Coffee Intake and Neurocognitive Performance in HIV/HCV Coinfected Patients (ANRS CO13 HEPAVIH)
Abstract
1. Introduction
2. Materials and Methods
3. Results
3.1. Study Population
3.2. Outcomes
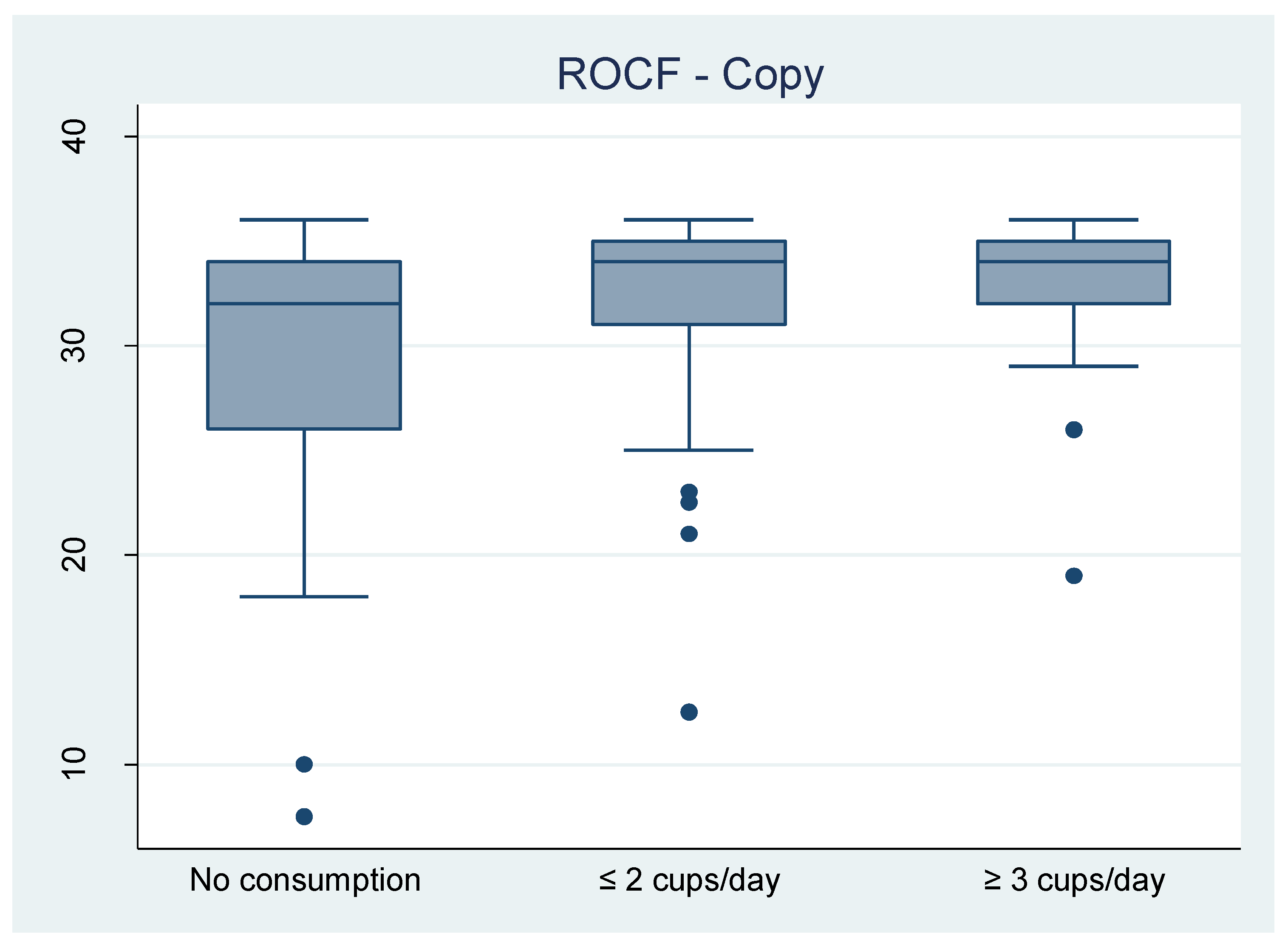
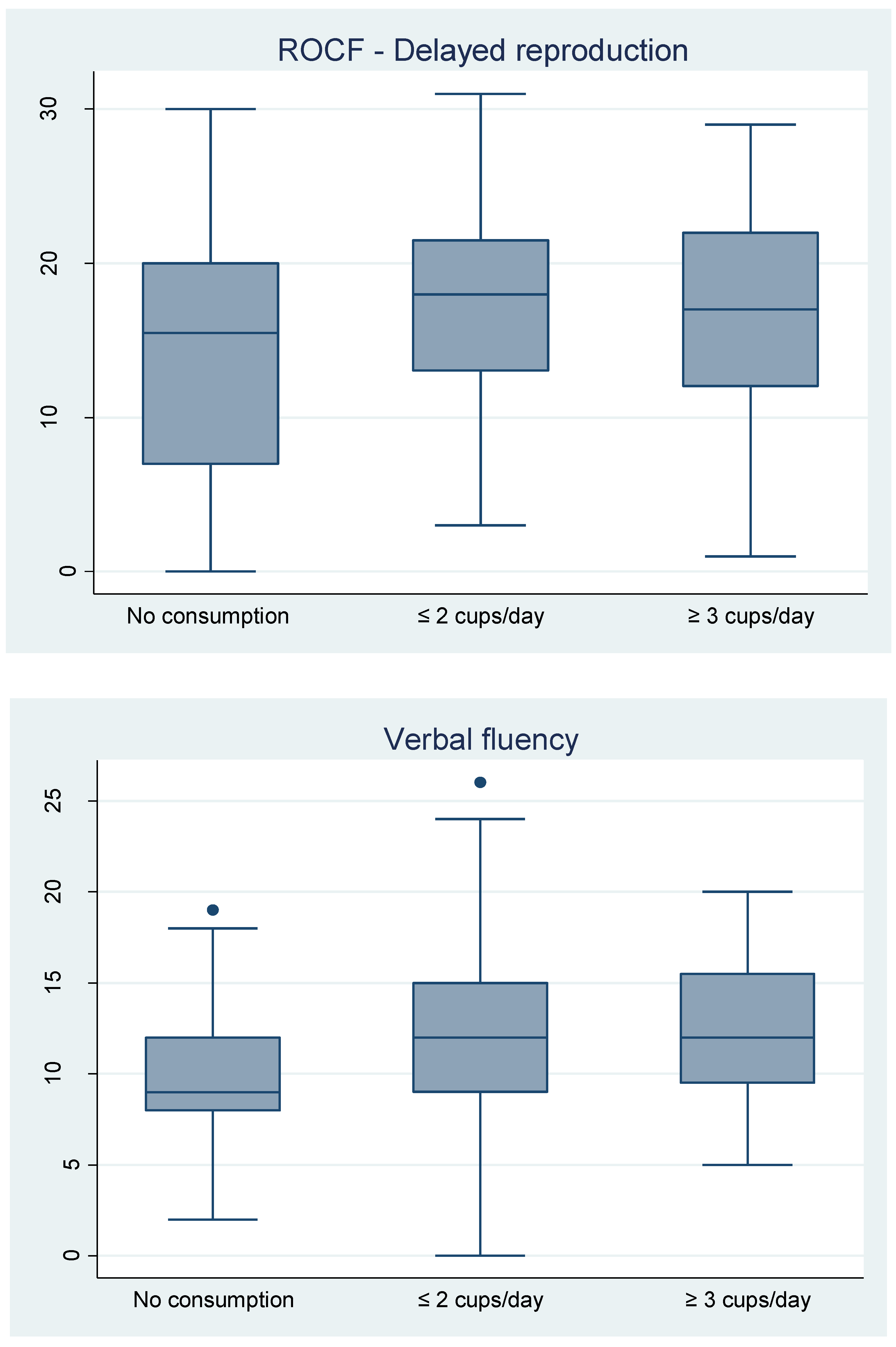
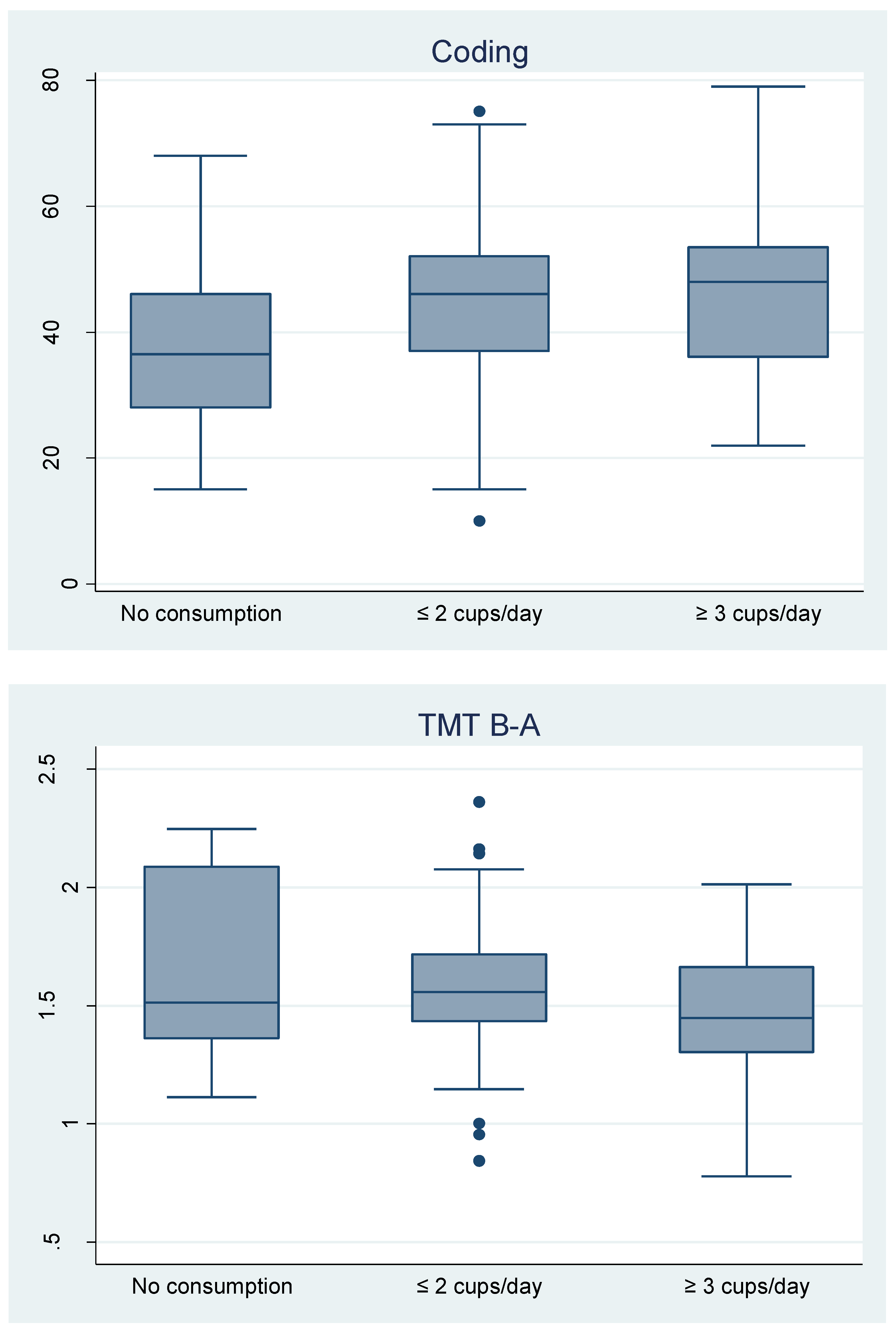
3.3. Coffee Consumption Associated with Neurocognitive Performance in HIV-HCV Coinfected People
4. Discussion
5. Conclusions
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
Appendix A
References
- Heckman, M.A.; Weil, J.; Mejia, E.G.D. Caffeine (1, 3, 7-trimethylxanthine) in Foods: A Comprehensive Review on Consumption, Functionality, Safety, and Regulatory Matters. J. Food Sci. 2010, 75, 77–87. [Google Scholar] [CrossRef] [PubMed]
- Gunter, M.J.; Murphy, N.; Cross, A.J.; Dossus, L.; Dartois, L.; Fagherazzi, G.; Kaaks, R.; Kühn, T.; Boeing, H.; Aleksandrova, K.; et al. Coffee Drinking and Mortality in 10 European Countries: A Multinational Cohort Study. Ann. Intern. Med. 2017, 167, 236–247. [Google Scholar] [CrossRef]
- Alicandro, G.; Tavani, A.; La Vecchia, C. Coffee and cancer risk: A summary overview. Eur. J. Cancer Prev. 2017, 26, 424–432. [Google Scholar] [CrossRef] [PubMed]
- Hodge, A.; Lim, S.; Goh, E.; Wong, O.; Marsh, P.; Knight, V.; Sievert, W.; De Courten, B. Coffee Intake Is Associated with a Lower Liver Stiffness in Patients with Non-Alcoholic Fatty Liver Disease, Hepatitis C., and Hepatitis B. Nutrients 2017, 9, 56. [Google Scholar] [CrossRef]
- Morisco, F.; Lembo, V.; Mazzone, G.; Camera, S.; Caporaso, N. Coffee and Liver Health. J. Clin. Gastroenterol. 2014, 48, 87–90. [Google Scholar] [CrossRef] [PubMed]
- Tanida, I.; Shirasago, Y.; Suzuki, R.; Abe, R.; Wakita, T.; Hanada, K.; Fukasawa, M. Inhibitory Effects of Caffeic Acid, a Coffee-Related Organic Acid, on the Propagation of Hepatitis C Virus. Jpn. J. Infect. Dis. 2015, 68, 268–275. [Google Scholar] [CrossRef] [PubMed]
- Freedman, N.D.; Curto, T.M.; Lindsay, K.L.; Wright, E.C.; Sinha, R.; Everhart, J.E. Coffee Consumption Is Associated With Response to Peginterferon and Ribavirin Therapy in Patients With Chronic Hepatitis C. Gastroenterology 2011, 140, 1961–1969. [Google Scholar] [CrossRef] [PubMed]
- Carrieri, M.P.; Protopopescu, C.; Marcellin, F.; Rosellini, S.; Wittkop, L.; Esterle, L.; Zucman, D.; Raffi, F.; Rosenthal, E.; Poizot-Martin, I.; et al. Protective effect of coffee consumption on all-cause mortality of French HIV-HCV co-infected patients. J. Hepatol. 2017, 67, 1157–1167. [Google Scholar] [CrossRef]
- Yaya, I.; Marcellin, F.; Costa, M.; Morlat, P.; Protopopescu, C.; Pialoux, G.; Santos, M.E.; Wittkop, L.; Esterle, L.; Gervais, A. Impact of Alcohol and Coffee Intake on the Risk of Advanced Liver Fibrosis: A Longitudinal Analysis in HIV-HCV Coinfected Patients (ANRS CO-13 HEPAVIH Cohort). Nutrients 2018, 10, 705. [Google Scholar] [CrossRef]
- Carrieri, M.P.; Lions, C.; Sogni, P.; Winnock, M.; Roux, P.; Mora, M.; Bonnard, P.; Salmon, D.; Dabis, F.; Spire, B. Association between elevated coffee consumption and daily chocolate intake with normal liver enzymes in HIV-HCV infected individuals: Results from the ANRS CO13 HEPAVIH cohort study. J. Hepatol. 2014, 60, 46–53. [Google Scholar] [CrossRef]
- Carrieri, M.P.; Cohen, J.; Salmon-Ceron, D.; Winnock, M. Coffee consumption and reduced self-reported side effects in HIV-HCV co-infected patients during PEG-IFN and ribavirin treatment: Results from ANRS CO13 HEPAVIH. J. Hepatol. 2012, 56, 745–747. [Google Scholar] [CrossRef] [PubMed]
- Hameleers, P.M.; Van Boxtel, M.J.; Hogervorst, E.; Riedel, W.J.; Houx, P.J.; Buntinx, F.; Jolles, J. Habitual caffeine consumption and its relation to memory, attention, planning capacity and psychomotor performance across multiple age groups. Hum. Psychopharmacol. Clin. Exp. 2000, 15, 573–581. [Google Scholar] [CrossRef] [PubMed]
- Wu, L.; Sun, D.; He, Y. Coffee intake and the incident risk of cognitive disorders: A dose–response meta-analysis of nine prospective cohort studies. Clin. Nutr. 2017, 36, 730–736. [Google Scholar] [CrossRef]
- Haller, S.; Montandon, M.-L.; Rodriguez, C.; Herrmann, F.; Giannakopoulos, P. Impact of Coffee, Wine, and Chocolate Consumption on Cognitive Outcome and MRI Parameters in Old Age. Nutrients 2018, 10, 1391. [Google Scholar] [CrossRef]
- Liu, Q.P.; Wu, Y.F.; Cheng, H.Y.; Xia, T.; Ding, H.; Wang, H.; Wang, Z.M.; Xu, Y. Habitual coffee consumption and risk of cognitive decline/dementia: A systematic review and meta-analysis of prospective cohort studies. Nutrition 2016, 32, 628–636. [Google Scholar] [CrossRef]
- Sheppard, D.P.; Iudicello, J.E.; Morgan, E.E.; Kamat, R.; Clark, L.R.; Avci, G.; Bondi, M.W.; Woods, S.P. Accelerated and Accentuated Neurocognitive Aging in HIV Infection. J. Neurovirol. 2017, 23, 492–500. [Google Scholar] [CrossRef]
- Barokar, J.; McCutchan, A.; Deutsch, R.; Tang, B.; Cherner, M.; Bharti, A.R. Neurocognitive impairment is worse in HIV/HCV-coinfected individuals with liver dysfunction. J. Neurovirol. 2019, 25, 792–799. [Google Scholar] [CrossRef]
- Fialho, R.; Pereira, M.; Bucur, M.; Fisher, M.; Whale, R.; Rusted, J. Cognitive impairment in HIV and HCV co-infected patients: A systematic review and meta-analysis. AIDS Care 2016, 28, 1481–1494. [Google Scholar] [CrossRef]
- Vivithanaporn, P.; Nelles, K.; DeBlock, L.; Newman, S.C.; Gill, M.J.; Power, C. Hepatitis C virus co-infection increases neurocognitive impairment severity and risk of death in treated HIV/AIDS. J. Neurol. Sci. 2012, 312, 45–51. [Google Scholar] [CrossRef]
- Vivithanaporn, P.; Maingat, F.; Lin, L.T.; Na, H.; Richardson, C.D.; Agrawal, B.; Cohen, É.A.; Jhamandas, J.H.; Power, C. Hepatitis C Virus Core Protein Induces Neuroimmune Activation and Potentiates Human Immunodeficiency Virus-1 Neurotoxicity. PLoS ONE 2010, 5, e12856. [Google Scholar] [CrossRef]
- Loko, M.A.; Salmon, D.; Carrieri, P.; Winnock, M.; Mora, M.; Merchadou, L.; Gillet, S.; Pambrun, E.; Delaune, J.; Valantin, M.A. The French national prospective cohort of patients co-infected with HIV and HCV (ANRS CO13 HEPAVIH): Early findings, 2006–2010. BMC Infect. Dis. 2010, 10, 303. [Google Scholar] [CrossRef] [PubMed]
- Michel, L.; Lions, C.; Winnock, M.; Lang, J.P.; Loko, M.A.; Rosenthal, E.; Marchou, B.; Valantin, M.A.; Morlat, P.; Roux, P.; et al. Psychiatric and substance use disorders in HIV/hepatitis C virus (HCV)-coinfected patients: Does HCV clearance matter? [Agence Nationale de Recherche sur le SIDA et les Hépatites Virales (ANRS) HEPAVIH CO13 cohort]. HIV Med. 2016, 17, 758–765. [Google Scholar] [CrossRef] [PubMed]
- Osterrieth, P.A. Le test de copie d’une figure complexe; contribution a l’etude de la perception et de la memoire. Arch. Psychol. 1944, 30, 205–550. [Google Scholar]
- Borkowski, J.G.; Benton, A.L.; Spreen, O. Word fluency and brain damage. Neuropsychologia 1967, 5, 135–140. [Google Scholar] [CrossRef]
- Wechsler, D. Wechsler adult intelligence scale–Fourth Edition (WAIS–IV). San Antonio TX NCS Pearson 2008, 22, 816–827. [Google Scholar]
- Reitan, R.M. Validity of the Trail Making Test as an indicator of organic brain damage. Percept. Mot. Ski. 1958, 8, 271–276. [Google Scholar] [CrossRef]
- Corrigan, J.D.; Hinkeldey, N.S. Relationships between Parts A and B of the Trail Making Test. J. Clin. Psychol. 1987, 43, 402–409. [Google Scholar] [CrossRef]
- Antinori, A.; Arendt, G.; Becker, J.T.; Brew, B.J.; Byrd, D.A.; Cherner, M.; Clifford, D.B.; Cinque, P.; Epstein, L.G.; Goodkin, K. Updated research nosology for HIV-associated neurocognitive disorders. Neurology 2007, 69, 1789–1799. [Google Scholar] [CrossRef]
- Bragança, M.; Marinho, M.; Marques, J.; Moreira, R.; Palha, A.; Marques-Teixeira, J.; Esteves, M. The influence of espresso coffee on neurocognitive function in HIV-infected patients. AIDS Care 2016, 28, 1149–1153. [Google Scholar] [CrossRef]
- Nehlig, A.; Daval, J.L.; Debry, G. Caffeine and the central nervous system: Mechanisms of action, biochemical, metabolic and psychostimulant effects. Brain Res. Rev. 1992, 17, 139–170. [Google Scholar] [CrossRef]
- Koppelstaetter, F.; Poeppel, T.D.; Siedentopf, C.M.; Ischebeck, A.; Kolbitsch, C.; Mottaghy, F.M.; Felber, S.R.; Jaschke, W.R.; Krause, B.J. Caffeine and Cognition in Functional Magnetic Resonance Imaging. J. Alzheimer’s Dis. 2010, 20, 71–84. [Google Scholar] [CrossRef] [PubMed]
- Cysneiros, R.M.; Farkas, D.; Harmatz, J.S.; von Moltke, L.L.; Greenblatt, D.J. Pharmacokinetic and Pharmacodynamic Interactions Between Zolpidem and Caffeine. Clin. Pharmacol. Ther. 2007, 82, 54–62. [Google Scholar] [CrossRef] [PubMed]
- Gutiérrez-Grobe, Y.; Chávez-Tapia, N.; Sánchez-Valle, V.; Gavilanes-Espinar, J.G.; Ponciano-Rodríguez, G.; Uribe, M.; Méndez-Sánchez, N. High coffee intake is associated with lower grade nonalcoholic fatty liver disease: The role of peripheral antioxidant activity. Ann. Hepatol. 2012, 11, 350–355. [Google Scholar] [CrossRef]
- Liang, N.; Kitts, D.D. Role of Chlorogenic Acids in Controlling Oxidative and Inflammatory Stress Conditions. Nutrients 2016, 8, 16. [Google Scholar] [CrossRef]
- Ivanov, A.V.; Bartosch, B.; Isaguliants, M.G. Oxidative Stress in Infection and Consequent Disease. Available online: https://www.hindawi.com/journals/omcl/2017/3496043/ (accessed on 4 August 2020).
- Yoshimura, H. The Potential of Caffeine for Functional Modification from Cortical Synapses to Neuron Networks in the Brain. Curr. Neuropharmacol. 2005, 3, 309–316. [Google Scholar] [CrossRef]
| N (%) | |
|---|---|
| Age, years | |
| Median (IQR) | 50 (48–53) |
| Gender | |
| Male | 93 (66.9) |
| Female | 46 (33.1) |
| High school certificate * | |
| No | 83 (59.7) |
| Yes | 56 (40.3) |
| Current MDD (N = 137) | |
| No | 107 (78.1) |
| Yes | 30 (21.9) |
| HIV-related characteristics: | |
| CD4 count, cells/mm3 (N = 138) | |
| Median (IQR) | 522 (346–726) |
| Detectable HIV viral load (N = 138) | |
| No | 126 (91.3) |
| Yes | 12 (8.7) |
| HCV-related characteristics: | |
| Ongoing HCV-treatment | |
| No | 116 (83.5) |
| Yes | 23 (16.6) |
| Presence of cirrhosis | |
| No | 106 (76.3) |
| Yes | 33 (23.7) |
| Cannabis use | |
| No | 81 (58.3) |
| Yes | 58 (41.7) |
| Coffee intake | |
| ≥3 cups/day | 40 (28.8) |
| ≤2 cups/day | 81 (58.3) |
| No consumption | 18 (13.0) |
| ROCF | Verbal Fluency (N = 134) | Coding (N = 135) | TMT B-A 1 (N = 132) | |||||||
|---|---|---|---|---|---|---|---|---|---|---|
| Copy (N = 134) | Delayed Reproduction (N = 131) 2 | |||||||||
| Coefficient (95% CI) | p-Value | Coefficient (95% CI) | p-Value | Coefficient (95% CI) | p-Value | Coefficient (95% CI) | p-Value | Coefficient (95% CI) | p-Value | |
| Coffee intake | ||||||||||
| ≤2 cups/day | 3.35 (−0.28 to 6.99) | 0.070 | 3.05 (−0.78 to 6.87) | 0.117 | 2.32 (−0.33 to 4.97) | 0.085 | 7.58 (0.18 to 14.97) | 0.045 | −0.11 (−0.28 to 0.07) | 0.226 |
| ≥3 cups/day | 4.63 (0.88 to 8.39) | 0.016 | 2.70 (−1.44 to 6.84) | 0.199 | 3.08 (0.18 to 5.97) | 0.037 | 9.24 (1.26 to 17.36) | 0.024 | −0.27 (−0.47 to −0.07) | 0.009 |
| Age | 0.10 (−0.04 to 0.25) | 0.165 | −0.09 (−0.26 to 0.09) | 0.333 | 0.03 (−0.12 to 0.16) | 0.701 | −0.82 (−1.18 to −0.46) | 0.000 | 0.00 (−0.01 to 0.01) | 0.608 |
| Educational level 3 | −1.19 (−2.79 to 0.41) | 0.145 | 2.06 (−0.08 to 4.20) | 0.059 | 0.59 (−1.25 to 2.42) | 0.527 | 1.03 (−2.93 to 5.00) | 0.607 | −0.06 (−0.17 to 0.05) | 0.302 |
| Current MDD | −1.88 (−4.61 to 0.85) | 0.176 | −2.81 (−5.23 to −0.38) | 0.024 | −0.73 (−2.74 to 1.29) | 0.477 | −6.75 (−11.50 to −2.00) | 0.006 | 0.05 ( −0.11 to 0.22) | 0.529 |
| Presence of cirrhosis | −2.28 (−4.49 to −0.07) | 0.043 | −1.12 (−3.60 to 1.38) | 0.380 | −1.07 (−3.04 to 0.89) | 0.282 | −4.38 (−9.23 to 0.47) | 0.076 | 0.07 (−0.06 to 0.19) | 0.288 |
| Ongoing HCV treatment | 0.26 (−1.67 to 2.18) | 0.792 | 0.13 (−3.15 to 3.40) | 0.939 | −2.43 (−4.72 to −0.13) | 0.039 | −9.01 (−14.14 to −3.88) | 0.001 | 0.00 (−0.14 to 0.15) | 0.988 |
| Detectable HIV viral load | 0.13 (−1.83 to 2.09) | 0.896 | −0.71 (−3.56 to 2.14) | 0.623 | −1.73 (−4.41 to 0.96) | 0.205 | −10.97 (−17.38 to −4.55) | 0.001 | 0.21 (0.05 to 0.38) | 0.013 |
| Cannabis use | −0.89 (−2.65 to 0.87) | 0.320 | −0.46 (−2.70 to 1.78) | 0.685 | −1.77 (−3.61 to 0.06) | 0.058 | −4.91 (−8.98 to −0.84) | 0.019 | 0.09 (−0.03 to 0.20) | 0.149 |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Antwerpes, S.; Protopopescu, C.; Morlat, P.; Marcellin, F.; Wittkop, L.; Di Beo, V.; Salmon-Céron, D.; Sogni, P.; Michel, L.; Carrieri, M.P.; et al. Coffee Intake and Neurocognitive Performance in HIV/HCV Coinfected Patients (ANRS CO13 HEPAVIH). Nutrients 2020, 12, 2532. https://doi.org/10.3390/nu12092532
Antwerpes S, Protopopescu C, Morlat P, Marcellin F, Wittkop L, Di Beo V, Salmon-Céron D, Sogni P, Michel L, Carrieri MP, et al. Coffee Intake and Neurocognitive Performance in HIV/HCV Coinfected Patients (ANRS CO13 HEPAVIH). Nutrients. 2020; 12(9):2532. https://doi.org/10.3390/nu12092532
Chicago/Turabian StyleAntwerpes, Saskia, Camelia Protopopescu, Philippe Morlat, Fabienne Marcellin, Linda Wittkop, Vincent Di Beo, Dominique Salmon-Céron, Philippe Sogni, Laurent Michel, Maria Patrizia Carrieri, and et al. 2020. "Coffee Intake and Neurocognitive Performance in HIV/HCV Coinfected Patients (ANRS CO13 HEPAVIH)" Nutrients 12, no. 9: 2532. https://doi.org/10.3390/nu12092532
APA StyleAntwerpes, S., Protopopescu, C., Morlat, P., Marcellin, F., Wittkop, L., Di Beo, V., Salmon-Céron, D., Sogni, P., Michel, L., Carrieri, M. P., & the ANRS CO13 HEPAVIH Study Group. (2020). Coffee Intake and Neurocognitive Performance in HIV/HCV Coinfected Patients (ANRS CO13 HEPAVIH). Nutrients, 12(9), 2532. https://doi.org/10.3390/nu12092532





