Nutritional Aspects in Inflammatory Bowel Diseases
Abstract
1. Introduction:
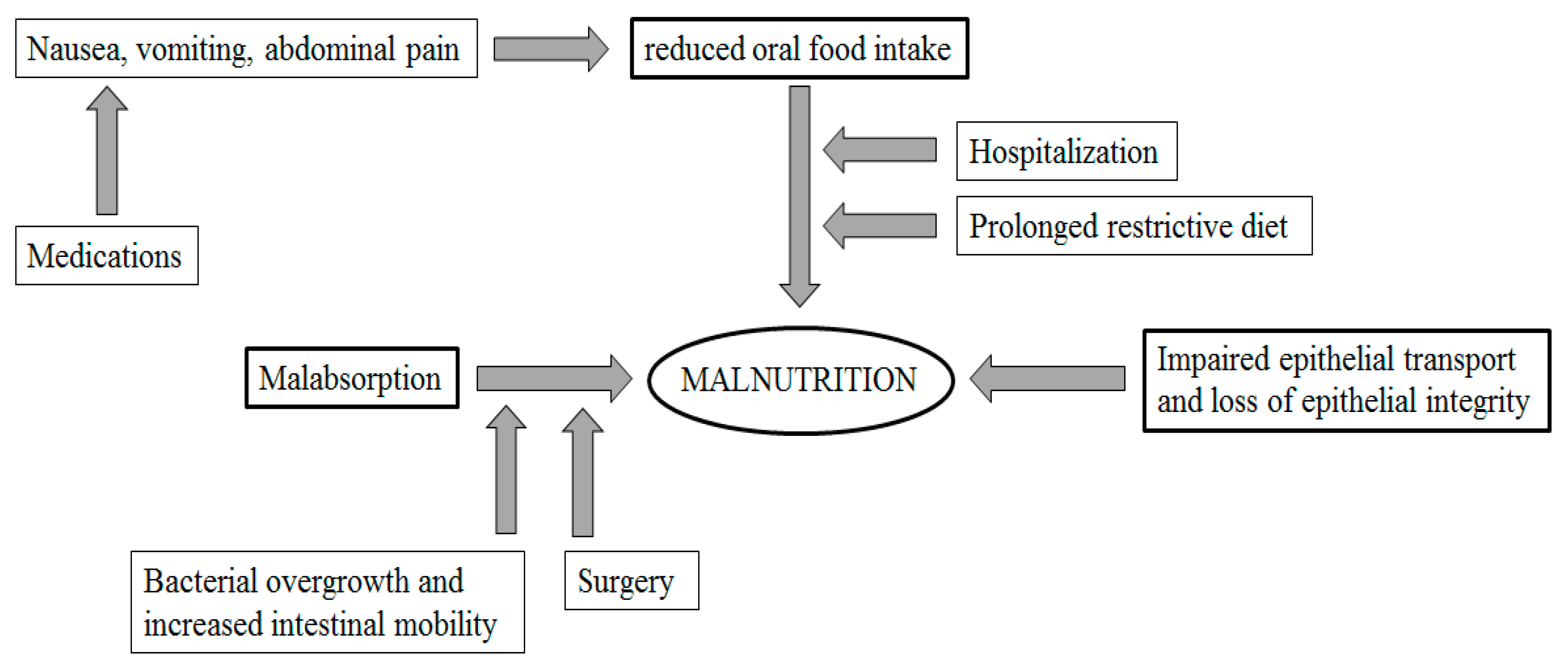
2. Mechanisms of Malnutrition in IBD
3. Clinical Aspects of Malnutrition in Patients with IBD
4. Overview of Nutritional Assessment
5. Role of Diet in IBD
6. Nutritional Treatment in the Management of IBD
7. Conclusions
Author Contributions
Funding
Conflicts of Interest
References
- Goh, J.; O’Morain, C.A. Review article: Nutrition and adult inflammatory bowel disease. Aliment. Pharmacol. Ther. 2003, 17, 307–320. [Google Scholar] [CrossRef]
- Clare, F.; Donnellan, L.H.; Simon, L. Nutritional management of Crohn’s disease. Ther. Adv. Gastroenterol. 2013, 6, 231–242. [Google Scholar]
- Lanfranchi, G.A.; Brignola, C.; Campieri, M.; Bazzocchi, G.; Pasquali, R.; Bassein, L.; Labo, G. Assessment of nutritional status in Crohn’s disease in remission or low activity. Hepatogastroenterology 1984, 31, 129–132. [Google Scholar] [PubMed]
- Hartman, C.; Eliakim, R.; Shamir, R. Nutritional status and nutritional therapy in inflammatory bowel diseases. World J. Gastroenterol. 2009, 15, 2570–2578. [Google Scholar] [CrossRef] [PubMed]
- Hanauer, S.B.; Stathopoulos, G. Risk benefit assessment of drugs used in the treatment of inflammatory bowel disease. Drug Saf. 1991, 6, 192–219. [Google Scholar] [CrossRef] [PubMed]
- Singleton, J.W.; Law, D.H.; Kelley, M.L., Jr.; Mekhjian, H.S.; Sturdevant, R.A. National Cooperative Crohn’s Disease Study: Adverse reactions to study drugs. Gastroenterology 1979, 77, 870–882. [Google Scholar] [CrossRef]
- H’ebuterne, F.J.; Al-Jaouni, R.; Schneider, S. Nutritional consequences and nutrition therapy in Crohn’s disease. Gastroenterol. Clin. Biol. 2009, 33, S235–S244. [Google Scholar] [CrossRef]
- Lucendo, A.J.; De Rezende, L.C. Importance of nutrition in inflammatory bowel disease. World J. Gastroenterol. 2009, 15, 2081–2088. [Google Scholar] [CrossRef]
- Capristo, E.; Addolorato, G.; Mingrone, G.; Greco, A.V.; Gasbarrini, G. Effect of disease localization on the anthropometric and metabolic features of Crohn’s disease. Am. J. Gastroenterol. 1998, 93, 2411–2419. [Google Scholar] [CrossRef]
- Morris, T.H.; Sorensen, S.H.; Turkington, J.; Batt, R.M. Diarrhoea and increased intestinal permeability in laboratory beagles associated with proximal small intestinal bacterial overgrowth. Lab. Anim. 1994, 28, 313–319. [Google Scholar] [CrossRef]
- MacMahon, M.; Lynch, M.; Mullins, E. Small intestinal bacterial overgrowth—An incidental finding? J. Am. Geriatr. Soc. 1994, 42, 146–149. [Google Scholar] [CrossRef]
- May, G.R.; Sutherland, L.R.; Meddings, J.B. Is small intestinal permeability really increased in relatives of patients with Crohn’s disease? Gastroenterology 1993, 104, 1627–1632. [Google Scholar] [CrossRef]
- Hollander, D. Permeability in Crohn’s disease: Altered barrier functions in healthy relatives? Gastroenterology 1993, 104, 1848–1851. [Google Scholar] [CrossRef]
- Riordan, S.M.; Mclver, C.J.; Thomas, D.H.; Duncombe, V.M.; Bolin, T.D.; Thomas, M.C. Luminal bacteria and small-intestinal permeability. Scand J. Gastroenterol. 1997, 32, 556–563. [Google Scholar] [CrossRef] [PubMed]
- Saltzman, J.R.; Russell, R.M. Nutral consequences of intestinal bacterial overgrowth. Compr.Ther. 1994, 20, 523. [Google Scholar] [PubMed]
- Hoverstad, T.; Bjorneklett, A.; Fausa, O.; Midtvedt, T. Shortchain fatty acids in the small-bowel bacterial overgrowth syndrome. Scand J. Gastroenterol. 1985, 20, 492–499. [Google Scholar] [CrossRef]
- Fromm, H.; Malavolti, M. Bile acid-induced diarrhoea. Clin. Gastroenterol. 1986, 15, 567–582. [Google Scholar]
- Hafkenscheid, J.C. Influence of bile acids on the (Na+-K+)-activated- and Mg2+-activated ATPase of rat colon. Pflugers. Arch. Eur. J. Physiol. 1977, 369, 203–206. [Google Scholar] [CrossRef]
- Kirwan, W.O.; Smith, A.N.; Mitchell, W.D.; Falconer, J.D.; Eastwood, M.A. Bile acids and colonic motility in the rabbit and the human. Gut 1975, 16, 894–902. [Google Scholar] [CrossRef]
- Krag, B.; Krag, E. Regional ileitis (Crohn’s disease). II. Electrolyte and water movement in the ileum during perfusion with bile acids. Scand J. Gastroenterol. 1976, 11, 487–490. [Google Scholar]
- Hofmann, A.F.; Poley, J.R. Role of bile acid malabsorption in pathogenesis of diarrhea and steatorrhea in patients with ileal resection. I. Response to cholestyramine or replacement of dietary long chain triglyceride by medium chain triglyceride. Gastroenterology 1972, 62, 918–934. [Google Scholar] [CrossRef]
- Hofmann, A.F.; Poley, J.R. Cholestyramine treatment of diarrhea associated with ileal resection. N. Engl. J. Med. 1969, 281, 397–402. [Google Scholar] [CrossRef] [PubMed]
- Borgstrom, B.; Lundh, G.; Hofmann, A. The site of absorption of conjugated bile salts in man. Gastroenterology 1963, 45, 229–238. [Google Scholar] [CrossRef]
- Jansen, I.; Prager, M.; Valentini, L.; Büning, C. Inflammation-driven malnutrition: A new screening tool predicts outcome in Crohn’s disease. Br. J. Nutr. 2016, 116, 1061–1067. [Google Scholar] [CrossRef] [PubMed]
- Takaoka, A.; Sasaki, M.; Nakanishi, N.; Kurihara, M.; Ohi, A.; Bamba, S.; Andoh, A. Nutritional Screening and Clinical Outcome in Hospitalized Patients with Crohn’s Disease. Ann. Nutr. Metab. 2017, 71, 266–272. [Google Scholar] [CrossRef] [PubMed]
- Cabré, E.; Gassull, M.A. Nutrition in inflammatory bowel disease: Impact on disease and therapy. Curr. Opin. Gastroenterol. 2001, 17, 342–349. [Google Scholar] [CrossRef] [PubMed]
- Han, P.D.; Burke, A.; Baldassano, R.N.; Rombeau, J.L.; Lichtenstein, G.R. Nutrition and inflammatory bowel disease. Gastroenterol. Clin. N. Am. 1999, 28, 423–443. [Google Scholar] [CrossRef]
- Bryant, R.V.; Trott, M.J.; Bartholomeusz, F.D.; Andrews, J.M. Systematic review: Body composition in adults with inflammatory bowel disease. Aliment. Pharmacol. Ther. 2013, 38, 213–225. [Google Scholar] [CrossRef]
- Tandon, P.; Raman, M.; Mourtzakis, M.; Merli, M. A Practical Approach to Nutritional Screening and Assessment in Cirrhosis. Hepatology 2017, 65, 1044–1057. [Google Scholar] [CrossRef]
- Seong, H.K.; Woo, K.J.; Soon, K.B.; Seung, H.C.; Moon, Y.K. Impact of sarcopenia on prognostic value of cirrhosis: Going beyond the hepatic venous pressure gradient and MELD score. J. Cachexia Sarcopenia Muscle 2018, 9, 860–870. [Google Scholar]
- Anna, E.B.; Nilay, H.; Samantha, K.; Matthew, M. Sarcopenia and frailty in chronic respiratory disease. Chron Respir. Dis. 2017, 14, 85–99. [Google Scholar]
- Biolo, G.; Cederholm, T.; Muscaritoli, M. Muscle contractile and metabolic dysfunction is a common feature of sarcopenia of aging and chronic diseases: From sarcopenic obesity to cachexia. Clin. Nutr. 2014, 33, 737–748. [Google Scholar] [CrossRef] [PubMed]
- Ryan, E.; McNicholas, D.; Creavin, B.; Kelly, M.E.; Walsh, T.; Beddy, D. Sarcopenia and Inflammatory Bowel Disease: A Systematic Review. Inflamm. Bowel Dis. 2019, 25, 67–73. [Google Scholar] [CrossRef]
- Adams, D.W.; Gurwara, S.; Silver, H.J. Sarcopenia is common in overweight patients with inflammatory bowel disease and may predict need for surgery. Inflamm. Bowel Dis. 2017, 23, 1182–1186. [Google Scholar] [CrossRef] [PubMed]
- Pedersen, M.; Cromwell, J.; Nau, P. Sarcopenia is a predictor of surgical morbidity in inflammatory bowel disease. Inflamm. Bowel Dis. 2017, 23, 1867–1872. [Google Scholar] [CrossRef]
- Bryant, R.V.; Ooi, S.; Schultzetal, C.G. Low muscle mass and sarcopenia: Common and predictive of osteopenia in inflammatory bowel disease. Aliment. Pharmacol. Ther. 2015, 41, 895–906. [Google Scholar] [CrossRef]
- Weisshof, R.; Chermes, I. Micronutrient deficiencies in inflammatory bowel disease. Curr. Opin. Clin. Nutr. Metab Care 2015, 18, 576–581. [Google Scholar] [CrossRef]
- Hwang, C.; Ross, V.; Mahadevan, U. Micronutrient deficiencies in inflammatory bowel disease: From A to zinc. Inflamm. Bowel Dis. 2012, 18, 1961–1981. [Google Scholar] [CrossRef]
- Gasche, C. Anemia in IBD: The overlooked villain. Inflamm. Bowel Dis. 2000, 6, 142–150. [Google Scholar] [CrossRef]
- Kulnigg, S.; Gasche, C. Systematic review: Managing anemia in Crohn’s disease. Aliment. Pharmacol. Ther. 2006, 24, 1507–1523. [Google Scholar] [CrossRef]
- Gisbert, J.P.; Gomollon, F. Common misconceptions in the diagnosis and management of anemia in inflammatory bowel disease. Am. J. Gastroenterol. 2008, 103, 1299–1307. [Google Scholar] [CrossRef] [PubMed]
- Goodhand, J.R.; Kamperidis, N.; Rao, A.; Laskaratos, F.; McDermott, A.; Wahed, M.; Naik, S.; Croft, N.M.; Lindsay, J.O.; Sanderson, I.R.; et al. Prevalence and management of anemia in children, adolescents, and adults with inflammatory bowel disease. Inflamm. Bowel Dis. 2012, 18, 513–519. [Google Scholar] [CrossRef] [PubMed]
- Gomollón, F.; Gisbert, J.P. Anemia and inflammatory bowel diseases. World J. Gastroenterol. 2009, 15, 4659e65. [Google Scholar] [CrossRef] [PubMed]
- Dignass, A.U.; Gasche, C.; Bettenworth, D.; Birgegård, G.; Danese, S.; Gisbert, J.P.; Gomollon, F.; Iqbal, T.; Katsanos, K.; Koutroubakis, I.; et al. European consensus on the diagnosis and management of iron deficiency and anaemia in inflammatory bowel diseases. J. Crohns Colitis 2015, 9, 211–222. [Google Scholar] [CrossRef] [PubMed]
- Massironi, S.; Rossi, R.E.; Cavalcoli, F.A.; Della Valle, S.; Fraquelli, M.; Conte, D. Nutritional deficiencies in inflammatory bowel disease: Therapeutic Approaches. Clin. Nutr. 2013, 32, 904–910. [Google Scholar] [CrossRef] [PubMed]
- Cantorna, M.T.; Zhu, Y.; Froicu, M.; Wittke, A. Vitamin D status, 1,25-dihydroxyvitamin D3, and the immune system. Am. J. Clin. Nutr. 2004, 80, 1717S–1720S. [Google Scholar] [CrossRef] [PubMed]
- Cantorna, M.T.; Mahon, B.D. D-hormone and the immune system. J. Rheumatol. Suppl. 2005, 76, 11–20. [Google Scholar]
- Ananthakrishnan, A.N.; Khalili, H.; Higuchi, L.M.; Bao, Y.; Korzenik, J.R.; Giovannucci, E.L.; Richter, J.M.; Fuchs, C.S.; Chan, A.T. Higher predicted vitamin d status is associated with reduced risk of Crohn’s disease. Gastroenterology 2012, 142, 482–489. [Google Scholar] [CrossRef]
- Yakut, M.; Ustün, Y.; Kabaçam, G.; Soykan, I. Serum vitamin B12 and folate status in patients with inflammatory bowel diseases. Eur. J. Intern. Med. 2010, 21, 320–323. [Google Scholar] [CrossRef]
- Talbot, R.W.; Heppell, J.; Dozois, R.R.; Beart, R.W., Jr. Vascular complications of inflammatory bowel disease. Mayo Clin. Proc. 1986, 61, 140–145. [Google Scholar] [CrossRef]
- Pohl, C.; Hombach, A.; Kruis, W. Chronic inflammatory bowel disease and cancer. Hepatogastroenterology 2000, 47, 57–70. [Google Scholar] [PubMed]
- Bermejo, F.; Algaba, A.; Guerra, I.; Chaparro, M.; De-La-Poza, G.; Valer, P.; Piqueras, B.; Bermejo, A.; García-Alonso, J.; Pérez, M.J.; et al. Should we monitor vitamin B12 and folate levels in Crohn’s disease patients? Scand. J. Gastroenterol. 2013, 11, 1272–1277. [Google Scholar] [CrossRef] [PubMed]
- Pan, Y.; Liu, Y.; Guo, H.; Jabir, M.S.; Liu, X.; Cui, W.; Li, D. Associations between Folate and Vitamin B12 Levels and Inflammatory Bowel Disease: A Meta-Analysis. Nutrients 2017, 13, 382. [Google Scholar] [CrossRef] [PubMed]
- Erzin, Y.; Uzun, H.; Celik, F.; Aydin, S.; Dirican, A.; Uzunismail, H. Hyperhomocysteinemia in inflammatory bowel disease patients without past intestinal resections: Correlations with cobalamin, pyridoxine, folate concentrations, acute phase reactants, disease activity, and prior thromboembolic complications. J. Gastroenterol. 2008, 42, 481–486. [Google Scholar] [CrossRef]
- Mowat, C.; Cole, A.; Windsor, A.; Ahmad, T.; Arnott, I.; Driscoll, R.; Mitton, S.; Orchard, T.; Rutter, M.; Younge, L.; et al. Guidelines for the management of Inflammatory Bowel Disease in adults. Gut 2011, 60, 571–607. [Google Scholar] [CrossRef]
- Lochs, H. Nutritional support in inflammatory bowel disease. In Basics in Clinical Nutrition, 3rd ed.; Sobotka, L., Ed.; Galen: Prague, Czech Republic, 2004; pp. 314–321. [Google Scholar]
- Mijač, D.D.; Janković, G.L.; Jorga, J.; Krstić, M.N. Nutritional status in patients with active inflammatory bowel disease: prevalence of malnutrition and methods for routine nutritional assessment. Eur. J. Intern. Med. 2010, 21, 315–319. [Google Scholar] [CrossRef]
- Cruz-Jentoft, A.J.; Baeyens, J.P.; Bauer, J.M. European Working Group on Sarcopenia in Older People. Sarcopenia: European consensus on definition and diagnosis: Report of the European Working Group on Sarcopenia in Older People. Age Ageing 2010, 39, 412–423. [Google Scholar] [CrossRef]
- Megan, P.R. Body Composition Measured by Dual-energy X-ray Absorptiometry Half-body Scans in Obese Adults. Obesity 2009, 17, 1281–1286. [Google Scholar]
- Emerenziani, S.; Biancone, L.; Guarino, M.P.L.; Balestrieri, P.; Stasi, E.; Ribolsi, M.; Rescio, M.P.; Altomare, A.; Cocca, S.; Pallone, F.; et al. Nutritional status and bioelectrical phase angle assessment in adult Crohn disease patients receiving anti-TNFα therapy. Dig. Liver Dis. 2017, 49, 495–499. [Google Scholar] [CrossRef]
- Kalyani, R.R.; Corriere, M.; Ferrucci, L.; Tandon, P. Age-related and disease muscle loss: the effect of diabetes, obesity, and other diseases. Lancet Diabetes Endocrinol. 2014, 2, 819–829. [Google Scholar] [CrossRef]
- Barbat-Artigas, S.; Rolland, Y.; Zamboni, M.; Aubertin-Leheudre, M. How to assess functional status: A new muscle quality index. J. Nutr. Health Aging 2012, 16, 67–77. [Google Scholar] [CrossRef]
- Goodpaster, B.H.; Park, S.W.; Harris, T.B.; Kritchevsky, S.B.; Nevitt, M.; Schwartz, A.V. The loss of skeletal muscle strength, mass, and quality in older adults: The health, aging and body composition study. J. Gerontol. A Biol. Sci. Med. Sci. 2006, 61, 1059–1064. [Google Scholar] [CrossRef] [PubMed]
- Brown, A.C.; Rampertab, S.D.; Mullin, G.E. Existing dietary guidelines for Crohn’s disease and ulcerative colitis. Expert Rev. Gastroenterol. Hepatol. 2011, 5, 411–425. [Google Scholar] [CrossRef] [PubMed]
- Hwang, C.; Ross, V.; Mahadevan, U. Popular exclusionary diets for inflammatory bowel disease: The search for a dietary culprit. Inflamm. Bowel Dis. 2014, 20, 732–741. [Google Scholar] [CrossRef] [PubMed]
- Levenstein, S.; Prantera, C.; Luzi, C.; D’Ubaldi, A. Low residue or normal diet in Crohn’s disease: A prospective controlled study in Italian patients. Gut 1985, 26, 989–993. [Google Scholar] [CrossRef] [PubMed]
- Brotherton, C.S.; Martin, C.A.; Long, M.D.; Kappelman, M.D.; Sandler, R.S. Avoidance of fiber is associated with greater risk of crohn’s disease flare in a 6-month period. Clin. Gastroenterol. Hepatol. 2016, 14, 1130–1136. [Google Scholar] [CrossRef]
- Jowett, S.L.; Seal, C.J.; Pearce, M.S.; Phillips, E.; Gregory, W.; Barton, J.R.; Welfare, M.R. Influence of dietary factors on the clinical course of ulcerative colitis: A prospective cohort study. Gut 2004, 53, 1479–1484. [Google Scholar] [CrossRef]
- Prince, A.C.; Myers, C.E.; Joyce, T.; Irving, P.; Lomer, M.; Whelan, K. Fermentable carbohydrate restriction (low fodmap diet) in clinical practice improves functional gastrointestinal symptoms in patients with inflammatory bowel disease. Inflamm. Bowel Dis. 2016, 22, 1129–1136. [Google Scholar] [CrossRef]
- Penagini, F.; Dilillo, D.; Borsani, B.; Cococcioni, L.; Galli, E.; Bedogni, G.; Zuin, G.; Zuccotti, G.V. Nutrition in pediatric inflammatory bowel disease: from etiology to treatment. A systematic review. Nutrients 2016, 8, 334. [Google Scholar] [CrossRef]
- Società Italiana di Nutrizione Parenterale e Enterale (SINPE). Linee Guida SINPE per la Nutrizione Artificiale Ospedaliera 2002. Rivista Italiana di Nutrizione Parenterale e Enterale 2002, S5, S5e8. [Google Scholar]
- Muller, C.; Compher, D.; Druyan, M.E.; the American Society for Parenteral and Enteral Nutrition (ASPEN). ASPEN Clinical Guidelines: Nutrition screening, assessment, and intervention in adults. J. Parenter Enteral. Nutr. 2011, 35, 16e24. [Google Scholar]
- Bannerjee, K.; Camacho-Hübner, C.; Babinsk, K.; Dryhurst, K.M.; Edwards, R.; Savage, M.O. Anti-inflammatory and growth-stimulating effects precede nutritional restitution during enteral feeding in Crohn’s disease. J. Pedriatr. Gastroenterol. Nutr. 2004, 38, 270–275. [Google Scholar] [CrossRef] [PubMed]
- Guagnozzi, D.; González-Castillo, S.; Olveira, A.; Lucendo, A.J. Nutritional treatment in inflammatory bowel disease. An update. Rev. Esp. Enferm. Dig. 2012, 104, 479–488. [Google Scholar] [CrossRef] [PubMed]
- Griffiths, A.M.; Ohlsson, A.; Sherman, P.M.; Sutherland, L.R. Meta-analysis of enteral nutrition as a primary treatment of active Crohn’s disease. Gastroenterology 1995, 108, 1056e67. [Google Scholar] [CrossRef]
- Zachos, M.; Tondeur, M.; Griffiths, A.M. Enteral nutritional therapy for induction of remission in Crohn’s disease. Cochrane Database Syst. Rev. 2007, 1, CD000542. [Google Scholar] [CrossRef]
- Dziechciarz, P.; Horvath, A.; Shamir, R.; Szajewska, H. Meta-analysis: Enteral nutrition in active Crohn’s disease in children. Aliment. Pharmacol. Ther. 2007, 26, 795e806. [Google Scholar] [CrossRef]
- Heuschkel, R.B.; Menache, C.C.; Megerian, J.T.; Baird, A.E. Enteral nutrition and corticosteroids in the treatment of acute Crohn’s disease in children. J. Pediatr. Gastroenterol. Nutr. 2000, 31, 8e15. [Google Scholar] [CrossRef]
- Forbes, A.; Escher, J.; Hébuterne, X.; Kłęk, S.; Krznaric, Z.; Schneider, S.; Shamir, R.; Stardelova, K.; Wierdsma, N.; Wiskin, A.E. ESPEN guideline: Clinical nutrition in inflammatory bowel disease. Clin. Nutr. 2017, 36, 321–347. [Google Scholar] [CrossRef]
- Nguyen, G.C.; Laveist, T.A.; Brant, S.R. The utilization of parenteral nutrition during the in-patient management of inflammatory bowel disease in the United States: A national survey. Aliment. Pharmacol. Ther. 2007, 26, 1499e50. [Google Scholar] [CrossRef]
| Frequency | ||
|---|---|---|
| CD | UC | |
| Weight loss | 65%–75% | 18%–62% |
| Anemia | 60%-80% | 66% |
| Iron deficiency | 39% | 81% |
| Vitamin B12 deficiency | 48% | 5% |
| Folic acid deficiency | 54% | 36% |
| Calcium deficiency | 13% | ND |
| Vitamin D deficiency | 75% | ND |
| Magnesium deficiency | 14%–33% | ND |
| Vitamin K deficiency | ND | ND |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Balestrieri, P.; Ribolsi, M.; Guarino, M.P.L.; Emerenziani, S.; Altomare, A.; Cicala, M. Nutritional Aspects in Inflammatory Bowel Diseases. Nutrients 2020, 12, 372. https://doi.org/10.3390/nu12020372
Balestrieri P, Ribolsi M, Guarino MPL, Emerenziani S, Altomare A, Cicala M. Nutritional Aspects in Inflammatory Bowel Diseases. Nutrients. 2020; 12(2):372. https://doi.org/10.3390/nu12020372
Chicago/Turabian StyleBalestrieri, Paola, Mentore Ribolsi, Michele Pier Luca Guarino, Sara Emerenziani, Annamaria Altomare, and Michele Cicala. 2020. "Nutritional Aspects in Inflammatory Bowel Diseases" Nutrients 12, no. 2: 372. https://doi.org/10.3390/nu12020372
APA StyleBalestrieri, P., Ribolsi, M., Guarino, M. P. L., Emerenziani, S., Altomare, A., & Cicala, M. (2020). Nutritional Aspects in Inflammatory Bowel Diseases. Nutrients, 12(2), 372. https://doi.org/10.3390/nu12020372






