Low Vitamin B12 and Lipid Metabolism: Evidence from Pre-Clinical and Clinical Studies
Abstract
1. Introduction
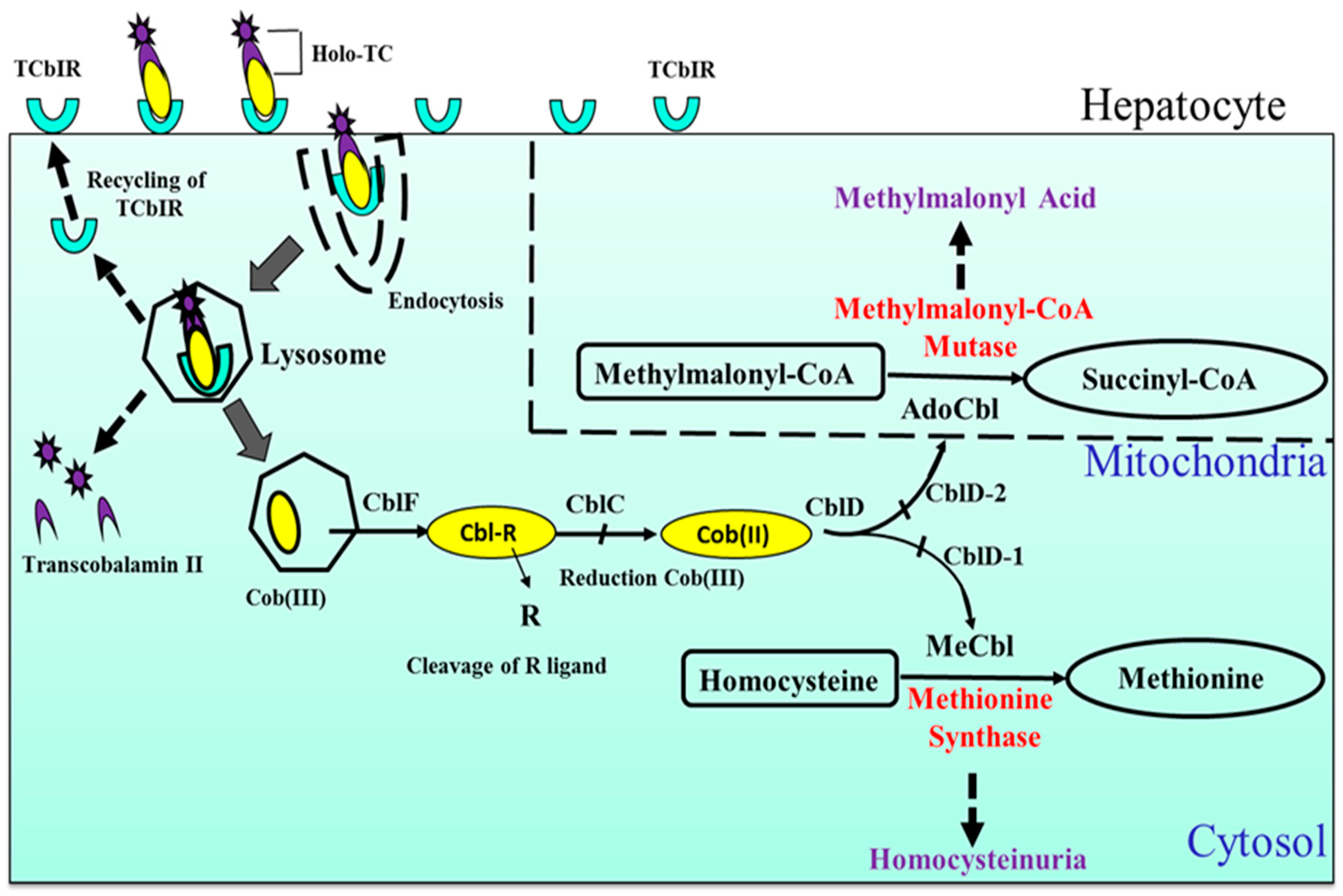
2. B12: Biochemical Structure, Sources, Bioavailability, Cellular Uptake and Metabolism
3. Vitamin B12 Deficiency: Diagnostic Markers and Risk Factors
4. Association of Low B12 with Cardiometabolic Risk
4.1. Evidence from Pre-Clinical Studies
4.1.1. Vitamin B12 and Obesity
4.1.2. Vitamin B12 and Insulin Resistance
4.1.3. Vitamin B12 and Dyslipidemia
4.1.4. Vitamin B12 and Cardiovascular Diseases
4.2. Evidence from Clinical Studies
4.2.1. Vitamin B12 and Obesity
4.2.2. Vitamin B12 and Insulin Resistance
4.2.3. Vitamin B12 and Dyslipidemia
4.2.4. Vitamin B12 and Cardiovascular Diseases
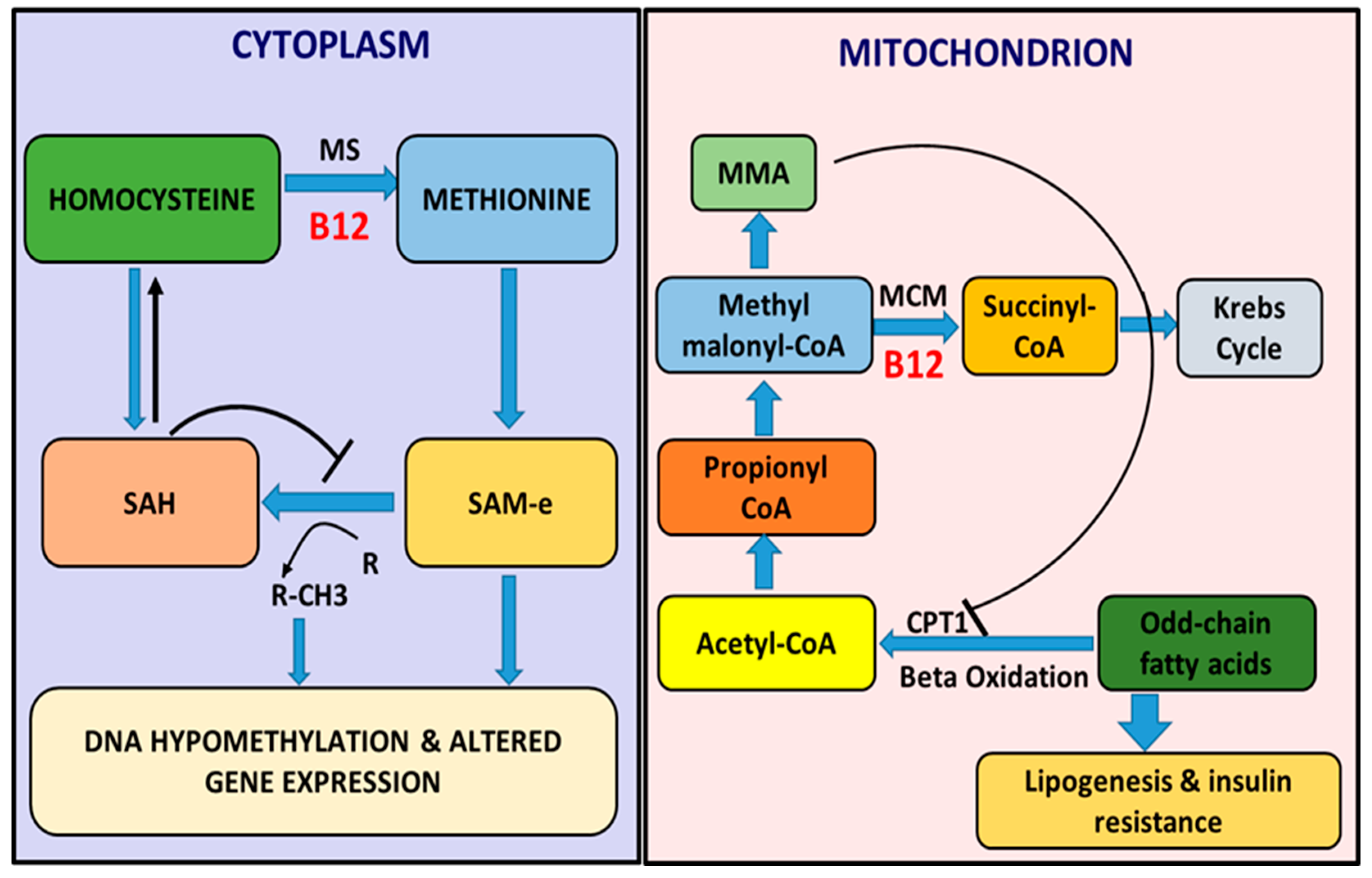
5. Molecular Mechanisms Regulating Low B12 and Lipogenesis
6. Epigenetic Mechanisms Underlying Low B12 Levels in Lipid Metabolism
6.1. DNA Methylation and Regulation of Lipid Metabolism through Low B12
6.2. MicroRNAs (miRNAs) and Regulation of Lipid Metabolism through Low B12
6.3. Modifications of Histones and Regulation of Lipid Metabolism through Low B12
7. Impact of One-Carbon Micronutrient Supplementation on Lipid Metabolism
8. Conclusions and Prospects
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
Abbreviations
| A | |
| AdoCbl–5′Adenosyl cobalamin | Adenosyl cobalamin |
| AGPAT3 | Acylglycerol−3-phosphate O-acyltransferases 3 |
| B | |
| BMI | Body mass index |
| C | |
| CAD | Coronary artery disease |
| CHD | Coronary heart disease |
| CKD | Chronic kidney disease |
| CpG | 5′cytosine-phosphate-guanine-3′ |
| CPT1α | Carnitine palmitoyl transferase I alpha |
| CVD | Cardiovascular diseases |
| D | |
| DAG | Diacylglycerol |
| DGAT 1&2 | Diacylglycerol acyltransferase 1&2 |
| DKA | Diabetic keto acidosis |
| DM | Diabetes mellitus |
| DMB | 5, 6-dimethylbenzimidazole |
| DNMTs | DNA methyl transferases |
| E | |
| ESRD | End-stage renal disease |
| ESR1 | Estrogen receptor 1 |
| ETC | Electron transport chain |
| F | |
| FAO | Fatty acid oxidation |
| FAS | Fatty acid synthase |
| FFA | Free fatty acids |
| G | |
| GDM | Gestational diabetes mellitus |
| GIT | Gastrointestinal tract |
| GPAT | Glycerol-3-phosphate acyltransferase |
| H | |
| HATS | Histone acetyltransferases |
| HC | Haptocorrin |
| HDACs | Histone deacetylases |
| HDL-C | High-density lipoprotein cholesterol |
| HFD | High fat diet |
| tHcy | total homocysteine |
| HMGCR | 3-hydroxy-3-methylglutaryl-CoA reductase |
| HMGCS | 3-hydroxy-3-methylglutaryl-CoA synthase |
| HoloTC | Holotranscobalamin |
| HOMA-IR | Homeostasis model of insulin resistance |
| I | |
| IDF | International Diabetes Federation |
| IF | Intrinsic factor |
| IR | Insulin resistance |
| L | |
| LCFAs | Long-chain fatty acids |
| LDL-C | Low-density lipoprotein cholesterol |
| LDLR | Low-density lipoprotein receptor |
| LXR-α | Liver X receptor alpha |
| M | |
| MCM | Methyl malonyl CoA mutase |
| MeCbl | Methyl-cobalamin |
| MetS | Metabolic syndrome |
| MI | Myocardial infarction |
| MMA | Methyl malonic acid |
| MS | Methionine synthase |
| MP | Methylation potential |
| miRNAs | MicroRNAs |
| N | |
| NAFLD | Non-alcoholic fatty liver disease |
| NASH | Non-alcoholic steatohepatitis |
| P | |
| PPAR-γ | Peroxisome proliferator-activated receptor gamma |
| S | |
| SAM | S-adenosyl methionine |
| SAH | S- adenosyl homocysteine |
| ScAT | Subcutaneous adipose tissues |
| SREBF1&2 | Sterol regulatory element binding protein 1 and 2 |
| stRNAs | Small temporal RNAs |
| T | |
| TCA | Tricarboxylic acid |
| TC | Transcobalamin |
| TCR or TCbIR | Transcobalamin receptor |
| T2D | Type 2 diabetes mellitus |
| TG | Triglyceride/Triacylglycerol |
| TNFα | Tumor necrosis factor-alpha |
| V | |
| VLDL | Very low-density lipoprotein |
| W | |
| WHO | World Health Organization |
References
- Gomez-Hernandez, A.; Beneit, N.; Diaz-Castroverde, S.; Escribano, O. Differential Role of Adipose Tissues in Obesity and Related Metabolic and Vascular Complications. Int. J. Endocrinol. 2016, 2016, 1216783. [Google Scholar] [CrossRef] [PubMed]
- Mathieu, P.; Lemieux, I.; Despres, J.P. Obesity, inflammation, and cardiovascular risk. Clin. Pharmacol. Ther. 2010, 87, 407–416. [Google Scholar] [CrossRef] [PubMed]
- Tremmel, M.; Gerdtham, U.G.; Nilsson, P.M.; Saha, S. Economic Burden of Obesity: A Systematic Literature Review. Int. J. Environ. Res. Public Health 2017, 14, 435. [Google Scholar] [CrossRef]
- De Benoist, B. Conclusions of a WHO Technical Consultation on folate and vitamin B12 deficiencies. Food Nutr. Bull. 2008, 29, S238–S244. [Google Scholar] [CrossRef] [PubMed]
- Green, R. Metabolite assays in cobalamin and folate deficiency. Baillieres Clin. Haematol. 1995, 8, 533–566. [Google Scholar] [CrossRef]
- Waldmann, A.; Koschizke, J.W.; Leitzmann, C.; Hahn, A. German vegan study: Diet, life-style factors, and cardiovascular risk profile. Ann. Nutr. Metab. 2005, 49, 366–372. [Google Scholar] [CrossRef]
- Khan, K.M.; Jialal, I. Folic Acid (Folate) Deficiency. In StatPearls; StatPearls Publishing LLC.: Treasure Island, FL, USA, 2019. [Google Scholar]
- Green, R.; Allen, L.H.; Bjorke-Monsen, A.L.; Brito, A.; Gueant, J.L.; Miller, J.W.; Molloy, A.M.; Nexo, E.; Stabler, S.; Toh, B.H.; et al. Vitamin B12 deficiency. Nat. Rev. Dis. Primers 2017, 3, 17040. [Google Scholar] [CrossRef]
- Adaikalakoteswari, A.; Jayashri, R.; Sukumar, N.; Venkataraman, H.; Pradeepa, R.; Gokulakrishnan, K.; Anjana, R.M.; McTernan, P.G.; Tripathi, G.; Patel, V.; et al. Vitamin B12 deficiency is associated with adverse lipid profile in Europeans and Indians with type 2 diabetes. Cardiovasc. Diabetol. 2014, 13, 129. [Google Scholar] [CrossRef]
- Ghosh, S.; Sinha, J.K.; Putcha, U.K.; Raghunath, M. Severe but Not Moderate Vitamin B12 Deficiency Impairs Lipid Profile, Induces Adiposity, and Leads to Adverse Gestational Outcome in Female C57BL/6 Mice. Front. Nutr. 2016, 3, 1. [Google Scholar] [CrossRef]
- MEDLINE/PubMed. Available online: http://www.ncbi.nlm.nih.gov/pubmed/ (accessed on 19 June 2020).
- Global Health (CABI). Available online: https://www.ebscohost.com/academic/global-health/ (accessed on 2 May 2020).
- Fang, H.; Kang, J.; Zhang, D. Microbial production of vitamin B 12: A review and future perspectives. Microb. Cell Factories 2017, 16, 15. [Google Scholar] [CrossRef]
- Stabler, S.P.; Allen, R.H. Vitamin B12 deficiency as a worldwide problem. Ann. Rev. Nutr. 2004, 24, 299–326. [Google Scholar] [CrossRef] [PubMed]
- Smith, A.D.; Warren, M.J.; Refsum, H. Vitamin B12. Adv. Food Nutr Res. 2018, 83, 215–279. [Google Scholar] [CrossRef] [PubMed]
- Smith, E.L. Purification of anti-pernicious anaemia factors from liver. Nature 1948, 161, 638. [Google Scholar] [CrossRef] [PubMed]
- Rickes, E.L.; Brink, N.G.; Koniuszy, F.R.; Wood, T.R.; Folkers, K. Crystalline Vitamin B12. Science 1948, 107, 396–397. [Google Scholar] [CrossRef]
- Hodgkin, D.C.; Kamper, J.; Mackay, M.; Pickworth, J.; Trueblood, K.N.; White, J.G. Structure of vitamin B12. Nature 1956, 178, 64–66. [Google Scholar] [CrossRef]
- Froese, D.S.; Gravel, R.A. Genetic disorders of vitamin B(1)(2) metabolism: Eight complementation groups—Eight genes. Expert Rev. Mol. Med. 2010, 12, e37. [Google Scholar] [CrossRef]
- Watanabe, F. Vitamin B12 Sources and Bioavailability. Exp. Biol. Med. 2007, 232, 1266–1274. [Google Scholar] [CrossRef]
- Ball, G.F.M. Vitamin B 12. In Bioavailability and Analysis of Vitamins in Foods; Springer: New York, NY, USA, 1998; pp. 497–515. [Google Scholar]
- Heyssel, R.M.; Bozian, R.C.; Darby, W.J.; Bell, M.C. Vitamin B12 turnover in man. The assimilation of vitamin B12 from natural foodstuff by man and estimates of minimal daily dietary requirements. Am. J. Clin. Nutr. 1966, 18, 176–184. [Google Scholar] [CrossRef]
- Sato, K.; Wang, X.; Mizoguchi, K. A modified form of a vitamin B12 compound extracted from whey fermented by Lactobacillus helveticus. J. Dairy Sci. 1997, 80, 2701–2705. [Google Scholar] [CrossRef]
- O’Leary, F.; Samman, S. Vitamin B12 in health and disease. Nutrients 2010, 2, 299–316. [Google Scholar] [CrossRef]
- Linden, D.; William-Olsson, L.; Ahnmark, A.; Ekroos, K.; Hallberg, C.; Sjogren, H.P.; Becker, B.; Svensson, L.; Clapham, J.C.; Oscarsson, J.; et al. Liver-directed overexpression of mitochondrial glycerol-3-phosphate acyltransferase results in hepatic steatosis, increased triacylglycerol secretion and reduced fatty acid oxidation. FASEB J. 2006, 20, 434–443. [Google Scholar] [CrossRef] [PubMed]
- Rizzo, G.; Laganà, A.S. A review of vitamin B12. Mol. Nutr. 2020, 105–129. [Google Scholar] [CrossRef]
- Joske, R.A. The vitamin B12 content of human liver tissue obtained by aspiration biopsy. Gut 1963, 4, 231–235. [Google Scholar] [CrossRef] [PubMed]
- Shinton, N.K. Vitamin B 12 and folate metabolism. Br. Med. J. 1972, 1, 556–559. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Sukumar, N.; Adaikalakoteswari, A.; Venkataraman, H.; Maheswaran, H.; Saravanan, P. Vitamin B12 status in women of childbearing age in the UK and its relationship with national nutrient intake guidelines: Results from two National Diet and Nutrition Surveys. BMJ Open 2016, 6, e011247. [Google Scholar] [CrossRef]
- Papp, F.; Rácz, G.; Lénárt, I.; Kóbor, J.; Bereczki, C.; Karg, E.; Baráth, Á. Maternal and neonatal vitamin B12 deficiency detected by expanded newborn screening. Orv. Hetil. 2017, 158, 1909–1918. [Google Scholar] [CrossRef]
- Sloan, J.L.; Carrillo, N.; Adams, D.; Venditti, C.P. Disorders of intracellular cobalamin metabolism. In GeneReviews®[Internet]; University of Washington: Seattle, WA, USA, 2018. [Google Scholar]
- McLean, E.; De Benoist, B.; Allen, L.H. Review of the magnitude of folate and vitamin B12 deficiencies worldwide. Food Nutr. Bull. 2008, 29, S38–S51. [Google Scholar] [CrossRef]
- Saravanan, P.; Yajnik, C.S. Role of maternal vitamin B12 on the metabolic health of the offspring: A contributor to the diabetes epidemic? Br. J. Diabetes Vasc. Dis. 2010, 10, 109–114. [Google Scholar] [CrossRef]
- Hunt, A.; Harrington, D.; Robinson, S. Vitamin B12 deficiency. BMJ 2014, 349, g5226. [Google Scholar] [CrossRef]
- Kumar, K.A.; Lalitha, A.; Pavithra, D.; Padmavathi, I.J.; Ganeshan, M.; Rao, K.R.; Venu, L.; Balakrishna, N.; Shanker, N.H.; Reddy, S.U.; et al. Maternal dietary folate and/or vitamin B12 restrictions alter body composition (adiposity) and lipid metabolism in Wistar rat offspring. J. Nutr. Biochem. 2013, 24, 25–31. [Google Scholar] [CrossRef]
- Sinclair, K.D.; Allegrucci, C.; Singh, R.; Gardner, D.S.; Sebastian, S.; Bispham, J.; Thurston, A.; Huntley, J.F.; Rees, W.D.; Maloney, C.A.; et al. DNA methylation, insulin resistance, and blood pressure in offspring determined by maternal periconceptional B vitamin and methionine status. Proc. Natl. Acad. Sci. USA 2007, 104, 19351–19356. [Google Scholar] [CrossRef] [PubMed]
- Cooney, C.A.; Dave, A.A.; Wolff, G.L. Maternal methyl supplements in mice affect epigenetic variation and DNA methylation of offspring. J. Nutr. 2002, 132, 2393S–2400S. [Google Scholar] [CrossRef] [PubMed]
- Shampa, G.; Kumar, S.J.; Bojanapalli, M.; Kumar, P.U.; Manchala, R. Chronic transgenerational vitamin B12 deficiency of severe and moderate magnitudes modulates adiposity—Probable underlying mechanisms. BioFactors 2017, 43, 400–414. [Google Scholar] [CrossRef]
- Ahmad, S.; Kumar, K.A.; Basak, T.; Bhardwaj, G.; Yadav, D.K.; Lalitha, A.; Chandak, G.R.; Raghunath, M.; Sengupta, S. PPAR signaling pathway is a key modulator of liver proteome in pups born to vitamin B(12) deficient rats. J. Proteom. 2013, 91, 297–308. [Google Scholar] [CrossRef] [PubMed]
- Adaikalakoteswari, A.; Finer, S.; Voyias, P.D.; McCarthy, C.M.; Vatish, M.; Moore, J.; Smart-Halajko, M.; Bawazeer, N.; Al-Daghri, N.M.; McTernan, P.G.; et al. Vitamin B12 insufficiency induces cholesterol biosynthesis by limiting s-adenosylmethionine and modulating the methylation of SREBF1 and LDLR genes. Clin. Epigenet. 2015, 7, 14. [Google Scholar] [CrossRef]
- Adaikalakoteswari, A.; Vatish, M.; Alam, M.T.; Ott, S.; Kumar, S.; Saravanan, P. Metabolism. Low Vitamin B12 in Pregnancy Is Associated With Adipose-Derived Circulating miRs Targeting PPAR γ and Insulin Resistance. J. Clin. Endocrinol. Metab. 2017, 102, 4200–4209. [Google Scholar] [CrossRef]
- Lodhi, R.; Panchal, A. Interrelationship of Vitamin B12, Androgens and Cortisol in Chronic Stress and Associated Vascular Dysfunction. J. Pharm. Sci. Biosci. Res. 2014, 4, 293–300. [Google Scholar]
- Hagar, H.H. Folic acid and vitamin B12 supplementation attenuates isoprenaline-induced myocardial infarction in experimental hyperhomocysteinemic rats. Pharmacol. Res. 2002, 46, 213–219. [Google Scholar] [CrossRef]
- O’Malley, E.G.; Reynolds, C.M.E.; Cawley, S.; Woodside, J.V.; Molloy, A.M.; Turner, M.J. Folate and vitamin B12 levels in early pregnancy and maternal obesity. Eur. J. Obstet. Gynecol. Reprod. Biol. 2018, 231, 80–84. [Google Scholar] [CrossRef]
- Sukumar, N.; Venkataraman, H.; Wilson, S.; Goljan, I.; Selvamoni, S.; Patel, V.; Saravanan, P. Vitamin B12 Status among Pregnant Women in the UK and Its Association with Obesity and Gestational Diabetes. Nutrients 2016, 8, 768. [Google Scholar] [CrossRef]
- Yajnik, C.S.; Deshpande, S.S.; Jackson, A.A.; Refsum, H.; Rao, S.; Fisher, D.J.; Bhat, D.S.; Naik, S.S.; Coyaji, K.J.; Joglekar, C.V.; et al. Vitamin B12 and folate concentrations during pregnancy and insulin resistance in the offspring: The Pune Maternal Nutrition Study. Diabetologia 2008, 51, 29–38. [Google Scholar] [CrossRef]
- Özer, S.; Sönmezgöz, E.; Demir, O. Negative correlation among vitamin B12 levels, obesity severity and metabolic syndrome in obese children: A case control study. J. Pak. Med. Assoc. 2017, 67, 1648–1653. [Google Scholar] [PubMed]
- Wiebe, N.; Field, C.J.; Tonelli, M. A systematic review of the vitamin B12, folate and homocysteine triad across body mass index. Obes. Rev. Offic. J. Int. Assoc. Study Obes. 2018, 19, 1608–1618. [Google Scholar] [CrossRef] [PubMed]
- Knight, B.A.; Shields, B.M.; Brook, A.; Hill, A.; Bhat, D.S.; Hattersley, A.T.; Yajnik, C.S. Lower circulating B12 is associated with higher obesity and insulin resistance during pregnancy in a non-diabetic white British population. PLoS ONE 2015, 10, e0135268. [Google Scholar] [CrossRef] [PubMed]
- Stewart, C.P.; Christian, P.; Schulze, K.J.; Arguello, M.; LeClerq, S.C.; Khatry, S.K.; West, J.K.P. Low Maternal Vitamin B-12 Status Is Associated with Offspring Insulin Resistance Regardless of Antenatal Micronutrient Supplementation in Rural Nepal. J. Nutr. 2011, 141, 1912–1917. [Google Scholar] [CrossRef] [PubMed]
- Mamabolo, R.L.; Alberts, M.; Levitt, N.S. The effect of maternal glucose metabolism, iron, vitamin B12 and folate status on pregnancy outcomes. S. Afr. J. Clin. Nutr. 2006, 19, 120–130. [Google Scholar] [CrossRef]
- Ho, M.; Halim, J.H.; Gow, M.L.; El-Haddad, N.; Marzulli, T.; Baur, L.A.; Cowell, C.T.; Garnett, S.P. Vitamin B12 in obese adolescents with clinical features of insulin resistance. Nutrients 2014, 6, 5611–5618. [Google Scholar] [CrossRef] [PubMed]
- Baltaci, D.; Kutlucan, A.; Turker, Y.; Yilmaz, A.; Karacam, S.; Deler, H.; Ucgun, T.; Kara, I.H. Association of vitamin B12 with obesity, overweight, insulin resistance and metabolic syndrome, and body fat composition; primary care-based study. Med. Glas Zenica 2013, 10, 203–210. [Google Scholar]
- Kaya, C.; Cengiz, S.D.; Satiroglu, H. Obesity and insulin resistance associated with lower plasma vitamin B12 in PCOS. Reprod. Biomed. Online 2009, 19, 721–726. [Google Scholar] [CrossRef]
- Bhargava, S.K.; Sachdev, H.S.; Fall, C.H.; Osmond, C.; Lakshmy, R.; Barker, D.J.; Biswas, S.K.; Ramji, S.; Prabhakaran, D.; Reddy, K.S. Relation of serial changes in childhood body-mass index to impaired glucose tolerance in young adulthood. N. Engl. J. Med. 2004, 350, 865–875. [Google Scholar] [CrossRef]
- Abdullah, N.; Mohamed, S.; Abdulrahman, R. Relation between vitamin B12 and Non-alcoholic fatty Liver Disease: A Hospital Based Study. Int. J. Adv. Res. 2015, 3, 1335–1343. [Google Scholar]
- Saraswathy, K.N.; Joshi, S.; Yadav, S.; Garg, P.R. Metabolic distress in lipid & one carbon metabolic pathway through low vitamin B-12: A population based study from North India. Lipids Health Dis. 2018, 17, 96. [Google Scholar] [CrossRef] [PubMed]
- Guarnizo-Poma, M.; Urrunaga-Pastor, D.; Montero-Suyo, C.; Lazaro-Alcantara, H.; Paico-Palacios, S.; Pantoja-Torres, B.; Benites-Zapata, V.A. Association between serum vitamin B12 levels and metabolic syndrome in a euthyroid population. Diabetes Metab. Syndr. 2018, 12, 943–948. [Google Scholar] [CrossRef] [PubMed]
- Sachdev, P. Homocysteine and neuropsychiatric disorders. Braz. J. Psychiatr. 2004, 26, 50–56. [Google Scholar] [CrossRef]
- Mager, A.; Orvin, K.; Koren-Morag, N.; Lev, I.E.; Assali, A.; Kornowski, R.; Shohat, M.; Battler, A.; Hasdai, D. Impact of homocysteine-lowering vitamin therapy on long-term outcome of patients with coronary artery disease. Am. J. Cardiol. 2009, 104, 745–749. [Google Scholar] [CrossRef]
- Mao, X.; Xing, X.; Xu, R.; Gong, Q.; He, Y.; Li, S.; Wang, H.; Liu, C.; Ding, X.; Na, R. Folic acid and vitamins D and B12 correlate with homocysteine in Chinese patients with type-2 diabetes mellitus, hypertension, or cardiovascular disease. Medicine 2016, 95, e2652. [Google Scholar] [CrossRef]
- Cui, R.; Iso, H.; Date, C.; Kikuchi, S.; Tamakoshi, A.J.S. Dietary folate and vitamin b6 and B12 intake in relation to mortality from cardiovascular diseases: Japan collaborative cohort study. Stroke 2010, 41, 1285–1289. [Google Scholar] [CrossRef]
- Albert, C.M.; Cook, N.R.; Gaziano, J.M.; Zaharris, E.; MacFadyen, J.; Danielson, E.; Buring, J.E.; Manson, J.E. Effect of folic acid and B vitamins on risk of cardiovascular events and total mortality among women at high risk for cardiovascular disease: A randomized trial. Jama 2008, 299, 2027–2036. [Google Scholar] [CrossRef]
- Lee, B.; Huang, M.; Chung, L.; Cheng, C.; Lin, K.; Su, K.; Huang, Y.-C. Folic acid and vitamin B 12 are more effective than vitamin B 6 in lowering fasting plasma homocysteine concentration in patients with coronary artery disease. Eur. J. Clin. Nutr. 2004, 58, 481. [Google Scholar] [CrossRef]
- Setola, E.; Monti, L.D.; Galluccio, E.; Palloshi, A.; Fragasso, G.; Paroni, R.; Magni, F.; Sandoli, E.P.; Lucotti, P.; Costa, S.; et al. Insulin resistance and endothelial function are improved after folate and vitamin B12 therapy in patients with metabolic syndrome: Relationship between homocysteine levels and hyperinsulinemia. Eur. J. Endocrinol. 2004, 151, 483–489. [Google Scholar] [CrossRef]
- Mendonça, N.; Jagger, C.; Granic, A.; Martin-Ruiz, C.; Mathers, J.C.; Seal, C.J.; Hill, T.R. Elevated total homocysteine in all participants and plasma vitamin B12 concentrations in women are associated with all-cause and cardiovascular mortality in the very old: The Newcastle 85+ Study. J. Gerontol. Ser. A 2018, 73, 1258–1264. [Google Scholar]
- Chakraverty, R.; Chakraborty, P. Recent Insights into the Role of Vitamin B12 and Vitamin D upon Cardiovascular Mortality: A Systematic Review. Acta Sci. Pharm. Sci. 2018, 2, 61–65. [Google Scholar]
- Ryan-Harshman, M.; Aldoori, W. Vitamin B12 and health. Can. Fam. Phys. 2008, 54, 536–541. [Google Scholar]
- Robinson, K. Renal disease, homocysteine, and cardiovascular complications. Circulation 2004, 109, 294–295. [Google Scholar] [CrossRef] [PubMed]
- Langan, R.C.; Goodbred, A. Vitamin B12 deficiency: Recognition and management. Am. Fam. Phys. 2017, 96, 384–389. [Google Scholar]
- McMahon, G.M.; Hwang, S.-J.; Tanner, R.M.; Jacques, P.F.; Selhub, J.; Muntner, P.; Fox, C.S. The association between vitamin B12, albuminuria and reduced kidney function: An observational cohort study. BMC Nephrol. 2015, 16, 7. [Google Scholar] [CrossRef]
- Capelli, I.; Cianciolo, G.; Gasperoni, L.; Zappulo, F.; Tondolo, F.; Cappuccilli, M.; La Manna, G. Folic Acid and Vitamin B12 Administration in CKD, Why Not? Nutrients 2019, 11, 383. [Google Scholar] [CrossRef]
- Lee, J.H.; Friso, S.; Choi, S.W. Epigenetic mechanisms underlying the link between non-alcoholic fatty liver diseases and nutrition. Nutrients 2014, 6, 3303–3325. [Google Scholar] [CrossRef]
- Zhao, M.; Ralat, M.A.; Da Silva, V.; Garrett, T.J.; Melnyk, S.; James, S.J.; Gregory, J.F., III. Vitamin B-6 restriction impairs fatty acid synthesis in cultured human hepatoma (HepG2) cells. Am. J. Physiol. Endocrinol. Metab. 2013, 304, E342–E351. [Google Scholar] [CrossRef]
- Mooney, S.; Leuendorf, J.E.; Hendrickson, C.; Hellmann, H. Vitamin B6: A long known compound of surprising complexity. Molecules 2009, 14, 329–351. [Google Scholar] [CrossRef]
- Sun, C.; Fan, J.G.; Qiao, L. Potential epigenetic mechanism in non-alcoholic Fatty liver disease. Int. J. Mol. Sci. 2015, 16, 5161–5179. [Google Scholar] [CrossRef] [PubMed]
- Gallego-Duran, R.; Romero-Gomez, M. Epigenetic mechanisms in non-alcoholic fatty liver disease: An emerging field. World J. Hepatol. 2015, 7, 2497–2502. [Google Scholar] [CrossRef] [PubMed]
- Takahashi-Iniguez, T.; Garcia-Hernandez, E.; Arreguin-Espinosa, R.; Flores, M.E. Role of vitamin B12 on methylmalonyl-CoA mutase activity. J. Zhejiang Univ. Sci. B 2012, 13, 423–437. [Google Scholar] [CrossRef] [PubMed]
- Finer, S.; Saravanan, P.; Hitman, G.; Yajnik, C. The role of the one-carbon cycle in the developmental origins of Type 2 diabetes and obesity. Diabetes Med. 2014, 31, 263–272. [Google Scholar] [CrossRef]
- Rush, E.C.; Katre, P.; Yajnik, C.S. Vitamin B12: One carbon metabolism, fetal growth and programming for chronic disease. Eur. J. Clin. Nutr. 2014, 68, 2–7. [Google Scholar] [CrossRef]
- Yajnik, C.S. Fetal programming of diabetes: Still so much to learn! Diabetes Care 2010, 33, 1146–1148. [Google Scholar] [CrossRef]
- Varma, B.A.; Bashetti, S.; Vijayaraghavan, R.; Sailesh, K.S. Folic Acid, Vitamin B12, And DNA Methylation: An Update. Asian J. Pharm. Clin. Res. 2018, 11, 17–20. [Google Scholar] [CrossRef]
- Yu, D.; Du, Z.; Pian, L.; Li, T.; Wen, X.; Li, W.; Kim, S.-J.; Xiao, J.; Cohen, P.; Cui, J. Mitochondrial DNA hypomethylation is a biomarker associated with induced senescence in human fetal heart mesenchymal stem cells. Stem Cells Int. 2017, 2017, 1–12. [Google Scholar] [CrossRef]
- Iacobazzi, V.; Castegna, A.; Infantino, V.; Andria, G. Mitochondrial DNA methylation as a next-generation biomarker and diagnostic tool. Mol. Genet. Metab. 2013, 110, 25–34. [Google Scholar] [CrossRef]
- Yi, P.; Melnyk, S.; Pogribna, M.; Pogribny, I.P.; Hine, R.J.; James, S.J. Increase in plasma homocysteine associated with parallel increases in plasma S-adenosylhomocysteine and lymphocyte DNA hypomethylation. J. Biol. Chem. 2000, 275, 29318–29323. [Google Scholar] [CrossRef]
- Dominguez-Salas, P.; Cox, S.E.; Prentice, A.M.; Hennig, B.J.; Moore, S.E. Maternal nutritional status, C(1) metabolism and offspring DNA methylation: A review of current evidence in human subjects. Proc. Nutr. Soc. 2012, 71, 154–165. [Google Scholar] [CrossRef] [PubMed]
- Skjaerven, K.H.; Jakt, L.M.; Fernandes, J.M.O.; Dahl, J.A.; Adam, A.C.; Klughammer, J.; Bock, C.; Espe, M. Parental micronutrient deficiency distorts liver DNA methylation and expression of lipid genes associated with a fatty-liver-like phenotype in offspring. Sci. Rep. 2018, 8, 3055. [Google Scholar] [CrossRef] [PubMed]
- Pogribny, I.P.; James, S.J.; Beland, F.A. Molecular alterations in hepatocarcinogenesis induced by dietary methyl deficiency. Mol. Nutr. Food Res. 2012, 56, 116–125. [Google Scholar] [CrossRef] [PubMed]
- Pooya, S.; Blaise, S.; Moreno Garcia, M.; Giudicelli, J.; Alberto, J.M.; Gueant-Rodriguez, R.M.; Jeannesson, E.; Gueguen, N.; Bressenot, A.; Nicolas, B.; et al. Methyl donor deficiency impairs fatty acid oxidation through PGC-1alpha hypomethylation and decreased ER-alpha, ERR-alpha, and HNF-4alpha in the rat liver. J. Hepatol. 2012, 57, 344–351. [Google Scholar] [CrossRef] [PubMed]
- Byrne, C.D.; Olufadi, R.; Bruce, K.D.; Cagampang, F.R.; Ahmed, M.H. Metabolic disturbances in non-alcoholic fatty liver disease. Clin. Sci. Lond. 2009, 116, 539–564. [Google Scholar] [CrossRef]
- Choi, S.W.; Friso, S.; Ghandour, H.; Bagley, P.J.; Selhub, J.; Mason, J.B. Vitamin B-12 deficiency induces anomalies of base substitution and methylation in the DNA of rat colonic epithelium. J. Nutr. 2004, 134, 750–755. [Google Scholar] [CrossRef]
- Kulkarni, A.; Dangat, K.; Kale, A.; Sable, P.; Chavan-Gautam, P.; Joshi, S. Effects of altered maternal folic acid, vitamin B12 and docosahexaenoic acid on placental global DNA methylation patterns in Wistar rats. PLoS ONE 2011, 6, e17706. [Google Scholar] [CrossRef]
- Nilsson, E.; Matte, A.; Perfilyev, A.; De Mello, V.D.; Käkelä, P.; Pihlajamäki, J.; Ling, C. Epigenetic Alterations in Human Liver From Subjects With Type 2 Diabetes in Parallel With Reduced Folate Levels. J. Clin. Endocrinol. Metab. 2015, 100, E1491–E1501. [Google Scholar] [CrossRef]
- Cordero, P.; Gómez-Úriz, A.M.; Campion, J.; Milagro, F.; Martinez, J.A. Dietary supplementation with methyl donors reduces fatty liver and modifies the fatty acid synthase DNA methylation profile in rats fed an obesogenic diet. Genes Nutr. 2013, 8, 105. [Google Scholar] [CrossRef]
- Da Silva, R.P.; Kelly, K.B.; Al Rajabi, A.; Jacobs, R.L. Novel insights on interactions between folate and lipid metabolism. Biofactors 2014, 40, 277–283. [Google Scholar] [CrossRef]
- Cordero, P.; Campion, J.; Milagro, F.I.; Martinez, J.A. Transcriptomic and epigenetic changes in early liver steatosis associated to obesity: Effect of dietary methyl donor supplementation. Mol. Genet. Metab. 2013, 110, 388–395. [Google Scholar] [CrossRef] [PubMed]
- He, L.; Hannon, G.J. MicroRNAs: Small RNAs with a big role in gene regulation. Nat. Rev. Genet. 2004, 5, 522–531. [Google Scholar] [CrossRef] [PubMed]
- Finch, M.L.; Marquardt, J.U.; Yeoh, G.C.; Callus, B.A. Regulation of microRNAs and their role in liver development, regeneration and disease. Int. J. Biochem. Cell Biol. 2014, 54, 288–303. [Google Scholar] [CrossRef] [PubMed]
- Ferreira, D.M.; Simao, A.L.; Rodrigues, C.M.; Castro, R.E. Revisiting the metabolic syndrome and paving the way for microRNAs in non-alcoholic fatty liver disease. FEBS J. 2014, 281, 2503–2524. [Google Scholar] [CrossRef]
- Hamam, D.; Ali, D.; Kassem, M.; Aldahmash, A.; Alajez, N.M. microRNAs as regulators of adipogenic differentiation of mesenchymal stem cells. Stem Cells Dev. 2014, 24, 417–425. [Google Scholar] [CrossRef]
- Xie, H.; Lim, B.; Lodish, H.F. MicroRNAs induced during adipogenesis that accelerate fat cell development are downregulated in obesity. Diabetes 2009, 58, 1050–1057. [Google Scholar] [CrossRef]
- Davalos, A.; Goedeke, L.; Smibert, P.; Ramirez, C.M.; Warrier, N.P.; Andreo, U.; Cirera-Salinas, D.; Rayner, K.; Suresh, U.; Pastor-Pareja, J.C.; et al. miR-33a/b contribute to the regulation of fatty acid metabolism and insulin signaling. Proc. Natl. Acad. Sci. USA 2011, 108, 9232–9237. [Google Scholar] [CrossRef]
- Severson, T.J.; Besur, S.; Bonkovsky, H.L. Genetic factors that affect nonalcoholic fatty liver disease: A systematic clinical review. World J. Gastroenterol. 2016, 22, 6742. [Google Scholar] [CrossRef]
- Cheung, O.; Puri, P.; Eicken, C.; Contos, M.J.; Mirshahi, F.; Maher, J.W.; Kellum, J.M.; Min, H.; Luketic, V.A.; Sanyal, A.J. Nonalcoholic steatohepatitis is associated with altered hepatic MicroRNA expression. Hepatology 2008, 48, 1810–1820. [Google Scholar] [CrossRef]
- Elmen, J.; Lindow, M.; Schutz, S.; Lawrence, M.; Petri, A.; Obad, S.; Lindholm, M.; Hedtjarn, M.; Hansen, H.F.; Berger, U.; et al. LNA-mediated microRNA silencing in non-human primates. Nature 2008, 452, 896–899. [Google Scholar] [CrossRef]
- Sacco, J.; Adeli, K. MicroRNAs: Emerging roles in lipid and lipoprotein metabolism. Curr. Opin. Lipidol. 2012, 23, 220–225. [Google Scholar] [CrossRef] [PubMed]
- Ghosh, S.; Sinha, J.K.; Khandelwal, N.; Chakravarty, S.; Kumar, A.; Raghunath, M. Increased stress and altered expression of histone modifying enzymes in brain are associated with aberrant behaviour in vitamin B12 deficient female mice. Nutr. Neurosci. 2018, 1–10. [Google Scholar] [CrossRef] [PubMed]
- Garcia, B.A.; Luka, Z.; Loukachevitch, L.V.; Bhanu, N.V.; Wagner, C. Folate deficiency affects histone methylation. Med. Hypotheses 2016, 88, 63–67. [Google Scholar] [CrossRef] [PubMed]
- Li, J.; Huang, J.; Li, J.-S.; Chen, H.; Huang, K.; Zheng, L. Accumulation of endoplasmic reticulum stress and lipogenesis in the liver through generational effects of high fat diets. J. Hepatol. 2012, 56, 900–907. [Google Scholar] [CrossRef] [PubMed]
- Choi, S.-W.; Friso, S. Epigenetics: A new bridge between nutrition and health. Adv. Nutr. 2010, 1, 8–16. [Google Scholar] [CrossRef] [PubMed]
- Mehedint, M.G.; Niculescu, M.D.; Craciunescu, C.N.; Zeisel, S.H. Choline deficiency alters global histone methylation and epigenetic marking at the Re1 site of the calbindin 1 gene. FASEB J. 2010, 24, 184–195. [Google Scholar] [CrossRef] [PubMed]
- Okamura, M.; Inagaki, T.; Tanaka, T.; Sakai, J. Role of histone methylation and demethylation in adipogenesis and obesity. Organogenesis 2010, 6, 24–32. [Google Scholar] [CrossRef]
- Tateishi, K.; Okada, Y.; Kallin, E.M.; Zhang, Y. Role of Jhdm2a in regulating metabolic gene expression and obesity resistance. Nature 2009, 458, 757. [Google Scholar] [CrossRef]
- Postic, C.; Girard, J. Contribution of de novo fatty acid synthesis to hepatic steatosis and insulin resistance: Lessons from genetically engineered mice. J. Clin. Investig. 2008, 118, 829–838. [Google Scholar] [CrossRef]
- Jones, K.M.; Ramirez-Zea, M.; Zuleta, C.; Allen, L.H. Prevalent vitamin B-12 deficiency in twelve-month-old Guatemalan infants is predicted by maternal B-12 deficiency and infant diet. J. Nutr. 2007, 137, 1307–1313. [Google Scholar] [CrossRef]
- Wang, L.J.; Zhang, H.W.; Zhou, J.Y.; Liu, Y.; Yang, Y.; Chen, X.L.; Zhu, C.H.; Zheng, R.D.; Ling, W.H.; Zhu, H.L. Betaine attenuates hepatic steatosis by reducing methylation of the MTTP promoter and elevating genomic methylation in mice fed a high-fat diet. J. Nutr. Biochem. 2014, 25, 329–336. [Google Scholar] [CrossRef] [PubMed]
- Yadav, D.K.; Shrestha, S.; Lillycrop, K.A.; Joglekar, C.V.; Pan, H.; Holbrook, J.D.; Fall, C.H.; Yajnik, C.S.; Chandak, G.R. Vitamin B12 supplementation influences methylation of genes associated with Type 2 diabetes and its intermediate traits. Epigenomics 2018, 10, 71–90. [Google Scholar] [CrossRef] [PubMed]
- Devi, S.; Mukhopadhyay, A.; Dwarkanath, P.; Thomas, T.; Crasta, J.; Thomas, A.; Sheela, C.; Hsu, J.W.; Tang, G.J.; Jahoor, F.; et al. Combined Vitamin B-12 and Balanced Protein-Energy Supplementation Affect Homocysteine Remethylation in the Methionine Cycle in Pregnant South Indian Women of Low Vitamin B-12 Status–4. J. Nutr. 2017, 147, 1094–1103. [Google Scholar] [CrossRef]
- Kuniskii, D.G. Effect of methionine and vitamins B12 and B15 on the content and distribution of proteins, glycogen and lipids in the hepatic lobules of chickens. Arkhiv Anat. Gistol. Embriol. 1980, 79, 97–101. [Google Scholar]
- Duggan, C.; Srinivasan, K.; Thomas, T.; Samuel, T.; Rajendran, R.; Muthayya, S.; Finkelstein, J.L.; Lukose, A.; Fawzi, W.; Allen, L.H.; et al. Vitamin B-12 supplementation during pregnancy and early lactation increases maternal, breast milk, and infant measures of vitamin B-12 status. J. Nutr. 2014, 144, 758–764. [Google Scholar] [CrossRef]
| (a) Reduced B12 Intake i. Malnutrition ii. Vegetarian diet iii. Alcohol abuse iv. Old age (>75 years) |
| (b) An Impairment of B12 Bioavailability Via Gastric Wall Damage (with a Decrease in Intrinsic Factor) |
| i. Total (in certain stomach cancers) or partial gastrectomy including bariatric surgery. |
| ii. Atrophic autoimmune gastritis (such as pernicious anemia) or other gastritis (e.g., Helicobactor pylori). |
| (c) Impairment of Absorption Via the Intestines |
| i. Blind-loop syndrome |
| ii. Overgrowth of bacteria, giardiasis and tapeworm infections |
| iii. Ileal resection iv. Crohn’s disease |
| (d) Inherited (Congenital) Disorders of B12 Deficiency |
| i. Defect of the intrinsic factor receptor such as in ImerslundGräsback syndrome |
| ii. Juvenile pernicious anemia—Congenital intrinsic factor (IF) deficiency |
| iii. Cobalamin mutation (C-G−1 gene) |
| iv. Deficiency in Transcobalamin (TC) v. Methylmalonic acidemia, homocystinuria and combined methylmalonic acidemia and homocystinuria [31] |
| (e) Increased B12 Requirements |
| i. Hemolytic anemic conditions |
| ii. HIV infection |
| (f) Drugs |
| i. Metformin ii. Proton pump inhibitors iii. Prolonged use of histamine receptor 2 (H2) blockers (especially >12 months) |
| Obesity | Insulin Resistance | Dyslipidemia | Cardiovascular Diseases |
|---|---|---|---|
| a. Increased visceral adiposity in Wistar rats [35]. | Increased resistance to insulin and elevated blood pressure in sheep [36,37] | a. Increased adiposity, TG and total cholesterol levels in Wistar rat models [35]. | a. Disruption of androgen testosterone levels associated with vascular dysfunction in Sprague–Dawley rat model due to low B12 [42] |
| b. Higher adiposity in female C57 BL/6 mice [10]. | b. Increased plasma TG, cholesterol and some pro-inflammatory markers [38] | b. Reduction in myocardial infarction (MI) risk and tHcy levels due to B12 and/ or folate supplementation in rat models [43] | |
| c. Increased body weight in Wistar rats [35,38] | c. Increased cholesterol levels in human adipocyte cell line (Chub-S7) [40] | ||
| d. Higher total body fat in Wistar rats [35,38] | d. Increased TG in human adipocyte cell line (Chub-S7) [41]. |
| Obesity | Insulin Resistance | Dyslipidemia | Cardiovascular Diseases |
|---|---|---|---|
| a. Low B12 (<150 pmol/L) was associated with increased adiposity with higher T2D risk in pregnant women [46] | b. Low B12 (<180 pmol/L [49]) was associated with increased resistance to insulin in White Caucasian pregnant women without GDM. | a. Low B12 (<148 pmol/L) was associated with elevated levels of LDL-cholesterol, total-cholesterol and cholesterol-to-HDL ratio in pregnant and non-pregnant women at childbearing age [40] | a. B12 was negatively correlated with tHcy levels in Chinese-CVD patients ≥ 65 years of age (median low B12 = 4.19 pmol/L) [61]. |
| b. Low B12 (median−203 pmol/L [44] and <148 pmol/L [48]) levels were associated with increased BMI in maternal and general and/or clinal populations respectively | b. Prediction of higher risk of resistance to insulin in children born to low B12 (<150 pmol/L [46], 148 pmol/L [50]) mothers | b. Low B12 (≤220 pg/mL) was associated with both low HDL and hyperhomocysteinemia in North Indian population [57] | b. Low B12 (<148 pmol/L) and high tHcy levels were associated with higher risk of all-cause and CVD deaths in aged women [66] |
| c. Low B12 (102–208 pmol/L interquartile range) was associated with obesity in children compared to healthy volunteers [47]. | c. Low B12 (≤150 pmol/L [29], <148 pmol/L [52], <200 pg/mL [53], <178 pg/mL [54]) levels were associated with increased IR in adult patients, polycystic ovarian syndrome women and obese adolescents | c. B12 negatively correlated with markers of MetS such as low HDL and high TG levels in erythroid patients (Low B12 range 180–301 pmol/L) [58] | c. B12 supplementation reduced the risk of stroke in patients with CVD and/or renal disease [67]. |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Boachie, J.; Adaikalakoteswari, A.; Samavat, J.; Saravanan, P. Low Vitamin B12 and Lipid Metabolism: Evidence from Pre-Clinical and Clinical Studies. Nutrients 2020, 12, 1925. https://doi.org/10.3390/nu12071925
Boachie J, Adaikalakoteswari A, Samavat J, Saravanan P. Low Vitamin B12 and Lipid Metabolism: Evidence from Pre-Clinical and Clinical Studies. Nutrients. 2020; 12(7):1925. https://doi.org/10.3390/nu12071925
Chicago/Turabian StyleBoachie, Joseph, Antonysunil Adaikalakoteswari, Jinous Samavat, and Ponnusamy Saravanan. 2020. "Low Vitamin B12 and Lipid Metabolism: Evidence from Pre-Clinical and Clinical Studies" Nutrients 12, no. 7: 1925. https://doi.org/10.3390/nu12071925
APA StyleBoachie, J., Adaikalakoteswari, A., Samavat, J., & Saravanan, P. (2020). Low Vitamin B12 and Lipid Metabolism: Evidence from Pre-Clinical and Clinical Studies. Nutrients, 12(7), 1925. https://doi.org/10.3390/nu12071925







