Rapid Weight Gain, Infant Feeding Practices, and Subsequent Body Mass Index Trajectories: The CALINA Study
Abstract
1. Introduction
2. Materials and Methods
2.1. Design and Study Population
2.2. Measurements
2.2.1. Anthropometry (Outcome)
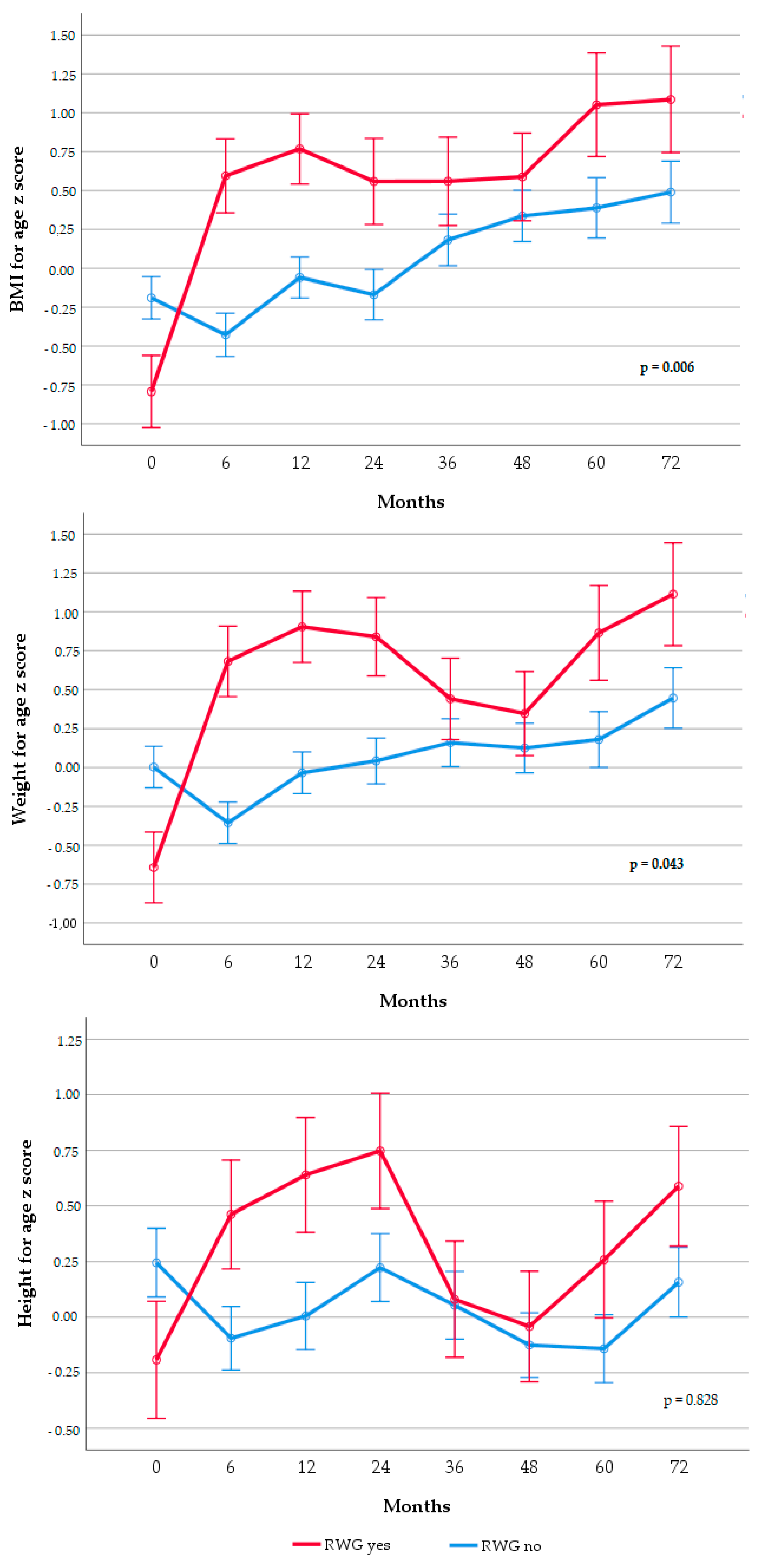
2.2.2. Rapid Weight Gain (Exposure)
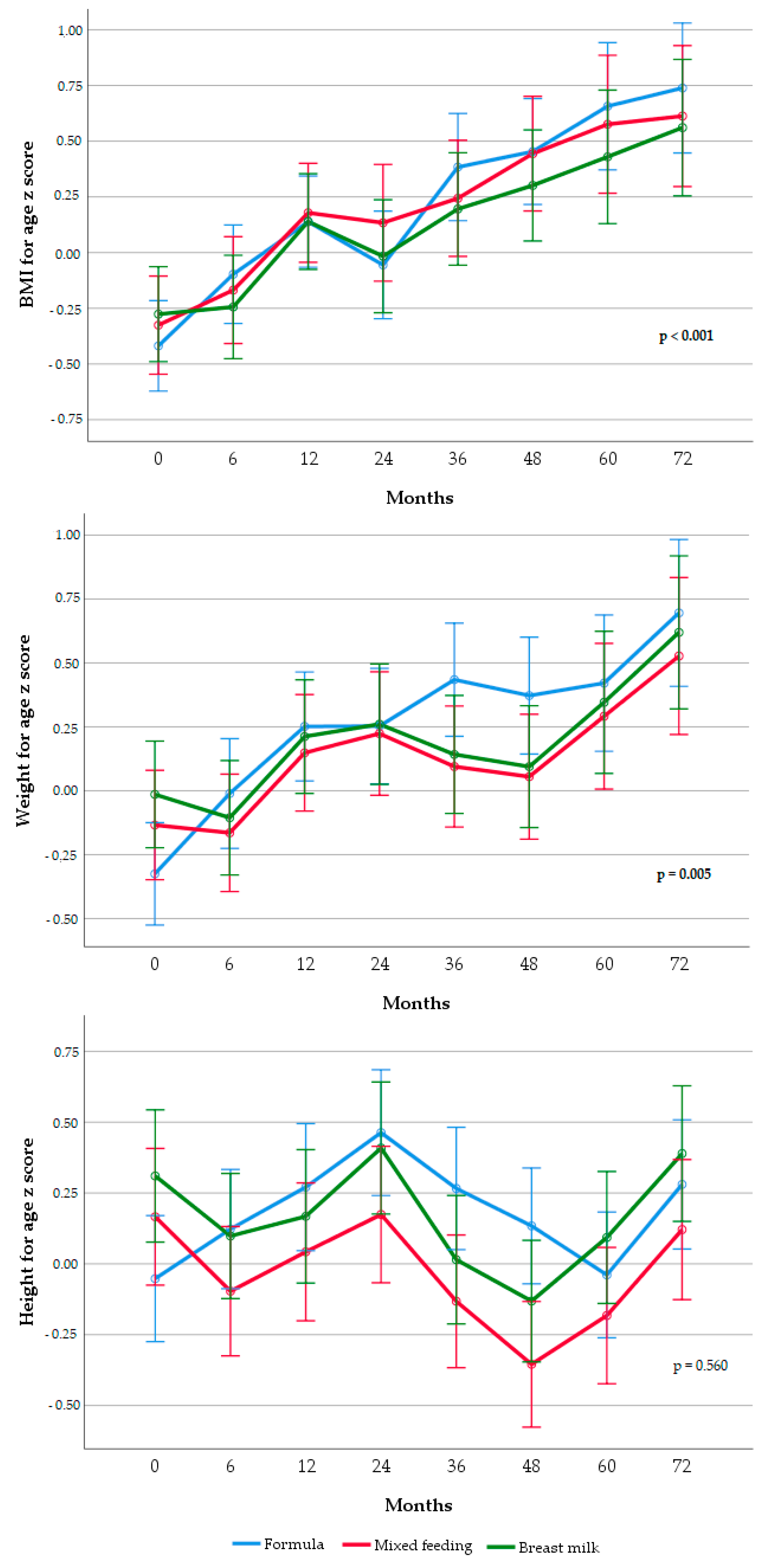
2.2.3. Type of Infant Feeding (Mediator)
2.2.4. Covariates
2.3. Statistical Analyses
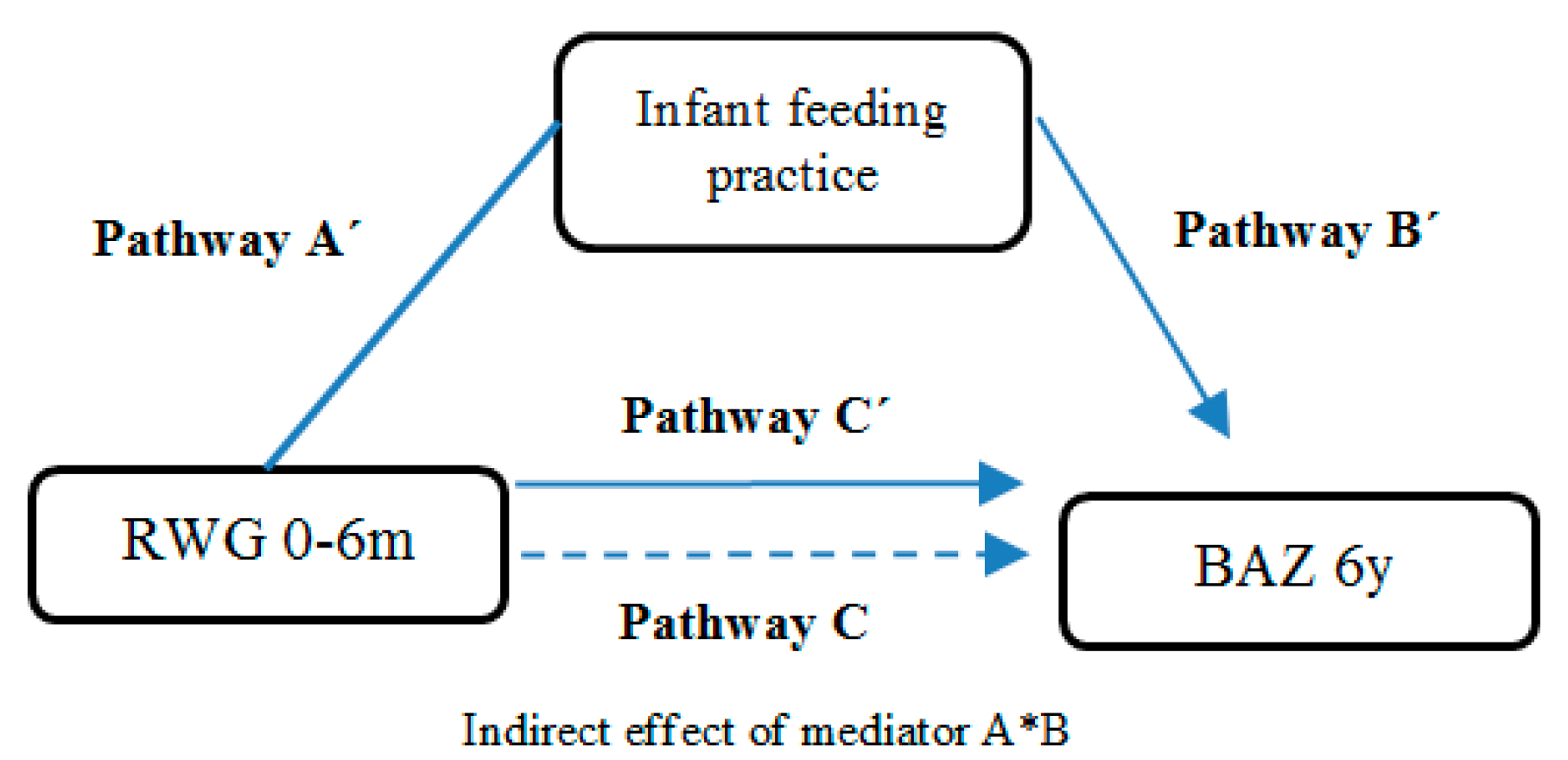
2.4. Mediation Analyses
3. Results
Mediation Results
4. Discussion
Strengths and Limitations
5. Conclusions
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- Statistics. Statistics—EASO: The European Association for the Study of Obesity. 2020. Available online: https://easo.org/media-portal/statistics/ (accessed on 15 June 2020).
- Wijnhoven, T.; van Raaij, J.; Spinelli, A.; Rito, A.; Hovengen, R.; Kunesova, M.; Starc, G.; Rutter, H.; Sjöberg, A.; Petrauskiene, A.; et al. WHO European Childhood Obesity Surveillance Initiative 2008: Weight, height and body mass index in 6–9-year-old children. Pediatr. Obes. 2013, 8. [Google Scholar] [CrossRef] [PubMed]
- World Health Organization (WHO). Obesity. Available online: https://www.who.int/health-topics/obesity#tab=tab_1 (accessed on 15 June 2020).
- Martínez García, R.; Jiménez Ortega, A.; González Torres, H.; Ortega, R. Prevention of obesity from perinatal stage. Nutr. Hosp. 2017, 34. [Google Scholar] [CrossRef]
- Woo Baidal, J.; Locks, L.; Cheng, E.; Blake-Lamb, T.; Perkins, M.; Taveras, E. Risk Factors for Childhood Obesity in the First 1000 Days: A Systematic Review. Am. J. Prev. Med. 2016, 50. [Google Scholar] [CrossRef]
- González-Muniesa, P.; Mártinez-González, M.; Hu, F.; Després, J.; Matsuzawa, Y.; Loos, R.; Moreno, L.; Bray, G.; Martinez, J. Obesity. Nat. Rev. Dis. Primers 2017, 3. [Google Scholar] [CrossRef]
- Larque, E.; Labayen, I.; Flodmark, C.E.; Lissau, I.; Czernin, S.; Moreno, L.A.; Pietrobelli, A.; Widhalm, K. From conception to infancy—Early risk factors for childhood obesity. Nat. Rev. Endocrinol. 2019, 15, 456–478. [Google Scholar] [CrossRef]
- Davanzo, R.; Romagnoli, C.; Corsello, G. Position Statement on Breastfeeding from the Italian Pediatric Societies. Ital. J. Pediatr. 2015, 41. [Google Scholar] [CrossRef]
- Gartner, L.; Morton, J.; Lawrence, R.; Naylor, A.; O’Hare, D.; Schanler, R.; Eidelman, A. Breastfeeding and the use of human milk. Pediatrics 2005, 115. [Google Scholar] [CrossRef]
- World Health Organization. Indicators for Assessing Infant and Young Child Feeding Practices. Available online: https://www.who.int/nutrition/publications/iycf_indicators_for_peer_review.pdf (accessed on 28 September 2020).
- Yan, J.; Liu, L.; Zhu, Y.; Huang, G.; Wang, P.P. The association between breastfeeding and childhood obesity: A meta-analysis. BMC Public Health 2014, 14, 1267. [Google Scholar] [CrossRef]
- Iguacel, I.; Monje, L.; Cabero, M.; Moreno Aznar, L.; Samper, M.; Rodríguez-Palmero, M.; Rivero, M.; Rodríguez, G. Feeding patterns and growth trajectories in breast-fed and formula-fed infants during the introduction of complementary food. Nutr. Hosp. 2019, 36. [Google Scholar] [CrossRef]
- Yang, S.; Mei, H.; Mei, H.; Yang, Y.; Li, N.; Tan, Y.; Zhang, Y.; Zhang, D.; Zhang, Y.; Peng, A.; et al. Risks of maternal prepregnancy overweight/obesity, excessive gestational weight gain, and bottle-feeding in infancy rapid weight gain: Evidence from a cohort study in China. Sci. China Life Sci. 2019, 62. [Google Scholar] [CrossRef]
- Wood, C.; Witt, W.; Skinner, A.; Yin, H.; Rothman, R.; Sanders, L.; Delamater, A.; Flower, K.; Kay, M.; Perrin, E. Effects of Breastfeeding, Formula Feeding, and Complementary Feeding on Rapid Weight Gain in the First Year of Life. Acad. Pediatr. 2020. [Google Scholar] [CrossRef] [PubMed]
- Rzehak, P.; Sausenthaler, S.; Koletzko, S.; Bauer, C.; Schaaf, B.; von Berg, A.; Berdel, D.; Borte, M.; Herbarth, O.; Krämer, U.; et al. Period-specific growth, overweight and modification by breastfeeding in the GINI and LISA birth cohorts up to age 6 years. Eur. J. Epidemiol. 2009, 24, 449–467. [Google Scholar] [CrossRef] [PubMed]
- Bell, K.; Wagner, C.; Feldman, H.; Shypailo, R.; Belfort, M. Associations of infant feeding with trajectories of body composition and growth. Am. J. Clin. Nutr. 2017, 106. [Google Scholar] [CrossRef]
- Mihrshahi, S.; Battistutta, D.; Magarey, A.; Daniels, L.A. Determinants of rapid weight gain during infancy: Baseline results from the NOURISH randomised controlled trial. BMC Pediatr. 2011, 11, 99. [Google Scholar] [CrossRef]
- Olivares, J.; Rodríguez, G.; Samper, P. Valoración del Crecimiento y la Alimentación Durante la Lactancia y la Primera Infancia en Atención Primaria; Prensas Universitarias de Zaragoza: Zaragoza, Spain, 2009. [Google Scholar]
- World Medical Assembly. World Medical Assembly. Declaration of Helsinki (1964). BMJ 1996. [Google Scholar] [CrossRef]
- WHO Multicentre Growth Reference Study Group. WHO Child Growth Standards: Methods and Development: Length/Height-for-Age, Weight-for-Age, Weight-for-Length, Weight-for-Height and Body Mass Index-for-; World Health Organization: Geneva, Switzerland, 2006. [Google Scholar]
- Monteiro, P.; Victora, C. Rapid Growth in Infancy and Childhood and Obesity in Later Life—A Systematic Review. Obes. Rev. Off. J. Int. Assoc. Study Obes. 2005, 6. [Google Scholar] [CrossRef] [PubMed]
- Rovine, M.J.; McDermott, P.A. Latent Growth Curve and Repeated Measures ANOVA Contrasts: What the Models are Telling You. Multivar. Behav. Res. 2018, 53. [Google Scholar] [CrossRef]
- Cooper, H. APA Handbook of Research Methods in Psychology; American Psychological Association: Washington, DC, USA, 2012; Volume 2. [Google Scholar]
- Hayes, A.F.; Rockwood, N.J. Regression-based statistical mediation and moderation analysis in clinical research: Observations, recommendations, and implementation. Behav. Res. Ther. 2017, 98. [Google Scholar] [CrossRef]
- World Health Organization, (WHO). Global Database on Child Growth and Malnutrition. The Z-Score or Standard Deviation Classification. Available online: https://www.who.int/nutgrowthdb/about/introduction/en/index4.html (accessed on 29 September 2020).
- Woo, J.; Sucharew, H.; Su, W.; Khoury, P.; Daniels, S.; Kalkwarf, H. Infant Weight and Length Growth Trajectories Modeled Using Superimposition by Translation and Rotation Are Differentially Associated with Body Composition Components at 3 and 7 Years of Age. J. Pediatr. 2018, 196. [Google Scholar] [CrossRef]
- Zheng, M.; Bowe, S.; Hesketh, K.; Bolton, K.; Laws, R.; Kremer, P.; Ong, K.; Lioret, S.; Denney-Wilson, E.; Campbell, K. Relative effects of postnatal rapid growth and maternal factors on early childhood growth trajectories. Paediatr. Perinat. Epidemiol. 2019, 33. [Google Scholar] [CrossRef]
- Salahuddin, M.; Pérez, A.; Ranjit, N.; Hoelscher, D.; Kelder, S. The associations of large-for-gestational-age and infant feeding practices with children’s body mass index z-score trajectories: The Early Childhood Longitudinal Study, Birth Cohort. Clin. Obes. 2017, 7. [Google Scholar] [CrossRef] [PubMed]
- Appleton, J.; Russell, C.G.; Laws, R.; Fowler, C.; Campbell, K.; Denney-Wilson, E. Infant formula feeding practices associated with rapid weight gain: A systematic review. Matern Child Nutr. 2018, 14. [Google Scholar] [CrossRef]
- Li, R.; Magadia, J.; Fein, S.B.; Grummer-Strawn, L.M. Risk of bottle-feeding for rapid weight gain during the first year of life. Arch. Pediatr. Adolesc. Med. 2012, 166, 431–436. [Google Scholar] [CrossRef]
- Disantis, K.; Collins, B.; Fisher, J.; Davey, A. Do infants fed directly from the breast have improved appetite regulation and slower growth during early childhood compared with infants fed from a bottle? Int. J. Behav. Nutr. Phys. Act. 2011, 8. [Google Scholar] [CrossRef]
- Bammann, K.; Peplies, J.; De Henauw, S.; Hunsberger, M.; Molnar, D.; Moreno, L.A.; Tornaritis, M.; Veidebaum, T.; Ahrens, W.; Siani, A. Early life course risk factors for childhood obesity: The IDEFICS case-control study. PLoS ONE 2014, 9, e86914. [Google Scholar] [CrossRef] [PubMed]
- Ortega-García, J.A.; Kloosterman, N.; Alvarez, L.; Tobarra-Sánchez, E.; Cárceles-Álvarez, A.; Pastor-Valero, R.; López-Hernández, F.A.; Sánchez-Solis, M.; Claudio, L. Full Breastfeeding and Obesity in Children: A Prospective Study from Birth to 6 Years. Child Obes. 2018, 14, 327–337. [Google Scholar] [CrossRef] [PubMed]
- Nanri, H.; Shirasawa, T.; Ochiai, H.; Nomoto, S.; Hoshino, H.; Kokaze, A. Rapid weight gain during infancy and early childhood is related to higher anthropometric measurements in preadolescence. Child Care Health Dev. 2017, 43, 435–440. [Google Scholar] [CrossRef]
- Stettler, N.; Zemel, B.S.; Kumanyika, S.; Stallings, V.A. Infant weight gain and childhood overweight status in a multicenter, cohort study. Pediatrics 2002, 109, 194–199. [Google Scholar] [CrossRef]
- Rotevatn, T.A.; Overgaard, C.; Melendez-Torres, G.J.; Mortensen, R.N.; Ullits, L.R.; Høstgaard, A.M.B.; Torp-Pedersen, C.; Bøggild, H. Infancy weight gain, parental socioeconomic position, and childhood overweight and obesity: A Danish register-based cohort study. BMC Public Health 2019, 19. [Google Scholar] [CrossRef]
- Singhal, A. Long-Term Adverse Effects of Early Growth Acceleration or Catch-up Growth. Ann. Nutr. Metab. 2017, 70. [Google Scholar] [CrossRef]
- Zheng, M.; Lamb, K.E.; Grimes, C.; Laws, R.; Bolton, K.; Ong, K.K.; Campbell, K. Rapid weight gain during infancy and subsequent adiposity: A systematic review and meta-analysis of evidence. Obes. Rev. 2018, 19, 321–332. [Google Scholar] [CrossRef] [PubMed]
- Nguyen, A.; Jen, V.; Jaddoe, V.; Rivadeneira, F.; Jansen, P.; Ikram, M.; Voortman, T. Diet quality in early and mid-childhood in relation to trajectories of growth and body composition. Clin. Nutr. 2020, 39. [Google Scholar] [CrossRef] [PubMed]
- Abdella, H.; El Farssi, H.; Broom, D.; Hadden, D.; Dalton, C. Eating Behaviours and Food Cravings; Influence of Age, Sex, BMI and FTO Genotype. Nutrients 2019, 11, 377. [Google Scholar] [CrossRef] [PubMed]
- Vaughn, A.E.; Ward, D.S.; Fisher, J.O.; Faith, M.S.; Hughes, S.O.; Kremers, S.P.; Musher-Eizenman, D.R.; O’Connor, T.M.; Patrick, H.; Power, T.G. Fundamental constructs in food parenting practices: A content map to guide future research. Nutr. Rev. 2016, 74, 98–117. [Google Scholar] [CrossRef]
- Gao, Z. Growth Trajectories of Young Children’s Objectively Determined Physical Activity, Sedentary Behavior, and Body Mass Index. Child. Obes. 2018, 14. [Google Scholar] [CrossRef]
- Bruun, S.; Buhl, S.; Husby, S.; Jacobsen, L.; Michaelsen, K.; Sørensen, J.; Zachariassen, G. Breastfeeding, Infant Formula, and Introduction to Complementary Foods-Comparing Data Obtained by Questionnaires and Health Visitors’ Reports to Weekly Short Message Service Text Messages. Breastfeed. Med. Off. J. Acad. Breastfeed. Med. 2017, 12. [Google Scholar] [CrossRef]
| Total | RWG Yes | RWG No | p-Value | |
|---|---|---|---|---|
| % (n) | 862 | 28.31 (244) | 71.69 (618) | |
| Girls | 47.2 (407) | 48.4 (118) | 46.8 (289) | 0.672 |
| Boys | 52.8 (455) | 51.6(126) | 53.2 (329) | |
| Gestational age at birth mean ± SD | 39.16 ± 1.33 | 38.53 ± 1.46 (244) | 39.41 ± 1.91 (618) | 0.000 0.000 |
| Small for gestational age, % (n) | 11.4 (98) | 26.6 (65) | 5.3 (33) | |
| Normal for gestational age, % (n) | 88.6 (764) | 66.3 (179) | 94.7 (585) | |
| Birth weight mean ± SD (n) | 3263.41 ± 0.98 (862) | 2973.12 ± 406.98 (244) | 3378.02 ± 415.11 (618) | 0.000 |
| BAz mean ± SEM (n) | ||||
| At birth | –0.31 ± 0.03 (855) | −0.87 ± 0.06 (242) | −0.09 ± 0.04 (613) | 0.000 |
| 6 months | −0.08 ± 0.04 (851) | 0.61 ± 0.07 (239) | −0.35 ± 0.04 (612) | 0.000 |
| 12 months | 0.25 ± 0.03 (840) | 0.75 ± 0.06 (237) | 0.05 ± 0.04 (603) | 0.000 |
| 24 months | 0.11 ± 0.04 (802) | 0.60 ± 0.07 (220) | −0.07 ± 0.04 (582) | 0.000 |
| 36 months | 0.26 ± 0.04 (771) | 0.43 ± 0.08 (214) | 0.20 ± 0.05 (557) | 0.013 |
| 48 months | 0.41 ± 0.04 (753) | 0.54 ± 0.09 (213) | 0.36 ± 0.05 (540) | 0.064 |
| 60 months | 0.62 ± 0.07 (316) | 1.07 ± 0.14 (88) | 0.44 ± 0.08 (228) | 0.000 |
| 72 months | 0.62 ± 0.04 (862) | 1.03 ± 0.08 (244) | 0.45 ± 0.05(618) | 0.000 |
| Delta in WAz mean ± SD (n) | 0.11 ± 1.05 (862) | 1.34 ± 0.58 (244) | −0.38 ± 0.76 (618) | 0.000 |
| Infant feeding practice in the 1st 120 days, % (n) | 0.136 | |||
| Formula | 34.2 (295) | 38.5 (94) | 32.5 (201) | |
| Mixed (Formula + Breast milk) | 27.7 (239) | 28.3 (69) | 27.5 (170) | |
| Breast milk | 38.1 (328) | 33.2 (81) | 40.0 (247) | |
| Maternal education, % (n) | 0.009 | |||
| None or basic | 24.6 (212) | 32.4 (77) | 22.3 (135) | |
| Intermediate | 34.6 (296) | 30.7 (73) | 36.9 (223) | |
| High | 38.9 (335) | 37.0 (88) | 40.8 (247) | |
| Paternal education, % (n) | 0.326 | |||
| None or basic | 29.8 (257) | 34.5 (79) | 29.6 (178) | |
| Intermediate | 42.0 (362) | 42.8 (98) | 43.9 (264) | |
| High | 24.5 (211) | 22.7 (52) | 26.5 (159) | |
| Parental origin/ethnicity, % (n) | 0.325 | |||
| Spanish | 84.5 (728) | 82.9 (194) | 85.6 (518) | |
| Immigrant | 15.3 (132) | 17.1 (40) | 14.4 (87) | |
| Parental BMI, kg/m2 | ||||
| Mothers mean ± SD (n) | 23.65 ± 4.45 (836) | 24.03 ± 4.76 (239) | 23.49 ± 4.32 (597) | 0.117 |
| Fathers mean ± SD (n) | 26.19 ± 3.38 (805) | 26.37 ± 3.26 (223) | 26.11 ± 3.43 (582) | 0.332 |
| Maternal smoking during pregnancy, % (n) | 0.094 | |||
| Yes | 18.2 (157) | 21.7 (53) | 16.8 (104) | |
| No | 81.2 (705) | 78.3 (191) | 83.2 (514) | |
| Center, % (n) | 0.226 | |||
| Huesca | 73.8 (636) | 77.9 (190) | 72.2 (446) | |
| Teruel | 17.2 (148) | 14.8 (36) | 18.1 (112) | |
| Zaragoza | 9.0 (78) | 7.4 (18) | 9.7 (60) |
| BMI z-Scores b | RWG c | Maternal Education d | Paternal Education d | Birth Weight | Maternal BMI e | Paternal BMI e | Infant Feeding Practice f |
|---|---|---|---|---|---|---|---|
| BAz 1 years | 0.304 *** | −0.061 * | −0.046 | 0.207 *** | 0.131 *** | 0.112 *** | −0.007 |
| BAz 2 years | 0.256 *** | −0.062 * | −0.055 * | 0.215 *** | 0.151 *** | 0.117 *** | −0.006 |
| BAz 3 years | 0.077 ** | −0.063 * | −0.52 * | 0.020 | 0.002 | −0.006 | 0.019 |
| BAz 4 years | 0.047 | −0.038 | −0.040 | 0.060 | −0.008 | 0.021 | 0.023 |
| BAz 5 years | 0.154 ** | −0.041 | −0.036 | 0.189 | 0.227 *** | 0.189 *** | 0.057 |
| BAz 6 years | 0.193 *** | −0.117 *** | −0.122 *** | 0.141 *** | 0.208 *** | 0.192 *** | 0.093 ** |
| Infant feeding practice f | 0.084 ** | - | - |
| Pathway A’ β (95% CI) | Pathway B’ β (95% CI) | Pathway C’ β (95% CI) | Pathway C β (95% CI) | Indirect Effect of Mediator A*B β, SE (95% CI) | Mediation | |
|---|---|---|---|---|---|---|
| (A)n = 862 | 0.128 (0.002; 0.254) * | 0.118 (0.021; 0.215) * | 0.562 (0.379; 0.745) *** | 0.577 (0.394; 0.760) *** | 0.015, SE = 0.01 (−0.001; 0.039) | - |
| (B)n = 767 | −0.036 (−0.185; 0.112) | 0.114 (0.015; 0.212) * | 0.784 (0.579; 0.990) *** | 0.780 (0.575; 0.986) *** | −0.004. SE = 0.0094 (−0.026; 0.013) | - |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Flores-Barrantes, P.; Iguacel, I.; Iglesia-Altaba, I.; Moreno, L.A.; Rodríguez, G. Rapid Weight Gain, Infant Feeding Practices, and Subsequent Body Mass Index Trajectories: The CALINA Study. Nutrients 2020, 12, 3178. https://doi.org/10.3390/nu12103178
Flores-Barrantes P, Iguacel I, Iglesia-Altaba I, Moreno LA, Rodríguez G. Rapid Weight Gain, Infant Feeding Practices, and Subsequent Body Mass Index Trajectories: The CALINA Study. Nutrients. 2020; 12(10):3178. https://doi.org/10.3390/nu12103178
Chicago/Turabian StyleFlores-Barrantes, Paloma, Isabel Iguacel, Iris Iglesia-Altaba, Luis A. Moreno, and Gerardo Rodríguez. 2020. "Rapid Weight Gain, Infant Feeding Practices, and Subsequent Body Mass Index Trajectories: The CALINA Study" Nutrients 12, no. 10: 3178. https://doi.org/10.3390/nu12103178
APA StyleFlores-Barrantes, P., Iguacel, I., Iglesia-Altaba, I., Moreno, L. A., & Rodríguez, G. (2020). Rapid Weight Gain, Infant Feeding Practices, and Subsequent Body Mass Index Trajectories: The CALINA Study. Nutrients, 12(10), 3178. https://doi.org/10.3390/nu12103178







