Towards a More Sustainable Nutrition: Complementary Feeding and Early Taste Experiences as a Basis for Future Food Choices
Abstract
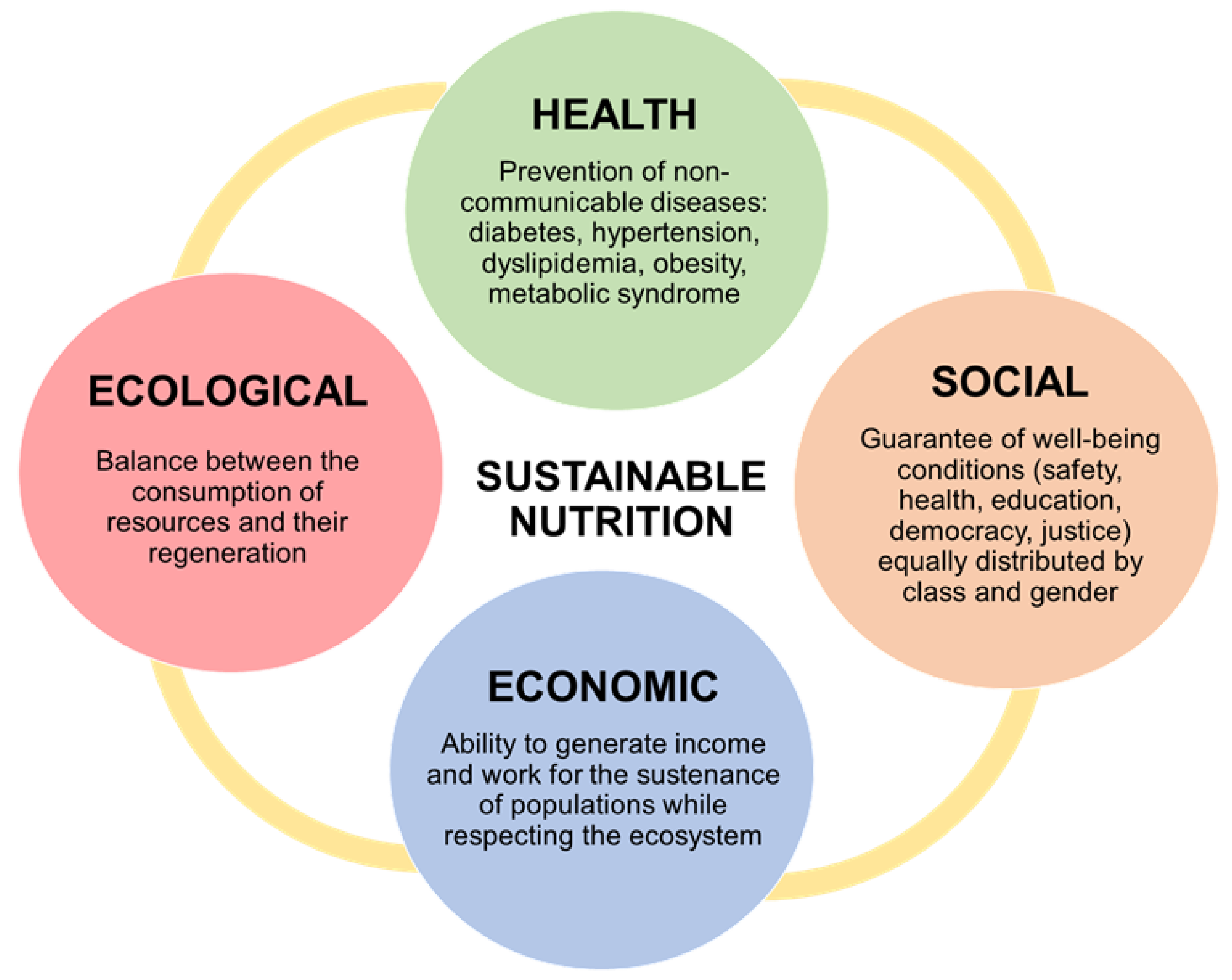
:1. Sustainable Nutrition: Definition and Principal Models
1.1. The Mediterranean Diet: Characteristic, Health and Ecological Outcomes
1.2. The New Nordic Diet: Characteristic, Health and Ecological Outcome
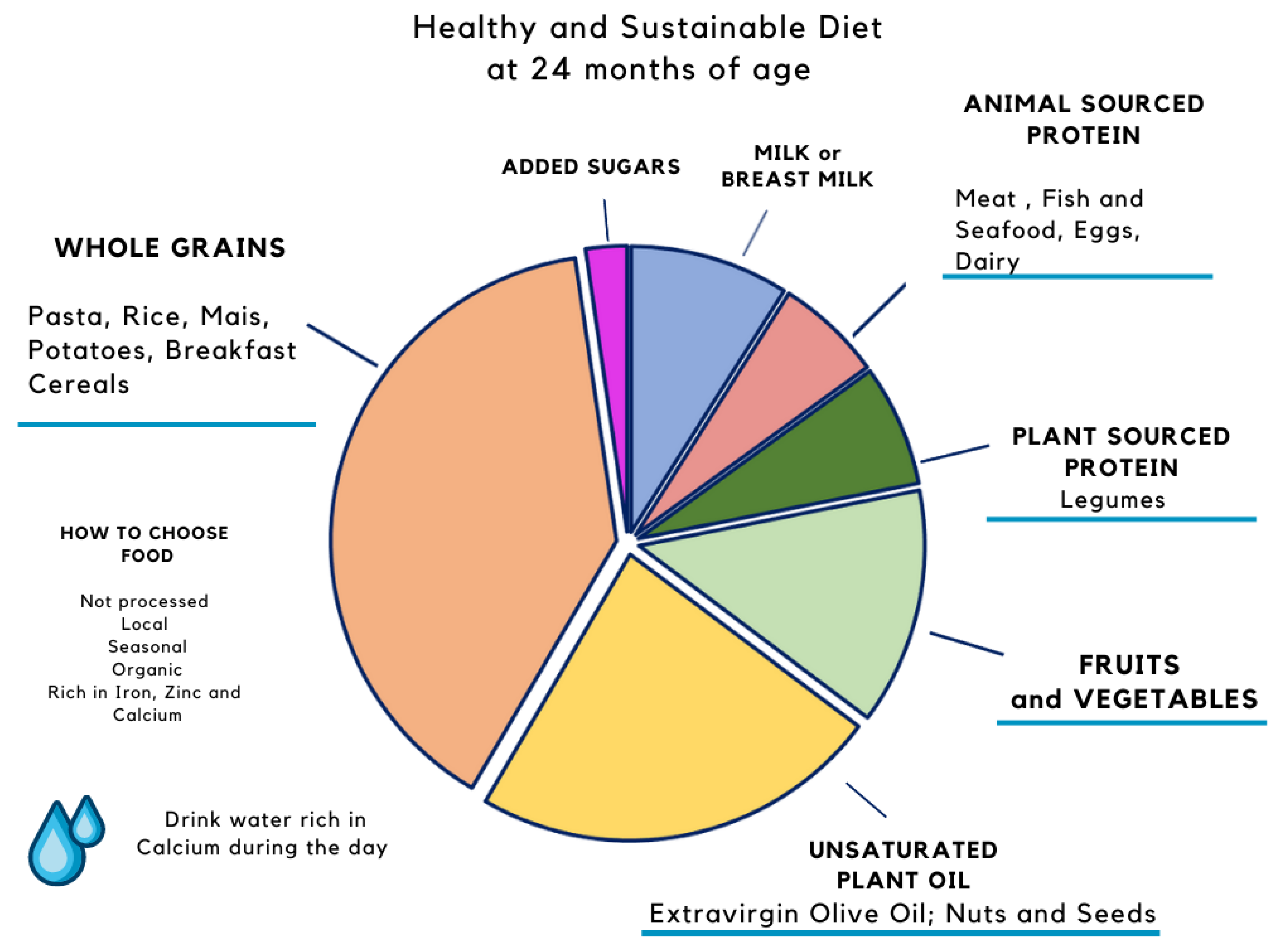
2. Complementary Feeding and Early-Life Experiences
2.1. Timing for Complementary Feeding
2.2. Child’s Taste Experiences
2.3. The Role of Family Environment
3. Tracking of Nutritional Habits and Cultural Values Connected to Sustainability
3.1. The Influence of Breastfeeding
3.2. The Influence of Parental Role
3.3. The Influence of Cultural Values
3.4. Early Taste Experiences and Later Food Preferences
3.5. The Adult Approach to a Sustainable Nutrition
4. Conclusions
Author Contributions
Funding
Conflicts of Interest
References
- Burlingame, B.; Dernini, S. Sustainable Diets and Biodiversity Directions and Solutions for Policy, Research and Action; FAO Headquarters: Rome, Italy, 2012. [Google Scholar]
- von Koerber, K.; Bader, N.; Leitzmann, C. Wholesome nutrition: An example for a sustainable diet. Proc. Nutr. Soc. 2017, 76, 34–41. [Google Scholar] [CrossRef] [Green Version]
- Hachem, F.; Vanham, D.; Moreno, L.A. Territorial and sustainable healthy diets. Food Nutr. Bull. 2020, 41, S87–S103. [Google Scholar] [CrossRef] [PubMed]
- Belahsen, R. Nutrition transition and food sustainability. Proc. Nutr. Soc. 2014, 73, 385–388. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Ulaszewska, M.M.; Luzzani, G.; Pignatelli, S.; Capri, E. Assessment of diet-related GHG emissions using the environmental hourglass approach for the Mediterranean and new Nordic diets. Sci. Total Environ. 2017, 574, 829–836. [Google Scholar] [CrossRef]
- Davis, C.; Bryan, J.; Hodgson, J.; Murphy, K. Definition of the Mediterranean diet; a literature review. Nutrients 2015, 7, 9139–9153. [Google Scholar] [CrossRef]
- Adamsson, V.; Reumark, A.; Fredriksson, I.B.; Hammarström, E.; Vessby, B.; Johansson, G.; Risérus, U. Effects of a healthy Nordic diet on cardiovascular risk factors in hypercholesterolaemic subjects: A randomized controlled trial (NORDIET). J. Intern. Med. 2011, 269, 150–159. [Google Scholar] [CrossRef] [PubMed]
- Sofi, F.; Abbate, R.; Gensini, G.F.; Casini, A. Accruing evidence on benefits of adherence to the Mediterranean diet on health: An updated systematic review and meta-analysis. Am. J. Clin. Nutr. 2010, 92, 1189–1196. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Bonaccio, M.; Pounis, G.; Cerletti, C.; Donati, M.B.; Iacoviello, L.; de Gaetano, G. Mediterranean diet, dietary polyphenols and low grade inflammation: Results from the MOLI-SANI study. Br. J. Clin. Pharmacol. 2017, 83, 107–113. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Toledo, E.; Salas-Salvadó, J.; Donat-Vargas, C.; Buil-Cosiales, P.; Estruch, R.; Ros, E.; Corella, D.; Fitó, M.; Hu, F.B.; Arós, F. Mediterranean diet and invasive breast cancer risk among women at high cardiovascular risk in the PREDIMED trial: A randomized clinical trial. JAMA Intern. Med. 2015, 175, 1752–1760. [Google Scholar] [CrossRef]
- Becerra-Tomás, N.; Blanco Mejía, S.; Viguiliouk, E.; Khan, T.; Kendall, C.W.; Kahleova, H.; Rahelić, D.; Sievenpiper, J.L.; Salas-Salvadó, J. Mediterranean diet, cardiovascular disease and mortality in diabetes: A systematic review and meta-analysis of prospective cohort studies and randomized clinical trials. Crit. Rev. Food Sci. Nutr. 2020, 60, 1207–1227. [Google Scholar] [CrossRef]
- Rosato, V.; Temple, N.J.; La Vecchia, C.; Castellan, G.; Tavani, A.; Guercio, V. Mediterranean diet and cardiovascular disease: A systematic review and meta-analysis of observational studies. Eur. J. Nutr. 2019, 58, 173–191. [Google Scholar] [CrossRef] [PubMed]
- Sayón-Orea, C.; Razquin, C.; Bulló, M.; Corella, D.; Fitó, M.; Romaguera, D.; Vioque, J.; Alonso-Gómez, Á.M.; Wärnberg, J.; Martínez, J.A. Effect of a nutritional and behavioral intervention on energy-reduced Mediterranean diet adherence among patients with metabolic syndrome: Interim analysis of the PREDIMED-Plus randomized clinical trial. JAMA 2019, 322, 1486–1499. [Google Scholar] [CrossRef]
- UNESCO. Convention for the Safeguarding of the Intangible Cultural Heritage, 9th Session. 2014. Available online: https://ich.unesco.org/en/8com (accessed on 30 June 2020).
- Dernini, S.; Berry, E.M. Mediterranean diet: From a healthy diet to a sustainable dietary pattern. Front. Nutr. 2015, 2, 15. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Serra-Majem, L.; Tomaino, L.; Dernini, S.; Berry, E.M.; Lairon, D.; Ngo de la Cruz, J.; Bach-Faig, A.; Donini, L.M.; Medina, F.-X.; Belahsen, R. Updating the mediterranean diet pyramid towards sustainability: Focus on environmental concerns. Int. J. Environ. Res. Public Health 2020, 17, 8758. [Google Scholar] [CrossRef] [PubMed]
- Mithril, C.; Dragsted, L.O.; Meyer, C.; Tetens, I.; Biltoft-Jensen, A.; Astrup, A. Dietary composition and nutrient content of the New Nordic Diet. Public Health Nutr. 2013, 16, 777–785. [Google Scholar] [CrossRef] [Green Version]
- Ramezani-Jolfaie, N.; Mohammadi, M.; Salehi-Abargouei, A. Effects of a healthy Nordic diet on weight loss in adults: A systematic review and meta-analysis of randomized controlled clinical trials. Eat. Weight Disord. 2019, 1–10. [Google Scholar] [CrossRef]
- Hansen, C.P.; Overvad, K.; Kyrø, C.; Olsen, A.; Tjønneland, A.; Johnsen, S.P.; Jakobsen, M.U.; Dahm, C.C. Adherence to a healthy Nordic diet and risk of stroke: A Danish cohort study. Stroke 2017, 48, 259–264. [Google Scholar] [CrossRef]
- Kanerva, N.; Harald, K.; Männistö, S.; Kaartinen, N.E.; Maukonen, M.; Haukkala, A.; Jousilahti, P. Adherence to the healthy Nordic diet is associated with weight change during 7 years of follow-up. Br. J. Nutr. 2018, 120, 101–110. [Google Scholar] [CrossRef] [Green Version]
- Poulsen, S.K.; Crone, C.; Astrup, A.; Larsen, T.M. Long-term adherence to the New Nordic Diet and the effects on body weight, anthropometry and blood pressure: A 12-month follow-up study. Eur. J. Nutr. 2015, 54, 67–76. [Google Scholar] [CrossRef]
- Skreden, M.; Hillesund, E.R.; Wills, A.K.; Brantsæter, A.L.; Bere, E.; Øverby, N.C. Adherence to the New Nordic Diet during pregnancy and subsequent maternal weight development: A study conducted in the Norwegian Mother and Child Cohort Study (MoBa). Br. J. Nutr. 2018, 119, 1286–1294. [Google Scholar] [CrossRef] [Green Version]
- Olsen, A.; Egeberg, R.; Halkjær, J.; Christensen, J.; Overvad, K.; Tjønneland, A. Healthy aspects of the Nordic diet are related to lower total mortality. J. Nutr. 2011, 141, 639–644. [Google Scholar] [CrossRef]
- Jalilpiran, Y.; Jayedi, A.; Djafarian, K.; Shab-Bidar, S. The Nordic diet and the risk of non-communicable chronic disease and mortality: A systematic review and dose-response meta-analysis of prospective cohort studies. Crit. Rev. Food Sci. Nutr. 2020, 1–13. [Google Scholar] [CrossRef]
- Damsgaard, C.T.; Dalskov, S.-M.; Laursen, R.P.; Ritz, C.; Hjorth, M.F.; Lauritzen, L.; Sørensen, L.B.; Petersen, R.A.; Andersen, M.R.; Stender, S. Provision of healthy school meals does not affect the metabolic syndrome score in 8–11-year-old children, but reduces cardiometabolic risk markers despite increasing waist circumference. Br. J. Nutr. 2014, 112, 1826–1836. [Google Scholar] [CrossRef] [Green Version]
- Andersen, R.; Biltoft-Jensen, A.; Christensen, T.; Andersen, E.W.; Ege, M.; Thorsen, A.V.; Dalskov, S.-M.; Damsgaard, C.T.; Astrup, A.; Michaelsen, K.F. Dietary effects of introducing school meals based on the New Nordic Diet–a randomised controlled trial in Danish children. The OPUS School Meal Study. Br. J. Nutr. 2014, 111, 1967–1976. [Google Scholar] [CrossRef] [Green Version]
- Renzella, J.; Townsend, N.; Jewell, J.; Breda, J.; Roberts, N.; Rayner, M.; Wickramasinghe, K. What National and Subnational Interventions and Policies Based on Mediterranean and Nordic Diets Are Recommended or Implemented in the WHO European Region, and Is There Evidence of Effectiveness in Reducing Noncommunicable Diseases? Health Evidence Network (HEN) Synthesis Report 58; WHO Regional Office for Europe: Copenhagen, Denmark, 2018. [Google Scholar]
- World Health Organization. Complementary Feeding: Report of the Global Consultation, and Summary of Guiding Principles for Complementary Feeding of the Breastfed Child; WHO: Geneva, Switzerland, 2002. [Google Scholar]
- Agostoni, C.; Decsi, T.; Fewtrell, M.; Goulet, O.; Kolacek, S.; Koletzko, B.; Michaelsen, K.F.; Moreno, L.; Puntis, J.; Rigo, J. Complementary feeding: A commentary by the ESPGHAN Committee on Nutrition. J. Pediatric Gastroenterol. Nutr. 2008, 46, 99–110. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Thompson, A.L.; Bentley, M.E. The critical period of infant feeding for the development of early disparities in obesity. Soc. Sci. Med. 2013, 97, 288–296. [Google Scholar] [CrossRef] [Green Version]
- Springmann, M.; Wiebe, K.; Mason-D’Croz, D.; Sulser, T.B.; Rayner, M.; Scarborough, P. Health and nutritional aspects of sustainable diet strategies and their association with environmental impacts: A global modelling analysis with country-level detail. Lancet Planet. Health 2018, 2, e451–e461. [Google Scholar] [CrossRef] [Green Version]
- Lind, T.; Johansson, U.; Öhlund, I.; Lindberg, L.; Lönnerdal, B.; Tennefors, C.; Hernell, O. Study protocol: Optimized complementary feeding study (OTIS): A randomized controlled trial of the impact of a protein-reduced complementary diet based on Nordic foods. BMC Public Health 2019, 19, 134. [Google Scholar] [CrossRef] [Green Version]
- Mikkilä, V.; Räsänen, L.; Raitakari, O.; Pietinen, P.; Viikari, J. Consistent dietary patterns identified from childhood to adulthood: The cardiovascular risk in Young Finns Study. Br. J. Nutr. 2005, 93, 923–931. [Google Scholar] [CrossRef] [PubMed]
- Sprake, E.F.; Russell, J.M.; Cecil, J.E.; Cooper, R.J.; Grabowski, P.; Pourshahidi, L.K.; Barker, M.E. Dietary patterns of university students in the UK: A cross-sectional study. Nutr. J. 2018, 17, 90. [Google Scholar] [CrossRef]
- Appannah, G.; Murray, K.; Trapp, G.; Dymock, M.; Oddy, W.H.; Ambrosini, G.L. Dietary pattern trajectories across adolescence and early adulthood and their associations with childhood and parental factors. Am. J. Clin. Nutr. 2020. [Google Scholar] [CrossRef]
- McEvoy, C.T.; Hoang, T.; Sidney, S.; Steffen, L.M.; Jacobs, D.R., Jr.; Shikany, J.M.; Wilkins, J.T.; Yaffe, K. Dietary patterns during adulthood and cognitive performance in midlife: The CARDIA study. Neurology 2019, 92, e1589–e1599. [Google Scholar] [CrossRef]
- Northstone, K.; Emmett, P.M. Are dietary patterns stable throughout early and mid-childhood? A birth cohort study. Br. J. Nutr. 2008, 100, 1069–1076. [Google Scholar] [CrossRef] [Green Version]
- Devine, C.M.; Connors, M.; Bisogni, C.A.; Sobal, J. Life-course influences on fruit and vegetable trajectories: Qualitative analysis of food choices. J. Nutr. Educ. 1998, 30, 361–370. [Google Scholar] [CrossRef]
- Skinner, J.D.; Carruth, B.R.; Bounds, W.; Ziegler, P.; Reidy, K. Do food-related experiences in the first 2 years of life predict dietary variety in school-aged children? J. Nutr. Educ. Behav. 2002, 34, 310–315. [Google Scholar] [CrossRef]
- Burnier, D.; Dubois, L.; Girard, M. Exclusive breastfeeding duration and later intake of vegetables in preschool children. Eur. J. Clin. Nutr. 2011, 65, 196–202. [Google Scholar] [CrossRef] [Green Version]
- Coulthard, H.; Harris, G.; Emmett, P. Long-term consequences of early fruit and vegetable feeding practices in the United Kingdom. Public Health Nutr. 2010, 13, 2044–2051. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Mennella, J.A.; Lukasewycz, L.D.; Castor, S.M.; Beauchamp, G.K. The timing and duration of a sensitive period in human flavor learning: A randomized trial. Am. J. Clin. Nutr. 2011, 93, 1019–1024. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Baird, J.; Fisher, D.; Lucas, P.; Kleijnen, J.; Roberts, H.; Law, C. Being big or growing fast: Systematic review of size and growth in infancy and later obesity. BMJ 2005, 331, 929. [Google Scholar] [CrossRef] [Green Version]
- Günther, A.L.; Buyken, A.E.; Kroke, A. Protein intake during the period of complementary feeding and early childhood and the association with body mass index and percentage body fat at 7 y of age. Am. J. Clin. Nutr. 2007, 85, 1626–1633. [Google Scholar] [CrossRef] [PubMed]
- Koletzko, B.; von Kries, R.; Closa, R.; Escribano, J.; Scaglioni, S.; Giovannini, M.; Beyer, J.; Demmelmair, H.; Gruszfeld, D.; Dobrzanska, A.; et al. Lower protein in infant formula is associated with lower weight up to age 2 y: A randomized clinical trial. Am. J. Clin. Nutr. 2009, 89, 1836–1845. [Google Scholar] [PubMed] [Green Version]
- Barker, D.J.; Osmond, C.; Forsén, T.J.; Kajantie, E.; Eriksson, J.G. Trajectories of growth among children who have coronary events as adults. N. Engl. J. Med. 2005, 353, 1802–1809. [Google Scholar] [CrossRef]
- Scaglioni, S.; De Cosmi, V.; Ciappolino, V.; Parazzini, F.; Brambilla, P.; Agostoni, C. Factors Influencing Children’s Eating Behaviours. Nutrients 2018, 10, 706. [Google Scholar] [CrossRef] [Green Version]
- Lioret, S.; McNaughton, S.A.; Spence, A.C.; Crawford, D.; Campbell, K.J. Tracking of dietary intakes in early childhood: The Melbourne InFANT Program. Eur. J. Clin. Nutr. 2013, 67, 275–281. [Google Scholar] [CrossRef] [PubMed]
- Gulev, R.E. Exploring cultural values connected to sustainability: Why some people are more likely to act in a sustainable manner than others. Int. J. Sustain. Econ. 2012, 4, 286–299. [Google Scholar] [CrossRef]
- De Cosmi, V.; Scaglioni, S.; Agostoni, C. Early Taste Experiences and Later Food Choices. Nutrients 2017, 9, 107. [Google Scholar] [CrossRef] [Green Version]
- Laura Censi, M.G.; Roccaldo, R.; Martone, D. Abitudini Alimentari e Stile di Vita Degli Adolescenti: Lo Studio ALIADO; CREA. Consiglio per la Ricerca in Agricoltura e l’Analisi dell’Economia Agraria: Roma, Italy, 2015. [Google Scholar]
- Cacau, L.T.; De Carli, E.; de Carvalho, A.M.; Lotufo, P.A.; Moreno, L.A.; Bensenor, I.M.; Marchioni, D.M. Development and Validation of an Index Based on EAT-Lancet Recommendations: The Planetary Health Diet Index. Nutrients 2021, 13, 1698. [Google Scholar] [CrossRef] [PubMed]

Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Mazzocchi, A.; De Cosmi, V.; Scaglioni, S.; Agostoni, C. Towards a More Sustainable Nutrition: Complementary Feeding and Early Taste Experiences as a Basis for Future Food Choices. Nutrients 2021, 13, 2695. https://doi.org/10.3390/nu13082695
Mazzocchi A, De Cosmi V, Scaglioni S, Agostoni C. Towards a More Sustainable Nutrition: Complementary Feeding and Early Taste Experiences as a Basis for Future Food Choices. Nutrients. 2021; 13(8):2695. https://doi.org/10.3390/nu13082695
Chicago/Turabian StyleMazzocchi, Alessandra, Valentina De Cosmi, Silvia Scaglioni, and Carlo Agostoni. 2021. "Towards a More Sustainable Nutrition: Complementary Feeding and Early Taste Experiences as a Basis for Future Food Choices" Nutrients 13, no. 8: 2695. https://doi.org/10.3390/nu13082695
APA StyleMazzocchi, A., De Cosmi, V., Scaglioni, S., & Agostoni, C. (2021). Towards a More Sustainable Nutrition: Complementary Feeding and Early Taste Experiences as a Basis for Future Food Choices. Nutrients, 13(8), 2695. https://doi.org/10.3390/nu13082695






