Changes of Exercise, Screen Time, Fast Food Consumption, Alcohol, and Cigarette Smoking during the COVID-19 Pandemic among Adults in the United States
Abstract
:1. Introduction
2. Methods
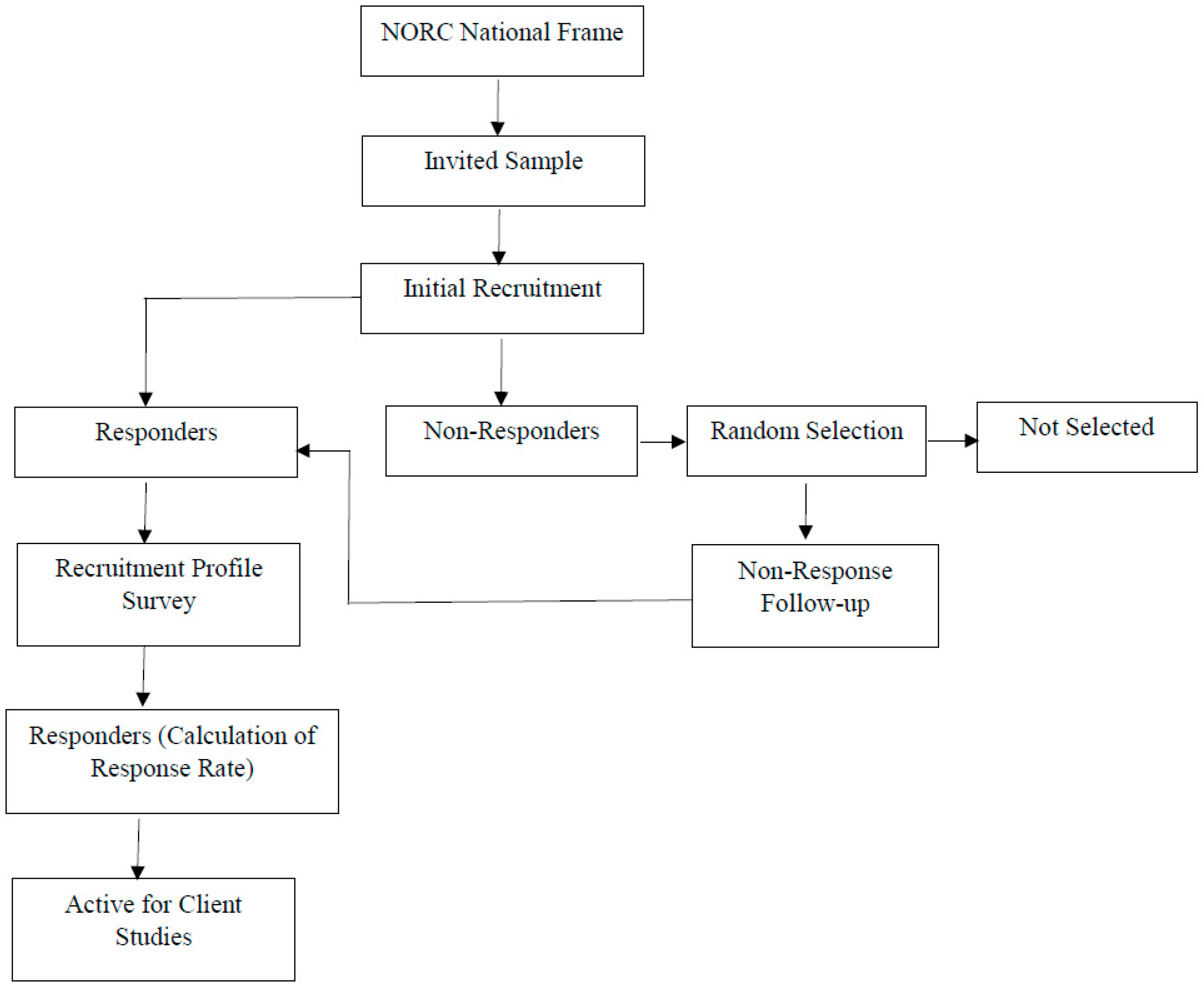
2.1. Study Design and Population
2.2. Survey Design and Measures
2.3. Statistical Analysis
3. Results
3.1. Characteristics of Study Participants
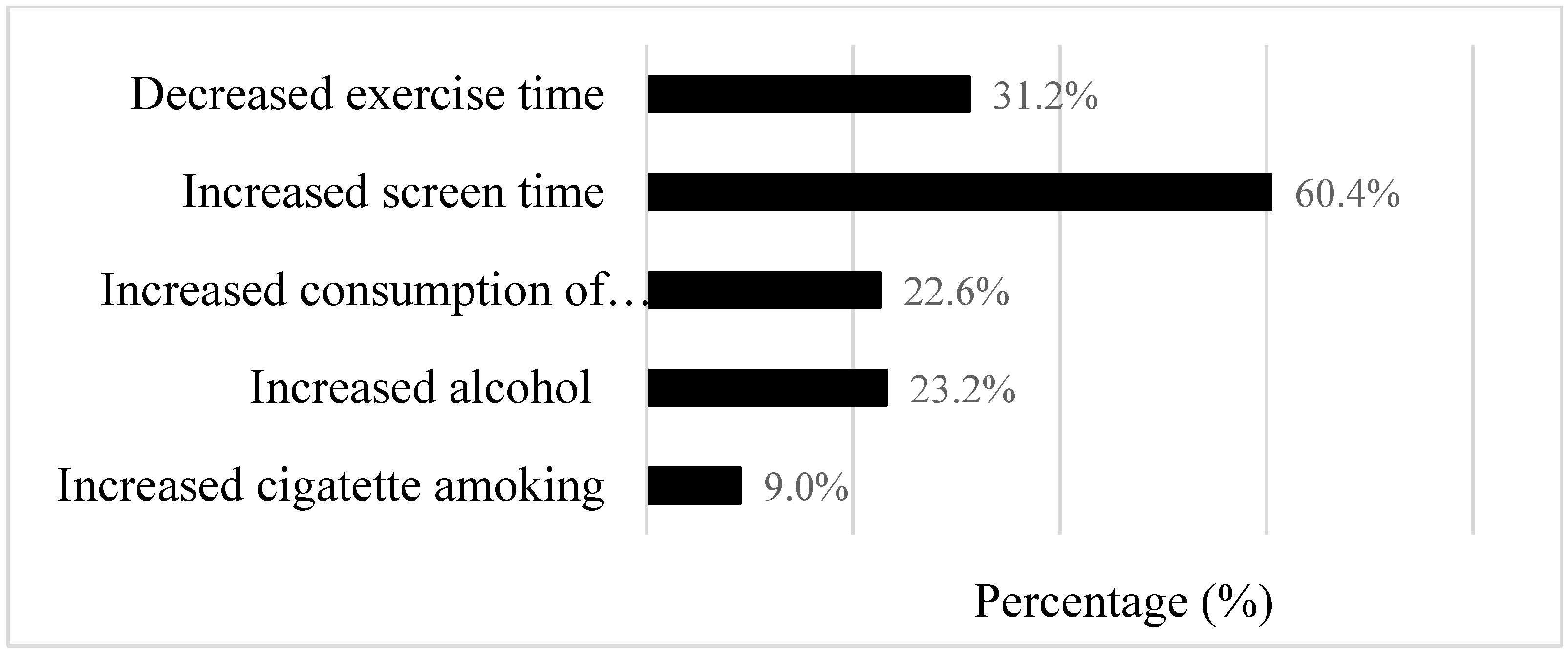
3.2. Lifestyle Behaviors before and during the COVID-19 Pandemic
3.3. Sociodemographic Factors Associated with Changes in Individual Lifestyle Behaviors
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Piret, J.; Boivin, G. Pandemics Throughout History. Front. Microbiol. 2020, 11, 631736. [Google Scholar] [CrossRef] [PubMed]
- Wiersinga, W.J.; Prescott, H.C. What Is COVID-19? JAMA 2020, 324, 816. [Google Scholar] [CrossRef] [PubMed]
- Wiersinga, W.J.; Rhodes, A.; Cheng, A.C.; Peacock, S.J.; Prescott, H.C. Pathophysiology, Transmission, Diagnosis, and Treatment of Coronavirus Disease 2019 (COVID-19): A Review. JAMA 2020, 324, 782–793. [Google Scholar] [CrossRef] [PubMed]
- WHO. WHO COVID-19 Dashboard. Available online: https://covid19.who.int (accessed on 6 September 2021).
- Lau, J.T.; Yang, X.; Tsui, H.; Pang, E.; Kim, J.H. SARS preventive and risk behaviours of Hong Kong air travellers. Epidemiol. Infect. 2004, 132, 727–736. [Google Scholar] [CrossRef] [PubMed]
- Tan, X.; Li, S.; Wang, C.; Chen, X.; Wu, X. Severe acute respiratory syndrome epidemic and change of people’s health behavior in China. Health Educ. Res. 2004, 19, 576–580. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Moore, S.A.; Faulkner, G.; Rhodes, R.E.; Brussoni, M.; Chulak-Bozzer, T.; Ferguson, L.J.; Mitra, R.; O’Reilly, N.; Spence, J.C.; Vanderloo, L.M.; et al. Impact of the COVID-19 virus outbreak on movement and play behaviours of Canadian children and youth: A national survey. Int. J. Behav. Nutr. Phys. Act. 2020, 17, 85. [Google Scholar] [CrossRef] [PubMed]
- Ferrante, G.; Camussi, E.; Piccinelli, C.; Senore, C.; Armaroli, P.; Ortale, A.; Garena, F.; Giordano, L. Did social isolation during the SARS-CoV-2 epidemic have an impact on the lifestyles of citizens? Epidemiol. Prev. 2020, 44 (Suppl. 2), 353–362. [Google Scholar] [PubMed]
- Di Renzo, L.; Gualtieri, P.; Pivari, F.; Soldati, L.; Attina, A.; Cinelli, G.; Leggeri, C.; Caparello, G.; Barrea, L.; Scerbo, F.; et al. Eating habits and lifestyle changes during COVID-19 lockdown: An Italian survey. J. Transl. Med. 2020, 18, 229. [Google Scholar] [CrossRef] [PubMed]
- Werneck, A.O.; Silva, D.R.; Malta, D.C.; Gomes, C.S.; Souza-Junior, P.R.; Azevedo, L.O.; Barros, M.B.; Szwarcwald, C.L. Associations of sedentary behaviours and incidence of unhealthy diet during the COVID-19 quarantine in Brazil. Public Health Nutr. 2021, 24, 422–426. [Google Scholar] [CrossRef] [PubMed]
- Sidor, A.; Rzymski, P. Dietary Choices and Habits during COVID-19 Lockdown: Experience from Poland. Nutrients 2020, 12, 1657. [Google Scholar] [CrossRef] [PubMed]
- Ammar, A.; Brach, M.; Trabelsi, K.; Chtourou, H.; Boukhris, O.; Masmoudi, L.; Bouaziz, B.; Bentlage, E.; How, D.; Ahmed, M.; et al. Effects of COVID-19 Home Confinement on Eating Behaviour and Physical Activity: Results of the ECLB-COVID19 International Online Survey. Nutrients 2020, 12, 1583. [Google Scholar] [CrossRef] [PubMed]
- Barone Gibbs, B.; Kline, C.E.; Huber, K.A.; Paley, J.L.; Perera, S. Covid-19 shelter-at-home and work, lifestyle and well-being in desk workers. Occup. Med. 2021, 71, 86–94. [Google Scholar] [CrossRef] [PubMed]
- Grossman, E.R.; Benjamin-Neelon, S.E.; Sonnenschein, S. Alcohol Consumption during the COVID-19 Pandemic: A Cross-Sectional Survey of US Adults. Int. J. Environ. Res. Public Health 2020, 17, 9189. [Google Scholar] [CrossRef] [PubMed]
- Pollard, M.S.; Tucker, J.S.; Green, H.D., Jr. Changes in Adult Alcohol Use and Consequences During the COVID-19 Pandemic in the US. JAMA Netw. Open 2020, 3, e2022942. [Google Scholar] [CrossRef] [PubMed]
- Montgomery R, D.J.; Ganesh, N. Response rate Calculation Methodology for Recruitment of a Two-Phase Probability-Based Panel: The Case of AmeriSpeak; University of Chicago National Opinion Research Center white Pape. 2016. Available online: https://www.google.com/url?sa=t&rct=j&q=&esrc=s&source=web&cd=&cad=rja&uact=8&ved=2ahUKEwiEwt7B25jzAhXSLH0KHRZKBBQQFnoECAIQAQ&url=https%3A%2F%2Famerispeak.norc.org%2FDocuments%2FResearch%2FNORC_Labs_and_Amerispeak_launch_plans_Nov_2016_DTP_Formatted.pdf&usg=AOvVaw2upuCUtFKREntT7zZI83n9 (accessed on 16 March 2021).
- Karaca-Mandic, P.; Georgiou, A.; Sen, S. Assessment of COVID-19 Hospitalizations by Race/Ethnicity in 12 States. JAMA Intern. Med. 2021, 181, 131–134. [Google Scholar] [CrossRef] [PubMed]
- Laurencin, C.T.; McClinton, A. The COVID-19 Pandemic: A Call to Action to Identify and Address Racial and Ethnic Disparities. Morb. Mortal. Wkly. Rep. 2020, 7, 398–402. [Google Scholar] [CrossRef] [PubMed]
- Moore, J.T.; Ricaldi, J.N.; Rose, C.E.; Fuld, J.; Parise, M.; Kang, G.J.; Driscoll, A.K.; Norris, T.; Wilson, N.; Rainisch, G.; et al. Disparities in Incidence of COVID-19 Among Underrepresented Racial/Ethnic Groups in Counties Identified as Hotspots During June 5-18, 2020–22 States, February-June 2020. Morb. Mortal. Wkly. Rep. 2020, 69, 1122–1126. [Google Scholar]
- Tai, D.B.G.; Shah, A.; Doubeni, C.A.; Sia, I.G.; Wieland, M.L. The Disproportionate Impact of COVID-19 on Racial and Ethnic Minorities in the United States. Clin. Infect. Dis. 2021, 72, 703–706. [Google Scholar] [CrossRef] [PubMed]
- Grundy, E.J.; Suddek, T.; Filippidis, F.T.; Majeed, A.; Coronini-Cronberg, S. Smoking, SARS-CoV-2 and COVID-19: A review of reviews considering implications for public health policy and practice. Tob. Induc. Dis. 2020, 18, 58. [Google Scholar] [CrossRef] [PubMed]
- Vardavas, C.I.; Nikitara, K. COVID-19 and smoking: A systematic review of the evidence. Tob. Induc. Dis. 2020, 18, 20. [Google Scholar] [CrossRef] [PubMed]
- Blog, H.H. Available online: https://www.health.harvard.edu/blog/eating-during-covid-19-improve-your-mood-and-lower-stress-2020040719409 (accessed on 13 September 2021).
- Academy of Nutrition and Dietetics. Eating well during Coronavirus/COVID-19. Available online: https://www.eatright.org/coronavirus (accessed on 13 September 2021).
| Characteristics | % (N) |
|---|---|
| Age groups | |
| 18–29 years | 20.5 (568) |
| 30–44 years | 25.5 (880) |
| 45–59 years | 24.2 (573) |
| ≥60 years | 29.8 (688) |
| Female | 51.7 (1413) |
| Race/ethnicity | |
| Non-Hispanic White | 61.3 (514) |
| Non-Hispanic Black | 11.9 (590) |
| Asian and Pacific Islander | 6.4 (1012) |
| Hispanic | 16.7 (532) |
| American Indian or others | 3.6 (58) |
| Education | |
| High school or less | 38.0 (583) |
| Associates | 27.7 (1073) |
| Bachelor’s or higher | 34.3 (1053) |
| Marital status | |
| Married/living with a partner | 58.2 (1444) |
| Widowed/divorced/separated | 17.0 (404) |
| Never married | 24.8 (861) |
| Annual household income | |
| <$25,000 | 18.8 (562) |
| $25,000–$49,999 | 22.5 (625) |
| ≥$50,000 | 58.6 (1522) |
| Health insurance before the pandemic | |
| Private | 52.7 (1480) |
| Uninsured | 8.3 (222) |
| Medicare | 21.3 (535) |
| Medicaid | 17.7 (452) |
| Variables | Before the Pandemic | During the Pandemic | p Values |
|---|---|---|---|
| Total exercise time (min/day), mean (SE) | 38.65 (2.02) | 32.06 (1.66) | <0.001 |
| Exercise time categories, % (N) | <0.001 | ||
| 0 min/day | 15.3 (379) | 20.9 (508) | |
| 1–30 min/day | 28.3 (722) | 33.7 (888) | |
| ≥30 min/day | 56.4 (1517) | 45.4 (1222) | |
| Total screen time (hours/day), mean (SE) | 5.06 (0.13) | 6.79 (0.14) | <0.001 |
| Screen time categories, % (N) | <0.001 | ||
| 0 h/day | 2.1 (52) | 1.6 (47) | |
| <0 and <4 h/day | 38.4 (988) | 18.7 (474) | |
| ≥4 h/day | 59.5 (1576) | 79.8 (2095) | |
| Fast-food meals intake (time/week), median (IQR) | 1.41 (2.55) | 0.96 (2.74) | <0.001 |
| Fast-food meals intake categories, % (N) | <0.001 | ||
| 0 time/week | 15.0 (400) | 25.0 (663) | |
| 1–2 time/week | 47.3 (1142) | 41.7 (1036) | |
| ≥3 times/week | 37.7 (1061) | 33.3 (904) | |
| Alcohol drinking (drinks/week) among drinkers, median (IQR) | 3.01 (5.13) | 4.24 (6.92) | <0.001 |
| Alcohol drinking categories, % (N) | <0.001 | ||
| 0 drink/week | 50.6 (1409) | 49.8 (1416) | |
| 1–4 drinks/week | 28.5 (806) | 24.6 (687) | |
| ≥5 drinks/week | 20.9 (395) | 25.7 (507) | |
| Cigarette smoking (times/day) among smokers, median (IQR) | 9.29 (10.32) | 9.80 (12.93) | <0.001 |
| Cigarette smoking categories, % (N) | <0.001 | ||
| Non-smokers | 82.9 (2190) | 82.4 (2185) | |
| 1–5 cigarettes/day | 5.8 (181) | 3.9 (135) | |
| 6–10 cigarettes/day | 5.4 (143) | 5.8 (149) | |
| ≥11 cigarettes/day | 5.8 (99) | 7.9 (144) |
| Characteristics | Exercise Time | Screen Time | Fast-Food Meals Intake | Alcohol Drinking | Cigarette Smoking | |||||
|---|---|---|---|---|---|---|---|---|---|---|
| OR (95% CI) | p | OR (95% CI) | p | OR (95% CI) | p | OR (95% CI) | p | OR (95% CI) | p | |
| Age, years | ||||||||||
| 18–29 | 1.07 (0.65, 1.75) | 0.79 | 1.25 (0.75, 2.10) | 0.39 | 2.24 (1.24, 4.05) | 0.01 | 2.24 (1.23, 4.09) | 0.01 | 2.83 (0.95, 8.40) | 0.06 |
| 30–44 | 1.77 (1.13, 2.77) | 0.01 | 1.21 (0.78, 1.85) | 0.40 | 1.95 (1.16, 3.27) | 0.01 | 2.34 (1.42, 3.86) | 0.001 | 4.74 (1.80, 12.48) | 0.002 |
| 45–59 | 1.17 (0.72, 1.90) | 0.52 | 0.82 (0.52, 1.28) | 0.38 | 1.21 (0.71, 2.04) | 0.49 | 1.33 (0.75, 2.36) | 0.34 | 3.37 (1.28, 8.85) | 0.01 |
| ≥60 | Reference | Reference | Reference | Reference | Reference | |||||
| Sex | ||||||||||
| Male | Reference | Reference | Reference | Reference | Reference | |||||
| Female | 1.21 (0.91, 1.60) | 0.20 | 1.72 (1.29, 2.30) | <0.001 | 0.95 (0.70, 1.29) | 0.75 | 1.00 (0.72, 1.40) | 1.00 | 1.31 (0.80, 2.15) | 0.28 |
| Race/ethnicity | ||||||||||
| Non-Hispanic White | Reference | Reference | Reference | Reference | Reference | |||||
| Non-Hispanic Black | 1.64 (1.17, 2.28) | 0.004 | 1.30 (0.95, 1.79) | 0.11 | 1.49 (1.03, 2.17) | 0.03 | 1.45 (1.02, 2.06) | 0.04 | 0.98 (0.55, 1.75) | 0.95 |
| Hispanic | 2.30 (1.64, 3.24) | <0.001 | 1.92 (1.35, 2.72) | <0.001 | 1.75 (1.21, 2.52) | 0.003 | 1.59 (1.09, 2.33) | 0.02 | 0.73 (0.40, 1.34) | 0.31 |
| Asian/Pacific Islander | 1.35 (1.00, 1.83) | 0.05 | 1.03 (0.77, 1.37) | 0.86 | 1.05 (0.74, 1.48) | 0.79 | 0.51 (0.35, 0.74) | 0.001 | 0.53 (0.29, 0.97) | 0.04 |
| American Indian or other | 3.56 (1.80, 7.07) | <0.001 | 1.22 (0.58, 2.54) | 0.60 | 3.65 (1.79, 7.43) | <0.001 | 2.04 (0.96, 4.33) | 0.06 | 1.79 (0.62, 5.14) | 0.28 |
| Education | ||||||||||
| High school or less | Reference | Reference | Reference | Reference | Reference | |||||
| Associate degree | 1.46 (1.03, 2.08) | 0.03 | 1.21 (0.85, 1.73) | 0.30 | 1.11 (0.78, 1.56) | 0.57 | 1.16 (0.76, 1.76) | 0.49 | 0.96 (0.55, 1.67) | 0.88 |
| Bachelor degree or higher | 1.79 (1.20, 2.67) | 0.004 | 1.90 (1.27, 2.85) | 0.002 | 1.05 (0.69, 1.60) | 0.83 | 1.78 (1.11, 2.87) | 0.02 | 0.52 (0.22, 1.24) | 0.14 |
| Marital Status, % (N) | ||||||||||
| Married/Living with partner | Reference | Reference | Reference | Reference | Reference | |||||
| Widowed/Divorced/Separated | 1.26 (0.80, 1.97) | 0.32 | 0.82 (0.54, 1.26) | 0.37 | 1.01 (0.65, 1.57) | 0.96 | 1.08 (0.65, 1.81) | 0.77 | 1.34 (0.62, 2.89) | 0.45 |
| Never married | 1.43 (1.02, 2.01) | 0.04 * | 1.02 (0.69, 1.49) | 0.93 | 0.76 (0.50, 1.16) | 0.20 | 1.02 (0.69, 1.51) | 0.94 | 1.00 (0.51, 1.96) | 1.00 |
| Annual household income | ||||||||||
| <$25,000 | Reference | Reference | Reference | Reference | Reference | |||||
| $25,000–$49,999 | 1.05 (0.70, 1.58) | 0.82 | 1.04 (0.67, 1.60) | 0.87 | 0.64 (0.41, 1.02) | 0.06 | 1.00 (0.62, 1.61) | 1.00 | 0.37 (0.21, 0.67) | 0.001 |
| ≥$50,000 | 1.08 (0.70, 1.66) | 0.74 | 1.36 (0.91, 2.06) | 0.14 | 0.64 (0.41, 1.01) | 0.05 | 1.08 (0.68, 1.71) | 0.74 | 0.22 (0.11, 0.43) | <0.001 |
| Health Insurance | ||||||||||
| Private | Reference | Reference | Reference | Reference | Reference | |||||
| Uninsured | 0.89 (0.53, 1.52) | 0.68 | 1.37 (0.77, 2.44) | 0.29 | 0.97 (0.55, 1.73) | 0.92 | 0.74 (0.31, 1.76) | 0.50 | 1.14 (0.47, 2.80) | 0.77 |
| Medicare | 1.63 (1.06, 2.52) | 0.03 | 1.06 (0.69, 1.62) | 0.80 | 1.04 (0.63, 1.72) | 0.88 | 0.61 (0.36, 1.03) | 0.07 | 0.91 (0.34, 2.43) | 0.85 |
| Medicaid | 1.51 (0.95, 2.39) | 0.08 | 1.22 (0.78, 1.91) | 0.39 | 1.38 (0.89, 2.15) | 0.15 | 1.09 (0.68, 1.73) | 0.73 | 2.30 (1.03, 5.17) | 0.04 |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Chen, L.; Li, J.; Xia, T.; Matthews, T.A.; Tseng, T.-S.; Shi, L.; Zhang, D.; Chen, Z.; Han, X.; Li, Y.; et al. Changes of Exercise, Screen Time, Fast Food Consumption, Alcohol, and Cigarette Smoking during the COVID-19 Pandemic among Adults in the United States. Nutrients 2021, 13, 3359. https://doi.org/10.3390/nu13103359
Chen L, Li J, Xia T, Matthews TA, Tseng T-S, Shi L, Zhang D, Chen Z, Han X, Li Y, et al. Changes of Exercise, Screen Time, Fast Food Consumption, Alcohol, and Cigarette Smoking during the COVID-19 Pandemic among Adults in the United States. Nutrients. 2021; 13(10):3359. https://doi.org/10.3390/nu13103359
Chicago/Turabian StyleChen, Liwei, Jian Li, Tong Xia, Timothy A. Matthews, Tung-Sung Tseng, Lu Shi, Donglan Zhang, Zhuo Chen, Xuesong Han, Yan Li, and et al. 2021. "Changes of Exercise, Screen Time, Fast Food Consumption, Alcohol, and Cigarette Smoking during the COVID-19 Pandemic among Adults in the United States" Nutrients 13, no. 10: 3359. https://doi.org/10.3390/nu13103359
APA StyleChen, L., Li, J., Xia, T., Matthews, T. A., Tseng, T.-S., Shi, L., Zhang, D., Chen, Z., Han, X., Li, Y., Li, H., Wen, M., & Su, D. (2021). Changes of Exercise, Screen Time, Fast Food Consumption, Alcohol, and Cigarette Smoking during the COVID-19 Pandemic among Adults in the United States. Nutrients, 13(10), 3359. https://doi.org/10.3390/nu13103359









