Food Addiction: Implications for the Diagnosis and Treatment of Overeating
Abstract
1. Introduction
1.1. Impaired Control
1.1.1. Impulsivity
1.1.2. Reward Sensitivity
1.2. Craving
1.3. Social Impairment
1.4. Repeated Use Despite Negative Consequences
1.5. Physiological Criteria
2. Neurobiological Similarities between Palatable Foods and Drugs of Abuse
2.1. Neurobiology of Reward Sensitivity
2.2. Neurobiology of Inhibitory Control
3. Treatment Implications
3.1. Cognitive Interventions
3.2. Neuromodulation Interventions
3.3. Therapeutic Interventions
4. Conclusions
Author Contributions
Funding
Conflicts of Interest
References
- WHO. Obesity and Overweight; World Health Organization: Geneva, Switzerland, 2003. [Google Scholar]
- Global Burden of Disease Collaborative Network. Global Burden of Disease Study. Obesity Prevalence 1990–2013; Institute for Health Metrics and Evaluation (IHME): Seattle, WA, USA, 2014. [Google Scholar]
- Ng, M.; Fleming, T.; Robinson, M.; Thomson, B.; Graetz, N.; Margono, C.; Mullany, E.C.; Biryukov, S.; Abbafati, C.; Abera, S.F.; et al. Global, regional, and national prevalence of overweight and obesity in children and adults during 1980–2013: A systematic analysis for the Global burden of disease study 2013. Lancet 2014, 384, 766–781. [Google Scholar] [CrossRef]
- WHO. Obesity and Overweight; World Health Organization: Geneva, Switzerland, 2018. [Google Scholar]
- Butland, B.; Jebb, S.; Kopelman, P.; McPherson, K.; Thomas, S.; Mardell, J.; Parry, V. Tackling Obesities: Future Choices—Project Report, 2nd ed.; Foresight Programme of the Government Office for Science: London, UK, 2007. Available online: www.bis.gov.uk/assets/bispartners/foresight/docs/obesity/17.pdf (accessed on 28 September 2018).
- Cummins, S.; Macintyre, S. Food environments and obesity—Neighbourhood or nation? Int. J. Epidemiol. 2006, 35, 100–104. [Google Scholar] [CrossRef] [PubMed]
- Jeffery, R.W.; Utter, J. The changing environment and population obesity in the United States. Obes. Res. 2003, 11, 12S–22S. [Google Scholar] [CrossRef] [PubMed]
- Levitsky, D.A. The non-regulation of food intake in humans: Hope for reversing the epidemic of obesity. Physiol. Behav. 2005, 86, 623–632. [Google Scholar] [CrossRef] [PubMed]
- Schulte, E.M.; Avena, N.M.; Gearhardt, A.N. Which foods may be addictive? The roles of processing, fat content, and glycemic load. PLoS ONE 2015, 10, e0117959. [Google Scholar] [CrossRef] [PubMed]
- Blundell, J.E.; Burley, V.J.; Cotton, J.R.; Lawton, C.L. Dietary fat and the control of energy intake: Evaluating the effects of fat on meal size and postmeal satiety. Am. J. Clin. Nutr. 1993, 57, 772S–778S. [Google Scholar] [CrossRef] [PubMed]
- Drewnowski, A.; Brunzell, J.; Sande, K.; Iverius, P.; Greenwood, M. Sweet tooth reconsidered: Taste responsiveness in human obesity. Physiol. Behav. 1985, 35, 617–622. [Google Scholar] [CrossRef]
- Drewnowski, A.; Kurth, C.; Holden-Wiltse, J.; Saari, J. Food preferences in human obesity: Carbohydrates versus fats. Appetite 1992, 18, 207–221. [Google Scholar] [CrossRef]
- Davis, C. An introduction to the Special Issue on ‘food addiction’. Appetite 2017, 115, 1–2. [Google Scholar] [CrossRef] [PubMed]
- Avena, N.M.; Gearhardt, A.N.; Gold, M.S.; Wang, G.-J.; Potenza, M.N. Tossing the baby out with the bathwater after a brief rinse? The potential downside of dismissing food addiction based on limited data. Nat. Rev. Neurosci. 2012, 13, 514. [Google Scholar] [CrossRef]
- Corsica, J.A.; Pelchat, M.L. Food addiction: True or false? Curr. Opin. Gastroenterol. 2010, 26, 165–169. [Google Scholar] [CrossRef] [PubMed]
- Meule, A.; Gearhardt, A. Food addiction in the light of DSM-5. Nutrients 2014, 6, 3653–3671. [Google Scholar] [CrossRef] [PubMed]
- Rogers, P.J.; Smit, H.J. Food craving and food “addiction”: A critical review of the evidence from a biopsychosocial perspective. Pharmacol. Biochem. Behav. 2000, 66, 3–14. [Google Scholar] [CrossRef]
- Volkow, N.D.; Wise, R.A.; Baler, R. The dopamine motive system: Implications for drug and food addiction. Nat. Rev. Neurosci. 2017, 18, 741–752. [Google Scholar] [CrossRef] [PubMed]
- Ziauddeen, H.; Farooqi, I.S.; Fletcher, P.C. Food addiction: is there a baby in the bathwater? Nat. Rev. Neurosci. 2012, 13, 514. [Google Scholar] [CrossRef]
- Ziauddeen, H.; Farooqi, I.S.; Fletcher, P.C. Obesity and the brain: how convincing is the addiction model? Nat. Rev. Neurosci. 2012, 13, 279–286. [Google Scholar] [CrossRef] [PubMed]
- Frascella, J.; Potenza, M.N.; Brown, L.L.; Childress, A.R. Carving addiction at a new joint? Shared brain vulnerabilities open the way for non-substance addictions. Ann. N. Y. Acad. Sci. 2010, 1187, 294–315. [Google Scholar] [CrossRef]
- Orford, J. Addiction as excessive appetite. Addiction 2001, 96, 15–31. [Google Scholar] [CrossRef]
- American Psychiatric Association. Diagnostic and Statistical Manual of Mental Disorders, 5th ed.; American Psychiatric Association: Washington, DC, USA, 2013. [Google Scholar]
- Potenza, M.N. Biological contributions to addictions in adolescents and adults: Prevention, treatment and policy implications. J. Adolesc. Health 2013, 52, S22–S32. [Google Scholar] [CrossRef]
- Worhunsky, P.D.; Malison, R.T.; Rogers, R.D.; Potenza, M.N. Altered neural correlates of reward and loss processing during simulated slot-machine fMRI in pathological gambling and cocaine dependence. Drug Alcohol Depend. 2014, 145, 77–86. [Google Scholar] [CrossRef]
- Barry, D.; Clarke, M.; Petry, N.M. Obesity and its relationship to addictions: Is overeating a form of addictive behavior? Am. J. Addict. 2009, 18, 439–451. [Google Scholar] [CrossRef] [PubMed]
- Cassin, S.E.; Buchman, D.Z.; Leung, S.E.; Kantarovich, K.; Hawa, A.; Carter, A.; Sockalingam, S. Ethical, Stigma, and policy implications of food addiction: A scoping review. Nutrients 2019, 11, 710. [Google Scholar] [CrossRef] [PubMed]
- Gearhardt, A.N.; Grilo, C.M.; Dileone, R.J.; Brownell, K.D.; Potenza, M.N. Can food be addictive? Public health and policy implications. Addiction 2011, 106, 1208–1212. [Google Scholar] [CrossRef] [PubMed]
- Volkow, N.D.; Wise, R.A. How can drug addiction help us understand obesity? Nat. Neurosci. 2005, 8, 555–560. [Google Scholar] [CrossRef] [PubMed]
- Wilson, G.T. Eating disorders, obesity and addiction. Eur. Eat. Disord. Rev. 2010, 18, 341–351. [Google Scholar] [CrossRef] [PubMed]
- Davis, C.; Carter, J.C. Compulsive overeating as an addiction disorder. A review of theory and evidence. Appetite 2009, 53, 1–8. [Google Scholar] [CrossRef] [PubMed]
- Meule, A.; von Rezori, V.; Blechert, J. Food addiction and bulimia nervosa. Eur. Eat. Dis. Rev. 2014, 22, 331–337. [Google Scholar] [CrossRef] [PubMed]
- Shell, A.G.; Firmin, M.W. Binge eating disorder and substance use disorder: A case for food addiction. Psychol. Stud. 2017, 62, 370–376. [Google Scholar] [CrossRef]
- Smith, D.G.; Robbins, T.W. The neurobiological underpinnings of obesity and binge eating: A rationale for adopting the food addiction model. Biol. Psychiatr. 2013, 73, 804–810. [Google Scholar] [CrossRef]
- Cassin, S.E.; Von Ranson, K.M. Is binge eating experienced as an addiction? Appetite 2007, 49, 687–690. [Google Scholar] [CrossRef]
- Gearhardt, A.N.; White, M.A.; Masheb, R.M.; Morgan, P.T.; Crosby, R.D.; Grilo, C.M. An examination of the food addiction construct in obese patients with binge eating disorder. Int. J. Eat. Dis. 2012, 45, 657–663. [Google Scholar] [CrossRef] [PubMed]
- Gearhardt, A.N.; Corbin, W.R.; Brownell, K.D. Preliminary validation of the Yale food addiction scale. Appetite 2009, 52, 430–436. [Google Scholar] [CrossRef] [PubMed]
- Gearhardt, A.N.; Corbin, W.R.; Brownell, K.D. Development of the Yale food addiction scale version 2.0. Psychol. Addict. Behav. 2016, 30, 113–121. [Google Scholar] [CrossRef] [PubMed]
- Gearhardt, A.N.; Roberto, C.A.; Seamans, M.J.; Corbin, W.R.; Brownell, K.D. Preliminary validation of the Yale food addiction scale for children. Eat. Behav. 2013, 14, 508–512. [Google Scholar] [CrossRef]
- Murphy, C.M.; Stojek, M.K.; MacKillop, J. Interrelationships among impulsive personality traits, food addiction, and body mass index. Appetite 2014, 73, 45–50. [Google Scholar] [CrossRef]
- Curtis, C.; Davis, C. A qualitative study of binge eating and obesity from an addiction perspective. Eat. Dis. 2014, 22, 19–32. [Google Scholar] [CrossRef]
- Pretlow, R.A. Addiction to highly pleasurable food as a cause of the childhood obesity epidemic: A qualitative internet study. Eat. Disord. 2011, 19, 295–307. [Google Scholar] [CrossRef]
- French, S.; Jeffery, R.; Sherwood, N.; Neumark-Sztainer, D. Prevalence and correlates of binge eating in a nonclinical sample of women enrolled in a weight gain prevention program. Int. J. Obes. 1999, 23, 576–585. [Google Scholar] [CrossRef]
- Lu, H.K.; Mannan, H.; Hay, P. Exploring relationships between recurrent binge eating and illicit substance use in a non-clinical sample of women over two years. Behav. Sci. 2017, 7, 46. [Google Scholar] [CrossRef]
- MacDiarmid, J.; Loe, J.; Kyle, J.; McNeill, G. “It was an education in portion size”. Experience of eating a healthy diet and barriers to long term dietary change. Appetite 2013, 71, 411–419. [Google Scholar] [CrossRef]
- Bacon, L.; Aphramor, L. Weight science: Evaluating the evidence for a paradigm shift. Nutr. J. 2011, 10, 9. [Google Scholar] [CrossRef] [PubMed]
- Dansinger, M.L.; Gleason, J.A.; Griffith, J.L.; Selker, H.P.; Schaefer, E.J. Comparison of the Atkins, Ornish, Weight Watchers, and Zone Diets for Weight Loss and Heart Disease Risk Reduction. JAMA 2005, 293, 43. [Google Scholar] [CrossRef] [PubMed]
- Jeffery, R.W.; Epstein, L.H.; Wilson, G.T.; Drewnowski, A.; Stunkard, A.J.; Wing, R.R. Long-term maintenance of weight loss: Current status. Health Psychol. 2000, 19, 5–16. [Google Scholar] [CrossRef] [PubMed]
- Lowe, M.R.; Annunziato, R.A.; Markowitz, J.T.; Didie, E.; Bellace, D.L.; Riddell, L.; Maille, C.; McKinney, S.; Stice, E. Multiple types of dieting prospectively predict weight gain during the freshman year of college. Appetite 2006, 47, 83–90. [Google Scholar] [CrossRef] [PubMed]
- Mann, T.; Tomiyama, A.J.; Westling, E.; Lew, A.-M.; Samuels, B.; Chatman, J. Medicare’s search for effective obesity treatments: Diets are not the answer. Am. Psychol. 2007, 62, 220–233. [Google Scholar] [CrossRef] [PubMed]
- Pietiläinen, K.H.; Saarni, S.E.; Kaprio, J.; Rissanen, A. Does dieting make you fat? A twin study. Int. J. Obes. 2012, 36, 456–464. [Google Scholar] [CrossRef] [PubMed]
- Ifland, J.; Preuss, H.; Marcus, M.; Rourke, K.; Taylor, W.; Burau, K.; Jacobs, W.; Kadish, W.; Manso, G. Refined food addiction: A classic substance use disorder. Med. Hypotheses 2009, 72, 518–526. [Google Scholar] [CrossRef] [PubMed]
- Russell-Mayhew, S.; Von Ranson, K.M.; Masson, P.C. How does overeaters anonymous help its members? A qualitative analysis. Eur. Eat. Disord. Rev. 2010, 18, 33–42. [Google Scholar] [CrossRef] [PubMed]
- Dawe, S.; Loxton, N.J. The role of impulsivity in the development of substance use and eating disorders. Neurosci. Biobehav. Rev. 2004, 28, 343–351. [Google Scholar] [CrossRef]
- Gullo, M.; Dawe, S. Impulsivity and adolescent substance use: Rashly dismissed as “all-bad”? Neurosci. Biobehav. Rev. 2008, 32, 1507–1518. [Google Scholar] [CrossRef] [PubMed]
- Schulte, E.M.; Grilo, C.M.; Gearhardt, A.N. Shared and unique mechanisms underlying binge eating disorder and addictive disorders. Clin. Psychol. Rev. 2016, 44, 125–139. [Google Scholar] [CrossRef] [PubMed]
- De Wit, H. Impulsivity as a determinant and consequence of drug use: A review of underlying processes. Addict. Biol. 2008, 14, 22–31. [Google Scholar] [CrossRef] [PubMed]
- Hershberger, A.R.; Um, M.; Cyders, M.A. The relationship between the UPPS-P impulsive personality traits and substance use psychotherapy outcomes: A meta-analysis. Drug Alcohol Depend. 2017, 178, 408–416. [Google Scholar] [CrossRef] [PubMed]
- Iacono, W.G.; Malone, S.M.; McGue, M. Behavioral disinhibition and the development of early-onset addiction: Common and specific influences. Annu. Rev. Clin. Psychol. 2008, 4, 325–348. [Google Scholar] [CrossRef]
- Verdejo-García, A.; Lawrence, A.J.; Clark, L. Impulsivity as a vulnerability marker for substance-use disorders: Review of findings from high-risk research, problem gamblers and genetic association studies. Neurosci. Biobehav. Rev. 2008, 32, 777–810. [Google Scholar] [CrossRef]
- Billieux, J.; Gay, P.; Rochat, L.; Khazaal, Y.; Zullino, D.; Van Der Linden, M. Lack of inhibitory control predicts cigarette smoking dependence: Evidence from a non-deprived sample of light to moderate smokers. Drug Alcohol Depend. 2010, 112, 164–167. [Google Scholar] [CrossRef] [PubMed]
- Butler, G.; Montgomery, A. Impulsivity, risk taking and recreational ‘ecstasy’ (MDMA) use. Drug Alcohol Depend. 2004, 76, 55–62. [Google Scholar] [CrossRef]
- García-Marchena, N.; De Guevara-Miranda, D.L.; Pedraz, M.; Araos, P.F.; Rubio, G.; Ruiz, J.J.; Pavón, F.J.; Serrano, A.; Castilla-Ortega, E.; Santín, L.J.; et al. Higher impulsivity as a distinctive trait of severe cocaine addiction among individuals treated for cocaine or alcohol use disorders. Front. Psychol. 2018, 9, 26. [Google Scholar] [CrossRef] [PubMed]
- Lawrence, A.J.; Luty, J.; Bogdan, N.A.; Sahakian, B.J.; Clark, L. Impulsivity and response inhibition in alcohol dependence and problem gambling. Psychopharmacology 2009, 207, 163–172. [Google Scholar] [CrossRef]
- Monterosso, J.R.; Aron, A.R.; Cordova, X.; Xu, J.; London, E.D. Deficits in response inhibition associated with chronic methamphetamine abuse. Drug Alcohol Depend. 2005, 79, 273–277. [Google Scholar] [CrossRef]
- Verdejo-García, A.J.; Perales, J.C.; Pérez-García, M. Cognitive impulsivity in cocaine and heroin polysubstance abusers. Addict. Behav. 2007, 32, 950–966. [Google Scholar] [CrossRef] [PubMed]
- Noël, X.; Van Der Linden, M.; Brevers, D.; Campanella, S.; Verbanck, P.; Hanak, C.; Kornreich, C.; Verbruggen, F. Separating intentional inhibition of prepotent responses and resistance to proactive interference in alcohol-dependent individuals. Drug Alcohol Depend. 2013, 128, 200–205. [Google Scholar] [CrossRef] [PubMed]
- Emery, R.L.; Levine, M.D. Questionnaire and behavioral task measures of impulsivity are differentially associated with body mass index: A comprehensive meta-analysis. Psychol. Bull. 2017, 143, 868–902. [Google Scholar] [CrossRef] [PubMed]
- Guerrieri, R.; Nederkoorn, C.; Jansen, A. The interaction between impulsivity and a varied food environment: Its influence on food intake and overweight. Int. J. Obes. 2008, 32, 708–714. [Google Scholar] [CrossRef] [PubMed]
- Jentsch, J.D.; Pennington, Z.T. Reward, interrupted: Inhibitory control and its relevance to addictions. Neuropharmacology 2014, 76, 479–486. [Google Scholar] [CrossRef] [PubMed]
- Meule, A. Impulsivity and overeating: A closer look at the subscales of the Barratt impulsiveness scale. Front. Psychol. 2013, 4, 177. [Google Scholar] [CrossRef]
- Chalmers, D.K.; Bowyer, C.A.; Olenick, N.L. Problem drinking and obesity: A comparison in personality patterns and lifestyle. Int. J. Addict. 1990, 25, 803–817. [Google Scholar] [CrossRef]
- Davis, C.; Levitan, R.D.; Carter, J.; Kaplan, A.S.; Reid, C.; Curtis, C.; Patte, K.; Kennedy, J.L. Personality and eating behaviors: A case-control study of binge eating disorder. Int. J. Eat. Disord. 2008, 41, 243–250. [Google Scholar] [CrossRef]
- Rydén, A.; Sullivan, M.; Torgerson, J.S.; Karlsson, J.; Lindroos, A.-K.; Taft, C. Severe obesity and personality: A comparative controlled study of personality traits. Int. J. Obes. 2003, 27, 1534–1540. [Google Scholar] [CrossRef]
- Batterink, L.; Yokum, S.; Stice, E. Body mass correlates inversely with inhibitory control in response to food among adolescent girls: An fMRI study. NeuroImage 2010, 52, 1696–1703. [Google Scholar] [CrossRef]
- Davis, C.; Patte, K.; Curtis, C.; Reid, C. Immediate pleasures and future consequences. A neuropsychological study of binge eating and obesity. Appetite 2010, 54, 208–213. [Google Scholar] [CrossRef] [PubMed]
- Nederkoorn, C.; Braet, C.; Van Eijs, Y.; Tanghe, A.; Jansen, A. Why obese children cannot resist food: The role of impulsivity. Eat. Behav. 2006, 7, 315–322. [Google Scholar] [CrossRef] [PubMed]
- Friese, M.; Hofmann, W. Control me or I will control you: Impulses, trait self-control, and the guidance of behavior. J. Res. Personal. 2009, 43, 795–805. [Google Scholar] [CrossRef]
- Friese, M.; Hofmann, W.; Wänke, M. When impulses take over: Moderated predictive validity of explicit and implicit attitude measures in predicting food choice and consumption behaviour. Br. J. Soc. Psychol. 2008, 47, 397–419. [Google Scholar] [CrossRef] [PubMed]
- Hofmann, W.; Friese, M.; Roefs, A. Three ways to resist temptation: The independent contributions of executive attention, inhibitory control, and affect regulation to the impulse control of eating behavior. J. Exp. Soc. Psychol. 2009, 45, 431–435. [Google Scholar] [CrossRef]
- Crescioni, A.W.; Ehrlinger, J.; Alquist, J.L.; Conlon, K.E.; Baumeister, R.F.; Schatschneider, C.; Dutton, G.R. High trait self-control predicts positive health behaviors and success in weight loss. J. Health Psychol. 2011, 16, 750–759. [Google Scholar] [CrossRef] [PubMed]
- De Boer, B.J.; van Hooft, E.A.J.; Bakker, A.B. Stop and start control: A distinction within self-control. Eur. J. Personal. 2011, 25, 349–362. [Google Scholar] [CrossRef]
- Gerrits, J.H.; O’Hara, R.E.; Piko, B.F.; Gibbons, F.X.; De Ridder, D.T.D.; Keresztes, N.; Kamble, S.V.; De Wit, J.B.F. Self-control, diet concerns and eater prototypes influence fatty foods consumption of adolescents in three countries. Health Educ. Res. 2010, 25, 1031–1041. [Google Scholar] [CrossRef]
- Jasinska, A.J.; Yasuda, M.; Burant, C.F.; Gregor, N.; Khatri, S.; Sweet, M.; Falk, E.B. Impulsivity and inhibitory control deficits are associated with unhealthy eating in young adults. Appetite 2012, 59, 738–747. [Google Scholar] [CrossRef]
- Allan, J.L.; Johnston, M.; Campbell, N. Unintentional eating. What determines goal-incongruent chocolate consumption? Appetite 2010, 54, 422–425. [Google Scholar] [CrossRef]
- Allom, V.; Mullan, B. Individual differences in executive function predict distinct eating behaviours. Appetite 2014, 80, 123–130. [Google Scholar] [CrossRef] [PubMed]
- Guerrieri, R.; Nederkoorn, C.; Jansen, A. How impulsiveness and variety influence food intake in a sample of healthy women. Appetite 2007, 48, 119–122. [Google Scholar] [CrossRef] [PubMed]
- Churchill, S.; Jessop, D.C. Reflective and non-reflective antecedents of health-related behaviour: Exploring the relative contributions of impulsivity and implicit self-control to the prediction of dietary behaviour. Br. J. Health Psychol. 2011, 16, 257–272. [Google Scholar] [CrossRef] [PubMed]
- Meule, A.; De Zwaan, M.; Müller, A. Attentional and motor impulsivity interactively predict ‘food addiction’ in obese individuals. Compr. Psychiatr. 2017, 72, 83–87. [Google Scholar] [CrossRef] [PubMed]
- VanderBroek-Stice, L.; Stojek, M.K.; Beach, S.R.H.; Vandellen, M.R.; MacKillop, J. Multidimensional assessment of impulsivity in relation to obesity and food addiction. Appetite 2017, 112, 59–68. [Google Scholar] [CrossRef] [PubMed]
- Appelhans, B.M.; Woolf, K.; Pagoto, S.L.; Schneider, K.L.; Whited, M.C.; Liebman, R. Inhibiting food reward: Delay discounting, food reward sensitivity, and palatable food intake in overweight and obese women. Obesity 2011, 19, 2175–2182. [Google Scholar] [CrossRef] [PubMed]
- Dissabandara, L.O.; Loxton, N.J.; Dias, S.R.; Dodd, P.R.; Daglish, M.; Stadlin, A. Dependent heroin use and associated risky behaviour: The role of rash impulsiveness and reward sensitivity. Addict. Behav. 2014, 39, 71–76. [Google Scholar] [CrossRef]
- Franken, I.H.; Muris, P. Individual differences in reward sensitivity are related to food craving and relative body weight in healthy women. Appetite 2005, 45, 198–201. [Google Scholar] [CrossRef]
- Davis, C.; Patte, K.; Levitan, R.; Reid, C.; Tweed, S.; Curtis, C. From motivation to behaviour: A model of reward sensitivity, overeating, and food preferences in the risk profile for obesity. Appetite 2007, 48, 12–19. [Google Scholar] [CrossRef]
- De Cock, N.; Van Lippevelde, W.; Goossens, L.; De Clercq, B.; Vangeel, J.; Lachat, C.; Beullens, K.; Huybregts, L.; Vervoort, L.; Eggermont, S.; et al. Sensitivity to reward and adolescents’ unhealthy snacking and drinking behavior: The role of hedonic eating styles and availability. Int. J. Behav. Nutr. Phys. Act. 2016, 13, 17. [Google Scholar] [CrossRef]
- Lawrence, N.S.; Hinton, E.C.; Parkinson, J.A.; Lawrence, A.D. Nucleus accumbens response to food cues predicts subsequent snack consumption in women and increased body mass index in those with reduced self-control. NeuroImage 2012, 63, 415–422. [Google Scholar] [CrossRef] [PubMed]
- Davis, C.; Strachan, S.; Berkson, M. Sensitivity to reward: Implications for overeating and overweight. Appetite 2004, 42, 131–138. [Google Scholar] [CrossRef] [PubMed]
- Volkow, N.D.; Fowler, J.S.; Wang, G.-J. The addicted human brain: Insights from imaging studies. J. Clin. Investig. 2003, 111, 1444–1451. [Google Scholar] [CrossRef] [PubMed]
- Volkow, N.D.; Wang, G.-J.; Telang, F.; Fowler, J.S.; Thanos, P.K.; Logan, J.; Alexoff, D.; Ding, Y.-S.; Wong, C.; Ma, Y.; et al. Low dopamine striatal D2 receptors are associated with prefrontal metabolism in obese subjects: Possible contributing factors. NeuroImage 2008, 42, 1537–1543. [Google Scholar] [CrossRef] [PubMed]
- Wang, G.J.; Volkow, N.D.; Logan, J.; Pappas, N.R.; Wong, C.T.; Zhu, W.; Netusil, N.; Fowler, J.S. Brain dopamine and obesity. Lancet 2001, 357, 354–357. [Google Scholar] [CrossRef]
- Blum, K.; Braverman, E.R.; Holder, J.M.; Lubar, J.F.; Monastra, V.J.; Miller, D.; Lubar, J.O.; Chen, T.J.; Comings, D.E. The reward deficiency syndrome: A biogenetic model for the diagnosis and treatment of impulsive, addictive and compulsive behaviors. J. Psychoact. Drugs 2000, 32, 1–112. [Google Scholar] [CrossRef]
- Bowirrat, A.; Oscar-Berman, M. Relationship between dopaminergic neurotransmission, alcoholism, and reward deficiency syndrome. Am. J. Med. Genet. Part B Neuropsychiatr. Genet. 2005, 132, 29–37. [Google Scholar] [CrossRef]
- Burger, K.S.; Stice, E. Variability in reward responsivity and obesity: Evidence from brain imaging studies. Curr. Drug Abus. Rev. 2011, 4, 182–189. [Google Scholar] [CrossRef]
- Robinson, T. The neural basis of drug craving: An incentive-sensitization theory of addiction. Brain Res. Rev. 1993, 18, 247–291. [Google Scholar] [CrossRef]
- Robinson, T.E.; Berridge, K.C. Incentive-sensitization and addiction. Addiction 2001, 96, 103–114. [Google Scholar] [CrossRef]
- Robinson, T.E.; Berridge, K.C. Addiction. Annu. Rev. Psychol. 2003, 54, 25–53. [Google Scholar] [CrossRef] [PubMed]
- Berridge, K.C. ‘Liking’ and ‘wanting’ food rewards: Brain substrates and roles in eating disorders. Physiol. Behav. 2009, 97, 537–550. [Google Scholar] [CrossRef] [PubMed]
- Berridge, K.C.; Ho, C.-Y.; Richard, J.M.; DiFeliceantonio, A.G. The tempted brain eats: Pleasure and desire circuits in obesity and eating disorders. Brain Res. 2010, 1350, 43–64. [Google Scholar] [CrossRef] [PubMed]
- Hetherington, M.; Pirie, L.; Nabb, S.; Hetherington, M. Stimulus satiation: Effects of repeated exposure to foods on pleasantness and intake. Appetite 2002, 38, 19–28. [Google Scholar] [CrossRef] [PubMed]
- Ersche, K.D.; Jones, P.S.; Williams, G.B.; Turton, A.J.; Robbins, T.W.; Bullmore, E.T. Abnormal brain structure implicated in stimulant drug addiction. Science 2012, 335, 601–604. [Google Scholar] [CrossRef] [PubMed]
- Everitt, B.J.; Belin, D.; Economidou, D.; Pelloux, Y.; Dalley, J.W.; Robbins, T.W. Neural mechanisms underlying the vulnerability to develop compulsive drug-seeking habits and addiction. Philos. Trans. R. Soc. B Biol. Sci. 2008, 363, 3125–3135. [Google Scholar] [CrossRef] [PubMed]
- Flagel, S.B.; Akil, H.; Robinson, T.E. Individual differences in the attribution of incentive salience to reward-related cues: Implications for addiction. Neuropharmacology 2009, 56, 139–148. [Google Scholar] [CrossRef]
- Saunders, B.T.; Robinson, T.E. Individual variation in resisting temptation: Implications for addiction. Neurosci. Biobehav. Rev. 2013, 37, 1955–1975. [Google Scholar] [CrossRef] [PubMed]
- Kekic, M.; McClelland, J.; Campbell, I.; Nestler, S.; Rubia, K.; David, A.S.; Schmidt, U. The effects of prefrontal cortex transcranial direct current stimulation (tDCS) on food craving and temporal discounting in women with frequent food cravings. Appetite 2014, 78, 55–62. [Google Scholar] [CrossRef]
- Weingarten, H.P.; Elston, D. The phenomenology of food cravings. Appetite 1990, 15, 231–246. [Google Scholar] [CrossRef]
- Pelchat, M.L. Food cravings in young and elderly adults. Appetite 1997, 28, 103–113. [Google Scholar] [CrossRef] [PubMed]
- Lopez, R.B.; Hofmann, W.; Wagner, D.D.; Kelley, W.M.; Heatherton, T.F. Neural predictors of giving in to temptation in daily life. Psychol. Sci. 2014, 25, 1337–1344. [Google Scholar] [CrossRef] [PubMed]
- Cocores, J.A.; Gold, M.S. The Salted Food Addiction Hypothesis may explain overeating and the obesity epidemic. Med. Hypotheses 2009, 73, 892–899. [Google Scholar] [CrossRef] [PubMed]
- Corsica, J.A.; Spring, B.J. Carbohydrate craving: A double-blind, placebo controlled test of the self-medication hypothesis. Eat. Behav. 2008, 9, 447–454. [Google Scholar] [CrossRef] [PubMed]
- Hill, A.J.; Heaton-Brown, L. The experience of food craving: A prospective investigation in healthy women. J. Psychosom. Res. 1994, 38, 801–814. [Google Scholar] [CrossRef]
- Massey, A.; Hill, A.J. Dieting and food craving. A descriptive, quasi-prospective study. Appetite 2012, 58, 781–785. [Google Scholar] [CrossRef]
- Rozin, P.; Levine, E.; Stoess, C. Chocolate craving and liking. Appetite 1991, 17, 199–212. [Google Scholar] [CrossRef]
- Cepeda-Benito, A.; Gleaves, D.H.; Williams, T.L.; Erath, S.A. The development and validation of the state and trait food-cravings questionnaires. Behav. Ther. 2000, 31, 151–173. [Google Scholar] [CrossRef]
- Hill, A.J.; Weaver, C.F.; Blundell, J.E. Food craving, dietary restraint and mood. Appetite 1991, 17, 187–197. [Google Scholar] [CrossRef]
- Nicholls, W.; Hulbert-Williams, L. British english translation of the food craving inventory (FCI-UK). Appetite 2013, 67, 37–43. [Google Scholar] [CrossRef]
- Nijs, I.M.; Franken, I.H.; Muris, P. The modified trait and state food-cravings questionnaires: Development and validation of a general index of food craving. Appetite 2007, 49, 38–46. [Google Scholar] [CrossRef] [PubMed]
- White, M.A.; Whisenhunt, B.L.; Williamson, D.A.; Greenway, F.L.; Netemeyer, R.G. Development and validation of the food-craving inventory. Obes. Res. 2002, 10, 107–114. [Google Scholar] [CrossRef] [PubMed]
- Benton, D.; Greenfield, K.; Morgan, M. The development of the attitudes to chocolate questionnaire. Personal. Individ. Differ. 1998, 24, 513–520. [Google Scholar] [CrossRef]
- Boswell, R.G.; Kober, H. Food cue reactivity and craving predict eating and weight gain: A meta-analytic review. Obes. Rev. 2016, 17, 159–177. [Google Scholar] [CrossRef] [PubMed]
- Burton, P.; Smit, H.J.; Lightowler, H.J. The influence of restrained and external eating patterns on overeating. Appetite 2007, 49, 191–197. [Google Scholar] [CrossRef] [PubMed]
- Dalton, M.; Blundell, J.; Finlayson, G.S. Examination of food reward and energy intake under laboratory and free-living conditions in a trait binge eating subtype of obesity. Front. Psychol. 2013, 4, 757. [Google Scholar] [CrossRef] [PubMed]
- Lafay, L.; Mennen, L.; Charles, M.A.; Eschwège, E.; Borys, J.-M. Gender differences in the relation between food cravings and mood in an adult community: Results from the Fleurbaix Laventie Ville Sant study. Int. J. Eat. Disord. 2001, 29, 195–204. [Google Scholar] [CrossRef]
- Davis, C.; Curtis, C.; Levitan, R.D.; Carter, J.C.; Kaplan, A.S.; Kennedy, J.L. Evidence that ‘food addiction’ is a valid phenotype of obesity. Appetite 2011, 57, 711–717. [Google Scholar] [CrossRef]
- Meule, A. Food cravings in food addiction: Exploring a potential cut-off value of the food cravings questionnaire-trait-reduced. Eat. Weight Dis. Stud. Anorex. Bulim. Obes. 2018, 23, 39–43. [Google Scholar] [CrossRef]
- Meule, A.; Kübler, A. Food cravings in food addiction: The distinct role of positive reinforcement. Eat. Behav. 2012, 13, 252–255. [Google Scholar] [CrossRef]
- Mussell, M.P.; Mitchell, J.E.; De Zwaan, M.; Crosby, R.D.; Seim, H.C.; Crow, S.J. Clinical characteristics associated with binge eating in obese females: A descriptive study. Int. J. Obes. Relat. Metab. Disord. J. Int. Assoc. Stud. Obes. 1996, 20, 324–331. [Google Scholar]
- Ng, L.; Davis, C. Cravings and food consumption in binge eating disorder. Eat. Behav. 2013, 14, 472–475. [Google Scholar] [CrossRef]
- Van den Eynde, F.; Koskina, A.; Syrad, H.; Guillaume, S.; Broadbent, H.; Campbell, I.C.; Schmidt, U. State and trait food craving in people with bulimic eating disorders. Eat. Behav. 2012, 13, 414–417. [Google Scholar] [CrossRef] [PubMed]
- Bottlender, M.; Soyka, M. Impact of craving on alcohol relapse during, and 12 months following, outpatient treatment. Alcohol Alcohol. 2004, 39, 357–361. [Google Scholar] [CrossRef] [PubMed]
- Litt, M.D.; Cooney, N.L.; Morse, P. Reactivity to alcohol-related stimuli in the laboratory and in the field: Predictors of craving in treated alcoholics. Addiction 2000, 95, 889–900. [Google Scholar] [CrossRef] [PubMed]
- Paliwal, P.; Hyman, S.M.; Sinha, R. Craving predicts time to cocaine relapse: Further validation of the now and brief versions of the cocaine craving questionnaire. Drug Alcohol Depend. 2008, 93, 252–259. [Google Scholar] [CrossRef] [PubMed]
- Gendall, K.A.; Sullivan, P.F.; Joyce, P.R.; Fear, J.L.; Bulik, C.M. Psychopathology and personality of young women who experience food cravings. Addict. Behav. 1997, 22, 545–555. [Google Scholar] [CrossRef]
- Meule, A.; Lutz, A.; Vögele, C.; Kübler, A. Food cravings discriminate differentially between successful and unsuccessful dieters and non-dieters. Validation of the food cravings questionnaires in German. Appetite 2012, 58, 88–97. [Google Scholar] [CrossRef]
- Meule, A.; Westenhöfer, J.; Kübler, A. Food cravings mediate the relationship between rigid, but not flexible control of eating behavior and dieting success. Appetite 2011, 57, 582–584. [Google Scholar] [CrossRef]
- Carter, B.L.; Tiffany, S.T. Meta-analysis of cue-reactivity in addiction research. Addiction 1999, 94, 327–340. [Google Scholar] [CrossRef]
- Davidson, D.; Tiffany, S.T.; Johnston, W.; Flury, L.; Li, T.-K. Using the cue-availability paradigm to assess cue reactivity. Alcohol. Clin. Exp. Res. 2003, 27, 1251–1256. [Google Scholar] [CrossRef]
- Mahler, S.V.; De Wit, H. Cue-Reactors: Individual differences in cue-induced craving after food or smoking abstinence. PLoS ONE 2010, 5, e15475. [Google Scholar] [CrossRef] [PubMed]
- Styn, M.A.; Bovbjerg, D.H.; Lipsky, S.; Erblich, J. Cue-induced cigarette and food craving: A common effect? Addict. Behav. 2013, 38, 1840–1843. [Google Scholar] [CrossRef] [PubMed]
- Cornell, C.E.; Rodin, J.; Weingarten, H. Stimulus-induced eating when satiated. Physiol. Behav. 1989, 45, 695–704. [Google Scholar] [CrossRef]
- Nederkoorn, C.; Smulders, F.; Jansen, A. Cephalic phase responses, craving and food intake in normal subjects. Appetite 2000, 35, 45–55. [Google Scholar] [CrossRef] [PubMed]
- Meule, A.; Küppers, C.; Harms, L.; Friederich, H.-C.; Schmidt, U.; Blechert, J.; Brockmeyer, T. Food cue-induced craving in individuals with bulimia nervosa and binge-eating disorder. PLoS ONE 2018, 13, e0204151. [Google Scholar] [CrossRef] [PubMed]
- Karhunen, L.J.; Lappalainen, R.I.; Tammela, L.; Turpeinen, A.K.; Uusitupa, M.I.J. Subjective and physiological cephalic phase responses to food in obese binge-eating women. Int. J. Eat. Disord. 1997, 21, 321–328. [Google Scholar] [CrossRef]
- Sobik, L.; Hutchison, K.; Craighead, L. Cue-elicited craving for food: A fresh approach to the study of binge eating. Appetite 2005, 44, 253–261. [Google Scholar] [CrossRef]
- Kjelgaard, H.H.; Holstein, B.E.; Due, P.; Brixval, C.S.; Rasmussen, M. Adolescent weight status: Associations with structural and functional dimensions of social relations. J. Adolesc. Health 2017, 60, 460–468. [Google Scholar] [CrossRef]
- Schwimmer, J.B.; Burwinkle, T.M.; Varni, J.W. Health-Related quality of life of severely obese children and adolescents. JAMA 2003, 289, 1813. [Google Scholar] [CrossRef]
- Williams, J.; Wake, M.; Hesketh, K.; Maher, E.; Waters, E. Health-Related quality of life of overweight and obese children. JAMA 2005, 293, 70–76. [Google Scholar] [CrossRef] [PubMed]
- Griffiths, L.J.; Wolke, D.; Page, A.S.; Horwood, J.P. Obesity and bullying: Different effects for boys and girls. Arch. Dis. Child. 2006, 91, 121–125. [Google Scholar] [CrossRef] [PubMed]
- Pearce, M.J.; Boergers, J.; Prinstein, M.J. Adolescent obesity, overt and relational peer victimization, and romantic relationships. Obes. Res. 2002, 10, 386–393. [Google Scholar] [CrossRef] [PubMed]
- Hayden-Wade, H.A.; Stein, R.I.; Ghaderi, A.; Saelens, B.E.; Zabinski, M.F.; Wilfley, D.E. Prevalence, characteristics, and correlates of teasing experiences among overweight children vs. non-overweight peers. Obes. Res. 2005, 13, 1381–1392. [Google Scholar] [CrossRef] [PubMed]
- Neumark-Sztainer, D.; Falkner, N.; Story, M.; Perry, C.; Hannan, P.J.; Mulert, S. Weight-teasing among adolescents: Correlations with weight status and disordered eating behaviors. Int. J. Obes. 2002, 26, 123–131. [Google Scholar] [CrossRef] [PubMed]
- Puhl, R.; Brownell, K.D. Bias, Discrimination, and Obesity. Obes. Res. 2001, 9, 788–805. [Google Scholar] [CrossRef] [PubMed]
- Puhl, R.M.; Heuer, C.A. The stigma of obesity: A review and update. Obesity 2009, 17, 941–964. [Google Scholar] [CrossRef] [PubMed]
- Puhl, R.M.; Latner, J.D. Stigma, obesity, and the health of the nation’s children. Psychol. Bull. 2007, 133, 557–580. [Google Scholar] [CrossRef]
- Chen, E.Y.; Brown, M. Obesity stigma in sexual relationships. Obes. Res. 2005, 13, 1393–1397. [Google Scholar] [CrossRef]
- Chao, A.M.; Shaw, J.A.; Pearl, R.L.; Alamuddin, N.; Hopkins, C.M.; Bakizada, Z.M.; Wadden, T.A. Prevalence and psychosocial correlates of food addiction in persons with obesity seeking weight reduction. Compr. Psychiatr. 2017, 73, 97–104. [Google Scholar] [CrossRef]
- Blomquist, K.K.; Ansell, E.B.; White, M.A.; Masheb, R.M.; Grilo, C.M. Interpersonal problems and developmental trajectories of binge eating disorder. Compr. Psychiatr. 2012, 53, 1088–1095. [Google Scholar] [CrossRef] [PubMed]
- Lo Coco, G.; Gullo, S.; Salerno, L.; Iacoponelli, R. The association among interpersonal problems, binge behaviors, and self-esteem, in the assessment of obese individuals. Compr. Psychiatr. 2011, 52, 164–170. [Google Scholar] [CrossRef] [PubMed]
- Jia, H.; Lubetkin, E.I. Trends in quality-adjusted life-years lost contributed by smoking and obesity. Am. J. Prev. Med. 2010, 38, 138–144. [Google Scholar] [CrossRef] [PubMed]
- Bray, G.A. Medical consequences of obesity. J. Clin. Endocrinol. Metab. 2004, 89, 2583–2589. [Google Scholar] [CrossRef] [PubMed]
- Carpenter, K.M.; Hasin, D.S.; Allison, D.B.; Faith, M.S. Relationships between obesity and DSM-IV major depressive disorder, suicide ideation, and suicide attempts: Results from a general population study. Am. J. Public Health 2000, 90, 251–257. [Google Scholar] [PubMed]
- Haslam, D.W.; James, W.P.T. Obesity. Lancet 2005, 366, 1197–1209. [Google Scholar] [CrossRef]
- Kahn, S.E.; Hull, R.L.; Utzschneider, K.M. Mechanisms linking obesity to insulin resistance and type 2 diabetes. Nature 2006, 444, 840–846. [Google Scholar] [CrossRef] [PubMed]
- Lopresti, A.L.; Drummond, P.D. Obesity and psychiatric disorders: Commonalities in dysregulated biological pathways and their implications for treatment. Prog. Neuro Psychopharmacol. Biol. Psychiatr. 2013, 45, 92–99. [Google Scholar] [CrossRef]
- Luppino, F.S.; de Wit, L.M.; Bouvy, P.F.; Stijnen, T.; Cuijpers, P.; Penninx, B.W.J.H.; Zitman, F.G. Overweight, obesity, and depression: A systematic review and meta-analysis of longitudinal studies. Arch. Gen. Psychiatr. 2010, 67, 220–229. [Google Scholar] [CrossRef]
- Mannan, M.; Mamun, A.; Doi, S.; Clavarino, A. Prospective associations between depression and obesity for adolescent males and females—A systematic review and meta-analysis of longitudinal studies. PLoS ONE 2016, 11, 0157240. [Google Scholar] [CrossRef]
- Mokdad, A.H.; Ford, E.S.; Bowman, B.A.; Dietz, W.H.; Vinicor, F.; Bales, V.S.; Marks, J.S. Prevalence of obesity, diabetes, and obesity-related health risk factors, 2001. JAMA 2003, 289, 76–79. [Google Scholar] [CrossRef] [PubMed]
- Van Gaal, L.F.; Mertens, I.L.; De Block, C.E. Mechanisms linking obesity with cardiovascular disease. Nature 2006, 444, 875–880. [Google Scholar] [CrossRef] [PubMed]
- Elkins, G.; Whitfield, P.; Marcus, J.; Symmonds, R.; Rodriguez, J.; Cook, T. Noncompliance with behavioral recommendations following bariatric surgery. Obes. Surg. 2005, 15, 546–551. [Google Scholar] [CrossRef]
- Toussi, R.; Fujioka, K.; Coleman, K.J. Pre- and postsurgery behavioral compliance, patient health, and postbariatric surgical weight loss. Obesity 2009, 17, 996–1002. [Google Scholar] [CrossRef] [PubMed]
- Colantuoni, C.; Schwenker, J.; McCarthy, J.; Rada, P.; Ladenheim, B.; Cadet, J.-L.; Schwartz, G.J.; Moran, T.H.; Hoebel, B.G. Excessive sugar intake alters binding to dopamine and mu-opioid receptors in the brain. NeuroReport 2001, 12, 3549–3552. [Google Scholar] [CrossRef]
- Rada, P.; Avena, N.; Hoebel, B. Daily bingeing on sugar repeatedly releases dopamine in the accumbens shell. Neuroscience 2005, 134, 737–744. [Google Scholar] [CrossRef] [PubMed]
- Harrison, D.M. Oral sucrose for pain management in infants: Myths and misconceptions. J. Neonatal Nurs. 2008, 14, 39–46. [Google Scholar] [CrossRef]
- King, J.M. Patterns of sugar consumption in early infancy. Community Dent. Oral Epidemiol. 1978, 6, 47–52. [Google Scholar] [CrossRef]
- Rossow, I.; Kjaernes, U.; Holst, D. Patterns of sugar consumption in early childhood. Community Dent. Oral Epidemiol. 1990, 18, 12–16. [Google Scholar] [CrossRef]
- Slater, R.; Cornelissen, L.; Fabrizi, L.; Patten, D.; Yoxen, J.; Worley, A.; Boyd, S.; Meek, J.; Fitzgerald, M. Oral sucrose as an analgesic drug for procedural pain in newborn infants: A randomised controlled trial. Lancet 2010, 376, 1225–1232. [Google Scholar] [CrossRef]
- Nielsen, S.J.; Popkin, B.M. Patterns and trends in food portion sizes, 1977–1998. JAMA 2003, 289, 450–453. [Google Scholar] [CrossRef] [PubMed]
- Wideman, C.H.; Nadzam, G.R.; Murphy, H.M. Implications of an animal model of sugar addiction, withdrawal and relapse for human health. Nutr. Neurosci. 2005, 8, 269–276. [Google Scholar] [CrossRef] [PubMed]
- Avena, N.M.; Rada, P.; Hoebel, B.G. Evidence for sugar addiction: Behavioral and neurochemical effects of intermittent, excessive sugar intake. Neurosci. Biobehav. Rev. 2008, 32, 20–39. [Google Scholar] [CrossRef] [PubMed]
- Galic, M.A.; Persinger, M.A. Voluminous sucrose consumption in female rats: Increased “nippiness” during periods of sucrose removal and possible oestrus periodicity. Psychol. Rep. 2002, 90, 58–60. [Google Scholar] [CrossRef] [PubMed]
- Avena, N.M.; Bocarsly, M.E.; Rada, P.; Kim, A.; Hoebel, B.G. After daily bingeing on a sucrose solution, food deprivation induces anxiety and accumbens dopamine/acetylcholine imbalance. Physiol. Behav. 2008, 94, 309–315. [Google Scholar] [CrossRef] [PubMed]
- Hetherington, M.M.; MacDiarmid, J.I. “Chocolate addiction”: A preliminary study of its description and its relationship to problem eating. Appetite 1993, 21, 233–246. [Google Scholar] [CrossRef] [PubMed]
- Carnell, S.; Gibson, C.; Benson, L.; Ochner, C.N.; Geliebter, A. Neuroimaging and obesity: Current knowledge and future directions. Obes. Rev. 2012, 13, 43–56. [Google Scholar] [CrossRef]
- Parvaz, M.A.; Alia-Klein, N.; Woicik, P.A.; Volkow, N.D.; Goldstein, R.Z. Neuroimaging for drug addiction and related behaviors. Rev. Neurosci. 2011, 22, 609–624. [Google Scholar] [CrossRef] [PubMed]
- Zhang, Y.; von Deneen, K.M.; Tian, J.; Gold, M.S.; Liu, Y. Food addiction and neuroimaging. Curr. Pharm. Des. 2011, 17, 1149–1157. [Google Scholar] [CrossRef] [PubMed]
- Goldstein, R.Z.; Volkow, N.D. Drug addiction and its underlying neurobiological basis: Neuroimaging evidence for the involvement of the frontal cortex. Am. J. Psychiatr. 2002, 159, 1642–1652. [Google Scholar] [CrossRef]
- Goldstein, R.Z.; Volkow, N.D. Dysfunction of the prefrontal cortex in addiction: Neuroimaging findings and clinical implications. Nat. Rev. Neurosci. 2011, 12, 652–669. [Google Scholar] [CrossRef] [PubMed]
- Koob, G.F.; Volkow, N.D. Neurobiology of addiction: A neurocircuitry analysis. Lancet Psychiatr. 2016, 3, 760–773. [Google Scholar] [CrossRef]
- Volkow, N.D.; Wang, G.-J.; Fowler, J.S.; Telang, F. Overlapping neuronal circuits in addiction and obesity: Evidence of systems pathology. Philos. Trans. R. Soc. B Biol. Sci. 2008, 363, 3191–3200. [Google Scholar] [CrossRef] [PubMed]
- Volkow, N.D.; Wang, G.-J.; Tomasi, D.; Baler, R.D. The addictive dimensionality of obesity. Biol. Psychiatr. 2013, 73, 811–818. [Google Scholar] [CrossRef] [PubMed]
- Pierce, R.C.; Kumaresan, V. The mesolimbic dopamine system: The final common pathway for the reinforcing effect of drugs of abuse? Neurosci. Biobehav. Rev. 2006, 30, 215–238. [Google Scholar] [CrossRef] [PubMed]
- Hernández, L.; Hoebel, B.G. Food reward and cocaine increase extracellular dopamine in the nucleus accumbens as measured by microdialysis. Life Sci. 1988, 42, 1705–1712. [Google Scholar] [CrossRef]
- Radhakishun, F.S.; Van Ree, J.M.; Westerink, B.H. Scheduled eating increases dopamine release in the nucleus accumbens of food-deprived rats as assessed with on-line brain dialysis. Neurosci. Lett. 1988, 85, 351–356. [Google Scholar] [CrossRef]
- Yoshida, M.; Yokoo, H.; Mizoguchi, K.; Kawahara, H.; Tsuda, A.; Nishikawa, T.; Tanaka, M. Eating and drinking cause increased dopamine release in the nucleus accumbens and ventral tegmental area in the rat: Measurement by in vivo microdialysis. Neurosci. Lett. 1992, 139, 73–76. [Google Scholar] [CrossRef]
- Martel, P.; Fantino, M. Influence of the amount of food ingested on mesolimbic dopaminergic system activity: A microdialysis study. Pharmacol. Biochem. Behav. 1996, 55, 297–302. [Google Scholar] [CrossRef]
- Martel, P.; Fantino, M. Mesolimbic dopaminergic system activity as a function of food reward: A microdialysis study. Pharmacol. Biochem. Behav. 1996, 53, 221–226. [Google Scholar] [CrossRef]
- Carelli, R.M.; Ijames, S.G.; Crumling, A.J. Evidence that separate neural circuits in the nucleus accumbens encode cocaine versus “natural” (water and food) reward. J. Neurosci. 2000, 20, 4255–4266. [Google Scholar] [CrossRef] [PubMed]
- Caine, S.B.; Koob, G.F. Effects of mesolimbic dopamine depletion on responding maintained by cocaine and food. J. Exp. Anal. Behav. 1994, 61, 213–221. [Google Scholar] [CrossRef] [PubMed]
- Rothemund, Y.; Preuschhof, C.; Bohner, G.; Bauknecht, H.-C.; Klingebiel, R.; Flor, H.; Klapp, B.F. Differential activation of the dorsal striatum by high-calorie visual food stimuli in obese individuals. NeuroImage 2007, 37, 410–421. [Google Scholar] [CrossRef]
- Small, D.M.; Jones-Gotman, M.; Dagher, A. Feeding-induced dopamine release in dorsal striatum correlates with meal pleasantness ratings in healthy human volunteers. NeuroImage 2003, 19, 1709–1715. [Google Scholar] [CrossRef]
- Volkow, N.D.; Wang, G.-J.; Fowler, J.S.; Logan, J.; Jayne, M.; Franceschi, D.; Wong, C.; Gatley, S.J.; Gifford, A.N.; Ding, Y.-S.; et al. Nonhedonic food motivation in humans involves dopamine in the dorsal striatum and methylphenidate amplifies this effect. Synapse 2002, 44, 175–180. [Google Scholar] [CrossRef] [PubMed]
- Volkow, N.D.; Wang, G.-J.; Maynard, L.; Jayne, M.; Fowler, J.S.; Zhu, W.; Logan, J.; Gatley, S.J.; Ding, Y.-S.; Wong, C.; et al. Brain dopamine is associated with eating behaviors in humans. Int. J. Eat. Disord. 2003, 33, 136–142. [Google Scholar] [CrossRef] [PubMed]
- Stoeckel, L.E.; Weller, R.E.; Cook, E.W.; Twieg, D.B.; Knowlton, R.C.; Cox, J.E.; Iii, E.W.C. Widespread reward-system activation in obese women in response to pictures of high-calorie foods. NeuroImage 2008, 41, 636–647. [Google Scholar] [CrossRef]
- Stice, E.; Spoor, S.; Bohon, C.; Small, D.M. Relation between obesity and blunted striatal response to food is moderated by TaqIA A1 allele. Science 2008, 322, 449–452. [Google Scholar] [CrossRef]
- Wang, G.-J.; Volkow, N.D.; Felder, C.; Fowler, J.S.; Levy, A.V.; Pappas, N.R.; Wong, C.T.; Zhu, W.; Netusil, N. Enhanced resting activity of the oral somatosensory cortex in obese subjects. NeuroReport 2002, 13, 1151–1155. [Google Scholar] [CrossRef] [PubMed]
- Bello, N.T.; Lucas, L.R.; Hajnal, A. Repeated sucrose access influences dopamine D2 receptor density in the striatum. NeuroReport 2002, 13, 1575–1578. [Google Scholar] [CrossRef] [PubMed]
- Johnson, P.M.; Kenny, P.J. Dopamine D2 receptors in addiction-like reward dysfunction and compulsive eating in obese rats. Nat. Neurosci. 2010, 13, 635–641. [Google Scholar] [CrossRef] [PubMed]
- Volkow, N.D.; Wang, G.-J.; Fowler, J.S.; Tomasi, D.; Telang, F.; Baler, R. Addiction: Decreased reward sensitivity and increased expectation sensitivity conspire to overwhelm the brain’s control circuit. BioEssays 2010, 32, 748–755. [Google Scholar] [CrossRef] [PubMed]
- Fehr, C.; Yakushev, I.; Hohmann, N.; Buchholz, H.G.; Landvogt, C.; Deckers, H.; Eberhardt, A.; Smolka, M.N.; Scheurich, A.; Dielentheis, T.; et al. Association of low striatal dopamine D 2 receptor availability with nicotine dependence similar to that seen with other drugs of abuse. Am. J. Psychiatr. 2008, 165, 507–514. [Google Scholar] [CrossRef] [PubMed]
- Heinz, A. Correlation Between Dopamine D2 Receptors in the Ventral Striatum and Central Processing of Alcohol Cues and Craving. Am. J. Psychiatr. 2004, 161, 1783–1789. [Google Scholar] [CrossRef] [PubMed]
- Volkow, N.D.; Fowler, J.S.; Wang, G.-J.; Hitzemann, R.; Logan, J.; Schlyer, D.J.; Dewey, S.L.; Wolf, A.P. Decreased dopamine D2 receptor availability is associated with reduced frontal metabolism in cocaine abusers. Synapse 1993, 14, 169–177. [Google Scholar] [CrossRef]
- Volkow, N.D.; Wang, G.-J.; Fowler, J.S.; Logan, J.; Hitzemann, R.; Ding, Y.-S.; Pappas, N.; Shea, C.; Piscani, K. Decreases in dopamine receptors but not in dopamine transporters in alcoholics. Alcohol. Clin. Exp. Res. 1996, 20, 1594–1598. [Google Scholar] [CrossRef] [PubMed]
- Volkow, N.D.; Chang, L.; Wang, G.-J.; Fowler, J.S.; Ding, Y.-S.; Sedler, M.; Logan, J.; Franceschi, D.; Gatley, J.; Hitzemann, R.; et al. Low level of brain dopamine D2 receptors in methamphetamine abusers: Association with metabolism in the orbitofrontal cortex. Am. J. Psychiatr. 2001, 158, 2015–2021. [Google Scholar] [CrossRef]
- Thanos, P.K.; Volkow, N.D.; Freimuth, P.; Umegaki, H.; Ikari, H.; Roth, G.; Ingram, D.K.; Hitzemann, R. Overexpression of dopamine D2 receptors reduces alcohol. J. Neurochem. 2001, 78, 1094–1103. [Google Scholar] [CrossRef]
- Volkow, N.D.; Wang, G.-J.; Begleiter, H.; Porjesz, B.; Fowler, J.S.; Telang, F.; Wong, C.; Ma, Y.; Logan, J.; Goldstein, R.; et al. High levels of dopamine D2 receptors in unaffected members of alcoholic families. Arch. Gen. Psychiatr. 2006, 63, 999–1008. [Google Scholar] [CrossRef]
- Reinholz, J.; Skopp, O.; Breitenstein, C.; Bohr, I.; Winterhoff, H.; Knecht, S. Compensatory weight gain due to dopaminergic hypofunction: New evidence and own incidental observations. Nutr. Metab. 2008, 5, 35. [Google Scholar] [CrossRef]
- Wang, G.; Volkow, N.D.; Thanos, P.K.; Fowler, J.S. Similarity between obesity and drug addiction as assessed by neurofunctional imaging: A concept review. J. Addict. Dis. 2004, 23, 39–53. [Google Scholar] [CrossRef] [PubMed]
- Hardman, C.A.; Herbert, V.M.; Brunstrom, J.M.; Munafò, M.R.; Rogers, P.J.; Brunstrom, J. Dopamine and food reward: Effects of acute tyrosine/phenylalanine depletion on appetite. Physiol. Behav. 2012, 105, 1202–1207. [Google Scholar] [CrossRef] [PubMed]
- Geiger, B.M.; Haburcak, M.; Avena, N.M.; Moyer, M.C.; Hoebel, B.G.; Pothos, E.N. Deficits of mesolimbic dopamine neurotransmission in rat dietary obesity. Neuroscience 2009, 159, 1193–1199. [Google Scholar] [CrossRef] [PubMed]
- Baptista, T.; Parada, M.; Hernández, L. Long term administration of some antipsychotic drugs increases body weight and feeding in rats. Are D2 dopamine receptors involved? Pharmacol. Biochem. Behav. 1987, 27, 399–405. [Google Scholar] [CrossRef]
- Clifton, P.G.; Rusk, I.N.; Cooper, S.J. Effects of dopamine D1 and dopamine D2 antagonists on the free feeding and drinking patterns of rats. Behav. Neurosci. 1991, 105, 272–281. [Google Scholar] [CrossRef]
- Scislowski, P.; Tozzo, E.; Zhang, Y.; Phaneuf, S.; Prevelige, R.; Cincotta, A. Biochemical mechanisms responsible for the attenuation of diabetic and obese conditions in ob/ob mice treated with dopaminergic agonists. Int. J. Obes. 1999, 23, 425–431. [Google Scholar] [CrossRef]
- Goudie, A.J.; Cooper, G.D.; Halford, J.C.G. Antipsychotic-induced weight gain. Diabetes Obes. Metab. 2005, 7, 478–487. [Google Scholar] [CrossRef]
- Cincotta, A.H.; Meier, A.H. Bromocriptine (Ergoset) reduces body weight and improves glucose tolerance in obese subjects. Diabetes Care 1996, 19, 667–670. [Google Scholar] [CrossRef]
- Manning, P.J.; Grattan, D.; Merriman, T.; Manning, T.; Williams, S.; Sutherland, W. Pharmaceutical interventions for weight-loss maintenance: No effect from cabergoline. Int. J. Obes. 2018, 42, 1871–1879. [Google Scholar] [CrossRef]
- Gibson, C.D.; Karmally, W.; McMahon, D.J.; Wardlaw, S.L.; Korner, J. Randomized pilot study of cabergoline, a dopamine receptor agonist: Effects on body weight and glucose tolerance in obese adults. Diabetes Obes. Metab. 2012, 14, 335–340. [Google Scholar] [CrossRef]
- Frank, G.K.W.; Shott, M.E.; Hagman, J.O.; Schiel, M.A.; DeGuzman, M.C.; Rossi, B. The Partial Dopamine D2 Receptor Agonist Aripiprazole is Associated With Weight Gain in Adolescent Anorexia Nervosa. Int. J. Eat. Disord. 2017, 50, 447–450. [Google Scholar] [CrossRef] [PubMed]
- Steele, K.E.; Prokopowicz, G.P.; Schweitzer, M.A.; Magunsuon, T.H.; Lidor, A.O.; Kuwabawa, H.; Kuma, A.; Brasic, J.; Wong, D.F. Alterations of central dopamine receptors before and after gastric bypass surgery. Obes. Surg. 2010, 20, 369–374. [Google Scholar] [CrossRef] [PubMed]
- Van Der Zwaal, E.M.; De Weijer, B.A.; Van De Giessen, E.M.; Janssen, I.; Berends, F.J.; Van De Laar, A.; Ackermans, M.T.; Fliers, E.; La Fleur, S.E.; Booij, J.; et al. Striatal dopamine D2/3 receptor availability increases after long-term bariatric surgery-induced weight loss. Eur. Neuropsychopharmacol. 2016, 26, 1190–1200. [Google Scholar] [CrossRef] [PubMed]
- Ochner, C.N.; Kwok, Y.; Conceição, E.; Pantazatos, S.P.; Puma, L.M.; Carnell, S.; Teixeira, J.; Hirsch, J.; Geliebter, A. Selective reduction in neural responses to high calorie foods following gastric bypass surgery. Ann. Surg. 2011, 253, 502–507. [Google Scholar] [CrossRef] [PubMed]
- Ghahremani, D.G.; Lee, B.; Robertson, C.L.; Tabibnia, G.; Morgan, A.T.; De Shetler, N.; Brown, A.K.; Monterosso, J.R.; Aron, A.A.; Mandelkern, M.A.; et al. Striatal dopamine D₂/D₃ receptors mediate response inhibition and related activity in frontostriatal neural circuitry in humans. J. Neurosci. 2012, 32, 7316–7324. [Google Scholar] [CrossRef] [PubMed]
- Lavagnino, L.; Arnone, D.; Cao, B.; Soares, J.C.; Selvaraj, S. Inhibitory control in obesity and binge eating disorder: A systematic review and meta-analysis of neurocognitive and neuroimaging studies. Neurosci. Biobehav. Rev. 2016, 68, 714–726. [Google Scholar] [CrossRef] [PubMed]
- Volkow, N.D.; Wang, G.-J.; Telang, F.; Fowler, J.S.; Goldstein, R.Z.; Alia-Klein, N.; Logan, J.; Wong, C.; Thanos, P.K.; Ma, Y.; et al. Inverse association between BMI and prefrontal metabolic activity in healthy adults. Obesity 2009, 17, 60–65. [Google Scholar] [CrossRef] [PubMed]
- Le, D.S.N.T.; Pannacciulli, N.; Chen, K.; Del Parigi, A.; Salbe, A.D.; Reiman, E.M.; Krakoff, J. Less activation of the left dorsolateral prefrontal cortex in response to a meal: A feature of obesity. Am. J. Clin. Nutr. 2006, 84, 725–731. [Google Scholar] [CrossRef]
- Le, D.S.N.; Pannacciulli, N.; Chen, K.; Salbe, A.D.; Hill, O.J.; Wing, R.R.; Reiman, E.M.; Krakoff, J. Less activation in the left dorsolateral prefrontal cortex in the reanalysis of the response to a meal in obese than in lean women and its association with successful weight loss. Am. J. Clin. Nutr. 2007, 86, 573–579. [Google Scholar] [CrossRef]
- Gautier, J.F.; Chen, K.; Salbe, A.D.; Bandy, D.; Pratley, R.E.; Heiman, M.; Ravussin, E.; Reiman, E.M.; Tataranni, P.A. Differential brain responses to satiation in obese and lean men. Diabetes 2000, 49, 838–846. [Google Scholar] [CrossRef]
- Del Parigi, A.; Chen, K.; Salbe, A.D.; Hill, J.O.; Wing, R.R.; Reiman, E.M.; Tataranni, P.A. Successful dieters have increased neural activity in cortical areas involved in the control of behavior. Int. J. Obes. 2007, 31, 440–448. [Google Scholar] [CrossRef] [PubMed]
- Hollmann, M.; Hellrung, L.; Pleger, B.; Schlögl, H.; Kabisch, S.; Stumvoll, M.; Villringer, A.; Horstmann, A. Neural correlates of the volitional regulation of the desire for food. Int. J. Obes. 2012, 36, 648–655. [Google Scholar] [CrossRef] [PubMed]
- McCaffery, J.M.; Haley, A.P.; Sweet, L.H.; Phelan, S.; Raynor, H.A.; Del Parigi, A.; Cohen, R.; Wing, R.R. Differential functional magnetic resonance imaging response to food pictures in successful weight-loss maintainers relative to normal-weight and obese controls. Am. J. Clin. Nutr. 2009, 90, 928–934. [Google Scholar] [CrossRef] [PubMed]
- Weygandt, M.; Mai, K.; Dommes, E.; Leupelt, V.; Hackmack, K.; Kahnt, T.; Rothemund, Y.; Spranger, J.; Haynes, J.-D. The role of neural impulse control mechanisms for dietary success in obesity. NeuroImage 2013, 83, 669–678. [Google Scholar] [CrossRef] [PubMed]
- Nederkoorn, C.; Houben, K.; Hofmann, W.; Roefs, A.; Jansen, A. Control yourself or just eat what you like? Weight gain over a year is predicted by an interactive effect of response inhibition and implicit preference for snack foods. Health Psychol. 2010, 29, 389–393. [Google Scholar] [CrossRef] [PubMed]
- Cohen, J.; Yates, K.F.; Duong, M.; Convit, A. Obesity, orbitofrontal structure and function are associated with food choice: A cross-sectional study. BMJ Open 2011, 1, e000175. [Google Scholar] [CrossRef] [PubMed]
- Maayan, L.; Hoogendoorn, C.; Sweat, V.; Convit, A. Disinhibited eating in obese adolescents is associated with orbitofrontal volume reductions and executive dysfunction. Obesity 2011, 19, 1382–1387. [Google Scholar] [CrossRef] [PubMed]
- Masouleh, S.K.; Arelin, K.; Horstmann, A.; Lampe, L.; Kipping, J.A.; Luck, T.; Riedel-Heller, S.G.; Schroeter, M.L.; Stumvoll, M.; Villringer, A.; et al. Higher body mass index in older adults is associated with lower gray matter volume: Implications for memory performance. Neurobiol. Aging 2016, 40, 1–10. [Google Scholar] [CrossRef]
- Pannacciulli, N.; Del Parigi, A.; Chen, K.; Le, D.S.N.; Reiman, E.M.; Tataranni, P.A. Brain abnormalities in human obesity: A voxel-based morphometric study. NeuroImage 2006, 31, 1419–1425. [Google Scholar] [CrossRef]
- Taki, Y.; Kinomura, S.; Sato, K.; Inoue, K.; Goto, R.; Okada, K.; Uchida, S.; Kawashima, R.; Fukuda, H. Relationship between body mass index and gray matter volume in 1428 healthy individuals. Obesity 2008, 16, 119–124. [Google Scholar] [CrossRef]
- Walther, K.; Birdsill, A.C.; Glisky, E.L.; Ryan, L. Structural brain differences and cognitive functioning related to body mass index in older females. Hum. Brain Mapp. 2010, 31, 1052–1064. [Google Scholar] [CrossRef] [PubMed]
- Yao, L.; Li, W.; Dai, Z.; Dong, C. Eating behavior associated with gray matter volume alternations: A voxel based morphometry study. Appetite 2016, 96, 572–579. [Google Scholar] [CrossRef] [PubMed]
- Yokum, S.; Stice, E. Cognitive regulation of food craving: Effects of three cognitive reappraisal strategies on neural response to palatable foods. Int. J. Obes. 2013, 37, 1565–1570. [Google Scholar] [CrossRef] [PubMed]
- Bechara, A. Decision making, impulse control and loss of willpower to resist drugs: A neurocognitive perspective. Nat. Neurosci. 2005, 8, 1458–1463. [Google Scholar] [CrossRef] [PubMed]
- Davis, C.; Levitan, R.D.; Muglia, P.; Bewell, C.; Kennedy, J.L. Decision-making deficits and overeating: A risk model for obesity. Obes. Res. 2004, 12, 929–935. [Google Scholar] [CrossRef] [PubMed]
- Elias, M.F.; Elias, P.K.; Sullivan, L.M.; Wolf, P.A.; D’Agostino, R.B. Obesity, diabetes and cognitive deficit: The Framingham heart study. Neurobiol. Aging 2005, 26, 11–16. [Google Scholar] [CrossRef] [PubMed]
- Gunstad, J.; Paul, R.H.; Cohen, R.A.; Tate, D.F.; Spitznagel, M.B.; Gordon, E. Elevated body mass index is associated with executive dysfunction in otherwise healthy adults. Compr. Psychiatr. 2007, 48, 57–61. [Google Scholar] [CrossRef] [PubMed]
- Lowe, C.J.; Reichelt, A.C.; Hall, P.A. The prefrontal cortex and obesity: A health neuroscience perspective. Trends Cogn. Sci. 2019, 23, 349–361. [Google Scholar] [CrossRef] [PubMed]
- Blum, K.; Braverman, E.R.; Wood, R.C.; Gill, J.; Li, C.; Chen, T.J.; Taub, M.; Montgomery, A.R.; Sheridan, P.J.; Cull, J.G. Increased prevalence of the Taq I A1allele of the dopamine receptor gene (DRD2) in obesity with comorbid substance use disorder: A preliminary report. Pharmacogenetics 1996, 6, 297–305. [Google Scholar] [CrossRef] [PubMed]
- Comings, D.E.; Muhleman, D.; Ahn, C.; Gysin, R.; Flanagan, S.D. The dopamine D2 receptor gene: A genetic risk factor in substance abuse. Drug Alcohol Depend. 1994, 34, 175–180. [Google Scholar] [CrossRef]
- Han, D.H.; Yoon, S.J.; Sung, Y.H.; Lee, Y.S.; Kee, B.S.; Lyoo, I.K.; Renshaw, P.F.; Cho, S.C. A preliminary study: Novelty seeking, frontal executive function, and dopamine receptor (D2) TaqI A gene polymorphism in patients with methamphetamine dependence. Compr. Psychiatr. 2008, 49, 387–392. [Google Scholar] [CrossRef] [PubMed]
- Jönsson, E.G.; Nöthen, M.M.; Grünhage, F.; Farde, L.; Nakashima, Y.; Propping, P.; Sedvall, G.C.; Nöthen, M.; Jönsson, E. Polymorphisms in the dopamine D2 receptor gene and their relationships to striatal dopamine receptor density of healthy volunteers. Mol. Psychiatr. 1999, 4, 290–296. [Google Scholar] [CrossRef]
- Noble, E. Addiction and its reward process through polymorphisms of the D2 dopamine receptor gene: A review. Eur. Psychiatr. 2000, 15, 79–89. [Google Scholar] [CrossRef]
- Spitz, M.R.; Detry, M.A.; Pillow, P.; Hu, Y.; Amos, C.I.; Hong, W.K.; Wu, X. Variant alleles of the D2 dopamine receptor gene and obesity. Nutr. Res. 2000, 20, 371–380. [Google Scholar] [CrossRef]
- Eisenberg, D.T.; MacKillop, J.; Modi, M.; Beauchemin, J.; Dang, D.; Lisman, S.A.; Lum, J.K.; Wilson, D.S. Examining impulsivity as an endophenotype using a behavioral approach: A DRD2 TaqI A and DRD4 48-bp VNTR association study. Behav. Brain Funct. 2007, 3, 2. [Google Scholar] [CrossRef] [PubMed]
- Kirsch, P.; Reuter, M.; Mier, D.; Lonsdorf, T.; Stark, R.; Gallhofer, B.; Vaitl, D.; Hennig, J. Imaging gene–substance interactions: The effect of the DRD2 TaqIA polymorphism and the dopamine agonist bromocriptine on the brain activation during the anticipation of reward. Neurosci. Lett. 2006, 405, 196–201. [Google Scholar] [CrossRef]
- Klein, T.A.; Neumann, J.; Reuter, M.; Hennig, J.; Von Cramon, D.Y.; Ullsperger, M. Genetically determined differences in learning from errors. Science 2007, 318, 1642–1645. [Google Scholar] [CrossRef]
- Montag, C.; Weber, B.; Jentgens, E.; Elger, C.; Reuter, M. An epistasis effect of functional variants on the BDNF and DRD2 genes modulates gray matter volume of the anterior cingulate cortex in healthy humans. Neuropsychology 2010, 48, 1016–1021. [Google Scholar] [CrossRef]
- Gasquoine, P.G. Localization of function in anterior cingulate cortex: From psychosurgery to functional neuroimaging. Neurosci. Biobehav. Rev. 2013, 37, 340–348. [Google Scholar] [CrossRef]
- Peoples, L.L. Will, anterior cingulate cortex, and addiction. Science 2002, 296, 1623–1624. [Google Scholar] [CrossRef]
- Brody, A.L.; Mandelkern, M.A.; Olmstead, R.E.; Jou, J.; Tiongson, E.; Allen, V.; Scheibal, D.; London, E.D.; Monterosso, J.R.; Tiffany, S.T.; et al. Neural substrates of resisting craving during cigarette cue exposure. Biol. Psychiatr. 2007, 62, 642–651. [Google Scholar] [CrossRef] [PubMed]
- Pursey, K.M.; Stanwell, P.; Gearhardt, A.N.; Collins, C.E.; Burrows, T.L. The prevalence of food addiction as assessed by the Yale food addiction scale: A systematic review. Nutrients 2014, 6, 4552–4590. [Google Scholar] [CrossRef] [PubMed]
- Carter, J.C.; Van Wijk, M.; Rowsell, M. Symptoms of ‘food addiction’ in binge eating disorder using the Yale food addiction scale version 2.0. Appetite 2019, 133, 362–369. [Google Scholar] [CrossRef] [PubMed]
- De Vries, S.-K.; Meule, A. Food addiction and bulimia nervosa: New data based on the Yale food addiction scale 2.0. Eur. Eat. Disord. Rev. 2016, 24, 518–522. [Google Scholar] [CrossRef] [PubMed]
- Hall, P.A.; Fong, G.T.; Epp, L.J.; Elias, L.J. Executive function moderates the intention-behavior link for physical activity and dietary behavior. Psychol. Health 2008, 23, 309–326. [Google Scholar] [CrossRef] [PubMed]
- Hall, P.A. Executive control resources and frequency of fatty food consumption: Findings from an age-stratified community sample. Health Psychol. 2012, 31, 235–241. [Google Scholar] [CrossRef] [PubMed]
- Alcorn, J.L.; Marks, K.R.; Stoops, W.W.; Rush, C.R.; Lile, J.A. Attentional bias to cannabis cues in cannabis users but not cocaine users. Addict. Behav. 2019, 88, 129–136. [Google Scholar] [CrossRef] [PubMed]
- Bradley, B.; Field, M.; Mogg, K.; De Houwer, J. Attentional and evaluative biases for smoking cues in nicotine dependence: Component processes of biases in visual orienting. Behav. Pharmacol. 2004, 15, 29–36. [Google Scholar] [CrossRef]
- Field, M.; Eastwood, B.; Bradley, B.P.; Mogg, K. Selective processing of cannabis cues in regular cannabis users. Drug Alcohol Depend. 2006, 85, 75–82. [Google Scholar] [CrossRef]
- Qureshi, A.; Monk, R.L.; Pennington, C.R.; Wilcockson, T.D.; Heim, D. Alcohol-related attentional bias in a gaze contingency task: Comparing appetitive and non-appetitive cues. Addict. Behav. 2019, 90, 312–317. [Google Scholar] [CrossRef]
- Field, M.; Cox, W. Attentional bias in addictive behaviors: A review of its development, causes, and consequences. Drug Alcohol Depend. 2008, 97, 1–20. [Google Scholar] [CrossRef] [PubMed]
- Franken, I.H. Drug craving and addiction: Integrating psychological and neuropsychopharmacological approaches. Prog. Neuro Psychopharmacol. Biol. Psychiatr. 2003, 27, 563–579. [Google Scholar] [CrossRef]
- Detandt, S.; Verbanck, P.; Bazan, A.; Quertemont, E. Smoking addiction: The shift from head to hands: Approach bias towards smoking-related cues in low-dependent versus dependent smokers. J. Psychopharmacol. 2017, 31, 819–829. [Google Scholar] [CrossRef] [PubMed]
- Weckler, H.; Kong, G.; Larsen, H.; Cousijn, J.; Wiers, R.W.; Krishnan-Sarin, S. Impulsivity and approach tendencies towards cigarette stimuli: Implications for cigarette smoking and cessation behaviors among youth. Exp. Clin. Psychopharmacol. 2017, 25, 363–372. [Google Scholar] [CrossRef] [PubMed]
- Watson, P.; De Wit, S.; Hommel, B.; Wiers, R.W. Motivational mechanisms and outcome expectancies underlying the approach bias toward addictive substances. Front. Psychol. 2012, 3, 440. [Google Scholar] [CrossRef] [PubMed]
- Beraha, E.M.; Cousijn, J.; Hermanides, E.; Goudriaan, A.E.; Wiers, R.W. Implicit Associations and Explicit Expectancies toward Cannabis in Heavy Cannabis Users and Controls. Front. Psychol. 2013, 4, 1–9. [Google Scholar] [CrossRef]
- De Houwer, J.; Custers, R.; De Clercq, A. Do smokers have a negative implicit attitude toward smoking? Cogn. Emot. 2006, 20, 1274–1284. [Google Scholar] [CrossRef]
- Houben, K.; Wiers, R.W. Are drinkers implicitly positive about drinking alcohol? Personalizing the alcohol-IAT to reduce negative extrapersonal contamination. Alcohol Alcohol. 2007, 42, 301–307. [Google Scholar] [CrossRef]
- McCarthy, D.M.; Thompsen, D.M. Implicit and explicit measures of alcohol and smoking cognitions. Psychol. Addict. Behav. 2006, 20, 436–444. [Google Scholar] [CrossRef]
- Brignell, C.; Griffiths, T.; Bradley, B.P.; Mogg, K. Attentional and approach biases for pictorial food cues. Influence of external eating. Appetite 2009, 52, 299–306. [Google Scholar] [CrossRef]
- Deluchi, M.; Costa, F.S.; Friedman, R.; Gonçalves, R.; Bizarro, L. Attentional bias to unhealthy food in individuals with severe obesity and binge eating. Appetite 2017, 108, 471–476. [Google Scholar] [CrossRef] [PubMed]
- Hardman, C.A.; Scott, J.; Field, M.; Jones, A. To eat or not to eat. The effects of expectancy on reactivity to food cues. Appetite 2014, 76, 153–160. [Google Scholar] [CrossRef] [PubMed]
- Popien, A.; Frayn, M.; Von Ranson, K.M.; Sears, C.R. Eye gaze tracking reveals heightened attention to food in adults with binge eating when viewing images of real-world scenes. Appetite 2015, 91, 233–240. [Google Scholar] [CrossRef] [PubMed]
- Field, M.; Werthmann, J.; Franken, I.; Hofmann, W.; Hogarth, L.; Roefs, A. The role of attentional bias in obesity and addiction. Health Psychol. 2016, 35, 767–780. [Google Scholar] [CrossRef] [PubMed]
- Stojek, M.; Shank, L.M.; Vannucci, A.; Bongiorno, D.M.; Nelson, E.E.; Waters, A.J.; Engel, S.G.; Boutelle, K.N.; Pine, D.S.; Yanovski, J.A.; et al. A systematic review of attentional biases in disorders involving binge eating. Appetite 2018, 123, 367–389. [Google Scholar] [CrossRef]
- Castellanos, E.H.; Charboneau, E.; Dietrich, M.S.; Park, S.; Bradley, B.P.; Mogg, K.; Cowan, R.L.; Bradley, B. Obese adults have visual attention bias for food cue images: Evidence for altered reward system function. Int. J. Obes. 2009, 33, 1063–1073. [Google Scholar] [CrossRef]
- Iceta, S.; Benoit, J.; Cristini, P.; Lambert-Porcheron, S.; Segrestin, B.; Laville, M.; Poulet, E.; Disse, E. Attentional bias and response inhibition in severe obesity with food disinhibition: A study of P300 and N200 event-related potential. Int. J. Obes. 2019, 1. [Google Scholar] [CrossRef]
- Nijs, I.M.; Muris, P.; Euser, A.S.; Franken, I.H. Differences in attention to food and food intake between overweight/obese and normal-weight females under conditions of hunger and satiety. Appetite 2010, 54, 243–254. [Google Scholar] [CrossRef]
- Werthmann, J.; Roefs, A.; Nederkoorn, C.; Mogg, K.; Bradley, B.P.; Jansen, A. Can (not) take my eyes off it: Attention bias for food in overweight participants. Health Psychol. 2011, 30, 561–569. [Google Scholar] [CrossRef]
- Hardman, C.A.; Rogers, P.J.; Etchells, K.A.; Houstoun, K.V.E.; Munafò, M.R. The effects of food-related attentional bias training on appetite and food intake. Appetite 2013, 71, 295–300. [Google Scholar] [CrossRef]
- Kemps, E.; Tiggemann, M.; Orr, J.; Grear, J. Attentional retraining can reduce chocolate consumption. J. Exp. Psychol. Appl. 2013, 20, 94–102. [Google Scholar] [CrossRef] [PubMed]
- Schmitz, F.; Svaldi, J. Effects of bias modification training in binge eating disorder. Behav. Ther. 2017, 48, 707–717. [Google Scholar] [CrossRef] [PubMed]
- Werthmann, J.; Field, M.; Roefs, A.; Nederkoorn, C.; Jansen, A. Attention bias for chocolate increases chocolate consumption—An attention bias modification study. J. Behav. Ther. Exp. Psychiatr. 2014, 45, 136–143. [Google Scholar] [CrossRef] [PubMed]
- Zhang, S.; Cui, L.; Sun, X.; Zhang, Q. The effect of attentional bias modification on eating behavior among women craving high-calorie food. Appetite 2018, 129, 135–142. [Google Scholar] [CrossRef] [PubMed]
- Smith, E.; Treffiletti, A.; Bailey, E.P.; Moustafa, A. The effect of attentional bias modification training on food intake in overweight and obese women. J. Health Psychol. 2018, 1–11. [Google Scholar] [CrossRef] [PubMed]
- Kakoschke, N.L.; Kemps, E.; Tiggemann, M. Attentional bias modification encourages healthy eating. Eat. Behav. 2014, 15, 120–124. [Google Scholar] [CrossRef] [PubMed]
- Kemps, E.; Tiggemann, M.; Elford, J. Sustained effects of attentional re-training on chocolate consumption. J. Behav. Ther. Exp. Psychiatr. 2015, 49, 94–100. [Google Scholar] [CrossRef] [PubMed]
- Veenstra, E.M.; De Jong, P.J. Restrained eaters show enhanced automatic approach tendencies towards food. Appetite 2010, 55, 30–36. [Google Scholar] [CrossRef]
- Becker, D.; Jostmann, N.B.; Wiers, R.W.; Holland, R.W. Approach avoidance training in the eating domain: Testing the effectiveness across three single session studies. Appetite 2015, 85, 58–65. [Google Scholar] [CrossRef]
- Brockmeyer, T.; Hahn, C.; Reetz, C.; Schmidt, U.; Friederich, H.-C. Approach bias and cue reactivity towards food in people with high versus low levels of food craving. Appetite 2015, 95, 197–202. [Google Scholar] [CrossRef]
- Havermans, R.C.; Giesen, J.C.; Houben, K.; Jansen, A. Weight, gender, and snack appeal. Eat. Behav. 2011, 12, 126–130. [Google Scholar] [CrossRef] [PubMed]
- Mehl, N.; Mueller-Wieland, L.; Mathar, D.; Horstmann, A. Retraining automatic action tendencies in obesity. Physiol. Behav. 2018, 192, 50–58. [Google Scholar] [CrossRef] [PubMed]
- Mogg, K.; Bradley, B.P.; O’Neill, B.; Bani, M.; Merlo-Pich, E.; Koch, A.; Bullmore, E.T.; Nathan, P.J. Effect of dopamine D₃ receptor antagonism on approach responses to food cues in overweight and obese individuals. Behav. Pharmacol. 2012, 23, 603–608. [Google Scholar] [CrossRef] [PubMed]
- Kemps, E.; Tiggemann, M.; Martin, R.; Elliott, M. Implicit approach–avoidance associations for craved food cues. J. Exp. Psychol. Appl. 2013, 19, 30–38. [Google Scholar] [CrossRef] [PubMed]
- Schumacher, S.E.; Kemps, E.; Tiggemann, M. Bias modification training can alter approach bias and chocolate consumption. Appetite 2016, 96, 219–224. [Google Scholar] [CrossRef] [PubMed]
- Brockmeyer, T.; Hahn, C.; Reetz, C.; Schmidt, U.; Friederich, H.-C. Approach Bias Modification in Food Craving-A Proof-of-Concept Study. Eur. Eat. Disord. Rev. 2015, 23, 352–360. [Google Scholar] [CrossRef] [PubMed]
- De Houwer, J. A conceptual and theoretical analysis of evaluative conditioning. Span. J. Psychol. 2007, 10, 230–241. [Google Scholar] [CrossRef] [PubMed]
- De Houwer, J.; Thomas, S.; Baeyens, F. Association learning of likes and dislikes: A review of 25 years of research on human evaluative conditioning. Psychol. Bull. 2001, 127, 853–869. [Google Scholar] [CrossRef] [PubMed]
- Dwyer, D.M.; Jarratt, F.; Dick, K. Evaluative conditioning with foods as CSs and body shapes as USs: No evidence for sex differences, extinction, or overshadowing. Cogn. Emot. 2007, 21, 281–299. [Google Scholar] [CrossRef]
- Hollands, G.J.; Prestwich, A.; Marteau, T.M. Using aversive images to enhance healthy food choices and implicit attitudes: An experimental test of evaluative conditioning. Health Psychol. 2011, 30, 195–203. [Google Scholar] [CrossRef]
- Lascelles, K.R.; Field, A.P.; Davey, G.C. Using foods as CSs and body shapes as UCSs: A putative role for associative learning in the development of eating disorders. Behav. Ther. 2003, 34, 213–235. [Google Scholar] [CrossRef][Green Version]
- Lebens, H.; Roefs, A.; Martijn, C.; Houben, K.; Nederkoorn, C.; Jansen, A. Making implicit measures of associations with snack foods more negative through evaluative conditioning. Eat. Behav. 2011, 12, 249–253. [Google Scholar] [CrossRef] [PubMed]
- Wang, Y.; Wang, G.; Zhang, D.; Wang, L.; Cui, X.; Zhu, J.; Fang, Y. Learning to dislike chocolate: Conditioning negative attitudes toward chocolate and its effect on chocolate consumption. Front. Psychol. 2017, 8, 1–7. [Google Scholar] [CrossRef] [PubMed]
- Walsh, E.M.; Kiviniemi, M.T. Changing how I feel about the food: Experimentally manipulated affective associations with fruits change fruit choice behaviors. J. Behav. Med. 2014, 37, 322–331. [Google Scholar] [CrossRef] [PubMed]
- Shaw, J.A.; Forman, E.M.; Espel, H.M.; Butryn, M.L.; Herbert, J.D.; Lowe, M.R.; Nederkoorn, C. Can evaluative conditioning decrease soft drink consumption? Appetite 2016, 105, 60–70. [Google Scholar] [CrossRef]
- Houben, K.; Havermans, R.C.; Wiers, R.W. Learning to dislike alcohol: Conditioning negative implicit attitudes toward alcohol and its effect on drinking behavior. Psychopharmacology 2010, 211, 79–86. [Google Scholar] [CrossRef] [PubMed]
- Zerhouni, O.; Houben, K.; El Methni, J.; Rutte, N.; Werkman, E.; Wiers, R.W. I didn’t feel like drinking, but I guess why: Evaluative conditioning changes on explicit attitudes toward alcohol and healthy foods depends on contingency awareness. Learn. Motiv. 2019, 66, 1–12. [Google Scholar] [CrossRef]
- Hofmann, W.; De Houwer, J.; Perugini, M.; Baeyens, F.; Crombez, G. Evaluative conditioning in humans: A meta-analysis. Psychol. Bull. 2010, 136, 390–421. [Google Scholar] [CrossRef]
- Benedict, T.; Richter, J.; Gast, A. The influence of misinformation manipulations on evaluative conditioning. Acta Psychol. 2019, 194, 28–36. [Google Scholar] [CrossRef]
- Aron, A.R.; Robbins, T.W.; Poldrack, R.A. Inhibition and the right inferior frontal cortex. Trends Cogn. Sci. 2004, 8, 170–177. [Google Scholar] [CrossRef]
- Aron, A.R.; Robbins, T.W.; Poldrack, R.A. Inhibition and the right inferior frontal cortex: One decade on. Trends Cogn. Sci. 2014, 18, 177–185. [Google Scholar] [CrossRef] [PubMed]
- Logan, G.D. Executive control of thought and action. Acta Psychol. 1985, 60, 193–210. [Google Scholar] [CrossRef]
- Logan, G.D.; Cowan, W.B. On the ability to inhibit thought and action: A theory of an act of control. Psychol. Rev. 1984, 91, 295–327. [Google Scholar] [CrossRef]
- Logan, G.D.; Schachar, R.J.; Tannock, R. Impulsivity and inhibitory control. Psychol. Sci. 1997, 8, 60–64. [Google Scholar] [CrossRef]
- Miyake, A.; Friedman, N.P.; Emerson, M.J.; Witzki, A.H.; Howerter, A.; Wager, T.D. The unity and diversity of executive functions and their contributions to complex “frontal lobe” tasks: A latent variable analysis. Cogn. Psychol. 2000, 41, 49–100. [Google Scholar] [CrossRef] [PubMed]
- Nigg, J.T.; Wong, M.M.; Martel, M.M.; Jester, J.M.; Puttler, L.I.; Glass, J.M.; Adams, K.M.; Fitzgerald, H.E.; Zucker, R.A. Poor response inhibition as a predictor of problem drinking and illicit drug use in adolescents at risk for alcoholism and other substance use disorders. J. Am. Acad. Child Adolesc. Psychiatr. 2006, 45, 468–475. [Google Scholar] [CrossRef]
- Krishnan-Sarin, S.; Reynolds, B.; Duhig, A.M.; Smith, A.; Liss, T.; McFetridge, A.; Cavallo, D.A.; Carroll, K.M.; Potenza, M.N. Behavioral impulsivity predicts treatment outcome in a smoking cessation program for adolescents. Drug Alcohol Depend. 2007, 88, 79–82. [Google Scholar] [CrossRef]
- Czapla, M.; Simon, J.J.; Richter, B.; Kluge, M.; Friederich, H.C.; Herpertz, S.; Loeber, S. The impact of cognitive impairment and impulsivity on relapse of alcohol-dependent patients: Implications for psychotherapeutic treatment. Addict. Biol. 2016, 21, 873–884. [Google Scholar] [CrossRef]
- Houben, K.; Wiers, R.W. Response inhibition moderates the relationship between implicit associations and drinking behavior. Alcohol. Clin. Exp. Res. 2009, 33, 626–633. [Google Scholar] [CrossRef]
- Nederkoorn, C.; Smulders, F.T.; Havermans, R.C.; Roefs, A.; Jansen, A. Impulsivity in obese women. Appetite 2006, 47, 253–256. [Google Scholar] [CrossRef]
- Price, M.; Lee, M.; Higgs, S. Food-specific response inhibition, dietary restraint and snack intake in lean and overweight/obese adults: A moderated-mediation model. Int. J. Obes. 2016, 40, 877. [Google Scholar] [CrossRef] [PubMed]
- Houben, K. Overcoming the urge to splurge: Influencing eating behavior by manipulating inhibitory control. J. Behav. Ther. Exp. Psychiatr. 2011, 42, 384–388. [Google Scholar] [CrossRef] [PubMed]
- Nederkoorn, C.; Dassen, F.C.; Franken, L.; Resch, C.; Houben, K. Impulsivity and overeating in children in the absence and presence of hunger. Appetite 2015, 93, 57–61. [Google Scholar] [CrossRef] [PubMed]
- Houben, K.; Nederkoorn, C.; Jansen, A. Eating on impulse: The relation between overweight and food-specific inhibitory control. Obesity 2014, 22, e6–e8. [Google Scholar] [CrossRef] [PubMed]
- Mühlberg, C.; Mathar, D.; Villringer, A.; Horstmann, A.; Neumann, J. Stopping at the sight of food—How gender and obesity impact on response inhibition. Appetite 2016, 107, 663–676. [Google Scholar] [CrossRef] [PubMed]
- Meule, A.; Lutz, A.P.; Vögele, C.; Kübler, A. Impulsive reactions to food-cues predict subsequent food craving. Eat. Behav. 2014, 15, 99–105. [Google Scholar] [CrossRef] [PubMed]
- Allan, J.L.; Johnston, M.; Campbell, N. Missed by an inch or a mile? Predicting the size of intention–behaviour gap from measures of executive control. Psychol. Health 2011, 26, 635–650. [Google Scholar] [CrossRef]
- Rosval, L.; Steiger, H.; Bruce, K.; Israël, M.; Richardson, J.; Aubut, M. Impulsivity in women with eating disorders: Problem of response inhibition, planning, or attention? Int. J. Eat. Disord. 2006, 39, 590–593. [Google Scholar] [CrossRef]
- Bowley, C.; Faricy, C.; Hegarty, B.; Johnstone, S.J.; Smith, J.L.; Kelly, P.J.; Rushby, J.A. The effects of inhibitory control training on alcohol consumption, implicit alcohol-related cognitions and brain electrical activity. Int. J. Psychophysiol. 2013, 89, 342–348. [Google Scholar] [CrossRef]
- Di Lemma, L.C.G.; Field, M. Cue avoidance training and inhibitory control training for the reduction of alcohol consumption: A comparison of effectiveness and investigation of their mechanisms of action. Psychopharmacology 2017, 234, 2489–2498. [Google Scholar] [CrossRef]
- Houben, K.; Havermans, R.C.; Nederkoorn, C.; Jansen, A. Beer à no-go: Learning to stop responding to alcohol cues reduces alcohol intake via reduced affective associations rather than increased response inhibition. Addiction 2012, 107, 1280–1287. [Google Scholar] [CrossRef] [PubMed]
- Houben, K.; Nederkoorn, C.; Wiers, R.W.; Jansen, A. Resisting temptation: Decreasing alcohol-related affect and drinking behaviour by training response inhibition. Drug Alcohol Depend. 2011, 116, 132–136. [Google Scholar] [CrossRef] [PubMed]
- Kilwein, T.M.; Bernhardt, K.A.; Stryker, M.L.; Looby, A. Decreased alcohol consumption after pairing alcohol-related cues with an inhibitory response. J. Subst. Use 2017, 23, 154–161. [Google Scholar] [CrossRef]
- Verbruggen, F.; Adams, R.; Chambers, C.D. Proactive motor control reduces monetary risk taking in gambling. Psychol. Sci. 2012, 23, 805–815. [Google Scholar] [CrossRef] [PubMed]
- Verbruggen, F.; Adams, R.C.; Van’t Wout, F.; Stevens, T.; McLaren, I.P.L.; Chambers, C.D. Are the effects of response inhibition on gambling long-lasting? PLoS ONE 2013, 7, e70155. [Google Scholar] [CrossRef] [PubMed]
- Adams, R.C.; Lawrence, N.S.; Verbruggen, F.; Chambers, C.D. Training response inhibition to reduce food consumption: Mechanisms, stimulus specificity and appropriate training protocols. Appetite 2017, 109, 11–23. [Google Scholar] [CrossRef] [PubMed]
- Houben, K.; Jansen, A. Training inhibitory control. A recipe for resisting sweet temptations. Appetite 2011, 56, 345–349. [Google Scholar] [CrossRef]
- Houben, K.; Jansen, A. Chocolate equals stop. Chocolate-specific inhibition training reduces chocolate intake and go associations with chocolate. Appetite 2015, 87, 318–323. [Google Scholar] [CrossRef]
- Lawrence, N.S.; Verbruggen, F.; Morrison, S.; Adams, R.C.; Chambers, C.D. Stopping to food pictures reduces food intake: Effects of cue specificity, control conditions and individual differences. Appetite 2015, 85, 91–103. [Google Scholar] [CrossRef]
- Oomen, D.; Grol, M.; Spronk, D.; Booth, C.; Fox, E. Beating uncontrolled eating: Training inhibitory control to reduce food intake and food cue sensitivity. Appetite 2018, 131, 73–83. [Google Scholar] [CrossRef]
- Camp, B.; Lawrence, N.S. Giving pork the chop: Response inhibition training to reduce meat intake. Appetite 2019, 141, 104315. [Google Scholar] [CrossRef] [PubMed]
- Chen, Z.; Holland, R.W.; Quandt, J.; Dijksterhuis, A.; Veling, H. When mere action versus inaction leads to robust preference change. J. Personal. Soc. Psychol. 2019. [Google Scholar] [CrossRef] [PubMed]
- Porter, L.; Bailey-Jones, C.; Priudokaite, G.; Allen, S.; Wood, K.; Stiles, K.; Lawrence, N.S. From cookies to carrots; the effect of inhibitory control training on children’s snack selections. Appetite 2018, 124, 111–123. [Google Scholar] [CrossRef] [PubMed]
- Van Koningsbruggen, G.M.; Veling, H.; Stroebe, W.; Aarts, H. Comparing two psychological interventions in reducing impulsive processes of eating behaviour: Effects on self-selected portion size. Br. J. Health Psychol. 2013, 19, 767–782. [Google Scholar] [CrossRef] [PubMed]
- Veling, H.; Aarts, H.; Stroebe, W. Using stop signals to reduce impulsive choices for palatable unhealthy foods. Br. J. Health Psychol. 2013, 18, 354–368. [Google Scholar] [CrossRef] [PubMed]
- Veling, H.; Aarts, H.; Stroebe, W. Stop signals decrease choices for palatable foods through decreased food evaluation. Front. Psychol. 2013, 4, 875. [Google Scholar] [CrossRef] [PubMed]
- Gish, M.Y. Addiction to food: How go/no-go tasks affect appetite. Biomed. Health Sci. Res. 2015, 6, 221–231. [Google Scholar] [CrossRef][Green Version]
- Veling, H.; van Koningsbruggen, G.M.; Aarts, H.; Stroebe, W. Targeting impulsive processes of eating behavior via the internet. Effects on body weight. Appetite 2014, 78, 102–109. [Google Scholar] [CrossRef]
- Allom, V.; Mullan, B.; Hagger, M. Does inhibitory control training improve health behaviour? A meta-analysis. Health Psychol. Rev. 2015, 10, 1–38. [Google Scholar] [CrossRef]
- Jones, A.; Di Lemma, L.C.; Robinson, E.; Christiansen, P.; Nolan, S.; Tudur-Smith, C.; Field, M. Inhibitory control training for appetitive behaviour change: A meta-analytic investigation of mechanisms of action and moderators of effectiveness. Appetite 2016, 97, 16–28. [Google Scholar] [CrossRef]
- Lawrence, N.S.; O’Sullivan, J.; Parslow, D.; Javaid, M.; Adams, R.C.; Chambers, C.D.; Kos, K.; Verbruggen, F. Training response inhibition to food is associated with weight loss and reduced energy intake. Appetite 2015, 95, 17–28. [Google Scholar] [CrossRef] [PubMed]
- Kakoschke, N.L.; Kemps, E.; Tiggemann, M. The effect of combined avoidance and control training on implicit food evaluation and choice. J. Behav. Ther. Exp. Psychiatr. 2017, 55, 99–105. [Google Scholar] [CrossRef] [PubMed]
- Schakel, L.; Veldhuijzen, D.S.; Van Middendorp, H.; Van Dessel, P.; De Houwer, J.; Bidarra, R.; Evers, A.W.M. The effects of a gamified approach avoidance training and verbal suggestions on food outcomes. PLoS ONE 2018, 13, e0201309. [Google Scholar] [CrossRef] [PubMed]
- Chen, Z.; Veling, H.; Dijksterhuis, A.; Holland, R.W. Do impulsive individuals benefit more from food go/no-go training? Testing the role of inhibition capacity in the no-go devaluation effect. Appetite 2018, 124, 99–110. [Google Scholar] [CrossRef] [PubMed]
- McLaren, I.P.L.; Verbruggen, F. Association and inhibition. In The Wiley Blackwell Handbook on the Cognitive Neuroscience of Learning; Murphy, R.A., Honey, R.C., Eds.; John Wiley and Sons: Chichester, UK, 2016. [Google Scholar]
- Veling, H.; Holland, R.W.; Van Knippenberg, A. When approach motivation and behavioral inhibition collide: Behavior regulation through stimulus devaluation. J. Exp. Soc. Psychol. 2008, 44, 1013–1019. [Google Scholar] [CrossRef]
- Verbruggen, F.; Best, M.; Bowditch, W.A.; Stevens, T.; McLaren, I.P. The inhibitory control reflex. Neuropsychology 2014, 65, 263–278. [Google Scholar] [CrossRef] [PubMed]
- Alonso-Alonso, M. Translating tDCS into the field of obesity: Mechanism-driven approaches. Front. Hum. Neurosci. 2013, 7, 512. [Google Scholar]
- Feil, J.; Zangen, A. Brain stimulation in the study and treatment of addiction. Neurosci. Biobehav. Rev. 2010, 34, 559–574. [Google Scholar] [CrossRef] [PubMed]
- Hall, P.A.; Vincent, C.M.; Burhan, A.M. Non-invasive brain stimulation for food cravings, consumption, and disorders of eating: A review of methods, findings and controversies. Appetite 2018, 124, 78–88. [Google Scholar] [CrossRef]
- Lowe, C.J.; Vincent, C.; Hall, P.A. Effects of noninvasive brain stimulation on food cravings and consumption: A meta-analytic review. Psychosom. Med. 2017, 79, 2–13. [Google Scholar] [CrossRef]
- Nardone, R.; Bergmann, J.; Christova, M.; Lochner, P.; Tezzon, F.; Golaszewski, S.; Trinka, E.; Brigo, F. Non-invasive brain stimulation in the functional evaluation of alcohol effects and in the treatment of alcohol craving: A review. Neurosci. Res. 2012, 74, 169–176. [Google Scholar] [CrossRef] [PubMed]
- Song, S.; Zilverstand, A.; Gui, W.; Li, H.J.; Zhou, X. Effects of single-session versus multi-session non-invasive brain stimulation on craving and consumption in individuals with drug addiction, eating disorders or obesity: A meta-analysis. Brain Stimul. 2018, 12, 606–618. [Google Scholar] [CrossRef] [PubMed]
- Maizey, L.; Allen, C.P.; Dervinis, M.; Verbruggen, F.; Varnava, A.; Kozlov, M.; Adams, R.C.; Stokes, M.; Klemen, J.; Bungert, A.; et al. Comparative incidence rates of mild adverse effects to transcranial magnetic stimulation. Clin. Neurophysiol. 2013, 124, 536–544. [Google Scholar] [CrossRef] [PubMed]
- Matsumoto, H.; Ugawa, Y. Adverse effects of tDCS and tACS: A review. Clin. Neurophysiol. Pract. 2017, 2, 19–25. [Google Scholar] [CrossRef] [PubMed]
- Pascual-Leone, A.; Houser, C.; Reese, K.; Shotland, L.; Grafman, J.; Sato, S.; Valls-Sole, J.; Brasil-Neto, J.; Wassermann, E.; Cohen, L.; et al. Safety of rapid-rate transcranial magnetic stimulation in normal volunteers. Electroencephalogr. Clin. Neurophysiol. Potentials Sect. 1993, 89, 120–130. [Google Scholar] [CrossRef]
- Poreisz, C.; Boros, K.; Antal, A.; Paulus, W. Safety aspects of transcranial direct current stimulation concerning healthy subjects and patients. Brain Res. Bull. 2007, 72, 208–214. [Google Scholar] [CrossRef] [PubMed]
- Rossi, S.; Hallett, M.; Rossini, P.M.; Pascual-Leone, A. Safety, ethical considerations, and application guidelines for the use of transcranial magnetic stimulation in clinical practice and research. Clin. Neurophysiol. 2009, 120, 2008–2039. [Google Scholar] [CrossRef] [PubMed]
- Taylor, R.; Gálvez, V.; Loo, C. Transcranial magnetic stimulation (TMS) safety: A practical guide for psychiatrists. Australas. Psychiatr. 2018, 26, 189–192. [Google Scholar] [CrossRef]
- Fitzgerald, P.; Fountain, S.; Daskalakis, Z. A comprehensive review of the effects of rTMS on motor cortical excitability and inhibition. Clin. Neurophysiol. 2006, 117, 2584–2596. [Google Scholar] [CrossRef]
- Amiaz, R.; Levy, D.; Vainiger, D.; Grunhaus, L.; Zangen, A. Repeated high-frequency transcranial magnetic stimulation over the dorsolateral prefrontal cortex reduces cigarette craving and consumption. Addiction 2009, 104, 653–660. [Google Scholar] [CrossRef]
- Bolloni, C.; Panella, R.; Pedetti, M.; Frascella, A.G.; Gambelunghe, C.; Piccoli, T.; Maniaci, G.; Brancato, A.; Cannizzaro, C.; Diana, M. Bilateral transcranial magnetic stimulation of the prefrontal cortex reduces cocaine intake: A pilot study. Front. Psychol. 2016, 7, 101. [Google Scholar] [CrossRef]
- Mishra, B.R.; Praharaj, S.K.; Katshu, M.Z.U.H.; Sarkar, S.; Nizamie, S.H. Comparison of anticraving efficacy of right and left repetitive transcranial magnetic stimulation in alcohol dependence: A randomized double-blind study. J. Neuropsychiatry Clin. Neurosci. 2015, 27, 54. [Google Scholar] [CrossRef] [PubMed]
- Su, H.; Zhong, N.; Gan, H.; Wang, J.; Han, H.; Chen, T.; Li, X.; Ruan, X.; Zhu, Y.; Jiang, H.; et al. High frequency repetitive transcranial magnetic stimulation of the left dorsolateral prefrontal cortex for methamphetamine use disorders: A randomised clinical trial. Drug Alcohol Depend. 2017, 175, 84–91. [Google Scholar] [CrossRef] [PubMed]
- Terraneo, A.; Leggio, L.; Saladini, M.; Ermani, M.; Bonci, A.; Gallimberti, L.; Information, P.E.K.F.C. Transcranial magnetic stimulation of dorsolateral prefrontal cortex reduces cocaine use: A pilot study. Eur. Neuropsychopharmacol. 2016, 26, 37–44. [Google Scholar] [CrossRef] [PubMed]
- Beeli, G.; Casutt, G.; Baumgartner, T.; Jäncke, L. Modulating presence and impulsiveness by external stimulation of the brain. Behav. Brain Funct. 2008, 4, 33. [Google Scholar] [CrossRef] [PubMed]
- Garavan, H.; Hester, R.; Murphy, K.; Fassbender, C.; Kelly, C. Individual differences in the functional neuroanatomy of inhibitory control. Brain Res. 2006, 1105, 130–142. [Google Scholar] [CrossRef] [PubMed]
- Oldrati, V.; Patricelli, J.; Colombo, B.; Antonietti, A. The role of dorsolateral prefrontal cortex in inhibition mechanism: A study on cognitive reflection test and similar tasks through neuromodulation. Neuropsychology 2016, 91, 499–508. [Google Scholar] [CrossRef] [PubMed]
- Zheng, D.; Oka, T.; Bokura, H.; Yamaguchi, S. The key locus of common response inhibition network for no-go and stop signals. J. Cogn. Neurosci. 2008, 20, 1434–1442. [Google Scholar] [CrossRef] [PubMed]
- Diana, M. The dopamine hypothesis of drug addiction and its potential therapeutic value. Front. Psychol. 2011, 2, 64. [Google Scholar] [CrossRef] [PubMed]
- Strafella, A.P.; Paus, T.; Barrett, J.; Dagher, A. Repetitive Transcranial Magnetic Stimulation of the Human Prefrontal Cortex Induces Dopamine Release in the Caudate Nucleus. J. Neurosci. 2001, 21, RC157. [Google Scholar] [CrossRef] [PubMed]
- Batista, E.K.; Klauss, J.; Fregni, F.; Nitsche, M.A.; Nakamura-Palacios, E.M. A Randomized Placebo-Controlled Trial of Targeted Prefrontal Cortex Modulation with Bilateral tDCS in Patients with Crack-Cocaine Dependence. Int. J. Neuropsychopharmacol. 2015, 18, 066. [Google Scholar] [CrossRef] [PubMed]
- Boggio, P.S.; Liguori, P.; Sultani, N.; Rezende, L.; Fecteau, S.; Fregni, F. Cumulative priming effects of cortical stimulation on smoking cue-induced craving. Neurosci. Lett. 2009, 463, 82–86. [Google Scholar] [CrossRef] [PubMed]
- Boggio, P.S.; Sultani, N.; Fecteau, S.; Merabet, L.; Mecca, T.; Pascual-Leone, A.; Basaglia, A.; Fregni, F. Prefrontal cortex modulation using transcranial DC stimulation reduces alcohol craving: A double-blind, sham-controlled study. Drug Alcohol Depend. 2008, 92, 55–60. [Google Scholar] [CrossRef] [PubMed]
- Boggio, P.S.; Zaghi, S.; Villani, A.B.; Fecteau, S.; Pascual-Leone, A.; Fregni, F. Modulation of risk-taking in marijuana users by transcranial direct current stimulation (tDCS) of the dorsolateral prefrontal cortex (DLPFC). Drug Alcohol Depend. 2010, 112, 220–225. [Google Scholar] [CrossRef] [PubMed]
- Fecteau, S.; Agosta, S.; Hone-Blanchet, A.; Fregni, F.; Boggio, P.; Ciraulo, D.; Pascual-Leone, A. Modulation of smoking and decision-making behaviors with transcranial direct current stimulation in tobacco smokers: A preliminary study. Drug Alcohol Depend. 2014, 140, 78–84. [Google Scholar] [CrossRef] [PubMed]
- Klauss, J.; Anders, Q.S.; Felippe, L.V.; Nitsche, M.A.; Nakamura-Palacios, E.M. Multiple sessions of transcranial direct current stimulation (tDCS) reduced craving and relapses for alcohol use: A randomized placebo-controlled trial in alcohol use disorder. Front. Pharmacol. 2018, 9, 716. [Google Scholar] [CrossRef] [PubMed]
- Antal, A.; Terney, D.; Poreisz, C.; Paulus, W. Towards unravelling task-related modulations of neuroplastic changes induced in the human motor cortex. Eur. J. Neurosci. 2007, 26, 2687–2691. [Google Scholar] [CrossRef] [PubMed]
- Liebetanz, D.; Nitsche, M.A.; Tergau, F.; Paulus, W. Pharmacological approach to the mechanisms of transcranial DC-stimulation-induced after-effects of human motor cortex excitability. Brain 2002, 125, 2238–2247. [Google Scholar] [CrossRef] [PubMed]
- Nitsche, M.A.; Paulus, W. Excitability changes induced in the human motor cortex by weak transcranial direct current stimulation. J. Physiol. 2000, 527, 633–639. [Google Scholar] [CrossRef]
- Nitsche, M.; Schauenburg, A.; Lang, N.; Liebetanz, D.; Exner, C.; Paulus, W.; Tergau, F. Facilitation of implicit motor learning by weak transcranial direct current stimulation of the primary motor cortex in the human. J. Cogn. Neurosci. 2003, 15, 619–626. [Google Scholar] [CrossRef]
- Nitsche, M.A.; Seeber, A.; Frommann, K.; Klein, C.C.; Rochford, C.; Nitsche, M.S.; Fricke, K.; Liebetanz, D.; Lang, N.; Antal, A.; et al. Modulating parameters of excitability during and after transcranial direct current stimulation of the human motor cortex. J. Physiol. 2005, 568, 291–303. [Google Scholar] [CrossRef] [PubMed]
- Priori, A. Brain polarization in humans: A reappraisal of an old tool for prolonged non-invasive modulation of brain excitability. Clin. Neurophysiol. 2003, 114, 589–595. [Google Scholar] [CrossRef]
- Nitsche, M.A.; Paulus, W. Sustained excitability elevations induced by transcranial DC motor cortex stimulation in humans. Neurology 2001, 57, 1899–1901. [Google Scholar] [CrossRef]
- Gandiga, P.C.; Hummel, F.C.; Cohen, L.G. Transcranial DC stimulation (tDCS): A tool for double-blind sham-controlled clinical studies in brain stimulation. Clin. Neurophysiol. 2006, 117, 845–850. [Google Scholar] [CrossRef] [PubMed]
- Nitsche, M.A.; Cohen, L.G.; Wassermann, E.M.; Priori, A.; Lang, N.; Antal, A.; Paulus, W.; Hummel, F.; Boggio, P.S.; Fregni, F.; et al. Transcranial direct current stimulation: State of the art 2008. Brain Stimul. 2008, 1, 206–223. [Google Scholar] [CrossRef] [PubMed]
- Stagg, C.J.; Nitsche, M.A. Physiological basis of transcranial direct current stimulation. Neuroscience 2011, 17, 37–53. [Google Scholar] [CrossRef]
- Wiers, R.W.; Gladwin, T.E.; Hofmann, W.; Salemink, E.; Ridderinkhof, K.R. Cognitive bias modification and cognitive control training in addiction and related psychopathology: Mechanisms, clinical perspectives, and ways forward. Clin. Psychol. Sci. 2013, 1, 192–212. [Google Scholar] [CrossRef]
- Goldman, R.L.; Borckardt, J.J.; Frohman, H.A.; O’Neil, P.M.; Madan, A.; Campbell, L.K.; Budak, A.; George, M.S. Prefrontal cortex transcranial direct current stimulation (tDCS) temporarily reduces food cravings and increases the self-reported ability to resist food in adults with frequent food craving. Appetite 2011, 56, 741–746. [Google Scholar] [CrossRef]
- Kim, S.H.; Chung, J.H.; Kim, T.H.; Lim, S.H.; Kim, Y.; Lee, Y.A.; Song, S.W. The effects of repetitive transcranial magnetic stimulation on eating behaviors and body weight in obesity: A randomized controlled study. Brain Stimul. 2018, 11, 528–535. [Google Scholar] [CrossRef]
- Lapenta, O.M.; Di Sierve, K.; De Macedo, E.C.; Fregni, F.; Boggio, P.S. Transcranial direct current stimulation modulates ERP-indexed inhibitory control and reduces food consumption. Appetite 2014, 83, 42–48. [Google Scholar] [CrossRef]
- Ljubisavljevic, M.; Maxood, K.; Bjekic, J.; Oommen, J.; Nagelkerke, N. Long-Term effects of repeated prefrontal cortex transcranial direct current stimulation (tDCS) on food craving in normal and overweight young adults. Brain Stimul. 2016, 9, 826–833. [Google Scholar] [CrossRef] [PubMed]
- Montenegro, R.A.; Okano, A.H.; Cunha, F.A.; Gurgel, J.L.; Fontes, E.B.; Farinatti, P.T. Prefrontal cortex transcranial direct current stimulation associated with aerobic exercise change aspects of appetite sensation in overweight adults. Appetite 2012, 58, 333–338. [Google Scholar] [CrossRef] [PubMed]
- Ray, M.K.; Sylvester, M.D.; Osborn, L.; Helms, J.; Turan, B.; Burgess, E.E.; Boggiano, M.M. The critical role of cognitive-based trait differences in transcranial direct current stimulation (tDCS) suppression of food craving and eating in frank obesity. Appetite 2017, 116, 568–574. [Google Scholar] [CrossRef]
- Uher, R.; Yoganathan, D.; Mogg, A.; Eranti, S.V.; Treasure, J.; Campbell, I.C.; McLoughlin, D.M.; Schmidt, U. Effect of left prefrontal repetitive transcranial magnetic stimulation on food craving. Biol. Psychiatr. 2005, 58, 840–842. [Google Scholar] [CrossRef]
- Van den Eynde, F.; Claudino, A.M.; Mogg, A.; Horrell, L.; Stahl, D.; Ribeiro, W.; Uher, R.; Campbell, I.; Schmidt, U. Repetitive transcranial magnetic stimulation reduces cue-induced food craving in bulimic disorders. Biol. Psychiatr. 2010, 67, 793–795. [Google Scholar] [CrossRef]
- Barth, K.S.; Rydin-Gray, S.; Kose, S.; Borckardt, J.J.; O’Neil, P.M.; Shaw, D.; Madan, A.; Budak, A.; George, M.S. Food Cravings and the Effects of Left Prefrontal Repetitive Transcranial Magnetic Stimulation Using an Improved Sham Condition. Front. Psychol. 2011, 2, 9. [Google Scholar] [CrossRef]
- Fregni, F.; Orsati, F.; Pedrosa, W.; Fecteau, S.; Tome, F.A.; Nitsche, M.A.; Mecca, T.; Macedo, E.C.; Pascual-Leone, A.; Boggio, P.S. Transcranial direct current stimulation of the prefrontal cortex modulates the desire for specific foods. Appetite 2008, 51, 34–41. [Google Scholar] [CrossRef] [PubMed]
- Jansen, J.M.; Daams, J.G.; Koeter, M.W.; Veltman, D.J.; Brink, W.V.D.; Goudriaan, A.E. Effects of non-invasive neurostimulation on craving: A meta-analysis. Neurosci. Biobehav. Rev. 2013, 37, 2472–2480. [Google Scholar] [CrossRef] [PubMed]
- Ray, M.K.; Sylvester, M.D.; Helton, A.; Pittman, B.R.; Wagstaff, L.E.; McRae, T.R.; Turan, B.; Fontaine, K.R.; Amthor, F.R.; Boggiano, M.M.; et al. The effect of expectation on transcranial direct current stimulation (tDCS) to suppress food craving and eating in individuals with overweight and obesity. Appetite 2019, 136, 1–7. [Google Scholar] [CrossRef] [PubMed]
- Sedgmond, J.; Lawrence, N.S.; Verbruggen, F.; Morrison, S.; Chambers, C.D.; Adams, R.C. Prefrontal brain stimulation during food-related inhibition training: Effects on food craving, food consumption and inhibitory control. R. Soc. Open Sci. 2019, 6, 181186. [Google Scholar] [CrossRef]
- Hanlon, C.A.; Hartwell, K.J.; Canterberry, M.; Li, X.; Owens, M.; LeMatty, T.; Prisciandaro, J.J.; Borckardt, J.; Brady, K.T.; George, M.S. Reduction of cue-induced craving through realtime neurofeedback in nicotine users: The role of region of interest selection and multiple visits. Psychiatr. Res. 2013, 213, 79–81. [Google Scholar] [CrossRef] [PubMed]
- Hartwell, K.J.; Prisciandaro, J.J.; Borckardt, J.; Li, X.; George, M.S.; Brady, K.T. Real-time fMRI in the treatment of nicotine dependence: A conceptual review and pilot studies. Psychol. Addict. Behav. 2013, 27, 501–509. [Google Scholar] [CrossRef] [PubMed]
- Li, X.; Hartwell, K.J.; Borckardt, J.; Prisciandaro, J.J.; Saladin, M.E.; Morgan, P.S.; Johnson, K.A.; LeMatty, T.; Brady, K.T.; George, M.S. Volitional reduction of anterior cingulate cortex activity produces decreased cue craving in smoking cessation: A preliminary real-time fMRI study. Addict. Biol. 2012, 18, 739–748. [Google Scholar] [CrossRef] [PubMed]
- Dehghani-Arani, F.; Rostami, R.; Nadali, H. Neurofeedback training for opiate addiction: Improvement of mental health and craving. Appl. Psychophysiol. Biofeedback 2013, 38, 133–141. [Google Scholar] [CrossRef] [PubMed]
- Dehghani-Arani, F.; Rostami, R.; Nostratabadi, M. Effectiveness of neurofeedback training as a treatment for opioid-dependent patients. Clin. EEG Neurosci. 2010, 41, 170–177. [Google Scholar] [CrossRef] [PubMed]
- Horrell, T.; El-Baz, A.; Baruth, J.; Tasman, A.; Sokhadze, G.; Stewart, C.; Sokhadze, E. Neurofeedback Effects on Evoked and Induced EEG Gamma Band Reactivity to Drug-related Cues in Cocaine Addiction. J. Neurother. 2010, 14, 195–216. [Google Scholar] [CrossRef] [PubMed]
- Scott, W.C.; Kaiser, D.; Othmer, S.; Sideroff, S.I. Effects of an EEG biofeedback protocol on a mixed substance abusing population. Am. J. Drug Alcohol Abus. 2005, 31, 455–469. [Google Scholar] [CrossRef]
- Dewiputri, W.I.; Auer, T. Functional Magnetic Resonance Imaging (fMRI) neurofeedback: Implementations and applications. Malays. J. Med Sci. 2013, 20, 5–15. [Google Scholar]
- Frank, S.; Lee, S.; Preissl, H.; Schultes, B.; Birbaumer, N.; Veit, R. The obese brain athlete: Self-regulation of the anterior insula in adiposity. PLoS ONE 2012, 7, e42570. [Google Scholar] [CrossRef]
- Frank, S.; Kullmann, S.; Veit, R. Food related processes in the insular cortex. Front. Hum. Neurosci. 2013, 7, 499. [Google Scholar] [CrossRef]
- Ihssen, N.; Sokunbi, M.O.; Lawrence, A.D.; Lawrence, N.S.; Linden, D.E. Neurofeedback of visual food cue reactivity: A potential avenue to alter incentive sensitization and craving. Brain Imaging Behav. 2017, 11, 915–924. [Google Scholar] [CrossRef]
- Kohl, S.H.; Veit, R.; Spetter, M.S.; Günther, A.; Rina, A.; Lührs, M.; Birbaumer, N.; Preissl, H.; Hallschmid, M. Real-time fMRI neurofeedback training to improve eating behavior by self-regulation of the dorsolateral prefrontal cortex: A randomized controlled trial in overweight and obese subjects. NeuroImage 2019, 191, 596–609. [Google Scholar] [CrossRef] [PubMed]
- Spetter, M.S.; Malekshahi, R.; Birbaumer, N.; Lührs, M.; Van Der Veer, A.H.; Scheffler, K.; Spuckti, S.; Preissl, H.; Veit, R.; Hallschmid, M. Volitional regulation of brain responses to food stimuli in overweight and obese subjects: A real-time fMRI feedback study. Appetite 2017, 112, 188–195. [Google Scholar] [CrossRef] [PubMed]
- Weiner, S. The addiction of overeating: Self-help groups as treatment models. J. Clin. Psychol. 1998, 54, 163–167. [Google Scholar] [CrossRef]
- Magill, M.; Ray, L.A. Cognitive-behavioural treatment with alcohol and illicit drug users: A meta-analysis of randomized controlled trials. J. Stud. Alcohol Drugs 2009, 70, 516–527. [Google Scholar] [CrossRef] [PubMed]
- Göhner, W.; Schlatterer, M.; Seelig, H.; Frey, I.; Berg, A.; Fuchs, R. Two-Year follow-up of an interdisciplinary cognitive-behavioral intervention program for obese adults. J. Psychol. 2012, 146, 371–391. [Google Scholar] [CrossRef] [PubMed]
- Marchesini, G.; Natale, S.; Chierici, S.; Manini, R.; Besteghi, L.; Di Domizio, S.; Sartini, A.; Pasqui, F.; Baraldi, L.; Forlani, G.; et al. Effects of cognitive–behavioural therapy on health-related quality of life in obese subjects with and without binge eating disorder. Int. J. Obes. 2002, 26, 1261–1267. [Google Scholar] [CrossRef] [PubMed]
- Linardon, J.; Wade, T.D.; Garcia, X.D.L.P.; Brennan, L. The efficacy of cognitive-behavioral therapy for eating disorders: A systematic review and meta-analysis. J. Consult. Clin. Psychol. 2017, 85, 1080–1094. [Google Scholar] [CrossRef] [PubMed]
- Vanderlinden, J.; Adriaensen, A.; Vancampfort, D.; Pieters, G.; Probst, M.; Vansteelandt, K. A Cognitive-behavioral therapeutic program for patients with obesity and binge eating disorder: Short- and long- term follow-up data of a prospective study. Behav. Modif. 2012, 36, 670–686. [Google Scholar] [CrossRef] [PubMed]
- Wilfley, D.E.; Welch, R.R.; Stein, R.I.; Spurrell, E.B.; Cohen, L.R.; Saelens, B.E.; Dounchis, J.Z.; Frank, M.A.; Wiseman, C.V.; Matt, G.E. A randomized comparison of group cognitive-behavioral therapy and group interpersonal psychotherapy fort the treatment of overweight individuals with binge-eating disorder. Arch. Gen. Psychiatr. 2002, 59, 713721. [Google Scholar] [CrossRef] [PubMed]
- Wilson, G.T.; Fairburn, C.C.; Agras, W.S.; Walsh, B.T.; Kraemer, H. Cognitive-behavioral therapy for bulimia nervosa: Time course and mechanisms of change. J. Consult. Clin. Psychol. 2002, 70, 267–274. [Google Scholar] [CrossRef] [PubMed]
- Gearhardt, A.N.; Corbin, W.R.; Brownell, K.D. Food addiction: An examination of the diagnostic criteria for dependence. J. Addict. Med. 2009, 3, 1–8. [Google Scholar] [CrossRef] [PubMed]
- Earnshaw, V.; Smith, L.; Copenhaver, M. Drug addiction stigma in the context of methadone maintenance therapy: An investigation into understudied sources of stigma. Int. J. Ment. Healthy Addict. 2013, 11, 110–122. [Google Scholar] [CrossRef] [PubMed]
- DePierre, J.A.; Puhl, R.M.; Luedicke, J. A new stigmatized identity? Comparisons of a “food addict” label with other stigmatized health conditions. Basic Appl. Soc. Psychol. 2013, 35, 10–21. [Google Scholar] [CrossRef]
- Rasmussen, N. Stigma and the addiction paradigm for obesity: Lessons from 1950s America. Addiction 2015, 110, 217–225. [Google Scholar] [CrossRef] [PubMed]
- Hardman, C.A.; Rogers, P.J.; Dallas, R.; Scott, J.; Ruddock, H.K.; Robinson, E. “Food addiction is real”. The effects of exposure to this message on self-diagnosed food addiction and eating behaviour. Appetite 2015, 91, 179–184. [Google Scholar] [CrossRef] [PubMed]
- Latner, J.D.; Puhl, R.M.; Murakami, J.M.; O’Brien, K.S. Food addiction as a causal model of obesity. Effects on stigma, blame, and perceived psychopathology. Appetite 2014, 77, 79–84. [Google Scholar] [CrossRef]
- Reid, J.; O’Brien, K.S.; Puhl, R.; Hardman, C.A.; Carter, A. Food addiction and its potential links with weight stigma. Curr. Addict. Rep. 2018, 5, 192–201. [Google Scholar] [CrossRef]
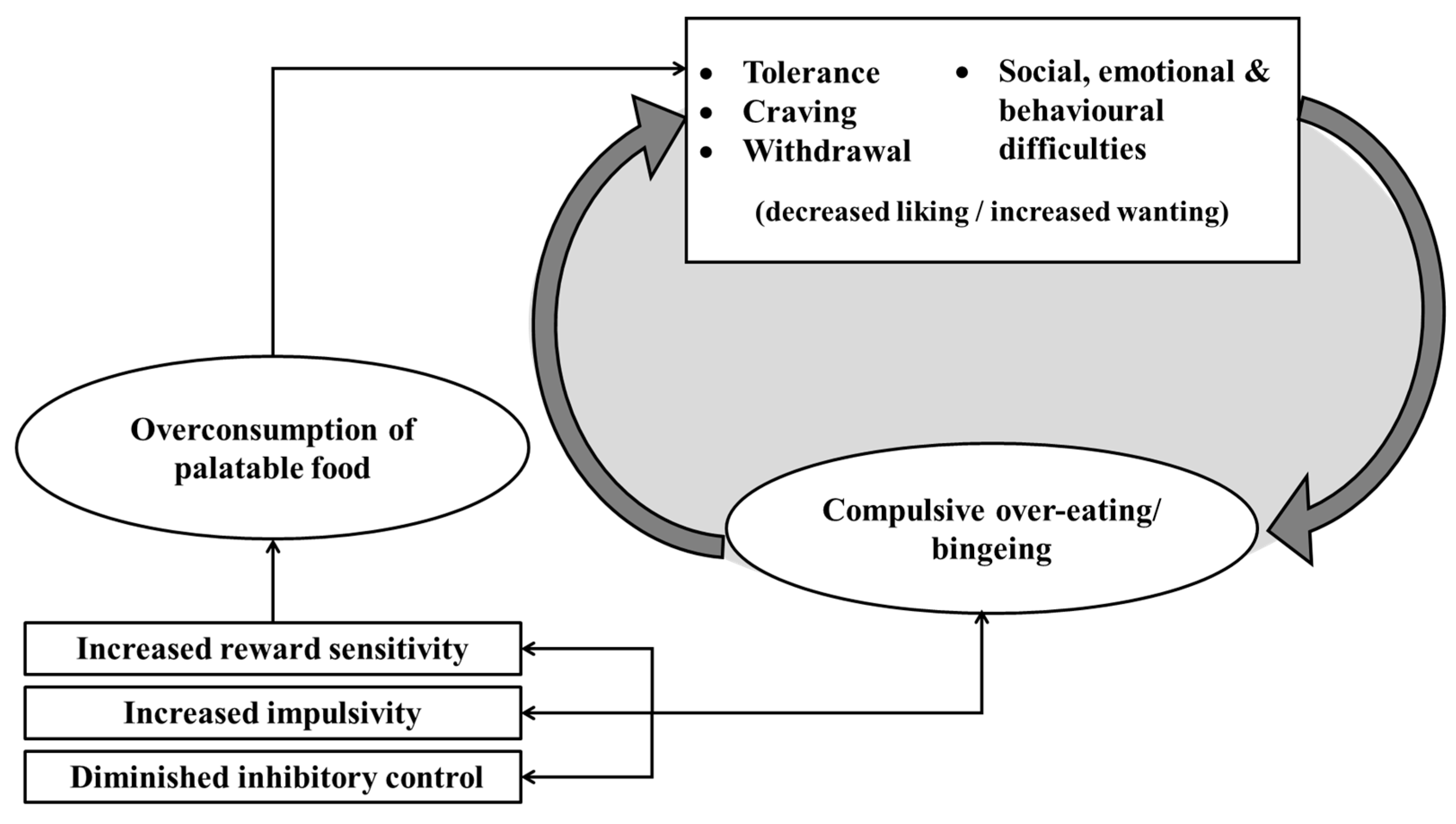
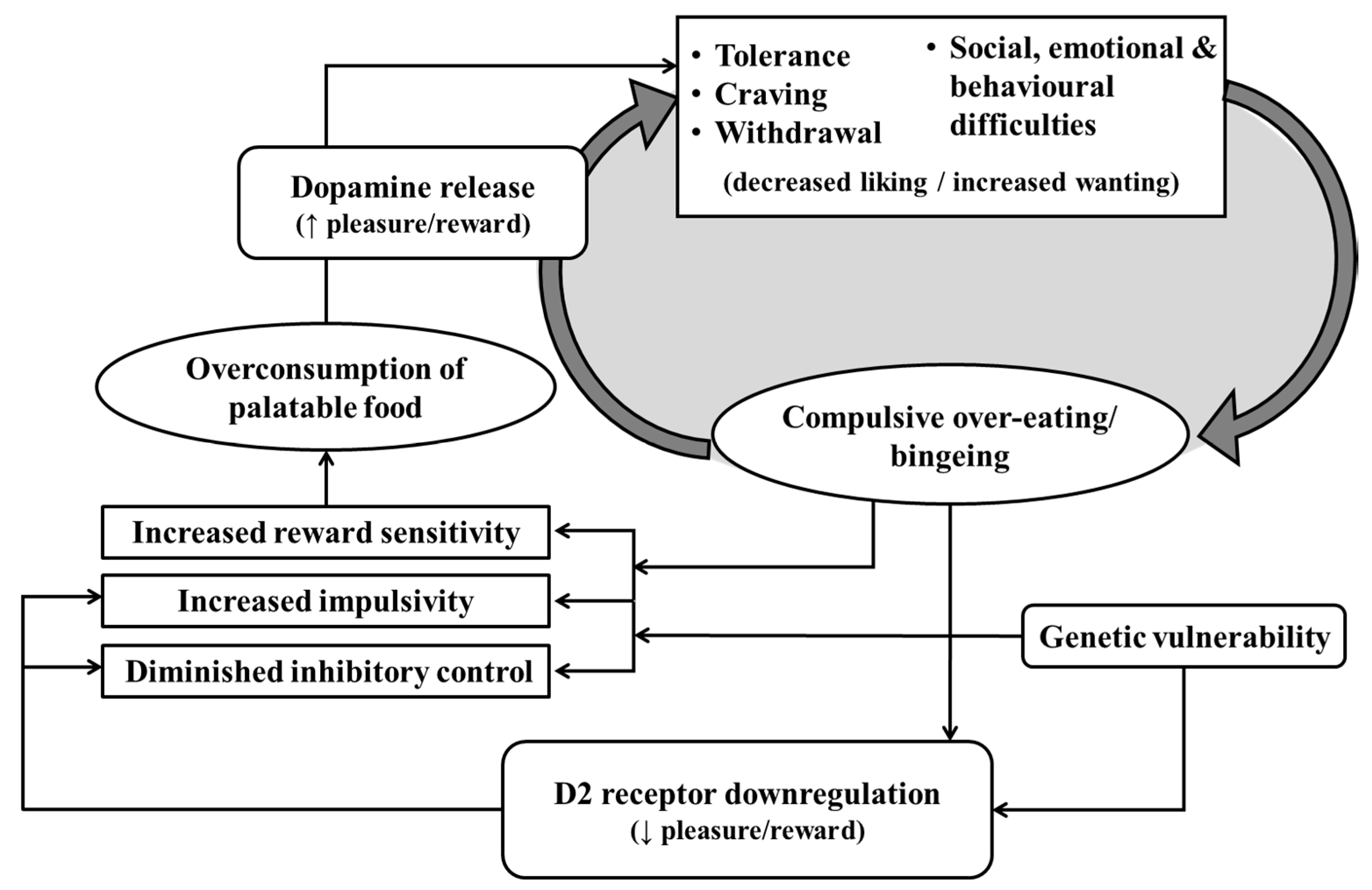
© 2019 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Adams, R.C.; Sedgmond, J.; Maizey, L.; Chambers, C.D.; Lawrence, N.S. Food Addiction: Implications for the Diagnosis and Treatment of Overeating. Nutrients 2019, 11, 2086. https://doi.org/10.3390/nu11092086
Adams RC, Sedgmond J, Maizey L, Chambers CD, Lawrence NS. Food Addiction: Implications for the Diagnosis and Treatment of Overeating. Nutrients. 2019; 11(9):2086. https://doi.org/10.3390/nu11092086
Chicago/Turabian StyleAdams, Rachel C., Jemma Sedgmond, Leah Maizey, Christopher D. Chambers, and Natalia S. Lawrence. 2019. "Food Addiction: Implications for the Diagnosis and Treatment of Overeating" Nutrients 11, no. 9: 2086. https://doi.org/10.3390/nu11092086
APA StyleAdams, R. C., Sedgmond, J., Maizey, L., Chambers, C. D., & Lawrence, N. S. (2019). Food Addiction: Implications for the Diagnosis and Treatment of Overeating. Nutrients, 11(9), 2086. https://doi.org/10.3390/nu11092086




