School-Based Interventions in Low Socioeconomic Settings to Reduce Obesity Outcomes among Preschoolers: A Scoping Review
Abstract
1. Introduction
2. Materials and Methods
2.1. Search Strategy
2.2. Inclusion and Exclusion Criteria
2.3. Data Extraction and Synthesis
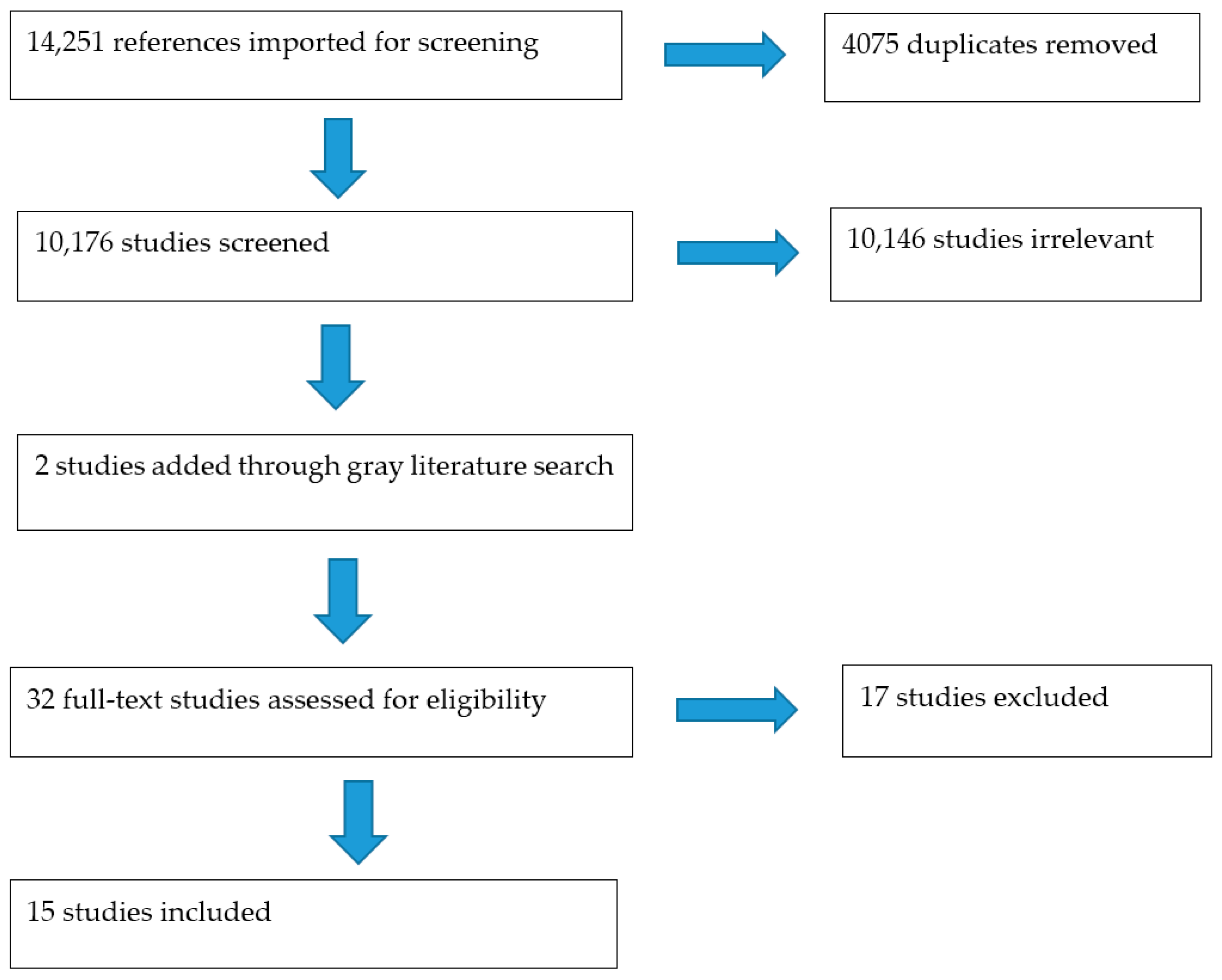
3. Results
3.1. Successful Interventions
3.2. Inconvlusive Interventions
3.3. Theoretical Frameworks
4. Discussion
5. Conclusions
Supplementary Materials
Author Contributions
Conflicts of Interest
References
- World Health Organization. Available online: https://www.who.int/news-room/fact-sheets/detail/obesity-and-overweight (accessed on 12 June 2019).
- Defining Childhood Obesity. Overweight & Obesity. CDC. Available online: https://www.cdc.gov/obesity/childhood/defining.html (accessed on 14 June 2019).
- Cole, T.J.; Flegal, K.M.; Nicholls, D.; Jackson, A.A. Body Mass Index Cut Offs to Define Thinness in Children and Adolescents: International Survey. BMJ 2007, 335, 194. [Google Scholar] [CrossRef] [PubMed]
- Ogden, C.L.; Carroll, M.D.; Lawman, H.G.; Fryar, C.D.; Kruszon-Moran, D.; Kit, B.K.; Flegal, K.M. Trends in Obesity Prevalence Among Children and Adolescents in the United States, 1988–1994 Through 2013–2014. JAMA 2016, 315, 2292–2299. [Google Scholar] [CrossRef] [PubMed]
- Skinner, A.C.; Ravanbakht, S.N.; Skelton, J.A.; Perrin, E.M.; Armstrong, S.C. Prevalence of Obesity and Severe Obesity in US Children, 1999–2016. Pediatrics 2018, 141, e20173459. [Google Scholar] [CrossRef] [PubMed]
- The State of Obesity. Available online: https://www.stateofobesity.org/childhood-obesity-trends/ (accessed on 21 September 2018).
- Lobstein, T.; Baur, L.; Uauy, R. Obesity in Children and Young People: A Crisis in Public Health. Obes. Rev. 2004, 5 (Suppl. 1), 4–85. [Google Scholar] [CrossRef] [PubMed]
- Centers for Disease Control and Prevention. Available online: https://www.cdc.gov/nchs/data/factsheets/factsheet_nhanes.htm (accessed on 21 September 2018).
- Howe, L.D.; Tilling, K.; Galobardes, B.; Smith, G.D.; Ness, A.R.; Lawlor, D.A. Socioeconomic Disparities in Trajectories of Adiposity across Childhood. Int. J. Pediatr. Obes. 2011, 6 (Suppl. 3), e144–e153. [Google Scholar] [CrossRef] [PubMed]
- Nekitsing, C.; Hetherington, M.M.; Blundell-Birtill, P. Developing Healthy Food Preferences in Preschool Children Through Taste Exposure, Sensory Learning, and Nutrition Education. Curr. Obes. Rep. 2018, 7, 60–67. [Google Scholar] [CrossRef] [PubMed]
- Boocock, S.S. Early Childhood Programs in Other Nations: Goals and Outcomes. Future Child. 1995, 5, 94–114. [Google Scholar] [CrossRef] [PubMed]
- Davis, S.M.; Myers, O.B.; Cruz, T.H.; Morshed, A.B.; Canaca, G.F.; Keane, P.C.; O’Donald, E.R. CHILE: Outcomes of a Group Randomized Controlled Trial of an Intervention to Prevent Obesity in Preschool Hispanic and American Indian Children. Prev. Med. 2016, 89, 162–168. [Google Scholar] [CrossRef] [PubMed]
- Coen, V.D.; Bourdeaudhuij, I.D.; Vereecken, C.; Verbestel, V.; Haerens, L.; Huybrechts, I.; Lippevelde, W.V.; Maes, L. Effects of a 2-Year Healthy Eating and Physical Activity Intervention for 3–6-Year-Olds in Communities of High and Low Socio-Economic Status: The POP (Prevention of Overweight among Pre-School and School Children) Project. Public Health Nutr. 2012, 15, 1737–1745. [Google Scholar] [CrossRef]
- Summerbell, C.D.; Waters, E.; Edmunds, L.; Kelly, S.A.; Brown, T.; Campbell, K.J. Interventions for Preventing Obesity in Children. Cochrane Database Syst. Rev. 2005, CD001871. [Google Scholar] [CrossRef]
- Laws, R.; Campbell, K.J.; van der Pligt, P.; Russell, G.; Ball, K.; Lynch, J.; Crawford, D.; Taylor, R.; Askew, D.; Denney-Wilson, E. The Impact of Interventions to Prevent Obesity or Improve Obesity Related Behaviours in Children (0–5 Years) from Socioeconomically Disadvantaged and/or Indigenous Families: A Systematic Review. BMC Public Health 2014, 14, 779. [Google Scholar] [CrossRef] [PubMed]
- Verjans-Janssen, S.R.B.; van de Kolk, I.; Van Kann, D.H.H.; Kremers, S.P.J.; Gerards, S.M.P.L. Effectiveness of School-Based Physical Activity and Nutrition Interventions with Direct Parental Involvement on Children’s BMI and Energy Balance-Related Behaviors—A Systematic Review. PLoS ONE 2018, 13, e0204560. [Google Scholar] [CrossRef] [PubMed]
- Bürgi, F.; Niederer, I.; Schindler, C.; Bodenmann, P.; Marques-Vidal, P.; Kriemler, S.; Puder, J.J. Effect of a Lifestyle Intervention on Adiposity and Fitness in Socially Disadvantaged Subgroups of Preschoolers: A Cluster-Randomized Trial (Ballabeina). Prev. Med. 2012, 54, 335–340. [Google Scholar] [CrossRef] [PubMed]
- Fitzgibbon, M.L.; Stolley, M.R.; Schiffer, L.; Kong, A.; Braunschweig, C.L.; Gomez-Perez, S.L.; Odoms-Young, A.; Van Horn, L.; Christoffel, K.K.; Dyer, A.R. Family-Based Hip-Hop to Health: Outcome Results. Obesity (Silver Spring) 2013, 21, 274–283. [Google Scholar] [CrossRef]
- Fitzgibbon, M.L.; Stolley, M.R.; Schiffer, L.; Van Horn, L.; KauferChristoffel, K.; Dyer, A. Two-Year Follow-up Results for Hip-Hop to Health Jr.: A Randomized Controlled Trial for Overweight Prevention in Preschool Minority Children. J. Pediatr. 2005, 146, 618–625. [Google Scholar] [CrossRef]
- Jouret, B.; Ahluwalia, N.; Dupuy, M.; Cristini, C.; Nègre-Pages, L.; Grandjean, H.; Tauber, M. Prevention of Overweight in Preschool Children: Results of Kindergarten-Based Interventions. Int. J. Obes. 2009, 33, 1075–1083. [Google Scholar] [CrossRef]
- Kaufman-Shriqui, V.; Fraser, D.; Friger, M.; Geva, D.; Bilenko, N.; Vardi, H.; Elhadad, N.; Mor, K.; Feine, Z.; Shahar, D.R. Effect of a School-Based Intervention on Nutritional Knowledge and Habits of Low-Socioeconomic School Children in Israel: A Cluster-Randomized Controlled Trial. Nutrients 2016, 8, 234. [Google Scholar] [CrossRef]
- Puder, J.J.; Marques-Vidal, P.; Schindler, C.; Zahner, L.; Niederer, I.; Bürgi, F.; Ebenegger, V.; Nydegger, A.; Kriemler, S. Effect of Multidimensional Lifestyle Intervention on Fitness and Adiposity in Predominantly Migrant Preschool Children (Ballabeina): Cluster Randomised Controlled Trial. BMJ 2011, 343, d6195. [Google Scholar] [CrossRef]
- Sadeghi, B.; Kaiser, L.L.; Schaefer, S.; Tseregounis, I.E.; Martinez, L.; Gomez-Camacho, R.; de la Torre, A. Multifaceted Community-Based Intervention Reduces Rate of BMI Growth in Obese Mexican-Origin Boys. Pediatr. Obes. 2017, 12, 247–256. [Google Scholar] [CrossRef]
- Rush, E.; Reed, P.; McLennan, S.; Coppinger, T.; Simmons, D.; Graham, D. A School-Based Obesity Control Programme: Project Energize. Two-Year Outcomes. Br. J. Nutr. 2012, 107, 581–587. [Google Scholar] [CrossRef] [PubMed]
- Bock, F.D.; Breitenstein, L.; Fischer, J.E. Positive Impact of a Pre-School-Based Nutritional Intervention on Children’s Fruit and Vegetable Intake: Results of a Cluster-Randomized Trial. Public Health Nutr. 2012, 15, 466–475. [Google Scholar] [CrossRef]
- Fitzgibbon, M.L.; Stolley, M.R.; Schiffer, L.; Van Horn, L.; KauferChristoffel, K.; Dyer, A. Hip-Hop to Health Jr. for Latino Preschool Children. Obesity (Silver Spring) 2006, 14, 1616–1625. [Google Scholar] [CrossRef]
- Fitzgibbon, M.L.; Stolley, M.R.; Schiffer, L.A.; Braunschweig, C.L.; Gomez, S.L.; Van Horn, L.; Dyer, A.R. Hip-Hop to Health Jr. Obesity Prevention Effectiveness Trial: Postintervention Results. Obesity (Silver Spring) 2011, 19, 994–1003. [Google Scholar] [CrossRef]
- Kong, A.; Buscemi, J.; Stolley, M.R.; Schiffer, L.A.; Kim, Y.; Braunschweig, C.L.; Gomez-Perez, S.L.; Blumstein, L.B.; Van Horn, L.; Dyer, A.R.; et al. Hip-Hop to Health Jr. Randomized Effectiveness Trial: 1-Year Follow-up Results. Am. J. Prev. Med. 2016, 50, 136–144. [Google Scholar] [CrossRef] [PubMed]
- Nemet, D.; Geva, D.; Eliakim, A. Health Promotion Intervention in Low Socioeconomic Kindergarten Children. J. Pediatr. 2011, 158, 796–801.e1. [Google Scholar] [CrossRef]
- Waters, E.; de Silva-Sanigorski, A.; Hall, B.J.; Brown, T.; Campbell, K.J.; Gao, Y.; Armstrong, R.; Prosser, L.; Summerbell, C.D. Interventions for Preventing Obesity in Children. Cochrane Database Syst. Rev. 2011, CD001871. [Google Scholar] [CrossRef]
- Oakes, J.M.; Rossi, P.H. The Measurement of SES in Health Research: Current Practice and Steps toward a New Approach. Soc. Sci. Med. 2003, 56, 769–784. [Google Scholar] [CrossRef]
- The Condition of Education—Glossary. Available online: https://nces.ed.gov/programs/coe/glossary.asp (accessed on 15 June 2019).
- WHO. Commission on Social Determinants of Health (Report); World Health Organization: Geneva, Switzerland, 2008; Available online: https://www.who.int/social_determinants/thecommission/finalreport/en/ (accessed on 15 June 2019).
- Serving Vulnerable and Underserved Populations. 130p. Available online: https://marketplace.cms.gov/technical-assistance-resources/training-materials/vulnerable-and-underserved-populations.pdf (accessed on 15 June 2019).
- Reid, K.W.; Vittinghoff, E.; Kushel, M.B. Association between the Level of Housing Instability, Economic Standing and Health Care Access: A Meta-Regression. J. Health Care Poor Underserved 2008, 19, 1212–1228. [Google Scholar] [CrossRef] [PubMed]
- Farrow, C.V.; Blissett, J. Controlling Feeding Practices: Cause or Consequence of Early Child Weight? Pediatrics 2007, 121, e164–e169. [Google Scholar] [CrossRef] [PubMed]
- Addessi, E.; Galloway, A.T.; Visalberghi, E.; Birch, L.L. Specific Social Influences on the Acceptance of Novel Foods in 2–5-Year-Old Children. Appetite 2005, 45, 264–271. [Google Scholar] [CrossRef] [PubMed]
- Ash, T.; Agaronov, A.; Young, T.; Aftosmes-Tobio, A.; Davison, K.K. Family-Based Childhood Obesity Prevention Interventions: A Systematic Review and Quantitative Content Analysis. Int. J. Behav. Nutr. Phys. Act. 2017, 14, 113. [Google Scholar] [CrossRef] [PubMed]
- Ling, J.; Robbins, L.B.; Wen, F. Interventions to Prevent and Manage Overweight or Obesity in Preschool Children: A Systematic Review. Int. J. Nurs. Stud. 2016, 53, 270–289. [Google Scholar] [CrossRef] [PubMed]
- Bleich, S.N.; Vercammen, K.A.; Zatz, L.Y.; Frelier, J.M.; Ebbeling, C.B.; Peeters, A. Interventions to Prevent Global Childhood Overweight and Obesity: A Systematic Review. Lancet Diabetes Endocrinol. 2018, 6, 332–346. [Google Scholar] [CrossRef]
- Skouteris, H.; McCabe, M.; Swinburn, B.; Newgreen, V.; Sacher, P.; Chadwick, P. Parental Influence and Obesity Prevention in Pre-Schoolers: A Systematic Review of Interventions. Obes. Rev. 2011, 12, 315–328. [Google Scholar] [CrossRef] [PubMed]
- Faith, M.S.; Scanlon, K.S.; Birch, L.L.; Francis, L.A.; Sherry, B. Parent-Child Feeding Strategies and Their Relationships to Child Eating and Weight Status. Obes. Res. 2004, 12, 1711–1722. [Google Scholar] [CrossRef] [PubMed]
- Rao, M.; Afshin, A.; Singh, G.; Mozaffarian, D. Do Healthier Foods and Diet Patterns Cost More than Less Healthy Options? A Systematic Review and Meta-Analysis. BMJ Open 2013, 3, e004277. [Google Scholar] [CrossRef]
- McDermott, A.J.; Stephens, M.B. Cost of Eating: Whole Foods Versus Convenience Foods in a Low-Income Model. Fam. Med. 2010, 42, 280–284. [Google Scholar]
- Ogden, C.L.; Lamb, M.M.; Carroll, M.D.; Flegal, K.M. Obesity and Socioeconomic Status in Children and Adolescents: United States, 2005–2008. NCHS Data Brief 2010. [Google Scholar] [CrossRef]
- Freedman, D.S.; Mei, Z.; Srinivasan, S.R.; Berenson, G.S.; Dietz, W.H. Cardiovascular Risk Factors and Excess Adiposity Among Overweight Children and Adolescents: The Bogalusa Heart Study. J. Pediatr. 2007, 150, 12–17.e2. [Google Scholar] [CrossRef]
- Falbe, J.; Cadiz, A.A.; Tantoco, N.K.; Thompson, H.R.; Madsen, K.A. Active and Healthy Families: A Randomized Controlled Trial of a Culturally Tailored Obesity Intervention for Latino Children. Acad. Pediatr. 2015, 15, 386–395. [Google Scholar] [CrossRef]
- Juckett, G. Caring for Latino Patients. AFP 2013, 87, 48–54. [Google Scholar]
- Crawford, P.B.; Gosliner, W.; Anderson, C.; Strode, P.; Becerra-Jones, Y.; Samuels, S.; Carroll, A.M.; Ritchie, L.D. Counseling Latina Mothers of Preschool Children about Weight Issues: Suggestions for a New Framework. J. Am. Diet. Assoc. 2004, 104, 387–394. [Google Scholar] [CrossRef] [PubMed]
- Lindsay, A.C.; Sussner, K.M.; Greaney, M.L.; Peterson, K.E. Latina Mothers’ Beliefs and Practices Related to Weight Status, Feeding, and the Development of Child Overweight. Public Health Nurs. 2011, 28, 107–118. [Google Scholar] [CrossRef] [PubMed]
- Tovar, A.; Renzaho, A.M.N.; Guerrero, A.D.; Mena, N.; Ayala, G.X. A Systematic Review of Obesity Prevention Intervention Studies among Immigrant Populations in the US. Curr. Obes. Rep. 2014, 3, 206–222. [Google Scholar] [CrossRef] [PubMed]
| Reference | Country | Study Design | Sample Size | Population (age) | Follow-Up | Components | Intervention Target Population | Outcomes |
|---|---|---|---|---|---|---|---|---|
| Successful interventions | ||||||||
| Coen et al. 2011 [13] | Belgium | Cluster-RCT in six communities paired by SES 31 schools Intervention group: 18 Control group: 13 | 1589 | Ages 3–6 years old | 2 years | Nutrition, PA, Screen time, | Children, Community, Schools (teachers), Parents | Primary outcome: BMI z-score |
| Burgi et al. 2012 [17] | Switzerland | Cluster-RCT 40 preschools Intervention: 20 schools Control: 20 schools | 652 | Socially disadvantaged—preschoolers (72% migrant, 38% low EL for parents), average age 5.2 ± 0.6 years | 1 year | PA, Nutrition, Sleep, Media use, | Children, Teachers, Parents | Primary outcomes: %BF, WC Secondary outcome: Aerobic fitness |
| Fitzgibbon et al. 2013 [18] | Chicago, United States | Cluster-RCT 4 schools randomized into WCI (intervention, 2 schools) or GHI (control, 2 schools) | 146 | Hispanic children (low income minority), 3–5 years old | 14 weeks intervention. 1 year follow-up. | Nutrition, PA | Children, Parents | Primary outcomes: BMI, BMI z-score |
| Fitzgibbon et al. 2005 [19] | Chicago, United States | RCT | 420 | Average age: 4 years | 2 years | Nutrition, PA, Media Use, | Children, Parents | Primary outcome: BMI Secondary outcome: Calories from saturated fat |
| Jouret et al. 2009 [20] | France | RCT 79 kindergarten (schools) randomized into two intervention groups: EPIPOI-1 group EPIPOI-2 group. Control data retrieved by the Division of School Health | 1780 | 3–4 years old, 5–6 years old | 2 years | Nutrition, PA, Media Use, | Children, Teachers, Parents, Physicians at the school | Primary outcome: BMI z-score |
| Kaufman-Shriqui et al. 2016 [21] | Israel | RCT 16 schools randomized into intervention group (11 schools; IArm) control group (5 schools; CArm) | 258 | Low SES school children, ages 4–7 years | 6 months | Nutrition, PA | Children, Mothers, Teachers to make healthy choices in a SES area. | Primary outcome: BMI z-score Secondary outcomes: food variety, habitual water drinking, fruit and vegetable intake, sugar sweetened beverage intake, overall packed lunch score, screen time |
| Puder et al. 2011 [22] | Switzerland | RCT single-blinded 40 preschools; randomization of classes 1:1 | 652 | 4–6 years old in high migrant populations | 1 school year | PA, Nutrition, Media use, Sleep, Environment, | Children, Parents, Teachers, School Curriculum, Class environment | Primary outcomes: %BF, sum of skinfolds, WC. Secondary outcomes: motor agility, PA, nutrition habits, media use, aerobic fitness |
| Sadeghi et al. 2016 [23] | California, United States | Quasi-experimental intervention Intervention and comparison community | 422 | Children from Mexican origin communities, 3–8 years old | 3 years | Nutrition, PA, Economic, | Children, Community, Parents, Schools | Primary outcomes: BMI, skin fold thickness, WC |
| Rush et al. 2012 [24] | New Zealand | RCT 124 schools were randomized with stratification by SES and rurality to either the intervention (n = 62) or control group (n = 62) | 1926 | 5 years old | 2 years | PA, nutrition | Children, Teachers, Graduates or PE teachers, Parents, Local community | Primary outcomes: %BF |
| Inconclusive Interventions | ||||||||
| Davis et al. 2016 [12] | New Mexico, United States | Cluster RCT Intervention group: 8 centers Comparison group: 8 centers | 1816 | American Indian and Hispanics, 4 years of age or younger | 2 school years | Nutrition, PA, Behavior, change, Policy change | Children, Teachers, Health care providers, Food service staff, Parents | Primary outcomes: BMI |
| Bock et al. 2011 [25] | Germany | RCT Children were randomized into intervention group (n = 10) or waiting-list control arm (n = 8). Control received same intervention six months later | 377 | 3–6 years old | 1 year | Nutrition | Children, Parents | Secondary outcomes: fruit and vegetable intake |
| Fitzgibbon et al. 2011 [27] | Chicago, United States | RCT 18 schools randomized into either TD-WCI intervention or TD-GHI control groups | 618 | African American children, 3–5 years old | 14 weeks | PA, Nutrition | Children, Teachers, Parents | Secondary outcomes: PA, screen time |
| Kong et al. 2016 [28] | Chicago, United States | RCT 18 schools randomized into either TD-WCI intervention or TD-GHI control groups | 618 | Primarily African American children, 3–5 years old | 1 year | Nutrition, PA | Children, Parents, Teachers | Secondary outcomes: diet quality, screen time |
| Nemet et al. 2011 [29] | Israel | RCT | 725 | 3.8–6.8 years old | 1 school year | Nutrition, PA | Children, Parents | Secondary outcomes: PA, nutrition knowledge, fitness improvement |
| Null Interventions | ||||||||
| Fitzgibbon et al. 2006 [26] | Chicago, United States | RCT 12 schools randomized into intervention or control group | 420 | Latino children, 3–5 years old | 2 years | Nutrition, PA | Children, Parents | No outcomes |
| Reference | Intervention/Study Name 1 | Theoretical Framework | Detailed Description of Intervention | Detailed Description of Results |
|---|---|---|---|---|
| Successful interventions | ||||
| Coen et al. 2011 [13] | POP (Prevention of Overweight among Pre-school and school children) | Socioecological model of health | Community: Two intervention meetings were held in each community that provided brochures and information about local health topics. Schools: Schools received seven modules that described how to implement the intervention effectively. Schools were advised to designate five “healthy weeks” per intervention year with an hour of class time each week for extracurricular healthy activities (i.e., tasting vegetables), improve their playground, revise snack policies, and communicate/distribute educational materials to parents. Parents: Parents were given a poster with target messages and key points to help them encourage healthy behavior with their children. They were also given five letters describing, in detail, the intervention topics with tips, tricks, and recipes that they can try with their children. Lastly, they received a report of their child’s food intake, such as fruits and vegetable intake, as well as PA and screen time with ways they can make improvements. | No significant effects in BMI z-score occurred in the total sample, but there was a statistically significant decrease of 0.11 in BMI z-score in the low SES intervention group (p = 0.01) compared to their pair low SES control group (BMI increased by 0.04 (F = 6.26, p = 0.01)). No significant effects on consumption of water, milk, vegetables, soft drinks, fruits, sweet and savory snacks, PA, or screen time. |
| Burgi et al. 2012 [17] | Ballabeina study | N/A | Culturally tailored intervention Children: PA program 4 days/week for 45 min/session. Sessions aimed to increase aerobic fitness and coordination. Each had themes, such as Spiderman. Health promoters and teachers led the sessions. Twenty-two lessons on nutrition, screen time, and sleep in addition to healthy snacks were given to the students. Teachers: Attended two three-hour workshops to learn the content they will be teaching and share experiences. They received hands on training from health promoters. Parents: Attended three informative sessions discussing PA promotion, nutrition, screen time, and sleep. Informative brochures, worksheets, and exercises were handed out that preschoolers brought home. These handouts were translated in 10 different languages. | Children of migrant/non-migrant parents: Both migrant/non-migrant preschoolers benefitted from the intervention. Both groups had a significant change in %BF (−1.42%; p = 0.013 for non-migrants; −1.14%; p = 0.015 for migrants) and waist circumference (−0.86 cm, p = 0.01 for non-migrants; −1.02 cm; p = 0.003 for migrants). Aerobic fitness change was more significant in non-migrant preschoolers compared to migrant preschoolers, while agility changes were only significant in migrant groups. Specifically, preschoolers of African descent improved their aerobic fitness the most (p = 0.02). Children of low EL parents: Low EL children did not benefit from the intervention as much as middle/high EL parents’ children (differences were only borderline significant: p for interaction ≥0.2 for adiposity and agility; p for interaction = 0.06 for aerobic fitness) except for waist circumference (middle/high EL p = 0.004; low EL p = 0.017). No significant effects in the BMI z-score occurred in the total sample. No effects between SES, BMI, and behavior. |
| Fitzgibbon et al. 2013 [18] | Hip Hop to Health | Social cognitive theory, self-determination theory, health belief model | 14-week intervention led by bilingual educators. Children: Intervention included 20 min nutrition lesson/20 min aerobic PA. To enhance the original intervention, a Spanish language CD was handed out to supplement the material. Control group received one intervention/week (20 min) that consisted of dental health, calling 911, and seat belt safety. Parents: Parent intervention still included educational handouts on nutrition and PA geared toward lower income Hispanics. Parents of preschoolers received 90-min classes (60 min discussion on nutrition and 30-min PA time) | BMI and BMI z-score were significantly lower in both groups after one-year follow-up. The difference between groups was statistically significant for BMI change adjusted for different covariates including BMI at baseline (0.22 kg/m2 (0.02–0.041); p < 0.005) MVPA and accelerometer counts/min were higher in intervention group than in control group, but the difference was not statistically significant. No difference between screen time in intervention (3.4 (0.5) h/day at follow-up) and control group (3.3 (0.5) h/day at follow-up). No significant differences in diet in intervention or control group. |
| Fitzgibbon et al. 2005 [19] | Hip Hop to Health Jr. | N/A | 14-week intervention led by teachers Children: Intervention included a 20-min lesson that focused on healthy eating or an exercise concept, followed by 20 min of PA. The lessons incorporated hand puppets to teach the food pyramid, “go and grow” foods and reducing tv viewing. PA sessions included a 5-min warm-up, 10 min of aerobic activity, and 5 min of warm-down. Children in the control group received a 20-min lesson for 14 weeks on general health concepts. Parents: Weekly newsletters were sent home that addressed the children’s curriculum and included a homework assignment. Assignments were made to reinforce concepts in the newsletter. $5 grocery coupon was given for each assignment they finished. EX: Keep track of your child’s fruit and vegetable intake for one week and think of ways you can increase your family’s fruit and vegetable intake. | Intervention group had significant smaller increases in BMI than the control group at the one-year follow up (CI −0.91 to −0.14) and two-year follow-up (CI −0.98 to −0.10). Intervention group also demonstrated a difference in calories from saturated fat at the one-year follow-up compared to the control group (11.6% vs. 12.8%; p = 0.002). |
| Jouret et al. 2009 [20] | Epidemiologie et prevention de l’obesite’ infantile, EPIPOI | N/A | Children: Three groups that children were put into: EPIPOI-1, EPIPOI-2, and control. EPIPOI-1 that followed “basic strategy”, which gave an overview of weight and health; and EPIPOI-2 received basic strategy and reinforced strategy (education program to target healthy nutrition, PA, and less screen time). Ten 20-min sessions (5 sessions/year) were given to the children. They incorporated activities/games that aimed to gain knowledge about the food groups, eating balanced meals, having breakfast, limiting sugar-sweetened beverages, drinking water, and increasing PA. Kids received a cassette and story book to reinforce the messages. Parents: Parents were provided information to enhance what the students were learning in the classroom. | BMI z-score were lower in both intervention (change EPIPOI-1: 0.35 (0.19; 1.04); change EPIPOI-2: 0.50 (0.17; 1.01) groups compared to control (change in control: 1.35 (0.57; 1.82); EPIPOI-1 vs. control p < 0.001; EPIPOI-2 vs. control p < 0.001) in underprivileged areas but no difference between intervention groups. |
| Kaufman-Shriqui et al. 2016 [21] | Intervention in Israel | N/A | IArm: received nutrition intervention and PA Carm: PA only. Children: All lessons were delivered by clinical dietitians, PA teachers, and economists that specialize with budget planning. Main themes were discussing healthy affordable nutrition, nutrition recommendations (increase fruits/vegetables, water intake, legumes, and decrease high fat, sugar, and sweet beverages), and how to pack healthy lunches. Increasing PA. Mothers and children received lessons structured around these themes in addition to children receiving 10, 45-min weekly lessons given by dietitians. Lectures, stories, games, and songs were utilized to enforce learning. All children received 15 weeks of PA for 45 min/session. Parents: Parents in intervention group attended meetings that were centered around low SES nutrition options and how to pack healthy lunches. IArm teachers received special training to enhance the intervention (teachers were trained to compliment students who brought in healthy lunches). | BMI z-score decreased in the entire study population by 0.1 (p = 0.003). Intervention group showed a greater increase in food variety, habitual water drinking, fruit and vegetable intake and a decrease in sugar-sweetened beverage. Overall packed lunch score improved significantly in intervention group (decrease in non-healthy snacks/sweetened beverages, and an increase in fruits and vegetables) (p < 0.001). Consumption of water increased in Iarm group (p = 0.02). Average PA time decreased more from baseline in control group than in intervention group (−0.42 ± 0.01 h (−18.4%), −0.21 ± 0.01 h (−8.4%)). Mean screen time increased in both groups but significantly more in control group. Nutrition knowledge increased significantly in intervention group by 16% at month three and 39% at month six. |
| Puder et al. 2011 [22] | Ballabeina study | N/A | Culturally tailored intervention Children: Participated in four 45-min PA sessions/week, which targeted aerobic fitness by playing games (taught by exercise physiologist). Health promoters (exercise physiologists) taught one PA session/week in the beginning and then reduced to twice/month while teachers taught the remaining sessions. Twenty-two lessons on nutrition, media use, and sleep were taught. The lessons were based on the five recommendations of the Swiss Society of Nutrition (drink water, eat fruits and vegetables, eat regularly, make clever choices, and turn your screen off when you eat). Children received funny cards about PA or nutrition every other week to take home. CDs were also created to support PA time. Healthy snacks were promoted as well as stickers were posted in the classroom that enhanced the intervention. Teachers: Attended two workshops before the intervention started. They received all materials for the lessons in advance. They learned how to lead the PA session by hands-on training by the health promoters in advance. Parents: Attended three meetings that discussed the importance of PA, nutrition, screen time, and sleep. Materials to enhance the topics were provided, such as brochures. Handouts were offered in 10 different languages. Environmental factors: School environment was adapted to promote PA. Movement corners in classrooms were provided, such as hammocks, balls, cords, climbing walls. A poster of the “Ballabeina track” was hung in the classroom that included the themes and stickers to track their progress. Control group: no intervention. One 45-min PA lesson once/week plus one discussion for the parents. | No different in BMI compared to controls (p = 0.31), but intervention group showed a reduction by 5% in BF (−1.1%, −2.0 to −0.2; p = 0.02),10% in sum of skinfolds (−2.78 mm (−4.35 to −1.2)), and 2% waist circumference F, (−1.0 cm, −1.6 to −0.4; p = 0.001). Intervention group also demonstrated improved motor agility (p = 0.004), but not improved balance. Beneficial effects were also seen in PA, nutrition habits, and media use. Significant increase in aerobic fitness in intervention group compared to the control group (p = 0.01). |
| Sadeghi et al. 2016 [23] | Ninos Sanos, Familia Sana (NSFS) intervention | Social cognitive theory, health belief model | Nutrition: Education was delivered to parents during “family nights” and to the children during school hours. Nutrition lessons consisted of skill building and parenting skills through interactive methods. A nutrition educator delivered the materials to the parents and planned a different topic each month. Ten sessions were offered, but only 5 were mandatory for parents. Teachers delivered the nutrition lessons to the children during school time. The lessons were based on UCCE curriculum, which included “Reading across MyPyramid.” PA: PA sessions were integrated with sport play and active recreation for kids (SPARK) in addition to the original PE curriculum. Originally teachers instructed PE, but with the intervention, the school hired a PE teacher. Teachers were provided with SPARK materials (CDs, binders, equipment). Lessons lasted 20–30 min. Preschool teachers gave lessons daily. Economic: Designed to encourage nutritious foods that are budget friendly. Modeled after WIC. Families received $25 vouchers that could only be used to purchase fruits and vegetables. | Girls: triceps skin fold thickness increased significantly in control than intervention (p = 0.05). No other significant change within the first year of intervention. Intervention was successful as reducing the change in BMI from baseline in boys who were obese only (ß-coefficient = −1.94, p = 0.05). Boys in intervention group demonstrated a small decrease in waist circumference (ß-coefficient = −5.2, p = 0.04) compared to the comparison group. |
| Rush et al. 2012 [24] | Project Energize | N/A | Children: Classes included games, fitness activities, ball activities, and sports-related games to keep the kids moving. They also promoted lunchtime games, bike days, and leadership training so that students could lead a PA session before and after school. Healthy-eating initiatives were also enforced, such as removing pastry-based pies and big cookies in the schools and adding fruit, low-fat yogurt, and filled rolls. Fund raising included selling water and non-food items instead of baked goods and sugary sweets. Teachers also taught lessons, such as why drinking water/milk instead of sugary drinks are important and how to pack healthy lunches/snacks on a budget. Parents: A school newsletter was sent out every week with a “nutrition nugget” that was featured. They included 30 smart swaps (replacing instant noodles with baked beans etc.) and discussing what are “every day,” “sometimes”, and “occasional” foods. A home-school link program was established for parents to attend 45-min sessions that highlighted healthy dietary choices. They received laminated cards and magnets that reinforced nutrition goals. Assistance was provided to parents, teachers, and local community by organizing activities with dietitians and professional development leaders to discuss nutrition. Control group did not receive resources. | BF% standard deviation score was improved in 5–7-year old (effect of the intervention −0.14 (−0.26, −0.01), p = 0.03). However, the statistically significant difference disappears after adjusting by cluster. The effects of the intervention occurred more in rural and schools with higher SES (although they were not statistically significant; p = 0.08). |
| Inconclusive interventions | ||||
| Davis et al. 2016 [12] | Child Health Initiative for Lifelong Eating and Exercise (CHILE) intervention | N/A | Intervention occurred at 16 different Head Start centers in rural American Indian and Hispanic communities that focused on six components: At least 30 min of PA daily and time to taste new vegetables, development training for staff, integrating policy and behavior change with food preparation staff, take home materials for the family, grocery store component to increase availability of healthier food options; and ask local healthcare providers to emphasize healthy eating and OA during routine patient visits. | At the end of the intervention period, no significant difference in BMI in the intervention and comparison groups were found. Values were almost the same. |
| Bock et al. 2011 [25] | ‘Come aboard the health boat’ intervention in Germany | Theory of social learning | Nutrition experts gave the intervention in 2-h sessions, 15 times. These sessions occurred once a week over six months during preschool hours. Five of the sessions involved parents, which focused on the nutritional needs of their children. Activities conducted with the children included eating meals together as a class, teachers, and parents, addressing healthy drinking behaviors, playing with pirate dolls who enjoyed eating fruits and vegetables, and trying new healthy foods. | No significant effects on BMI, WTHR, or skinfold. In the subgroups of overweight and obese children (n 18 with pre- and post-term measurements), bivariate analyses also showed no significant effect of the intervention on BMI, WTHR and skinfold sum (data was not shown). There was a significant difference in the pre and post intervention fruit and vegetable intake (increase from 0.17 at baseline on a 6-point ordinal scale to 0.22 points post intervention, p < 0.001 and p < 0.05 respectively). Post intervention produced a change in vegetable consumption (p = 0.027). No significant effects on water intake and high-energy drinks. |
| Fitzgibbon et al. 2011 [27] | Hip-Hop to Health Jr. obesity prevention | Social cognitive theory, self-determination theory | Children: Childhood educators taught either a 14-week PA and nutrition intervention program (twice per week) or a general health. Each intervention session had a theme that included a 20-min lesson on PA and nutrition and a 20 min physical activity session. Lessons included the pyramid puppets, which represented the seven different food groups. PA sessions included songs and raps that had scripted exercise routines. Parents: Parents received educational handouts that corresponded with their child’s health homework. $5 incentive was given to parents for each homework assignment completed and returned. They were also given the same PA CD that the teachers play for the preschoolers, so they could implement PA at home. | No significant differences between groups in BMI post intervention. No difference in TV watching between groups and in diet (energy intake, dietary fat, consumption of fruits or vegetables). Preschoolers in the intervention group engaged in more moderate and vigorous PA than preschoolers in control school (p = 0.02) and had less total screen time than control group (p = 0.01). |
| Kong et al. 2016 [28] | Hip-Hop to Health Jr. | N/A | Eighteen schools were randomized into two groups: a teacher-delivered intervention curriculum or a teacher-delivered general health curriculum. Children: Intervention curriculum targeted PA, diet, and decreased TV time. Delivered two times/week for 14 weeks. Sessions were theme based with a 20-min lesson on healthy eating or PA and a 20-min session with a PA component. CDs were given out to families and also used in the classroom. In food-themed lessons, the children helped prepare snacks and took part in food tastings. The difference between other Hip-Hop to Health interventions was that there was a modification to lesson frequency. Teachers were allowed to present the lessons twice/week instead of thrice/week. The third lesson per week was now optional and reinforced the content learned during the week instead of introducing new material. The PA portion was led by the teacher with the guidance of the CD. Parents: Parents still had the same home assignments (completing and turning in homework assignments with kids and receiving the same PA CD). | BMI z-score change was not significantly different after intervention between the two groups (p = 0.83). TV viewing time did not change post intervention. Fruit consumption and overall diet quality in intervention group remained the same but decreased in control group. Significant between group differences include whole fruit (p = 0.02), total fruit (p = 0.003), SoFAAS (p = 0.02), and whole grains (p = 0.02). Between group difference for fruit/day was 0.35 servings/day (SE = 0.14, p = 0.02). Although, HEI-2005 scores worsened in the control group, which suggest that early intervention might improve diet quality over a longer period of time. Screen time was reduced in intervention group but was not sustained throughout the year follow-up. A limitation to the intervention was that teachers did not deliver the intervention with as much intensity as the research team. Specifically, the PA portion was not consistent because the teachers themselves were not as active and it was a challenge to teach PA. |
| Nemet et al. 2011 [29] | “It fits me” intervention in Israel | N/A | Intervention lasted one school-year. Children: Nutrition lessons were modeled after the nutrition program “It Fits Me” from the Israeli Ministry of Education. Topics taught included healthy food choices, vitamins, food preparation, cooking methods, and fast food vs. home-cooked meals. Children were then asked to talk about what they learned with their parents. PA sessions were 45 min/day, six days/week. Five sessions were taught by preschool teachers and one session was taught by a professional youth coach. Children were then encouraged to increase PA after school and decrease sedentary activities. CD’s with songs were often used to enhance the nutrition and PA lessons. Control group continued the regular school curriculum. Parents: Monthly flyers were sent home to reinforce material, which also encouraged discussion time with their children about what they have been learning in class. Parents and their children attended two “healthy day festivals” that focused on the intervention themes. Parents and children participated in activities and parents also had the option to attend lectures by the study team. | No differences in BMI, but nutrition knowledge and preferences, PA knowledge and preferences, and fitness improvement all increased (p < 0.05). At the end of the school year there was a larger decrease in overweight children in the intervention group (−31.9%) compared to the control group (−17.5%). |
| Null interventions | ||||
| Fitzgibbon et al. 2006 [26] | Hip-Hop to Health Jr. | Social cognitive theory, self-determination theory | A 14-week (3 sessions/week) intervention consisting of diet and PA. Each session included 20 min of food pyramid education with hand puppets and 20 min of aerobic activity. The intervention targeted decreased fat intake, increase fruit/vegetable intake, decreased sedentary behavior, and increased PA. Delivered in Spanish and English. Parents received weekly educational letters that enhanced the child’s curriculum and homework assignments that were turned in for monetary compensation. | No differences in BMI and BMI z-score from baseline to post intervention (p = 0.56). No significant differences between saturated fat/fiber consumption. No significant differences in PA or screen time. |
© 2019 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Luybli, M.; Schmillen, H.; Sotos-Prieto, M. School-Based Interventions in Low Socioeconomic Settings to Reduce Obesity Outcomes among Preschoolers: A Scoping Review. Nutrients 2019, 11, 1518. https://doi.org/10.3390/nu11071518
Luybli M, Schmillen H, Sotos-Prieto M. School-Based Interventions in Low Socioeconomic Settings to Reduce Obesity Outcomes among Preschoolers: A Scoping Review. Nutrients. 2019; 11(7):1518. https://doi.org/10.3390/nu11071518
Chicago/Turabian StyleLuybli, Megan, Hanna Schmillen, and Mercedes Sotos-Prieto. 2019. "School-Based Interventions in Low Socioeconomic Settings to Reduce Obesity Outcomes among Preschoolers: A Scoping Review" Nutrients 11, no. 7: 1518. https://doi.org/10.3390/nu11071518
APA StyleLuybli, M., Schmillen, H., & Sotos-Prieto, M. (2019). School-Based Interventions in Low Socioeconomic Settings to Reduce Obesity Outcomes among Preschoolers: A Scoping Review. Nutrients, 11(7), 1518. https://doi.org/10.3390/nu11071518





