Abstract
Children with autism spectrum disorder (ASD) report a higher frequency and severity of gastrointestinal disorders (GID) than typically developing (TD) children. GID-associated discomfort increases feelings of anxiety and frustration, contributing to the severity of ASD. Emerging evidence supports the biological intersection of neurodevelopment and microbiome, indicating the integral contribution of GM in the development and function of the nervous system, and mental health, and disease balance. Dysbiotic GM could be a contributing factor in the pathogenesis of GID in children with ASD. High-fat diets may modulate GM through accelerated growth of bile-tolerant bacteria, altered bacterial ratios, and reduced bacterial diversity, which may increase the risk of GID. Notably, saturated fatty acids are considered to have a pronounced effect on the increase of bile-tolerant bacteria and reduction in microbial diversity. Additionally, omega-3 exerts a favorable impact on GM and gut health due to its anti-inflammatory properties. Despite inconsistencies in the data elaborated in the review, the dietary fat composition, as part of an overall dietary intervention, plays a role in modulating GID, specifically in ASD, due to the altered microbiome profile. This review emphasizes the need to conduct future experimental studies investigating the effect of diets with varying fatty acid compositions on GID-specific microbiome profiles in children with ASD.
1. Introduction
Autism spectrum disorder (ASD) is a neurodevelopmental condition that is characterized by challenges in social skills and communication, along with the presence of restricted and repetitive behaviors [1]. A high rate of both mental and physical conditions is reported in individuals with ASD [2], including epilepsy, sleep disorders, anxiety, bipolar disorder, attention deficit hyperactivity disorder, and gastrointestinal disorders (GID) [3]. Moreover, the increasing worldwide prevalence of ASD [4], along with unmet health needs, contributes to a high disease burden in individuals with ASD [2]. Children with ASD commonly develop several gut-related comorbidities with gastrointestinal symptoms associated with increased gut epithelial barrier permeability, the decreased expression of brush border disaccharidases in the gut epithelium, and altered gut microbiome (GM) composition [5]. When untreated, GID can contribute to increased medical costs, trigger sleep disturbances, and increase social withdrawal and anxiety [6,7,8]. Additionally, GI symptoms may appear and manifest as behavioral changes [9]. The unpleasant feeling associated with GID, such as pain and discomfort, may lead to feelings of anxiety, frustration, and irritability [6,10], which may increase the risk of aggression and self-abuse [10], especially if children are unable to express this discomfort verbally, thus increasing the severity of ASD itself.
GID in children with ASD are consistently reported to be of a higher frequency and severity than in typically developing (TD) children [10]. Various studies reported GID prevalence, ranging from 23% to 85%, with diarrhea and constipation being the most common [6,10]. In a recent review of 114 reports on ASD and GID, the authors reported the prevalence rate of 4.3–45.5% for constipation, 2.3–75.6% for diarrhea, and 4.2–96.8% for the presence of any GI symptoms [11]. This variety in GID frequency could be considered to be reflective of the heterogeneity of the ASD condition itself; however, there is at least a three times higher risk of GID in children with ASD in contrast to TD children, [6]. For example, Adams et al. (2011) reported that the prevalence of moderate–severe diarrhea and/or constipation was 63% in children with ASD compared to only 2% in TD children [10]. A higher prevalence of GID in female than male children with ASD has been reported [12,13]. Children with ASD tend to more commonly present GI symptoms early in life than TD children [14]. Further, the Norwegian Mother and Child Cohort Study showed that, in contrast to TD children, children with ASD had greater odds of having mother-reported constipation in the ages of 6–18 months and 18–36 months, and reported diarrhea in the ages of 18–36 months [15]. Several causes have been postulated for the higher prevalence rate of GID in children with ASD. For example, constipation may be attributed to a restricted diet usually low in fiber, side effects of medications, and/or irregular toileting behaviors due to developmental deficits [8,16,17]; however, not all of these factors were consistently associated with GID [18]. Diarrhea can also be caused due to the side effects of medications [7] and by other intestinal conditions, such as food allergies and/or intolerances [19]. Additionally, the GM could play a significant role [5].
The commensal bacteria of GM communicate with each other and with the gut epithelium of the host to maintain the gut homeostasis and improve the host immunity [20,21]. This communication is mediated by bacterial structural components and metabolites that act as signaling molecules for interaction with the gut epithelial cells as well as the cells of the immune system [21]. This interaction is essential for the maintenance of tissue homeostasis by a complex and coordinated set of innate and adaptive immune responses against different triggers such as food-derived antigens, metabolites, and pathogens [20]. GM is involved in gastrointestinal physiology, metabolism, nutrition, immune function, in addition to brain functions, including behavior of an individual [22]. Growing evidence suggests that the gut has a strong bidirectional communication with the brain, which is vital for maintaining brain functions and gut homeostasis. Microbiome–gut–brain axis mediates this communication between GM and the central nervous system (CNS). It plays a crucial role in several brain processes such as neuroinflammation, neurotransmission, the synthesis of neurotransmitters, and the regulation of complex behavioral functions such as anxiety, stress, and sociability [22]. For example, the intakes of prebiotics and probiotics and dietary polyphenols increase the production of phenolic acids from the microbial metabolism, exerting desirable effects in terms of neuroprotection [23]. GM is beneficial to the host at a healthy state, and its disruption (known as dysbiosis) can lead to several diseases [24]. It is hypothesized that dysbiosis contributes to the development of GI problems, which occur partly due to the disrupted communication between the microbiome, intestines, and brain [25]. An abnormal GM has been associated with several diseases, such as inflammatory bowel disease (IBD) [26], mood disorders [27], and ASD [28]. Several studies have shown alterations in the composition of the GM and metabolic products of the GM in children with ASD [29,30]. Various classes of bacteria have been found to be significantly different in children with ASD. For example, Bacteroidales, found significantly lower in children with ASD, have been suggested to affect brain function and development of neurological function, and the alternation of food intake has been demonstrated to improve neurodevelopment by interfering with GM composition [31]. Although specific bacterial strain-induced behavioral alterations in animal experiments have demonstrated the effect of GM in regulating certain processes of the CNS, such findings in humans scarce understand the underlying mechanisms [29].
The growing focus on the microbiome–gut–brain axis has encouraged many investigators to develop ways for the reversal of GM alterations as therapeutic interventions for alleviating ASD symptoms. Dietary patterns, antibiotic use, and infections are often associated with the alternations in GM composition and the loss of gut homeostasis, which have been implicated in the pathogenesis of gut as well as brain disorders. Probiotic therapy, for example, in managing GI dysfunction, has been shown as a promising approach, beneficially altering fecal microbiota, and reducing the severity of ASD symptoms in children [32]. Dietary manipulations for GID are considered an important part of the overall therapeutic plan. Dietary fat plays a significant role; however, in comparison with other nutrients, the relationship of dietary fat and the microbiome is more complicated and is not yet fully understood. Factors such as the dietary fat percentage and the fatty acid profile of the diet affect the GM community and the inflammatory response [33]. GM can be affected by several dietary factors. Treatments based on the microbiome modulation with prebiotic, probiotic, and dietary interventions may influence not only the gut, but also brain health and behavior.
Interestingly, significant differences are reported in the GM of children with ASD and TD [10], some of which are correlated with gastrointestinal health, ASD severity, or both [10,29]. Defining a specific microbiome profile in children with ASD and exploring whether it is related to GID would provide more of an insight on the etiology of GID and present new therapeutic alternatives for ASD. The aim of this review is to investigate the role of dietary fat in modulating GID, mainly through its effects on the GM balance and their byproducts. The article is divided into two main sections. The first section reviews the literature on GM composition and the association with behavior and GID, and the second section summarizes the evidence on the effect of dietary fat on GM composition and gut health. The evidence available in context to individuals/children with ASD is included.
2. Methods
A title/abstract-specific search was performed on PubMed. Google scholar was used as a secondary strategy for retrieving more articles, in addition to the reference list of the identified trials and reviews. The search included publications from any date up to August 2021. Two search strategies were employed: The first used autism-related terms (e.g., ‘Autism’, ‘Autism, infantile’, ‘Autistics disorder’) and keywords related to gut microbiome (e.g., gut microbiome, microbiota, or flora). The second used dietary-fats related terms (e.g., saturated fatty acids, monounsaturated fatty acids, polyunsaturated fatty acids, and omega-3 fatty acids (including EPA and DHA)) in addition to gut-microbiome related terms. All study designs, including review articles, were included in this review. Due to the lack of published articles on the effect of dietary fats in children/individuals with ASD, articles exploring its effect in different population groups and animal models were included to establish its association with GM. With that, it was compared to the altered GM composition in ASD.
3. GM and GID in Children with ASD
The human microbiome consists of the 10–100 trillion symbiotic microbial cells, the majority of which reside in the gut, making GM the largest microbiome in the human body [34]. Various techniques have been used to study GM, including culture, polymerase chain reaction (PCR), real-time PCR, and microarray [35]. Given the advancements in genomic techniques, next generation sequencing (NGS) by targeted 16s rRNA sequencing, or even shotgun metagenomic sequencing, were employed to determine the composition of GM; however, differences may arise due to sample handling; DNA extraction; sequencing of different regions of DNA; varying coverage achieved by PCR primers; sequencing depth; and bioinformatic and statistical methods used for analysis [36]. Nevertheless, NGS expands our ability to understand the human microbiome and its association with various diseases, including ASD.
Generally, the heterogeneous GM colonizing the intestine, particularly the large intestine, is an essential component for supporting nutrition and metabolism [37], and forms a shield-like barrier to protect itself from pathogens and to support the gut immunity and overall intestinal integrity [37,38]. The essential GM, also known as normal flora, consists mainly of four major phyla (Bacteroidetes, Firmicutes, Proteobacteria, and Actinobacteria), in addition to two minor phyla (Verrucomicrobia and Fusobacteria) [24]. These phyla include several genera, mainly Bacteroides, Bifidobacterium, Lactobacilli, Streptococci (aerobic and anaerobic), Clostridia, Eubacteria, and Enterobacterium [38,39,40].
In a healthy gut, the Firmicutes predominate the small intestines, and the Bacteroidetes predominantly populate the colon [39]. Both Bacteroidetes and Firmicutes help in the metabolism of undigested food remains. Colonic bacteria including Bacteroides, Roseburia, Bifidobacterium and Enterobacteriaceae are involved in the fermentation of carbohydrates and indigestible oligosaccharides [41], which results in the synthesis of various short-chain fatty acids (SCFAs), including butyrate, propionate, and acetate [42]. These SCFAs play an important role in gut health as they exert anti-inflammatory, anti-tumorigenic, and immunomodulatory effects, preserving the intestinal barrier integrity [28,42,43]. Moreover, they are considered to be an energy supply for epithelial cells, specifically butyrate, that preserves the colonocytes function and homeostasis [42], supports normal bowel movements [44], and enhances intestinal barrier integrity [45]. Other bacteria such as Bacteroides thetaiotaomicron have been shown to induce greater expression of colipase, an enzyme required by pancreatic lipase for lipid digestion. Lactobacillus plantarum maintains intestinal barrier integrity and prevents the entry of gut bacteria, bacterial toxins, partially digested fats, and proteins into the bloodstream, thus preventing leaky gut [46].
Dysbiosis refers to the imbalance of microbial communities in a host [47]. It can occur as a result of losing beneficial microorganisms, increased growth of pathogenic microorganisms, or due to a loss of microbial diversity [47]. This can alter the levels of SCFAs, thereby contributing to the gut inflammatory process [43,48]. Dysbiosis can manifest as GID, including constipation, diarrhea, abdominal pain, bloating, and withholding [49], through its effect on immune dysregulation, altered signaling (e.g., altered serotonin synthesis), and intestinal barrier dysfunction [50]. Dysbiosis associated with specific diseases is characterized by unique compositional and functional changes in the microbiome [47].
Interestingly, the intestinal microbiome is capable of bidirectional interactions with the higher brain center via endocrine, neural, and immune system signaling [51]. This brain–gut–microbiome axis explains how changes in GM can be associated with both ASD and GID [49].
In dysbiosis, some pathogenic bacteria in the presence of a weakened immune system may lead to neurological disorders. Toxins produced by the bacteria may build up in the bloodstream, leading to confusion, delirium, and even a coma [46]. Specifically for ASD, significant differences are reported in the GM of children with ASD and TD children [10]. Strong evidence in animal models proves the relationship between the GM alterations and autism, whereby GM transplantation from human autistic donors into germ-free mice led to the induction of autistic behaviors in mice [52].
Both animal and clinical studies have demonstrated that modifying GM can treat ASD-related behaviors [49,52,53] by modulating the neural excitability and structuring the amygdala—the main hub—for regulating fear and social behaviors [54]. Moreover, GM influences the production and expression of neurotransmitters and neuromodulators [55,56], which activate or inhibit central neurons [57]. Members of the genera Lactobacillus and Bifidobacterium synthesize gamma-aminobutyric acid (GABA); Lactobacillus synthesizes acetylcholine; Bacillus and Serratia synthesize dopamine; Candida, Streptococcus, Escherichia, and Enterococcus synthesize serotonin; and Escherichia, Bacillus and Saccharomyces synthesize norepinephrine [58]. Alterations in these molecules mediate the effect of GM on brain development [59,60]. Animal studies have proven that the modulation of the GM can affect the manifestations of oxytocin, vasopressin, and brain-derived neurotrophic factor (BDNF), and improve the function of microglial cells, thus it can enhance behavior, learning, and memory in humans [59,61]. BDNF is a member of neurotrophins family, which regulate the function of nervous system [62]. Changes in BDNF can manifest as behavioral abnormalities, including anxiety-like behaviors [63]. The GM plays an interesting role in ASD, as it can influence both behavioral symptoms and ASD-related GID. This connection is highlighted in Figure 1.
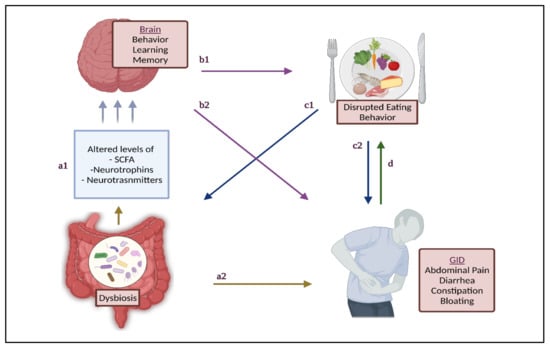
Figure 1.
The brain–gut–microbiome axis in the etiology of gastrointestinal disorders in autism spectrum disorder: (a1) Signaling molecules from GM communicate with various organs, including the brain affecting ASD-related behavior. (a2) Dysbiosis contributes to GID. (b1) ASD severity may increase risk of disrupted eating behavior, affecting the quantity and quality of food intake. (b2) ASD severity manifests as a lack of ability to communicate GID presence, contributing to increased symptoms and severity. (c1) Disrupted eating behavior compromises diet quality, contributing to altered GM composition. (c2) Disrupted eating behavior contributes to GID directly and indirectly through (a2). (d) GID presence and severity contributes to compromised eating, thereby disrupted eating behavior. ASD: autism spectrum disorder; GID: gastrointestinal disorders; GM: gut microbiome; SCFA: short-chain fatty acids.
Behavioral changes can also impact eating behaviors, which in turn contribute to GID, dysbiosis, and dysbiosis-related GID. Wallisch et al. found that children with ASD who were picky eaters were significantly more likely to have behavioral differences compared to non-picky eaters [64]. Further-more, picky eating was also significantly associated with increased odds of GI symptoms and sleep disturbances in children with ASD [12]. Sleep disturbances in turn increase the risk of lower scores in social cognition and communication, intellectual development, and the performance of daily living skills [12]. Eating behaviors can also impact GM due to the compromised diet quality. For example, it has been reported that children with ASD have a significantly lower fiber intake compared to TD children [65,66], and have a high preference towards sweet snacks and soft drinks [67,68,69]. Picky eating also affects GID risk. For example, higher food fussiness has been found to increase the risk of functional constipation, and functional constipation occurrence predicted a greater risk of picky eating in children, indicating the presence of a bi-directional relationship between food intake and GID, leading to the developing of a vicious cycle between these two factors [70]. Addressing these complications can prove to be more challenging in ASD, as the child’s food preferences, lack of acceptance of new foods, and lack of parental knowledge may pose limitations in adhering to nutritional advice [71].
Defining a specific GM composition for children with ASD is not yet possible [42]. However, some common observations have been reported. Most notably, children with ASD have a significantly decreased ratio of Bacteriodetes/Firmicutes phyla. Bacteriodetes is a phylum that includes 241 genera classified in 4 classes, including: Bacteroidia, Flavobacteria, Sphingobacteria, and Cytophagia [72], while Firmicutes include 421 genera classified in 7 classes, including Bacilli, Clostridia, Erysipelotrichia, Limnochordia, Negativicutes, Thermolithobacteria, and Tissierellia [73]. It is difficult to compare microbiome at phyla level to reach a conclusion about the GM composition; however, it has been observed that children with ASD have a higher count of Clostridium (phylum: Firmicutes), Lactobacillus (phylum: Firmicutes), Sutterella (phylum: Proteobacteria), and Desulfovibrio (phylum: Proteobacteria), and a lower count of Bifidobacterium (phylum: Actinobacteria) and Akkermansia muciniphila (phylum: Verrucomicrobia) [42]. According to a recent systematic review on GM alterations in ASD [74], Lactobacillus, Bacteroides, Desulfovibrio, and Clostridium were increased in individuals with ASD relative to healthy controls in certain studies, while Bifidobacterium, Blautia, Dialister, Prevotella, Veillonella, and Turicibacter were consistently decreased. The heterogeneity in the results may be attributed to the variations in the methodological approaches used in different studies, such as sample sources, storage temperature, methods of DNA extraction, primers used in PCR, 16S rDNA sequencing platforms, and data analysis methods [74]. Other possible causes of heterogeneity can be related to the study participants’ characteristics, including age, gender, type of control (sibling vs. non-sibling), dietary factors, and GI symptoms [74]. Thus, well-designed studies are needed for a better understanding of the significance of GM in ASD.
Desulfovibrio was shown to be higher in ASD [75,76], and exhibited a positive correlation with the severity of autism manifestations [75]. Desulfovibrio is a genus of Gram-negative, sulfate-reducing bacteria and is a major producer of hydrogen sulfide (H2S) in the gut [77]. H2S produced by Desulfovibrio was found toxic to the gut epithelial cells of individuals with ASD [78]. High levels of H2S may cause mucus disruption and inflammation, while low levels can directly stabilize the mucus layers of the gut, prevent fragmentation and adherence of the microbiota biofilm to the epithelium, inhibit the invasion of pathogenic bacteria, and help resolve inflammation and tissue injury [79]. Gut Desulfovibrio was associated with an increase in the self-reported severity of gastrointestinal symptoms in adults [80], however Desulfovibrio abundance was not found to be correlated to GI symptoms in children with ASD [75]. It was noted that there is a dose response in ASD severity with increased Desulfovibrio, which was hypothesized to be attributed to its production of lipopolysaccharides (LPS) and reduction of sulfate, otherwise required for other physiological reactions [81]. It has been reported that children with ASD had significantly more ear infections and were given significantly more antibiotics than those who developed normally [78]. Desulfovibrio is often resistant to these agents, which suppress certain members of the normal flora, allowing for the overgrowth of Desulfovibrio to higher levels, with a higher production of harmful compounds such as LPS and H2S [78]. Because of these toxic byproducts, gastrointestinal inflammation and subsequent neuro-inflammation associated with leaky gut syndrome can occur in children with ASD [82].
A surge in bacteria that synthesize propionic-acid such as Bacteroides and Clostridia (some species) may increase the risk of deterioration in social behavior [42]. Injecting propionic acid into the cerebral ventricles of rats has led to the development of biological, chemical, and pathological changes that are characteristic of autism [83]. In an animal-model study, the effects of prenatal propionic acid on the social behavior of neonatal, adolescent, and adult rats suggested an impairment in social recognition, mediated by the olfactory system in the young rats; adolescent males showed increased levels of locomotor activity compared to females and approached the novel objects more in contrast to the controls [84]. Clostridium species counts are consistently high in children with ASD [10,42]. A significant positive correlation was found between the relative abundance of Clostridium species and the Childhood Autism Rating Scale score in children with ASD [85]. Clostridium histolyticum and Clostridium perfringens were consistently reported to be increased in the stool samples of children with ASD [86]. Clostridium histolyticum contributes to gut dysfunction [10], and Clostridia toxins contribute to behavioral changes by altering neurotransmitter function [87]. Another study reported an increase in Clostridium histolyticum in stools from individuals with ASD compared to healthy controls [88]. Reducing Clostridium numbers can dampen both gastrointestinal and behavioral symptoms [86].
Luna et al. conducted a study on 35 children, 14 of which were diagnosed with both ASD and functional gastrointestinal disorders (FGID), and compared their GM profiles to TD children with and without FGID [49]. Children with ASD and FGID had a different profile than TD children with FGID. Children with ASD had a statistically significant higher number of Clostridiales, specifically Clostridium lituseburense, Lachnoclostridium bolteae, Lachnoclostridium hathewayi, and Flavonifractor plautii, and a lower number in other Clostridiales, including Dorea formicigenerans and Blautia luti (p < 0.05 for all bacteria) [89]. These differences in microbiome between children with ASD also provide an explanation of ASD-related behavior [42]. A difference in the GM has also been observed when challenged with GID. Chronic constipation, for example, can be characterized by a relative decrease in Lactobacillus and Bifidobacterium [90,91,92], and an increase in potentially pathogenic microorganisms such as Pseudomonas aeruginosa and Campylobacter jejuni [93]. A decrease in Veillonella has been reported in subjects with autism that may disturb the fermentation of lactate in children with ASD [94]. On the other hand, patients with FGID, including irritable bowel syndrome, have higher counts of Veillonella and Lactobacillus, along with high production of SCFAs including acetic acid and propionic acids [95].
In a study comparing GM in ASD children and healthy control groups, the functional analysis of SCFA-producing bacteria demonstrated that butyrate and lactate producers were less abundant in the stools of the ASD group, while mucin-degraders and other SCFA-producers were more abundant in the ASD group [94]. Butyric acid can promote the synthesis of mucin and enhance intestinal tight junction integrity. The depletion of butyrate-producing bacteria and enrichment of mucin-degraders can be linked to the observed abnormal intestinal permeability reported in individuals with autism [96]. Butyrate is recognized as an anti-inflammatory SCFA that contributes to colon health and has been demonstrated to rescue ASD cells during oxidative stress and enhance mitochondrial function in the context of physiological stress. Butyrate can also modulate the synthesis of the neurotransmitters dopamine, norepinephrine, and epinephrine. Butyrate can also modulate neurotransmitter gene expression and the ASD-related genes in cell line models [97].
In children with ASD, differences in GM profiles reported some common species that were correlated with GID. Table 1 lists the types of bacteria that were found to be significantly altered (increased or decreased) in children with ASD suffering from GID.

Table 1.
Variations in bacterial species with functional gastrointestinal disorders in children with autism spectrum disorder.
Additionally, variation in GM between children with ASD and TD children, both presenting with GID, were noted. For example, children with ASD had decreased levels of Flavonifractor plautii, Bacteroides eggerthii, Bacteroides uniformis, Flavonifractor prausnitzii, and Clostridium clariflavum in functional constipation [89], an increase in Clostridium aldenense, decreases in Bacteroides luti, Bifidobacterium adolescentis, Eubacterium ventriosum, Anoxystipes fissicatena, Coprococcus comes, Eubacterium ramulus, and Phascolarctobacterium faecium in aerophagia [89], decreases in Akkermansia muciniphila, Coprococcus catus, Odoribacter splanchnicus, Clostridium lactatifermentans, and Ruminococcus lactaris in abdominal migraine [89], an increase in Clostridium aldenense in irritable bowel syndrome [89], and increases in Bacteriodaceae, Lachnospiraceae, Prevotellaceae, and Ruminococcaceae in abdominal pain [106].
Alpha diversity is defined as the mean diversity of species (or other taxonomic groups) within a microbial community. Alpha diversity metrics summarize the structure of a community with respect to its richness (number of taxonomic groups), evenness (distribution of abundances of the groups), or both [107]. Based on a recent systematic review, there were no consistent patterns of alpha diversity in children with ASD compared to siblings and healthy controls, though a few studies reported significant differences [108]. A study comparing the GM in ASD and healthy children in China reported a significant increase in bacterial richness in the ASD group compared with healthy children [109]. Another study compared the GM of subjects with autism with gastrointestinal symptoms, siblings not showing autistic symptoms (sibling controls), and the non-sibling control subjects. Significantly more diversity and richness of microbial communities were found in ASD compared to the other groups [76]. The increased richness in ASD children was attributed to an increase in the harmful genera or species contributing to the severity of autistic symptoms (listed in Table 1).
The analysis of the beta diversity (a measure of diversity of microbial community composition between different groups) showed that the GM in the ASD group was distinct from that of the healthy control group [109]. However, there is inconsistency in the available data regarding significant differences in the beta diversity between ASD and siblings without autistic symptoms and non-sibling control subjects. For instance, a study investigating GM in ASD children with and without GI dysfunction reported that there was no clustering of samples from ASD children, regardless of the autism severity and GI dysfunction. This indicated a non-significant difference in the bacterial composition within and between the autistic and control groups [110]. The same study also indicated that there were non-significant differences within the ASD group when comparing those with and without GI dysfunction.
GM composition is influenced by a variety of factors, including age, body mass index, and genetic disposition, and other external factors such as diet, antibiotic treatments, exercise frequency, and environmental pollutants [38,111,112,113]. Dietary factors influence GM through acting as substrates to different microbial species, and through altering the gut environment (e.g., pH levels and bile acid (BA) concentrations), influencing microbial growth [111]. Dietary approaches with varying compositions of fiber, proteins, and fats, such as the Western diet, Mediterranean diet, and others, promote the growth of different species of bacteria [114]. Of these macronutrients, both the quantity and quality of dietary fats are proposed to be major factors in promoting this change due to their direct effects on BA concentrations [111]. These associations will be explored more closely in Section 3.
Dietary interventions are poised to play a key role in the brain-gut-microbiome axis in order to maintain both the brain health and gut health by preserving a healthy balance of the GM. In children with ASD, who already have an altered GM profile, translating the effects of external factors such as diet into clinical practice can lead to the potential treatment or management of ASD symptom severity and GID.
4. Dietary Fat and Gut Health
The term fat usually refers to all “fatty” substances found in food and the body [115]. In dietary terms, “lipids” is a broader term which encompasses fats, usually in the form of triglycerides (TG), cholesterol, and phospholipids, all of which are found in varying concentrations in different foods [115]. TG make up about 95% of all lipids in the diet [116], and are composed of one glycerol molecule and three attached fatty acids. The fatty acids are mainly what define the health and metabolic effect of the fat. They can either be saturated, monounsaturated, or polyunsaturated fatty acids based on the number of double bonds that exist in the carbon–carbon skeleton of the fatty acid [115].
Theoretically, fatty acids are not thought of as a diet source for gut bacteria, due to the need of oxygen for the metabolism of fat, and the gut is inhabited mostly by anaerobes [117]. Nonetheless, bacteria has been found to interact with fat, as fatty acid intermediates have been detected in the intestine [117]. Some fatty acids exert antimicrobial activity that affects the survival of certain bacterial species [117,118]. For instance, bacterial growth hindrance or cell death may result from the toxic compounds generated by the action of free fatty acids (FFAs) on the cell membrane, causing disruption of enzymatic activities, leading to interferences with energy production, and impairment in nutrient absorption [43]. The presence of fat in the distal intestines may induce a loss of diversity in the microbiome community due to this antimicrobial activity [119]. Due to this effect of fat on the microbiome, the composition of fat, and its effects on the GM, are interesting areas of investigation; being easily manipulated through diet can be a target for non-invasive preventive and therapeutic interventions.
4.1. Saturated Fatty Acids
Saturated fatty acids (SFAs) are composed only of carbon –carbon single bonds, and are usually solid at room temperature [115]. While they are primarily found in animal products, such as meat, butter, and dairy products [120], they are also found in large concentrations in tropical plant oils, such as palm and coconut oils [115].
High SFAs intake has been generally reported to have a negative influence on GM, which could increase correlated GID, as illustrated in Figure 2. One of the major mechanisms includes an increase in BA concentration [121], which has a direct antimicrobial effect on GM [122]. BAs are secreted as a result of fat ingestion, specifically as a response to cholecystokinin [123]. Approximately 94% of BAs are absorbed from the distal small intestines, and the rest are lost through feces. Primary BAs (e.g., cholic acid and chenodeoxyvholic acid) received from the liver can be converted into secondary BAs (deoxycholic acid and lithocholic acid [124]) by gut bacteria [119] [123,125]. BAs play an interesting role in gut health, as they have a potential pathogenic role in inflammation on one hand, and in intestinal mucosal defense on the other [126]. For example, ursodeoxycholic acid administration resulted in favorable intestinal changes, reduced intestinal permeability, and decreased free radical generation; however, at higher doses, the same BA was found to be cytotoxic [126]. Preserving the dynamic equilibrium between GM and BA composition is essential to avoid pathological states [122]. Secondary BAs were found to be accumulated in individuals following the Western diet, especially deoxycholic acid [122]. These secondary BAs are more potent antimicrobial agents [122], and have been associated with gut inflammation by causing oxidative stress, cytotoxicity by causing damages to the cell membrane, and can even be carcinogenic [119,125,127]. To demonstrate the effect of a high input of BAs, feeding rats high levels of cholic acid led to an expansion of the secondary BA-producing bacteria (of the phylum Firmicutes), along with an increase in Firmicutes from 54% in the control group to 93–98%, including a significant expansion in many species found in Clostridium cluster XIVa [122]. This increase in BAs also led to a reduction of Bacteroidetes and Actinobacteria [122]. The overlap of GI and ASD symptoms may be explained by shared pathophysiological mechanisms that include intestinal inflammation, as evident from the endoscopy in children, with ASD showing that different segments of the GI tract may be affected with inflammation, as upper and lower endoscopy results showed reflux esophagitis, chronic gastritis and duodenitis, and ileocolotis [128]. Although ASD is a genetically determined brain disorder, GI inflammation may contribute to brain dysfunction [128].
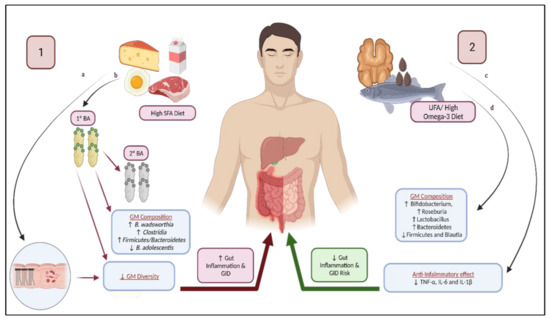
Figure 2.
Dietary fat composition and risk of gastrointestinal disorders: (1) High SFA diet contributes to GID through modulation of GM. (a) SFA increases FA overflow to the distal intestines, reducing GM diversity, thus contributing to GID. (b) SFA increases the levels of primary and secondary bile acids, contributes to changes in GM composition, reduced GM diversity, and gastrointestinal inflammation, thus increasing the risk of GID. (2) Unsaturated fats, particularly high omega-3 diets, reduces GID risk due to (c) significant reduction of proinflammatory cytokines and (d) its favorable impact on GM composition and diversity, increasing SCFA levels. BA: bile acid; GM: gut microbiome; GID: gastrointestinal disorders; SFA: saturated fatty acids; SCFA: short-chain fatty acids.
Interestingly, studies have found that SFAs can change the BA pool and thus contribute to intestinal inflammation and alter the microbiome [119], specifically in regards to the bacterium Bilophila wadsworthia, including increased inflammation, increased intestinal permeability with higher mucosal, and systemic immune responses [129]. These effects may increase the likelihood of abdominal pain and GID, such as diarrhea [130]. Milk-fat (high in SFA) consumption also promotes the growth of Bilophila wadsworthia and intestinal inflammation, as this sulphate-reducing bacteria can increase the concentration of hydrogen sulphide and disrupt the epithelial tissue in the intestinal mucosa [131]. SFA can also contribute to GID due to other microbiome-related changes, including the increase in Clostridium clusters. de Wit et al. (2012) conducted a trial on mice that received four diets, either low-fat, high-fat with high SFA (palm oil), high-fat with high MUFA (olive oil), or high-fat with high polyunsaturated fatty acids (PUFA) (safflower oil) After 8 weeks, the group that consumed palm oil (high SFA) had an increased Firmicutes/Bacteroidetes ratio. Firmicutes had a high proportion of Clostridium clusters XI, XVII, and XVIII. Clostridium cluster XI specifically contributes to the production of deoxycholic acid and is considered a harmful bacteria for the large intestines [132]. Moreover, high palm oil intake was associated with reduced microbial diversity [132].
Microbial diversity is an important marker of health [129], as the diversity of bacterial species maintains the intestinal ecosystem [133], increases the functional resilience of microbial community [117], and decreases shifts in the microbiome as a response to environmental changes (e.g., diet) [129]. For instance, patients with inflammatory bowel disease exhibit lower microbial diversity that increases during remission [133]. High SFA intake through palm oil intake also induces an overflow of fatty acids to the distal parts of the intestines [132]. The concentration of GM increases steadily along the gastrointestinal tract, starting from 101 bacteria/gram content in the stomach, to 1012 bacteria/gram in the colon [134], and the bacteria inhabiting the stomach and proximal duodenum are usually bile resistant [134]. An overflow of dietary fats to the distal intestines is suggested to be strongly involved in changing the GM composition [135], also observed after administering a high palm oil diet [132]. This overflow of dietary fats from palm oil was greater than safflower or olive oils [132].
A review by Nogay and Nahikian-Nelms (2021) also supported the increase in the Firmicutes in mice. Observational studies comparing the diets of children following either mainly the Western diet or a predominantly vegetarian diet reported profound differences in the distribution of bacteria phyla, in which the Western diet showed an increased prevalence of Firmicutes, and a decreased prevalence of Bacteroidetes and Actinobacteria [136]. High SFA intake has been suggested to have promoted the growth of pathogenic bacteria through increasing taurine-conjugated BAs [137]. A high intake of SFA through animal-based protein, one of the hallmarks of the Western diet [138], increased the number of Clostridia and decreased the count of Bifidobacterium adolescentis [139]. Bifidobacterium adolescentis was reported to downregulate nuclear-factor kappa B [140], a protein complex that induces an inflammatory state [141] and inhibits the production of LPS in the gut [140]. LPS are endotoxins found in Gram-negative bacteria, much of which are part of the human gut. Bacteroides, for example [142], have been found to actually increase with high-fat feeding [143], along with Clostridium and Ruminoccoccus [42]. LPS have been found to increase visceral hypersensitivity [144], which is implicated in the pathogenesis of abdominal pain and discomfort [145].
Bile-tolerant anaerobes such as Bilophila wadsworthia and the Alistipes genus increase in the Western diet along with high milk-fat consumption [146]. The Alistipes genus is relatively new, and is reported to have contrasting evidence regarding its pathogenic and/or protective roles [147]. A study which analyzed the microbiome of 22 children with irritable bowel syndrome found an abundance of the Alistipes genus (four specific taxa within this genus) and a positive correlation with a greater frequency of pain [148].
The reviewed literature suggests that high intakes of SFA exert unfavorable effects on the GM composition, leading to the overgrowth of specific species and reduced GM diversity that have been correlated with GID. Dietary patterns with high SFA levels such as the Western diet should be discouraged. Furthermore, these GM changes can translate into other metabolic disorders such as insulin resistance and inflammation [114].
4.2. Unsaturated Fatty Acids
Unsaturated fatty acids (UFAs) contain one or more double bonds in the carbon–carbon skeleton of the fatty acids, are predominantly found in plant products, and are usually liquid at room temperature [115]. Those with only one double bond, referred to as monounsaturated fatty acids (MUFA), are found in highest concentration in olive, peanut, and canola oils, avocado, and some nuts and seeds; those with two or more double bonds are referred to as polyunsaturated fatty acids (PUFA), and are found in other oils (sunflower, corn, and soybean), walnuts, flaxseeds, and fish [115].
Essential fatty acids (EFA) are a category of PUFA that are not synthesized by humans, and include both omega-3 (alpha-linolenic acid) and omega-6 (linoleic acid) and their derivatives, and are thought to exert a positive effect on GI health through their effect on the GM (Figure 2) [149]. Children with ASD have been found to have disturbed concentrations of omega-3 and omega-6, and decreased omega-3 levels [87,119,150], possibly due to nutritional deficiency or genetic defects [87]. An adequate balance of EFA is essential for brain development, and is therefore considered a possible biomarker for ASD, and omega-3 supplementation can potentially improve behavioral measures in children with ASD [151]. Low omega-3 levels, or a disturbed omega-3/omega-6 ratio, increases inflammatory cytokine and oxidative stress [150]. Dietary flaxseed oil (high omega-3) was found to significantly reduce proinflammatory biomarkers such as plasma IL-6, IL-1b, and TNF-a, in rats [149]. GID in which inflammation plays a role may benefit from Docosahexaenoic acid (DHA), an omega-3 supplementation [152]. Menni et al. (2017) noted that increased serum DHA was associated with bacterial groups that were negatively correlated with intestinal inflammation and Crohn’s disease [153]. In addition, low omega-3 levels can lead to the malfunction of neurotransmitters, as EFA can modulate the expression and action of neurotransmitters including serotonin, dopamine, and acetylcholine [154].
Watson et al. reported that, following an 8-week supplementation with omega-3 in healthy middle-aged women, Bifidobacterium, Roseburia, and Lactobacillus increased [155]. Roseburia is considered to play a major role in gut health due to its anti-inflammatory and immunity-maintenance properties [156]. In one study comparing children with ASD to healthy children, some Roseburia species were higher in children with ASD and others were higher in healthy children [157]. Menni et al. (2017) also reported the strongest correlation of omega-3 with an increase in the Lachnospiraceae family, which includes Roseburia. [153]. Omega-3 administration in rats also showed a favorable impact on GM. Comparing different types of fats, corn oil diets increased the abundance of Firmicutes in rats, which was reversed through the administration of flaxseed oil. Therefore, flaxseed oil reduced the Firmicutes/Bacteroidetes ratio and also reduced Blautia abundance [149]. Furthermore, the abundance of Firmicutes and Blautia was significantly correlated with higher LPS, while Bacteroidetes was correlated with lower LPS levels [149]. Although the theoretical evidence supports the possibility of favorable role of omega-3 on GM, a recent observational study on 120 children with ASD judged that there were actually no significant associations between GI symptoms and dietary omega-3 intake [158]. Additionally, in a supplementation trial of omega-3 in children with ASD, there were no significant differences in the occurrence of adverse events, including a range of GI symptoms in omega-3 supplemented and placebo groups [159]. In 19 patients who received the omega-3 supplement, there were complaints of abdominal pain (n = 6), diarrhea (n = 5), and constipation (n = 7) [159]. Considering the high prevalence of GID in ASD, a treatment that does not cause GID warrants high importance.
Regarding high UFA diets, fish oil-fed and lard-fed mice were compared; an increase in Actinobacteria (including Bifidobacterium), lactic acid bacteria (including Lactobacillus), and Verrucomicrobia (including Akkermansia muciniphila) was observed in the high fish oil diet [160]. In contrast, lard-fed mice showed an increase in Bacteroides, Turicibacter, and Bilophila [160]. On the other hand, a decrease in Bifidobacterium after the addition of walnuts and almonds (high in MUFA and PUFA), and an increase in other genera, including Clostridium and Roseburia, were observed [161,162]. Akkermansia muciniphila was significantly decreased in children with ASD and was associated with abdominal migraine [89].
The data on MUFA and GM is limited and inconsistent, therefore its effect is still inconclusive. Singh et al. (2017) reviewed that MUFA does not lead to significant shifts in any bacterial genera. Oleic acid, a type of MUFA found in olive oil, increases F. prausnitzii [163], contradictory to a previously reported decrease in cases of constipation [89]. F. prausnitzii is a positive indicator of intestinal health due to its anti-inflammatory properties [163]. In contrast, Bailey and Hoschler (2018) found that, when mice were either fed canola oil (high MUFA) or palm oil (high SFA), the canola oil group had a higher plasma LPS. Supplementation with omega-3 fatty acids and consumption of high oleic canola oil have shown to increase the levels Faecalibacterium belonging to the Firmicutes phyla [164]. Mandal et al. (2016) concluded that MUFA intake in pregnant women was associated with an increase in Firmicutes, Proteobacteria and Bacteroidetes, and a reduction of Actinobacteria/Proteobacteria [165]. An increase in Proteobacteria was similar to SFA, as it is pathogenic and proinflammatory [165]. Due to the conflicting evidence on MUFA, and the lack of literature in children specifically with ASD, the effect remains inconclusive.
UFA is suggested to have a beneficial impact on GM and gut health. While it could be postulated that replacing SFA with UFA would lead to a more favorable impact on GM, mainly because of the beneficial effect in the limited availability of SFAs, the results are inconsistent and inconclusive. Omega-3 is hypothesized to play a positive effect on GM; still, experimental evidence to support this association, specifically in children with ASD, is lacking.
4.3. High-Fat Diets
Various dietary interventions are proposed for children with ASD, the ketogenic diet is one of them [166]. The ketogenic diet is a dietary pattern that is high-fat, moderate-protein, and low-carbohydrate, used traditionally for controlling seizures in patients with epilepsy [167]. A systematic review summarized that such a diet was promising in attenuating ASD-related behaviors in mice and humans [168]. However, ketogenic dieting should be recommended with caution, as the high-fat percentage (65–90%) can be associated with GID and may lead to nutritional deficiencies, due to low tolerability and the high food selectivity in children with ASD [150]. Gastrointestinal side effects of ketogenic diets in children with ASD included constipation, diarrhea, and vomiting, which occurred within 2–4 weeks of the ketogenic diet onset [169].
Due to the need of BAs for the emulsification of dietary fat, an increase in dietary fat intake is correlated with an increase in the production and secretion of BAs, which are consistent with a higher level of secondary BA in fecal samples [124]. Thus, the consumption of high-fat diets encourages the growth of bile-tolerant bacteria, which are usually Gram-negative bacterial species [119]. Although bacteria from the class Clostridia are Gram-positive, they are also bile-resistant, and therefore increase with high-fat feeding. These include the two families of Ruminococcaceae and Blautia [119]. These families may be negatively associated with gut health, and increased abdominal symptoms in animal models [170]. Regarding human studies, in a Swedish study of 159 individuals (52 cases of abdominal pain and 107 controls with no pain), Blautia was significantly increased in the cases with abdominal pain (p = 0.045) [170]. Mimicking the effect of high-fat diets by providing cholic acid (BA), supplements resulted in an increased Firmicutes/Bacteroidetes ratio and decreased bacterial diversity [119]. More specifically, in an animal model study, the authors concluded that the increase in Firmicutes was driven by an increase in Clostridia and Erysipelotrichi classes [171]. From Clostridia, the genus Blautia, and the genus Allobaculum from Erysipelotrichi, dominated [171]. The results on Allobaculum were inconsistent, as another animal study found that its level decreased in high-fat diets, but increased with high-protein diets [172]. This data indicates that high-fat diets may have unfavorable effects on the GM profile, and a higher risk of GID, due to the association of dysbiosis with gut health. Other effects of high fat diets include decreasing the Roseburia species [173].
Another concern with high-fat diets is related to the increase in LPS. Dietary fat influences GM through: (1) an increase in the absorption of LPS, related to chylomicron formation, and (2) the growth of Gram-negative bacteria, which increases LPS concentrations [142]. LPS can migrate, along with the chylomicron, from the intestines to systemic circulation through absorption [142], with a potent inflammatory effect that contributes to the development of metabolic diseases [174]. In the intestines, LPS may induce severe inflammation and increases the risk of gut-related complications, including diarrhea and abdominal pain [175]. A diet consisting of 72% energy from fat resulted in a 2–3 times increase in circulating LPS in a murine animal study [119]. Additionally, increased LPS is a significant marker of consideration, independently and inversely correlated with lower socialization scores in subjects with ASD [176]. In contrast, Bifidobacterium increases as a response to low-fat diets [177], and plays a beneficial role in decreasing LPS levels [178], contributing to restoring intestinal health.
Mediated through the effects of high concentrations of BAs and LPS, it is possible that high-fat diets increase the risk of GID, especially in children with ASD for whom ketogenic diets are considered. Further research with long-term trials is warranted to develop appropriate dietary fat recommendations, particularly in the context of children with ASD.
5. Limitations and Recommendations
There are some limitations in this review. Most of the evidence presented is extracted from either animal studies or from human studies that present several limitations, such as the inclusion of observational study designs and small sample sizes, thus introducing a risk of bias. Lang et al. (2018) concluded that demographic and anthropometric traits overpower the effect of diet in influencing GM. Heterogeneity in the results regarding GM composition may also be due to methodological variations [74]. Therefore, robust study designs with large samples can help in controlling the confounding factors and present more conclusive evidence. The lack of studies exploring dietary fat specifically in children with ASD is the major limitation. Nevertheless, this review highlights a gap in the literature, creating the need for future studies utilizing an experimental approach to explore the effect of dietary interventions with varying quantities of total fat, fatty acid composition in GM, and the presence of GID, as it can be employed as a promising therapeutic approach. Furthermore, the relation between the severity of behavioral ASD symptoms with GM composition and GID must be explored in future studies. This will help in designing interventional protocols through appropriate dietary regimes, particularly in regard to dietary fats, to reduce the severity of the disease in children with ASD.
6. Conclusions
Data from the literature suggests that children with ASD have different microbiome profiles than TD children, which contribute to both behavioral disorders and GID. Some of these bacteria are increased or decreased by modulating dietary fat. This review proposes that dietary fat intake, as part of the overall diet, may influence the presence and severity of GID through various mechanisms, although experimental data is too scarce to reach affirmations. SFAs were consistently shown to be associated with a negative impact on GM, which could be translated into GID based on the available evidence. Evidence regarding UFAs is inconclusive due to the inconsistent reporting of results; however, omega-3 is hypothesized to reduce GID due to its anti-inflammatory effect and its favorable impact on the GM. High-fat diets exhibited a negative influence on GM, mainly through increased LPS and BA levels, however data is insufficient to suggest specific recommendations. As GID are related to gut dysbiosis, dietary interventions based on GM modulation can serve as an effective therapeutic tool to treat the GID-associated symptoms and severity in children with ASD by restoring the normal GM, limiting inflammation, and restoring epithelial barrier function.
Author Contributions
Conceptualization, A.A. (Amita Attlee) and M.K.; resources, M.K. and A.A. (Asma Ahmadani); writing—original draft preparation, M.K. and A.A. (Asma Ahmadani); writing—review and editing, M.K., A.A. (Asma Ahmadani), A.A. (Amita Attlee) and F.A.M.; supervision, A.A. (Amita Attlee). All authors have read and agreed to the published version of the manuscript.
Funding
This review is published under the research funded by United Arab Emirates University (Grant # G00003323).
Institutional Review Board Statement
Not applicable.
Informed Consent Statement
Not applicable.
Data Availability Statement
Not applicable.
Acknowledgments
Conflicts of Interest
The authors declare no conflict of interest.
References
- Shedlock, K.; Susi, A.; Gorman, G.H.; Hisle-Gorman, E.; Erdie-Lalena, C.R.; Nylund, C.M. Autism Spectrum Disorders and Metabolic Complications of Obesity. J. Pediatr. 2016, 178, 183–187.e1. [Google Scholar] [CrossRef]
- Murphy, C.M.; Wilson, C.E.; Robertson, D.M.; Ecker, C.; Daly, E.M.; Hammond, N.; Galanopoulos, A.; Dud, I.; Murphy, D.G.; McAlonan, G.M. Autism Spectrum Disorder in Adults: Diagnosis, Management, and Health Services Development. Neuropsychiatr. Dis. Treat. 2016, 12, 1669–1686. [Google Scholar] [CrossRef]
- Bauman, M.L. Medical Comorbidities in Autism: Challenges to Diagnosis and Treatment. Neurotherapeutics 2010, 7, 320–327. [Google Scholar] [CrossRef]
- Chiarotti, F.; Venerosi, A. Epidemiology of Autism Spectrum Disorders: A Review of Worldwide Prevalence Estimates Since 2014. Brain Sci. 2020, 10, 274. [Google Scholar] [CrossRef] [PubMed]
- Martínez-González, A.E.; Andreo-Martínez, P. The Role of Gut Microbiota in Gastrointestinal Symptoms of Children with ASD. Medicina 2019, 55, 408. [Google Scholar] [CrossRef] [PubMed]
- Chaidez, V.; Hansen, R.L.; Hertz-Picciotto, I. Gastrointestinal Problems in Children with Autism, Developmental Delays or Typical Development. J. Autism Dev. Disord. 2014, 44, 1117–1127. [Google Scholar] [CrossRef] [PubMed]
- Kuddo, T.; Nelson, K.B. How Common Are Gastrointestinal Disorders in Children with Autism? Curr. Opin. Pediatrics 2003, 15, 339–343. [Google Scholar] [CrossRef] [PubMed]
- Sparks, B.; Cooper, J.; Hayes, C.; Williams, K. Constipation in Children with Autism Spectrum Disorder Associated with Increased Emergency Department Visits and Inpatient Admissions. J. Pediatrics 2018, 202, 194–198. [Google Scholar] [CrossRef] [PubMed]
- Furuta, G.T.; Williams, K.; Kooros, K.; Kaul, A.; Panzer, R.; Coury, D.L.; Fuchs, G. Management of Constipation in Children and Adolescents With Autism Spectrum Disorders. Pediatrics 2012, 130, S98–S105. [Google Scholar] [CrossRef]
- Adams, J.B.; Johansen, L.J.; Powell, L.D.; Quig, D.; Rubin, R.A. Gastrointestinal Flora and Gastrointestinal Status in Children with Autism--Comparisons to Typical Children and Correlation with Autism Severity. BMC Gastroenterol. 2011, 11, 22. [Google Scholar] [CrossRef]
- Holingue, C.; Newill, C.; Lee, L.-C.; Pasricha, P.J.; Fallin, M.D. Gastrointestinal Symptoms in Autism Spectrum Disorder: A Review of the Literature on Ascertainment and Prevalence. Autism Res. 2018, 11, 24–36. [Google Scholar] [CrossRef]
- Yang, X.-L.; Liang, S.; Zou, M.-Y.; Sun, C.-H.; Han, P.-P.; Jiang, X.-T.; Xia, W.; Wu, L.-J. Are Gastrointestinal and Sleep Problems Associated with Behavioral Symptoms of Autism Spectrum Disorder? Psychiatry Res. 2018, 259, 229–235. [Google Scholar] [CrossRef]
- Masi, A.; Breen, E.J.; Alvares, G.A.; Glozier, N.; Hickie, I.B.; Hunt, A.; Hui, J.; Beilby, J.; Ravine, D.; Wray, J.; et al. Cytokine Levels and Associations with Symptom Severity in Male and Female Children with Autism Spectrum Disorder. Mol. Autism 2017, 8, 63. [Google Scholar] [CrossRef]
- Niehus, R.; Lord, C. Early Medical History of Children with Autism Spectrum Disorders. J. Dev. Behav. Pediatrics 2006, 27, S120. [Google Scholar] [CrossRef]
- Bresnahan, M.; Hornig, M.; Schultz, A.F.; Gunnes, N.; Hirtz, D.; Lie, K.K.; Magnus, P.; Reichborn-Kjennerud, T.; Roth, C.; Schjølberg, S.; et al. Association of Maternal Report of Infant and Toddler Gastrointestinal Symptoms with Autism: Evidence from a Prospective Birth Cohort. JAMA Psychiatry 2015, 72, 466–474. [Google Scholar] [CrossRef] [PubMed]
- Ibrahim, S.H.; Voigt, R.G.; Katusic, S.K.; Weaver, A.L.; Barbaresi, W.J. Incidence of Gastrointestinal Symptoms in Children With Autism: A Population-Based Study. Pediatrics 2009, 124, 680–686. [Google Scholar] [CrossRef] [PubMed]
- Pang, K.H.; Croaker, G.D.H. Constipation in Children with Autism and Autistic Spectrum Disorder. Pediatr. Surg. Int. 2011, 27, 353–358. [Google Scholar] [CrossRef] [PubMed]
- Gorrindo, P.; Williams, K.C.; Lee, E.B.; Walker, L.S.; McGrew, S.G.; Levitt, P. Gastrointestinal Dysfunction in Autism: Parental Report, Clinical Evaluation, and Associated Factors. Autism Res. 2012, 5, 101–108. [Google Scholar] [CrossRef] [PubMed]
- Ming, X.; Brimacombe, M.; Chaaban, J.; Zimmerman-Bier, B.; Wagner, G.C. Autism Spectrum Disorders: Concurrent Clinical Disorders. J. Child. Neurol. 2008, 23, 6–13. [Google Scholar] [CrossRef] [PubMed]
- Belkaid, Y.; Hand, T. Role of the Microbiota in Immunity and Inflammation. Cell 2014, 157, 121–141. [Google Scholar] [CrossRef] [PubMed]
- Zheng, D.; Liwinski, T.; Elinav, E. Interaction between Microbiota and Immunity in Health and Disease. Cell Res. 2020, 30, 492–506. [Google Scholar] [CrossRef]
- Oh, D.; Cheon, K.-A. Alteration of Gut Microbiota in Autism Spectrum Disorder: An Overview. Soa Chongsonyon Chongsin Uihak 2020, 31, 131–145. [Google Scholar] [CrossRef] [PubMed]
- Rosario, D.; Boren, J.; Uhlen, M.; Proctor, G.; Aarsland, D.; Mardinoglu, A.; Shoaie, S. Systems Biology Approaches to Understand the Host–Microbiome Interactions in Neurodegenerative Diseases. Front. Neurosci. 2020, 14, 716. [Google Scholar] [CrossRef] [PubMed]
- Suganya, K.; Koo, B.-S. Gut–Brain Axis: Role of Gut Microbiota on Neurological Disorders and How Probiotics/Prebiotics Beneficially Modulate Microbial and Immune Pathways to Improve Brain Functions. Int. J. Mol. Sci. 2020, 21, 7551. [Google Scholar] [CrossRef] [PubMed]
- Kang, D.-W.; Adams, J.B.; Gregory, A.C.; Borody, T.; Chittick, L.; Fasano, A.; Khoruts, A.; Geis, E.; Maldonado, J.; McDonough-Means, S.; et al. Microbiota Transfer Therapy Alters Gut Ecosystem and Improves Gastrointestinal and Autism Symptoms: An Open-Label Study. Microbiome 2017, 5, 10. [Google Scholar] [CrossRef] [PubMed]
- Zuo, T.; Ng, S.C. The Gut Microbiota in the Pathogenesis and Therapeutics of Inflammatory Bowel Disease. Front. Microbiol. 2018, 9, 2247. [Google Scholar] [CrossRef] [PubMed]
- Huang, T.-T.; Lai, J.-B.; Du, Y.-L.; Xu, Y.; Ruan, L.-M.; Hu, S.-H. Current Understanding of Gut Microbiota in Mood Disorders: An Update of Human Studies. Front. Genet. 2019, 10, 98. [Google Scholar] [CrossRef]
- Fattorusso, A.; Di Genova, L.; Dell’Isola, G.B.; Mencaroni, E.; Esposito, S. Autism Spectrum Disorders and the Gut Microbiota. Nutrients 2019, 11, 521. [Google Scholar] [CrossRef]
- Garcia-Gutierrez, E.; Narbad, A.; Rodríguez, J.M. Autism Spectrum Disorder Associated With Gut Microbiota at Immune, Metabolomic, and Neuroactive Level. Front. Neurosci. 2020, 14, 578666. [Google Scholar] [CrossRef] [PubMed]
- Ye, F.; Gao, X.; Wang, Z.; Cao, S.; Liang, G.; He, D.; Lv, Z.; Wang, L.; Xu, P.; Zhang, Q. Comparison of Gut Microbiota in Autism Spectrum Disorders and Neurotypical Boys in China: A Case-Control Study. Synth. Syst. Biotechnol. 2021, 6, 120–126. [Google Scholar] [CrossRef]
- Sun, H.; You, Z.; Jia, L.; Wang, F. Autism Spectrum Disorder Is Associated with Gut Microbiota Disorder in Children. BMC Pediatr. 2019, 19, 516. [Google Scholar] [CrossRef]
- Patusco, R.; Ziegler, J. Role of Probiotics in Managing Gastrointestinal Dysfunction in Children with Autism Spectrum Disorder: An Update for Practitioners. Adv. Nutr. 2018, 9, 637–650. [Google Scholar] [CrossRef] [PubMed]
- Myles, I.A.; Fontecilla, N.M.; Janelsins, B.M.; Vithayathil, P.J.; Segre, J.A.; Datta, S.K. Parental Dietary Fat Intake Alters Offspring Microbiome and Immunity. J. Immunol. 2013, 191, 3200–3209. [Google Scholar] [CrossRef] [PubMed]
- Ursell, L.K.; Metcalf, J.L.; Parfrey, L.W.; Knight, R. Defining the Human Microbiome. Nutr. Rev. 2012, 70, S38–S44. [Google Scholar] [CrossRef] [PubMed]
- Galluzzi, L.; Magnani, M.; Saunders, N.; Harms, C.; Bruce, I.J. Current Molecular Techniques for the Detection of Microbial Pathogens. Sci. Progress 2007, 90, 29–50. [Google Scholar] [CrossRef]
- Bharti, R.; Grimm, D.G. Current Challenges and Best-Practice Protocols for Microbiome Analysis. Brief. Bioinform. 2021, 22, 178–193. [Google Scholar] [CrossRef] [PubMed]
- DuPont, A.W.; DuPont, H.L. The Intestinal Microbiota and Chronic Disorders of the Gut. Nat. Rev. Gastroenterol. Hepatol. 2011, 8, 523–531. [Google Scholar] [CrossRef] [PubMed]
- Salminen, S.; Isolauri, E.; Onnela, T. Gut Flora in Normal and Disordered States. CHE 1995, 41, 5–15. [Google Scholar] [CrossRef]
- Bull, M.J.; Plummer, N.T. Part 1: The Human Gut Microbiome in Health and Disease. Integr. Med. 2014, 13, 17–22. [Google Scholar]
- Ranucci, G.; Buccigrossi, V.; de Freitas, M.B.; Guarino, A.; Giannattasio, A. Early-Life Intestine Microbiota and Lung Health in Children. J. Immunol. Res. 2017, 2017, e8450496. [Google Scholar] [CrossRef]
- Macfarlane, S.; Macfarlane, G.T. Regulation of Short-Chain Fatty Acid Production. Proc. Nutr. Soc. 2003, 62, 67–72. [Google Scholar] [CrossRef] [PubMed]
- Nogay, N.H.; Nahikian-Nelms, M. Can We Reduce Autism-Related Gastrointestinal and Behavior Problems by Gut Microbiota Based Dietary Modulation? A Review. Nutr. Neurosci. 2021, 24, 327–338. [Google Scholar] [CrossRef] [PubMed]
- Coelho, O.G.L.; Cândido, F.G.; Alfenas, R.d.C.G. Dietary Fat and Gut Microbiota: Mechanisms Involved in Obesity Control. Crit. Rev. Food Sci. Nutr. 2019, 59, 3045–3053. [Google Scholar] [CrossRef] [PubMed]
- Richards, J.L.; Yap, Y.A.; McLeod, K.H.; Mackay, C.R.; Mariño, E. Dietary Metabolites and the Gut Microbiota: An Alternative Approach to Control Inflammatory and Autoimmune Diseases. Clin. Transl. Immunol. 2016, 5, e82. [Google Scholar] [CrossRef]
- Kelly, C.J.; Zheng, L.; Campbell, E.L.; Saeedi, B.; Scholz, C.C.; Bayless, A.J.; Wilson, K.E.; Glover, L.E.; Kominsky, D.J.; Magnuson, A.; et al. Crosstalk between Microbiota-Derived Short-Chain Fatty Acids and Intestinal Epithelial HIF Augments Tissue Barrier Function. Cell Host Microbe 2015, 17, 662–671. [Google Scholar] [CrossRef] [PubMed]
- Faruqui, N.A.; Prium, D.H.; Mowna, S.A.; Ullah, M.A.; Araf, Y.; Sarkar, B.; Zohora, U.S.; Rahman, M.S. Gut Microorganisms and Neurological Disease Perspectives. Future Neurol. 2021. [Google Scholar] [CrossRef]
- Tiffany, C.R.; Bäumler, A.J. Dysbiosis: From Fiction to Function. Am. J. Physiol. Gastrointest. Liver Physiol. 2019, 317, G602–G608. [Google Scholar] [CrossRef]
- Silva, Y.P.; Bernardi, A.; Frozza, R.L. The Role of Short-Chain Fatty Acids From Gut Microbiota in Gut-Brain Communication. Front. Endocrinol. 2020, 11. [Google Scholar] [CrossRef] [PubMed]
- Luna, R.A.; Savidge, T.C.; Williams, K.C. The Brain-Gut-Microbiome Axis: What Role Does It Play in Autism Spectrum Disorder? Curr. Dev. Disord. Rep. 2016, 3, 75–81. [Google Scholar] [CrossRef]
- Singh, R.; Zogg, H.; Wei, L.; Bartlett, A.; Ghoshal, U.C.; Rajender, S.; Ro, S. Gut Microbial Dysbiosis in the Pathogenesis of Gastrointestinal Dysmotility and Metabolic Disorders. J. Neurogastroenterol. Motil. 2021, 27, 19–34. [Google Scholar] [CrossRef]
- Carabotti, M.; Scirocco, A.; Maselli, M.A.; Severi, C. The Gut-Brain Axis: Interactions between Enteric Microbiota, Central and Enteric Nervous Systems. Ann. Gastroenterol. 2015, 28, 203–209. [Google Scholar]
- Sharon, G.; Cruz, N.J.; Kang, D.-W.; Gandal, M.J.; Wang, B.; Kim, Y.-M.; Zink, E.M.; Casey, C.P.; Taylor, B.C.; Lane, C.J.; et al. Human Gut Microbiota from Autism Spectrum Disorder Promote Behavioral Symptoms in Mice. Cell 2019, 177, 1600–1618.e17. [Google Scholar] [CrossRef]
- Sandler, R.H.; Finegold, S.M.; Bolte, E.R.; Buchanan, C.P.; Maxwell, A.P.; Väisänen, M.L.; Nelson, M.N.; Wexler, H.M. Short-Term Benefit from Oral Vancomycin Treatment of Regressive-Onset Autism. J. Child. Neurol. 2000, 15, 429–435. [Google Scholar] [CrossRef]
- Ristori, M.V.; Quagliariello, A.; Reddel, S.; Ianiro, G.; Vicari, S.; Gasbarrini, A.; Putignani, L. Autism, Gastrointestinal Symptoms and Modulation of Gut Microbiota by Nutritional Interventions. Nutrients 2019, 11, 2812. [Google Scholar] [CrossRef] [PubMed]
- Pulikkan, J.; Mazumder, A.; Grace, T. Role of the Gut Microbiome in Autism Spectrum Disorders. In Reviews on Biomarker Studies in Psychiatric and Neurodegenerative Disorders; Guest, P.C., Ed.; Advances in Experimental Medicine and Biology; Springer International Publishing: Cham, Switzerland, 2019; pp. 253–269. ISBN 978-3-030-05542-4. [Google Scholar]
- Barrett, E.; Ross, R.P.; O’Toole, P.W.; Fitzgerald, G.F.; Stanton, C. γ-Aminobutyric Acid Production by Culturable Bacteria from the Human Intestine. J. Appl. Microbiol. 2012, 113, 411–417. [Google Scholar] [CrossRef] [PubMed]
- Li, Q.; Han, Y.; Dy, A.B.C.; Hagerman, R.J. The Gut Microbiota and Autism Spectrum Disorders. Front. Cell. Neurosci. 2017, 11, 120. [Google Scholar] [CrossRef]
- Lyte, M. Probiotics Function Mechanistically as Delivery Vehicles for Neuroactive Compounds: Microbial Endocrinology in the Design and Use of Probiotics. Bioessays 2011, 33, 574–581. [Google Scholar] [CrossRef] [PubMed]
- Desbonnet, L.; Clarke, G.; Traplin, A.; O’Sullivan, O.; Crispie, F.; Moloney, R.D.; Cotter, P.D.; Dinan, T.G.; Cryan, J.F. Gut Microbiota Depletion from Early Adolescence in Mice: Implications for Brain and Behaviour. Brain Behav. Immun. 2015, 48, 165–173. [Google Scholar] [CrossRef]
- Huang, F.; Wu, X. Brain Neurotransmitter Modulation by Gut Microbiota in Anxiety and Depression. Front. Cell Dev. Biol. 2021, 9, 472. [Google Scholar] [CrossRef]
- Erny, D.; Hrabě de Angelis, A.L.; Jaitin, D.; Wieghofer, P.; Staszewski, O.; David, E.; Keren-Shaul, H.; Mahlakoiv, T.; Jakobshagen, K.; Buch, T.; et al. Host Microbiota Constantly Control Maturation and Function of Microglia in the CNS. Nat. Neurosci. 2015, 18, 965–977. [Google Scholar] [CrossRef]
- Huang, E.J.; Reichardt, L.F. Neurotrophins: Roles in Neuronal Development and Function. Annu. Rev. Neurosci. 2001, 24, 677–736. [Google Scholar] [CrossRef] [PubMed]
- Suliman, S.; Hemmings, S.; Seedat, S. Brain-Derived Neurotrophic Factor (BDNF) Protein Levels in Anxiety Disorders: Systematic Review and Meta-Regression Analysis. Front. Integr. Neurosci. 2013, 7, 55. [Google Scholar] [CrossRef] [PubMed]
- Wallisch, A.; Nowell, S.; Little, L. Picky Eating in Children with Autism Spectrum Disorder (ASD): An Examination of Behavioral Profiles. Am. J. Occup. 2020, 74, 7411510297p1. [Google Scholar] [CrossRef]
- Meguid, N.A.; Anwar, M.; Bjørklund, G.; Hashish, A.; Chirumbolo, S.; Hemimi, M.; Sultan, E. Dietary Adequacy of Egyptian Children with Autism Spectrum Disorder Compared to Healthy Developing Children. Metab. Brain Dis. 2017, 32, 607–615. [Google Scholar] [CrossRef]
- Al-Kindi, N.M.; Al-Farsi, Y.M.; Waly, M.I.; A-Shafaee, M.S.; Bakheit, C.S. Dietary Intake and Food Preferences of Autistic Children Versus Children with Typical Development: A Comparative Cross-Sectional Study. EC Nutr. 2016, 6, 72–85. [Google Scholar]
- El Khatib, A.A.; El Tekeya, M.M.; El Tantawi, M.A.; Omar, T. Oral Health Status and Behaviours of Children with Autism Spectrum Disorder: A Case-Control Study. Int. J. Paediatr. Dent. 2014, 24, 314–323. [Google Scholar] [CrossRef] [PubMed]
- Murshid, E.Z. Diet, Oral Hygiene Practices and Dental Health in Autistic Children in Riyadh, Saudi Arabia. Oral Health Dent. Manag. 2014, 13, 91–96. [Google Scholar] [PubMed]
- Hammouda, S.A.I.; Farghal, S.; Al-Harbi, G.; Abduallah, M.; Al-Rehaly, R.; Al-Johani, G. Assessment of Nutritional Risk Factors Predisposing to Autism among Saudi Children. Int. J. Nutraceuticals Funct. Foods Nov. Foods. 2018, 6. [Google Scholar] [CrossRef]
- Tharner, A.; Jansen, P.W.; Kiefte-de Jong, J.C.; Moll, H.A.; Hofman, A.; Jaddoe, V.W.V.; Tiemeier, H.; Franco, O.H. Bidirectional Associations between Fussy Eating and Functional Constipation in Preschool Children. J. Pediatrics 2015, 166, 91–96.e1. [Google Scholar] [CrossRef]
- Ismail, N.A.S.; Ramli, N.S.; Hamzaid, N.H.; Hassan, N.I. Exploring Eating and Nutritional Challenges for Children with Autism Spectrum Disorder: Parents’ and Special Educators’ Perceptions. Nutrients 2020, 12, 2530. [Google Scholar] [CrossRef]
- Thomas, F.; Hehemann, J.-H.; Rebuffet, E.; Czjzek, M.; Michel, G. Environmental and Gut Bacteroidetes: The Food Connection. Front. Microbiol. 2011, 2. [Google Scholar] [CrossRef]
- Seong, C.N.; Kang, J.W.; Lee, J.H.; Seo, S.Y.; Woo, J.J.; Park, C.; Bae, K.S.; Kim, M.S. Taxonomic Hierarchy of the Phylum Firmicutes and Novel Firmicutes Species Originated from Various Environments in Korea. J. Microbiol. 2018, 56, 1–10. [Google Scholar] [CrossRef]
- Liu, F.; Li, J.; Wu, F.; Zheng, H.; Peng, Q.; Zhou, H. Altered Composition and Function of Intestinal Microbiota in Autism Spectrum Disorders: A Systematic Review. Transl. Psychiatry 2019, 9, 1–13. [Google Scholar] [CrossRef] [PubMed]
- Tomova, A.; Husarova, V.; Lakatosova, S.; Bakos, J.; Vlkova, B.; Babinska, K.; Ostatnikova, D. Gastrointestinal Microbiota in Children with Autism in Slovakia. Physiol. Behav. 2015, 138, 179–187. [Google Scholar] [CrossRef] [PubMed]
- Finegold, S.M.; Dowd, S.E.; Gontcharova, V.; Liu, C.; Henley, K.E.; Wolcott, R.D.; Youn, E.; Summanen, P.H.; Granpeesheh, D.; Dixon, D.; et al. Pyrosequencing Study of Fecal Microflora of Autistic and Control Children. Anaerobe 2010, 16, 444–453. [Google Scholar] [CrossRef]
- Dordević, D.; Jančíková, S.; Vítězová, M.; Kushkevych, I. Hydrogen Sulfide Toxicity in the Gut Environment: Meta-Analysis of Sulfate-Reducing and Lactic Acid Bacteria in Inflammatory Processes. J. Adv. Res. 2021, 27, 55–69. [Google Scholar] [CrossRef]
- Finegold, S.M. Desulfovibrio Species Are Potentially Important in Regressive Autism. Med. Hypotheses 2011, 77, 270–274. [Google Scholar] [CrossRef] [PubMed]
- Buret, A.G.; Allain, T.; Motta, J.-P.; Wallace, J.L. Effects of Hydrogen Sulfide on the Microbiome: From Toxicity to Therapy. Antioxid. Redox Signal. 2021. [Google Scholar] [CrossRef]
- Kumbhare, S.V.; Francis-Lyon, P.A.; Kachru, D.; Uday, T.; Irudayanathan, C.; Muthukumar, K.M.; Ricchetti, R.R.; Singh-Rambiritch, S.; Ugalde, J.A.; Dulai, P.S.; et al. Digital Therapeutics Care Utilizing Genetic and Gut Microbiome Signals for the Management of Functional Gastrointestinal Disorders: Results from a Preliminary Retrospective Study. medRxiv 2021. [Google Scholar] [CrossRef]
- Finegold, S.M.; Downes, J.; Summanen, P.H. Microbiology of Regressive Autism. Anaerobe 2012, 18, 260–262. [Google Scholar] [CrossRef] [PubMed]
- Heberling, C.; Dhurjati, P. Novel Systems Modeling Methodology in Comparative Microbial Metabolomics: Identifying Key Enzymes and Metabolites Implicated in Autism Spectrum Disorders. Int. J. Mol. Sci. 2015, 16, 8949–8967. [Google Scholar] [CrossRef]
- MacFabe, D.F.; Cain, D.P.; Rodriguez-Capote, K.; Franklin, A.E.; Hoffman, J.E.; Boon, F.; Taylor, A.R.; Kavaliers, M.; Ossenkopp, K.-P. Neurobiological Effects of Intraventricular Propionic Acid in Rats: Possible Role of Short Chain Fatty Acids on the Pathogenesis and Characteristics of Autism Spectrum Disorders. Behav. Brain Res. 2007, 176, 149–169. [Google Scholar] [CrossRef] [PubMed]
- Foley, K.A.; MacFabe, D.F.; Vaz, A.; Ossenkopp, K.; Kavaliers, M. Sexually Dimorphic Effects of Prenatal Exposure to Propionic Acid and Lipopolysaccharide on Social Behavior in Neonatal, Adolescent, and Adult Rats: Implications for Autism Spectrum Disorders. Int. J. Dev. Neurosci. 2014, 39, 68–78. [Google Scholar] [CrossRef] [PubMed]
- Iovene, M.R.; Bombace, F.; Maresca, R.; Sapone, A.; Iardino, P.; Picardi, A.; Marotta, R.; Schiraldi, C.; Siniscalco, D.; Serra, N.; et al. Intestinal Dysbiosis and Yeast Isolation in Stool of Subjects with Autism Spectrum Disorders. Mycopathologia 2017, 182, 349–363. [Google Scholar] [CrossRef] [PubMed]
- Sabit, H.; Tombuloglu, H.; Rehman, S.; Almandil, N.B.; Cevik, E.; Abdel-Ghany, S.; Rashwan, S.; Abasiyanik, M.F.; Yee Waye, M.M. Gut Microbiota Metabolites in Autistic Children: An Epigenetic Perspective. Heliyon 2021, 7, e06105. [Google Scholar] [CrossRef]
- Madore, C.; Leyrolle, Q.; Lacabanne, C.; Benmamar-Badel, A.; Joffre, C.; Nadjar, A.; Layé, S. Neuroinflammation in Autism: Plausible Role of Maternal Inflammation, Dietary Omega 3, and Microbiota. Neural Plast. 2016, 2016, 3597209. [Google Scholar] [CrossRef] [PubMed]
- Parracho, H.M.; Bingham, M.O.; Gibson, G.R.; McCartney, A.L. Differences between the Gut Microflora of Children with Autistic Spectrum Disorders and That of Healthy Children. J. Med Microbiol. 2005, 54, 987–991. [Google Scholar] [CrossRef] [PubMed]
- Luna, R.A.; Oezguen, N.; Balderas, M.; Venkatachalam, A.; Runge, J.K.; Versalovic, J.; Veenstra-VanderWeele, J.; Anderson, G.M.; Savidge, T.; Williams, K.C. Distinct Microbiome-Neuroimmune Signatures Correlate with Functional Abdominal Pain in Children With Autism Spectrum Disorder. Cell. Mol. Gastroenterol. Hepatol. 2017, 3, 218–230. [Google Scholar] [CrossRef] [PubMed]
- Khalif, I.L.; Quigley, E.M.M.; Konovitch, E.A.; Maximova, I.D. Alterations in the Colonic Flora and Intestinal Permeability and Evidence of Immune Activation in Chronic Constipation. Dig. Liver Dis. 2005, 37, 838–849. [Google Scholar] [CrossRef] [PubMed]
- De Moraes, J.G.; Motta, M.E.F.d.A.; Beltrão, M.F.d.S.; Salviano, T.L.; da Silva, G.A.P. Fecal Microbiota and Diet of Children with Chronic Constipation. Int. J. Pediatrics 2016, 2016, e6787269. [Google Scholar] [CrossRef] [PubMed]
- Chassard, C.; Dapoigny, M.; Scott, K.P.; Crouzet, L.; Del’homme, C.; Marquet, P.; Martin, J.C.; Pickering, G.; Ardid, D.; Eschalier, A.; et al. Functional Dysbiosis within the Gut Microbiota of Patients with Constipated-Irritable Bowel Syndrome. Aliment. Pharmacol. Ther. 2012, 35, 828–838. [Google Scholar] [CrossRef]
- Zhao, Y.; Yu, Y.-B. Intestinal Microbiota and Chronic Constipation. Springerplus 2016, 5, 1130. [Google Scholar] [CrossRef]
- Zhang, M.; Ma, W.; Zhang, J.; He, Y.; Wang, J. Analysis of Gut Microbiota Profiles and Microbe-Disease Associations in Children with Autism Spectrum Disorders in China. Sci. Rep. 2018, 8, 13981. [Google Scholar] [CrossRef]
- Tana, C.; Umesaki, Y.; Imaoka, A.; Handa, T.; Kanazawa, M.; Fukudo, S. Altered Profiles of Intestinal Microbiota and Organic Acids May Be the Origin of Symptoms in Irritable Bowel Syndrome. Neurogastroenterol. Motil. 2010, 22, 512–519, e114. [Google Scholar] [CrossRef] [PubMed]
- De Magistris, L.; Familiari, V.; Pascotto, A.; Sapone, A.; Frolli, A.; Iardino, P.; Carteni, M.; De Rosa, M.; Francavilla, R.; Riegler, G.; et al. Alterations of the Intestinal Barrier in Patients with Autism Spectrum Disorders and in Their First-Degree Relatives. J. Pediatr. Gastroenterol. Nutr. 2010, 51, 418–424. [Google Scholar] [CrossRef] [PubMed]
- Nankova, B.B.; Agarwal, R.; MacFabe, D.F.; La Gamma, E.F. Enteric Bacterial Metabolites Propionic and Butyric Acid Modulate Gene Expression, Including CREB-Dependent Catecholaminergic Neurotransmission, in PC12 Cells--Possible Relevance to Autism Spectrum Disorders. PLoS ONE 2014, 9, e103740. [Google Scholar] [CrossRef]
- Vriesman, M.H.; Koppen, I.J.N.; Camilleri, M.; Di Lorenzo, C.; Benninga, M.A. Management of Functional Constipation in Children and Adults. Nat. Rev. Gastroenterol. Hepatol. 2020, 17, 21–39. [Google Scholar] [CrossRef]
- Strati, F.; Cavalieri, D.; Albanese, D.; De Felice, C.; Donati, C.; Hayek, J.; Jousson, O.; Leoncini, S.; Renzi, D.; Calabrò, A.; et al. New Evidences on the Altered Gut Microbiota in Autism Spectrum Disorders. Microbiome 2017, 5, 24. [Google Scholar] [CrossRef]
- Liu, S.; Li, E.; Sun, Z.; Fu, D.; Duan, G.; Jiang, M.; Yu, Y.; Mei, L.; Yang, P.; Tang, Y. Altered Gut Microbiota and Short Chain Fatty Acids in Chinese Children with Autism Spectrum Disorder. Sci. Rep. 2019, 9, 1–9. [Google Scholar] [CrossRef] [PubMed]
- Fu, S.-C.; Lee, C.-H.; Wang, H. Exploring the Association of Autism Spectrum Disorders and Constipation through Analysis of the Gut Microbiome. Int. J. Environ. Res. Public Health 2021, 18, 667. [Google Scholar] [CrossRef] [PubMed]
- Dan, Z.; Mao, X.; Liu, Q.; Guo, M.; Zhuang, Y.; Liu, Z.; Chen, K.; Chen, J.; Xu, R.; Tang, J.; et al. Altered Gut Microbial Profile Is Associated with Abnormal Metabolism Activity of Autism Spectrum Disorder. Gut Microbes 2020, 11, 1246–1267. [Google Scholar] [CrossRef] [PubMed]
- Wang, L.; Christophersen, C.T.; Sorich, M.J.; Gerber, J.P.; Angley, M.T.; Conlon, M.A. Increased Abundance of Sutterella Spp. and Ruminococcus Torques in Feces of Children with Autism Spectrum Disorder. Mol. Autism 2013, 4, 42. [Google Scholar] [CrossRef]
- Wang, L.; Christophersen, C.T.; Sorich, M.J.; Gerber, J.P.; Angley, M.T.; Conlon, M.A. Low Relative Abundances of the Mucolytic Bacterium Akkermansia Muciniphila and Bifidobacterium Spp. in Feces of Children with Autism. Appl. Env. Microbiol. 2011, 77, 6718–6721. [Google Scholar] [CrossRef]
- Kong, X.; Liu, J.; Cetinbas, M.; Sadreyev, R.; Koh, M.; Huang, H.; Adeseye, A.; He, P.; Zhu, J.; Russell, H.; et al. New and Preliminary Evidence on Altered Oral and Gut Microbiota in Individuals with Autism Spectrum Disorder (ASD): Implications for ASD Diagnosis and Subtyping Based on Microbial Biomarkers. Nutrients 2019, 11, 2128. [Google Scholar] [CrossRef] [PubMed]
- Rose, D.R.; Yang, H.; Serena, G.; Sturgeon, C.; Ma, B.; Careaga, M.; Hughes, H.K.; Angkustsiri, K.; Rose, M.; Hertz-Picciotto, I.; et al. Differential Immune Responses and Microbiota Profiles in Children with Autism Spectrum Disorders and Co-Morbid Gastrointestinal Symptoms. Brain Behav. Immun. 2018, 70, 354–368. [Google Scholar] [CrossRef]
- Willis, A.D. Rarefaction, Alpha Diversity, and Statistics. Front. Microbiol. 2019, 10, 2407. [Google Scholar] [CrossRef] [PubMed]
- Ho, L.K.H.; Tong, V.J.W.; Syn, N.; Nagarajan, N.; Tham, E.H.; Tay, S.K.; Shorey, S.; Tambyah, P.A.; Law, E.C.N. Gut Microbiota Changes in Children with Autism Spectrum Disorder: A Systematic Review. Gut Pathog. 2020, 12, 6. [Google Scholar] [CrossRef] [PubMed]
- Li, N.; Yang, J.; Zhang, J.; Liang, C.; Wang, Y.; Chen, B.; Zhao, C.; Wang, J.; Zhang, G.; Zhao, D.; et al. Correlation of Gut Microbiome Between ASD Children and Mothers and Potential Biomarkers for Risk Assessment. Genom. Proteom. Bioinform. 2019, 17, 26–38. [Google Scholar] [CrossRef] [PubMed]
- Gondalia, S.V.; Palombo, E.A.; Knowles, S.R.; Cox, S.B.; Meyer, D.; Austin, D.W. Molecular Characterisation of Gastrointestinal Microbiota of Children with Autism (with and without Gastrointestinal Dysfunction) and Their Neurotypical Siblings. Autism Res. 2012, 5, 419–427. [Google Scholar] [CrossRef]
- Flint, H.J.; Duncan, S.H.; Scott, K.P.; Louis, P. Links between Diet, Gut Microbiota Composition and Gut Metabolism. Proc. Nutr. Soc. 2015, 74, 13–22. [Google Scholar] [CrossRef]
- Jin, Y.; Wu, S.; Zeng, Z.; Fu, Z. Effects of Environmental Pollutants on Gut Microbiota. Environ. Pollut. 2017, 222, 1–9. [Google Scholar] [CrossRef]
- Rinninella, E.; Raoul, P.; Cintoni, M.; Franceschi, F.; Miggiano, G.A.D.; Gasbarrini, A.; Mele, M.C. What Is the Healthy Gut Microbiota Composition? A Changing Ecosystem across Age, Environment, Diet, and Diseases. Microorganisms 2019, 7, 14. [Google Scholar] [CrossRef]
- Singh, R.K.; Chang, H.-W.; Yan, D.; Lee, K.M.; Ucmak, D.; Wong, K.; Abrouk, M.; Farahnik, B.; Nakamura, M.; Zhu, T.H.; et al. Influence of Diet on the Gut Microbiome and Implications for Human Health. J. Transl. Med. 2017, 15, 73. [Google Scholar] [CrossRef]
- Clifford, J.; Kozil, A. Dietary Fat and Cholesterol. Available online: https://extension.colostate.edu/topic-areas/nutrition-food-safety-health/dietary-fat-and-cholesterol-9-319/ (accessed on 14 April 2021).
- APUS: An Introduction to Nutrition (Byerley). Available online: https://med.libretexts.org/Courses/American_Public_University/APUS%3A_An_Introduction_to_Nutrition_(Byerley) (accessed on 14 April 2021).
- Lang, J.M.; Pan, C.; Cantor, R.M.; Tang, W.H.W.; Garcia-Garcia, J.C.; Kurtz, I.; Hazen, S.L.; Bergeron, N.; Krauss, R.M.; Lusis, A.J. Impact of Individual Traits, Saturated Fat, and Protein Source on the Gut Microbiome. mBio 2018, 9. [Google Scholar] [CrossRef] [PubMed]
- Cândido, F.G.; Valente, F.X.; Grześkowiak, Ł.M.; Moreira, A.P.B.; Rocha, D.M.U.P.; Alfenas, R.d.C.G. Impact of Dietary Fat on Gut Microbiota and Low-Grade Systemic Inflammation: Mechanisms and Clinical Implications on Obesity. Int. J. Food Sci. Nutr. 2018, 69, 125–143. [Google Scholar] [CrossRef] [PubMed]
- Bailey, M.A.; Holscher, H.D. Microbiome-Mediated Effects of the Mediterranean Diet on Inflammation. Adv. Nutr. 2018, 9, 193–206. [Google Scholar] [CrossRef] [PubMed]
- Harvard—School of Public Health Types of Fat. Available online: https://www.hsph.harvard.edu/nutritionsource/what-should-you-eat/fats-and-cholesterol/types-of-fat/ (accessed on 14 April 2021).
- Christie, W. Sterols: 5. Bile Acids and Alcohols. 2021. Available online: https://www.lipidmaps.org/resources/lipidweb/lipidweb_html/lipids/simple/bileacids/index.htm (accessed on 27 April 2021).
- Ridlon, J.M.; Kang, D.J.; Hylemon, P.B.; Bajaj, J.S. Bile Acids and the Gut Microbiome. Curr. Opin. Gastroenterol. 2014, 30, 332–338. [Google Scholar] [CrossRef]
- Hall, J.E.; Guyton, A.C. Guyton and Hall Textbook of Medical Physiology, 12th ed.; Saunders/Elsevier: Philadelphia, PA, USA, 2011; ISBN 978-1-4160-4574-8. [Google Scholar]
- Ajouz, H.; Mukherji, D.; Shamseddine, A. Secondary Bile Acids: An Underrecognized Cause of Colon Cancer. World J. Surg. Oncol. 2014, 12, 164. [Google Scholar] [CrossRef] [PubMed]
- Zeng, H.; Umar, S.; Rust, B.; Lazarova, D.; Bordonaro, M. Secondary Bile Acids and Short Chain Fatty Acids in the Colon: A Focus on Colonic Microbiome, Cell Proliferation, Inflammation, and Cancer. Int. J. Mol. Sci. 2019, 20, 1214. [Google Scholar] [CrossRef] [PubMed]
- Pavlidis, P.; Powell, N.; Vincent, R.P.; Ehrlich, D.; Bjarnason, I.; Hayee, B. Systematic Review: Bile Acids and Intestinal Inflammation-Luminal Aggressors or Regulators of Mucosal Defence? Aliment. Pharmacol. Ther. 2015, 42, 802–817. [Google Scholar] [CrossRef]
- Winston, J.A.; Theriot, C.M. Diversification of Host Bile Acids by Members of the Gut Microbiota. Gut Microbes 2020, 11, 158–171. [Google Scholar] [CrossRef]
- Wasilewska, J.; Klukowski, M. Gastrointestinal Symptoms and Autism Spectrum Disorder: Links and Risks—A Possible New Overlap Syndrome. Pediatric Health Med. 2015, 6, 153–166. [Google Scholar] [CrossRef] [PubMed]
- Natividad, J.M.; Lamas, B.; Pham, H.P.; Michel, M.-L.; Rainteau, D.; Bridonneau, C.; da Costa, G.; van Hylckama Vlieg, J.; Sovran, B.; Chamignon, C.; et al. Bilophila Wadsworthia Aggravates High Fat Diet Induced Metabolic Dysfunctions in Mice. Nat. Commun. 2018, 9, 2802. [Google Scholar] [CrossRef]
- Zhou, Q.; Zhang, B.; Verne, G.N. Intestinal Membrane Permeability and Hypersensitivity In the Irritable Bowel Syndrome. Pain 2009, 146, 41–46. [Google Scholar] [CrossRef] [PubMed]
- Turnbaugh, P.J. Fat, Bile and Gut Microbes. Nature 2012, 487, 47–48. [Google Scholar] [CrossRef]
- De Wit, N.; Derrien, M.; Bosch-Vermeulen, H.; Oosterink, E.; Keshtkar, S.; Duval, C.; de Vogel-van den Bosch, J.; Kleerebezem, M.; Müller, M.; van der Meer, R. Saturated Fat Stimulates Obesity and Hepatic Steatosis and Affects Gut Microbiota Composition by an Enhanced Overflow of Dietary Fat to the Distal Intestine. Am. J. Physiol. Gastrointest. Liver Physiol. 2012, 303, G589–G599. [Google Scholar] [CrossRef] [PubMed]
- Gong, D.; Gong, X.; Wang, L.; Yu, X.; Dong, Q. Involvement of Reduced Microbial Diversity in Inflammatory Bowel Disease. Gastroenterol. Res. Pract. 2016, 2016, e6951091. [Google Scholar] [CrossRef]
- Dieterich, W.; Schink, M.; Zopf, Y. Microbiota in the Gastrointestinal Tract. Med. Sci. 2018, 6, 116. [Google Scholar] [CrossRef] [PubMed]
- Jurgoński, A.; Juśkiewicz, J.; Zduńczyk, Z. A High-Fat Diet Differentially Affects the Gut Metabolism and Blood Lipids of Rats Depending on the Type of Dietary Fat and Carbohydrate. Nutrients 2014, 6, 616–626. [Google Scholar] [CrossRef]
- De Filippo, C.; Cavalieri, D.; Paola, M.D.; Ramazzotti, M.; Poullet, J.B.; Massart, S.; Collini, S.; Pieraccini, G.; Lionetti, P. Impact of Diet in Shaping Gut Microbiota Revealed by a Comparative Study in Children from Europe and Rural Africa. Proc. Natl. Acad. Sci. USA 2010, 107, 14691–14696. [Google Scholar] [CrossRef]
- Devkota, S.; Wang, Y.; Musch, M.; Leone, V.; Fehlner-Peach, H.; Nadimpalli, A.; Antonopoulos, D.A.; Jabri, B.; Chang, E.B. Dietary Fat-Induced Taurocholic Acid Production Promotes Pathobiont and Colitis in IL-10−/− Mice. Nature 2012, 487, 104–108. [Google Scholar] [CrossRef] [PubMed]
- Statovci, D.; Aguilera, M.; MacSharry, J.; Melgar, S. The Impact of Western Diet and Nutrients on the Microbiota and Immune Response at Mucosal Interfaces. Front. Immunol. 2017, 8. [Google Scholar] [CrossRef] [PubMed]
- Hentges, D.J.; Maier, B.R.; Burton, G.C.; Flynn, M.A.; Tsutakawa, R.K. Effect of a High-Beef Diet on the Fecal Bacterial Flora of Humans. Cancer Res. 1977, 37, 568–571. [Google Scholar]
- Wang, G.; Jiao, T.; Xu, Y.; Li, D.; Si, Q.; Hao, J.; Zhao, J.; Zhang, H.; Chen, W. Bifidobacterium Adolescentis and Lactobacillus Rhamnosus Alleviate Non-Alcoholic Fatty Liver Disease Induced by a High-Fat, High-Cholesterol Diet through Modulation of Different Gut Microbiota-Dependent Pathways. Food Funct. 2020, 11, 6115–6127. [Google Scholar] [CrossRef] [PubMed]
- Ito, Y.; Kikuchi, E.; Tanaka, N.; Kosaka, T.; Suzuki, E.; Mizuno, R.; Shinojima, T.; Miyajima, A.; Umezawa, K.; Oya, M. Down-Regulation of NF Kappa B Activation Is an Effective Therapeutic Modality in Acquired Platinum-Resistant Bladder Cancer. BMC Cancer 2015, 15, 1–11. [Google Scholar] [CrossRef] [PubMed]
- Ahola, A.J.; Lassenius, M.I.; Forsblom, C.; Harjutsalo, V.; Lehto, M.; Groop, P.-H. Dietary Patterns Reflecting Healthy Food Choices Are Associated with Lower Serum LPS Activity. Sci. Rep. 2017, 7, 6511. [Google Scholar] [CrossRef]
- Pendyala, S.; Walker, J.M.; Holt, P.R. A High-Fat Diet Is Associated With Endotoxemia That Originates From the Gut. Gastroenterology 2012, 142, 1100–1101.e2. [Google Scholar] [CrossRef]
- Nozu, T.; Miyagishi, S.; Nozu, R.; Takakusaki, K.; Okumura, T. Lipopolysaccharide Induces Visceral Hypersensitivity: Role of Interleukin-1, Interleukin-6, and Peripheral Corticotropin-Releasing Factor in Rats. J. Gastroenterol. 2017, 52, 72–80. [Google Scholar] [CrossRef] [PubMed]
- Delvaux, M. Role of Visceral Sensitivity in the Pathophysiology of Irritable Bowel Syndrome. Gut 2002, 51, i67–i71. [Google Scholar] [CrossRef][Green Version]
- David, L.A.; Maurice, C.F.; Carmody, R.N.; Gootenberg, D.B.; Button, J.E.; Wolfe, B.E.; Ling, A.V.; Devlin, A.S.; Varma, Y.; Fischbach, M.A.; et al. Diet Rapidly and Reproducibly Alters the Human Gut Microbiome. Nature 2014, 505, 559–563. [Google Scholar] [CrossRef] [PubMed]
- Parker, B.J.; Wearsch, P.A.; Veloo, A.C.M.; Rodriguez-Palacios, A. The Genus Alistipes: Gut Bacteria With Emerging Implications to Inflammation, Cancer, and Mental Health. Front. Immunol. 2020, 11, 906. [Google Scholar] [CrossRef] [PubMed]
- Saulnier, D.M.; Riehle, K.; Mistretta, T.-A.; Diaz, M.-A.; Mandal, D.; Raza, S.; Weidler, E.M.; Qin, X.; Coarfa, C.; Milosavljevic, A.; et al. Gastrointestinal Microbiome Signatures of Pediatric Patients with Irritable Bowel Syndrome. Gastroenterology 2011, 141, 1782–1791. [Google Scholar] [CrossRef] [PubMed]
- Zhu, L.; Sha, L.; Li, K.; Wang, Z.; Wang, T.; Li, Y.; Liu, P.; Dong, X.; Dong, Y.; Zhang, X.; et al. Dietary Flaxseed Oil Rich in Omega-3 Suppresses Severity of Type 2 Diabetes Mellitus via Anti-Inflammation and Modulating Gut Microbiota in Rats. Lipids Health Dis. 2020, 19, 20. [Google Scholar] [CrossRef] [PubMed]
- Sivamaruthi, B.S.; Suganthy, N.; Kesika, P.; Chaiyasut, C. The Role of Microbiome, Dietary Supplements, and Probiotics in Autism Spectrum Disorder. Int. J. Env. Res. Public Health 2020, 17, 2647. [Google Scholar] [CrossRef]
- Parellada, M.; Llorente, C.; Calvo, R.; Gutierrez, S.; Lázaro, L.; Graell, M.; Guisasola, M.; Dorado, M.L.; Boada, L.; Romo, J.; et al. Randomized Trial of Omega-3 for Autism Spectrum Disorders: Effect on Cell Membrane Composition and Behavior. Eur. Neuropsychopharmacol. 2017, 27, 1319–1330. [Google Scholar] [CrossRef] [PubMed]
- Tabbaa, M.; Golubic, M.; Roizen, M.F.; Bernstein, A.M. Docosahexaenoic Acid, Inflammation, and Bacterial Dysbiosis in Relation to Periodontal Disease, Inflammatory Bowel Disease, and the Metabolic Syndrome. Nutrients 2013, 5, 3299–3310. [Google Scholar] [CrossRef]
- Menni, C.; Zierer, J.; Pallister, T.; Jackson, M.A.; Long, T.; Mohney, R.P.; Steves, C.J.; Spector, T.D.; Valdes, A.M. Omega-3 Fatty Acids Correlate with Gut Microbiome Diversity and Production of N-Carbamylglutamate in Middle Aged and Elderly Women. Sci. Rep. 2017, 7, 11079. [Google Scholar] [CrossRef] [PubMed]
- Das, U.N. Autism as a Disorder of Deficiency of Brain-Derived Neurotrophic Factor and Altered Metabolism of Polyunsaturated Fatty Acids. Nutrition 2013, 29, 1175–1185. [Google Scholar] [CrossRef]
- Watson, H.; Mitra, S.; Croden, F.C.; Taylor, M.; Wood, H.M.; Perry, S.L.; Spencer, J.A.; Quirke, P.; Toogood, G.J.; Lawton, C.L.; et al. A Randomised Trial of the Effect of Omega-3 Polyunsaturated Fatty Acid Supplements on the Human Intestinal Microbiota. BMJ 2017, 11. [Google Scholar] [CrossRef] [PubMed]
- Tamanai-Shacoori, Z.; Smida, I.; Bousarghin, L.; Loreal, O.; Meuric, V.; Fong, S.B.; Bonnaure-Mallet, M.; Jolivet-Gougeon, A. Roseburia Spp.: A Marker of Health? Future Microbiol. 2017, 12, 157–170. [Google Scholar] [CrossRef]
- De Angelis, M.; Francavilla, R.; Piccolo, M.; De Giacomo, A.; Gobbetti, M. Autism Spectrum Disorders and Intestinal Microbiota. Gut Microbes 2015, 6, 207–213. [Google Scholar] [CrossRef] [PubMed]
- Ferguson, B.J.; Dovgan, K.; Severns, D.; Martin, S.; Marler, S.; Gross Margolis, K.; Bauman, M.L.; Veenstra-VanderWeele, J.; Sohl, K.; Beversdorf, D.Q. Lack of Associations Between Dietary Intake and Gastrointestinal Symptoms in Autism Spectrum Disorder. Front. Psychiatry 2019, 10, 528. [Google Scholar] [CrossRef]
- Mankad, D.; Dupuis, A.; Smile, S.; Roberts, W.; Brian, J.; Lui, T.; Genore, L.; Zaghloul, D.; Iaboni, A.; Marcon, P.; et al. A Randomized, Placebo Controlled Trial of Omega-3 Fatty Acids in the Treatment of Young Children with Autism. Mol. Autism 2015, 6, 18. [Google Scholar] [CrossRef] [PubMed]
- Caesar, R.; Tremaroli, V.; Kovatcheva-Datchary, P.; Cani, P.D.; Bäckhed, F. Crosstalk between Gut Microbiota and Dietary Lipids Aggravates WAT Inflammation through TLR Signaling. Cell Metab. 2015, 22, 658–668. [Google Scholar] [CrossRef] [PubMed]
- Holscher, H.D.; Taylor, A.M.; Swanson, K.S.; Novotny, J.A.; Baer, D.J. Almond Consumption and Processing Affects the Composition of the Gastrointestinal Microbiota of Healthy Adult Men and Women: A Randomized Controlled Trial. Nutrients 2018, 10, 126. [Google Scholar] [CrossRef] [PubMed]
- Holscher, H.D.; Guetterman, H.M.; Swanson, K.S.; An, R.; Matthan, N.R.; Lichtenstein, A.H.; Novotny, J.A.; Baer, D.J. Walnut Consumption Alters the Gastrointestinal Microbiota, Microbially Derived Secondary Bile Acids, and Health Markers in Healthy Adults: A Randomized Controlled Trial. J. Nutr. 2018, 148, 861–867. [Google Scholar] [CrossRef] [PubMed]
- Pu, S.; Khazanehei, H.; Jones, P.J.; Khafipour, E. Interactions between Obesity Status and Dietary Intake of Monounsaturated and Polyunsaturated Oils on Human Gut Microbiome Profiles in the Canola Oil Multicenter Intervention Trial (COMIT). Front. Microbiol. 2016, 7, 1612. [Google Scholar] [CrossRef] [PubMed]
- Costantini, L.; Molinari, R.; Farinon, B.; Merendino, N. Impact of Omega-3 Fatty Acids on the Gut Microbiota. Int. J. Mol. Sci. 2017, 18, 2645. [Google Scholar] [CrossRef] [PubMed]
- Mandal, S.; Godfrey, K.; McDonald, D.; Treuren, W.; Bjørnholt, J.; Midtvedt, T.; Moen, B.; Rudi, K.; Knight, R.; Brantsaeter, A.L.; et al. Fat and Vitamin Intakes during Pregnancy Have Stronger Relations with a Pro-Inflammatory Maternal Microbiota than Does Carbohydrate Intake. Microbiome 2016, 4, 1–11. [Google Scholar] [CrossRef]
- Berding, K.; Donovan, S.M. Microbiome and Nutrition in Autism Spectrum Disorder: Current Knowledge and Research Needs. Nutr. Rev. 2016, 74, 723–736. [Google Scholar] [CrossRef] [PubMed]
- Academy of Nutrition and Dietetics What Is the Ketogenic Diet. Available online: https://www.eatright.org/health/weight-loss/fad-diets/what-is-the-ketogenic-diet (accessed on 28 April 2021).
- Castro, K.; Faccioli, L.S.; Baronio, D.; Gottfried, C.; Perry, I.S.; dos Santos Riesgo, R. Effect of a Ketogenic Diet on Autism Spectrum Disorder: A Systematic Review. Res. Autism Spectr. Disord. 2015, 20, 31–38. [Google Scholar] [CrossRef]
- Varesio, C.; Grumi, S.; Zanaboni, M.P.; Mensi, M.M.; Chiappedi, M.; Pasca, L.; Ferraris, C.; Tagliabue, A.; Borgatti, R.; De Giorgis, V. Ketogenic Dietary Therapies in Patients with Autism Spectrum Disorder: Facts or Fads? A Scoping Review and a Proposal for a Shared Protocol. Nutrients 2021, 13, 2057. [Google Scholar] [CrossRef]
- Hadizadeh, F.; Bonfiglio, F.; Belheouane, M.; Vallier, M.; Sauer, S.; Bang, C.; Bujanda, L.; Andreasson, A.; Agreus, L.; Engstrand, L.; et al. Faecal Microbiota Composition Associates with Abdominal Pain in the General Population. Gut 2018, 67, 778–779. [Google Scholar] [CrossRef]
- Islam, K.B.M.S.; Fukiya, S.; Hagio, M.; Fujii, N.; Ishizuka, S.; Ooka, T.; Ogura, Y.; Hayashi, T.; Yokota, A. Bile Acid Is a Host Factor That Regulates the Composition of the Cecal Microbiota in Rats. Gastroenterology 2011, 141, 1773–1781. [Google Scholar] [CrossRef]
- Meng, Y.; Li, X.; Zhang, J.; Wang, C.; Lu, F. Effects of Different Diets on Microbiota in The Small Intestine Mucus and Weight Regulation in Rats. Sci. Rep. 2019, 9, 8500. [Google Scholar] [CrossRef] [PubMed]
- Neyrinck, A.M.; Possemiers, S.; Verstraete, W.; De Backer, F.; Cani, P.D.; Delzenne, N.M. Dietary Modulation of Clostridial Cluster XIVa Gut Bacteria (Roseburia Spp.) by Chitin–Glucan Fiber Improves Host Metabolic Alterations Induced by High-Fat Diet in Mice. J. Nutr. Biochem. 2012, 23, 51–59. [Google Scholar] [CrossRef] [PubMed]
- Conlon, M.A.; Bird, A.R. The Impact of Diet and Lifestyle on Gut Microbiota and Human Health. Nutrients 2014, 7, 17–44. [Google Scholar] [CrossRef] [PubMed]
- Zhang, L.; Wei, X.; Zhang, R.; Si, D.; Petitte, J.N.; Ahmad, B.; Zhang, M. A Novel Peptide Ameliorates LPS-Induced Intestinal Inflammation and Mucosal Barrier Damage via Its Antioxidant and Antiendotoxin Effects. Int. J. Mol. Sci. 2019, 20, 3974. [Google Scholar] [CrossRef] [PubMed]
- Emanuele, E.; Orsi, P.; Boso, M.; Broglia, D.; Brondino, N.; Barale, F.; di Nemi, S.U.; Politi, P. Low-Grade Endotoxemia in Patients with Severe Autism. Neurosci. Lett. 2010, 471, 162–165. [Google Scholar] [CrossRef] [PubMed]
- Fava, F.; Gitau, R.; Griffin, B.A.; Gibson, G.R.; Tuohy, K.M.; Lovegrove, J.A. The Type and Quantity of Dietary Fat and Carbohydrate Alter Faecal Microbiome and Short-Chain Fatty Acid Excretion in a Metabolic Syndrome “at-Risk” Population. Int. J. Obes. 2013, 37, 216–223. [Google Scholar] [CrossRef] [PubMed]
- Rodes, L.; Khan, A.; Paul, A.; Coussa-Charley, M.; Marinescu, D.; Tomaro-Duchesneau, C.; Shao, W.; Kahouli, I.; Prakash, S. Effect of Probiotics Lactobacillus and Bifidobacterium on Gut-Derived Lipopolysaccharides and Inflammatory Cytokines: An in Vitro Study Using a Human Colonic Microbiota Model. J. Microbiol. Biotechnol. 2013, 23, 518–526. [Google Scholar] [CrossRef] [PubMed]
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).