Socioeconomic Inequalities in the Retail Food Environment around Schools in a Southern European Context
Abstract
1. Introduction
2. Materials and Methods
2.1. Study Design and Sample
2.2. Neighborhood-Level Socioeconomic Status
2.3. Food Environment Assessment
2.4. Population Density
2.5. Statistical Analysis
3. Results
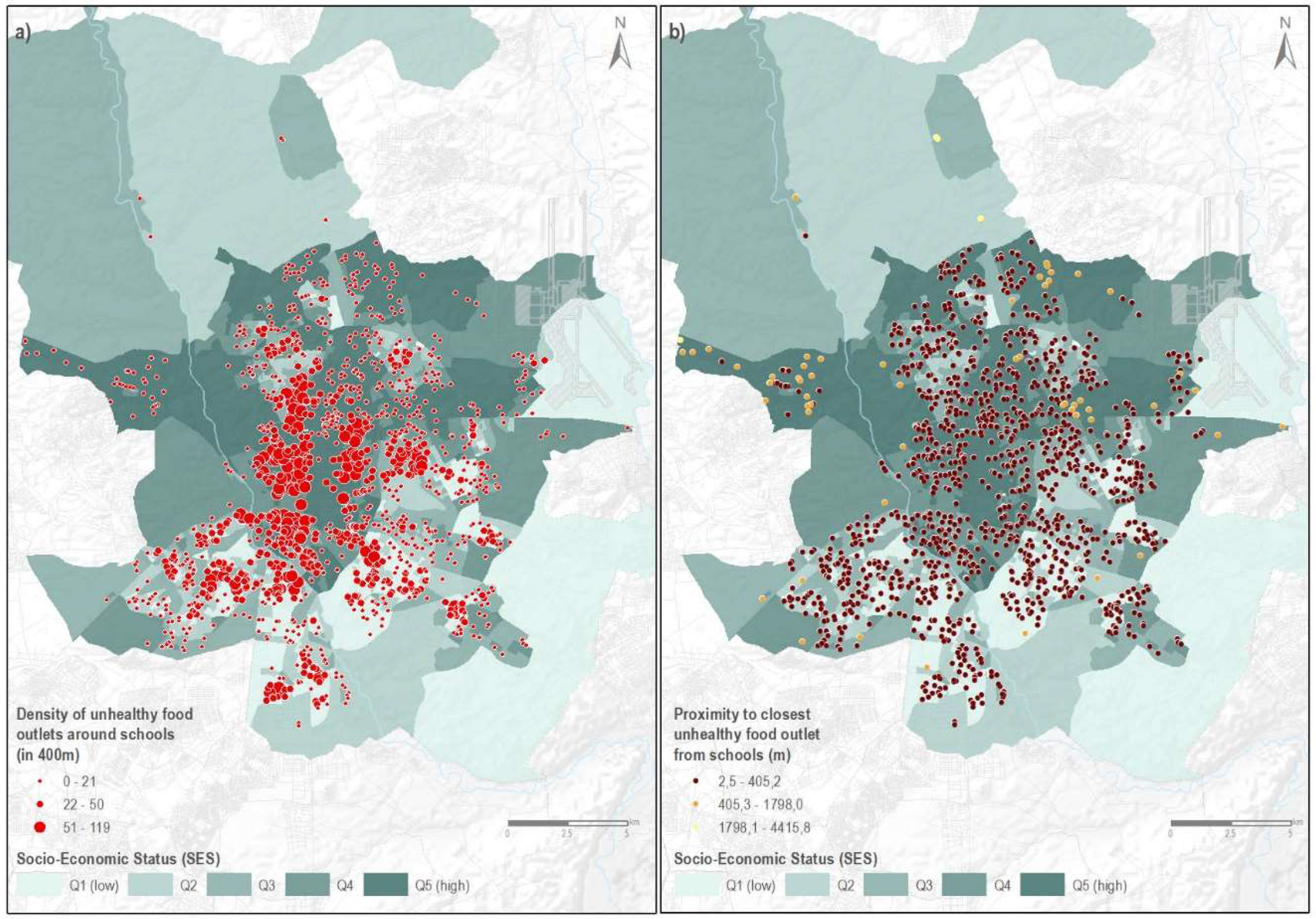
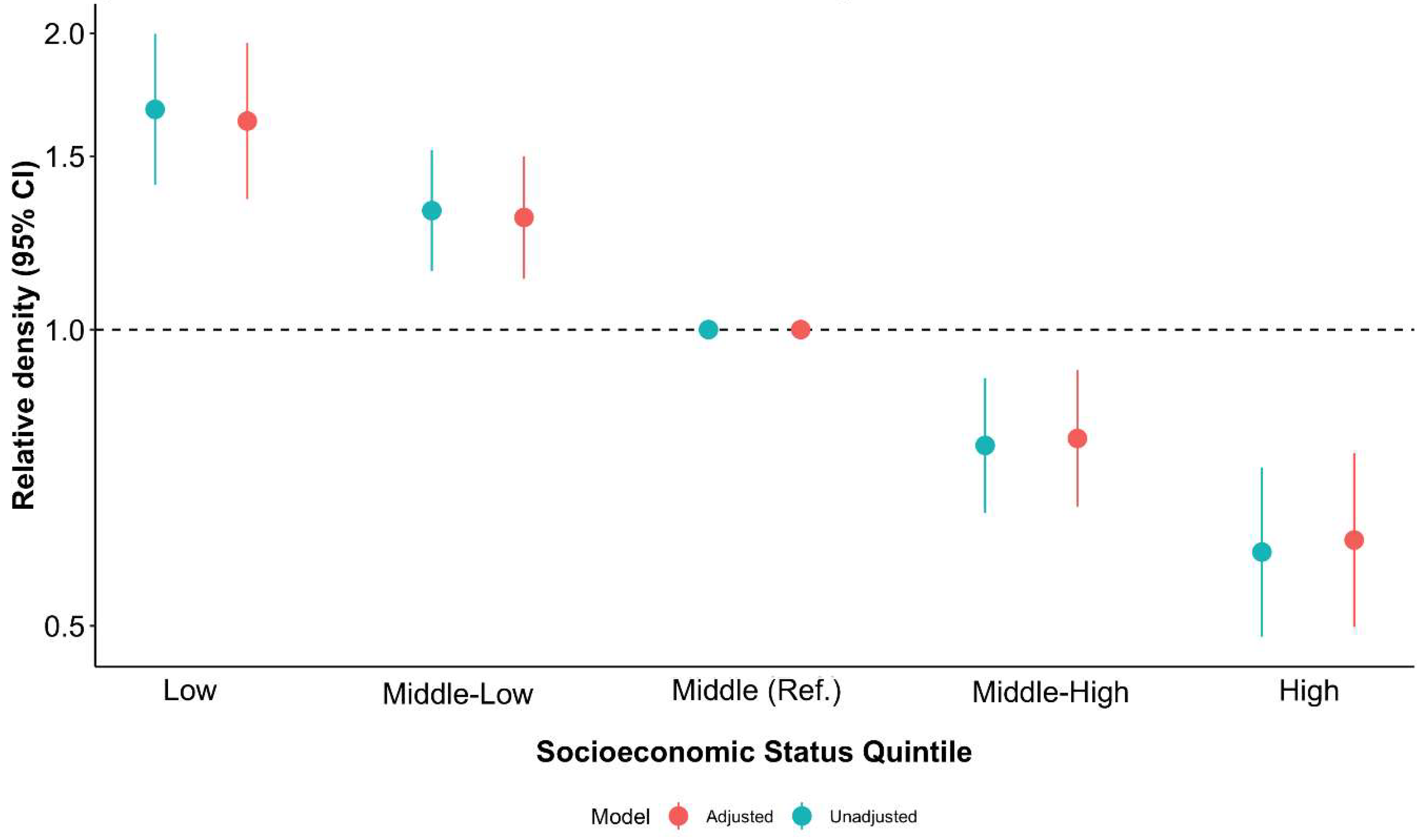
3.1. Counts of Unhealthy Food Outlets and Neighborhood-level SES
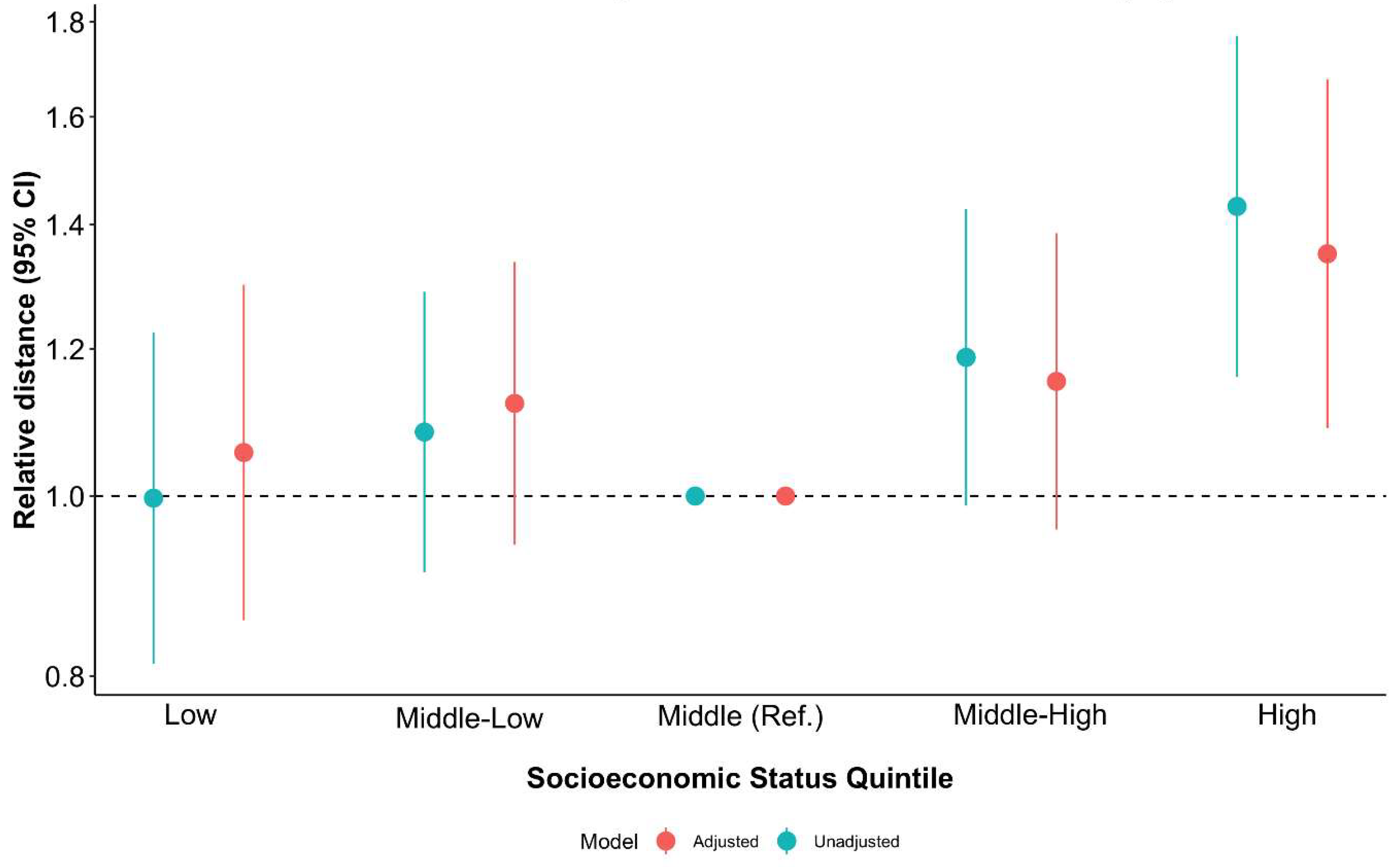
3.2. Distance to the Nearest Unhealthy Outlet and Neighborhood-Level SES
4. Discussion
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Conflicts of Interest
References
- Swinburn, B.A.; Kraak, V.I.; Allender, S.; Atkins, V.J.; Baker, P.I.; Bogard, J.R.; Brinsden, H.; Calvillo, A.; De Schutter, O.; Devarajan, R.; et al. The Global Syndemic of Obesity, Undernutrition, and Climate Change: The Lancet Commission report. Lancet 2019, 393, 791–846. [Google Scholar] [CrossRef]
- Abarca-Gómez, L.; Abdeen, Z.A.; Hamid, Z.A.; Abu-Rmeileh, N.M.; Acosta-Cazares, B.; Acuin, C.; Adams, R.J.; Aekplakorn, W.; Afsana, K.; Aguilar-Salinas, C.A.; et al. Worldwide trends in body-mass index, underweight, overweight, and obesity from 1975 to 2016: A pooled analysis of 2416 population-based measurement studies in 128·9 million. Lancet 2017, 390, 2627–2642. [Google Scholar] [CrossRef]
- Ahrens, W.; Pigeot, I.; Pohlabeln, H.; De Henauw, S.; Lissner, L.; Molnár, D.; Moreno, L.A.; Tornaritis, M.; Veidebaum, T.; Siani, A. Prevalence of overweight and obesity in European children below the age of 10. Int. J. Obes. 2014, 38, S99–S107. [Google Scholar] [CrossRef] [PubMed]
- Lien, N.; Henriksen, H.B.; Nymoen, L.L.; Wind, M.; Klepp, K.-I. Availability of data assessing the prevalence and trends of overweight and obesity among European adolescents. Public Health Nutr. 2010, 13, 1680–1687. [Google Scholar] [CrossRef] [PubMed]
- Ministerio de Salud, Consumo y Bienestar Social. Escuesta Nacional de Salud 2017. Available online: https://www.mscbs.gob.es/estadEstudios/estadisticas/encuestaNacional/encuesta2017.htm (accessed on 23 May 2019).
- Owen, C.G.; Whincup, P.H.; Orfei, L.; Chou, Q.-A.; Rudnicka, A.R.; Wathern, A.K.; Kaye, S.J.; Eriksson, J.G.; Osmond, C.; Cook, D.G. Is body mass index before middle age related to coronary heart disease risk in later life? Evidence from observational studies. Int. J. Obes. 2009, 33, 866–877. [Google Scholar] [CrossRef] [PubMed]
- Park, M.H.; Falconer, C.; Viner, R.M.; Kinra, S. The impact of childhood obesity on morbidity and mortality in adulthood: A systematic review. Obes. Rev. 2012, 13, 985–1000. [Google Scholar] [CrossRef] [PubMed]
- Birch, L.L.; Fisher, J.O. Development of eating behaviors among children and adolescents. Pediatrics 1998, 101, 539–549. [Google Scholar] [PubMed]
- Swinburn, B.A.; Sacks, G.; Hall, K.D.; McPherson, K.; Finegood, D.T.; Moodie, M.L.; Gortmaker, S.L. The global obesity pandemic: Shaped by global drivers and local environments. Lancet 2011, 378, 804–814. [Google Scholar] [CrossRef]
- Story, M.; Kaphingst, K.M.; Robinson-O’Brien, R.; Glanz, K. Creating Healthy Food and Eating Environments: Policy and Environmental Approaches. Annu. Rev. Public Health 2008, 29, 253–272. [Google Scholar] [CrossRef]
- Franco, M.; Bilal, U.; Díez, J. Food Environment. Encycl. Food Health 2016, 4, 22–26. [Google Scholar]
- Glanz, K.; Sallis, J.F.; Saelens, B.E.; Frank, L.D. Healthy Nutrition Environments: Concepts and Measures. Am. J. Health Promot. 2005, 19, 330–333. [Google Scholar] [CrossRef] [PubMed]
- Katz, D.L. School-Based Interventions for Health Promotion and Weight Control: Not Just Waiting on the World to Change. Annu. Rev. Public Health 2009, 30, 253–272. [Google Scholar] [CrossRef] [PubMed]
- Bramante, C.T.; Thornton, R.L.J.; Bennett, W.L.; Zhang, A.; Wilson, R.F.; Bass, E.B.; Tseng, E. Systematic Review of Natural Experiments for Childhood Obesity Prevention and Control. Am. J. Prev. Med. 2019, 56, 147–158. [Google Scholar] [CrossRef] [PubMed]
- Oosterhoff, M.; Joore, M.; Ferreira, I. The effects of school-based lifestyle interventions on body mass index and blood pressure: A multivariate multilevel meta-analysis of randomized controlled trials. Obes. Rev. 2016, 17, 1131–1153. [Google Scholar] [CrossRef] [PubMed]
- Amini, M.; Djazayery, A.; Majdzadeh, R.; Taghdisi, M.H.; Jazayeri, S. Effect of school-based interventions to control childhood obesity: A review of reviews. Int. J. Prev. Med. 2015, 6, 68. [Google Scholar] [PubMed]
- Gittelsohn, J.; Kumar, M.B. Preventing childhood obesity and diabetes: Is it time to move out of the school? Pediatr. Diabetes 2007, 8, 55–69. [Google Scholar] [CrossRef]
- Lucan, S.C. Concerning Limitations of Food-Environment Research: A Narrative Review and Commentary Framed around Obesity and Diet-Related Diseases in Youth. J. Acad. Nutr. Diet. 2015, 115, 205–212. [Google Scholar] [CrossRef]
- Engler-Stringer, R.; Le, H.; Gerrard, A.; Muhajarine, N. The community and consumer food environment and children’s diet: A systematic review. BMC Public Health 2014, 14, 522. [Google Scholar] [CrossRef]
- Timmermans, J.; Dijkstra, C.; Kamphuis, C.; Huitink, M.; van der Zee, E.; Poelman, M. “Obesogenic” School Food Environments? An Urban Case Study in The Netherlands. Int. J. Environ. Res. Public Health 2018, 15, 619. [Google Scholar] [CrossRef]
- Williams, J.; Scarborough, P.; Matthews, A.; Cowburn, G.; Foster, C.; Roberts, N.; Rayner, M. A systematic review of the influence of the retail food environment around schools on obesity-related outcomes. Obes. Rev. 2014, 15, 359–374. [Google Scholar] [CrossRef]
- Vandevijvere, S.; Sushil, Z.; Exeter, D.J.; Swinburn, B. Obesogenic Retail Food Environments Around New Zealand Schools. Am. J. Prev. Med. 2016, 51, e57–e66. [Google Scholar] [CrossRef] [PubMed]
- Nielsen, S. Trends in Food Locations and Sources among Adolescents and Young Adults. Prev. Med. 2002, 35, 107–113. [Google Scholar] [CrossRef] [PubMed]
- Green, M.A.; Radley, D.; Lomax, N.; Morris, M.A.; Griffiths, C. Is adolescent body mass index and waist circumference associated with the food environments surrounding schools and homes? A longitudinal analysis. BMC Public Health 2018, 18, 482. [Google Scholar] [CrossRef] [PubMed]
- Nykiforuk, C.I.J.; Campbell, E.J.; Macridis, S.; McKennitt, D.; Atkey, K.; Raine, K.D. Adoption and diffusion of zoning bylaws banning fast food drive-through services across Canadian municipalities. BMC Public Health 2018, 18, 137. [Google Scholar] [CrossRef] [PubMed]
- Greater London Authority The London Plan, The Spatial Development Strategy for Greater London; Greater London Authority: London, UK, 2017.
- Franco, M.; Sanz, B.; Otero, L.; Domínguez-Vila, A.; Caballero, B. Prevention of childhood obesity in Spain: A focus on policies outside the health sector. SESPAS report 2010. Gac. Sanit. 2010, 24, 49–55. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Neira, M.; de Onis, M. Preventing obesity: A public health priority in Spain. Lancet 2005, 365, 1386. [Google Scholar] [CrossRef]
- Monroy-Parada, D.X.; Jácome-González, M.L.; Moya-Geromini, M.Á.; Rodríguez-Artalejo, F.; Royo-Bordonada, M.Á. Adherence to nutritional recommendations in vending machines at secondary schools in Madrid (Spain), 2014–2015. Gac. Sanit. 2018, 32, 459–465. [Google Scholar] [CrossRef]
- Zenk, S.N.; Powell, L.M. US secondary schools and food outlets. Health Place 2008, 14, 336–346. [Google Scholar] [CrossRef]
- Flavián, C.; Haberberg, A.; Polo, Y. Food retailing strategies in the European union. A comparative analysis in the UK and Spain. J. Retail. Consum. Serv. 2002, 9, 125–138. [Google Scholar] [CrossRef]
- Pettinger, C.; Holdsworth, M.; Gerber, M. “All under one roof?” Differences in food availability and shopping patterns in Southern France and Central England. Eur. J. Public Health 2008, 18, 109–114. [Google Scholar] [CrossRef][Green Version]
- Diez, J.; Bilal, U.; Cebrecos, A.; Buczynski, A.; Lawrence, R.S.; Glass, T.; Escobar, F.; Gittelsohn, J.; Franco, M. Understanding differences in the local food environment across countries: A case study in Madrid (Spain) and Baltimore (USA). Prev. Med. 2016, 89, 237–244. [Google Scholar] [CrossRef] [PubMed]
- Bilal, U.; Díez, J.; Alfayate, S.; Gullón, P.; Del Cura, I.; Escobar, F.; Sandín, M.; Franco, M. Population cardiovascular health and urban environments: The Heart Healthy Hoods exploratory study in Madrid, Spain. BMC Med. Res. Methodol. 2016, 16, 104. [Google Scholar] [CrossRef] [PubMed]
- Cebrecos, A.; Domínguez-Berjón, M.F.; Duque, I.; Franco, M.; Escobar, F. Geographic and statistic stability of deprivation aggregated measures at different spatial units in health research. Appl. Geogr. 2018, 95, 9–18. [Google Scholar] [CrossRef]
- Gullón, P.; Bilal, U.; Cebrecos, A.; Badland, H.M.; Galán, I.; Franco, M. Intersection of neighborhood dynamics and socioeconomic status in small-area walkability: The Heart Healthy Hoods project. Int. J. Health Geogr. 2017, 16, 21. [Google Scholar] [CrossRef] [PubMed]
- Bilal, U.; Hill-Briggs, F.; Sánchez-Perruca, L.; Del Cura-González, I.; Franco, M. Association of neighbourhood socioeconomic status and diabetes burden using electronic health records in Madrid (Spain): The Heart Healthy Hoods study. BMJ Open 2018, 8, e021143. [Google Scholar] [CrossRef] [PubMed]
- Borrell, C.; Malmusi, D.; Muntaner, C. Introduction to the “Evaluating the Impact of Structural Policies on Health Inequalities and Their Social Determinants and Fostering Change” (SOPHIE) Project. Int. J. Health Serv. 2017, 47, 10–17. [Google Scholar] [CrossRef]
- Bilal, U.; Jones-Smith, J.; Diez, J.; Lawrence, R.S.; Celentano, D.D.; Franco, M. Neighborhood social and economic change and retail food environment change in Madrid (Spain): The heart healthy hoods study. Health Place 2018, 51, 107–117. [Google Scholar] [CrossRef]
- Eurostat Statistical Classification of Economic Activities in the European Community; Eurostat: Luxembourg, 2008.
- Zuniga-Teran, A.A.; Orr, B.J.; Gimblett, R.H.; Chalfoun, N.V.; Marsh, S.E.; Guertin, D.P.; Going, S.B. Designing healthy communities: Testing the walkability model. Front. Archit. Res. 2017, 6, 63–73. [Google Scholar] [CrossRef]
- Elbel, B.; Tamura, K.; McDermott, Z.T.; Duncan, D.T.; Athens, J.K.; Wu, E.; Mijanovich, T.; Schwartz, A.E. Disparities in food access around homes and schools for New York City children. PLoS ONE 2019, 14, e0217341. [Google Scholar] [CrossRef]
- Neckerman, K.M.; Bader, M.D.M.; Richards, C.A.; Purciel, M.; Quinn, J.W.; Thomas, J.S.; Warbelow, C.; Weiss, C.C.; Lovasi, G.S.; Rundle, A. Disparities in the Food Environments of New York City Public Schools. Am. J. Prev. Med. 2010, 39, 195–202. [Google Scholar] [CrossRef]
- Mackenbach, J.D.; Charreire, H.; Glonti, K.; Bárdos, H.; Rutter, H.; Compernolle, S.; De Bourdeaudhuij, I.; Nijpels, G.; Brug, J.; Oppert, J.-M.; et al. Exploring the Relation of Spatial Access to Fast-food outlets with Body Weight: A Mediation Analysis. Environ. Behav. 2018. [Google Scholar] [CrossRef]
- Bader, M.D.M.; Schwartz-Soicher, O.; Jack, D.; Weiss, C.C.; Richards, C.A.; Quinn, J.W.; Lovasi, G.S.; Neckerman, K.M.; Rundle, A.G. More neighborhood retail associated with lower obesity among New York City public high school students. Health Place 2013, 23, 104–110. [Google Scholar] [CrossRef] [PubMed]
- Lamb, K.E.; Thornton, L.; Cerin, E.; Ball, K. Statistical Approaches Used to Assess the Equity of Access to Food Outlets: A Systematic Review. AIMS Public Health 2015, 2, 358–401. [Google Scholar] [CrossRef] [PubMed]
- Thornton, L.E.; Cameron, A.J.; McNaughton, S.A.; Waterlander, W.E.; Sodergren, M.; Svastisalee, C.; Blanchard, L.; Liese, A.D.; Battersby, S.; Carter, M.-A.; et al. Does the availability of snack foods in supermarkets vary internationally? Int. J. Behav. Nutr. Phys. Act. 2013, 10, 56. [Google Scholar] [CrossRef] [PubMed]
- Charlton, E.L.; Kähkönen, L.A.; Sacks, G.; Cameron, A.J. Supermarkets and unhealthy food marketing: An international comparison of the content of supermarket catalogues/circulars. Prev. Med. 2015, 81, 168–173. [Google Scholar] [CrossRef] [PubMed]
- Bivoltsis, A.; Cervigni, E.; Trapp, G.; Knuiman, M.; Hooper, P.; Ambrosini, G.L. Food environments and dietary intakes among adults: Does the type of spatial exposure measurement matter? A systematic review. Int. J. Health Geogr. 2018, 17, 19. [Google Scholar] [CrossRef] [PubMed]
- Pearson, N.; Biddle, S.J.H.; Gorely, T. Family correlates of fruit and vegetable consumption in children and adolescents: A systematic review. Public Health Nutr. 2009, 12, 267–283. [Google Scholar] [CrossRef]
- Van der Horst, K.; Oenema, A.; Ferreira, I.; Wendel-Vos, W.; Giskes, K.; van Lenthe, F.; Brug, J. A systematic review of environmental correlates of obesity-related dietary behaviors in youth. Health Educ. Res. 2006, 22, 203–226. [Google Scholar] [CrossRef]
- Rasmussen, M.; Krølner, R.; Klepp, K.I.; Lytle, L.; Brug, J.; Bere, E.; Due, P. Determinants of fruit and vegetable consumption among children and adolescents: A review of the literature. Part I: Quantitative studies. Int. J. Behav. Nutr. Phys. Act. 2006, 3, 22. [Google Scholar] [CrossRef]
- Verloigne, M.; Van Lippevelde, W.; Maes, L.; Brug, J.; De Bourdeaudhuij, I. Family- and school-based correlates of energy balance-related behaviours in 10–12-year-old children: A systematic review within the ENERGY (European Energy balance Research to prevent excessive weight Gain among Youth) project. Public Health Nutr. 2012, 15, 1380–1395. [Google Scholar] [CrossRef]
- Ball, K.; Timperio, A.; Crawford, D. Neighbourhood socioeconomic inequalities in food access and affordability. Health Place 2009, 15, 578–585. [Google Scholar] [CrossRef] [PubMed]
- Smith, D.; Cummins, S.; Clark, C.; Stansfeld, S. Does the local food environment around schools affect diet? Longitudinal associations in adolescents attending secondary schools in East London. BMC Public Health 2013, 13, 70. [Google Scholar] [CrossRef] [PubMed]
- Shier, V.; An, R.; Sturm, R. Is there a robust relationship between neighbourhood food environment and childhood obesity in the USA? Public Health 2012, 126, 723–730. [Google Scholar] [CrossRef] [PubMed]
- An, R.; Maurer, G. Consumption of sugar-sweetened beverages and discretionary foods among US adults by purchase location. Eur. J. Clin. Nutr. 2016, 70, 1396. [Google Scholar] [CrossRef] [PubMed]
- Howard Wilsher, S.; Harrison, F.; Yamoah, F.; Fearne, A.; Jones, A. The relationship between unhealthy food sales, socio-economic deprivation and childhood weight status: Results of a cross-sectional study in England. Int. J. Behav. Nutr. Phys. Act. 2016, 13, 21. [Google Scholar] [CrossRef] [PubMed]
- Machado, P.P.; Claro, R.M.; Martins, A.P.B.; Costa, J.C.; Levy, R.B. Is food store type associated with the consumption of ultra-processed food and drink products in Brazil? Public Health Nutr. 2018, 21, 201–209. [Google Scholar] [CrossRef] [PubMed]
- Güsewell, S.; Floris, J.; Berlin, C.; Zwahlen, M.; Rühli, F.; Bender, N.; Staub, K. Spatial Association of Food Sales in Supermarkets with the Mean BMI of Young Men: An Ecological Study. Nutrients 2019, 11, 579. [Google Scholar] [CrossRef] [PubMed]
- Macintyre, S. Deprivation amplification revisited; or, is it always true that poorer places have poorer access to resources for healthy diets and physical activity? Int. J. Behav. Nutr. Phys. Act. 2007, 4, 32. [Google Scholar] [CrossRef]
- Thornton, L.E.; Lamb, K.E.; Ball, K. Fast food restaurant locations according to socioeconomic disadvantage, urban–regional locality, and schools within Victoria, Australia. SSM-Popul. Health. 2016, 2, 1–9. [Google Scholar] [CrossRef]
- Soltero, E.G.; Ortiz Hernández, L.; Jauregui, E.; Lévesque, L.; Lopez, Y.; Taylor, J.; Barquera, S.; Lee, R.E. Characterization of the School Neighborhood Food Environment in Three Mexican Cities. Ecol. Food Nutr. 2017, 56, 139–151. [Google Scholar] [CrossRef]
- Villanueva, R.; Albaladejo, R.; Astasio, P.; Ortega, P.; Santos, J.; Regidor, E. Socio-economic environment, area facilities and obesity and physical inactivity among children. Eur. J. Public Health 2016, 26, 267–271. [Google Scholar] [CrossRef] [PubMed]
- Díez, J.; Bilal, U.; Franco, M. Unique features of the Mediterranean food environment: Implications for the prevention of chronic diseases Rh: Mediterranean food environments. Eur. J. Clin. Nutr. 2018, 28, 1. [Google Scholar] [CrossRef] [PubMed]
- Thornton, L.E.; Cameron, A.J.; McNaughton, S.A.; Worsley, A.; Crawford, D.A. The availability of snack food displays that may trigger impulse purchases in Melbourne supermarkets. BMC Public Health 2012, 12, 194. [Google Scholar] [CrossRef] [PubMed]
- Battersby, J.; Peyton, S. The Geography of Supermarkets in Cape Town: Supermarket Expansion and Food Access. Urban Forum 2014, 25, 153–164. [Google Scholar] [CrossRef]
- Cutumisu, N.; Traoré, I.; Paquette, M.-C.; Cazale, L.; Camirand, H.; Lalonde, B.; Robitaille, E. Association between junk food consumption and fast-food outlet access near school among Quebec secondary-school children: Findings from the Quebec Health Survey of High School Students (QHSHSS) 2010–11. Public Health Nutr. 2017, 20, 927–937. [Google Scholar] [CrossRef] [PubMed]
- Virtanen, M.; Kivimäki, H.; Ervasti, J.; Oksanen, T.; Pentti, J.; Kouvonen, A.; Halonen, J.I.; Kivimäki, M.; Vahtera, J. Fast-food outlets and grocery stores near school and adolescents’ eating habits and overweight in Finland. Eur. J. Public Health 2015, 25, 650–655. [Google Scholar] [CrossRef]
- Baek, J.; Sanchez-Vaznaugh, E.V.; Sánchez, B.N. Hierarchical Distributed-Lag Models: Exploring Varying Geographic Scale and Magnitude in Associations between the Built Environment and Health. Am. J. Epidemiol. 2016, 183, 583–592. [Google Scholar] [CrossRef]
- Sturm, R.; Hattori, A. Diet and obesity in Los Angeles County 2007–2012: Is there a measurable effect of the 2008 “Fast-Food Ban”? Soc. Sci. Med. 2015, 133, 205–211. [Google Scholar] [CrossRef]
- Gittelsohn, J.; Rowan, M.; Gadhoke, P. Interventions in small food stores to change the food environment, improve diet, and reduce risk of chronic disease. Prev. Chronic Dis. 2012, 9, E59. [Google Scholar] [CrossRef]
- Calancie, L.; Leeman, J.; Jilcott Pitts, S.B.; Khan, L.K.; Fleischhacker, S.; Evenson, K.R.; Schreiner, M.; Byker, C.; Owens, C.; McGuirt, J.; et al. Nutrition-Related Policy and Environmental Strategies to Prevent Obesity in Rural Communities: A Systematic Review of the Literature, 2002–2013. Prev. Chronic Dis. 2015, 12, 140540. [Google Scholar] [CrossRef]
| Characteristics | Availability | Distance | ||
|---|---|---|---|---|
| Median (IQR) 1 | p-Value 2 | Median (IQR) 1 | p-Value 2 | |
| Type of school | 0.0037 | 0.0011 | ||
| Preschools | 16 (8–31) | 82 (48.10–151.85) | ||
| Primary schools | 18 (9–36) | 90.07 (57.93–141.01) | ||
| Secondary schools | 17 (8–35) | 100.80 (55.21–171.13) | ||
| Funding | 0.0001 | 0.0001 | ||
| Public | 16 (9–29) | 100.78 (62.40–153.68) | ||
| Private | 14 (5–31) | 90.41 (47.61–188.85) | ||
| Concerted | 23 (12–44) | 74.16 (48.22–126.77) | ||
| Neighborhood-level SES | 0.0001 | 0.0001 | ||
| Low-SES | 24 (13–37) | 77.09 (46.50–129.26) | ||
| Middle-low | 18 (13–30) | 81.35 (54.65–128.57) | ||
| Middle | 16 (8–36) | 77.52 (43.59–127.63) | ||
| Middle-high | 19 (7–43) | 92.01 (52.83–162.77) | ||
| High-SES | 8 (3–16) | 145.92 (77.48–254.71) | ||
| Population density (103 residents/km2) | 0.0001 | 0.0001 | ||
| Low | 22 (13–39) | 71.52 (44.85–125.07] | ||
| Medium | 21 (10–39) | 83.99 (51.85–139.69] | ||
| High | 10 (4–21) | 123.26 (69.24–193.26] | ||
© 2019 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Díez, J.; Cebrecos, A.; Rapela, A.; Borrell, L.N.; Bilal, U.; Franco, M. Socioeconomic Inequalities in the Retail Food Environment around Schools in a Southern European Context. Nutrients 2019, 11, 1511. https://doi.org/10.3390/nu11071511
Díez J, Cebrecos A, Rapela A, Borrell LN, Bilal U, Franco M. Socioeconomic Inequalities in the Retail Food Environment around Schools in a Southern European Context. Nutrients. 2019; 11(7):1511. https://doi.org/10.3390/nu11071511
Chicago/Turabian StyleDíez, Julia, Alba Cebrecos, Alba Rapela, Luisa N. Borrell, Usama Bilal, and Manuel Franco. 2019. "Socioeconomic Inequalities in the Retail Food Environment around Schools in a Southern European Context" Nutrients 11, no. 7: 1511. https://doi.org/10.3390/nu11071511
APA StyleDíez, J., Cebrecos, A., Rapela, A., Borrell, L. N., Bilal, U., & Franco, M. (2019). Socioeconomic Inequalities in the Retail Food Environment around Schools in a Southern European Context. Nutrients, 11(7), 1511. https://doi.org/10.3390/nu11071511







