Exploring the Diets of Adults with Obesity and Type II Diabetes from Nine Diverse Countries: Dietary Intakes, Patterns, and Quality
Abstract
1. Introduction
2. Materials and Methods
2.1. Subjects
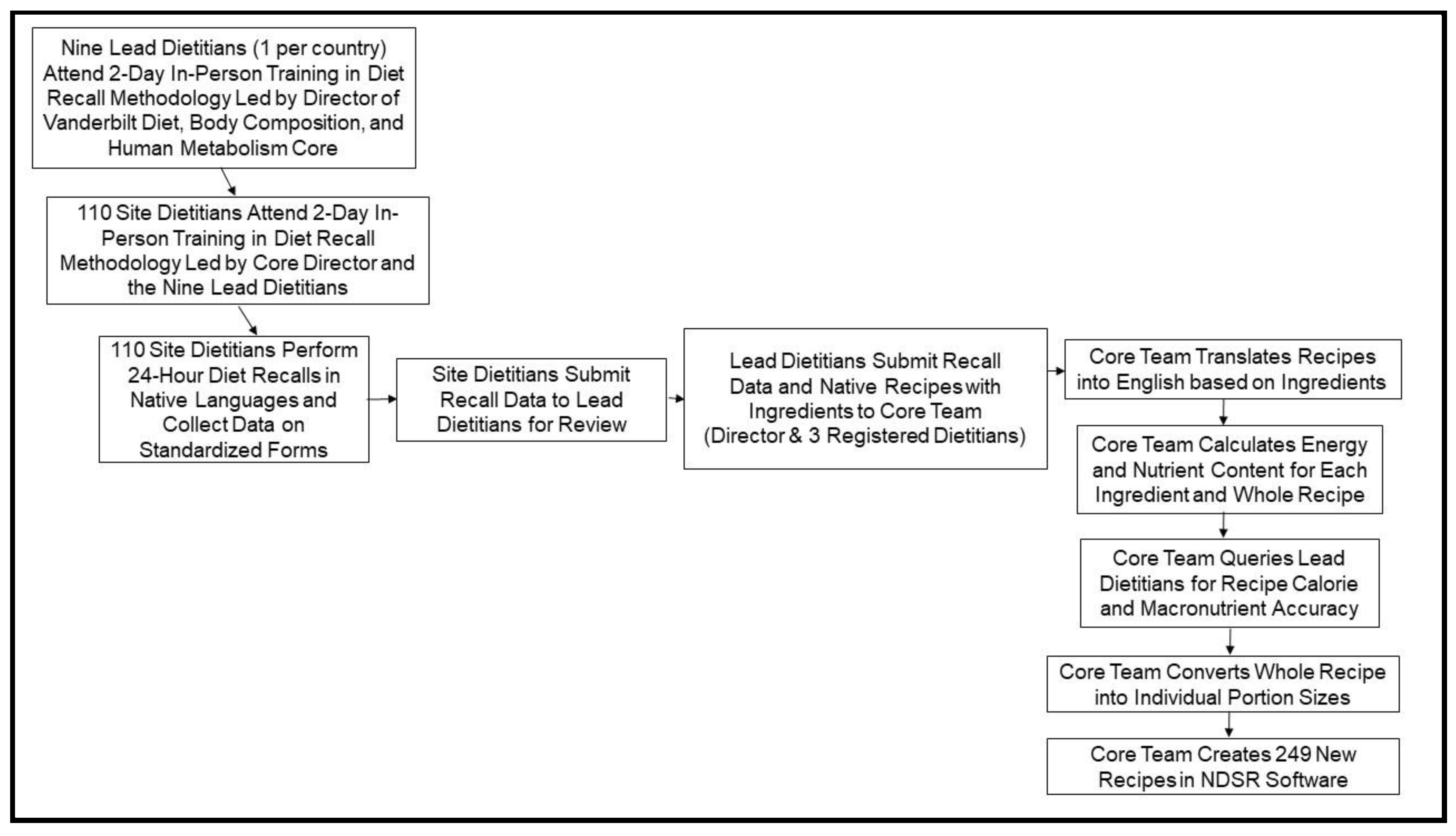
2.2. Diet Assessment
2.3. Diet Data Analysis
2.4. Statistical Analysis
3. Results
3.1. Demographics
3.2. Dietary Intakes
3.3. Dietary Patterns
3.4. Dietary Quality
4. Discussion
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
Abbreviations
| BMI | body mass index |
| Core | Vanderbilt diet, body composition, and human metabolism core |
| EPIC | European prospective investigation of cancer |
| FPG | fasting plasma glucose |
| HbA1c | hemoglobin A1c |
| HEI | healthy eating index |
| HOMA-IR | homeostasis model of insulin resistance |
| IPAQ | international physical activity questionnaire |
| IRB | institutional review board |
| Kg | kilogram |
| M | meter |
| Mol | mole |
| Mmol | milli mole |
| MUFA | Monounsaturated fat |
| NDSR | nutrition data system for research |
| PCA | principal component analysis |
| PUFA | Polyunsaturated fat |
| SFA | Saturated fat |
| SPSS | statistical package for social sciences |
| T2DM | type 2 diabetes mellitus |
References
- Bommer, C.; Sagalova, V.; Heesemann, E.; Manne-Goehler, J.; Atun, R.; Barnighausen, T.; Davies, J.; Vollmer, S. Global Economic Burden of Diabetes in Adults: Projections From 2015 to 2030. Diabetes Care 2018. [Google Scholar] [CrossRef]
- Stratton, I.M.; Adler, A.I.; Neil, H.A.; Matthews, D.R.; Manley, S.E.; Cull, C.A.; Hadden, D.; Turner, R.C.; Holman, R.R. Association of glycaemia with macrovascular and microvascular complications of type 2 diabetes (UKPDS 35): Prospective observational study. BMJ 2000, 321, 405–412. [Google Scholar] [CrossRef] [PubMed]
- Hu, F.B.; Manson, J.E.; Stampfer, M.J.; Colditz, G.; Liu, S.; Solomon, C.G.; Willett, W.C. Diet, lifestyle, and the risk of type 2 diabetes mellitus in women. N. Engl. J. Med. 2001, 345, 790–797. [Google Scholar] [CrossRef] [PubMed]
- Knowler, W.C.; Barrett-Connor, E.; Fowler, S.E.; Hamman, R.F.; Lachin, J.M.; Walker, E.A.; Nathan, D.M.; Diabetes Prevention Program Research Group. Reduction in the incidence of type 2 diabetes with lifestyle intervention or metformin. N. Engl. J. Med. 2002, 346, 393–403. [Google Scholar] [CrossRef]
- Dyson, P.A.; Twenefour, D.; Breen, C.; Duncan, A.; Elvin, E.; Goff, L.; Hill, A.; Kalsi, P.; Marsland, N.; McCardle, P.; et al. Diabetes UK evidence-based nutrition guidelines for the prevention and management of diabetes. Diabet Med. 2018. [Google Scholar] [CrossRef]
- Handelsman, Y.; Bloomgarden, Z.T.; Grunberger, G.; Umpierrez, G.; Zimmerman, R.S.; Bailey, T.S.; Blonde, L.; Bray, G.A.; Cohen, A.J.; Dagogo-Jack, S.; et al. American Association of Clinical Endocrinologists and American College of Endocrinology—Clinical Practice Guidelines for Developing a Diabetes Mellitus Comprehensive Care Plan—2015—Executive Summary. Endocr. Pract. 2015, 21, 413–437. [Google Scholar] [CrossRef]
- Shrivastava, S.R.; Shrivastava, P.S.; Ramasamy, J. World Health Organization advocates for a healthy diet for all: Global perspective. J. Res. Med. Sci. 2016, 21, 44. [Google Scholar] [CrossRef]
- Bantle, J.P.; Wylie-Rosett, J.; Albright, A.L.; Apovian, C.M.; Clark, N.G.; Franz, M.J.; Hoogwerf, B.J.; Lichtenstein, A.H.; Mayer-Davis, E.; et al.; American Diabetes Association Nutrition recommendations and interventions for diabetes: A position statement of the American Diabetes Association. Diabetes Care 2008, 31 (Suppl. 1), S61–S78. [Google Scholar] [CrossRef] [PubMed]
- Cordain, L.; Eaton, S.B.; Sebastian, A.; Mann, N.; Lindeberg, S.; Watkins, B.A.; O’Keefe, J.H.; Brand-Miller, J. Origins and evolution of the Western diet: Health implications for the 21st century. Am. J. Clin. Nutr. 2005, 81, 341–354. [Google Scholar] [CrossRef]
- Oberlander, L.; Disdier, A.C.; Etile, F. Globalisation and national trends in nutrition and health: A grouped fixed-effects approach to intercountry heterogeneity. Health Econ. 2017, 26, 1146–1161. [Google Scholar] [CrossRef]
- Oggioni, C.; Lara, J.; Wells, J.C.; Soroka, K.; Siervo, M. Shifts in population dietary patterns and physical inactivity as determinants of global trends in the prevalence of diabetes: An ecological analysis. Nutr. Metab. Cardiovasc. Dis. 2014, 24, 1105–1111. [Google Scholar] [CrossRef] [PubMed]
- Niswender, K.; Piletic, M.; Andersen, H.; Conradsen Hiort, L.; Hollander, P. Weight change upon once-daily initiation of insulin detemir with or without dietary intervention in overweight or obese insulin-naive individuals with type 2 diabetes: Results from the DIET trial. Diabetes Obes. Metab. 2014, 16, 186–192. [Google Scholar] [CrossRef]
- Moshfegh, A.J.; Borrud, L.; Perloff, B.; LaComb, R. Improved Method for the 24-hour Dietary Recall for Use in National Surveys. FASEB J. 1999, 13, A603. [Google Scholar]
- Moshfegh, A.J.; Rhodes, D.G.; Baer, D.J.; Murayi, T.; Clemens, J.C.; Rumpler, W.V.; Paul, D.R.; Sebastian, R.S.; Kuczynski, K.J.; Ingwersen, L.A.; et al. The US Department of Agriculture Automated Multiple-Pass Method reduces bias in the collection of energy intakes. Am. J. Clin. Nutr. 2008, 88, 324–332. [Google Scholar] [CrossRef]
- Conway, J.M.; Ingwersen, L.A.; Moshfegh, A.J. Accuracy of dietary recall using the USDA five-step multiple-pass method in men: An observational validation study. J. Am. Diet. Assoc. 2004, 104, 595–603. [Google Scholar] [CrossRef]
- Conway, J.M.; Ingwersen, L.A.; Vinyard, B.T.; Moshfegh, A.J. Effectiveness of the US Department of Agriculture 5-step multiple-pass method in assessing food intake in obese and nonobese women. Am. J. Clin. Nutr. 2003, 77, 1171–1178. [Google Scholar] [CrossRef]
- Ahuja, J.K.; Moshfegh, A.J.; Holden, J.M.; Harris, E. USDA food and nutrient databases provide the infrastructure for food and nutrition research, policy, and practice. J. Nutr. 2013, 143, 241S–249S. [Google Scholar] [CrossRef]
- Guenther, P.M.; Kirkpatrick, S.I.; Reedy, J.; Krebs-Smith, S.M.; Buckman, D.W.; Dodd, K.W.; Casavale, K.O.; Carroll, R.J. The Healthy Eating Index-2010 is a valid and reliable measure of diet quality according to the 2010 Dietary Guidelines for Americans. J. Nutr. 2014, 144, 399–407. [Google Scholar] [CrossRef] [PubMed]
- Krebs-Smith, S.M.; Pannucci, T.E.; Subar, A.F.; Kirkpatrick, S.I.; Lerman, J.L.; Tooze, J.A.; Wilson, M.M.; Reedy, J. Update of the Healthy Eating Index: HEI-2015. J. Acad. Nutr. Diet. 2018, 118, 1591–1602. [Google Scholar] [CrossRef]
- Guenther, P.M.; Casavale, K.O.; Reedy, J.; Kirkpatrick, S.I.; Hiza, H.A.; Kuczynski, K.J.; Kahle, L.L.; Krebs-Smith, S.M. Update of the Healthy Eating Index: HEI-2010. J. Acad. Nutr. Diet. 2013, 113, 569–580. [Google Scholar] [CrossRef]
- Gorst-Rasmussen, A.; Dahm, C.C.; Dethlefsen, C.; Scheike, T.; Overvad, K. Exploring dietary patterns by using the treelet transform. Am. J. Epidemiol. 2011, 173, 1097–1104. [Google Scholar] [CrossRef] [PubMed]
- Liu, R.X.; Kuang, J.; Gong, Q.; Hou, X.L. Principal component regression analysis with SPSS. Comput. Methods Programs Biomed. 2003, 71, 141–147. [Google Scholar] [CrossRef]
- Hallal, P.C.; Victora, C.G. Reliability and validity of the International Physical Activity Questionnaire (IPAQ). Med. Sci. Sports Exerc. 2004, 36, 556. [Google Scholar] [CrossRef]
- Craig, C.L.; Marshall, A.L.; Sjostrom, M.; Bauman, A.E.; Booth, M.L.; Ainsworth, B.E.; Pratt, M.; Ekelund, U.; Yngve, A.; Sallis, J.F.; et al. International physical activity questionnaire: 12-country reliability and validity. Med. Sci. Sports Exerc. 2003, 35, 1381–1395. [Google Scholar] [CrossRef]
- World Health Organization. Coronavirus Disease (COVID-19) Data. Available online: https://apps.who.int/infobase/Indicators.aspx (accessed on 4 April 2020).
- Fung, T.T.; Schulze, M.; Manson, J.E.; Willett, W.C.; Hu, F.B. Dietary patterns, meat intake, and the risk of type 2 diabetes in women. Arch. Intern. Med. 2004, 164, 2235–2240. [Google Scholar] [CrossRef]
- van Dam, R.M.; Rimm, E.B.; Willett, W.C.; Stampfer, M.J.; Hu, F.B. Dietary patterns and risk for type 2 diabetes mellitus in U.S. men. Ann. Intern. Med. 2002, 136, 201–209. [Google Scholar] [CrossRef]
- Ajala, O.; English, P.; Pinkney, J. Systematic review and meta-analysis of different dietary approaches to the management of type 2 diabetes. Am. J. Clin. Nutr. 2013, 97, 505–516. [Google Scholar] [CrossRef]
- Esposito, K.; Maiorino, M.I.; Bellastella, G.; Chiodini, P.; Panagiotakos, D.; Giugliano, D. A journey into a Mediterranean diet and type 2 diabetes: A systematic review with meta-analyses. BMJ Open 2015, 5, e008222. [Google Scholar] [CrossRef]
- Huo, R.; Du, T.; Xu, Y.; Xu, W.; Chen, X.; Sun, K.; Yu, X. Effects of Mediterranean-style diet on glycemic control, weight loss and cardiovascular risk factors among type 2 diabetes individuals: A meta-analysis. Eur. J. Clin. Nutr. 2015, 69, 1200–1208. [Google Scholar] [CrossRef]
- Carter, P.; Achana, F.; Troughton, J.; Gray, L.J.; Khunti, K.; Davies, M.J. A Mediterranean diet improves HbA1c but not fasting blood glucose compared to alternative dietary strategies: A network meta-analysis. J. Hum. Nutr. Diet. 2014, 27, 280–297. [Google Scholar] [CrossRef]
- Itsiopoulos, C.; Brazionis, L.; Kaimakamis, M.; Cameron, M.; Best, J.D.; O’Dea, K.; Rowley, K. Can the Mediterranean diet lower HbA1c in type 2 diabetes? Results from a randomized cross-over study. Nutr. Metab. Cardiovasc. Dis. 2011, 21, 740–747. [Google Scholar] [CrossRef]
- Koloverou, E.; Panagiotakos, D.B.; Pitsavos, C.; Chrysohoou, C.; Georgousopoulou, E.N.; Grekas, A.; Christou, A.; Chatzigeorgiou, M.; Skoumas, I.; Tousoulis, D.; et al. Adherence to Mediterranean diet and 10-year incidence (2002–2012) of diabetes: Correlations with inflammatory and oxidative stress biomarkers in the ATTICA cohort study. Diabetes Metab. Res. Rev. 2016, 32, 73–81. [Google Scholar] [CrossRef]
- Diaz-Lopez, A.; Babio, N.; Martinez-Gonzalez, M.A.; Corella, D.; Amor, A.J.; Fito, M.; Estruch, R.; Aros, F.; Gomez-Gracia, E.; Fiol, M.; et al. Mediterranean Diet, Retinopathy, Nephropathy, and Microvascular Diabetes Complications: A Post Hoc Analysis of a Randomized Trial. Diabetes Care 2015, 38, 2134–2141. [Google Scholar] [CrossRef] [PubMed]
- Martinez-Gonzalez, M.A.; Salas-Salvado, J.; Estruch, R.; Corella, D.; Fito, M.; Ros, E.; Predimed, I. Benefits of the Mediterranean Diet: Insights From the PREDIMED Study. Prog. Cardiovasc. Dis. 2015, 58, 50–60. [Google Scholar] [CrossRef]
- Schwedhelm, C.; Iqbal, K.; Knuppel, S.; Schwingshackl, L.; Boeing, H. Contribution to the understanding of how principal component analysis-derived dietary patterns emerge from habitual data on food consumption. Am. J. Clin. Nutr. 2018, 107, 227–235. [Google Scholar] [CrossRef]
- Vernarelli, J.A.; Mitchell, D.C.; Rolls, B.J.; Hartman, T.J. Dietary energy density is associated with obesity and other biomarkers of chronic disease in US adults. Eur. J. Nutr. 2015, 54, 59–65. [Google Scholar] [CrossRef]
- Mendoza, J.A.; Drewnowski, A.; Christakis, D.A. Dietary energy density is associated with obesity and the metabolic syndrome in U.S. adults. Diabetes Care 2007, 30, 974–979. [Google Scholar] [CrossRef]
- Wang, J.; Luben, R.; Khaw, K.T.; Bingham, S.; Wareham, N.J.; Forouhi, N.G. Dietary energy density predicts the risk of incident type 2 diabetes: The European Prospective Investigation of Cancer (EPIC)-Norfolk Study. Diabetes Care 2008, 31, 2120–2125. [Google Scholar] [CrossRef]
- InterAct, C.; van den Berg, S.W.; van der, A.D.; Spijkerman, A.M.; van Woudenbergh, G.J.; Tijhuis, M.J.; Amiano, P.; Ardanaz, E.; Beulens, J.W.; Boeing, H.; et al. The association between dietary energy density and type 2 diabetes in Europe: Results from the EPIC-InterAct Study. PLoS ONE 2013, 8, e59947. [Google Scholar] [CrossRef]
- Lee, Y.M.; Kim, S.A.; Lee, I.K.; Kim, J.G.; Park, K.G.; Jeong, J.Y.; Jeon, J.H.; Shin, J.Y.; Lee, D.H. Effect of a Brown Rice Based Vegan Diet and Conventional Diabetic Diet on Glycemic Control of Patients with Type 2 Diabetes: A 12-Week Randomized Clinical Trial. PLoS ONE 2016, 11, e0155918. [Google Scholar] [CrossRef]
- Tonstad, S.; Stewart, K.; Oda, K.; Batech, M.; Herring, R.P.; Fraser, G.E. Vegetarian diets and incidence of diabetes in the Adventist Health Study-2. Nutr. Metab. Cardiovasc. Dis. 2013, 23, 292–299. [Google Scholar] [CrossRef] [PubMed]
- Mamluk, L.; O’Doherty, M.G.; Orfanos, P.; Saitakis, G.; Woodside, J.V.; Liao, L.M.; Sinha, R.; Boffetta, P.; Trichopoulou, A.; Kee, F. Fruit and vegetable intake and risk of incident of type 2 diabetes: Results from the consortium on health and ageing network of cohorts in Europe and the United States (CHANCES). Eur. J. Clin. Nutr. 2017, 71, 83–91. [Google Scholar] [CrossRef]
- Satija, A.; Bhupathiraju, S.N.; Rimm, E.B.; Spiegelman, D.; Chiuve, S.E.; Borgi, L.; Willett, W.C.; Manson, J.E.; Sun, Q.; Hu, F.B. Plant-Based Dietary Patterns and Incidence of Type 2 Diabetes in US Men and Women: Results from Three Prospective Cohort Studies. PLoS Med. 2016, 13, e1002039. [Google Scholar] [CrossRef]
| Argentina | Germany | Poland | Serbia | Slovakia | Slovenia | Spain | Turkey | USA | p Value a | |
|---|---|---|---|---|---|---|---|---|---|---|
| Total Amount (g) | 2356.3 ± 99.2 | 2821.9 ± 152.7 | 2599.2 ± 110.9 | 2565.2 ± 133.3 | 2634.6 ± 100.6 | 2647.9 ± 260.6 | 2726.0 ± 176.6 | 3647.3 ± 250.3 | 2894.1 ± 64.3 | <0.001 |
| Energy (kcal) | 1768.3 ± 89.8 | 2271.7 ± 189.9 | 1708.1 ± 89.8 | 1882.9 ± 122.7 | 1611.4 ± 78.9 | 1967.5 ± 235.9 | 2245.3 ± 228.0 | 1952.7 ± 163.6 | 2115.4 ± 54.9 | 0.001 |
| Protein (%kcal) | 20.5 ± 0.9 | 18.4 ± 1.1 | 20.5 ± 0.6 | 19.9 ± 1.1 | 19.9 ± 0.8 | 18.4 ± 1.0 | 16.6 ± 1.0 | 18.3 ± 1.1 | 17.7 ± 0.3 | 0.001 |
| Fat (%kcal) | 34.5 ± 1.1 | 39.8 ± 1.5 | 34.4 ± 1.2 | 36.2 ± 2.1 | 37.5 ± 1.7 | 32.9 ± 2.1 | 38.2 ± 2.7 | 32.9 ± 1.8 | 38.1 ± 0.6 | 0.009 |
| SFA (%total fat) | 35.1 ± 1.2 | 35.0 ± 1.7 | 33.6 ± 1.1 | 34.3 ± 1.4 | 34.8 ± 1.4 | 30.4 ± 1.6 | 29.4 ± 1.9 | 33.4 ± 1.5 | 33.6 ± 0.5 | 0.12 |
| MUFA (%total fat) | 35.8 ± 0.8 | 34.3 ± 1.7 | 35.4 ± 0.8 | 34.0 ± 0.8 | 36.2 ± 0.9 | 36.0 ± 1.4 | 43.7 ± 1.8 | 39.4 ± 1.8 | 36.9 ± 0.3 | 0.002 |
| PUFA (%total fat) | 20.0 ± 1.3 | 14.9 ± 1.4 | 18.5 ± 1.1 | 20.8 ± 1.7 | 19.7 ± 1.6 | 24.6 ± 2.4 | 19.9 ± 1.8 | 19.4 ± 1.3 | 21.2 ± 0.5 | <0.001 |
| Unsat:SFA (ratio) | 0.7 ± 0.1 | 0.5 ± 0.1 | 0.6 ± 0.1 | 0.7 ± 0.9 | 0.6 ± 0.1 | 0.9 ± 0.1 | 0.8 ± 0.1 | 0.6 ± 0.1 | 0.7 ± 0.0 | 0.05 |
| Trans Fat (g) | 3.4 ± 0.2 | 4.1 ± 0.6 | 2.4 ± 0.3 | 2.7 ± 0.3 | 2.2 ± 0.2 | 2.9 ± 0.6 | 3.0 ± 0.4 | 3.6 ± 0.6 | 3.9 ± 0.2 | 0.008 |
| Carbohydrate (%kcal) | 44.6 ± 1.7 | 40.3 ± 1.9 | 44.9 ± 1.4 | 43.1 ± 2.2 | 40.7 ± 1.9 | 45.6 ± 2.4 | 43.2 ± 2.9 | 48.8 ± 2.0 | 43.8 ± 0.7 | 0.16 |
| Available CHO (g) | 182.2 ± 11.0 | 194.8 ± 21.8 | 163.6 ± 9.8 | 169.9 ± 10.7 | 147.5 ± 9.0 | 192.5 ± 21.5 | 210.5 ± 21.5 | 209.9 ± 16.0 | 210.9 ± 5.9 | 0.001 |
| Starch (g) | 94.2 ± 7.6 | 107.3 ± 14.8 | 96.8 ± 6.2 | 100.8 ± 7.7 | 81.0 ± 5.2 | 111.6 ± 13.6 | 104.1 ± 12.3 | 108.0 ± 9.5 | 113.3 ± 3.7 | 0.10 |
| Total Sugars (g) | 74.7 ± 5.6 | 74.5 ± 8.7 | 56.4 ± 4.5 | 56.2 ± 5.5 | 53.8 ± 4.5 | 64.7 ± 8.6 | 89.6 ± 12.6 | 84.1 ± 8.3 | 84.9 ± 3.5 | <0.001 |
| Added Sugars (g) | 32.1 ± 4.5 | 47.0 ± 7.7 | 17.6 ± 2.3 | 15.7 ± 2.2 | 23.8 ± 3.1 | 19.2 ± 4.6 | 39.4 ± 8.8 | 29.2 ± 5.0 | 52.9 ± 3.3 | <0.001 |
| Sucrose (g) | 23.4 ± 2.6 | 39.6 ± 7.2 | 16.8 ± 2.1 | 13.7 ± 1.8 | 21.9 ± 2.8 | 17.7 ± 4.1 | 28.5 ± 6.5 | 22.3 ± 3.4 | 33.8 ± 2.1 | <0.001 |
| Fructose (g) | 19.8 ± 1.7 | 10.5 ± 1.3 | 15.7 ± 1.6 | 13.6 ± 2.2 | 11.7 ± 1.2 | 20.5 ± 3.2 | 25.5 ± 4.8 | 23.3 ± 2.4 | 18.7 ± 1.1 | 0.001 |
| Total Dietary Fiber (g) | 22.0 ± 1.4 | 19.0 ± 1.5 | 21.5 ± 1.6 | 18.6 ± 1.4 | 17.1 ± 1.3 | 28.2 ± 4.7 | 23.6 ± 3.2 | 27.1 ± 2.9 | 19.4 ± 0.6 | <0.001 |
| Glycemic Index (%) | 85.4 ± 1.4 | 80.3 ± 1.8 | 74.0 ± 1.5 | 79.8 ± 2.0 | 81.0 ± 1.3 | 80.9 ± 1.5 | 83.9 ± 1.9 | 83.9 ± 2.1 | 85.7 ± 0.5 | <0.001 |
| Glycemic Load (g) | 158.9 ± 10.5 | 159.2 ± 20.3 | 122.8 ± 8.6 | 136.3 ± 9.8 | 118.6 ± 7.0 | 156.5 ± 18.4 | 180.2 ± 20.0 | 177.9 ± 14.9 | 181.4 ± 5.4 | <0.001 |
| Sodium (mg) | 3115.8 ± 218.1 | 3663.6 ± 323.2 | 4313.4 ± 257.0 | 3779.4 ± 259.4 | 4134.4 ± 415.0 | 3936.0 ± 558.8 | 4075.5 ± 441.0 | 4509.4 ± 500.1 | 4047.7 ± 126.9 | 0.05 |
| Water (ml) | 1999.0 ± 90.8 | 2377.1 ± 138.6 | 2246.7 ± 103.0 | 2189.6 ± 121.1 | 2314.6 ± 93.0 | 2246.3 ± 236.5 | 2300.4 ± 159.4 | 3259.0 ± 242.4 | 2488.1 ± 59.4 | <0.001 |
| USA (N = 316) | Argentina (N = 63) | ||||||||
|---|---|---|---|---|---|---|---|---|---|
| Factor | 1 | 2 | 3 | 4 | Factor | 1 | 2 | 3 | 4 |
| Eigenvalue | 1.65 | 1.53 | 1.37 | 1.32 | Eigenvalue | 1.84 | 1.63 | 1.47 | 1.28 |
| Variance (%) | 11.79 | 10.93 | 9.78 | 9.43 | Variance (%) | 16.7 | 14.8 | 13.4 | 11.6 |
| Fruits | 0.54 | 0.23 | Fruits | 0.39 | 0.30 | 0.31 | |||
| Vegetables | 0.38 | Vegetables | 0.24 | 0.61 | 0.22 | 0.28 | |||
| Grains, Breads, Starches, Cereals | 0.38 | 0.57 | Grains, Breads, Starches, Cereals | 0.52 | |||||
| Red Meats | 0.43 | 0.36 | Red Meats | 0.85 | |||||
| White Meats and Fish | 0.74 | White Meats and Fish | 0.79 | 0.21 | |||||
| Legumes and Plant-Based Proteins | 0.50 | Legumes and Plant-Based Proteins | |||||||
| Dairy | 0.52 | Dairy | |||||||
| Desserts and Sweets | 0.28 | 0.41 | Desserts and Sweets | 0.30 | |||||
| Fats (Monounsaturated) | 0.59 | Fats (Monounsaturated) | 0.77 | 0.26 | |||||
| Fats (Polyunsaturated and Saturated) | 0.73 | Fats (Polyunsaturated and Saturated) | 0.83 | ||||||
| Water | 0.26 | Water | 0.25 | ||||||
| Beverages (Noncaloric) | 0.58 | Beverages (Noncaloric) | 0.64 | ||||||
| Beverages (Sweetened) | Beverages (Sweetened) | ||||||||
| Alcohol | 0.52 | Alcohol | |||||||
| Germany (N = 42) | Poland (N = 44) | ||||||||
| Factor | 1 | 2 | 3 | Factor | 1 | 2 | 3 | ||
| Eigenvalue | 2.53 | 1.72 | 1.53 | Eigenvalue | 2.07 | 1.97 | 1.64 | ||
| Variance (%) | 21.05 | 14.35 | 12.77 | Variance (%) | 18.8 | 17.9 | 14.9 | ||
| Fruits | 0.63 | Fruits | 0.45 | 0.33 | |||||
| Vegetables | 0.21 | Vegetables | 0.71 | ||||||
| Grains, Breads, Starches, Cereals | 0.90 | Grains, Breads, Starches, Cereals | 0.80 | ||||||
| Red Meat | 0.23 | Red Meats | |||||||
| White Meats and Fish | White Meats and Fish | 0.42 | 0.46 | 0.48 | |||||
| Legumes and Plant-Based Proteins | Legumes and Plant-Based Proteins | ||||||||
| Dairy | 0.60 | Dairy | 0.27 | ||||||
| Sweets | 0.95 | Desserts and Sweets | 0.24 | 0.50 | |||||
| Fats (Monounsaturated) | 0.74 | Fats (Monounsaturated) | 0.71 | ||||||
| Fats (Polyunsaturated and Saturated) | 0.88 | Fats (Polyunsaturated and Saturated) | 0.78 | 0.36 | |||||
| Water | 0.75 | Water | 0.54 | ||||||
| Beverages (Noncaloric) | 0.64 | Beverages (Noncaloric) | 0.59 | ||||||
| Beverages (Sweetened) | Beverages (Sweetened) | ||||||||
| Alcohol | Alcohol | ||||||||
| Serbia (N = 39) | Slovakia (N = 31) | ||||||||
| Factor | 1 | 2 | 3 | 4 | Factor | 1 | 2 | 3 | 4 |
| Eigenvalue | 1.75 | 1.58 | 1.52 | 1.49 | Eigenvalue | 2.04 | 1.90 | 1.77 | 1.60 |
| Variance (%) | 15.89 | 14.36 | 13.82 | 13.55 | Variance (%) | 17 | 15.9 | 14.8 | 13.4 |
| Fruits | 0.52 | Fruits | 0.78 | ||||||
| Vegetables | 0.41 | 0.67 | Vegetables | 0.62 | |||||
| Grains, Breads, Starches, Cereals | 0.59 | 0.29 | Grains, Breads, Starches, Cereals | 0.32 | 0.59 | 0.32 | |||
| Red Meats | 0.21 | 0.32 | Red Meats | ||||||
| White Meats and Fish | 0.75 | White Meats and Fish | 0.93 | ||||||
| Legumes and Plant-Based Proteins | Legumes and Plant-Based Proteins | ||||||||
| Dairy | 0.80 | Dairy | 0.31 | 0.62 | 0.35 | ||||
| Desserts and Sweets | 0.89 | Desserts and Sweets | 0.59 | 0.23 | |||||
| Fats (Monounsaturated) | 0.80 | Fats (Monounsaturated) | 0.20 | ||||||
| Fats (Polyunsaturated and Saturated) | 0.72 | Fats (Polyunsaturated and Saturated) | 0.76 | 0.29 | |||||
| Water | Water | 0.73 | |||||||
| Beverages (Noncaloric) | 0.71 | 0.46 | Beverages (Noncaloric) | 0.49 | 0.25 | ||||
| Beverages (Sweetened) | Beverages (Sweetened) | 0.82 | |||||||
| Alcohol | Alcohol | ||||||||
| Slovenia (N = 22) | Spain (N = 27) | ||||||||
| Factor | 1 | 2 | 3 | 4 | Factor | 1 | 2 | 3 | 4 |
| Eigenvalue | 3.10 | 3.02 | 1.69 | 1.43 | Eigenvalue | 2.31 | 2.11 | 1.67 | 1.65 |
| Variance (%) | 23.83 | 23.21 | 12.99 | 9.53 | Variance (%) | 17.79 | 16.24 | 12.83 | 12.69 |
| Fruits | 0.22 | 0.72 | Fruits | 0.21 | 0.67 | ||||
| Vegetables | 0.75 | 0.31 | Vegetables | 0.74 | |||||
| Grains, Breads, Starches, Cereals | 0.93 | 0.56 | Grains, Breads, Starches, Cereals | 0.68 | 0.27 | ||||
| Red Meats | 0.82 | Red Meats | 0.38 | 0.70 | |||||
| White Meats and Fish | 0.24 | White Meats and Fish | 0.60 | 0.25 | |||||
| Legumes and Plant-Based Proteins | 0.29 | 0.60 | 0.56 | Legumes and Plant-Based Proteins | |||||
| Dairy | 0.42 | 0.59 | 0.35 | Dairy | 0.36 | ||||
| Desserts and Sweets | 0.50 | 0.68 | Desserts and Sweets | 0.85 | |||||
| Fats (Monounsaturated) | 0.29 | 0.46 | Fats (Monounsaturated) | 0.77 | 0.29 | ||||
| Fats (Polyunsaturated and Saturated) | 0.69 | Fats (Polyunsaturated and Saturated) | 0.81 | ||||||
| Water | 0.29 | 0.44 | Water | ||||||
| Beverages (Noncaloric) | 0.72 | Beverages (Noncaloric) | 0.58 | 0.53 | |||||
| Beverages (Sweetened) | Beverages (Sweetened) | 0.52 | 0.40 | ||||||
| Alcohol | Alcohol | 0.23 | |||||||
| Turkey (N = 31) | |||||||||
| Factor | 1 | 2 | 3 | ||||||
| Eigenvalue | 2.85 | 2.04 | 1.85 | ||||||
| Variance (%) | 23.78 | 17.03 | 15.44 | ||||||
| Fruits | 0.61 | ||||||||
| Vegetables | 0.78 | ||||||||
| Grains, Breads, Starches, Cereals | 0.78 | ||||||||
| Red Meats | 0.87 | ||||||||
| White Meats and Fish | |||||||||
| Legumes and Plant-Based Proteins | 0.69 | ||||||||
| Dairy | 0.82 | ||||||||
| Desserts and Sweets | 0.28 | ||||||||
| Fats (Monounsaturated) | 0.94 | ||||||||
| Fats (Polyunsaturated and Saturated) | 0.87 | ||||||||
| Water | 0.20 | ||||||||
| Beverages (Noncaloric) | |||||||||
| Beverages (Sweetened) | |||||||||
| Alcohol |
| Pattern Label | Most Frequent Food Groups | Country Factor | |||
|---|---|---|---|---|---|
| 1 | 2 | 3 | 4 | ||
| Mediterranean-like | Fruits, Grains, White Meats, Fish, Dairy, Monounsaturated Fats | Poland Slovakia | Argentina | Spain | Serbia Slovenia |
| Calorie Dense | Grains, Starches, Meats, Desserts, Sweets, Fats, Alcohol | Germany USA Spain | Turkey | Slovakia | |
| Vegetarian-Lacto | Fruits, Vegetables, Legumes, Dairy, Desserts, Sweets, Fats, Water | Serbia | Poland Slovenia | Argentina | |
| Vegan | Fruits, Vegetables, Grains, Legumes, Water | Serbia | Germany Slovenia Turkey | ||
| Hearty | Vegetables, Breads, Starches, Red Meats, Dairy | Turkey | Germany | Serbia | |
| Varied | Vegetables, Grains, Breads, Starches, Red Meats, Legumes, Dairy, Fats, Water | Slovenia | Spain | ||
| Vegetarian-Pesco | Fruits, Vegetables, Legumes, Fish, Desserts, Sweets, Fats | Argentina | Poland | ||
| Low Carbohydrate | Fruits, Vegetables, Red or White Meats | USA | Argentina | ||
| High Fat | Red Meats, Legumes, Desserts, Polyunsaturated/Saturated Fats | Spain USA | |||
| Breakfast | Cereals, Grains, Breads, Dairy, Fats | Slovakia | USA | ||
| Bland | White Meats, Fish, Dairy, Polyunsaturated/Saturated Fats | Slovakia | |||
| Score Range | Argentina | Germany | Poland | Serbia | Slovakia | Slovenia | Spain | Turkey | USA | p Value a | |
|---|---|---|---|---|---|---|---|---|---|---|---|
| Adequacy Components b | |||||||||||
| Total Fruits | 0–5 | 2.56 ± 0.03 | 1.48 ± 0.04 | 2.18 ± 0.04 | 2.08 ± 0.04 | 2.19 ± 0.05 | 2.22 ± 0.08 | 3.00 ± 0.06 | 2.74 ± 0.06 | 1.69 ± 0.10 | 0.001 |
| Whole Fruits | 0–5 | 2.49 ± 0.04 | 1.71 ± 0.05 | 3.00 ± 0.05 | 2.67 ± 0.06 | 3.32 ± 0.06 | 3.11 ± 0.10 | 3.81 ± 0.06 | 3.55 ± 0.05 | 1.95 ± 0.12 | 0.001 |
| Total Vegetables | 0–5 | 3.22 ± 0.03 | 2.83 ± 0.04 | 4.14 ± 0.03 | 2.87 ± 0.04 | 3.52 ± 0.05 | 4.28 ± 0.06 | 2.67 ± 0.06 | 4.23 ± 0.04 | 2.95 ± 0.09 | 0.001 |
| Greens and Beans | 0–5 | 0.71 ± 0.03 | 1.29 ± 0.05 | 0.82 ± 0.04 | 0.74 ± 0.05 | 1.32 ± 0.07 | 2.89 ± 0.13 | 1.30 ± 0.08 | 2.68 ± 0.08 | 1.41 ± 0.12 | 0.001 |
| Whole Grains | 0–10 | 1.79 ± 0.05 | 2.21 ± 0.09 | 2.48 ± 0.09 | 2.03 ± 0.10 | 3.71 ± 0.14 | 3.56 ± 0.26 | 2.15 ± 0.14 | 2.77 ± 0.13 | 3.38 ± 0.23 | 0.14 |
| Dairy | 0–10 | 5.62 ± 0.06 | 4.71 ± 0.09 | 4.00 ± 0.08 | 6.67 ± 0.10 | 3.74 ± 0.10 | 5.00 ± 0.21 | 4.89 ± 0.12 | 6.39 ± 0.08 | 4.58 ± 0.19 | 0.001 |
| Total Protein foods | 0–5 | 4.00 ± 0.03 | 3.60 ± 0.04 | 4.64 ± 0.02 | 4.13 ± 0.04 | 4.71 ± 0.03 | 4.61 ± 0.05 | 4.33 ± 0.05 | 3.65 ± 0.06 | 4.52 ± 0.06 | 0.001 |
| Seafood and Plant Proteins | 0–5 | 0.16 ± 0.01 | 0.93 ± 0.04 | 1.70 ± 0.05 | 1.21 ± 0.05 | 1.84 ± 0.08 | 2.61 ± 0.13 | 2.11 ± 0.09 | 2.35 ± 0.07 | 2.33 ± 0.13 | 0.001 |
| Fatty Acids c | 0–10 | 4.19 ± 0.06 | 2.71 ± 0.08 | 3.84 ± 0.08 | 3.97 ± 0.10 | 4.13 ± 0.11 | 6.06 ± 0.19 | 6.44 ± 0.15 | 4.61 ± 0.11 | 4.63 ± 0.20 | 0.005 |
| Moderation Components d | |||||||||||
| Refined Grains | 0–10 | 4.78 ± 0.07 | 5.81 ± 0.09 | 5.09 ± 0.09 | 4.72 ± 0.11 | 7.29 ± 0.11 | 7.61 ± 0.18 | 6.56 ± 0.13 | 5.06 ± 0.13 | 6.15 ± 0.21 | 0.003 |
| Sodium | 0–10 | 4.00 ± 0.06 | 5.07 ± 0.10 | 0.95 ± 0.06 | 2.05 ± 0.07 | 2.03 ± 0.10 | 2.17 ± 0.17 | 3.56 ± 0.13 | 1.74 ± 0.10 | 2.88 ± 0.17 | 0.001 |
| Added Sugars | 0–10 | 6.42 ± 0.19 | 7.63 ± 0.15 | 5.11 ± 0.06 | 5.08 ± 0.10 | 4.57 ± 0.04 | 4.94 ± 0.14 | 5.90 ± 0.12 | 5.95 ± 0.06 | 7.90 ± 0.20 | 0.001 |
| Saturated Fats | 0–10 | 6.38 ± 0.13 | 6.49 ± 0.12 | 6.70 ± 0.14 | 6.38 ± 0.05 | 5.33 ± 0.06 | 5.45 ± 0.09 | 6.21 ± 0.11 | 6.23 ± 0.07 | 6.97 ± 0.16 | 0.002 |
| Total HEI Score | 0–10 | 50.38 ± 0.21 | 47.93 ± 0.31 | 51.80 ± 0.24 | 51.87 ± 0.35 | 56.06 ± 0.33 | 63.78 ± 0.65 | 55.89 ± 0.05 | 58.35 ± 0.37 | 52.21 ± 0.04 | 0.001 |
| Poor Diet Quality | Needs Improvement | Good Diet Quality | |
|---|---|---|---|
| <51 | 51–80 | >80 | |
| (percentage obtaining score) | |||
| Argentina | 42.6 | 55.8 | 1.6 |
| Germany | 62.2 | 37.8 | 0.0 |
| Poland | 43.2 | 56.8 | 0.0 |
| Serbia | 41.7 | 55.5 | 2.8 |
| Slovakia | 26.7 | 73.3 | 0.0 |
| Slovenia | 11.8 | 82.3 | 5.9 |
| Spain | 32.0 | 64.0 | 4.0 |
| Turkey | 27.6 | 69.0 | 3.4 |
| United States | 42.5 | 56.4 | 1.1 |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Willey, J.; Wakefield, M.; Silver, H.J. Exploring the Diets of Adults with Obesity and Type II Diabetes from Nine Diverse Countries: Dietary Intakes, Patterns, and Quality. Nutrients 2020, 12, 2027. https://doi.org/10.3390/nu12072027
Willey J, Wakefield M, Silver HJ. Exploring the Diets of Adults with Obesity and Type II Diabetes from Nine Diverse Countries: Dietary Intakes, Patterns, and Quality. Nutrients. 2020; 12(7):2027. https://doi.org/10.3390/nu12072027
Chicago/Turabian StyleWilley, Jade, Marian Wakefield, and Heidi J. Silver. 2020. "Exploring the Diets of Adults with Obesity and Type II Diabetes from Nine Diverse Countries: Dietary Intakes, Patterns, and Quality" Nutrients 12, no. 7: 2027. https://doi.org/10.3390/nu12072027
APA StyleWilley, J., Wakefield, M., & Silver, H. J. (2020). Exploring the Diets of Adults with Obesity and Type II Diabetes from Nine Diverse Countries: Dietary Intakes, Patterns, and Quality. Nutrients, 12(7), 2027. https://doi.org/10.3390/nu12072027




