Effects of Continuous Intake of Rosemary Extracts on Mental Health in Working Generation Healthy Japanese Men: Post-Hoc Testing of a Randomized Controlled Trial
Abstract
1. Introduction
2. Materials and Methods
2.1. Study Protocol and Participants
2.2. Test Foods
2.3. Survey Questionnaires
2.4. Statistical Analysis
3. Results
3.1. Baseline Characteristics
3.2. POMS T-Scores Pre- and Post-Intervention
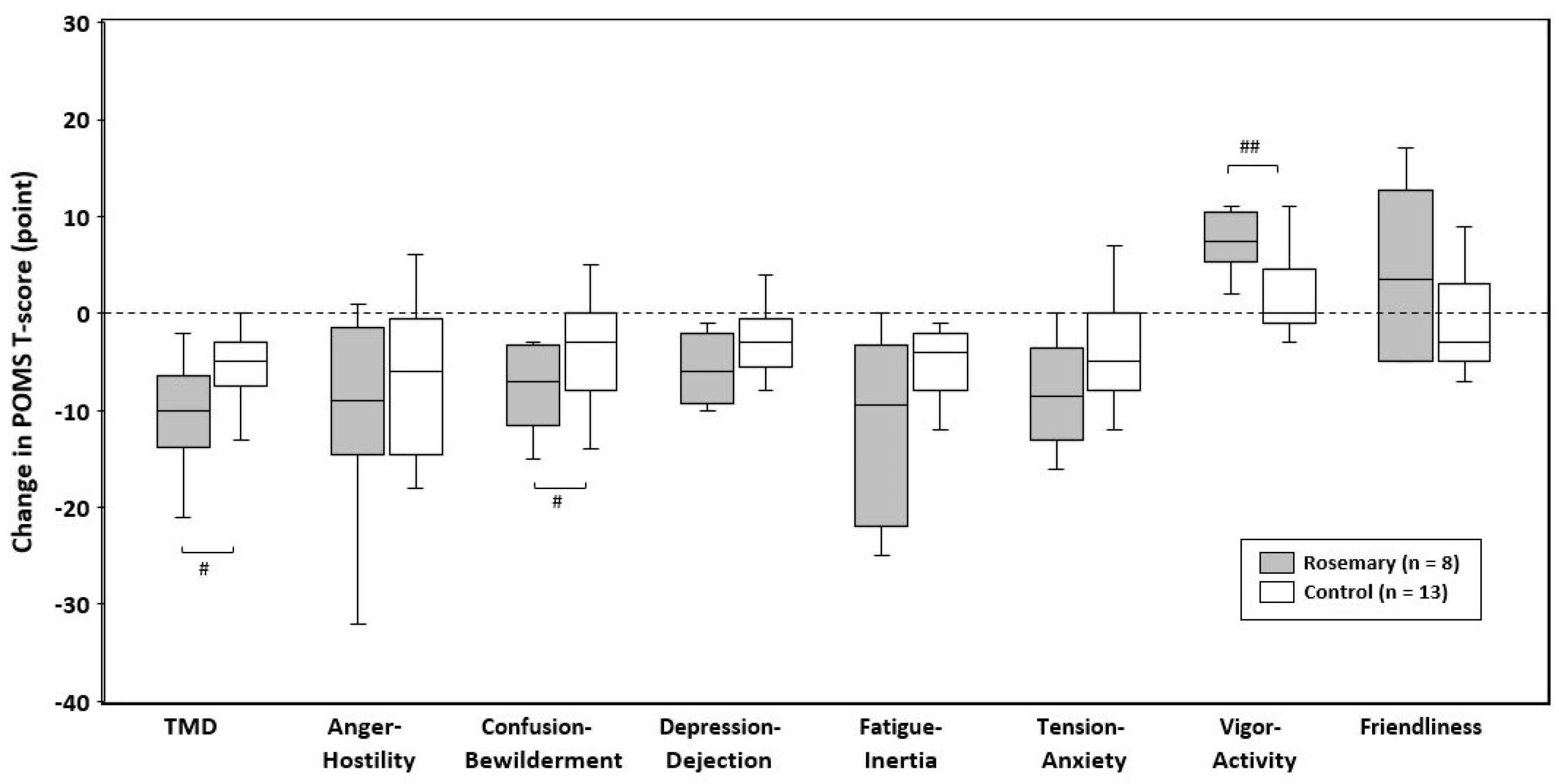
3.3. Changes in POMS T-Scores during the Intervention
3.4. VAS Scores Pre- and Post-Intervention
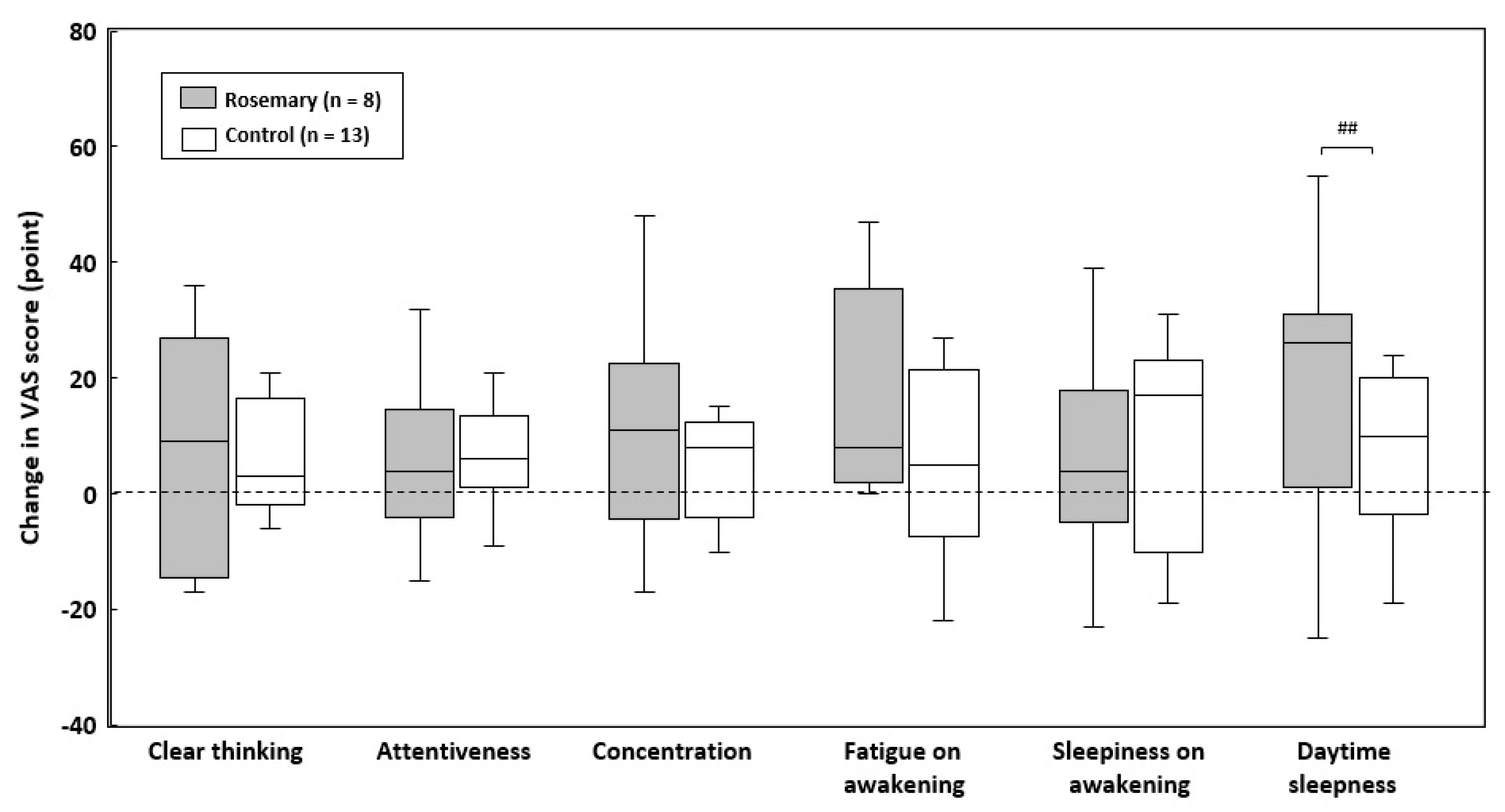
3.5. Changes in VAS Scores during the Intervention
3.6. NCI and Cognitive Domain Scores Calculated in Cognitrax Pre- and Post-Intervention
4. Discussion
5. Conclusions
Author Contributions
Funding
Conflicts of Interest
References
- La Torre, G.; Sestili, C.; Mannocci, A.; Sinopoli, A.; De Paolis, M.; De Francesco, S.; Rapaccini, L.; Barone, M.; Iodice, V.; Lojodice, B.; et al. Association between Work Related Stress and Health Related Quality of Life: The Impact of Socio-Demographic Variables. A Cross Sectional Study in a Region of Central Italy. Int. J. Environ. Res. Public Health 2018, 15, 159. [Google Scholar] [CrossRef] [PubMed]
- Patrão, A.L.; Almeida, M.C.; Matos, S.M.A.; Chor, D.; Aquino, E.M.L. Work-related stress and cognitive performance among middle-aged adults: The Brazilian longitudinal study of adult health (ELSA-Brasil). BMJ Open 2017, 7, e015705. [Google Scholar] [CrossRef] [PubMed]
- Rajgopal, T. Mental well-being at the workplace. Indian J. Occup. Environ. Med. 2010, 14, 63–65. [Google Scholar] [CrossRef] [PubMed]
- Nowakowska-Domagala, K.; Jablkowska-Górecka, K.; Kostrzanowska-Jarmakowska, L.; Mortoń, M.; Stecz, P. The Interrelationships of Coping Styles and Professional Burnout among Physiotherapists. Medicine 2015, 94, e906. [Google Scholar] [CrossRef] [PubMed]
- Rose, D.M.; Seidler, A.; Nübling, M.; Latza, U.; Brähler, E.; Klein, E.M.; Wiltink, J.; Michal, M.; Nickels, S.; Wild, P.; et al. Associations of fatigue to work-related stress, mental and physical health in an employed community sample. BMC Psychiatry 2017, 17, 167. [Google Scholar] [CrossRef] [PubMed]
- Jason, L.A.; Porter, N.; Herrington, J.; Sorenson, M.; Kubow, S. Kindling and Oxidative Stress as Contributors to Myalgic Encephalomyelitis/Chronic Fatigue Syndrome. J. Behav. Neurosci. Res. 2009, 7, 1–17. [Google Scholar] [PubMed]
- Li, Y.; Sun, X.; Ge, H.; Liu, J.-W.; Chen, L. The Status of Occupational Stress and Its Influence the Quality of Life of Copper-Nickel Miners in Xinjiang, China. Int. J. Environ. Res. Public Health 2019, 16, 353. [Google Scholar] [CrossRef]
- Jang, Y.-G.; Hwang, K.-A.; Choi, K. Rosmarinic Acid, a Component of Rosemary Tea, Induced the Cell Cycle Arrest and Apoptosis through Modulation of HDAC2 Expression in Prostate Cancer Cell Lines. Nutrients 2018, 10, 1784. [Google Scholar] [CrossRef]
- Andrade, J.M.; Faustino, C.; Garcia, C.; Ladeiras, D.; Reis, C.P.; Rijo, P. Rosmarinus officinalis L.: An update review of its phytochemistry and biological activity. Futur. Sci. OA 2018, 4, FSO283. [Google Scholar] [CrossRef]
- Sasaki, K.; El Omri, A.; Kondo, S.; Han, J.; Isoda, H. Rosmarinus officinalis polyphenols produce anti-depressant like effect through monoaminergic and cholinergic functions modulation. Behav. Brain Res. 2013, 238, 86–94. [Google Scholar] [CrossRef]
- Kondo, S.; El Omri, A.; Han, J.; Isoda, H. Antidepressant-like effects of rosmarinic acid through mitogen-activated protein kinase phosphatase-1 and brain-derived neurotrophic factor modulation. J. Funct. Foods 2015, 14, 758–766. [Google Scholar] [CrossRef]
- Rasoolijazi, H.; Mehdizadeh, M.; Soleimani, M.; Nikbakht, F.; Farsani, M.E.; Ababzadeh, S. The effect of rosemary extract on spatial memory, learning and antioxidant enzymes activities in the hippocampus of middle-aged rats. Med. J. Islam. Repub. Iran. 2015, 29, 187. [Google Scholar] [PubMed]
- Farr, S.A.; Niehoff, M.L.; Ceddia, M.A.; Herrlinger, K.A.; Lewis, B.J.; Feng, S.; Welleford, A.S.; Butterfield, D.A.; Morley, J.E. Effect of botanical extracts containing carnosic acid or rosmarinic acid on learning and memory in SAMP8 mice. Physiol. Behav. 2016, 165, 328–338. [Google Scholar] [CrossRef] [PubMed]
- Nematolahi, P.; Mehrabani, M.; Karami-Mohajeri, S.; Dabaghzadeh, F. Effects of Rosmarinus officinalis L. on memory performance, anxiety, depression, and sleep quality in university students: A randomized clinical trial. Complement. Ther. Clin. Pr. 2018, 30, 24–28. [Google Scholar] [CrossRef]
- Perry, N.; Menzies, R.; Hodgson, F.; Wedgewood, P.; Howes, M.-J.; Brooker, H.; Wesnes, K.; Perry, E. A randomised double-blind placebo-controlled pilot trial of a combined extract of sage, rosemary and melissa, traditional herbal medicines, on the enhancement of memory in normal healthy subjects, including influence of age. Phytomedicine 2018, 39, 42–48. [Google Scholar] [CrossRef]
- Lindheimer, J.B.; Loy, B.D.; O’Connor, P.J. Short-Term Effects of Black Pepper (Piper nigrum) and Rosemary (Rosmarinus officinalis and Rosmarinus eriocalyx) on Sustained Attention and on Energy and Fatigue Mood States in Young Adults with Low Energy. J. Med. Food 2013, 16, 765–771. [Google Scholar] [CrossRef]
- Pengelly, A.; Snow, J.; Mills, S.Y.; Scholey, A.; Wesnes, K.; Butler, L.R. Short-Term Study on the Effects of Rosemary on Cognitive Function in an Elderly Population. J. Med. Food 2012, 15, 10–17. [Google Scholar] [CrossRef]
- Araki, R.; Sasaki, K.; Onda, H.; Nakamura, S.; Kassai, M.; Kaneko, T.; Isoda, H.; Hashimoto, K. Continuous intake of rosemary extracts may improve the mood states, fatigue, and cognitive function of healthy adult Japanese men. Pharmacometrics 2020, 98, 61–68. (In Japanese) [Google Scholar]
- Fuller-Thomson, E.; Nimigon, J. Factors associated with depression among individuals with chronic fatigue syndrome: Findings from a nationally representative survey. Fam. Pr. 2008, 25, 414–422. [Google Scholar] [CrossRef]
- Heuchert, J.P.; McNair, D.M. Profile of Mood States, 2nd ed.; POMS 2; Multi-Health Systems Inc.: North Tonawanda, NY, USA, 2012. [Google Scholar]
- Nieto, G.; Ros, G.; Castillo, J. Antioxidant and Antimicrobial Properties of Rosemary (Rosmarinus officinalis, L.): A Review. Medicines 2018, 5, 98. [Google Scholar] [CrossRef]
- Nie, J.; Li, R.; Wang, Y.; Tan, J.; Tang, S.; Jiang, Z.-T. Antioxidant activity evaluation of rosemary ethanol extract and their cellular antioxidant activity toward HeLa cells. J. Food Biochem. 2019, 43, e12851. [Google Scholar] [CrossRef] [PubMed]
- Gualtieri, C.T.; Johnson, L.G. Reliability and validity of a computerized neurocognitive test battery, CNS Vital Signs. Arch. Clin. Neuropsychol. 2006, 21, 623–643. [Google Scholar] [CrossRef] [PubMed]
- Kurebayashi, Y.; Otaki, J. Correlations between physical activity and neurocognitive domain functions in patients with schizophrenia: A cross-sectional study. BMC Psychiatry 2017, 17, 4. [Google Scholar] [CrossRef] [PubMed]
- Saitou, K.; Ochiai, R.; Kozuma, K.; Sato, H.; Koikeda, T.; Osaki, N.; Katsuragi, Y. Effect of Chlorogenic Acids on Cognitive Function: A Randomized, Double-Blind, Placebo-Controlled Trial. Nutrients 2018, 10, 1337. [Google Scholar] [CrossRef] [PubMed]
- Beck, A.T.; Steer, R.A.; Brown, G.K. Manual for Beck Depression Inventory-II; Psychological Corporation: New York, NY, USA, 1996. [Google Scholar]
- Boolani, A.; O’Connor, P.J.; Reid, J.; Ma, S.; Mondal, S. Predictors of feelings of energy differ from predictors of fatigue. Fatigue Biomed. Health Behav. 2018, 7, 12–28. [Google Scholar] [CrossRef]
- Takeuchi, H.; Taki, Y.; Nouchi, R.; Yokoyama, R.; Kotozaki, Y.; Nakagawa, S.; Sekiguchi, A.; Iizuka, K.; Yamamoto, Y.; Hanawa, S.; et al. Shorter sleep duration and better sleep quality are associated with greater tissue density in the brain. Sci. Rep. 2018, 8, 5833. [Google Scholar] [CrossRef]
- Kreibig, S.D. Autonomic nervous system activity in emotion: A review. Biol. Psychol. 2010, 84, 394–421. [Google Scholar] [CrossRef]
- El Omri, A.; Han, J.; Yamada, P.; Kawada, K.; Abdrabbah, M.B.; Isoda, H. Rosmarinus Officinalis polyphenols activate cholinergic activities in PC12 cells through phosphorylation of ERK1/2. J. Ethnopharmacol. 2010, 131, 451–458. [Google Scholar] [CrossRef]
- Gustafson, K.M.; Colombo, J.; Carlson, S.E. Docosahexaenoic acid and cognitive function: Is the link mediated by the autonomic nervous system? Prostaglandins Leukot. Essent. Fat. Acids 2008, 79, 135–140. [Google Scholar] [CrossRef]
- Spirduso, W.W. Physical Fitness, Aging, and Psychomotor Speed: A Review. J. Gerontol. 1980, 35, 850–865. [Google Scholar] [CrossRef]
- Lin, Y.-T.; Wu, Y.-C.; Sun, G.-C.; Ho, C.-Y.; Wong, T.-Y.; Lin, C.-H.; Chen, H.-H.; Yeh, T.-C.; Li, C.-J.; Tseng, C.-J.; et al. Effect of Resveratrol on Reactive Oxygen Species-Induced Cognitive Impairment in Rats with Angiotensin II-Ind uced Early Alzheimer’s Disease. J. Clin. Med. 2018, 7, 329. [Google Scholar] [CrossRef] [PubMed]
- Euston, D.R.; Gruber, A.J.; McNaughton, B.L. The Role of Medial Prefrontal Cortex in Memory and Decision Making. Neuron 2012, 76, 1057–1070. [Google Scholar] [CrossRef] [PubMed]
- Ochsner, K.N.; Hughes, B.; Robertson, E.R.; Cooper, J.C.; Gabrieli, J.D.E. Neural Systems Supporting the Control of Affective and Cognitive Conflicts. J. Cogn. Neurosci. 2009, 21, 1841–1854. [Google Scholar] [CrossRef] [PubMed]
- El Omri, A.; Han, J.; Ben Abdrabbah, M.; Isoda, H. Down regulation effect of Rosmarinus officinalis polyphenols on cellular stress proteins in rat pheochromocytoma PC12 cells. Cytotechnology 2011, 64, 231–240. [Google Scholar] [CrossRef][Green Version]
- Ghaffari, H.; Venkataramana, M.; Ghassam, B.J.; Nayaka, S.C.; Nataraju, A.; Geetha, N.; Prakash, H.S. Rosmarinic acid mediated neuroprotective effects against H2O2-induced neuronal cell damage in N2A cells. Life Sci. 2014, 113, 7–13. [Google Scholar] [CrossRef]
- Qu, L.; Xu, H.; Jia, W.; Jiang, H.; Xie, J. Rosmarinic acid protects against MPTP-induced toxicity and inhibits iron-induced α-synuclein aggregation. Neuropharmacology 2019, 144, 291–300. [Google Scholar] [CrossRef]
- Ito, N.; Yabe, T.; Gamo, Y.; Nagai, T.; Oikawa, T.; Yamada, H.; Hanawa, T. Rosmarinic Acid from Perillae Herba Produces an Antidepressant-Like Effect in Mice through Cell Proliferation in the Hippocampus. Biol. Pharm. Bull. 2008, 31, 1376–1380. [Google Scholar] [CrossRef]
- Ghazizadeh, J.; Hamedeyazdan, S.; Torbati, M.; Farajdokht, F.; Fakhari, A.; Mahmoudi, J.; Araj-Khodaei, M.; Sadigh-Eteghad, S. Melissa officinalis L. Hydro-alcoholic extract inhibits anxiety and depression through prevention of central oxidative stress and apoptosis. Exp. Physiol. 2020, 105, 707–720. [Google Scholar] [CrossRef]
- Herman, J.P.; McKlveen, J.M.; Ghosal, S.; Kopp, B.; Wulsin, A.; Makinson, R.; Scheimann, J.; Myers, B. Regulation of the Hypothalamic-Pituitary-Adrenocortical Stress Response. Compr. Physiol. 2016, 6, 603–621. [Google Scholar] [CrossRef]
- Moss, M.; Oliver, L. Plasma 1,8-cineole correlates with cognitive performance following exposure to rosemary essential oil aroma. Ther. Adv. Psychopharmacol. 2012, 2, 103–113. [Google Scholar] [CrossRef]
- Maynard, M.E.; Underwood, E.L.; Redell, J.B.; Zhao, J.; Kobori, N.; Hood, K.N.; Moore, A.N.; Dash, P.K. Carnosic Acid Improves Outcome after Repetitive Mild Traumatic Brain Injury. J. Neurotrauma 2019, 36, 2147–2152. [Google Scholar] [CrossRef] [PubMed]
- Tashjian, S.M.; Galván, A. Neural recruitment related to threat perception differs as a function of adolescent sleep. Dev. Sci. 2020, 23, e12933. [Google Scholar] [CrossRef] [PubMed]

| T-Score (Point) | Rosemary (n = 8) | Control (n = 13) | pb | |
|---|---|---|---|---|
| TMD | 0 week | 57.0 (53.5–59.5) a | 54.0 (54.0–56.0) | 0.374 |
| 4 week | 47.5 (45.0–50.5) * | 50.0 (48.0–51.0) ** | 0.051 c | |
| Anger- Hostility | 0 week | 53.0 (47.0–60.0) | 52.0 (49.0–61.0) | 0.804 |
| 4 week | 45.0 (43.0–47.0) * | 48.0 (44.0–53.0) * | 0.483 c | |
| Confusion- Bewilderment | 0 week | 55.5 (46.5–62.0) | 55.0 (49.0–59.0) | 0.916 |
| 4 week | 46.5 (40.0–54.0) * | 50.0 (47.0–55.0) * | 0.040 c | |
| Depression- Dejection | 0 week | 54.0 (47.5–57.0) | 50.0 (49.0–53.0) | 0.456 |
| 4 week | 46.5 (41.5–53.0) * | 46.0 (44.0–49.0) * | 0.058 c | |
| Fatigue- Inertia | 0 week | 61.0 (58.0–66.0) | 57.0 (55.0–59.0) | 0.053 |
| 4 week | 50.0 (45.0–53.0) * | 55.0 (46.0–55.0) ** | 0.076 c | |
| Tension- Anxiety | 0 week | 57.0 (56.5–60.0) | 56.0 (53.0–61.0) | 0.645 |
| 4 week | 48.0 (44.0–57.0) * | 53.0 (49.0–57.0) | 0.171 c | |
| Vigor- Activity | 0 week | 46.0 (37.5–47.0) | 44.0 (39.0–47.0) | 0.972 |
| 4 week | 53.0 (47.5–56.5) * | 44.0 (41.0–52.0) | 0.010 c | |
| Friendliness | 0 week | 51.0 (33.0–54.5) | 47.0 (42.0–50.0) | 0.645 |
| 4 week | 49.5 (43.5–55.5) | 45.0 (40.0–47.0) | 0.307 c | |
| Score (Point) | Rosemary (n = 8) | Control (n = 13) | pb | |
|---|---|---|---|---|
| Clear thinking | 0 week | 42.0 (25.5–59.0) a | 37.0 (31.0–43.0) | 0.645 |
| 4 week | 46.0 (43.5–55.5) | 45.0 (33.0–50.0) | 0.351 c | |
| Attentiveness | 0 week | 41.5 (26.5–55.5) | 35.0 (29.0–44.0) | 0.456 |
| 4 week | 44.0 (40.5–54.0) | 40.0 (33.0–50.0) * | 0.441 c | |
| Concentration | 0 week | 42.5 (20.0–51.5) | 35.0 (28.0–55.0) | 0.916 |
| 4 week | 50.5 (45.5–55.5) | 49.0 (33.0–49.0) | 0.127 c | |
| Fatigue on awakening | 0 week | 25.5 (20.5–33.0) | 28.0 (24.0–37.0) | 0.336 |
| 4 week | 48.5 (32.0–57.0) * | 32.0 (30.0–51.0) | 0.463 c | |
| Sleepiness on awakening | 0 week | 34.0 (30.5–51.5) | 31.0 (21.0–39.0) | 0.301 |
| 4 week | 47.0 (38.5–50.0) | 43.0 (30.0–51.0) | 0.840 c | |
| Daytime sleepiness | 0 week | 40.0 (19.5–50.0) | 31.0 (23.0–38.0) | 0.645 |
| 4 week | 57.5 (50.5–69.0) * | 45.0 (25.0–51.0) | 0.019 c | |
| T-Score (Point) | Rosemary (n = 8) | Control (n = 13) | pb | |
|---|---|---|---|---|
| NCI | 0 week | 107.0 (101.0–110.0) a | 108.0 (102.0–113.0) | 0.547 |
| 4 week | 107.0 (99.5–114.0) | 107.0 (94.0–114.0) | 0.195 c | |
| Composite memory | 0 week | 103.5 (95.5–113.5) | 114.0 (107.0–119.0) | 0.121 |
| 4 week | 96.0 (92.5–103.0) | 109.0 (94.0–112.0) | 0.584 c | |
| Verbal memory | 0 week | 103.5 (95.5–111.3) | 115.0 (106.0–125.0) | 0.053 |
| 4 week | 108.0 (95.3–114.3) | 109.0 (96.0–123.0) | 0.575 c | |
| Visual memory | 0 week | 106.0 (96.0–111.5) | 109.0 (100.0–113.0) | 0.645 |
| 4 week | 92.5 (86.5–96.0) * | 104.0 (87.0–112.0) | 0.237 c | |
| Psychomotor speed | 0 week | 111.5 (102.0–126.0) | 116.0 (106.0–126.0) | 0.697 |
| 4 week | 126.0 (100.0–133.0) * | 123.0 (107.0–134.0) | 0.442 c | |
| Reaction time | 0 week | 95.5 (90.0–100.5) | 99.0 (88.0–103.0) | 0.645 |
| 4 week | 98.0 (93.5–100.5) | 96.0 (91.0–102.0) | 0.443 c | |
| Complex attention | 0 week | 107.5 (105.0–112.5) | 108.0 (98.0–114.0) | 0.697 |
| 4 week | 113.5 (98.0–114.5) | 108.0 (88.0–113.0) | 0.394 c | |
| Cognitive flexibility | 0 week | 108.5 (104.0–114.0) | 109.0 (104.0–111.0) | 0.804 |
| 4 week | 112.5 (108.0–118.0) | 110.0 (91.0–113.0) | 0.265 c | |
| Processing speed | 0 week | 111.5 (104.0–117.5) | 117.0 (111.0–124.0) | 0.301 |
| 4 week | 116.0 (108.0–123.5) | 121.0 (113.0–132.0) | 0.172 c | |
| Executive function | 0 week | 109.0 (103.5–114.5) | 109.0 (104.0–113.0) | 0.972 |
| 4 week | 113.0 (108.5–118.5) | 109.0 (94.0–113.0) | 0.127 c | |
| Simple attention | 0 week | 106.0 (89.5–107.0) | 106.0 (85.0–107.0) | 0.645 |
| 4 week | 106.5 (106.0–107.0) | 106.0 (82.0–107.0) | 0.381 c | |
| Motor speed | 0 week | 113.5 (91.0–125.5) | 105.0 (99.0–122.0) | 0.697 |
| 4 week | 125.5 (92.5–131.0) | 109.0 (99.0–117.0) | 0.333 c | |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Araki, R.; Sasaki, K.; Onda, H.; Nakamura, S.; Kassai, M.; Kaneko, T.; Isoda, H.; Hashimoto, K. Effects of Continuous Intake of Rosemary Extracts on Mental Health in Working Generation Healthy Japanese Men: Post-Hoc Testing of a Randomized Controlled Trial. Nutrients 2020, 12, 3551. https://doi.org/10.3390/nu12113551
Araki R, Sasaki K, Onda H, Nakamura S, Kassai M, Kaneko T, Isoda H, Hashimoto K. Effects of Continuous Intake of Rosemary Extracts on Mental Health in Working Generation Healthy Japanese Men: Post-Hoc Testing of a Randomized Controlled Trial. Nutrients. 2020; 12(11):3551. https://doi.org/10.3390/nu12113551
Chicago/Turabian StyleAraki, Risa, Kazunori Sasaki, Hiroyuki Onda, Syunsuke Nakamura, Masahiro Kassai, Toshiyuki Kaneko, Hiroko Isoda, and Koichi Hashimoto. 2020. "Effects of Continuous Intake of Rosemary Extracts on Mental Health in Working Generation Healthy Japanese Men: Post-Hoc Testing of a Randomized Controlled Trial" Nutrients 12, no. 11: 3551. https://doi.org/10.3390/nu12113551
APA StyleAraki, R., Sasaki, K., Onda, H., Nakamura, S., Kassai, M., Kaneko, T., Isoda, H., & Hashimoto, K. (2020). Effects of Continuous Intake of Rosemary Extracts on Mental Health in Working Generation Healthy Japanese Men: Post-Hoc Testing of a Randomized Controlled Trial. Nutrients, 12(11), 3551. https://doi.org/10.3390/nu12113551





