Google Scholar] [CrossRef]
- Jackson, J.K.; Patterson, A.J.; MacDonald-Wicks, L.K.; Oldmeadow, C.; McEvoy, M.A. The role of inorganic nitrate and nitrite in cardiovascular disease risk factors: A systematic review and meta-analysis of human evidence. Nutr. Rev. 2018, 76, 348–371. [Google Scholar] [CrossRef]
- Kapil, V.; Khambata, R.S.; Jones, D.A.; Rathod, K.; Primus, C.; Massimo, G.; Fukuto, J.M.; Ahluwalia, A. The Noncanonical Pathway for In Vivo Nitric Oxide Generation: The Nitrate-Nitrite-Nitric Oxide Pathway. Pharm. Rev 2020, 72, 692–766. [Google Scholar] [CrossRef] [PubMed]
- Clifford, T.; Babateen, A.; Shannon, O.M.; Capper, T.; Ashor, A.; Stephan, B.; Robinson, L.; O’Hara, J.P.; Mathers, J.C.; Stevenson, E.; et al. Effects of inorganic nitrate and nitrite consumption on cognitive function and cerebral blood flow: A systematic review and meta-analysis of randomized clinical trials. Crit. Rev. Food Sci. Nutr. 2019, 59, 2400–2410. [Google Scholar] [CrossRef] [PubMed]
- Presley, T.D.; Morgan, A.R.; Bechtold, E.; Clodfelter, W.; Dove, R.W.; Jennings, J.M.; Kraft, R.A.; King, S.B.; Laurienti, P.J.; Rejeski, W.J.; et al. Acute effect of a high nitrate diet on brain perfusion in older adults. Nitric Oxide Biol. Chem. 2011, 24, 34–42. [Google Scholar] [CrossRef] [PubMed]
- Wightman, E.L.; Haskell-Ramsay, C.F.; Thompson, K.G.; Blackwell, J.R.; Winyard, P.G.; Forster, J.; Jones, A.M.; Kennedy, D.O. Dietary nitrate modulates cerebral blood flow parameters and cognitive performance in humans: A double-blind, placebo-controlled, crossover investigation. Physiol. Behav. 2015, 149, 149–158. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Strazzullo, P.; D’Elia, L.; Kandala, N.-B.; Cappuccio, F.P. Salt intake, stroke, and cardiovascular disease: Meta-analysis of prospective studies. BMJ 2009, 339, b4567. [Google Scholar] [CrossRef] [Green Version]
- Mente, A.; O’Donnell, M.; Rangarajan, S.; McQueen, M.; Dagenais, G.; Wielgosz, A.; Lear, S.; Ah, S.T.L.; Wei, L.; Diaz, R.; et al. Urinary sodium excretion, blood pressure, cardiovascular disease, and mortality: A community-level prospective epidemiological cohort study. Lancet 2018, 392, 496–506. [Google Scholar] [CrossRef]
- He, F.J.; MacGregor, G.A. Role of salt intake in prevention of cardiovascular disease: Controversies and challenges. Nat. Rev. Cardiol. 2018, 15, 371–377. [Google Scholar] [CrossRef]
- He, F.J.; Li, J.; Macgregor, G.A. Effect of longer term modest salt reduction on blood pressure: Cochrane systematic review and meta-analysis of randomised trials. BMJ 2013, 346, f1325. [Google Scholar] [CrossRef] [Green Version]
- Hughes, D.; Judge, C.; Murphy, R.; Loughlin, E.; Costello, M.; Whiteley, W.; Bosch, J.; O’Donnell, M.J.; Canavan, M. Association of Blood Pressure Lowering With Incident Dementia or Cognitive Impairment: A Systematic Review and Meta-analysis. JAMA 2020, 323, 1934–1944. [Google Scholar] [CrossRef]
- Fiocco, A.J.; Shatenstein, B.; Ferland, G.; Payette, H.; Belleville, S.; Kergoat, M.J.; Morais, J.A.; Greenwood, C.E. Sodium intake and physical activity impact cognitive maintenance in older adults: The NuAge Study. Neurobiol. Aging 2012, 33, 829.e21–829.e28. [Google Scholar] [CrossRef]
- Haring, B.; Wu, C.; Coker, L.H.; Seth, A.; Snetselaar, L.; Manson, J.E.; Rossouw, J.E.; Wassertheil-Smoller, S. Hypertension, Dietary Sodium, and Cognitive Decline: Results From the Women’s Health Initiative Memory Study. Am. J. Hypertens 2016, 29, 202–216. [Google Scholar] [CrossRef] [Green Version]
- Nowak, K.L.; Fried, L.; Jovanovich, A.; Ix, J.; Yaffe, K.; You, Z.; Chonchol, M. Dietary Sodium/Potassium Intake Does Not Affect Cognitive Function or Brain Imaging Indices. Am. J. Nephrol. 2018, 47, 57–65. [Google Scholar] [CrossRef]
- Rush, T.M.; Kritz-Silverstein, D.; Laughlin, G.A.; Fung, T.T.; Barrett-Connor, E.; McEvoy, L.K. Association between dietary sodium intake and cognitive function in older adults. J. Nutr. Health Aging 2017, 21, 276–283. [Google Scholar] [CrossRef] [PubMed]
- Mohan, D.; Yap, K.H.; Reidpath, D.; Soh, Y.C.; McGrattan, A.; Stephan, B.C.M.; Robinson, L.; Chaiyakunapruk, N.; Siervo, M. Link Between Dietary Sodium Intake, Cognitive Function, and Dementia Risk in Middle-Aged and Older Adults: A Systematic Review. J. Alzheimer’s Dis. JAD 2020, 76, 1347–1373. [Google Scholar] [CrossRef] [PubMed]
- McGrattan, A.; van Aller, C.; Narytnyk, A.; Reidpath, D.; Keage, H.; Mohan, D.; Su, T.T.; Stephan, B.; Robinson, L.; Siervo, M. Nutritional interventions for the prevention of cognitive impairment and dementia in developing economies in East-Asia: A systematic review and meta-analysis. Crit. Rev. Food Sci. Nutr. 2020, 1–18. [Google Scholar] [CrossRef] [PubMed]
- McGrattan, A.; Mohan, D.; Chua, P.W.; Mat Hussin, A.; Soh, Y.C.; Alawad, M.; Bin Kassim, Z.; Bin Mohd Ghazali, A.N.; Stephan, B.; Allotey, P.; et al. Feasibility and acceptability of a dietary intervention study to reduce salt intake and increase high-nitrate vegetable consumption among middle-aged and older Malaysian adults with elevated blood pressure: A study protocol. BMJ Open 2020, 10, e035453. [Google Scholar] [CrossRef] [PubMed]
- Craig, P.; Dieppe, P.; Macintyre, S.; Michie, S.; Nazareth, I.; Petticrew, M. Developing and evaluating complex interventions: The new Medical Research Council guidance. BMJ 2008, 337, a1655. [Google Scholar] [CrossRef] [Green Version]
- Ibrahim, N.M.; Shohaimi, S.; Chong, H.T.; Rahman, A.H.; Razali, R.; Esther, E.; Basri, H.B. Validation study of the Mini-Mental State Examination in a Malay-speaking elderly population in Malaysia. Dement. Geriatr. Cogn. Disord. 2009, 27, 247–253. [Google Scholar] [CrossRef]
- World Health Organization. Guideline: Sodium Intake for Adults and Children; World Health Organization: Geneva, Switzerland, 2012. [Google Scholar]
- National Coordinating Committee on Food and Nutrition. Malaysian Dietary Guidelines; Ministry of Health Malaysia: Putrajaya, Malaysia, 2010.
- Uschner, D.; Schindler, D.; Hilgers, R.-D.; Heussen, N. randomizeR: An R package for the assessment and implementation of randomization in clinical trials. J. Stat. Softw. 2018, 85, 1–22. [Google Scholar] [CrossRef] [Green Version]
- Sahathevan, R.; Mohd Ali, K.; Ellery, F.; Mohamad, N.F.; Hamdan, N.; Mohd Ibrahim, N.; Churilov, L.; Cumming, T.B. A Bahasa Malaysia version of the Montreal Cognitive Assessment: Validation in stroke. Int. Psychogeriatr. 2014, 26, 781–786. [Google Scholar] [CrossRef]
- Jamaluddin, R.; Othman, Z.; Musa, K.I.; Alwi, M.N.M. Validation of the Malay version of auditory verbal learning test (MVAVLT) among schizophrenia patients in hospital Universiti Sains Malaysia (HUSM), Malaysia. ASEAN J. Psychiatry 2009, 10, 54–74. [Google Scholar]
- Institute for Public Health (IPH). National Health and Morbidity Survey 2014: Malaysian Adult Nutrition Survey. Vol. 1: Methodology and General Findings; Institute for Public Health, Ministry of Health Malaysia: Kuala Lumpur, Malaysia, 2014.
- Whitehead, A.L.; Julious, S.A.; Cooper, C.L.; Campbell, M.J. Estimating the sample size for a pilot randomised trial to minimise the overall trial sample size for the external pilot and main trial for a continuous outcome variable. Stat. Methods Med. Res. 2015, 25, 1057–1073. [Google Scholar] [CrossRef] [PubMed]
- Mishra, P.; Pandey, C.M.; Singh, U.; Gupta, A.; Sahu, C.; Keshri, A. Descriptive statistics and normality tests for statistical data. Ann. Card. Anaesth. 2019, 22, 67–72. [Google Scholar] [CrossRef] [PubMed]
- Forsat, N.D.; Palmowski, A.; Palmowski, Y.; Boers, M.; Buttgereit, F. Recruitment and Retention of Older People in Clinical Research: A Systematic Literature Review. J. Am. Geriatr. Soc. 2020, 68, 2955–2963. [Google Scholar] [CrossRef] [PubMed]
- Fiordelli, M.; Fadda, M.; Amati, R.; Albanese, E. Older adults’ motivations to participate or not in epidemiological research. Qualitative inquiry on a study into dementia in Switzerland. PLoS ONE 2021, 16, e0247141. [Google Scholar] [CrossRef]
- Bardach, S.H.; Yarbrough, M.; Walker, C.; Alfred, D.L.; Ighodaro, E.; Kiviniemi, M.T.; Jicha, G.A. Insights From African American Older Adults on Brain Health Research Engagement: “Need to See the Need”. J. Appl. Gerontol. 2020, 40, 201–208. [Google Scholar] [CrossRef] [PubMed]
- Jefferson, A.L.; Lambe, S.; Chaisson, C.; Palmisano, J.; Horvath, K.J.; Karlawish, J. Clinical Research Participation among Aging Adults Enrolled in an Alzheimer’s Disease Center Research Registry. J. Alzheimer’s Dis. 2011, 23, 443–452. [Google Scholar] [CrossRef]
- Treweek, S.; Lockhart, P.; Pitkethly, M.; Cook, J.A.; Kjeldstrøm, M.; Johansen, M.; Taskila, T.K.; Sullivan, F.M.; Wilson, S.; Jackson, C.; et al. Methods to improve recruitment to randomised controlled trials: Cochrane systematic review and meta-analysis. BMJ Open 2013, 3, e002360. [Google Scholar] [CrossRef] [Green Version]
- Holzer, J.K.; Ellis, L.; Merritt, M.W. Why we need community engagement in medical research. J. Investig. Med. Off. Publ. Am. Fed. Clin. Res. 2014, 62, 851–855. [Google Scholar] [CrossRef] [Green Version]
- Hinton, L.; Carter, K.; Reed, B.R.; Beckett, L.; Lara, E.; DeCarli, C.; Mungas, D. Recruitment of a community-based cohort for research on diversity and risk of dementia. Alzheimer Dis. Assoc. Disord. 2010, 24, 234–241. [Google Scholar] [CrossRef] [Green Version]
- Romero, H.R.; Welsh-Bohmer, K.A.; Gwyther, L.P.; Edmonds, H.L.; Plassman, B.L.; Germain, C.M.; McCart, M.; Hayden, K.M.; Pieper, C.; Roses, A.D. Community engagement in diverse populations for Alzheimer disease prevention trials. Alzheimer Dis. Assoc. Disord. 2014, 28, 269–274. [Google Scholar] [CrossRef] [Green Version]
- Wallace, R.; Lo, J.; Devine, A. Tailored Nutrition Education in the Elderly Can Lead to Sustained Dietary Behaviour Change. J. Nutr. Health Aging 2016, 20, 8–15. [Google Scholar] [CrossRef]
- Young, K.; Bunn, F.; Trivedi, D.; Dickinson, A. Nutritional education for community dwelling older people: A systematic review of randomised controlled trials. Int. J. Nurs. Stud. 2011, 48, 751–780. [Google Scholar] [CrossRef] [Green Version]
- Lyons, B.P. Nutrition education intervention with community-dwelling older adults: Research challenges and opportunities. J. Community Health 2014, 39, 810–818. [Google Scholar] [CrossRef]
- Shahar, S.; Adznam, S.N.A.; Rahman, S.A.; Yusoff, N.A.M.; Yassin, Z.; Arshad, F.; Sakian, N.I.M.; Salleh, M.; Samah, A.A. Development and analysis of acceptance of a nutrition education package among a rural elderly population: An action research study. BMC Geriatr. 2012, 12, 24. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Vasiloglou, M.F.; Fletcher, J.; Poulia, K.-A. Challenges and Perspectives in Nutritional Counselling and Nursing: A Narrative Review. J. Clin. Med. 2019, 8, 1489. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Leon, N.; Surender, R.; Bobrow, K.; Muller, J.; Farmer, A. Improving treatment adherence for blood pressure lowering via mobile phone SMS-messages in South Africa: A qualitative evaluation of the SMS-text Adherence SuppoRt (StAR) trial. BMC Fam. Pract. 2015, 16, 80. [Google Scholar] [CrossRef] [Green Version]
- Hacking, D.; Haricharan, H.J.; Brittain, K.; Lau, Y.K.; Cassidy, T.; Heap, M. Hypertension Health Promotion via Text Messaging at a Community Health Center in South Africa: A Mixed Methods Study. JMIR Mhealth Uhealth 2016, 4, e22. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Ibrahim, A.; Chong, M.C.; Khoo, S.; Wong, L.P.; Chung, I.; Tan, M.P. Virtual Group Exercises and Psychological Status among Community-Dwelling Older Adults during the COVID-19 Pandemic—A Feasibility Study. Geriatrics 2021, 6, 31. [Google Scholar] [CrossRef]
- Ridda, I.; MacIntyre, C.R.; Lindley, R.I.; Tan, T.C. Difficulties in recruiting older people in clinical trials: An examination of barriers and solutions. Vaccine 2010, 28, 901–906. [Google Scholar] [CrossRef]
- Sano, M.; Egelko, S.; Zhu, C.W.; Li, C.; Donohue, M.C.; Ferris, S.; Kaye, J.; Mundt, J.C.; Sun, C.-K.; Aisen, P.S.; et al. Participant satisfaction with dementia prevention research: Results from Home-Based Assessment trial. Alzheimer’s Dement. 2018, 14, 1397–1405. [Google Scholar] [CrossRef]
- Kim, H.J.; Baek, M.J.; Kim, S. Alternative type of the trail making test in nonnative English-speakers: The trail making test-black & white. PLoS ONE 2014, 9, e89078. [Google Scholar] [CrossRef]
- Hashimoto, R.; Meguro, K.; Lee, E.; Kasai, M.; Ishii, H.; Yamaguchi, S. Effect of age and education on the Trail Making Test and determination of normative data for Japanese elderly people: The Tajiri Project. Psychiatry Clin. Neurosci. 2006, 60, 422–428. [Google Scholar] [CrossRef] [PubMed]
- Ivery, J.M.; Benton, L.; Harrison, A.; Paul, M.; Cortés, M. The DASH Pilot Project: Developing Community-Based Nutrition Education for Older Adults. J. Gerontol. Soc. Work 2017, 60, 286–299. [Google Scholar] [CrossRef] [PubMed]
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).