Mixing of Apples and Oranges in Milk Research: A Cohort Analysis of Non-Fermented Milk Intake and All-Cause Mortality
Abstract
1. Introduction
2. Materials and Methods
3. Results
4. Discussion
Author Contributions
Funding
Conflicts of Interest
References
- Willett, W.C.; Ludwig, D.S. Milk and Health. N. Engl. J. Med. 2020, 382, 644–654. [Google Scholar] [CrossRef] [PubMed]
- Tognon, G.; Nilsson, L.M.; Shungin, D.; Lissner, L.; Jansson, J.H.; Renstrom, F.; Wennberg, M.; Winkvist, A.; Johansson, I. Nonfermented milk and other dairy products: Associations with all-cause mortality. Am. J. Clin. Nutr. 2017, 105, 1502–1511. [Google Scholar] [CrossRef] [PubMed]
- Ding, M.; Li, J.; Qi, L.; Ellervik, C.; Zhang, X.; Manson, J.E.; Stampfer, M.; Chavarro, J.E.; Rexrode, K.M.; Kraft, P.; et al. Associations of dairy intake with risk of mortality in women and men: Three prospective cohort studies. BMJ 2019, 367, l6204. [Google Scholar] [CrossRef] [PubMed]
- Michaëlsson, K.; Wolk, A.; Langenskiöld, S.; Basu, S.; Warensjö Lemming, E.; Melhus, H.; Byberg, L. Milk intake and risk of mortality and fractures in women and men: Cohort studies. BMJ 2014, 349, g6015. [Google Scholar] [CrossRef] [PubMed]
- Larsson, S.C.; Andersson, S.O.; Johansson, J.E.; Wolk, A. Cultured milk, yoghurt, and dairy intake in relation to bladder cancer risk in a prospective study of Swedish women and men. Am. J. Clin. Nutr. 2008, 88, 1083–1087. [Google Scholar] [CrossRef] [PubMed]
- Wang, C.; Yatsuya, H.; Tamakoshi, K.; Iso, H.; Tamakoshi, A. Milk drinking and mortality: Findings from the Japan collaborative cohort study. J. Epidemiol. 2015, 25, 66–73. [Google Scholar] [CrossRef] [PubMed]
- Michaelsson, K.; Byberg, L. Interpretation of milk research results. Osteoporos. Int. 2018, 29, 773–775. [Google Scholar] [CrossRef] [PubMed]
- Kirkpatrick, S.I.; Dodd, K.W.; Reedy, J.; Krebs-Smith, S.M. Income and race/ethnicity are associated with adherence to food-based dietary guidance among US adults and children. J. Acad. Nutr. Diet. 2012, 112, 624–635.e626. [Google Scholar] [CrossRef] [PubMed]
- Dubois, L.; Girard, M. Social position and nutrition: A gradient relationship in Canada and the USA. Eur. J. Clin. Nutr. 2001, 55, 366–373. [Google Scholar] [CrossRef] [PubMed]
- Lee, S.; Kawachi, I.; Berkman, L.F.; Grodstein, F. Education, other socioeconomic indicators, and cognitive function. Am. J. Epidemiol. 2003, 157, 712–720. [Google Scholar] [CrossRef] [PubMed]
- Melnik, B.C.; Schmitz, G. MicroRNAs: Milk’s epigenetic regulators. Best Pract. Res. Clin. Endocrinol. Metab. 2017, 31, 427–442. [Google Scholar] [CrossRef] [PubMed]
- Melnik, B.C. Milk—A nutrient system of mammalian evolution promoting mTORC1-dependent translation. Int. J. Mol. Sci. 2015, 16, 17048–17087. [Google Scholar] [CrossRef] [PubMed]
| Categories of Total Milk Intake | ||||
|---|---|---|---|---|
| <1 Glass/Day | 1 to <2 Glasses/Day | 2 To <3 Glasses/Day | ≥3 Glasses/Day | |
| (<200 mL/Day) | (200–399 mL/Day) | (400–599 mL/Day) | (≥600 mL/Day) | |
| N | 16,926 | 23,438 | 15,461 | 5608 |
| Age (years) at entry | 53.2 (9.6) | 54.0 (9.7) | 54.1 (9.9) | 52.8 (9.6) |
| Body mass index (kg/m2) | 24.4 (3.9) | 24.7 (3.8) | 25.0 (4.0) | 24.9 (4.2) |
| Height (m) | 1.64 (0.06) | 1.64 (0.06) | 1.64 (0.06) | 1.64 (0.06) |
| Total milk intake (mL/day) | 17.3 (37.3) | 201.6 (14.9) | 400.2 (6.0) | 676.8 (151.9) |
| Low fat (0.5%) milk intake (mL/day) | 6.4 (24.2) | 81.1 (99.4) | 176.5 (198.8) | 288.9 (345.5) |
| Medium fat (1.5%) milk intake (mL/day) | 5.7 (23.6) | 56.9 (91.0) | 102.4 (174.8) | 154.6 (292.1) |
| High fat (3%) milk intake (mL/day) | 5.3 (19.6) | 63.7 (93.5) | 121.1 (183.8) | 233.8 (338.1) |
| Soured milk/yogurt, mean (SD) | 102.4 (117.2) | 97.6 (101.2) | 93.3 (105.1) | 87.0 (113.1) |
| Cheese, gram/day, mean (SD) | 26.8 (21.3) | 26.2 (19.6) | 26.8 (19.9) | 27.7 (22.0) |
| Energy intake (kcal/day) | 1412 (433) | 1535 (414) | 1707 (435) | 1965 (527) |
| Calcium intake (mg/day) | 716 (221) | 895 (192) | 1043 (202) | 1194 (245) |
| Education (≤9 years) n (%) | 13,094 (78.9) | 18,497 (80.3) | 12,388 (81.6) | 4377 (79.3) |
| Education (10–12 years) n (%) | 1259 (7.6) | 1576 (6.8) | 972 (6.4) | 368 (6.7) |
| Education (>12 years) n (%) | 868 (5.2) | 1106 (4.8) | 594 (3.9) | 254 (4.6) |
| Education (other) n (%) | 1375 (8.3) | 1867 (8.1) | 1232 (8.1) | 519 (9.4) |
| Married/cohabiting n (%) | 12,814 (76.4) | 17,932 (77.2) | 11,565 (75.5) | 4117 (74.1) |
| 0 Charlson comorbidities n (%) | 15,745 (93.0) | 21,884 (93.4) | 14,385 (93.0) | 5146 (91.8) |
| 1 Charlson comorbidity n (%) | 1048 (6.2) | 1350 (5.8) | 927 (6.0) | 390 (7.0) |
| 2 or more Charlson comorbidities n (%) | 133 (0.8) | 204 (0.9) | 149 (1.0) | 72 (1.3) |
| Low Fat Milk (0.5% fat) | |||||
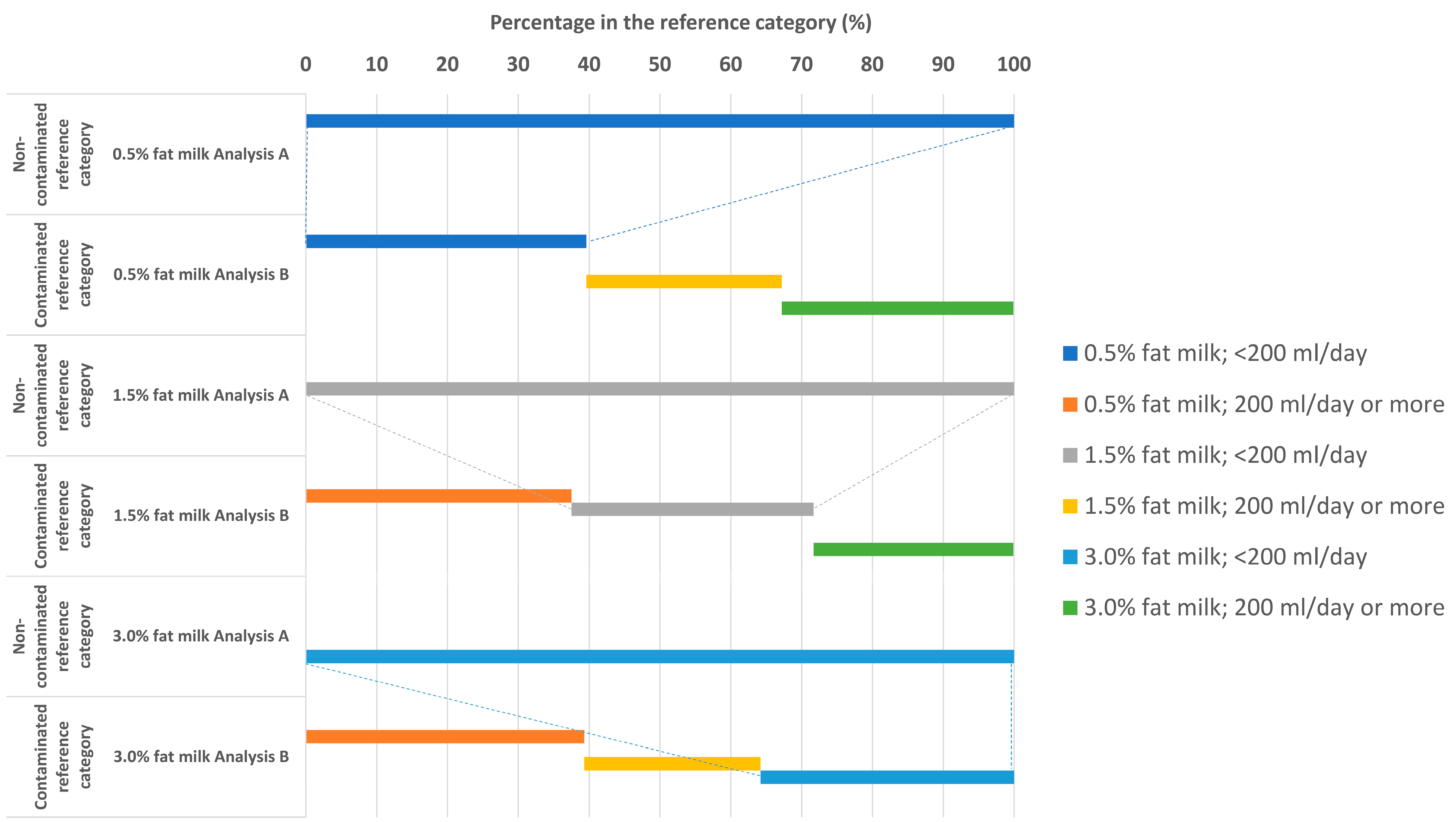
| (A) Restriction to Those Consuming Less than One Serving Per Day of Other Types of Milk (1.5% or 3% fat) | |||||
| Milk Intake Category (0.5% fat) | |||||
| <200 mL/day | 200–399 mL/day | 400–599 mL/day | ≥600 mL/day | Per 200 mL/day (continuous) | |
| N deaths | 7650 | 3119 | 1804 | 598 | 13,171 |
| Person-years at risk | 534,282 | 215,813 | 118,779 | 39,127 | 908,001 |
| Death rate (95% CI) | 14.3 | 14.5 | 15.2 | 15.3 | 14.5 |
| HR (95% CI), model 1 | 1.00 (1.00–1.00) | 1.15 (1.10–1.20) | 1.55 (1.48–1.64) | 1.90 (1.75–2.06) | 1.14 (1.12–1.16) |
| HR (95% CI), model 2 | 1.00 (1.00–1.00) | 1.11 (1.07–1.16) | 1.39 (1.32–1.47) | 1.71 (1.57–1.86) | 1.12 (1.10–1.14) |
| (B) Retain All Types of Milk Consumers in the Analysis (full Cohort; “Contaminated” Reference Category) | |||||
| Milk Intake Category (0.5% fat) | |||||
| <200 mL/day | 200–399 mL/day | 400–599 mL/day | ≥600 mL/day | Per 200 mL/day | |
| N deaths | 16,292 | 3518 | 2028 | 683 | 22,521 |
| Person-years at risk | 1,031,416 | 235,664 | 128,988 | 42,608 | 1,438,676 |
| Death rate (95% CI) | 15.8 | 14.9 | 15.7 | 16.0 | 15.7 |
| HR (95% CI), model 1 | 1.00 (1.00–1.00) | 0.92 (0.89–0.95) | 1.19 (1.13–1.24) | 1.38 (1.28–1.50) | 0.99 (0.98–1.01) |
| HR (95% CI), model 2 | 1.00 (1.00–1.00) | 0.96 (0.92–0.99) | 1.14 (1.09–1.20) | 1.34 (1.24–1.45) | 1.02 (1.00–1.03) |
| HR (95% CI), model 3 | 1.00 (1.00–1.00) | 0.98 (0.95–1.02) | 1.19 (1.14–1.25) | 1.41 (1.30–1.52) | 1.02 (1.00–1.03) |
| Medium Fat Milk (1.5% fat) | |||||
| (A) Restriction to Those Consuming less than One Serving Per day of Other Types of Milk (0.5% or 3% fat) | |||||
| Milk Intake Category (1.5% fat) | |||||
| <200 mL/day | 200–399 mL/day | 400–599 mL/day | ≥600 mL/day | Per 200 mL/day | |
| N deaths | 7650 | 2220 | 1177 | 357 | 11,404 |
| Person-years at risk | 534,282 | 135,782 | 65,636 | 20,109 | 755,809 |
| Death rate (95% CI) | 14.3 | 16.3 | 17.9 | 17.8 | 15.1 |
| HR (95% CI), model 1 | 1.00 (1.00–1.00) | 1.25 (1.19–1.31) | 1.75 (1.64–1.86) | 2.10 (1.89–2.34) | 1.19 (1.16–1.21) |
| HR (95% CI), model 2 | 1.00 (1.00–1.00) | 1.21 (1.15–1.27) | 1.54 (1.44–1.64) | 1.82 (1.63–2.04) | 1.15 (1.13–1.18) |
| (B) Retain all Types of Milk Consumers in the Analysis (Full Cohort; “Contaminated” Reference Category) | |||||
| Milk Intake Category (1.5% fat) | |||||
| <200 mL/day | 200–399 mL/day | 400–599 mL/day | ≥600 mL/day | Per 200 mL/day | |
| N deaths | 17,683 | 2926 | 1462 | 450 | 22,521 |
| Person-years at risk | 1,168,398 | 168,026 | 78,108 | 24,143 | 1,438,676 |
| Death rate (95% CI) | 15.1 | 17.4 | 18.7 | 18.6 | 15.7 |
| HR (95% CI), model 1 | 1.00 (1.00–1.00) | 0.93 (0.90–0.97) | 1.22 (1.16–1.29) | 1.47 (1.34–1.61) | 0.98 (0.96–1.00) |
| HR (95% CI), model 2 | 1.00 (1.00–1.00) | 0.97 (0.93–1.00) | 1.17 (1.11–1.24) | 1.38 (1.25–1.51) | 1.00 (0.98–1.02) |
| HR (95% CI), model 3 | 1.00 (1.00–1.00) | 0.96 (0.93–1.00) | 1.19 (1.13–1.26) | 1.38 (1.25–1.52) | 0.99 (0.97–1.01) |
| High Fat Milk (3% fat) | |||||
| (A) Restriction to Those Consuming Less than One Serving Per Day of Other Types of Milk (0.5% or 1.5% fat) | |||||
| Milk Intake Category (3% fat) | |||||
| <200 mL/day | 200–399 mL/day | 400–599 mL/day | ≥600 mL/day | Per 200 mL/day | |
| N deaths | 7650 | 2464 | 1402 | 518 | 12,034 |
| Person-years at risk | 534,282 | 144,657 | 78,282 | 30,487 | 787,708 |
| Death rate (95% CI) | 14.3 | 17.0 | 17.9 | 17.0 | 15.3 |
| HR (95% CI), model 1 | 1.00 (1.00–1.00) | 1.45 (1.39–1.52) | 1.99 (1.88–2.11) | 2.52 (2.30–2.76) | 1.31 (1.29–1.34) |
| HR (95% CI), model 2 | 1.00 (1.00–1.00) | 1.24 (1.18–1.30) | 1.60 (1.50–1.70) | 1.95 (1.77–2.15) | 1.20 (1.18–1.23) |
| (B) Retain All Types of Milk Consumers in the Analysis (Full Cohort; “Contaminated” Reference Category) | |||||
| Milk Intake Category (3% fat) | |||||
| <200 mL/day | 200–399 mL/day | 400–599 mL/day | ≥600 mL/day | Per 200 mL/day | |
| N deaths | 17,183 | 2977 | 1725 | 636 | 22,521 |
| Person-years at risk | 1,142,947 | 166,735 | 92,019 | 36,975 | 1,438,676 |
| Death rate (95% CI) | 15.0 | 17.9 | 18.7 | 17.2 | 15.7 |
| HR (95% CI), model 1 | 1.00 (1.00–1.00) | 1.11 (1.06–1.15) | 1.40 (1.33–1.47) | 1.61 (1.49–1.74) | 1.11 (1.09–1.13) |
| HR (95% CI), model 2 | 1.00 (1.00–1.00) | 1.02 (0.98–1.06) | 1.21 (1.15–1.27) | 1.40 (1.29–1.52) | 1.05 (1.04–1.07) |
| HR (95% CI), model 3 | 1.00 (1.00–1.00) | 1.05 (1.01–1.10) | 1.27 (1.21–1.34) | 1.47 (1.35–1.60) | 1.07 (1.05–1.08) |
| Total Milk Intake | Milk Intake Category (any fat content) | ||||
| <200 mL/day | 200–399 mL/day | 400–599 mL/day | ≥600 mL/day | Per 200 mL/day | |
| N deaths | 8332 | 8381 | 4296 | 1512 | 22,521 |
| Person-years at risk | 573,831 | 515,685 | 258,732 | 90,429 | 1,438,676 |
| Death rate (95% CI) | 14.5 | 16.3 | 16.6 | 16.7 | 15.7 |
| HR (95% CI), model 1 | 1.00 (1.00–1.00) | 1.28 (1.24–1.32) | 1.81 (1.74–1.87) | 2.18 (2.06–2.30) | 1.18 (1.16–1.19) |
| HR (95% CI), model 2 | 1.00 (1.00–1.00) | 1.18 (1.14–1.22) | 1.55 (1.49–1.61) | 1.83 (1.72–1.94) | 1.13 (1.11–1.15) |
| HR (95% CI), model 3 | 1.00 (1.00–1.00) | 1.19 (1.15–1.23) | 1.58 (1.51–1.64) | 1.84 (1.74–1.96) | 1.13 (1.11–1.14) |
| Type of Milk by Fat Content (Differences in mL/Day) | ||||
|---|---|---|---|---|
| Total | 0.5% Fat | 1.5% Fat | 3% Fat | |
| Education | ||||
| ≤9 years | reference | reference | reference | reference |
| 10–12 years | −13.0 (−19.5 to −6.6) | −0.6 (−6.3 to 5.1) | −1.1 (−5.7 to 3.5) | −9.9 (−15.1 to −4.7) |
| >12 years | −19.4 (−27.1 to −11.6) | −3.9 (−10.8 to 2.9) | 7.9 (2.4 to 13.5) | −20.3 (−26.5 to −14.0) |
| Other | 2.8 (−3.1 to 8.8) | −3.2 (−8.4 to 2.0) | 7.0 (2.8 to 11.3) | −0.6 (−5.4 to 4.1) |
| Marital status | ||||
| Married or cohabiting | reference | reference | reference | reference |
| Unmarried or living alone | 12.7 (8.9 to 16.6) | −13.0 (−16.4 to −9.7) | 10.1 (7.4 to 12.8) | 13.3 (10.3 to 16.4) |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Michaëlsson, K.; Byberg, L. Mixing of Apples and Oranges in Milk Research: A Cohort Analysis of Non-Fermented Milk Intake and All-Cause Mortality. Nutrients 2020, 12, 1393. https://doi.org/10.3390/nu12051393
Michaëlsson K, Byberg L. Mixing of Apples and Oranges in Milk Research: A Cohort Analysis of Non-Fermented Milk Intake and All-Cause Mortality. Nutrients. 2020; 12(5):1393. https://doi.org/10.3390/nu12051393
Chicago/Turabian StyleMichaëlsson, Karl, and Liisa Byberg. 2020. "Mixing of Apples and Oranges in Milk Research: A Cohort Analysis of Non-Fermented Milk Intake and All-Cause Mortality" Nutrients 12, no. 5: 1393. https://doi.org/10.3390/nu12051393
APA StyleMichaëlsson, K., & Byberg, L. (2020). Mixing of Apples and Oranges in Milk Research: A Cohort Analysis of Non-Fermented Milk Intake and All-Cause Mortality. Nutrients, 12(5), 1393. https://doi.org/10.3390/nu12051393






