Association of Dietary Acid Load with the Prevalence of Metabolic Syndrome among Participants in Baseline Survey of the Japan Multi-Institutional Collaborative Cohort Study
Abstract
1. Introduction
2. Materials and Methods
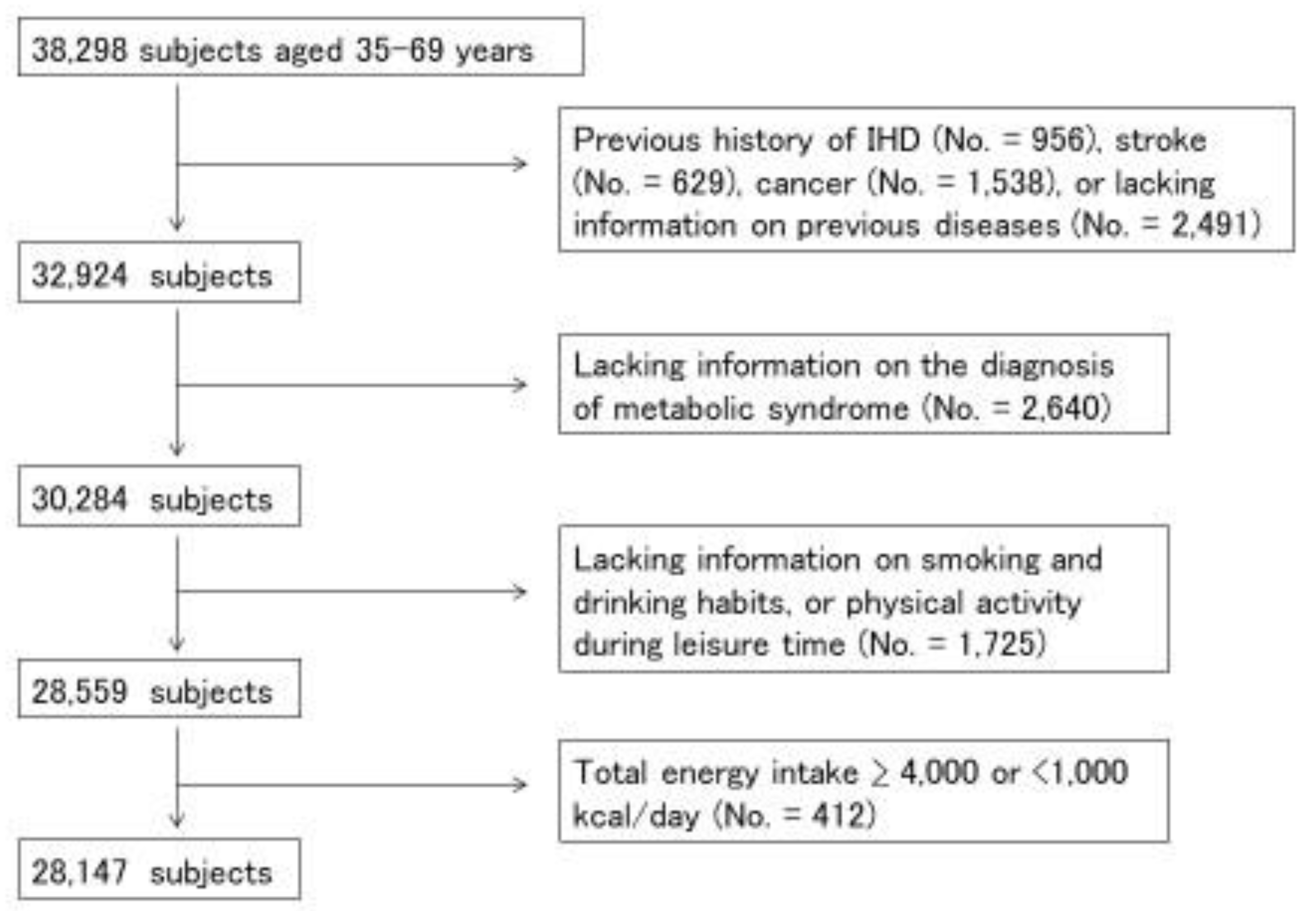
2.1. Study Subjects
2.2. Food-Frequency Questionnaire (FFQ) and Covariates
2.3. Metabolic-Syndrome Diagnosis
2.4. Dietary-Acid-Load Estimation
2.5. Statistical Analysis
3. Results
4. Discussion
5. Concluisons
Supplementary Materials
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- Alberti, K.G.; Eckel, R.H.; Grundy, S.M.; Zimmet, P.Z.; Cleeman, J.I.; Donato, K.A.; Fruchart, J.C.; James, W.P.; Loria, C.M.; Smith, S.C., Jr. International Diabetes Federation Task Force on Epidemiology and Prevention; Hational Heart, Lung, and Blood Institute; American Heart Association; World Heart Federation; International Atherosclerosis Society; International Association for the Study of Obesity. Harmonizing the metabolic syndrome: A joint interim statement of the International Diabetes Federation Task Force on Epidemiology and Prevention; National Heart, Lung, and Blood Institute; American Heart Association; World Heart Federation; International Atherosclerosis Society; and International Association for the Study of Obesity. Circulation 2009, 120, 1640–1645. [Google Scholar] [PubMed]
- Sattar, N.; Gaw, A.; Scherbakova, O.; Ford, I.; O’Reilly, D.S.; Haffner, S.M.; Isles, C.; Macfarlane, P.W.; Packard, C.J.; Cobbe, S.M.; et al. Metabolic syndrome with and without C-reactive protein as a predictor of coronary heart disease and diabetes in the West of Scotland Coronary Prevention Study. Circulation 2003, 108, 414–419. [Google Scholar] [CrossRef] [PubMed]
- Galassi, A.; Reynolds, K.; He, J. Metabolic syndrome and risk of cardiovascular disease: A meta-analysis. Am. J. Med. 2006, 119, 812–819. [Google Scholar] [CrossRef] [PubMed]
- Rodríguez-Monforte, M.; Sánchez, E.; Barrio, F.; Costa, B.; Flores-Mateo, G. Metabolic syndrome and dietary patterns: A systematic review and meta-analysis of observational studies. Eur. J. Nutr. 2017, 56, 925–947. [Google Scholar] [CrossRef] [PubMed]
- Asghari, G.; Yuzbashian, E.; Mirmiran, P.; Hooshmand, F.; Najafi, R.; Azizi, F. Dietary Approaches to Stop Hypertension (DASH) dietary pattern is associated with reduced incidence of metabolic syndrome in children and adolescents. J. Pediatr. 2016, 174, 178–184. [Google Scholar] [CrossRef] [PubMed]
- Godos, J.; Zappalà, G.; Bernardini, S.; Giambini, I.; Bes-Rastrollo, M.; Martinez-Gonzalez, M. Adherence to the Mediterranean diet is inversely associated with metabolic syndrome occurrence: A meta-analysis of observational studies. Int. J. Food Sci. Nutr. 2017, 68, 138–148. [Google Scholar] [CrossRef]
- Fagherazzi, G.; Vilier, A.; Bonnet, F.; Lajous, M.; Balkau, B.; Boutron-Rualt, M.C.; Clavel-Chapelon, F. Dietary acid load and risk of type 2 diabetes: The E3N-EPIC cohort study. Diabetologia 2014, 57, 313–320. [Google Scholar] [CrossRef]
- Akter, S.; Kurotani, K.; Kashino, I.; Goto, A.; Mizoue, T.; Noda, M.; Sawada, N.; Tsugane, S. Japan Public Health Center–based Prospective Study Group. High dietary acid load score is associated with increased risk of type 2 diabetes in Japanese men: The Japan Public Health Center-based Prospective Study. J. Nutr. 2016, 146, 1076–1083. [Google Scholar]
- Kiefte-de Jong, J.C.; Li, Y.; Chen, M.; Curhan, G.C.; Mattei, J.; Malik, V.S.; Forman, J.P.; Franco, O.H.; Hu, F.B. Diet-dependent acid load and type 2 diabetes: Pooled results from three prospective cohort studies. Diabetologia 2017, 60, 270–279. [Google Scholar] [CrossRef]
- Malik, V.S.; Li, Y.; Tobias, D.K.; Pan, A.; Hu, F.B. Dietary protein intake and risk of type 2 diabetes in US men and women. Am. J. Epidemiol. 2016, 183, 715–728. [Google Scholar] [CrossRef]
- Farwell, W.R.; Taylor, E.N. Serum bicarbonate, anion gap and insulin resistance in the National Health and Nutrition Examination Survey. Diabet. Med. 2008, 25, 798–804. [Google Scholar] [CrossRef] [PubMed]
- Akter, S.; Eguchi, M.; Kuwahara, K.; Kochi, T.; Ito, R.; Kurotani, K.; Tsuruoka, H.; Nanri, A.; Kabe, I.; Mizoue, T. High dietary acid load is associated with insulin resistance: The Furukawa Nutrition and Health Study. Clin. Nutr. 2016, 35, 453–459. [Google Scholar] [CrossRef] [PubMed]
- Zhang, L.; Curhan, G.C.; Forman, J.P. Diet-dependent net acid load and risk of incident hypertension in United States women. Hypertension 2009, 54, 751–755. [Google Scholar] [CrossRef] [PubMed]
- Akter, S.; Eguchi, M.; Kurotani, K.; Kochi, T.; Pham, N.M.; Ito, R.; Kuwahara, K.; Tsuruoka, H.; Mizoue, T.; Kabe, I.; et al. High dietary acid load is associated with increased prevalence of hypertension: The Furukawa Nutrition and Health Study. Nutrition 2015, 31, 298–303. [Google Scholar] [CrossRef]
- Parohan, M.; Sadeghi, A.; Nasiri, M.; Maleki, V.; Khodadost, M.; Pirouzi, A.; Sadeghi, O. Dietary acid load and risk of hypertension: A systematic review and dose-response meta-analysis of observational studies. Nutr. Metab. Cardiovasc. Dis. 2019, 29, 665–675. [Google Scholar] [CrossRef]
- Murakami, K.; Livingstone, M.B.E.; Okubo, H.; Sasaki, S. Higher dietary acid load is weakly associated with higher adiposity measures and blood pressure in Japanese adults: The National Health and Nutrition Survey. Nutr. Res. 2017, 44, 67–75. [Google Scholar] [CrossRef]
- Remer, T.; Dimitriou, T.; Manz, F. Dietary potential renal acid load and renal net acid excretion in healthy, free-living children and adolescents. Am. J. Clin. Nutr. 2003, 77, 1255–1260. [Google Scholar] [CrossRef]
- Frassetto, L.A.; Todd, K.M.; Morris, R.C., Jr.; Sebastian, A. Estimation of net endogenous noncarbonic acid production in humans from diet potassium and protein contents. Am. J. Clin. Nutr. 1998, 68, 576–583. [Google Scholar] [CrossRef]
- Iwase, H.; Tanaka, M.; Kobayashi, Y.; Wada, S.; Kuwahata, M.; Kido, Y.; Hamaguchi, M.; Asano, M.; Yamazaki, M.; Hasegawa, G.; et al. Lower vegetable protein intake and higher dietary acid load associated with lower carbohydrate intake are risk factors for metabolic syndrome in patients with type 2 diabetes: Post-hoc analysis of a cross-sectional study. J. Diabetes Investig. 2015, 6, 465–472. [Google Scholar] [CrossRef]
- Mozaffari, H.; Namazi, N.; Larijani, B.; Bellissimo, N.; Azadbakht, L. Association of dietary acid load with cardiovascular risk factors and the prevalence of metabolic syndrome in Iranian women: A cross-sectional study. Nutrition 2019, 67–68, 110570. [Google Scholar] [CrossRef]
- Hamajima, N. J-MICC Study Group. The Japan Multi-Institutional Collaborative Cohort Study (J-MICC Study) to detect gene-environment interactions for cancer. Asian Pac. J. Cancer Prev. 2007, 8, 317–323. [Google Scholar] [PubMed]
- Tokudome, Y.; Goto, C.; Imaeda, N.; Hasegawa, T.; Kato, R.; Hirose, K.; Tajima, K.; Tokudome, S. Relative validity of a short food frequency questionnaire for assessing nutrient intake versus three-day weighed diet records in middle-aged Japanese. J. Epidemiol. 2005, 15, 135–145. [Google Scholar] [CrossRef] [PubMed]
- Imaeda, N.; Goto, C.; Tokudome, Y.; Hirose, K.; Tajima, K.; Tokudome, S. Reproducibility of a short food frequency questionnaire for Japanese general population. J. Epidemiol. 2007, 17, 100–107. [Google Scholar] [CrossRef] [PubMed]
- Lauria, M.W.; Moreira, L.M.; Machado-Coelho, G.L.; Neto, R.M.; Soares, M.M.; Ramos, A.V. Ability of body mass index to predict abnormal waist circumference: Receiving operating characteristics analysis. Diabetol. Metab. Syndr. 2013, 19, 74. [Google Scholar] [CrossRef] [PubMed]
- Iwasaki, Y.; Arisawa, K.; Katsuura-Kamano, S.; Uemura, H.; Tsukamoto, M.; Kadomatsu, Y.; Okada, R.; Hishida, A.; Tanaka, K.; Hara, M.; et al. Associations of nutrient patterns with the prevalence of metabolic syndrome: Results from the baseline data of the Japan Multi-Institutional Collaborative Cohort Study. Nutrients 2019, 30, E990. [Google Scholar] [CrossRef]
- Xu, H.; Jia, T.; Huang, X.; Risérus, U.; Cederholm, T.; Arnlöv, J.; Sjögren, P.; Lindholm, B.; Carrero, J.J. Dietary acid load, insulin sensitivity and risk of type 2 diabetes in community-dwelling older men. Diabetologia 2014, 57, 1561–1568. [Google Scholar] [CrossRef]
- Taylor, E.N.; Forman, J.P.; Farwell, W.R. Serum anion gap and blood pressure in the national health and nutrition examination survey. Hypertension 2007, 50, 320–324. [Google Scholar] [CrossRef]
- Farhangi, M.A.; Nikniaz, L.; Nikniaz, Z. Higher dietary acid load potentially increases serum triglyceride and obesity prevalence in adults: An updated systematic review and meta-analysis. PLoS ONE 2020, 14, e0216547. [Google Scholar] [CrossRef]
- Baldini, N.; Avnet, S. The effects of systemic and local acidosis on insulin resistance and signaling. Int. J. Mol. Sci. 2018, 30, E126. [Google Scholar] [CrossRef]
- Rylander, R.; Remer, T.; Berkemeyer, S.; Vormann, J. Acid-base status affects renal magnesium losses in healthy, elderly persons. J. Nutr. 2006, 136, 2374–2377. [Google Scholar] [CrossRef]
- Barbagallo, M.; Dominguez, L.J. Magnesium and type 2 diabetes. World J. Diabetes 2015, 6, 1152–1157. [Google Scholar] [CrossRef] [PubMed]
- Ahn, C.; Kang, J.H.; Jeung, E.B. Calcium homeostasis in diabetes mellitus. J. Vet. Sci. 2017, 18, 261–266. [Google Scholar] [CrossRef] [PubMed]
- Rice, B.H.; Cifelli, C.J.; Pikosky, M.A.; Miller, G.D. Dairy components and risk factors for cardiometabolic syndrome: Recent evidence and opportunities for future research. Adv. Nutr. 2011, 2, 396–407. [Google Scholar] [CrossRef] [PubMed]
| Q1 (No. = 7036) | Q2 (No. = 7037) | Q3 (No. = 7037) | Q4 (No. = 7037) | p-Value b | |
|---|---|---|---|---|---|
| Age (years) a | 57 (48, 63) | 56 (47, 63) | 55 (46, 62) | 54 (45, 62) | <0.001 |
| Sex | |||||
| Men | 2791 (39.7) | 3486 (49.5) | 3731 (53.0) | 4034 (57.3) | <0.001 |
| Women | 4245 (60.3) | 3551 (50.5) | 3306 (47.0) | 3003 (42.7) | |
| Smoking habit | |||||
| Current | 1018 (14.5) | 1252 (17.8) | 1192 (16.9) | 1227 (17.4) | <0.001 |
| Past | 1430 (20.3) | 1637 (23.3) | 1740 (24.7) | 1929 (27.4) | |
| No | 4588 (65.2) | 4148 (59.0) | 4105 (58.3) | 3881 (55.2) | |
| Drinking habit | |||||
| Current | 3654 (51.9) | 4087 (58.1) | 4247 (60.4) | 4333 (61.6) | <0.001 |
| Past | 107 (1.5) | 119 (1.7) | 105 (1.5) | 116 (1.7) | |
| No | 3275 (46.6) | 2831 (40.2) | 2685 (38.2) | 2588 (36.8) | |
| Exercise during leisure time (MET-hours/week) | 7.65 (0.875, 20.85) | 6.45 (0.425, 18) | 5.1 (0.425, 17.85) | 5.1 (0, 17.6) | <0.001 |
| Body mass index (kg/m2) | 22.4 (20.5, 24.6) | 22.7 (20.7, 24.8) | 22.9 (20.9, 25.1) | 23.0 (21.0, 25.4) | <0.001 |
| Systolic blood pressure (mmHg) | 124 (111, 136) | 124 (112, 136) | 124 (113, 136) | 126 (114, 138) | <0.001 |
| Diastolic blood pressure (mmHg) | 76 (68.5, 83) | 76 (70, 84) | 77 (70, 84) | 78 (70, 85) | <0.001 |
| Serum triglycerides (mg/dL) | 89 (64, 127) | 93 (67, 135) | 95 (67, 137) | 96 (68, 143) | <0.001 |
| Serum HDL cholesterol (mg/dL) | 64 (53, 76) | 63 (52, 75) | 62 (52, 74) | 62 (51, 74) | <0.001 |
| Fasting blood glucose (mg/dL) | 93 (87, 100) | 93 (88, 101) | 94 (88, 102) | 94 (88, 102) | <0.001 |
| Energy intake(kcal/day) | 1683 (1519, 1907) | 1696 (1510, 1933) | 1699 (1509, 1934) | 1686 (1499, 1922) | 0.03 |
| Protein (g/day) | 51 (45, 58) | 52 (46, 58) | 52 (46, 59) | 54 (48, 61) | <0.001 |
| Fat (g/day) | 42 (35, 50) | 42 (36, 49) | 43 (36, 50) | 44 (38, 52) | <0.001 |
| Carbohydrate (g/day) | 241 (212, 282) | 240 (208, 285) | 239 (207, 284) | 234 (201, 276) | <0.001 |
| Soluble dietary fiber (g/day) | 2.2 (1.8, 2.6) | 1.8 (1.5, 2.2) | 1.7 (1.4, 2.1) | 1.7 (1.4, 2.0) | <0.001 |
| Insoluble dietary fiber (g/day) | 8.7(7.2, 10.5) | 7.4 (6.3, 8.7) | 6.9 (6.0, 8.1) | 6.6 (5.8, 7.6) | <0.001 |
| Saturated fatty acids (g/day) | 11(9, 13) | 11 (9, 13) | 11 (9, 13) | 11 (9, 13) | 0.32 |
| Monounsaturated fatty acids (g/day) | 16(13, 19) | 15 (13, 18) | 16 (13, 18) | 16 (14, 19) | <0.001 |
| n-3 polyunsaturated fatty acids (mg/day) | 2164(1831, 2535) | 2135 (1802, 2486) | 2142 (1809, 2527) | 2235 (1911, 2626) | <0.001 |
| n-6 polyunsaturated fatty acids (mg/day) | 11,058(9272, 13,241) | 10,618 (9011, 12,658) | 10,525 (8917, 12,596) | 10,450 (8816, 12,571) | <0.001 |
| Cholesterol (mg/day) | 226(177, 276) | 228 (184, 282) | 235 (185, 288) | 242 (195, 303) | <0.001 |
| Potassium (mg/day) | 2451(2184, 2763) | 2116 (1915, 2337) | 1928 (1736, 2131) | 1718 (1539, 1916) | <0.001 |
| Calcium (mg/day) | 538 (440, 652) | 503 (411, 601) | 481 (394, 571) | 444 (367, 534) | <0.001 |
| Sodium (mg/day) | 1719 (1473, 2065) | 1680 (1437, 1971) | 1665 (1419, 1947) | 1658 (1389, 1949) | <0.001 |
| Beef, pork (times/week) | 1.5 (1.5, 3.5) | 1.5 (1.5, 3.5) | 1.5 (1.5, 3.5) | 1.5 (1.5, 3.5) | <0.001 |
| Fish (times/week) | 1.5 (1.5, 3.5) | 1.5 (1.5, 3.5) | 3.5 (1.5, 3.5) | 3.5 (1.5, 3.5) | <0.001 |
| Milk (times/week) | 3.5 (0.5, 7) | 3.5 (0.5, 7) | 1.5 (0.5, 7) | 1.5 (0, 5.5) | <0.001 |
| Yogurt (times/week) | 1.5 (0.5, 5.5) | 1.5 (0.5, 3.5) | 1.5 (0, 3.5) | 0.5 (0, 3.5) | <0.001 |
| Egg (times/week) | 3.5 (1.5, 3.5) | 3.5 (1.5, 5.5) | 3.5 (1.5, 5.5) | 3.5 (1.5, 5.5) | <0.001 |
| Green leafy vegetables (times/week) | 3.5 (3.5, 7) | 3.5 (1.5, 3.5) | 1.5 (1.5, 3.5) | 1.5 (0.5, 1.5) | <0.001 |
| Green yellow vegetables (times/week) | 3.5 (1.5, 5.5) | 1.5 (1.5, 3.5) | 1.5 (1.5, 3.5) | 1.5 (0.5, 1.5) | <0.001 |
| Cabbage (times/week) | 3.5 (1.5, 5.5) | 3.5 (1.5, 3.5) | 1.5 (1.5, 3.5) | 1.5 (1.5, 3.5) | <0.001 |
| Radish (times/week) | 1.5 (1.5, 3.5) | 1.5 (1.5, 3.5) | 1.5 (0.5, 1.5) | 1.5 (0.5, 1.5) | <0.001 |
| Orange (times/week) | 1.5 (0.5, 5.5) | 1.5 (0.5, 3.5) | 1.5 (0.5, 3.5) | 0.5 (0.5, 1.5) | <0.001 |
| Other fruits (times/week) | 3.5 (0.5, 5.5) | 1.5 (0.5, 3.5) | 1.5 (0.5, 3.5) | 0.5 (0.5, 1.5) | <0.001 |
| Rice (cups/week) | 15.5 (12.5, 19.5) | 14.5 (11.0, 19.5) | 14.0 (11.0, 19.5) | 14.0 (9.0, 16.5) | <0.001 |
| Nutrient pattern scores | |||||
| Factor 1 (fiber, iron, potassium and vitamins pattern) | 0.82 (0.18, 1.45) | 0.10 (–0.48, 0.63) | –0.25 (–0.77, 0.29) | –0.64 (–1.15, –0.14) | <0.001 |
| Factor 2 (fat and fat-soluble vitamins pattern) | –0.24 (–0.91, 0.44) | –0.18 (–0.79, 0.50) | –0.08 (–0.69, 0.62) | 0.21 (–0.39, 0.91) | <0.001 |
| NEAP (mEq/day) | 35.2 (32.0, 37.4) | 42.0 (40.6, 43.5) | 47.5 (46.1, 49.1) | 55.7 (52.9, 59.9) | - |
| Q1 (No. = 7036) | Q2 (No. = 7037) | Q3 (No. = 7037) | Q4 (No. = 7037) | |||
|---|---|---|---|---|---|---|
| OR | OR (95% CI) | OR (95% CI) | OR (95% CI) | p for Trend | ||
| Metabolic syndrome | ||||||
| No. of cases (%) | 977 (13.9) | 1069 (15.2) | 1171 (16.6) | 1410 (20.0) | ||
| Model 1 a | 1.00 | 1.03 (0.93–1.13) | 1.12 (1.02–1.23) | 1.39 (1.26–1.52) | <0.001 | |
| Model 2 b | 1.00 | 0.99 (0.90–1.09) | 1.05 (0.95–1.16) | 1.25 (1.12–1.39) | <0.001 | |
| Model 3 c | 1.00 | 1.02 (0.93–1.13) | 1.11 (1.01–1.22) | 1.35 (1.23–1.49) | <0.001 | |
| Model 4 d | 1.00 | 1.03 (0.94–1.13) | 1.13 (1.02–1.24) | 1.39 (1.27–1.53) | <0.001 | |
| Obesity | ||||||
| No. of cases (%) | 1482 (21.1) | 1631 (23.2) | 1786 (25.4) | 1998 (28.4) | ||
| Model 1 | 1.00 | 1.07 (0.98–1.16) | 1.18 (1.08–1.27) | 1.35 (1.24–1.46) | <0.001 | |
| Model 2 | 1.00 | 1.05 (0.97–1.14) | 1.14 (1.04–1.24) | 1.27 (1.16–1.39) | <0.001 | |
| Model 3 | 1.00 | 1.06 (0.98–1.15) | 1.17 (1.07–1.26) | 1.31 (1.21–1.42) | <0.001 | |
| Model 4 | 1.00 | 1.07 (0.98–1.16) | 1.18 (1.09–1.28) | 1.35 (1.25–1.47) | <0.001 | |
| High blood pressure | ||||||
| No. of cases (%) | 3124 (44.4) | 3133 (44.5) | 3325 (47.3) | 3444 (48.9) | ||
| Model 1 | 1.00 | 0.99 (0.92 – 1.06) | 1.11 (1.03–1.19) | 1.21 (1.12–1.30) | <0.001 | |
| Model 2 | 1.00 | 0.95 (0.88 – 1.03) | 1.04 (0.96–1.13) | 1.10 (1.01–1.19) | 0.005 | |
| Model 3 | 1.00 | 0.98 (0.91 – 1.05) | 1.09 (1.02–1.18) | 1.18 (1.09–1.27) | <0.001 | |
| Model 4 | 1.00 | 0.98 (0.91 – 1.05) | 1.10 (1.02–1.18) | 1.18 (1.10–1.27) | <0.001 | |
| High serum triglycerides | ||||||
| No. of cases (%) | 1177 (16.7) | 1366 (19.4) | 1426 (20.3) | 1619 (23.0) | ||
| Model 1 | 1.00 | 1.07 (0.98–1.17) | 1.08 (0.99–1.19) | 1.21 (1.11–1.32) | <0.001 | |
| Model 2 | 1.00 | 1.01 (0.92–1.11) | 1.00 (0.91–1.10) | 1.08 (0.98–1.20) | 0.13 | |
| Model 3 | 1.00 | 1.06 (0.97–1.16) | 1.08 (0.99–1.18) | 1.21 (1.10–1.32) | <0.001 | |
| Model 4 | 1.00 | 1.07 (0.98–1.17) | 1.09 (1.00–1.19) | 1.22 (1.12–1.33) | <0.001 | |
| Low HDL cholesterol | ||||||
| No. of cases (%) | 637 (9.1) | 600 (8.5) | 569 (8.1) | 595 (8.5) | ||
| Model 1 | 1.00 | 0.99 (0.88–1.12) | 0.97 (0.86–1.09) | 1.05 (0.93–1.19) | 0.54 | |
| Model 2 | 1.00 | 0.95 (0.84–1.07) | 0.90 (0.79–1.03) | 0.96 (0.84–1.11) | 0.49 | |
| Model 3 | 1.00 | 0.99 (0.88–1.12) | 0.97 (0.85–1.09) | 1.05 (0.93–1.19) | 0.53 | |
| Model 4 | 1.00 | 1.02 (0.91–1.15) | 1.01 (0.89–1.14) | 1.14 (1.01–1.29) | 0.06 | |
| High blood glucose | ||||||
| No. of cases (%) | 1893 (26.9) | 2024 (28.8) | 2161 (30.7) | 2304 (32.7) | ||
| Model 1 | 1.00 | 1.04 (0.96–1.12) | 1.14 (1.05–1.23) | 1.26 (1.17–1.36) | <0.001 | |
| Model 2 | 1.00 | 1.01 (0.93–1.10) | 1.09 (1.00–1.18) | 1.17 (1.07–1.28) | <0.001 | |
| Model 3 | 1.00 | 1.04 (0.96–1.12) | 1.13 (1.05–1.23) | 1.25 (1.16–1.36) | <0.001 | |
| Model 4 | 1.00 | 1.04 (0.96–1.12) | 1.13 (1.05–1.22) | 1.25 (1.15–1.35) | <0.001 | |
| OR | OR (95% CI) | OR (95% CI) | OR (95% CI) | p for Trend | p Interaction | |
|---|---|---|---|---|---|---|
| Men | Q1 (No. = 3510) | Q2 (No. = 3511) | Q3 (No. = 3510) | Q4 (No. = 3511) | ||
| No. of cases (%) | 721 (20.5) | 723 (20.6) | 786 (22.4) | 925 (26.3) | ||
| Model 1 a | 1.00 | 1.00 (0.89–1.12) | 1.11 (0.99–1.24) | 1.38 (1.23–1.55) | <0.001 | 0.61 d |
| Model 2 b | 1.00 | 0.96 (0.85–1.08) | 1.03 (0.91–1.17) | 1.23 (1.08–1.40) | <0.001 | 0.75 |
| Womenc | Q1 (No. = 3526) | Q2 (No. = 3526) | Q3 (No. = 3526) | Q4 (No. = 3527) | ||
| No. of cases (%) | 349 (9.9) | 351 (10.0) | 344 (9.8) | 428 (12.1) | ||
| Model 1 | 1.00 | 1.04 (0.89–1.22) | 1.02 (0.87–1.20) | 1.41 (1.20–1.64) | <0.001 | |
| Model 2 | 1.00 | 0.98 (0.83–1.16) | 0.93 (0.78–1.11) | 1.21 (1.01–1.46) | 0.05 | |
| Age <55 years | Q1 (No. = 3342) | Q2 (No. = 3342) | Q3 (No. = 3342) | Q4 (No. = 3342) | ||
| No. of cases (%) | 363 (10.9) | 415 (12.4) | 453 (13.6) | 514 (15.4) | ||
| Model 1 | 1.00 | 1.03 (0.88–1.20) | 1.12 (0.96–1.31) | 1.30 (1.12–1.52) | <0.001 | 0.44 e |
| Model 2 | 1.00 | 1.00 (0.85–1.17) | 1.06 (0.90–1.25) | 1.19 (1.01–1.41) | 0.02 | 0.33 |
| Age ≥55 years | Q1 (No. = 3694) | Q2 (No. = 3695) | Q3 (No. = 3695) | Q4 (No. = 3695) | ||
| No. of cases (%) | 582 (15.8) | 675 (18.3) | 708 (19.2) | 917 (24.8) | ||
| Model 1 | 1.00 | 1.08 (0.96–1.23) | 1.11 (0.98–1.26) | 1.46 (1.29–1.65) | <0.001 | |
| Model 2 | 1.00 | 1.03 (0.91–1.18) | 1.02 (0.89–1.17) | 1.30 (1.13–1.49) | <0.001 | |
| BMI < 25 kg/m2 | Q1 (No. = 5312) | Q2 (No. = 5313) | Q3 (No. = 5312) | Q4 (No. = 5313) | ||
| No. of cases (%) | 242 (4.6) | 266 (5.0) | 245 (4.6) | 348 (6.5) | ||
| Model 1 | 1.00 | 1.04 (0.87–1.25) | 0.95 (0.79–1.14) | 1.37 (1.15–1.63) | 0.001 | 0.34 f |
| Model 2 | 1.00 | 1.00 (0.83–1.21) | 0.88 (0.72–1.07) | 1.22 (1.00–1.50) | 0.08 | 0.34 |
| BMI ≥ 25 kg/m2 c | Q1 (No. = 1724) | Q2 (No. = 1724) | Q3 (No. = 1724) | Q4 (No. = 1725) | ||
| No. of cases (%) | 843 (48.9) | 835 (48.4) | 917 (53.2) | 931 (54.0) | ||
| Model 1 | 1.00 | 0.95 (0.83–1.09) | 1.13 (0.98–1.29) | 1.19 (1.03–1.37) | 0.003 | |
| Model 2 | 1.00 | 0.93 (0.81–1.08) | 1.09 (0.94–1.27) | 1.14 (0.97–1.33) | 0.03 |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Arisawa, K.; Katsuura-Kamano, S.; Uemura, H.; Van Tien, N.; Hishida, A.; Tamura, T.; Kubo, Y.; Tsukamoto, M.; Tanaka, K.; Hara, M.; et al. Association of Dietary Acid Load with the Prevalence of Metabolic Syndrome among Participants in Baseline Survey of the Japan Multi-Institutional Collaborative Cohort Study. Nutrients 2020, 12, 1605. https://doi.org/10.3390/nu12061605
Arisawa K, Katsuura-Kamano S, Uemura H, Van Tien N, Hishida A, Tamura T, Kubo Y, Tsukamoto M, Tanaka K, Hara M, et al. Association of Dietary Acid Load with the Prevalence of Metabolic Syndrome among Participants in Baseline Survey of the Japan Multi-Institutional Collaborative Cohort Study. Nutrients. 2020; 12(6):1605. https://doi.org/10.3390/nu12061605
Chicago/Turabian StyleArisawa, Kokichi, Sakurako Katsuura-Kamano, Hirokazu Uemura, Nguyen Van Tien, Asahi Hishida, Takashi Tamura, Yoko Kubo, Mineko Tsukamoto, Keitaro Tanaka, Megumi Hara, and et al. 2020. "Association of Dietary Acid Load with the Prevalence of Metabolic Syndrome among Participants in Baseline Survey of the Japan Multi-Institutional Collaborative Cohort Study" Nutrients 12, no. 6: 1605. https://doi.org/10.3390/nu12061605
APA StyleArisawa, K., Katsuura-Kamano, S., Uemura, H., Van Tien, N., Hishida, A., Tamura, T., Kubo, Y., Tsukamoto, M., Tanaka, K., Hara, M., Takezaki, T., Nishimoto, D., Koyama, T., Ozaki, E., Suzuki, S., Nishiyama, T., Kuriki, K., Kadota, A., Takashima, N., ... Wakai, K. (2020). Association of Dietary Acid Load with the Prevalence of Metabolic Syndrome among Participants in Baseline Survey of the Japan Multi-Institutional Collaborative Cohort Study. Nutrients, 12(6), 1605. https://doi.org/10.3390/nu12061605






