Associations of Skipping Breakfast, Lunch, and Dinner with Weight Gain and Overweight/Obesity in University Students: A Retrospective Cohort Study
Abstract
1. Introduction
2. Materials and Methods
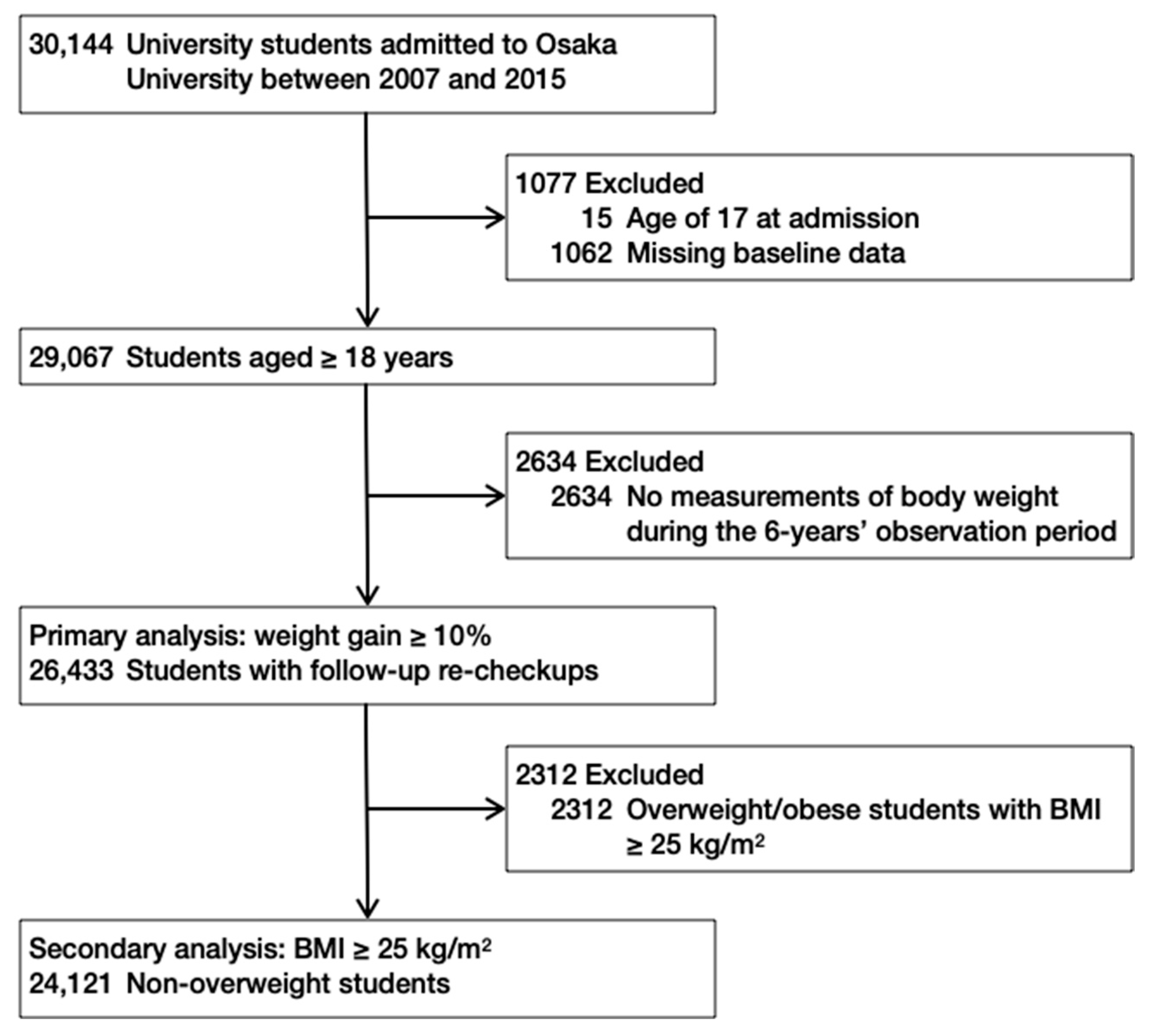
2.1. Participants
2.2. Measurements
2.3. Statistical Analysis
3. Results
4. Discussion
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Jayedi, A.; Rashidy-Pour, A.; Khorshidi, M.; Shab-Bidar, S. Body mass index, abdominal adiposity, weight gain and risk of developing hypertension: A systematic review and dose–response meta-analysis of more than 2.3 million participants. Obes. Rev. 2018, 19, 654–667. [Google Scholar] [CrossRef] [PubMed]
- Vazquez, G.; Duval, S.; Jacobs, D.R.; Silventoinen, K. Comparison of body mass index, waist circumference, and waist/hip ratio in predicting incident diabetes: A meta-analysis. Epidemiol. Rev. 2007, 29, 115–128. [Google Scholar] [CrossRef] [PubMed]
- Chen, Y.; Copeland, W.K.; Vedanthan, R.; Grant, E.; Lee, J.E.; Gu, D.; Gupta, P.C.; Ramadas, K.; Inoue, M.; Tsugane, S.; et al. Association between body mass index and cardiovascular disease mortality in east Asians and south Asians: Pooled analysis of prospective data from the Asia Cohort Consortium. BMJ 2013, 347, 1–19. [Google Scholar] [CrossRef] [PubMed]
- Di Angelantonio, E.; Bhupathiraju, S.N.; Wormser, D.; Gao, P.; Kaptoge, S.; de Gonzalez, A.B.; Cairns, B.J.; Huxley, R.; Jackson, C.L.; Joshy, G.; et al. Body-mass index and all-cause mortality: Individual-participant-data meta-analysis of 239 prospective studies in four continents. Lancet 2016, 388, 776–786. [Google Scholar] [CrossRef]
- The, N.S.; Suchindran, C.; North, K.E.; Popkin, B.M.; Gordon-Larsen, P. Association of adolescent obesity with risk of severe obesity in adulthood. JAMA 2010, 304, 2042–2047. [Google Scholar] [CrossRef]
- Wang, Z.; Peng, Y.; Liu, M. Age Variation in the Association Between Obesity and Mortality in Adults. Obesity 2017, 25, 2137–2141. [Google Scholar] [CrossRef]
- Brown, C. The information trail of the “Freshman 15”—A systematic review of a health myth within the research and popular literature. Health Inf. Libr. J. 2008, 25, 1–12. [Google Scholar] [CrossRef]
- Crombie, A.P.; Ilich, J.Z.; Dutton, G.R.; Panton, L.B.; Abood, D.A. The freshman weight gain phenomenon revisited. Nutr. Rev. 2009, 67, 83–94. [Google Scholar] [CrossRef]
- St-Onge, M.P.; Ard, J.; Baskin, M.L.; Chiuve, S.E.; Johnson, H.M.; Kris-Etherton, P.; Varady, K. Meal Timing and Frequency: Implications for Cardiovascular Disease Prevention: A Scientific Statement from the American Heart Association. Circulation 2017, 135, e96–e121. [Google Scholar] [CrossRef]
- Schoenfeld, B.J.; Aragon, A.A.; Krieger, J.W. Effects of meal frequency on weight loss and body composition: A meta-analysis. Nutr. Rev. 2015, 73, 69–82. [Google Scholar] [CrossRef]
- Odegaard, A.O.; Jacobs, D.R.; Steffen, L.M.; Van Horn, L.; Ludwig, D.S.; Pereira, M.A. Breakfast frequency and development of metabolic risk. Diabetes Care 2013, 36, 3100–3106. [Google Scholar] [CrossRef] [PubMed]
- Ma, X.; Chen, Q.; Pu, Y.; Guo, M.; Jiang, Z.; Huang, W.; Long, Y.; Xu, Y. Skipping breakfast is associated with overweight and obesity: A systematic review and meta-analysis. Obes. Res. Clin. Pract. 2020, 14, 1–8. [Google Scholar] [CrossRef]
- Marín-Guerrero, A.C.; Gutiérrez-Fisac, J.L.; Guallar-Castillón, P.; Banegas, J.R.; Rodríguez-Artalejo, F. Eating behaviours and obesity in the adult population of Spain. Br. J. Nutr. 2008, 100, 1142–1148. [Google Scholar] [CrossRef] [PubMed]
- Azadbakht, L.; Akbari, F.; Qorbani, M.; Esmaeil Motlagh, M.; Ardalan, G.; Heshmat, R.; Daneshzad, E.; Kelishadi, R. Dinner consumption and cardiovascular disease risk factors among a nationally representative sample of Iranian adolescents: The CASPIAN-III Study. J. Cardiovasc. Thorac. Res. 2019, 11, 138–146. [Google Scholar] [CrossRef] [PubMed]
- McCrory, M.A. Meal skipping and variables related to energy balance in adults: A brief review, with emphasis on the breakfast meal. Physiol. Behav. 2014, 134, 51–54. [Google Scholar] [CrossRef]
- Ford, C.; Chang, S.; Vitolins, M.Z.; Fenton, J.I.; Howard, B.V.; Rhee, J.J.; Stefanick, M.; Chen, B.; Snetselaar, L.; Urrutia, R.; et al. Evaluation of diet pattern and weight gain in postmenopausal women enrolled in the Women’s Health Initiative Observational Study. Br. J. Nutr 2017, 117, 1189–1197. [Google Scholar] [CrossRef] [PubMed]
- Hirko, K.A.; Kantor, E.D.; Cohen, S.S.; Blot, W.J.; Stampfer, M.J.; Signorello, L.B. Body mass index in young adulthood, obesity trajectory, and premature mortality. Am. J. Epidemiol. 2015, 182, 441–450. [Google Scholar] [CrossRef]
- Wu, Y.; Zhai, L.; Zhang, D. Sleep duration and obesity among adults: A meta-analysis of prospective studies. Sleep Med. 2014, 15, 1456–1462. [Google Scholar] [CrossRef]
- Okada, C.; Imano, H.; Muraki, I.; Yamada, K.; Iso, H. The Association of Having a Late Dinner or Bedtime Snack and Skipping Breakfast with Overweight in Japanese Women. J. Obes. 2019, 2019, 1–5. [Google Scholar] [CrossRef]
- Klein, D. Implementing a General Framework for Assessing Interrater Agreement in Stata. Stata J. 2018, 18, 871–901. [Google Scholar] [CrossRef]
- Koren, J.P.; Herta, J.; Fürbass, F.; Pirker, S.; Reiner-Deitemyer, V.; Riederer, F.; Flechsenhar, J.; Hartmann, M.; Kluge, T.; Baumgartner, C. Automated long-term EEG review: Fast and precise analysis in critical care patients. Front. Neurol. 2018, 9, 454. [Google Scholar] [CrossRef] [PubMed]
- Pot, G.K.; Hardy, R.; Stephen, A.M. Irregularity of energy intake at meals: Prospective associations with the metabolic syndrome in adults of the 1946 British birth cohort. Br. J. Nutr. 2016, 115, 315–323. [Google Scholar] [CrossRef] [PubMed]
- Batista-Jorge, G.C.; Barcala-Jorge, A.S.; Oliveira Dias, A.F.; Silveira, M.F.; De Farias Lelis, D.; Oliveira Andrade, J.M.; Claro, R.M.; De Paula, A.M.B.; Guimaraes, A.L.S.; Ferreira, A.V.; et al. Nutritional Status Associated to Skipping Breakfast in Brazilian Health Service Patients. Ann. Nutr. Metab. 2016, 69, 31–40. [Google Scholar] [CrossRef] [PubMed]
- Zeballos, E.; Todd, J.E. The effects of skipping a meal on daily energy intake and diet quality. Public Health Nutr. 2020. [Google Scholar] [CrossRef] [PubMed]
- Kuroda, T.; Onoe, Y.; Yoshikata, R.; Ohta, H. Relationship between skipping breakfast and bone mineral density in young Japanese women. Asia Pac. J. Clin. Nutr. 2013, 22, 583–589. [Google Scholar] [CrossRef]
- Reedy, J.; Krebs-Smith, S.M.; Miller, P.E.; Liese, A.D.; Kahle, L.L.; Park, Y.; Subar, A.F. Higher diet quality is associated with decreased risk of all-cause, cardiovascular disease, and cancer mortality among older adults. J. Nutr. 2014, 144, 881–889. [Google Scholar] [CrossRef]
- Gao, S.K.; Beresford, S.A.A.; Frank, L.L.; Schreiner, P.J.; Burke, G.L.; Fitzpatrick, A.L. Modifications to the healthy eating index and its ability to predict obesity: The multi-ethnic study of atherosclerosis. Am. J. Clin. Nutr. 2008, 88, 64–69. [Google Scholar] [CrossRef]
- Schlesinger, S.; Neuenschwander, M.; Schwedhelm, C.; Hoffmann, G.; Bechthold, A.; Boeing, H.; Schwingshackl, L. Food Groups and Risk of Overweight, Obesity, and Weight Gain: A Systematic Review and Dose-Response Meta-Analysis of Prospective Studies. Adv. Nutr. 2019, 10, 205–218. [Google Scholar] [CrossRef]
- Sato-Mito, N.; Sasaki, S.; Murakami, K.; Okubo, H.; Takahashi, Y.; Shibata, S.; Yamada, K.; Sato, K. The midpoint of sleep is associated with dietary intake and dietary behavior among young Japanese women. Sleep Med. 2011, 12, 289–294. [Google Scholar] [CrossRef]
- Maukonen, M.; Kanerva, N.; Partonen, T.; Männistö, S. Chronotype and energy intake timing in relation to changes in anthropometrics: A 7-year follow-up study in adults. Chronobiol. Int. 2019, 36, 27–41. [Google Scholar] [CrossRef]
- Pelletier, J.E.; Lytle, L.A.; Laska, M.N. Stress, Health Risk Behaviors, and Weight Status Among Community College Students. Health Educ. Behav. 2015, 43, 139–144. [Google Scholar] [CrossRef] [PubMed]
- Fowler-Brown, A.G.; Bennett, G.G.; Goodman, M.S.; Wee, C.C.; Corbie-Smith, G.M.; James, S.A. Psychosocial stress and 13-year BMI change among blacks: The pitt county study. Obesity 2009, 17, 2106–2109. [Google Scholar] [CrossRef] [PubMed]
- Mouchacca, J.; Abbott, G.R.; Ball, K. Associations between psychological stress, eating, physical activity, sedentary behaviours and body weight among women: A longitudinal study. BMC Public Health 2013, 13. [Google Scholar] [CrossRef] [PubMed]
- Lim, H.-S.; Yoo, J.-J. Association between Health Indicators and Health-Related Quality of Life according to Physical Activity of Older Women. Healthcare 2020, 8, 507. [Google Scholar] [CrossRef] [PubMed]
- Littman, A.J.; Kristal, A.R.; White, E. Effects of physical activity intensity, frequency, and activity type on 10-y weight change in middle-aged men and women. Int J. Obes. 2005, 29, 524–533. [Google Scholar] [CrossRef] [PubMed]
- Wagner, A.; Simon, C.; Ducimetière, P.; Montaye, M.; Bongard, V.; Yarnell, J.; Bingham, A.; Hedelin, G.; Amouyel, P.; Ferrières, J.; et al. Leisure-time physical activity and regular walking or cycling to work are associated with adiposity and 5 y weight gain in middle-aged men: The PRIME Study. Int J. Obes. 2001, 25, 940–948. [Google Scholar] [CrossRef] [PubMed]
- Smith, K.J.; Gall, S.L.; McNaughton, S.A.; Cleland, V.J.; Otahal, P.; Dwyer, T.; Venn, A.J. Lifestyle behaviours associated with 5-year weight gain in a prospective cohort of Australian adults aged 26–36 years at baseline. BMC Public Health 2017, 17, 54. [Google Scholar] [CrossRef]
- Kahleova, H.; Lloren, J.I.; Mashchak, A.; Hill, M.; Fraser, G.E. Meal Frequency and Timing Are Associated with Changes in Body Mass Index in Adventist Health Study 2. J. Nutr. 2017, 147, 1722–1728. [Google Scholar] [CrossRef]
- van der Heijden, A.A.W.A.; Hu, F.B.; Rimm, E.B.; van Dam, R.M. A Prospective Study of Breakfast Consumption and Weight Gain among U.S. Men. Obesity 2007, 15, 2463–2469. [Google Scholar] [CrossRef]
- Forkert, E.C.O.; De Moraes, A.C.F.; Carvalho, H.B.; Manios, Y.; Widhalm, K.; González-Gross, M.; Gutierrez, A.; Kafatos, A.; Censi, L.; De Henauw, S.; et al. Skipping breakfast is associated with adiposity markers especially when sleep time is adequate in adolescents. Sci. Rep. 2019, 9, 1–10. [Google Scholar] [CrossRef]
| Dinner frequency | All | Eating Every Day | Skipping ≥Occasionally | p |
|---|---|---|---|---|
| Number | 17,573 | 17,307 | 266 | |
| Baseline characteristics at admission | ||||
| Age, 18 years, n (%) | 11,342 (64.5) | 11,228 (64.9) | 114 (42.9) | <0.001 |
| 19 | 5625 (32.0) | 5508 (31.8) | 117 (44.0) | |
| 20 | 387 (2.2) | 367 (2.1) | 20 (7.5) | |
| 21–60 | 219 (1.2) | 204 (1.2) | 15 (5.6) | |
| Height (cm) | 171.3 ± 5.7 | 171.3 ± 5.7 | 171.2 ± 5.6 | 0.763 |
| Body weight, kg | 63.4 ± 9.4 | 63.3 ± 9.3 | 67.1 ± 12.8 | <0.001 |
| BMI, kg/m2 | 21.6 ± 2.9 | 21.6 ± 2.9 | 22.9 ± 4.1 | <0.001 |
| <25.0 kg/m2, n (%) | 15,656 (89.1) | 15,450 (89.3) | 206 (77.4) | <0.001 |
| ≥25.0 | 1917 (10.9) | 1857 (10.7) | 60 (22.6) | |
| Smokers, n (%) | 97 (0.6) | 84 (0.5) | 13 (4.9) | <0.001 |
| Drinkers, n (%) | 1658 (9.4) | 1596 (9.2) | 62 (23.3) | <0.001 |
| Sleep duration, <5 h, n (%) | 547 (3.1) | 532 (3.1) | 15 (5.6) | <0.001 |
| 5–6 | 5604 (31.9) | 5494 (31.7) | 110 (41.4) | |
| 6–7 | 8473 (48.2) | 8375 (48.4) | 98 (36.8) | |
| 7–8 | 2521 (14.3) | 2485 (14.4) | 36 (13.5) | |
| ≥8 | 428 (2.4) | 421 (2.4) | 7 (2.6) | |
| Breakfast, eating every day, n (%) | 14,233 (81.0) | 14,115 (81.6) | 118 (44.4) | <0.001 |
| Skipping occasionally | 2275 (12.9) | 2170 (12.5) | 105 (39.5) | |
| Skipping ≥ often | 1065 (6.1) | 1022 (5.9) | 43 (16.2) | <0.001 |
| Lunch, eating every day, n (%) | 16,448 (93.6) | 16,327 (94.3) | 121 (45.5) | <0.001 |
| Skipping ≥ occasionally | 1125 (6.4) | 980 (5.7) | 145 (54.5) | |
| Dinner time, before 7 PM, n (%) | 3255 (18.5) | 3201 (18.5) | 54 (20.3) | <0.001 |
| 7–9 PM | 11,453 (65.2) | 11,310 (65.3) | 143 (53.8) | |
| 9–11 PM | 2681 (15.3) | 2624 (15.2) | 57 (21.4) | |
| After 11 PM | 184 (1.0) | 172 (1.0) | 12 (4.5) | |
| Observation period and outcome incidences | ||||
| Observation period (years) | 3.0 ± 0.9 | 3.0 ± 0.9 | 3.0 ± 1.0 | 0.704 |
| Weight gain ≥10%, n (%) | 1896 (10.8) | 1857 (10.7) | 39 (14.7) | 0.040 |
| IR per 1000 PY (95% CI) | 36.1 (34.5, 37.8) | 35.9 (34.3, 37.6) | 49.4 (36.1, 67.6) | |
| BMI ≥ 25 kg/m2, n (%) | 671 (4.3) | 653 (4.2) | 18 (8.7) | 0.001 |
| IR per 1000 PY (95% CI) | 14.1 (13.1, 15.2) | 13.9 (12.9, 15.0) | 29.0 (18.3, 46.0) | |
| Dinner frequency | All | Eating Every Day | Skipping ≥Occasionally | p |
|---|---|---|---|---|
| Number | 8860 | 8502 | 358 | |
| Baseline characteristics at admission | ||||
| Age, 18 years, n (%) | 6537 (73.8) | 6336 (74.5) | 201 (56.1) | <0.001 |
| 19 | 2052 (23.2) | 1926 (22.7) | 126 (35.2) | |
| 20 | 160 (1.8) | 145 (1.7) | 15 (4.2) | |
| 21–60 | 111 (1.3) | 95 (1.1) | 16 (4.5) | |
| Height, cm | 158.4 ± 5.2 | 158.4 ± 5.2 | 158.7 ± 5.1 | 0.250 |
| Body weight, kg | 51.5 ± 6.8 | 51.4 ± 6.8 | 53.1 ± 7.0 | <0.001 |
| BMI, kg/m2 | 20.5 ± 2.4 | 20.5 ± 2.4 | 21.1 ± 2.4 | <0.001 |
| <25.0 kg/m2, n (%) | 8465 (95.5) | 8134 (95.7) | 331 (92.5) | 0.004 |
| ≥25.0 | 395 (4.5) | 368 (4.3) | 27 (7.5) | |
| Smokers, n (%) | 13 (0.1) | 11 (0.1) | 2 (0.6) | 0.038 |
| Drinkers, n (%) | 418 (4.7) | 367 (4.3) | 51 (14.2) | <0.001 |
| Sleep duration, <5 h, n (%) | 264 (3.0) | 246 (2.9) | 18 (5.0) | 0.003 |
| 5–6 | 3159 (35.7) | 3018 (35.5) | 141 (39.4) | |
| 6–7 | 4209 (47.5) | 4070 (47.9) | 139 (38.8) | |
| 7–8 | 1109 (12.5) | 1057 (12.4) | 52 (14.5) | |
| ≥8 | 119 (1.3) | 111 (1.3) | 8 (2.2) | |
| Breakfast, eating every day, n (%) | 7793 (88.0) | 7538 (88.7) | 255 (71.2) | <0.001 |
| Skipping occasionally | 782 (8.8) | 707 (8.3) | 75 (20.9) | |
| Skipping ≥ often | 285 (3.2) | 257 (3.0) | 28 (7.8) | |
| Lunch, eating every day, n (%) | 8451 (95.4) | 8178 (96.2) | 273 (76.3) | <0.001 |
| Skipping ≥ occasionally | 409 (4.6) | 324 (3.8) | 85 (23.7) | |
| Dinner time, before 7 PM, n (%) | 2288 (25.8) | 2185 (25.7) | 103 (28.8) | 0.111 |
| 7–9 PM | 5611 (63.3) | 5405 (63.6) | 206 (57.5) | |
| 9–11 PM | 920 (10.4) | 873 (10.3) | 47 (13.1) | |
| After 11 PM | 41 (0.5) | 39 (0.5) | 2 (0.6) | |
| Observation period and incidence of outcomes | ||||
| Observation period (years) | 2.9 ± 1.0 | 2.9 ± 1.0 | 2.8 ± 1.1 | 0.708 |
| Weight gain ≥10%, n (%) | 1518 (17.1) | 1436 (16.9) | 82 (22.9) | 0.041 |
| IR per 1000 PY (95% CI) | 58.1 (55.3, 61.1) | 57.2 (54.3, 60.2) | 80.3 (64.7, 99.7) | |
| BMI ≥ 25 kg/m2, n (%) | 266 (3.1) | 248 (3.0) | 18 (5.4) | 0.015 |
| IR per 1000 PY (95% CI) | 10.0 (8.9, 11.3) | 9.7 (8.6, 11.0) | 17.8 (11.2, 28.2) | |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Yamamoto, R.; Tomi, R.; Shinzawa, M.; Yoshimura, R.; Ozaki, S.; Nakanishi, K.; Ide, S.; Nagatomo, I.; Nishida, M.; Yamauchi-Takihara, K.; et al. Associations of Skipping Breakfast, Lunch, and Dinner with Weight Gain and Overweight/Obesity in University Students: A Retrospective Cohort Study. Nutrients 2021, 13, 271. https://doi.org/10.3390/nu13010271
Yamamoto R, Tomi R, Shinzawa M, Yoshimura R, Ozaki S, Nakanishi K, Ide S, Nagatomo I, Nishida M, Yamauchi-Takihara K, et al. Associations of Skipping Breakfast, Lunch, and Dinner with Weight Gain and Overweight/Obesity in University Students: A Retrospective Cohort Study. Nutrients. 2021; 13(1):271. https://doi.org/10.3390/nu13010271
Chicago/Turabian StyleYamamoto, Ryohei, Ryohei Tomi, Maki Shinzawa, Ryuichi Yoshimura, Shingo Ozaki, Kaori Nakanishi, Seiko Ide, Izumi Nagatomo, Makoto Nishida, Keiko Yamauchi-Takihara, and et al. 2021. "Associations of Skipping Breakfast, Lunch, and Dinner with Weight Gain and Overweight/Obesity in University Students: A Retrospective Cohort Study" Nutrients 13, no. 1: 271. https://doi.org/10.3390/nu13010271
APA StyleYamamoto, R., Tomi, R., Shinzawa, M., Yoshimura, R., Ozaki, S., Nakanishi, K., Ide, S., Nagatomo, I., Nishida, M., Yamauchi-Takihara, K., Kudo, T., & Moriyama, T. (2021). Associations of Skipping Breakfast, Lunch, and Dinner with Weight Gain and Overweight/Obesity in University Students: A Retrospective Cohort Study. Nutrients, 13(1), 271. https://doi.org/10.3390/nu13010271





