Ultra-Processed Foods and Health Outcomes: A Narrative Review
Abstract
1. Introduction
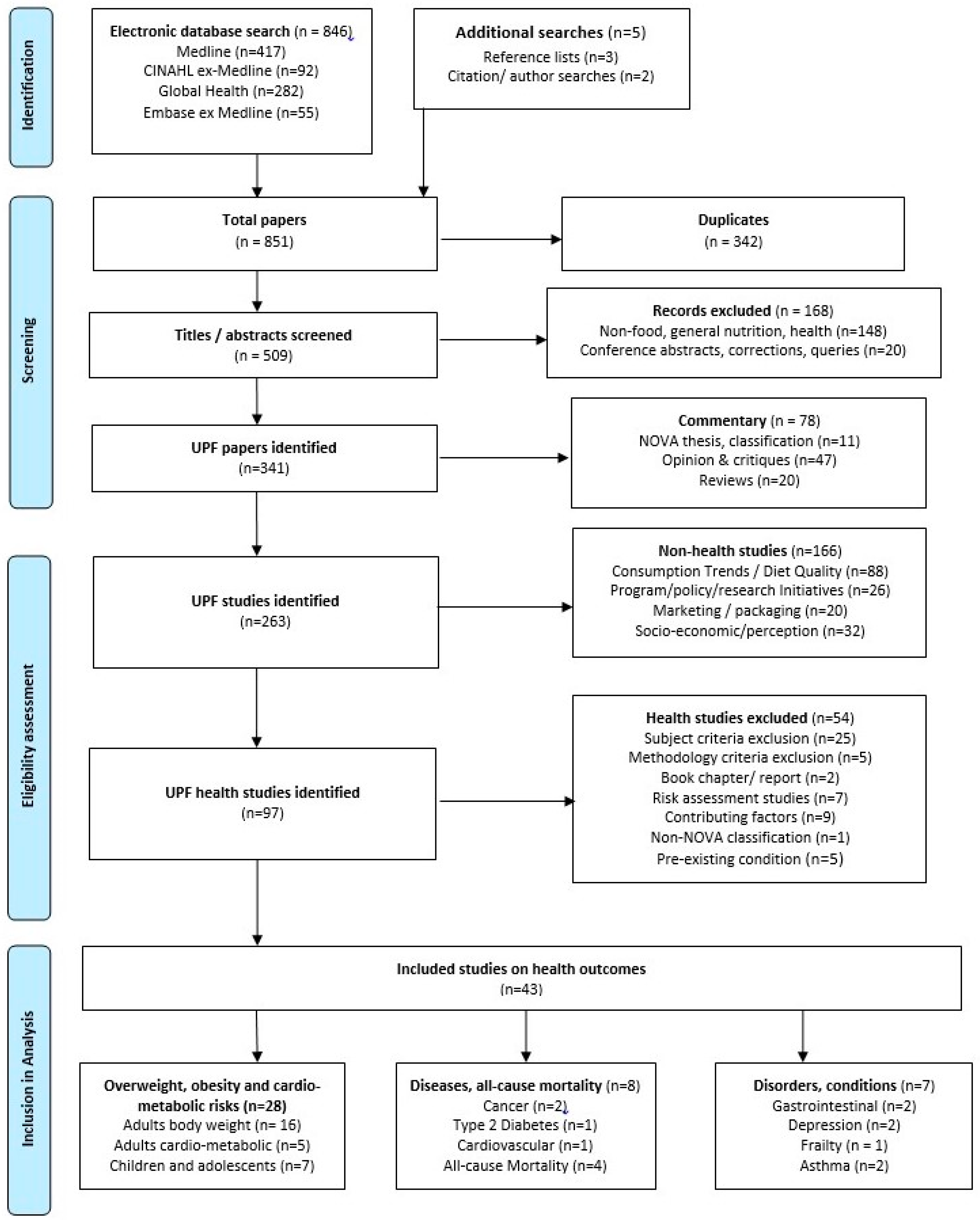
2. Materials and Methods
2.1. Search Process
2.2. Data Extraction, Synthesis, Analysis and Quality Appraisal
| Study Details | UPF Exposure | Outcomes | Results | |||||
|---|---|---|---|---|---|---|---|---|
| Publication Author(s) Year | Study Type (Year) Setting | Population (Number) | Extraction Level | Relative exposure [UPF Reference Year] | Data Collection Method | Health Outcome(s) (Study Definition) | Data Collection Method | Key Findings |
| Overweight and obesity | ||||||||
| Juul 2015 [36] | Ecological (1960–2010) Sweden | Adults ≥18 years (n = −4000 household) | National + household sampling | National: per capita UPF consumption + Household: UPF % share food purchase (kg or litre per capita per annum) [NOVA.2014] [29] | National: Swedish BOA net food ** available Household: 2-week purchase record by interview | BMI classified in prevalence overweight (BMI ≥ 25) and obesity (BMI ≥ 30) | National population statistics | From 1980 to 2008: rise in overweight prevalence for men from 35% to 54–56% and women from 26% to 39%; and obesity prevalence for men rose from 4.5% to 11% and for women from 5% to 10%. From 1960 to 2010 rise in UPF consumption of 142% tracks increase in overweight and obesity prevalence. |
| Monteiro 2017 [52] | Ecological (1991–2008) Europe | Adults ≥ 18 years except Belgium ≥ 15 years (n = 19 countries) | Household (National Sample) | UPF % total E purchases (continuous) [NOVA.2018] [30] | Belgium, Sweden, Germany = one month food ** purchase record; all others = 14 day record g/mL. | BMI classified in prevalence obesity (BMI ≥ 30) | National reports | UPF ranged 10.2–50.7% (median 26.4) of household total E in food purchases. Each 1% increase in UPF E availability was associated with 0.25% increase in obesity prevalence. |
| Vandevijvere 2019 [37] | Ecological (Repeated cross-sectional) (2002–2014) Global | Adults ≥18 years (n = 80 countries) | National | UPF total sales (volume/capita) [NOVA.2018] [30] | Volume sales of UPF (137 items from 212 food ** subgroups) | Mean population BMI | National reports | Increases in UPF volume sales/capita were directly associated with mean BMI trajectories. Every standard deviation increase in volume sales of UPF, mean BMI increased by 0.195 kg/m2 for men and 0.072 kg/m2 for women (drinks only), and 0.316 kg/m2 for men (foods only). |
| Canella 2014 [53] | Cross-sectional (2008–2009) Brazil | All ages (n = 55,970 households; 190,159) individuals) | Household (National Sample) | UPF % total E purchases (quartiles) [NOVA.2012] [54] | 7-day food ** purchase record | BMI classified in excess weight (BMI > 25), obesity (BMI > 30) WHO BMI for age Z scores [children] | Trained personnel | UPF contributed 25.5% of total E purchased. Participants living in household strata belonging to the upper quartile of UPF consumption had higher mean BMI (Z score) (β = 0.19; 95% CI 0.14, 0.25) prevalence of obesity (β = 3.72; 95% CI 2.50, 4.94) and prevalence of excess weight (β = 6.27; 95% CI 4.15, 8.39), compared with those in the lowest quartile. As UPF consumption rose from Quartile 1 to Quartile 4, the prevalence of excess weight rose from 34.1% to 43.9%, and prevalence of obesity rose from 9.8% to 13.1%. |
| Adams 2015 [55] | Cross-sectional (2008–2012) UK | Adults > 18 years (n = 2174) | Individual (National Sample) | UPF % total E intake (continuous) [NOVA.2010] [25] | 4-day food ** intake diary | BMI classified in overweight (BMI ≥ 25); obesity (BMI ≥ 30) | Trained personnel | UPF contributed 53% of total E intake. UPF consumption was not significantly associated with BMI, overweight and obesity, and obesity. |
| Louzada ‡ 2015 [56] | Cross-sectional (2008–2009) Brazil | Adults > 20 years; children > 10 years (n = 30,243) | Individual (National Sample) | UPF % total E intake (quintiles) [NOVA.2012] [54] | 2 × 24-h food ** intake record | BMI classified in excess weight (BMI ≥ 25), obesity (BMI ≥ 30) [adults]; WHO BMI for age Z scores [children] | Trained personnel | UPF contributed to 29.6% of total E intake. Individuals in the upper quintile of UPF intake had significantly higher BMI (0.94 kg/m2; 95% CI = 0.42, 1.47) and higher odds of being obese (OR = 1.98; 95% CI = 1.26, 3.12) compared with the lowest quintile. No significant association with excess weight was found. |
| Nardocci 2018 [57] | Cross-sectional (2004–2005) Canada | Adults > 18 years (19,363) | Individual (National Sample) | UPF % total E intake (quintiles, and continuous) [NOVA2016.2018] [30,58] | 1 × 24-h recall | BMI classified in overweight (25.0 ≤ BMI < 30.0); obesity (BMI ≥ 30) | Trained personnel | UPF contributed 45.1% of total E intake. Individuals in highest quintile UPF intake significantly had higher odds of being obese (OR = 1.32, 95% CI 1.05, 1.57, and overweight (OR = 1.03; 95% CI 1.01, 1.07), compared with individuals in lowest quintile. |
| Juul 2018 [59] | Cross-sectional (2005–2014) USA | Adults 20–64 years (15,977) | Individual (National sample) | UPF % total E intake (quintiles) [NOVA.2014] [29] | 2 available 24-h recall or 1 day otherwise | BMI classified in overweight and obesity (BMI ≥ 25), obesity (BMI ≥ 30); WC classified in abdominal obesity (AO) [men ≥ 102 cm, women ≥ 88 cm) | Trained personnel | UPF contributed 56.1% of total E intake. Individuals in the highest quintile of UPF intake had significantly higher BMI (1.61 kg/m²; 95% CI 1.11, 2.10), and WC (4.07 cm, 95% CI 2.94, 5.19), and higher odds of having excess weight (OR = 1.48; 95% CI 1.25 to 1.76), obesity (OR = 1.53, 95% CI 1.29, 1.81), and abdominal obesity (OR = 1.62; 95% CI 1.39 to 1.89) compared with those in the lowest quintile. |
| Rauber 202 [60] | Cross-sectional (2008–2016) UK | Adults 19−96 years (n = 6143) | Individual (National sample) | UPF % total E intake (quartiles) [NOVA.2019] [21] | 4-day food ** intake diary | BMI classified in obesity (BMI ≥ 30). WC classified in AO | Trained personnel | UPF contributed 54.3% of total E intake. Individuals in the highest quartile of UPF intake had higher BMI (1.66 kg/m2; 95%CI 0.96, 2.36) and WC (3.56cm, 95% CI 1.79, 5.33), and higher odds of obesity (OR = 1.90, 95% CI 1.39, 2.61) compared with the lowest quartile. |
| Julia 2018 [61] | Cross-sectional (2014) France | Adults Mean 43.8 years (n = 74,470) | Individual | UPF % total grams (quartiles) [NOVA.2016] [22,33] | 3 × 24 h records | BMI classified in overweight (25–29.9), obesity (≥30) | Self-report # | UPF contributed 18.4% of total weight intake, and 35.9% of total E intake. Higher consumption of UPF by % E intake was independently associated with overweight (p < 0.0001); and higher intake by energy-weighted UPF was independently associated with overweight, and obesity (both p < 0.0001). |
| Silva 2018 [62] | Cross-sectional (2008–2010) Brazil | Active and retired civil servants 35–64 years (n = 8977) | Individual | UPF % total E intake (quartiles) [NOVA.2016] [22] | 114 item-FFQ | BMI classified in overweight (25.0-29.9); obesity (≥30); WC classified in increased WC (men ≥ 94; women ≥ 80); significantly increased WC (men ≥ 102; women ≥ 88) | Trained personnel | UPF contributed 22.7% of total E intake. Individuals in highest quartile UPF intake had significantly higher BMI (0.80 kg/m2; 95% CI 0.53, 1.07), WC (1.71 cm; 95% CI 1.02, 2.40), and higher odds of being overweight (OR = 1.31; 95% CI 1.13, 1.51), obese (OR = 1.41, 95% CI 1.18, 1.69), increased WC (OR = 1.31, 95% CI 0.96, 1.32), and significantly increased WC (OR = 1.41; 95% CI 1.20, 1.66), compared with individuals in the lowest quartile. |
| Da Silveira 2017 [63] | Cross-sectional (2015) Brazil | Vegetarians > 16 years (n = 503) | Individual | UPF intake frequency (≥3 times per day) [DGB.2014] [28] | FFQ (number of items not specified) | BMI classified in overweight BMI ≥ 25 (16–59 years), BMI ≥ 27 (≥60 years) | Self-report # | Higher intake of UPF (≥3 times/day) was independently associated with overweight (OR = 2.33; 95% CI 1.36, 4.03). |
| Ali 2020 [64] | Cross-sectional (2018) Malaysia | Adults 18–59 years (n = 167) University personnel | Individual | UPF % total E intake (+continuous) [NOVA. 2018] [30] | 2-day 24 h recall | BMI % Body fat | Trained personnel | UPF contributed 23 % of total E intake. No significant findings between ultra-processed food consumption BMI, body fat percent (p = 0.954). |
| Mendonca 2016 [65] | Prospective Cohort (1999–2012) 8.9 years median follow-up Spain | Adults Mean 37.6 years (n = 8451) | Individual | UPF intake servings/day (quartiles) [NOVA.2016] [22] | 136-item FFQ | BMI classified in overweight/obesity (BMI ≥ 25), obesity (BMI ≥ 30). | Self-report # | Participants in the highest quartile of UPF consumption were at a higher risk of developing overweight/obesity (HR = 1.26; 95% CI 1.10, 1.45) compared with those in the lowest quartile of consumption. |
| Canhada 2020 [66] | Prospective Cohort (2008–2010) 3.8 years median follow-up Brazil | Adults 35–74 years (n = 11,827) | Individual | UPF % total E intake (quartiles) [NOVA 2016] [22] | 114-item FFQ | Large weight gain (≥1·68 kg/year) Large WC gain (≥2·42 cm/year) Overweight/obesity (BMI ≥ 25 kg/m2) Obesity (BMI ≥ 30) | Trained personnel | UPF contributed 24.6% of total E intake. Participants in the highest quartile of UPF intake had greater risk of large weight (RR = 1.27; 95% CI 1.07, 1.50) and waist gains (RR = 1.33; 95% CI 1.12, 1.58), and of developing overweight/obesity (RR = 1.20; 95% CI 1.03, 1.40) compared with individuals in the lowest quartile. |
| Hall et al. 2019 [67] | Randomised Controlled Trial (2018, 4 weeks) USA | Weight stable adults Mean 31.2 years (n = 20) | Individual | Whole diet UPF vs. MPF diet (ad libitum) [NOVA.2018] [30] | Diets designed and analysed using ProNutra software | Energy Intake (kcal) Change in body weight (kg) | Trained personnel | Energy intake was greater during exposure to the UPF diet (508 ± 106 kcal/day; p = 0.0001). Participants gained 0.9 ± 0.3 kg (p = 0.009) during the UPF diet, and lost 0.9 ± 0.3 kg (p = 0.007) during the MPF diet. |
| Cardio-metabolic risks | ||||||||
| Lavigne- Robichaud 2017 [68] | Cross-sectional (2005–2009) Canada | Adults ≥ 18 years (n = 811) | Individual | UPF total E % intake (quintiles) [NOVA.2010] [25] | 1 × 24-h food ** recall | Metabolic syndrome (MetS) (≥3 factor: high WC, HT TAG, BG; low HDL-C) | Trained personnel | UPF contributed 51.9% of total E intake. Those in highest quintile of UPF intake significantly associated with higher prevalence of MetS (OR = 1.90; 95% CI 1.14), higher prevalence of reduced HDL-C (OR = 2.05; 95% CI 1.25, 3.38), elevated fasting plasma glucose (OR = 1.76, 95% CI 1.04, 2.97) compared with those in the lowest quintile. |
| Nasreddine 2018 [69] | Cross-sectional (2014) Lebanon | Adults ≥18 years (n = 302) | Individual | UPF ‘pattern’ vs. MPF and PF ‘pattern’ (quartiles) [NOVA.2012] [54] | 88-item FFQ | Metabolic syndrome (≥3 factors: high WC, HT, TAG, BG; low HDL-C) | Trained personnel | UPF vs. MPF were 36.5% vs. 27.1% of total E intake. Those in highest quartile MPF/PF significantly lower odds MetS (OR = 0.18, 95% CI 0.04, 0.77); hyperglycaemia (OR = 0.25, 95% CI 0.07, 0.98), low HDL-C (OR = 0.17, 95% CI 0.05, 0.60) compared with those in the lowest quartile. No significant association between MetS and UPF. |
| Lopes 2019 [70] | Cross-sectional (2008–2010) Brazil | Adults 35–74 years (n = 8468) | Individual | UPF % total E intake (terciles) [NOVA 2016] [22] | 114–item FFQ | C-reactive protein (CRP) level (mg/L) | Trained personnel | UPF contributed to 20% total E intake. Women in highest tercile UPF intake had higher levels of CRP (arithmetic mean = 1.14; 95% CI: 1.04–1.24) than lowest tercile of intake, no significance when controlling for BMI. No significant association was observed in men. |
| Martinez Steele 2019 [71] | Cross-sectional (2009–2014) US | Adults ≥ 20 years (n = 6385) | Individual (National sample) | UPF Total E % intake (quintiles and continuous) [NOVA.2018.2019] [21,30] | 2 available ×24-h recall, or 1 day otherwise. | Metabolic syndrome (≥3 factor of high WC, HT, TAG, BG; low HDL) | Trained personnel | UPF contributed 55.5% of total E intake. The highest quintile of UPF consumption was associated with higher MetS prevalence (PR = 1.28; 95% CI 1.09, 1.50) compared with the lowest quintile of UPF consumption. Each 10% increase in the consumption of UPF was associated with 4% increase in MetS prevalence (PR = 1.04; 95% CI 1.02, 1.07) |
| Mendonca 2017 [72] | Prospective Cohort (1999–2013) 9.1 years median follow-up Spain | Adult graduates (n = 14,790) | Individual | UPF E intake servings per day (tertiles) [NOVA.2016] [22] | 136-item FFQ | Hypertension (BP: Systolic ≥ 140 mm Hg and/or Diastolic ≥ 90 mm Hg) | Self-report ξ | Participants in the highest tertile of UPF intake had higher risk of developing hypertension (HR = 1.21; 95% CI 1.06–1.37) compared with those in the lowest tertile of intake. |
| Study Details | UPF Exposure | Outcomes | Results | |||||
|---|---|---|---|---|---|---|---|---|
| Publication Author(s) Year | Study Type (Year) Setting | Population (Number) | Extraction Level | Relative exposure [UPF Reference Year] | Data Collection Method | Health Outcome (Study Definition) | Data Collection Method | Key Findings |
| Overweight and obesity | ||||||||
| Louzada * 2015 [56] | Cross-sectional (2008-2009) Brazil | Children 10 to 19 years (n = 7534) | Individua (National Sample) | UPF % total E intake (quintiles) [NOVA.2012] [54] | 2 × 24-h food ** intake record | WHO BMI-for-age Z-scores, in excess weight and obesity. | Trained personnel | UPF contribution ranged from ≤17% in lowest quintile to ≥52% in highest quintile. No significant association of UPF intake with mean BMI, excess weight or obesity was found. |
| Enes 2019 [73] | Cross-sectional (2016) Brazil | Adolescents 10–18 years (n = 200) | Individual | UPF % total E intake (quartiles) [NOVA.2018] [30] | 58-items FFQ | Overweight Obesity BMI-for-age Z-scores | Trained personnel | UPF contributed 50.6% of total E intake. No association with UPF and anthropometric indicators. |
| Cunha et al. 2018 [74] | Prospective Cohort (2010–2012), 3 years median follow-up Brazil | Adolescents 15.7 years baseline, 17.6 years follow-up (n = 1035) | Individual | UPF intake (times/day) and daily E (kcal/day) [NOVA.2010] [25] | 72-item FFQ | Trajectories of BMI (kg/m2)% body fat | Trained personnel | Baseline UPF intake was 9.7–12.5 times/day (boys) and 10.9–13.1 times/day (girls). There was no significant difference in BMI and % body fat trajectories during follow-up. |
| Cardio-metabolic risk | ||||||||
| Tavares 2012 [75] | Cross-sectional (2006-2007) Brazil | Adolescents 12–19 years (n = 210) | Individual | UPF E intake (kJ) (quartiles)[NOVA.2009] [9] | 90-item FFQ | Metabolic syndrome (MetS) (≥3 factor of high WC, HT, TAG, BG; low HDL) | Trained personnel (assumed) | Highest intake of UPF (>3rd quartile) was associated with higher MetS prevalence (PR = 2.49; p = 0.012) than the lowest consumption. |
| Melo 2017 [76] | Cross-sectional (2012) Brazil | Adolescents 14–19 years (n = 249) | Individual | UPF intake frequency (<3 per week vs. ≥3 per week) [DGB.2014] [28] | 84- item FFQ | Excess weight (BMI-for-age) High waist circumference High blood pressure | Trained personnel | UPF intake was ≥ 3 × week in 46.2% of adolescents. MPF intake inversely associated with excess weight. UPF intake was not significantly associated with excess weight, high WC and high blood pressure. |
| Rauber 2015 [77] | Prospective cohort (2001–2006) Brazil | Children 3–4 years at baseline; 7–8 years at follow-up (n = 345) | Individual | UPF % total E intake [NOVA.2014] [29,54] | 2 × 24-h recall | Changes in lipid concentrations | Trained personnel | UPF contributed 42.6% at pre-school, 49.2% at school age of % E intake. For every 1% increase E intake from UPF, total cholesterol increased 0.43 mg/dL (p = 0.046), and LDL-C increased 0.369 mg/dL (p = 0.047) from age 3–4 to 7–8 years. |
| Costa 2019 [78] | Prospective Cohort (2001–2006), median follow-up age 4 to 8 years. Brazil | Children 4 years at baseline; 8 years at follow-up (n = 307) | Individual | UPF % total E intake [NOVA.2018] [30] | 2 × 24-h recalls | Changes in BMI (kg/m2), Waist circumference (cm) Glucose profile and insulin resistance | Trained personnel | UPF contributed 41.8% preschool, 47.8% at school age of % E intake. Consumption of UPF consumption at age 4 was associated with increased delta waist circumference (B = 0.07 cm; 95% CI 0.01, 0.013) from age 4 to 8 years. No significant associations were observed for BMI, glucose profile and insulin resistance. |
| Leffa 2020 [79] | Prospective cohort (2011–2015) Brazil | Children 3 years at baseline; 6 years at follow-up (n = 308) | Individual | UPF % total E intake [NOVA.2018.2019] [21,30] | 2 × 24-h recalls | Total cholesterol (TC) TAG | Trained personnel | UPF contributed 43.4% age 3 years, and 47.7% at age 6 years of % E intake. Those children in the highest tertile of consumption of UPF at age 3 had higher levels of TC (B = 0.22 mmol/L; 95 CI 0.04, 0.39) and TAG (B = 0.11 mmol/L; 95% CI 0.01, 0.20) at age 6 than those in the lowest tertile. |
3. Results
3.1. Overveiew of Identified Studies
3.2. Ultra-processed Food Consumption
3.3. Studies Using Overweight, Obesity and Cardio-metabolic Risks as Outcomes (Adults)
3.3.1. Overweight, Obesity and Related Factors
3.3.2. Cardio-Metabolic Risks
3.4. Overweight, Obesity and Cardio-Metabolic Risks as Outcomes (Children and Adolescents)
3.5. Studies Using Diseases and Mortality as Outcomes
3.5.1. Cancer
3.5.2. Cardiovascular Disease
3.5.3. Type 2 Diabetes
3.5.4. Mortality
3.6. Studies Using Other Disorders and Conditions as Outcomes
3.6.1. Gastrointestinal disorders
3.6.2. Depression
3.6.3. Frailty
3.6.4. Asthma
3.7. Quality Appraisal
4. Discussion
4.1. Overweight, Obesity and Cardio-Metabolic Risks as Outcomes (Adults)
4.2. Overweight, Obesity Cardio-Metabolic Risk as Outcomes (Children and Adolescents)
4.3. Diseases and Mortality as Outcomes
4.4. Studies that Investigated Other Disorders and Conditions as Outcomes
4.5. Dietary Assessment, UPF Definitions and Confounding Variables
4.6. Consistency with Findings in Other Reviews and Studies
4.7. Proposed Mechanism of Effects
4.8. Strength and Limitations
4.9. Future Priorities for Nutrition Research and Policy Practice
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Conflicts of Interest
Abbreviations
| BMI | Body Mass Index |
| CRP | C-reactive protein |
| CVD | Cardiovascular disease |
| DALY | Disability life adjusted years |
| FFQ | Food frequency questionnaire |
| GBD | Global burden of disease |
| HDL | High-density lipoprotein cholesterol |
| IBS | Irritable bowel syndrome |
| LDL | Low density lipoprotein cholesterol |
| NCD | Non-communicable disease |
| MPF | Unprocessed and minimally processed foods |
| NHANES | National Health and Nutrition Examination Survey |
| PCI | Processed culinary ingredients |
| PF | Processed foods |
| SSB | Sugar-sweetened beverages |
| UPF | Ultra-processed foods |
| WHO | World Health Organization |
References
- Lawrence, M.A.; Baker, P.I. Ultra-processed food and adverse health outcomes. BMJ 2019, 365, l2289. [Google Scholar] [CrossRef]
- Costa, C.S.; Del-Ponte, B.; Assunção, M.C.F.; Santos, I.S. Consumption of ultra-processed foods and body fat during childhood and adolescence: A systematic review. Public Health Nutr. 2018, 21, 148–159. [Google Scholar] [CrossRef] [PubMed]
- Fardet, A.; Rock, E. Ultra-processed foods: A new holistic paradigm? Trends Food Sci. Technol. 2019, 93, 174–184. [Google Scholar] [CrossRef]
- Poti, J.M.; Braga, B.; Qin, B. Ultra-processed food intake and obesity: What really matters for health-processing or nutrient content? Curr. Obes. Rep. 2017, 6, 420–431. [Google Scholar] [CrossRef]
- Silva Meneguelli, T.; Viana Hinkelmann, J.; Hermsdorff, H.H.M.; Zulet, M.Á.; Martínez, J.A.; Bressan, J. Food consumption by degree of processing and cardiometabolic risk: A systematic review. Int. J. Food Sci. Nutr. 2020, 1–15. [Google Scholar] [CrossRef] [PubMed]
- Pan American Health Organization. Ultra-Processed Food and Drink Products in Latin America: Sales, Sources, Nutrient Profiles, and Policy Implications; PAHO: Washington, DC, USA, 2019; p. 57. [Google Scholar]
- Monteiro, C.; Cannon, G.; Lawrence, M.; Costa Louzada, M.L.; Machado, P.P. Ultra-Processed Foods, Diet Quality, and Health Using the NOVA Classification System; FAO: Rome, Italy, 2019; p. 44. [Google Scholar]
- Monteiro, C.A.; Cannon, G. The role of the transnational ultra-processed food industry in the pandemic of obesity and its associated diseases: Problems and solutions. World Nutr. 2019, 10, 89–99. [Google Scholar] [CrossRef]
- Monteiro, C.A. Nutrition and health. The issue is not food, nor nutrients, so much as processing. Public Health Nutr. 2009, 12, 729–731. [Google Scholar] [CrossRef] [PubMed]
- Afshin, A.; Sur, P.J.; Fay, K.A.; Cornaby, L.; Ferrara, G.; Salama, J.S.; Mullany, E.C.; Abate, K.H.; Abbafati, C.; Abebe, Z.; et al. Health effects of dietary risks in 195 countries, 1990–2017: A systematic analysis for the Global Burden of Disease Study 2017. Lancet 2019, 393, 1958–1972. [Google Scholar] [CrossRef]
- Australian Institute of Health and Welfare. Australian Burden of Disease Study: Impact and Causes of Illness and Death in Australia 2015; Australian Burden of Disease Series no.19, Cat.no. BOD 22; AIHW: Canberra, Australia, 2019.
- Tapsell, L.C.; Neale, E.P.; Satija, A.; Hu, F.B. Foods, nutrients, and dietary patterns: Interconnections and implications for dietary guidelines. Adv. Nutr. 2016, 7, 445–454. [Google Scholar] [CrossRef] [PubMed]
- Mozaffarian, D.; Hao, T.; Rimm, E.B.; Willett, W.C.; Hu, F.B. Changes in diet and lifestyle and long-term weight gain in women and men. N. Engl. J. Med. 2011, 364, 2392–2404. [Google Scholar] [CrossRef]
- Onvani, S.; Haghighatdoost, F.; Surkan, P.J.; Larijani, B.; Azadbakht, L. Adherence to the Healthy Eating Index and Alternative Healthy Eating Index dietary patterns and mortality from all causes, cardiovascular disease and cancer: A meta-analysis of observational studies. J. Hum. Nutr. Diet. 2017, 30, 216–226. [Google Scholar] [CrossRef]
- Hernandez-Ruiz, A.; Garcia-Villanova, B.; Guerra Hernandez, E.J.; Amiano, P.; Azpiri, M.; Molina-Montes, E. Description of indexes based on the adherence to the Mediterranean dietary pattern: A review. Nutr. Hosp. 2015, 32, 1872–1884. [Google Scholar] [CrossRef] [PubMed]
- Salehi-Abargouei, A.; Maghsoudi, Z.; Shirani, F.; Azadbakht, L. Effects of Dietary Approaches to Stop Hypertension (DASH)-style diet on fatal or nonfatal cardiovascular diseases–incidence: A systematic review and meta-analysis on observational prospective studies. Nutrition 2013, 29, 611–618. [Google Scholar] [CrossRef]
- Fung, T.T.; Stampfer, M.J.; Manson, J.E.; Rexrode, K.M.; Willett, W.C.; Hu, F.B. Prospective study of major dietary patterns and stroke risk in women. Stroke 2004, 35, 2014–2019. [Google Scholar] [CrossRef]
- Heidemann, C.; Schulze, M.B.; Franco, O.H.; van Dam, R.M.; Mantzoros, C.S.; Hu, F.B. Dietary patterns and risk of mortality from cardiovascular disease, cancer, and all causes in a prospective cohort of women. Circulation 2008, 118, 230–237. [Google Scholar] [CrossRef] [PubMed]
- Hu, F.B.; Rimm, E.B.; Stampfer, M.J.; Ascherio, A.; Spiegelman, D.; Willett, W.C. Prospective study of major dietary patterns and risk of coronary heart disease in men. Am. J. Clin. Nutr. 2000, 72, 912–921. [Google Scholar] [CrossRef]
- Reedy, J.; Mitrou, P.N.; Krebs-Smith, S.M.; Wirfalt, E.; Flood, A.; Kipnis, V.; Leitzmann, M.; Mouw, T.; Hollenbeck, A.; Schatzkin, A.; et al. Index-based dietary patterns and risk of colorectal cancer: The NIH-AARP Diet and Health Study. Am. J. Epidemiol. 2008, 168, 38–48. [Google Scholar] [CrossRef]
- Monteiro, C.A.; Cannon, G.; Levy, R.B.; Moubarac, J.C.; Louzada, M.L.; Rauber, F.; Khandpur, N.; Cediel, G.; Neri, D.; Martinez-Steele, E.; et al. Ultra-processed foods: What they are and how to identify them. Public Health Nutr. 2019, 22, 936–941. [Google Scholar] [CrossRef] [PubMed]
- Monteiro, C.; Cannon, G.; Levy, R.; Moubarac, J.C.; Jaime, P.; Martins, A.P.; Canella, D.; Louzada, M.L.; Parra, D. NOVA. The star shines bright. Food classification. Public Health. World Nutr. J. 2016, 7, 28–38. [Google Scholar]
- Monteiro, C.A.; Mondini, L.; Costa, R. Secular changes in dietary patterns in the metropolitan areas of Brazil (1988–1996). Rev. Saude Publica 2000, 34, 251–258. [Google Scholar] [CrossRef]
- Levy-Costa, R.B.; Sichieri, R.; Pontes, N.d.S.; Monteiro, C.A. Household food availability in Brazil: Distribution and trends (1974–2003). Rev. Saude Publica 2005, 39, 530–540. [Google Scholar] [CrossRef] [PubMed]
- Monteiro, C.A.; Levy, R.B.; Claro, R.M.; de Castro, I.R.R.; Cannon, G. A new classification of foods based on the extent and purpose of their processing. Cad. Saude Publica 2010, 26, 2039–2049. [Google Scholar] [CrossRef]
- Monteiro, C. The big issue is ultra-processing [Commentary]. World Nutr. J. 2010, 1, 237–269. [Google Scholar]
- Monteiro, C.A.; Levy, R.B.; Claro, R.M.; de Castro, I.R.R.; Cannon, G. Increasing consumption of ultra-processed foods and likely impact on human health: Evidence from Brazil. Public Health Nutr. 2011, 14, 5–13. [Google Scholar] [CrossRef] [PubMed]
- Ministry of Health of Brazil, Secretariat of Health Care, Primary Health Care Department. Dietary Guidelines for the Brazilian Population, 2nd ed.; Ministry of Health Brazil: Brasilia, Brazil, 2014.
- Moubarac, J.C.; Parra, D.C.; Cannon, G.; Monteiro, C.A. Food Classification Systems Based on Food Processing: Significance and Implications for Policies and Actions: A Systematic Literature Review and Assessment. Curr. Obes. Rep. 2014, 3, 256–272. [Google Scholar] [CrossRef] [PubMed]
- Monteiro, C.A.; Cannon, G.; Moubarac, J.C.; Levy, R.B.; Louzada, M.L.C.; Jaime, P.C. The UN Decade of Nutrition, the NOVA food classification and the trouble with ultra-processing. Public Health Nutr. 2018, 21, 5–17. [Google Scholar] [CrossRef]
- Monteiro, C.A.; Moubarac, J.C.; Cannon, G.; Ng, S.W.; Popkin, B. Ultra-processed products are becoming dominant in the global food system. Obes. Rev. 2013, 14 (Suppl. 2), 21–28. [Google Scholar] [CrossRef]
- Machado, P.P.; Steele, E.M.; Levy, R.B.; Sui, Z.; Rangan, A.; Woods, J.; Gill, T.; Scrinis, G.; Monteiro, C.A. Ultra-processed foods and recommended intake levels of nutrients linked to non-communicable diseases in Australia: Evidence from a nationally representative cross-sectional study. BMJ Open 2019, 9, e029544. [Google Scholar] [CrossRef] [PubMed]
- Martínez Steele, E.; Baraldi, L.G.; da Costa Louzada, M.L.; Moubarac, J.C.; Mozaffarian, D.; Monteiro, C.A. Ultra-processed foods and added sugars in the US diet: Evidence from a nationally representative cross-sectional study. BMJ Open 2016, 6, e009892. [Google Scholar] [CrossRef]
- Cediel, G.; Reyes, M.; da Costa Louzada, M.L.; Martinez Steele, E.; Monteiro, C.A.; Corvalán, C.; Uauy, R. Ultra-processed foods and added sugars in the Chilean diet (2010). Public Health Nutr. 2018, 21, 125–133. [Google Scholar] [CrossRef]
- Marrón-Ponce, J.A.; Sánchez-Pimienta, T.G.; da Costa Louzada, M.L.; Batis, C. Energy contribution of NOVA food groups and sociodemographic determinants of ultra-processed food consumption in the Mexican population. Public Health Nutr. 2018, 21, 87–93. [Google Scholar] [CrossRef] [PubMed]
- Juul, F.; Hemmingsson, E. Trends in consumption of ultra-processed foods and obesity in Sweden between 1960 and 2010. Public Health Nutr. 2015, 18, 3096–3107. [Google Scholar] [CrossRef] [PubMed]
- Vandevijvere, S.; Jaacks, L.M.; Monteiro, C.A.; Moubarac, J.C.; Girling-Butcher, M.; Lee, A.C.; Pan, A.; Bentham, J.; Swinburn, B. Global trends in ultraprocessed food and drink product sales and their association with adult body mass index trajectories. Obes. Rev. 2019, 20, 10–19. [Google Scholar] [CrossRef] [PubMed]
- Marrón-Ponce, J.A.; Tolentino-Mayo, L.; Hernández-F, M.; Batis, C. Trends in ultra-processed food purchases from 1984 to 2016 in Mexican households. Nutrients 2018, 11, 45. [Google Scholar] [CrossRef] [PubMed]
- Fardet, A. Characterization of the Degree of Food Processing in Relation with Its Health Potential and Effects. Adv. Food Nutr. Res. 2018, 85, 79–129. [Google Scholar] [CrossRef]
- Grant, M.J.; Booth, A. A typology of reviews: An analysis of 14 review types and associated methodologies. Health Inf. Libr. J. 2009, 26, 91–108. [Google Scholar] [CrossRef]
- Ferrari, R. Writing narrative style literature reviews. Med Writ. 2015, 24, 230–235. [Google Scholar] [CrossRef]
- Academy of Nutrition and Dietetics. Guide for Authors: Narrative Review Checklist. Journal of the Academy of Nutrition and Dietetics. Available online: https://www.elsevier.com/__data/promis_misc/ANDJ%20Narrative%20Review%20Checklist.pdf (accessed on 17 May 2020).
- Liberati, A.; Altman, D.G.; Mulrow, C.; Gotzsche, P.C.; Ioannidis, J.P.A.; Clarke, M.; Devereauz, P.J.; Kleijnen, J.; Moher, D. The PRISMA statment for reporting systematic reviews and meta-analyses of studies that evaluate health care interventions: Explanation and elaboration. Ann. Intern. Med. 2009, 151, W65–W94. [Google Scholar] [CrossRef]
- Moher, D.; Liberati, A.; Tetzlaff, J.; Altman, D.G.; Prisma Group. Preferred reporting items for systematic reviews and meta-analyses: The PRISMA Statement. PLoS Med. 2009, 6, e1000097. [Google Scholar] [CrossRef]
- World Health Organization. International Classification of Diseases, 11th Revision (ICD-11). 2019. Available online: https://icd.who.int/browse11/l-m/en (accessed on 11 June 2019).
- World Health Organization. Physical Status: The Use and Interpretation of Anthropometry: WHO Technical Report Series 854; WHO: Geneva, Switzerland, 1995; p. 463. [Google Scholar]
- World Health Organization. Preventing and Managing the Global Epidemic: Report of a WHO Consultation: WHO Technical Report Series 894; WHO: Geneva, Switzerland, 2000; p. 252. [Google Scholar]
- World Health Organization. Obesity and Overweight. 2020. Available online: https://www.who.int/news-room/fact-sheets/detail/obesity-and-overweight (accessed on 11 May 2020).
- Critical Appraisal Skills Programme. CASP Randomised Controlled Trial Checklist. 2018. Available online: https://casp-uk.net/wp-content/uploads/2018/2001/CASP-Qualitative-Checklist-2018.pdf (accessed on 28 January 2020).
- National Heart Lung and Blood Institute. Quality Assessment Tool for Observational Cohort and Cross-Sectional Studies. 2020. Available online: https://www.nhlbi.nih.gov/health-topics/study-quality-assessment-tools (accessed on 28 January 2020).
- Scottish Intercolleiate Guidelines Network. SIGN Methodology Checklist: Case-Control Studies. 2012. Available online: https://www.sign.ac.uk/checklists-and-notes (accessed on 28 January 2020).
- Monteiro, C.A.; Moubarac, J.-C.; Levy, R.B.; Canella, D.S.; Louzada, M.L.d.C.; Cannon, G. Household availability of ultra-processed foods and obesity in nineteen European countries. Public Health Nutr. 2018, 21, 18–26. [Google Scholar] [CrossRef]
- Canella, D.S.; Levy, R.B.; Martins, A.P.B.; Claro, R.M.; Moubarac, J.-C.; Baraldi, L.G.; Cannon, G.; Monteiro, C.A. Ultra-processed food products and obesity in Brazilian households (2008–2009). PLos ONE 2014, 9, e92752. [Google Scholar] [CrossRef] [PubMed]
- Monteiro, C.A.; Cannon, G.; Levy, R.; Claro, R.; Moubarac, J.-C. The food system. Ultra-processing: The big issue for nutrition, disease, health, well-being. [Commentary]. World Nutr. 2012, 3, 527–569. [Google Scholar]
- Adams, J.; White, M. Characterisation of UK diets according to degree of food processing and associations with socio-demographics and obesity: Cross-sectional analysis of UK National Diet and Nutrition Survey (2008-12). Int. J. Behav. Nutr. Phys. Act. 2015, 12, 160. [Google Scholar] [CrossRef] [PubMed]
- Louzada, M.L.d.C.; Baraldi, L.G.; Steele, E.M.; Martins, A.P.B.; Canella, D.S.; Moubarac, J.-C.; Levy, R.B.; Cannon, G.; Afshin, A.; Imamura, F.; et al. Consumption of ultra-processed foods and obesity in Brazilian adolescents and adults. Prev. Med. 2015, 81, 9–15. [Google Scholar] [CrossRef]
- Nardocci, M.; Leclerc, B.-S.; Louzada, M.-L.; Monteiro, C.A.; Batal, M.; Moubarac, J.-C. Consumption of ultra-processed foods and obesity in Canada. Can. J. Public Health 2019, 110, 4–14. [Google Scholar] [CrossRef]
- Moubarac, J.C.; Batal, M.; da Costa Louzada, M.L.; Martinez Steele, E.; Monteiro, C.A. Consumption of ultra-processed foods predicts diet quality in Canada. Appetite 2017, 108, 512–520. [Google Scholar] [CrossRef]
- Juul, F.; Martinez-Steele, E.; Parekh, N.; Monteiro, C.A.; Chang, V.W. Ultra-processed food consumption and excess weight among US adults. Br. J. Nutr. 2018, 120, 90–100. [Google Scholar] [CrossRef] [PubMed]
- Rauber, F.; Steele, E.M.; Louzada, M.; Millett, C.; Monteiro, C.A.; Levy, R.B. Ultra-processed food consumption and indicators of obesity in the United Kingdom population (2008–2016). PLoS ONE 2020, 15, e0232676. [Google Scholar] [CrossRef]
- Julia, C.; Martinez, L.; Allès, B.; Touvier, M.; Hercberg, S.; Méjean, C.; Kesse-Guyot, E. Contribution of ultra-processed foods in the diet of adults from the French NutriNet-Santé study. Public Health Nutr. 2018, 21, 27–37. [Google Scholar] [CrossRef]
- Silva, F.M.; Giatti, L.; de Figueiredo, R.C.; Molina, M.D.C.B.; de Oliveira Cardoso, L.; Duncan, B.B.; Barreto, S.M. Consumption of ultra-processed food and obesity: Cross sectional results from the Brazilian Longitudinal Study of Adult Health (ELSA-Brasil) cohort (2008–2010). Public Health Nutr. 2018, 21, 2271–2279. [Google Scholar] [CrossRef]
- da Silveira, J.A.C.; Meneses, S.S.; Quintana, P.T.; Santos, V.d.S. Association between overweight and consumption of ultra-processed food and sugar-sweetened beverages among vegetarians. Rev. Nutr. 2017, 30, 431–441. [Google Scholar] [CrossRef]
- Ali, A.; Khasbullah, N.; Ahmad, F.T.; Yosof, H.M. Ultra-processed food consumption in relation to BMI and body fat percentage of adults in Terengganu. Malay J. Med. Health Sci. 2020, 16, 37–43. [Google Scholar]
- de Deus Mendonça, R.; Marçal Pimenta, A.; Gea, A.; Fuente-Arrillaga, C.d.l.; Martinez-Gonzalez, M.A.; Lopes, A.C.S.; Bes-Rastrollo, M. Ultraprocessed food consumption and risk of overweight and obesity: The University of Navarra Follow-Up (SUN) cohort study. Am. J. Clin. Nutr. 2016, 104, 1433–1440. [Google Scholar] [CrossRef] [PubMed]
- Canhada, S.L.; Luft, V.C.; Giatti, L.; Duncan, B.B.; Chor, D.; Fonseca, M.d.J.M.d.; Matos, S.M.A.; Molina, M.D.C.B.; Barreto, S.M.; Levy, R.B.; et al. Ultra-processed foods, incident overweight and obesity, and longitudinal changes in weight and waist circumference: The Brazilian Longitudinal Study of Adult Health (ELSA-Brasil). Public Health Nutr. 2020, 23, 1076–1086. [Google Scholar] [CrossRef] [PubMed]
- Hall, K.; Ayuketah, A.; Brychta, R.; Cai, H.; Cassimatis, T.; Chen, K.Y.; Chung, S.T.; Costa, E.; Courville, A.; Darcey, V.; et al. Ultra-processed diets cause excess calorie intake and weight gain: An inpatient randomized controlled trial of ad libitim food intake. Cell Metab. 2019, 30, 67–77. [Google Scholar] [CrossRef] [PubMed]
- Lavigne-Robichaud, M.; Moubarac, J.C.; Lantagne-Lopez, S.; Johnson-Down, L.; Batal, M.; Laouan Sidi, E.A.; Lucas, M. Diet quality indices in relation to metabolic syndrome in an Indigenous Cree (Eeyouch) population in northern Québec, Canada. Public Health Nutr. 2018, 21, 172–180. [Google Scholar] [CrossRef]
- Nasreddine, L.; Tamim, H.; Itani, L.; Nasrallah, M.P.; Isma’eel, H.; Nakhoul, N.F.; Abou-Rizk, J.; Naja, F. A minimally processed dietary pattern is associated with lower odds of metabolic syndrome among Lebanese adults. Public Health Nutr. 2018, 21, 160–171. [Google Scholar] [CrossRef]
- Lopes, A.E.d.S.C.; Araújo, L.F.; Levy, R.B.; Barreto, S.M.; Giatti, L. Association between consumption of ultra-processed foods and serum C-reactive protein levels: Cross-sectional results from the ELSA-Brasil study. Sao Paulo Med. J. 2019, 137, 169–176. [Google Scholar] [CrossRef]
- Martínez Steele, E.; Juul, F.; Neri, D.; Rauber, F.; Monteiro, C.A. Dietary share of ultra-processed foods and metabolic syndrome in the US adult population. Prev. Med. 2019, 125, 40–48. [Google Scholar] [CrossRef]
- de Deus Mendonça, R.; Souza Lopes, A.C.; Pimenta, A.M.; Gea, A.; Martinez-Gonzalez, M.A.; Bes-Rastrollo, M. Ultra-processed food consumption and the incidence of hypertension in a mediterranean cohort: The seguimiento Universidad de Navarra project. Am. J. Hypertens. 2017, 30, 358–366. [Google Scholar] [CrossRef]
- Enes, C.C.; Camargo, C.M.d.; Justino, M.I.C. Ultra-processed food consumption and obesity in adolescents. Rev. Nutr. 2019, 32. [Google Scholar] [CrossRef]
- Cunha, D.B.; da Costa, T.H.M.; da Veiga, G.V.; Pereira, R.A.; Sichieri, R. Ultra-processed food consumption and adiposity trajectories in a Brazilian cohort of adolescents: ELANA study. Nutr. Diabetes 2018, 8, 1–9. [Google Scholar] [CrossRef] [PubMed]
- Tavares, L.F.; Fonseca, S.C.; Garcia Rosa, M.L.; Yokoo, E.M. Relationship between ultra-processed foods and metabolic syndrome in adolescents from a Brazilian family doctor program. Public Health Nutr. 2012, 15, 82–87. [Google Scholar] [CrossRef] [PubMed]
- de Melo, I.S.V.; Costa, C.A.C.B.; dos Santos, J.V.L.; dos Santos, A.F.; de Menezes Toledo Florêncio, T.M.; Bueno, N.B. Consumption of minimally processed food is inversely associated with excess weight in adolescents living in an underdeveloped city. PLoS ONE 2017, 12, e0188401. [Google Scholar] [CrossRef]
- Rauber, F.; Campagnolo, P.D.; Hoffman, D.J.; Vitolo, M.R. Consumption of ultra-processed food products and its effects on children’s lipid profiles: A longitudinal study. Nutr. Metab. Cardiovasc. Dis. NMCD 2015, 25, 116–122. [Google Scholar] [CrossRef]
- Costa, C.S.; Rauber, F.; Leffa, P.S.; Sangalli, C.N.; Campagnolo, P.D.B.; Vitolo, M.R. Ultra-processed food consumption and its effects on anthropometric and glucose profile: A longitudinal study during childhood. Nutr. Metab. Cardiovasc. Dis. NMCD 2019, 29, 177–184. [Google Scholar] [CrossRef]
- Leffa, P.S.; Hoffman, D.J.; Rauber, F.; Sangalli, C.N.; Valmorbida, J.L.; Vitolo, M.R. Longitudinal associations between ultra-processed foods and blood lipids in childhood. Br. J. Nutr. 2020, 1–8. [Google Scholar] [CrossRef]
- Melo, B.; Rezende, L.; Machado, P.; Gouveia, N.; Levy, R. Associations of ultra-processed food and drink products with asthma and wheezing among Brazilian adolescents. Pediatr. Allergy Immunol. 2018, 29, 504–511. [Google Scholar] [CrossRef]
- Queiroz, S.A.; de Sousa, I.M.; Silva, F.R.M.; Lyra, C.O.; Fayh, A.P.T. Nutritional and environmental risk factors for breast cancer: A case-control study. Sci. Med. 2018, 28, 1–8. [Google Scholar] [CrossRef]
- Machado Azeredo, C.; Cortese, M.; Costa, C.D.S.; Bjornevik, K.; Barros, A.J.D.; Barros, F.C.; Santos, I.S.; Matijasevich, A. Ultra-processed food consumption during childhood and asthma in adolescence: Data from the 2004 Pelotas birth cohort study. Pediatr. Allergy Immunol. 2020, 31, 27–37. [Google Scholar] [CrossRef]
- Srour, B.; Fezeu, L.K.; Kesse-Guyot, E.; Alles, B.; Mejean, C.; Andrianasolo, R.M.; Chazelas, E.; Deschasaux, M.; Hercberg, S.; Galan, P.; et al. Ultra-processed food intake and risk of cardiovascular disease: Prospective cohort study (NutrNet-Sante). BMJ 2019, 365, l1451. [Google Scholar] [CrossRef] [PubMed]
- Fiolet, T.; Srour, B.; Sellem, L.; Kesse-Guyot, E.; Allès, B.; Méjean, C.; Deschasaux, M.; Fassier, P.; Latino-Martel, P.; Beslay, M.; et al. Consumption of ultra-processed foods and cancer risk: Results from NutriNet-Santé prospective cohort. BMJ 2018, 360, k322. [Google Scholar] [CrossRef]
- Schnabel, L.; Buscail, C.; Sabate, J.-M.; Bouchoucha, M.; Kesse-Guyot, E.; Allès, B.; Touvier, M.; Monteiro, C.A.; Hercberg, S.; Benamouzig, R.; et al. Association between ultra-processed food consumption and functional gastrointestinal disorders: Results from the French NutriNet-Santé cohort. Am. J. Gastroenterol. 2018, 113, 1217–1228. [Google Scholar] [CrossRef]
- Schnabel, L.; Kesse-Guyot, E.; Allès, B.; Touvier, M.; Srour, B.; Hercberg, S.; Buscail, C.; Julia, C. Association between ultraprocessed food consumption and risk of mortality among middle-aged adults in France. JAMA Int. Med. 2019, 179, 490–498. [Google Scholar] [CrossRef]
- Srour, B.; Fezeu, L.K.; Kesse-Guyot, E.; Allès, B.; Debras, C.; Druesne-Pecollo, N.; Chazelas, E.; Deschasaux, M.; Hercberg, S.; Galan, P.; et al. Ultraprocessed food consumption and risk of type 2 diabetes among participants of the NutriNet-Santé prospective cohort. JAMA Int. Med. 2019, 180, 283–291. [Google Scholar] [CrossRef]
- Vasseur, P.; Dugelay, E.; Benamouzig, R.; Savoye, G.; Lan, A.; Srour, B.; Hercberg, S.; Touvier, M.; Hugot, J.-P.; Julia, C.; et al. Dietary patterns, ultra-processed food, and the risk of inflammatory bowel diseases in the NutriNet-Santé Cohort. Inflamm. Bowel Dis. 2020. [Google Scholar] [CrossRef]
- Adjibade, M.; Julia, C.; Allès, B.; Touvier, M.; Lemogne, C.; Srour, B.; Hercberg, S.; Galan, P.; Assmann, K.E.; Kesse-Guyot, E. Prospective association between ultra-processed food consumption and incident depressive symptoms in the French NutriNet-Santé cohort. BMC Med. 2019, 17, 78. [Google Scholar] [CrossRef]
- Gómez-Donoso, C.; Sánchez-Villegas, A.; Martínez-González, M.A.; Gea, A.; Mendonça, R.d.D.; Lahortiga-Ramos, F.; Bes-Rastrollo, M. Ultra-processed food consumption and the incidence of depression in a Mediterranean cohort: The SUN project. Eur. J. Nutr. 2019, 59, 1093–1103. [Google Scholar] [CrossRef]
- Rico-Campa, A.; Martinez-Gonzalez, M.A.; Alvarez-Alvarez, I.; de Deus Mendonca, R.; Fuente-Arrillaga, C.d.l.; Gomez-Donoso, C. Association between consumption of ultraprocessed foods and all cause mortality: SUN prospective cohort study. BMJ 2019, 365, 1949. [Google Scholar] [CrossRef]
- Blanco-Rojo, R.; Sandoval-Insausti, H.; López-Garcia, E.; Graciani, A.; Ordovás, J.M.; Banegas, J.R.; Rodríguez-Artalejo, F.; Guallar-Castillón, P. Consumption of ultra-processed foods and mortality: A national prospective cohort in Spain. Mayo Clin. Proc. 2019, 94, 2178–2188. [Google Scholar] [CrossRef]
- Sandoval-Insausti, H.; Blanco-Rojo, R.; Graciani, A.; Lopez-Garcia, E.; Moreno-Franco, B.; Laclaustra, M.; Donat-Vargas, C.; Ordovas, J.M.; Rodriguez-Artalejo, F.; Guallar-Castillón, P. Ultra-processed food consumption and incident frailty: A prospective cohort study of older adults. J. Gerontol. Ser. A Biol. Sci. Med. Sci. 2019, 75, 1126–1133. [Google Scholar] [CrossRef]
- Kim, H.; Hu, E.A.; Rebholz, C.M. Ultra-processed food intake and mortality in the USA: Results from the third National Health and Nutrition Examination Survey (NHANES III, 1988–1994). Public Health Nutr. 2019, 22, 1777–1785. [Google Scholar] [CrossRef]
- Mendonca, R.D.; Pimenta, A.M.; Gea, A.; de la Fuente-Arrillaga, C.; Martinez-Gonzalez, M.A.; Lopes, A.C.S.; Bes-Rastrollo, M. Reply to T Bhurosy et al. Am. J. Clin. Nutr. 2017, 105, 1012–1013. [Google Scholar] [CrossRef]
- Mendonca, R.D.; Pimenta, A.M.; Gea, A.; de la Fuente-Arrillaga, C.; Martinez-Gonzalez, M.A.; Lopes, A.C.S.; Bes-Rastrollo, M. Reply to JM Cullin and CI Fernández. Am. J. Clin. Nutr. 2017, 105, 1013–1014. [Google Scholar] [CrossRef][Green Version]
- Cannon, C.P. Cardiovascular disease and modifiable cardiometabolic risk factors. Clin. Cornerstone 2007, 8, 11–28. [Google Scholar] [CrossRef]
- Zinöcker, M.K.; Lindseth, I.A. The Western diet-microbiome-host interaction and its role in metabolic disease. Nutrients 2018, 10, 365. [Google Scholar] [CrossRef]
- Strasser, B. Immune-mediated inflammation as a driver of obesity and comorbid conditions. Obesity 2017, 25, 987–988. [Google Scholar] [CrossRef]
- Stecher, B. The role of inflammation, nutrient availability and the commensal microbiota in enteric pathogen infection. Microbiol. Spectr. 2015, 3. [Google Scholar] [CrossRef]
- Ogata, B.N.; Hayes, D. Position of the Academy of Nutrition and Dietetics: Nutrition guidance for healthy children ages 2 to 11 years. J. Acad. Nutr. Diet. 2014, 114, 1257–1276. [Google Scholar] [CrossRef]
- Veronese, N.; Sigeirsdottir, K.; Eiriksdottir, G.; Marques, E.A.; Chalhoub, D.; Phillips, C.L.; Launer, L.J.; Maggi, S.; Gudnason, V.; Harris, T.B. Frailty and risk of cardiovascular diseases in older persons: The age, gene/environment susceptibility-Reykjavik Study. Rejuvenation Res. 2017, 20, 517–524. [Google Scholar] [CrossRef]
- Shim, J.S.; Oh, K.; Kim, H.C. Dietary assessment methods in epidemiologic studies. Epidemiol. Health 2014, 36, e2014009. [Google Scholar] [CrossRef]
- Martínez, S.E.; Popkin, B.M.; Swinburn, B.; Monteiro, C.A. The share of ultra-processed foods and the overall nutritional quality of diets in the US: Evidence from a nationally representative cross-sectional study. Popul. Health Metr. 2017, 15, 6. [Google Scholar] [CrossRef] [PubMed]
- FAO. Guidelines on the Collection of Information on Food Processing through Food Consumption Surveys; FAO: Rome, Italy, 2015. [Google Scholar]
- Leme, A.C.B.; Fisberg, R.M.; Thompson, D.; Philippi, S.T.; Nicklas, T.; Baranowski, T. Brazilian children’s dietary intake in relation to Brazil’s new nutrition guidelines: A systematic review. Curr. Nutr. Rep. 2019, 8, 145–166. [Google Scholar] [CrossRef] [PubMed]
- Kimenju, S.C. Ultra-Processed Foods and Obesity in Central Kenya. In Advances in Food Security and Sustainability; Barling, D., Fanzo, J., Eds.; Academic Press: Cambridge, MA, USA; Elsevier: New York, NY, USA, 2018; Volume 3, pp. 69–92. [Google Scholar]
- Bielemann, R.M.; Motta, J.V.S.; Minten, G.C.; Horta, B.L.; Gigante, D.P. Consumption of ultra-processed foods and their impact on the diet of young adults. Rev. Saude Publica 2015, 49, 28. [Google Scholar] [CrossRef] [PubMed]
- Latasa, P.; da Coasta Louzada, M.L.; Martinez Steele, E.; Monteiro, C.A. Added sugars and ultra-processed foods in Spanish households (1990–2010). Eur. J. Clin. Nutr. 2018, 72, 1404–1412. [Google Scholar] [CrossRef]
- Vandevijvere, S.; De Ridder, K.; Fiolet, T.; Bel, S.; Tafforeau, J. Consumption of ultra-processed food products and diet quality among children, adolescents and adults in Belgium. Eur. J. Nutr. 2018, 58, 3267–3278. [Google Scholar] [CrossRef]
- Martínez Steele, E.; Monteiro, C.A. Association between dietary share of ultra-processed foods and urinary concentrations of phytoestrogens in the US. Nutrients 2017, 9, 209. [Google Scholar] [CrossRef]
- Luiten, C.M.; Steenhuis, I.H.; Eyles, H.; Ni Mhurchu, C.; Waterlander, W.E. Ultra-processed foods have the worst nutrient profile, yet they are the most available packaged products in a sample of New Zealand supermarkets. Public Health Nutr. 2016, 19, 530–538. [Google Scholar] [CrossRef]
- Ni Mhurchu, C.; Brown, R.; Jiang, Y.; Eyles, H.; Dunford, E.; Neal, B. Nutrient profile of 23,596 packaged supermarket foods and non-alcoholic beverages in Australia and New Zealand. Public Health Nutr. 2016, 19, 401–408. [Google Scholar] [CrossRef]
- Poti, J.; Mendez, M.; Ng, S.; Popkin, B. Is the degree of food processing and convenience linked with the nutritional quality of foods purchased by US households? Am. J. Clin. Nutr. 2015, 101, 1251–1262. [Google Scholar] [CrossRef]
- Fardet, A. Minimally processed foods are more satiating and less hyperglycemic than ultra-processed foods: A preliminary study with 98 ready-to-eat foods. Food Funct. 2016, 7, 2338–2346. [Google Scholar] [CrossRef]
- Fardet, A.; Méjean, C.; Labouré, H.; Andreeva, V.A.; Feron, G. The degree of processing of foods which are most widely consumed by the French elderly population is associated with satiety and glycemic potentials and nutrient profiles. Food Funct. 2017, 8, 651–658. [Google Scholar] [CrossRef] [PubMed]
- De Graaf, C.; Kok, F.J. Slow food, fast food and the control of food intake. Nat. Rev. Endocrinol. 2010, 6, 290–293. [Google Scholar] [CrossRef] [PubMed]
- Small, D.; DiFeliceantonio, A. Processed foods and food reward. Science 2019, 363, 346–347. [Google Scholar] [CrossRef]
- European Food Safety Authority. EEFS Panel on Contaminants in the Food Chain (CONTAM). Scientific opinion on acrylamide in food. EFSA J. 2015, 13, 4104. [Google Scholar] [CrossRef]
- Gibis, M. Heterocyclic aromatic amines in cooked meat products: Causes, formation, occurrence, and risk assessment. Compr. Rev. Food Sci. Food Saf. 2016, 15, 269–302. [Google Scholar] [CrossRef]
- Lerner, A.; Matthias, T. Changes in intestinal tight junction permeability associated with industrial food additives explain the rising incidence of autoimmune disease. Autoimmun. Rev. 2015, 14, 479–489. [Google Scholar] [CrossRef] [PubMed]
- Miclotte, L.; Van de Wiele, T. Food processing, gut microbiota and the globesity problem. Crit. Rev. Food Sci. Nutr. 2019, 1–14. [Google Scholar] [CrossRef]
- Ayton, A.; Ibrahim, A. The Western diet: A blind spot of eating disorder research?– A narrative review and recommendations for treatment and research. Nutr. Rev. 2019. [Google Scholar] [CrossRef]
- Alexy, U.; Sichert-Hellert, W.; Rode, T.; Kersting, M. Convenience food in the diet of children and adolescents: Consumption and composition. Br. J. Nutr. 2008, 99, 345–351. [Google Scholar] [CrossRef][Green Version]
- Bellisle, F. Meals and snacking, diet quality and energy balance. Physiol. Behav. 2014, 134, 38–43. [Google Scholar] [CrossRef] [PubMed]
- Peltner, J.; Thiele, S. Convenience-based food purchase patterns: Identification and associations with dietary quality, sociodemographic factors and attitudes. Public Health Nutr. 2018, 21, 558–570. [Google Scholar] [CrossRef] [PubMed]
- Gordon, E.L.; Ariel-Donges, A.H.; Bauman, V.; Merlo, L.J. What is the evidence for “food addiction”? A systematic review. Nutrients 2018, 10, 477. [Google Scholar] [CrossRef] [PubMed]
- Filgueiras, A.R.; Pires de Almeida, V.B.; Koch Nogueira, P.C.; Alvares Domene, S.M.; Eduardo da Silva, C.; Sesso, R.; Sawaya, A.L. Exploring the consumption of ultra-processed foods and its association with food addiction in overweight children. Appetite 2019, 135, 137–145. [Google Scholar] [CrossRef]
- Lobstein, T.; Dibb, S. Evidence of a possible link between obesogenic food advertising and child overweight. Obes. Rev. 2005, 6, 203–208. [Google Scholar] [CrossRef]
- Mallarino, C.; Gómez, L.F.; González-Zapata, L.; Cadena, Y.; Parra, D.C. Advertising of ultra-processed foods and beverages: Children as a vulnerable population. Revista Saúde Pública 2013, 47, 1006–1010. [Google Scholar] [CrossRef]
- Pulker, C.E.; Scott, J.A.; Pollard, C.M. Ultra-processed family foods in Australia: Nutrition claims, health claims and marketing techniques. Public Health Nutr. 2018, 21, 38–48. [Google Scholar] [CrossRef]
- Gibney, M.J. Ultra-processed foods: Definitions and policy issues. Curr. Dev. Nutr. 2018, 3, nzy077. [Google Scholar] [CrossRef]
- Gibney, M.J. Ultraprocessed foods and their application to nutrition policy. Nutr. Today 2020, 55, 16–21. [Google Scholar] [CrossRef]
- Djupegot, I.L.; Nenseth, C.B.; Bere, E.; Bjørnarå, H.B.T.; Helland, S.H.; Øverby, N.C.; Torstveit, M.K.; Stea, T.H. The association between time scarcity, sociodemographic correlates and consumption of ultra-processed foods among parents in Norway: A cross-sectional study. BMC Public Health 2017, 17, 447. [Google Scholar] [CrossRef]
- Vale, D.; Morais, C.M.M.d.; Pedrosa, L.d.F.C.; Ferreira, M.Â.F.; Oliveira, Â.G.R.d.C.; Lyra, C.d.O. Spatial correlation between excess weight, purchase of ultra-processed foods, and human development in Brazil. Ciência Saúde Coletiva 2019, 24, 983–996. [Google Scholar] [CrossRef]
| Description | |
|---|---|
| Inclusion criteria |
|
| Exclusion criteria |
|
| Study Details | UPF Exposure | Outcomes | Results | |||||
|---|---|---|---|---|---|---|---|---|
| Publication Author(s) Year | Study Type (Year) Setting | Population (Number) | Extraction Level | Relative exposure [UPF reference year] | Data Collection Method | Health Outcome | Data Collection Method | Key Findings |
| Cancer | ||||||||
| Queiroz 2018 [81] | Case control study (2015) Brazil | Adult women Mean 53.1 years (n = 118) | Individual | UPF ≥ 5 day/week {NOVA.2010] [25] | 98-item FFQ, 12-month recall | Breast cancer (BC) | Diagnosed BC | Regular consumption UPF (≥5 day/week) identified as risk factors for BC (OR = 2.35, 95% CI 1.08–5.12). |
| Fiolet 2018 [84] | Prospective Cohort (2017), 5 years median follow-up France | Adults ≥ 18 years Mean 42.8 (n = 104,980) | Individual | UPF % g (quartiles) [NOVA 2018] [30] | 3 × 24-h records | Overall, breast, prostate, and colorectal cancer | Self-report or/physician contact | UPF contribution in proportion of grams ranged from 18.7% lowest quartile to 32.3% in highest. A 10% increase in proportion of UPF consumption associated with a significant increase in overall (HR = 1.12; 95% CI 1.06; 1.18; p for trend <0.001) and BC risk (HR = 1.11; 95% CI 1.02; 1.22, P trend = 0.02). No significant associations were found for prostate and colorectal cancers (p = 0.8 and p = 0.2, respectively). |
| Cardiovascular disease (CVD) | ||||||||
| Srour 2019 [83] | Prospective cohort (2019), 5.2 years median follow-up France | Adults ≥18 years (n = 105,109) | Individual | UPF % grams (quartiles) [NOVA.2018] [30] | 3 × 24 h records | Cardiovascular (CVD), coronary heart (CHD), cerebrovascular disease | Medical records, committee of doctors | UPF contribution averaged 17. 4% of total grams. A 10% increase in proportion of UPF consumption was associated with significant higher risk of overall CVD (HR = 1.12; 95% CI 1.05; −1.20, p < 0.001); CHD (HR = 1.13; 95% CI 1.10; −1.24, p = 0.02); and cerebrovascular disease (HR = 1.11; 95% CI 1.01–1.21; p = 0.02). |
| Type 2 Diabetes (T2D) | ||||||||
| Srour 2019 [87] | Prospective cohort (2017), 6.0 years median follow-up France | Adults ≥ 18 Mean 42.7 years (n = 104,707) | Individual | UPF % g [NOVA.2018] [30] | 3 × 24 h records | Type 2 Diabetes (T2D) | ICD-10 code or T2D medication | Mean UPF contribution was 17.3% by weight, and 29.95% by % E intake. A 10% increase in the proportion of UPF consumption was associated with a significant higher risk of T2D (HR = 1.15; 95% CI 1.06; 1.25; p = 0.001). |
| Mortality | ||||||||
| Kim 2019 [94] | Prospective cohort (2011), 19 years median follow-up USA | Adults ≥20 years (n = 11,898) | Individual | UPF frequency (times/day) (quartiles) [NOVA.2018] [30] | 81-item FFQ, and 24-h recall | All-cause mortality (ACM) CVD mortality | National death index. CVD items 100–169 ICD-10 | Participants consumed UPF a mean 4 times/day. Individuals in the highest quartile of frequency of UPF consumption had significantly higher risk of ACM, (HR = 1.31; 95% CI 1.09; 1.58, p-trend = 0.001). No significant association was observed with CVD mortality. |
| Schnabel 2019 [86] | Prospective Cohort (2017), (median follow-up 7.1 years) France | Adults ≥ 45 years (n = 44,551) | Individual | UPF % g [NOVA 2018] [30] | 3 × 24-h food record | ACM | National death registries. Causes by ICD-10 | UPF contributed 14.4% total weight, and 29.9% total E intake. A 10% increase in the proportion of UPF consumption was associated with a significant higher risk of ACM 1.14 (95% CI, 1.04–1.27; p = 0.008). |
| Rico-Campà 2019 [91] | Prospective Cohort (2014), (median follow-up 10.4 years) Spain | Adults 20−91 years (n = 19,899) | Individual | UPF servings/day (quartiles) [NOVA.2016] [22] | 136-item FFQ | ACM CVD mortality Cancer mortality | Next of kin/Registries | UPF consumption ranged from 1.4 servings a day in lowest quintile to 5.3 servings a day in highest quintile. Individuals in the highest quartile of UPF consumption were at higher risk of ACM (HR = 1.62; 95% CI 1.13; 2.33) than those in the lowest quartile. No significant associations were found for cardiovascular and cancer mortality. |
| Blanco-Rojo 2019 [92] | Prospective Cohort (2016), (mean follow-up 7.7 years) Spain | Adults Mean 46.9 years (n = 11,898) | Individual | UPF % total E intake (quartiles) [NOVA.2018] [30] | 880-item FFQ | ACM | National Death Index | UPF contributed 24.4% total E intake. Individuals in the highest quartile of UPF consumption were at higher risk of ACM (HR = 1.46; 95% CI 1.04-2.05; P trend = 0.03), than those in the lowest quartile. |
| Study Details | UPF Exposure | Outcomes | Results | |||||
|---|---|---|---|---|---|---|---|---|
| Publication Author(s) Year | Study Type (Year) Setting | Population (Number) | Extraction Level | Relative exposure [UPF Reference Year] | Data Collection Method | Health Outcome (Study Definition) | Data Collection Method | Key Findings |
| Gastrointestinal Disease | ||||||||
| Schnabel 2018 [85] | Cross-sectional (2013) France | Age ≥ 18 years (mean 50.4) (n = 33,343) | Individual | UPF % total grams (quartiles) [NOVA.2018] [30] | 3 × 24-h records | Functional gastrointestinal disorders (Rome III criteria) | Self-report * | UPF contributed to 16% of total food intake by weight; 33.0% by total E intake. Individuals in the highest quartile of UPF intake had significantly higher risk of IBS (OR = 1.25; 95% CI 1.12; 1.39) and FDy (OR = 1.25; CI 95% 1.05; 1.47) but not FDy alone, compared with those in the lowest quartile. |
| Vasseur 2020 [88] | Prospective cohort (2016) 2.3 years mean follow-up France | Adults ≥ 18 years (mean 43.3) (n = 105,832) | Individual | UPF % total grams (tertiles) [NOVA.2018] [30] | 3 × 24 h records | Inflammatory bowel disease | Self-report ** | UPF contributed 17% food intake by weight in grams. No significant association was found with UPF consumption and IBD (p = 0.03). |
| Depression | ||||||||
| Adjibade 2019 [89] | Prospective Cohort (2012), 5.4 years mean follow-up France | Adults age 18–86 years (n= 26,730) | Individual | UPF % total grams (quartiles) [NOVA.2018] [30] | 3 × 24 h records | Depression (CES-D scale) | Self-report * | UPF contributed 5% by weight in grams and 32% E intake. Individuals in the highest quartile of UPF intake had significantly higher risk of developing depressive symptoms (HR = 1.30; 95% CI 1.15–1.47) than those in the lowest quartile. Each 10% increase in UPF consumption was HR of 1.21 (95% CI, 1.15–1.27). |
| Gomez-Donoso, 2019 [90] | Prospective cohort (2016), 10.3 years median follow-up Spain | Adults (mean 36.7 years) (n = 14,907) | Individual | UPF energy adjusted kcal/day (quartiles) [NOVA.2016] [22] | 136–item FFQ | Depression | Self-report ** | Individuals in highest quartile UPF had significantly higher risk of depression (HR = 1.33; 95% CI 1.07–1.64); p trend = 0.004), than individuals in lowest quartile of consumption, after confounder adjustment. |
| Frailty | ||||||||
| Sandoval-Insausti 2019 [93] | Prospective Cohort (2008–2010), 3.5 years median follow-up Spain | Adults ≥ 60 years (N = 1822) | Individual | UPF intake % total E (quartiles) [NOVA2018] [30] | Validated interview computerized diet history | Frailty (Fried’s criteria) | Trained personnel | UPF contributed mean of 19.3% total E intake. Individuals in the highest quartile of UPF intake had higher risk of frailty (OR = 3.67; 95% CI 2.00, 6.76) than those in the lowest quartile of intake. |
| Asthma (children and adolescents) | ||||||||
| Melo et al. 2018 [80] | Cross-sectional (2012) Brazil | Grade 9 students (n = 109,104) | Individual | UPF score, intake per week (quintiles) [NOVA 2018] [30] | 6-UPF sub-categories FFQ | Asthma, wheezing in past 12 months | Self-report * | Individuals in the highest quintile of the UPF intake score had higher odds of having asthma (OR = 1.27; 95% CI 1.15, 1.41) or wheezing (OR = 1.42; 95% CI 1.35 to 1.50), than those in the lowest quintile. |
| Azeredo 2020 [82] | Prospective Cohort (2004–2010) Brazil | Children mean age 6.8 years baseline; 11.0 years at follow-up (n = 2190) | Individual | UPF % total E intake (quintiles) [NOVA.2018] [30] | 55 (age 6) and 88 items (age 11) FFQ. | Wheezing, whistling or asthma in past 12 months | Self-report * | UPF contribution to total E intake was 42.3% at 6 years, and 33.7% at 11 years. Consumption of UPF at age 6 was not significantly associated with wheeze, asthma or severe asthma at age 11. |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Elizabeth, L.; Machado, P.; Zinöcker, M.; Baker, P.; Lawrence, M. Ultra-Processed Foods and Health Outcomes: A Narrative Review. Nutrients 2020, 12, 1955. https://doi.org/10.3390/nu12071955
Elizabeth L, Machado P, Zinöcker M, Baker P, Lawrence M. Ultra-Processed Foods and Health Outcomes: A Narrative Review. Nutrients. 2020; 12(7):1955. https://doi.org/10.3390/nu12071955
Chicago/Turabian StyleElizabeth, Leonie, Priscila Machado, Marit Zinöcker, Phillip Baker, and Mark Lawrence. 2020. "Ultra-Processed Foods and Health Outcomes: A Narrative Review" Nutrients 12, no. 7: 1955. https://doi.org/10.3390/nu12071955
APA StyleElizabeth, L., Machado, P., Zinöcker, M., Baker, P., & Lawrence, M. (2020). Ultra-Processed Foods and Health Outcomes: A Narrative Review. Nutrients, 12(7), 1955. https://doi.org/10.3390/nu12071955





