Alcohol and the Brain
Abstract
1. Structural and Volumetric Changes
1.1. Structural Alterations in Adults
1.2. Structural Alterations in Adolescents
1.3. Pre-Natal Alcohol Exposure
1.4. Conclusion
2. Neurotoxic Properties of Alcohol
2.1. Thiamine Deficiency
2.2. Neurotoxicity of Acetaldehyde
2.3. Alcohol and Neuroinflammation
2.4. Conclusion
3. Functional Brain Changes
3.1. Reward Processing
3.2. Impulsivity
3.3. Emotional Regulation
3.4. Resting State Functional Connectivity
3.5. Conclusion
4. Neurochemical Dysfunction in Alcoholism
4.1. Dopamine
4.2. GABA
4.3. Opioids
4.4. Other Neurochemical Systems
4.5. Conclusion
5. Summary
Funding
Conflicts of Interest
References
- Diagnostic and Statistical Manual of Mental Disorders: DSM-5TM, 5th ed.; American Psychiatric Publishing: Arlington, VA, USA, 2013; p. xliv.
- World Health Organization. Global Status Report on Alcohol and Health 2018; World Health Organization: Geneva, Switzerland, 2018. [Google Scholar]
- Weisner, C.; Matzger, H.; Kaskutas, L.A. How important is treatment? One-year outcomes of treated and untreated alcohol-dependent individuals. Addiction 2003, 98, 901–911. [Google Scholar]
- Kranzler, H.R.; Van Kirk, J. Efficacy of naltrexone and acamprosate for alcoholism treatment: A meta-analysis. Alcohol. Clin. Exp. Res. 2001, 25, 1335–1341. [Google Scholar] [CrossRef]
- Pettinati, H.M.; Rabinowitz, A.R. New pharmacotherapies for treating the neurobiology of alcohol and drug addiction. Psychiatry 2006, 3, 14. [Google Scholar]
- Akbar, M.; Egli, M.; Cho, Y.-E.; Song, B.-J.; Noronha, A. Medications for alcohol use disorders: An overview. Pharmacol. Ther. 2018, 185, 64–85. [Google Scholar] [CrossRef]
- Courville, C.B. Effects of Alcohol on the Nervous System of Man; San Lucas Press: Oxford, UK, 1955. [Google Scholar]
- Brewer, C.; Perrett, L. Brain damage due to alcohol consumption: An air-encephalographic, psychometric and electroencephalographic study. Br. J. Addict. 1971, 66, 170–182. [Google Scholar] [CrossRef]
- Jernigan, T.L.; Zatz, L.M.; Ahumada, A.J., Jr.; Pfefferbaum, A.; Tinklenberg, J.R.; Moses, J.A., Jr. CT measures of cerebrospinal fluid volume in alcoholics and normal volunteers. Psychiatry Res. 1982, 7, 9–17. [Google Scholar] [CrossRef]
- Pfefferbaum, A.; Rosenbloom, M.; Crusan, K.; Jernigan, T.L. Brain CT changes in alcoholics: Effects of age and alcohol consumption. Alcohol. Clin. Exp. Res. 1988, 12, 81–87. [Google Scholar] [CrossRef]
- Bühler, M.; Mann, K. Alcohol and the human brain: A systematic review of different neuroimaging methods. Alcohol. Clin. Exp. Res. 2011, 35, 1771–1793. [Google Scholar] [CrossRef]
- Chye, Y.; Mackey, S.; Gutman, B.A.; Ching, C.R.; Batalla, A.; Blaine, S.; Brooks, S.; Caparelli, E.C.; Cousijn, J.; Dagher, A. Subcortical surface morphometry in substance dependence: An ENIGMA addiction working group study. Addict. Biol. 2020, 25, e12830. [Google Scholar] [CrossRef]
- Mackey, S.; Allgaier, N.; Chaarani, B.; Spechler, P.; Orr, C.; Bunn, J.; Allen, N.B.; Alia-Klein, N.; Batalla, A.; Blaine, S. Mega-analysis of gray matter volume in substance dependence: General and substance-specific regional effects. Am. J. Psychiatry 2019, 176, 119–128. [Google Scholar] [CrossRef]
- Li, L.; Yu, H.; Liu, Y.; Meng, Y.-j.; Li, X.-j.; Zhang, C.; Liang, S.; Li, M.-l.; Guo, W.; Deng, W. Lower regional grey matter in alcohol use disorders: Evidence from a voxel-based meta-analysis. BMC Psychiatry 2021, 21, 1–11. [Google Scholar] [CrossRef] [PubMed]
- Xiao, P.; Dai, Z.; Zhong, J.; Zhu, Y.; Shi, H.; Pan, P. Regional gray matter deficits in alcohol dependence: A meta-analysis of voxel-based morphometry studies. Drug Alcohol Depend. 2015, 153, 22–28. [Google Scholar] [CrossRef]
- Yang, X.; Tian, F.; Zhang, H.; Zeng, J.; Chen, T.; Wang, S.; Jia, Z.; Gong, Q. Cortical and subcortical gray matter shrinkage in alcohol-use disorders: A voxel-based meta-analysis. Neurosci. Biobehav. Rev. 2016, 66, 92–103. [Google Scholar] [CrossRef] [PubMed]
- Monnig, M.A.; Tonigan, J.S.; Yeo, R.A.; Thoma, R.J.; McCrady, B.S. White matter volume in alcohol use disorders: A meta-analysis. Addict. Biol. 2013, 18, 581–592. [Google Scholar] [CrossRef]
- Hampton, W.H.; Hanik, I.M.; Olson, I.R. Substance abuse and white matter: Findings, limitations, and future of diffusion tensor imaging research. Drug Alcohol Depend. 2019, 197, 288–298. [Google Scholar] [CrossRef]
- Zahr, N.M.; Pitel, A.-L.; Chanraud, S.; Sullivan, E.V. Contributions of studies on alcohol use disorders to understanding cerebellar function. Neuropsychol. Rev. 2010, 20, 280–289. [Google Scholar] [CrossRef] [PubMed]
- Carlen, P.L.; Wortzman, G.; Holgate, R.; Wilkinson, D.; Rankin, J. Reversible cerebral atrophy in recently abstinent chronic alcoholics measured by computed tomography scans. Science 1978, 200, 1076–1078. [Google Scholar] [CrossRef]
- Ishikawa, Y.; Meyer, J.S.; Tanahashi, N.; Hata, T.; Velez, M.; Fann, W.E.; Kandula, P.; Motel, K.F.; Rogers, R.L. Abstinence improves cerebral perfusion and brain volume in alcoholic neurotoxicity without Wernicke-Korsakoff syndrome. J. Cereb. Blood Flow Metab. 1986, 6, 86–94. [Google Scholar] [CrossRef]
- Durazzo, T.C.; Mon, A.; Gazdzinski, S.; Yeh, P.-H.; Meyerhoff, D.J. Serial longitudinal MRI data indicates non-linear regional gray matter volume recovery in abstinent alcohol dependent individuals. Addict. Biol. 2015, 20, 956. [Google Scholar] [CrossRef]
- Gazdzinski, S.; Durazzo, T.C.; Meyerhoff, D.J. Temporal dynamics and determinants of whole brain tissue volume changes during recovery from alcohol dependence. Drug Alcohol Depend. 2005, 78, 263–273. [Google Scholar] [CrossRef]
- Zou, X.; Durazzo, T.C.; Meyerhoff, D.J. Regional brain volume changes in alcohol-dependent individuals during short-term and long-term abstinence. Alcohol. Clin. Exp. Res. 2018, 42, 1062–1072. [Google Scholar] [CrossRef]
- Meyerhoff, D.J.; Durazzo, T.C. Not all is lost for relapsers: Relapsers with low WHO risk drinking levels and complete abstainers have comparable regional gray matter volumes. Alcohol. Clin. Exp. Res. 2020, 44, 1479–1487. [Google Scholar] [CrossRef]
- Gazdzinski, S.; Durazzo, T.C.; Mon, A.; Yeh, P.-H.; Meyerhoff, D.J. Cerebral white matter recovery in abstinent alcoholics—A multimodality magnetic resonance study. Brain 2010, 133, 1043–1053. [Google Scholar] [CrossRef]
- Pfefferbaum, A.; Rosenbloom, M.J.; Chu, W.; Sassoon, S.A.; Rohlfing, T.; Pohl, K.M.; Zahr, N.M.; Sullivan, E.V. White matter microstructural recovery with abstinence and decline with relapse in alcohol dependence interacts with normal ageing: A controlled longitudinal DTI study. Lancet Psychiatry 2014, 1, 202–212. [Google Scholar] [CrossRef]
- Cardenas, V.A.; Durazzo, T.C.; Gazdzinski, S.; Mon, A.; Studholme, C.; Meyerhoff, D.J. Brain morphology at entry into treatment for alcohol dependence is related to relapse propensity. Biol. Psychiatry 2011, 70, 561–567. [Google Scholar] [CrossRef]
- Cardenas, V.A.; Studholme, C.; Gazdzinski, S.; Durazzo, T.C.; Meyerhoff, D.J. Deformation-based morphometry of brain changes in alcohol dependence and abstinence. Neuroimage 2007, 34, 879–887. [Google Scholar] [CrossRef]
- Durazzo, T.C.; Mon, A.; Gazdzinski, S.; Meyerhoff, D.J. Regional brain volume changes in alcohol-dependent individuals during early abstinence: Associations with relapse following treatment. Addict. Biol. 2017, 22, 1416–1425. [Google Scholar] [CrossRef]
- Zou, Y.; Murray, D.E.; Durazzo, T.C.; Schmidt, T.P.; Murray, T.A.; Meyerhoff, D.J. White matter microstructural correlates of relapse in alcohol dependence. Psychiatry Res. Neuroimaging 2018, 281, 92–100. [Google Scholar] [CrossRef]
- Oscar-Bemian, M.; Schendan, H.E. Asymmetries of brain function in alcoholism: Relationship to aging. In Neurobehavior of Language and Cognition; Springer: Berlin/Heidelberg, Germany, 2002; pp. 213–240. [Google Scholar]
- Guggenmos, M.; Schmack, K.; Sekutowicz, M.; Garbusow, M.; Sebold, M.; Sommer, C.; Smolka, M.N.; Wittchen, H.-U.; Zimmermann, U.S.; Heinz, A. Quantitative neurobiological evidence for accelerated brain aging in alcohol dependence. Transl. Psychiatry 2017, 7, 1–7. [Google Scholar] [CrossRef]
- Pfefferbaum, A.; Adalsteinsson, E.; Sullivan, E.V. Dysmorphology and microstructural degradation of the corpus callosum: Interaction of age and alcoholism. Neurobiol. Aging 2006, 27, 994–1009. [Google Scholar] [CrossRef]
- Pfefferbaum, A.; Lim, K.O.; Zipursky, R.B.; Mathalon, D.H.; Rosenbloom, M.J.; Lane, B.; Ha, C.N.; Sullivan, E.V. Brain gray and white matter volume loss accelerates with aging in chronic alcoholics: A quantitative MRI study. Alcohol. Clin. Exp. Res. 1992, 16, 1078–1089. [Google Scholar] [CrossRef]
- Sorg, S.F.; Squeglia, L.M.; Taylor, M.J.; Alhassoon, O.M.; Delano-Wood, L.M.; Grant, I. Effects of aging on frontal white matter microstructure in alcohol use disorder and associations with processing speed. J. Stud. Alcohol Drugs 2015, 76, 296–306. [Google Scholar] [CrossRef]
- Sullivan, E.V.; Zahr, N.M.; Sassoon, S.A.; Thompson, W.K.; Kwon, D.; Pohl, K.M.; Pfefferbaum, A. The role of aging, drug dependence, and hepatitis C comorbidity in alcoholism cortical compromise. JAMA Psychiatry 2018, 75, 474–483. [Google Scholar] [CrossRef]
- Thayer, R.E.; Hagerty, S.L.; Sabbineni, A.; Claus, E.D.; Hutchison, K.E.; Weiland, B.J. Negative and interactive effects of sex, aging, and alcohol abuse on gray matter morphometry. Hum. Brain Mapp. 2016, 37, 2276–2292. [Google Scholar] [CrossRef]
- Cole, J.H.; Franke, K. Predicting age using neuroimaging: Innovative brain ageing biomarkers. Trends Neurosci. 2017, 40, 681–690. [Google Scholar] [CrossRef]
- Kawano, Y. Physio-pathological effects of alcohol on the cardiovascular system: Its role in hypertension and cardiovascular disease. Hypertens. Res. 2010, 33, 181–191. [Google Scholar] [CrossRef]
- Kubota, M.; Nakazaki, S.; Hirai, S.; Saeki, N.; Yamaura, A.; Kusaka, T. Alcohol consumption and frontal lobe shrinkage: Study of 1432 non-alcoholic subjects. J. Neurol. Neurosurg. Psychiatry 2001, 71, 104–106. [Google Scholar] [CrossRef]
- McEvoy, L.K.; Fennema-Notestine, C.; Elman, J.A.; Eyler, L.T.; Franz, C.E.; Hagler, D.J., Jr.; Hatton, S.N.; Lyons, M.J.; Panizzon, M.S.; Dale, A.M. Alcohol intake and brain white matter in middle aged men: Microscopic and macroscopic differences. NeuroImage Clin. 2018, 18, 390–398. [Google Scholar] [CrossRef]
- Sachdev, P.S.; Chen, X.; Wen, W.; Anstry, K.J. Light to moderate alcohol use is associated with increased cortical gray matter in middle-aged men: A voxel-based morphometric study. Psychiatry Res. Neuroimaging 2008, 163, 61–69. [Google Scholar] [CrossRef]
- Daviet, R.; Aydogan, G.; Jagannathan, K.; Spilka, N.; Koellinger, P.D.; Kranzler, H.R.; Nave, G.; Wetherill, R.R. Multimodal brain imaging study of 36,678 participants reveals adverse effects of moderate drinking. bioRxiv 2021. [Google Scholar] [CrossRef]
- Morris, V.L.; Owens, M.M.; Syan, S.K.; Petker, T.D.; Sweet, L.H.; Oshri, A.; MacKillop, J.; Amlung, M. Associations between drinking and cortical thickness in younger adult drinkers: Findings from the Human Connectome Project. Alcohol. Clin. Exp. Res. 2019, 43, 1918–1927. [Google Scholar] [CrossRef] [PubMed]
- Topiwala, A.; Ebmeier, K.P.; Maullin-Sapey, T.; Nichols, T.E. No safe level of alcohol consumption for brain health: Observational cohort study of 25,378 UK Biobank participants. medRxiv 2021. [Google Scholar] [CrossRef]
- Topiwala, A.; Allan, C.L.; Valkanova, V.; Zsoldos, E.; Filippini, N.; Sexton, C.; Mahmood, A.; Fooks, P.; Singh-Manoux, A.; Mackay, C.E. Moderate alcohol consumption as risk factor for adverse brain outcomes and cognitive decline: Longitudinal cohort study. BMJ 2017, 357, j2353. [Google Scholar] [CrossRef]
- Ning, K.; Zhao, L.; Matloff, W.; Sun, F.; Toga, A.W. Association of relative brain age with tobacco smoking, alcohol consumption, and genetic variants. Sci. Rep. 2020, 10, 1–10. [Google Scholar] [CrossRef] [PubMed]
- Sowell, E.R.; Thompson, P.M.; Toga, A.W. Mapping changes in the human cortex throughout the span of life. Neurosci. 2004, 10, 372–392. [Google Scholar] [CrossRef]
- National Institute on Alcohol Abuse and Alcoholism. Drinking Levels Defined. Available online: https://www.niaaa.nih.gov/alcohol-health/overview-alcohol-consumption/moderate-binge-drinking (accessed on 1 November 2021).
- Lees, B.; Meredith, L.R.; Kirkland, A.E.; Bryant, B.E.; Squeglia, L.M. Effect of alcohol use on the adolescent brain and behavior. Pharmacol. Biochem. Behav. 2020, 192, 172906. [Google Scholar] [CrossRef]
- Pfefferbaum, A.; Kwon, D.; Brumback, T.; Thompson, W.K.; Cummins, K.; Tapert, S.F.; Brown, S.A.; Colrain, I.M.; Baker, F.C.; Prouty, D. Altered brain developmental trajectories in adolescents after initiating drinking. Am. J. Psychiatry 2018, 175, 370–380. [Google Scholar] [CrossRef] [PubMed]
- Sullivan, E.V.; Brumback, T.; Tapert, S.F.; Brown, S.A.; Baker, F.C.; Colrain, I.M.; Prouty, D.; De Bellis, M.D.; Clark, D.B.; Nagel, B.J. Disturbed cerebellar growth trajectories in adolescents who initiate alcohol drinking. Biol. Psychiatry 2020, 87, 632–644. [Google Scholar] [CrossRef]
- Squeglia, L.M.; Cservenka, A. Adolescence and drug use vulnerability: Findings from neuroimaging. Curr. Opin. Behav. Sci. 2017, 13, 164–170. [Google Scholar] [CrossRef]
- Jones, S.A.; Nagel, B.J. Altered frontostriatal white matter microstructure is associated with familial alcoholism and future binge drinking in adolescence. Neuropsychopharmacology 2019, 44, 1076–1083. [Google Scholar] [CrossRef]
- Weiland, B.J.; Korycinski, S.T.; Soules, M.; Zubieta, J.-K.; Zucker, R.A.; Heitzeg, M.M. Substance abuse risk in emerging adults associated with smaller frontal gray matter volumes and higher externalizing behaviors. Drug Alcohol Depend. 2014, 137, 68–75. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Nguyen, V.T.; Chong, S.; Tieng, Q.M.; Mardon, K.; Galloway, G.J.; Kurniawan, N.D. Radiological studies of fetal alcohol spectrum disorders in humans and animal models: An updated comprehensive review. Magn. Reson. Imaging 2017, 43, 10–26. [Google Scholar] [CrossRef] [PubMed]
- Treit, S.; Jeffery, D.; Beaulieu, C.; Emery, D. Radiological findings on structural magnetic resonance imaging in fetal alcohol spectrum disorders and healthy controls. Alcohol. Clin. Exp. Res. 2020, 44, 455–462. [Google Scholar] [CrossRef]
- Lebel, C.; Roussotte, F.; Sowell, E.R. Imaging the impact of prenatal alcohol exposure on the structure of the developing human brain. Neuropsychol. Rev. 2011, 21, 102–118. [Google Scholar] [CrossRef] [PubMed]
- O’Leary-Moore, S.K.; Parnell, S.E.; Lipinski, R.J.; Sulik, K.K. Magnetic resonance-based imaging in animal models of fetal alcohol spectrum disorder. Neuropsychol. Rev. 2011, 21, 167–185. [Google Scholar] [CrossRef]
- Martin, P.R.; Singleton, C.K.; Hiller-Sturmhöfel, S. The role of thiamine deficiency in alcoholic brain disease. Alcohol Res. Health 2003, 27, 134. [Google Scholar]
- Thomson, A.D. Mechanisms of vitamin deficiency in chronic alcohol misusers and the development of the Wernicke-Korsakoff syndrome. Alcohol Alcohol. 2000, 35, 2. [Google Scholar] [CrossRef]
- Thomson, A.D.; Marshall, E.J. The natural history and pathophysiology of Wernicke’s encephalopathy and Korsakoff’s psychosis. Alcohol Alcohol. 2006, 41, 151–158. [Google Scholar] [CrossRef]
- Behse, F.; Buchthal, F. Alcoholic neuropathy: Clinical, electrophysiological, and biopsy findings. Ann. Neurol. Off. J. Am. Neurol. Assoc. Child Neurol. Soc. 1977, 2, 95–110. [Google Scholar] [CrossRef]
- McLean, C.; Tapsell, L.; Grafenauer, S.; McMahon, A.T. Systematic review of nutritional interventions for people admitted to hospital for alcohol withdrawal. Nutr. Diet. 2020, 77, 76–89. [Google Scholar] [CrossRef] [PubMed]
- Thomson, A.D.; Baker, H.; Leevy, C.M. Patterns of 35S-thiamine hydrochloride absorption in the malnourished alcoholic patient. J. Lab. Clin. Med. 1970, 76, 34–45. [Google Scholar]
- Gastaldi, G.; Casirola, D.; Ferrari, G.; Rindi, G. Effect of chronic ethanol administration on thiamine transport in microvillous vesicles of rat small intestine. Alcohol Alcohol. 1989, 24, 83–89. [Google Scholar] [CrossRef] [PubMed]
- Reidling, J.C.; Said, H.M. Adaptive regulation of intestinal thiamin uptake: Molecular mechanism using wild-type and transgenic mice carrying hTHTR-1 and-2 promoters. Am. J. Physiol.-Gastrointest. Liver Physiol. 2005, 288, G1127–G1134. [Google Scholar] [CrossRef] [PubMed]
- Marcé-Grau, A.; Martí-Sánchez, L.; Baide-Mairena, H.; Ortigoza-Escobar, J.D.; Pérez-Dueñas, B. Genetic defects of thiamine transport and metabolism: A review of clinical phenotypes, genetics, and functional studies. J. Inherit. Metab. Dis. 2019, 42, 581–597. [Google Scholar] [CrossRef]
- Traviesa, D. Magnesium deficiency: A possible cause of thiamine refractoriness in Wernicke-Korsakoff encephalopathy. J. Neurol. Neurosurg. Psychiatry 1974, 37, 959–962. [Google Scholar] [CrossRef]
- Bates, M.E.; Bowden, S.C.; Barry, D. Neurocognitive impairment associated with alcohol use disorders: Implications for treatment. Exp. Clin. Psychopharmacol. 2002, 10, 193. [Google Scholar] [CrossRef] [PubMed]
- Pitel, A.L.; Rivier, J.; Beaunieux, H.; Vabret, F.; Desgranges, B.; Eustache, F. Changes in the episodic memory and executive functions of abstinent and relapsed alcoholics over a 6-month period. Alcohol. Clin. Exp. Res. 2009, 33, 490–498. [Google Scholar] [CrossRef]
- Oscar-Berman, M.; Marinković, K. Alcohol: Effects on neurobehavioral functions and the brain. Neuropsychol. Rev. 2007, 17, 239–257. [Google Scholar] [CrossRef]
- Brion, M.; Pitel, A.-L.; Beaunieux, H.; Maurage, P. Revisiting the continuum hypothesis: Toward an in-depth exploration of executive functions in korsakoff syndrome. Front. Hum. Neurosci. 2014, 8, 498. [Google Scholar] [CrossRef] [PubMed]
- Guo, R.; Ren, J. Alcohol and Acetaldehyde in Public Health: From Marvel to Menace. Int. J. Environ. Res. Public Health 2010, 7, 1285–1301. [Google Scholar] [CrossRef]
- Niemelä, O. Distribution of ethanol-induced protein adducts in vivo: Relationship to tissue injury. Free Radic. Biol. Med. 2001, 31, 1533–1538. [Google Scholar] [CrossRef]
- Quertemont, E.; Eriksson, C.J.P.; Zimatkin, S.M.; Pronko, P.S.; Diana, M.; Pisano, M.; Rodd, Z.A.; Bell, R.R.; Ward, R.J. Is Ethanol a Pro-Drug? Acetaldehyde Contribution to Brain Ethanol Effects. Alcohol. Clin. Exp. Res. 2005, 29, 1514–1521. [Google Scholar] [CrossRef]
- Eriksson, C.J.P. The Role of Acetaldehyde in the Actions of Alcohol (Update 2000). Alcohol. Clin. Exp. Res. 2001, 25, 15S–32S. [Google Scholar] [CrossRef]
- Takeuchi, M.; Saito, T. Cytotoxicity of Acetaldehyde-Derived Advanced Glycation End-Products (AA-AGE) in Alcoholic-Induced Neuronal Degeneration. Alcohol. Clin. Exp. Res. 2005, 29, 220S–224S. [Google Scholar] [CrossRef] [PubMed]
- Ferrier, L.; Bérard, F.; Debrauwer, L.; Chabo, C.; Langella, P.; Buéno, L.; Fioramonti, J. Impairment of the intestinal barrier by ethanol involves enteric microflora and mast cell activation in rodents. Am. J. Pathol. 2006, 168, 1148–1154. [Google Scholar] [CrossRef] [PubMed]
- Crews, F.T.; Sarkar, D.K.; Qin, L.; Zou, J.; Boyadjieva, N.; Vetreno, R.P. Neuroimmune function and the consequences of alcohol exposure. Alcohol Res. Curr. Rev. 2015, 37, 331. [Google Scholar]
- He, J.; Crews, F.T. Increased MCP-1 and microglia in various regions of the human alcoholic brain. Exp. Neurol. 2008, 210, 349–358. [Google Scholar] [CrossRef] [PubMed]
- Lovinger, D.M.; White, G.; Weight, F.F. Ethanol inhibits NMDA-activated ion current in hippocampal neurons. Science 1989, 243, 1721–1724. [Google Scholar] [CrossRef]
- Fliegel, S.; Brand, I.; Spanagel, R.; Noori, H.R. Ethanol-induced alterations of amino acids measured by in vivo microdialysis in rats: A meta-analysis. Silico Pharmacol. 2013, 1, 7. [Google Scholar] [CrossRef] [PubMed]
- Ward, R.J.; Lallemand, F.; de Witte, P. Biochemical and neurotransmitter changes implicated in alcohol-induced brain damage in chronic or ‘binge drinking’ alcohol abuse. Alcohol Alcohol 2009, 44, 128–135. [Google Scholar] [CrossRef]
- Munhoz, C.D.; Sorrells, S.F.; Caso, J.R.; Scavone, C.; Sapolsky, R.M. Glucocorticoids Exacerbate Lipopolysaccharide-Induced Signaling in the Frontal Cortex and Hippocampus in a Dose-Dependent Manner. J. Neurosci. 2010, 30, 13690. [Google Scholar] [CrossRef]
- Socodato, R.; Portugal, C.C.; Canedo, T.; Domith, I.; Oliveira, N.A.; Paes-de-Carvalho, R.; Relvas, J.B.; Cossenza, M. c-Src deactivation by the polyphenol 3-O-caffeoylquinic acid abrogates reactive oxygen species-mediated glutamate release from microglia and neuronal excitotoxicity. Free Radic. Biol. Med. 2015, 79, 45–55. [Google Scholar] [CrossRef] [PubMed]
- Henriques, J.F.; Portugal, C.C.; Canedo, T.; Relvas, J.B.; Summavielle, T.; Socodato, R. Microglia and alcohol meet at the crossroads: Microglia as critical modulators of alcohol neurotoxicity. Toxicol. Lett. 2018, 283, 21–31. [Google Scholar] [CrossRef]
- Alfonso-Loeches, S.; Pascual-Lucas, M.; Blanco, A.M.; Sanchez-Vera, I.; Guerri, C. Pivotal Role of TLR4 Receptors in Alcohol-Induced Neuroinflammation and Brain Damage. J. Neurosci. 2010, 30, 8285–8295. [Google Scholar] [CrossRef] [PubMed]
- McClain, J.A.; Morris, S.A.; Deeny, M.A.; Marshall, S.A.; Hayes, D.M.; Kiser, Z.M.; Nixon, K. Adolescent binge alcohol exposure induces long-lasting partial activation of microglia. Brain Behav. Immun. 2011, 25 (Suppl. 1), S120–S128. [Google Scholar] [CrossRef] [PubMed]
- Zhao, Y.N.; Wang, F.; Fan, Y.X.; Ping, G.F.; Yang, J.Y.; Wu, C.F. Activated microglia are implicated in cognitive deficits, neuronal death, and successful recovery following intermittent ethanol exposure. Behav. Brain Res. 2013, 236, 270–282. [Google Scholar] [CrossRef] [PubMed]
- Stowell, R.D.; Majewska, A.K. Acute ethanol exposure rapidly alters cerebellar and cortical microglial physiology. Eur. J. Neurosci. 2020, 54, 5834–5843. [Google Scholar] [CrossRef]
- Ward, R.J.; Lallemand, F.; de Witte, P. Influence of adolescent heavy session drinking on the systemic and brain innate immune system. Alcohol Alcohol 2014, 49, 193–197. [Google Scholar] [CrossRef]
- Qin, L.; He, J.; Hanes, R.N.; Pluzarev, O.; Hong, J.S.; Crews, F.T. Increased systemic and brain cytokine production and neuroinflammation by endotoxin following ethanol treatment. J. Neuroinflamm. 2008, 5, 10. [Google Scholar] [CrossRef]
- Saba, W.; Goutal, S.; Auvity, S.; Kuhnast, B.; Coulon, C.; Kouyoumdjian, V.; Buvat, I.; Leroy, C.; Tournier, N. Imaging the neuroimmune response to alcohol exposure in adolescent baboons: A TSPO PET study using 18F-DPA-714. Addict. Biol. 2018, 23, 1000–1009. [Google Scholar] [CrossRef]
- Hillmer, A.T.; Sandiego, C.M.; Hannestad, J.; Angarita, G.A.; Kumar, A.; McGovern, E.M.; Huang, Y.; O’Connor, K.C.; Carson, R.E.; O’Malley, S.S.; et al. In vivo imaging of translocator protein, a marker of activated microglia, in alcohol dependence. Mol. Psychiatry 2017, 22, 1759–1766. [Google Scholar] [CrossRef]
- Kalk, N.; Guo, Q.; Owen, D.; Cherian, R.; Erritzoe, D.; Gilmour, A.; Ribeiro, A.; McGonigle, J.; Waldman, A.; Matthews, P. Decreased hippocampal translocator protein (18 kDa) expression in alcohol dependence: A [11C] PBR28 PET study. Transl. Psychiatry 2017, 7, e996. [Google Scholar] [CrossRef]
- Knutson, B.; Adams, C.M.; Fong, G.W.; Hommer, D. Anticipation of increasing monetary reward selectively recruits nucleus accumbens. J. Neurosci. 2001, 21, RC159. [Google Scholar] [CrossRef]
- Courtney, K.E.; Schacht, J.P.; Hutchison, K.; Roche, D.J.; Ray, L.A. Neural substrates of cue reactivity: Association with treatment outcomes and relapse. Addict. Biol. 2016, 21, 3–22. [Google Scholar] [CrossRef] [PubMed]
- Luijten, M.; Schellekens, A.F.; Kühn, S.; Machielse, M.W.; Sescousse, G. Disruption of reward processing in addiction: An image-based meta-analysis of functional magnetic resonance imaging studies. JAMA Psychiatry 2017, 74, 387–398. [Google Scholar] [CrossRef]
- Bach, P.; Weil, G.; Pompili, E.; Hoffmann, S.; Hermann, D.; Vollstädt-Klein, S.; Mann, K.; Perez-Ramirez, U.; Moratal, D.; Canals, S. Incubation of neural alcohol cue reactivity after withdrawal and its blockade by naltrexone. Addict. Biol. 2020, 25, e12717. [Google Scholar] [CrossRef] [PubMed]
- Vollstädt-Klein, S.; Wichert, S.; Rabinstein, J.; Bühler, M.; Klein, O.; Ende, G.; Hermann, D.; Mann, K. Initial, habitual and compulsive alcohol use is characterized by a shift of cue processing from ventral to dorsal striatum. Addiction 2010, 105, 1741–1749. [Google Scholar] [CrossRef] [PubMed]
- Everitt, B.J.; Robbins, T.W. Neural systems of reinforcement for drug addiction: From actions to habits to compulsion. Nat. Neurosci. 2005, 8, 1481–1489. [Google Scholar] [CrossRef]
- Büchel, C.; Peters, J.; Banaschewski, T.; Bokde, A.L.; Bromberg, U.; Conrod, P.J.; Flor, H.; Papadopoulos, D.; Garavan, H.; Gowland, P. Blunted ventral striatal responses to anticipated rewards foreshadow problematic drug use in novelty-seeking adolescents. Nat. Commun. 2017, 8, 1–11. [Google Scholar] [CrossRef]
- Dager, A.D.; Anderson, B.M.; Rosen, R.; Khadka, S.; Sawyer, B.; Jiantonio-Kelly, R.E.; Austad, C.S.; Raskin, S.A.; Tennen, H.; Wood, R.M. Functional magnetic resonance imaging (fMRI) response to alcohol pictures predicts subsequent transition to heavy drinking in college students. Addiction 2014, 109, 585–595. [Google Scholar] [CrossRef] [PubMed]
- Mitchell, M.R.; Potenza, M.N. Recent insights into the neurobiology of impulsivity. Curr. Addict. Rep. 2014, 1, 309–319. [Google Scholar] [CrossRef]
- De Wit, H. Impulsivity as a determinant and consequence of drug use: A review of underlying processes. Addict. Biol. 2009, 14, 22–31. [Google Scholar] [CrossRef]
- Leigh, B.C. Peril, chance, adventure: Concepts of risk, alcohol use and risky behavior in young adults. Addiction 1999, 94, 371–383. [Google Scholar] [CrossRef]
- Taylor, E.M.; Murphy, A.; Boyapati, V.; Ersche, K.D.; Flechais, R.; Kuchibatla, S.; McGonigle, J.; Metastasio, A.; Nestor, L.; Orban, C. Impulsivity in abstinent alcohol and polydrug dependence: A multidimensional approach. Psychopharmacology 2016, 233, 1487–1499. [Google Scholar] [CrossRef]
- Norman, A.L.; Pulido, C.; Squeglia, L.M.; Spadoni, A.D.; Paulus, M.P.; Tapert, S.F. Neural activation during inhibition predicts initiation of substance use in adolescence. Drug Alcohol Depend. 2011, 119, 216–223. [Google Scholar] [CrossRef]
- Wetherill, R.R.; Squeglia, L.M.; Yang, T.T.; Tapert, S.F. A longitudinal examination of adolescent response inhibition: Neural differences before and after the initiation of heavy drinking. Psychopharmacology 2013, 230, 663–671. [Google Scholar] [CrossRef] [PubMed]
- Kirby, K.N.; Maraković, N.N. Delay-discounting probabilistic rewards: Rates decrease as amounts increase. Psychon. Bull. Rev. 1996, 3, 100–104. [Google Scholar] [CrossRef] [PubMed]
- Ortner, C.N.; MacDonald, T.K.; Olmstead, M.C. Alcohol intoxication reduces impulsivity in the delay-discounting paradigm. Alcohol Alcohol. 2003, 38, 151–156. [Google Scholar] [CrossRef]
- Dougherty, D.M.; Marsh-Richard, D.M.; Hatzis, E.S.; Nouvion, S.O.; Mathias, C.W. A test of alcohol dose effects on multiple behavioral measures of impulsivity. Drug Alcohol Depend. 2008, 96, 111–120. [Google Scholar] [CrossRef]
- McCarthy, D.M.; Niculete, M.E.; Treloar, H.R.; Morris, D.H.; Bartholow, B.D. Acute alcohol effects on impulsivity: Associations with drinking and driving behavior. Addiction 2012, 107, 2109–2114. [Google Scholar] [CrossRef] [PubMed]
- Herman, A.M.; Duka, T. Facets of impulsivity and alcohol use: What role do emotions play? Neurosci. Biobehav. Rev. 2019, 106, 202–216. [Google Scholar] [CrossRef] [PubMed]
- Gowin, J.L.; Vatsalya, V.; Westman, J.G.; Schwandt, M.L.; Bartlett, S.; Heilig, M.; Momenan, R.; Ramchandani, V.A. The effect of varenicline on the neural processing of fearful faces and the subjective effects of alcohol in heavy drinkers. Alcohol. Clin. Exp. Res. 2016, 40, 979–987. [Google Scholar] [CrossRef] [PubMed]
- Zhang, R.; Volkow, N.D. Brain default-mode network dysfunction in addiction. Neuroimage 2019, 200, 313–331. [Google Scholar] [CrossRef] [PubMed]
- Orban, C.; McGonigle, J.; Flechais, R.S.; Paterson, L.M.; Elliott, R.; Erritzoe, D.; Ersche, K.D.; Murphy, A.; Nestor, L.J.; Passetti, F. Chronic alcohol exposure differentially modulates structural and functional properties of amygdala: A cross-sectional study. Addict. Biol. 2021, 26, e12980. [Google Scholar] [CrossRef]
- Beck, A.; Wüstenberg, T.; Genauck, A.; Wrase, J.; Schlagenhauf, F.; Smolka, M.N.; Mann, K.; Heinz, A. Effect of brain structure, brain function, and brain connectivity on relapse in alcohol-dependent patients. Arch. Gen. Psychiatry 2012, 69, 842–852. [Google Scholar] [CrossRef]
- Erritzoe, D.; Zafar, R.; Nutt, D. Meta-analysis and systematic review of the dopamine DRD2/3 receptors in Addiction. Manuscript in prep.
- Volkow, N.D.; Wang, G.-J.; Telang, F.; Fowler, J.S.; Logan, J.; Jayne, M.; Ma, Y.; Pradhan, K.; Wong, C. Profound decreases in dopamine release in striatum in detoxified alcoholics: Possible orbitofrontal involvement. J. Neurosci. 2007, 27, 12700–12706. [Google Scholar] [CrossRef] [PubMed]
- Volkow, N.D.; Wiers, C.E.; Shokri-Kojori, E.; Tomasi, D.; Wang, G.-J.; Baler, R. Neurochemical and metabolic effects of acute and chronic alcohol in the human brain: Studies with positron emission tomography. Neuropharmacology 2017, 122, 175–188. [Google Scholar] [CrossRef]
- Heinz, A.; Siessmeier, T.; Wrase, J.; Hermann, D.; Klein, S.; Grüsser-Sinopoli, S.M.; Flor, H.; Braus, D.F.; Buchholz, H.G.; Gründer, G. Correlation between dopamine D2 receptors in the ventral striatum and central processing of alcohol cues and craving. Am. J. Psychiatry 2004, 161, 1783–1789. [Google Scholar] [CrossRef]
- Gilman, S.; Adams, K.M.; Johnson-Greene, D.; Koeppe, R.A.; Junck, L.; Kluin, K.J.; Martorello, S.; Heumann, M.; Hill, E. Effects of disulfiram on positron emission tomography and neuropsychological studies in severe chronic alcoholism. Alcohol. Clin. Exp. Res. 1996, 20, 1456–1461. [Google Scholar] [CrossRef] [PubMed]
- Heinz, A.; Siessmeier, T.; Wrase, J.; Buchholz, H.G.; Gründer, G.; Kumakura, Y.; Cumming, P.; Schreckenberger, M.; Smolka, M.N.; Rösch, F. Correlation of alcohol craving with striatal dopamine synthesis capacity and D2/3 receptor availability: A combined [18F] DOPA and [18F] DMFP PET study in detoxified alcoholic patients. Am. J. Psychiatry 2005, 162, 1515–1520. [Google Scholar] [CrossRef]
- Rominger, A.; Cumming, P.; Xiong, G.; Koller, G.; Böning, G.; Wulff, M.; Zwergal, A.; Förster, S.; Reilhac, A.; Munk, O. [18F] fallypride PET measurement of striatal and extrastriatal dopamine D2/3 receptor availability in recently abstinent alcoholics. Addict. Biol. 2012, 17, 490–503. [Google Scholar] [CrossRef] [PubMed]
- Repo, E.; Kuikka, J.T.; Bergström, K.A.; Karhu, J.; Hiltunen, J.; Tiihonen, J.; Kuikka, J. Dopamine transporter and D2-receptor density in late-onset alcoholism. Psychopharmacology 1999, 147, 314–318. [Google Scholar] [CrossRef]
- Narendran, R.; Mason, N.S.; Paris, J.; Himes, M.L.; Douaihy, A.B.; Frankle, W.G. Decreased prefrontal cortical dopamine transmission in alcoholism. Am. J. Psychiatry 2014, 171, 881–888. [Google Scholar] [CrossRef] [PubMed]
- Erritzoe, D.; Tziortzi, A.; Bargiela, D.; Colasanti, A.; Searle, G.E.; Gunn, R.N.; Beaver, J.D.; Waldman, A.; Nutt, D.J.; Bani, M. In vivo imaging of cerebral dopamine D3 receptors in alcoholism. Neuropsychopharmacology 2014, 39, 1703–1712. [Google Scholar] [CrossRef]
- Murphy, A.; Nestor, L.J.; McGonigle, J.; Paterson, L.; Boyapati, V.; Ersche, K.D.; Flechais, R.; Kuchibatla, S.; Metastasio, A.; Orban, C. Acute D3 antagonist GSK598809 selectively enhances neural response during monetary reward anticipation in drug and alcohol dependence. Neuropsychopharmacology 2017, 42, 1049–1057. [Google Scholar] [CrossRef] [PubMed]
- Zafar, R.; Wall, M.; Erritzoe, D.; Nutt, D. Role of D3 Receptor antagonism in alcohol dependence: A combined PET/MRI investigation. Manuscript in prep.
- Martinez, D.; Gil, R.; Slifstein, M.; Hwang, D.-R.; Huang, Y.; Perez, A.; Kegeles, L.; Talbot, P.; Evans, S.; Krystal, J. Alcohol dependence is associated with blunted dopamine transmission in the ventral striatum. Biol. Psychiatry 2005, 58, 779–786. [Google Scholar] [CrossRef]
- Begleiter, H.; Porjesz, B. What is inherited in the predisposition toward alcoholism? A proposed model. Alcohol. Clin. Exp. Res. 1999, 23, 1125–1135. [Google Scholar] [CrossRef] [PubMed]
- Abi-Dargham, A.; Krystal, J.H.; Anjilvel, S.; Scanley, B.E.; Zoghbi, S.; Baldwin, R.M.; Rajeevan, N.; Ellis, S.; Petrakis, I.L.; Seibyl, J.P. Alterations of benzodiazepine receptors in type II alcoholic subjects measured with SPECT and [123I] iomazenil. Am. J. Psychiatry 1998, 155, 1550–1555. [Google Scholar] [CrossRef]
- Lingford-Hughes, A.R.; Acton, P.; Gacinovic, S.; Suckling, J.; Busatto, G.; Boddington, S.; Bullmore, E.; Woodruff, P.; Costa, D.; Pilowsky, L. Reduced levels of GABA-benzodiazepine receptor in alcohol dependency in the absence of grey matter atrophy. Br. J. Psychiatry 1998, 173, 116–122. [Google Scholar] [CrossRef] [PubMed]
- Lingford-Hughes, A.; Wilson, S.; Cunningham, V.J.; Feeney, A.; Stevenson, B.; Brooks, D.; Nutt, D.J. GABA-benzodiazepine receptor function in alcohol dependence: A combined 11 C-flumazenil PET and pharmacodynamic study. Psychopharmacology 2005, 180, 595–606. [Google Scholar] [CrossRef]
- Lingford-Hughes, A.; Reid, A.G.; Myers, J.; Feeney, A.; Hammers, A.; Taylor, L.G.; Rosso, L.; Turkheimer, F.; Brooks, D.J.; Grasby, P. A [11C] Ro15 4513 PET study suggests that alcohol dependence in man is associated with reduced α5 benzodiazepine receptors in limbic regions. J. Psychopharmacol. 2012, 26, 273–281. [Google Scholar] [CrossRef] [PubMed]
- Volkow, N.D.; Wang, G.J.; Begleiter, H.; Hitzemann, R.; Pappas, N.; Burr, G.; Pascani, K.; Wong, C.; Fowler, J.S.; Wolf, A.P. Regional brain metabolic response to lorazepam in subjects at risk for alcoholism. Alcohol. Clin. Exp. Res. 1995, 19, 510–516. [Google Scholar] [CrossRef] [PubMed]
- Weerts, E.M.; Wand, G.S.; Kuwabara, H.; Munro, C.A.; Dannals, R.F.; Hilton, J.; Frost, J.J.; McCaul, M.E. Positron emission tomography imaging of mu-and delta-opioid receptor binding in alcohol-dependent and healthy control subjects. Alcohol. Clin. Exp. Res. 2011, 35, 2162–2173. [Google Scholar] [CrossRef]
- Mitchell, J.M.; O’Neil, J.P.; Janabi, M.; Marks, S.M.; Jagust, W.J.; Fields, H.L. Alcohol consumption induces endogenous opioid release in the human orbitofrontal cortex and nucleus accumbens. Sci. Transl. Med. 2012, 4, 116ra116. [Google Scholar] [CrossRef] [PubMed]
- Heinz, A.; Reimold, M.; Wrase, J.; Hermann, D.; Croissant, B.; Mundle, G.; Dohmen, B.M.; Braus, D.H.; Schumann, G.; Machulla, H.-J. Correlation of stable elevations in striatal μ-opioid receptor availability in detoxified alcoholic patients with alcohol craving: A positron emission tomography study using carbon 11–labeled carfentanil. Arch. Gen. Psychiatry 2005, 62, 57–64. [Google Scholar] [CrossRef]
- Hermann, D.; Hirth, N.; Reimold, M.; Batra, A.; Smolka, M.N.; Hoffmann, S.; Kiefer, F.; Noori, H.R.; Sommer, W.H.; Reischl, G. Low μ-opioid receptor status in alcohol dependence identified by combined positron emission tomography and post-mortem brain analysis. Neuropsychopharmacology 2017, 42, 606–614. [Google Scholar] [CrossRef]
- Mann, K.; Torup, L.; Sørensen, P.; Gual, A.; Swift, R.; Walker, B.; van den Brink, W. Nalmefene for the management of alcohol dependence: Review on its pharmacology, mechanism of action and meta-analysis on its clinical efficacy. Eur. Neuropsychopharmacol. 2016, 26, 1941–1949. [Google Scholar] [CrossRef]
- Parsons, L.H.; Hurd, Y.L. Endocannabinoid signalling in reward and addiction. Nat. Rev. Neurosci. 2015, 16, 579–594. [Google Scholar] [CrossRef] [PubMed]
- Neumeister, A.; Normandin, M.D.; Murrough, J.W.; Henry, S.; Bailey, C.R.; Luckenbaugh, D.A.; Tuit, K.; Zheng, M.Q.; Galatzer-Levy, I.R.; Sinha, R. Positron emission tomography shows elevated cannabinoid CB 1 receptor binding in men with alcohol dependence. Alcohol. Clin. Exp. Res. 2012, 36, 2104–2109. [Google Scholar] [CrossRef]
- Hirvonen, J.; Zanotti-Fregonara, P.; Umhau, J.C.; George, D.T.; Rallis-Frutos, D.; Lyoo, C.H.; Li, C.-T.; Hines, C.S.; Sun, H.; Terry, G.E. Reduced cannabinoid CB 1 receptor binding in alcohol dependence measured with positron emission tomography. Mol. Psychiatry 2013, 18, 916–921. [Google Scholar] [CrossRef]
- Brown, A.K.; George, D.T.; Fujita, M.; Liow, J.S.; Ichise, M.; Hibbeln, J.; Ghose, S.; Sangare, J.; Hommer, D.; Innis, R.B. PET [11C] DASB imaging of serotonin transporters in patients with alcoholism. Alcohol. Clin. Exp. Res. 2007, 31, 28–32. [Google Scholar] [CrossRef] [PubMed]
- Szabo, Z.; Owonikoko, T.; Peyrot, M.; Varga, J.; Mathews, W.B.; Ravert, H.T.; Dannals, R.F.; Wand, G. Positron emission tomography imaging of the serotonin transporter in subjects with a history of alcoholism. Biol. Psychiatry 2004, 55, 766–771. [Google Scholar] [CrossRef] [PubMed]
- Martinez, D.; Slifstein, M.; Gil, R.; Hwang, D.-R.; Huang, Y.; Perez, A.; Frankle, W.G.; Laruelle, M.; Krystal, J.; Abi-Dargham, A. Positron emission tomography imaging of the serotonin transporter and 5-HT1A receptor in alcohol dependence. Biol. Psychiatry 2009, 65, 175–180. [Google Scholar] [CrossRef] [PubMed]
- Kumar, J.; Ismail, Z.; Hatta, N.H.; Baharuddin, N.; Hapidin, H.; Get Bee, Y.-T.; Yap, E.; Pakri Mohamed, R.M. Alcohol addiction-metabotropic glutamate receptor subtype 5 and its Ligands: How They All Come Together? Curr. Drug Targets 2018, 19, 907–915. [Google Scholar] [CrossRef] [PubMed]
- Akkus, F.; Mihov, Y.; Treyer, V.; Ametamey, S.M.; Johayem, A.; Senn, S.; Rösner, S.; Buck, A.; Hasler, G. Metabotropic glutamate receptor 5 binding in male patients with alcohol use disorder. Transl. Psychiatry 2018, 8, 1–8. [Google Scholar] [CrossRef]
- Erol, A.; Karpyak, V.M. Sex and gender-related differences in alcohol use and its consequences: Contemporary knowledge and future research considerations. Drug Alcohol Depend. 2015, 156, 1–13. [Google Scholar] [CrossRef]
- Verplaetse, T.L.; Cosgrove, K.P.; Tanabe, J.; McKee, S.A. Sex/gender differences in brain function and structure in alcohol use: A narrative review of neuroimaging findings over the last 10 years. J. Neurosci. Res. 2021, 99, 309–323. [Google Scholar] [CrossRef]
- McCaul, M.E.; Roach, D.; Hasin, D.S.; Weisner, C.; Chang, G.; Sinha, R. Alcohol and women: A brief overview. Alcohol. Clin. Exp. Res. 2019, 43, 774. [Google Scholar] [CrossRef]
- Fairbanks, J.; Umbreit, A.; Kolla, B.P.; Karpyak, V.M.; Schneekloth, T.D.; Loukianova, L.L.; Sinha, S. Evidence-based pharmacotherapies for alcohol use disorder: Clinical pearls. In Mayo Clinic Proceedings; Elsevier: Amsterdam, The Netherlands, 2020; pp. 1964–1977. [Google Scholar]
| Receptor system | Striatal D2/3 | Midbrain D3 | Extrastriatal D2/3 | GABA-A | µ-opioid | CB1 | SERT | mGluR5 |
| Strength of evidence |  |  |  |  |  | 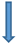 |  | 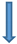 |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Nutt, D.; Hayes, A.; Fonville, L.; Zafar, R.; Palmer, E.O.C.; Paterson, L.; Lingford-Hughes, A. Alcohol and the Brain. Nutrients 2021, 13, 3938. https://doi.org/10.3390/nu13113938
Nutt D, Hayes A, Fonville L, Zafar R, Palmer EOC, Paterson L, Lingford-Hughes A. Alcohol and the Brain. Nutrients. 2021; 13(11):3938. https://doi.org/10.3390/nu13113938
Chicago/Turabian StyleNutt, David, Alexandra Hayes, Leon Fonville, Rayyan Zafar, Emily O.C. Palmer, Louise Paterson, and Anne Lingford-Hughes. 2021. "Alcohol and the Brain" Nutrients 13, no. 11: 3938. https://doi.org/10.3390/nu13113938
APA StyleNutt, D., Hayes, A., Fonville, L., Zafar, R., Palmer, E. O. C., Paterson, L., & Lingford-Hughes, A. (2021). Alcohol and the Brain. Nutrients, 13(11), 3938. https://doi.org/10.3390/nu13113938






