A Mentor-Led Text-Messaging Intervention Increases Intake of Fruits and Vegetables and Goal Setting for Healthier Dietary Consumption among Rural Adolescents in Kentucky and North Carolina, 2017
Abstract
1. Introduction
2. Materials and Methods
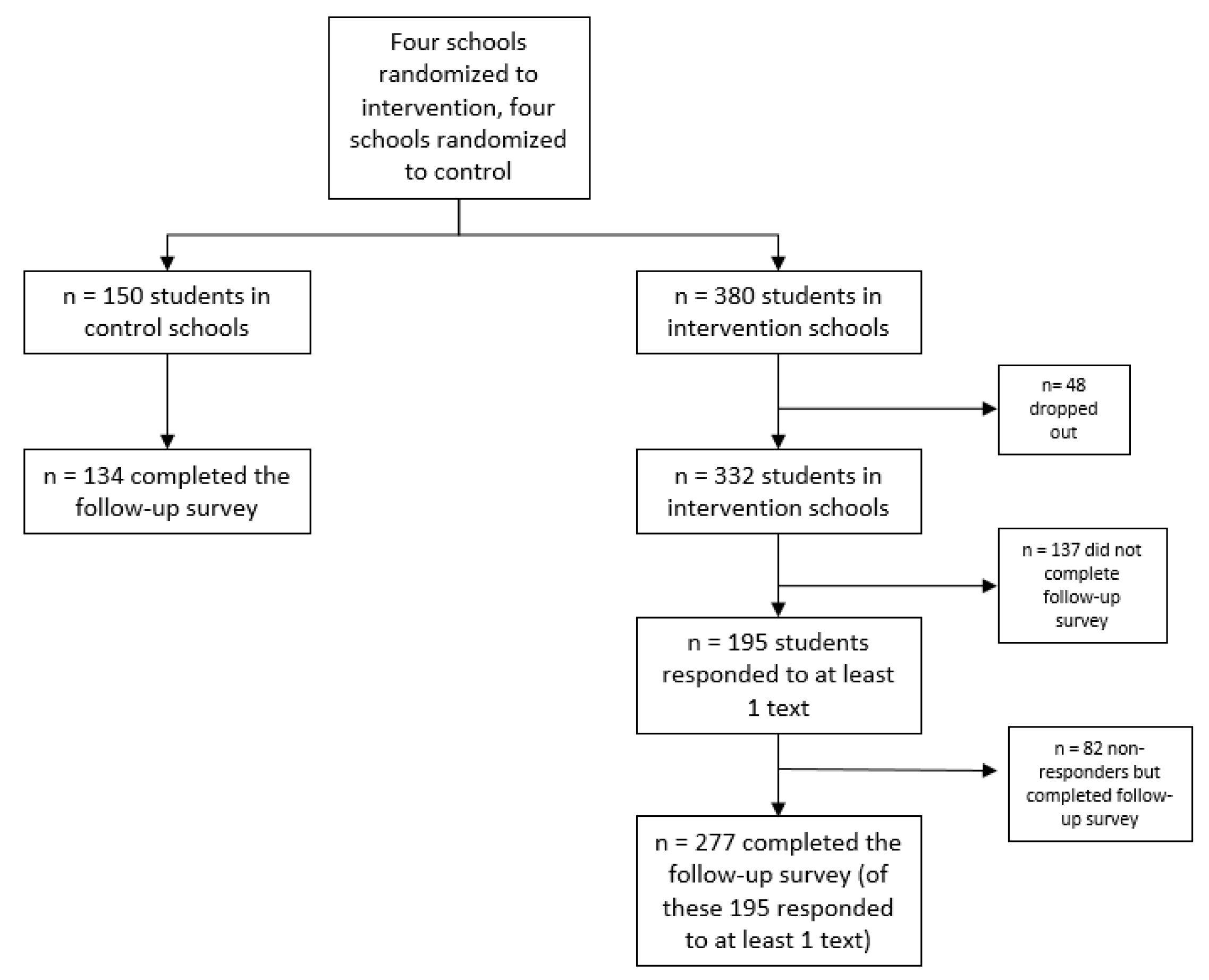
2.1. Recruitment and Randomization of Included High Schools
2.2. Recruitment and Enrollment of High School Students
2.3. “Go Big and Bring it Home” (GBBH) Intervention Components
2.4. Dependent Variables
3. Results
4. Discussion
5. Conclusions
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- Lutfiyya, M.N.; Lipsky, M.S.; Wisdom-Behounek, J.; Inpanbutr-Martinkus, M. Is rural residency a risk factor for overweight and obesity for U.S. Children? Obesity 2007, 15, 2348–2356. [Google Scholar] [CrossRef] [PubMed]
- Johnson, C.M.; Sharkey, J.R.; Dean, W.R. Eating behaviors and social capital are associated with fruit and vegetable intake among rural adults. J. Hunger. Environ. Nutr. 2010, 5, 302–315. [Google Scholar] [CrossRef] [PubMed]
- James, C.V.; Moonesinghe, R.; Wilson-Frederick, S.M.; Hall, J.E.; Penman-Aguilar, A.; Bouye, K. Racial/ethnic health disparities among rural adults—USA, 2012–2015. MMWR Surveill. Summ. 2017, 66, 1. [Google Scholar] [CrossRef] [PubMed]
- Trivedi, T.; Liu, J.; Probst, J.; Merchant, A.; Jhones, S.; Martin, A.B. Obesity and obesity-related behaviors among rural and urban adults in the USA. Rural Remote Health 2015, 15, 3267. [Google Scholar] [PubMed]
- Powell, L.M.; Nguyen, B.T. Fast-food and full-service restaurant consumption among children and adolescents: Effect on energy, beverage, and nutrient intake. JAMA Pediatr. 2013, 167, 14–20. [Google Scholar] [CrossRef] [PubMed]
- Deierlein, A.L.; Galvez, M.P.; Yen, I.H.; Pinney, S.M.; Biro, F.M.; Kushi, L.H.; Teitelbaum, S.; Wolff, M.S. Local food environments are associated with girls' energy, sugar-sweetened beverage and snack-food intakes. Public Health Nutr. 2014, 17, 2194–2200. [Google Scholar] [CrossRef] [PubMed]
- Hebden, L.; Hector, D.; Hardy, L.L.; King, L. A fizzy environment: Availability and consumption of sugar-sweetened beverages among school students. Prev. Med. 2013, 56, 416–418. [Google Scholar] [CrossRef] [PubMed]
- Van de Gaar, V.M.; van Grieken, A.; Jansen, W.; Raat, H. Children's sugar-sweetened beverages consumption: Associations with family and home-related factors, differences within ethnic groups explored. BMC Public Health 2017, 17, 195. [Google Scholar] [CrossRef] [PubMed]
- Bogart, L.M.; Elliott, M.N.; Ober, A.J.; Klein, D.J.; Hawes-Dawson, J.; Cowgill, B.O.; Uyeda, K.; Schuster, M.A. Home sweet home: Parent and home environmental factors in adolescent consumption of sugar-sweetened beverages. Acad. Pediatr. 2017, 17, 529–536. [Google Scholar] [CrossRef] [PubMed]
- Pearson, N.; Biddle, S.J.; Gorely, T. Family correlates of fruit and vegetable consumption in children and adolescents: A systematic review. Public Health Nutr. 2009, 12, 267–283. [Google Scholar] [CrossRef] [PubMed]
- Cole-Lewis, H.; Kershaw, T. Text messaging as a tool for behavior change in disease prevention and management. Epidemiol. Rev. 2010, 32, 56–69. [Google Scholar] [CrossRef] [PubMed]
- Muench, F.; van Stolk-Cooke, K.; Kuerbis, A.; Stadler, G.; Baumel, A.; Shao, S.; McKay, J.R.; Morgenstern, J. A randomized controlled pilot trial of different mobile messaging interventions for problem drinking compared to weekly drink tracking. PLoS ONE 2017, 12, e0167900. [Google Scholar] [CrossRef] [PubMed]
- Suffoletto, B.; Kristan, J.; Chung, T.; Jeong, K.; Fabio, A.; Monti, P.; Clark, D.B. An interactive text message intervention to reduce binge drinking in young adults: A randomized controlled trial with 9-month outcomes. PLoS ONE 2015, 10, e0142877. [Google Scholar] [CrossRef] [PubMed]
- Keating, S.R.; McCurry, M.K. Systematic review of text messaging as an intervention for adolescent obesity. J. Am. Assoc. Nurse Pract. 2015, 27, 714–720. [Google Scholar] [CrossRef] [PubMed]
- Kerr, D.A.; Harray, A.J.; Pollard, C.M.; Dhaliwal, S.S.; Delp, E.J.; Howat, P.A.; Pickering, M.R.; Ahmad, Z.; Meng, X.; Pratt, I.S.; et al. The connecting health and technology study: A 6-month randomized controlled trial to improve nutrition behaviours using a mobile food record and text messaging support in young adults. Int. J. Behav. Nutr. Phys. Act. 2016, 13, 52. [Google Scholar] [CrossRef] [PubMed]
- Hall, A.K.; Cole-Lewis, H.; Bernhardt, J.M. Mobile text messaging for health: A systematic review of reviews. Annu. Rev. Public Health 2015, 36, 393–415. [Google Scholar] [CrossRef] [PubMed]
- Flores Mateo, G.; Granado-Font, E.; Ferre-Grau, C.; Montana-Carreras, X. Mobile phone apps to promote weight loss and increase physical activity: A systematic review and meta-analysis. J. Med. Internet Res. 2015, 17, e253. [Google Scholar] [CrossRef] [PubMed]
- Trude, A.C.B.; Surkan, P.J.; Cheskin, L.J.; Gittelsohn, J. A multilevel, multicomponent childhood obesity prevention group-randomized controlled trial improves healthier food purchasing and reduces sweet-snack consumption among low-income african-american youth. Nutr. J. 2018, 17, 96. [Google Scholar] [CrossRef] [PubMed]
- Ludwig, K.; Arthur, R.; Sculthorpe, N.; Fountain, H.; Buchan, D.S. Text messaging interventions for improvement in physical activity and sedentary behavior in youth: Systematic review. JMIR Mhealth Uhealth 2018, 6, e10799. [Google Scholar] [CrossRef] [PubMed]
- Carfora, V.; Caso, D.; Conner, M. Randomized controlled trial of a messaging intervention to increase fruit and vegetable intake in adolescents: Affective versus instrumental messages. Br. J. Health Psychol. 2016, 21, 937–955. [Google Scholar] [CrossRef] [PubMed]
- Pedersen, S.; Gronhoj, A.; Thogersen, J. Texting your way to healthier eating? Effects of participating in a feedback intervention using text messaging on adolescents' fruit and vegetable intake. Health Educ. Res. 2016, 31, 171–184. [Google Scholar] [CrossRef] [PubMed]
- O'Donnell, S.; Greene, G.W.; Blissmer, B. The effect of goal setting on fruit and vegetable consumption and physical activity level in a web-based intervention. J. Nutr. Educ. Behav. 2014, 46, 570–575. [Google Scholar] [CrossRef] [PubMed]
- Muench, F.; Baumel, A. More than a text message: Dismantling digital triggers to curate behavior change in patient-centered health interventions. J. Med. Internet Res. 2017, 19, e147. [Google Scholar] [CrossRef] [PubMed]
- Gustafson, A.; Jilcott Pitts, S.; McDonald, J.; Ford, H.; Connelly, P.; Gillespie, R.; Liu, E.; Bush, H.; Brancato, C.; Babatande, T.; et al. Direct effects of the home, school, and consumer food environments on the association between food purchasing patterns and dietary intake among rural adolescents in kentucky and north carolina, 2017. Int. J. Environ. Res. Public Health. 2017, 14, 1255. [Google Scholar] [CrossRef] [PubMed]
- Joseph, R.P.; Pekmezi, D.; Dutton, G.R.; Cherrington, A.L.; Kim, Y.I.; Allison, J.J.; Durant, N.H. Results of a culturally adapted internet-enhanced physical activity pilot intervention for overweight and obese young adult african american women. J. Transcult. Nurs. 2016, 27, 136–146. [Google Scholar] [CrossRef] [PubMed]
- Fitzgerald, A.; Heary, C.; Kelly, C.; Nixon, E.; Shevlin, M. Self-efficacy for healthy eating and peer support for unhealthy eating are associated with adolescents' food intake patterns. Appetite 2013, 63, 48–58. [Google Scholar] [CrossRef] [PubMed]
- Greene, G.W.; Resnicow, K.; Thompson, F.E.; Peterson, K.E.; Hurley, T.G.; Hebert, J.R.; Toobert, D.J.; Williams, G.C.; Elliot, D.L.; Goldman Sher, T.; et al. Correspondence of the nci fruit and vegetable screener to repeat 24-h recalls and serum carotenoids in behavioral intervention trials. J. Nutr. 2008, 138, 200S–204S. [Google Scholar] [CrossRef] [PubMed]
- Hedrick, V.E.; Savla, J.; Comber, D.L.; Flack, K.D.; Estabrooks, P.A.; Nsiah-Kumi, P.A.; Ortmeier, S.; Davy, B.M. Development of a brief questionnaire to assess habitual beverage intake (bevq-15): Sugar-sweetened beverages and total beverage energy intake. J. Acad. Nutr. Diet. 2012, 112, 840–849. [Google Scholar] [CrossRef] [PubMed]
- Gustafson, A.; McGladrey, M.; Liu, E.; Peritore, N.; Webber, K.; Butterworth, B.; Vail, A. Examining key stakeholder and community residents' understanding of environmental influences to inform place-based interventions to reduce obesity in rural communities, kentucky 2015. J. Rural Health 2018, 34, 388–395. [Google Scholar] [CrossRef] [PubMed]
- Stata Software; Version 2017; StataCorp LP: College Station, TX, USA, 2017.
- Albani, V.; Butler, L.T.; Traill, W.B.; Kennedy, O.B. Fruit and vegetable intake: Change with age across childhood and adolescence. Br. J. Nutr. 2017, 117, 759–765. [Google Scholar] [CrossRef] [PubMed]
- Harris, C.; Flexeder, C.; Thiering, E.; Buyken, A.; Berdel, D.; Koletzko, S.; Bauer, C.P.; Bruske, I.; Koletzko, B.; Standl, M.; et al. Changes in dietary intake during puberty and their determinants: Results from the giniplus birth cohort study. BMC Public Health 2015, 15, 841. [Google Scholar] [CrossRef] [PubMed]
- Stluka, S.; Moore, L.; Eicher-Miller, H.A.; Franzen-Castle, L.; Henne, B.; Mehrle, D.; Remley, D.; McCormack, L. Voices for food: Methodologies for implementing a multi-state community-based intervention in rural, high poverty communities. BMC Public Health 2018, 18, 1055. [Google Scholar] [CrossRef] [PubMed]
- Shearer, C.; Rainham, D.; Blanchard, C.; Dummer, T.; Lyons, R.; Kirk, S. Measuring food availability and accessibility among adolescents: Moving beyond the neighbourhood boundary. Soc. Sci. Med. 2015, 133, 322–330. [Google Scholar] [CrossRef] [PubMed]
- Verstraeten, R.; Leroy, J.L.; Pieniak, Z.; Ochoa-Aviles, A.; Holdsworth, M.; Verbeke, W.; Maes, L.; Kolsteren, P. Individual and environmental factors influencing adolescents' dietary behavior in low- and middle-income settings. PLoS ONE 2016, 11, e0157744. [Google Scholar] [CrossRef] [PubMed]
- Surkan, P.J.; Coutinho, A.J.; Christiansen, K.; Dennisuk, L.A.; Suratkar, S.; Mead, E.; Sharma, S.; Gittelsohn, J. Healthy food purchasing among african american youth: Associations with child gender, adult caregiver characteristics and the home food environment. Public Health Nutr. 2011, 14, 670–677. [Google Scholar] [CrossRef] [PubMed]
- Nollen, N.L.; Mayo, M.S.; Carlson, S.E.; Rapoff, M.A.; Goggin, K.J.; Ellerbeck, E.F. Mobile technology for obesity prevention: A randomized pilot study in racial- and ethnic-minority girls. Am. J. Prev. Med. 2014, 46, 404–408. [Google Scholar] [CrossRef] [PubMed]
- Kristal, A.R.; Vizenor, N.C.; Patterson, R.E.; Neuhouser, M.L.; Shattuck, A.L.; McLerran, D. Precision and bias of food frequency-based measures of fruit and vegetable intakes. Cancer Epidemiol. Biomarkers Prev. 2000, 9, 939–944. [Google Scholar] [PubMed]
- Miller, T.M.; Abdel-Maksoud, M.F.; Crane, L.A.; Marcus, A.C.; Byers, T.E. Effects of social approval bias on self-reported fruit and vegetable consumption: A randomized controlled trial. Nutr. J. 2008, 7, 18. [Google Scholar] [CrossRef] [PubMed]
| Intervention (n = 277) | Control (n = 134) | ||
|---|---|---|---|
| Age (mean) | 15 (0.07) | 15 (0.10) | p = 0.80 |
| Gender | p = 0.70 | ||
| Female | 61% | 67% | |
| Male | 38% | 30% | |
| Other (Male to Female; Female to Male; Other) | |||
| Race | |||
| White | 72% | 55% | p = 0.01 |
| Other (African American/Hispanic) | 28% | 45% | p = 0.01 |
| Dietary Intake and Body Mass Index | |||
| Fruit and vegetable servings (mean and SE) | 3.83 (0.24) | 5.56 (0.54) | p = 0.01 |
| Sugar-sweetened beverage calories (mean and SE) | 439 (31) | 470 (54) | p = 0.6 |
| Sugar-sweetened beverage grams (mean and SE) | 1112 (79) | 1200 (140) | p = 0.6 |
| BMI Z-score percentile (mean and SE) | 0.76 (0.02) | 0.72 (0.02) | p = 0.9 |
| Food Shopping Practices | p = 0.60 | ||
| Buy fruit and vegetables (mean times per week purchased) | 16 (0.99) | 13 (0.92) | |
| Buy fast food (mean times per week) | 31 (0.99) | 27 (1.26) | |
| Buy healthy snack foods (mean times per week) | 8.74 (0.54) | 6.39 (0.59) | |
| Buy less-healthy snack | 15.88 (0.84) | 13.58 (1.05) | |
| Buy SSB | 10.33 (0.48) | 9.95 (0.68) | |
| Buy water or no-calorie beverages | 5.38 (0.30) | 5.22 (0.40) | |
| Where Food is Purchased | p = 0.07 | ||
| Fruit and Vegetables | |||
| Supermarket | 86% | 98% | |
| Convenience Stores | 13% | 10% | |
| Fast Food | 1% | 4% | |
| Sugar-Sweetened Beverages (regular soda; fruit punch; sports drink; energy drink; sweet tea) | |||
| Supermarket | 83% | 92% | |
| Convenience Stores | 32% | 24% | |
| Fast Food | 27% | 22% | |
| Water or Low-Calorie Beverages (water; flavored water; unsweet tea) | |||
| Supermarket | 78% | 86% | |
| Convenience Stores | 7% | 7% | |
| Fast Food | 15% | 14% | |
| Healthy Snacks (pretzels; low-fat chips; granola bars; nuts/seeds; yogurt) | |||
| Supermarket | 87% | 90% | |
| Convenience Stores | 14% | 13% | |
| Fast Food | 6% | 9% | |
| Less-Healthy Snacks (full-calorie chips; cookies; cakes; donuts; chocolate candy; sugar candy; ice cream; popsicles; snow cones) | |||
| Supermarket | 88% | 90% | |
| Convenience Stores | 28% | 18% | |
| Fast Food | 11% | 12% | |
| Home Availability (Always Available) | |||
| Fruit and Vegetable | 45% | 50% | |
| Vegetables Served at Dinner | 39% | 25% | |
| Junk Food | 31% | 31% | |
| Soda | 36% | 36% | |
| Snacks | 27% | 30% | |
| Candy | 19% | 18% | |
| Core Constructs (I know I can) | |||
| Self-Efficacy | |||
| Choose Fruit | 63% | 51% | |
| Choose Vegetables | 47% | 25% | |
| Choose Healthy Snacks | 53% | 42% | |
| Goal Setting | |||
| Fruit Goal Almost Always | 10% | 10% | |
| Veggie Goal Almost Always | 10% | 8% | |
| Sugar-Free Beverage Goal | 19% | 12% | |
| Level of Engagement | |||
| Text messages returned (mean total messages over eight weeks) | 11.34 (0.73) | N/A | |
| Avid responder (returned at least two messages per week) | 63% | N/A | |
| Dietary Intake and BMI | Change within Intervention Participants | Change within Control Participants | Difference between Intervention and Control Participants Postintervention |
|---|---|---|---|
| Fruit and vegetable servings/day | 0.71 (−0.02, 1.45) | −1.52 (−2.48, −0.56) * | 1.28 (1.11, 1.48) * |
| Sugar-sweetened beverage calories | −61 (−125, 80) * | −39 (−149, 71) | −39 (−164, 85) |
| Total beverage calories | −26 (−139, 87) | −118 (−320, 83) | 14.99 (−186, 216) |
| Body Mass Index Z-score percentile | −0.005 (−0.02, 0.009) | 0.002 (−0.01, 0.02) | 0.99 (0.92, 1.07) |
| Food shopping practices (number of times an item was purchased over 7 days) | |||
| Fruit and vegetable purchases over 7 days | 2.55 (0.69, 4.42) * | 1.39 (−0.65, 3.44) | 1.07 (0.94, 1.22) |
| Less-healthy snack purchases over 7 days | 0.82 (−0.88, 2.53) | −0.18 (−2.13, 1.75) | 1.06 (0.85, 1.33) |
| Healthy snack purchases over 7 days | 1.81 (0.68, 2.94) * | 1.87 (0.54, 3.20) * | 1.02 (0.84, 1.23) |
| SSB beverage purchases over 7 days | 0.26 (−0.71, 1.24) | −0.25 (−1.64, 1.14) | 1.02 (0.85, 1.21) |
| Water or no-calorie beverage purchases | 0.87 (0.18, 1.56) * | 0.36 (−0.58, 1.31) | 1.03 (0.88, 1.21) |
| Home Availability (Percent Change Reported) | |||
| Fruit and vegetables | p = 0.3 | p = 0.02 | p = 0.03 |
| Never | <1% | 7% | |
| Sometimes | 4% | 6% | |
| Always | 5% | −13% | |
| Vegetables served at dinner | p = 0.08 | p = 0.2 | p = 0.03 |
| Never | −2% | −12% | |
| Sometimes | 7% | 11% | |
| Always | −5% | −3% | |
| Junk food | p = 0.008 | p = 0.68 | p = 0.01 |
| Never | 8% | 1% | |
| Sometimes | −4% | 3% | |
| Always | −5% | −4% | |
| Soda | p = 0.07 | p = 0.23 | p = 0.05 |
| Never | 6% | <1% | |
| Sometimes | −3% | 6% | |
| Always | −3% | −6% | |
| Odds Ratio 95% CI | |
|---|---|
| Self-Efficacy | |
| Fruit | 0.93 (0.73, 1.29) |
| Vegetable | 1.59 (1.19, 2.13) * |
| Healthy Snacks | 0.72 (0.48, 1.09) |
| Goal Setting | |
| Fruit | 1.52 (1.18, 1.95) * |
| Vegetable | 1.75 (1.19, 2.58) * |
| Sugar-Free Beverage | 1.94 (1.18, 3.27) * |
© 2019 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Gustafson, A.; Jilcott Pitts, S.B.; McQuerry, K.; Babtunde, O.; Mullins, J. A Mentor-Led Text-Messaging Intervention Increases Intake of Fruits and Vegetables and Goal Setting for Healthier Dietary Consumption among Rural Adolescents in Kentucky and North Carolina, 2017. Nutrients 2019, 11, 593. https://doi.org/10.3390/nu11030593
Gustafson A, Jilcott Pitts SB, McQuerry K, Babtunde O, Mullins J. A Mentor-Led Text-Messaging Intervention Increases Intake of Fruits and Vegetables and Goal Setting for Healthier Dietary Consumption among Rural Adolescents in Kentucky and North Carolina, 2017. Nutrients. 2019; 11(3):593. https://doi.org/10.3390/nu11030593
Chicago/Turabian StyleGustafson, Alison, Stephanie B. Jilcott Pitts, Kristen McQuerry, Oyinlola Babtunde, and Janet Mullins. 2019. "A Mentor-Led Text-Messaging Intervention Increases Intake of Fruits and Vegetables and Goal Setting for Healthier Dietary Consumption among Rural Adolescents in Kentucky and North Carolina, 2017" Nutrients 11, no. 3: 593. https://doi.org/10.3390/nu11030593
APA StyleGustafson, A., Jilcott Pitts, S. B., McQuerry, K., Babtunde, O., & Mullins, J. (2019). A Mentor-Led Text-Messaging Intervention Increases Intake of Fruits and Vegetables and Goal Setting for Healthier Dietary Consumption among Rural Adolescents in Kentucky and North Carolina, 2017. Nutrients, 11(3), 593. https://doi.org/10.3390/nu11030593






