Does a 12-Month Transitional Care Model Intervention by Geriatric-Experienced Care Professionals Improve Nutritional Status of Older Patients after Hospital Discharge? A Randomized Controlled Trial
Abstract
:1. Introduction
2. Materials and Methods
2.1. Trail Design, Registration, and Ethical Approvement
2.2. Participants
2.3. Randomization
2.4. Study Timeline
2.5. Study Staff
2.6. Pathfinders’ Educational Training
2.7. Intervention
2.8. Control Group
2.9. Data Collection
2.9.1. Participants’ Characteristics at Baseline
2.9.2. Nutritional Assessment
2.10. Outcome Measures
2.11. Power Calculation
2.12. Statistical Analysis
3. Results
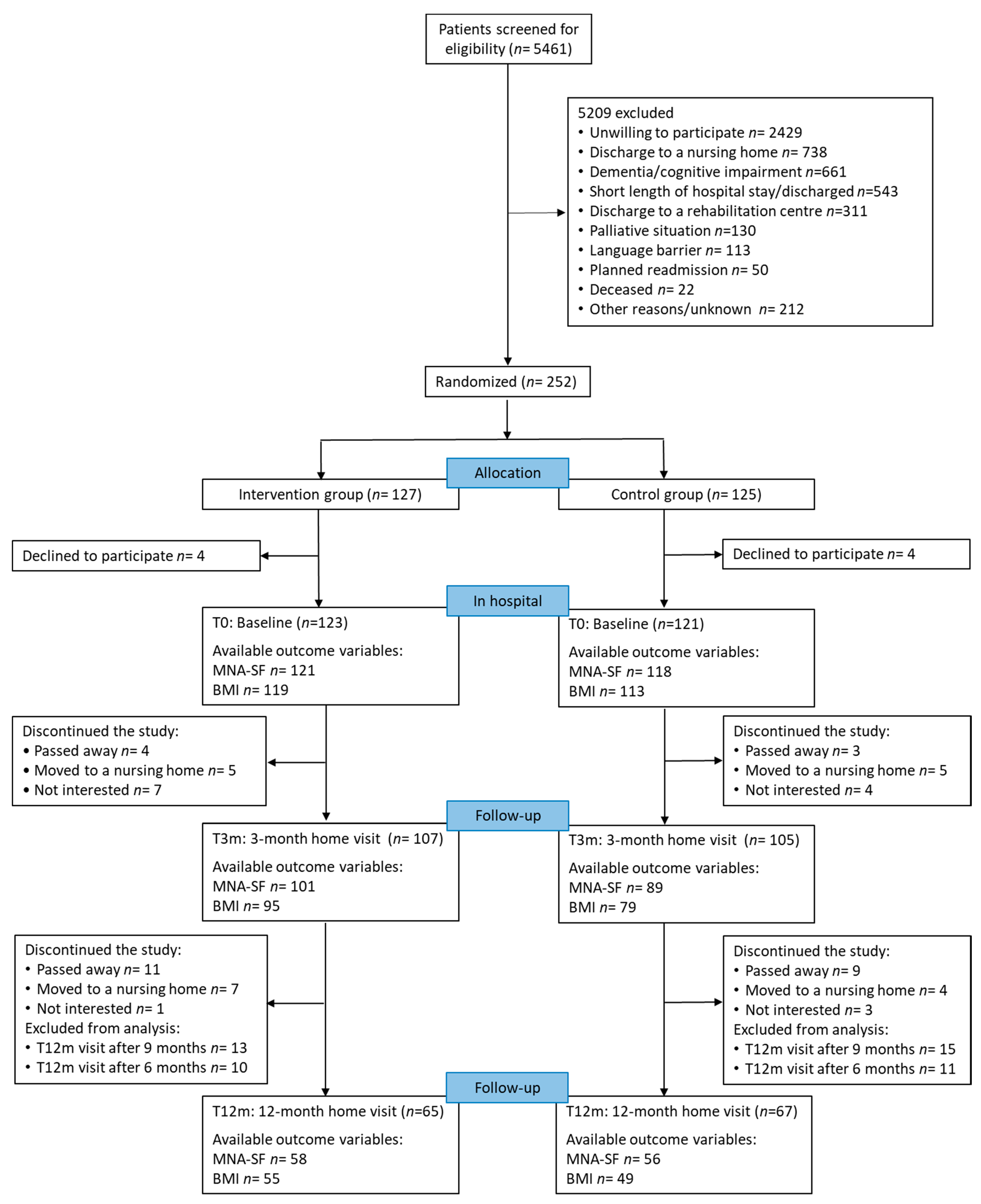
3.1. Participants’ Flow during the Study
3.2. Participants’ Characteristics at Hospital Discharge
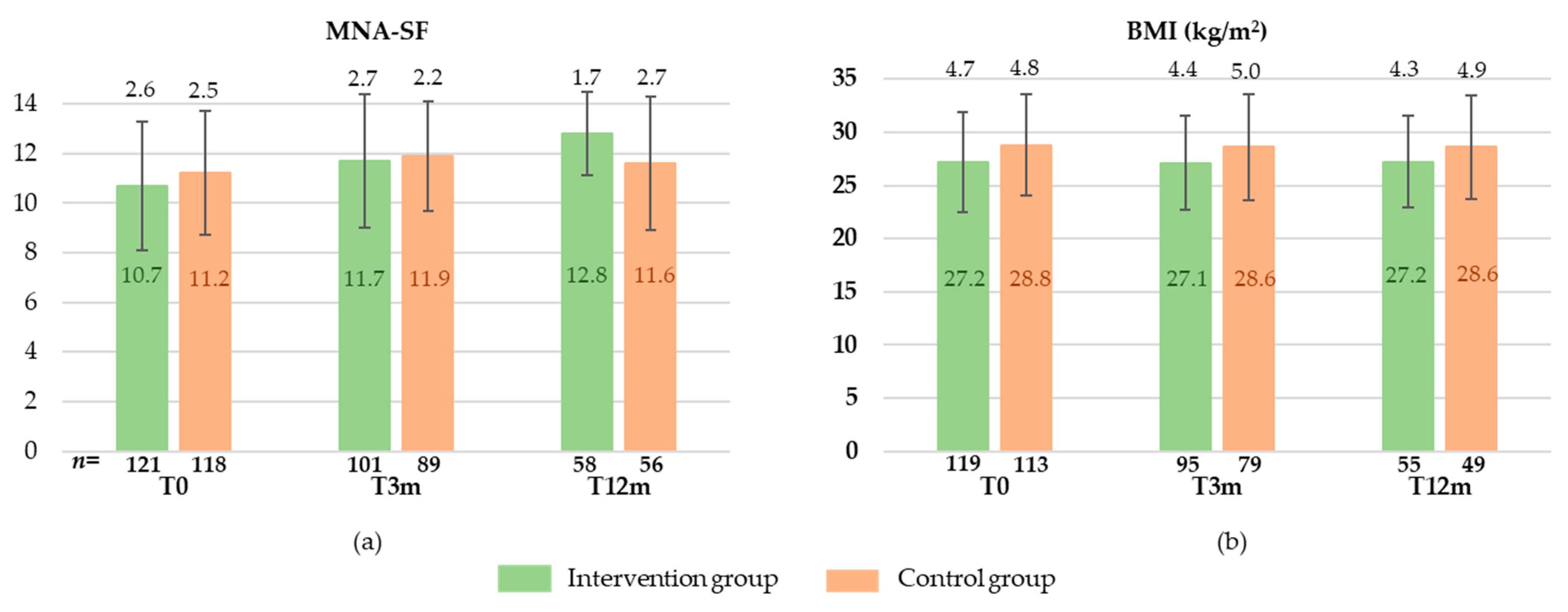
3.3. Nutritional Status
4. Discussion
Strengths and Limitations
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
Appendix A
| Not Drop-Out (181) | Drop-Out (63) | p | ||
|---|---|---|---|---|
| Age (years), median (P25–P75) | 80.0 (78.0–84.0) | 84.0 (79.0–89.0) | 0.001 | |
| Female, % | 58.0 | 50.8 | 0.320 | |
| Living situation: alone, % | 74.6 | 74.6 | 0.998 | |
| GDS, % | Severely depressed | 1.7 | 0.0 | 0.283 |
| Moderately depressed | 14.0 | 15.9 | ||
| No depression | 82.6 | 74.6 | ||
| Missing | 1.7 | 9.5 | ||
| Barthel-ADL, % | Severe limitation | 1.7 | 3.2 | 0.214 |
| Moderate limitation | 9.9 | 12.7 | ||
| Slight limitation | 86.7 | 77.8 | ||
| Missing | 1.7 | 6.3 | ||
| Number of medications/day [n] Median (P25–P75) | (175) 8.0 (5.0–11.0) | (53) 9.0 (6.0–12.0) | 0.398 | |
| BMI, % | Low (<22 kg/m2) | 7.2 | 9.5 | 0.063 |
| Normal (22–30 kg/m2) | 56.9 | 68.3 | ||
| High (≥30 kg/m2) | 31.5 | 15.9 | ||
| Missing | 4.4 | 6.3 | ||
| MNA-SF, % | Malnutrition | 12.7 | 11.1 | 0.013 |
| At risk of malnutrition | 33.1 | 50.8 | ||
| Well-nourished | 53.6 | 31.7 | ||
| Missing | 0.0 | 6.3 | ||
References
- Cereda, E.; Pedrolli, C.; Klersy, C.; Bonardi, C.; Quarleri, L.; Cappello, S.; Turri, A.; Rondanelli, M.; Caccialanza, R. Nutritional status in older persons according to healthcare setting: A systematic review and meta-analysis of prevalence data using MNA®. Clin. Nutr. 2016, 35, 1282–1290. [Google Scholar] [CrossRef]
- Pedersen, J.L.; Pedersen, P.U.; Damsgaard, E. Early nutritional follow-up after discharge prevents deterioration of ADL functions in malnourished, independent, geriatric patients who live alone–A randomized clinical trial. J. Nutr. Health Aging 2016, 20, 845–853. [Google Scholar] [CrossRef]
- Vearing, R.; Casey, S.; Zaremba, C.; Bowden, S.; Ferguson, A.; Goodisson, C.; Potter, J.; Evry, N.; Charlton, K. Evaluation of the impact of a post-hospital discharge Transitional Aged Care Service on frailty, malnutrition and functional ability. Nutr. Diet. 2019, 76, 472–479. [Google Scholar] [CrossRef]
- Kaiser, M.J.; Bauer, J.M.; Rämsch, C.; Uter, W.; Guigoz, Y.; Cederholm, T.; Thomas, D.R.; Anthony, P.S.; Charlton, K.E.; Maggio, M. Frequency of malnutrition in older adults: A multinational perspective using the mini nutritional assessment. J. Am. Geriatr. Soc. 2010, 58, 1734–1738. [Google Scholar] [CrossRef]
- Charlton, K.; Nichols, C.; Bowden, S.; Milosavljevic, M.; Lambert, K.; Barone, L.; Mason, M.; Batterham, M. Poor nutritional status of older subacute patients predicts clinical outcomes and mortality at 18 months of follow-up. Eur. J. Clin. Nutr. 2012, 66, 1224–1228. [Google Scholar] [CrossRef]
- Beck, A.M.; Kjær, S.; Hansen, B.S.; Storm, R.L.; Thal-Jantzen, K. Study protocol: Follow-up home visits with nutrition: A randomised controlled trial. BMC Geriatr. 2011, 11, 90. [Google Scholar] [CrossRef] [Green Version]
- Avelino-Silva, T.J.; Jaluul, O. Malnutrition in hospitalized older patients: Management strategies to improve patient care and clinical outcomes. Int. J. Gerontol. 2017, 11, 56–61. [Google Scholar] [CrossRef]
- Munk, T.; Svendsen, J.A.; Knudsen, A.W.; Østergaard, T.B.; Beck, A.M. Effect of nutritional interventions on discharged older patients: Study protocol for a randomized controlled trial. Trials 2020, 21, 365. [Google Scholar] [CrossRef] [PubMed]
- Beck, A.M.; Kjær, S.; Hansen, B.S.; Storm, R.L.; Thal-Jantzen, K.; Bitz, C. Follow-up home visits with registered dietitians have a positive effect on the functional and nutritional status of geriatric medical patients after discharge: A randomized controlled trial. Clin. Rehabil. 2013, 27, 483–493. [Google Scholar] [CrossRef] [PubMed]
- Beelen, J.; de Roos, N.M.; de Groot, L.C. A 12-week intervention with protein-enriched foods and drinks improved protein intake but not physical performance of older patients during the first 6 months after hospital release: A randomised controlled trial. Br. J. Nutr. 2017, 117, 1541–1549. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Ingstad, K.; Uhrenfeldt, L.; Kymre, I.G.; Skrubbeltrang, C.; Pedersen, P. Effectiveness of individualised nutritional care plans to reduce malnutrition during hospitalisation and up to 3 months post-discharge: A systematic scoping review. BMJ Open 2020, 10, e040439. [Google Scholar] [CrossRef]
- Sauer, A.C.; Alish, C.J.; Strausbaugh, K.; West, K.; Quatrara, B. Nurses needed: Identifying malnutrition in hospitalized older adults. Nurs. Open 2016, 2, 21–25. [Google Scholar] [CrossRef] [Green Version]
- Volkert, D.; Kiesswetter, E.; Cederholm, T.; Donini, L.M.; Eglseer, D.; Norman, K.; Schneider, S.M.; Ströbele-Benschop, N.; Torbahn, G.; Wirth, R. Development of a model on determinants of malnutrition in aged persons: A MaNuEL project. Gerontol. Geriatr. Med. 2019, 5, 2333721419858438. [Google Scholar] [CrossRef]
- Finlayson, K.; Chang, A.M.; Courtney, M.D.; Edwards, H.E.; Parker, A.W.; Hamilton, K.; Pham, T.D.X.; O’Brien, J. Transitional care interventions reduce unplanned hospital readmissions in high-risk older adults. BMC Health Serv. Res. 2018, 18, 956. [Google Scholar] [CrossRef] [Green Version]
- Naylor, M.D.; Brooten, D.A.; Campbell, R.L.; Maislin, G.; McCauley, K.M.; Schwartz, J.S. Transitional care of older adults hospitalized with heart failure: A randomized, controlled trial. J. Am. Geriatr. Soc. 2004, 52, 675–684. [Google Scholar] [CrossRef]
- Lehnert, O.; Müller, M.L. Neue Wege Im Entlassmanagement. Kosten Reduzieren, Erlöse Sichern, Versorgung Gestalten. Professional Process; 2011; pp. 26–31. [Google Scholar]
- Gesundheitswesen DDVfSAi. Entlassungsmanagement Durch Soziale Arbeit in Krankenhäusern und Rehabilitationskliniken; Deutsche Vereinigung für Soziale Arbeit im Gesundheitswesen e.V. (DVSG): Berlin, Germany, 2013. [Google Scholar]
- Naylor, M.; Brooten, D.; Jones, R.; Lavizzo-Mourey, R.; Mezey, M.; Pauly, M. Comprehensive discharge planning for the hospitalized elderly: A randomized clinical trial. Ann. Intern. Med. 1994, 120, 999–1006. [Google Scholar] [CrossRef]
- Morkisch, N.; Upegui-Arango, L.D.; Cardona, M.I.; van den Heuvel, D.; Rimmele, M.; Sieber, C.C.; Freiberger, E. Components of the transitional care model (TCM) to reduce readmission in geriatric patients: A systematic review. BMC Geriatr. 2020, 20, 1–18. [Google Scholar] [CrossRef] [PubMed]
- Rimmele, M.; Wirth, J.; Britting, S.; Gehr, T.; Hermann, M.; van den Heuvel, D.; Kestler, A.; Koch, T.; Schoeffski, O.; Volkert, D. Improvement of transitional care from hospital to home for older patients, the TIGER study: Protocol of a randomised controlled trial. BMJ Open 2021, 11, e037999. [Google Scholar] [CrossRef]
- Yesavage, J.A.; Brink, T.L.; Rose, T.L.; Lum, O.; Huang, V.; Adey, M.; Leirer, V.O. Development and validation of a geriatric depression screening scale: A preliminary report. J. Psychiatr. Res. 1982, 17, 37–49. [Google Scholar] [CrossRef]
- Mahoney, F.I.; Barthel, D.W. Functional evaluation: The Barthel Index: A simple index of independence useful in scoring improvement in the rehabilitation of the chronically ill. Md. State Med. J. 1965, 14, 61–65. [Google Scholar] [PubMed]
- Volkert, D.; Saeglitz, C.; Gueldenzoph, H.; Sieber, C.; Stehle, P. Undiagnosed malnutrition and nutrition-related problems in geriatric patients. J. Nutr. Health Aging 2010, 14, 387–392. [Google Scholar] [CrossRef] [PubMed]
- Vellas, B.; Guigoz, Y.; Garry, P.J.; Nourhashemi, F.; Bennahum, D.; Lauque, S.; Albarede, J.-L. The Mini Nutritional Assessment (MNA) and its use in grading the nutritional state of elderly patients. Nutrition 1999, 15, 116–122. [Google Scholar] [CrossRef]
- Cederholm, T.; Jensen, G.; Correia, M.I.T.; Gonzalez, M.C.; Fukushima, R.; Higashiguchi, T.; Baptista, G.; Barazzoni, R.; Blaauw, R.; Coats, A.J. GLIM criteria for the diagnosis of malnutrition–A consensus report from the global clinical nutrition community. J. Cachexia Sarcopenia Muscle 2019, 10, 207–217. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Beck, A.; Andersen, U.; Leedo, E.; Jensen, L.; Martins, K.; Quvang, M.; Rask, K.; Vedelspang, A.; Rønholt, F. Does adding a dietician to the liaison team after discharge of geriatric patients improve nutritional outcome: A randomised controlled trial. Clin. Rehabil. 2015, 29, 1117–1128. [Google Scholar] [CrossRef] [PubMed]
- Terp, R.; Jacobsen, K.O.; Kannegaard, P.; Larsen, A.-M.; Madsen, O.R.; Noiesen, E. A nutritional intervention program improves the nutritional status of geriatric patients at nutritional risk—a randomized controlled trial. Clin. Rehabil. 2018, 32, 930–941. [Google Scholar] [CrossRef] [PubMed]
- Feldblum, I.; German, L.; Castel, H.; Harman-Boehm, I.; Shahar, D.R. Individualized nutritional intervention during and after hospitalization: The nutrition intervention study clinical trial. J. Am. Geriatr. Soc. 2011, 59, 10–17. [Google Scholar] [CrossRef]
| Signs of Nutritional Problems | Possible Interventions |
|---|---|
|
|
|
|
|
|
|
|
|
|
|
|
| Variables | All Participants | Completed the 12-Month | |||||
|---|---|---|---|---|---|---|---|
| IG (121) | CG (118) | p | IG (58) | CG (56) | p | ||
| Age (years), median (P25–P75) | 82.0 (79.0–85.0) | 80.0 (77.7–84.0) | 0.042 | 81.5 (78.0–85.2) | 80.0 (77.0–82.7) | 0.031 | |
| Female, % | 55.4 | 56.8 | 0.826 | 55.2 | 64.3 | 0.321 | |
| Living situation: alone, % | 75.2 | 75.4 | 0.969 | 79.3 | 76.8 | 0.745 | |
| GDS, % | Severely depressed | 1.7 | 0.8 | 0.452 | 3.4 | 1.8 | 0.680 |
| Moderately depressed | 14.0 | 9.3 | 10.3 | 14.6 | |||
| No depression | 82.6 | 87.3 | 84.5 | 82.2 | |||
| Missing | 1.7 | 2.5 | 1.7 | 1.8 | |||
| Barthel-ADL, % | Severe limitation | 0.8 | 2.5 | 0.643 | 0.0 | 1.8 | 0.322 |
| Moderate limitation | 10.7 | 9.3 | 12.1 | 5.4 | |||
| Slight limitation | 87.6 | 88.1 | 87.9 | 92.9 | |||
| Missing | 0.8 | 0.0 | 0.0 | 0.0 | |||
| Number of medications/day, (n) median (P25–P75) | (111) 9.0 (6.0–11.0) | (115) 8.0 (5.0–11.0) | 0.158 | (53) 8.0 (6.0–10.0) | (56) 7.0 (5.0–12.0) | 0.865 | |
| BMI, % | Low (<22 kg/m2) | 10.7 | 5.1 | 0.182 | 8.6 | 5.4 | 0.196 |
| Normal (22–30 kg/m2) | 62.8 | 59.3 | 67.2 | 51.8 | |||
| High (≥30 kg/m2) | 24.8 | 31.4 | 24.1 | 37.5 | |||
| Missing | 1.7 | 4.2 | 0.0 | 5.4 | |||
| MNA-SF, % | Malnutrition | 13.2 | 11.9 | 0.704 | 12.1 | 16.1 | 0.798 |
| At risk of malnutrition | 40.5 | 36.4 | 37.9 | 33.9 | |||
| Well-nourished | 46.3 | 51.7 | 50.0 | 50.0 | |||
| Change from Baseline to T3m | p | Change from Baseline to T12m | p | ||||
|---|---|---|---|---|---|---|---|
| IG | CG | IG | CG | ||||
| MNA-SF | Total group | (101) 0.8 | (89) 0.7 | 0.783 | (58) 1.9 | (56) 0.5 | 0.017 |
| Model 1 | (0.3–1.4) | (0.1–1.4) | (1.2–2.6) | (−0.4–1.4) | |||
| Malnourished | (12) 4.3 | (11) 4.4 | (7) 6.0 | (9) 4.4 | |||
| (2.9–5.7) | (2.9–5.8) | (4.2–7.7) | (2.9–6.0) | ||||
| At risk of malnutrition | (39) 1.6 | (33) 1.8 | 0.645 | (22) 2.6 | (19) 1.3 | 0.921 | |
| (0.8–2.3) | (1.0–2.7) | (1.6–3.8) | (0.2–2.4) | ||||
| Well-nourished | (50) −0.5 | (45) −1.0 | (29) 0.4 | (28) −1.3 | |||
| (−1.2–0.1) | (−1.7–−0.2) | (−0.5–1.2) | (−2.2–−0.4) | ||||
| MNA-SF | Total group | (100) 0.6 | (89) 0.4 | 0.708 | (58) 1.4 | (56) 0.0 | 0.012 |
| Model 2 | (−0.1–1.3) | (−0.3–1.1) | (0.5–2.3) | (−0.9–0.8) | |||
| Malnourished | (12) 4.4 | (11) 4.3 | (7) 5.4 | (9) 4.1 | |||
| (2.9–5.8) | (2.8–5.9) | (3.8–7.1) | (2.6–5.6) | ||||
| At risk of malnutrition | (39) 1.5 | (33) 1.9 | 0.529 | (22) 2.4 | (19) 1.0 | 0.807 | |
| (0.7–2.3) | (1.0–2.7) | (1.3–3.2) | (0.0–2.0) | ||||
| Well-nourished | (49) −0.8 | (45) −1.3 | (29) −0.2 | (28) −1.9 | |||
| (−1.5–−0.1) | (−2.1–−0.7) | (−1.0–0.7) | (−2.8–−1.1) | ||||
| BMI | Total value | (95) −0.3 | (79) 0.0 | 0.233 | (55) 0.1 | (49) −0.7 | 0.058 |
| Model 1 | (−0.6–0.0) | (−0.4–0.4) | (−0.4–0.6) | (−1.3–0.0) | |||
| Low (<22 kg/m2) | (9) 0.5 | (5) 0.7 | (5) 2.0 | (3) 2.0 | |||
| (−0.5–1.5) | (−0.7–2.0) | (0.2–4.3) | (−0.2–4.3) | ||||
| Normal (22–30) | (60) −0.2 | (49) −0.2 | 0.297 | (36) 0.2 | (26) −0.6 | 0.815 | |
| (−0.6–0.2) | (−0.6–0.3) | (−0.5–0.8) | (−1.4–0.2) | ||||
| High (≥30) | (26) −0.7 | (25) 0.2 | (14) −0.8 | (20) −1.2 | |||
| (−1.3–−0.1) | (−0.4–0.8) | (−1.8–0.3) | (−2.1–−0.3) | ||||
| BMI | Total value | (94) −0.2 | (79) 0.0 | 0.29 | (55) 0.0 | (49) −0.9 | 0.034 |
| Model 2 | (−0.6–0.1) | (−0.4–0.4) | (−0.7–0.6) | (−1.6–−0.2) | |||
| Low (<22 kg/m2) | (9) 0.6 | (5) 0.7 | (5) 2.1 | (3) 1.6 | |||
| (−0.4–1.6) | (−0.7–2.1) | (0.3–3.9) | (−0.7–3.9) | ||||
| Normal (22–30) | (60) −0.2 | (49) −0.2 | 0.305 | (36) 0.0 | (26) −0.8 | 0.896 | |
| (−0.6–0.2) | (−0.6–0.3) | (−0.7–0.7) | (−1.6–0.0) | ||||
| High (≥30) | (25) −0.7 | (25) −0.1 | (14) −1.0 | (20) −1.4 | |||
| (−1.4–−0.1) | (−0.5–0.8) | (−2.2–0.2) | (−2.4–−0.5) | ||||
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Chareh, N.; Rappl, A.; Rimmele, M.; Wingenfeld, K.; Freiberger, E.; Sieber, C.C.; Volkert, D. Does a 12-Month Transitional Care Model Intervention by Geriatric-Experienced Care Professionals Improve Nutritional Status of Older Patients after Hospital Discharge? A Randomized Controlled Trial. Nutrients 2021, 13, 3023. https://doi.org/10.3390/nu13093023
Chareh N, Rappl A, Rimmele M, Wingenfeld K, Freiberger E, Sieber CC, Volkert D. Does a 12-Month Transitional Care Model Intervention by Geriatric-Experienced Care Professionals Improve Nutritional Status of Older Patients after Hospital Discharge? A Randomized Controlled Trial. Nutrients. 2021; 13(9):3023. https://doi.org/10.3390/nu13093023
Chicago/Turabian StyleChareh, Neshat, Anja Rappl, Martina Rimmele, Klaus Wingenfeld, Ellen Freiberger, Cornel C. Sieber, and Dorothee Volkert. 2021. "Does a 12-Month Transitional Care Model Intervention by Geriatric-Experienced Care Professionals Improve Nutritional Status of Older Patients after Hospital Discharge? A Randomized Controlled Trial" Nutrients 13, no. 9: 3023. https://doi.org/10.3390/nu13093023
APA StyleChareh, N., Rappl, A., Rimmele, M., Wingenfeld, K., Freiberger, E., Sieber, C. C., & Volkert, D. (2021). Does a 12-Month Transitional Care Model Intervention by Geriatric-Experienced Care Professionals Improve Nutritional Status of Older Patients after Hospital Discharge? A Randomized Controlled Trial. Nutrients, 13(9), 3023. https://doi.org/10.3390/nu13093023







