Multilevel Understanding of the Impact of Individual- and School-Level Determinants on Lipid Profiles in Adolescents: The Cross-Level Interaction of Food Environment and Body Mass Index
Abstract
1. Introduction
2. Materials and Methods
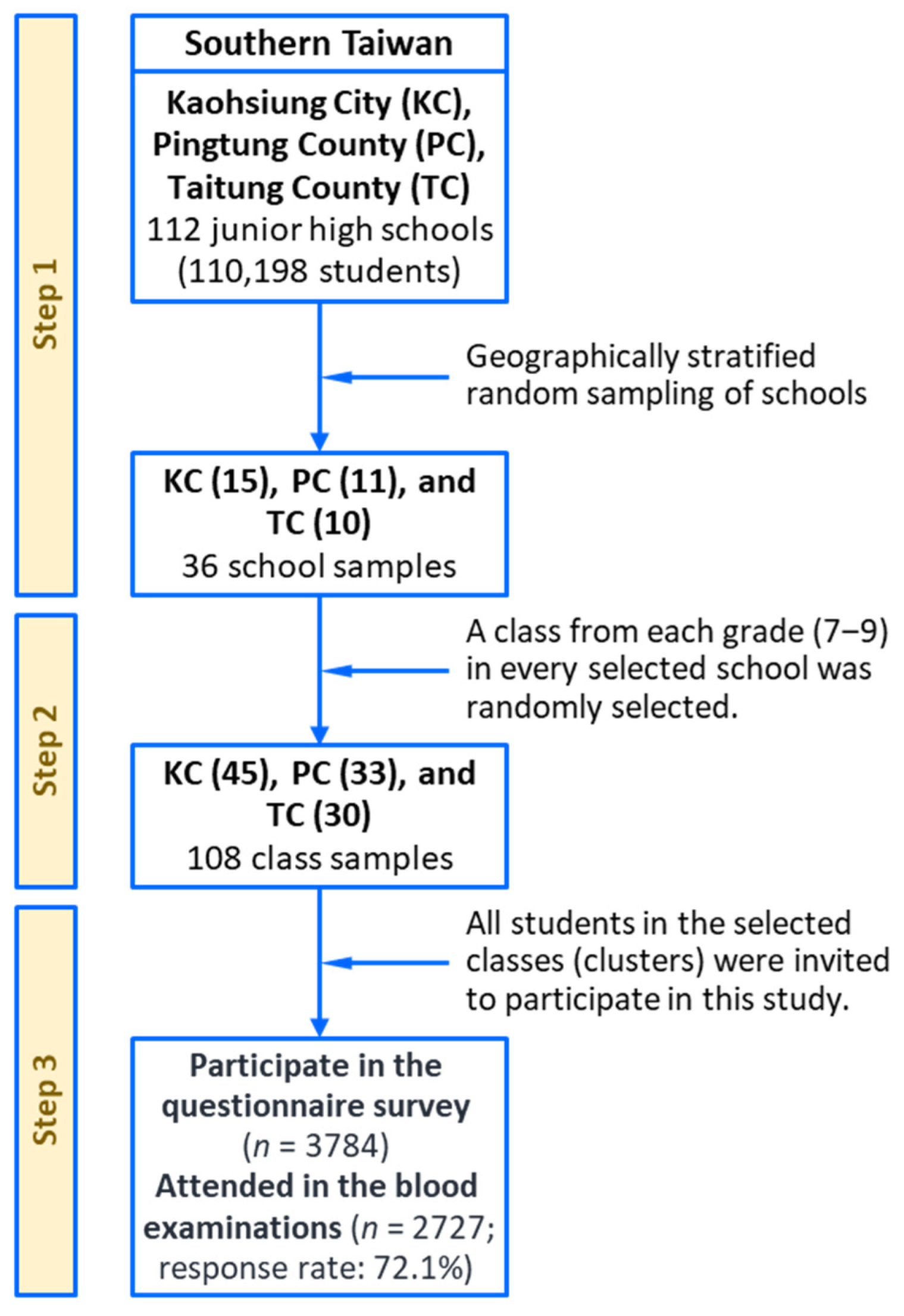
2.1. Participants
2.2. Individual-Level Factors
2.3. School-Level Factors
2.4. Lipid Measurements
2.5. Statistical Analysis
3. Results
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
Abbreviations
References
- Kopin, L.; Lowenstein, C. Dyslipidemia. Ann. Intern. Med. 2017, 167, ITC81–ITC96. [Google Scholar] [CrossRef] [PubMed]
- Vekic, J.; Zeljkovic, A.; Stefanovic, A.; Jelic-Ivanovic, Z.; Spasojevic-Kalimanovska, V. Obesity and dyslipidemia. Metabolism 2019, 92, 71–81. [Google Scholar] [CrossRef] [PubMed]
- Warraich, H.J.; Rana, J.S. Dyslipidemia in diabetes mellitus and cardiovascular disease. Cardiovasc. Endocrinol. 2017, 6, 27–32. [Google Scholar] [CrossRef] [PubMed]
- Stanley, T.L.; Chen, M.L.; Goodman, E. The typology of metabolic syndrome in the transition to adulthood. J. Clin. Endocrinol. Metab. 2014, 99, 1044–1052. [Google Scholar] [CrossRef]
- Magnussen, C.G.; Koskinen, J.; Chen, W.; Thomson, R.; Schmidt, M.D.; Srinivasan, S.R.; Kivimaki, M.; Mattsson, N.; Kahonen, M.; Laitinen, T.; et al. Pediatric metabolic syndrome predicts adulthood metabolic syndrome, subclinical atherosclerosis, and type 2 diabetes mellitus but is no better than body mass index alone: The Bogalusa Heart Study and the Cardiovascular Risk in Young Finns Study. Circulation 2010, 122, 1604–1611. [Google Scholar] [CrossRef]
- Morrison, J.A.; Friedman, L.A.; Gray-McGuire, C. Metabolic syndrome in childhood predicts adult cardiovascular disease 25 years later: The Princeton Lipid Research Clinics Follow-up Study. Pediatrics 2007, 120, 340–345. [Google Scholar] [CrossRef]
- Morrison, J.A.; Friedman, L.A.; Wang, P.; Glueck, C.J. Metabolic syndrome in childhood predicts adult metabolic syndrome and type 2 diabetes mellitus 25 to 30 years later. J. Pediatr. 2008, 152, 201–206. [Google Scholar] [CrossRef]
- Merlo, J.; Chaix, B.; Yang, M.; Lynch, J.; Rastam, L. A brief conceptual tutorial of multilevel analysis in social epidemiology: Linking the statistical concept of clustering to the idea of contextual phenomenon. J. Epidemiol. Community Health 2005, 59, 443–449. [Google Scholar] [CrossRef]
- Merlo, J.; Yang, M.; Chaix, B.; Lynch, J.; Rastam, L. A brief conceptual tutorial on multilevel analysis in social epidemiology: Investigating contextual phenomena in different groups of people. J. Epidemiol. Community Health 2005, 59, 729–736. [Google Scholar] [CrossRef]
- Merlo, J.; Chaix, B.; Yang, M.; Lynch, J.; Rastam, L. A brief conceptual tutorial on multilevel analysis in social epidemiology: Interpreting neighbourhood differences and the effect of neighbourhood characteristics on individual health. J. Epidemiol. Community Health 2005, 59, 1022–1028. [Google Scholar] [CrossRef]
- Yang, B.Y.; Markevych, I.; Heinrich, J.; Bloom, M.S.; Qian, Z.; Geiger, S.D.; Vaughn, M.; Liu, S.; Guo, Y.; Dharmage, S.C.; et al. Residential greenness and blood lipids in urban-dwelling adults: The 33 Communities Chinese Health Study. Environ. Pollut. 2019, 250, 14–22. [Google Scholar] [CrossRef] [PubMed]
- Twohig-Bennett, C.; Jones, A. The health benefits of the great outdoors: A systematic review and meta-analysis of greenspace exposure and health outcomes. Environ. Res. 2018, 166, 628–637. [Google Scholar] [CrossRef] [PubMed]
- Peterson, A.L.; McBride, P.E. A review of guidelines for dyslipidemia in children and adolescents. WMJ 2012, 111, 274–281. [Google Scholar] [PubMed]
- Daniels, S.R. Guidelines for screening, prevention, diagnosis and treatment of dyslipidemia in children and adolescents. In Endotext; Feingold, K.R., Anawalt, B., Boyce, A., Chrousos, G., de Herder, W.W., Dungan, K., Grossman, A., Hershman, J.M., Hofland, J., Kaltsas, G., et al., Eds.; MDtext.com, Inc.: South Dartmouth, MA, USA, 2000. [Google Scholar]
- Lin, W.T.; Lee, C.Y.; Tsai, S.; Huang, H.L.; Wu, P.W.; Chin, Y.T.; Seal, D.W.; Chen, T.; Chao, Y.Y.; Lee, C.H. Clustering of metabolic risk components and associated lifestyle factors: A nationwide adolescent study in Taiwan. Nutrients 2019, 11, 584. [Google Scholar] [CrossRef] [PubMed]
- Austin, S.B.; Melly, S.J.; Sanchez, B.N.; Patel, A.; Buka, S.; Gortmaker, S.L. Clustering of fast-food restaurants around schools: A novel application of spatial statistics to the study of food environments. Am. J. Public Health 2005, 95, 1575–1581. [Google Scholar] [CrossRef] [PubMed]
- Merlo, J.; Asplund, K.; Lynch, J.; Rastam, L.; Dobson, A. Population effects on individual systolic blood pressure: A multilevel analysis of the World Health Organization MONICA Project. Am. J. Epidemiol. 2004, 159, 1168–1179. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Wu, P.W.; Lai, Y.W.; Chin, Y.T.; Tsai, S.; Yang, T.M.; Lin, W.T.; Lee, C.Y.; Tsai, W.C.; Huang, H.L.; Seal, D.W.; et al. Stability and transformation of metabolic syndrome in adolescents: A prospective assessment in relation to the change of cardiometabolic risk factors. Nutrients 2022, 14, 744. [Google Scholar] [CrossRef]
- Lin, W.T.; Huang, H.L.; Huang, M.C.; Chan, T.F.; Ciou, S.Y.; Lee, C.Y.; Chiu, Y.W.; Duh, T.H.; Lin, P.L.; Wang, T.N.; et al. Effects on uric acid, body mass index and blood pressure in adolescents of consuming beverages sweetened with high-fructose corn syrup. Int. J. Obes. 2013, 37, 532–539. [Google Scholar] [CrossRef]
- Chan, T.F.; Lin, W.T.; Huang, H.L.; Lee, C.Y.; Wu, P.W.; Chiu, Y.W.; Huang, C.C.; Tsai, S.; Lin, C.L.; Lee, C.H. Consumption of sugar-sweetened beverages is associated with components of the metabolic syndrome in adolescents. Nutrients 2014, 6, 2088–2103. [Google Scholar] [CrossRef]
- Lin, W.T.; Chan, T.F.; Huang, H.L.; Lee, C.Y.; Tsai, S.; Wu, P.W.; Yang, Y.C.; Wang, T.N.; Lee, C.H. Fructose-rich beverage intake and central adiposity, uric acid, and pediatric insulin resistance. J. Pediatr. 2016, 171, 90–96.e1. [Google Scholar] [CrossRef]
- Lee, C.Y.; Lin, W.T.; Tsai, S.; Hung, Y.C.; Wu, P.W.; Yang, Y.C.; Chan, T.F.; Huang, H.L.; Weng, Y.L.; Chiu, Y.W.; et al. Association of parental overweight and cardiometabolic diseases and pediatric adiposity and lifestyle factors with cardiovascular risk factor clustering in adolescents. Nutrients 2016, 8, 567. [Google Scholar] [CrossRef] [PubMed]
- Huang, M.C.; Lin, K.D.; Chen, H.J.; Wu, Y.J.; Chang, C.I.; Shin, S.J.; Hung, H.C.; Lee, C.H.; Huang, Y.F.; Hsu, C.C. Validity of a short food frequency questionnaire assessing macronutrient and fiber intakes in patients of Han Chinese descent with type 2 diabetes. Int. J. Environ. Res. Public Health 2018, 15, 1142. [Google Scholar] [CrossRef] [PubMed]
- Wu, P.W.; Tsai, S.; Lee, C.Y.; Lin, W.T.; Chin, Y.T.; Huang, H.L.; Seal, D.W.; Chen, T.; Lee, C.H. Contribution of insulin resistance to the relationship between sugar-sweetened beverage intake and a constellation of cardiometabolic abnormalities in adolescents. Int. J. Obes. 2021, 45, 828–839. [Google Scholar] [CrossRef] [PubMed]
- Taiwanese Food and Nutrients Databank. (Chinese Version Webpage). Available online: https://consumer.fda.gov.tw/FoodAnalysis/ingredients.htm (accessed on 10 October 2012).
- Ridley, K.; Ainsworth, B.E.; Olds, T.S. Development of a compendium of energy expenditures for youth. Int. J. Behav. Nutr. Phys. Act. 2008, 5, 45. [Google Scholar] [CrossRef] [PubMed]
- Google Maps Web Mapping Platform. Google. Mountain View, California, U.S. (Chinese Version Webpage). Available online: https://www.google.com.tw/maps/@23.763184,120.4923129,11.6z?hl=zh-TW (accessed on 23 January 2008).
- Allain, C.C.; Poon, L.S.; Chan, C.S.; Richmond, W.; Fu, P.C. Enzymatic determination of total serum cholesterol. Clin. Chem. 1974, 20, 470–475. [Google Scholar] [CrossRef]
- Chen, Y.K.; Lee, C.H.; Wu, I.C.; Liu, J.S.; Wu, D.C.; Lee, J.M.; Goan, Y.G.; Chou, S.H.; Huang, C.T.; Lee, C.Y.; et al. Food intake and the occurrence of squamous cell carcinoma in different sections of the esophagus in Taiwanese men. Nutrition 2009, 25, 753–761. [Google Scholar] [CrossRef]
- Lee, C.H.; Ko, A.M.; Yang, F.M.; Hung, C.C.; Warnakulasuriya, S.; Ibrahim, S.O.; Zain, R.B.; Ko, Y.C. Association of DSM-5 Betel-Quid Use Disorder With Oral Potentially Malignant Disorder in 6 Betel-Quid Endemic Asian Populations. JAMA Psychiatry 2018, 75, 261–269. [Google Scholar] [CrossRef]
- Martakis, K.; Stark, C.; Rehberg, M.; Jackels, M.; Schoenau, E.; Duran, I. Association of muscle mass and fat mass on low-density-lipoprotein cholesterol and triglyceride plasma concentration in children and adolescents. J. Pediatr. Endocrinol. Metab. 2021, 34, 1273–1282. [Google Scholar] [CrossRef]
- Duran, I.; Martakis, K.; Alberg, E.; Jackels, M.; Ewert, K.R.; Schoenau, E. Association of Trunk/Leg Fat Mass Ratio with Low-Density Lipoproteins-Cholesterol and Triglycerides Concentration in Children and Adolescents: A Cross-Sectional, Retrospective Study. Child. Obes. 2020, 16, 428–439. [Google Scholar] [CrossRef]
- Kondo, T.; Kimata, A.; Yamamoto, K.; Ueyama, S.; Ueyama, J.; Yatsuya, H.; Tamakoshi, K.; Hori, Y. Multilevel analyses of effects of variation in body mass index on serum lipid concentrations in middle-aged Japanese men. Nagoya J. Med. Sci. 2009, 71, 19–28. [Google Scholar]
- Chin, Y.T.; Lin, W.T.; Wu, P.W.; Tsai, S.; Lee, C.Y.; Seal, D.W.; Chen, T.; Huang, H.L.; Lee, C.H. Characteristic-grouped adiposity indicators for identifying metabolic syndrome in adolescents: Develop and valid risk screening tools using dual population. Nutrients 2020, 12, 3165. [Google Scholar] [CrossRef] [PubMed]
- Ghomari-Boukhatem, H.; Bouchouicha, A.; Mekki, K.; Chenni, K.; Belhadj, M.; Bouchenak, M. Blood pressure, dyslipidemia and inflammatory factors are related to body mass index in scholar adolescents. Arch. Med. Sci. 2017, 13, 46–52. [Google Scholar] [CrossRef] [PubMed]
- Mena-Sanchez, G.; Becerra-Tomas, N.; Babio, N.; Salas-Salvado, J. Dairy product consumption in the prevention of metabolic syndrome: A systematic review and meta-analysis of prospective cohort studies. Adv. Nutr. 2019, 10, S144–S153. [Google Scholar] [CrossRef] [PubMed]
- Li, S.; Cao, M.; Yang, C.; Zheng, H.; Zhu, Y. Association of sugar-sweetened beverage intake with risk of metabolic syndrome among children and adolescents in urban China. Public Health Nutr. 2020, 23, 2770–2780. [Google Scholar] [CrossRef] [PubMed]
- WHO. Global Recommendations on Physical Activity for Health; WHO Guidelines Approved by the Guidelines Review Committee; World Health Organization: Geneva, Switzerland, 2010. [Google Scholar]
- Jia, P.; Xue, H.; Cheng, X.; Wang, Y. Effects of school neighborhood food environments on childhood obesity at multiple scales: A longitudinal kindergarten cohort study in the USA. BMC Med. 2019, 17, 99. [Google Scholar] [CrossRef] [PubMed]

| Factors | Participant | Triglycerides | HDL Cholesterol | LDL Cholesterol | Total Cholesterol | ||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| n = 2727 | Mean | β a | pb | Mean | β a | pb | Mean | β a | pb | Mean | β a | pb | |
| Categorical factors | |||||||||||||
| Sex | |||||||||||||
| Boy | 48.7% | 75.78 | Ref. | 55.79 | Ref. | 87.98 | Ref. | 157.29 | Ref. | ||||
| Girl | 51.3% | 75.44 | −0.33 | 0.819 | 58.32 | 2.53 | <0.001 | 91.45 | 3.47 | 0.001 | 164.47 | 7.17 | <0.001 |
| Ethnicity | |||||||||||||
| Fukienese | 69.9% | 76.55 | Ref. | 57.92 | Ref. | 90.13 | Ref. | 161.90 | Ref. | ||||
| Hakka | 10.1% | 76.06 | −0.49 | 0.846 | 55.81 | −2.11 | 0.018 | 91.56 | 1.43 | 0.421 | 162.41 | 0.51 | 0.811 |
| Mainland | 10.8% | 80.82 | 4.27 | 0.084 | 58.69 | 0.77 | 0.377 | 91.74 | 1.61 | 0.352 | 164.27 | 2.36 | 0.250 |
| Aboriginal | 9.1% | 64.12 | −12.43 | <0.001 | 49.42 | −8.51 | <0.001 | 81.38 | −8.75 | <0.001 | 146.21 | −15.69 | <0.001 |
| Continuous factors | |||||||||||||
| Age, year | 13.43 ± 1.03 | −0.13 | 0.857 | −0.38 | 0.125 | −0.85 | 0.083 | −2.21 | <0.001 | ||||
| Daily calorie intake, × 103 kcal | 2.06 ± 0.69 | −0.19 | 0.857 | 0.02 | 0.966 | −0.73 | 0.321 | −1.34 | 0.126 | ||||
| Individual-Level Factors | Participant | Triglycerides | HDL Cholesterol | LDL Cholesterol | Total Cholesterol | ||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| n = 2727 | aMean a | adj.β a | pa | aMean a | adj.β a | pa | aMean a | adj.β a | pa | aMean a | adj.β a | pa | |
| Milk intake, serving | |||||||||||||
| <1 per week | 32.4% | 74.67 | Ref. | 56.49 | Ref. | 88.07 | Ref. | 158.77 | Ref. | ||||
| ≥1 per week | 67.6% | 76.10 | 1.42 | 0.374 | 57.54 | 1.06 | 0.061 | 90.73 | 2.67 | 0.018 | 162.32 | 3.55 | 0.007 |
| Dairy product intake, serving | |||||||||||||
| <1 per week | 54.4% | 76.10 | Ref. | 56.18 | Ref. | 89.49 | Ref. | 160.00 | Ref. | ||||
| ≥1 per week | 45.6% | 75.17 | −0.93 | 0.540 | 58.26 | 2.08 | <0.001 | 90.14 | 0.64 | 0.546 | 162.29 | 2.29 | 0.069 |
| Egg intake, serving | |||||||||||||
| <4 per week | 59.4% | 75.09 | Ref. | 56.85 | Ref. | 90.31 | Ref. | 161.11 | Ref. | ||||
| ≥4 per week | 40.6% | 76.00 | 0.91 | 0.557 | 57.70 | 0.84 | 0.125 | 89.25 | −1.06 | 0.329 | 161.26 | 0.15 | 0.904 |
| Meat intake, serving | |||||||||||||
| <4 per week | 52.6% | 75.58 | Ref. | 57.45 | Ref. | 89.47 | Ref. | 160.78 | Ref. | ||||
| ≥4 per week | 47.4% | 75.54 | −0.04 | 0.978 | 56.69 | −0.76 | 0.172 | 90.03 | 0.56 | 0.610 | 161.10 | 0.33 | 0.802 |
| Fresh fruit intake, serving | |||||||||||||
| <1 per week | 16.3% | 76.27 | Ref. | 56.31 | Ref. | 88.30 | Ref. | 159.33 | Ref. | ||||
| ≥1 per week | 83.7% | 75.53 | −0.74 | 0.710 | 57.27 | 0.96 | 0.172 | 90.06 | 1.76 | 0.205 | 161.34 | 2.02 | 0.219 |
| Fried food intake, serving | |||||||||||||
| <1 per week | 36.1% | 74.76 | Ref. | 57.04 | Ref. | 88.80 | Ref. | 159.87 | Ref. | ||||
| ≥1 per week | 63.9% | 76.20 | 1.44 | 0.373 | 57.04 | 0.00 | 0.999 | 90.28 | 1.48 | 0.184 | 161.49 | 1.63 | 0.218 |
| SSB intake, mL | |||||||||||||
| Non-intake | 11.6% | 74.66 | Ref. | 58.11 | Ref. | 86.80 | Ref. | 159.59 | Ref. | ||||
| 1–350 per day | 39.2% | 74.75 | 0.09 | 0.971 | 57.03 | −1.07 | 0.205 | 87.47 | 0.67 | 0.688 | 158.80 | −0.79 | 0.691 |
| 351–500 per day | 25.5% | 74.78 | 0.12 | 0.962 | 57.38 | −0.73 | 0.418 | 91.03 | 4.23 | 0.018 | 162.03 | 2.44 | 0.248 |
| >500 per day | 23.7% | 78.38 | 3.72 | 0.159 | 56.38 | −1.73 | 0.062 | 93.63 | 6.83 | < 0.001 | 164.11 | 4.52 | 0.037 |
| Physical activity, MET-min. | |||||||||||||
| ≥2140.5 per week | 32.9% | 72.37 | Ref. | 57.90 | Ref. | 88.03 | Ref. | 159.85 | Ref. | ||||
| 952.5–2140.5 per week | 42.9% | 76.80 | 4.43 | 0.010 | 56.87 | −1.03 | 0.088 | 89.98 | 1.95 | 0.104 | 161.03 | 1.18 | 0.405 |
| <952.5 per week | 24.2% | 77.89 | 5.52 | 0.007 | 56.37 | −1.54 | 0.031 | 91.71 | 3.67 | 0.009 | 162.40 | 2.55 | 0.128 |
| Body mass index b | 21.3 ± 4.5 | - | 2.66 | <0.001 | - | −0.84 | <0.001 | - | 1.36 | <0.001 | - | 0.71 | <0.001 |
| School-Level Factors | Participant | Triglycerides | HDL Cholesterol | LDL Cholesterol | Total Cholesterol | ||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| n = 2727 | aMean a | adj.β a | pa | aMean a | adj.β a | pa | aMean a | adj.β a | pa | aMean a | adj.β a | pa | |
| Health promotion program in school, no. | |||||||||||||
| 0–1 per year | 45.2% | 76.91 | Ref. | 59.57 | Ref. | 93.06 | Ref. | 166.28 | Ref. | ||||
| ≥2 per year | 54.8% | 74.53 | −2.39 | 0.108 | 55.04 | −4.53 | <0.001 | 87.04 | −6.02 | <0.001 | 156.60 | −9.68 | <0.001 |
| Food environment near the school | |||||||||||||
| Food outlet no. b | |||||||||||||
| 1–45 within 600 m | 49.1% | 71.83 | Ref. | 52.01 | Ref. | 87.44 | Ref. | 153.55 | Ref. | ||||
| 46–140 within 600 m | 20.7% | 83.54 | 11.70 | <0.001 | 60.55 | 8.54 | <0.001 | 92.23 | 4.79 | <0.001 | 168.82 | 15.27 | <0.001 |
| ≥141 within 600 m | 30.3% | 76.32 | 4.48 | 0.010 | 62.96 | 10.95 | <0.001 | 91.83 | 4.39 | <0.001 | 167.66 | 14.10 | <0.001 |
| Fast-food restaurant no. | |||||||||||||
| 0–1 within 600 m | 77.1% | 75.16 | Ref. | 55.62 | Ref. | 89.14 | Ref. | 159.31 | Ref. | ||||
| ≥2 within 600 m | 22.9% | 77.09 | 1.93 | 0.274 | 62.02 | 6.39 | <0.001 | 91.84 | 2.70 | 0.027 | 166.56 | 7.25 | <0.001 |
| Beverage shop no. | |||||||||||||
| 0–15 within 600 m | 49.4% | 71.90 | Ref. | 52.04 | Ref. | 87.48 | Ref. | 153.62 | Ref. | ||||
| ≥16 within 600 m | 50.6% | 79.22 | 7.31 | <0.001 | 62.01 | 9.97 | <0.001 | 91.98 | 4.51 | <0.001 | 168.14 | 14.52 | <0.001 |
| Eatery no. | |||||||||||||
| 0–40 within 600 m | 49.1% | 71.81 | Ref. | 52.02 | Ref. | 87.44 | Ref. | 153.55 | Ref. | ||||
| ≥41 within 600 m | 50.9% | 79.27 | 7.45 | <0.001 | 61.98 | 9.96 | <0.001 | 91.99 | 4.55 | <0.001 | 168.13 | 14.58 | <0.001 |
| Convenience store no. | |||||||||||||
| 0–5 within 600 m | 37.0% | 76.55 | Ref. | 54.30 | Ref. | 91.10 | Ref. | 160.20 | Ref. | ||||
| ≥6 within 600 m | 63.0% | 75.05 | −1.50 | 0.328 | 58.73 | 4.43 | <0.001 | 88.97 | −2.12 | 0.047 | 161.43 | 1.23 | 0.330 |
| Multilevel Effects | Model I a | Model II b | Model III c | |||
|---|---|---|---|---|---|---|
| Base Model | adj.β | (95% CI) | adj.β | (95% CI) | ||
| Fixed effects | ||||||
| Individual-level factors | ||||||
| Physical activity, MET-min/week | ||||||
| 952.5–2140.5 vs. ≥2140.5 | 3.72 | (0.58, 6.86) | 3.83 | (0.69, 6.97) | ||
| <952.5 vs. ≥2140.5 | 5.17 | (1.45, 8.90) | 5.25 | (1.53, 8.97) | ||
| Body mass index, 1-unit kg/m2 | 2.57 | (2.16, 2.97) | 2.59 | (2.18, 2.99) | ||
| School-level factors | ||||||
| Health promotion program, no./year | ||||||
| ≥2 vs. 0–1 | −1.11 | (−6.76, 4.54) | ||||
| Food outlet, no.within 600 m | ||||||
| ≥46 vs. 1–45 | 6.90 | (1.40, 12.39) | ||||
| Random effects | σ2 | (SE) | σ2 | (SE) | σ2 | (SE) |
| Variance between schools | 77.82 | (23.56) | 71.55 | (21.48) | 59.82 | (18.58) |
| Variance between individuals | 1340.99 | (36.57) | 1188.97 | (32.62) | 1187.82 | (32.59) |
| BMI-TG slope variance between schools | 0.64 * | (0.33) | 0.64 * | (0.33) | ||
| Covariance between intercept and slope | 4.31 * | (2.04) | 3.66 * | (1.92) | ||
| PCV explained by new model d | ||||||
| Between schools | Ref. | 8.1% | 23.1% | |||
| Between individuals | Ref. | 11.3% | 11.4% | |||
| Variance partition coefficient d | 0.055 | 0.057 | 0.048 | |||
| Multilevel Effects | Model I a | Model II b | Model III c | |||
|---|---|---|---|---|---|---|
| Base Model | adj.β | (95% CI) | adj.β | (95% CI) | ||
| Fixed effects | ||||||
| Individual-level factors | ||||||
| Dairy product intake, serving/week | ||||||
| ≥1 vs. <1 | 0.94 | (0.08, 1.80) | 0.92 | (0.06, 1.78) | ||
| Physical activity, MET-min/week | ||||||
| 952.5–2140.5 vs. 2140.5 | −0.47 | (−1.46, 0.52) | −0.48 | (−1.47, 0.51) | ||
| <952.5 vs. ≥2140.5 | −0.45 | (−1.63, 0.73) | −0.47 | (−1.65, 0.71) | ||
| Body mass index, 1-unit kg/m2 | −0.89 | (−0.98, −0.80) | −0.89 | (−0.98, −0.80) | ||
| School-level factors | ||||||
| Health promotion program, no./year | ||||||
| ≥2 vs. 0–1 | −4.53 | (−8.21, −0.84) | ||||
| Food outlet, no. within 600 m | ||||||
| 46–140 vs. 1–45 | 5.98 | (1.99, 9.96) | ||||
| ≥141 vs. 1–45 | 9.91 | (6.01, 13.80) | ||||
| Random effects | σ2 | (SE) | σ2 | (SE) | σ2 | (SE) |
| Variance between schools | 58.43 | (14.36) | 60.36 | (14.79) | 26.84 | (7.03) |
| Variance between individuals | 129.08 | (3.52) | 112.85 | (3.14) | 113.03 | (3.15) |
| PCV explained by new model | ||||||
| Between schools | Ref. | −3.3% | 54.1% | |||
| Between individuals | Ref. | 12.6% | 12.4% | |||
| Variance partition coefficient | 0.312 | 0.348 | 0.192 | |||
| LDL Cholesterol | Total Cholesterol | |||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|
| Multilevel Effects | Model I a | Model II b | Model III c | Model I a | Model II b | Model III c | ||||||
| Base model | adj.β | (95% CI) | adj.β | (95% CI) | Base model | adj.β | (95% CI) | adj.β | (95% CI) | |||
| Fixed effects | ||||||||||||
| Individual-level factors | ||||||||||||
| Milk intake, serving/week | ||||||||||||
| ≥1 vs. <1 | 3.05 | (0.97, 5.13) | 2.94 | (0.86, 5.02) | 3.19 | (0.83, 5.55) | 3.13 | (0.77, 5.49) | ||||
| SSB intake, mL/day | ||||||||||||
| 1–350 vs. non-intake | 1.35 | (−1.79, 4.49) | 1.52 | (−1.62, 4.66) | 1.62 | (−1.95, 5.18) | 1.73 | (−1.83, 5.29) | ||||
| 351–500 vs. non-intake | 4.12 | (0.76, 7.48) | 4.25 | (0.89, 7.60) | 4.65 | (0.84, 8.46) | 4.71 | (0.91, 8.52) | ||||
| >500 vs. non-intake | 5.87 | (2.40, 9.34) | 5.97 | (2.50, 9.45) | 6.00 | (2.07, 9.94) | 6.12 | (2.18, 10.05) | ||||
| Physical activity, MET-min./week | ||||||||||||
| 952.5–2140.5 vs. ≥2140.5 | 2.24 | (−0.03, 4.51) | 2.23 | (−0.05, 4.50) | 1.90 | (−0.67, 4.48) | 1.90 | (−0.67, 4.48) | ||||
| <952.5 vs. ≥2140.5 | 4.15 | (1.45, 6.84) | 4.16 | (1.47, 6.86) | 3.88 | (0.82, 6.94) | 3.86 | (0.80, 6.92) | ||||
| Body mass index, 1-unit kg/m2 | 1.27 | (1.06, 1.48) | 1.27 | (1.06, 1.48) | 0.53 | (0.29, 0.77) | 0.52 | (0.28, 0.76) | ||||
| School-level factors | ||||||||||||
| Health promotion program, no./year | ||||||||||||
| ≥2 vs. 0–1 | −5.27 | (−10.51, −0.02) | −8.36 | (−17.46, 0.75) | ||||||||
| Food outlet, no.within 600 m | ||||||||||||
| 46–140 vs. 1–45 | 3.92 | (−2.54, 10.37) | 13.2 | (3.13, 23.19) | ||||||||
| ≥141 vs. 1–45 | 4.23 | (−1.58, 10.04) | 13.3 | (3.66, 23.03) | ||||||||
| Random effects | σ2 | (SE) | σ2 | (SE) | σ2 | (SE) | σ2 | (SE) | σ2 | (SE) | σ2 | (SE) |
| Variance between schools | 67.20 | (18.63) | 61.22 | (17.18) | 48.49 | (14.11) | 247.21 | (61.97) | 241.90 | (60.83) | 162.59 | (42.10) |
| Variance between individuals | 630.88 | (17.21) | 594.33 | (16.53) | 593.85 | (16.52) | 777.93 | (21.21) | 762.92 | (21.21) | 762.77 | (21.21) |
| PCV explained by new model | ||||||||||||
| Between schools | Ref. | 8.9% | 27.8% | Ref. | 2.1% | 34.2% | ||||||
| Between individuals | Ref. | 5.8% | 5.9% | Ref. | 1.9% | 1.9% | ||||||
| Variance partition coefficient | 0.096 | 0.093 | 0.075 | 0.241 | 0.241 | 0.176 | ||||||
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Lin, W.-T.; Chin, Y.-T.; Wu, P.-W.; Tsai, S.; Chen, M.-H.; Chang, C.-I.; Yang, Y.-C.; Lee, C.-Y.; Seal, D.W.; Lee, C.-H. Multilevel Understanding of the Impact of Individual- and School-Level Determinants on Lipid Profiles in Adolescents: The Cross-Level Interaction of Food Environment and Body Mass Index. Nutrients 2022, 14, 2068. https://doi.org/10.3390/nu14102068
Lin W-T, Chin Y-T, Wu P-W, Tsai S, Chen M-H, Chang C-I, Yang Y-C, Lee C-Y, Seal DW, Lee C-H. Multilevel Understanding of the Impact of Individual- and School-Level Determinants on Lipid Profiles in Adolescents: The Cross-Level Interaction of Food Environment and Body Mass Index. Nutrients. 2022; 14(10):2068. https://doi.org/10.3390/nu14102068
Chicago/Turabian StyleLin, Wei-Ting, Yu-Ting Chin, Pei-Wen Wu, Sharon Tsai, Meng-Hsueh Chen, Chiao-I Chang, Yu-Cheng Yang, Chun-Ying Lee, David W. Seal, and Chien-Hung Lee. 2022. "Multilevel Understanding of the Impact of Individual- and School-Level Determinants on Lipid Profiles in Adolescents: The Cross-Level Interaction of Food Environment and Body Mass Index" Nutrients 14, no. 10: 2068. https://doi.org/10.3390/nu14102068
APA StyleLin, W.-T., Chin, Y.-T., Wu, P.-W., Tsai, S., Chen, M.-H., Chang, C.-I., Yang, Y.-C., Lee, C.-Y., Seal, D. W., & Lee, C.-H. (2022). Multilevel Understanding of the Impact of Individual- and School-Level Determinants on Lipid Profiles in Adolescents: The Cross-Level Interaction of Food Environment and Body Mass Index. Nutrients, 14(10), 2068. https://doi.org/10.3390/nu14102068






